IN A RECENT COLLABORATIVE REanalysis
|
|
|
- Brooke Caldwell
- 6 years ago
- Views:
Transcription
1 ORIGINAL CONTRIBUTION Menopausal Estrogen and Estrogen-Progestin Replacement Therapy and Breast Cancer Risk Catherine Schairer, PhD Jay Lubin, PhD Rebecca Troisi, ScD Susan Sturgeon, DrPH Louise Brinton, PhD Robert Hoover, MD IN A RECENT COLLABORATIVE REanalysis of more than 90% of the world s epidemiological data on the relationship between menopausal hormone replacement therapy (HRT) and breast cancer risk, it was found that longer durations of recent, but not past, use of HRT increased breast cancer risk, particularly among leaner women and for tumors that were less clinically advanced. 1 Unresolved issues include the extent to which the findings were due to a biological effect of hormones rather than issues of screening and ascertainment. The data were also insufficient to determine whether a combined estrogen-progestin regimen increased risk beyond that associated with estrogen alone. In 1994, we published data on HRT and breast cancer risk from a follow-up study conducted among former participants in a breast cancer screening program. 2 were diagnosed through Those data were included in the collaborative analysis. 1 In this article, we expand our previous analysis to include cases diagnosed in the follow-up study through 1995, almost doubling the total number of cases. The collection of additional data on mammographic screening and use of the combined estrogen-progestin regimen allowed us to address some issues left unresolved. For editorial comment see p 534. Context Whether menopausal hormone replacement therapy using a combined estrogen-progestin regimen increases risk of breast cancer beyond that associated with estrogen alone is unknown. Objective To determine whether increases in risk associated with the estrogenprogestin regimen are greater than those associated with estrogen alone. Design Cohort study of follow-up data for from the Breast Cancer Detection Demonstration Project, a nationwide breast cancer screening program. Setting Twenty-nine screening centers throughout the United States. Participants A total of postmenopausal women (mean age at start of followup, 58 years). Main Outcome Measure Incident breast cancers by recency, duration, and type of hormone use. Results During follow-up, 2082 cases of breast cancer were identified. Increases in risk with estrogen only and estrogen-progestin only were restricted to use within the previous 4 years (relative risk [], 1.2 [95% confidence interval {CI}, ] and 1.4 [95% CI, ], respectively); the relative risk increased by 0.01 (95% CI, ) with each year of estrogen-only use and by 0.08 (95% CI, ) with each year of estrogen-progestin only use among recent users, after adjustment for mammographic screening, age at menopause, body mass index (BMI), education, and age. The P value associated with the test of homogeneity of these estimates was.02. Among women with a BMI of 24.4 kg/m 2 or less, increases in with each year of estrogenonly use and estrogen-progestin only use among recent users were 0.03 (95% CI, ) and 0.12 (95% CI, ), respectively. These associations were evident for the majority of invasive tumors with ductal histology and regardless of extent of invasive disease. Risk in heavier women did not increase with use of estrogen only or estrogen-progestin only. Conclusion Our data suggest that the estrogen-progestin regimen increases breast cancer risk beyond that associated with estrogen alone. JAMA. 2000;283: METHODS Follow-up Study Study subjects were participants in the Breast Cancer Detection Demonstration Project (BCDDP) conducted between 1973 and We previously described a follow-up study begun in 1979 involving a subset of BCDDP participants. 2 In brief, the follow-up study included (1) all screening participants who underwent breast surgery during the screening period, with no evidence of malignant disease (n = ); (2) all subjects who had recommendations by the project for a surgical consultation but did not have either a biopsy or aspiration performed (n = 9628); and (3) a sample of women who had neither surgery nor recommendation for Author Affiliations: National Cancer Institute, Division of Cancer Epidemiology and Genetics, Rockville, Md (Drs Schairer, Lubin, Troisi, Sturgeon, Brinton, and Hoover); Social and Scientific Systems Inc, Bethesda, Md (Dr Troisi); and the Department of Biostatistics and Epidemiology, University of Massachusetts, Amherst (Dr Sturgeon). Corresponding Author and Reprints: Catherine Schairer, PhD, National Cancer Institute, Division of Cancer Epidemiology and Genetics, 6120 Executive Blvd, EPS Room 7080-MSC 7234, Rockville, MD ( schairec@exchange.nih.gov) American Medical Association. All rights reserved. JAMA, January 26, 2000 Vol 283, No
2 surgical consultation during screening participation (n = ). The follow-up study was approved by the Institutional Review Board at the National Cancer Institute. Informed consent was obtained from participants. The follow-up study was carried out in 3 phases. Our previous analysis involved the first 2 phases of the study, in which annual telephone interviews were conducted between 1979 and 1986 and 1 mailed questionnaire was administered between 1987 and The current analysis includes data from these earlier phases as well as from the latest phase of the study, during which 1 mailed questionnaire was administered between 1993 and December 1995 to study subjects not known to be deceased and who completed a questionnaire in Nonrespondents to the mailed questionnaire were interviewed by telephone, if possible. Information collected from phase 1 of the study included recognized breast cancer risk factors; breast cancer screening practices, including number of mammograms for a routine reason or because of a problem since the last interview; and breast procedures undergone since the last examination by the screening program or the last interview. In addition, information was collected on age at first use and duration of use of female hormones (excluding creams) other than oral contraceptives. Information was not obtained on type of hormone used. During phase 2 of the study, information on breast procedures and previously collected risk factors was updated. Information was obtained on use of menopausal hormones in the form of shots, creams, patches, or pills since the last interview; those who had used pills provided information on ever use of menopausal estrogens and progestins in the same month, duration of use of estrogens and progestins, and number of days in the month progestins were used. Information on breast cancer screening practices was not collected during phase 2. In phase 3 of follow-up, previously collected information, including use of estrogens and progestins, was updated; information was also collected on mammographic and physical examinations of the breast for a routine reason or because of a problem in the 5 years prior to the interview. Level of education was recorded on a form completed at entry to the screening program. Height and weight measurements were recorded on forms at each screening visit. Current height and weight measurements were available from the questionnaire. Analytic Data Set This analysis was limited to women who were menopausal before the start of the follow-up period or who became menopausal during the course of the study. Menopausal women were defined as those who did not have a menstrual period for at least 3 months prior to an interview because of natural menopause or a bilateral oophorectomy. In addition, women who stopped menstruating because of a hysterectomy but who retained at least 1 ovary or whose ovarian status was uncertain were considered to have reached menopause by age 57 years (the 75th percentile for age at menopause in the study population) or their age at hysterectomy, whichever was later. However, they were assigned an unknown value for their specific ages at menopause in the analyses. Those reporting prophylactic bilateral mastectomies or a diagnosis of breast cancer before the start of follow-up were excluded. Those reporting use of menopausal hormones in the form of shots, patches, or creams (n = 6212) were also excluded because detailed information regarding timing of use was not available. Most study subjects (86%) were white. There were small percentages of black (5%), Hispanic (2%), and Asian American (5%) women, as well as those with other or unknown race/ethnicity (1%). After all exclusions, subjects were available for analysis. A total of (85%) of these subjects completed a phase 2 questionnaire; (84%) of those who completed a phase 2 questionnaire also completed a phase 3 questionnaire. Phase 3 questionnaires were not completed by those who completed phase 2 for reasons including death (6%); loss to follow-up (0.5%); and illness, refusal, or because contact with study subjects at a current telephone number was not made by the end of the study period (9.5%). During follow-up, 2082 breast cancer cases were identified in study subjects through self-reports or reports of breast cancer on death certificates; 1054 of these cases were included in our previous analysis. 2 Pathology reports were obtained for 1713 of these cases (82%); reports were not obtained for 237 cases (11%) because they were not received before the end of the study period, because of nonresponse of physicians or hospitals, or because permission to retrieve medical records was not received from the study subject. Pathology reports for the 132 cases (6%) identified by death certificate also were not retrieved. A total of 255 (15%) cancers for which pathology reports were available were in situ and 1456 (85%) were invasive. It was uncertain whether 2 cases were in situ or invasive. Invasive tumors were further classified into 2 groups based on histology: (1) mucinous, medullary, tubular, or papillary carcinomas (n = 76) or (2) ductal or lobular carcinomas (n = 916). A total of 788 in the second group were ductal carcinomas, 104 were lobular carcinomas, and 24 were comedocarcinomas or Paget disease with infiltrating ductal carcinoma. Histology was not available for 464 invasive cases, largely from those whose disease was diagnosed during phase 1 of the study, because pathology reports were no longer available from which to code histology. Because the accuracy of selfreporting was high among those with pathology reports (97% were confirmed as cancers), cancers without pathology reports (n = 369) were included in the analyses but were not categorized as in situ or invasive. Nodal status was available for 1253 (86%) of the invasive cases; 903 (72%) were node negative and 350 were (28%) node positive. Tumor size was available for 1041 (71%) of invasive cases: 486 JAMA, January 26, 2000 Vol 283, No American Medical Association. All rights reserved.
