Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, cont
|
|
|
- Steven Nicholas Sherman
- 5 years ago
- Views:
Transcription
1 Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at Brian T. Welch, BS Thomas D. Atwell, MD Douglas A. Nichols, MD C. Thomas Wass, MD Matthew R. Callstrom, MD Bradley C. Leibovich, MD Paul C. Carpenter, MD Jayawant N. Mandrekar, PhD J. William Charboneau, MD Percutaneous Image-guided Adrenal Cryoablation: Procedural Considerations and Technical Success1 Purpose: Materials and Methods: To assess safety, technical success, complications, and hemodynamic changes associated with the adrenal cryoablation procedure. This retrospective review was approved by the institutional review board, with waiver of informed consent, and was compliant with the Health Insurance Portability and Accountability Act. Adult patients with adrenal metastasis who were treated with adrenal cryoablation between May 2005 and October 2009 were eligible for this review. Twelve patients (undergoing 13 procedures) with single adrenal tumors were included in the analysis. For statistical analysis, hemodynamic data were averaged for the patient undergoing the procedure twice. Technical success, safety, and local control were analyzed according to standard criteria. Hemodynamic changes during the procedure were analyzed and compared with data from an unmatched cohort of patients who underwent kidney (not in the upper pole) cryoablation (Wilcoxon rank sum test). A further subanalysis of hemodynamic changes was performed on the basis of whether preprocedural a - or b -adrenergic blockade was used. ORIGINAL RESEARCH n VASCULAR AND INTERVENTIONAL RADIOLOGY 1 From Mayo Medical School (B.T.W.), Rochester, Minn; Departments of Radiology (T.D.A., D.A.N., M.R.C., J.W.C.), Anesthesiology (C.T.W.), Urology (B.C.L.), Endocrinology (P.C.C.), and Biostatistics (J.M.), Mayo Clinic, 200 First St SW, Rochester, MN Received April 9, 2010; revision requested June 21; fi nal revision received July 7; accepted July 27; fi nal version accepted August 2. Address correspondence to B.T.W. ( Welch.brian@mayo.edu ). q RSNA, 2010 Results: Conclusion: With adrenal cryoablation, local control was achieved following treatment in 11 (92%; 95% confidence interval: 65.1%, 99.6%) of 12 tumors. One patient with known adrenal insufficiency underwent conservative ablation and developed ipsilateral adrenal recurrence, which was retreated. Five patients developed hypertensive crisis during the final, active thaw phase of the cryoablation procedure, and one patient developed hypertensive crisis in the immediate postablation period. Patients undergoing adrenal cryoablation experienced a significant increase in systolic blood pressure ( P =.005), pulse pressure ( P =.02), and mean arterial pressure ( P =.01) when compared with the cohort of kidney cryoablation patients. Adrenal cryoablation patients who were not premedicated with an a -blocker ( n = 5) had a higher level of systolic blood pressure increase during the cryoablation procedure when compared with their counterparts who were premedicated ( n = 7) ( P =.034). Adrenal cryoablation is technically feasible with a high rate of local control. Patients premedicated with the a -blocker phenoxybenzamine appear to have a reduced risk of hypertensive crisis. q RSNA, 2010 Radiology: Volume 258: Number 1 January 2011 n radiology.rsna.org 301
2 Neoplasms of the adrenal gland occur in approximately 1% of the general population, with metastases comprising the most common malignant adrenal neoplasm ( 1 ). Lung cancer is the most common primary origin of adrenal metastasis, but renal cell carcinoma (RCC), melanoma, and gastrointestinal tumors also have a predilection for the adrenal gland ( 1 ). In selected patients with isolated metastatic disease of the adrenal gland, adrenalectomy has been associated with increased survival ( 2 5 ). Percutaneous ablation is evolving into an effective method of focal tumor treatment. In particular, radiofrequency (RF) ablation has been established as a safe and effective treatment for adrenal tumors ( 6 8 ). With RF ablation, pulses of RF waves are used to generate thermal injury and subsequent cell death, whereas with cryoablation, argon gas currently is used via the Joule- Thomson effect to create subfreezing temperatures and induction of cell lysis. An important advantage of cryoablation is the capability to allow visualization of treatment progression and tumor coverage with monitoring of the development and progression of a low-attenuation ice ball with computed tomographic (CT) imaging. Cryoablation has been effectively used to treat neoplasms of the liver, kidney, prostate, lung, and soft tissue ( 9 15 ). Cryoablation of the adrenal gland is a promising technique for percutaneous treatment of adrenal metastasis, with limited experience reported in the literature ( 5,16 ). Thus, our purpose Advances in Knowledge n Adrenal cryoablation patients who were not premedicated with an a -blocker had a higher level of systolic blood pressure increase during the cryoablation procedure compared with their counterparts who were premedicated ( P =.034). n Local control was achieved fol- lowing adrenal cryoablation in 11 (92%) of 12 tumors. was to assess safety, technical success, complications, and hemodynamic changes associated with the adrenal cryoablation procedure. Materials and Methods This retrospective review was approved by the institutional review board and was compliant with the Health Insurance Portability and Accountability Act. Although informed consent was obtained prior to each ablation procedure, consent specific for this review was waived by the institutional review board. The inclusion criterion was that the patients were adults with an adrenal metastasis who underwent percutaneous image-guided adrenal cryoablation between May 2005 and October Patients with metastatic adrenal tumors of up to 5 cm were selected to undergo cryoablation. Moreover, patients were screened for pheochromocytoma with urine or plasma metanephrine level analysis prior to consideration for treatment with cryoablation. Twelve patients (11 men, one woman; mean age, 70 years; range, years) with single adrenal tumors (total, 12 tumors) matched these criteria ( Table 1 ) and underwent a total of 13 cryoablation procedures; one patient underwent two procedures, including retreatment. In all cases, patients had imaging findings consistent with adrenal metastatic disease. Four of 12 patients underwent adrenal biopsy to achieve pathologic Implications for Patient Care n Cryoablation for the treatment of metastatic disease involving the adrenal gland can be performed safely and with high local control rates. n Patients with metastatic disease involving the adrenal gland who are undergoing ablation of the tumor should be premedicated with an a -blocker (10 60 mg oral phenoxybenzamine for days prior to ablation coupled with subsequent titration of a b -blocker). confirmation of metastatic disease. The remaining patients were suspected of having metastatic disease owing to positron emission tomographic findings positive for disease, new lesions noted on images, or distinct interval growth. The primary tumor in six of 12 patients was RCC ( Table 1 ). Other primary histologic findings included hepatocellular carcinoma, melanoma, squamous cell lung carcinoma, neuroendocrine large cell carcinoma of the lung, penile squamous cell carcinoma, and urothelial carcinoma. Seven of ten patients with available primary tumor pathologic findings had neoplasms of a high grade (grade 3 or 4) ( 17 ). Eight patients were seen by an endocrinologist prior to the procedure for discussion of the use of a - or b -adrenergic blockade. The decision to consult an endocrinologist was made by the referring physician. Initiation of such premedication (including medication choices and dosages) prior to cryoablation was left to the discretion of the individual endocrinologist. Five patients were receiving a - and b -blockers, two patients were re ceiving a -blockers alone, two patients were receiving b -blockers alone, and three patients received no a - or b -blockers ( Table 2 ). All procedures were performed with patients receiving a general anesthetic. Published online before print /radiol Radiology 2011; 258: Abbreviations: DBP = diastolic blood pressure MAP = mean arterial pressure PP = pulse pressure RCC = renal cell carcinoma RF = radiofrequency SBP = systolic blood pressure Author contributions: Guarantors of integrity of entire study, B.T.W., D.A.N.; study concepts/study design or data acquisition or data analysis/ interpretation, all authors; manuscript drafting or manuscript revision for important intellectual content, all authors; approval of final version of submitted manuscript, all authors; literature research, B.T.W., T.D.A., D.A.N., C.T.W., M.R.C., P.C.C.; clinical studies, B.T.W., T.D.A., D.A.N., M.R.C., P.C.C.; statistical analysis, B.T.W., P.C.C., J.N.M.; and manuscript editing, B.T.W., T.D.A., D.A.N., C.T.W., M.R.C., B.C.L., P.C.C., J.N.M. Potential conflicts of interest are listed at the end of this article. 302 radiology.rsna.org n Radiology: Volume 258: Number 1 January 2011
