Blood Cell Identification Graded
|
|
|
- Kristian Williams
- 5 years ago
- Views:
Transcription
1 Blood Cell Identification Graded BCK/BCP-11 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Neutrophil, segmented or band Neutrophil with Pelger-Huët nucleus (acquired or congenital) Good Unacceptable The arrowed cell is a segmented/band neutrophil and was correctly identified by 93.8% of referees and 99.1% of participants. Segmented neutrophils have condensed nuclear chromatin and segmented or lobated nuclei (2 to 5 lobes typically). Lobes are connected by a thin filament. 5
2 Blood Cell Identification Graded BCK/BCP-12 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Eosinophil Good The arrowed cell is an eosinophil and was correctly identified by 100% of referees and 99.8% of participants. Eosinophils are typically easily recognized due to their characteristic coarse, orange-red granules of uniform size. These granules exhibit a refractile appearance and typically do not overlie the nucleus of the cell. The nucleus is usually segmented into two or more lobes separated by a thin filament, with lobes being of equal size and exhibit the same nuclear characteristics as neutrophilic leukocytes. 6
3 Blood Cell Identification Graded BCK/BCP-13 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Monocyte Good Macrophage Unacceptable The arrowed cell is a monocyte and was correctly identified by 93.8% of referees and 97.6% of participants. Slightly larger than neutrophils, monocytes are usually round but may exhibit cytoplasmic extensions. The cytoplasm of monocytes is abundant and gray to gray-blue and may contain fine azurophilic granules or vacuoles. The nucleus is usually indented and often kidney-bean shaped with condensed chromatin, but less dense than that of a neutrophil or lymphocyte. Macrophages or histiocytes are found in tissues, rather than peripheral blood. 7
4 Blood Cell Identification Graded BCK/BCP-14 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Lymphocyte Good nrbc Unacceptable The arrowed cell is a lymphocyte and was correctly identified by 93.8% of referees and 96.8% of participants. A lymphocyte is a small, round to ovoid cell which may range in size from 7 to 15 μm with variable N:C ratios. While most lymphocytes are small with round to oval nuclei, some normal lymphocytes are medium-sized due to an increased amount of cytoplasm. Chromatin is diffusely dense or coarse and clumped. Nucleoli, if present, are small and inconspicuous. In contrast, 6.2% of referees and 0.3% of participants identified the arrowed cell as a nucleated red blood cell. Nucleated red blood cells have dense round nuclei and pink cytoplasm, rather than the basophilic cytoplasm present in the lymphocyte. 8
5 Blood Cell Identification Graded BCK/BCP-15* BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Lymphoma cell Good Blast cell Unacceptable Monocyte, immature Unacceptable promyelocyte Lymphocyte, reactive Unacceptable Lymphoblast Unacceptable The arrowed cell is a lymphoma cell and was correctly identified by 37.5% of referees and 39.3% of participants. Lymphoma cells may show a variety of morphologic characteristics depending on the underlying type of lymphoma. In this case, the large size of the cell, moderate amount of deeply basophilic cytoplasm, angulated nuclei and prominent nucleoli suggest a large cell lymphoma. These cells can be easily confused with blasts, and additional studies may be necessary to make the correct diagnosis. An accurate clinical history can greatly aid the identification of these cells. In contrast, blast cells have a nucleus with finely reticulated chromatin. Myeloblasts may exhibit a few delicate granules or Auer rods, whereas lymphoblasts often have scant basophilic cytoplasm with nuclei containing finely dispersed chromatin or dense, but not clumped chromatin. See discussion on the following page regarding reactive lymphocytes versus lymphoma cells. * Not graded due to lack of referee and participant consensus. 9
6 Discussion Case History The patient is a 58-year-old male with a history of diffuse large B-cell lymphoma treated 8 months previously, now thought clinically to be in relapse. Hemoglobin=11.1 g/dl, WBC=11.1 x 10 9 /L, PLT=383 x 10 9 /L. This case is an example of a patient with lymphoma, which now involves the peripheral blood. Lymphomas typically start in lymph nodes or extranodal tissues, spreading to adjacent lymph nodes and usually show a predilection for hematopoietic organs, including bone marrow and spleen. Blood involvement by lymphoma typically suggests that the bone marrow is involved by lymphoma. Components of the blood are produced in the bone marrow; therefore, when lymphoma is in the blood, that usually means it is in the bone marrow. Exceptions do exist, such as Sezary syndrome (lymphoma is in the blood, but not in the marrow), which will not be addressed in this discussion. Frequency of peripheral blood involvement by lymphoma depends on the underlying type of lymphoma (See Table 1 on page 14). In a recent study of lymphomas involving the bone marrow, the peripheral blood was involved in 29 percent of cases with available peripheral blood smears for review. In these cases, peripheral blood involvement by lymphoma was associated with higher white blood cell counts (12,000 vs. 5,480/μL, P= [probability or p value]), as well as higher absolute lymphocyte counts (6,840 vs. 1,180/μL; P=0.0005) and higher percentage of lymphocytes (45 vs. 24%, P < ). 1 Unlike acute leukemia, which typically presents with thrombocytopenia and marked anemia, lymphomatous involvement of the blood may minimally affect the hemoglobin and platelet counts, if at all. A bone marrow diagnosis of lymphoma should prompt a careful review of a concurrent peripheral blood smear. In this discussion, features distinguishing reactive lymphocytes from lymphoma cells will be discussed, as well as the morphologic features of lymphomas that commonly involve the peripheral blood. Reactive Lymphocytes versus Lymphoma Distinguishing reactive lymphocytes from lymphoma cells can be challenging, but a number of key features should be kept in mind. First, age of the patient is essential. Many of the lymphomas which involve peripheral blood are much more common in middle aged to elderly adults than children or infants. For example, certain lymphomas (i.e., Burkitt) are more commonly seen in children. Second, accurate clinical history can be critical, since any prior diagnosis of lymphoma can aid in the identification of these cells. Third, a well-prepared and stained peripheral blood smear can be your greatest friend. Old blood and ill prepared samples can lead to misdiagnoses or simply misses. Once you are looking at the peripheral smear, perform a scan at 10X examining the overall slide before going to higher magnification. Reactive lymphocytosis will show a wide range of cellular sizes and shapes. The classic example is infectious mononucleosis (Epstein-Barr viral infection) in which a variety of lymphocytes are seen, ranging from small lymphocytes with round nuclei and condensed chromatin to reactive lymphocytes with abundant pale blue cytoplasm, round to oval nuclei and moderately condensed chromatin. (Images 1 and 2 of reactive lymphs from cases of infectious mononucleosis are seen on the following page.) The cytoplasm of these reactive lymphocytes may hug adjacent red cells and show a basophilic rim at their margins. Immunoblasts are often 10