3 680 (65%) were smaller than 2 cm and 361 (35%) were 2 cm or larger. Analysis Follow-up began at the date of the baseline interview or date of menopause, whichever was later. Person-years accrued until the earliest of the following dates: diagnosis of breast cancer, a second prophylactic mastectomy, death (including cases identified by death certificate), or date of last contact. Data were analyzed using Poisson regression methods. We calculated relative risks (s) and 95% confidence intervals (CIs) for categorized variables using standard likelihood ratio methods. 3 For a continuous variable (eg, duration of estrogen use), the was modeled as a linear excess (E) as follows: (t, z, d) = (t, z, 0) (1 + d), where d is duration of hormone use, the parameter is the change in the E ( 1) per unit d, (t, z, 0) is the risk at time t for those with covariate vector z and no hormone use, and (t, z, d) is the risk at time t for those with covariate vector z and d years of hormone use. The background risk (t, z, 0) was modeled by means of stratification. Likelihood-based methods were used to obtain CIs for the linear E model. 4 Score tests were used to test for the statistical significance of trends and to assess quadratic departures from linearity in the linear E model. No such departures were detected. Tests of homogeneity of the effects of estrogen and estrogenprogestin were assessed by score tests in which the effects of the 2 regimens were first assumed to be the same and then were allowed to vary. Similarly, score tests were used to assess the homogeneity of hormonal effects by categories of body mass index (BMI). Variables included as time-dependent factors were attained age, BMI, use of female hormones for menopausal reasons, and mammographic examinations of the breast. Hormone use was calculated to 1 year prior to attained (or current) age to eliminate exposure that was most likely not causal. Data on BMI and mammographic examinations were calculated to attained age. Because information on progestin use was not collected until the interview, progestin use was unknown for the 6928 subjects who did not answer this interview. For these subjects and those who were uncertain whether they had used progestins, person-years and cases associated with estrogen use were included in the estrogen (progestin unknown) category if the subject had undergone a natural menopause; otherwise, they were included in the estrogen only category because women with a surgical menopause were less likely to have used progestins. Information on episodes of hormone use that occurred before breast cancer diagnosis may have been reported by study subjects after diagnosis. For instance, a subject may have reported on a 1994 interview that she had been diagnosed as having breast cancer in 1993 and that she had used hormones between 1991 and 1992 (before diagnosis). For this same study subject, all hormone use that was reported on interviews completed prior to 1993 would have been reported before breast cancer diagnosis. An individual who responded to the 1994 interview but did not report breast cancer on that interview would have reported any hormone use in a manner similar to this hypothetical case. We assessed the influence of mammographic screening (ie, mammograms as part of routine screening rather than for a problem) during the follow-up period by categorizing personyears and cases in a time-dependent manner into 1 of the following 4 groups: (1) no mammographic screening, defined as the period of time from the start of the follow-up study to the first screening mammogram during the follow-up study; (2) sporadic mammographic screening, defined as the period of 1 year following the first screening mammogram and subsequent periods more than 1 year after a screening mammogram; (3) annual mammographic screening, defined as the period of time within 1 year of the second and subsequent screening mammograms; and (4) unknown mammographic screening type. We chose to adjust for mammographic screening in this manner, rather than controlling for number of screening mammograms, because cancer detection rates associated with the first mammogram during the BCDDP screening program were markedly higher than those associated with subsequent mammograms, while cancer detection rates were remarkably constant for the second and subsequent mammograms. 5 A similar variable was created for clinical breast examinations by a health care professional during the follow-up period. For the follow-up period until the questionnaire, we calculated BMI from information obtained from the screening visit closest in time to the baseline follow-up interview; for the subsequent period we calculated BMI from current height and weight from the questionnaire. For analytic purposes, BMI data were grouped into quintiles. Because there was virtually no difference in the prevalence of hormone use in the lowest 2 quintiles, they were combined in the analyses. To control as completely as possible for the confounding effects of age at menopause, we created narrow categories for the most commonly reported ages at menopause and broader categories for the less commonly reported ages. We performed selected analyses excluding subjects with unknown age at menopause to address theoretical concerns that including these women would seriously underestimate the risk associated with HRT. 6 RESULTS The mean duration of follow-up was 10.2 years, with a median of 12.3 years, a maximum of 16.0 years, and a minimum of less than 1 year. During follow-up, person-years were accumulated for the subjects. The average age at start of follow-up was 58 years. Forty-two percent of person-years were associated with no use of hormones, 38% with estrogen-only use, 4% with combined estrogen-progestin only use, 6% with estrogen-progestin use among those who also used estrogen alone, 5% with estrogen use with uncertain or unascertained progestin 2000 American Medical Association. All rights reserved. JAMA, January 26, 2000 Vol 283, No
4 use, 1% with progestin-only use or progestin use with uncertain estrogen use, and 5% with uncertain hormone use. The primary type of estrogen used was conjugated estrogens (Premarin) and the primary progestin was medroxyprogesterone acetate. Ever Use and Recency of Use Relative risks associated with ever use of different hormone regimens after adjustment for attained age, age at menopause, education, BMI, and mammographic screening are shown in TABLE 1. Adjustment for race, period of followup, age at first live birth, family history of breast cancer, history of benign breast disease, and clinical breast examinations did not alter these estimates. There were slight increases in risk associated with all regimens of use except progestin only. Most subsequent analyses are restricted to nonhormone use, use of estrogen only, and use of estrogen-progestin only. Increases in risk associated with use of estrogen only and estrogen-progestin only were largely restricted to recent use of hormones (defined as current use and past use occurring within the previous 4 years) (TABLE 1). Relative risks were 1.2 (95% CI, ) and 1.4 (95% CI, ), respectively. The mean person-year weighted duration of combined estrogen-progestin use among recent users was less than half that among recent users of estrogens alone (3.6 vs 10.3 years). Table 1. Relative Risk of Breast Cancer Associated With Use of Estrogen and Estrogen-Progestin Replacement Therapy Person-Years * Ever use No use (Referent) Estrogen only ( ) Estrogen-progestin only ( ) Estrogen alone and estrogen-progestin ( ) Progestin only ( ) Estrogen (progestin unknown) ( ) Progestin (estrogen unknown) Unknown use ( ) Years since last use Estrogen only Current ( ) ( ) ( ) ( ) ( ) Estrogen-progestin only Current ( ) ( ) ( ) ( ) ( ) * indicates relative risk; CI, confidence interval. Data are adjusted for attained age, education, body mass index, age at menopause, and mammographic screening. Ellipses indicate data not applicable. Duration of Use Observed and predicted s associated with duration of estrogen-only use and estrogen-progestin only use among recent users are shown in the FIGURE. Based on the linear excess risk model, the of breast cancer increased by 0.01 (95% CI, ) for each year of estrogen-only use (P =.01 for trend) and by 0.08 (95% CI, ) for each year of estrogen-progestin only use (P =.01 for trend). The P value for the test of homogeneity of these estimates was.02. Results were similar when analyses were restricted to the category of annual mammographic screening, which included 24% of the personyears in the study. To assess the impact of excluding women with an unknown age at menopause on the analysis, we restricted data to recent users with a known ageat menopause. Relative risks were changed only slightly; in contrast with estimates of 0.01 and 0.08 for all data, the increase in for each year of estrogen-only use was 0.02 (95% CI, ) and for each year of estrogen-progestin only use was 0.06 (95% CI, to 0.15). The P value for the test of homogeneity of these associations was.23. We also examined associations among women with a known age at menopause but unadjusted for age at menopause; the increase in for each year of estrogen-only use was 0.01 (95% CI, ) and for estrogen-progestin only use was 0.07 (95% CI, ), suggesting that ignoring age at menopause entirely had little effect on the estimates. When analyses included all recent users of estrogen-progestin (ie, including those who also used estrogen alone and those with an unknown age at menopause), the increased by 0.05 (95% CI, ) with each year of use. The P value associated with the test of homogeneity of this estimate and that associated with duration of use of estrogen alone was.07. There was no association between duration of use of estrogen alone and risk of breast cancer among past users. Duration by Days in the Month Progestins Were Used Among recent users who used progestins for fewer than 15 days per month, the s associated with less than 4 and 4 or more years of use of estrogen-progestin only were 1.1 (95% CI, ) and 1.5 (95% CI, ), respectively, based on 26 and 22 cases. The median number of days progestins were used in this group was 10. There were too few cases who had used progestins for 15 or more days per month (n = 12) to derive stable estimates according to duration of use. A substantial number of cases (n = 33) 488 JAMA, January 26, 2000 Vol 283, No American Medical Association. All rights reserved.