3 Table 1 Primary Characteristics for 12 Adrenal Cryoablation Patients Patient No./ Age (y)/sex Primary Location Grade Original Treatment Adrenal Location No. of Probes Used Adrenal Lesion Size (cm) * Follow-up (mo) 1/85/M RCC (clear cell) 2 Left partial nephrectomy Left /66/M Melanoma Unknown Surgery, chemotherapy Right /68/M Hepatocellular carcinoma 3 Right hepatectomy Left /63/M RCC 1 Right radical nephrectomy Left /67/M RCC 3 Right radical nephrectomy Left /65/M RCC 3 Right radical nephrectomy Left /64/M RCC 4 Right radical nephrectomy Right /71/F Squamous cell carcinoma of lung 3 Chemotherapy, radiation therapy Right /71/F Squamous cell carcinoma of lung Right /69/M RCC 2 Right radical nephrectomy Left /71/M Urothelial carcinoma 3 Radical cystectomy Left /70/M Penile squamous cell carcinoma 3 Partial penectomy Right /75/M Neuroendocrine large cell carcinoma of lung Unknown Chemotherapy Right * Anteroposterior dimension. Table 2 a - and b -Adrenergic Blockade and Intraprocedural Hemodynamics Patient No. a - or b-blocker Used * Consultation with Endocrinologist Intraprocedural Blood Pressure (mm Hg) Baseline Maximum 1 Metoprolol, 75 mg twice a day; long term per home regimen No 121/66 300/170 2 Labetalol, 200 mg twice a day for 4 days; labetalol, 400 mg on the morning of procedure Yes 118/61 240/125 3 Phenoxybenzamine, 40 mg daily for 7 days No 93/55 168/81 4 Phenoxybenzamine, 30 mg twice a day for 7 days; metoprolol, 75 mg daily; long term Yes 101/61 167/102 per home regimen 5 No a - or b-blocker used No 85/52 162/91 6 Phenoxybenzamine, 30 mg daily for 6 days; metoprolol, 50 mg on the night before and Yes 105/80 144/78 the morning of procedure 7 No a - or b-blocker used Yes 94/65 216/122 8 No a - or b-blocker used Yes 124/64 191/88 8 No a - or b-blocker used Yes 106/53 186/81 9 Phenoxybenzamine, 10 mg twice a day for 7 days Yes 98/60 136/84 10 Metoprolol, 50 mg daily; long term per home regimen No 104/59 218/ Phenoxybenzamine, 10 mg twice a day for 5 days; atenolol, 50 mg daily; long term Yes 90/61 157/84 per home regimen 12 Phenoxybenzamine, 10 mg twice a day for 7 days; metoprolol, 50 mg on the night before and the morning of procedure Yes 95/58 168/64 * Trade and manufacturers names for the drugs are as follows: metoprolol, NovaPlus, Irving, Tex; labetalol, Hospira, Lake Forest, Ill; phenoxybenzamine, WellSpring Pharmaceutical, Sarasota, Fla; and atenolol, AstraZeneca, Wilmington, Del. For patient 8 who underwent two procedures (one as retreatment), the average baseline intraprocedural blood pressure was 115/58.5 mm Hg, and the average maximum intraprocedural blood pressure was 188.5/84.5 mm Hg. Continuous radial arterial blood pressure monitoring was performed, with values pertaining to hemodynamics recorded. Direct, arterial blood pressure monitoring enabled prompt detection of a change in hemodynamics by the anesthesia care team. The same cryoablation system (Healthtronics/Endocare, Irvine, Calif) was used in all treatments. CT guidance was used to place the cryoprobes in the adrenal tumor. The total number of probes placed was Radiology: Volume 258: Number 1 January 2011 n radiology.rsna.org 303
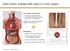
4 Grade 2 clear cell RCC in an 85-year-old man who underwent partial left nephrectomy. (a) Transverse contrast-enhanced CT demonstrates a normal appearance to the left adrenal 1 year after surgery. (b) Transverse contrast-enhanced CT 2 years after surgery shows a new 2.8-cm left adrenal mass, consistent with RCC metastasis. (c) Unenhanced CT during ablation procedure demonstrates the ice ball encompassing the lesion 10 minutes into the ablation procedure. (d) Transverse contrast-enhanced CT 37 months after ablation reveals no evidence of residual tumor in the left adrenal. based on tumor size, with a goal to provide an ice ball that would completely encompass the tumor by 5 mm or more beyond the tumor margin. CT monitor ing was used during the procedure with an open 40-section CT system (Somatom Sensation; Siemens, Munich, Germany). Limited CT images without contrast material were obtained every 2 minutes during the freezing portions of the cycle to monitor the ice ball growth; the specific CT technique was governed by automated exposure control (typically, 120 kvp and approximately 240 ma). Each lesion received a single treatment cycle of freezing, thawing, and freezing again. Duration of the freezing was based on the growth of the ice ball relative to the tumor; the goal was to extend the ice ball 5 mm beyond the tumor margin during the freezing cycle. The first, passive thaw occurs when the temperature of the probe is held just below freezing by using intermittent pulses of argon gas. Following the ablation treatment, the probes were actively thawed by using helium gas and were withdrawn. Routine imaging with either contrast material enhanced CT or magnetic resonance (MR) imaging was performed within 24 hours of the cryoablation treatment to assess for potential complications (Figure ). Additional follow-up imaging with contrast-enhanced (Omnipaque; GE Healthcare, Milwaukee, Wis) CT or MR imaging was performed at 3 6-month intervals, as deemed appropriate by the primary clinician. The specific imaging protocol was defined by the radiologist responsible for the imaging but was typically tailored to the general malignancy diagnosis. Technical success was defined as coverage of the tumor by the ice ball during CT monitoring ( 18 ). If incomplete ablation occurred for any reason, this was deemed a technical failure, and the patient was considered for further treatment, including surgical resection. A retrospective review of blood pressure changes during the cryoablation procedure was performed. Two specific measurements were recorded for the purpose of this study: the patient s blood pressure immediately before placement of the cryoprobes and the maximum systolic blood pressure (SBP) and corresponding diastolic blood pressure (DBP) during the remainder of the procedure, including the immediate postablation period. An unmatched (unmatched for age, tumor size, and tumor location) cohort of 13 patients (nine men, four women; mean age, 71 years; range, years) who underwent percutaneous image-guided cryoablation of the kidney served as a control group (kidney cohort) for statistical analysis of these hemodynamic changes. Hemodynamic monitoring in these patients was performed by using an automatic blood pressure cuff, with recordings taken every minute. These patients were selected on the basis of similarity of tumor size (anteroposterior) relative to the tumor size in patients in the adrenal co hort (mean, 2.3 cm; range, cm); only cases in which ablation of the lower pole of the kidney was performed were used to avoid possible confounding owing to adrenal injury. A further subanalysis of blood pressure changes was performed on the basis of whether an a - or a b -blocker was administered; patients who were premedicated with an a -blocker ( n = 7) were compared with those who had received no a -blocker ( n = 5). One patient underwent two cryoablation procedures. This patient had known adrenal insufficiency at the time of the initial ablation treatment and was treated conservatively, with greater emphasis on adrenal preservation over tumor margins to preserve underlying adrenal function. To avoid biasing the hemodynamic data pool, the hemodynamic changes for the two procedures in this patient were averaged. 304 radiology.rsna.org n Radiology: Volume 258: Number 1 January 2011
5 Classification of hemodynamic changes during the cryoablation procedure was done in accordance with Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure version 7 guidelines. Specifically, patients were designated as having a hypertensive crisis if they had an increase of SBP to greater than 180 mm Hg or of DBP to greater than 120 mm Hg ( 19 ). Moreover, procedural complications were evaluated on the basis of accepted standardized criteria set forth in the Common Terminology Criteria for Adverse Events, version 3.0, guidelines ( 20 ). Routine clinical follow-up was maintained by the patient s primary clinician, as documented in our electronic medical record. Patients were also asked to send pertinent cross-sectional images obtained outside our facility to us for our review. Changes, relative to baseline values, in SBP, DBP, pulse pressure (PP), and mean arterial pressure (MAP) were calculated. SBP was continuously monitored via the radial arterial catheter. PP was calculated by using the following formula: PP = SBP 2 DBP. MAP was calculated by using the following formula: MAP = [(2 DBP)+SBP]/3. Comparison of these changes between the kidney cohort and those of the adrenal cohort and between patients with a -adrenergic blockade and patients with no a -adrenergic blockade were made by using the Wilcoxon rank sum test owing to the smaller sample size and the non-gaussian nature of the data. P values less than.05 were considered to indicate a significant difference. Statistical analysis was performed by using software (SAS version 9.0; SAS, Cary, NC). In light of the small sample size, the Blyth-Still-Casella