S.C. Oncologia Medica, Azienda Ospedaliera, Perugia, Italy; b. Medical Oncology Clinic, Jules Bordet Institute, Brussels, Belgium
|
|
|
- Kimberly Matthews
- 6 years ago
- Views:
Transcription
1 This material is protected by U.S. Copyright law. Unauthorized reproduction is prohibited. For reprints contact: Breast Cancer Breast Cancer: Achievements in Adjuvant Systemic Therapies in the Pre-Genomic Era Mariantonietta Colozza, a Evandro de Azambuja, b Fatima Cardoso, b Chantal Bernard, b Martine J. Piccart b a S.C. Oncologia Medica, Azienda Ospedaliera, Perugia, Italy; b Medical Oncology Clinic, Jules Bordet Institute, Brussels, Belgium Key Words. Breast cancer Adjuvant Chemotherapy Endocrine therapy Trastuzumab Taxanes Learning Objectives After completing this course, the reader will be able to: 1. Identify the available adjuvant systemic therapies for breast cancer patients. 2. Identify the role of taxanes in node-positive breast cancer patients. 3. Discuss the most useful endocrine therapy in pre- and postmenopausal patients with breast cancer. CME Access and take the CME test online and receive 1 AMA PRA category 1 credit at CME.TheOncologist.com Abstract In recent decades, the use of adjuvant systemic therapies for early breast cancer has increased extensively and has most likely contributed to the decline in breast cancer mortality observed in the U.S. and in some European countries. The last few years have witnessed accelerated progress in the treatment of early breast cancer, with the introduction of taxanes and aromatase inhibitors and, most impressively, trastuzumab to the adjuvant portfolio. When compared with anthracycline-based regimens, the addition of taxanes to treatments for patients with node-positive breast cancer has shown benefits in disease-free survival and, in some trials, in overall survival; however, these drugs are not yet universally accepted as standard treatment. Significant improvements in endocrine therapy in both pre- and postmenopausal patients with endocrine-responsive disease have been made. In the postmenopausal setting, aromatase inhibitors have shown superiority over tamoxifen in a direct comparison upfront or when given in sequence after 2 5 years of tamoxifen, but the optimal modality of administration remains unclear. For premenopausal women, ovarian function suppression with luteinizing hormone-releasing hormone analogues combined with tamoxifen has generated similar results to cyclophosphamide, methotrexate, 5-fluorouracil (CMF) based regimens. Recently, trastuzumab has had a dramatic impact on the evolution of human epidermal growth factor receptor 2 (HER-2) positive early breast cancer treated with standard adjuvant modalities; specifically, relapses, including distant relapses, have been halved. In this review, we summarize these main achievements, discuss the currently available adjuvant treatment options for breast cancer patients, and emphasize the need for more efficient translational research to improve individual treatment tailoring. The Oncologist 2006;11: Correspondence: Martine Piccart, M.D., Ph.D., Jules Bordet Institute, Boulevard de Waterloo, 125, 1000 Brussels, Belgium. Telephone: ; Fax: ; martine.piccart@bordet.be Received October 6, 2005; accepted for publication November 29, AlphaMed Press /2006/$20.00/0 The Oncologist 2006;11:
2 112 Achievements in Early Breast Cancer Introduction The hypothesis that adjuvant systemic treatment would reduce the risk for recurrence and improve the chances of survival in women with primary breast cancer (BC) was formulated in the late 1960s to early 1970s. Since then, significant advances have been made through the conduct of a large number of prospective, randomized clinical trials analyzing different strategies, chemotherapeutic regimens, and durations of treatment; however, only a few of these trials had sufficient statistical power. Therefore, in 1985, a meta-analysis of adjuvant clinical trials was undertaken by the Early Breast Cancer Trialists Collaborative Group (EBCTCG) in an attempt to provide reliable estimations of relative and absolute average treatment benefits. Since then it has been updated every 5 years [1 3]. From hundreds of randomized controlled adjuvant trials and from the metaanalyses of these trials [1 3], the benefits associated with the adjuvant use of tamoxifen (Nolvadex ; AstraZeneca Pharmaceuticals, Wilmington, DE), ovarian ablation (OA), and chemotherapy (CT) are now level 1 evidence based. Optimal administration of these therapies in combination or in sequence reduces the relative risk (RR) for recurrence and death by more than 50%, with long-lasting benefits exceeding years [4]. In recent years, three influential groups have published consensus guidelines for the systemic adjuvant therapy of BC patients [5 8]. While these guidelines do facilitate evidence-based practice, they are not perfect and reach somewhat different recommendations, particularly for premenopausal women with hormone receptor (HR) positive tumors and for node (N)-negative patients with small tumors. These differences may be explained, at least in part, by the panel members selection process, with expert opinions replacing evidence-based recommendations when the latter are difficult to formulate in view of conflicting or complex data [9, 10]. As the result of a major shift in thinking, risk relapse is no longer the major determinant in the new 2005 St. Gallen algorithm for clinical decision making: it comes second after the determination of endocrine responsiveness. The rationale for this shift is at least threefold: (a) there is growing evidence of much larger benefits from CT in endocrine nonresponsive disease; (b) substantial additional progress has been made lately in adjuvant endocrine therapy (ET), reducing the magnitude of additional benefit brought by CT in endocrine-responsive disease; and (c) gene-expression profiling studies nicely substantiate that estrogen receptor (ER) status is the major factor, and these studies are likely to improve prediction of response to treatment in the near future. The St. Gallen risk classification has also undergone fine-tuning: N-positive disease is no longer a symptom of high risk, with the one to three positive nodes group joining the intermediate risk category in cases of negative human epidermal growth factor receptor (HER) 2 status; positive HER-2 status, in contrast, is sufficient to upgrade a N-negative patient to an intermediate risk category [11]. Despite the advances made, we are still treating the majority of patients based on empirical evidence medicine, with the result that only a proportion of them truly benefit. Fortunately, in recent years, significant progress has been made in molecular oncology. Translational research is now taking the center stage, facilitating the creation of a link between basic and clinical research. Improvement in the understanding of the disease at the molecular level will hopefully allow us to define subsets of patients with different prognoses and responsiveness to treatments. Based on published results in the era of so-called empirical oncology, the most important advances, and the new standards of care for endocrine, cytotoxic, and biological therapies, are summarized in this paper. Adjuvant Endocrine Therapy For decades, tamoxifen has been the most important hormonal agent for the adjuvant treatment of HR-positive BC patients. The first adjuvant trials began in the mid to late 1970s using a 1-year treatment duration. Subsequently, because preliminary results from clinical trials showed that the treatment benefit was higher with extended tamoxifen use, and because the drug has a good safety profile, tamoxifen began to be administered for longer periods [4]. The earliest trials included mainly N-positive postmenopausal patients independent of HR status, while the latest ones have included patients with HR-positive or unknown tumors, independently of nodal or menopausal status. The EBCTCG meta-analysis [3] convincingly showed that tamoxifen administered for 5 years to women with ERpositive tumors reduces the risk for recurrence and death, with absolute improvements in 10-year survival of 12.6% for N-positive and 5.3% for N-negative patients. These benefits are independent of patient age, menopausal status, progesterone receptor status, and the use of adjuvant CT. However, given the fact that no advantage was demonstrated in women with ER-negative tumors, ET is no longer recommended for these patients. The optimal duration of tamoxifen administration is still undefined, even if it is well known that 5 years of treatment is superior to shorter periods. A prolongation of the duration (10 years or indefinitely) did not provide further benefit and was associated with a worse outcome in two relatively small trials [12, 13]. However, in a small study enrolling N-positive patients also treated with CT, a statistically significant advantage in time to first recurrence or contralateral BC was observed [14]. The Oncologist
3 Colozza, Azambuja, Cardoso et al. 113 Currently, two large randomized trials are trying to answer this question of optimal duration. The Adjuvant Tamoxifen Longer Against Shorter (ATLAS) study has randomized 15,254 patients with ER-positive or unknown BC between tamoxifen given for 5 years and tamoxifen given for 10 years [15]. Similarly, the adjuvant Tamoxifen Treatment, offer more? (attom) study was just closed after reaching an accrual of 8,625 patients. Tamoxifen is quite well tolerated, and the most common side effects consist of hot flushes and vaginal discharge; however, a two- to threefold higher risk for uterine cancer and thromboembolic events in postmenopausal patients has been reported. These risks are lower in premenopausal women, and overall, the benefits obtained with tamoxifen outweigh its side effects. In addition, tamoxifen has favorable effects on bone density [16 19] and lipid profiles [16, 20, 21]. Postmenopausal Patients A revolutionary change in the adjuvant treatment of postmenopausal BC women has occurred since the publication of the results of the first large adjuvant trials that investigated the use of third-generation aromatase inhibitors (AIs) as replacement for or in sequence with tamoxifen. Table 1 and Table 2 summarize the efficacy and safety of adjuvant AIs, respectively. In the Arimidex, Tamoxifen Alone or in Combination (ATAC) trial [22], anastrozole (Arimidex ; AstraZeneca Pharmaceuticals) yielded a statistically significant longer disease-free survival (DFS) time and time to recurrence (BC events) in comparison with tamoxifen and with the combination of both agents in HR-positive patients. Anastrozole also significantly reduced the incidence of primary contralateral BC in the overall population. At a median follow-up of 68 months, an absolute difference in DFS of 2.4% in the overall population and 2.9% in the HR-positive subgroup was reported [23 25]. Based on these results, the U.S. Food and Drug Administration (FDA) approved anastrozole for adjuvant therapy in Recently, the preliminary results of the Breast International Group (BIG) 1-98 study, a large four-arm trial comparing letrozole (Femara ; Novartis Pharmaceuticals Corporation, East Hanover, NJ) with tamoxifen, as well as the sequencing of both agents, have been presented [26, 27]. At this primary core analysis of 8,010 patients, all events and follow-up beyond the switch in the two sequential arms have been excluded. The analysis demonstrated that, in comparison with tamoxifen, letrozole produced a significantly longer DFS time; with a median follow-up of 2.2 years, an absolute benefit of 2.6% in DFS was seen. Other trials with different designs have evaluated AIs in postmenopausal women with HR-positive or unknown tumors. In the National Cancer Institute of Canada Clinical Trials Group (NCIC CTG) MA.17/BIG 1-97 trial, patients who were disease free after 5 years of tamoxifen were randomized to receive either letrozole for an additional 5 years or placebo [28, 29]. That trial was stopped prematurely because of the results of its first interim analysis, which showed an absolute difference in the rate of events (locoregional, distant recurrence, and contralateral BC) of 3.5% in favor of the letrozole arm at a median follow-up of 30 months. The actuarial calculation projected an absolute difference of 4.6% over 4 years. Also demonstrated was a survival benefit (hazard ratio, 0.61; 95% confidence interval [CI], ; p =.04) in the subgroup of N-positive patients, known to carry the highest annual risk for late relapses. Importantly, letrozole does not seem to significantly alter serum cholesterol, high-density lipoprotein cholesterol, low-density lipoprotein cholesterol, triglyc- Table 1. Comparison of the five adjuvant trials with aromatase inhibitors: maturity and magnitude of benefit ATAC [25] IES [31] MA.17 [29] ARNO 95/ ABCSG 8 [33, 36] BIG 1-98 [26, 27] No. of randomized patients 6,186 4,742 5,187 3,224 8,010 Percent of patients still 0% >10% >99% 45% 14% receiving treatment at the time of reporting Follow-up (months) No. of events 1, Distant events (%) 699 (57%) 288 (58%) 134 (54%) 121 (68%) 408 (63%) Absolute benefit in DFS 3.7% at 6 years 4.7% at 3 years 3.5% at 2.5 years; projected 4.6% at 4 years 3.1% at 3 years 2.6% at 2.2 years Abbreviations: ABCSG, Austrian Breast and Colorectal Cancer Study Group; ARNO, Arimidex -Nolvadex ; ATAC, Arimidex, Tamoxifen Alone or in Combination; BIG, Breast International Group; DFS, disease-free survival; IES, Intergroup Exemestane Study; MA.17, National Cancer Institute of Canada Clinical Trials Group MA.17 trial.
