Consensus Guideline on Hereditary Genetic Testing for Patients With and Without Breast Cancer
|
|
|
- Sherman Clark
- 6 years ago
- Views:
Transcription
1 Consensus Guideline on Hereditary Genetic Testing for Patients With and Without Breast Cancer Purpose: To outline an approach to hereditary cancer genetic testing for patients with and without breast cancer Associated ASBrS Guidelines or Quality Measures: 1. BRCA Genetic Testing for Patients With and Without Breast Cancer, September 13, BRCA Genetic Testing for Patients With and Without Breast Cancer, September 30, BRCA Genetic Testing for Patients With and Without Breast Cancer, June 12, 2006 Methods: Literature review included large datasets, basic science publications, and recent updated national guidelines. This is not a complete systematic review, but a comprehensive review of the modern literature on this subject. Pending Approval: The ASBrS Research Committee developed a consensus document that was reviewed and approved by the ASBrS Board of Directors. Summary of Data Reviewed: Indications In 2016, more than 245,000 new cases of breast cancer will be diagnosed in the United States, and more than 40,000 patients will die from breast cancer. 1 Approximately 5-10% of breast cancer is associated with a hereditary predisposition from an inherited germline mutation 2, with 50% of mutations occurring in the BRCA1 and BRCA2 genes. 3-8 Identifying patients who are mutation carriers may reduce the risk of future cancer and may prevent death from cancer through risk-reducing interventions While mutations in BRCA1, BRCA2, and other hereditary cancer predisposition genes are rare in the general population, occurring in 1 per individuals or less, an individual with a personal and family history with high-risk characteristics can help identify patients more likely to be mutation carriers Breast surgeons are ideally positioned to identify high-risk individuals, encourage and provide access for hereditary cancer genetic testing, and propose individualized management strategies for those patients who test positive In many areas of the country, breast surgeons can fill the unmet need for appropriate counseling of these high-risk patients. Breast surgeons can also identify patients at high risk for other hereditary breast cancer syndromes, such as Li-Fraumeni syndrome (TP53 mutation), Cowden syndrome (PTEN mutation), and ATM carriers This knowledge can influence radiation therapy as well as chemotherapy decisions
2 The following personal and/or family characteristics suggest a high-risk individual who would be a candidate for genetic testing: a. Age onset of breast cancer 50 b. Triple-negative tumor (ER-PR-HER2-) and age 60 c. Ashkenazi Jewish heritage and breast cancer at any age d. Two or more primary breast cancers (cancers can be asynchronous, synchronous, bilateral, or multicentric) e. First-degree relative with breast cancer age 50 f. Two relatives on the same side of the family with breast cancer and/or pancreatic cancer g. Family or personal history of ovarian cancer, fallopian cancer, or primary peritoneal cancer h. Male breast cancer i. Known mutation carrier in the family Risk Assessment Tools In addition to National Comprehensive Cancer Network (NCCN) guidelines for identifying patients appropriate for genetic testing, 26 there are numerous models and online calculators available to predict the likelihood of carrying a BRCA1 or BRCA2 mutation based on family and personal history. 33,34 In general, patients with a 5-10% or greater likelihood of carrying one of these genes is recommended to consider testing and/or genetic counseling. 35 Online Risk Models: (not an exclusive list of all calculators) BRCA Risk Calculator: B-RST: Penn II Risk Model: Implications Identifying a mutation in a hereditary cancer predisposition gene has implications for patients and their families. Before testing, patients need to be made aware of these implications (pre-test counseling) and when results become available, patients should be reminded of these implications and appropriate interventions and consultations should be recommended (post-test 21, 26, 35 counseling). The following is a list of pathogenic mutations in hereditary cancer genes with current NCCN guidelines for clinical management: 26 Guidelines accessed December 9, The current version of the guidelines is available online at Gene Risk Breast Management Options* BRCA1 Breast cancer (up to 67%) Contralateral breast cancer (up to 30%) Ovarian cancer (up to 45%) 50 BRCA2 Breast cancer (up to 66%) Contralateral breast cancer Annual breast MRI (start age 25) Annual breast MRI (start age 25)
3 (up to 30%) Ovarian cancer (up to 12%) Male breast cancer Prostate cancer Pancreatic cancer 50 TP53 Breast cancer Soft tissue sarcomas Osteosarcomas Brain tumors Adrenocortical carcinoma Multiple primary tumors PALB2 Breast cancer (33%, but 58% with 2 first-degree relatives) Pancreatic cancer Male breast cancer CDH1 Breast cancer (39% of lobular carcinoma) Gastric cancer Colorectal cancer PTEN Breast cancer Thyroid cancer Endometrial cancer Colorectal cancer Kidney cancer CHEK2 Breast cancer (20%, but increases with 44% with first- and second-degree relatives) 30% risk of contralateral breast cancer Male breast cancer Colon cancer Prostate cancer Thyroid cancer Kidney cancer ATM Breast cancer (rare mutations with a 40-60%) STK-11 Breast cancer Ovarian cancer Colorectal cancer Duodenal cancer Pancreatic cancer NF1 Breast Cancer before age 50 GIST Chemoprevention Annual breast MRI (start age 20) Annual breast MRI (start age 30) Annual breast MRI (start age 30) Annual breast MRI (start age 30) or 5-10 years before youngest patient with breast cancer MRI (start age 40) Annual mammogram based on family history Annual breast MRI (starting at age 40) Annual mammogram Discuss risk-reducing mastectomy based on family history Annual breast MRI (start age 30) Annual breast MRI (start age 30-50)
4 NBN Breast Cancer Annual breast MRI (start age 40) Annual mammograms *Guidelines are also available on screening and prophylaxis for non-breast-affected organs. In addition to the breast-management recommendations above, prophylactic oophorectomy has been shown to reduce the risk of breast cancer by more than 50% in premenopausal women with BRCA2 mutation, with less benefit to those patients with a BRCA1 mutation. 9,10,16,36 Patients with BRCA1 or BRCA2 mutations should consider prophylactic bilateral salpingo-oophorectomy after child-bearing or between the ages of to reduce ovarian and fallopian tube cancer risk. Limitations There are limitations to genetic testing. Patients should be aware that negative test results do not eliminate the risk of developing breast cancer, even in a family with a known mutation. The probability of false negative results can be as high as 6-8% when the criterion is a 10% mutation probability estimated by genetic counselors or the computer model BRCAPRO. 54 In patients with no known family mutation, a negative test does not change the patient s risk of developing breast cancer from the risk before testing. In a patient with a known family mutation, the patient who tests negative has a risk similar to the general population or higher depending on both maternal and paternal lineages. Not all mutation carriers will develop breast cancer, regardless of intervention chosen or not chosen, due to the variable penetrance of some gene mutations and other possible environmental interactions. 5,18,19 The BRCA Decision Tool, can be useful to known BRCA mutation carriers to predict likelihood of developing breast or ovarian cancer and likelihood of dying from either disease based on patient age and a variety of interventions chosen for screening and prophylaxis. 37 Lastly, not all cancer predisposition genes are known or completely understood, and further information pertinent to a patient s test may become available years later. 4,5,7 Certified Genetic Counselors The American College of Surgeons Commission on Cancer accreditation program mandates that cancer risk assessment, genetic counseling, and genetic testing services be provided to patients by a qualified genetic professional either on site or by referral. 55 A systematic review of the literature concluded that genetic counseling, whether by a geneticist, breast surgeon, oncology nurse, or other person with expertise and experience in cancer genetics, reduces distress, improves risk perception, and reduces intention for testing. 56 While breast surgeons can initiate and guide genetic testing for their patients, board-certified genetic counselors (CGCs), when available, may be beneficial for further counseling and recommendations. For families with more complex cancer histories, a CGC may help determine extent of testing, identify family members to be tested, and provide further guidance beyond that of a breast surgeon. This is especially important when identifying cancer risk in non-breast tissues such as ovaries, thyroid, stomach, and colorectal. 22,24,31,38,39 A CGC can provide a strategy for surveillance and intervention and often provides resources to patients undergoing the recommended regimen. Furthermore, when patients are found to carry a pathogenic mutation or a variant of uncertain significance (see below), a CGC may help guide additional family testing and screening.