procedure was used to generate a 95% confidence interval for local control achieved with cryoablation. Results Twelve patients with 12 adrenal tumors underwent 13 cryoablation procedures. Adrenal metastases ranged in size (anteroposterior) from 1.2 to 4.5 cm (mean, 2.7 cm). One patient with a 1.8-cm right adrenal metastasis developed ipsilateral adrenal recurrence of disease and was retreated with cryoablation 7 months after the original procedure ( Table 1 ). The number of probes used for the ablation procedure ranged from one to three, with a mean of 1.8. Overall, local control was achieved following the treatment of 11 (92%; 95% confidence interval: 65.1%, 99.6%) of 12 tumors. In none of the other patients was subsequent adrenal tumor treatment necessitated, and the mean follow-up time was 18 months (range, 3 55 months). Six (46%) of 13 cryoablation procedures were complication free. During six (46%) of the 13 cryoablation procedures in five patients, patients experienced hypertensive crisis, with the patient undergoing two procedures having hypertensive crisis during each procedure. More important, although an increase in blood pressure was seen during the initial passive thaw, five episodes of hypertensive crisis occurred during the final, active thaw cycle (with the patient undergoing two procedures experiencing one episode of hypertensive crisis during the active thaw and one episode during the immediate postablation time period in the recovery area). Each episode of hypertensive crisis was successfully managed by the anesthesia team with normalization of hemodynamic status. Five of six patients who experienced hypertensive crisis had received no a -blockers prior to the cryoablation procedure; the patient who underwent two procedures had received no a -blockers during either procedure ( Table 2 ). The sixth patient received dual a - and b -blockers, with labetalol as opposed to phenoxybenzamine, owing to close proximity to the procedure date (less than 5 7 days). None of the patients who received pretreatment with phenoxybenzamine experienced a hypertensive crisis during adrenal cryoablation. One (8%) additional procedure of 13 was complicated by a pleural effusion with delayed-onset pneumonia requiring a six-day hospitalization at an outside hospital. This complication was defined as a grade 2 complication because it was symptomatic but required less than two sessions of therapeutic thoracentesis, according to Common Terminology Criteria for Adverse Events, version 3.0 ( 20 ). There were no cardiac rhythm changes in any of the patients. Patients who underwent adrenal cryoablation experienced a significant increase in SBP ( P =.005), PP ( P =.02), and MAP ( P =.01) when they were compared with the cohort of patients who underwent kidney cryoablation ( Table 3 ). The adrenal cryoablation cohort also had an increase in DBP, but this difference was not significant ( P =.07). Adrenal cryoablation patients who were not premedicated with an a -blocker had a higher level of SBP increase during the cryoablation procedure when compared with their counterparts who were premedicated with an a -blocker ( P =.034) ( Table 4 ). Although changes in DBP, PP, and MAP were not significant, patients without a -blocker premedication had a relatively higher increase in these hemodynamic factors during the procedure compared with those with a -blocker premedication ( P =.07,.17,.06, respectively) ( Table 4 ). Discussion Improvements in technique and technology for percutaneous ablation of neoplastic lesions have resulted in an expanding frontier of potential roles in tumor treatment. This expansion has included treatment of adrenal tumors. Wood et al ( 7 ) have shown that RF ablation of adrenal neoplasms was effective, with complete ablation achieved in eight (67%) of 12 tumors of 5 cm or smaller. Mayo-Smith and Dupuy ( 8 ) successfully treated 11 of 13 adrenal tumors by using single-session RF ablation. To the best of our knowledge, only case reports describing adrenal tumor cryoablation exist ( 21,22 ). A noteworthy attribute of cryoablation when compared with other methods of percutaneous ablation is the capability for monitoring the ablation procedure with either CT or MR imaging. For our study, limited nonenhanced CT imaging was used to visualize ice ball progression. The capability to accurately monitor cryoablation progression may diminish the likelihood of collateral Radiology: Volume 258: Number 1 January 2011 n radiology.rsna.org 305
6 Table 3 Comparison of Change in Hemodynamic Status during Adrenal and Kidney Cryoablation Variable Kidney Cohort ( n = 13) * Adrenal Cohort ( n = 12) * P Value Baseline SBP 117 (100, 143) 100 (85, 121)... Baseline DBP 66 (50, 91) 61 (52, 80)... Maximum SBP 155 (145, 209) 168 (136, 300)... Maximum DBP 82 (55, 115) 88 (64, 170)... Baseline PP 51 (26, 76) 38 (25, 57)... Maximum PP 82 (30, 121) 91 (52, 130)... Baseline MAP 83 (66, 99) 74 (63, 88)... Maximum MAP 109 (86, 128) 117 (99, 213)... D SBP 42 (12, 78) 74 (38, 179).005 D DBP 18 ( 217, 54) 33 ( 22, 104).07 D PP 29 ( 214, 56) 48 (14, 75).02 D MAP 27 ( 27, 50) 46 (12, 129).01 * Numbers are medians, and numbers in parentheses are minimum and maximum values. Table 4 Comparison of Hemodynamic Change in Adrenal Cryoablation Patients with and without a -Blocker Premedication Variable With a -Blocker Premedication ( n = 7) * Without a -Blocker Premedication ( n = 5) * P Value D SBP 67 (38, 122) 114 (74, 179).034 D DBP 24 ( ) 45 (26, 104).07 D PP 44 (14, 67) 65 (38, 75).17 D MAP 38 (12, 83) 68 (42, 129).06 * Numbers are medians, and numbers in parentheses are minimum and maximum values. thermal injury and adjacent organ damage. This contrasts with RF ablation, where the ablation procedure can be monitored with MR imaging, although monitoring with this modality can be technically challenging. As a result, most centers use CT or ultrasonography for electrode placement and use experience to predict tissue coverage, which can be difficult. Our case series is the first, to our knowledge, to include analysis of hemodynamic change during percutaneous adrenal cryoablation. Our results illustrate a significant increase in change in SBP, PP, and MAP in patients undergoing adrenal cryoablation when compared with their kidney cryoablation counterparts. Given the catecholamine-secreting nature of the adrenal gland, these results are not unexpected. Six patients in our study experienced hypertensive crisis during the cryoablation procedure, a complication observed by others ( 21 ). Five of the six cases of hypertensive crisis occurred during the final, active thaw cycle, with the remaining episode occurring during the immediate postablation period. During the first, passive thaw, mild blood pressure changes may be observed, and other researchers ( 21 ) have noted episodes of hypertensive crisis during this period. However, during the final, active thaw, helium gas is passed within the cryoprobe, resulting in increased temperatures to thaw the tumor to allow probe removal. With active thawing of the treated tumor, we hypothesize that there is greater release of catecholamines from lysed cells. Increased vigilance and coordination with the anesthesia team is important during this time of the procedure. We use direct, arterial blood pressure monitoring in all adrenal ablation procedures. Direct, arterial blood pressure monitoring enables prompt detection of hemodynamic changes. Although the method of hemodynamic monitoring may differ on the basis of institutional preference, close communication with the anesthesia care team during adrenal cryoablation is vital to ensure patient safety. Our analysis of the hemodynamic changes in patients with metastatic disease involving the adrenal gland who were premedicated with a -blockers suggests that these patients should be pharmacologically pretreated in a way similar to that for the pretreatment of patients undergoing adrenalectomy for pheochromocytoma. More specifically, pretreatment with 10 to 60 mg of oral phenoxybenzamine for days prior to ablation coupled with subsequent titration of b -blocker is suggested. a -Blockers are used be cause of their capability to mitigate or prevent catecholaminemediated vasoconstriction during or following tumor manipulation. b -Blockers also have a role in the treatment of these patients; however, it deserves mention that b -blockers are not administered independent of a -adrenergic blockade because the former decrease myocardial contractility, which in the face of increased systemic vascular resistance may result in heart failure. Administration of both classes of medications should be guided by one with expertise in such medical treatment (eg, an endocrinologist). Should breakthrough hypertension occur during the procedure, management of the acute crisis necessitates close coordination between the anesthesia and radiology care teams, with diligent monitoring, as well as aggressive management of the patient s hemodynamic status ( 22 ). These recommendations may also extend to ablation of lesions in the posterior aspect of the right lobe of the liver owing to the risk of adjacent right adrenal injury and subsequent hypertensive crisis ( 23 ). Cryoablation for the treatment of metastatic disease involving the adrenal gland can be performed safely and with high local control rates. However, cryoablation is not without limitations. Primarily, the cryoablation technique precludes the capability to obtain tissue 306 radiology.rsna.org n Radiology: Volume 258: Number 1 January 2011