7 frequently present, being large lymphocytes with round to oval nuclei containing one or more prominent nucleoli. The cytoplasm of an immunoblast is abundant and deeply basophilic. Plasmacytoid lymphocytes may also be seen. In contrast, while reactive lymphocytes are heterogenous, lymphoma cells tend to be homogenous. A peripheral blood smear may contain a subset of lymphoma cells amidst a background of small lymphocytes, but those lymphoma cells will resemble one another. Lymphoma cells can exhibit a variety of morphologic appearances depending on the underlying type of lymphoma, as discussed below. Lymphoma cells can show various sizes and shapes, ranging from 8 to 30 μm in size and nuclear:cytoplasm ratios from 3:1 to 7:1, again depending on the type of lymphoma. Image 1: Reactive lymphocytes (Infectious mononucleosis) Image 2: Reactive lymphocyte (Infectious mononucleosis) (Source: Figure H1-18. In: Glassy EF, ed. Color Atlas of Hematology. Northfield, IL: College of American Pathologists;1998:225.) Splenic Marginal Zone Lymphoma The World Health Organization (WHO) recognizes 3 types of marginal zone lymphomas: splenic, nodal and extranodal. A high frequency of blood involvement by splenic marginal zone lymphoma is well described. 1-3 Splenomegaly, often with anemia or thrombocytopenia, is often accompanied by peripheral blood containing lymphoma cells with villous lymphocytes, in which bipolar cytoplasmic projections are present. These lymphoma cells are larger than typical lymphocytes with abundant pale blue or blue-grey cytoplasm, round to oval nuclei containing condensed chromatin with usually a single nucleolus. (See Image 3: Splenic marginal zone lymphoma on the following page.) However, not all cases of splenic marginal zone lymphoma in the blood will contain lymphoma cells with prominent villi. These morphologic features often overlap with hairy cell leukemia. Hairy cells, in contrast have homogenous chromatin and lack nucleoli, with spiky cytoplasmic projections extending from the entire periphery of the cell. (See Image 4: Hairy cell on the following page.) Immunophenotyping is often necessary to distinguish these two disorders. 11
8 Image 3: Splenic marginal zone lymphoma Image 4: Hairy Cell leukemia; hairy cell is to the left, while a reactive lymphocyte is seen at right. Mantle Cell Lymphoma The high frequency of peripheral blood involvement by mantle cell lymphoma is now being recognized. 4-6 Frequencies as high as 77 percent peripheral blood involvement have been reported. 4 In mantle cell lymphoma, lymphoid cells may range from small to intermediate sized lymphoid cells with irregular nuclear contours to large blast-like cells resembling acute leukemia. Typical mantle cell lymphoma cells are larger than lymphocytes with folded nuclei and a small amount of basophilic cytoplasm. (See Image 5: Mantle cell lymphoma below.) Nuclei, while condensed contain more reticular chromatin, and may contain a single prominent nucleolus resembling prolymphocytes. Blastic or blastoid variants of mantle cell lymphoma are the size of large cell lymphoma cells (20 to 30 μm) and have moderate amount of basophilic cytoplasm, and nuclei while round to oval, may be indented or convoluted. (See Image 6: Mantle cell lymphoma blastic variant below.) Chromatin is less condensed, resembling blastic chromatin, although these lymphoma cells are typically more variable than blasts seen in acute leukemia. Image 5: Mantle cell lymphoma Image 6: Mantle cell lymphoma, blastic variant 12
9 Burkitt Lymphoma Burkitt or Burkitt-like lymphoma cells are morphologically identical to the cells seen in Burkitt leukemia. The distinction rests on whether there is less than or greater than 25 percent bone marrow involvement, respectively. The Burkitt cell is moderate in size (10 to 25 μm) with an oval to round nucleus, moderately coarse chromatin, and 1-3 prominent nucleoli. (See Image 7: Burkitt cell below.) A moderate amount of deeply basophilic cytoplasm is present and typically contains multiple small vacuoles. Burkitt-like lymphoma resembles Burkitt lymphoma, but is accompanied by greater pleomorphism in cell size and shape. Image 7: Burkitt cell Diffuse Large B-cell Lymphoma Surprisingly, a relatively high rate (32 percent) of diffuse large B-cell lymphoma in the blood may be seen, although this is likely underrecognized. 1,7 Large cell lymphomas show some of the most abnormal morphology of the lymphomas. In the past, these lymphomas have been called histiocytic lymphoma or reticulum cell sarcoma, but now are simply termed large cell lymphoma. Immunophenotypic studies are necessary to classify whether these lymphomas are of B-, T- or NK-cell origin. They may resemble a proliferation of immunoblasts with 1-2 prominent nucleoli, or in other cases present with deep convolutions with occasional nucleoli. These cells are large with small to moderate amounts of deeply basophilic cytoplasm, occasionally vacuolated, and often show angulated and folded nuclear contours. (See blood cell images BCK/BCP-11 through 15.) While these cells can be confused with blasts, large cell lymphoma cells vary in size more than blasts and lack the smooth, even chromatin found in blasts. Additional studies such as flow cytometry immunophenotyping or bone marrow biopsy may be necessary for correct identification. Follicular Lymphoma Follicular lymphoma, when it involves the blood, shows a characteristic morphology. These lymphoma cells are slightly bigger than normal lymphocytes with a clefted appearance and moderately coarse chromatin. (See Image 8: Follicular lymphoma on the following page.) Cytoplasm is typically scant, but may be moderate, and the majority of nuclei show folds and convolutions. Nucleoli may be present. Other types of lymphoma cells also show angulated nuclei, including mantle cell lymphoma and Sezary cells. Mantle cell lymphoma cells lack the coarse chromatin of follicular lymphoma and are usually larger in size with gentle 13
10 nuclear folds, not the deep clefts and possible lobes of follicular lymphoma. Sezary cells show convoluted nuclear membranes with a cerebriform appearance and contain dark, hyperchromatic chromatin lacking nucleoli typically. (See Image 9: Sezary cell below.) The distinction among the lymphoma types typically requires immunophenotyping. Image 8: Follicular lymphoma Image 9: Sezary cell (Source: Figure HE-11. In: Glassy EF, ed. Color Atlas of Hematology. Northfield, IL: College of American Pathologists;1998:251.) Table 1. Frequency of Peripheral Blood Involvement by Bone Marrow Lymphoma (adapted from 1 ) Type of lymphoma PB disease /total samples Percentage of PB involvement (%) Marginal zone lymphoma a 8/10 80 High grade lymphoma, NOS b 1/2 50 Mantle cell lymphoma 11/23 48 Burkitt lymphoma 2/5 40 Diffuse large B-cell 12/38 32 lymphoma Mature T-cell & NK-cell lymphomas 6/20 30 Low grade B-cell lymphoma, 5/18 28 NOS b Follicular lymphoma 9/46 20 Lymphoplasmacytic 2/21 10 lymphoma Small lymphocytic 1/10 10 lymphoma c Total 57/ PB=peripheral blood. a. 8 of 9 cases of splenic marginal zone lymphoma showed PB involvement. b. A small number of cases with limited material were classified as high-grade, not otherwise specified and low-grade, not otherwise specified. c. Not meeting criteria for chronic lymphocytic leukemia. 14