5 Multi-Gene Panel Testing Genetic testing has expanded recently due to improved technology with next-generation sequencing and more access to testing options While BRCA1 and BRCA2 remain the most likely genes to be mutated in a family with high breast and ovarian cancer risk, there are now more than two dozen genes that can be tested either in sequence or simultaneously with BRCA testing that also confer hereditary cancer risk to a variable degree. 3,6,21,45-48 Numerous recent studies have shown that panel testing can significantly increase the rate of detection of pathogenic mutations, with the most frequently identified mutations being in PALB2, CHEK2, and ATM. 3,21,47 Of concern with this newer application of testing is that many genes with mutations do not yet have standard management guidelines available due to limited available data. 26 Furthermore, many genes found on panels, such as CHEK2 and ATM, will have a low-tomoderate penetrance, meaning that many carriers will not express the malignant phenotype. This poses challenges for creating reliable management guidelines; however, much of this will likely be overcome in time as data accumulate. 21,40,45 Breast surgeons can consider panel testing for patients who qualify for hereditary breast cancer testing to more efficiently and cost-effectively evaluate genes that confer risk and affect management recommendations. 26 This approach is not only more efficient in evaluating patients at risk compared to sequential gene sequencing (i.e., evaluating BRCA mutations first, then selecting additional genes if BRCA tests are negative), but it is also more cost-effective. 4,22,48 Insurance companies are urged to incorporate these advantages of panel testing into the algorithm of allowed hereditary cancer genetic testing for patients at high risk. The panel chosen may depend on family cancer history (if a pattern of cancers emerges that is suitable for Cowden s syndrome, then a panel that includes PTEN, for example, may be considered), test availability, and insurance coverage. Variant of Uncertain Significance (VUS) In the process of genetic testing, VUSs will be identified. These are DNA polymorphisms that are neither confirmed benign nor pathogenic, with the majority eventually re-classified as benign. 45,49 The American College of Medical Genetics has published guidelines for reporting DNA sequence variations. 57 The rate of identifying VUSs will be high initially with newer genes and then will decrease as data accrue over time. Current reported rates of identifying a VUS with newer multi-gene panel testing range from %. 21,45-47 There are still VUSs identified with BRCA testing. However, the rates are generally much lower, ranging from 2-5%, now that testing of these two genes has been available for nearly 20 years. ASBrS Recommendations for Genetic Testing: 1. Breast surgeons, CGCs and other trained cancer-liaison staff with in-depth knowledge of genetic testing indications, implications, and limitations can provide genetic testing services and recommendations to their patients. Use of specialized risk-assessment services and certified genetic counselors when patient history and test results are more complex is encouraged. Testing qualified patients can include BRCA1 and BRCA2 only, or additional genes (i.e., panel testing) related to hereditary breast cancer, so long as it is within guidelines, and the provider feels comfortable with recommendations.
6 2. Patients with a personal history of breast cancer: Always obtain information about family history of cancer. Ideally, a three-generation pedigree including maternal and paternal lineage should be obtained. This information can be used to guide the type of testing to be performed and the selection of patients who may benefit from further counseling with a CGC. Patients with a personal history of breast cancer meet criteria for genetic testing with any of the following characteristics: a. Age onset of breast cancer 50 b. Triple-negative tumor (ER-PR-HER2-) and age 60 c. Ashkenazi Jewish heritage and breast cancer at any age d. Two or more primary breast cancers (cancers can be asynchronous, synchronous, bilateral, or multicentric) e. First-degree relative with breast cancer age 50 f. Two relatives on the same side of the family with breast cancer and/or pancreatic cancer g. Family or personal history of ovarian cancer, fallopian cancer, or primary peritoneal cancer h. Male breast cancer i. Known mutation carrier in the family 3. Patients without a personal history of breast cancer: Patients should be made aware that testing an affected relative first when available can be more informative than testing themselves since a negative result will not give them more insight into their family history. If an affected relative is not available, patients should be reminded of limitations of testing. Ideally, a three-generation pedigree including maternal and paternal lineage should be obtained. This information can be used to guide the type of testing to be performed and the selection of patients who may benefit from further counseling with a CGC. Patients without a personal history of breast cancer meet criteria for genetic testing for the following family history: a. First- or second-degree relative with early age onset of breast cancer 45 b. Ashkenazi Jewish heritage and family history of breast cancer at any age c. Two or more primary breast cancers (cancers can be asynchronous, synchronous, bilateral, or multicentric) in a single family member d. Two or more relatives on the same side of the family with breast cancer and/or pancreatic cancer e. Family or personal history of ovarian cancer, fallopian cancer, or primary peritoneal cancer f. Male breast cancer g. Known mutation carrier in the family References: 1. National Cancer Institute. Cancer Stat Fact Sheets. Accessed July 17, 2016.
7 2. The Cancer Genome Atlas Network. Comprehensive molecular portraits of human breast tumours. Nature. 2012;490: Castera L, Krieger S, Rousselin A, et al. Next-generation sequencing for the diagnosis of hereditary breast and ovarian cancer using genomic capture targeting multiple candidate genes. Eur J Hum Genet. 2014;22: Walsh T, Lee MK, Casadei S, et al. Detection of inherited mutations for breast and ovarian cancer using genomic capture and massively parallel sequencing. Proc Natl Acad Sci USA. 2010;107: van der Groep P, van der Wall E, van Diest PJ. Pathology of hereditary breast cancer. Cell Oncol (Dordr). 2011;34: Walsh T, King MC. Ten genes for inherited breast cancer. Cancer Cell. 2007; 11: Meindl A, Ditsch N, Kast K, Schmutzler RK. Hereditary breast and ovarian cancer: new genes, new treatments, new concepts. Dtsch Arztebl Int. 2011;108: National Research Genome Institute (NIH). Learning about the BRCAX study. Accessed April 12, Domchek SM, Friebel TM, Singer CF, et al. Association of risk-reducing surgery in BRCA1 or BRCA2 mutation carriers with cancer risk and mortality. JAMA. 2010; 304: Kauff ND, Satagopan JM, Robson ME, et al. Risk-reducing salpingo-oophorectomy in women with a BRCA1 or BRCA2 mutation. N Engl J Med. 2002;346: Hartmann LC, Sellers TA, Schaid DJ, et al. Efficacy of bilateral prophylactic mastectomy in BRCA1 and BRCA2 gene mutation carriers. J Natl Cancer Inst. 2001;93: Kurian AW, Sigal BM, Plevrittis SK. Survival analysis of cancer risk reduction strategies for BRCA1/2 mutation carriers. J Clin Oncol. 2010;28: Narod SA, Offit K. Prevention and management of hereditary breast cancer. J Clin Oncol. 2005;23: Eisen A, Lubinski J, KlijnJ, et al. Breast cancer risk following bilateral oophorectomy in BRCA1 and BRCA2 mutation carriers: international case-control study. J Clin Oncol. 2005;23: Narod SA, Brunet JS, Ghadirian P, et al. Tamoxifen and risk of contralateral breast cancer in BRCA1 and BRCA2 mutation carriers: a case-control study. Lancet. 2000;356: Rebbeck TR, Lynch HT, Neuhausen SL, et al. Prophylactic oophorectomy in carriers of BRCA1 or BRCA2 mutations. N Engl J Med. 2002;346: Rebbeck TR, Friebel T, Lynch HT, et al. Bilateral prophylactic mastectomy reduces breast cancer risk in BRCA1 and BRCA2 mutation carriers: The PROSE Study Group. J Clin Oncol. 2004;22: Antoniou A, Pharoah PD, Narod S, et al. Average risks of breast and ovarian cancer associated with BRCA1 or BRCA2 mutations detected in case series unselected for family history: a combined analysis of 22 studies. Am J Hum Genet. 2003;72: Claus EB, Schildkraut JM, Thompson WD, Risch NJ. The genetic attributable risk of breast and ovarian cancer. Cancer. 1996;77: Robson ME, Boyd J, Borgen PI, et al. Hereditary breast cancer. Curr Probl Surg. 2001;38:
8 21. Kapoor NS, Curcio LD, Blakemore CA, et al. Multigene panel testing detects equal rates of pathogenic BRCA1/2 mutations and has a higher diagnostic yield compared to limited BRCA1/2 analysis alone in patients at risk for hereditary breast cancer. Ann Surg Oncol. 2015;22: Domchek, SM, Bradbury A, Garber JE, Offit K, Robson ME. Multiplex genetic testing for cancer susceptibility: out on the high wire without a net? J Clin Oncol. 2013;31: Garber JE, Offit K. Hereditary cancer predisposition syndromes. J Clin Oncol. 2005; 23: Li FP, Fraumeni JF, Mulvihill JJ, et al. A cancer family syndrome in twenty-four kindreds. Cancer Res. 1988;48: Lindor NM, McMaster ML, Lindor CJ, Greene MH. Li-Fraumeni syndrome. In: Concise Handbook of Familial Cancer Susceptibility Syndromes. 2nd ed. J Natl Cancer Inst Monogr. 2008;38: National Comprehensive Cancer Network. Genetic/Familial High-Risk Assessment: Breast and Ovarian. NCCN Clinical Practice Guidelines in Oncology. Accessed July 17, Ford D, Easton DF, Bishop DT, Narod SA, Goldgar DE. Breast Cancer Linkage Consortium: Risks of cancer in BRCA1-mutation carriers. Lancet. 1994;343: King MC, Marks JH, Mandell JB, and the New York Breast Cancer Study Group. Breast and ovarian cancer risks due to inherited mutations in BRCA1 and BRCA2. Science. 2003;302: Struewing JP, Hartge P, Wacholder S, et al. The risk of cancer associated with specific mutations of BRCA1 and BRCA2 among Ashkenazi Jews. N Engl J Med. 1997; 336: Couch FJ, Johnson MR, Rabe KG, et al. The prevalence of BRCA2 mutations in familial pancreatic cancer. Cancer Epidemiol Biomarkers Prev. 2007;16: Hall MJ, Dignam JJ, Olopade OI. Family history of pancreatic cancer in a high-risk cancer clinic: implications for risk assessment. J Genet Couns. 2008;17: Gonzalez-Angolo AM, Timms KM, Liu S, et al. Incidence and outcome of BRCA mutations in unselected patients with triple-receptor negative breast cancer. Clin Cancer Res. 2011;17: Evans DG, Eccles DM, Rahman N, et al. A new scoring system for the chances of identifying a BRCA 1/2 mutation outperforms existing models including BRCAPRO. J Med Genet. 2004;41: Gilpin CA, Carson N, Hunter AG. A preliminary validation of a family history assessment form to select women at risk for breast or ovarian cancer for referral to a genetics center. Clin Genet. 2000;58: Nelson H, Pappas M, Zakher B, et al. Risk assessment, genetic counseling, and genetic testing for BRCA-related cancer in women: a systematic review to update the U.S. Preventive Services Task Force recommendation. Ann Intern Med. 2014;160: Burke W, Daly M, Garber J, et al. Recommendations for follow-up care of individuals with an inherited predisposition to cancer. II. BRCA1 and BRCA2. JAMA. 1997;277:
9 37. Stanford Medicine Cancer Institute. Decision tool for women with BRCA mutations. Accessed August Anderson R, Haidle J. Legal considerations in clinical cancer genetics. Community Oncol. 2006;3: Doherty J, Bonadies DC, Matloff ET. Testing for hereditary breast cancer: panel or targeted testing? Experience from a clinical cancer genetics practice. J Genet Couns. 2015;24: Rainville IR, Rana HQ. Next-generation sequencing for inherited breast cancer risk: counseling through the complexity. Curr Oncol Rep. 2014;16: Ku CS, Cooper DN, Iacopetta B, et al. Integrating next generation sequencing into the diagnostic testing of inherited cancer predisposition. Clin Genet. 2013; 83: Simen B, Yin L, Goswami C, et al. Validation of a next-generation-sequencing cancer panel for use in the clinical laboratory. Arch Pathol Lab Med. 2015;139: Association for Molecular Pathology v Myriad Genetics, Inc., 569 US (2013). 44. Azvolinsky, A. Supreme Court ruling broadens BRCA testing options. J Natl Cancer Inst. 2013;105: LaDuca H, Stuenkel AJ, Dolinsky JS, et al. Utilization of multigene panels in hereditary cancer predisposition testing: analysis of more than 2,000 patients. Genet Med. 2014;16: Kurian AW, Hare EE, Mills MA, et al. Clinical evaluation of a multiple-gene sequencing panel for hereditary cancer risk assessment. J Clin Oncol. 2014;32: Tung N, Battelli C, Allen B, et al. Frequency of mutations in individuals with breast cancer referred for BRCA1 and BRCA2 testing using next-generation sequencing with a 25-gene panel. Cancer. 2015;121: Yorczyk A, Robinson LS, Ross TS. Use of panel tests in place of single gene tests in the cancer genetics clinic. Clin Genet. 2015;88: King MC, Levy-Lahad E, Lahad A. Population-based screening for BRCA1 and BRCA2: 2014 Lasker Award. JAMA. 2014;312: Hartmann LC, Lindor NM. The role of risk-reducing surgery in hereditary breast and ovarian cancer. N Engl J Med. 2016;374: Pierce LJ, Haffty BG. Radiotherapy in the treatment of hereditary breast cancer. Semin Radiat Oncol. 2011;21: Sikov WM. Assessing the role of platinum agents in aggressive breast cancers. Curr Oncol Rep. 2015;17: Livraghi L, Garber JE. PARP inhibitors in the management of breast cancer: current data and future prospects. BMC Med. 2015;13: Euhus DM, Smith KC, Robinson L, et al. Pretest prediction of BRCA1 or BRCA2 mutation by risk counselors and the computer model BRCAPRO. J Natl Cancer Inst. 2002;94: American College of Surgeons. Cancer. Accessed July 17, Nelson HD, Fu R, Goddard K, et al. Risk assessment, genetic counseling, and genetic testing for BRCA-related cancer: Systematic Review to Update the U.S. Preventive Services Task Force Recommendation. Evidence Syntheses, No Accessed July 17, Richards S, Aziz N, Bale S, et al. Standards and guidelines for the interpretation of
10 sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17: This statement was developed by the Society s Research committee, and on March 14, 2017, was approved by the Board of Directors.
Consensus Guideline on Genetic Testing for Hereditary Breast Cancer
 Consensus Guideline on Genetic Testing for Hereditary Breast Cancer Purpose: To outline recommendations for genetic testing that medical professionals can use to assess hereditary risk for breast cancer
Consensus Guideline on Genetic Testing for Hereditary Breast Cancer Purpose: To outline recommendations for genetic testing that medical professionals can use to assess hereditary risk for breast cancer
Hereditary Breast and Ovarian Cancer Rebecca Sutphen, MD, FACMG
 Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
Hereditary Breast and Ovarian Cancer 2015 Rebecca Sutphen, MD, FACMG Among a consecutive series of 11,159 women requesting BRCA testing over one year, 3874 responded to a mailed survey. Most respondents
Identification of patients suggestive of hereditary breast and ovarian cancer syndrome that warrants further professional evaluation.
 Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
Allina Breast Program Committee Consensus Guidelines These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes are not clearly desirable to all patients Identification
Management of BRCA Positive Breast Cancer. Archana Ganaraj, MD February 17, 2018 UPDATE ON WOMEN S HEALTH
 Management of BRCA Positive Breast Cancer Archana Ganaraj, MD February 17, 2018 UPDATE ON WOMEN S HEALTH The number of American women who have lost their lives to breast cancer outstrips the total number
Management of BRCA Positive Breast Cancer Archana Ganaraj, MD February 17, 2018 UPDATE ON WOMEN S HEALTH The number of American women who have lost their lives to breast cancer outstrips the total number
6/8/17. Genetics 101. Professor, College of Medicine. President & Chief Medical Officer. Hereditary Breast and Ovarian Cancer 2017
 Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
Genetics 101 Hereditary Breast and Ovarian Cancer 2017 Rebecca Sutphen, MD, FACMG Professor, College of Medicine President & Chief Medical Officer INVASIVE CANCER GENETICALLY ALTERED CELL HYPERPLASIA DYSPLASIA
Assessment and Management of Genetic Predisposition to Breast Cancer. Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18
 Assessment and Management of Genetic Predisposition to Breast Cancer Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18 Overview The role of the Cancer Genetics team NICE guidelines for Familial Breast
Assessment and Management of Genetic Predisposition to Breast Cancer Dr Munaza Ahmed Consultant Clinical Geneticist 2/7/18 Overview The role of the Cancer Genetics team NICE guidelines for Familial Breast
Why Test for Hereditary Cancer in Preventive Care?
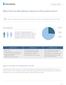 Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Reference #: SYS-PC-VPCI-CG-002. Origination Date: June 2012 Next Review Date: April 2019 Effective Date: April 2016
 Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
Oncology Service Line-Allina Health System-wide Consensus Guidelines: Identification of Breast Cancer Patients at Risk for Inherited Cancer Risks These guidelines apply to clinical interventions that have
Use of panel tests in place of single gene tests in the cancer genetics clinic
 Clin Genet 2015: 88: 278 282 Printed in Singapore. All rights reserved CLINICAL GENETICS doi: 10.1111/cge.12488 Short Report se of panel tests in place of single gene tests in the cancer genetics clinic
Clin Genet 2015: 88: 278 282 Printed in Singapore. All rights reserved CLINICAL GENETICS doi: 10.1111/cge.12488 Short Report se of panel tests in place of single gene tests in the cancer genetics clinic
BRCAplus. genetic testing for hereditary breast cancer
 BRCAplus genetic testing for hereditary breast cancer Developed in collaboration with Fox Chase Cancer Center and the Arcadia University Genetic Counseling Program. Causes of Hereditary Breast Cancer familial
BRCAplus genetic testing for hereditary breast cancer Developed in collaboration with Fox Chase Cancer Center and the Arcadia University Genetic Counseling Program. Causes of Hereditary Breast Cancer familial
Multigene Panel Testing for Hereditary Cancer Risk
 Multigene Panel Testing for Hereditary Cancer Risk Dana Zakalik, M.D. Director, Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Annual Meeting November 4, 2015 Outline
Multigene Panel Testing for Hereditary Cancer Risk Dana Zakalik, M.D. Director, Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Annual Meeting November 4, 2015 Outline
Predictive and Diagnostic Testing for Cancer in Women. Aparna Rajadhyaksha MD
 Predictive and Diagnostic Testing for Cancer in Women Aparna Rajadhyaksha MD Hereditary Cancer s in Women BRCA1 &2 Other Breast Cancer Genes Li Fraumeni PTEN CHEK2 BRCA1&2 t BRCA1 is part of a complex
Predictive and Diagnostic Testing for Cancer in Women Aparna Rajadhyaksha MD Hereditary Cancer s in Women BRCA1 &2 Other Breast Cancer Genes Li Fraumeni PTEN CHEK2 BRCA1&2 t BRCA1 is part of a complex
Importance of Family History in Gynecologic Cancer Prevention. Objectives. Genetic Counselors. Angela Thompson, MS, CGC
 Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Importance of Family History in Gynecologic Cancer Prevention Angela Thompson, MS, CGC Genetic Counselor Froedtert & The Medical College of Wisconsin Objectives Introduce role of genetic counselor Discuss
Assessing Your Patient s Breast Cancer Risk: Is Genetic Testing Necessary?
 May 16, 2016 Assessing Your Patient s Breast Cancer Risk: Is Genetic Testing Necessary? Presenter: Emily Kuchinsky, MS, CGC 1 Experiences with Genetic Testing Adverse Events in Cancer Genetic Testing:
May 16, 2016 Assessing Your Patient s Breast Cancer Risk: Is Genetic Testing Necessary? Presenter: Emily Kuchinsky, MS, CGC 1 Experiences with Genetic Testing Adverse Events in Cancer Genetic Testing:
GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER. Dr Abhijit Dixit. Family Health Clinical Genetics
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review
GENETIC MANAGEMENT OF A FAMILY HISTORY OF BREAST AND / OR OVARIAN CANCER Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review
Genetic Testing: who, what, why?
 Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
Genetic Testing: who, what, why? Gina Westhoff MD LMG Gynecologic Oncology March 16, 2019 Disclosures Speaker for Merck (unrelated to today s topic) Objectives Determine who should undergo genetic risk
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor/Cancer Risk Counselor Banner Good Samaritan Cancer Screening & Prevention Program Objectives Describe the role
Hereditary Breast and Ovarian Cancer Screening & Genetic Counseling
 Hereditary Breast and Ovarian Cancer Screening & Genetic Counseling Cecelia Bellcross, PhD, MS, CGC Emory University School of Medicine Department of Human Genetics The First Line of Defense February 21,
Hereditary Breast and Ovarian Cancer Screening & Genetic Counseling Cecelia Bellcross, PhD, MS, CGC Emory University School of Medicine Department of Human Genetics The First Line of Defense February 21,
GENETIC TESTING FOR HEREDITARY CANCER
 UnitedHealthcare Oxford Clinical Policy GENETIC TESTING FOR HEREDITARY CANCER Policy Number: DIAGNOSTIC 004.27 T2 Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
UnitedHealthcare Oxford Clinical Policy GENETIC TESTING FOR HEREDITARY CANCER Policy Number: DIAGNOSTIC 004.27 T2 Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS
Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective
 Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective Sarah L. Campian, MS CGC Certified Genetic Counselor Nancy & James Grosfeld Cancer Genetics Center Objectives Identify patients/families
Germline Multigene Panel Testing in Oncology: Genetic Counseling Perspective Sarah L. Campian, MS CGC Certified Genetic Counselor Nancy & James Grosfeld Cancer Genetics Center Objectives Identify patients/families
GYNplus. genetic testing for hereditary ovarian and/or uterine cancer
 GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
GYNplus genetic testing for hereditary ovarian and/or uterine cancer What Are the Causes of Hereditary Ovarian and Uterine Cancer? uterine cancer ovarian cancer sporadic 70-80% hereditary 5% Lynch syndrome
P NK. Breast Cancer Genetic Risk Test. Test Report
 Test Report CONTENTS SECTION 1 1-1. Patient Information 1-2. Test Report Summary 1-3. Test Report Details 1-4. List of Genes Tested SECTION 2 2-1. About the Test 2-2. References 1-1. Patient Information
Test Report CONTENTS SECTION 1 1-1. Patient Information 1-2. Test Report Summary 1-3. Test Report Details 1-4. List of Genes Tested SECTION 2 2-1. About the Test 2-2. References 1-1. Patient Information
Genetics and Cancer Care. Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP
 Genetics and Cancer Care Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP Faculty/Presenter Disclosure Faculty: Cynthia Forster-Gibson Relationships with commercial interests:
Genetics and Cancer Care Cynthia Forster-Gibson, MD, PhD and Loren Mackay- Loder, MSc Genetics Program, THP Faculty/Presenter Disclosure Faculty: Cynthia Forster-Gibson Relationships with commercial interests:
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer
 GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
GYNplus: A Genetic Test for Hereditary Ovarian and/or Uterine Cancer Causes of Hereditary Ovarian and Uterine Cancer uterine cancer ovarian cancer Sporadic 75-90% Sporadic 70-80% Hereditary, 5% Lynch syndrome
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017
 Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
Hereditary Cancer Update Strengthening Linkages Workshop April 22, 2017 Renée Perrier, MD MSc FRCPC Clinical Assistant Professor University of Calgary, Department of Medical Genetics Medical Director,
Germline Testing for Hereditary Cancer with Multigene Panel
 Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Germline Testing for Hereditary Cancer with Multigene Panel Po-Han Lin, MD Department of Medical Genetics National Taiwan University Hospital 2017-04-20 Disclosure No relevant financial relationships with
Genetic Risk Assessment for Cancer
 Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
Genetic Risk Assessment for Cancer Jennifer Siettmann, MS CGC Certified Genetic Counselor Banner MD Anderson Cancer Center Objectives Describe the role of genetic counseling and genetic testing in patient
BRCA2 gene. Associated Syndrome Name: Hereditary Breast and Ovarian Cancer syndrome (HBOC) BRCA2 Summary Cancer Risk Table. BRCA2 gene Overview
 BRCA gene Associated Syndrome Name: Hereditary Breast and Cancer syndrome (HBOC) BRCA Summary Cancer Risk Table Male Breast GENETIC RISK Female Breast Elevated Risk Elevated Risk BRCA gene Overview Hereditary
BRCA gene Associated Syndrome Name: Hereditary Breast and Cancer syndrome (HBOC) BRCA Summary Cancer Risk Table Male Breast GENETIC RISK Female Breast Elevated Risk Elevated Risk BRCA gene Overview Hereditary
Genetic Determinants, Risk Assessment and Management
 Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer
 Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_breast_and_ovarian_cancer 8/1997 8/2017
Corporate Medical Policy Genetic Testing for Breast and Ovarian Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_breast_and_ovarian_cancer 8/1997 8/2017
Page 1 of 8 TABLE OF CONTENTS
 Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
Page 1 of 8 TABLE OF CONTENTS Patient Evaluation and Recommendation..Page 2 Testing and Follow-up..Page 3 Genetic Counseling Referral Criteria.....Page 4-5 Patient Education..Page 6 Suggested Readings...Page
Germline Genetic Testing for Breast Cancer Risk
 Kathmandu, Bir Hospital visit, August 2018 Germline Genetic Testing for Breast Cancer Risk Evidence-based Genetic Screening Rodney J. Scott Demography in New South Wales (total population ~ 7,000,000)
Kathmandu, Bir Hospital visit, August 2018 Germline Genetic Testing for Breast Cancer Risk Evidence-based Genetic Screening Rodney J. Scott Demography in New South Wales (total population ~ 7,000,000)
Perception of Screening and Risk Reduction Surgeries in Patients Tested for a BRCA Deleterious Mutation
 Perception of Screening and Risk Reduction Surgeries in Patients Tested for a BRCA Deleterious Mutation Jennifer K. Litton, MD 1, Shannon N. Westin, MD 2, Kaylene Ready, CGC 1, Charlotte C. Sun, MD 2,
Perception of Screening and Risk Reduction Surgeries in Patients Tested for a BRCA Deleterious Mutation Jennifer K. Litton, MD 1, Shannon N. Westin, MD 2, Kaylene Ready, CGC 1, Charlotte C. Sun, MD 2,
Breast Cancer Risk Assessment: Genetics, Risk Models, and Screening. Amie Hass, MSN, ARNP, FNP-BC Hall-Perrine Cancer Center
 Breast Cancer Risk Assessment: Genetics, Risk Models, and Screening Amie Hass, MSN, ARNP, FNP-BC Hall-Perrine Cancer Center Disclosure- I DO NOT HAVE any relevant financial interest with any entity producing,
Breast Cancer Risk Assessment: Genetics, Risk Models, and Screening Amie Hass, MSN, ARNP, FNP-BC Hall-Perrine Cancer Center Disclosure- I DO NOT HAVE any relevant financial interest with any entity producing,
Accuracy of the BRCAPRO Model Among Women With Bilateral Breast Cancer
 Accuracy of the BRCAPRO Model Among Women With Bilateral Breast Cancer Kaylene J. Ready, MS 1, Kristen J. Vogel, MS 2, Deann P. Atchley, PhD 1, Kristine R. Broglio, MS 1, Kimberly K. Solomon, MBA 1, Christopher
Accuracy of the BRCAPRO Model Among Women With Bilateral Breast Cancer Kaylene J. Ready, MS 1, Kristen J. Vogel, MS 2, Deann P. Atchley, PhD 1, Kristine R. Broglio, MS 1, Kimberly K. Solomon, MBA 1, Christopher
Prophylactic mastectomy, a look at the problem
 www.clinicaloncology.com.ua 1 Prophylactic mastectomy, a look at the problem I.I.Smolanka, S.Y.Skliar, A.D.Loboda The National Cancer Institute, Kiev Summary: The question of the bilateral prophylactic
www.clinicaloncology.com.ua 1 Prophylactic mastectomy, a look at the problem I.I.Smolanka, S.Y.Skliar, A.D.Loboda The National Cancer Institute, Kiev Summary: The question of the bilateral prophylactic
Approximately 5% to 10% of breast cancer (BC) is hereditary in nature. Since. By Dawna Gilchrist, MD, FRCPC, FCCMG
 By Dawna Gilchrist, MD, FRCPC, FCCMG Approximately 5% to 10% of breast cancer (BC) is hereditary in nature. Since the discovery of the genes BRCA 1 and 2 in the early 1990s, genetic counselling and testing
By Dawna Gilchrist, MD, FRCPC, FCCMG Approximately 5% to 10% of breast cancer (BC) is hereditary in nature. Since the discovery of the genes BRCA 1 and 2 in the early 1990s, genetic counselling and testing
Hereditary Cancer Risk Assessment for Gynecological Cancers. FarrNezhatMD.com
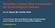 Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
Hereditary Cancer Risk Assessment for Gynecological Cancers FarrNezhatMD.com Image credit: PLOS blogs 5-10% hereditary 10-20% 70-80% sporadic Genetic Changes and Cancer Cancer begins with a genetic
HEREDITY & CANCER: Breast cancer as a model
 HEREDITY & CANCER: Breast cancer as a model Pierre O. Chappuis, MD Divisions of Oncology and Medical Genetics University Hospitals of Geneva, Switzerland Genetics, Cancer and Heredity Cancers are genetic
HEREDITY & CANCER: Breast cancer as a model Pierre O. Chappuis, MD Divisions of Oncology and Medical Genetics University Hospitals of Geneva, Switzerland Genetics, Cancer and Heredity Cancers are genetic
Medical Policy Manual. Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer. Date of Origin: January 27, 2011
 Medical Policy Manual Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer Date of Origin: January 27, 2011 Section: Genetic Testing Last Reviewed Date: July 2014 Policy No: 02 Effective
Medical Policy Manual Topic: Genetic Testing for Hereditary Breast and/or Ovarian Cancer Date of Origin: January 27, 2011 Section: Genetic Testing Last Reviewed Date: July 2014 Policy No: 02 Effective
BRCA Precertification Information Request Form
 BRCA Precertification Information Request Form Failure to complete this form in its entirety may result in the delay of review. Fax to: BRCA Precertification Department Fax number: 1-860-975-9126 Section
BRCA Precertification Information Request Form Failure to complete this form in its entirety may result in the delay of review. Fax to: BRCA Precertification Department Fax number: 1-860-975-9126 Section
No Sib Pair Concordance for Breast or Ovarian Cancer in BRCA1 Mutation Carriers
 Hereditary Cancer in Clinical Practice 2007; 5(2) pp. 67-71 No Sib Pair Concordance for Breast or Ovarian Cancer in BRCA1 Mutation Carriers Pål Møller 1, Lovise Mºhle 1, Neal Clark 1, Jaran Apold 2 1 Section
Hereditary Cancer in Clinical Practice 2007; 5(2) pp. 67-71 No Sib Pair Concordance for Breast or Ovarian Cancer in BRCA1 Mutation Carriers Pål Møller 1, Lovise Mºhle 1, Neal Clark 1, Jaran Apold 2 1 Section
Does Cancer Run in Your Family?
 Does Cancer Run in Your Family? A Patient s Guide to Hereditary Breast and Ovarian Cancer Syndrome What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that
Does Cancer Run in Your Family? A Patient s Guide to Hereditary Breast and Ovarian Cancer Syndrome What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that
A Patient s Guide to Hereditary Cancer. Is Hereditary Cancer Testing Right for You?
