ORIGINAL CONTRIBUTION. Progressive Multifocal Leukoencephalopathy and Relapsing-Remitting Multiple Sclerosis
|
|
|
- Marilyn Rose
- 5 years ago
- Views:
Transcription
1 ORIGINAL CONTRIBUTION Progressive Multifocal Leukoencephalopathy and Relapsing-Remitting Multiple Sclerosis A Comparative Study Aaron Boster, MD; Stephanie Hreha, BS; Joseph R. Berger, MD; Fen Bao, MS; Ramya Penmesta, MS; Alexandros Tselis, MD, PhD; Christina Endress, BS; Imad Zak, MD; Jai Perumal, MD; Christina Caon, MSN, NP-C; Jose Vazquez, MD; Kenneth L. Tyler, MD; Michael K. Racke, MD; Scott Millis, PhD; Omar Khan, MD Objective: To identify clinical and magnetic resonance imaging (MRI) features that distinguish progressive multifocal leukoencephalopathy (PML) from relapsing-remitting multiple sclerosis (RRMS). Design: Retrospective medical record review. Setting: Two urban teaching hospitals in Detroit, Michigan. Patients: Forty-five confirmed PML cases and 100 patients with RRMS. Main Outcome Measures: Clinical and MRI features distinguishing PML from RRMS. Results: Overall, monosymptomatic presentations were more common in multiple sclerosis (MS) than PML (85% vs 47%; P.01). However, patients with PML presented more often with hemiparesis (24% vs 5%; P=.001) and altered mentation (19% vs 0%; P.0001), whereas brainstem (2% vs 18%; P=.007) presentations were more common in patients with RRMS. Spinal cord and optic neuritis presentations were seen in 18% and 33% of patients with RRMS, respectively, but not in patients with PML (P.0001). Brain MRI scans, available in 35 (78%) PML cases, revealed 7 lesion types. Large, confluent T2- weighted lesions (74% vs 2%; P.0001) and deep gray matter lesions (31% vs 7%; P.001) were more frequent in patients with PML than patients with RRMS. Crescentic cerebellar lesions (23% vs 0%; P.001) were seen only in patients with PML. Gadolinium-enhancing (23%), transcallosal (9%), and periventricular (9%) lesions were noted in patients with PML. Brain magnetization transfer ratio (MTR) was low in both PML and MS lesions. However, normal-appearing brain tissue MTR in PML was higher than normal-appearing brain tissue MTR in RRMS (44.15% vs 41.04%; P=.002), suggesting that PML may be relatively more focal than MS. Conclusions: There appear to be differences between the clinical and MRI characteristics of PML and RRMS, which may help distinguish new MS activity from PML. Magnetization transfer ratio studies may provide additional clues in improving early detection of PML in patients with preexisting MS and warrant further investigation. Arch Neurol. 2009;66(5): Author Affiliations are listed at the end of this article. PROGRESSIVE MULTIFOCAL LEUkoencephalopathy (PML) is a demyelinating opportunistic infection of the central nervous system caused by the JC virus (JCV), typically seen in the setting of an immunocompromised host. 1-4 Since the inception of the AIDS pandemic, PML has been chiefly observed in the setting of human immunodeficiency virus (HIV) infection. However, the occurrence of PML in 2 patients with multiple sclerosis (MS) treated with natalizumab (NTZ) 5,6 raised concerns about the appearance of PML in the setting of MS. Natalizumab, a humanized monoclonal antibody against 4 integrin, inhibits the binding of lymphocytes and monocytes to their endothelial receptor, vascular cell adhesion molecule 1, and prevents inflammatory cells from entering into the brain and other tissues. Impaired central nervous system immunosurveillance 7 and the release of B cells from the bone marrow and spleen 8 have been suggested as the underlying mechanisms for the development of PML with NTZ. The risk for developing NTZ-associated PML had been estimated to be 1:1000 after a mean of approximately 18 months of treatment. 9 As of September 2008, approximately patients worldwide have received NTZ, 6600 of whom have been exposed for at least 18 months. 10 Including the 2 most recent cases of PML reported in NTZtreated patients with MS, 11 there have been a total of 5 cases of PML (4 in MS) reported in patients exposed to NTZ. Other therapies that have been proposed for the treatment of MS have also 593
2 Table 1. Patient Demographics and Clinical Presentations PML (n=45) been associated with the risk of PML. This includes rituximab, which demonstrated positive results in a phase 2 relapsing-remitting MS (RRMS) study. 12 However, rituximab has been associated with PML in patients with lymphoproliferative disorders and systemic lupus erythematosus. 13,14 Similarly, other immunosuppressive agents that have been used for MS, including mycophenolate mofetil, methotrexate, azathioprine, and cyclophosphamide, have been associated with PML in the context of rheumatologic disorders or cancer In the aftermath of NTZ-treated patients with RRMS developing PML, criteria to recognize PML and monitor patients with MS undergoing treatment with NTZ have been proposed. 18,19 Therefore, we conducted a study with the primary objective of identifying clinical and magnetic resonance imaging (MRI) characteristics of PML that may assist in distinguishing it from RRMS. We also explored magnetization transfer ratio (MTR) imaging in distinguishing PML from MS as a secondary goal of this study. METHODS The study was approved by the local Human Investigations Committee. We conducted a retrospective medical record review of all PML cases at 2 urban teaching hospitals in Detroit, Michigan, from 1988 to The medical records were queried with the search term progressive multifocal leukoencephalopathy, PML, and the corresponding International Statistical Classification of Diseases and Related Health Problems, Ninth Revision code. Only cases confirmed by either JCV cerebrospinal fluid polymerase chain reaction or tissue diagnosis (brain biopsy or autopsy) were included in our analysis. Demographic and clinical characteristics of all confirmed cases of PML were obtained from hospital medical records. All brain MRI scans (n=35) were reviewed as a group by 4 investigators (A.B., O.K., A.T., and I.Z.) including a neuroradiologist. Brain MRI scans were obtained on 1.0-T (n=4) or 1.5-T (n=31) scanners according to the protocol instituted for clinical scans at the 2 hospitals, which typically included axial % RRMS (n=100) P Value Adjusted P Value a Age, y, mean (SD) 41 (9) 34 (6.8).001 Sex, F/M 22/78 71/ Ethnicity African American White Other 5 3 Monosymptomatic presentation Hemiparesis Altered mental status Brainstem Cerebellar Optic neuritis Acute spinal cord presentation Abbreviations: PML, progressive multifocal leukoencephalopathy; RRMS, relapsing-remitting multiple sclerosis. a Hommel-adjusted P value. T2-weighted, fluid-attenuated inversion recovery (FLAIR), and T1-weighted images. Sagittal T2-weighted or FLAIR images were obtained in all but 6 cases. All scans also included postcontrast T1-weighted images acquired after the intravenous administration of 0.1 mmol/kg of gadolinium. Additionally, in 4 patients with PML, brain magnetic transfer (MT) imaging was performed according to previously published techniques to examine brain MT ratio (MTR), which measures changes reflecting injury to myelin and the axonal membrane. 20,21 Brain MTR was examined globally in the normal-appearing brain tissue (NABT) as well as regionally by placing regions of interest (ROIs) in NABT as well as PML lesions. Clinical and MRI characteristics of the first 100 consecutive patients with clinically definite RRMS from our center database were used as controls for comparison. The patients with RRMS selected as the control group were diagnosed with clinically definite RRMS according to the McDonald criteria 22 and, therefore, more likely to be representative of the current population of patients with newly diagnosed RRMS. Clinical presentations in patients with RRMS were recorded from the onset of initial symptoms. Statistical analysis was performed using the t test, 2, and the Mann-Whitney U test as appropriate with a 95% level of significance. All P values.05 were regarded as statistically significant. Data are quoted as mean (SD) unless otherwise stated. To correct for the multiple comparisons made in our analysis, we applied maximum experimentwise error rate (Hommel method). 23 Adjusted P values are shown in the Tables. RESULTS BASELINE CHARACTERISTICS Of the 128 medical records of suspected PML cases generated from the query, only 45 were confirmed PML cases included in the analysis. Progressive multifocal leukoencephalopathy was confirmed by positive JCV cerebrospinal fluid polymerase chain reaction in 16 cases (36%) and by brain biopsy or autopsy in 29 cases (64%). Demographic data are summarized in Table 1. Fortytwo of 45 cases (93%) were HIV positive. The 3 non- HIV PML cases (7%) included acute myelocytic leukemia, idiopathic CD4 lymphopenia, and monoclonal gammopathy of unknown significance. Patients with PML presented at an older age than the RRMS cohort (mean [SD], 41 [9] years vs 34 [6.8] years; P=.001). More men (78% vs 29%; P.0001) and more African American individuals (69% vs 16%; P.0001) presented with PML compared with the RRMS cohort. NEUROLOGICAL PRESENTATIONS Clinical presentations at onset are summarized in Table 1. Overall, monosymptomatic presentations were more common in RRMS (85% vs 47%; P.01). However, patients with PML presented more often with hemiparesis (24% vs 5%; P=.001) and altered mental status (19% vs 0%; P.0001) than patients with RRMS. Brainstem dysfunction was more common in patients with RRMS than in patients with PML (18% vs 2%; P=.007). Acute spinal cord presentation and optic neuritis occurred in patients with RRMS but not patients with PML (18% vs 0% and 33% vs 0%, respectively; P.0001). Complete or partial recovery was commonly observed in patients with 594