4 114 Achievements in Early Breast Cancer Table 2. Comparison of the five adjuvant trials with aromatase inhibitors: safety profile ATAC [25] IES [31] MA.17 [29] ARNO 95/ABCSG 8 [33] BIG 1-98 [26, 27] Anastrozole Tam Exemestane Tam Letrozole Placebo Anastrozole Tam Letrozole Tam Thromboembolic NA NA events (%) Endometrial cancer (%) Bone fractures (%) Osteoporosis (%) NA NA NA NA NA NA Arthralgia and NA a NA a myalgia (%) Hot flushes (%) NA a NA a Cardiovascular events (%) NA NA b 0.12 b a Data available only for ABCSG trial 8. b Myocardial infarction. Abbreviations: ABCSG, Austrian Breast and Colorectal Cancer Study Group; ARNO, Arimidex -Nolvadex ; ATAC, Arimidex Tamoxifen Alone or in Combination; BIG, Breast International Group; DFS, disease-free survival; IES, Intergroup Exemestane Study; MA.17, National Cancer Institute of Canada Clinical Trials Group MA.17 trial; NA, not available; Tam, tamoxifen. erides, or lipoprotein-a in nonhyperlipidemic postmenopausal women with primary BC pretreated with 5 years of adjuvant tamoxifen therapy and then receiving up to 36 months of letrozole [30]. The sequential use of AIs after 2 3 years of tamoxifen in comparison with tamoxifen alone for a total duration of 5 years in both arms has been evaluated in three trials. The largest is the Intergroup Exemestane Study (IES/BIG 2-97), which investigated the sequential use of exemestane (Aromasin ; Pfizer Pharmaceuticals, New York) after 2 3 years of tamoxifen in 4,742 patients [31, 32]. At a median follow-up of 30.6 months, when the majority of patients (>90%) had completed their planned treatment, a 27% relative reduction in the risk for events was noted, with an absolute benefit in DFS of 4.7% at 3 years after randomization. Based on these results, the FDA approved exemestane for adjuvant therapy in October Two smaller trials analyzed switching to anastrozole and have confirmed the previous results [33 36]. A pooled analysis from two trials sharing the same design showed, at a median follow-up of 28 months, a hazard ratio for event-free survival (EFS) of 0.60 in favor of anastrozole (95% CI, ; p =.0009). The 3-year EFS rates were 92.7% for tamoxifen and 95.8% for anastrozole. In this patient population not exposed to any adjuvant CT, no difference has emerged in overall survival (OS) (p =.16) [33, 36]. In terms of tolerability, a higher incidence of bone fractures, greater risk for osteoporosis, and joint symptoms are the most common side effects associated with the use of AIs. However, some clinical differences in toxicities between the AIs are beginning to appear, such as more cardiac deaths and deaths resulting from cerebrovascular events observed with letrozole in the BIG 1-98 trial [26, 27] and a higher rate of myocardial infarction with exemestane in the IES trial [32], even if with nonstatistically significant differences. These events are worrisome but still preliminary, and further investigations are warranted. Despite all these encouraging results, concerns remain because of the relatively short median follow-up time of the majority of these trials, and because of the uncertainties about the consequences of long-term estrogen deprivation. Furthermore, unanswered remaining questions include: what is the best modality to administer AIs (upfront? in sequence? which sequence?)? What is the optimal duration of the treatment? And which patients will benefit the most from each approach? It is expected that in the near future techniques such as genomics and proteomics will facilitate the individualization of adjuvant ET options (Fig. 1). Premenopausal Patients OA/ovarian suppression, tamoxifen, or the combination are the therapeutic options for adjuvant ET in premenopausal, HR-positive women. Ovarian Ablation Surgical or radiation OA as a single treatment modality began to be evaluated in 1948 but, initially, the results of these trials were interpreted as negative because of study design limitations (small sample size and inclusion of patients not selected according to menopausal and HR sta- The Oncologist
5 Colozza, Azambuja, Cardoso et al. 115 Figure 1. Adjuvant aromatase inhibitors in postmenopausal hormone receptor positive breast cancer. Abbreviations: AI, aromatase inhibitor; ER +, estrogen receptor positive; Tam, tamoxifen; y, years. tus). However, when analyzed in the EBCTCG meta-analysis, OA produced longer survival times (absolute reduction, 9.8%) and a lower rate of BC recurrence (absolute reduction, 8.5%) in women <50 years old [1]. These benefits were independent of age and N status, but were greater in women with ER-positive tumors. Through indirect comparisons, the magnitude of benefit obtained with OA appeared to be similar to the one derived from adjuvant CT or tamoxifen alone. No advantage was obtained by combining OA and CT in comparison with CT alone [1, 37]. The permanent amenorrhea often induced by CT in women older than 40 can partially explain these negative results [38, 39]. OA/Ovarian Suppression with or Without Tamoxifen Compared with Chemotherapy Recently, medical OA (moa) with luteinizing hormonereleasing hormone (LHRH) analogues has been substituted for OA. Several trials have compared OA/mOA with or without tamoxifen with CT in premenopausal patients with HR-positive tumors, as shown in Table 3. The first four studies compared OA [40, 41] or 2 years of moa [42 44] with cyclophosphamide, methotrexate, and 5-fluorouracil (CMF) in N-positive premenopausal patients, and they did not find any statistically significant difference in DFS or OS. In another trial, stage I/II N-negative patients were randomized to receive classic CMF for six cycles or the same CT followed by 2 years of goserelin (Zoladex ; AstraZeneca Pharmaceuticals) or goserelin alone [45]. About 30% of the patients were ER negative. In the overall population, and in the ER-positive subgroup, no statistically significant differences in DFS and OS were reported (only a trend toward longer DFS with the combined treatment in patients <40 years of age and with ER-positive tumors); however, CMF was superior to goserelin alone in the ER-negative subgroup. A comparison between CT with CMF or 5-fluorouracil, doxorubicin/epirubicin, and cyclophosphamide (FAC/ FEC) regimens and OA or moa plus tamoxifen was performed in four trials [46 49], but in only one did the complete estrogen blockade significantly improve relapse-free survival over CT [47]. Based on these results, the combination of moa and tamoxifen was selected as a standard treatment option for premenopausal patients with HR-positive tumors by the St. Gallen Consensus [6, 7]. However, CT plus tamoxifen was preferred by the National Institutes of Health (NIH) Consensus panelists [5], while OA was left as an alternative option for selected patients. Two other trials have evaluated the addition of moa to standard adjuvant treatment. In the first one, the addition of goserelin and tamoxifen to the CAF regimen resulted in a significantly longer DFS time, while no advantage was observed with the addition of goserelin alone in N-positive HR-positive BC patients [50, 51]. Subgroup analysis suggested that younger patients and those who did not become amenorrheic after CT got the largest benefit from the addition of goserelin to CAF. Conversely, the addition of tamoxifen seemed more effective in older women and in those who experienced CT-induced amenorrhea. The second trial adjuvant Zoladex in Premenopausal Patients (ZIPP) used a 2 2 factorial design to compare 2 years of tamoxifen with 2 years of goserelin and with the combination of the two or no further treatment in premenopausal patients independently of ER status. Patients had received a standard treatment with surgery, with or without radiotherapy, with or without CT, and with or without tamoxifen. Goserelin prolonged EFS (RR, 0.80; 95% CI, ), although
6 116 Achievements in Early Breast Cancer Table 3. Randomized trials comparing ovarian ablation with or without tamoxifen with chemotherapy in premenopausal patients Study Treatments Stage Results Scottish [40] CMF q3w versus OA II No difference Scandinavian [41] CMF q3w versus OA II No difference Zebra ZEBRA [42, 43] CMF q4w versus G 2 yrs N + No difference for ER + TABLE [44] CMF q4w versus L 2 yrs N + No difference IBCSG VIII [45] CMF c ± G versus G 2 yrs N No difference for ER + GROCTA 02 [46] CMF q4w versus OA/G + Tam N /N + No difference ABCSG 5 [47] CMF q4w versus G 3 yrs + Tam I/II Better RFS for OA + TAM French [49] FAC versus AO + Tam N + No difference FASG 06 [48] FEC versus T 3 yrs + Tam N + No difference IBCSG [115] OA + Tam + AC/EC versus OA + Tam N + No difference Abbreviations: ABCSG, Austrian Breast and Colorectal Cancer Study Group; AC, doxorubicin and cyclophosphamide; CMF, cyclophosphamide, methotrexate, and 5-fluorouracil; EC, epirubicin and cyclophosphamide; ER +, estrogen receptor positive; FAC, 5-fluorouracil, doxorubicin, and cyclophosphamide; FASG, French Adjuvant Study Group; FEC, 5-fluorouracil, epirubicin, and cyclophosphamide; G, goserelin; GROCTA, Gruppo di Ricerca in Oncologia Clinica e Terapie Associate (Italian Breast Cancer Adjuvant Study Group); IBCSG, International Breast Cancer Study Group; N, node negative; L, leuprorelin; N +, node positive; OA, ovarian ablation; q3w, every 3 weeks; q4w, every 4 weeks; RFS. relapse-free survival; T, triptorelin; TABLE, Takeda Adjuvant Breast Cancer Study with Leuprorelin Acetate; Tam, tamoxifen; yrs, years; ZEBRA, Zoladex Early Breast Cancer Research Association. the results of a subgroup analysis suggest a greater effect in ER-positive patients not receiving CT [52]. The most commonly reported toxicities with moa include hypertension, diabetes, bone loss, and weight gain. All these toxicities should be taken into consideration when selecting a treatment for which data are, as yet, inconclusive. There are still some unanswered questions regarding (a) the selection of patients who can really benefit from moa plus tamoxifen as the only adjuvant treatment or in addition to CT, (b) the optimal treatment duration of LHRH analogues, and (c) the long-term side effects of these agents. Three ongoing important trials are trying to answer some of these questions. The suppression ovarian function trial (SOFT)/BIG 2-02 trial is comparing tamoxifen with tamoxifen plus ovarian function suppression (OFS) and with exemestane plus OFS in patients that still have menses 6 months after stopping CT. For those patients considered candidates for ovarian suppression from the beginning, the tamoxifen and exemestane trial (TEXT)/BIG 3-02 trial is randomizing patients to either OFS with or without CT plus tamoxifen or OFS with or without CT plus exemestane [53]. A third trial, the Premenopausal Endocrine Responsive Chemotherapy (PERCHE) trial is trying to answer the question of whether CT adds benefits to combined ET. Adjuvant Chemotherapy The EBCTCG meta-analysis [2] demonstrated that adjuvant CT significantly reduces the risk for relapse and death in operable BC patients regardless of age, N status, HR status, and menopausal status, although the absolute advantage is proportional to the risk for relapse and decreases with increasing age. Furthermore, in N-positive patients, anthracycline-based CT is associated with a 4% absolute reduction in the risk for recurrence and death above that seen with CMF after 10 years of follow-up. The role of adjuvant taxanes has not yet been examined in the EBCTCG metaanalyses, and there is a lack of data regarding their optimal schedule and timing of administration. Because of the small number of patients older than 70 years treated with adjuvant CT, that meta-analysis does not allow us to define the role of CT in elderly patients. Recently, data from N-positive patients 65 years old enrolled in four Cancer and Leukemia Group B (CALGB) randomized trials of adjuvant chemotherapy were retrospectively analyzed, but the number of patients aged 70 years was only 159 [54]. Although the older patients obtained the same benefits as younger patients with more effective regimens, two constraints must be stressed: the limited number of patients aged 70 years and a possible selection bias, with only healthy and higher-risk older patients being offered the option of participating in clinical trials. The results of several ongoing randomized trials are, therefore, eagerly awaited. Figure 2 summarizes the guidelines for adjuvant CT in stage I BC from the NIH Consensus Conference [5, 55] and the St. Gallen Consensus [7]. Which Regimen Should Be Used? CMF The CMF regimen proposed by Bonadonna has been widely tested, and its long-term benefits in improving DFS The Oncologist