5 were uncertain how many days in the month they had used progestin. Variation by BMI Associations with duration of estrogenonly use among recent users varied significantly according to BMI (P =.002 for score test), with increases in risk evident only in women with a BMI of 24.4 kg/m 2 orless(table2).thesincreased by 0.03 (95% CI, ) for each year of estrogen-only use in this group. Associations with duration of estrogenprogestin only use among recent users did not vary significantly according to BMI (P =.42 for score test), although there was a significant increase in risk among lean women but not heavier women. The among lean women increased by 0.12 (95% CI, ) for each year of use. The P value associated with the test of homogeneity of this estimate and that associated with estrogenonly use in lean women was.06. When those with an unknown age at menopause were excluded, the increased by 0.05 for each year of estrogenonly use(95% CI, ) among lean women; the increase in the for each yearofestrogen-progestin onlyuseinlean womenwas0.11(95% CI, ). The P value associated with the test of homogeneity of these estimates was.36. Extent of Disease and Tumor Histology In recent estrogen-only users with BMI of 24.4 kg/m 2 or less, duration of use was associated with significant in- Table 2. Relative Risks Associated With Duration of Estrogen-Only Use and Estrogen-Progestin Only Use Among Recent Users by Body Mass Index (BMI) Duration of Use, y Body Mass Index (BMI) 24.4 kg/m kg/m 2 * * Estrogen Only No use (Referent) (Referent) ( ) ( ) ( ) ( ) ( ) ( ) 0.03 ( ) 0.01 ( 0.02 to 0.10) of use P value for trend Estrogen-Progestin Only No use (Referent) (Referent) ( ) ( ) ( ) ( ) ( ) ( ) 0.12 ( ) 0.04 ( 0.03 to 0.17) of use P value for trend * indicates relative risk; CI, confidence interval. Relative risks are adjusted for attained age, age at menopause, education, mammographic screening, and BMI. Figure. Observed Relative Risks and Fitted Linear Excess Relative Risk Model Associated With Duration of Estrogen-Only and Estrogen-Progestin Only Use Among Recent Users 2.5 Estrogen-Only Users vs Nonusers 2.5 Estrogen-Progestin Only Users vs Nonusers = y Relative Risk 1.5 = y Duration of Use Category, y <4 4-<8 8-<12 12-<16 16-< Duration of Use Category, y <2 2-<4 4-< Duration of Use, y 0 5 Duration of Use, y 10 Solid squares indicate observed relative risks (s); error bars, 95% confidence intervals (CIs). The solid line indicates the fitted linear excess ; the dashed lines indicate 95% CIs. Observed s are plotted at the person-year weighted mean value for duration of use for categories of estrogen-only use and estrogen-progestin only use. The number of cases in each category is also shown. For estrogen-progestin only use, the upper limits of the 95% CIs for 10-year duration (2.86) and for the linear excess (2.64) are not shown American Medical Association. All rights reserved. JAMA, January 26, 2000 Vol 283, No
6 Table 3. Relative Risks Associated With Estrogen-Only and Estrogen-Progestin Only Use Among Recent Users With BMI 24.4 kg/m 2 According to Extent of Invasive Disease* All Invasive Invasive, Node Negative Invasive, Node Positive Invasive, 2 cm Invasive, 2 cm Duration of Use, y Estrogen Only No use (Referent) (Referent) (Referent) (Referent) (Referent) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) 0.04 ( ) 0.03 ( ) 0.10 ( ) 0.05 ( ) 0.07 ( ) of use Estrogen-Progestin Only No use (Referent) (Referent) (Referent) (Referent) (Referent) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) 0... of use 0.13 ( ) 0.02 (Undefined-0.19) 0.21 ( ) 0.30 ( )... * indicates relative risk; CI, confidence interval; BMI, body mass index; and ellipses, data not applicable. Relative risks are adjusted for attained age, education, BMI, age at menopause, and mammographic screening. When CIs for increase in exclude 1.0, P values for trend are.05. Table 4. Relative Risks Associated With Duration of Estrogen-Only and Estrogen-Progestin Only Use Among Recent Users With BMI 24.4 kg/m 2 According to Histology of Invasive Disease* Ductal/Lobular Tumor Histology Ductal Only Duration of Use, y Estrogen Only No use (Referent) (Referent) ( ) ( ) ( ) ( ) ( ) ( ) 0.03 ( ) 0.03 ( ) of use P value for trend Estrogen-Progestin Only No use (Referent) (Referent) ( ) ( ) ( ) ( ) 0.17 ( ) 0.17 ( ) of use P value for trend * indicates relative risk; BMI, body mass index; CI, confidence interval. Relative risks are adjusted for attained age, age at menopause, education, mammographic screening, and BMI. creases in risk of both early- and laterstage invasive disease (TABLE 3). Estrogen-progestin only use was also associated with significant increases in risk of invasive cancer, but numbers were too small to draw conclusions regarding associations according to extent of invasive disease. There were no significant increases in risk of in situ disease associated with either regimen, but the number of cases was small. In recent users with BMI of 24.4 kg/m 2 or less, use of estrogen only and estrogen-progestin only were both associated with significant increases in risk of invasive tumors with ductal and/or lobular histologies (TABLE 4). Similar associations were evident when analyses were limited to invasive tumors with ductal histology. There were too few cases with other histologies to examine these associations. COMMENT Our results suggest that the combined estrogen-progestin regimen is associated withgreaterincreasesinbreastcancerrisk thanestrogenalone. Theseresultsareconsistentwiththosefromtherecentcollaborative analysis, although in that analysis, the effect of the combined estrogenprogestin regimen was evaluated among women who may also have used estrogen alone. 1 Recently published data also supportamoreadverseeffectonthebreast withtheestrogen-progestinregimenthan with estrogen alone. 7 Assessing the comparative risk of estrogen alone vs estrogen-progestin was complicated by the fact that use of estrogen alone was associated with increased risk in lean but not heavy women. We found differences between the 2 regimens among lean women but were unable to draw conclusions among heavier women. In the collaborative reanalysis, associations without regard to type of hormone were evident in lean but not heavy women. 1 Among lean women, we found no evidence that associations differed according to extent of disease. In the collaborative reanalysis, increases in risk 490 JAMA, January 26, 2000 Vol 283, No American Medical Association. All rights reserved.
7 were greater for localized than distant disease, but results according to extent of disease were not reported in lean women. 1 We also found significant increases in risk for the vast majority of invasive tumors classified as lobular and/or ductal carcinomas, results that are not consistent with those of Gapstur et al. 8 Their categories for duration of use ( 5or 5 years) may have obscured an effect of long-term use; in addition, they did not present results among lean women. In a survival analysis based on a different series of cases, we found that the reduction in breast cancer mortality among current hormone users at diagnosis was not due to earlier-stage disease or tumors with more favorable histologies in hormone users compared with nonusers, 9 consistent with the current analysis. The biological mechanisms underlying an effect of exogenous hormones on the breast are complex. In a study of proliferation of normal human breast tissue implanted into athymic nude mice, there appeared to be a maximally effective dosage of estradiol in regard to breast cell proliferation beyond which higher dosages had no effect. 10 This phenomenon may explain the lack of effect of exogenous estrogen on breast cancer risk in heavy women, who have relatively higher endogenous estrogen levels than lean women due to nonovarian synthesis of estrone as a result of the peripheral conversion of androgens. The fact that progesterone does not down-regulate estrogen and progesterone receptors in the breast may contribute to its adverse effects. 10,11 Moreover, the isozyme of 17 -hydroxysteroid dehydrogenase induced by progesterone in the breast predominantly catalyzes the conversion of the less potent estrone to the more potent estradiol. 12 Several methodological issues need to be considered in interpreting our results. The pattern of greater increases in risk associated with the estrogenprogestin regimen than with estrogen alone was evident when subjects with an unknown age at menopause were both included and excluded, although the disparity between the associations was slightly smaller when they were excluded. The lack of statistical significance for the test of the homogeneity of the associations of the 2 regimens after exclusion of those with an unknown age at menopause most likely resulted from the elimination of 17% of person-years and 20% of cases in the study, which reduced the information available for estimating increases in the s. We chose to present our main findings including women with an unknown age at menopause because age at menopause was not a substantial confounder of the hormone associations in these data and because excluding these women resulted in a substantial loss of information. Moreover, the estimates including and excluding these women were not meaningfully different, given the uncertainty in the estimates. Although we were not able to completely account for differences in mammographic screening according to hormone use, it is reassuring that results were similar when we restricted analyses to those who had undergone annual mammographic screening. Moreover, similar differences have been noted in other populations where mammographic screening is widespread 7 or where differences in mammographic screening have been taken into account in assessing risk of HRT. 13 Although our study may be subject to problems of recall in the reporting of menopausal hormone use, 14 such misclassification would most likely dilute the magnitude of the relationship between HRT and breast cancer risk. The fact that some episodes of hormone use that occurred before breast cancer diagnosis were reported after diagnosis raises the possibility of differential recall by cases and noncases. However, our results with regard to recency of use are very similar to those from a cohort study in which all hormone use was reported before diagnosis. 13 Moreover, in another cohort study in which all hormone use was reported before diagnosis, the estrogenprogestin regimen also was associated with greater increases in risk than estrogens alone. 7 Finally, in an early casecontrol study based on this study population in which hormone use was validated, there was no evidence of differential reporting of hormone use by cases and controls. 15 Our results, as well as those of others, suggest that in weighing the risks and benefits of menopausal HRT, it is important to consider the type of hormone regimen as well as individual characteristics of the woman, such as body mass index. Acknowledgment: We are indebted to Leslie Carroll and Heather Clancey of IMS Inc, Rockville, Md, for computer support. REFERENCES 1. Collaborative Group on Hormonal Factors in Breast Cancer. Breast cancer and hormone replacement therapy. Lancet. 1997;350: Schairer C, Byrne C, Keyl PM, et al. Menopausal estrogen and estrogen-progestin replacement therapy and risk of breast cancer (United States). Cancer Causes Control. 1994;5: Breslow NE, Day NE. Statistical Methods in Cancer Research: The Design and Analysis of Cohort Studies. Lyon, France: International Agency for Research on Cancer; Preston DL, Lubin JH, Pierce DA, McConney ME. EPICURE [software]. Release 2.0. Seattle, Wash: HiroSoft International Corp; Baker LH. Breast Cancer Detection Demonstration Project. CA Cancer J Clin. 1982;32: Pike MC, Ross RK, Spicer DV. Problems involved in including women with simple hysterectomy in epidemiologic studies measuring the effects of hormone replacement therapy on breast cancer risk. Am J Epidemiol. 1998;147: Persson I, Weiderpass E, Bergstrom R, Schairer C. Risks of breast and endometrial cancer after estrogen and estrogen-progestin replacement therapy. Cancer Causes Control. 1999;10: Gapstur SM, Morrow M, Sellers TA. Hormone replacement therapy and breast cancer with a favorable pathology. JAMA. 1999;281: Schairer C, Gail M, Byrne C, et al. Estrogen replacement therapy and breast cancer survival in a large screening study. J Natl Cancer Inst. 1999;91: Laidlaw IJ, Clarke RB, Howell A, et al. The proliferation of normal human breast tissue implanted into athymic nude mice is stimulated by estrogen but not progesterone. Endocrinology. 1995;136: Hargreaves DF, Knox F, Swindell R, Potten CS, Bundred NJ. Epithelial proliferation and hormone receptor status in the normal post-menopausal breast and the effects of hormone replacement therapy. Br J Cancer. 1998;78: Poutanen M, Isomaa V, Peltoketo H, Vihko R. Role of 17 -hydroxysteroid dehydrogenase type 1 in endocrine and intracrine estradiol biosynthesis. J Steroid Biochem Mol Biol. 1995;55: Colditz GA, Hankinson SE, Hunter DJ, et al. The use of estrogens and progestins and the risk of breast cancer in postmenopausal women. N Engl J Med. 1995; 332: Greendale GA, James MK, Espeland MA, Barrett- Connor E, for the PEPI Investigators. Can we measure prior postmenopausal estrogen/progestin use? Am J Epidemiol. 1997;146: Brinton LA, Hoover RN, Szklo M, et al. Menopausal estrogen use and risk of breast cancer. Cancer. 1981;47: American Medical Association. All rights reserved. JAMA, January 26, 2000 Vol 283, No
