Original Article Negative progesterone receptor status is an adverse prognostic factor for luminal B breast cancer
|
|
|
- Abigail Briggs
- 6 years ago
- Views:
Transcription
1 Int J Clin Exp Pathol 2017;10(2): /ISSN: /IJCEP Original Article Negative progesterone receptor status is an adverse prognostic factor for luminal B breast cancer Fan Wu, Weiwei Huang, Kan Chen, Nani Li, Jian Liu Department of Medical Oncology, Fujian Cancer Hospital, Fujian Medical University Cancer Hospital, Fuzhou, Fujian Province, China Received September 22, 2016; Accepted November 4, 2016; Epub February 1, 2017; Published February 15, 2017 Abstract: Progesterone receptor (PR) is involved in tumor but its prognostic value in breast cancer remains unclear. This study aimed to investigate whether PR status is a prognostic factor for luminal B breast cancer. Total 209 patients with invasive breast cancer were enrolled. We found that PR-negative luminal B breast cancer was significantly associated with older age. PR-negative subgroup showed significantly worse median disease-free survival (mdfs) than PR-positive subgroup with a hazard ratio (HR) of 1.80 (95% confidence interval [CI] ). PRnegative subgroup also had an increased risk for non-visceral metastases (HR=2.17, 95% CI ) as well as a trend toward higher risk for locoregional relapse (HR=2.23, 95% CI ), compared to PR-positive subgroup. Furthermore, in HER2-negative patients, the HRs for mdfs, non-visceral metastases, and locoregional relapse were 2.54 (95% CI: ), 2.79 (95% CI: ), and 4.23 (95% CI: ), respectively. Multivariate analysis showed that PR-negative status, lymph node positive cancer, and not receiving adjuvant radiotherapy were associated with reduced DFS and increased risk for non-visceral metastases and locoregional relapse. For patients with radiotherapy, PR-negative status remained a significant predictor of all outcomes, with HRs of 1.89 (95% CI: ), 2.67 (95% CI: ), and 2.47 (95% CI: ) for DFS, non-visceral metastases, and locoregional relapse, respectively. In conclusion, PR-negative status is an independent adverse prognostic factor for luminal B breast cancer. Keywords: Progesterone receptor, luminal B, breast cancer, prognostic factor Introduction Breast cancer is known to be a heterogeneous disease and can be divided into four molecular subtypes: luminal A, luminal B, HER2-enriched, and basal-like (triple negative) [1]. The evaluation of estrogen receptor (ER), progesterone receptor (PR), Ki-67, and HER2 by immunohistochemistry (IHC) has been used to identify the molecular subtypes of breast cancer [2, 3]. Luminal subtype breast cancers are proven to have better prognosis than HER2 and triple negative subtypes due to the expression of ER-associated genes and hormone receptor dependency. Luminal A is defined as ER-positive, PR-positive, HER2-negative, and low Ki- 67 expression, and has the best prognosis of the four subtypes. However, luminal B breast cancer is more aggressive and is characterized by increased expression of HER2-associated genes, as well as high expression of a proliferation signature, including genes such as CCNB1, MKI67, and MYBL [4]. Moreover, compared to luminal A, luminal B subtype is more complicated and heterogeneous because it includes PR negative or positive and HER2 negative or positive patients and those with different Ki-67 levels, with various clinical disease courses and outcomes. Therefore, it is important to identify prognostic factors of luminal B breast cancer to achieve the best possible treatment for individual patients. Young age, large tumor size, high tumor grade, lymphovascular invasion, cancer-positive lymph-nodes, cancer-positive margins, HER2 overexpression, and high recurrence risk based on multi-gene-expression assays, along with ER-negative/PR-negative status are generally considered poor prognosis factors for breast
2 cancer and have been used to guide clinical management [5]. However, the prognostic implication of PR in ER-positive/HER2-negative breast cancer remains unclear. Some studies indicated the possibility that low or negative expression of PR may be an independent prognosis factor in ER-positive breast cancer [6, 7]. However, these studies either focused on HER2-negative luminal B cohorts or undervalued the bias from the treatment of patient subgroups. In addition, little is known about the risk of visceral metastases. Therefore, this study aimed to evaluate the prognostic implication of PR status in luminal B breast cancer by comparing both HER2-negative (luminal B1) and HER2-positive (luminal B2) subtypes. Because not all patients received treatments such as radiotherapy, we analyzed prognostic factors in subgroups receiving different treatments to avoid treatment bias. Materials and methods Patient selection and classification The study cohort included 209 women with invasive breast cancer who received breast surgery at the Fujian Cancer Hospital, between January 2005 and June Male patients or patients with prior malignancy, synchronous bilateral breast cancer, and treatment with preoperative systemic therapy were excluded. Data on medical history, concurrent diseases, age, surgical information, pathological evaluation, and staging