7 Colozza, Azambuja, Cardoso et al. 117 and OS were confirmed after 30 years of follow-up [56]. This regimen is still used in the adjuvant setting, particularly in N-negative women and in cases of anthracycline contraindications. Anthracycline-Based Regimens A decade of clinical research has been necessary to firmly establish the superiority of anthracycline-based regimens (CAF [cyclophosphamide, doxorubicin, fluorouracil], CEF [cyclophosphamide, epirubicin, fluorouracil] or A/E [doxorubicin, epirubicin] CMF) over classic CMF or CMF-like regimens. Randomized adjuvant trials have generated conflicting results [57 62]. This can be explained by the number of patients enrolled and their selection, the different anthracycline-based and CMF-like regimens, and different doses of drugs in similar regimens. The EBCTCG meta-analysis shows that the benefits of adjuvant anthracyclines are persistent for 15 years, with a 26% reduction in BC death in young patients [2, 4]. The optimal anthracycline-based regimen, however, is still a matter of controversy. In Europe and Canada, a three-drug regimen is usually preferred (CAF/CEF, FAC/FEC, A/E CMF), especially for N-positive patients. In fact, no direct comparison between the two-drug doxorubicin cyclophosphamide (AC) regimen and the three-drug regimens has been conducted. However, both four cycles of AC [63, 64] and eight cycles of epirubicin cyclophosphamide (EC) [65] in quite large randomized trials have failed to demonstrate superiority to CMF. Another controversial issue is the optimal dose of anthracyclines, since a doseresponse relationship exists for both doxorubicin and epirubicin. There is a threshold dose above which no advantage in efficacy, but an increase in toxicity, has been reported, and a dose below which the efficacy is greatly reduced. This dose could be 60 mg/m 2 for doxorubicin, at least in the AC regimen [66], and mg/m 2 for epirubicin [60, 65, 67]. According to the EBCTCG meta-analysis, the optimal duration of adjuvant CT is 4 6 months [2]. The advantages of anthracycline-based CT must be carefully balanced against potential risks, particularly in the adjuvant setting [68]. Anthracycline-based CT toxicity depends on the administered dose (dose intensity and cumulative dose) as well as on the type of anthracycline used [69]. The most common acute hematological and nonhematological toxicities are reversible, and usually manageable. Of greater concern are two possible long-term toxicities: cardiac heart failure and secondary leukemia, although the incidence of both is quite low (~1%) [70, 71]. Furthermore, in premenopausal patients, a possible long-term sequela of CT is early menopause, with its accompanying symptoms and, consequently, greater risk for coronary heart disease and osteoporosis. The impact of these factors on overall mortality is minimal, but since they may significantly impair long-term quality of life, they must be taken into consideration. Taxane-Based Regimens In an attempt to further improve the survival benefit obtained with adjuvant CT, regimens containing taxanes have been investigated in several adjuvant trials. More than 30,000 women have been enrolled in studies comparing taxane- and anthracycline-based regimens, administered either concurrently or sequentially, with standard anthracycline-based regimens (first generation trials). Data are now available from five of these randomized trials [66, 72 77]. A second generation of taxane trials evaluating the best way to administer these drugs will enroll about 25,000 women. First Generation Trials Figure 2. Guideline recommendations for chemotherapy for stage I breast cancer patients according to National Cancer Institute (NCI), National Comprehensive Cancer Network (NCCN), and St. Gallen Consensus. Abbreviation: ER, estrogen receptor negative; ER +, estrogen receptor positive; T, tumor. Sequential anthracycline-taxane regimens Two large trials (more than 3,000 women in each) compared four cycles of paclitaxel (Taxol ; Bristol-Myers Squibb, Princeton, NJ) with no further treatment after four cycles of AC in N-positive BC patients [66, 76]. The CALGB 9344 trial, which also evaluated three different doses of doxoru-
8 118 Achievements in Early Breast Cancer bicin, showed a significant benefit in DFS and OS with the addition of paclitaxel [66, 78]. These results were confirmed at a longer follow-up (69 months) [66]. In an unplanned subset analysis, the advantage of adding paclitaxel to AC was limited to patients with ER-negative tumors who did not receive tamoxifen at the end of CT. In the National Surgical Adjuvant Breast and Bowel Project (NSABP) B28 trial, a higher dose of paclitaxel was given, and tamoxifen was administered concomitantly with CT. At a similar median follow-up, a significantly longer DFS time (RR, 0.83; 95% CI, ; p =.006) was reported in all subgroups of patients, but no difference in OS was found (RR, 0.93; 95% CI, ; p =.46). Toxicity with the addition of paclitaxel was considered acceptable [72, 76]. Both studies, however, have been criticized because the control arm was considered to be suboptimal. Another smaller randomized trial compared eight cycles of FAC with four cycles of paclitaxel followed by four cycles of FAC. The preliminary results suggest a lower risk of disease recurrence with the addition of paclitaxel to FAC, but the difference did not reach statistical significance [73]. Recently, the results of a French study have shown statistically significant longer DFS and OS times with the sequence of three courses of FEC followed by three courses of docetaxel (Taxotere ; Aventis Pharmaceuticals Inc., Bridgewater, NJ), in comparison with six courses of FEC. In a subgroup analysis, however, this advantage appeared to be limited to those patients with one to three positive nodes and to older women ( 50 years) [75]. Combined anthracycline taxane regimens The docetaxel, doxorubicin, cyclophosphamide (TAC) regimen was compared with FAC in N-positive patients [74, 77] and resulted in significantly lower risks for relapse and death. In a subgroup analysis, this benefit was independent of HR and HER-2 status but was confined to patients with one, two, or three positive nodes. Furthermore, there was a difference in the incidence of CT-induced amenorrhea between the two arms that could be a confounding factor for the larger population of endocrine-responsive patients [68]. Because of the significantly higher incidence of febrile neutropenia in the TAC arm, the use of prophylactic G-CSF is recommended with this regimen. The control arm of that study has also been criticized because the dose of doxorubicin is below the threshold. Recently presented at the 2005 Annual Meeting of the American Society of Clinical Oncology, the E2197 trial compares doxorubicin docetaxel (AT) (60 mg/m 2 for both drugs) with AC (60 mg/m 2 and 600 mg/m 2 ) every 3 weeks for four cycles. At a median follow-up of 59 months, no differences in either the DFS (87% in both arms; p =.7) or OS (94% vs. 93%; p =.49) rate were observed. More febrile neutropenia was seen in the AT arm than in the AC arm (28% vs. 10%, respectively) [79]. The Reposnant sur des Arguments Pronostiques et Prédictifs (RAPP-01) trial, which compared AT (60 mg/ m 2 and 75 mg/m 2 ) with AC (60 mg/m 2 and 600 mg/m 2 ), was prematurely closed because of a higher incidence of febrile neutropenia, with three deaths in the AT arm (40.8% vs. 7.1%, respectively; p <.001). A high risk for life-threatening complications associated with the AT regimen was found in this open-label controlled trial. However, the AT arm used a higher dose of docetaxel (75 mg/m 2 ) than in the E2197 trial [80]. Paclitaxel has been approved in the U.S. for the treatment of N-positive BC patients, and the AC regimen followed by paclitaxel is now the reference regimen in a majority of clinical trials for N-positive patients in the U.S.; in Europe, both the AC regimen followed by paclitaxel and the TAC regimen have recently been approved. Nevertheless, the role of taxanes in early BC remains controversial because of the suboptimal control arm used in three trials [66, 76, 77]. Issues such as septic deaths, typhlitis, neurotoxicity, cardiotoxicity, acute leukemia, and cognitive dysfunction need to be watched very closely. Additionally, there are still unanswered questions regarding the best taxane, the optimal schedule and dosing, and the real benefit of a taxane-containing regimen for the subset of patients with ER-positive tumors [81]. Notwithstanding these issues, the advantage in OS obtained in three trials [66, 75, 77] and in another dose-dense trial [82] cannot be ignored, and the prescription of taxane-based regimens to N-positive patients is a commendable option (Fig. 3). Dose-Dense Adjuvant Chemotherapy The rationale to use dose-dense rather than conventionally timed CT for the treatment of BC relies on the Skipper concept of tumor growth [83] and the Gompertzian model of growth exhibited by human solid tumors [84]. In preclinical studies, a simple manipulation, for example, giving high drug doses with shorter intervals between treatments, has shown considerably greater efficacy than conventionally timed CT by minimizing the regrowth of cancer cells between treatment cycles [85 87]. This concept was extended to encompass situations of heterogeneous drug sensitivity through the use of sequential dose-dense regimens [88 91]. A randomized adjuvant trial has tested these two mathematical concepts in N-positive BC patients using a 2 2 factorial design [82]. The same drugs (doxorubicin, cyclophosphamide, and paclitaxel) at identical doses per cycle, given according to two different schedules (con- The Oncologist
9 Colozza, Azambuja, Cardoso et al. 119 Figure 3. Trials using taxanes in adjuvant chemotherapy for patients with node-positive breast cancer. Abbreviations: AC, doxorubicin and cyclophosphamide; AT, doxorubicin and docetaxel; BCIRG, Breast Cancer International Research Group; CALGB, Cancer and Leukemia Group B; FAC, 5-fluorouracil, doxorubicin, and cyclophosphamide; FEC, 5-fluorouracil, epirubicin, and cyclophosphamide; MDACC, MD Anderson Cancer Center; NSABP, National Surgical Adjuvant Breast and Bowel Project; P, paclitaxel; PACS, Protocol Adjuvant dans le Cancer du Sein; T, docetaxel; TAC, docetaxel, doxorubicin, and cyclophosphamide. *Both trials enrolled node-positive and node-negative breast cancer patients. current or sequential) and two different treatment cycle intervals (every 3 weeks or every 2 weeks with G-CSF support), were compared. At a relatively short median follow-up (36 months), the dose-dense regimen resulted in longer DFS and OS times, while no difference in outcome was observed between the concurrent and sequential schedules. So far, no toxic deaths and no higher incidence of cardiotoxicity or secondary leukemia in the dose-dense arms have been seen. A retrospective analysis has shown that the benefits obtained with the dosedense regimen are limited to the subgroup of ER-positive patients [81]. That trial, however, was not powered for individual comparisons among the four treatment arms, and it remains to be determined whether the dose densification is necessary for all the drugs used. A two-arm European trial using the same drugs in N-positive ( 4) BC patients has reported, at a relatively short follow-up (28 months), similar results [92]. On the contrary, another adjuvant trial enrolling high-risk N-negative and N-positive BC patients has not found significant differences between standard FE(60)C and accelerated FEC with the support of G-CSF at a median follow-up of 6 years [93]. However, in an unplanned subgroup analysis, a longer OS time favoring the dose-dense arm was reported in younger patients (<50 years). The weaknesses of that study are its relatively small size and the suboptimal dose of epirubicin [65, 67]. Given the incremental costs associated with the dose-dense strategy, other confirmatory trials are necessary before its introduction in current clinical practice is warranted. Is HR Status a Potential Discriminator of CT Efficacy? Recently, the concept that HR-negative tumors are more responsive to CT has been reinforced, mainly from retrospective analyses. In the NSABP B-20 trial, a greater benefit from the addition of CT to tamoxifen in N-negative, ER-positive patients was observed in those with lower ER concentrations [94]. Similar results were reported in an exploratory analysis of biomarkers in a subgroup of postmenopausal N-positive, ER-positive patients enrolled in the U.S. Intergroup trial INT 100 and randomized to CT (CAF) or CT plus tamoxifen [95]. The effect of CT according to ER status was also reviewed in three successive CALGB CT trials, the first evaluating three different CAF regimens, the second evaluating the addition of paclitaxel to the AC regimen, and the third evaluating the efficacy of dose- regimens in comparison with standard CT [66, 81, 82, 96]. In all three trials, the overall differences in outcomes were almost exclusively limited to ER-negative patients. A refined analysis of the data from the EBCTCG metaanalysis further supports these observations and, in its last update, the 5-year gains from CT would be about twice as large for ER-poor disease as they are for tamoxifen-treated ER-positive disease [4, 97]. Chemoendocrine Therapy The combination of CT and ET is empirically based on the assumption that each modality exerts its effect on different tumor cells, according to endocrine responsiveness, and that the toxicities are diverse. There are theoretical argu-