3 RRMS following a relapse; patients with PML demonstrated progression of symptoms without improvement for the duration of available follow-up (data not shown). CONVENTIONAL MRI CHARACTERISTICS Brain MRI scans were available in 35 of 45 PML cases. Seven PML brain MRI lesion patterns were identified (Figure): (1) large, confluent, and granular T2- weighted hyperintense lesions, (2) T2-weighted hyperintense lesions of deep gray matter structures, (3) crescentshaped lesions of the cerebellar hemispheres, (4) gadolinium-enhanced T1-weighted lesions, (5) tumefactive lesions, (6) periventricular white matter lesions, and (7) transcallosal lesions. Compared with patients with RRMS, several brain MRI lesion patterns were seen more commonly in patients with PML (Table 2) including large, confluent, and granular lesions on T2-weighted sequences (74% vs 2%; P.0001), deep gray matter involvement (31% vs 7%; P.0001), and crescent-shaped cerebellar lesions (23% vs 0%; P.001). In contrast, gadolinium-enhanced lesions (23% vs 54%; P=.001) and periventricular white matter lesions (9% vs 89%; P.0001) were seen less commonly in patients with PML than patients with RRMS. Classic Dawson fingers were seen in 61% of RRMS MRI scans compared with only 1 (2.22%) PML MRI scan (P.001). Interestingly, 2 of the 3 PML brain MRI scans that demonstrated periventricular white matter lesions met Barkhof MRI criteria 24 for dissemination in space based on the presence of greater than 9 T2-weighted hyperintense lesions, 3 or more periventricular lesions, and the presence of infratentorial lesions. More than half of the PML scans (19 of 35; 54%) contained 2 or more of the lesion types described in Table 2. BRAIN MTR DATA Brain MTR data were acquired using previously published techniques 20,21 and analyzed in a 3-step manner. First, we examined the average brain MTR values in the PML lesions and compared them with MS lesions in patients with RRMS (Table 3). The average MTR values obtained from 6 PML and 12 RRMS lesions were 35.7% and 36.08%, respectively (P=.72). Second, we examined the MTR values obtained from ROIs placed in the NABT in patients with PML and RRMS. The average MTR obtained from 6 ROIs in NABT in patients with PML was significantly higher than the average MTR obtained from 12 ROIs in patients with RRMS (47.2% vs 41.03%; P=.001). Third, we examined the entire NABT MTR in 4 patients with PML and compared it with 12 patients with RRMS. The average NABT MTR in patients with PML was significantly higher than patients with RRMS (44.15% vs 41.04%; P=.002). COMMENT Many studies have previously described the clinical and MRI characteristics of PML, in both HIV-positive and HIVnegative populations. 1,4,25-28 Cognitive impairment and motor deficits are consistently reported at high frequency. Other presentations, including aphasia and visualspatial disorientation, dysarthria, incoordination, and sensory abnormalities, are commonly described. Symptom onset is reported as subacute to progressive and recovery of deficits is rare. The PML findings on brain MRI scans are described as bilateral, asymmetric subcorticalpredominant lesions that appear hyperintense on T2- weighted and FLAIR sequences and hypointense on T1- weighted sequences. Mass effect is typically absent or mild, but not invariably. When mass effect is observed, it is generally in the context of the immune reconstitution inflammatory syndrome (IRIS). 29,30 Patchy, irregular, peripheral postcontrast enhancement has been observed in up to 10% of HIV-associated PML cases 26 and more often occurs with IRIS Spinal cord and optic nerves are traditionally believed to be spared, although spinal cord abnormalities have been observed at autopsy in PML. 32 Compared with RRMS, PML may have a slower symptom onset with more frequent cognitive and behavioral presentations. Unlike RRMS, PML is generally not considered to include optic nerve or spinal cord involvement. In patients with PML, brain MRI scans may demonstrate larger, more diffuse, and less well-demarcated T2-weighted hyperintense lesions that tend to occupy the juxtacortical areas, with relative sparing of the periventricular region. Compared with the homogeneous or ring enhancement frequently seen in MS lesions, PML lesions enhance less frequently and generally in a sparse peripheral pattern, often in the context of IRIS. Moll and colleagues 33 recently compared pathologic changes in cortical demyelination in patients with PML and MS, finding intracortical and juxtacortical lesions in both but subpial lesions only in MS brains. Clinical characteristics were not compared in the study. In our study, hemiparesis and mental status changes occurred more commonly in PML than RRMS, whereas brainstem dysfunction was less common in PML, consistent with prior observations. Likewise, none of the PML cases in our study presented with a spinal cord syndrome or optic neuritis. Also in accord with prior observations, all PML cases in our study demonstrated disability progression, in contrast to the patients with RRMS, who frequently experienced short-term recovery following a relapse. These clinical findings help confirm differences in clinical presentations of PML and RRMS 18,19 and may provide clues in identifying the development of PML in patients with RRMS. A major focus of our study was to compare brain MRI characteristics of patients with PML and RRMS. We describe 7 patterns of brain MRI lesions in patients with PML. Large, confluent, and granular hyperintense T2- weighted lesions as well as deep gray matter lesions were more commonly seen in patients with PML than patients with RRMS, and crescent-shaped lesions in the cerebellar hemispheres were identified only in patients with PML. This raises the possibility that crescent-shaped cerebellar lesions may represent a unique PML MRI pattern, a finding that requires confirmation in a larger study. Periventricular white matter lesions and Dawson fingers, both common in RRMS, were rarely seen in PML scans. Gadolinium-enhancing lesions were noted in 595
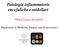
4 A B C D E F G Figure. The 7 identified progressive multifocal leukoencephalopathy brain magnetic resonance imaging lesion patterns. A, Large, confluent, granular T2-weighted lesions (arrows). B, Deep gray matter involvement (arrow). C, Crescent-shaped cerebellar lesion. D, Gadolinium-enhancing lesions (arrow). E, Tumefactive lesion (arrow). F, Multiple sclerosis like appearance. G, Transcallosal lesion (arrow). All brain magnetic resonance images are axial T2-weighted except for part D, which is an axial T1-weighted image acquired after the intravenous administration of gadolinium. 596
5 Table 2. Brain MRI Characteristics in PML and RRMS a MRI Pattern PML (n=35) No. (%) RRMS (n=100) P Value Adjusted P Value b Large, confluent, granular T2-weighted lesions 26 (74) 2 (2) Deep gray matter involvement 11 (31) 7 (7) Crescent cerebellar lesions 8 (23) Gadolinium-enhancing lesions 8 (23) 54 (54) Tumefactive lesions 1 (3) 6 (6) Periventricular white matter lesions 3 (9) 89 (89) Transcallosal 3 (9) 3 (3) Abbreviations: MRI, magnetic resonance imaging; PML, progressive multifocal leukoencephalopathy; RRMS, relapsing-remitting multiple sclerosis. a Classic Dawson fingers lesions were seen in 61% of RRMS MRI brain scans compared with 2.22% of PML MRI brain scans (adjusted P.001). b Hommel-adjusted P value. approximately one-fourth of PML scans. We cannot rule out the possibility that a percentage of the HIV-positive patients with PML had IRIS at the time of their MRI scan, contributing to MRI gadolinium enhancement. However, 2 of the 3 HIV-negative patients with PML also had gadolinium-enhancing lesions. These findings support observations made by Huang et al, 27 suggesting that brain MRI gadolinium enhancement may be seen in HIVnegative patients with PML, cautioning that the presence of gadolinium enhancement should not preclude PML. All but one of the enhancing PML brain lesions in our cohort demonstrated subtle contrast enhancement largely limited to the rim of the lesion. This appearance is quite different than most RRMS lesions, which typically tend to demonstrate a homogeneous pattern of enhancement. 34 One PML lesion did contain an open ring enhancing lesion, similar in appearance to ring-enhancing MS lesions 35 seen in 6% of the RRMS cohort in our study. Magnetization transfer imaging has received considerable attention as a novel imaging technique to detect and quantify microstructural changes associated with myelin tissue and axonal injury. 36 It is based on the exchange of magnetization between protons bound to macromolecules (myelin) and those in free water. This allows the calculation of MTR that reflects the efficiency of such an exchange before and after the application of an offresonance saturation pulse. Low MTR indicates a reduced capacity of the macromolecules in brain tissue to exchange magnetization with the surrounding water molecules, indicative of damage to myelin or to the axonal membrane. Postmortem studies have shown that MTR is strongly associated with the percentage of residual axons and the degree of demyelination both in T2-visible lesions and the NABT. 37 Previously, brain MTR measured from T2-visible PML lesions and the NABT of patients with PML has been shown to be significantly low compared with age-matched controls. 