 A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
A Patient s Guide to Hereditary Cancer Is Hereditary Cancer Testing Right for You? What is Hereditary Cancer? Most cancers occur in people who do not have a strong family history of that cancer. This is
Genetic Panel Testing and Implications for Cancer Care
 Genetic Panel Testing and Implications for Cancer Care Dana Zakalik, M.D. Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Board of Directors Meeting September 28, 2016
Genetic Panel Testing and Implications for Cancer Care Dana Zakalik, M.D. Nancy and James Grosfeld Cancer Genetics Center Professor, OUWB Medical School MCC Board of Directors Meeting September 28, 2016
Cancer Genomics 101. BCCCP 2015 Annual Meeting
 Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
The best way of detection of and screening for breast cancer in women with genetic or hereditary risk
 The best way of detection of and screening for breast cancer in women with genetic or hereditary risk Ingrid Vogelaar Introduction Each year almost 1.2 million women are diagnosed with breast cancer worldwide.
The best way of detection of and screening for breast cancer in women with genetic or hereditary risk Ingrid Vogelaar Introduction Each year almost 1.2 million women are diagnosed with breast cancer worldwide.
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME E GEN DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME DNA PROTEIN. A gene is made up of DNA. It carries instructions to make proteins.
 WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
WHAT IS A GENE? CHROMOSOME GENE DNA A gene is made up of DNA. It carries instructions to make proteins. The proteins have specific jobs that help your body work normally. PROTEIN 1 WHAT HAPPENS WHEN THERE
OBJECTIVES 8/25/2017. An attempt to organize the chaos
 High Risk for Breast Cancer and Genetics: Who? What? Where? When? An attempt to organize the chaos Presented at Winds of Change Conference November 3, 2017 by Carol Hager, MSN, CRNP and Allison Haener,
High Risk for Breast Cancer and Genetics: Who? What? Where? When? An attempt to organize the chaos Presented at Winds of Change Conference November 3, 2017 by Carol Hager, MSN, CRNP and Allison Haener,
Updates in Cancer Genetics & Genomics
 Updates in Cancer Genetics & Genomics Jennifer R. Klemp, PhD, MPH, MA Associate Professor of Medicine, Division of Clinical Oncology Director, Cancer Survivorship Co-Program Leader, Cancer Prevention and
Updates in Cancer Genetics & Genomics Jennifer R. Klemp, PhD, MPH, MA Associate Professor of Medicine, Division of Clinical Oncology Director, Cancer Survivorship Co-Program Leader, Cancer Prevention and
GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T. Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics
 GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics The Medical/Surgical/Radiation Oncologist s View of Genetics Cancer
GEN ETICS AN D GEN OM ICS IN CANCER PREVENTION AN D TREATM EN T Robert Nathan Slotnick MD PhD Director, Medical Genetics and Genomics The Medical/Surgical/Radiation Oncologist s View of Genetics Cancer
So, Who are the appropriate individuals that should consider genetic counseling and genetic testing?
 Hello, I m Banu Arun, Professor of Breast Medical Oncology and Co-Director of Clinical Cancer Genetics at the University of Texas MD Anderson Cancer Center. Today I will be discussing with you Hereditary
Hello, I m Banu Arun, Professor of Breast Medical Oncology and Co-Director of Clinical Cancer Genetics at the University of Texas MD Anderson Cancer Center. Today I will be discussing with you Hereditary
A guide to genetic testing for hereditary cancers
 Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Cancer Testing Solutions A guide to genetic testing for hereditary cancers The benefit of knowing TM Hereditary cancer genetic testing can play a critical role in managing health Cancer touches millions
Germline Mutations Hereditary Breast and Ovarian Cancer Risk and Management Issues
 Germline Mutations Hereditary Breast and Ovarian Cancer Risk and Management Issues Jeffrey N. Weitzel, M.D. Cancer Screening & Prevention Program Timeline of Important Events in DNA Patenting (Top) and
Germline Mutations Hereditary Breast and Ovarian Cancer Risk and Management Issues Jeffrey N. Weitzel, M.D. Cancer Screening & Prevention Program Timeline of Important Events in DNA Patenting (Top) and
GeneHealth BreastGene_New qxp_Layout 1 21/02/ :42 Page 3 BreastGene GeneHealth UK
 GeneHealth BreastGene_New 8.2.17.qxp_Layout 1 21/02/2017 16:42 Page 3 BreastGene GeneHealth UK BreastGene What is hereditary breast cancer? Breast cancer is the most common cancer in the UK. Unfortunately
GeneHealth BreastGene_New 8.2.17.qxp_Layout 1 21/02/2017 16:42 Page 3 BreastGene GeneHealth UK BreastGene What is hereditary breast cancer? Breast cancer is the most common cancer in the UK. Unfortunately
Objectives. Case Study #1 1/28/14. A Collaborative Practice Approach to Genetic Testing in Cancer: Translating Science Into Clinical Practice
 A Collaborative Practice Approach to Genetic Testing in Cancer: Translating Science Into Clinical Practice Heather Hampel, MS, CGC Associate Director, Division of Human Genetics Professor, Department of
A Collaborative Practice Approach to Genetic Testing in Cancer: Translating Science Into Clinical Practice Heather Hampel, MS, CGC Associate Director, Division of Human Genetics Professor, Department of
So, now, that we have reviewed some basics of cancer genetics I will provide an overview of some common syndromes.
 Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Hello. My name is Maureen Mork and I m a Certified Genetic Counselor in the Clinical Cancer Genetics Program at The University of Texas MD Anderson Cancer Center. I ll be lecturing today on the Cancer
Corporate Medical Policy
 Corporate Medical Policy Moderate Penetrance Variants Associated with Breast Cancer in File Name: Origination: Last CAP Review: Next CAP Review: Last Review: moderate_penetrance_variants_associated_with_breast_cancer_
Corporate Medical Policy Moderate Penetrance Variants Associated with Breast Cancer in File Name: Origination: Last CAP Review: Next CAP Review: Last Review: moderate_penetrance_variants_associated_with_breast_cancer_
WHAT DO GENES HAVE TO DO WITH IT? Breast Cancer Risk Assessment and Risk Reduction in 2016
 WHAT DO GENES HAVE TO DO WITH IT? Breast Cancer Risk Assessment and Risk Reduction in 2016 39 th Annual CANP Educational Conference March 17 20, 2016 Collaborate. Educate. Advocate. Karen Herold, DNP,
WHAT DO GENES HAVE TO DO WITH IT? Breast Cancer Risk Assessment and Risk Reduction in 2016 39 th Annual CANP Educational Conference March 17 20, 2016 Collaborate. Educate. Advocate. Karen Herold, DNP,
Primary Care Approach to Genetic Cancer Syndromes
 Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Primary Care Approach to Genetic Cancer Syndromes Jason M. Goldman, MD, FACP FAU School of Medicine Syndromes Hereditary Breast and Ovarian Cancer (HBOC) Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
How to spot heritable breast cancer: A primary care physician s guide
 PERSONALIZING PATIENT CARE CME CREDIT EDUCATIONAL OBJECTIVE: Readers will refer patients for genetic counseling if the personal and family histories suggest they may have an inherited predisposition to
PERSONALIZING PATIENT CARE CME CREDIT EDUCATIONAL OBJECTIVE: Readers will refer patients for genetic counseling if the personal and family histories suggest they may have an inherited predisposition to
MP Genetic Testing for BRCA1 or BRCA2 for Hereditary Breast/Ovarian Cancer Syndrome and Other High-Risk Cancers
 Medical Policy MP 2.04.02 Genetic Testing for BRCA1 or BRCA2 for Hereditary Breast/Ovarian Cancer Syndrome and Other High-Risk BCBSA Ref. Policy: 2.04.02 Last Review: 11/15/2018 Effective Date: 02/15/2019
Medical Policy MP 2.04.02 Genetic Testing for BRCA1 or BRCA2 for Hereditary Breast/Ovarian Cancer Syndrome and Other High-Risk BCBSA Ref. Policy: 2.04.02 Last Review: 11/15/2018 Effective Date: 02/15/2019
Genetic testing for hereditary cancer
 Genetic testing for hereditary cancer THE GENETICS OF HEREDITARY CANCER About half of all men and one-third of all women in the US will develop cancer during their lifetimes. Approximately 5% to 10% of
Genetic testing for hereditary cancer THE GENETICS OF HEREDITARY CANCER About half of all men and one-third of all women in the US will develop cancer during their lifetimes. Approximately 5% to 10% of
Presymptomatic diagnosis of hereditary breast cancer
 Presymptomatic diagnosis of hereditary breast cancer Published Oct 5, 2000 Version 1 Findings by SBU Alert The discovery that mutations in two specific genes increase the risk for breast cancer and ovarian
Presymptomatic diagnosis of hereditary breast cancer Published Oct 5, 2000 Version 1 Findings by SBU Alert The discovery that mutations in two specific genes increase the risk for breast cancer and ovarian
Utilization of BRCA Testing. Breast and Ovarian Cancer in Texas
 Utilization of BRCA Testing in Older Ode Women with Breast and Ovarian Cancer in Texas Ana M. Rodriguez, MD Assistant Professor Department of Obstetrics and Gynecology University of Texas Medical Branch
Utilization of BRCA Testing in Older Ode Women with Breast and Ovarian Cancer in Texas Ana M. Rodriguez, MD Assistant Professor Department of Obstetrics and Gynecology University of Texas Medical Branch
Are you at risk of Hereditary Cancer? Your Guide to the Answers
 Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Are you at risk of Hereditary Cancer? Your Guide to the Answers What is Hereditary Cancer? The genes we are born with may contribute to our risk of developing certain types of cancer, including breast,
Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center
 Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center Following this presentation you will be able to: Identify cancer survivors in your practice who might benefit from genetic counseling
Carol Christianson, MS, CGC Genetic Counselor West Michigan Cancer Center Following this presentation you will be able to: Identify cancer survivors in your practice who might benefit from genetic counseling
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 BRCA1 and BRCA2 Testing Page 1 of 33 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: BRCA1 and BRCA2 Testing Pre-Determination of Services IS REQUIRED by the Member
BRCA1 and BRCA2 Testing Page 1 of 33 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: BRCA1 and BRCA2 Testing Pre-Determination of Services IS REQUIRED by the Member
Genetic Testing For Ovarian Cancer: When, How And Who? Judith Balmaña, MD, PhD University Hospital Vall d Hebron Barcelona, Spain
 Genetic Testing For Ovarian Cancer: When, How And Who? Judith Balmaña, MD, PhD University Hospital Vall d Hebron Barcelona, Spain Why Would We Consider Genetic Testing in Patients With Ovarian Cancer?
Genetic Testing For Ovarian Cancer: When, How And Who? Judith Balmaña, MD, PhD University Hospital Vall d Hebron Barcelona, Spain Why Would We Consider Genetic Testing in Patients With Ovarian Cancer?
BRCA 1/2. Breast cancer testing THINK ABOUT TOMORROW, TODAY
 BRCA 1/2 Breast cancer testing THINK ABOUT TOMORROW, TODAY 5 10% of patients with breast and/or ovarian cancer have a hereditary form1. For any individual carrying a mutation in BRCA1 or BRCA2, the lifetime
BRCA 1/2 Breast cancer testing THINK ABOUT TOMORROW, TODAY 5 10% of patients with breast and/or ovarian cancer have a hereditary form1. For any individual carrying a mutation in BRCA1 or BRCA2, the lifetime
Family Assessment. Objectives. Comprehensive Family History Important Inexpensive Underutilized genetic tool
 Besides the BRCA genes, what else to consider in hereditary breast and ovarian cancer? Laurie M. Connors DNP, APNG, FNP-BC, AGN-BC Objectives Evaluate personal & family history to assess risk for hereditary
Besides the BRCA genes, what else to consider in hereditary breast and ovarian cancer? Laurie M. Connors DNP, APNG, FNP-BC, AGN-BC Objectives Evaluate personal & family history to assess risk for hereditary
JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T
 VOLUME 25 NUMBER 11 APRIL 1 27 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Meta-Analysis of BRCA1 and BRCA2 Penetrance Sining Chen and Giovanni Parmigiani From the Departments of Environmental
VOLUME 25 NUMBER 11 APRIL 1 27 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Meta-Analysis of BRCA1 and BRCA2 Penetrance Sining Chen and Giovanni Parmigiani From the Departments of Environmental
The Genetics of Breast and Ovarian Cancer Prof. Piri L. Welcsh
 The Genetics of Breast Piri L. Welcsh, PhD Research Assistant Professor University of Washington School of Medicine Division of Medical Genetics 1 Genetics of cancer All cancers arise from genetic and
The Genetics of Breast Piri L. Welcsh, PhD Research Assistant Professor University of Washington School of Medicine Division of Medical Genetics 1 Genetics of cancer All cancers arise from genetic and
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2
 GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2 Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific
GENETIC TESTING FOR HEREDITARY BREAST AND OVARIAN CANCER BRCA1 BRCA2 Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific
 Page 1 of 5 Home > Research & Grants > Research and Scientific Programs > What is genetic testing for breast cancer and who should get it? What is genetic testing for breast cancer and who should get it?
Page 1 of 5 Home > Research & Grants > Research and Scientific Programs > What is genetic testing for breast cancer and who should get it? What is genetic testing for breast cancer and who should get it?
HBOC Syndrome A review of BRCA 1/2 testing, Cancer Risk Assessment, Counseling and Beyond.