procedures such as chest radiographs or computed tomography (CT) scan, upper abdominal ultrasound examination, and bone scan were retrieved retrospectively. We compared two subgroups of luminal B breast cancer: luminal B1 and luminal B2. In this study, luminal B1 was defined as ER positive, PR positive or negative, HER2 negative, as well as Ki-67 14% (when PR is positive). Luminal B2 was defined as ER positive, PR positive or negative, HER2 positive (over-expressed and/or amplified), and any Ki-67 [8, 9]. ERnegative and PR-positive patients were excluded because many studies showed that there was actually no such phenotype in breast cancer [10, 11]. Tumors were classified histologically according to the World Health Organization Classification of Tumors [12]. Tumor staging was assessed according to the guide of American Joint Committee on Cancer (AJCC) [13]. Formalin-fixed, paraffin-embedded tissue samples were subjected to IHC staining for ER, PR, HER2, with primary antibodies against ER (SP1, Dako, Denmark), PR (PgR 636, Dako, Denmark), HER2 (4B5, Roche, Switzerland), and Ki67 (MIB-1, Dako, Denmark). IHC staining was routinely carried out by using Ventana BenchMark XT system (Ventana Medical Systems, Tucson, AZ, USA). All procedures were performed in the BenchMark automatically. A fluorescence in situ hybridization (FISH) test for HER2 gene amplification was performed when HER2 was IHC 2+ by using the PathVysion HER-2 DNA FISH Kit (Vysis Inc, Downers Grove, IL) following the manufacturer s instructions. ER and PR positive status was defined as the presence of greater than 1% of tumor cells with nuclear staining. Ki-67 index was expressed as the percentage of cells with positive nuclear staining among at least 1000 invasive cells in the area scored. HER2 over-expression (3+) was defined as complete and intense circumferential membrane staining of tumor cells. Tumor cells with weak to moderate circumferential membrane immunoreactivity were defined as HER2 (2+) and further examined by FISH for gene amplification. HER2 0 was defined as no staining, and 1+ was defined as incomplete membrane staining that was faint/barely perceptible and within >10% of the invasive tumor cells [14]. Patients were considered HER2- positive if they were either IHC 3+ or IHC 2+ with a FISH test showing HER-2 amplification. Treatment Of 209 patients, all of them received hormonal therapy and 207 patients received adjuvant chemotherapy. A total of 104 out of 209 patients received adjuvant radiation therapy, and 70 of 84 HER2-positive patients received adjuvant trastuzumab treatment. Follow-up Patients were followed up every 3 months after the completion of chemotherapy or radiotherapy. For patients lost to follow-up at our hospital, attempts were made to obtain information via telephonic contact. In total, 15 patients (7%) were lost to follow-up, and we censored these 902 Int J Clin Exp Pathol 2017;10(2):
3 Figure 1. Histological and immunohistochemical analysis of breast cancer tiisues. A. HE staining of PR-positive tissue. B. PR staining of PR-positive tissue. C. HE staining of PR-negative tissue. D. PR staining of PR-negative tissue. Magnification: 100. patients in the analysis. Latest follow-up was at the end of December Median follow-up time was 31 months (range 1 to 109 months). Disease free survival (DFS) was defined as the time from the date of diagnosis to the first event (relapse or metastasis or death). This retrospective study has been approved by the Ethical Committees of Fujian Cancer Hospital. Statistics The chi-square test or the Fisher s exact test was used to assess the distribution of baseline characteristics between the PR-negative and PR-positive subgroups. Survival plots and cumulative incidences were drawn using the Kaplan-Meier method. The univariate analysis of the prognosis differences between the subgroups was conducted by using the Logrank test. A Cox multivariate regression model was used to identify clinicopathological factors affecting the prognosis in the entire cohort and subgroups, using multivariate analysis. The major covariables were age, surgeon type, histologic type, tumor size, lymph node status, HER2 status, Ki-67% staining, radiotherapy, and trastuzumab treatment. Only patients with information for all of the covariates metastases included all sites of recurrence except locoregional relapses and contralateral breast cancer as the first of subsequent events [17]. Results were included in the Cox regression analyses. Results that had p-value <0.05 were statistically significant. SPSS 19.0 software was used for statistical analysis. The primary end-points were DFS, incidence of non-visceral metastases, visceral metastases, locoregional relapse, and distant metastases [15, 16]. Non-visceral metastasis is defined as cancer spread to the soft tissues, lymph nodes, or bone, while visceral metastasis involves the visceral organs, such as the liver, lung, brain, and pleura. Locoregional relapse is defined as breast cancer recurrence in the ipsilateral breast or axillary lymph nodes, or in the chest wall and skin of the ipsilateral breast. Distant Relationship between clinicopathologic characteristics and PR expression Typical histological