Feasibility Study of Docetaxel with Cyclophosphamide as Adjuvant Chemotherapy for Japanese Breast Cancer Patients
|
|
|
- Allison Chapman
- 5 years ago
- Views:
Transcription
1 Jpn J Clin Oncol 2009;39(8) doi: /jjco/hyp050 Original Articles Feasibility Study of Docetaxel with Cyclophosphamide as Adjuvant Chemotherapy for Japanese Breast Cancer Patients Daisuke Takabatake 1, Naruto Taira 2, Fumikata Hara 1, Tadahiko Sien 2, Sachiko Kiyoto 1, Seiki Takashima 1, Kenjiro Aogi 1, Shozo Ohsumi 1, Hiroyoshi Doihara 2 and Shigemitu Takashima 1 1 Department of Breast Oncology, National Hospital Organization Shikoku Cancer Center, Ehime and 2 Department of Cancer and Thoracic Surgery, Okayama University Graduate School of Medicine, Okayama, Japan Received March 17, 2009; accepted April 25, 2009; published online June 1, 2009 Objective: The 7-year follow-up of the US oncology 9735 trial demonstrated the superiority of TC [docetaxel (DTX)/cyclophosphamide (CPA)] to doxorubicin/cpa therapy. To introduce TC therapy in Japan, the verification of the safety and tolerability is essential. We performed a collaborative prospective safety study with Okayama University to introduce TC therapy. Methods: The subjects were 53 patients aged from 33 to 67 years at intermediate risk based on the St Gallen risk classification who underwent radical surgery for primary breast cancer between August 2007 and December As post-operative adjuvant chemotherapy, four cycles of TC (DTX 75 mg/m 2 þ CPA 600 mg/m 2 ) were administered at 3-week intervals. Adverse events were evaluated based on National Cancer Institute Common Terminology Criteria for Adverse Events ver The safety and completion rate were evaluated as the primary and secondary endpoints, respectively. Results: Regarding hematological toxicity, Grade (G) 4 neutropenia occurred in 71.7% and G3 in 26.4%. G3 4 leukopenia developed in 32.1% and 56.6%, respectively, G4 anemia in 1.9% and G1 2 anemia in 26.4%. Regarding non-hematological toxicity, systemic malaise, skin eruption, edema, myalgia, arthralgia and nausea were noted in most patients. The completion rate was 94.3%, dose reduction was necessary in 7.5% and granulocyte colonystimulating factor (G-CSF) support was required in 17.0%. On comparison between patients aged 65 years or older and younger than 65 years, the completion rate, dose reduction and incidence of febrile neutropenia (FN) were higher in the elderly patients. G-CSF support was more often needed in this subgroup. Conclusions: TC therapy is tolerable for Japanese patients, but attention should be paid to the development of FN and neutropenia. The completion rate was lower in the elderly patients, showing that tolerability was not necessarily favorable. Key words: breast cancer docetaxel cyclophosphamide adjuvant therapy safety INTRODUCTION The standard regimen most widely adopted for post-operative adjuvant chemotherapy for breast cancer is combination chemotherapy with drugs including anthracycline. Taxanes are also key drugs of post-operative adjuvant chemotherapy for breast cancer, and the efficacy of taxanes administered in addition to anthracycline regimens has been demonstrated by many randomized control trials (RCTs) (3). The US For reprints and all correspondence: Naruto Taira, Department of Cancer and Thoracic Surgery, Okayama University Graduate School of Medicine, Shikata, Okayama , Japan. ntaira@md.okayama-u.ac.jp oncology 9735 trial (USON9735) was the first RCT in which anthracycline and taxane were directly compared as postoperative adjuvant chemotherapies for breast cancer, and the analytical results of a 7-year median follow-up have been reported (1,2). AC [doxorubicin 60 mg/m 2 i.v. on day 1; cyclophosphamide (CPA) 600 mg/m 2 i.v. on day 1; every 21 days 4 cycles] and TC [docetaxel (DTX) 75 mg/m 2 i.v. on day 1; CPA 600 mg/m 2 i.v. on day 1; every 21 days 4 cycles] were compared as post-operative adjuvant chemotherapies for Stages I, II and III resectable invasive breast cancer. The primary endpoints were disease-free survival (DFS) and overall survival (OS). The lymph node metastasis # The Author (2009). Published by Oxford University Press. All rights reserved.
2 Jpn J Clin Oncol 2009;39(8) 479 positivity rate was 50% in the patients, and 16% of the patients were 65 years of age or older. DFS was 81% in the TC group and 75% in the AC group (P ¼ 0.033), and OS was 87% in the former and 82% in the latter (P ¼ 0.032), showing that TC therapy was significantly superior regarding the two parameters. Concerning the safety profile, the incidence of febrile neutropenia (FN) was slightly higher in the TC than in the AC group, but long-term bone marrow toxicity and cardiotoxicity were low, showing that the therapy was feasible. It was also reported that the tolerability of elderly patients at 65 years of age or older was favorable, showing the superiority of TC therapy. Based on these, the standard post-operative adjuvant chemotherapy for earlystage breast cancer may change from the current regimens including anthracyclines to taxane-based regimens without anthracycline. There are racial differences in the effects and adverse effects of chemotherapy. The standard regimens to administer many therapeutic drugs for breast cancer employed in Western countries are also applicable for Japanese, but the recommended doses of some drugs established by Phase II dose-setting studies conducted in Japan are lower than those in Western countries. The standard dose of DTX for every 3-week administration in monotherapy is 100 mg/m 2 in Western countries, but 70 mg/m 2 in Japan. Moreover, there is no safety data concerning the combination of DTX and CPA in Japan. To introduce the TC regimen (75/600) adopted in the USON9735 into Japan, the confirmation of its safety in Japanese is essential. Based on this background, we performed a study to confirm the safety of the TC regimen (75/600) of the USON9735. PATIENTS AND METHODS Of patients who underwent radical surgery for primary breast cancer at the Shikoku Cancer Center and Okayama University Hospital, those who met the following inclusion criteria were selected: an age between 20 and 70 years, and a risk category of intermediate or higher employing the 10th St Gallen risk classification assessed based on the clinical background and post-operative pathological diagnosis, i.e. hormone receptor-negative cases, lymph node metastasispositive cases and lymph node metastasis-negative cases, hormone receptor-positive cases meeting one of the following conditions: a 2 cm or greater diameter of tissue invasion, histological grade of 2 3, 35 years of age or younger, the presence of severe vascular invasion and HER2-positivity. Estrogen (ER) and progesterone receptors were assessed by immunostaining, and a positive cell rate of 10% or higher was regarded as positive. HER2 was assessed by the Hercep test, and scores of 0 and 1þ were regarded as negative, and 3þ as positive. In cases graded 2þ, the HER2/neu amplification rate was determined, and a 2.2 or higher rate was regarded as positive. Other inclusion criteria were the absence of distant metastasis and severe complications with a performance status of 0 or 1 and sufficient bone marrow, liver and renal functions. Written informed consent was obtained from all patients. Patients with pre-operative chemotherapy, a past medical history of drug allergy which may interfere with the therapy, inflammatory and bilateral breast cancers, double cancer and a past medical history of psychiatric diseases were excluded. In the administration, after pre-treatment with 8 mg dexamethasone and 5-hydroxytryptamine (HT) 3 receptor blockade, 75 mg/m 2 DTX was administered by drip infusion for 60 min, followed by the administration of 600 mg/m 2 CPA for 30 min on day 1. From 12 h later, oral dexamethasone 4 mg was administrated twice daily for 2 days. These were administered every 21 days four times (four cycles). Blood testing was performed on the day of administration in each cycle to decide on the next administration. The criteria for initiating administration were as follows, and administration was postponed until all items recovered: WBC 3000/mm 2, neutrophil count 1500/mm 2,neuropathyGrade (G) 2, edema G2, liver dysfunction G1 and renal dysfunction G1. When these did not recover for 21 days from the scheduled administration day, the protocol was discontinued. When the following adverse reactions were noted in the previous cycle, the first dose reduction was performed based on the dose reduction criteria: (i) G3 or severer nonhematological toxicity, (ii) G4 or severer hematological toxicity excluding leukopenia and neutropenia and (iii) G4 leukopenia and neutropenia persisting for 7 days or longer. The level of first dose reduction was as follows: DTX, 60 mg/m 2 and CPA, 500 mg/m 2. When these adverse reactions were present after the dose reduction, the protocol was discontinued. Regarding supportive therapy, preventive antibiotic administration was prohibited, but administration for FN decided on by the attending physician was accepted. The preventive administration of granulocyte colony-stimulating factor (G-CSF) was also prohibited based on the ASCO 2006 guidelines, but according to the decision by the attending physician, the following administration criteria were accepted: (i) fever (388C) development with a neutrophil count of,1000/mm 2 or a neutrophil count of 500/mm 2 after the completion of drug administration, (ii) when an identical chemotherapy is employed after meeting the condition (i), the subsequent administration starts when the neutrophil count reaches 1000/mm 2. The primary endpoint was set as the safety. The types and grades of adverse reactions were identified following the National Cancer Institute (NCI) Common Terminology Criteria for Adverse Events (CTCAE) ver. 3.0, and the incidences of G3 or severer adverse reactions were evaluated. The secondary endpoint was set as the protocol treatment completion rate. During the protocol treatment period, the body weight and temperature were measured, and blood testing was performed to investigate adverse reactions once a week at the outpatient clinic. Expecting of the number of patients in our institutions for a year who correspond to inclusion criteria, the target number of enrollments was set