38,39 However, no study has been done comparing the brain MTR of PML with RRMS. We examined MTR of T2-visible lesions as well as NABT in PML and RRMS. Relative to normal tissue, lesions in both disorders demonstrated low MTR values, consistent with the underlying demyelinating pathology, but without any significant difference between the 2 groups. In contrast, NABT MTR, examined by ROI Table 3. MTR Analysis for PML and RRMS Region Mean MTR, % P Value PML lesions (n=6) 35.7 MS lesions (n=12) PML NABT ROI (n=6) 47.2 MS NABT ROI (n=12) PML NABT (n=4) MS NABT (n=12) Adjusted P Value a Abbreviations: MS, multiple sclerosis; MTR, magnetization transfer ratio; NABT, normal-appearing brain tissue; PML, progressive multifocal leukoencephalopathy; ROI, region of interest; RRMS, relapsing-remitting multiple sclerosis. a Hommel-adjusted P value. or globally, was significantly lower in RRMS than PML. Both regional and global reductions in the NABT MTR of patients with RRMS compared with relatively normal MTR in the NABT of patients with PML suggest that PML may be a more focal disease than RRMS. Nonconventional brain MRI studies have demonstrated diffuse and subtle tissue damage in otherwise NABT in RRMS even early in the disease course. 40,41 These observations could have significant implications by potentially detecting PML when it is relatively more focal. Chen et al 42 recently used voxel-based MTR to characterize the evolution of demyelination and remyelination in gadolinium-enhancing MS lesions, finding a significant decrease in MTR at the time of enhancement and partial recovery over the next 4 months, followed by apparent stabilization. In contrast, MTR of T2-visible PML brain lesions has been found to be very low and did not change significantly during a 9-month follow-up. 38,39 These MTR differences may reflect the different underlying pathophysiology of demyelination in the 2 conditions; whereas MS lesions are related to inflammation that may later resolve, JCV infection of oligodendrocytes is believed to lead to cell death. When evaluating a new brain MRI lesion in a patient with MS considered at risk for PML, one could use serial voxelbased MTR to discern whether the lesion is from MS (reversible inflammatory demyelination) or PML (irreversible infectious demyelination). Monthly brain MTR evaluation using a voxel-based approach demonstrating 597
6 varying degrees of remyelination within a suspected lesion would likely suggest that the lesion is secondary to MS. In contrast, consistently low MTR values observed uniformly in all voxels within the suspected lesion would be more likely to be PML. Such an approach may facilitate a timely window of opportunity to intervene, including the use of plasma exchange for rapid removal of the potentially offending agent NTZ 43 as well as initiation of other recently proposed interventions. 44 Nonetheless, this requires further work to evaluate the utility of MTR in a larger cohort. There are several limitations of our study, including the retrospective and cross-sectional design. Besides a modest sample size, 93% of PML cases were HIV positive, many with AIDS. There was no clinical correlation between the PML brain MRI lesion appearance and the clinical presentation. This could have been because of the relatively small sample size and that brain MRI scans in our study were not obtained according to a standardized protocol. Brain MTR data suggest interesting differences between PML and MS lesions. However, longitudinal studies in a larger number of patients are needed to not only confirm our findings but also study the evolution of PML lesions, regionally and globally. Moreover, there may be technical difficulties in implementing MTR protocols across multiple sites. In our data set, we had access to only 7 spinal cord MRI scans and the presence or absence of spinal cord involvement was judged solely on the basis of clinical presentation. Although we found no PML presentations consistent with a spinal cord syndrome, one such case has been recently reported. 32 It is possible that dedicated spinal cord MRI scans in patients with PML may identify MRI-visible spinal cord pathology at onset. Our preliminary study identifies differences in clinical and MRI features of PML and MS that confirm prior expert opinions 18,19 and may assist clinicians in earlier detection of PML in patients with RRMS. Even though effective therapies for PML are lacking, early identification of PML provides the best opportunity to intervene. In the patient with MS, the immediate discontinuation of the medication that may be contributing to the development of PML is of paramount importance. 44 Our study also explored the use of MT imaging as a novel imaging modality. Brain MTR data suggest PML may be relatively more focal than RRMS. This distinction deserves further exploration in a larger study as it may provide critical clues to the evolution of PML in patients with RRMS. Furthermore, serial brain voxel-based MTR may assist in distinguishing the etiology of a new suspected T2-weighted brain lesion in a patient with MS at risk for PML. Nonetheless, diagnosing PML against the background of preexisting MS remains challenging and complex, warranting larger multicenter studies to better define the disease, particularly in non HIV-positive patients. Accepted for Publication: October 30, Author Affiliations: Image Analysis Laboratory, Multiple Sclerosis Center, Department of Neurology (Drs Boster, Tselis, Zak, Perumal, and Khan and Mss Hreha, Bao, Penmesta, Endress, and Caon), Department of Radiology (Dr Zak), and Department of Physical Medicine and Rehabilitation and Division of Biostatistics and Clinical Translational Science (Dr Millis), Wayne State University School of Medicine, The Detroit Medical Center (Drs Boster, Tselis, Perumal, and Khan and Mss Hreha, Bao, Penmesta, and Caon), and Division of Infectious Diseases, Henry Ford Hospital (Dr Vazquez), Detroit, Michigan; Multiple Sclerosis Center, Division of Neuroimmunology, Department of Neurology, Ohio State University, Columbus (Drs Boster and Racke); Department of Neurology, University of Kentucky College of Medicine, Lexington (Dr Berger); and Departments of Neurology, Medicine, and Microbiology, University of Colorado Health Sciences Center and Denver Veterans Affairs Medical Center, Denver (Dr Tyler). Correspondence: Omar Khan, MD, Department of Neurology, Wayne State University School of Medicine, 4201 St Antoine, 8D-UHC, Detroit, MI (okhan@med.wayne.edu). Author Contributions: Study concept and design: Boster, Tselis, Zak, Perumal, Tyler, and Khan. Acquisition of data: Boster, Hreha, Bao, Tselis, Endress, Zak, Perumal, Caon, Vazquez, and Khan. Analysis and interpretation of data: Boster, Berger, Bao, Penmesta, Tyler, Racke, Millis, and Khan. Drafting of the manuscript: Boster, Hreha, Berger, Bao, Penmesta, Tselis, Endress, Zak, Perumal, Caon, and Khan. Critical revision of the manuscript for important intellectual content: Boster, Vazquez, Tyler, Racke, Millis, and Khan. Statistical analysis: Boster, Bao, Penmesta, and Millis. Obtained funding: Khan. Administrative, technical, and material support: Boster, Hreha, Zak, Caon, Racke, and Khan. Study supervision: Boster, Berger, Tselis, Vazquez, and Khan. Financial Disclosure: Dr Tyler has received consulting fees from Biogen Idec, Elan, Boehringer-Ingelheim, and Genentech for expert consultation in the areas of JCV infection and PML. Funding/Support: Dr Boster is a recipient of the Partners Multiple Sclerosis Fellowship Award. Dr Perumal is a recipient of the National Multiple Sclerosis Society Sylvia Lawry Fellowship Award. This study was supported in part by the Wayne State University Neuroscience Program. Additional Contributions: Richard Ransohoff (Cleveland Clinic) provided helpful comments. REFERENCES 1. Brooks BR, Walker DL. Progressive multifocal leukoencephalopathy. Neurol Clin. 1984;2(2): Padgett BL, Walker DL, ZuRhein GM, Eckroade RJ, Dessel BH. Cultivation of papovalike virus from human brain with progressive multifocal leucoencephalopathy. Lancet. 1971;1(7712): Astrom KE, Mancall EL, Richardson EP Jr. Progressive multifocal leukoencephalopathy: a hitherto unrecognized complication of chronic lymphatic leukaemia and Hodgkin s disease. Brain. 1958;81(1): Aksamit AJ. Review of progressive multifocal leukoencephalopathy and natalizumab. Neurologist. 2006;12(6): Kleinschmidt-DeMasters BK, Tyler KL. Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon beta-1a for multiple sclerosis. N Engl J Med. 2005;353(4): Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med. 2005;353(4):