11 References 1. Arber DA, George TI. Bone marrow biopsy involvement by non-hodgkin s lymphoma. Frequency of lymphoma types, patterns, blood involvement and discordance with other sites in 450 specimens. Am J Surg Pathol. 2005;29: Isaacson PG, Matutes E, Burke M, et al. The histopathology of splenic lymphoma with villous l ymphocytes. Blood. 1994;84: Kent SA, Variakojis D, Peterson LC. Comparative study of marginal zone lymphoma involving bone marrow. Am J Clin Pathol. 2002;117: Cohen PL, Kurtin PJ, Donovan KA, et al. Bone marrow and peripheral blood involvement in mantle cell lymphoma. Br J Haematol. 1998;101: Matutes E, Parry-Jones N, Brito-Babapulle V, et al. The leukemic presentation of mantle-cell lymphoma: disease features and prognostic factors in 58 patients. Leuk Lymphoma. 2004;45: Wong K-F, Chan JKC, So JCC, et al. Mantle cell lymphoma in leukemic phase: characterization of its broad cytologic spectrum with emphasis on the importance of distinction from other chronic lymphoproliferative disorders. Cancer. 1999;86: Schnitzer B, Kass L. Leukemic phase of reticulum cell sarcoma (histiocytic lymphoma): a clinicopathologic and ultrastructural study. Cancer. 1973;31: Tracy I. George, MD Hematology and Clinical Microscopy Committee 15
12 Blood Cell Identification Ungraded BCK/BCP-16 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Blast cell Educational Myeloblast Educational Lymphoblast Educational The arrowed cell is a blast (or myeloblast). Myeloblasts are the most immature cells in the myeloid series. The myeloblast is a large cell, millimicrons in diameter with a high nuclear to cytoplasmic (N:C ratio), generally round nuclear membranes, a distinct nucleolus and basophilic cytoplasm. The blasts are normally confined to the bone marrow, but may be released into the peripheral blood in malignant and reactive states. 16
13 Blood Cell Identification Ungraded BCK/BCP-17 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Neutrophil, promyelocyte Educational Neutrophil, myelocyte Educational Eosinophil, any stage Educational Neutrophil promyelocyte, abnormal with/without Auer rod(s) Educational The promyelocyte is a round to oval cell that usually is slightly larger than a myeloblast; millimicrons in diameter. Promyelocytes have nuclear to cytoplasmic ratios in the range of 5:1 to 3:1, with fine nuclear chromatin and a single prominent nucleolus. In the basophilic cytoplasm, distinct azurophilic (primary) granules are present. Promyelocytes are confined to the bone marrow, except in pathologic states. 17
14 Blood Cell Identification Ungraded BCK/BCP-18 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Neutrophil, myelocyte Educational The arrowed cell is a myelocyte. Myelocytes are smaller in diameter than the earlier precursors with round to oval nuclei, no nucleoli and chromatin clumping. The cytoplasm is amphophilic with both azurophilic and specific granules present. 18
15 Blood Cell Identification Ungraded BCK/BCP-19 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Neutrophil with toxic granules Educational Neutrophil, segmented or Educational band Neutrophil, dysplastic nucleus Educational Neutrophil necrobiosis (degenerated neutrophil) Educational The leukocytes in the slide are neutrophils/neutrophils with toxic granulation. Neutrophils generally constitute 5-10% of peripheral blood leukocytes. Neutrophils have a nuclear to cytoplasmic ratio of 1:3 with dense nuclear chromatin. The nucleus is segmented or lobated with pale cytoplasm which contains specific granules. Toxic granulation is the presence of large purple or dark blue cytoplasmic granules representing primary granules in the cytoplasm of neutrophils. Toxic changes in neutrophils may be seen in a response to infection, burns, trauma or other acute stimuli. 19
16 Blood Cell Identification Ungraded BCK/BCP-20 BCK BCP Referees Participants Participants Performance Identification No. % No. % No. % Evaluation Neutrophil, toxic (to include toxic granulation and/or Döhle bodies, and/or toxic vacuolization) Neutrophil, segmented or band Neutrophil with Pelger-Huët nucleus (acquired or congenital) Educational Educational Educational The arrowed cell is a neutrophil with a Döhle body. Neutrophils with cytoplasmic Döhle bodies may be seen as a response to various toxic stimuli. Döhle bodies are single or multiple blue or gray-blue cytoplasmic inclusions of variable size and shape. They may be seen in neutrophils, bands, or metamyelocytes. Döhle bodies may be seen in association with neutrophilic toxic granulation or toxic vacuolization. 20
17 Discussion Case History The patient is a 71-year-old Hispanic female with breast cancer. The patient was recently treated and also received G-CSF that was discontinued a couple of days before the blood smear was obtained. Additional laboratory data reveals: White blood cell count =15.2 x 10 9 /L Hemoglobin = 10.0 g/dl Platelets = 325 x 10 9 /L This case demonstrates the peripheral blood cell count and morphologic changes that can be seen in patients who receive recombinant hematopoietic growth factors. Hematopoietic growth factors are proteins that bind to receptors on the cell surface with the primary result of activating cellular proliferation and promoting differentiation and maturation of hematopoietic progenitors. These growth factors are naturally made in the body. Recombinant DNA technology has allowed production of synthetic growth factors, which are now available for use in patients with cytopenias. While different growth factors have varied affects on different cell systems, in general they stimulate lymphocytic, hematopoietic and nonhematopoietic cell lineages. The following is a list of the growth factors that are most commonly used clinically: Granulocyte/colony stimulating factor (G-CSF) Granulocyte/monocyte colony stimulating factor (GM-CSF) Interleukin (IL-3) Erythropoietin Thrombopoietin Granulocyte colony stimulating factor (G-CSF) regulates the proliferation and maturation of neutrophilic granulocytic progenitors by binding to receptors on committed granulocyte precursors. G-CSF also increases the functionality of granulocytes by enhancing granulocytic, monocytic and macrophage cells involved in antigen presentation and cell-mediated immunity. The maturation time of myeloid progenitors in the bone marrow is shortened from 5 days to as little as one day. The gene for G-CSF is located on chromosome 17 (17q11-23). Granulocyte/monocyte colony stimulating factor (GM-CSF) is a potent stimulus for the growth of granulocytic, erythrocytic, macrophage and megakaryocytic progenitors. The GM-CSF receptor is expressed on granulocyte, erythrocyte, megakaryocyte and macrophage progenitor cells, as well as mature neutrophils, monocytes, macrophages, dendritic cells, plasma cells, certain T-lymphocytes, and vascular endothelial cells. Although GM-CSF has greater activity on immature progenitors than does G-CSF, its proliferative effects are less significant than those of interleukin 3 (IL-3). GM-CSF also enhances the function of mature granulocytic cells and monocytes. The gene for GM-CSF is located on chromosome 5 (5q23-31). 21