3 480 Feasibility study of TC for Japanese breast cancer patients to 50. This study was approved by the Institutional Review Board. The standard treatment arm in the USON9735 was AC (60/600), and the tolerability against this regimen has been reported and widely adopted in Japan. The dose of TC superior to AC shown by this trial should be accepted from a dose density viewpoint. Although a dose-setting study is necessary for the safety confirmation of translational combination therapy, the initial dose was set to TC (75/600). To ensure the safety of patients, an early stopping rule was established, in which enrollment was suspended after five early cases were enrolled until the completion of the protocol treatment in all five cases, and adverse reactions were evaluated. When the following adverse reactions were noted in two or more of the five cases, the study protocol was reviewed: (i) G3 or severer edema, (ii) G3 or severer peripheral neuropathy, (iii) FN, (iv) other G4 hematological toxicity and (iv) discontinuation of the protocol treatment due to an adverse reaction. The adverse event profiles of the five cases were submitted to the Effect/Safety Evaluation Committee to examine the feasibility of study continuation. RESULTS Enrollment was initiated in May 2007, and the five early cases were enrolled by July The protocol treatment was completed in four of the five cases, clearing the early stopping rule. Continuation of the study without protocol revision was approved by the Effect/Safety Evaluation Committee. Enrollment was re-started in September 2007, 53 were registered by October 2008 and the protocol treatment of the 53 cases was completed by January Adverse events could be adequately assessed in all patients. The clinicopathological background factors of the patients are shown in Table 1. The median age was 54 years (33 67 years) and five patients (9.4%) were 65 years of age or older. Thirty-eight cases (71.7%) were ER-positive, 12 (22.6%) were HER2-positive, the mean tumor size was 1.94 cm ( cm), and 22 cases (41.5%) were lymph node metastasis-positive, with a mean number of lymph node metastases of 1.4 (1 3). The protocol treatment was completed in 50 of the 53 cases, with a completion rate of 94.3%. The protocol was discontinued in three due to fatigue, skin eruption, G4 leukopenia and neutropenia based on the judgment by the attending physician or patient s request. One was a 62-year-old female in whom G4 leukopenia and neutropenia occurred after the first cycle, and the dose was reduced following the dose reduction criteria in the second cycle, but her attending physician decided on discontinuation due to G4 hematological toxicity. The second case was a 67-year-old female in whom G4 leukopenia and neutropenia and G2 fatigue developed following the first cycle, and the treatment was discontinued based on the patient s request. The third case was a 61-year-old female in whom G4 leukopenia and neutropenia Table 1. Patients characteristics Category n % Age, Median age 54 (33 67) Menopause Pre Post ER þ PgR þ HER2 Positive Negative T T T T N Nuclear grade Number of pn Risk category Intermediate High Surgery Bp Bt ER, estrogen receptor; PgR, progesterone receptor; pn, pathological N; Bp, breast conserving; Bt, mastectomy.
4 Jpn J Clin Oncol 2009;39(8) 481 Table 2. Hematologic toxicity Table 3. Non-hematologic toxicity Grade Grade n % n % n % n % Neutropenia Leucopenia Febrile neutropenia Anemia andg3systemicskineruptiondevelopedfollowingthefirst cycle, and her attending physician decided on the discontinuation. Dose reduction conflicting with the dose reduction criteria was necessary in four cases (7.5%). On hematological toxicity evaluation following the NCI-CTCAE, G3 4 leukopenia developed in 47 (88.7%), G3 4 neutropenia in 52 (98.1%) and FN in 15 (28.3%). G-CSF was administered to nine (17.0%). G4 anemia occurred in one (1.9%) (Table 2). Regarding non-hematological toxicity, hair loss occurred in most patients, and G2 or milder fatigue in 42 (79.2%). Edema occurred in 13 (24.5%), but all were G1, and could be resolved by diuretic treatment. G2 or milder arthralgia and myalgia occurred in 20 (37.8%) and 21 (39.7%), respectively. Peripheral neuropathy developed in 12 (22.7%), but the severity was G2 or milder (Table 3). As another non-hematological toxicity, skin eruption accompanied by pruritus appeared at a high incidence. In one case (1.9%), systemic skin eruption developed and was graded G3. As subgroup analysis by age, the patients were divided into those aged 65 years or older and those younger than 65 years, as in the USON9735. Dose reduction was necessary in 2 of 48 patients younger than 65 years (4.2%), and 2 of 5 patients aged 65 years or older (40%). All patients in the younger group completed the protocol treatment, whereas only two of the five patients (40%) completed the treatment in the elderly group, with higher dose reduction rate, decreasing the completion rate. FN developed in 11 (22.9%) in the younger group and 4 (80%) in the elderly group, showing that the incidence of FN was also higher, and G-CSF support was more often needed in the elderly patients (Table 4). DISCUSSION Although the importance of systemic drug therapy to improve the prognosis of breast cancer is widely recognized, combination chemotherapy including anthracycline has been employed as the standard post-operative adjuvant chemotherapy after initial cyclophosphamide, methotrexate, 5-FU n % n % n % Fatigue Aiopeicia Arthralgia Myalgia Nausea Vomiting Constipation Diarrhea Edema GOT, GPT Nail change Rash Stomatitis Watery eye Neuropathy Cystitis GOT, glutamic oxaloacetic transaminase; GPT, glutamic pyruvic transaminase. Table 4. Summary by age group 65 (n ¼ 5),65 (n ¼ 48) Completion rate 40% 100% Dose reduction 40% 4.2% G-CSF support 40% 14.6% Febrile neutropenia 80% 22.9% G-CSF, granulocyte colony-stimulating factor. therapy (4 6). Many clinical studies have since been performed, and the efficacy of additional taxane administration for lymph node metastasis-positive and -negative high-risk cases was demonstrated, which attracted attention to taxanes for post-operative adjuvant therapy (7,8). Although the efficacy of anthracyclines was established, the development of cardiotoxicity and myelodysplasia as late adverse effects was often problematic. An increase in the incidence of cardiotoxicity to 4 18% in a cumulative dose-dependent manner has been reported (9). Three fatal cases due to heart disease and osteomyelodysplasia syndrome were also reported in the USON9735, for which the involvement of adriamycin could not be ruled out because of the administration of the AC arm alone (1). As HER2 and Topo IIa gene aberrations attract attention as anthracycline efficacy predicting factors, the
5 482 Feasibility study of TC for Japanese breast cancer patients individualized administration of anthracycline in consideration of these predictive factors may also progress in the future (10,11). In addition, a recurrence-inhibitory effect of trastuzumab in HER2-overexpressing patients has been demonstrated, and the frequency of combining trastuzumab with cytotoxic drugs or consecutive administration has increased, with which the usefulness of taxanes with lowerlevel cardiotoxic adverse effects has been increasing (12,13). As the superiority of TC to AC therapy was demonstrated in the USON9735 (1,2), taxane regimens not including anthracycline may become a major trend in the future, and this trend may not be ignored in Japan. Regarding the safety, although the 9735 trial reported favorable tolerability (1), it is well known that there exists ethnic or racial difference in pharmacokinetics and pharmacodynamics. These have been attributed to the distinctions in the genetics, physiological and pathological factors. Moreover, these differences are also known to be influenced by several extrinsic factors such as socioeconomic backgrounds, culture, diet and environments (14,15). Therefore, the verification of tolerability and adverse effects is an important clinical task to introduce TC therapy into Japan. This is the first report on the safety of TC therapy in Japanese patients. The overall completion rate was 94.3%, similar to that (93%) in the USON9735. The protocol treatment was discontinued in three cases (5.7%). Dose reduction was necessary in 7.5%. The dose intensities of DTX and CPA were 98.5% and 98.7%, respectively. The completion rate was mostly favorable, and fewer cases required dose reduction, but hematological toxicity: G3 4 leucopenia and