and immunohistochemical staining of PR-negative and PR-positive cancers were shown in Figure 1. Patients characteristics are shown in Table 1. PR-negative luminal B breast cancer was associated with older age (48.5 vs. 43.0), and there were less young patients (<40 years) in the PR-negative subgroup than the PR-positive subgroup (18.0% vs. 37.1%). There was no correlation among PR status and surgeon type, histologic type, tumor size, lymph node status, TNM stage, HER2 status, or Ki-67% staining. A total of 207 patients received chemotherapy and 104 (49.8%) patients received adjuvant radiotherapy, as well as 70 (33.5%) patients received adjuvant trastuzumab treatment across the entire cohort. No differences were observed in the distribution of adjuvant chemotherapy, adjuvant radiotherapy, and trastuzum- 903 Int J Clin Exp Pathol 2017;10(2):
4 Table 1. Baseline characteristics between PR negative and positive subgroups Characteristics PR negative N=50 PR positive N=159 n % n % Median age (y) 48.5 ( ) 43.0 ( ) Young age (<40 y) Yes No Surgeon type Mastectomy Conservative Histologic type Ductal Lobular Tumor size T T T T Lymph node status Negative Positive Positive lymph node numbers TNM stage I II III HER2 status Negative Positive Unknown Ki-67% staining < > Unknown Adjuvant chemotherapy Yes No Adjuvant radiotherapy Yes No Trastuzumab treatment Yes No P ab treatment among the PR-negative and PR-positive subgroups. Relationship between PR status and patient outcomes On the univariate analysis, the PR-negative luminal B breast cancer subgroup showed worse DFS when compared to the PR-positive subgroup, with a mdfs of 45 months (95% CI: ) vs. 65 months (95% CI: ) (logrank P=0.037), and a HR of 1.80 (95% CI ) across the entire cohort. At 3 and 5 years, patients with PR-negative tumors had a DFS rate of 63.7% (95% CI: ) and 37.0% (95% CI: ), and patients with PR-positive tumors had a DFS rate of 70.2% (95% CI: ) and 50.7% (95% CI: ), respectively. Survival plots of the two subgroups are shown in Figure 2. Moreover, the PR-negative subgroup had an increased risk for non-visceral metastases when compared to the PR-positive subgroup, with a HR of 2.17 ( ) (P= 0.018) (Figure 3). There was no difference in risk for visceral metastases (P=0.685). As for the endpoints of locoregional relapse or distant metastases, the PR-negative subgroup showed a trend toward higher risk compared to the PR-positive subgroup, with a HR of 2.23 ( ) for locoregional relapse (P=0.058) 904 Int J Clin Exp Pathol 2017;10(2):
5 ) (P=0.044) (Figure 6). No differences between groups were observed for visceral metastases (P=0.159). Furthermore, the PR negative-subgroup had a higher risk of locoregional relapse when compared to the PRpositive subgroup, with a HR 4.23 (95% CI ) (P=0.022) (Figure 7), but no differences between groups were observed for distant metastases (P=0.204). Figure 2. DFS of luminal B breast cancer according to PR status. For 84 HER2-positive patients (luminal B2 subtype), there was no difference in mdfs between the PR-negative and the PR-positive subgroups (log-rank P=0.803). There was also no difference in risk for non-visceral or visceral metastases (P=0.382, 0.506) or in risk for locoregional relapse or distant metastases (P=0.842, 0.873). Figure 3. Non-visceral metastases in luminal B breast cancer according to PR status. (Figure 4), but there was no difference in risk for distant metastases (P=0.251). To further analyze the prognostic effect of PR, we divided the entire cohort into 2 subtypes: the luminal B1 subtype (HER2-negative) and the luminal B2 subtype (HER2-positive). Among 118 HER2-negative patients, the PRnegative subgroup showed worse mdfs compared to the PR-positive subgroup, with a HR of 2.54 (95% CI: ). The mdfs of the PR-negative subgroup was 45 months (95% CI ), however the mdfs of the PRpositive subgroup was unreached (log-rank P=0.014) (Figure 5). In addition, the PR-negative subgroup showed a higher risk of non-visceral metastases when compared to the PRpositive subgroup, with a HR of 2.79 (95% CI Multivariate analysis showed that PR-negative status (HR=1.89, 95% CI ), lymph node positive status (HR=3.82, 95% CI ), and not receiving adjuvant radiotherapy (HR=2.84, 95% CI ) were parame- ters associated with an increased risk for worse DFS, as well as for non-visceral metastases and locoregional relapse. Tumor size had a marginal increased risk with respect to worse DFS, but not with respect to non-visceral metastases or locoregional relapse. However, Ki- 67 (cutoff point 20%) seemed to be an insignificant covariate with all outcomes, including DFS, non-visceral metastases, and locoregional relapse (Table 2). Since only some of the patients who were stage T3/4 or lymph node positive needed to receive radiotherapy, we further performed Cox analysis of patients who received radiotherapy to avoid treatment bias. PR-negative status remained a significant predictor of all outcomes considered in this subgroup, with HRs of 2.99 (95% CI ), 3.76 (95% CI ), 905 Int J Clin Exp Pathol 2017;10(2):