10 120 Achievements in Early Breast Cancer ments suggesting that the simultaneous administration of these two therapies may not be optimal, because an interaction between the different mechanisms of action may occur. Preclinical data have demonstrated that ET slows tumor growth, which may make tumor cells less susceptible to cell cycle-specific cytotoxic agents [98]. The combination treatment has also been associated with a higher risk for thromboembolic events [99]. Furthermore, tamoxifen may alter membrane lipids, thereby changing diffusion rates of some drugs; it also seems to antagonize both the calmodulin and Ca 2+ channels, potentially modifying drug uptake [100]. On the other hand, tamoxifen demonstrated an additive effect when it was combined with doxorubicin and cyclophosphamide in vitro [101]. The EBCTCG meta-analysis [2] and several adjuvant trials have shown that the combination of CT and ET significantly increases the benefits to patients in terms of DFS and OS obtained with either modality alone for endocrineresponsive tumors. This advantage has been observed in N-positive patients with CMF-containing regimens [102] as well as anthracycline-based regimens [64, ]. With N-negative patients, contrasting results have been reported in two large randomized trials enrolling different patient populations according to menopausal and HR status [107, 108]. The best modality of administration was evaluated in postmenopausal N-positive patients with ER-positive tumors randomized to receive either tamoxifen alone or chemotherapy (CAF) plus tamoxifen given concomitantly or sequentially. At a median follow-up of 10 years, there was a statistically significant longer DFS time for patients receiving CT and tamoxifen sequentially [95]. A trend favoring the sequential addition of tamoxifen to EC was obtained at a shorter follow-up time in a small trial with a similar design that included N-positive postmenopausal patients not selected for HR status [109]. Biological Therapy Trastuzumab Clinical Trials The exciting results obtained with the use of trastuzumab (Herceptin ; Genentech, Inc., South San Francisco, CA) in metastatic BC (MBC) patients whose tumors displayed overexpression and/or amplification of HER-2 has led to a new generation of adjuvant trials in this subset of patients. In an attempt to reduce the risk for cardiotoxicity, sequential anthracycline- and taxane-based regimens, with trastuzumab starting concomitantly or after the taxanes and given for 1 year, have been chosen for three trials (North Central Cancer Treatment Group [NCCTG] N9831, NSABP B31, and Breast Cancer International Research Group [BCIRG] 006). One of these trials, BCIRG 006, also includes a third arm, in which trastuzumab is administered upfront in combination with a regimen containing carboplatin (Paraplatin ; Bristol-Myers Squibb) and docetaxel. The fourth trial, the HERceptin Adjuvant (HERA) study, explored the benefit of trastuzumab given at the completion of locoregional therapy and adjuvant CT, and enrolled patients regardless of the type of adjuvant CT administered. That trial also evaluated different durations of trastuzumab administration (1 or 2 years) and used a 3-weekly schedule that is considered as effective as the weekly schedule in MBC [110, 111]. All trials are represented in Figure 4. The results of three of these trials were recently published. The largest trial, HERA, enrolled 5,090 patients from December 2001 to April 2005, and patients were randomized between observation, and 1 or 2 years of adjuvant 3-weekly trastuzumab after completion of CT. In the first and only interim analysis, patients in the 1- year arm had a 46% lower risk for relapse (DFS, 85.8% vs. 77.4%; hazard ratio, 0.54; p <.0001) than patients in the observation arm [112]. Similar results were obtained in a pooled analysis of two U.S. trials (NSABP B31 and NCCTG N9831) comparing four cycles of AC followed by four cycles of paclitaxel with or without weekly trastuzumab in 3,351 HER-2 positive patients. At a median follow-up of 2 years, statistically significant greater DFS (87% vs. 75%; hazard ratio, 0.48; p = ) and OS (91% vs. 78%; hazard ratio, 0.67; p =.015) rates in favor of trastuzumab were observed [113]. The efficacy results of both trials are presented in Table 4, and a summary of cardiac toxicity is presented in Table 5. The NCCTG N9831 is a three-arm trial comparing two different modalities of trastuzumab administration (concomitant with paclitaxel or sequential to paclitaxel) with a control arm. In the joint analysis, the concurrent administration of paclitaxel and trastuzumab was compared with the control arm, but in an unplanned interim analysis, the concurrent administration of trastuzumab and paclitaxel resulted in a longer DFS time in comparison with the sequential one [114] Despite the exciting results obtained with adjuvant trastuzumab, there are still several unresolved issues such as the best modality of trastuzumab administration, the duration, the long-term efficacy, and the toxicity. Conclusions and Future Perspectives The achievements of the so-called pregenomic era have been quite substantial and have led to a long-expected decrease in BC mortality, despite its increased incidence. Large randomized trials and meta-analyses have been instrumental in showing small, but consistent and additive, improvements in DFS and OS. The Oncologist
11 Colozza, Azambuja, Cardoso et al. 121 Figure 4. Overview of adjuvant trials with trastuzumab in patients with HER-2 overexpressing and/or amplified breast cancers. The Breast Cancer International Research Group (BCIRG) trial enrolled only patients that were HER-2 positive by fluorescence in situ hybridization (FISH). Abbreviations: AC, doxorubicin and cyclophosphamide; HERA, HERceptin Adjuvant; IHC, immunohistochemistry; NCCTG, North Central Cancer Treatment Group; NSABP, National Surgical Adjuvant Breast and Bowel Project; T: paclitaxel Table 4. Summary of results showing the efficacy of adjuvant trastuzumab in early breast cancer patients North American trials [113] HERA trial [112] HR p value Absolute gain at 4 years HR p value Absolute gain at 2 years DFS p = % 0.54 < % TTDR or DDFS p = % 0.51 < % OS p =.015 4% % Abbreviations: DDFS, distant disease-free survival; DFS, disease-free survival; HERA, HERceptin Adjuvant; HR, hazard ratio; OS, overall survival; TTDR, time to distant relapse. Table 5. Summary of cardiac toxicity in randomized trials with adjuvant trastuzumab in early breast cancer patients NSABP B31 [113] N 9831 [114] HERA [112] AC T AC TH AC T AC TH AC T H Obs 1 year H CHF NYHA class 3 4 Cumulative incidence at 3 years (3.3%) 12 (2.2%) 0 9 (0.5%) 0.6% 4% NA NA NA NA NA Cardiac deaths 1 0 NA NA NA 1 0 Abbreviations: AC, doxorubicin and cyclophosphamide; CHF NYHA class 3 4, congestive heart failure New York Heart Association class 3 4; H, trastuzumab; HERA, HERceptin Adjuvant; NSABP, National Surgical Adjuvant Breast and Bowel Project; NA, not available; Obs, observation arm; T, paclitaxel; TH, paclitaxel and trastuzumab. In ET, tamoxifen, the gold standard for decades, has been one of the most impressive lifesaving drugs in oncology. Third generation AIs have the potential to further enhance these benefits. CT regimens, namely CMF-like, anthracycline-based, and, more recently, anthracyclineand taxane-based regimens, have led to significantly longer DFS and OS times for almost all BC patients, particularly those with endocrine-nonresponsive disease. The discovery and clinical application of targeted drugs, of which trastuzumab is the paradigm, represent another important strategy in the fight against the disease. The lessons learned from this era, and the hypotheses generated by those trials, have set the stage for the central role that translational research needs to take in the coming years. With new technologies (i.e., genomics and proteinomics), intelligent use of research opportuni-
12 122 Achievements in Early Breast Cancer ties in the neoadjuvant setting, and new biological drugs, this type of research will certainly lead to even greater achievements in the management of early BC. More specifically, it will lead to the improved individualization of adjuvant treatment. Disclosure of Potential Conflicts of Interest Martine Piccart has acted as a consultant for sanofi-aventis, Bristol-Myers Squibb, GlaxoSmithKline, Johnson and Johnson, Novartis, Pfizer, and AstraZeneca. References 1 Early Breast Cancer Trialists Collaborative Group. Ovarian ablation in early breast cancer: overview of the randomised trials. Lancet 1996;348: Early Breast Cancer Trialists Collaborative Group. Polychemotherapy for early breast cancer: an overview of the randomised trials. Lancet 1998;352: Early Breast Cancer Trialists Collaborative Group. Tamoxifen for early breast cancer: an overview of the randomised trials. Lancet 1998;351: Early Breast Cancer Trialists Collaborative Group. Effects of chemotherapy and hormonal therapy for early breast cancer on recurrence and 15-year survival: an overview of the randomised trials. Lancet 2005;365: The National Institutes of Health Consensus Development Conference: Adjuvant Therapy for Breast Cancer. Bethesda, Maryland, USA. November 1-3, Proceedings. J Natl Cancer Inst Monogr 2001;(30): Goldhirsch A, Glick JH, Gelber RD et al. Meeting highlights: International Consensus Panel on the Treatment of Primary Breast Cancer. Seventh International Conference on Adjuvant Therapy of Primary Breast Cancer. J Clin Oncol 2001;19: Goldhirsch A, Wood WC, Gelber RD et al. Meeting highlights: updated international expert consensus on the primary therapy of early breast cancer. J Clin Oncol 2003;21: Carlson RW, Anderson BO, Bensinger W et al. NCCN Practice Guidelines for Breast Cancer. Oncology (Williston Park) 2000;14: Davidson NE, Levine M. Breast cancer consensus meetings: vive la difference? J Clin Oncol 2002;20: Baum M, Ravdin PM. Decision-making in early breast cancer: guidelines and decision tools. Eur J Cancer 2002;38: Goldhirsch A, Glick JH, Gelber RD et al. Meeting highlights: international expert consensus on the primary therapy of early breast cancer Ann Oncol 2005;16: Fisher B, Dignam J, Bryant J et al. Five versus more than five years of tamoxifen for lymph node-negative breast cancer: updated findings from the National Surgical Adjuvant Breast and Bowel Project B-14 randomized trial. J Natl Cancer Inst 2001;93: Stewart HJ, Prescott RJ, Forrest AP. Scottish adjuvant tamoxifen trial: a randomized study updated to 15 years. J Natl Cancer Inst 2001;93: Bryant J, Fisher B, Dignam J. Duration of adjuvant tamoxifen therapy. J Natl Cancer Inst Monogr 2001;(30): ATLAS. Adjuvant Tamoxifen Longer Against Shorter. Available at Accessed August 29, Chang J, Powles TJ, Ashley SE et al. The effect of tamoxifen and hormone replacement therapy on serum cholesterol, bone mineral density and coagulation factors in healthy postmenopausal women participating in a randomised, controlled tamoxifen prevention study. Ann Oncol 1996;7: Powles TJ, Hickish T, Kanis JA et al. Tamoxifen preserves bone mineral density in postmenopausal women but causes loss of bone density in premenopausal women. Proc Am Soc Clin Oncol 1995;14: Love RR, Mazess RB, Barden HS et al. Effects of tamoxifen on bone mineral density in postmenopausal women with breast cancer. N Engl J Med 1992;326: Love RR, Barden HS, Mazess RB et al. Effect of tamoxifen on lumbar spine bone mineral density in postmenopausal women after 5 years. Arch Intern Med 1994;154: Jaiyesimi IA, Buzdar AU, Decker DA et al. Use of tamoxifen for breast cancer: twenty-eight years later. J Clin Oncol 1995;13: Bertelli G, Pronzato P, Amoroso D et al. Adjuvant tamoxifen in primary breast cancer: influence on plasma lipids and antithrombin III levels. Breast Cancer Res Treat 1988;12: Baum M, Budzar AU, Cuzick J et al. Anastrozole alone or in combination with tamoxifen versus tamoxifen alone for adjuvant treatment of postmenopausal women with early breast cancer: first results of the ATAC randomised trial. Lancet 2002;359: Baum M, Buzdar A, Cuzick J et al. Anastrozole alone or in combination with tamoxifen versus tamoxifen alone for adjuvant treatment of postmenopausal women with early-stage breast cancer: results of the ATAC (Arimidex, Tamoxifen Alone or in Combination) trial efficacy and safety update analyses. Cancer 2003;98: Dowsett M. Analysis of time to recurrence in the ATAC (arimidex, tamoxifen, alone or in combination) trial according to estrogen receptor and progesterone receptor status. Breast Cancer Res Treat 2003;83:S2. 25 Howell A, Cuzick J, Baum M et al. Results of the ATAC (Arimidex, Tamoxifen, Alone or in Combination) trial after completion of 5 yearsʼ adjuvant treatment for breast cancer. Lancet 2005;365: Thurlimann B. Keshaviah A, Coates AS et al. A comparison of letrozole and tamoxifen in postmenopausal women with early breast cancer. N Eng J Med 2005;353: Thurlimann B, Keshaviah A, Mouridsen HT et al. BIG 1-98: randomized double-blind phase III study to evaluate letrozole (L) vs. tamoxifen (T) as adjuvant endocrine therapy for postmenopausal women with receptorpositive breast cancer. J Clin Oncol 2005;23:6S. 28 Goss PE, Ingle JN, Martino S et al. A randomized trial of letrozole in postmenopausal women after five years of tamoxifen therapy for early-stage breast cancer. N Engl J Med 2003;349: Goss PE, Ingle JN, Martino S et al. Randomized trial of letrozole following tamoxifen as extended adjuvant therapy in receptor-positive breast cancer: updated findings from NCIC CTG MA.17. J Natl Cancer Inst 2005;97: Wasan KM, Goss PE, Pritchard PH et al. The influence of letrozole on serum lipid concentrations in postmenopausal women with primary breast cancer who have completed 5 years of adjuvant tamoxifen (NCIC CTG MA.17L). Ann Oncol 2005;16: Coombes RC, Hall E, Gibson LJ et al. A randomized trial of exemestane after two to three years of tamoxifen therapy in postmenopausal women with primary breast cancer. N Engl J Med 2004;350: The Oncologist