7 7. Stüve O. The effects of natalizumab on the innate and adaptive immune system in the central nervous system. J Neurol Sci. 2008;274(1-2): Ransohoff RM. Natalizumab and PML. Nat Neurosci. 2005;8(10): Yousry TA, Major EO, Ryschkewitsch C, et al. Evaluation of patients treated with natalizumab for progressive multifocal leukoencephalopathy. N Engl J Med. 2006; 354(9): Panzara M, Baldinetti F, Belcher G, et al. Natalizumab utilization and safety in patients with relapsing multiple sclerosis: updated results from TOUCH and TYGRIS. Mult Scler. 2008;14(suppl 1):S172 (P488). 11. Gold R. Occurrence of progressive multifocal leukoencephalopathy in two patients relapsing-remitting MS treated with natalizumab: late breaking news. Mult Scler. 2008;14(suppl 1):OP Hauser SL, Waubant E, Arnold DL, et al; HERMES Trial Group. B-cell depletion with rituximab in relapsing-remitting multiple sclerosis. N Engl J Med. 2008; 358(7): Information for Healthcare Professionals Rituximab (marketed as Rituxan) Information. US Food and Drug Administration Center for Drug Evaluation and Research Web site. Published December Accessed Molloy ES, Calabrese LH. Progressive multifocal leukoencephalopathy in patients with rheumatic diseases: are patients with systemic lupus erythematosus at particular risk? Autoimmun Rev. 2008;8(2): Davies SL, Moral MA. Spotlight on: clinical development of mycophenolate mofetil in multiple sclerosis. Drug News Perspect. 2006;19(10): Pagnoux C, Hayem G, Roux F, et al. JC virus leukoencephalopathy complicating Wegner s granulomatosis. Joint Bone Spine. 2003;70(5): Warnatz K, Peter HH, Schumacher M, et al. Infectious CNS disease as a differential diagnosis is systemic rheumatic diseases: three case reports and a review of the literature. Ann Rheum Dis. 2003;62(1): Berger JR, Houff S. Progressive multifocal leukoencephalopathy: lessons from AIDS and natalizumab. Neurol Res. 2006;28(3): Kappos L, Bates D, Hartung HP, et al. Natalizumab treatment for multiple sclerosis: recommendations for patient selection and monitoring. Lancet Neurol. 2007; 6(5): Filippi M, Rocca MA, Rizzo G, et al. Magnetization transfer ratios in multiple sclerosis lesions enhancing after different doses of gadolinium. Neurology. 1998; 50(5): Filippi M, Iannucci G, Tortorella C, et al. Comparison of MS clinical phenotypes using conventional and magnetization transfer MRI. Neurology. 1999;52(3): McDonald WI, Compston A, Edan G, et al. Recommended diagnostic criteria for multiple sclerosis: guidelines from the International Panel on the diagnosis of multiple sclerosis. Ann Neurol. 2001;50(1): Hommel G. A stagewise rejective multiple test procedure based on a modified Bonferroni test. Biometrika. 1988;75(2): Barkhof F, Filippi M, Miller DH, et al. Comparison of MRI criteria at first presentation to predict conversion to clinically definite multiple sclerosis. Brain. 1997; 120(pt 11): Whiteman ML, Post MJ, Berger JR, Tate LG, Bell MD, Limonte LP. Progressive multifocal leukoencephalopathy in 47 HIV-seropositive patients: neuroimaging with clinical and pathologic correlation. Radiology. 1993;187(1): Berger JR, Pall L, Lanska D, Whiteman M. Progressive multifocal leukoencephalopathy in patients with HIV infection. J Neurovirol. 1998;4(1): Huang D, Cossoy M, Li M, et al. Inflammatory progressive multifocal leukoencephalopathy in human immunodeficiency virus-negative patients. Ann Neurol. 2007;62(1): Chowdhary S, Chalmers LM, Chamberlain M. Non-HIV-related progressive multifocal leukoencephalopathy (PML): a tertiary cancer center experience. J Neuroimaging. 2007;17(1): Hoffmann C, Horst HA, Albrecht H, Schlote W. Progressive multifocal leucoencephalopathy with unusual inflammatory response during antiretroviral treatment. J Neurol Neurosurg Psychiatry. 2003;74(8): Vendrely A, Bienvenu B, Gasnault J, Thiebault JB, Salmon D, Gray F. Fulminant inflammatory leukoencephalopathy associated with HAART-induced immune restoration in AIDS-related progressive multifocal leukoencephalopathy. Acta Neuropathol. 2005;109(4): Martinez JV, Mazziotti JV, Efron ED, et al. Immune reconstitution inflammatory syndrome associated with PML in AIDS: a treatable disorder. Neurology. 2006; 67(9): Bernal-Cano F, Joseph JT, Koralnik IJ. Spinal cord lesions of progressive multifocal leukoencephalopathy in an acquired immunodeficiency syndrome patient. J Neurovirol. 2007;13(5): Moll NM, Rietsch AM, Ransohoff AJ, et al. Cortical demyelination in PML and MS: similarities and differences. Neurology. 2008;70(5): Barkhof F, Scheltens P, Frequin ST, et al. Relapsing-remitting multiple sclerosis: sequential enhanced MR imaging vs clinical findings in determining disease activity. AJR Am J Roentgenol. 1992;159(5): Morgen K, Jeffries NO, Stone R, et al. Ring-enhancement in multiple sclerosis: marker of disease severity. Mult Scler. 2001;7(3): Filippi M, Rocca MA. Magnetization transfer magnetic resonance imaging in the assessment of neurological diseases. J Neuroimaging. 2004;14(4): Schmierer K, Scaravilli F, Altmann DR, Barker GJ, Miller DH. Magnetization transfer ratio and myelin in postmortem multiple sclerosis brain. Ann Neurol. 2004; 56(3): Kasner SE, Galetta SL, McGowan JC, Grossman RI. Magnetization transfer imaging in progressive multifocal leukoencephalopathy. Neurology. 1997;48(2): Armand JP, Dousset V, Franconi JM, et al. Progressive multifocal leukoencephalopathy: study of the demyelination by magnetization transfer [in French]. J Radiol. 1997;78(2): De Stefano N, Narayanan S, Francis GS, et al. Evidence of axonal damage in the early stages of multiple sclerosis and its relevance to disability. Arch Neurol. 2001; 58(1): Pike GB, De Stefano N, Narayanan S, et al. Multiple sclerosis: magnetization transfer MR imaging of white matter before lesion appearance on T2-weighted images. Radiology. 2000;215(3): Chen JT, Collins DL, Atkins HL, Freedman MS, Arnold DL; Canadian MS/BMT Study Group. Magnetization transfer ratio evolution with demyelination and remyelination in multiple sclerosis lesions. Ann Neurol. 2008;63(2): Khatri B FR, Koo A, Lynn F, Duda P, Jurgensen S, Panzara M, Giovannoni G. Plasma exchange accelerates the decline of serum natalizumab concentration in patients with multiple sclerosis: results of the Natalizumab PLEX Study. Neurology. 2008;70(11)(supp 1):A227-A Stüve O, Marra CM, Cravens PD, et al. Potential risk of progressive multifocal leukoencephalopathy with natalizumab therapy: possible interventions. Arch Neurol. 2007;64(2): Announcement Visit As an individual subscriber to Archives of Neurology, you have full-text online access to the journal from 1998 forward. In addition, you can find abstracts to the journal as far back as
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI
 Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
Risk of Natalizumab-Associated Progressive Multifocal Leukoencephalopathy
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Risk of Natalizumab-Associated Progressive Multifocal Leukoencephalopathy Gary Bloomgren, M.D., Sandra Richman, M.D., Christophe Hotermans,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Risk of Natalizumab-Associated Progressive Multifocal Leukoencephalopathy Gary Bloomgren, M.D., Sandra Richman, M.D., Christophe Hotermans,
MULTIPLE SCLEROSIS - REVIEW AND UPDATE
 MULTIPLE SCLEROSIS - REVIEW AND UPDATE Luka Vlahovic, MD Neuroimmunology/Multiple Sclerosis Creighton University Medical Center MS is primary demyelinating disease of the central nervous system. MS is
MULTIPLE SCLEROSIS - REVIEW AND UPDATE Luka Vlahovic, MD Neuroimmunology/Multiple Sclerosis Creighton University Medical Center MS is primary demyelinating disease of the central nervous system. MS is
Update: PML in MS. Kenneth Tyler, MD Reuler Lewin Family Professor & Chair Department of Neurology University of Colorado School of Medicine
 Update: PML in MS Kenneth Tyler, MD Reuler Lewin Family Professor & Chair Department of Neurology University of Colorado School of Medicine There are no FDA Approved Drugs for Treatment of PML: All Medications
Update: PML in MS Kenneth Tyler, MD Reuler Lewin Family Professor & Chair Department of Neurology University of Colorado School of Medicine There are no FDA Approved Drugs for Treatment of PML: All Medications
Mellen Center Approaches: Natalizumab
 Cleveland Clinic Mellen Center for Multiple Sclerosis Treatment and Research 216.444.8600 Mellen Center Approaches: Natalizumab Who should be considered for Natalizumab therapy? In the phase II and phase
Cleveland Clinic Mellen Center for Multiple Sclerosis Treatment and Research 216.444.8600 Mellen Center Approaches: Natalizumab Who should be considered for Natalizumab therapy? In the phase II and phase
1 MS Lesions in T2-Weighted Images
 1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
Natalizumab (Tysabri; Biogen Idec, Inc, Elan Pharmaceuticals,
 n report n Recommendations for the Selection, Treatment, and Management of Patients Utilizing Natalizumab Therapy for Multiple Sclerosis John Foley, MD Abstract Natalizumab is an integrin receptor antagonist
n report n Recommendations for the Selection, Treatment, and Management of Patients Utilizing Natalizumab Therapy for Multiple Sclerosis John Foley, MD Abstract Natalizumab is an integrin receptor antagonist
The following MS experts were involved in the development of this Position Statement:
 Position Statement for TYSABRI (natalizumab) and STRATIFY JCV TM in Multiple Sclerosis Rationale for this Position Statement This Position Statement was developed by ten Australian neurologists who specialise
Position Statement for TYSABRI (natalizumab) and STRATIFY JCV TM in Multiple Sclerosis Rationale for this Position Statement This Position Statement was developed by ten Australian neurologists who specialise
MEDIA BACKGROUNDER. Multiple Sclerosis: A serious and unpredictable neurological disease
 MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
MEDIA BACKGROUNDER Multiple Sclerosis: A serious and unpredictable neurological disease Multiple sclerosis (MS) is a complex chronic inflammatory disease of the central nervous system (CNS) that still
The TOUCH Program and Risk Management. Updated Safety Results From the Use of Natalizumab in Patients With Relapsing Multiple
 1 The TOUCH Program and Risk Management Plan for the Administration i ti of Natalizumab: Updated Safety Results From the Use of Natalizumab in Patients With Relapsing Multiple Sclerosis and Crohn s Disease
1 The TOUCH Program and Risk Management Plan for the Administration i ti of Natalizumab: Updated Safety Results From the Use of Natalizumab in Patients With Relapsing Multiple Sclerosis and Crohn s Disease
ORIGINAL CONTRIBUTION. Immune Reconstitution Inflammatory Syndrome in Patients With Multiple Sclerosis Following Cessation of Natalizumab Therapy
 ONLINE FIRST ORIGINAL CONTRIBUTION Immune Reconstitution Inflammatory Syndrome in Patients With Multiple Sclerosis Following Cessation of Natalizumab Therapy Augusto Miravalle, MD; Rikke Jensen, MD; R.
ONLINE FIRST ORIGINAL CONTRIBUTION Immune Reconstitution Inflammatory Syndrome in Patients With Multiple Sclerosis Following Cessation of Natalizumab Therapy Augusto Miravalle, MD; Rikke Jensen, MD; R.