6 Figure 4. Locoregional relapse in luminal B breast cancer according to PR status. However, of the four subtypes of breast cancer, luminal B is the most heterogeneous, comprising a group of patients with ER-positive, PR positive or negative, HER2 positive or negative, and different Ki-67 level statuses. Endocrine therapy is essential for the luminal B subtype, and trastuzumab is needed for patients with HER2-positive status. However, there is still a lack of consensus about using chemotherapy for patients with luminal B cancer. It is important to find prognostic factors that will help physicians chose treatment for this subtype. Here we focus on PR status, which may have prognostic significance [21]. Figure 5. DFS of HER2-negative luminal B (luminal B1) breast cancer according to PR status. and 6.32 (95% CI ) for worse DFS, non-visceral metastases, and locoregional relapse, respectively. However, tumor size, Ki-67 status, and lymph node status did not increase the risk for worse DFS, non-visceral metastases, or locoregional relapse in patients who received radiotherapy (Table 3). Discussion It is widely accepted that different clinical and pathological characteristics combined with multi-parameter gene expression profiling provide useful prognostic information for patients with breast cancer [18-20]. Physicians should consider tailoring different treatments to various distinct subtypes of patients in order to make an appropriate therapeutic choice. Previous studies have shown that PR-negative breast cancers are more frequent in postmenopausal patients [22]. In our study, we also find PR-positive expression is more likely in young women. Distributions of other baseline characteristics between PR-negative and PR-positive groups show no difference, which indicates that the characteristics are tolerably bal- anced between the two subgroups. PR is an ER-induced gene target, so the different distribution of PR may be due to estrogen-mediated PR transcriptional activity caused by high level of estrogen in young women [23, 24]. However, whether PR is a prognostic factor still remains unclear because different studies show inconsistent results. Cuzick et al. showed that PR-negative status was a poor prognostic factor for distant recurrences in both univariate and multivariate analysis models [3]. Other studies reported that PR negativity was significantly associated with a poor prognosis in luminal B breast cancer, mostly in HER2-negative subgroup [6, 25], but another study did not support that PR was one of the adverse prognostic factors for breast cancer [26]. 906 Int J Clin Exp Pathol 2017;10(2):
7 Figure 6. Non-visceral metastases in HER2-negative luminal B (luminal B1) breast cancer according to PR status. Figure 7. Locoregional relapse in HER2-negative luminal B (luminal B1) breast cancer according to PR status. From the univariate analysis in our study, we observed that PR-negative patients had poorer survival than PR-positive patients did, across the luminal B cohort (HR 1.80, 95% CI ), but particularly in the luminal B1 subtype (HR 2.54, 95% CI ) rather than the luminal B2 subtype. Increased risk of nonvisceral metastases and locoregional relapse were also observed in the PR-negative luminal B1 subtype. These results are consistent with previous studies [6, 25]. For those patients with luminal B2 subtype, the prognostic role of PR may be weaken by an over-activated HER2 pathway, which down-regulates PR expression [22, 27]. Furthermore, our study suggests that PR is an important independent prognostic factor, and that performing multivariate analysis could properly define subgroups with distinct prognoses in luminal B breast cancer patients to inform treatment choices. Other poor prognostic factors include positive lymph nodes and not receiving adjuvant radiotherapy. In addition, our data show that PR-negative status indicates a higher risk of non-visceral metastases and locoregional relapse, which is seldom reported in other papers. It has been confirmed that the survival time is lower for patients who develop visceral metastases or distant recurrences than those who develop non-visceral metastases or local relapse, and those with visceral metastases are often regarded as less likely to respond to hormonal therapy than those with nonvisceral metastases; consequently such patients tend to receive chemotherapy [28]. This may explain why a PRnegative status modestly increases the risk when compared with the presence of positive lymph nodes or having received radiotherapy. To avoid the bias of adjuvant radiotherapy, which is only needed in particular patient groups, but not in the entire cohort, multivariate Cox s analysis was performed for patients who received radiotherapy. The results showed that PR status is the only prognostic factor in luminal B breast cancer. PR mediates progesterone s effects on the development of mammary gland and breast cancer [29]. The predictive value of PR has been described as the dependence of PR expression on a functional ER and PR pathway, and the loss of PR indicates nonfunctional ER signaling and resistance to hormonal therapy [30, 31]. Other studies indicate that ER downregulates PR expression through crosstalking with other signaling pathways. Previous studies have also shown that high growth factor signaling may be associated with decreased PR expression through the PI3K/Akt/mTOR signal- 907 Int J Clin Exp Pathol 2017;10(2):