Key Words. Adjuvant therapy Breast cancer Taxanes Anthracyclines
 The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
HORMONAL THERAPY IN ADJUVANT CARE
 ADVANCES IN ENDOCRINE THERAPY FOR BREAST CANCER* Matthew J. Ellis, MD, PhD ABSTRACT Endocrine therapy is used frequently in breast cancer management, particularly in the setting of adjuvant care, but outstanding
ADVANCES IN ENDOCRINE THERAPY FOR BREAST CANCER* Matthew J. Ellis, MD, PhD ABSTRACT Endocrine therapy is used frequently in breast cancer management, particularly in the setting of adjuvant care, but outstanding
Breast Cancer. Controversies in the Therapy of Early Stage Breast Cancer. The Oncologist 2005;10:
 This material is protected by U.S. Copyright law. Unauthorized reproduction is prohibited. For reprints contact: Reprints@AlphaMedPress.com Breast Cancer Controversies in the Therapy of Early Stage Breast
This material is protected by U.S. Copyright law. Unauthorized reproduction is prohibited. For reprints contact: Reprints@AlphaMedPress.com Breast Cancer Controversies in the Therapy of Early Stage Breast
Extended Adjuvant Endocrine Therapy
 Extended Adjuvant Endocrine Therapy After all, 5 years Tamoxifen works.. For women with ER+ primary breast cancer, previous studies have shown that treatment with tamoxifen for 5 years has a carry-over
Extended Adjuvant Endocrine Therapy After all, 5 years Tamoxifen works.. For women with ER+ primary breast cancer, previous studies have shown that treatment with tamoxifen for 5 years has a carry-over
Adjuvant treatment for early breast cancer
 Annals of Oncology 16 (Supplement 2): ii182 ii187, 2005 doi:10.1093/annonc/mdi709 Adjuvant treatment for early breast cancer I. Smith The Royal Marsden Hospital, London, UK Introduction Survival rates
Annals of Oncology 16 (Supplement 2): ii182 ii187, 2005 doi:10.1093/annonc/mdi709 Adjuvant treatment for early breast cancer I. Smith The Royal Marsden Hospital, London, UK Introduction Survival rates
Extended Hormonal Therapy
 Extended Hormonal Therapy Dr. Caroline Lohrisch, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Optimal Endocrine Therapy for Women with Hormone Receptor Positive Early
Extended Hormonal Therapy Dr. Caroline Lohrisch, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Optimal Endocrine Therapy for Women with Hormone Receptor Positive Early
OPTIMAL ENDOCRINE THERAPY IN EARLY BREAST CANCER
 OPTIMAL ENDOCRINE THERAPY IN EARLY BREAST CANCER STEPHEN E. JONES, M.D. US ONCOLOGY RESEARCH THE WOODLANDS, TX TOPICS PREMENOPAUSAL BREAST CANCER POSTMENOPAUSAL BREAST CANCER THE FUTURE TOPICS PREMENOPAUSAL
OPTIMAL ENDOCRINE THERAPY IN EARLY BREAST CANCER STEPHEN E. JONES, M.D. US ONCOLOGY RESEARCH THE WOODLANDS, TX TOPICS PREMENOPAUSAL BREAST CANCER POSTMENOPAUSAL BREAST CANCER THE FUTURE TOPICS PREMENOPAUSAL
Choosing between different hormonal therapies. Rudy Van den Broecke UZ Ghent
 Choosing between different hormonal therapies Rudy Van den Broecke UZ Ghent What is the golden standard in premenopausal hormonal sensitive early breast cancer? Ovarian Suppression alone 5 years Tamoxifen
Choosing between different hormonal therapies Rudy Van den Broecke UZ Ghent What is the golden standard in premenopausal hormonal sensitive early breast cancer? Ovarian Suppression alone 5 years Tamoxifen
William J. Gradishar MD
 Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2013 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2013 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
Best of San Antonio 2008
 Best of San Antonio 2008 Ellie Guardino, MD/PhD Assistant Professor Stanford University BIG 1 98: a randomized double blind phase III study evaluating letrozole and tamoxifen given in sequence as adjuvant
Best of San Antonio 2008 Ellie Guardino, MD/PhD Assistant Professor Stanford University BIG 1 98: a randomized double blind phase III study evaluating letrozole and tamoxifen given in sequence as adjuvant
Should premenopausal HR+ve breast cancer receive LHRH?
 Should premenopausal HR+ve breast cancer receive LHRH? Hesham Elghazaly, MD Prof. Clinical Oncology, Ain Shams University President of the BGICS Should premenopausal HR+ve breast cancer receive LHRH? NO?
Should premenopausal HR+ve breast cancer receive LHRH? Hesham Elghazaly, MD Prof. Clinical Oncology, Ain Shams University President of the BGICS Should premenopausal HR+ve breast cancer receive LHRH? NO?
Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer
 Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer Angelo Di Leo «Sandro Pitigliani» Medical Oncology Unit Hospital of Prato Istituto Toscano Tumori Prato, Italy NOAH: Phase III, Open-Label Trial
Neo-adjuvant and adjuvant treatment for HER-2+ breast cancer Angelo Di Leo «Sandro Pitigliani» Medical Oncology Unit Hospital of Prato Istituto Toscano Tumori Prato, Italy NOAH: Phase III, Open-Label Trial
Nadia Harbeck Breast Center University of Cologne, Germany
 Evidence in Favor of Taxane Based Combinations and No Anthracycline in Adjuvant and Metastatic Settings Nadia Harbeck Breast Center University of Cologne, Germany Evidence in Favor of Taxane Based Combinations
Evidence in Favor of Taxane Based Combinations and No Anthracycline in Adjuvant and Metastatic Settings Nadia Harbeck Breast Center University of Cologne, Germany Evidence in Favor of Taxane Based Combinations
ORMONOTERAPIA ADIUVANTE: QUALE LA DURATA OTTIMALE? MARIANTONIETTA COLOZZA
 ORMONOTERAPIA ADIUVANTE: QUALE LA DURATA OTTIMALE? MARIANTONIETTA COLOZZA THE NATURAL HISTORY OF HORMONE RECEPTOR- POSITIVE BREAST CANCER IS VERY LONG Recurrence hazard rate 0.3 0.2 0.1 0 ER+ (n=2,257)
ORMONOTERAPIA ADIUVANTE: QUALE LA DURATA OTTIMALE? MARIANTONIETTA COLOZZA THE NATURAL HISTORY OF HORMONE RECEPTOR- POSITIVE BREAST CANCER IS VERY LONG Recurrence hazard rate 0.3 0.2 0.1 0 ER+ (n=2,257)
Adjuvant Endocrine Therapy: How Long is Long Enough?
 Adjuvant Endocrine Therapy: How Long is Long Enough? Harold J. Burstein, MD, PhD Dana-Farber Cancer Institute Harvard Medical School Boston, Massachusetts hburstein@partners.org I have no conflicts to
Adjuvant Endocrine Therapy: How Long is Long Enough? Harold J. Burstein, MD, PhD Dana-Farber Cancer Institute Harvard Medical School Boston, Massachusetts hburstein@partners.org I have no conflicts to
Recent advances in adjuvant systemic treatment for breast cancer: all systems go!
 REVIEW ARTICLE Recent advances in adjuvant systemic treatment for breast cancer: all systems go! P.N. Fishman MD* and S. Verma MD MSEd* KEY WORDS Breast cancer, adjuvant, treatment 1. INTRODUCTION Breast
REVIEW ARTICLE Recent advances in adjuvant systemic treatment for breast cancer: all systems go! P.N. Fishman MD* and S. Verma MD MSEd* KEY WORDS Breast cancer, adjuvant, treatment 1. INTRODUCTION Breast
Adjuvant Systemic Therapy in Early Stage Breast Cancer
 Adjuvant Systemic Therapy in Early Stage Breast Cancer Julie R. Gralow, M.D. Director, Breast Medical Oncology Jill Bennett Endowed Professor of Breast Cancer Professor, Global Health University of Washington
Adjuvant Systemic Therapy in Early Stage Breast Cancer Julie R. Gralow, M.D. Director, Breast Medical Oncology Jill Bennett Endowed Professor of Breast Cancer Professor, Global Health University of Washington
Considerations in Adjuvant Chemotherapy. Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology
 Considerations in Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic Treatment
Considerations in Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic Treatment
 Mdi Medical Management of Breast Cancer Morbidity and Mortality Aug 13, 2009 Irina Kovatch, PGY3 Introduction Metastatic disease is the principal cause of death from breast cancer Metastatic events often
Mdi Medical Management of Breast Cancer Morbidity and Mortality Aug 13, 2009 Irina Kovatch, PGY3 Introduction Metastatic disease is the principal cause of death from breast cancer Metastatic events often
TRANSPARENCY COMMITTEE OPINION. 15 February 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 February 2006 Taxotere 20 mg, concentrate and solvent for solution for infusion B/1 vial of Taxotere and 1 vial
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 February 2006 Taxotere 20 mg, concentrate and solvent for solution for infusion B/1 vial of Taxotere and 1 vial
Evolving Insights into Adjuvant Chemotherapy. Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology
 Evolving Insights into Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic
Evolving Insights into Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology 80 70 60 50 40 30 20 10 0 EBCTCG 2005/6 Overview Control Arms with No Systemic
Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA
 Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA The fascinating history of Herceptin 1981 1985 1987 1990 1992 1998 2000 2005 2006 2008 2011 Murine
Sustained benefits for women with HER2-positive early breast cancer JORGE MADRID BIG GOCCHI PROTOCOLO HERA The fascinating history of Herceptin 1981 1985 1987 1990 1992 1998 2000 2005 2006 2008 2011 Murine
Treatment of HER-2 positive breast cancer
 EJC SUPPLEMENTS 6 (2008) 21 25 available at www.sciencedirect.com journal homepage: www.ejconline.com Treatment of HER-2 positive breast cancer Matteo Clavarezza, Marco Venturini * Ospedale Sacro Cuore
EJC SUPPLEMENTS 6 (2008) 21 25 available at www.sciencedirect.com journal homepage: www.ejconline.com Treatment of HER-2 positive breast cancer Matteo Clavarezza, Marco Venturini * Ospedale Sacro Cuore
Endocrine Therapy in Premenopausal Breast Cancer. Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology, PA US Oncology
 Endocrine Therapy in Premenopausal Breast Cancer Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology, PA US Oncology Ovarian Ablation or Suppression vs. Not in ER + or ER UK Breast Cancer
Endocrine Therapy in Premenopausal Breast Cancer Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology, PA US Oncology Ovarian Ablation or Suppression vs. Not in ER + or ER UK Breast Cancer
Breast Cancer? Breast cancer is the most common. What s New in. Janet s Case
 Focus on CME at The University of Calgary What s New in Breast Cancer? Theresa Trotter, MD, FRCPC Breast cancer is the most common malignancy affecting women in Canada, accounting for almost a third of
Focus on CME at The University of Calgary What s New in Breast Cancer? Theresa Trotter, MD, FRCPC Breast cancer is the most common malignancy affecting women in Canada, accounting for almost a third of
A review of adjuvant hormonal therapy in
 REVIEW Endocrine-Related Cancer (2004) 11 391 406 A review of adjuvant hormonal therapy in breast cancer Kellie L Jones and Aman U Buzdar 1 Department of Pharmacy, University of Texas M.D. Anderson Cancer
REVIEW Endocrine-Related Cancer (2004) 11 391 406 A review of adjuvant hormonal therapy in breast cancer Kellie L Jones and Aman U Buzdar 1 Department of Pharmacy, University of Texas M.D. Anderson Cancer
Update from the 25th Annual San Antonio Breast Cancer Symposium December 11 14, 2002
 Update from the 25th Annual San Antonio Breast Cancer Symposium December 11 14, 2002 Nearly 5,000 physicians, oncologists, radiologists, epidemiologists, basic scientists, and breast cancer advocates from
Update from the 25th Annual San Antonio Breast Cancer Symposium December 11 14, 2002 Nearly 5,000 physicians, oncologists, radiologists, epidemiologists, basic scientists, and breast cancer advocates from
Breast cancer has the highest incidence among those
 Medical Treatment of Breast Cancer Young Seon Hong, M.D. Department of Internal Medicine Catholic University of Korea, St. Mary's Hospital E mail : y331@cmc.cuk.ac.kr Abstract Breast cancer has the highest
Medical Treatment of Breast Cancer Young Seon Hong, M.D. Department of Internal Medicine Catholic University of Korea, St. Mary's Hospital E mail : y331@cmc.cuk.ac.kr Abstract Breast cancer has the highest
Adjuvant Chemotherapy + Trastuzumab
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Chemotherapy + Trastuzumab (Optimal Drugs / Dosage / Trastuzumab) Adjuvant Chemotherapy (Optimal Drugs / Optimal Dosage
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Chemotherapy + Trastuzumab (Optimal Drugs / Dosage / Trastuzumab) Adjuvant Chemotherapy (Optimal Drugs / Optimal Dosage
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
JOURNAL OF CLINICAL ONCOLOGY R E V I E W A R T I C L E
 NUMBER MARCH VOLUME 23 d 8 d 10 2005 JOURNAL OF CLINICAL ONCOLOGY R E V I E W A R T I C L E Adjuvant Endocrine Therapy for Premenopausal Women With Early Breast Cancer Silvia Dellapasqua, Marco Colleoni,
NUMBER MARCH VOLUME 23 d 8 d 10 2005 JOURNAL OF CLINICAL ONCOLOGY R E V I E W A R T I C L E Adjuvant Endocrine Therapy for Premenopausal Women With Early Breast Cancer Silvia Dellapasqua, Marco Colleoni,
Seigo Nakamura,M.D.,Ph.D.