7 margins for pathologic analysis. Therefore, treatment success is ultimately determined by using serial follow-up imaging without pathologic confirmation. Although complication rates are low with the use of cryoablation, hemorrhage and collateral tissue injury are the most common risks associated with this treatment ( 24 ). There were also several limitations to this specific study. The primary study limitation was our small sample size ( n = 12). Another limitation of the study was possible bias in the selection of patients for consultation with an endocrinologist prior to ablation. Patients in this study were seen by an endocrinologist at the discretion of the referring physician. Although our mean follow-up period was 18 months, further investigation with long-term follow-up is necessary to show durability of treatment. Disclosures of Potential Conflicts of Interest: B.T.W. No potential conflicts of interest to disclose. T.D.A. No potential conflicts of interest to disclose. D.A.N. No potential conflicts of interest to disclose. C.T.W. No potential conflicts of interest to disclose. M.R.C. Financial activities related to the present article: none to disclose. Financial activities not related to the present article: received funding for a separate research study from Endocare and research grants from Siemens Medical Systems. Other relationships: none to disclose. B.C.L. No potential conflicts of interest to disclose. P.C.C. No potential conflicts of interest to disclose. J.N.M. No potential conflicts of interest to disclose. J.W.C. No potential conflicts of interest to disclose. References 1. Beland MD, Mayo-Smith WW. Ablation of adrenal neoplasms. Abdom Imaging 2009 ; 34 ( 5 ): Paul CA, Virgo KS, Wade TP, Audisio RA, Johnson FE. Adrenalectomy for isolated adrenal metastases from non-adrenal cancer. Int J Oncol 2000 ; 17 ( 1 ): Lo CY, van Heerden JA, Soreide JA, et al. Adrenalectomy for metastatic disease to the adrenal glands. Br J Surg 1996 ; 83 ( 4 ): Kim SH, Brennan MF, Russo P, Burt ME, Coit DG. The role of surgery in the treatment of clinically isolated adrenal metastasis. Cancer 1998 ; 82 ( 2 ): Uberoi J, Munver R. Surgical management of metastases to the adrenal gland: open, laparoscopic, and ablative approaches. Curr Urol Rep 2009 ; 10 ( 1 ): Nahum Goldberg S, Dupuy DE. Image-guided radiofrequency tumor ablation: challenges and opportunities. I. J Vasc Interv Radiol 2001 ; 12 ( 9 ): Wood BJ, Abraham J, Hvizda JL, Alexander HR, Fojo T. Radiofrequency ablation of adrenal tumors and adrenocortical carcinoma metastases. Cancer 2003 ; 97 ( 3 ): Mayo-Smith WW, Dupuy DE. Adrenal neoplasms: CT-guided radiofrequency ablation preliminary results. Radiology 2004 ; 231 ( 1 ): Onik G. Image-guided prostate cryosurgery: state of the art. Cancer Contr 2001 ; 8 ( 6 ): Sewell PE Jr, Jackson MS, Dhillon GS. Percutaneous MRI guided cryosurgery of bone tumors [abstr]. Radiology 2002 ; 225 ( P ): Shingleton WB, Sewell PE Jr. Percutaneous renal tumor cryoablation with magnetic resonance imaging guidance. J Urol 2001 ; 165 ( 3 ): Sewell PE, Howard JC, Shingleton WB, Harrison RB. Interventional magnetic resonance image-guided percutaneous cryoablation of renal tumors. South Med J 2003 ; 96 ( 7 ): Beland MD, Dupuy DE, Mayo-Smith WW. Percutaneous cryoablation of symptomatic extraabdominal metastatic disease: preliminary results. AJR Am J Roentgenol 2005 ; 184 ( 3 ): Wang H, Littrup PJ, Duan Y, Zhang Y, Feng H, Nie Z. Thoracic masses treated with percutaneous cryotherapy: initial experience with more than 200 procedures. Radiology 2005 ; 235 ( 1 ): Shafir M, Shapiro R, Sung M, Warner R, Sicular A, Klipfel A. Cryoablation of unresectable malignant liver tumors. Am J Surg 1996 ; 171 ( 1 ): Schulsinger DA, Sosa RE, Perlmutter AA, Vaughan ED Jr. Acute and chronic interstitial cryotherapy of the adrenal gland as a treatment modality. J Endourol 1999 ; 13 ( 4 ): American Joint Committee on Cancer. AJCC Cancer Staging Manual. 6th ed. New York, NY : Springer, Goldberg SN, Grassi CJ, Cardella JF, et al. Image-guided tumor ablation: standardization of terminology and reporting criteria. J Vasc Interv Radiol 2005 ; 16 ( 6 ): Varon J. Treatment of acute severe hypertension: current and newer agents. Drugs 2008 ; 68 ( 3 ): Trotti A, Colevas A, Setser A, et al. CTCAE v3.0: development of a comprehensive grading system for the adverse effects of cancer treatment. Semin Radiat Oncol 2003 ; 13 ( 3 ): Tsoumakidou G, Buy X, Zickler P, Zupan M, Douchet MP, Gangi A. Life-threatening complication during percutaneous ablation of adrenal gland metastasis: Takotsubo syndrome. Cardiovasc Intervent Radiol 2010 ; 33 ( 3 ): Atwell TD, Wass CT, Charboneau JW, Callstrom MR, Farrell MA, Sengupta S. Malignant hypertension during cryoablation of an adrenal gland tumor. J Vasc Interv Radiol 2006 ; 17 ( 3 ): Onik G, Onik C, Medary I, et al. Life-threatening hypertensive crises in two patients undergoing hepatic radiofrequency ablation. AJR Am J Roentgenol 2003 ; 181 ( 2 ): Seifert JK, Morris DL. World survey on the complications of hepatic and prostate cryotherapy. World J Surg 1999 ; 23 ( 2 ): ; discussion Radiology: Volume 258: Number 1 January 2011 n radiology.rsna.org 307
Percutaneous cryoablation of lung tumors
 Percutaneous cryoablation of lung tumors Poster No.: C-0811 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit C. Pusceddu 1, L. Melis 1, G. B. Meloni 2 ; 1 Cagliari/IT, 2 Sassari/IT Lung,
Percutaneous cryoablation of lung tumors Poster No.: C-0811 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit C. Pusceddu 1, L. Melis 1, G. B. Meloni 2 ; 1 Cagliari/IT, 2 Sassari/IT Lung,
Percutaneous Renal Cryoablation After Partial Nephrectomy: Technical Feasibility, Complications and Outcomes
 Percutaneous Renal Cryoablation After Partial Nephrectomy: Technical Feasibility, Complications and Outcomes Ryan M. Hegg, Grant D. Schmit,* Stephen A. Boorjian, Robert J. McDonald, A. Nicholas Kurup,
Percutaneous Renal Cryoablation After Partial Nephrectomy: Technical Feasibility, Complications and Outcomes Ryan M. Hegg, Grant D. Schmit,* Stephen A. Boorjian, Robert J. McDonald, A. Nicholas Kurup,
Imaging-Guided Adrenal Tumor Ablation
 Genitourinary Imaging Review Uppot and Gervais Imaging-Guided Adrenal Tumor Ablation Genitourinary Imaging Review FOCUS ON: Raul N. Uppot 1 Debra A. Gervais 1,2 Uppot RN, Gervais DA Keywords: cryoablation,
Genitourinary Imaging Review Uppot and Gervais Imaging-Guided Adrenal Tumor Ablation Genitourinary Imaging Review FOCUS ON: Raul N. Uppot 1 Debra A. Gervais 1,2 Uppot RN, Gervais DA Keywords: cryoablation,
General summary GENERAL SUMMARY
 General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
Currently, radiofrequency (RF) ablation is the most commonly
 Diagn Interv Radiol 2010; 16:90 95 Turkish Society of Radiology 2010 INTERVENTIONAL RADIOLOGY REVIEW Percutaneous cryoablation techniques and clinical applications Servet Tatlı, Murat Acar, Kemal Tuncalı,
Diagn Interv Radiol 2010; 16:90 95 Turkish Society of Radiology 2010 INTERVENTIONAL RADIOLOGY REVIEW Percutaneous cryoablation techniques and clinical applications Servet Tatlı, Murat Acar, Kemal Tuncalı,
Is renal cryoablation becoming an effective alternative to partial nephrectomy?
 Is renal cryoablation becoming an effective alternative to partial nephrectomy? J GARNON 1, G TSOUMAKIDOU 1, H LANG 2, A GANGI 1 1 department of interventional radiology 2 department of urology University
Is renal cryoablation becoming an effective alternative to partial nephrectomy? J GARNON 1, G TSOUMAKIDOU 1, H LANG 2, A GANGI 1 1 department of interventional radiology 2 department of urology University
PerCryo Ablation CLINICAL DATA REVIEW 2015
 PerCryo Ablation CLINICAL DATA REVIEW 2015 The information contained in this booklet is being provided as a representative summary only and does not contain all available published data on cryoablation.
PerCryo Ablation CLINICAL DATA REVIEW 2015 The information contained in this booklet is being provided as a representative summary only and does not contain all available published data on cryoablation.
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation. Basics. What is Percutaneous Ablation? Where are your kidneys?
 Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
Corporate Medical Policy
 Corporate Medical Policy Cryosurgical Ablation of Primary or Metastatic Liver Tumors File Name: Origination: Last CAP Review: Next CAP Review: Last Review: cryosurgical_ablation_of_primary_or_metastatic_liver_tumors
Corporate Medical Policy Cryosurgical Ablation of Primary or Metastatic Liver Tumors File Name: Origination: Last CAP Review: Next CAP Review: Last Review: cryosurgical_ablation_of_primary_or_metastatic_liver_tumors
Radiofrequency Ablation (RFA) For Lung Tumors: Seven Years Experience.