2015 Diagnostic Slide Session
 2015 Diagnostic Slide Session Case 3 R.S. Tashjian, MD A.M. Langer-Gould, MD S. Natarajan, MD B.K. Kleinschmidt-DeMasters, MD H.V. Vinters, MD Disclosures No financial disclosures or conflicts of interest
2015 Diagnostic Slide Session Case 3 R.S. Tashjian, MD A.M. Langer-Gould, MD S. Natarajan, MD B.K. Kleinschmidt-DeMasters, MD H.V. Vinters, MD Disclosures No financial disclosures or conflicts of interest
PATIENT INFORMATION: Patient Surname First Name Middle Initial Sex Date of Birth Alberta Personal Health Number M / F Year Month Day
 Applicant must be covered on an Alberta Government sponsored drug program. Page 1 of 6 PATIENT INFORMATION: Patient Surname First Name Middle Initial Sex Date of Birth Alberta Personal Health Number M
Applicant must be covered on an Alberta Government sponsored drug program. Page 1 of 6 PATIENT INFORMATION: Patient Surname First Name Middle Initial Sex Date of Birth Alberta Personal Health Number M
MRI in MS: the radiologist perspective
 MS Preceptorship - Updating Knowledge in Multiple Sclerosis - June, 1-3 2010 Barcelona MRI in MS: the radiologist perspective Àlex Rovira Unidad de Resonancia Magnética Servicio de Radiología Hospital
MS Preceptorship - Updating Knowledge in Multiple Sclerosis - June, 1-3 2010 Barcelona MRI in MS: the radiologist perspective Àlex Rovira Unidad de Resonancia Magnética Servicio de Radiología Hospital
Evaluation of Patients Treated with Natalizumab for Progressive Multifocal Leukoencephalopathy
 The new england journal of medicine original article Evaluation of Patients Treated with Natalizumab for Progressive Multifocal Leukoencephalopathy Tarek A. Yousry, Dr.Med.Habil., Eugene O. Major, Ph.D.,
The new england journal of medicine original article Evaluation of Patients Treated with Natalizumab for Progressive Multifocal Leukoencephalopathy Tarek A. Yousry, Dr.Med.Habil., Eugene O. Major, Ph.D.,
Patologie infiammatorie encefaliche e midollari
 Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Tumefactive multiple sclerosis lesions: Diagnostic challenge for the radiologist
 Tumefactive multiple sclerosis lesions: Diagnostic challenge for the radiologist Poster No.: C-0679 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Gargallo Vaamonde, M. Iridoy Zulet, I. Rubio
Tumefactive multiple sclerosis lesions: Diagnostic challenge for the radiologist Poster No.: C-0679 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Gargallo Vaamonde, M. Iridoy Zulet, I. Rubio
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Pharmacy Management Drug Policy
 SUBJECT: Multiple Sclerosis, Crohn s Disease POLICY NUMBER: PHARMACY-53 EFFECTIVE DATE: 4/08 LAST REVIEW DATE: 12/18/2018 If the member s subscriber contract excludes coverage for a specific service or
SUBJECT: Multiple Sclerosis, Crohn s Disease POLICY NUMBER: PHARMACY-53 EFFECTIVE DATE: 4/08 LAST REVIEW DATE: 12/18/2018 If the member s subscriber contract excludes coverage for a specific service or
Neuroimaging and Other Biomarkers. MRI for Diagnosis, Prognosis and Treatment Decisions in MS
 Neuroimaging and Other Biomarkers MRI for Diagnosis, Prognosis and Treatment Decisions in MS Eric Klawiter, MD MSc Massachusetts General Hospital May 30, 2014 Disclosures and Funding Disclosures: Consulting
Neuroimaging and Other Biomarkers MRI for Diagnosis, Prognosis and Treatment Decisions in MS Eric Klawiter, MD MSc Massachusetts General Hospital May 30, 2014 Disclosures and Funding Disclosures: Consulting
Biologics and Beyond: Treatment of Multiple Sclerosis. Rita Jebrin, PharmD, BCPS
 Biologics and Beyond: Treatment of Multiple Sclerosis Rita Jebrin, PharmD, BCPS Disclosure Information Biologics and Beyond: Treatment of Multiple Sclerosis Rita Jebrin, PharmD, BCPS I have no financial
Biologics and Beyond: Treatment of Multiple Sclerosis Rita Jebrin, PharmD, BCPS Disclosure Information Biologics and Beyond: Treatment of Multiple Sclerosis Rita Jebrin, PharmD, BCPS I have no financial
Case Report. Abstract. Introduction. Case Report. Bela Purohit 1,2 Eranga Ganewatte 1 Spyros S. Kollias 1
 Case Report Natalizumab-Related Progressive Multifocal Leukoencephalopathy-Immune Reconstitution Inflammatory Syndrome: A Case Report Highlighting Clinical and MRI Features Bela Purohit 1,2 Eranga Ganewatte
Case Report Natalizumab-Related Progressive Multifocal Leukoencephalopathy-Immune Reconstitution Inflammatory Syndrome: A Case Report Highlighting Clinical and MRI Features Bela Purohit 1,2 Eranga Ganewatte
Switching from natalizumab to fingolimod: an observational study
 Acta Neurol Scand 2013: 128: e6 e10 DOI: 10.1111/ane.12082 Ó 2013 John Wiley & Sons A/S ACTA NEUROLOGICA SCANDINAVICA Clinical Commentary Switching from natalizumab to fingolimod: an observational study
Acta Neurol Scand 2013: 128: e6 e10 DOI: 10.1111/ane.12082 Ó 2013 John Wiley & Sons A/S ACTA NEUROLOGICA SCANDINAVICA Clinical Commentary Switching from natalizumab to fingolimod: an observational study
MAGNIMS MRI in monitoring disease activity and progression
 Teaching Course 3 MAGNIMS MRI in monitoring disease activity and progression Chairs: C. Enzinger (Graz, AT) N. De Stefano (Siena, IT) 7 Chances and challenges in monitoring disease activity and progression
Teaching Course 3 MAGNIMS MRI in monitoring disease activity and progression Chairs: C. Enzinger (Graz, AT) N. De Stefano (Siena, IT) 7 Chances and challenges in monitoring disease activity and progression
MRI diagnostic criteria for multiple sclerosis: an update
 MRI diagnostic criteria for multiple sclerosis: an update Poster No.: C-0285 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Valls Masot, A. M. Quiles Granado, J. Puig Alcántara, L. RamióTorrentà,
MRI diagnostic criteria for multiple sclerosis: an update Poster No.: C-0285 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Valls Masot, A. M. Quiles Granado, J. Puig Alcántara, L. RamióTorrentà,
CHAIR SUMMIT 7TH ANNUAL #CHAIR2014. Master Class for Neuroscience Professional Development. September 11 13, Westin Tampa Harbour Island
 #CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Use of MRI in Clinical Decision- Making
#CHAIR2014 7TH ANNUAL CHAIR SUMMIT Master Class for Neuroscience Professional Development September 11 13, 2014 Westin Tampa Harbour Island Sponsored by #CHAIR2014 Use of MRI in Clinical Decision- Making
The Role of MRI in Multiple Sclerosis
 September 2006 The Role of MRI in Multiple Sclerosis David Cochran, Harvard Medical School Year IV Meet our patient WM 49yoF presents to Multiple Sclerosis Clinic for follow-up regarding worsening symptoms
September 2006 The Role of MRI in Multiple Sclerosis David Cochran, Harvard Medical School Year IV Meet our patient WM 49yoF presents to Multiple Sclerosis Clinic for follow-up regarding worsening symptoms
Demyelinating Diseases of the Brain
 Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
EMA confirms recommendations to minimise risk of brain infection PML with Tysabri
 25/04/2016 EMA/266665/2016 EMA confirms recommendations to minimise risk of brain infection PML with Tysabri More frequent MRI scans should be considered for patients at higher risk On 25 February 2016,
25/04/2016 EMA/266665/2016 EMA confirms recommendations to minimise risk of brain infection PML with Tysabri More frequent MRI scans should be considered for patients at higher risk On 25 February 2016,
Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome)
 J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
Case Report PML-IRIS during Fingolimod Diagnosed after Natalizumab Discontinuation
 Case Reports in Neurological Medicine, Article ID 307872, 4 pages http://dx.doi.org/10.1155/2014/307872 Case Report PML-IRIS during Fingolimod Diagnosed after Natalizumab Discontinuation J. Killestein,
Case Reports in Neurological Medicine, Article ID 307872, 4 pages http://dx.doi.org/10.1155/2014/307872 Case Report PML-IRIS during Fingolimod Diagnosed after Natalizumab Discontinuation J. Killestein,
All relapsing multiple sclerosis patients should be managed at a specialist clinic- YES. Dr W J Brownlee FRACP 1. O Ciccarelli FRCP 1,2
 All relapsing multiple sclerosis patients should be managed at a specialist clinic- YES Dr W J Brownlee FRACP 1 O Ciccarelli FRCP 1,2 1 Queen Square Multiple Sclerosis Centre, Department of Neuroinflammation,
All relapsing multiple sclerosis patients should be managed at a specialist clinic- YES Dr W J Brownlee FRACP 1 O Ciccarelli FRCP 1,2 1 Queen Square Multiple Sclerosis Centre, Department of Neuroinflammation,
Hot Topics Multiple Sclerosis. Natalie Parks, MD, FRCPC Assistant Professor, Dalhousie University June 27, 2018
 Hot Topics Multiple Sclerosis Natalie Parks, MD, FRCPC Assistant Professor, Dalhousie University June 27, 2018 Disclosures Natalie Parks has received compensation from Biogen, EMD Serono, Roche, and Sanofi
Hot Topics Multiple Sclerosis Natalie Parks, MD, FRCPC Assistant Professor, Dalhousie University June 27, 2018 Disclosures Natalie Parks has received compensation from Biogen, EMD Serono, Roche, and Sanofi
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
MRI and differential diagnosis in patients suspected of having MS
 Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Magnetic resonance imaging in multiple sclerosis
 APRIL 2002 103 Magnetic resonance imaging in multiple sclerosis Beside the ability to detect the Olga Ciccarelli and David H. Miller NMR Unit, Institute of Neurology, University College London, Queen Square,
APRIL 2002 103 Magnetic resonance imaging in multiple sclerosis Beside the ability to detect the Olga Ciccarelli and David H. Miller NMR Unit, Institute of Neurology, University College London, Queen Square,
Natalizumab (Tysabri, Biogen Idec and Elan), a monoclonal antibody
 The new england journal of medicine brief report Treatment of Progressive Multifocal Leuko encephalopathy Associated with Natalizumab Werner Wenning, M.D., Aiden Haghikia, M.D., Jörg Laubenberger, M.D.,
The new england journal of medicine brief report Treatment of Progressive Multifocal Leuko encephalopathy Associated with Natalizumab Werner Wenning, M.D., Aiden Haghikia, M.D., Jörg Laubenberger, M.D.,
Update in Multiple Sclerosis
 Update in Multiple Sclerosis Kyle Smoot, MD Providence MS Center Portland, OR 1 Disclosures Research funds from Biogen. Consulting fees from Acorda, Biogen, EMDSerono, Genzyme, Novartis, and Teva. 2 Outline
Update in Multiple Sclerosis Kyle Smoot, MD Providence MS Center Portland, OR 1 Disclosures Research funds from Biogen. Consulting fees from Acorda, Biogen, EMDSerono, Genzyme, Novartis, and Teva. 2 Outline
Life Long Brain Health and DMT Comparative Effectiveness
 Life Long Brain Health and DMT Comparative Effectiveness Timothy Vollmer, MD Professor of Neurology University of Colorado Denver Medical Director- RMMSC and Co-Director Rocky Mountain MS Center at CU
Life Long Brain Health and DMT Comparative Effectiveness Timothy Vollmer, MD Professor of Neurology University of Colorado Denver Medical Director- RMMSC and Co-Director Rocky Mountain MS Center at CU
Spinal cord MR imaging in Multiple Sclerosis
 43ème CONGRÈS ANNUEL de la Société Française de NeuroRadiologie 30 mars au 1 er avril 2016 Novotel Paris Tour Eiffel Spinal cord MR imaging in Multiple Sclerosis Àlex Rovira Unitat de Neurorradiología.