 Seigo Nakamura,M.D.,Ph.D. Professor of Surgery Director of Breast Center Showa University Hospital Chairman of the board of directors Japan Breast Cancer Society Inhibition of Estrogen-Dependent Growth
Seigo Nakamura,M.D.,Ph.D. Professor of Surgery Director of Breast Center Showa University Hospital Chairman of the board of directors Japan Breast Cancer Society Inhibition of Estrogen-Dependent Growth
Adjuvant chemotherapy of breast cancer
 Journal of BUON 10: 175-180, 2005 2005 Zerbinis Medical Publications. Printed in Greece REVIEW ARTICLE Adjuvant chemotherapy of breast cancer S. Bešlija Department of Medical Oncology, Institute of Oncology,
Journal of BUON 10: 175-180, 2005 2005 Zerbinis Medical Publications. Printed in Greece REVIEW ARTICLE Adjuvant chemotherapy of breast cancer S. Bešlija Department of Medical Oncology, Institute of Oncology,
ATAC Trial. 10 year median follow-up data. Approval Code: AZT-ARIM-10005
 ATAC Trial 10 year median follow-up data Approval Code: AZT-ARIM-10005 Background FDA post-approval commitment analysis to update DFS, TTR, OS and Safety Prof. Jack Cuzick on behalf of ATAC/LATTE Trialists
ATAC Trial 10 year median follow-up data Approval Code: AZT-ARIM-10005 Background FDA post-approval commitment analysis to update DFS, TTR, OS and Safety Prof. Jack Cuzick on behalf of ATAC/LATTE Trialists
Hormone therapy in Breast Cancer patients with comorbidities
 Hormone therapy in Breast Cancer patients with comorbidities Diana Crivellari Centro di Riferimento Oncologico Aviano- ITALY Madrid November 9th, 2007 Main issues Comorbidities in elderly women Hormonal
Hormone therapy in Breast Cancer patients with comorbidities Diana Crivellari Centro di Riferimento Oncologico Aviano- ITALY Madrid November 9th, 2007 Main issues Comorbidities in elderly women Hormonal
Ovarian Ablation as Adjuvant Therapy for Breast Cancer
 Ovarian Ablation as Adjuvant Therapy for Breast Cancer Nancy E. Davidson Ovarian ablation was the first form of systemic treatment for breast cancer. Its efficacy as a palliative treatment for young women
Ovarian Ablation as Adjuvant Therapy for Breast Cancer Nancy E. Davidson Ovarian ablation was the first form of systemic treatment for breast cancer. Its efficacy as a palliative treatment for young women
Coming of Age: Breast Cancer in Seniors HYMAN B. MUSS
 The Oncologist Understanding and Treating Triple-Negative Breast Cancer Across the Age Spectrum Coming of Age: Breast Cancer in Seniors HYMAN B. MUSS The University of North Carolina Lineberger Cancer
The Oncologist Understanding and Treating Triple-Negative Breast Cancer Across the Age Spectrum Coming of Age: Breast Cancer in Seniors HYMAN B. MUSS The University of North Carolina Lineberger Cancer
What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland
 What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland Outline Early breast cancer Advanced breast cancer Open questions Outline Early breast cancer
What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland Outline Early breast cancer Advanced breast cancer Open questions Outline Early breast cancer
Adjuvant Systemic Therapies in Breast Cancer
 Adjuvant Systemic Therapies in Breast Cancer Leonel F. Hernandez-Aya, MD a, Ana M. Gonzalez-Angulo, MD, MSc b,c,d, * KEYWORDS Adjuvant Breast cancer Adjuvant endocrine Adjuvant chemotherapy Adjuvant HER-2-targeted
Adjuvant Systemic Therapies in Breast Cancer Leonel F. Hernandez-Aya, MD a, Ana M. Gonzalez-Angulo, MD, MSc b,c,d, * KEYWORDS Adjuvant Breast cancer Adjuvant endocrine Adjuvant chemotherapy Adjuvant HER-2-targeted
Clinical Expert Submission Template
 Clinical Expert Submission Template Thank you for agreeing to give us a personal statement on your view of the technology and the way it should be used in the NHS. Health care professionals can provide
Clinical Expert Submission Template Thank you for agreeing to give us a personal statement on your view of the technology and the way it should be used in the NHS. Health care professionals can provide
Review Recent advances in systemic therapy Advances in adjuvant systemic chemotherapy of early breast cancer Sara López-Tarruella and Miguel Martín
 Review Recent advances in systemic therapy Advances in adjuvant systemic chemotherapy of early breast cancer Sara López-Tarruella and Miguel Martín Medical Oncology Department, Clínico San Carlos Hospital,
Review Recent advances in systemic therapy Advances in adjuvant systemic chemotherapy of early breast cancer Sara López-Tarruella and Miguel Martín Medical Oncology Department, Clínico San Carlos Hospital,
American Society of Clinical Oncology June , New Orleans
 American Society of Clinical Oncology June 5-8 2004, New Orleans The 2004 annual meeting of the American Society of Clinical Oncology (ASCO) was held June 5 8 in New Orleans, Louisiana. This conference
American Society of Clinical Oncology June 5-8 2004, New Orleans The 2004 annual meeting of the American Society of Clinical Oncology (ASCO) was held June 5 8 in New Orleans, Louisiana. This conference
Non-Anthracycline Adjuvant Therapy: When to Use?