8 LETTERS the cap, whether in quarterly or annually capped plans, we identified the first month of the year in which the capped limit was exceeded. Unlike Rector, we were not able to identify and exclude members who disenrolled nonvoluntarily. Like Rector, we used an extended Cox model with the internally defined time-dependent variable of reaching the cap to analyze the relationship between reaching the cap and disenrollment from the health plan. 2 Models were estimated for each plan and each year controlling for participant age, sex, and chronic disease score. 3 Results. The percentages of members reaching their annual prescription cap for plans A, B, and C, respectively, were 22.6%, 0.7%, and 1.6% in 1997 and 12%, 4.1%, and 3.9% in Disenrollment rates among those enrolled in the first 3 months of each year for plans A, B, and C, respectively, were 19.3%, 28.9%, and 6.8% in 1997 and 10.4%, 22.9%, and 14.0% in Among those disenrolling in 1997, 21%, 7%, and 7%, respectively, reenrolled in The risk of disenrollment across all plans and both years was significantly associated with older age, greater disease burden (ie, higher chronic disease score), and reaching the cap. In 1997, the relative risks (s) of disenrollment in any given month for those reaching the cap for the 3 plans were 2.62 (95% confidence interval [CI], ), 2.21 (95% CI, ), and 2.24 (95% CI, ); in 1998, the s of disenrollment were 3.04 (95% CI, ), 1.79 (95% CI, ), and 2.30 (95% CI, ) in plans A, B, and C, respectively. Comment. Exhaustion of prescription coverage, whether administered on a quarterly or annual basis, was associated with a 2- to 3-fold increase in the of disenrollment. These findings expand on those of Rector and suggest that this relationship holds under various scenarios including variation in underlying use, cap amounts, and cap administration. Emily R. Cox, PhD Brenda R. Motheral, PhD Kathi Fairman, MA Express Scripts Inc Maryland Heights, Mo Funding/Support: This research was funded by The Robert Wood Johnson Foundation s Changes in Health Care Financing and Organization (HCFO) Initiative. 1. Rector TS. Exhaustion of drug benefits and disenrollment of Medicare beneficiaries from managed care organizations. JAMA. 2000;283: Crowley J, Hu M. Covariance analysis of heart transplant data. J Am Stat Assoc. 1977;72: Clark DO, Korff MV, Saunders K, Baluch WM, Simon GE. A chronic disease score with empirically derived weights. Med Care. 1995;33: COECTIONS Incorrect Unit of Measure and Numbers: In the Original Contribution entitled Cognitive-Behavioral Therapy, Imipramine, or Their Combination for Panic Disorder published in the May 17, 2000, issue of THE JOURNAL (2000;283: ), the units of measure for imipramine and desipramine should be ng/ml instead of ng/dl on page 2532 and ng/ml instead of mg/ml on page On page 2530 under Study Design patients randomized to CBT+placebo should number 5 per block of 24, not 25. In the Treatment Conditions section on page 2531, near the end of the third paragraph,... the dosage [of imipramine] could be increased up to 300 mg/d by week 5 should read week 7. Author Omitted: In the Caring for the Critically Ill Patient article entitled Ketoconazole for Early Treatment of Acute Lung Injury and Acute Respiratory Distress Syndrome published in the April 19, 2000, issue of THE JOURNAL (2000;283: ), an author was inadvertently omitted from the ARDS Network listing on page Brian Christman, MD, should have been listed with the Vanderbilt University group and identified as an author. Acknowledgment Omission: In the Original Contribution entitled Menopausal Estrogen and Estrogen-Progestin Replacement Therapy and Breast Cancer Risk published in the January 26, 2000, issue of THE JOURNAL (2000;283: ), acknowledgments were omitted. The authors wish to thank the Breast Cancer Detection Demonstration Project study participants as well as Susan Englehart, Cathy Ann Grundmayer, and the staff at Westat Inc, Rockville, Md, for conduct of the Breast Cancer Detection Demonstration Project Follow-up Study. Incorrect Data in Table: In the Original Contribution entitled Estrogen Replacement Therapy for Treatment of Mild to Moderate Alzheimer Disease: A Randomized Controlled Trial published in the February 23, 2000, issue of THE JOURNAL (2000;283: ), incorrect data appeared in Table 3 on page In the placebo group column, the mean (SD) changes in scores at 12 months for the Emotional Face Recognition Test and the Grooved Pegboard Test should have been 5.7 (22.4) and 5.2 (42.4), respectively. Photo Misidentification: In the Medical News & Perspectives article entitled Psychiatrists Help Survivors in the Balkans published in the March 8, 2000, issue of THE JOURNAL (2000;283: ), the photo on page 1278 identified as Ismet Ceric, MD, should have been identified as Vlado Jukić, MD. Acknowledgment Omission: In the Original Contribution entitled Vaginal Misoprostol Administered 1, 2, or 3 Days After Mifepristone for Early Medical Abortion: A Randomized Trial published in the October 18, 2000, issue of THE JOURNAL (2000;284: ), an acknowledgment was omitted. The authors wish to acknowledge the contributions of Larry Lader, president of the Abortion Rights Mobilization, for making the study possible American Medical Association. All rights reserved. (Reprinted) JAMA, November 22/29, 2000 Vol 284, No
Postmenopausal hormone therapy and cancer risk
 International Congress Series 1279 (2005) 133 140 www.ics-elsevier.com Postmenopausal hormone therapy and cancer risk P. Kenemans*, R.A. Verstraeten, R.H.M. Verheijen Department of Obstetrics and Gynaecology,
International Congress Series 1279 (2005) 133 140 www.ics-elsevier.com Postmenopausal hormone therapy and cancer risk P. Kenemans*, R.A. Verstraeten, R.H.M. Verheijen Department of Obstetrics and Gynaecology,
Hormone Replacement Therapy and Risk of Breast Cancer With a Favorable Histology
 ORIGINAL CONTRIBUTION Hormone Replacement Therapy and Risk of Breast Cancer With a Favorable Histology Results of the Iowa Women s Health Study Susan M. Gapstur, PhD Monica Morrow, MD Thomas A. Sellers,
ORIGINAL CONTRIBUTION Hormone Replacement Therapy and Risk of Breast Cancer With a Favorable Histology Results of the Iowa Women s Health Study Susan M. Gapstur, PhD Monica Morrow, MD Thomas A. Sellers,
In 1981, we published results from a case-control. study involving 881 cases and 863 controls. not associated with any substantial overall risk,
 Br. J. Cancer (1986) 54, 825-832 Menopausal oestrogens and breast cancer risk: An expanded case-control study L.A. Brinton, R. Hoover & J.F. Fraumeni, Jr Environmental Epidemiology Branch, National Cancer
Br. J. Cancer (1986) 54, 825-832 Menopausal oestrogens and breast cancer risk: An expanded case-control study L.A. Brinton, R. Hoover & J.F. Fraumeni, Jr Environmental Epidemiology Branch, National Cancer
THE POSSIBLE ASSOCIATION BEtween
 ORIGINAL CONTRIBUTION Hormone Replacement Therapy in Relation to Breast Cancer Chi-Ling Chen, PhD Noel S. Weiss, MD, DrPH Polly Newcomb, PhD William Barlow, PhD Emily White, PhD THE POSSIBLE ASSOCIATION
ORIGINAL CONTRIBUTION Hormone Replacement Therapy in Relation to Breast Cancer Chi-Ling Chen, PhD Noel S. Weiss, MD, DrPH Polly Newcomb, PhD William Barlow, PhD Emily White, PhD THE POSSIBLE ASSOCIATION
Copyright, 1995, by the Massachusetts Medical Society
 Copyright, 1995, by the Massachusetts Medical Society Volume 332 JUNE 15, 1995 Number 24 THE USE OF ESTROGENS AND PROGESTINS AND THE RISK OF BREAST CANCER IN POSTMENOPAUSAL WOMEN GRAHAM A. COLDITZ, M.B.,
Copyright, 1995, by the Massachusetts Medical Society Volume 332 JUNE 15, 1995 Number 24 THE USE OF ESTROGENS AND PROGESTINS AND THE RISK OF BREAST CANCER IN POSTMENOPAUSAL WOMEN GRAHAM A. COLDITZ, M.B.,
Estrogen, Estrogen Plus Progestin Therapy, and Risk of Breast Cancer
 Vol. 11, 909s 917s, January 15, 2005 (Suppl.) Clinical Cancer Research 909s Estrogen, Estrogen Plus Progestin Therapy, and Risk of Breast Cancer Graham A. Colditz Channing Laboratory, Department of Medicine,
Vol. 11, 909s 917s, January 15, 2005 (Suppl.) Clinical Cancer Research 909s Estrogen, Estrogen Plus Progestin Therapy, and Risk of Breast Cancer Graham A. Colditz Channing Laboratory, Department of Medicine,
THERE IS CONSIDERABLE EVIdence
 ORIGINAL CONTRIBUTION Relationship Between Long Durations and Different Regimens of Hormone Therapy and Risk of Breast Cancer Christopher I. Li, MD, PhD Kathleen E. Malone, PhD Peggy L. Porter, MD Noel
ORIGINAL CONTRIBUTION Relationship Between Long Durations and Different Regimens of Hormone Therapy and Risk of Breast Cancer Christopher I. Li, MD, PhD Kathleen E. Malone, PhD Peggy L. Porter, MD Noel
Current Use of Unopposed Estrogen and Estrogen Plus Progestin and the Risk of Acute Myocardial Infarction Among Women With Diabetes
 Current Use of Unopposed Estrogen and Estrogen Plus Progestin and the Risk of Acute Myocardial Infarction Among Women With Diabetes The Northern California Kaiser Permanente Diabetes Registry, 1995 1998
Current Use of Unopposed Estrogen and Estrogen Plus Progestin and the Risk of Acute Myocardial Infarction Among Women With Diabetes The Northern California Kaiser Permanente Diabetes Registry, 1995 1998
5. Summary of Data Reported and Evaluation
 326 5. Summary of Data Reported and Evaluation 5.1 Exposure data Combined estrogen progestogen menopausal therapy involves the co-administration of an estrogen and a progestogen to peri- or postmenopausal
326 5. Summary of Data Reported and Evaluation 5.1 Exposure data Combined estrogen progestogen menopausal therapy involves the co-administration of an estrogen and a progestogen to peri- or postmenopausal
A literature review examining the association between the duration of hormone replacement therapy (HRT) and the risk of breast cancer in women
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A literature review examining the association between the duration of hormone replacement therapy (HRT)
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A literature review examining the association between the duration of hormone replacement therapy (HRT)
Hormones and Healthy Bones Joint Project of National Osteoporosis Foundation and Association of Reproductive Health Professionals
 Hormones and Healthy Bones Joint Project of National Osteoporosis Foundation and Association of Reproductive Health Professionals Literature Review (January 2009) Hormone Therapy for Women Women's Health
Hormones and Healthy Bones Joint Project of National Osteoporosis Foundation and Association of Reproductive Health Professionals Literature Review (January 2009) Hormone Therapy for Women Women's Health
Hormones. Synthetic. Bioidentical. vs. SPECIAL REPORT. for Menopause. by Dr. Mark Stengler
 SPECIAL REPORT Synthetic vs. Bioidentical Hormones for Menopause by Dr. Mark Stengler www.markstengler.com All rights reserved. This program, or parts thereof, may not be reproduced in any form without
SPECIAL REPORT Synthetic vs. Bioidentical Hormones for Menopause by Dr. Mark Stengler www.markstengler.com All rights reserved. This program, or parts thereof, may not be reproduced in any form without
2. Studies of Cancer in Humans
 346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
Recreational physical activity and risk of triple negative breast cancer in the California Teachers Study
 Ma et al. Breast Cancer Research (2016) 18:62 DOI 10.1186/s13058-016-0723-3 RESEARCH ARTICLE Open Access Recreational physical activity and risk of triple negative breast cancer in the California Teachers
Ma et al. Breast Cancer Research (2016) 18:62 DOI 10.1186/s13058-016-0723-3 RESEARCH ARTICLE Open Access Recreational physical activity and risk of triple negative breast cancer in the California Teachers
Research. Breast cancer represents a major
 Research GENERAL GYNECOLOGY Gynecologic conditions in participants in the NSABP breast cancer prevention study of tamoxifen and raloxifene (STAR) Carolyn D. Runowicz, MD; Joseph P. Costantino, DrPH; D.