18 Interleukin-3 also known as multi-csf stimulates the bone marrow stem cells and thereby the growth of granulocytes and monocytes, and to a lesser degree megakaryocytic and erythroid precursors. The gene for IL-3 is located on the long arm of chromosome 5. Erythropoietin (EPO) is the primary regulator for erythropoiesis. EPO stimulates and induces maturation of colony forming units erythroid (CFU-E) and a subset of the burst-forming units erythroid (BFU-E). The gene for EPO is located on chromosome 7. Thrombopoietin is a primary stimulator of megakaryocytic proliferation, causing a significant rise in the platelet count. All of the growth factors work by interacting with specific receptors on target cells. For example: EPO binds to EPO receptors on committed red blood cell precursors GM-CSF and IL-3 bind to receptors on early granulocyte precursors G-CSF binds to receptors on slightly more mature committed granulocytic precursors Due to the diversity in the clinical indications for using hematopoietic growth factors, it is important for laboratory professionals and pathologists to recognize the peripheral blood and bone marrow findings in patients on such factors. Although there is some variability in the peripheral blood findings related to which growth factor the patient has received, peripheral neutrophilia is expected. The growth factors utilize three mechanisms that lead to the increase in neutrophils. These include: demargination of neutrophils from the marginated pool mobilization of the maturation-storage bone marrow compartment increased neutrophil production As a response, the granulocytic series is frequently left-shifted with myeloid elements including blasts, promyelocytes, myelocytes and metamyelocytes present. Challenges BCK/BCP-16, BCK/BCP-17 and BCK/BCP-18 demonstrate a blast (myeloblast), promyelocyte and myelocyte, respectively, which were identified in the peripheral blood of this patient. In addition to the increased number of mature and immature granulocytic elements, toxic changes are frequently seen. Toxic granulation, Döhle bodies and toxic vacuoles, all changes more commonly associated with infection, can be seen as a response to hematopoietic growth factors. Challenges BCK/BCP-19 and BCK/BCP-20 exhibit a neutrophil with toxic granulation and a neutrophil with a Döhle body, respectively. The two major differential diagnostic categories of a peripheral blood granulocytosis include reactive neutrophilia and neoplastic neutrophilia (myeloproliferative disorders). Reactive neutrophilia may be due to a infectious process; as a response to drug or hormonal therapy; in patients with burns, acute trauma or myocardial infarction; in inflammatory disorders such as collagen vascular or other autoimmune disorders; as a response to stress or severe exercise; in pregnancy; in uremic patients; and in patients with acute hemorrhage or hemolysis. In the myeloproliferative disorders the white blood cell count is usually more pronounced than in reactive processes. Chronic myelogenous leukemia (CML) is the most common 22
19 myeloproliferative disorder, with essential thrombocythemia, polycythemia vera, myelofibrosis and chronic myeloproliferative disorder, non-specified completing the list. In some patients a peripheral monocytosis and circulating nucleated red blood cells are also identified as a response to growth factors. Less commonly, dyspoietic myeloid elements are seen as a response to the synthetic growth factors. The dyspoietic features can include cells, which exhibit nuclear-cytoplasmic dyssynchrony and nuclear segmentation defects. In patients with a known diagnosis of acute myeloid leukemia receiving chemotherapy, the distinction of persistent or relapsed leukemia from regenerating bone marrow related to growth factors can be quite challenging. The findings of blasts with Auer rods, the presence of more differentiated myeloid elements, and the presence of erythroid or megakaryocytic elements as would be expected in regeneration, can be helpful in this distinction. However, sometimes ancillary studies, to include cytogenetic analysis and flow cytometric analysis may be necessary to confirm the absence of leukemic blasts. In patients with a known diagnosis of the myelodysplastic syndrome, administration of synthetic growth factor may lead to a left-shift in the myeloid series, raising the concern of transformation of the myelodysplastic syndrome into acute leukemia. Close attention to morphologic details, in conjunction with cytogenetic analysis and flow cytometric analysis may be necessary to make this distinction. Examination of the bone marrow of the patient receiving growth factors reveals panhyperplasia, involving all three cell lines. However, myeloid hyperplasia is most pronounced and can be significantly left-shifted. As the duration of therapy persists, the left-shifted myelopoiesis becomes less pronounced and the myeloid to erythroid ratio typically normalizes. Clinical indications for use of the hematopoietic growth factors have been an area of intense study since their discovery in the mid 1990 s. In addition to reviewing patient s peripheral blood and bone marrow responses to the growth factors, the incidence of neutropenic fever, rate of infections, duration of hospitalization, morbidity and mortality have all been outcomes, which have been reviewed in patients receiving growth factors. In 1994 the American Society of Clinical Oncology issued recommendations for the use of hematopoietic colony-stimulating factors. These clinical practice guidelines have been reviewed with the most recent guidelines released in November The current recommendations are that colony stimulating factors are recommended in some situations: 1. To reduce the likelihood of febrile neutropenia when the expected incidence is >40 percent 2. After documented febrile neutropenia in a prior chemotherapy cycle to avoid infectious complications 3. To maintain dose intensity in subsequent treatment cycles when chemotherapy dose reduction is not appropriate 4. After high-dose chemotherapy with autologous progenitor cell transplantation 23
20 It is not recommended, based on current evidence, that colony stimulating factors should routinely be used in patients with neutropenia who are afebrile. The therapeutic use of CSF in addition to antibiotics at the onset of febrile neutropenia should be reserved for patients at high risk for septic complications. It is not recommended that CSF be used concurrently with chemotherapy and radiation therapy. The clinical indications for use of CSF in the pediatric population are similar. While it is recognized that administering growth factors can significantly shorten the duration of severe neutropenia, however, this does not always lead to shortened hospital stays or decreased rate of infection. Recombinant erythropoietin (epoetin) is recommended in patients with chronic anemias to enhance erythrocyte production. Epoetin is recommended for patients with a chemotherapy-associated anemia who have a hemoglobin < 10.0 g/dl. In some chemotherapy patients, epoetin may be given when the anemia is less severe (<12.0 but >10.0 g/dl). Epoetin is also recommended for patients with chronic renal disease or other chronic disease causing significant anemia. The side effects, adverse reactions, complications of growth factors are generally mild and the drugs are well tolerated. Diarrhea and fluid retention may be seen as a side effect in patients receiving erythropoietin. GM-CSF has a risk of fever, headaches, skin rash, pericardial effusions and medullary bone pain. Medullary bone pain is the most common acute adverse reaction seen in the pediatric population. Bone pain, skin rash, allergic reactions and splenomegaly may be seen in patients receiving G-CSF. Summary As hematopoietic growth factors are frequently used in patients receiving chemotherapy, in patients with the myelodysplastic syndrome, and in patients with chronic anemias, it is important for those in laboratory medicine to recognize the peripheral blood and bone marrow findings related to these agents. 24