8 Table 2. Multivariate analysis for DFS, non-visceral metastases and locoregional relapse in luminal B breast cancer patients Risk factor DFS Non-visceral metastases Locoregional relapse HR 95% CI P HR 95% CI P HR 95% CI P PR Positive Negative Ki-67 staining <20% % Tumor size T T Lymph node status Negative Positive Adjuvant radiotherapy Yes No Table 3. Multivariate analysis for DFS, non-visceral metastases and locoregional relapse in luminal B breast cance patients with adjuvant radiotherapy Risk factor DFS Non-visceral metastases Locoregional relapse HR 95% CI P HR 95% CI P HR 95% CI P PR Positive Negative Ki-67 staining <20% % Tumor size T T Lymph node status Negative Positive ing cascade [22, 32], Loss of Phosphatase and tensin homolog (PTEN), which is a negative regulator of this pathway, is also associated with down-regulation of PR [33]. More recently, data show that PR can interact with ER by re-directing ER chromatin binding and altering the expression of target genes, which is associated with low tumorgenicity and better prognosis [21]. Hence, increases in growth factor activity may be a mechanism that results in ER-positive/PRnegative breast cancer and causes anti-estrogen therapy resistance or insensitivity. Combination use of anti-estrogen therapy (e.g. TAM, aromatase inhibitors, fulvestrant, or ovarian ablation) and mtor inhibitor (e.g. everolimus) or PIK3CA inhibitors may be a promising solution [34-36]. In contrast, anti-estrogen therapy combined with native progesterone may improve drug efficacy in ER-positive/PR-positive breast cancer [37]. There are several limitations to this study. First, it is a retrospective analysis and must be interpreted with caution because of the increased 908 Int J Clin Exp Pathol 2017;10(2):
9 likelihood of false-positive and false-negative results. Second, the sample size of this study is not enough to draw a convincing result, and the relatively small numbers in certain subgroups widens the CIs of the outcomes. Last, the St. Gallen Consensus has considered PR expression cutoff values as high as 20% to redefine the luminal A subtype since 2013 [8]. Since all the patients in this study cohort received a therapeutic regimen based on recommendations from the 2011 St. Gallen Consensus, we did not use the new definition of luminal B tumors in order to avoid bias in this retrospective study. Our result may still be meaningful because the new definition increases the luminal B breast cancer population, but the best way to find out is to conduct further research. In summary, this study suggests that PR is an independent adverse prognostic factor for DFS and is significantly associated with both increased non-visceral metastases and locoregional relapse risk in patients with luminal B breast cancer. Although expansion of the cohort and longer follow-up is needed, our results may be useful in counseling individual patients with luminal B breast cancer about their treatment options. Acknowledgements This study was funded by the National Clinical Key Specialty Construction Program, Fujian Natural Science Foundation (grant number 2015J01381), and Training Project of Young Talents in Fujian Health System (grant number 2015-ZQN-JC-6). Disclosure of conflict of interest None. Address correspondence to: Dr. Jian Liu, Department of Medical Oncology, Fujian Cancer Hospital, Fujian Medical University Cancer Hospital, Fuzhou , Fujian Province, China. liujianfj@126.com References [1] Perou CM, Sørlie T, Eisen MB, van de Rijn M, Jeffrey SS, Rees CA, Pollack JR, Ross DT, Johnsen H, Akslen LA, Fluge O, Pergamenschikov A, Williams C, Zhu SX, Lønning PE, Børresen-Dale AL, Brown PO, Botstein D. Molecular portraits of human breast tumors. Nature 2000; 406: [2] Cheang MC, Chia SK, Voduc D, Gao D, Leung S, Snider J, Watson M, Davies S, Bernard PS, Parker JS, Perou CM, Ellis MJ, Nielsen TO. Ki67 index, HER2 status, and prognosis of patients with luminal B breast cancer. J Natl Cancer Inst 2009; 101: [3] Cuzick J, Dowsett M, Pineda S, Wale C, Salter J, Quinn E, Zabaglo L, Mallon E, Green AR, Ellis IO, Howell A, Buzdar AU, Forbes JF. Prognostic value of a combined estrogen receptor, progesterone receptor, Ki-67, and human epidermal growth factor receptor 2 immunohistochemical score and comparison with the Genomic Health recurrence score in early breast cancer. J Clin Oncol 2011; 29: [4] Oh DS, Troester MA, Usary J, Hu Z, He X, Fan C, Wu J, Carey LA, Perou CM. Estrogen-regulated genes predict survival in hormone receptorpositive breast cancers. J Clin Oncol 2006; 24: [5] Soerjomataram I, Louwman MW, Ribot JG, Roukema JA, Coebergh JW. An overview of prognostic factors for long-term survivors of breast cancer. Breast Cancer Res Treat 2008; 107: [6] Sato K, Miyashita M, Ishida T, Suzuki A, Tada H, Watanabe G, Sato-Tadano A, Watanabe M, Ohuchi N. Prognostic significance of the progesterone receptor status in Ki67-high and -low luminal B-like HER2-negative breast cancers. Breast Cancer 2014; 23: [7] Nishimukai A, Yagi T, Yanai A, Miyagawa Y, Enomoto Y, Murase K, Imamura M, Takatsuka Y, Sakita I, Hatada T, Miyoshi Y. High Ki-67 expression and low progesterone receptor