 Radiofrequency Ablation (RFA) For Lung Tumors: Seven Years Experience. Poster No.: C-1619 Congress: ECR 2011 Type: Scientific Exhibit Authors: G. DE VENUTO 1, G. XHEPA 1, M. DE CHIARA 1, M. Mangini 2,
Radiofrequency Ablation (RFA) For Lung Tumors: Seven Years Experience. Poster No.: C-1619 Congress: ECR 2011 Type: Scientific Exhibit Authors: G. DE VENUTO 1, G. XHEPA 1, M. DE CHIARA 1, M. Mangini 2,
oth percutaneous radiofrequency ablation (RFA) and cryoablation have shown favorable local tumor
 Vascular and Interventional Radiology Original Research Atwell et al. Radiofrequency Ablation and Cryoablation of Small Renal Masses Vascular and Interventional Radiology Original Research Thomas D. Atwell
Vascular and Interventional Radiology Original Research Atwell et al. Radiofrequency Ablation and Cryoablation of Small Renal Masses Vascular and Interventional Radiology Original Research Thomas D. Atwell
Percutaneous Radiofrequency Ablation of Lung Malignant Tumours: Survival, disease progression and complication rates
 Percutaneous Radiofrequency Ablation of Lung Malignant Tumours: Survival, disease progression and complication rates Poster No.: C-2576 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit
Percutaneous Radiofrequency Ablation of Lung Malignant Tumours: Survival, disease progression and complication rates Poster No.: C-2576 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit
CRYOABLATION OF SOLID TUMORS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-05 Effective Date: 06/16/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-05 Effective Date: 06/16/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
HEPATIC METASTASES. We can state 3 types of metastases depending on their treatment options:
 HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
THE FACTS YOU NEED TO KNOW
 PHEOCHROMOCYTOMA THE FACTS YOU NEED TO KNOW Pheochromocytoma is a part of the pheochromocytoma and paraganglioma group of syndromes. A pheochromocytoma is a tumor arising in the adrenal gland medulla.
PHEOCHROMOCYTOMA THE FACTS YOU NEED TO KNOW Pheochromocytoma is a part of the pheochromocytoma and paraganglioma group of syndromes. A pheochromocytoma is a tumor arising in the adrenal gland medulla.
Index. C Cancer, Carcinoid syndrome, 413. D DCIS. See Ductal carcinoma in situ (DCIS) DEB-TACE. See Drug eluting beads-tace (DEB-TACE)
 Index A Ablation, 179 199, 843 853 devices, 179, 199 liver tumors, 527 techniques, 516 Ablative radiation therapy, 456 Accelerated partial breast, 894, 896 898 Adaptive radiation therapy, 586, 598, 602
Index A Ablation, 179 199, 843 853 devices, 179, 199 liver tumors, 527 techniques, 516 Ablative radiation therapy, 456 Accelerated partial breast, 894, 896 898 Adaptive radiation therapy, 586, 598, 602
Mahrad Paymani, MD Lake Medical Imaging
 Mahrad Paymani, MD Lake Medical Imaging Background: My name is Mahrad Paymani. I am an Interventional and General Radiologist. I attended four years of college (at UNC Greensboro), four years of medical
Mahrad Paymani, MD Lake Medical Imaging Background: My name is Mahrad Paymani. I am an Interventional and General Radiologist. I attended four years of college (at UNC Greensboro), four years of medical
Less is more: Merit of Non-Surgical Management of Kidney Cancer
 Less is more: Merit of Non-Surgical Management of Kidney Cancer S A T U R D A Y, A U G U S T 2 0 G H A S S A N E L - H A D D A D, MD A S S I S TA N T M E M B E R, VA S C U L A R A N D I N T E R V E N T
Less is more: Merit of Non-Surgical Management of Kidney Cancer S A T U R D A Y, A U G U S T 2 0 G H A S S A N E L - H A D D A D, MD A S S I S TA N T M E M B E R, VA S C U L A R A N D I N T E R V E N T
RENAL CANCER. Dr. Giandomenico Roviello. Oncologia Medica Ospedale San Donato Arezzo
 RENAL CANCER Dr. Giandomenico Roviello Oncologia Medica Ospedale San Donato Arezzo Abstracts Abstract Number: 433. Cryoablation of ct1 renal masses in the healthy patient: Early outcomes from Mayo Clinic.
RENAL CANCER Dr. Giandomenico Roviello Oncologia Medica Ospedale San Donato Arezzo Abstracts Abstract Number: 433. Cryoablation of ct1 renal masses in the healthy patient: Early outcomes from Mayo Clinic.
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer
 Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
RFA of Tumors of the Lung: How and Why. Radiofrequency Ablation. Radiofrequency Ablation. RFA of pulmonary metastases. Radiofrequency Ablation of Lung
 RFA of Tumors of the Lung: How and Why Radiofrequency Ablation of Lung Ernest Scalzetti MD SUNY Upstate Medical University Syracuse NY FDA WARNING: Off-label use of a medical device Radiofrequency Ablation
RFA of Tumors of the Lung: How and Why Radiofrequency Ablation of Lung Ernest Scalzetti MD SUNY Upstate Medical University Syracuse NY FDA WARNING: Off-label use of a medical device Radiofrequency Ablation
CT-Guided Percutaneous Microwave Ablation of Adrenal Malignant Carcinoma
 CT-Guided Percutaneous Microwave Ablation of Adrenal Malignant Carcinoma Preliminary Results Xin Li, MD; Weijun Fan, MD; Liang Zhang, MD; Ming Zhao, MD; Zilin Huang, MD; Wang Li, MD; Yangkui Gu, MD; Fei
CT-Guided Percutaneous Microwave Ablation of Adrenal Malignant Carcinoma Preliminary Results Xin Li, MD; Weijun Fan, MD; Liang Zhang, MD; Ming Zhao, MD; Zilin Huang, MD; Wang Li, MD; Yangkui Gu, MD; Fei
Complications of percutaneous lung radiofrequency ablation
 Complications of percutaneous lung radiofrequency ablation Poster No.: C-556 Congress: ECR 2009 Type: Educational Exhibit Topic: Interventional Radiology Authors: A. Afaq, S. Khan, U. Patel, E. Leen; London/UK
Complications of percutaneous lung radiofrequency ablation Poster No.: C-556 Congress: ECR 2009 Type: Educational Exhibit Topic: Interventional Radiology Authors: A. Afaq, S. Khan, U. Patel, E. Leen; London/UK
cryosurgical_ablation_of_miscellaneous_solid_tumors 1/2007 5/2017 5/2018 5/2017
 Corporate Medical Policy Cryosurgical Ablation of Miscellaneous Solid Tumors Other File Name: Origination: Last CAP Review: Next CAP Review: Last Review: cryosurgical_ablation_of_miscellaneous_solid_tumors
Corporate Medical Policy Cryosurgical Ablation of Miscellaneous Solid Tumors Other File Name: Origination: Last CAP Review: Next CAP Review: Last Review: cryosurgical_ablation_of_miscellaneous_solid_tumors
PerCryo Ablation CLINICAL DATA REVIEW 2016
 PerCryo Ablation CLINICAL DATA REVIEW 2016 The information contained in this booklet is being provided as a representative summary only and does not contain all available published data on cryoablation.
PerCryo Ablation CLINICAL DATA REVIEW 2016 The information contained in this booklet is being provided as a representative summary only and does not contain all available published data on cryoablation.