 Northwestern University Feinberg School of Medicine Non-Anthracycline Adjuvant Therapy: When to Use? William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley Center for
Northwestern University Feinberg School of Medicine Non-Anthracycline Adjuvant Therapy: When to Use? William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley Center for
Adjuvant Endocrine Therapy in Pre- and Postmenopausal Patients
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Endocrine Therapy in Pre- and Postmenopausal Patients Adjuvant Endocrine Therapy in Pre- and Postmenopausal Patients
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Endocrine Therapy in Pre- and Postmenopausal Patients Adjuvant Endocrine Therapy in Pre- and Postmenopausal Patients
Relative dose intensity delivered to patients with early breast cancer: Canadian experience
 M E D I C A L O N C O L O G Y Relative dose intensity delivered to patients with early breast cancer: Canadian experience S. Raza MD, S. Welch MD, and J. Younus MD ABSTRACT Adjuvant chemotherapy for early
M E D I C A L O N C O L O G Y Relative dose intensity delivered to patients with early breast cancer: Canadian experience S. Raza MD, S. Welch MD, and J. Younus MD ABSTRACT Adjuvant chemotherapy for early
EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY. Dr. Carlos Garbino
 EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY Dr. Carlos Garbino EARLY BREAST CANCER ADJUVANT CHEMOTHERAPY SUSTANTIVE DIFFICULTIES FOR A WORLDWIDE APPLICABILITY DUE TO IMPORTANT INEQUALITIES + IN DIFFERENT
EARLY STAGE BREAST CANCER ADJUVANT CHEMOTHERAPY Dr. Carlos Garbino EARLY BREAST CANCER ADJUVANT CHEMOTHERAPY SUSTANTIVE DIFFICULTIES FOR A WORLDWIDE APPLICABILITY DUE TO IMPORTANT INEQUALITIES + IN DIFFERENT
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29317 holds various files of this Leiden University dissertation. Author: Nes, Johanna Gerarda Hendrica van Title: Clinical aspects of endocrine therapy
Cover Page The handle http://hdl.handle.net/1887/29317 holds various files of this Leiden University dissertation. Author: Nes, Johanna Gerarda Hendrica van Title: Clinical aspects of endocrine therapy
Use of Ovarian Suppression and Ablation in Breast Cancer Treatment
 Use of Ovarian Suppression and Ablation in Breast Cancer Treatment Dr Marina Parton Consultant Medical Oncologist Royal Marsden and Kingston Hospitals Overview Breast cancer phenotypes Use of ovarian manipulation
Use of Ovarian Suppression and Ablation in Breast Cancer Treatment Dr Marina Parton Consultant Medical Oncologist Royal Marsden and Kingston Hospitals Overview Breast cancer phenotypes Use of ovarian manipulation
CASE STUDIES CLINICAL CASE SCENARIOS. Matthew J. Ellis, MD, PhD
 CLINICAL CASE SCENARIOS Matthew J. Ellis, MD, PhD Clinicians face daily challenges in the management of individual patients with breast cancer who demonstrate different characteristics in terms of estrogen
CLINICAL CASE SCENARIOS Matthew J. Ellis, MD, PhD Clinicians face daily challenges in the management of individual patients with breast cancer who demonstrate different characteristics in terms of estrogen
Adjuvant Hormonal Therapy in Peri- and Postmenopausal. Breast Cancer
 Breast Cancer Adjuvant Hormonal Therapy in Peri- and Postmenopausal Breast Cancer Paula D. Ryan, Paul E. Goss Massachusetts General Hospital, Boston, Massachusetts, USA Key Words. Breast cancer Aromatase
Breast Cancer Adjuvant Hormonal Therapy in Peri- and Postmenopausal Breast Cancer Paula D. Ryan, Paul E. Goss Massachusetts General Hospital, Boston, Massachusetts, USA Key Words. Breast cancer Aromatase
Terapia Hormonal da Paciente Premenopausa
 I Congresso de Oncologia D Or 5 e 6 de julho de 2013 Terapia Hormonal da Paciente Premenopausa Antonio C. Wolff, MD, FACP, FASCO Professor de Oncologia Programa de Câncer de Mama Johns Hopkins University
I Congresso de Oncologia D Or 5 e 6 de julho de 2013 Terapia Hormonal da Paciente Premenopausa Antonio C. Wolff, MD, FACP, FASCO Professor de Oncologia Programa de Câncer de Mama Johns Hopkins University
Integrated care: guidance on fracture prevention in cancer-associated bone disease; treatment options
 Paris, November 1st 2016 Integrated care: guidance on fracture prevention in cancer-associated bone disease; treatment options René Rizzoli MD International Osteoporosis Foundation and Division of Bone
Paris, November 1st 2016 Integrated care: guidance on fracture prevention in cancer-associated bone disease; treatment options René Rizzoli MD International Osteoporosis Foundation and Division of Bone
OPTIMIZING NONANTHRACYLINES FOR EARLY BREAST CANCER. Stephen E. Jones, M.D. US Oncology Research, McKesson Specialty Health The Woodlands, Tx
 OPTIMIZING NONANTHRACYLINES FOR EARLY BREAST CANCER Stephen E. Jones, M.D. US Oncology Research, McKesson Specialty Health The Woodlands, Tx ANTHRACYCLINES AND TAXANES ARE COMMONLY USED USED IN MOST REGIMENS
OPTIMIZING NONANTHRACYLINES FOR EARLY BREAST CANCER Stephen E. Jones, M.D. US Oncology Research, McKesson Specialty Health The Woodlands, Tx ANTHRACYCLINES AND TAXANES ARE COMMONLY USED USED IN MOST REGIMENS
The Latest Research: Hormonal Therapies
 The Latest Research: Hormonal Therapies Sameer Gupta, M.D., M.P.H 9/29/2018 Attending Physician, Hematology/Oncology Bryn Mawr Hospital Clinical Assistant Professor, Jefferson Medical College Disclosures
The Latest Research: Hormonal Therapies Sameer Gupta, M.D., M.P.H 9/29/2018 Attending Physician, Hematology/Oncology Bryn Mawr Hospital Clinical Assistant Professor, Jefferson Medical College Disclosures
Adjuvant Endocrine Therapy in Premenopausal Patients
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Endocrine Therapy in Premenopausal Patients Adjuvant Endocrine Therapy in Premenopausal Patients Version 2002: Scharl
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Adjuvant Endocrine Therapy in Premenopausal Patients Adjuvant Endocrine Therapy in Premenopausal Patients Version 2002: Scharl
Breast Cancer Earlier Disease. Stefan Aebi Luzerner Kantonsspital
 Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
38 years old, premenopausal, had L+snbx. Pathology: IDC Gr.II T-1.9cm N+2/4sn ER+100%st, PR+60%st, Her2-neg, KI %
 38 years old, premenopausal, had L+snbx Pathology: IDC Gr.II T-1.9cm N+2/4sn ER+100%st, PR+60%st, Her2-neg, KI67 5-10% Question: What will you do now? 1. Give adjuvant chemotherapy 2. Send for Oncotype
38 years old, premenopausal, had L+snbx Pathology: IDC Gr.II T-1.9cm N+2/4sn ER+100%st, PR+60%st, Her2-neg, KI67 5-10% Question: What will you do now? 1. Give adjuvant chemotherapy 2. Send for Oncotype
Treatment Options for Breast Cancer in Low- and Middle-Income Countries: Adjuvant and Metastatic Systemic Therapy
 Women s Empowerment Cancer Advocacy Network (WE CAN) Conference Bucharest, Romania October 2015 Treatment Options for Breast Cancer in Low- and Middle-Income Countries: Adjuvant and Metastatic Systemic
Women s Empowerment Cancer Advocacy Network (WE CAN) Conference Bucharest, Romania October 2015 Treatment Options for Breast Cancer in Low- and Middle-Income Countries: Adjuvant and Metastatic Systemic
Advances in Neoadjuvant and Adjuvant Therapy for Breast Cancer
 Advances in Neo and Adjuvant Therapy for Breast Cancer Nicole Kounalakis, MD, and Christina Finlayson, MD OVERVIEW Systemic therapy for breast cancer is evolving rapidly. The medical treatment of cancer
Advances in Neo and Adjuvant Therapy for Breast Cancer Nicole Kounalakis, MD, and Christina Finlayson, MD OVERVIEW Systemic therapy for breast cancer is evolving rapidly. The medical treatment of cancer
Endocrine Therapy for Early Breast Cancer: Updated Review
 REVIEWS AND CONTEMPORARY UPDATES Ochsner Journal 17:405 411, 2017 Ó Academic Division of Ochsner Clinic Foundation Endocrine Therapy for Early Breast Cancer: Updated Review Alexander Tremont, DO, 1 Jonathan
REVIEWS AND CONTEMPORARY UPDATES Ochsner Journal 17:405 411, 2017 Ó Academic Division of Ochsner Clinic Foundation Endocrine Therapy for Early Breast Cancer: Updated Review Alexander Tremont, DO, 1 Jonathan
William J. Gradishar MD
 Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2011 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2011 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER
 Contact: Anne Bancillon + 33 (0)6 70 93 75 28 STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER Key results of 42 nd annual meeting of the American Society of Clinical
Contact: Anne Bancillon + 33 (0)6 70 93 75 28 STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER Key results of 42 nd annual meeting of the American Society of Clinical
Postoperative Adjuvant Chemotherapies. Stefan Aebi Luzerner Kantonsspital
 Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
The worldwide overview: updated (2005-6) meta-analyses of hormonal treatment trials
 The worldwide overview: updated (2005-6) meta-analyses of hormonal treatment trials Richard Gray, for the Early Breast Cancer Trialists Collaborative Group (EBCTCG) Main questions, 2005-6 1) 5 years of
The worldwide overview: updated (2005-6) meta-analyses of hormonal treatment trials Richard Gray, for the Early Breast Cancer Trialists Collaborative Group (EBCTCG) Main questions, 2005-6 1) 5 years of
Matters of the heart: cardiac toxicity of adjuvant systemic therapy for earlystage breast cancer
 CARDIAC TOXICITY MEDICAL ONCOLOGY Matters of the heart: cardiac toxicity of adjuvant systemic therapy for earlystage breast cancer K. Towns MD,* P.L. Bedard MD, and S. Verma MD MSEd ABSTRACT Breast cancer
CARDIAC TOXICITY MEDICAL ONCOLOGY Matters of the heart: cardiac toxicity of adjuvant systemic therapy for earlystage breast cancer K. Towns MD,* P.L. Bedard MD, and S. Verma MD MSEd ABSTRACT Breast cancer
Breast Cancer Breast Managed Clinical Network
 Initial Evaluation Clinical Stage Pre-Treatment Evaluation Treatment and pathological stage Less than 4 positive lymph nodes Adjuvant Treatment ER Positive HER2 Negative (see page 2 & 3 ) HER2 Positive
Initial Evaluation Clinical Stage Pre-Treatment Evaluation Treatment and pathological stage Less than 4 positive lymph nodes Adjuvant Treatment ER Positive HER2 Negative (see page 2 & 3 ) HER2 Positive
The first randomized clinical trial of adjuvant
 ADJUVANT ENDOCRINE THERAPY FOR POSTMENOPAUSAL WOMEN WITH EARLY BREAST CANCER Aman U. Buzdar, MD* ABSTRACT The safety and efficacy of tamoxifen as adjuvant endocrine therapy for postmenopausal patients
ADJUVANT ENDOCRINE THERAPY FOR POSTMENOPAUSAL WOMEN WITH EARLY BREAST CANCER Aman U. Buzdar, MD* ABSTRACT The safety and efficacy of tamoxifen as adjuvant endocrine therapy for postmenopausal patients
SOFTly: The Long Natural History of [Trials for] [premenopausal] ER+ Breast Cancer
![SOFTly: The Long Natural History of [Trials for] [premenopausal] ER+ Breast Cancer SOFTly: The Long Natural History of [Trials for] [premenopausal] ER+ Breast Cancer](/thumbs/95/125806264.jpg) SOFTly: The Long Natural History of [Trials for] [premenopausal] ER+ Breast Cancer Charles Moertel Lecture May 12, 2017 Gini Fleming Charles Moertel Founder of NCCTG Dedication to high quality clinical
SOFTly: The Long Natural History of [Trials for] [premenopausal] ER+ Breast Cancer Charles Moertel Lecture May 12, 2017 Gini Fleming Charles Moertel Founder of NCCTG Dedication to high quality clinical
新竹馬偕紀念醫院癌症中心 乳癌化學治療藥物處方
 新竹馬偕紀念醫院癌症中心 乳癌化學治療藥物處方 文件修訂記錄 修正次數 修正日期 修正版別 修 改 內 容 1 2011.04.07 1.0 初次訂定 2 2013.05.08 2.0 修訂 3 2013.04.30 3.0 修訂 :Triple-Negative Breast Cancer 處方 新增 :Neoadjuvant-p7~8 4 2014.04.29 4.0 修訂 :FEC + Trastuzumab
新竹馬偕紀念醫院癌症中心 乳癌化學治療藥物處方 文件修訂記錄 修正次數 修正日期 修正版別 修 改 內 容 1 2011.04.07 1.0 初次訂定 2 2013.05.08 2.0 修訂 3 2013.04.30 3.0 修訂 :Triple-Negative Breast Cancer 處方 新增 :Neoadjuvant-p7~8 4 2014.04.29 4.0 修訂 :FEC + Trastuzumab
Evolving Insights into Adjuvant Chemotherapy. Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology
 Evolving Insights into Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology Dilemmas in Adjuvant Chemotherapy Is adjuvant chemotherapy effective in ER+
Evolving Insights into Adjuvant Chemotherapy Joyce O Shaughnessy, MD Baylor Sammons Cancer Center Texas Oncology US Oncology Dilemmas in Adjuvant Chemotherapy Is adjuvant chemotherapy effective in ER+
Herceptin Pivotal Studies
 Herceptin Pivotal Studies Nuhad K Ibrahim, MD, FACP Associate Professor of Medicine Breast Medical Oncology Department MD Anderson Cancer Center Houston, TX, USAE-mail: nibrahim@mdanderson.org Herceptin
Herceptin Pivotal Studies Nuhad K Ibrahim, MD, FACP Associate Professor of Medicine Breast Medical Oncology Department MD Anderson Cancer Center Houston, TX, USAE-mail: nibrahim@mdanderson.org Herceptin
The HERA Study Team. Presented by Ian E. Smith
 Trastuzumab Following Adjuvant Chemotherapy in HER2-Positive Early Breast Cancer (HERA Trial): Disease-Free and Overall Survival after 2 Year Median Follow-Up The HERA Study Team Presented by Ian E. Smith
Trastuzumab Following Adjuvant Chemotherapy in HER2-Positive Early Breast Cancer (HERA Trial): Disease-Free and Overall Survival after 2 Year Median Follow-Up The HERA Study Team Presented by Ian E. Smith
J Clin Oncol 23: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 23 NUMBER 30 OCTOBER 20 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Retrospective Analysis of Time to Recurrence in the ATAC Trial According to Hormone Receptor Status: An Hypothesis-Generating
VOLUME 23 NUMBER 30 OCTOBER 20 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Retrospective Analysis of Time to Recurrence in the ATAC Trial According to Hormone Receptor Status: An Hypothesis-Generating
Study Of Letrozole Extension. Coordinating Group IBCSG IBCSG BIG 1-07
 tudy Of Letrozole Extension Coordinating Group IBCSG IBCSG 35-07 BIG 1-07 A phase III trial evaluating the role of continuous letrozole versus intermittent letrozole following 4 to 6 years of prior adjuvant
tudy Of Letrozole Extension Coordinating Group IBCSG IBCSG 35-07 BIG 1-07 A phase III trial evaluating the role of continuous letrozole versus intermittent letrozole following 4 to 6 years of prior adjuvant
30 TH ANNUAL SAN ANTONIO BREAST CANCER SYMPOSIUM (SABCS) NEW ADVANCES IN THE TREATMENT OF BREAST CANCER
 EDUCATIONAL HIGHLIGHTS FROM DATA PRESENTED AT THE 30 TH ANNUAL SAN ANTONIO BREAST CANCER SYMPOSIUM (SABCS) NEW ADVANCES IN THE TREATMENT OF BREAST CANCER DECEMBER 13 16, 2007, SAN ANTONIO, TX, USA 2 CONTENTS
EDUCATIONAL HIGHLIGHTS FROM DATA PRESENTED AT THE 30 TH ANNUAL SAN ANTONIO BREAST CANCER SYMPOSIUM (SABCS) NEW ADVANCES IN THE TREATMENT OF BREAST CANCER DECEMBER 13 16, 2007, SAN ANTONIO, TX, USA 2 CONTENTS
Chemo-endocrine prevention of breast cancer
 Chemo-endocrine prevention of breast cancer Andrea DeCensi, MD Division of Medical Oncology Ospedali Galliera, Genova; Division of Cancer Prevention and Genetics, European Institute of Oncology, Milano;
Chemo-endocrine prevention of breast cancer Andrea DeCensi, MD Division of Medical Oncology Ospedali Galliera, Genova; Division of Cancer Prevention and Genetics, European Institute of Oncology, Milano;
Scottish Medicines Consortium
 Scottish Medicines Consortium anastrozole 1mg tablets (Arimidex ) No. (198/05) AstraZeneca UK Ltd New indication: for adjuvant treatment of postmenopausal women with hormone receptorpositive early invasive
Scottish Medicines Consortium anastrozole 1mg tablets (Arimidex ) No. (198/05) AstraZeneca UK Ltd New indication: for adjuvant treatment of postmenopausal women with hormone receptorpositive early invasive
4/13/2010. Silverman, Buchanan Breast, 2003
 Tailoring Breast Cancer Treatment: Has Personalized Medicine Arrived? Judith Luce, M.D. San Francisco General Hospital Avon Comprehensive Breast Care Center Outline First, treatment of DCIS Sorting risk
Tailoring Breast Cancer Treatment: Has Personalized Medicine Arrived? Judith Luce, M.D. San Francisco General Hospital Avon Comprehensive Breast Care Center Outline First, treatment of DCIS Sorting risk
The absolute benefit from chemotherapy for both older and younger patients appeared most significant in ER-negative populations.