expression could independently lead to a worse prognosis for postmenopausal patients with estrogen receptor-positive and HER2-negative breast cancer. Clin Breast Cancer 2015; 15: [8] Goldhirsch A, Winer EP, Coates AS, Gelber RD, Piccart-Gebhart M, Thürlimann B, Senn HJ; Panel members. Personalizing the treatment of women with early breast cancer: highlights of the St gallen international expert consensus on the primary therapy of early breast cancer Ann Oncol 2013; 24: [9] Prat A, Cheang MC, Martín M, Parker JS, Carrasco E, Caballero R, Tyldesley S, Gelmon K, Bernard PS, Nielsen TO, Perou CM. Prognostic significance of progesterone receptorpositive tumor cells within immunohistochemically defined luminal a breast cancer. J Clin Oncol 2013; 31: [10] Cserni G, Francz M, Kálmán E, Kelemen G, Komjáthy DC, Kovács I, Kulka J, Sarkadi L, 909 Int J Clin Exp Pathol 2017;10(2):
10 Udvarhelyi N, Vass L, Vörös A. Estrogen receptor negative and progesterone receptor positive breast carcinomas-how frequent are they? Pathol Oncol Res 2011; 17: [11] Hefti MM, Hu R, Knoblauch NW, Collins LC, Haibe-Kains B, Tamimi RM, Beck AH. Estrogen receptor negative/progesterone receptor positive breast cancer is not a reproducible subtype. Breast Cancer Res 2013; 15: R68. [12] Tavassoli F DP. Pathology and genetics of tumors of the breast and female genital organs. Lyon, France: IARC Press; pp [13] Edge S BD, Compton C. AJCC cancer staging handbook: from the AJCC cancer staging manual. 7th edition. New York: Springer; [14] Wolff AC, Hammond ME, Hicks DG, Dowsett M, McShane LM, Allison KH, Allred DC, Bartlett JM, Bilous M, Fitzgibbons P, Hanna W, Jenkins RB, Mangu PB, Paik S, Perez EA, Press MF, Spears PA, Vance GH, Viale G, Hayes DF; American Society of Clinical Oncology; College of American Pathologists. Recommendations for human epidermal growth factor receptor 2 testing in breast cancer: American society of clinical oncology/college of American pathologists clinical practice guideline update. Arch Pathol Lab Med 2014; 138: [15] Mauriac L, Pippen JE, Quaresma Albano J, Gertler SZ, Osborne CK. Fulvestrant (Faslodex ) versus anastrozole for the second-line treatment of advanced breast cancer in subgroups of postmenopausal women with visceral and non-visceral metastases: combined results from two multicentre trials. Eur J Cancer 2003; 39: [16] Cardoso F, Costa A, Norton L, Senkus E, Aapro M, André F, Barrios CH, Bergh J, Biganzoli L, Blackwell KL, Cardoso MJ, Cufer T, El Saghir N, Fallowfield L, Fenech D, Francis P, Gelmon K, Giordano SH, Gligorov J, Goldhirsch A, Harbeck N, Houssami N, Hudis C, Kaufman B, Krop I, Kyriakides S, Lin UN, Mayer M, Merjaver SD, Nordström EB, Pagani O, Partridge A, Penault-Llorca F, Piccart MJ, Rugo H, Sledge G, Thomssen C, Van t Veer L, Vorobiof D, Vrieling C, West N, Xu B, Winer E; European School of Oncology; European Society of Medical Oncology. ESO-ESMO 2nd international consensus guidelines for advanced breast cancer (ABC2). Breast 2014; 23: [17] Cardoso F, Harbeck N, Fallowfield L, Kyriakides S, Senkus E; ESMO Guidelines Working Group. Locally recurrent or metastatic breast cancer: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 2012; 23 Suppl 7: vii [18] Bastien RR, Rodríguez-Lescure Á, Ebbert MT, Prat A, Munárriz B, Rowe L, Miller P, Ruiz- Borrego M, Anderson D, Lyons B, Álvarez I, Dowell T, Wall D, Seguí MÁ, Barley L, Boucher KM, Alba E, Pappas L, Davis CA, Aranda I, Fauron C, Stijleman IJ, Palacios J, Antón A, Carrasco E, Caballero R, Ellis MJ, Nielsen TO, Perou CM, Astill M, Bernard PS, Martín M. PAM50 breast cancer subtyping by RT-qPCR and concordance with standard clinical molecular markers. BMC Med Genomics 2012; 5: 44. [19] Bayraktar S, Royce M, Stork-Sloots L, de Snoo F, Gluck S. Molecular subtyping predicts pathologic tumor response in early-stage breast cancer treated with neoadjuvant docetaxel plus capecitabine with or without trastuzumab chemotherapy. Med Oncol 2014; 31: 163. [20] Nielsen TO, Parker JS, Leung S, Voduc D, Ebbert M, Vickery T, Davies SR, Snider J, Stijleman IJ, Reed J, Cheang MC, Mardis ER, Perou CM, Bernard PS, Ellis MJ. A comparison of PAM50 intrinsic subtyping with immunohistochemistry and clinical prognostic factors in tamoxifen-treated estrogen receptor-positive breast cancer. Clin Cancer Res 2010; 16: [21] Mohammed H, Russell IA, Stark R, Rueda OM, Hickey TE, Tarulli GA, Serandour AA, Birrell SN, Bruna A, Saadi A, Menon S, Hadfield J, Pugh M, Raj GV, Brown GD, D Santos C, Robinson JL, Silva G, Launchbury R, Perou CM, Stingl J, Caldas C, Tilley WD, Carroll JS. Progesterone receptor modulates ERalpha action in breast cancer. Nature 2015; 523: [22] Arpino G, Weiss H, Lee AV, Schiff R, De Placido S, Osborne CK, Elledge RM. Estrogen receptorpositive, progesterone receptor-negative breast cancer: association with growth factor receptor expression and tamoxifen resistance. J Natl Cancer Inst 2005; 97: [23] Lee YJ, Gorski J. Estrogen-induced transcription of the progesterone receptor gene does not parallel estrogen receptor occupancy. Proc Natl Acad Sci U S A 1996; 93: [24] Thakkar JP, Mehta DG. A review of an unfavorable subset of breast cancer: estrogen receptor positive progesterone receptor negative. Oncologist 2011; 16: [25] Zong Y, Zhu L, Wu J, Chen X, Huang O, Fei X, He J, Chen W, Li Y, Shen K. Progesterone receptor status and Ki-67 index may predict early relapse in luminal B/HER2 negative breast cancer patients: a retrospective study. PLoS One 2014; 9: e [26] Cubukcu E, Kanat O, Fatih Olmez O, Kabul S, Canhoroz M, Avci N, Deligonul A, Hartavi M, Cubukcu S, Olmez F, Kurt E, Evrensel T, Gokgoz S, Manavoglu O. Prognostic significance of estrogen receptor, progesterone re- 910 Int J Clin Exp Pathol 2017;10(2):