Research GENERAL GYNECOLOGY Gynecologic conditions in participants in the NSABP breast cancer prevention study of tamoxifen and raloxifene (STAR) Carolyn D. Runowicz, MD; Joseph P. Costantino, DrPH; D.
Relation of Regimens of Combined Hormone Replacement Therapy to Lobular, Ductal, and Other Histologic Types of Breast Carcinoma
 2455 Relation of Regimens of Combined Hormone Replacement Therapy to Lobular, Ductal, and Other Histologic Types of Breast Carcinoma Janet R. Daling, Ph.D. 1,2 Kathleen E. Malone, Ph.D. 1,2 David R. Doody,
2455 Relation of Regimens of Combined Hormone Replacement Therapy to Lobular, Ductal, and Other Histologic Types of Breast Carcinoma Janet R. Daling, Ph.D. 1,2 Kathleen E. Malone, Ph.D. 1,2 David R. Doody,
Menopausal hormone therapy currently has no evidence-based role for
 IN PERSPECTIVE HT and CVD Prevention: From Myth to Reality Nanette K. Wenger, M.D. What the studies show, in a nutshell The impact on coronary prevention Alternative solutions Professor of Medicine (Cardiology),
IN PERSPECTIVE HT and CVD Prevention: From Myth to Reality Nanette K. Wenger, M.D. What the studies show, in a nutshell The impact on coronary prevention Alternative solutions Professor of Medicine (Cardiology),
Characteristics of respondents and non-respondents from a case-control study of breast cancer in younger women
 International Epidemiological Association 2000 Printed in Great Britain International Journal of Epidemiology 2000;29:793 798 Characteristics of respondents and non-respondents from a case-control study
International Epidemiological Association 2000 Printed in Great Britain International Journal of Epidemiology 2000;29:793 798 Characteristics of respondents and non-respondents from a case-control study
ARTICLES. Postmenopausal Hormone Therapy and Change in Mammographic Density
 ARTICLES Postmenopausal Hormone Therapy and Change in Mammographic Density Gail A. Greendale, Beth A. Reboussin, Stacey Slone, Carol Wasilauskas, Malcolm C. Pike, Giske Ursin Background: Mammographic density
ARTICLES Postmenopausal Hormone Therapy and Change in Mammographic Density Gail A. Greendale, Beth A. Reboussin, Stacey Slone, Carol Wasilauskas, Malcolm C. Pike, Giske Ursin Background: Mammographic density
Breast Cancer Risk Assessment and Prevention
 Breast Cancer Risk Assessment and Prevention Katherine B. Lee, MD, FACP October 4, 2017 STATISTICS More than 252,000 cases of breast cancer will be diagnosed this year alone. About 40,000 women will die
Breast Cancer Risk Assessment and Prevention Katherine B. Lee, MD, FACP October 4, 2017 STATISTICS More than 252,000 cases of breast cancer will be diagnosed this year alone. About 40,000 women will die
Discussing breast cancer and hormone replacement therapy with women
 INTERPRETING KEY TRIALS PELIN BATUR, MD Section of Women s Health, Department of General Internal Medicine, Gault Women s Health and Breast Pavilion, The Cleveland Clinic HOLLY L. THACKER, MD, FACP Departments
INTERPRETING KEY TRIALS PELIN BATUR, MD Section of Women s Health, Department of General Internal Medicine, Gault Women s Health and Breast Pavilion, The Cleveland Clinic HOLLY L. THACKER, MD, FACP Departments
Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors.
 Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors. Who needs surveillance? Chiarelli et al. Early menopause and Infertility
Evidence tables from the systematic literature search for premature ovarian insufficiency surveillance in female CAYA cancer survivors. Who needs surveillance? Chiarelli et al. Early menopause and Infertility
Breast Cancer Risk in Patients Using Hormonal Contraception
 Breast Cancer Risk in Patients Using Hormonal Contraception Bradley L. Smith, Pharm.D. Smith.bradley1@mayo.edu Pharmacy Ground Rounds Mayo Clinic Rochester April 3 rd, 2018 2017 MFMER slide-1 Presentation
Breast Cancer Risk in Patients Using Hormonal Contraception Bradley L. Smith, Pharm.D. Smith.bradley1@mayo.edu Pharmacy Ground Rounds Mayo Clinic Rochester April 3 rd, 2018 2017 MFMER slide-1 Presentation
Increased breast carcinoma risk is a major concern for women. Hormone Replacement Therapy in Relation to Breast Carcinoma Incidence Rate Ratios
 2328 Hormone Replacement Therapy in Relation to Breast Carcinoma Incidence Rate Ratios A Prospective Danish Cohort Study Anne Tjønneland, Ph.D. 1 Jane Christensen, M.Sc. 1 Birthe L. Thomsen, M.Sc. 1 Anja
2328 Hormone Replacement Therapy in Relation to Breast Carcinoma Incidence Rate Ratios A Prospective Danish Cohort Study Anne Tjønneland, Ph.D. 1 Jane Christensen, M.Sc. 1 Birthe L. Thomsen, M.Sc. 1 Anja
Downloaded from:
 Ellingjord-Dale, M; Vos, L; Tretli, S; Hofvind, S; Dos-Santos-Silva, I; Ursin, G (2017) Parity, hormones and breast cancer subtypes - results from a large nested case-control study in a national screening
Ellingjord-Dale, M; Vos, L; Tretli, S; Hofvind, S; Dos-Santos-Silva, I; Ursin, G (2017) Parity, hormones and breast cancer subtypes - results from a large nested case-control study in a national screening
Federal Judge Sets Trial Dates for Two Hormone Replacement Therapy Cases in Arkansas Thousands More Pending
 Federal Judge Sets Trial Dates for Two Hormone Replacement Therapy Cases in Arkansas Thousands More Pending Date Published: Sunday, February 12th, 2006 United States District Judge William Wilson in Little
Federal Judge Sets Trial Dates for Two Hormone Replacement Therapy Cases in Arkansas Thousands More Pending Date Published: Sunday, February 12th, 2006 United States District Judge William Wilson in Little
Abnormal Uterine Bleeding Case Studies
 Case Study 1 Abnormal Uterine Bleeding Case Studies Abigail, a 24 year old female, presents to your office complaining that her menstrual cycles have become a problem. They are now lasting 6 7 days instead
Case Study 1 Abnormal Uterine Bleeding Case Studies Abigail, a 24 year old female, presents to your office complaining that her menstrual cycles have become a problem. They are now lasting 6 7 days instead
COMMENTARY: DATA ANALYSIS METHODS AND THE RELIABILITY OF ANALYTIC EPIDEMIOLOGIC RESEARCH. Ross L. Prentice. Fred Hutchinson Cancer Research Center
 COMMENTARY: DATA ANALYSIS METHODS AND THE RELIABILITY OF ANALYTIC EPIDEMIOLOGIC RESEARCH Ross L. Prentice Fred Hutchinson Cancer Research Center 1100 Fairview Avenue North, M3-A410, POB 19024, Seattle,
COMMENTARY: DATA ANALYSIS METHODS AND THE RELIABILITY OF ANALYTIC EPIDEMIOLOGIC RESEARCH Ross L. Prentice Fred Hutchinson Cancer Research Center 1100 Fairview Avenue North, M3-A410, POB 19024, Seattle,
Effective Health Care Program
 Comparative Effectiveness Review Number 17 Effective Health Care Program Comparative Effectiveness of Medications To Reduce Risk of Primary Breast Cancer in Women Executive Summary Background Breast cancer
Comparative Effectiveness Review Number 17 Effective Health Care Program Comparative Effectiveness of Medications To Reduce Risk of Primary Breast Cancer in Women Executive Summary Background Breast cancer
Research Article An Estrogen Model: The Relationship between Body Mass Index, Menopausal Status, Estrogen Replacement Therapy, and Breast Cancer Risk
 Hindawi Publishing Corporation Computational and Mathematical Methods in Medicine Volume 202, Article ID 792375, 8 pages doi:0.55/202/792375 Research Article An Estrogen Model: The Relationship between
Hindawi Publishing Corporation Computational and Mathematical Methods in Medicine Volume 202, Article ID 792375, 8 pages doi:0.55/202/792375 Research Article An Estrogen Model: The Relationship between