Radiofrequency ablation of lung tumors using a multitined expandable. electrode: impact of the electrode's array diameter on local tumor
 1 Radiofrequency ablation of lung tumors using a multitined expandable electrode: impact of the electrode's array diameter on local tumor progression ABSTRACT Purpose: To retrospectively investigate the
1 Radiofrequency ablation of lung tumors using a multitined expandable electrode: impact of the electrode's array diameter on local tumor progression ABSTRACT Purpose: To retrospectively investigate the
Microwave ablation of liver metastases to overcome radiofrequency ablation limits
 Microwave ablation of liver metastases to overcome radiofrequency ablation limits Poster No.: C-2456 Congress: ECR 2012 Type: Scientific Exhibit Authors: G. Carrafiello 1, A. M. Ierardi 1, V. Molinelli
Microwave ablation of liver metastases to overcome radiofrequency ablation limits Poster No.: C-2456 Congress: ECR 2012 Type: Scientific Exhibit Authors: G. Carrafiello 1, A. M. Ierardi 1, V. Molinelli
Cryosurgical Ablation of Breast Fibroadenomas
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
ADRENAL INCIDENTALOMA. Jamii St. Julien
 ADRENAL INCIDENTALOMA Jamii St. Julien Outline Definition Differential Evaluation Treatment Follow up Questions Case Definition The phenomenon of detecting an otherwise unsuspected adrenal mass on radiologic
ADRENAL INCIDENTALOMA Jamii St. Julien Outline Definition Differential Evaluation Treatment Follow up Questions Case Definition The phenomenon of detecting an otherwise unsuspected adrenal mass on radiologic
RF Ablation: indication, technique and imaging follow-up
 RF Ablation: indication, technique and imaging follow-up Trongtum Tongdee, M.D. Radiology Department, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand Objective Basic knowledge
RF Ablation: indication, technique and imaging follow-up Trongtum Tongdee, M.D. Radiology Department, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand Objective Basic knowledge
Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation
 Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation Katie S. Nason, MD MPH AATS Focus on Thoracic: Mastering Surgical Innovation October 28, 2017 No disclosures Radiofrequency ablative
Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation Katie S. Nason, MD MPH AATS Focus on Thoracic: Mastering Surgical Innovation October 28, 2017 No disclosures Radiofrequency ablative
Percutaneous Ultrasound-guided Radiofrequency Ablation of Colorectal Liver Metastases
 Chin J Radiol 2005; 30: 153-158 153 Percutaneous Ultrasound-guided Radiofrequency Ablation of Colorectal Liver Metastases YI-YOU CHIOU YI-HONG CHOU JEN-HUEY CHIANG HSIN-KAI WANG CHENG-YEN CHANG Department
Chin J Radiol 2005; 30: 153-158 153 Percutaneous Ultrasound-guided Radiofrequency Ablation of Colorectal Liver Metastases YI-YOU CHIOU YI-HONG CHOU JEN-HUEY CHIANG HSIN-KAI WANG CHENG-YEN CHANG Department
Patient Selection for Ablative Therapies. Adrian D Joyce Leeds UK
 Patient Selection for Ablative Adrian D Joyce Leeds UK Therapy Renal Cell Ca USA: 30,000 new cases annually >12,000 deaths RCC accounts for 3% of all adult malignancy 40% of patients will die from their
Patient Selection for Ablative Adrian D Joyce Leeds UK Therapy Renal Cell Ca USA: 30,000 new cases annually >12,000 deaths RCC accounts for 3% of all adult malignancy 40% of patients will die from their
Stereotactic ablative body radiotherapy for renal cancer
 1 EVIDENCE SUMMARY REPORT Stereotactic ablative body radiotherapy for renal cancer Questions to be addressed 1. What is the clinical effectiveness of stereotactic ablative body radiotherapy for inoperable
1 EVIDENCE SUMMARY REPORT Stereotactic ablative body radiotherapy for renal cancer Questions to be addressed 1. What is the clinical effectiveness of stereotactic ablative body radiotherapy for inoperable
Staging & Current treatment of HCC
 Staging & Current treatment of HCC Dr.: Adel El Badrawy Badrawy; ; M.D. Staging & Current ttt of HCC Early stage HCC is typically silent. HCC is often advanced at first manifestation. The selective ttt
Staging & Current treatment of HCC Dr.: Adel El Badrawy Badrawy; ; M.D. Staging & Current ttt of HCC Early stage HCC is typically silent. HCC is often advanced at first manifestation. The selective ttt
St. Dominic s Annual Cancer Report Outcomes
 St. Dominic s 2017 Annual Cancer Report Outcomes Cancer Program Practice Profile Reports (CP3R) St. Dominic s Cancer Committee monitors and ensures that patients treated at St. Dominic Hospital receive
St. Dominic s 2017 Annual Cancer Report Outcomes Cancer Program Practice Profile Reports (CP3R) St. Dominic s Cancer Committee monitors and ensures that patients treated at St. Dominic Hospital receive
Synchronous Hepatic Cryotherapy and Resection
 HPB Surgery, 2000, Vol. 11, pp. 379-382 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 2000, Vol. 11, pp. 379-382 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
Populations Interventions Comparators Outcomes Individuals: With unresectable primary hepatocellular carcinoma amenable to locoregional therapy
 Protocol Cryosurgical Ablation of Primary or Metastatic Liver Tumors (70175) Medical Benefit Effective Date: 07/01/10 Next Review Date: 01/19 Preauthorization No Review Dates: 02/07, 02/08, 01/09, 01/10,
Protocol Cryosurgical Ablation of Primary or Metastatic Liver Tumors (70175) Medical Benefit Effective Date: 07/01/10 Next Review Date: 01/19 Preauthorization No Review Dates: 02/07, 02/08, 01/09, 01/10,
Endocrine MR. Jan 30, 2015 Michael LaFata, MD
 Endocrine MR Jan 30, 2015 Michael LaFata, MD Brief case 55-year-old female in ED PMH: HTN, DM2, HLD, GERD CC: Epigastric/LUQ abdominal pain, N/V x2 days AF, HR 103, BP 155/85, room air CMP: Na 133, K 3.6,
Endocrine MR Jan 30, 2015 Michael LaFata, MD Brief case 55-year-old female in ED PMH: HTN, DM2, HLD, GERD CC: Epigastric/LUQ abdominal pain, N/V x2 days AF, HR 103, BP 155/85, room air CMP: Na 133, K 3.6,
Section Activity Activity Description Details Reference(s)
 Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with Renal Cell Carcinoma AA Cancer Centre Referrals Not routine pre-op referral indicated
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with Renal Cell Carcinoma AA Cancer Centre Referrals Not routine pre-op referral indicated
Risk factors for occurrence of local tumor progression after percutaneous radiofrequency ablation for lung neoplasms
 Diagn Interv Radiol 2007; 13:199 203 Turkish Society of Radiology 2007 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Risk factors for occurrence of local tumor progression after percutaneous radiofrequency
Diagn Interv Radiol 2007; 13:199 203 Turkish Society of Radiology 2007 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Risk factors for occurrence of local tumor progression after percutaneous radiofrequency
ONCOLOGIC PERCUTANEOUS INTERVENTION: 2015 UPDATE HANH VU NGHIEM, MD OAKLAND UNIVERSITY WILLIAM BEAUMONT SCHOOL OF MEDICINE
 ONCOLOGIC PERCUTANEOUS INTERVENTION: 2015 UPDATE HANH VU NGHIEM, MD OAKLAND UNIVERSITY WILLIAM BEAUMONT SCHOOL OF MEDICINE ONCOLOGIC PERCUTANEOUS IMAGE GUIDED TUMOR ABLATION Evolving, growing and increasingly
ONCOLOGIC PERCUTANEOUS INTERVENTION: 2015 UPDATE HANH VU NGHIEM, MD OAKLAND UNIVERSITY WILLIAM BEAUMONT SCHOOL OF MEDICINE ONCOLOGIC PERCUTANEOUS IMAGE GUIDED TUMOR ABLATION Evolving, growing and increasingly
Multidisciplinary management of retroperitoneal sarcomas
 Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous cryotherapy for renal cancer Treating kidney tumours by freezing
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous cryotherapy for renal cancer Treating kidney tumours by freezing
Over 35,000 new cases of renal
 DEBRA A. GERVAIS, MD Director of Abdominal Interventional Radiology Assistant Professor of Radiology RONALD S. ARELLANO, MD Director of Abdominal Intervention Clinic Operations Instructor of Radiology
DEBRA A. GERVAIS, MD Director of Abdominal Interventional Radiology Assistant Professor of Radiology RONALD S. ARELLANO, MD Director of Abdominal Intervention Clinic Operations Instructor of Radiology
The Frequency and Significance of Small (15 mm) Hepatic Lesions Detected by CT
 535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
Cryosurgery in Cancer Treatment: Questions and Answers
 Cryosurgery in Cancer Treatment: Questions and Answers Key Points Cryosurgery is a technique for freezing and killing abnormal cells. It is used to treat some kinds of cancer and some precancerous or noncancerous
Cryosurgery in Cancer Treatment: Questions and Answers Key Points Cryosurgery is a technique for freezing and killing abnormal cells. It is used to treat some kinds of cancer and some precancerous or noncancerous
Published: Address correspondence to Vidal-Jove Joan:
 Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
BJUI. Solitary, isolated metastatic disease to the kidney: Memorial Sloan-Kettering Cancer Center experience
 ; 2010 Urological Oncology SOLITARY, ISOLATED METASTATIC DISEASE TO THE KIDNEY ADAMY ET AL. BJUI Solitary, isolated metastatic disease to the kidney: Memorial Sloan-Kettering Cancer Center experience Ari
; 2010 Urological Oncology SOLITARY, ISOLATED METASTATIC DISEASE TO THE KIDNEY ADAMY ET AL. BJUI Solitary, isolated metastatic disease to the kidney: Memorial Sloan-Kettering Cancer Center experience Ari
Imaging-Guided Percutaneous Cryotherapy of Bone and Soft-Tissue Tumors: What Is the Impact on the Muscles Around the Ablation Site?
 Vascular and Interventional Radiology Original Research Bing et al. Cryoablation of Bone and Soft-Tissue Tumors Vascular and Interventional Radiology Original Research Fabrice Bing 1 Julien Garnon 1 Georgia
Vascular and Interventional Radiology Original Research Bing et al. Cryoablation of Bone and Soft-Tissue Tumors Vascular and Interventional Radiology Original Research Fabrice Bing 1 Julien Garnon 1 Georgia
Saline-Infused Bipolar Radiofrequency Ablation of High-Risk Spinal and Paraspinal Neoplasms
 Radiofreque ncy blation of Spinal Neoplasms Radiofrequency blation Technical Innovation M E D E N T U R I L I M G I N G JR 2006; 186:S322 S326 0361 803X/06/1865 S322 merican Roentgen Ray Society Y O Xavier
Radiofreque ncy blation of Spinal Neoplasms Radiofrequency blation Technical Innovation M E D E N T U R I L I M G I N G JR 2006; 186:S322 S326 0361 803X/06/1865 S322 merican Roentgen Ray Society Y O Xavier
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Pheochromocytoma AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGY ILLINOIS CHAPTER OCTOBER 13, 2018
 Pheochromocytoma AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGY ILLINOIS CHAPTER OCTOBER 13, 2018 Steven A. De Jong, M.D., FACS, FACE Professor and Vice Chair of Surgery Chief, Division of General Surgery
Pheochromocytoma AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGY ILLINOIS CHAPTER OCTOBER 13, 2018 Steven A. De Jong, M.D., FACS, FACE Professor and Vice Chair of Surgery Chief, Division of General Surgery
Usefulness of R.E.N.A.L. Nephrometry Scoring System for Predicting Outcomes and Complications of Percutaneous Ablation of 751 Renal Tumors
 Usefulness of R.E.N.A.L. Nephrometry Scoring System for Predicting Outcomes and Complications of Percutaneous Ablation of 751 Renal Tumors Grant D. Schmit,* R. Houston Thompson, Anil N. Kurup, Adam J.