21 References 1. Sung L, Nathan PC, Lange B, Beyene J, Buchanan GR. Prophylactic granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor decrease febrile neutropenia after chemotherapy in children with cancer: A meta-analysis of randomized controlled trials. J Clin Onc Aug 15;22(16): American Society of Clinical Oncology. Use of hematopoietic colony-stimulating factors: evidencebased, practice guidelines. J Clin Oncol Nov 20;12: American Society of Clinical Oncology. Recommendations for the use of hematopoietic colonystimulating factors: evidence-based, clinical practice guidelines. J Clin Oncol. 1994;12: Hoelzer D. Hematopoietic growth factors-not whether, but when and where. N Engl J Med Jun 19;336(25): Wagner LM, Furman WL. Haemopoietic growth factors in paediatric oncology. Paediatr Drugs. 2001;3(3): Hartmann LC, Tschetter K, Habermann TM, et al. Granulocyte colon-stimulating factor in severe chemotherapy-induced afebrile neutropenia. N Engl J Med Jun 19;336(25): Schmitz LL, McClure JS, Litz CE, et al. Morphologic and quantitative changes in blood and marrow cells following growth factor therapy. Am J Clin Pathol Jan;101(1): Harris AC, Todd WM, Hackney MH, Ben-Ezra J. Bone marrow changes associated with recombinant granulocyte-macrophage and granulocyte colon-stimulating factors. Discrimination of granulocytic regeneration. Arch Pathol Lab Med Jun;118(6): Orazi A, Gordon MS, John K, Sledge G Jr, Neiman RS, Hoffman R. In vivo effects of recombinant human stem cell factor treatment. Am J Clin Pathol Feb;103(2): Meyerson H, Farhi DC, Rosenthal NS. Transient increase in blasts mimicking acute leukemia and progressing myelodysplasia in patients receiving growth factor. Am J Clin Pathol Jun;109(6): Pitrak DL. Effects of granulocyte colony-stimulating factor and granulocyte macrophage colonystimulating factor on the bactericidal functions of neutrophils. Curr Opin Hematol May;4(3): Glaspy JA, Golde DW. Clinical applications of myeloid growth factors. Semin Hematol Apr;26(2 Suppl 2): Rizzo JD, Lichtin AE, Woolf SH, et al. Use of epoetin in patients with cancer: evidence-based clinical practice guidelines of the American Society of Clinical Oncology and the American Society of Hematology. J Clin Oncol Oct;20(19): Kaushansky K. Lineage Specific hematopoietic growth factors. N Engl J Med May 11;354(19): Deborah A. Perry, MD Hematology and Clinical Microscopy Resource Committee 25
Blood Cell Identification Graded
 BCP-21 Blood Cell Identification Graded Case History The patient is a 37-year-old female with a history of multiple sickle cell crises. She now presents with avascular necrosis of the left hip. Laboratory
BCP-21 Blood Cell Identification Graded Case History The patient is a 37-year-old female with a history of multiple sickle cell crises. She now presents with avascular necrosis of the left hip. Laboratory
Participants Identification No. % Evaluation. Mitotic figure Educational Erythrocyte precursor, abnormal 1 0.
 Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
EDUCATIONAL COMMENTARY DIFFERENTIATING IMMATURE PERIPHERAL BLOOD CELLS
 Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Continuing Education on the left side of the
Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Continuing Education on the left side of the
EDUCATIONAL COMMENTARY MORPHOLOGIC ABNORMALITIES IN LEUKOCYTES
 EDUCATIONAL COMMENTARY MORPHOLOGIC ABNORMALITIES IN LEUKOCYTES Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
EDUCATIONAL COMMENTARY MORPHOLOGIC ABNORMALITIES IN LEUKOCYTES Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
Lymphoma Tumor Board Quiz! Laboratory Hematology: Basic Cell Morphology
 Lymphoma Tumor Board Quiz! Laboratory Hematology: Basic Cell Morphology CABOT RINGS Cabot rings in a patient with hemolytic anemia. Cabot ring (red arrow) and Howell-Jolly body (blue arrow). Observed in
Lymphoma Tumor Board Quiz! Laboratory Hematology: Basic Cell Morphology CABOT RINGS Cabot rings in a patient with hemolytic anemia. Cabot ring (red arrow) and Howell-Jolly body (blue arrow). Observed in
By Dr. Mohamed Saad Daoud
 By Dr. Mohamed Saad Daoud Part I Introduction Types of White Blood Cells Genesis of the White Blood Cells Life Span of the White Blood Cells Dr. Mohamed Saad Daoud 2 Leucocytes Introduction: Infectious
By Dr. Mohamed Saad Daoud Part I Introduction Types of White Blood Cells Genesis of the White Blood Cells Life Span of the White Blood Cells Dr. Mohamed Saad Daoud 2 Leucocytes Introduction: Infectious
VETERINARY HEMATOLOGY ATLAS OF COMMON DOMESTIC AND NON-DOMESTIC SPECIES COPYRIGHTED MATERIAL SECOND EDITION
 VETERINARY HEMATOLOGY ATLAS OF COMMON DOMESTIC AND NON-DOMESTIC SPECIES SECOND EDITION COPYRIGHTED MATERIAL CHAPTER ONE HEMATOPOIESIS GENERAL FEATURES All blood cells have a finite life span, but in normal
VETERINARY HEMATOLOGY ATLAS OF COMMON DOMESTIC AND NON-DOMESTIC SPECIES SECOND EDITION COPYRIGHTED MATERIAL CHAPTER ONE HEMATOPOIESIS GENERAL FEATURES All blood cells have a finite life span, but in normal
Participants Identification No. % Evaluation. Mitotic figure Educational Erythrocyte precursor, abnormal/
 Cell Identification BMD-09 Participants Identification No. % Evaluation Mitotic figure 233 96.7 Educational Erythrocyte precursor, abnormal/ 4 1.7 Educational dysplastic nuclear features Erythrocyte precursor
Cell Identification BMD-09 Participants Identification No. % Evaluation Mitotic figure 233 96.7 Educational Erythrocyte precursor, abnormal/ 4 1.7 Educational dysplastic nuclear features Erythrocyte precursor
Blood Cell Identification Graded
 Blood Cell Identification Graded Case History The patient is a 20-year-old female with sickle cell disease who presents with bilateral leg pain for 3 days. She is scheduled to have bilateral hip and leg
Blood Cell Identification Graded Case History The patient is a 20-year-old female with sickle cell disease who presents with bilateral leg pain for 3 days. She is scheduled to have bilateral hip and leg
Formation of Blood Cells
 Hematopoiesis Lecture Objectives Name organs responsible for hematopoiesis in the fetus. List the developmental stages of hematopoiesis both prenatally and postnatally. Outline the major steps of post
Hematopoiesis Lecture Objectives Name organs responsible for hematopoiesis in the fetus. List the developmental stages of hematopoiesis both prenatally and postnatally. Outline the major steps of post
Case 3. Ann T. Moriarty,MD
 Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Hematopathology Lab. Third year medical students
 Hematopathology Lab Third year medical students Objectives Identify the lesion Know the specific name of the lesion Know associated disease Know relevant pathologic background Spherocytes: appear small,
Hematopathology Lab Third year medical students Objectives Identify the lesion Know the specific name of the lesion Know associated disease Know relevant pathologic background Spherocytes: appear small,
EDUCATIONAL COMMENTARY DISTINGUISHING MORPHOLOGIC LOOK-ALIKES
 EDUCATIONAL COMMENTARY DISTINGUISHING MORPHOLOGIC LOOK-ALIKES Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
EDUCATIONAL COMMENTARY DISTINGUISHING MORPHOLOGIC LOOK-ALIKES Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Blood Cell Identification Graded
 Blood Cell Identification Graded Case History The patient was a five-day-old girl with an elevated unconjugated bilirubin and a weakly positive direct antiglobulin test (DAT). Her CBC showed: WBC = 11.0
Blood Cell Identification Graded Case History The patient was a five-day-old girl with an elevated unconjugated bilirubin and a weakly positive direct antiglobulin test (DAT). Her CBC showed: WBC = 11.0
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and
 Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
Megakaryocyte or Precursor, Normal
 Precursor, Normal SYNONYMS none VITAL STATISTICS size...20-160 µm in diameter N:C ratio...varible, depending on maturation of cell; early forms have a high N:C rato which decreases as cell matures and
Precursor, Normal SYNONYMS none VITAL STATISTICS size...20-160 µm in diameter N:C ratio...varible, depending on maturation of cell; early forms have a high N:C rato which decreases as cell matures and
Hemopoiesis and Blood
 Hemopoiesis and Blood Blood Cells o o o Erythrocytes Leukocytes Thrombocytes Function o Transport nutrients and wastes throughout the bloodstream, fight foreign antigens and blood coagulation. Location