neutropenia occurred in almost all cases. In the USON9735, the incidence of G3 4 neutropenia was 61%, slightly lower than that in the present study, but this difference may have been due to variation in the observation interval: every 3 weeks in the 9735 trial, whereas weekly in our study to closely observe adverse effects. Since the safety of TC therapy in Japanese was confirmed by this study, observation every 3 weeks and on the administration days may be sufficient for actual clinical practice. The incidence of FN in all cases was reported to be 5% in the USON9735, but attention should be paid to the fact that the administration of prophylactic antibiotics was accepted in the USON9735. No prophylactic administration was performed in our study, and the incidence was 28.3%. FN could be controlled by oral antibiotics in most cases, but G-CSF administration was necessary in 17%. Regarding hematological toxicity in AC therapy (60/600 mg/m 2 ), Tsutani et al. (16) reported that G3 4 neutropenia occurred in 24.3% and FN in 3.8% in Japanese. Based on these findings, the incidences of hematological toxicity and FN are apparently higher in TC than in AC therapy, to which closer attention should be paid. For actual clinical cases, prophylactic antibiotics administration may be considered. Regarding non-hematological toxicity, G2 or milder edema developed in 34% in the USON9735, whereas the grade was G1 or milder, and the incidence was only 24.5% in our study. Diuretics were administered to some cases, but most cases remitted under course observation alone. The incidences of nausea and vomiting were 35.9% and 7.5%, respectively, lower than those in the USON9735 (53% and 14%, respectively). Another non-hematological toxicity mentioned was skin eruption. The incidences of G1, G2 and G3 skin eruption were 34%, 18.9% and 1.9%, respectively, 55% in total. Skin eruption persisted after the completion of four cycles in some cases. The establishment of effective countermeasures against skin eruption in TC therapy is necessary. Regarding DTX-induced skin eruption, although several cases have been reported, no therapy has been established, and only symptomatic therapy is available (17 19). The incidence in DTX monotherapy is reported to be 20 48%, suggesting that the combination with CPA increases the rate of development (20). The subgroup analysis by age in the 9735 trial concluded that the incidence of adverse effects in elderly patients aged 65 years or older was not significantly different, and the tolerability of the elderly patients was favorable (1). In contrast, in our study, because of the small sample size, statistical comparison was not performed, the protocol treatment completion rate was lower in the patients aged 65 years or older than in those younger than 65 years (40% vs. 100%), the dose reduction rate was higher (40% vs. 4.2%) and the incidence of FN was higher (80% vs. 22.9%) (Table 4). Although the number of patients was small, it cannot be concluded that TC therapy is applicable for patients aged 65 years or older. Loibl et al. (21) investigated tolerability against taxane-based adjuvant therapy by age, in which the incidences of leukopenia and neutropenia increased with age, but the incidence of FN was similar. Regarding nonhematological toxicity, there was no age-related difference in the incidence of G1 2 fatigue, but the incidence of G3 4 fatigue was significantly higher in the elderly patients. Regarding skin eruption, there was no age-related difference in the incidence of G1 2, but that of G3 or severer skin eruption was significantly higher in the elderly patients (21). Although simple comparison with TC in the above reports is difficult because the regimen was different, these previous reports may support our study results regarding the feasibility of taxane-containing regimens for elderly patients. No significant difference was noted in non-hematological toxicity between the age groups, which may have been due to the small number of patients. This study confirmed that TC therapy can be safely performed in Japanese. Regarding hematological toxicity, since FN developed at a relatively high rate (28.3%), the use of prophylactic antibiotics should be considered. Regarding non-hematological toxicity, no severe edema developed, but skin eruption accompanied by pruritus appeared in about half of the patients, for which the establishment of supportive therapy may be necessary. On profiling adverse effects by age, the incidence of hematological toxicity markedly increased in patients aged 65 years or older, decreasing the treatment completion rate. The tolerability of patients aged
6 Jpn J Clin Oncol 2009;39(8) years or older is not favorable, and administration should be carefully decided upon. Conflict of interest statement None declared. References 1. Jones S, Holmes FA, O shaughnessy J, Blum JL, Vukelja SJ, McIntyre KJ, et al. Docetaxel with cyclophosphamide is associated with an overall survival benefit compared with doxorubicin and cyclophosphamide: 7-year follow-up of US Oncology Research Trial J Clin Oncol 2009;27: Jones SE, Savin MA, Holmes FA, O shaughnessy JA, Blum JL, Vukelja S, et al. Phase III trial comparing doxorubicin plus cyclophosphamide with docetaxel plus cyclophosphamide as adjuvant therapy for operable breast cancer. J Clin Oncol 2006;24: De Laurentiis M, Cancello G, D Agostino D, Giuliano M, Giordano A, Montagna E, et al. Taxane-based combinations as adjuvant chemotherapy of early breast cancer: a meta-analysis of randomized trials. J Clin Oncol 2008;26: Bonadonna G, Brusamolino E, Valagussa P, Rossi A, Brugnatelli L, Brambilla C, et al. Combination chemotherapy as an adjuvant treatment in operable breast cancer. N Engl J Med 1976;294: Early Breast Cancer Trialists Collaborative G. Effects of chemotherapy and hormonal therapy for early breast cancer on recurrence and 15-year survival: an overview of the randomised trials. Lancet 2005;365: Fisher B, Brown AM, Dimitrov NV, Poisson R, Redmond C, Margolese RG, et al. Two months of doxorubicin-cyclophosphamide with and without interval reinduction therapy compared with 6 months of cyclophosphamide, methotrexate, and fluorouracil in positive-node breast cancer patients with tamoxifen-nonresponsive tumors: results from the National Surgical Adjuvant Breast and Bowel Project B-15. J Clin Oncol 1990;8: Martin M, Pienkowski T, Mackey J, Pawlicki M, Guastalla JP, Weaver C, et al. Adjuvant docetaxel for node-positive breast cancer. N Engl J Med 2005;352: Roche H, Fumoleau P, Spielmann M, Canon JL, Delozier T, Serin D, et al. Sequential adjuvant epirubicin-based and docetaxel chemotherapy for node-positive breast cancer patients: the FNCLCC PACS 01 Trial. J Clin Oncol 2006;24: Singal PK, Iliskovic N. Doxorubicin-induced cardiomyopathy. N Engl J Med 1998;339: Di Leo A, Gancberg D, Larsimont D, Tanner M, Jarvinen T, Rouas G, et al. HER-2 amplification and topoisomerase IIalpha gene aberrations as predictive markers in node-positive breast cancer patients randomly treated either with an anthracycline-based therapy or with cyclophosphamide, methotrexate, and 5-fluorouracil. Clin Cancer Res 2002;8: Gennari A, Pronzato P. New understanding of the role of anthracyclines in early-stage breast cancer: patient selection considerations. Clin Breast Cancer 2008;8(Suppl 4):S Romond EH, Perez EA, Bryant J, Suman VJ, Geyer CE, Jr, Davidson NE, et al. Trastuzumab plus adjuvant chemotherapy for operable HER2-positive breast cancer. N Engl J Med 2005;353: Smith I, Procter M, Gelber RD, Guillaume S, Feyereislova A, Dowsett M, et al. 2-year follow-up of trastuzumab after adjuvant chemotherapy in HER2-positive breast cancer: a randomised controlled trial. Lancet 2007;369: International Conference on Harmonisation; guidance on ethnic factors in the acceptability of foreign clinical data; availability FDA (Notice). Fed Regist 1998;63: Chen ML. Ethnic or racial differences revisited: impact of dosage regimen and dosage form on pharmacokinetics and pharmacodynamics. Clin Pharmacokinet 2006;45: Tsutani Y, Saeki T, Aogi K, Ohsumi S, Takashima S. Toxicity of doxorubicin and cyclophosphamide (60 mg/600 mg/m 2 )inadjuvant chemotherapy for breast cancer. GanToKagakuRyoho2005;32: Baker J, Ajani J, Scotte F, Winther D, Martin M, Aapro MS, et al. Docetaxel-related side effects and their management. Eur J Oncol Nurs 2008;12: Chew L, Lee Chuen VS. Cutaneous reaction associated with weekly docetaxel administration. J Oncol Pharm Pract Moisidis C, Mobus V. Erythema multiforme major following docetaxel. Arch Gynecol Obstet 2005;271: Cortes JE, Pazdur R. Docetaxel. J Clin Oncol 1995;13: Loibl S, von Minckwitz G, Harbeck N, Janni W, Elling D, Kaufmann M, et al. Clinical feasibility of (neo)adjuvant taxane-based chemotherapy in older patients: analysis of.4500 patients from four German randomized breast cancer trials. Breast Cancer Res 2008;10:R77.
Docetaxel. Class: Antineoplastic agent, Antimicrotubular, Taxane derivative.
 Docetaxel Class: Antineoplastic agent, Antimicrotubular, Taxane derivative. Indications: -Breast cancer: -Non small cell lung cancer -Prostate cancer -Gastric adenocarcinoma _Head and neck cancer Unlabeled
Docetaxel Class: Antineoplastic agent, Antimicrotubular, Taxane derivative. Indications: -Breast cancer: -Non small cell lung cancer -Prostate cancer -Gastric adenocarcinoma _Head and neck cancer Unlabeled
Non-Anthracycline Adjuvant Therapy: When to Use?