Breast Cancer Prevention Studies. Key Points. Breast cancer prevention studies are clinical trials (research studies conducted with
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Breast Cancer Prevention
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Breast Cancer Prevention
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 336 J UNE 19, 1997 NUMBER 25 POSTMENOPAUSAL HORMONE THERAPY AND MORTALITY FRANCINE GRODSTEIN, SC.D., MEIR
The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 336 J UNE 19, 1997 NUMBER 25 POSTMENOPAUSAL HORMONE THERAPY AND MORTALITY FRANCINE GRODSTEIN, SC.D., MEIR
Preventing Breast Cancer in HT users by Manuel Neves-e-Castro Portuguese Menopause Society September 2004
 Preventing Breast Cancer in HT users by Manuel Neves-e-Castro Portuguese Menopause Society September 2004 I am also PRO!... because HT does not increase breast cancer, and overall, its benefits out weight
Preventing Breast Cancer in HT users by Manuel Neves-e-Castro Portuguese Menopause Society September 2004 I am also PRO!... because HT does not increase breast cancer, and overall, its benefits out weight
Development, validation and application of risk prediction models
 Development, validation and application of risk prediction models G. Colditz, E. Liu, M. Olsen, & others (Ying Liu, TA) 3/28/2012 Risk Prediction Models 1 Goals Through examples, class discussion, and
Development, validation and application of risk prediction models G. Colditz, E. Liu, M. Olsen, & others (Ying Liu, TA) 3/28/2012 Risk Prediction Models 1 Goals Through examples, class discussion, and
POSTMENOPAUSAL ESTROGEN USE
 ORIGINAL CONTRIBUTION Estrogen Replacement Therapy and Ovarian Cancer Mortality in a Large Prospective Study of US Women Carmen Rodriguez, MD, MPH Alpa V. Patel, MPH Eugenia E. Calle, PhD Eric J. Jacob,
ORIGINAL CONTRIBUTION Estrogen Replacement Therapy and Ovarian Cancer Mortality in a Large Prospective Study of US Women Carmen Rodriguez, MD, MPH Alpa V. Patel, MPH Eugenia E. Calle, PhD Eric J. Jacob,
Chapter 2 The Link Between Obesity and Breast Cancer Risk: Epidemiological Evidence
 Chapter 2 The Link Between Obesity and Breast Cancer Risk: Epidemiological Evidence 2.1 BMI and Breast Cancer Risk BMI is routinely used to qualify an individual s adiposity, yet it is simply a measure
Chapter 2 The Link Between Obesity and Breast Cancer Risk: Epidemiological Evidence 2.1 BMI and Breast Cancer Risk BMI is routinely used to qualify an individual s adiposity, yet it is simply a measure
Steven Jubelirer, MD Clinical Professor Medicine WVU Charleston Division Senior Research Scientist CAMC Research Institute
 Steven Jubelirer, MD Clinical Professor Medicine WVU Charleston Division Senior Research Scientist CAMC Research Institute Objectives Develop a systematic way to think about benefits and harms of cancer
Steven Jubelirer, MD Clinical Professor Medicine WVU Charleston Division Senior Research Scientist CAMC Research Institute Objectives Develop a systematic way to think about benefits and harms of cancer
Ardhanu Kusumanto Oktober Contraception methods for gyne cancer survivors
 Ardhanu Kusumanto Oktober 2017 Contraception methods for gyne cancer survivors Background cancer treatment Care of gyn cancer survivor Promotion of sexual, cardiovascular, bone, and brain health management
Ardhanu Kusumanto Oktober 2017 Contraception methods for gyne cancer survivors Background cancer treatment Care of gyn cancer survivor Promotion of sexual, cardiovascular, bone, and brain health management
LOBULAR CARCINOMA IN SITU: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE
 : WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
Hormone replacement therapy and breast density after surgical menopause
 Hormone replacement therapy and breast density after surgical menopause Freya Schnabel*; Sarah Pivo; Esther Dubrovsky; Jennifer Chun; Shira Schwartz; Amber Guth; Deborah Axelrod Department of Surgery,
Hormone replacement therapy and breast density after surgical menopause Freya Schnabel*; Sarah Pivo; Esther Dubrovsky; Jennifer Chun; Shira Schwartz; Amber Guth; Deborah Axelrod Department of Surgery,
Breast Cancer Risk Assessment among Bahraini Women. Majida Fikree, MD, MSc* Randah R Hamadeh, BSc, MSc, D Phil (Oxon)**
 Bahrain Medical Bulletin, Vol. 35, No.1, March 2013 Breast Cancer Risk Assessment among Bahraini Women Majida Fikree, MD, MSc* Randah R Hamadeh, BSc, MSc, D Phil (Oxon)** Objective: To estimate breast
Bahrain Medical Bulletin, Vol. 35, No.1, March 2013 Breast Cancer Risk Assessment among Bahraini Women Majida Fikree, MD, MSc* Randah R Hamadeh, BSc, MSc, D Phil (Oxon)** Objective: To estimate breast
Supplementary Online Content
 Supplementary Online Content The Premenopausal Breast Cancer Collaborative Group. Association body mass index and age with premenopausal breast cancer risk in premenopausal women. JAMA Oncol. Published
Supplementary Online Content The Premenopausal Breast Cancer Collaborative Group. Association body mass index and age with premenopausal breast cancer risk in premenopausal women. JAMA Oncol. Published
CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY
 Biomed. Papers 147(2), 211 219 (2003) D. Houserková, J. Matlochová, M. Hartlová 211 CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY Dana Houserková
Biomed. Papers 147(2), 211 219 (2003) D. Houserková, J. Matlochová, M. Hartlová 211 CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY Dana Houserková
Reproductive factors, age at maximum height, and risk of three histologic types of breast cancer
 Title: Reproductive factors, age at maximum height, and risk of three histologic types of breast cancer Authors: Elisabeth F. Beaber, M.P.H. 1, 2 Victoria L. Holt, Ph.D. 1,2 Kathleen E. Malone, Ph.D. 1,2
Title: Reproductive factors, age at maximum height, and risk of three histologic types of breast cancer Authors: Elisabeth F. Beaber, M.P.H. 1, 2 Victoria L. Holt, Ph.D. 1,2 Kathleen E. Malone, Ph.D. 1,2
5. Summary of Data Reported and Evaluation
 168 IARC MONOGRAPHS VOLUME 91 5. Summary of Data Reported and Evaluation 5.1 Exposure data The first oral hormonal contraceptives that were found to inhibit both ovulation and implantation were developed
168 IARC MONOGRAPHS VOLUME 91 5. Summary of Data Reported and Evaluation 5.1 Exposure data The first oral hormonal contraceptives that were found to inhibit both ovulation and implantation were developed
Breast Cancer in Childhood Cancer Survivors: The Impact of Screening on Morbidity
 Breast Cancer in Childhood Cancer Survivors: The Impact of Screening on Morbidity WORKING GROUP: This report will be written within the Cancer Control Working Group with oversight from the Second Malignant
Breast Cancer in Childhood Cancer Survivors: The Impact of Screening on Morbidity WORKING GROUP: This report will be written within the Cancer Control Working Group with oversight from the Second Malignant
Factors Associated with Early Versus Late Development of Breast and Ovarian Cancer in BRCA1 and BRCA2 Positive Women
 Texas Medical Center Library DigitalCommons@The Texas Medical Center UT GSBS Dissertations and Theses (Open Access) Graduate School of Biomedical Sciences 5-2010 Factors Associated with Early Versus Late
Texas Medical Center Library DigitalCommons@The Texas Medical Center UT GSBS Dissertations and Theses (Open Access) Graduate School of Biomedical Sciences 5-2010 Factors Associated with Early Versus Late
General practice. Abstract. Subjects and methods. Introduction. examining the effect of use of oral contraceptives on mortality in the long term.