Hemopoiesis and Blood Blood Cells o o o Erythrocytes Leukocytes Thrombocytes Function o Transport nutrients and wastes throughout the bloodstream, fight foreign antigens and blood coagulation. Location
Patterns of Lymphoid Neoplasia in Peripheral Blood. Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure
 Patterns of Lymphoid Neoplasia in Peripheral Blood Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure Dr Baltrucki has received an honorarium for his participation as a faculty presenter in this
Patterns of Lymphoid Neoplasia in Peripheral Blood Leon F. Baltrucki, M.D. Leon F. Baltrucki, M.D. Disclosure Dr Baltrucki has received an honorarium for his participation as a faculty presenter in this
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
DETERMINATION OF A LYMPHOID PROCESS
 Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Participants Identification No. % Evaluation
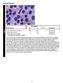 BMD-02 Cell Identification Participants Identification No. % Evaluation Erythrocyte precursor, normal 228 95.8 Educational Erythrocyte, normal 7 3.0 Educational Erythrocyte precursor with megaloblastic
BMD-02 Cell Identification Participants Identification No. % Evaluation Erythrocyte precursor, normal 228 95.8 Educational Erythrocyte, normal 7 3.0 Educational Erythrocyte precursor with megaloblastic
Blood Cell Identification: 2011-B Mailing: Acute Myeloid Leukemia (AML)
 Please Note: To view the Figures and Images contained within this education activity in color, access the electronic version of the reading. CASE HISTORY This peripheral blood smear is from a 51-year-old
Please Note: To view the Figures and Images contained within this education activity in color, access the electronic version of the reading. CASE HISTORY This peripheral blood smear is from a 51-year-old
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
12 Dynamic Interactions between Hematopoietic Stem and Progenitor Cells and the Bone Marrow: Current Biology of Stem Cell Homing and Mobilization
 Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 4 MYELOID NEOPLASMS
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
HISTOLOGY VIRTUAL LABORATORY BLOOD AND LYMPHATICS SYSTEM
 HISTOLOGY VIRTUAL LABORATORY BLOOD AND LYMPHATICS SYSTEM Login: http://histopath.westernu.edu Histology Atlas AND Virtual Histology links. I. HEMATOLOGY - PERIPHERAL BLOOD Purpose: To be able to identify
HISTOLOGY VIRTUAL LABORATORY BLOOD AND LYMPHATICS SYSTEM Login: http://histopath.westernu.edu Histology Atlas AND Virtual Histology links. I. HEMATOLOGY - PERIPHERAL BLOOD Purpose: To be able to identify
HEMATOLOGIC MORPHOLOGY- AECOM HEMATOLOGY COURSE
 Log Out Help current login :lcytryn@montefiore.org HEMATOLOGIC MORPHOLOGY- AECOM HEMATOLOGY COURSE Lawrence Cytryn, M.D. - Course Director 1998 Edward Burns, M.D. Images used by permission within AECOM
Log Out Help current login :lcytryn@montefiore.org HEMATOLOGIC MORPHOLOGY- AECOM HEMATOLOGY COURSE Lawrence Cytryn, M.D. - Course Director 1998 Edward Burns, M.D. Images used by permission within AECOM
Proper Slide Preparation
 Hematology Essentials: A Foundation for WBC Review Using Case Studies Christine Hinz, MS, MLS(ASCP) CM Proper Slide Preparation smooth, homogenous film 1/2 to 3/4 the slide length straight feather edge
Hematology Essentials: A Foundation for WBC Review Using Case Studies Christine Hinz, MS, MLS(ASCP) CM Proper Slide Preparation smooth, homogenous film 1/2 to 3/4 the slide length straight feather edge
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
EDUCATIONAL COMMENTARY BLOOD CELL IDENTIFICATION
 EDUCATIONAL COMMENTARY BLOOD CELL IDENTIFICATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click
EDUCATIONAL COMMENTARY BLOOD CELL IDENTIFICATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click
Blood Cell Identification Graded
 Blood Cell Identification Graded Case History A 51-year-old female presented with dyspnea on exertion. Laboratory results were as follows: WBC=5.5 X 10 9 /L; Hgb=4.2 g/dl; Hct=13.9%; MCV=78.7fL; RDW=30;
Blood Cell Identification Graded Case History A 51-year-old female presented with dyspnea on exertion. Laboratory results were as follows: WBC=5.5 X 10 9 /L; Hgb=4.2 g/dl; Hct=13.9%; MCV=78.7fL; RDW=30;
Introduction to Haematology. Prof Roger Pool Department of Haematology University of Pretoria
 Introduction to Haematology Prof Roger Pool Department of Haematology University of Pretoria Suggested reading Haematology at a Glance Atul Mehta & Victor Hoffbrand Second Edition Published by Blackwell
Introduction to Haematology Prof Roger Pool Department of Haematology University of Pretoria Suggested reading Haematology at a Glance Atul Mehta & Victor Hoffbrand Second Edition Published by Blackwell
Chapter 21 Outline. General Composition and Functions of Blood Blood Plasma Formed Elements in the Blood Hemopoiesis: Production of Formed Elements
 Chapter 21 Outline General Composition and Functions of Blood Blood Plasma Formed Elements in the Blood Hemopoiesis: Production of Formed Elements Introduction Blood serves many functions. Some examples
Chapter 21 Outline General Composition and Functions of Blood Blood Plasma Formed Elements in the Blood Hemopoiesis: Production of Formed Elements Introduction Blood serves many functions. Some examples
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم WBCs disorders *Slide 2: - we will focus on the disorders that are related to the # of WBCs - in children the # of lymphocyte is more than it in adults,sometimes more than neutrophils
بسم هللا الرحمن الرحيم WBCs disorders *Slide 2: - we will focus on the disorders that are related to the # of WBCs - in children the # of lymphocyte is more than it in adults,sometimes more than neutrophils
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Peripheral Blood Smear: Diagnostic Clues and Algorithms
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
ADx Bone Marrow Report. Patient Information Referring Physician Specimen Information
 ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
MORPHOLOGY OF BONE MARROW ASPIRATES. Dr.Prasanna N Kumar Head Department of Pathology, Oman Medical College, Oman
 MORPHOLOGY OF BONE MARROW ASPIRATES Dr.Prasanna N Kumar Head Department of Pathology, Oman Medical College, Oman BONE MARROW ASPIRATION Sites Sternum Anterior or posterior iliac spines Aspiration from
MORPHOLOGY OF BONE MARROW ASPIRATES Dr.Prasanna N Kumar Head Department of Pathology, Oman Medical College, Oman BONE MARROW ASPIRATION Sites Sternum Anterior or posterior iliac spines Aspiration from
Notes for the 2 nd histology lab
 Notes for the 2 nd histology lab Note : Please refer to the slides and see the morphological characteristics of each cell, as the practical exam will be in the form of figures. SLIDE #2 Erythropoiesis
Notes for the 2 nd histology lab Note : Please refer to the slides and see the morphological characteristics of each cell, as the practical exam will be in the form of figures. SLIDE #2 Erythropoiesis
Bone marrow histopathology in Ph - CMPDs. - the new WHO classification - Juergen Thiele Cologne, Germany
 Bone marrow histopathology in Ph - CMPDs - the new WHO classification - Juergen Thiele Cologne, Germany Current issues in MPNs concerning morphology 1.Prodromal stages of disease 2.Impact of histopathology
Bone marrow histopathology in Ph - CMPDs - the new WHO classification - Juergen Thiele Cologne, Germany Current issues in MPNs concerning morphology 1.Prodromal stages of disease 2.Impact of histopathology
Myelodysplastic Syndromes Myeloproliferative Disorders
 Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
Hematopoie)c System. Kris)ne Kra2s, M.D.