 Northwestern University Feinberg School of Medicine Non-Anthracycline Adjuvant Therapy: When to Use? William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley Center for
Northwestern University Feinberg School of Medicine Non-Anthracycline Adjuvant Therapy: When to Use? William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley Center for
Treatment of HER-2 positive breast cancer
 EJC SUPPLEMENTS 6 (2008) 21 25 available at www.sciencedirect.com journal homepage: www.ejconline.com Treatment of HER-2 positive breast cancer Matteo Clavarezza, Marco Venturini * Ospedale Sacro Cuore
EJC SUPPLEMENTS 6 (2008) 21 25 available at www.sciencedirect.com journal homepage: www.ejconline.com Treatment of HER-2 positive breast cancer Matteo Clavarezza, Marco Venturini * Ospedale Sacro Cuore
Nadia Harbeck Breast Center University of Cologne, Germany
 Evidence in Favor of Taxane Based Combinations and No Anthracycline in Adjuvant and Metastatic Settings Nadia Harbeck Breast Center University of Cologne, Germany Evidence in Favor of Taxane Based Combinations
Evidence in Favor of Taxane Based Combinations and No Anthracycline in Adjuvant and Metastatic Settings Nadia Harbeck Breast Center University of Cologne, Germany Evidence in Favor of Taxane Based Combinations
AC-DOCE Regimen. AC-DOCE+TRAS Regimen AC-DOCE AC-DOCE+TRAS. A - Regimen Name. Disease Site Breast. Adjuvant. Regimen Category. Evidence-Informed :
 Regimen Monograph Regimen Name Drug Regimen Cycle Frequency Premedication and Supportive Measures Dose Modifications Adverse Effects Interactions Drug Administration and Special Precautions Recommended
Regimen Monograph Regimen Name Drug Regimen Cycle Frequency Premedication and Supportive Measures Dose Modifications Adverse Effects Interactions Drug Administration and Special Precautions Recommended
OPTIMIZING NONANTHRACYLINES FOR EARLY BREAST CANCER. Stephen E. Jones, M.D. US Oncology Research, McKesson Specialty Health The Woodlands, Tx
 OPTIMIZING NONANTHRACYLINES FOR EARLY BREAST CANCER Stephen E. Jones, M.D. US Oncology Research, McKesson Specialty Health The Woodlands, Tx ANTHRACYCLINES AND TAXANES ARE COMMONLY USED USED IN MOST REGIMENS
OPTIMIZING NONANTHRACYLINES FOR EARLY BREAST CANCER Stephen E. Jones, M.D. US Oncology Research, McKesson Specialty Health The Woodlands, Tx ANTHRACYCLINES AND TAXANES ARE COMMONLY USED USED IN MOST REGIMENS
Use of Taxanes in Older Breast Cancer Patients
 SIOG Guidelines Update 2014: Use of Taxanes in Older Breast Cancer Patients Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Fundamental steps Task Force (TF) on
SIOG Guidelines Update 2014: Use of Taxanes in Older Breast Cancer Patients Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Fundamental steps Task Force (TF) on
TRANSPARENCY COMMITTEE OPINION. 15 February 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 February 2006 Taxotere 20 mg, concentrate and solvent for solution for infusion B/1 vial of Taxotere and 1 vial
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 February 2006 Taxotere 20 mg, concentrate and solvent for solution for infusion B/1 vial of Taxotere and 1 vial
Toxicities of Chemotherapy Regimens used in Early Breast Cancer
 Toxicities of Chemotherapy Regimens used in Early Breast Cancer CERCIT Workshop February 17, 2012 Carlos H Barcenas, M.D., M.S. Fellow Hematology-Oncology MD Anderson Cancer Center CERCIT Scholar Outline
Toxicities of Chemotherapy Regimens used in Early Breast Cancer CERCIT Workshop February 17, 2012 Carlos H Barcenas, M.D., M.S. Fellow Hematology-Oncology MD Anderson Cancer Center CERCIT Scholar Outline
Breast Pathway Group TC (Docetaxel / Cyclophosphamide) in Early Breast Cancer
 Breast Pathway Group TC (Docetaxel / Cyclophosphamide) in Early Breast Cancer Indication: Neoadjuvant or adjuvant treatment for patients in whom anthracyclines are contraindicated or inappropriate Regimen
Breast Pathway Group TC (Docetaxel / Cyclophosphamide) in Early Breast Cancer Indication: Neoadjuvant or adjuvant treatment for patients in whom anthracyclines are contraindicated or inappropriate Regimen
BCCA Protocol Summary for Adjuvant Therapy for Breast Cancer Using Fluorouracil, Epirubicin and Cyclophosphamide and DOCEtaxel
 BCCA Protocol Summary for Adjuvant Therapy for Breast Cancer Using Fluorouracil, Epirubicin Cyclophosphamide DOCEtaxel Protocol Code Tumour Group Contact Physician BRAJFECD Breast Dr. Stephen Chia ELIGIBILITY:
BCCA Protocol Summary for Adjuvant Therapy for Breast Cancer Using Fluorouracil, Epirubicin Cyclophosphamide DOCEtaxel Protocol Code Tumour Group Contact Physician BRAJFECD Breast Dr. Stephen Chia ELIGIBILITY:
The legally binding text is the original French version
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 29 November 2006 TAXOTERE 20 mg, concentrate and solvent for infusion in single-dose vials of 7 ml, individually packed
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 29 November 2006 TAXOTERE 20 mg, concentrate and solvent for infusion in single-dose vials of 7 ml, individually packed
BRLAACDT. Protocol Code. Breast. Tumour Group. Dr. Karen Gelmon. Contact Physician
 BCCA Protocol Summary for Treatment of Locally Advanced Breast Cancer using DOXOrubicin and Cyclophosphamide followed by DOCEtaxel and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group Contact Physician
BCCA Protocol Summary for Treatment of Locally Advanced Breast Cancer using DOXOrubicin and Cyclophosphamide followed by DOCEtaxel and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group Contact Physician
Vinorelbine, methotrexate and fluorouracil (VMF) as first-line therapy in metastatic breast cancer: a randomized phase II trial
 Original article Annals of Oncology 14: 699 703, 2003 DOI: 10.1093/annonc/mdg199 Vinorelbine, methotrexate and fluorouracil (VMF) as first-line therapy in metastatic breast cancer: a randomized phase II
Original article Annals of Oncology 14: 699 703, 2003 DOI: 10.1093/annonc/mdg199 Vinorelbine, methotrexate and fluorouracil (VMF) as first-line therapy in metastatic breast cancer: a randomized phase II
Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer
 Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer Angelo Di Leo «Sandro Pitigliani» Medical Oncology Unit Hospital of Prato Istituto Toscano Tumori Prato, Italy NOAH: Phase III, Open-Label Trial
Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer Angelo Di Leo «Sandro Pitigliani» Medical Oncology Unit Hospital of Prato Istituto Toscano Tumori Prato, Italy NOAH: Phase III, Open-Label Trial
New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer
 New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
Adjuvant Chemotherapy + Trastuzumab
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Chemotherapy + Trastuzumab (Optimal Drugs / Dosage / Trastuzumab) Adjuvant Chemotherapy (Optimal Drugs / Optimal Dosage
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Chemotherapy + Trastuzumab (Optimal Drugs / Dosage / Trastuzumab) Adjuvant Chemotherapy (Optimal Drugs / Optimal Dosage
Breast Pathway Group EC x 4 Docetaxel x 4: Epirubicin & Cyclophosphamide followed by Docetaxel in Early Breast Cancer
 Breast Pathway Group EC x 4 Docetaxel x 4: Epirubicin & Cyclophosphamide followed by Docetaxel in Early Breast Indication: Neoadjuvant therapy for high risk and fit breast cancer patients suitable for
Breast Pathway Group EC x 4 Docetaxel x 4: Epirubicin & Cyclophosphamide followed by Docetaxel in Early Breast Indication: Neoadjuvant therapy for high risk and fit breast cancer patients suitable for
Chemotherapy of Breast Cancer
 Japan - Taiwan Joint Symposium on Medical Oncology Session 7 Breast cancer journal homepage:www.cos.org.tw/web/index.asp Chemotherapy of Breast Cancer Mei-Ching Liu Department of Medicine, Koo Foundation
Japan - Taiwan Joint Symposium on Medical Oncology Session 7 Breast cancer journal homepage:www.cos.org.tw/web/index.asp Chemotherapy of Breast Cancer Mei-Ching Liu Department of Medicine, Koo Foundation
Relative dose intensity delivered to patients with early breast cancer: Canadian experience
 M E D I C A L O N C O L O G Y Relative dose intensity delivered to patients with early breast cancer: Canadian experience S. Raza MD, S. Welch MD, and J. Younus MD ABSTRACT Adjuvant chemotherapy for early
M E D I C A L O N C O L O G Y Relative dose intensity delivered to patients with early breast cancer: Canadian experience S. Raza MD, S. Welch MD, and J. Younus MD ABSTRACT Adjuvant chemotherapy for early
Breast Pathway Group EC x 4 Paclitaxel x 4 (3-weekly): Epirubicin & Cyclophosphamide x 4 followed by Paclitaxel x 4 (3-weekly) in Early Breast Cancer
 Breast Pathway Group EC x 4 Paclitaxel x 4 (3-weekly): Epirubicin & Cyclophosphamide x 4 followed by Paclitaxel x Indication: Neoadjuvant or adjuvant therapy for moderate to high risk node positive breast
Breast Pathway Group EC x 4 Paclitaxel x 4 (3-weekly): Epirubicin & Cyclophosphamide x 4 followed by Paclitaxel x Indication: Neoadjuvant or adjuvant therapy for moderate to high risk node positive breast
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1
 Important data from BCIRG 006 Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1 in the adjuvant treatment of HER2+ breast
Important data from BCIRG 006 Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1 in the adjuvant treatment of HER2+ breast
Adjuvant Systemic Therapy in Early Stage Breast Cancer
 Adjuvant Systemic Therapy in Early Stage Breast Cancer Julie R. Gralow, M.D. Director, Breast Medical Oncology Jill Bennett Endowed Professor of Breast Cancer Professor, Global Health University of Washington
Adjuvant Systemic Therapy in Early Stage Breast Cancer Julie R. Gralow, M.D. Director, Breast Medical Oncology Jill Bennett Endowed Professor of Breast Cancer Professor, Global Health University of Washington