11 ceptor, HER2/neu, Ki-67, and nm23 expression in patients with invasive breast cancer. J BUON 2013; 18: [27] Slamon DJ, Clark GM, Wong SG, Levin WJ, Ullrich A, McGuire WL. Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science 1987; 235: [28] Kuerer HM, Buzdar AU, Singletary SE. Biologic basis and evolving role of aromatase inhibitors in the management of invasive carcinoma of the breast. J Surg Oncol 2001; 77: [29] Conneely OM, Jericevic BM, Lydon JP. Progesterone receptors in mammary gland development and tumorigenesis. J Mammary Gland Biol Neoplasia 2003; 8: [30] Rakha EA, El-Sayed ME, Green AR, Paish EC, Powe DG, Gee J, Nicholson RI, Lee AH, Robertson JF, Ellis IO. Biologic and clinical characteristics of breast cancer with single hormone receptor positive phenotype. J Clin Oncol 2007; 25: [31] Jacobsen BM, Schittone SA, Richer JK, Horwitz KB. Progesterone-independent effects of human progesterone receptors (PRs) in estrogen receptor-positive breast cancer: PR isoformspecific gene regulation and tumor biology. Mol Endocrinol 2005; 19: [32] Zhang Y, Su H, Rahimi M, Tochihara R, Tang C. EGFRvIII-induced estrogen-independence, tamoxifen-resistance phenotype correlates with PgR expression and modulation of apoptotic molecules in breast cancer. J Int Cancer 2009; 125: [33] Shi W, Zhang X, Pintilie M, Ma N, Miller N, Banerjee D, Tsao MS, Mak T, Fyles A, Liu FF. Dysregulated PTEN-PKB and negative receptor status in human breast cancer. J Int Cancer 2003; 104: [34] Piccart M, Hortobagyi GN, Campone M, Pritchard KI, Lebrun F, Ito Y, Noguchi S, Perez A, Rugo HS, Deleu I, Burris HA 3rd, Provencher L, Neven P, Gnant M, Shtivelband M, Wu C, Fan J, Feng W, Taran T, Baselga J. Everolimus plus exemestane for hormone-receptor-positive, human epidermal growth factor receptor-2-negative advanced breast cancer: overall survival results from BOLERO-2dagger. Ann Oncol 2014; 25: [35] Ma CX, Luo J, Naughton M, Ademuyiwa F, Suresh R, Griffith M, Griffith OL, Skidmore ZL, Spies NC, Ramu A, Trani L, Pluard T, Nagaraj G, Thomas S, Guo Z, Hoog J, Han J, Mardis E, Lockhart C, Ellis MJ. A phase I trial of BKM120 (Buparlisib) in combination with fulvestrant in postmenopausal women with estrogen receptor-positive metastatic breast cancer. Clin Cancer Res 2016; 22: [36] Cairns L, Curigliano G. Highlights from the 38th SABCS annual meeting, 8th-12th December 2015, San Antonio, USA. Ecancermedicalscience 2016; 10: 618. [37] Fournier A, Berrino F, Clavel-Chapelon F. Unequal risks for breast cancer associated with different hormone replacement therapies: results from the E3N cohort study. Breast Cancer Res Treat 2008; 107: Int J Clin Exp Pathol 2017;10(2):
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Clinical and pathological portraits of axillary presentation breast cancer and effects of preoperative systemic therapy
 Case Series Clinical and pathological portraits of axillary presentation breast cancer and effects of preoperative systemic therapy Ling Xu 1*, Fang Li 1,2*, Yinhua Liu 1, Xuening Duan 1, Jingming Ye 1,
Case Series Clinical and pathological portraits of axillary presentation breast cancer and effects of preoperative systemic therapy Ling Xu 1*, Fang Li 1,2*, Yinhua Liu 1, Xuening Duan 1, Jingming Ye 1,
Immunohistochemical classification of breast tumours
 Immunohistochemical classification of breast tumours Workshop in Diagnostic Immunohistochemistry September 19 th - 21 th 2018 Anne-Vibeke Lænkholm Department of Surgical Pathology, Zealand University Hospital,
Immunohistochemical classification of breast tumours Workshop in Diagnostic Immunohistochemistry September 19 th - 21 th 2018 Anne-Vibeke Lænkholm Department of Surgical Pathology, Zealand University Hospital,
RNA preparation from extracted paraffin cores:
 Supplementary methods, Nielsen et al., A comparison of PAM50 intrinsic subtyping with immunohistochemistry and clinical prognostic factors in tamoxifen-treated estrogen receptor positive breast cancer.
Supplementary methods, Nielsen et al., A comparison of PAM50 intrinsic subtyping with immunohistochemistry and clinical prognostic factors in tamoxifen-treated estrogen receptor positive breast cancer.
Low ER+ Breast Cancer. Is This a Distinct Group? Nika C. Gloyeske, MD, David J. Dabbs, MD, and Rohit Bhargava, MD ABSTRACT
 Low ER+ Breast Cancer Is This a Distinct Group? Nika C. Gloyeske, MD, David J. Dabbs, MD, and Rohit Bhargava, MD From the Magee-Womens Hospital of University of Pittsburgh Medical Center, Pittsburgh, PA.
Low ER+ Breast Cancer Is This a Distinct Group? Nika C. Gloyeske, MD, David J. Dabbs, MD, and Rohit Bhargava, MD From the Magee-Womens Hospital of University of Pittsburgh Medical Center, Pittsburgh, PA.