 Hello, my name is Diane Hecht, and I am a Clinical Pharmacy Specialist at the University of Texas MD Anderson Cancer Center. It s my pleasure to talk to you today about the role of chemotherapy in this
Hello, my name is Diane Hecht, and I am a Clinical Pharmacy Specialist at the University of Texas MD Anderson Cancer Center. It s my pleasure to talk to you today about the role of chemotherapy in this
Emerging Approaches for (Neo)Adjuvant Therapy for ER+ Breast Cancer
 Emerging Approaches for (Neo)Adjuvant Therapy for E+ Breast Cancer Cynthia X. Ma, M.D., Ph.D. Associate Professor of Medicine Washington University in St. Louis Outline Current status of adjuvant endocrine
Emerging Approaches for (Neo)Adjuvant Therapy for E+ Breast Cancer Cynthia X. Ma, M.D., Ph.D. Associate Professor of Medicine Washington University in St. Louis Outline Current status of adjuvant endocrine
BREAST CANCER RISK REDUCTION (PREVENTION)
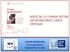 BREAST CANCER RISK REDUCTION (PREVENTION) Articles Anastrozole for prevention of breast cancer in high-risk postmenopausal women (IBIS-II): an international, double-blind, randomised placebo-controlled
BREAST CANCER RISK REDUCTION (PREVENTION) Articles Anastrozole for prevention of breast cancer in high-risk postmenopausal women (IBIS-II): an international, double-blind, randomised placebo-controlled
Anthracyclines for Breast Cancer? Are Adjuvant Anthracyclines Dispensible? Needs to be Answered in a Large Prospective Trial
 Anthracyclines for Breast Cancer? Are Adjuvant Anthracyclines Dispensible? Needs to be Answered in a Large Prospective Trial Joanne L. Blum, MD, PhD Baylor-Sammons Cancer Dallas, TX Early Breast Cancer
Anthracyclines for Breast Cancer? Are Adjuvant Anthracyclines Dispensible? Needs to be Answered in a Large Prospective Trial Joanne L. Blum, MD, PhD Baylor-Sammons Cancer Dallas, TX Early Breast Cancer
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012
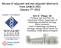 Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
It is a malignancy originating from breast tissue
 59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
The Three Ages of Systemic Adjuvant Therapy for EBC
 The Three Ages of Systemic Adjuvant Therapy for EBC 1896-2018 Nicholas Wilcken Westmead Hospital Petersham Institute University of Sydney Questions to be answered (concentrating on chemotherapy) Why should
The Three Ages of Systemic Adjuvant Therapy for EBC 1896-2018 Nicholas Wilcken Westmead Hospital Petersham Institute University of Sydney Questions to be answered (concentrating on chemotherapy) Why should
Update from the 29th Annual San Antonio Breast Cancer Symposium
 Update from the 29th Annual San Antonio Breast Cancer Symposium The San Antonio Breast Cancer Symposium is one of the most important breast cancer conferences. Approximately 8,000 physicians, oncologists,
Update from the 29th Annual San Antonio Breast Cancer Symposium The San Antonio Breast Cancer Symposium is one of the most important breast cancer conferences. Approximately 8,000 physicians, oncologists,
SANDRA M. SWAIN. Washington Cancer Institute, Washington, District of Columbia, USA
 The Oncologist Early-Stage Breast Cancer: Clinical Update Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast
The Oncologist Early-Stage Breast Cancer: Clinical Update Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast
NIH Public Access Author Manuscript Nat Rev Clin Oncol. Author manuscript; available in PMC 2012 December 10.
 NIH Public Access Author Manuscript Published in final edited form as: Nat Rev Clin Oncol. ; 9(4): 223 229. doi:10.1038/nrclinonc.2012.21. Use of neoadjuvant data to design adjuvant endocrine therapy trials
NIH Public Access Author Manuscript Published in final edited form as: Nat Rev Clin Oncol. ; 9(4): 223 229. doi:10.1038/nrclinonc.2012.21. Use of neoadjuvant data to design adjuvant endocrine therapy trials
Adjuvant therapy in early breast cancer
 Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Centro di Riferimento Regionale per la diagnosi e la terapia dei tumori del colon-retto. D.A. 26/10/2012 G.U.R.S. del 14/12/2012 parte I,
Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Centro di Riferimento Regionale per la diagnosi e la terapia dei tumori del colon-retto. D.A. 26/10/2012 G.U.R.S. del 14/12/2012 parte I,
Existe-t-il un sous groupe à risque qui pourrait bénéficier d une modification de la durée de traitement par trastuzumab? X. Pivot CHRU De Besançon
 Existe-t-il un sous groupe à risque qui pourrait bénéficier d une modification de la durée de traitement par trastuzumab? X. Pivot CHRU De Besançon In 25 results of 4 Adjuvant Herceptin trials have definitively
Existe-t-il un sous groupe à risque qui pourrait bénéficier d une modification de la durée de traitement par trastuzumab? X. Pivot CHRU De Besançon In 25 results of 4 Adjuvant Herceptin trials have definitively
Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1
 Important data from BCIRG 006 Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1 in the adjuvant treatment of HER2+ breast
Important data from BCIRG 006 Taxotere * and carboplatin plus Herceptin (trastuzumab) (TCH): the first approved non-anthracycline Herceptin-containing regimen 1 in the adjuvant treatment of HER2+ breast
Anthracyclines in the elderly breast cancer patients
 Anthracyclines in the elderly breast cancer patients Etienne GC Brain, MD PhD Medical Oncology Centre René Huguenin, Saint-Cloud & Group GERICO, FNCLCC, Paris Centre René Huguenin - Saint-Cloud Facts about
Anthracyclines in the elderly breast cancer patients Etienne GC Brain, MD PhD Medical Oncology Centre René Huguenin, Saint-Cloud & Group GERICO, FNCLCC, Paris Centre René Huguenin - Saint-Cloud Facts about
Start strong or switch? Adjuvant endocrine strategies for postmenopausal women with hormone-sensitive breast cancer
 Available online at www.sciencedirect.com Biomedicine & Pharmacotherapy 63 (2009) 1e10 Short review Start strong or switch? Adjuvant endocrine strategies for postmenopausal women with hormone-sensitive
Available online at www.sciencedirect.com Biomedicine & Pharmacotherapy 63 (2009) 1e10 Short review Start strong or switch? Adjuvant endocrine strategies for postmenopausal women with hormone-sensitive
New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer
 New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
Long Term Toxicity of Endocrine Therapy for premenopausal women with ER positive breast cancer
 Global Breast Cancer Conference 2017 21 st Apr, 2017@Chezu Island Long Term Toxicity of Endocrine Therapy for premenopausal women with ER positive breast cancer Shinji Ohno, M.D., Ph.D., F.A.C.S. Breast
Global Breast Cancer Conference 2017 21 st Apr, 2017@Chezu Island Long Term Toxicity of Endocrine Therapy for premenopausal women with ER positive breast cancer Shinji Ohno, M.D., Ph.D., F.A.C.S. Breast
Stopping a cancer trial early: is it really for the benefit of patients? What about the quality of data?
 Stopping a cancer trial early: is it really for the benefit of patients? What about the quality of data? Pinuccia Valagussa Fondazione Michelangelo, Milano I have no relevant relationships to disclose
Stopping a cancer trial early: is it really for the benefit of patients? What about the quality of data? Pinuccia Valagussa Fondazione Michelangelo, Milano I have no relevant relationships to disclose
8/8/2011. PONDERing the Need to TAILOR Adjuvant Chemotherapy in ER+ Node Positive Breast Cancer. Overview
 Overview PONDERing the Need to TAILOR Adjuvant in ER+ Node Positive Breast Cancer Jennifer K. Litton, M.D. Assistant Professor The University of Texas M. D. Anderson Cancer Center Using multigene assay
Overview PONDERing the Need to TAILOR Adjuvant in ER+ Node Positive Breast Cancer Jennifer K. Litton, M.D. Assistant Professor The University of Texas M. D. Anderson Cancer Center Using multigene assay
SANDRA M. SWAIN. Washington Cancer Institute, Washington, District of Columbia, USA
 The Oncologist Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast cancer Chemotherapy Taxane Trastuzumab Ki-67
The Oncologist Chemotherapy: Updates and New Perspectives SANDRA M. SWAIN Washington Cancer Institute, Washington, District of Columbia, USA Key Words. Breast cancer Chemotherapy Taxane Trastuzumab Ki-67
Early Stage Disease. Hope S. Rugo, MD Professor of Medicine Director Breast Oncology and Clinical Trials Education UCSF Comprehensive Cancer Center
 SABCS 2014: Early Stage Disease Hope S. Rugo, MD Professor of Medicine Director Breast Oncology and Clinical Trials Education UCSF Comprehensive Cancer Center Topics for Discussion Chemotherapy plus 10
SABCS 2014: Early Stage Disease Hope S. Rugo, MD Professor of Medicine Director Breast Oncology and Clinical Trials Education UCSF Comprehensive Cancer Center Topics for Discussion Chemotherapy plus 10
An updated review on the efficacy of adjuvant endocrine therapies in hormone receptor positive early breast cancer
 MEDICAL ONCOLOGY An updated review on the efficacy of adjuvant endocrine therapies in hormone receptor positive early breast cancer S. Verma m d,* S. Sehdev, A. Joy m d, Y. Madarnas m d, J. Younus m d,
MEDICAL ONCOLOGY An updated review on the efficacy of adjuvant endocrine therapies in hormone receptor positive early breast cancer S. Verma m d,* S. Sehdev, A. Joy m d, Y. Madarnas m d, J. Younus m d,