Key Words. Adjuvant therapy Breast cancer Taxanes Anthracyclines
 The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
Breast Cancer Earlier Disease. Stefan Aebi Luzerner Kantonsspital
 Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Clinical Expert Submission Template
 Clinical Expert Submission Template Thank you for agreeing to give us a personal statement on your view of the technology and the way it should be used in the NHS. Health care professionals can provide
Clinical Expert Submission Template Thank you for agreeing to give us a personal statement on your view of the technology and the way it should be used in the NHS. Health care professionals can provide
BREAST CANCER RISK REDUCTION (PREVENTION)
 BREAST CANCER RISK REDUCTION (PREVENTION) Articles Anastrozole for prevention of breast cancer in high-risk postmenopausal women (IBIS-II): an international, double-blind, randomised placebo-controlled
BREAST CANCER RISK REDUCTION (PREVENTION) Articles Anastrozole for prevention of breast cancer in high-risk postmenopausal women (IBIS-II): an international, double-blind, randomised placebo-controlled
Clinical Impact of primary prophylaxis for FN in breast cancer patients. Prof. Young Jin Suh The Catholic University of Korea
 Clinical Impact of primary prophylaxis for FN in breast cancer patients Prof. Young Jin Suh The Catholic University of Korea Objectives Describe the prevalence of febrile neutropenia in patients with breast
Clinical Impact of primary prophylaxis for FN in breast cancer patients Prof. Young Jin Suh The Catholic University of Korea Objectives Describe the prevalence of febrile neutropenia in patients with breast
NCCP Chemotherapy Regimen. DOXOrubicin, Cyclophosphamide (AC 60/600) 21 day followed by weekly PACLitaxel (80) and weekly Trastuzumab Therapy (AC-TH)
 DOXOrubicin, Cyclophosphamide (AC 60/600) 21 day followed by weekly PACLitaxel (80) and weekly Trastuzumab Therapy (AC-TH) Note: There is an option for Dose Dense DOXOrubicin, cyclophosphamide PACLitaxel
DOXOrubicin, Cyclophosphamide (AC 60/600) 21 day followed by weekly PACLitaxel (80) and weekly Trastuzumab Therapy (AC-TH) Note: There is an option for Dose Dense DOXOrubicin, cyclophosphamide PACLitaxel
In HER2+ breast cancer: 2 INDICATIONS. PERJETA + Herceptin-based therapy dosing durations 1 CONTINUE UNTIL PROGRESSION OR UNACCEPTABLE TOXICITY
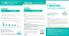 Recommended dosing for PERJETA + Herceptin-based treatment in HER2+ METASTATIC breast cancer TREAT HER 2 PROGRESSION OR UNACCEPTABLE TOXICITY METASTATIC: Administer every 3 weeks until disease progression
Recommended dosing for PERJETA + Herceptin-based treatment in HER2+ METASTATIC breast cancer TREAT HER 2 PROGRESSION OR UNACCEPTABLE TOXICITY METASTATIC: Administer every 3 weeks until disease progression
NCCP Chemotherapy Regimen
 Dose Dense DOXOrubicin, Cyclophosphamide (AC 60/600) 14 day followed by PACLitaxel (175) 14 day and Trastuzumab Therapy (DD AC-TH) Note: There is an option for Dose Dense DOXOrubicin, cyclophosphamide
Dose Dense DOXOrubicin, Cyclophosphamide (AC 60/600) 14 day followed by PACLitaxel (175) 14 day and Trastuzumab Therapy (DD AC-TH) Note: There is an option for Dose Dense DOXOrubicin, cyclophosphamide
Adjuvant chemotherapy of breast cancer
 Journal of BUON 10: 175-180, 2005 2005 Zerbinis Medical Publications. Printed in Greece REVIEW ARTICLE Adjuvant chemotherapy of breast cancer S. Bešlija Department of Medical Oncology, Institute of Oncology,
Journal of BUON 10: 175-180, 2005 2005 Zerbinis Medical Publications. Printed in Greece REVIEW ARTICLE Adjuvant chemotherapy of breast cancer S. Bešlija Department of Medical Oncology, Institute of Oncology,
Adjuvant Chemotherapy for Elderly Women with Breast Cancer: Matti S. Aapro, M.D. IMO Clinique de Genolier Switzerland
 SIOG Berlin October 2009 Adjuvant Chemotherapy for Elderly Women with Breast Cancer: Immediate Benefit and Long-Term Risk Matti S. Aapro, M.D. IMO Clinique de Genolier Switzerland 1 2 BACKGROUND MESSAGE
SIOG Berlin October 2009 Adjuvant Chemotherapy for Elderly Women with Breast Cancer: Immediate Benefit and Long-Term Risk Matti S. Aapro, M.D. IMO Clinique de Genolier Switzerland 1 2 BACKGROUND MESSAGE
Prophylaxis of febrile neutropenia :experiences with adjuvant TAC
 Prophylaxis of febrile neutropenia :experiences with adjuvant TAC 30 th Apr, 2016 Jihyoun Lee Breast center, Department of Surgery Soonchunhyang University Hospital Chemotherapy and the risk of febrile
Prophylaxis of febrile neutropenia :experiences with adjuvant TAC 30 th Apr, 2016 Jihyoun Lee Breast center, Department of Surgery Soonchunhyang University Hospital Chemotherapy and the risk of febrile
Docetaxel-EC: Docetaxel followed by Epirubicin / Cyclophosphamide in Breast Cancer
 Docetaxel-EC: Docetaxel followed by Epirubicin / Cyclophosphamide in Breast Cancer Indication: Neoadjuvant therapy f HER 2 negative high risk and fit Breast Cancer patients, suitable f a taxane containing
Docetaxel-EC: Docetaxel followed by Epirubicin / Cyclophosphamide in Breast Cancer Indication: Neoadjuvant therapy f HER 2 negative high risk and fit Breast Cancer patients, suitable f a taxane containing
Docetaxel plus Cyclophosphamide as Adjuvant Therapy for Early, Operable Breast Cancer
 CED-SOS Advice Report 9 EDUCATION AND INFORMATION 2012 Docetaxel plus Cyclophosphamide as Adjuvant Therapy for Early, Operable Breast Cancer M. Trudeau and J. Franek A Quality Initiative of the Program
CED-SOS Advice Report 9 EDUCATION AND INFORMATION 2012 Docetaxel plus Cyclophosphamide as Adjuvant Therapy for Early, Operable Breast Cancer M. Trudeau and J. Franek A Quality Initiative of the Program
METRIC Study Key Eligibility Criteria
 The METRIC Study METRIC Study Key Eligibility Criteria The pivotal METRIC Study is evaluating glembatumumab vedotin in patients with gpnmb overexpressing metastatic triple-negative breast cancer (TNBC).
The METRIC Study METRIC Study Key Eligibility Criteria The pivotal METRIC Study is evaluating glembatumumab vedotin in patients with gpnmb overexpressing metastatic triple-negative breast cancer (TNBC).
Received: 4 September 2010 / Accepted: 17 September 2010 / Published online: 14 October 2010 Ó Springer Science+Business Media, LLC.
 Breast Cancer Res Treat (2011) 125:115 120 DOI 10.1007/s10549-010-1187-2 CLINICAL TRIAL Adjuvant dose-dense doxorubicin plus cyclophosphamide followed by dose-dense nab-paclitaxel is safe in women with
Breast Cancer Res Treat (2011) 125:115 120 DOI 10.1007/s10549-010-1187-2 CLINICAL TRIAL Adjuvant dose-dense doxorubicin plus cyclophosphamide followed by dose-dense nab-paclitaxel is safe in women with
Health Industry Forum October 2, 2007 Scott Howell, MD Senior Director, Channel and Contracting Strategy Genentech
 1 Cost Effectiveness & Pricing/Reimbursement A Biotech Case Study Health Industry Forum October 2, 2007 Scott Howell, MD Senior Director, Channel and Contracting Strategy Genentech Disclaimer 2 The views
1 Cost Effectiveness & Pricing/Reimbursement A Biotech Case Study Health Industry Forum October 2, 2007 Scott Howell, MD Senior Director, Channel and Contracting Strategy Genentech Disclaimer 2 The views
Horizon Scanning Centre November Vinflunine (Javlor) monotherapy for advanced breast cancer SUMMARY NIHR HSC ID: 7887
 Horizon Scanning Centre November 2012 Vinflunine (Javlor) monotherapy for advanced breast cancer SUMMARY NIHR HSC ID: 7887 This briefing is based on information available at the time of research and a
Horizon Scanning Centre November 2012 Vinflunine (Javlor) monotherapy for advanced breast cancer SUMMARY NIHR HSC ID: 7887 This briefing is based on information available at the time of research and a
FDA APPROVES HERCEPTIN FOR THE ADJUVANT TREATMENT OF HER2-POSITIVE NODE-POSITIVE BREAST CANCER
 NEWS RELEASE Media Contact: Kimberly Ocampo (650) 467-0679 Investor Contact: Sue Morris (650) 225-6523 Advocacy Contact: Ajanta Horan (650) 467-1741 FDA APPROVES HERCEPTIN FOR THE ADJUVANT TREATMENT OF
NEWS RELEASE Media Contact: Kimberly Ocampo (650) 467-0679 Investor Contact: Sue Morris (650) 225-6523 Advocacy Contact: Ajanta Horan (650) 467-1741 FDA APPROVES HERCEPTIN FOR THE ADJUVANT TREATMENT OF
BRAJACTTG. Protocol Code. Breast. Tumour Group. Dr. Karen Gelmon. Contact Physician
 BC Cancer Protocol Summary for Adjuvant Therapy for Breast Cancer Using Dose Dense Therapy: DOXOrubicin and Cyclophosphamide Followed by PACLitaxel and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group
BC Cancer Protocol Summary for Adjuvant Therapy for Breast Cancer Using Dose Dense Therapy: DOXOrubicin and Cyclophosphamide Followed by PACLitaxel and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group
Lo Studio Geparsepto. Alessandra Fabi Oncologia Medica 1
 Lo Studio Geparsepto Alessandra Fabi Oncologia Medica 1 nab-paclitaxel Versus Solvent-Based Paclitaxel in Neoadjuvant Chemotherapy for Early Breast Cancer (GeparSepto GBG 69): A Randomised, Phase III Trial
Lo Studio Geparsepto Alessandra Fabi Oncologia Medica 1 nab-paclitaxel Versus Solvent-Based Paclitaxel in Neoadjuvant Chemotherapy for Early Breast Cancer (GeparSepto GBG 69): A Randomised, Phase III Trial
Sequential Dose-Dense Adjuvant Therapy With Doxorubicin, Paclitaxel, and Cyclophosphamide
 Sequential Dose-Dense Adjuvant Therapy With Doxorubicin, Paclitaxel, and Cyclophosphamide Review Article [1] April 01, 1997 By Clifford A. Hudis, MD [2] The recognition of paclitaxel's (Taxol's) activity
Sequential Dose-Dense Adjuvant Therapy With Doxorubicin, Paclitaxel, and Cyclophosphamide Review Article [1] April 01, 1997 By Clifford A. Hudis, MD [2] The recognition of paclitaxel's (Taxol's) activity
FDA Briefing Document Oncologic Drugs Advisory Committee Meeting. September 12, sbla /51 Pertuzumab (PERJETA ) Applicant: Genentech, Inc.