 Mortality associated with oral contraceptive use: 25 year follow up of cohort of 46 000 women from Royal College of General Practitioners oral contraception study Valerie Beral, Carol Hermon, Clifford
Mortality associated with oral contraceptive use: 25 year follow up of cohort of 46 000 women from Royal College of General Practitioners oral contraception study Valerie Beral, Carol Hermon, Clifford
Diseases of the breast (2 of 2) Breast cancer
 Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and breast cancer survivors. In partnership with
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 In partnership with Contents About World Cancer Research Fund International 1 Our
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 In partnership with Contents About World Cancer Research Fund International 1 Our
Breast cancer risk with postmenopausal hormonal treatment
 Human Reproduction Update, Vol.11, No.6 pp. 545 56, 25 Advance Access publication September 8, 25 doi:1.193/humupd/dmi28 Breast cancer risk with postmenopausal hormonal treatment John A.Collins 1,2,5,
Human Reproduction Update, Vol.11, No.6 pp. 545 56, 25 Advance Access publication September 8, 25 doi:1.193/humupd/dmi28 Breast cancer risk with postmenopausal hormonal treatment John A.Collins 1,2,5,
// Award Number: DAMD TITLE: Markers of Breast Cancer Risk in Women with Benign Breast Disease PRINCIPAL INVESTIGATOR:
 AD Award Number: DAMD17-00-1-0623 TITLE: Markers of Breast Cancer Risk in Women with Benign Breast Disease PRINCIPAL INVESTIGATOR: Margaret Mandelson, Ph.D. CONTRACTING ORGANIZATION: Group Health Cooperative
AD Award Number: DAMD17-00-1-0623 TITLE: Markers of Breast Cancer Risk in Women with Benign Breast Disease PRINCIPAL INVESTIGATOR: Margaret Mandelson, Ph.D. CONTRACTING ORGANIZATION: Group Health Cooperative
Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol
 Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Screening Mammograms: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Screening Mammograms:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Screening Mammograms:
Reliability of Reported Age at Menopause
 American Journal of Epidemiology Copyright 1997 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 146, No. 9 Printed in U.S.A Reliability of Reported Age at Menopause
American Journal of Epidemiology Copyright 1997 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 146, No. 9 Printed in U.S.A Reliability of Reported Age at Menopause
A Methodological Issue in the Analysis of Second-Primary Cancer Incidence in Long-Term Survivors of Childhood Cancers
 American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 11 Printed in U.S.A. DOI: 10.1093/aje/kwg278 PRACTICE OF EPIDEMIOLOGY
American Journal of Epidemiology Copyright 2003 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 158, No. 11 Printed in U.S.A. DOI: 10.1093/aje/kwg278 PRACTICE OF EPIDEMIOLOGY
Genetic Risk Evaluation and Testing Program
 INSTRUCTIONS: Please complete this form to the best of your ability PRIOR to your appointment. Please remember to list ALL relatives, both living and deceased, regardless of if they have had cancer or
INSTRUCTIONS: Please complete this form to the best of your ability PRIOR to your appointment. Please remember to list ALL relatives, both living and deceased, regardless of if they have had cancer or
breast cancer; relative risk; risk factor; standard deviation; strength of association
 American Journal of Epidemiology The Author 2015. Published by Oxford University Press on behalf of the Johns Hopkins Bloomberg School of Public Health. All rights reserved. For permissions, please e-mail:
American Journal of Epidemiology The Author 2015. Published by Oxford University Press on behalf of the Johns Hopkins Bloomberg School of Public Health. All rights reserved. For permissions, please e-mail:
Proportion of Breast Cancer Cases in the United States Explained by Well-Established Risk Factors
 Proportion of Breast Cancer Cases in the United States Explained by Well-Established Risk Factors M. Patricia Madigan, Regina G. Ziegler, Jacques Benichou, Celia Byrne, Robert N. Hoover* Background: Few
Proportion of Breast Cancer Cases in the United States Explained by Well-Established Risk Factors M. Patricia Madigan, Regina G. Ziegler, Jacques Benichou, Celia Byrne, Robert N. Hoover* Background: Few
ARTICLES. Validation of the Gail et al. Model of Breast Cancer Risk Prediction and Implications for Chemoprevention
 ARTICLES Validation of the Gail et al. Model of Breast Cancer Risk Prediction and Implications for Chemoprevention Beverly Rockhill, Donna Spiegelman, Celia Byrne, David J. Hunter, Graham A. Colditz Background:
ARTICLES Validation of the Gail et al. Model of Breast Cancer Risk Prediction and Implications for Chemoprevention Beverly Rockhill, Donna Spiegelman, Celia Byrne, David J. Hunter, Graham A. Colditz Background:
Prophylactic Mastectomy State of the Art
 Memorial Sloan-Kettering Cancer Center 1275 York Avenue, New York, NY 10065 6 th Brazilian Breast Cancer Conference Sao Paulo, Brazil 9 March 2012 Prophylactic Mastectomy State of the Art Monica Morrow
Memorial Sloan-Kettering Cancer Center 1275 York Avenue, New York, NY 10065 6 th Brazilian Breast Cancer Conference Sao Paulo, Brazil 9 March 2012 Prophylactic Mastectomy State of the Art Monica Morrow
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Interval Cancers in BreastScreen Aotearoa
 Interval Cancers in BreastScreen Aotearoa 2008 2009 Released 2018 nsu.govt.nz Citation: National Screening Unit. 2018. Interval Cancers in BreastScreen Aotearoa 2008 2009. Wellington: Ministry of Health.
Interval Cancers in BreastScreen Aotearoa 2008 2009 Released 2018 nsu.govt.nz Citation: National Screening Unit. 2018. Interval Cancers in BreastScreen Aotearoa 2008 2009. Wellington: Ministry of Health.
Patient Education. Breast Cancer Prevention. Cancer Center
 Patient Education Breast cancer affects one in nine women in the US by the time they reach their 80 s. It is the result of several mutations or alterations in the genes found in the DNA of normal breast
Patient Education Breast cancer affects one in nine women in the US by the time they reach their 80 s. It is the result of several mutations or alterations in the genes found in the DNA of normal breast
Chemo-endocrine prevention of breast cancer
 Chemo-endocrine prevention of breast cancer Andrea DeCensi, MD Division of Medical Oncology Ospedali Galliera, Genova; Division of Cancer Prevention and Genetics, European Institute of Oncology, Milano;
Chemo-endocrine prevention of breast cancer Andrea DeCensi, MD Division of Medical Oncology Ospedali Galliera, Genova; Division of Cancer Prevention and Genetics, European Institute of Oncology, Milano;
Nipple Aspirate Fluid Cytology and the Gail Model for Breast Cancer Risk Assessment in a Screening Population
 324 Cancer Epidemiology, Biomarkers & Prevention Nipple Aspirate Fluid Cytology and the Gail Model for Breast Cancer Risk Assessment in a Screening Population Jeffrey A. Tice, 1 Rei Miike, 2 Kelly Adduci,
324 Cancer Epidemiology, Biomarkers & Prevention Nipple Aspirate Fluid Cytology and the Gail Model for Breast Cancer Risk Assessment in a Screening Population Jeffrey A. Tice, 1 Rei Miike, 2 Kelly Adduci,
Anthropometric measures and serum estrogen metabolism in postmenopausal women: the Women s Health Initiative Observational Study
 Anthropometric measures and serum estrogen metabolism in postmenopausal women: the Women s Health Initiative Observational Study The Harvard community has made this article openly available. Please share
Anthropometric measures and serum estrogen metabolism in postmenopausal women: the Women s Health Initiative Observational Study The Harvard community has made this article openly available. Please share
Temporal trends in the incidence of molecular subtypes of breast cancer. Jonine D. Figueroa, Ph.D., M.P.H.
 Temporal trends in the incidence of molecular subtypes of breast cancer Jonine D. Figueroa, Ph.D., M.P.H. Epidemiology: Health data science Study of the distribution and determinants of health and disease
Temporal trends in the incidence of molecular subtypes of breast cancer Jonine D. Figueroa, Ph.D., M.P.H. Epidemiology: Health data science Study of the distribution and determinants of health and disease
The Decrease in Breast-Cancer Incidence in 2003 in the United States
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e s p e c i a l r e p o r t The Decrease in Breast-Cancer Incidence in 23 in the United States Peter M. Ravdin, Ph.D., M.D., Kathleen A. Cronin, Ph.D.,
T h e n e w e ng l a nd j o u r na l o f m e dic i n e s p e c i a l r e p o r t The Decrease in Breast-Cancer Incidence in 23 in the United States Peter M. Ravdin, Ph.D., M.D., Kathleen A. Cronin, Ph.D.,
Analysing research on cancer prevention and survival. Diet, nutrition, physical activity and breast cancer survivors. Revised 2018
 Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Analysing research on cancer prevention and survival Diet, nutrition, physical activity and breast cancer survivors 2014 Revised 2018 Contents World Cancer Research Fund Network 3 1. Summary of Panel judgements
Natural Hormones Replacement An Evidence and Practice Based Approach
 Natural Hormones Replacement An Evidence and Practice Based Approach Andres Ruiz, PharmD, MSc, FACA President/Partner Stonegate Pharmacy PRESENTED BY THE AMERICAN COLLEGE OF APOTHECARIES 2830 SUMMER OAKS
Natural Hormones Replacement An Evidence and Practice Based Approach Andres Ruiz, PharmD, MSc, FACA President/Partner Stonegate Pharmacy PRESENTED BY THE AMERICAN COLLEGE OF APOTHECARIES 2830 SUMMER OAKS
Dietary Fatty Acids and the Risk of Hypertension in Middle-Aged and Older Women
 07/14/2010 Dietary Fatty Acids and the Risk of Hypertension in Middle-Aged and Older Women First Author: Wang Short Title: Dietary Fatty Acids and Hypertension Risk in Women Lu Wang, MD, PhD, 1 JoAnn E.
07/14/2010 Dietary Fatty Acids and the Risk of Hypertension in Middle-Aged and Older Women First Author: Wang Short Title: Dietary Fatty Acids and Hypertension Risk in Women Lu Wang, MD, PhD, 1 JoAnn E.
Urinary Melatonin Levels and Risk of Postmenopausal Breast Cancer in the Women's Health Initiative Observational Study
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2012 Urinary Melatonin Levels and Risk of Postmenopausal Breast Cancer in the Women's Health Initiative
University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2012 Urinary Melatonin Levels and Risk of Postmenopausal Breast Cancer in the Women's Health Initiative
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Cancer Risks of Ovulation Induction
 Cancer Risks of Ovulation Induction 5th World Congress on Ovulation Induction September 13-15, 2007 Louise A. Brinton, Ph.D. National Cancer Institute Rockville, Maryland, USA Ovulation Induction and Cancer
Cancer Risks of Ovulation Induction 5th World Congress on Ovulation Induction September 13-15, 2007 Louise A. Brinton, Ph.D. National Cancer Institute Rockville, Maryland, USA Ovulation Induction and Cancer
Relationship between Menopausal Hormone Therapy and Risk of Ductal, Lobular, and Ductal-Lobular Breast Carcinomas
 43 Relationship between Menopausal Hormone Therapy and Risk of Ductal, Lobular, and Ductal-Lobular Breast Carcinomas Christopher I. Li, 1 Kathleen E. Malone, 1 Peggy L. Porter, 1,2,3 Thomas J. Lawton,
43 Relationship between Menopausal Hormone Therapy and Risk of Ductal, Lobular, and Ductal-Lobular Breast Carcinomas Christopher I. Li, 1 Kathleen E. Malone, 1 Peggy L. Porter, 1,2,3 Thomas J. Lawton,
BREAST CANCER. surgical treatment of. in pennsylvania EMBARGOED - Not for release before October 9, 2012.