 Hematopoie)c System Kris)ne Kra2s, M.D. Hematopoie)c System Lecture Objec)ves Describe the developmental stages of erythropoiesis. Describe the developmental stages of granulopoiesis. Describe the differences
Hematopoie)c System Kris)ne Kra2s, M.D. Hematopoie)c System Lecture Objec)ves Describe the developmental stages of erythropoiesis. Describe the developmental stages of granulopoiesis. Describe the differences
Leukocytosis - Some Learning Points
 Leukocytosis - Some Learning Points Koh Liang Piu Department of Hematology-Oncology National University Cancer Institute National University Health System Objectives of this talk: 1. To provide some useful
Leukocytosis - Some Learning Points Koh Liang Piu Department of Hematology-Oncology National University Cancer Institute National University Health System Objectives of this talk: 1. To provide some useful
Materials and Methods
 Peripheral Blood Morphologic Changes after High-Dose Antineoplastic Chemotherapy and Recombinant Human Granulocyte Colony-Stimulating Factor Administration DANIEL P. KERRIGAN, M.D., ANNIE CASTILLO, M.D.,
Peripheral Blood Morphologic Changes after High-Dose Antineoplastic Chemotherapy and Recombinant Human Granulocyte Colony-Stimulating Factor Administration DANIEL P. KERRIGAN, M.D., ANNIE CASTILLO, M.D.,
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor
 HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
Reactive and Neoplastic Lymphocytosis
 Reactive and Neoplastic Lymphocytosis Koranda A. Walsh, VMD, BS Assistant Professor, Clinical Pathobiology University of Pennsylvania School of Veterinary Medicine PLEASE NOTE: These notes are meant as
Reactive and Neoplastic Lymphocytosis Koranda A. Walsh, VMD, BS Assistant Professor, Clinical Pathobiology University of Pennsylvania School of Veterinary Medicine PLEASE NOTE: These notes are meant as
The spectrum of flow cytometry of the bone marrow
 The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls
 Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA. April 16, 2008
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
WBCs Disorders. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features and
WBCs Disorders Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features and
Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte-macrophage colonystimulating factor (G-CSF).
 Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte colony-stimulating factor(g-csf). Granulocyte-macrophage colonystimulating factor (G-CSF). Interleukin-11
Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte colony-stimulating factor(g-csf). Granulocyte-macrophage colonystimulating factor (G-CSF). Interleukin-11
2010 Hematopoietic and Lymphoid ICD-O Codes - Alphabetical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
2012 Hematopoietic and Lymphoid ICD-O Codes - Numerical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Blood Cell Identification Graded
 Blood Cell Identification Graded Case History An 11-year-old girl presented to the emergency room with wheezing and was diagnosed as having asthma. Her CBC showed WBC = 12.5 x 10 9 /L; Hgb = 12.4g/dL;
Blood Cell Identification Graded Case History An 11-year-old girl presented to the emergency room with wheezing and was diagnosed as having asthma. Her CBC showed WBC = 12.5 x 10 9 /L; Hgb = 12.4g/dL;
WHO Update to Myeloproliferative Neoplasms
 WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
Disclosures. Myeloproliferative Neoplasms: A Case-Based Approach. Objectives. Myeloproliferative Neoplasms. Myeloproliferative Neoplasms
 Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
The patient had a mild splenomegaly but no obvious lymph node enlargement. The consensus phenotype obtained from part one of the exercise was:
 Case History An 86 year old male was admitted to hospital with chest infection. Haematological examination subsequently revealed the following: Hb- 11.0 g/dl; WBC- 67.1 x 10^9/l; PLT- 99 x10^9/l; RBC-
Case History An 86 year old male was admitted to hospital with chest infection. Haematological examination subsequently revealed the following: Hb- 11.0 g/dl; WBC- 67.1 x 10^9/l; PLT- 99 x10^9/l; RBC-
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology. Songlin Zhang, MD, PhD LSUHSC-Shreveport
 From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
Leukocyte Disorders. Dr Alauldeen Mudhafar Zubair
 Leukocyte Disorders Dr Alauldeen Mudhafar Zubair Composition of blood Specialized connective tissue Blood cells (formed elements) suspended in plasma Blood volume: 5-6 liters (approx 1.5 gal) in males
Leukocyte Disorders Dr Alauldeen Mudhafar Zubair Composition of blood Specialized connective tissue Blood cells (formed elements) suspended in plasma Blood volume: 5-6 liters (approx 1.5 gal) in males
EDUCATIONAL COMMENTARY MORPHOLOGIC CHANGES IN PERIPHERAL BLOOD CELLS
 EDUCATIONAL COMMENTARY MORPHOLOGIC CHANGES IN PERIPHERAL BLOOD CELLS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
EDUCATIONAL COMMENTARY MORPHOLOGIC CHANGES IN PERIPHERAL BLOOD CELLS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
Evaluation of Bone Marrow Biopsies and Aspirates ANNA PORWIT DEPARTMENT OF PATHOLOGY, LUND UNIVERSITY
 Evaluation of Bone Marrow Biopsies and Aspirates ANNA PORWIT DEPARTMENT OF PATHOLOGY, LUND UNIVERSITY DISCLOSURES NONE Learning objectives To review the rules of BMA evaluation To review the main issues
Evaluation of Bone Marrow Biopsies and Aspirates ANNA PORWIT DEPARTMENT OF PATHOLOGY, LUND UNIVERSITY DISCLOSURES NONE Learning objectives To review the rules of BMA evaluation To review the main issues
Almost any suspected tumor can be aspirated easily and safely. Some masses are more risky to aspirate including:
 DOES THIS PATIENT HAVE CANCER? USING IN-HOUSE CYTOLOGY TO HELP YOU MAKE THIS DIAGNOSIS. Joyce Obradovich, DVM, Diplomate, ACVIM (Oncology) Animal Cancer & Imaging Center, Canton, Michigan Almost every
DOES THIS PATIENT HAVE CANCER? USING IN-HOUSE CYTOLOGY TO HELP YOU MAKE THIS DIAGNOSIS. Joyce Obradovich, DVM, Diplomate, ACVIM (Oncology) Animal Cancer & Imaging Center, Canton, Michigan Almost every