 /51 FDA Briefing Document Oncologic Drugs Advisory Committee Meeting September 12, 2013 /51 Pertuzumab (PERJETA ) Applicant: Genentech, Inc. Disclaimer: The attached package contains background information
/51 FDA Briefing Document Oncologic Drugs Advisory Committee Meeting September 12, 2013 /51 Pertuzumab (PERJETA ) Applicant: Genentech, Inc. Disclaimer: The attached package contains background information
BRAJACTT. Protocol Code. Breast. Tumour Group. Dr. Karen Gelmon. Contact Physician
 BC Cancer Protocol Summary for Adjuvant Therapy for Breast Cancer using DOXOrubicin and Cyclophosphamide followed by PACLitaxel and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group Contact Physician
BC Cancer Protocol Summary for Adjuvant Therapy for Breast Cancer using DOXOrubicin and Cyclophosphamide followed by PACLitaxel and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group Contact Physician
Weekly Paclitaxel for Metastatic Breast Cancer in Patients Previously Exposed to Paclitaxel
 www.journalofcancerology.com PERMANYER J Cancerol. 0;:-9 JOURNAL OF CANCEROLOGY CLINICAL CASE Weekly Paclitaxel for Metastatic Breast Cancer in Patients Previously Exposed to Paclitaxel Benjamín Dávalos-Félix,
www.journalofcancerology.com PERMANYER J Cancerol. 0;:-9 JOURNAL OF CANCEROLOGY CLINICAL CASE Weekly Paclitaxel for Metastatic Breast Cancer in Patients Previously Exposed to Paclitaxel Benjamín Dávalos-Félix,
BIOLOGICAL THERAPIES FOR BREAST CANCER Updates from the 2005 San Antonio Breast Cancer Symposium
 Emerging trends and recommendations BIOLOGICAL THERAPIES FOR BREAST CANCER Updates from the 2005 San Antonio Breast Cancer Symposium Joseph Ragaz, MD, FRCPC Top-line summary Here, Oncology Exchange presents
Emerging trends and recommendations BIOLOGICAL THERAPIES FOR BREAST CANCER Updates from the 2005 San Antonio Breast Cancer Symposium Joseph Ragaz, MD, FRCPC Top-line summary Here, Oncology Exchange presents
EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY. Dr. Carlos Garbino
 EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY Dr. Carlos Garbino EARLY BREAST CANCER ADJUVANT CHEMOTHERAPY SUSTANTIVE DIFFICULTIES FOR A WORLDWIDE APPLICABILITY DUE TO IMPORTANT INEQUALITIES + IN DIFFERENT
EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY Dr. Carlos Garbino EARLY BREAST CANCER ADJUVANT CHEMOTHERAPY SUSTANTIVE DIFFICULTIES FOR A WORLDWIDE APPLICABILITY DUE TO IMPORTANT INEQUALITIES + IN DIFFERENT
Novel Preoperative Therapies for HER2-Positive Breast Cancer. Debu Tripathy, MD University of Southern California Norris Comprehensive Cancer Center
 Novel Preoperative Therapies for HER2-Positive Breast Cancer Debu Tripathy, MD University of Southern California Norris Comprehensive Cancer Center Key Findings to Date in the Neoadjuvant Therapy of HER2+
Novel Preoperative Therapies for HER2-Positive Breast Cancer Debu Tripathy, MD University of Southern California Norris Comprehensive Cancer Center Key Findings to Date in the Neoadjuvant Therapy of HER2+
Breast Pathway Group Epirubicin & Cyclophosphamide x 4 followed by Carboplatin & Paclitaxel x 4 for Early Breast Cancer
 Breast Pathway Group Epirubicin & Cyclophosphamide x 4 followed by Carboplatin & Paclitaxel x 4 for Early Breast Cancer Indication: Neoadjuvant therapy for patients with BRCA1/2 mutations EC Regimen details:
Breast Pathway Group Epirubicin & Cyclophosphamide x 4 followed by Carboplatin & Paclitaxel x 4 for Early Breast Cancer Indication: Neoadjuvant therapy for patients with BRCA1/2 mutations EC Regimen details:
Breast Pathway Group Docetaxel in Advanced Breast Cancer
 Breast Pathway Group Docetaxel in Advanced Breast Cancer Indication: First-line palliative treatment, with or without trastuzumab, for advanced breast cancer in patients for whom an anthracycline is not
Breast Pathway Group Docetaxel in Advanced Breast Cancer Indication: First-line palliative treatment, with or without trastuzumab, for advanced breast cancer in patients for whom an anthracycline is not
A case of male inflammatory breast cancer
 Int Canc Conf J (2013) 2:183 187 DOI 10.1007/s13691-013-0087-9 CASE REPORT A case of male inflammatory cancer Miki Hyakudomi Toko Inao Yoshimitsu Minari Masayuki Itakura Riruke Maruyama Yoshitsugu Tajima
Int Canc Conf J (2013) 2:183 187 DOI 10.1007/s13691-013-0087-9 CASE REPORT A case of male inflammatory cancer Miki Hyakudomi Toko Inao Yoshimitsu Minari Masayuki Itakura Riruke Maruyama Yoshitsugu Tajima
Anthracyclines in the elderly breast cancer patients
 Anthracyclines in the elderly breast cancer patients Etienne GC Brain, MD PhD Medical Oncology Centre René Huguenin, Saint-Cloud & Group GERICO, FNCLCC, Paris Centre René Huguenin - Saint-Cloud Facts about
Anthracyclines in the elderly breast cancer patients Etienne GC Brain, MD PhD Medical Oncology Centre René Huguenin, Saint-Cloud & Group GERICO, FNCLCC, Paris Centre René Huguenin - Saint-Cloud Facts about
Evolving Insights into Adjuvant Chemotherapy. Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology
 Evolving Insights into Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic
Evolving Insights into Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic
In first-line HER2+ METASTATIC breast cancer TREAT HER 2 PROGRESSION OR UNACCEPTABLE TOXICITY
 In first-line HER2+ METASTATIC breast cancer TREAT HER 2 PROGRESSION OR UNACCEPTABLE TOXICITY The most common adverse reactions (>30) with PERJETA in combination with trastuzumab and docetaxel were diarrhea,
In first-line HER2+ METASTATIC breast cancer TREAT HER 2 PROGRESSION OR UNACCEPTABLE TOXICITY The most common adverse reactions (>30) with PERJETA in combination with trastuzumab and docetaxel were diarrhea,
Considerations in Adjuvant Chemotherapy. Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology
 Considerations in Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic Treatment
Considerations in Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic Treatment
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012
 Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER
 Contact: Anne Bancillon + 33 (0)6 70 93 75 28 STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER Key results of 42 nd annual meeting of the American Society of Clinical
Contact: Anne Bancillon + 33 (0)6 70 93 75 28 STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER Key results of 42 nd annual meeting of the American Society of Clinical
DR. BOMAN N. DHABHAR Consulting Oncologist Jaslok Hospital, Fortis Hospital Mulund, Wockhardt Hospital Mumbai & BND Onco Centre INDIA
 Recent Advances of Docetaxel in Management of Breast Cancer DR. BOMAN N. DHABHAR Consulting Oncologist Jaslok Hospital, Fortis Hospital Mulund, Wockhardt Hospital Mumbai & BND Onco Centre INDIA 1 ADJUVANT
Recent Advances of Docetaxel in Management of Breast Cancer DR. BOMAN N. DHABHAR Consulting Oncologist Jaslok Hospital, Fortis Hospital Mulund, Wockhardt Hospital Mumbai & BND Onco Centre INDIA 1 ADJUVANT
EC (Epirubicin Cyclophosphamide) Adjuvant/Neo-adjuvant regimen
 y Systemic Anti Cancer Treatment Protocol EC (Epirubicin Cyclophosphamide) Adjuvant/Neo-adjuvant regimen PROTOCOL REF: MPHAECANBR (Version No: 1.0) Approved for use in: ER positive, HER2 negative ( Luminal
y Systemic Anti Cancer Treatment Protocol EC (Epirubicin Cyclophosphamide) Adjuvant/Neo-adjuvant regimen PROTOCOL REF: MPHAECANBR (Version No: 1.0) Approved for use in: ER positive, HER2 negative ( Luminal
HIGHLIGHTS OF PRESCRIBING INFORMATION
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use PERJETA safely and effectively. See full prescribing information for PERJETA. PERJETA (pertuzumab)
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use PERJETA safely and effectively. See full prescribing information for PERJETA. PERJETA (pertuzumab)
J Clin Oncol 27: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 27 NUMBER 8 MARCH 1 29 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Docetaxel With Cyclophosphamide Is Associated With an Overall Survival Benefit Compared With Doxorubicin and Cyclophosphamide:
VOLUME 27 NUMBER 8 MARCH 1 29 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Docetaxel With Cyclophosphamide Is Associated With an Overall Survival Benefit Compared With Doxorubicin and Cyclophosphamide:
Receiving PERJETA + Herceptinbased therapy * after surgery