43ème CONGRÈS ANNUEL de la Société Française de NeuroRadiologie 30 mars au 1 er avril 2016 Novotel Paris Tour Eiffel Spinal cord MR imaging in Multiple Sclerosis Àlex Rovira Unitat de Neurorradiología.
Progressive Multifocal Leukoencephalopathy (PML)
 Progressive Multifocal Leukoencephalopathy (PML) By Jamie Meier Introduction: Progressive multifocal leukoencephalopathy (PML) occurs when change in an individual s immune status triggers reactivation
Progressive Multifocal Leukoencephalopathy (PML) By Jamie Meier Introduction: Progressive multifocal leukoencephalopathy (PML) occurs when change in an individual s immune status triggers reactivation
Novartis real-world data at AAN confirms benefit of Gilenya on four key measures of disease activity in relapsing MS
 Novartis International AG Novartis Global Communications CH-4002 Basel Switzerland http://www.novartis.com MEDIA RELEASE COMMUNIQUE AUX MEDIAS MEDIENMITTEILUNG Novartis real-world data at AAN confirms
Novartis International AG Novartis Global Communications CH-4002 Basel Switzerland http://www.novartis.com MEDIA RELEASE COMMUNIQUE AUX MEDIAS MEDIENMITTEILUNG Novartis real-world data at AAN confirms
Outcome of Drug-Induced PML
 Outcome of Drug-Induced PML Joseph R. Berger, M.D. University of Kentucky For Session 1: Overview of PML as an adverse event of immunobiologicals (MABs) Transatlantic Workshop: Drug-related PML London,
Outcome of Drug-Induced PML Joseph R. Berger, M.D. University of Kentucky For Session 1: Overview of PML as an adverse event of immunobiologicals (MABs) Transatlantic Workshop: Drug-related PML London,
Local Natalizumab Treatment Protocol
 Local Natalizumab Treatment Protocol 1. New medicine name: Natalizumab 300mg concentrate for solution for infusion (Natalizumab ) 2. Licensed indication(s): Natalizumab is indicated for single disease
Local Natalizumab Treatment Protocol 1. New medicine name: Natalizumab 300mg concentrate for solution for infusion (Natalizumab ) 2. Licensed indication(s): Natalizumab is indicated for single disease
Clinical and research application of MRI in diagnosis and monitoring of multiple sclerosis
 24-25 February 2016 - Siena, Italy Clinical and research application of MRI in diagnosis and monitoring of multiple sclerosis IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org How
24-25 February 2016 - Siena, Italy Clinical and research application of MRI in diagnosis and monitoring of multiple sclerosis IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org How
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview
 Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS
 NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS Jeffrey A. Cohen, MD Director, Experimental Therapeutics Mellen MS Center Neurological Institute Cleveland Clinic 2018 Regional MS Summit 30 June 2018 Disclosures
NEW DIAGNOSTIC CRITERIA FOR MULTIPLE SCLEROSIS Jeffrey A. Cohen, MD Director, Experimental Therapeutics Mellen MS Center Neurological Institute Cleveland Clinic 2018 Regional MS Summit 30 June 2018 Disclosures
MULTIPLE SCLEROSIS IN Managing the complexity of multiple sclerosis. Olga Ciccarelli and Alan Thompson
 MULTIPLE SCLEROSIS IN 2015 Managing the complexity of multiple sclerosis Olga Ciccarelli and Alan Thompson The application of imaging biomarkers has provided new insights into the mechanisms of damage
MULTIPLE SCLEROSIS IN 2015 Managing the complexity of multiple sclerosis Olga Ciccarelli and Alan Thompson The application of imaging biomarkers has provided new insights into the mechanisms of damage
Magnetization Transfer Study of HIV Encephalitis and Progressive Multifocal Leukoencephalopathy
 Magnetization Transfer Study of HIV Encephalitis and Progressive Multifocal Leukoencephalopathy Vincent Dousset, Jean-Pierre Armand, Denis Lacoste, Stéphane Mièze, Luc Letenneur, Jean-François Dartigues,
Magnetization Transfer Study of HIV Encephalitis and Progressive Multifocal Leukoencephalopathy Vincent Dousset, Jean-Pierre Armand, Denis Lacoste, Stéphane Mièze, Luc Letenneur, Jean-François Dartigues,
MRI dynamics of brain and spinal cord in progressive multiple sclerosis
 J7ournal of Neurology, Neurosurgery, and Psychiatry 1 996;60: 15-19 MRI dynamics of brain and spinal cord in progressive multiple sclerosis 1 5 D Kidd, J W Thorpe, B E Kendall, G J Barker, D H Miller,
J7ournal of Neurology, Neurosurgery, and Psychiatry 1 996;60: 15-19 MRI dynamics of brain and spinal cord in progressive multiple sclerosis 1 5 D Kidd, J W Thorpe, B E Kendall, G J Barker, D H Miller,
The relationship between PML-rituximab and other immunobiologicals: an overview
 The relationship between PML-rituximab and other immunobiologicals: an overview Renaud Du Pasquier, M.D. Associate professor in Neurology Neuroimmunology University Hospital of Vaud, Switzerland Transatlantic
The relationship between PML-rituximab and other immunobiologicals: an overview Renaud Du Pasquier, M.D. Associate professor in Neurology Neuroimmunology University Hospital of Vaud, Switzerland Transatlantic
Neuromyelitis optica (NMO), or Devic s disease, is a rare
 Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
Case Report Neuromyelitis Optica (NMO) Abstract NMO is a is a rare entity which involves the central nervous system acting as an inflammatory process by attacking the optic nerve (ON) and longitudinally
Title Progressive multifocal leukoencephalopathy with Behcet s disease: an insight into pathophysiology
 Title Progressive multifocal leukoencephalopathy with Behcet s disease: an insight into pathophysiology Authors Smriti Agarwal (MRCP, MD) 1, Jean Patrick (MRCP) 2, Joanne Jones (MRCP, PhD) 1, Rona Smith
Title Progressive multifocal leukoencephalopathy with Behcet s disease: an insight into pathophysiology Authors Smriti Agarwal (MRCP, MD) 1, Jean Patrick (MRCP) 2, Joanne Jones (MRCP, PhD) 1, Rona Smith
Program Highlights. A multidisciplinary AAN working group identified areas for improvement in the diagnosis and management of patients with MS
 CasePerspectives: Illuminating Dark Pathways in Complex MS Cases Program Highlights Stephen Krieger, MD Associate Professor of Neurology Corinne Goldsmith Dickinson Center for MS Director, Neurology Residency
CasePerspectives: Illuminating Dark Pathways in Complex MS Cases Program Highlights Stephen Krieger, MD Associate Professor of Neurology Corinne Goldsmith Dickinson Center for MS Director, Neurology Residency
Long-Term Changes of Magnetization Transfer Derived Measures from Patients with Relapsing-Remitting and Secondary Progressive Multiple Sclerosis
 AJNR Am J Neuroradiol 20:821 827, May 1999 Long-Term Changes of Magnetization Transfer Derived Measures from Patients with Relapsing-Remitting and Secondary Progressive Multiple Sclerosis Maria A. Rocca,
AJNR Am J Neuroradiol 20:821 827, May 1999 Long-Term Changes of Magnetization Transfer Derived Measures from Patients with Relapsing-Remitting and Secondary Progressive Multiple Sclerosis Maria A. Rocca,
Low sensitivity of McDonald MRI criteria in the diagnosis of multiple sclerosis among Asians
 Neurology Asia 2006; 11 : 129 133 Low sensitivity of McDonald MRI criteria in the diagnosis of multiple sclerosis among Asians 1 Heng-Thay CHONG MRCP, 1 Norlisah RAMLI FRCR, 2 Kwang-Ho LEE MD, 2 Byung-Joon
Neurology Asia 2006; 11 : 129 133 Low sensitivity of McDonald MRI criteria in the diagnosis of multiple sclerosis among Asians 1 Heng-Thay CHONG MRCP, 1 Norlisah RAMLI FRCR, 2 Kwang-Ho LEE MD, 2 Byung-Joon
ORIGINAL ARTICLE Thoracic spinal cord lesions are influenced by the degree of cervical spine involvement in multiple sclerosis
 (2015) 53, 520 525 & 2015 International Society All rights reserved 1362-4393/15 www.nature.com/sc ORIGINAL ARTICLE Thoracic spinal cord lesions are influenced by the degree of cervical spine involvement
(2015) 53, 520 525 & 2015 International Society All rights reserved 1362-4393/15 www.nature.com/sc ORIGINAL ARTICLE Thoracic spinal cord lesions are influenced by the degree of cervical spine involvement
Progressive Multifocal Leukoencephalopathy (PML) in Natalizumab-Treated Patients: Experience of the FDA Division of Neurology Products
 Progressive Multifocal Leukoencephalopathy (PML) in Natalizumab-Treated Patients: Experience of the FDA Division of Neurology Products M. Lisa Jones MD, MPH Russell Katz, M.D. Director Division of Neurology
Progressive Multifocal Leukoencephalopathy (PML) in Natalizumab-Treated Patients: Experience of the FDA Division of Neurology Products M. Lisa Jones MD, MPH Russell Katz, M.D. Director Division of Neurology
Central Nervous System Immune Reconstitution Disease: Pathology
 Central Nervous System Immune Reconstitution Disease: Pathology F.Gray, H.Adle-Biassette, F.Héran, G. Pialoux, A.Moulignier, APHP Hôpital Lariboisière Université Paris VII Introduction of HAART, which
Central Nervous System Immune Reconstitution Disease: Pathology F.Gray, H.Adle-Biassette, F.Héran, G. Pialoux, A.Moulignier, APHP Hôpital Lariboisière Université Paris VII Introduction of HAART, which