Usefulness of R.E.N.A.L. Nephrometry Scoring System for Predicting Outcomes and Complications of Percutaneous Ablation of 751 Renal Tumors Grant D. Schmit,* R. Houston Thompson, Anil N. Kurup, Adam J.
Daniela Faivovich K., MS VII Universidad de Chile Gillian Lieberman, MD Harvard Medical School
 Daniela Faivovich K., MS VII Universidad de Chile Gillian Lieberman, MD Harvard Medical School May 21st, 2010 56 year old male patient History of hypertension, hyperlipidemia and insulin-resistance 2009:
Daniela Faivovich K., MS VII Universidad de Chile Gillian Lieberman, MD Harvard Medical School May 21st, 2010 56 year old male patient History of hypertension, hyperlipidemia and insulin-resistance 2009:
Cryoablation of extra-abdominal desmoid tumours: initial experience and results
 Cryoablation of extra-abdominal desmoid tumours: initial experience and results Poster No.: C-2542 Congress: ECR 2013 Type: Scientific Exhibit Authors: G. Tsoumakidou, J. Garnon, I. Enescu, J.-P. Bergerat,
Cryoablation of extra-abdominal desmoid tumours: initial experience and results Poster No.: C-2542 Congress: ECR 2013 Type: Scientific Exhibit Authors: G. Tsoumakidou, J. Garnon, I. Enescu, J.-P. Bergerat,
Radiofrequency Ablation versus Microwave Ablation in HCC and Liver Metastases
 Radiofrequency Ablation versus Microwave Ablation in HCC and Liver Metastases Thomas J. Vogl, B. Panahi, N. Nour-Eldin I D I R: Institute of Diagnostic and Interventional Radiology Goethe University Frankfurt,
Radiofrequency Ablation versus Microwave Ablation in HCC and Liver Metastases Thomas J. Vogl, B. Panahi, N. Nour-Eldin I D I R: Institute of Diagnostic and Interventional Radiology Goethe University Frankfurt,
ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain
 ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain OUR APPROACH Incidental adrenal nodule/mass Isaac R Francis, M.B;B.S University of Michigan, Ann Arbor, Michigan Disclosures None (in memory) M Korobkin,
ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain OUR APPROACH Incidental adrenal nodule/mass Isaac R Francis, M.B;B.S University of Michigan, Ann Arbor, Michigan Disclosures None (in memory) M Korobkin,
Microwave ablation of lung tumors
 Microwave ablation of lung tumors Poster No.: C-2490 Congress: ECR 2012 Type: Scientific Exhibit Authors: G. Carrafiello 1, A. M. Ierardi 1, E. Macchi 1, N. Lucchina 1, V. Molinelli 1, E. Duka 1, C. Pellegrino
Microwave ablation of lung tumors Poster No.: C-2490 Congress: ECR 2012 Type: Scientific Exhibit Authors: G. Carrafiello 1, A. M. Ierardi 1, E. Macchi 1, N. Lucchina 1, V. Molinelli 1, E. Duka 1, C. Pellegrino
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Jason A. Pietryga, MD Michael D. Beland, MD Damian E. Dupuy, MD William W. Mayo-Smith, MD. Purpose: Materials and Methods: Results: Conclusion:
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Jason A. Pietryga,
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Jason A. Pietryga,
ADRENAL LESIONS 10/09/2012. Adrenal + lesion. Introduction. Common causes. Anatomy. Financial disclosure. Dr. Boraiah Sreeharsha. Nothing to declare
 ADRENAL LESIONS Financial disclosure Nothing to declare Dr. Boraiah Sreeharsha MBBS;FRCR;FRCPSC Introduction Adrenal + lesion Adrenal lesions are common 9% of the population Increase in the detection rate
ADRENAL LESIONS Financial disclosure Nothing to declare Dr. Boraiah Sreeharsha MBBS;FRCR;FRCPSC Introduction Adrenal + lesion Adrenal lesions are common 9% of the population Increase in the detection rate
Locoregional Treatments for HCC Applications in Transplant Candidates. Locoregional Treatments for HCC Applications in Transplant Candidates
 Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Combined Percutaneous Radiofrequency Ablation and Ethanol Injection of Renal Tumours: Midterm Results
 european urology 52 (2007) 777 784 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Combined Percutaneous Radiofrequency Ablation and Ethanol Injection of Renal
european urology 52 (2007) 777 784 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Combined Percutaneous Radiofrequency Ablation and Ethanol Injection of Renal
Radiofrequency Ablation of Liver Tumors
 Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Embolotherapy for Cholangiocarcinoma: 2016 Update
 Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Gold Anchor enables safe reach to inner organs
 Gold Anchor enables safe reach to inner organs Fine needles for cytology have been used >50 years in all parts of the human body with no to very little harm Gold Anchor comes pre-loaded in needles of the
Gold Anchor enables safe reach to inner organs Fine needles for cytology have been used >50 years in all parts of the human body with no to very little harm Gold Anchor comes pre-loaded in needles of the
NIH Public Access Author Manuscript Eur J Radiol. Author manuscript; available in PMC 2013 September 25.
 NIH Public Access Author Manuscript Published in final edited form as: Eur J Radiol. 2012 August ; 81(8): 1702 1706. doi:10.1016/j.ejrad.2011.04.067. Estimated effective dose of CT-guided percutaneous
NIH Public Access Author Manuscript Published in final edited form as: Eur J Radiol. 2012 August ; 81(8): 1702 1706. doi:10.1016/j.ejrad.2011.04.067. Estimated effective dose of CT-guided percutaneous
A fatal case of an adrenal gland melanoma with a mysterious primary lesion
 ISPUB.COM The Internet Journal of Urology Volume 6 Number 2 A fatal case of an adrenal gland melanoma with a mysterious primary lesion A Adam, M Engelbrecht, I van Heerden Citation A Adam, M Engelbrecht,
ISPUB.COM The Internet Journal of Urology Volume 6 Number 2 A fatal case of an adrenal gland melanoma with a mysterious primary lesion A Adam, M Engelbrecht, I van Heerden Citation A Adam, M Engelbrecht,
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22
 Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
What is the role of partial nephrectomy in the context of active surveillance and renal ablation?
 What is the role of partial nephrectomy in the context of active surveillance and renal ablation? Dogu Teber Department of Urology University Hospital Heidelberg Coming from Heidelberg obligates to speak
What is the role of partial nephrectomy in the context of active surveillance and renal ablation? Dogu Teber Department of Urology University Hospital Heidelberg Coming from Heidelberg obligates to speak
Ablative techniques have rapidly
 MTTHEW R. CLLSTROM, MD, PhD ssistant Professor of Radiology J. WILLIM CHRONEU, MD Professor of Radiology Mayo Clinic College of Medicine Rochester, Minnesota Percutaneous blation: Safe, Effective Treatment
MTTHEW R. CLLSTROM, MD, PhD ssistant Professor of Radiology J. WILLIM CHRONEU, MD Professor of Radiology Mayo Clinic College of Medicine Rochester, Minnesota Percutaneous blation: Safe, Effective Treatment
New Energy Sources for Local Ablation Therapy. Jeong Kyong Lee, MD Ewha Womans University
 New Energy Sources for Local Ablation Therapy Jeong Kyong Lee, MD Ewha Womans University New Energy Sources for Local Ablation Therapy Microwave Ablation Irreversible Electroporation Cryoablation Microwave
New Energy Sources for Local Ablation Therapy Jeong Kyong Lee, MD Ewha Womans University New Energy Sources for Local Ablation Therapy Microwave Ablation Irreversible Electroporation Cryoablation Microwave
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Traumatic and Non Traumatic Adrenal Emergencies
 Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
Freezing and Frying Renal Cancers:
 Freezing and Frying Renal Cancers: An Imaging Menu for Radiologists to Understand Intra- and Post-Procedural Imaging Findings after Renal Tumor Ablation Heidi Coy BS, Michael Douek MD, Steven Raman MD
Freezing and Frying Renal Cancers: An Imaging Menu for Radiologists to Understand Intra- and Post-Procedural Imaging Findings after Renal Tumor Ablation Heidi Coy BS, Michael Douek MD, Steven Raman MD
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Percutaneous ablation of renal cell carcinoma. Where do we stand now? Sanja Stojanović, Spasić Aleksandar
 Percutaneous ablation of renal cell carcinoma Where do we stand now? Sanja Stojanović, Spasić Aleksandar Clinical Center of Vojvodina / Center for Radiology Novi Sad Serbia Renal cell carcinoma approximately
Percutaneous ablation of renal cell carcinoma Where do we stand now? Sanja Stojanović, Spasić Aleksandar Clinical Center of Vojvodina / Center for Radiology Novi Sad Serbia Renal cell carcinoma approximately
Solitary Contralateral Adrenal Metastases after Nephrectomy for Renal Cell Carcinoma
 Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
REVIEW. Distinguishing benign from malignant adrenal masses
 Cancer Imaging (2003) 3, 102 110 DOI: 10.1102/1470-7330.2003.0006 CI REVIEW Distinguishing benign from malignant adrenal masses Isaac R Francis Professor of Radiology, Department of Radiology, University
Cancer Imaging (2003) 3, 102 110 DOI: 10.1102/1470-7330.2003.0006 CI REVIEW Distinguishing benign from malignant adrenal masses Isaac R Francis Professor of Radiology, Department of Radiology, University
The Effect of Cranial Electrotherapy on Preoperative Anxiety and Hemodynamic Responses
 The Effect of Cranial Electrotherapy on Preoperative Anxiety and Hemodynamic Responses Page 1 Cranial Electrotherapy (CES) is a non pharmaceutical treatment for anxiety, depression, insomnia, stress, headache
The Effect of Cranial Electrotherapy on Preoperative Anxiety and Hemodynamic Responses Page 1 Cranial Electrotherapy (CES) is a non pharmaceutical treatment for anxiety, depression, insomnia, stress, headache
Liver Perfusion Analysis New Frontiers in Dynamic Volume Imaging. Case Study Brochure Chang Gung Memorial Hospital.