 Treatment after surgery for HER2+ early breast cancer that has a high risk of coming back Receiving PERJETA + Herceptinbased therapy * after surgery PERJETA is part of an FDA-approved treatment regimen
Treatment after surgery for HER2+ early breast cancer that has a high risk of coming back Receiving PERJETA + Herceptinbased therapy * after surgery PERJETA is part of an FDA-approved treatment regimen
Novel Chemotherapy Agents for Metastatic Breast Cancer. Joanne L. Blum, MD, PhD Baylor-Sammons Cancer Center Dallas, TX
 Novel Chemotherapy Agents for Metastatic Breast Cancer Joanne L. Blum, MD, PhD Baylor-Sammons Cancer Center Dallas, TX New Chemotherapy Agents in Breast Cancer New classes of drugs Epothilones Halichondrin
Novel Chemotherapy Agents for Metastatic Breast Cancer Joanne L. Blum, MD, PhD Baylor-Sammons Cancer Center Dallas, TX New Chemotherapy Agents in Breast Cancer New classes of drugs Epothilones Halichondrin
BC Cancer Protocol Summary for Adjuvant Therapy for Breast Cancer Using DOCEtaxel, CARBOplatin, and Trastuzumab (HERCEPTIN)
 BC Cancer Protocol Summary for Adjuvant Therapy for Breast Cancer Using DOCEtaxel, CARBOplatin, and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group Contact Physician BRAJDCARBT Breast Dr. Susan Ellard
BC Cancer Protocol Summary for Adjuvant Therapy for Breast Cancer Using DOCEtaxel, CARBOplatin, and Trastuzumab (HERCEPTIN) Protocol Code Tumour Group Contact Physician BRAJDCARBT Breast Dr. Susan Ellard
Anthracyclines for Breast Cancer? Are Adjuvant Anthracyclines Dispensible? Needs to be Answered in a Large Prospective Trial
 Anthracyclines for Breast Cancer? Are Adjuvant Anthracyclines Dispensible? Needs to be Answered in a Large Prospective Trial Joanne L. Blum, MD, PhD Baylor-Sammons Cancer Dallas, TX Early Breast Cancer
Anthracyclines for Breast Cancer? Are Adjuvant Anthracyclines Dispensible? Needs to be Answered in a Large Prospective Trial Joanne L. Blum, MD, PhD Baylor-Sammons Cancer Dallas, TX Early Breast Cancer
National Horizon Scanning Centre. Bevacizumab (Avastin) in combination with non-taxanes for metastatic breast cancer - first line therapy
 Bevacizumab (Avastin) in combination with non-taxanes for metastatic breast cancer - first line therapy December 2007 This technology summary is based on information available at the time of research and
Bevacizumab (Avastin) in combination with non-taxanes for metastatic breast cancer - first line therapy December 2007 This technology summary is based on information available at the time of research and
Contemporary Chemotherapy-Based Strategies for First-Line Metastatic Breast Cancer
 Contemporary Chemotherapy-Based Strategies for First-Line Metastatic Breast Cancer Hope S. Rugo, MD Professor of Medicine Director, Breast Oncology and Clinical Trials Education University of California
Contemporary Chemotherapy-Based Strategies for First-Line Metastatic Breast Cancer Hope S. Rugo, MD Professor of Medicine Director, Breast Oncology and Clinical Trials Education University of California
Treatment of Early-Stage HER2+ Breast Cancer
 Treatment of Early-Stage HER2+ Breast Cancer Chau T. Dang, MD Chief, MSK Westchester Medical Oncology Service Breast Medicine Service Memorial Sloan Kettering Cancer Center Disclosures I have research
Treatment of Early-Stage HER2+ Breast Cancer Chau T. Dang, MD Chief, MSK Westchester Medical Oncology Service Breast Medicine Service Memorial Sloan Kettering Cancer Center Disclosures I have research
Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
 JBUON 2018; 23(4): 877-882 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
JBUON 2018; 23(4): 877-882 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
30 TH ANNUAL SAN ANTONIO BREAST CANCER SYMPOSIUM (SABCS) NEW ADVANCES IN THE TREATMENT OF BREAST CANCER
 EDUCATIONAL HIGHLIGHTS FROM DATA PRESENTED AT THE 30 TH ANNUAL SAN ANTONIO BREAST CANCER SYMPOSIUM (SABCS) NEW ADVANCES IN THE TREATMENT OF BREAST CANCER DECEMBER 13 16, 2007, SAN ANTONIO, TX, USA 2 CONTENTS
EDUCATIONAL HIGHLIGHTS FROM DATA PRESENTED AT THE 30 TH ANNUAL SAN ANTONIO BREAST CANCER SYMPOSIUM (SABCS) NEW ADVANCES IN THE TREATMENT OF BREAST CANCER DECEMBER 13 16, 2007, SAN ANTONIO, TX, USA 2 CONTENTS
DR LUIS MANSO UNIDAD TUMORES DE MAMA Y GINECOLÓGICOS HOSPITAL 12 DE OCTUBRE MADRID
 DR LUIS MANSO UNIDAD TUMORES DE MAMA Y GINECOLÓGICOS HOSPITAL 12 DE OCTUBRE MADRID RESUMEN DE ARTICULOS THERESA BOLERO 3 NOAH UP-DATE GEPAR SIXTO RADIOTHERAPY EBCTCG CTCs MISCELANEAS Lancet Oncol 2014;
DR LUIS MANSO UNIDAD TUMORES DE MAMA Y GINECOLÓGICOS HOSPITAL 12 DE OCTUBRE MADRID RESUMEN DE ARTICULOS THERESA BOLERO 3 NOAH UP-DATE GEPAR SIXTO RADIOTHERAPY EBCTCG CTCs MISCELANEAS Lancet Oncol 2014;
Metronomic chemotherapy for breast cancer
 Metronomic chemotherapy for breast cancer M. Colleoni International Breast Cancer Study Group (IBCSG), Division of Medical Senology, European Institute of Oncology Metronomic Scheduling and Inhibition
Metronomic chemotherapy for breast cancer M. Colleoni International Breast Cancer Study Group (IBCSG), Division of Medical Senology, European Institute of Oncology Metronomic Scheduling and Inhibition
Copyright, 1995, by the Massachusetts Medical Society
 Copyright, 99, by the Massachusetts Medical Society Volume 332 APRIL 6, 99 Number ADJUVANT CYCLOPHOSPHAMIDE, METHOTREXATE, AND FLUOROURACIL IN NODE- POSITIVE BREAST CANCER The Results of Years of Follow-up
Copyright, 99, by the Massachusetts Medical Society Volume 332 APRIL 6, 99 Number ADJUVANT CYCLOPHOSPHAMIDE, METHOTREXATE, AND FLUOROURACIL IN NODE- POSITIVE BREAST CANCER The Results of Years of Follow-up
新竹馬偕紀念醫院癌症中心 乳癌化學治療藥物處方
 新竹馬偕紀念醫院癌症中心 乳癌化學治療藥物處方 文件修訂記錄 修正次數 修正日期 修正版別 修 改 內 容 1 2011.04.07 1.0 初次訂定 2 2013.05.08 2.0 修訂 3 2013.04.30 3.0 修訂 :Triple-Negative Breast Cancer 處方 新增 :Neoadjuvant-p7~8 4 2014.04.29 4.0 修訂 :FEC + Trastuzumab
新竹馬偕紀念醫院癌症中心 乳癌化學治療藥物處方 文件修訂記錄 修正次數 修正日期 修正版別 修 改 內 容 1 2011.04.07 1.0 初次訂定 2 2013.05.08 2.0 修訂 3 2013.04.30 3.0 修訂 :Triple-Negative Breast Cancer 處方 新增 :Neoadjuvant-p7~8 4 2014.04.29 4.0 修訂 :FEC + Trastuzumab
TJ ISSN Introduction SHORT COMMUNICATION
 TJ ISSN 0300-8916 Tumori 2017; 103(1): e4-e8 DOI: 10.5301/tj.5000543 SHORT COMMUNICATION Efficacy and safety of vinorelbine-capecitabine oral metronomic combination in elderly metastatic breast cancer
TJ ISSN 0300-8916 Tumori 2017; 103(1): e4-e8 DOI: 10.5301/tj.5000543 SHORT COMMUNICATION Efficacy and safety of vinorelbine-capecitabine oral metronomic combination in elderly metastatic breast cancer
Policy No: dru281. Medication Policy Manual. Date of Origin: September 24, Topic: Perjeta, pertuzumab. Next Review Date: May 2015
 Medication Policy Manual Topic: Perjeta, pertuzumab Committee Approval Date: May 9, 2014 Policy No: dru281 Date of Origin: September 24, 2012 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Topic: Perjeta, pertuzumab Committee Approval Date: May 9, 2014 Policy No: dru281 Date of Origin: September 24, 2012 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
NCCP Chemotherapy Regimen
 INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 21 days Regimen *Reimbursement INDICATION ICD10 Code Status HER2 positive metastatic breast cancer (MBC) C50 00200a Hospital HER2 positive early breast
INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 21 days Regimen *Reimbursement INDICATION ICD10 Code Status HER2 positive metastatic breast cancer (MBC) C50 00200a Hospital HER2 positive early breast
EC-Docetaxel: Epirubicin / Cyclophosphamide followed by Docetaxel in Breast Cancer
 EC-Docetaxel: Epirubicin / Cyclophosphamide followed by Docetaxel in Breast Cancer Indication: Neoadjuvant therapy f high risk and fit Breast Cancer patients, suitable f a taxane containing regimen EC
EC-Docetaxel: Epirubicin / Cyclophosphamide followed by Docetaxel in Breast Cancer Indication: Neoadjuvant therapy f high risk and fit Breast Cancer patients, suitable f a taxane containing regimen EC
Breast Cancer Breast Managed Clinical Network
 Initial Evaluation Clinical Stage Pre-Treatment Evaluation Treatment and pathological stage Less than 4 positive lymph nodes Adjuvant Treatment ER Positive HER2 Negative (see page 2 & 3 ) HER2 Positive
Initial Evaluation Clinical Stage Pre-Treatment Evaluation Treatment and pathological stage Less than 4 positive lymph nodes Adjuvant Treatment ER Positive HER2 Negative (see page 2 & 3 ) HER2 Positive
Adjuvant chemotherapy in older breast cancer patients: how to decide?