Correspondence should be addressed to Mohamed-Ali Babi;
 Case eports in Neurological Medicine Volume 2015, Article ID 643216, 4 pages http://dx.doi.org/10.1155/2015/643216 Case eport JC Virus PC Detection Is Not Infallible: A Fulminant Case of Progressive Multifocal
Case eports in Neurological Medicine Volume 2015, Article ID 643216, 4 pages http://dx.doi.org/10.1155/2015/643216 Case eport JC Virus PC Detection Is Not Infallible: A Fulminant Case of Progressive Multifocal
MRI in Differential Diagnosis. CMSC, June 2, Jill Conway, MD, MA, MSCE
 MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
TYSABRI Treatment Initiation Form
 TYSABRI Treatment Initiation Form This form should be read carefully before starting treatment with TYSABRI. Please follow the advice in this form to ensure that you are fully informed of, and understand
TYSABRI Treatment Initiation Form This form should be read carefully before starting treatment with TYSABRI. Please follow the advice in this form to ensure that you are fully informed of, and understand
Neuroradiology of AIDS
 Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
Neurology and Neurometabolic Unit Department of Neurological and Behavioral Sciences University of Siena Siena, Italy
 Nicola De Stefano Neurology and Neurometabolic Unit Department of Neurological and Behavioral Sciences University of Siena Siena, Italy Declared receipt of honoraria or consultation fees from Novartis,
Nicola De Stefano Neurology and Neurometabolic Unit Department of Neurological and Behavioral Sciences University of Siena Siena, Italy Declared receipt of honoraria or consultation fees from Novartis,
Progressive Multifocal Leukoencephalopathy in a Patient Treated with Natalizumab
 brief report Progressive Multifocal Leukoencephalopathy in a Patient Treated with Natalizumab Annette Langer-Gould, M.D., Scott W. Atlas, M.D., Ari J. Green, M.D., Andrew W. Bollen, M.D., and Daniel Pelletier,
brief report Progressive Multifocal Leukoencephalopathy in a Patient Treated with Natalizumab Annette Langer-Gould, M.D., Scott W. Atlas, M.D., Ari J. Green, M.D., Andrew W. Bollen, M.D., and Daniel Pelletier,
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Magnetization-Transfer Histogram Analysis of the Cervical Cord in Patients with Multiple Sclerosis
 AJNR Am J Neuroradiol 20:1803 1808, November/December 1999 Magnetization-Transfer Histogram Analysis of the Cervical Cord in Patients with Multiple Sclerosis Marco Bozzali, Maria A. Rocca, Giuseppe Iannucci,
AJNR Am J Neuroradiol 20:1803 1808, November/December 1999 Magnetization-Transfer Histogram Analysis of the Cervical Cord in Patients with Multiple Sclerosis Marco Bozzali, Maria A. Rocca, Giuseppe Iannucci,
DOWNLOAD OR READ : MULTIPLE SCLEROSIS THE HISTORY OF A DISEASE PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : MULTIPLE SCLEROSIS THE HISTORY OF A DISEASE PDF EBOOK EPUB MOBI Page 1 Page 2 multiple sclerosis the history of a disease multiple sclerosis the history pdf multiple sclerosis the history
DOWNLOAD OR READ : MULTIPLE SCLEROSIS THE HISTORY OF A DISEASE PDF EBOOK EPUB MOBI Page 1 Page 2 multiple sclerosis the history of a disease multiple sclerosis the history pdf multiple sclerosis the history
RESEARCH/CLINICAL UPDATE. ADDITIONAL ROUTING Research Advocate Staff Liaison Chapter President I & R specialists
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Tel 212 986 3240 1 800 FIGHT MS Fax 212 986 7981 E-Mail: Nat@nmss.org www.nmss.org April 29, 2005 RESEARCH/CLINICAL UPDATE ADDITIONAL
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Tel 212 986 3240 1 800 FIGHT MS Fax 212 986 7981 E-Mail: Nat@nmss.org www.nmss.org April 29, 2005 RESEARCH/CLINICAL UPDATE ADDITIONAL
European Commission Grants Approval for Mavenclad (Cladribine Tablets)
 Your Contact Friederike Segeberg +49 6151 72-6328 Investor Relations +49 6151 72-3321 August 25, 2017 European Commission Grants Approval for Mavenclad (Cladribine Tablets) First oral short-course treatment
Your Contact Friederike Segeberg +49 6151 72-6328 Investor Relations +49 6151 72-3321 August 25, 2017 European Commission Grants Approval for Mavenclad (Cladribine Tablets) First oral short-course treatment
ORIGINAL CONTRIBUTION. Infratentorial Lesions Predict Long-term Disability in Patients With Initial Findings Suggestive of Multiple Sclerosis
 ORIGINAL CONTRIBUTION Infratentorial Lesions Predict Long-term Disability in Patients With Initial Findings Suggestive of Multiple Sclerosis Arjan Minneboo, MD; Frederick Barkhof, MD; Chris H. Polman,
ORIGINAL CONTRIBUTION Infratentorial Lesions Predict Long-term Disability in Patients With Initial Findings Suggestive of Multiple Sclerosis Arjan Minneboo, MD; Frederick Barkhof, MD; Chris H. Polman,
Neuroradiological, clinical and genetic characterization of new forms of hereditary leukoencephalopathies
 Neuroradiological, clinical and genetic characterization of new forms of hereditary leukoencephalopathies Principal Investigator: Dr. Donatella Tampieri, MD, FRCPC, Department of Neuroradiology, Montreal
Neuroradiological, clinical and genetic characterization of new forms of hereditary leukoencephalopathies Principal Investigator: Dr. Donatella Tampieri, MD, FRCPC, Department of Neuroradiology, Montreal
Multiple sclerosis (MS) is a disabling chronic demyelinating disease
 Diagn Interv Radiol 2010; 16:106 111 Turkish Society of Radiology 2010 NEURORADIOLOGY ORIGINAL ARTICLE Imaging of active multiple sclerosis plaques: efficiency of contrast-enhanced magnetization transfer
Diagn Interv Radiol 2010; 16:106 111 Turkish Society of Radiology 2010 NEURORADIOLOGY ORIGINAL ARTICLE Imaging of active multiple sclerosis plaques: efficiency of contrast-enhanced magnetization transfer
Clinician s view of Benefit-Risk
 Clinician s view of Benefit-Risk Gordon Francis, MD Novartis, Clinical Development Clinician s View of Benefit-Risk: a need for reliable metrics A tale of 3 drugs Natalizumab MS Crohn s Disease Fingolimod
Clinician s view of Benefit-Risk Gordon Francis, MD Novartis, Clinical Development Clinician s View of Benefit-Risk: a need for reliable metrics A tale of 3 drugs Natalizumab MS Crohn s Disease Fingolimod
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study
 Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Pediatric acute demyelinating encephalomyelitis in Denmark: a nationwide population-based study Magnus Spangsberg Boesen November, 2016 Supervisors: P. Born, P. Uldall, M. Blinkenberg, M. Magyari, F. Sellebjerg
Magnetic Resonance Imaging and Spectroscopy: Insights into the Pathology and Pathophysiology of Multiple Sclerosis.
 Chapter 10 (pp 139-167) of Multiple Sclerosis 2 - Blue Books of Practical Neurology, vol. 27. J.H Noseworthy, W.I. McDonald (eds.). Elsevier Science (USA), 2003. Magnetic Resonance Imaging and Spectroscopy:
Chapter 10 (pp 139-167) of Multiple Sclerosis 2 - Blue Books of Practical Neurology, vol. 27. J.H Noseworthy, W.I. McDonald (eds.). Elsevier Science (USA), 2003. Magnetic Resonance Imaging and Spectroscopy:
Relevance of Hypointense Lesions on Fast Fluid- Attenuated Inversion Recovery MR Images as a Marker of Disease Severity in Cases of Multiple Sclerosis
 AJNR Am J Neuroradiol 20:813 820, May 1999 Relevance of Hypointense Lesions on Fast Fluid- Attenuated Inversion Recovery MR Images as a Marker of Disease Severity in Cases of Multiple Sclerosis Marco Rovaris,
AJNR Am J Neuroradiol 20:813 820, May 1999 Relevance of Hypointense Lesions on Fast Fluid- Attenuated Inversion Recovery MR Images as a Marker of Disease Severity in Cases of Multiple Sclerosis Marco Rovaris,
Le Hua, MD. Disclosures Teaching and Speaking: Teva Neurosciences, Genzyme, Novartis Advisory Board: Genzyme, EMD Serono
 Le Hua, MD Le Hua, MD, is a staff neurologist at Cleveland Clinic Lou Ruvo Center for Brain Health in Las Vegas, NV. She is involved in clinical trials assessing new therapies for the treatment of MS and
Le Hua, MD Le Hua, MD, is a staff neurologist at Cleveland Clinic Lou Ruvo Center for Brain Health in Las Vegas, NV. She is involved in clinical trials assessing new therapies for the treatment of MS and
Carolyn Taylor, M.D. Swedish Neuroscience Center
 Carolyn Taylor, M.D. Swedish Neuroscience Center When should disease modifying therapy be discontinued in MS? Should we be using aggressive treatments earlier in the MS disease course and reserving the
Carolyn Taylor, M.D. Swedish Neuroscience Center When should disease modifying therapy be discontinued in MS? Should we be using aggressive treatments earlier in the MS disease course and reserving the
ORIGINAL CONTRIBUTION. Determinants of Cerebral Atrophy Rate at the Time of Diagnosis of Multiple Sclerosis. imaging (MRI) provides
 ORIGINAL CONTRIBUTION Determinants of Cerebral Atrophy Rate at the Time of Diagnosis of Multiple Sclerosis Bas Jasperse, MD; Arjan Minneboo, MD; Vincent de Groot, MD; Nynke F. Kalkers, MD, PhD; Paul E.