 PENNSYLVANIA HEALTH CARE COST CONTAINMENT COUNCIL EMBARGOED - Not for release before October 9, 2012. surgical treatment of BREAST CANCER in pennsylvania 2002 2011 October 2012 Factors That Increase the
PENNSYLVANIA HEALTH CARE COST CONTAINMENT COUNCIL EMBARGOED - Not for release before October 9, 2012. surgical treatment of BREAST CANCER in pennsylvania 2002 2011 October 2012 Factors That Increase the
W3C Life Sciences: Clinical Observations Interoperability: EMR + Clinical Trials Use-case for EMR + Clinical Trials Interoperability
 W3C Life Sciences: Clinical Observations Interoperability: EMR + Clinical Trials Use-case for EMR + Clinical Trials Interoperability Background: The key issue is to investigate whether some of the data
W3C Life Sciences: Clinical Observations Interoperability: EMR + Clinical Trials Use-case for EMR + Clinical Trials Interoperability Background: The key issue is to investigate whether some of the data
It is a malignancy originating from breast tissue
 59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
Low-Fat Dietary Pattern Intervention Trials for the Prevention of Breast and Other Cancers
 Low-Fat Dietary Pattern Intervention Trials for the Prevention of Breast and Other Cancers Ross Prentice Fred Hutchinson Cancer Research Center and University of Washington AICR, November 5, 2009 Outline
Low-Fat Dietary Pattern Intervention Trials for the Prevention of Breast and Other Cancers Ross Prentice Fred Hutchinson Cancer Research Center and University of Washington AICR, November 5, 2009 Outline
Learning Objectives. Peri menopause. Menopause Overview. Recommendation grading categories
 Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION A Population-Based Study of Bilateral Efficacy in Women at Elevated Risk for Breast Cancer in Community Practices Ann M. Geiger, PhD; Onchee Yu, MS; Lisa J. Herrinton, PhD; William
ORIGINAL INVESTIGATION A Population-Based Study of Bilateral Efficacy in Women at Elevated Risk for Breast Cancer in Community Practices Ann M. Geiger, PhD; Onchee Yu, MS; Lisa J. Herrinton, PhD; William
BASED ON CONCERNS that estrogen replacement
 Estrogen Replacement Therapy After Localized Breast Cancer: Clinical Outcome of 319 Women Followed Prospectively By Rena Vassilopoulou-Sellin, Lina Asmar, Gabriel N. Hortobagyi, Mary Jean Klein, Marsha
Estrogen Replacement Therapy After Localized Breast Cancer: Clinical Outcome of 319 Women Followed Prospectively By Rena Vassilopoulou-Sellin, Lina Asmar, Gabriel N. Hortobagyi, Mary Jean Klein, Marsha
Discussing Fertility Preservation with Breast Cancer Patients
 Chapter 35 Discussing Fertility Preservation with Breast Cancer Patients Jacqueline S. Jeruss J.S. Jeruss (B) Department of Surgery, Robert H. Lurie Comprehensive Cancer Center, Northwestern University
Chapter 35 Discussing Fertility Preservation with Breast Cancer Patients Jacqueline S. Jeruss J.S. Jeruss (B) Department of Surgery, Robert H. Lurie Comprehensive Cancer Center, Northwestern University
ORIGINAL INVESTIGATION. Hormone Therapy and the Impact of Estrogen Intake on the Risk of Ovarian Cancer. increasingly used in developed
 ORIGINAL INVESTIGATION Hormone Therapy and the Impact of Estrogen Intake on the Risk of Ovarian Cancer Eva Glud, MD, PhD; Susanne K. Kjaer, DMSc; Birthe L. Thomsen, MSc; Claus Høgdall, PhD; Lise Christensen,
ORIGINAL INVESTIGATION Hormone Therapy and the Impact of Estrogen Intake on the Risk of Ovarian Cancer Eva Glud, MD, PhD; Susanne K. Kjaer, DMSc; Birthe L. Thomsen, MSc; Claus Høgdall, PhD; Lise Christensen,
Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
THE WOMEN S HEALTH INITIAtive
 ORIGINAL CONTRIBUTION JAMA-EXPRESS Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women Principal Results From the Women s Health Initiative Randomized Controlled Trial Writing
ORIGINAL CONTRIBUTION JAMA-EXPRESS Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women Principal Results From the Women s Health Initiative Randomized Controlled Trial Writing
EPIDEMIOLOGY AND BIOSTATISTICS. Hormone Replacement Therapy and Lens Opacities
 Hormone Replacement Therapy and Lens Opacities The Salisbury Eye Evaluation Project EPIDEMIOLOGY AND BIOSTATISTICS Ellen E. Freeman, BA; Beatriz Munoz, MSc; Oliver D. Schein, MD; Sheila K. West, PhD Background:
Hormone Replacement Therapy and Lens Opacities The Salisbury Eye Evaluation Project EPIDEMIOLOGY AND BIOSTATISTICS Ellen E. Freeman, BA; Beatriz Munoz, MSc; Oliver D. Schein, MD; Sheila K. West, PhD Background:
THE SAFETY CHECK LIST BEFORE STARTING HT
 THE SAFETY CHECK LIST BEFORE STARTING HT This safety checklist was designed by the Endocrine Society in 2015 to minimize the chance of giving hormone therapy to women who may be negatively affected by
THE SAFETY CHECK LIST BEFORE STARTING HT This safety checklist was designed by the Endocrine Society in 2015 to minimize the chance of giving hormone therapy to women who may be negatively affected by
Breast Cancer. Dr. Andres Wiernik 2017
 Breast Cancer Dr. Andres Wiernik 2017 Agenda: The Facts! (Epidemiology/Risk Factors) Biological Classification/Phenotypes of Breast Cancer Treatment approach Local Systemic Agenda: The Facts! (Epidemiology/Risk
Breast Cancer Dr. Andres Wiernik 2017 Agenda: The Facts! (Epidemiology/Risk Factors) Biological Classification/Phenotypes of Breast Cancer Treatment approach Local Systemic Agenda: The Facts! (Epidemiology/Risk
1. Collaborative Group on Epidemiological Studies of Ovarian Cancer. Ovarian cancer and oral contraceptives: collaborative reanalysis of data from 45
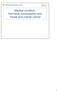 1 2 3 1. Collaborative Group on Epidemiological Studies of Ovarian Cancer. Ovarian cancer and oral contraceptives: collaborative reanalysis of data from 45 epidemiological studies including 23,257 women
1 2 3 1. Collaborative Group on Epidemiological Studies of Ovarian Cancer. Ovarian cancer and oral contraceptives: collaborative reanalysis of data from 45 epidemiological studies including 23,257 women
Serum estrogen level after hormone replacement therapy and body mass index in postmenopausal and bilaterally ovariectomized women
 Maturitas 50 (2005) 19 29 Serum estrogen level after hormone replacement therapy and body mass index in postmenopausal and bilaterally ovariectomized women Toshiyuki Yasui a,, Hirokazu Uemura a, Yuka Umino
Maturitas 50 (2005) 19 29 Serum estrogen level after hormone replacement therapy and body mass index in postmenopausal and bilaterally ovariectomized women Toshiyuki Yasui a,, Hirokazu Uemura a, Yuka Umino
Risk Factors for Breast Cancer in Elderly Women
 American Journal Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School Public Health All rights reserved Vol. 160, 9 Printed in U.S.A. DOI: 10.1093/aje/kwh276 Risk Factors for Breast Cancer
American Journal Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School Public Health All rights reserved Vol. 160, 9 Printed in U.S.A. DOI: 10.1093/aje/kwh276 Risk Factors for Breast Cancer
ORIGINAL INVESTIGATION. Physical Activity and Risk of Breast Cancer Among Postmenopausal Women
 ORIGINAL INVESTIGATION Physical Activity and Risk of Breast Cancer Among Postmenopausal Women A. Heather Eliassen, ScD; Susan E. Hankinson, RN, ScD; Bernard Rosner, PhD; Michelle D. Holmes, MD, DrPH; Walter
ORIGINAL INVESTIGATION Physical Activity and Risk of Breast Cancer Among Postmenopausal Women A. Heather Eliassen, ScD; Susan E. Hankinson, RN, ScD; Bernard Rosner, PhD; Michelle D. Holmes, MD, DrPH; Walter
Comparison And Application Of Methods To Address Confounding By Indication In Non- Randomized Clinical Studies
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 Dissertations and Theses 2013 Comparison And Application Of Methods To Address Confounding By Indication
University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 Dissertations and Theses 2013 Comparison And Application Of Methods To Address Confounding By Indication
preventive health care measure
 introduction 98 < pre- & post-esrd preventive care 1 < diabetic care 12 < cancer screening 14 < chapter summary 16 Chapter Five preventive health care measure SSo neither ought you to attempt to cure the
introduction 98 < pre- & post-esrd preventive care 1 < diabetic care 12 < cancer screening 14 < chapter summary 16 Chapter Five preventive health care measure SSo neither ought you to attempt to cure the
Asmall number of studies have examined
 Appendix B: Evidence on Hormone Replacement Therapy and Fractures B Asmall number of studies have examined directly the relationship between use of hormonal replacement therapy and risk of hip fracture
Appendix B: Evidence on Hormone Replacement Therapy and Fractures B Asmall number of studies have examined directly the relationship between use of hormonal replacement therapy and risk of hip fracture
Performance of the Breast Cancer Risk Assessment Tool Among Women Aged 75 Years and Older
 JNCI J Natl Cancer Inst (2016) 108(3): djv348 doi:10.1093/jnci/djv348 First published online November 30, 2015 Article Performance of the Breast Cancer Risk Assessment Tool Among Women Aged 75 Years and
JNCI J Natl Cancer Inst (2016) 108(3): djv348 doi:10.1093/jnci/djv348 First published online November 30, 2015 Article Performance of the Breast Cancer Risk Assessment Tool Among Women Aged 75 Years and
PFIZER INC. What is the difference in incidence of fracture in women who ever or never used DMPA for contraception?
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