 Adjuvant chemotherapy in older breast cancer patients: how to decide? H. Wildiers University Hospitals Leuven Belgium Wildiers H, Kunkler I, Lancet Oncol 2007 Biganzoli L, Wildiers H, Lancet Oncol. 2012
Adjuvant chemotherapy in older breast cancer patients: how to decide? H. Wildiers University Hospitals Leuven Belgium Wildiers H, Kunkler I, Lancet Oncol 2007 Biganzoli L, Wildiers H, Lancet Oncol. 2012
Phase II Study of Weekly Albumin-Bound Paclitaxel for Patients with Metastatic Breast Cancer Heavily Pretreated with Taxanes
 original contribution Phase II Study of Weekly Albumin-Bound for Patients with Metastatic Breast Cancer Heavily Pretreated with Taxanes Joanne L. Blum,1-3 Michael A. Savin,2,3 Gerald Edelman,2,3 John E.
original contribution Phase II Study of Weekly Albumin-Bound for Patients with Metastatic Breast Cancer Heavily Pretreated with Taxanes Joanne L. Blum,1-3 Michael A. Savin,2,3 Gerald Edelman,2,3 John E.
original article introduction original article
 Annals of Oncology 22: 1999 2006, 2011 doi:10.1093/annonc/mdq713 Published online 7 March 2011 PREPARE trial: a randomized phase III trial comparing preoperative, dose-dense, dose-intensified chemotherapy
Annals of Oncology 22: 1999 2006, 2011 doi:10.1093/annonc/mdq713 Published online 7 March 2011 PREPARE trial: a randomized phase III trial comparing preoperative, dose-dense, dose-intensified chemotherapy
Postoperative Adjuvant Chemotherapies. Stefan Aebi Luzerner Kantonsspital
 Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
The next wave of successful drug therapy strategies in HER2-positive breast cancer. Hans Wildiers University Hospitals Leuven Belgium
 The next wave of successful drug therapy strategies in HER2-positive breast cancer Hans Wildiers University Hospitals Leuven Belgium Trastuzumab in 1st Line significantly improved the prognosis of HER2-positive
The next wave of successful drug therapy strategies in HER2-positive breast cancer Hans Wildiers University Hospitals Leuven Belgium Trastuzumab in 1st Line significantly improved the prognosis of HER2-positive
Incidence of taxane-induced pain and distress in patients receiving chemotherapy for early-stage breast cancer: a retrospective, outcomes-based survey
 MEDICAL ONCOLOGY Incidence of taxane-induced pain and distress in patients receiving chemotherapy for early-stage breast cancer: a retrospective, outcomes-based survey S. Saibil MD PhD,* B. Fitzgerald
MEDICAL ONCOLOGY Incidence of taxane-induced pain and distress in patients receiving chemotherapy for early-stage breast cancer: a retrospective, outcomes-based survey S. Saibil MD PhD,* B. Fitzgerald
Activity of Combination Chemotherapy, Docetaxel and Epirubicin as Neoadjuvant Therapy for Women with Breast Cancer
 Activity of Combination Chemotherapy, Docetaxel and Epirubicin as Neoadjuvant Therapy for Women with Breast Cancer ARAFAT TFAYLI 1, JENNIFER HOLTER 1, ABBY BOVA 1, SIDDHARTHA VENKATAPPA 2, SUSIE BULLOCK
Activity of Combination Chemotherapy, Docetaxel and Epirubicin as Neoadjuvant Therapy for Women with Breast Cancer ARAFAT TFAYLI 1, JENNIFER HOLTER 1, ABBY BOVA 1, SIDDHARTHA VENKATAPPA 2, SUSIE BULLOCK
Accelerated approval of Perjeta for neoadjuvant use also converted to full approval
 Media Release Basel, 21 December 2017 FDA approves Roche s Perjeta (pertuzumab) for adjuvant treatment of specific type of early breast cancer Accelerated approval of Perjeta for neoadjuvant use also converted
Media Release Basel, 21 December 2017 FDA approves Roche s Perjeta (pertuzumab) for adjuvant treatment of specific type of early breast cancer Accelerated approval of Perjeta for neoadjuvant use also converted
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Herceptin) Reference Number: ERX.SPA.42 Effective Date: 07.01.16 Last Review Date: 05/17 Line of Business: Commercial [Prescription Drug Plan] Revision Log See Important Reminder at the
Clinical Policy: (Herceptin) Reference Number: ERX.SPA.42 Effective Date: 07.01.16 Last Review Date: 05/17 Line of Business: Commercial [Prescription Drug Plan] Revision Log See Important Reminder at the
Trastuzumab (IV) Monotherapy - 7 days
 INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 7 days Regimen *Reimbursement INDICATION ICD10 Code Status Treatment of patients with HER2 positive metastatic breast cancer (MBC) C50 00201a Hospital
INDICATIONS FOR USE: Trastuzumab (IV) Monotherapy - 7 days Regimen *Reimbursement INDICATION ICD10 Code Status Treatment of patients with HER2 positive metastatic breast cancer (MBC) C50 00201a Hospital
Review Recent advances in systemic therapy Advances in adjuvant systemic chemotherapy of early breast cancer Sara López-Tarruella and Miguel Martín
 Review Recent advances in systemic therapy Advances in adjuvant systemic chemotherapy of early breast cancer Sara López-Tarruella and Miguel Martín Medical Oncology Department, Clínico San Carlos Hospital,
Review Recent advances in systemic therapy Advances in adjuvant systemic chemotherapy of early breast cancer Sara López-Tarruella and Miguel Martín Medical Oncology Department, Clínico San Carlos Hospital,
Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA
 Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA The fascinating history of Herceptin 1981 1985 1987 1990 1992 1998 2000 2005 2006 2008 2011 Murine
Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA The fascinating history of Herceptin 1981 1985 1987 1990 1992 1998 2000 2005 2006 2008 2011 Murine
RESEARCH ARTICLE. Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India
 APJCP.2016.17.6.2995 RESEARCH ARTICLE Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India Dinesh Chandra Doval 1,2 *, P Suresh 1, Rupal Sinha 2, Saud Azam 2, Ullas Batra
APJCP.2016.17.6.2995 RESEARCH ARTICLE Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India Dinesh Chandra Doval 1,2 *, P Suresh 1, Rupal Sinha 2, Saud Azam 2, Ullas Batra
SANDRA M. SWAIN. Washington Cancer Institute, Washington, District of Columbia, USA
 The Oncologist Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast cancer Chemotherapy Taxane Trastuzumab Ki-67
The Oncologist Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast cancer Chemotherapy Taxane Trastuzumab Ki-67
It is a malignancy originating from breast tissue
 59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
Chapter 5 Stage III and IVa disease
 Page 55 Chapter 5 Stage III and IVa disease Overview Concurrent chemoradiotherapy (CCRT) is recommended for stage III and IVa disease. Recommended regimen for the chemotherapy portion generally include
Page 55 Chapter 5 Stage III and IVa disease Overview Concurrent chemoradiotherapy (CCRT) is recommended for stage III and IVa disease. Recommended regimen for the chemotherapy portion generally include
FEC Docetaxel (NEOADJUVANT): Fluorouracil/ Epirubicin/ Cyclophosphamide followed by Docetaxel* in Early Breast Cancer
 FEC Docetaxel (NEOADJUVANT): Fluouracil/ Epirubicin/ Cyclophosphamide followed by Docetaxel* in Early Breast Cancer Please, note that Neoadjuvant FEC-Docetaxel has only been approved f use in QEW Trust
FEC Docetaxel (NEOADJUVANT): Fluouracil/ Epirubicin/ Cyclophosphamide followed by Docetaxel* in Early Breast Cancer Please, note that Neoadjuvant FEC-Docetaxel has only been approved f use in QEW Trust
Objectives for Instrument Validation
 Validation of the Patient Neurotoxicity Questionnaire () During Taxane Chemotherapy in a Phase III Randomized Trial in Patients with Breast Cancer: N-SAS BC 02 Kojiro Shimozuma, MD, PhD 1,2, Yasuo Ohashi,
Validation of the Patient Neurotoxicity Questionnaire () During Taxane Chemotherapy in a Phase III Randomized Trial in Patients with Breast Cancer: N-SAS BC 02 Kojiro Shimozuma, MD, PhD 1,2, Yasuo Ohashi,