ORIGINAL CONTRIBUTION Determinants of Cerebral Atrophy Rate at the Time of Diagnosis of Multiple Sclerosis Bas Jasperse, MD; Arjan Minneboo, MD; Vincent de Groot, MD; Nynke F. Kalkers, MD, PhD; Paul E.
SHORTLY AFTER ITS FIRST DEpiction
 OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
Epidemiology, Diagnosis, Natural History & Clinical Course
 Epidemiology, Diagnosis, Natural History & Clinical Course Multiple Sclerosis Immune-mediated, chronic, inflammatory disease precipitated by unknown environmental factors in genetically susceptible individuals
Epidemiology, Diagnosis, Natural History & Clinical Course Multiple Sclerosis Immune-mediated, chronic, inflammatory disease precipitated by unknown environmental factors in genetically susceptible individuals
Visualisation of cortical MS lesions with MRI need not be further improved: Yes
 Controversies in Multiple Sclerosis Visualisation of cortical MS lesions with MRI need not be further improved: Yes Jeroen J.G. Geurts [1] & Declan T. Chard [2] 1. Dept. of Anatomy & Neurosciences, VUmc
Controversies in Multiple Sclerosis Visualisation of cortical MS lesions with MRI need not be further improved: Yes Jeroen J.G. Geurts [1] & Declan T. Chard [2] 1. Dept. of Anatomy & Neurosciences, VUmc
Myelitis. Case 2. History. Examination. Mahtab Ghadiri
 Case 2 Myelitis Mahtab Ghadiri History A 42-year-old man presented to the emergency department with altered sensation in the lower limbs and difficulty ambulating. He first noted paresthesia in his feet
Case 2 Myelitis Mahtab Ghadiri History A 42-year-old man presented to the emergency department with altered sensation in the lower limbs and difficulty ambulating. He first noted paresthesia in his feet
Quantitative Neuroimaging- Gray and white matter Alteration in Multiple Sclerosis. Lior Or-Bach Instructors: Prof. Anat Achiron Dr.
 Quantitative Neuroimaging- Gray and white matter Alteration in Multiple Sclerosis Lior Or-Bach Instructors: Prof. Anat Achiron Dr. Shmulik Miron INTRODUCTION Multiple Sclerosis general background Gray
Quantitative Neuroimaging- Gray and white matter Alteration in Multiple Sclerosis Lior Or-Bach Instructors: Prof. Anat Achiron Dr. Shmulik Miron INTRODUCTION Multiple Sclerosis general background Gray
Multiple sclerosis (MS) is an inflammatory disease of the central nervous. Magnetic Resonance Imaging in Multiple Sclerosis
 DIAGNOSIS AND MANAGEMENT UPDATE Magnetic Resonance Imaging in Multiple Sclerosis Salvatore Q. Napoli, MD, * Rohit Bakshi, MD * *Partners, Multiple Sclerosis Center, Boston, MA, Center for Neurological
DIAGNOSIS AND MANAGEMENT UPDATE Magnetic Resonance Imaging in Multiple Sclerosis Salvatore Q. Napoli, MD, * Rohit Bakshi, MD * *Partners, Multiple Sclerosis Center, Boston, MA, Center for Neurological
Interactive Cases: Demyelinating Diseases and Mimics. Disclosures. Case 1 25 yo F with nystagmus; look for tumor 4/14/2017
 Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Isolated Demyelinating Syndromes: Comparison of Different MR Imaging Criteria to Predict Conversion to Clinically Definite Multiple Sclerosis
 AJNR Am J Neuroradiol 21:702 706, April 2000 Isolated Demyelinating Syndromes: Comparison of Different MR Imaging Criteria to Predict Conversion to Clinically Definite Multiple Sclerosis Mar Tintoré, Alex
AJNR Am J Neuroradiol 21:702 706, April 2000 Isolated Demyelinating Syndromes: Comparison of Different MR Imaging Criteria to Predict Conversion to Clinically Definite Multiple Sclerosis Mar Tintoré, Alex
Provider Led Entity. CDI Quality Institute PLE Multiple Sclerosis (MS) AUC
 Provider Led Entity CDI Quality Institute PLE Multiple Sclerosis (MS) AUC Appropriateness of advanced imaging procedures* in patients with the following clinical presentations or diagnoses: 09/04/2018
Provider Led Entity CDI Quality Institute PLE Multiple Sclerosis (MS) AUC Appropriateness of advanced imaging procedures* in patients with the following clinical presentations or diagnoses: 09/04/2018
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow
 Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
MULTIPLE SCLEROSIS Update
 MULTIPLE SCLEROSIS Update E. Torage Shivapour, M.D. Clinical Professor Department of Neurology University of Iowa Hospitals & Clinics Disclosures I do not have any disclosures. Multiple Sclerosis Most
MULTIPLE SCLEROSIS Update E. Torage Shivapour, M.D. Clinical Professor Department of Neurology University of Iowa Hospitals & Clinics Disclosures I do not have any disclosures. Multiple Sclerosis Most
THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY
 THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY John R. Rinker, II, MD University of Alabama at Birmingham June 2, 2016 DISCLOSURES Research Support: Biogen Idec; Department of
THE NATURAL HISTORY OF MS: DIAGNOSIS, CLINICAL COURSE, AND EPIDEMIOLOGY John R. Rinker, II, MD University of Alabama at Birmingham June 2, 2016 DISCLOSURES Research Support: Biogen Idec; Department of
Imaging of Demyelinating Processes
 Acta Radiológica Portuguesa, Vol.XXI, nº 82, pág. 81-88, Abr.-Jun., 2009 Imaging of Demyelinating Processes Alice Boyd Smith, MD Chief, Neuroradiology - Department of Radiologic Pathology, Armed Forces
Acta Radiológica Portuguesa, Vol.XXI, nº 82, pág. 81-88, Abr.-Jun., 2009 Imaging of Demyelinating Processes Alice Boyd Smith, MD Chief, Neuroradiology - Department of Radiologic Pathology, Armed Forces
Progressive multifocal leukoencephalopathy (PML) Advances in the management of PML: Focus on natalizumab ABSTRACT APPROACH TO PML TREATMENT
 ROBERT FOX, MD Staff Neurologist and Medical Director, Mellen Center for Multiple Sclerosis, Neurological Institute, Cleveland Clinic, Cleveland, OH Advances in the management of PML: Focus on natalizumab
ROBERT FOX, MD Staff Neurologist and Medical Director, Mellen Center for Multiple Sclerosis, Neurological Institute, Cleveland Clinic, Cleveland, OH Advances in the management of PML: Focus on natalizumab
Neuroradiology Original Research
 MRI of Multiple Sclerosis Lesions Neuroradiology Original Research Ender Uysal 1 Sukru Mehmet Erturk 1 Hakan Yildirim 1 Feray Seleker 2 Muzaffer Basak 1 Uysal E, Erturk SM, Yildirim H, et al. Keywords:
MRI of Multiple Sclerosis Lesions Neuroradiology Original Research Ender Uysal 1 Sukru Mehmet Erturk 1 Hakan Yildirim 1 Feray Seleker 2 Muzaffer Basak 1 Uysal E, Erturk SM, Yildirim H, et al. Keywords:
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
ORIGINAL CONTRIBUTION Neuromyelitis Optica Treatment Analysis of 3 s Denis Bernardi Bichuetti, MD; Enedina Maria Lobato de Oliveira, MD, PhD; Daniel May Oliveira, MD; Nilton Amorin de Souza, MD; Alberto
Idiopathic Inflammatory Demyelinating Diseases of the Brainstem
 Idiopathic Inflammatory Demyelinating Diseases of the Brainstem 1 A. Rovira-Cañellas, 2 A. Rovira-Gols, 1 J. Sastre-Garriga, 1 C. Auger, 1 J. Munuera, 1 X. Montalban 1 Hospital Vall d Hebron, Barcelona.
Idiopathic Inflammatory Demyelinating Diseases of the Brainstem 1 A. Rovira-Cañellas, 2 A. Rovira-Gols, 1 J. Sastre-Garriga, 1 C. Auger, 1 J. Munuera, 1 X. Montalban 1 Hospital Vall d Hebron, Barcelona.
Medscape: What do you see as the main clinical implications of your results?
 http://www.medscape.com/px/viewindex/more?bucket=columns§ionid=2011 Treatment Optimization for Multiple Sclerosis: An Expert Interview With Mark Freedman, MD Posted 11/10/2004 Editor's Note: Multiple
http://www.medscape.com/px/viewindex/more?bucket=columns§ionid=2011 Treatment Optimization for Multiple Sclerosis: An Expert Interview With Mark Freedman, MD Posted 11/10/2004 Editor's Note: Multiple
Investor Update. Downloads. Services PDF. Basel, 17 July 2017
 Investor Update Basel, 17 July 2017 Roche s OCREVUS (ocrelizumab) approved for relapsing and primary progressive multiple sclerosis in Australia Second approval after the US for OCREVUS as the first and
Investor Update Basel, 17 July 2017 Roche s OCREVUS (ocrelizumab) approved for relapsing and primary progressive multiple sclerosis in Australia Second approval after the US for OCREVUS as the first and