 HBOC Syndrome A review of BRCA 1/2 testing, Cancer Risk Assessment, Counseling and Beyond. Conni Murphy, ARNP Cancer Risk Assessment and Genetics Program Jupiter Medical Center Learning Objectives Identify
HBOC Syndrome A review of BRCA 1/2 testing, Cancer Risk Assessment, Counseling and Beyond. Conni Murphy, ARNP Cancer Risk Assessment and Genetics Program Jupiter Medical Center Learning Objectives Identify
Managing Moderate Penetrance
 Managing Moderate Penetrance Thomas Slavin, MD, FACMG Assistant Clinical Professor, Department of Medical Oncology, Division of Clinical Cancer Genetics Program Member, Cancer Control and Population Sciences
Managing Moderate Penetrance Thomas Slavin, MD, FACMG Assistant Clinical Professor, Department of Medical Oncology, Division of Clinical Cancer Genetics Program Member, Cancer Control and Population Sciences
Genetic Testing for BRCA1 and BRCA2 Genes
 Genetic Testing for BRCA1 and BRCA2 Genes MP9478 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic counseling
Genetic Testing for BRCA1 and BRCA2 Genes MP9478 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below Pre and post-test genetic counseling
Gynecologic Cancers are many diseases. Gynecologic Cancers in the Age of Precision Medicine Advances in Internal Medicine. Speaker Disclosure:
 Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Advances in Internal Medicine Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Advances in Internal Medicine Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
HBOC. Jessica M. Salamone, ScM, CGC
 HBOC Jessica M. Salamone, ScM, CGC Certified Genetic Counselor Director of the Cancer Risk Assessment & Genetic Counseling Program Elizabeth Wende Breast Care, LLC Elizabeth Wende Breast Care Internationally
HBOC Jessica M. Salamone, ScM, CGC Certified Genetic Counselor Director of the Cancer Risk Assessment & Genetic Counseling Program Elizabeth Wende Breast Care, LLC Elizabeth Wende Breast Care Internationally
Clinical Policy Title: Genetic testing for breast and ovarian cancer
 Clinical Policy Title: Genetic testing for breast and ovarian cancer Clinical Policy Number: 02.01.02 Effective Date: September 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: May
Clinical Policy Title: Genetic testing for breast and ovarian cancer Clinical Policy Number: 02.01.02 Effective Date: September 1, 2013 Initial Review Date: March 21, 2013 Most Recent Review Date: May
Outline. Identifying your risk for hereditary breast or ovarian cancer. Genetics 101. What causes cancer? Genetics
 Identifying your risk for hereditary breast or ovarian cancer David Andorsky, MD Breanna Roscow, MS, CGC 303-993-0161 Outline Genetics and biology of hereditary cancer syndromes BRCA1 and BRCA2 Genetic
Identifying your risk for hereditary breast or ovarian cancer David Andorsky, MD Breanna Roscow, MS, CGC 303-993-0161 Outline Genetics and biology of hereditary cancer syndromes BRCA1 and BRCA2 Genetic
Gynecologic Cancers are many diseases. Speaker Disclosure: Gynecologic Cancer Care in the Age of Precision Medicine. Controversies in Women s Health
 Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Controversies in Women s Health Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
Gynecologic Cancer Care in the Age of Precision Medicine Gynecologic Cancers in the Age of Precision Medicine Controversies in Women s Health Lee-may Chen, MD Department of Obstetrics, Gynecology & Reproductive
WELCOME. Taking Care of Your Health. April 30, 8 am to noon
 WELCOME Taking Care of Your Health April 30, 8 am to noon Cancer: Know Your Risk Emily Kuchinsky, MS, CGC, Certified Genetic Counselor Sporadic Cancer Lifetime Probability- Women Family Cluster Risk factors
WELCOME Taking Care of Your Health April 30, 8 am to noon Cancer: Know Your Risk Emily Kuchinsky, MS, CGC, Certified Genetic Counselor Sporadic Cancer Lifetime Probability- Women Family Cluster Risk factors
The risk of ovarian cancer after breast cancer in BRCA1 and BRCA2 carriers
 Gynecologic Oncology 96 (2005) 222 226 www.elsevier.com/locate/ygyno The risk of ovarian cancer after breast cancer in BRCA1 and BRCA2 carriers Kelly A. Metcalfe a,b, *, Henry T. Lynch c, Parviz Ghadirian
Gynecologic Oncology 96 (2005) 222 226 www.elsevier.com/locate/ygyno The risk of ovarian cancer after breast cancer in BRCA1 and BRCA2 carriers Kelly A. Metcalfe a,b, *, Henry T. Lynch c, Parviz Ghadirian
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian
 Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
Expert Interview: Inherited Susceptibility to Cancer with Dr. Nicoleta Voian ANNOUNCER OPEN: Welcome to CME on ReachMD. This segment, entitled Inherited Susceptibility to Cancer: What Do Primary Care Providers
Inherited Cancer Genomics and Prevention:
 Inherited Cancer Genomics and Prevention: How much cancer risk is inherited? Clinical utility of germline genetic testing in precision prevention and targeted therapy Kenneth Offit MD MPH Chief, Clinical
Inherited Cancer Genomics and Prevention: How much cancer risk is inherited? Clinical utility of germline genetic testing in precision prevention and targeted therapy Kenneth Offit MD MPH Chief, Clinical
Hereditary breast cancer who to refer to a cancer genetics clinic and how to counsel patients with
 Hereditary breast cancer who to refer to a cancer genetics clinic and how to counsel patients with positive and negative results? SAMO Workshop Luzern 3./4.10.2014 Dr. med. Barbara Bolliger TumorTumor-
Hereditary breast cancer who to refer to a cancer genetics clinic and how to counsel patients with positive and negative results? SAMO Workshop Luzern 3./4.10.2014 Dr. med. Barbara Bolliger TumorTumor-
Cancer Survivorship Symposium Cancer and Heredity January 16, Jeanne P. Homer, MS Licensed Certified Genetic Counselor
 Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
Cancer Survivorship Symposium Cancer and Heredity January 16, 2017 Jeanne P. Homer, MS Licensed Certified Genetic Counselor Outline Cancer and Heredity Hereditary Cancer Risk Assessment & Genetic testing
The Next Generation of Hereditary Cancer Testing
 The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
Although multiple factors have been associated with increased
 ARTICLE Evaluation of a breast/ovarian cancer genetics referral screening tool in a mammography population Cecelia A. Bellcross, MS, PhD 1, Amy A. Lemke, MS, PhD 2, Laura S. Pape, MS 3, Angela L. Tess,
ARTICLE Evaluation of a breast/ovarian cancer genetics referral screening tool in a mammography population Cecelia A. Bellcross, MS, PhD 1, Amy A. Lemke, MS, PhD 2, Laura S. Pape, MS 3, Angela L. Tess,
Hereditary Cancer Update: What do GPOs need to know?
 Hereditary Cancer Update: What do GPOs need to know? Mary McCullum, RN, MSN, CON(C) Nurse Educator, Hereditary Cancer Program BC Cancer Agency October 1, 2016 Conflict of Interest Disclosure Nothing to
Hereditary Cancer Update: What do GPOs need to know? Mary McCullum, RN, MSN, CON(C) Nurse Educator, Hereditary Cancer Program BC Cancer Agency October 1, 2016 Conflict of Interest Disclosure Nothing to
Hereditary Breast and Ovarian Cancers: Risk Management Recommendations. Objectives
 Hereditary Breast and Ovarian Cancers: Risk Management Recommendations Tuya Pal, MD Moffitt Cancer Center Objectives 1 Identify genes associated with Hereditary Breast/Ovarian Cancer, including new and
Hereditary Breast and Ovarian Cancers: Risk Management Recommendations Tuya Pal, MD Moffitt Cancer Center Objectives 1 Identify genes associated with Hereditary Breast/Ovarian Cancer, including new and
Risk Assessment, Genetics, and Prevention
 Risk Assessment, Genetics, and Prevention Katherine D. Crew, MD MS Director, Clinical Breast Cancer Prevention Program Columbia University Medical Center 1 Outline Breast cancer risk factors Hereditary
Risk Assessment, Genetics, and Prevention Katherine D. Crew, MD MS Director, Clinical Breast Cancer Prevention Program Columbia University Medical Center 1 Outline Breast cancer risk factors Hereditary
The Value of Panel Testing in Inherited Breast Cancer Risk Assessment. Rodney J. Scott Division of Molecular Medicine
 The Value of Panel Testing in Inherited Breast Cancer Risk Assessment Rodney J. Scott Division of Molecular Medicine Mutation Detection Next Generation DNA sequencing has revolutionised mutation detection
The Value of Panel Testing in Inherited Breast Cancer Risk Assessment Rodney J. Scott Division of Molecular Medicine Mutation Detection Next Generation DNA sequencing has revolutionised mutation detection
patient guide BreastNext genetic testing for hereditary breast cancer Because knowing your risk can mean early detection and prevention
 patient guide BreastNext genetic testing for hereditary breast cancer Because knowing your risk can mean early detection and prevention Know the Basics Breast cancer is the most common cancer in women
patient guide BreastNext genetic testing for hereditary breast cancer Because knowing your risk can mean early detection and prevention Know the Basics Breast cancer is the most common cancer in women
Does Cancer Run in Your Family?
 Does Cancer Run in Your Family? Nancie Petrucelli, MS, CGC Clinical Assistant Professor Certified Genetic Counselor/Coordinator Cancer Genetic Counseling Service Karmanos Cancer Institute Wayne State University
Does Cancer Run in Your Family? Nancie Petrucelli, MS, CGC Clinical Assistant Professor Certified Genetic Counselor/Coordinator Cancer Genetic Counseling Service Karmanos Cancer Institute Wayne State University
Managing patients at genetic risk of breast cancer
 REVIEW EDUCATIONAL OBJECTIVE: Readers will recognize the risk of breast cancer in patients with hereditary cancer syndromes and arrange appropriate referrals for them HOLLY J. PEDERSON, MD Director, Medical
REVIEW EDUCATIONAL OBJECTIVE: Readers will recognize the risk of breast cancer in patients with hereditary cancer syndromes and arrange appropriate referrals for them HOLLY J. PEDERSON, MD Director, Medical