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities
 Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Juvenile Myelomonocytic Leukemia (JMML)
 Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
MYELODYSPLASTIC SYNDROMES
 MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
Chapter 10 Bone Marrow
 Chapter 10 Bone Marrow Contents Red Bone Marrow... 188 Hemopoiesis... 189 Early Steps in Hemopoiesis... 190 Late Steps in Hemopoiesis... 190 Yellow Bone Marrow... 197 Guide to Practical Histology: Bone
Chapter 10 Bone Marrow Contents Red Bone Marrow... 188 Hemopoiesis... 189 Early Steps in Hemopoiesis... 190 Late Steps in Hemopoiesis... 190 Yellow Bone Marrow... 197 Guide to Practical Histology: Bone
Blood & Blood Formation
 Module IB Blood & Blood Formation Histology and Embryology Martin Špaček, MD (m.spacek@centrum.cz) http://www.lf3.cuni.cz/histologie Approximately 7% of a person's weight is blood (about 5 L) Blood consists
Module IB Blood & Blood Formation Histology and Embryology Martin Špaček, MD (m.spacek@centrum.cz) http://www.lf3.cuni.cz/histologie Approximately 7% of a person's weight is blood (about 5 L) Blood consists
4. TEXTBOOK: ABUL K. ABBAS. ANDREW H. LICHTMAN. CELLULAR AND MOLECULAR IMMUNOLOGY. 5 TH EDITION. Chapter 2. pg
 LECTURE: 03 Title: CELLS INVOLVED IN THE IMMUNE RESPONSE LEARNING OBJECTIVES: The student should be able to: Identify the organs where the process of the blood formation occurs. Identify the main cell
LECTURE: 03 Title: CELLS INVOLVED IN THE IMMUNE RESPONSE LEARNING OBJECTIVES: The student should be able to: Identify the organs where the process of the blood formation occurs. Identify the main cell
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
CHAPTER:4 LEUKEMIA. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY 8/12/2009
 LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
ABERRANT EXPRESSION OF CD19 AND CD43
 ABERRANT EXPRESSION OF CD19 AND CD43 IN A PATIENT WITH THERAPY-RELATED ACUTE MYELOID LEUKEMIA AND A HISTORY OF MANTLE CELL LYMPHOMA Yen-Chuan Hsieh, 1 Chien-Liang Lin, 2 Chao-Jung Tsao, 2 Pin-Pen Hsieh,
ABERRANT EXPRESSION OF CD19 AND CD43 IN A PATIENT WITH THERAPY-RELATED ACUTE MYELOID LEUKEMIA AND A HISTORY OF MANTLE CELL LYMPHOMA Yen-Chuan Hsieh, 1 Chien-Liang Lin, 2 Chao-Jung Tsao, 2 Pin-Pen Hsieh,
Ordering Physician CLIENT,CLIENT. Collected REVISED REPORT
 HPWET Hematopathology Consultation, MML Embed Client Hematopathology Consult REVISED INAL DIAGNOSIS Interpretation Peripheral blood, bone marrow aspirate and biopsies, bilateral iliac crests: 1. Normocellular
HPWET Hematopathology Consultation, MML Embed Client Hematopathology Consult REVISED INAL DIAGNOSIS Interpretation Peripheral blood, bone marrow aspirate and biopsies, bilateral iliac crests: 1. Normocellular
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
EHE1-16 Participants Identification No. % Evaluation
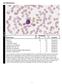 Cell Identification EHE1-16 Participants Identification No. % Evaluation Blast cell 154 90.1 Educational Lymphocyte 4 2.3 Educational Lymphocyte, reactive 1 0.6 Educational Lymphoma cell (malignant) 1
Cell Identification EHE1-16 Participants Identification No. % Evaluation Blast cell 154 90.1 Educational Lymphocyte 4 2.3 Educational Lymphocyte, reactive 1 0.6 Educational Lymphoma cell (malignant) 1
WHO Classification. B-cell chronic lymphocytic leukemia/small T-cell granular lymphocytic leukemia
 Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Hematology 101. Rachid Baz, M.D. 5/16/2014
 Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Blood: Functions. Liquid connective tissue 3 general functions 1. Transportation. 2. Regulation. 3. Protection
 Blood Elements Lecture Objectives List blood components. Classify formed elements of blood. Discuss the scientific basis of the above classification. Describe the basic structure of erythrocytes and criteria
Blood Elements Lecture Objectives List blood components. Classify formed elements of blood. Discuss the scientific basis of the above classification. Describe the basic structure of erythrocytes and criteria
Bone marrow aspiration as the initial diagnostic tool in the diagnosis of leukemia - A case study
 Original Research Article Bone marrow aspiration as the initial diagnostic tool in the diagnosis of leukemia - A case study Priyanka Poonam 1*, N.K. Bariar 2 1 Tutor, Department of Pathology, Patna Medical
Original Research Article Bone marrow aspiration as the initial diagnostic tool in the diagnosis of leukemia - A case study Priyanka Poonam 1*, N.K. Bariar 2 1 Tutor, Department of Pathology, Patna Medical
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
SH A CASE OF PERSISTANT NEUTROPHILIA: BCR-ABL
 SH2017-0124 A CASE OF PERSISTANT NEUTROPHILIA: BCR-ABL NEGATIVE John R Goodlad 1, Pedro Martin-Cabrera 2, Catherine Cargo 2 1. Department of Pathology, NHS Greater Glasgow & Clyde, QEUH, Glasgow 2. Haematological
SH2017-0124 A CASE OF PERSISTANT NEUTROPHILIA: BCR-ABL NEGATIVE John R Goodlad 1, Pedro Martin-Cabrera 2, Catherine Cargo 2 1. Department of Pathology, NHS Greater Glasgow & Clyde, QEUH, Glasgow 2. Haematological
Bone Marrow Pathology. Part 1. R.S. Riley, M.D., Ph.D.
 Bone Marrow Pathology Part 1 R.S. Riley, M.D., Ph.D. Bone Marrow Pathology Bone marrow basics Red cell diseases White cell diseases Other diseases Bone Marrow Pathology Bone marrow basics Hematopoiesis
Bone Marrow Pathology Part 1 R.S. Riley, M.D., Ph.D. Bone Marrow Pathology Bone marrow basics Red cell diseases White cell diseases Other diseases Bone Marrow Pathology Bone marrow basics Hematopoiesis
r). SUPPLEMENTARY/SECOND OPPORTUNITY EXAMINATION PAPER nnmlbih UNIVERSITY Sophia Blaauw INSTRUCTIONS FACULTY OF HEALTH AND APPLIED SCIENCES
 r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
HAEMATOLOGICAL MALIGNANCY
 HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms. Daniel A. Arber, MD Stanford University
 Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