 New Frontiers in Dynamic Volume Imaging dynamic volume CT Case Study Brochure Chang Gung Memorial Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2010-2011. All rights
New Frontiers in Dynamic Volume Imaging dynamic volume CT Case Study Brochure Chang Gung Memorial Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2010-2011. All rights
PERCUTANEOUS CRYOABLATION
 PERCUTANEOUS CRYOABLATION IS A MINIMALLY INVASIVE, IMAGE-GUIDED TREATMENT THAT DESTROYS (ABLATES) TUMORS AND OTHER TARGETED TISSUE WITH EXTREME COLD WHILE SPARING SURROUNDING HEALTHY TISSUE. What are some
PERCUTANEOUS CRYOABLATION IS A MINIMALLY INVASIVE, IMAGE-GUIDED TREATMENT THAT DESTROYS (ABLATES) TUMORS AND OTHER TARGETED TISSUE WITH EXTREME COLD WHILE SPARING SURROUNDING HEALTHY TISSUE. What are some
RECURRENT ADRENAL DISEASE. Megan Applewhite Endorama 2/19/2015 SR , SC
 RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Canadian Guidelines for Management of the Small Renal Mass (SRM)
 Canadian Guidelines for Management of the Small Renal Mass (SRM) Michael A.S. Jewett*, Ricardo Rendon, Louis Lacombe, Pierre I. Karakiewicz, Simon Tanguay, Wes Kassouf, Mike Leveridge, Ilias Cagiannos,
Canadian Guidelines for Management of the Small Renal Mass (SRM) Michael A.S. Jewett*, Ricardo Rendon, Louis Lacombe, Pierre I. Karakiewicz, Simon Tanguay, Wes Kassouf, Mike Leveridge, Ilias Cagiannos,
A case of micturition syncope
 A case of micturition syncope Kimberly Bundick, PA-S S L I D E 1 Agenda Purpose Utilize case to illustrate classic finding of an interesting pathology Agenda Case study Epidemiology, etiology of disease
A case of micturition syncope Kimberly Bundick, PA-S S L I D E 1 Agenda Purpose Utilize case to illustrate classic finding of an interesting pathology Agenda Case study Epidemiology, etiology of disease
STANDARDIZED MANAGEMENT RECOMMENDATIONS FOR ADRENAL NODULES: EVIDENCE-BASED CONSENSUS POWERSCRIBE MACROS FROM AN ACADEMIC/PRIVATE PRACTICE
 STANDARDIZED MANAGEMENT RECOMMENDATIONS FOR ADRENAL NODULES: EVIDENCE-BASED CONSENSUS POWERSCRIBE MACROS FROM AN ACADEMIC/PRIVATE PRACTICE COLLABORATIVE Pamela Johnson 1, Darcy Wolfman 2, Upma Rawal 3,
STANDARDIZED MANAGEMENT RECOMMENDATIONS FOR ADRENAL NODULES: EVIDENCE-BASED CONSENSUS POWERSCRIBE MACROS FROM AN ACADEMIC/PRIVATE PRACTICE COLLABORATIVE Pamela Johnson 1, Darcy Wolfman 2, Upma Rawal 3,
came from a carcinoma and in 12 from a sarcoma. Ninety lesions were intrapulmonary and the as the chest wall and pleura. Details of the primary
 Thorax 1982;37:366-370 Thoracic metastases MARY P SHEPHERD From the Thoracic Surgical Unit, Harefield Hospital, Harefield ABSTRACI One hundred and four patients are reviewed who were found to have thoracic
Thorax 1982;37:366-370 Thoracic metastases MARY P SHEPHERD From the Thoracic Surgical Unit, Harefield Hospital, Harefield ABSTRACI One hundred and four patients are reviewed who were found to have thoracic
Focal Ablative Therapies for Kidney Cancer
 Focal Ablative Therapies for Kidney Cancer Robert J. Hamilton, MD, MPH, FRCSC Staff Urologist, Princess Margaret Cancer Centre Assistant Prof., Dept. of Surgery (Urology), University of Toronto ICUC January
Focal Ablative Therapies for Kidney Cancer Robert J. Hamilton, MD, MPH, FRCSC Staff Urologist, Princess Margaret Cancer Centre Assistant Prof., Dept. of Surgery (Urology), University of Toronto ICUC January
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Renal Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Timothy L. Miao 1, Ania Z. Kielar 2,3, Rebecca M. Hibbert 2, Nicola Schieda 2,3
 DOES LESION T1 SIGNAL INTENSITY RELATIVE TO LIVER PARENCHYMA PREDICT VISIBILITY ON ULTRASOUND? A clinical tool to determine feasibility of ultrasound-guided percutaneous interventions Timothy L. Miao 1,
DOES LESION T1 SIGNAL INTENSITY RELATIVE TO LIVER PARENCHYMA PREDICT VISIBILITY ON ULTRASOUND? A clinical tool to determine feasibility of ultrasound-guided percutaneous interventions Timothy L. Miao 1,
Title: What is the role of pre-operative PET/PET-CT in the management of patients with
 Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Percutaneous Cryoablation of Lung Tumors: Feasibility and Safety
 CLINICAL STUDY Percutaneous Cryoablation of Lung Tumors: Feasibility and Safety Masanori Inoue, MD, Seishi Nakatsuka, MD, PhD, Hideki Yashiro, MD, Nobutake Ito, MD, Yotaro Izumi, MD, PhD, Yoshikane Yamauchi,
CLINICAL STUDY Percutaneous Cryoablation of Lung Tumors: Feasibility and Safety Masanori Inoue, MD, Seishi Nakatsuka, MD, PhD, Hideki Yashiro, MD, Nobutake Ito, MD, Yotaro Izumi, MD, PhD, Yoshikane Yamauchi,
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 4 CBULP 2010 004 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 4 CBULP 2010 004 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Bone HDR brachytherapy in a patient with recurrent Ewing s sarcoma of the acetabulum: Alternative to aggressive surgery
 Bone HDR brachytherapy in a patient with recurrent Ewing s sarcoma of the acetabulum: Alternative to aggressive surgery Rafael Martínez-Monge 1,* Agata Pérez-Ochoa 1, Mikel San Julián 2, Dámaso Aquerreta
Bone HDR brachytherapy in a patient with recurrent Ewing s sarcoma of the acetabulum: Alternative to aggressive surgery Rafael Martínez-Monge 1,* Agata Pérez-Ochoa 1, Mikel San Julián 2, Dámaso Aquerreta
Thermal Damage of the Genitofemoral Nerve Due to Radiofrequency Ablation of Renal Cell Carcinoma: A Potentially Avoidable Complication
 Avoidable Nerve Damage in Radiofrequency Ablation Interventional Radiology Technical Innovation Andreas Boss 1,2 Stephan Clasen 1 Markus Kuczyk 3 Aristotelis Anastasiadis 3 Diethard Schmidt 1 Claus D.
Avoidable Nerve Damage in Radiofrequency Ablation Interventional Radiology Technical Innovation Andreas Boss 1,2 Stephan Clasen 1 Markus Kuczyk 3 Aristotelis Anastasiadis 3 Diethard Schmidt 1 Claus D.