A Retrospective Analysis of Clinical Utility of AJCC 8th Edition Cancer Staging System for Breast Cancer
 Elmer ress Original Article World J Oncol. 2017;8(3):71-75 A Retrospective Analysis of Clinical Utility of AJCC 8th Edition Cancer Staging System for Breast Cancer Hui Hu a, Wei Wei a, Xin Yi a, Ling Xin
Elmer ress Original Article World J Oncol. 2017;8(3):71-75 A Retrospective Analysis of Clinical Utility of AJCC 8th Edition Cancer Staging System for Breast Cancer Hui Hu a, Wei Wei a, Xin Yi a, Ling Xin
Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer. Cheol Min Kang 2018/04/05
 Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
SCIENCE CHINA Life Sciences
 SCIENCE CHINA Life Sciences RESEARCH PAPER April 2013 Vol.56 No.4: 335 340 doi: 10.1007/s11427-013-4435-y Risk factors of recurrence in small-sized, node negative breast cancer in young women: a retrospective
SCIENCE CHINA Life Sciences RESEARCH PAPER April 2013 Vol.56 No.4: 335 340 doi: 10.1007/s11427-013-4435-y Risk factors of recurrence in small-sized, node negative breast cancer in young women: a retrospective
Hormone receptor and Her2 neu (Her2) analysis
 ORIGINAL ARTICLE Impact of Triple Negative Phenotype on Breast Cancer Prognosis Henry G. Kaplan, MD* and Judith A. Malmgren, PhD à *Swedish Cancer Institute at Swedish Medical Center; HealthStat Consulting
ORIGINAL ARTICLE Impact of Triple Negative Phenotype on Breast Cancer Prognosis Henry G. Kaplan, MD* and Judith A. Malmgren, PhD à *Swedish Cancer Institute at Swedish Medical Center; HealthStat Consulting
Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer
 Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Poor prognosis of single hormone receptorpositive breast cancer: similar outcome as triple-negative breast cancer
 Bae et al. BMC Cancer (2015) 15:138 DOI 10.1186/s12885-015-1121-4 RESEARCH ARTICLE Open Access Poor prognosis of single hormone receptorpositive breast cancer: similar outcome as triple-negative breast
Bae et al. BMC Cancer (2015) 15:138 DOI 10.1186/s12885-015-1121-4 RESEARCH ARTICLE Open Access Poor prognosis of single hormone receptorpositive breast cancer: similar outcome as triple-negative breast
Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
 JBUON 2018; 23(4): 877-882 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
JBUON 2018; 23(4): 877-882 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
Breast cancer in elderly patients (70 years and older): The University of Tennessee Medical Center at Knoxville 10 year experience
 Breast cancer in elderly patients (70 years and older): The University of Tennessee Medical Center at Knoxville 10 year experience Curzon M, Curzon C, Heidel RE, Desai P, McLoughlin J, Panella T, Bell
Breast cancer in elderly patients (70 years and older): The University of Tennessee Medical Center at Knoxville 10 year experience Curzon M, Curzon C, Heidel RE, Desai P, McLoughlin J, Panella T, Bell
Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer
 Original Articles Jpn J Clin Oncol 2012;42(6)471 476 doi:10.1093/jjco/hys046 Advance Access Publication 3 April 2012 Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer Junnan Li,
Original Articles Jpn J Clin Oncol 2012;42(6)471 476 doi:10.1093/jjco/hys046 Advance Access Publication 3 April 2012 Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer Junnan Li,
Morphological and Molecular Typing of breast Cancer
 Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological
Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological
Breast Cancer Earlier Disease. Stefan Aebi Luzerner Kantonsspital
 Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Journal of Breast Cancer
 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 215 June; 18(2): 149-159 Differences in Clinical Outcomes between Luminal A and B Type Breast Cancers according to the St. Gallen Consensus 213
Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 215 June; 18(2): 149-159 Differences in Clinical Outcomes between Luminal A and B Type Breast Cancers according to the St. Gallen Consensus 213
Advanced Breast Cancer
 Advanced Breast Cancer 4th ESO ESMO International Consensus Guidelines for Advanced Breast Cancer F. Cardoso, E. Senkus, A. Costa, E. Papadopoulos, M. Aapro, F. André, N. Harbeck, B. Aguilar Lopez, C.
Advanced Breast Cancer 4th ESO ESMO International Consensus Guidelines for Advanced Breast Cancer F. Cardoso, E. Senkus, A. Costa, E. Papadopoulos, M. Aapro, F. André, N. Harbeck, B. Aguilar Lopez, C.
Ki67 Index, HER2 Status, and Prognosis of Patients With Luminal B Breast Cancer
 ARTICLE Ki67 Index, HER2 Status, and Prognosis of Patients With Breast Cancer Maggie C. U. Cheang, Stephen K. Chia, David Voduc, Dongxia Gao, Samuel Leung, Jacqueline Snider, Mark Watson, Sherri Davies,
ARTICLE Ki67 Index, HER2 Status, and Prognosis of Patients With Breast Cancer Maggie C. U. Cheang, Stephen K. Chia, David Voduc, Dongxia Gao, Samuel Leung, Jacqueline Snider, Mark Watson, Sherri Davies,
A new way of looking at breast cancer tumour biology
 A new way of looking at breast cancer tumour biology Contents Intrinsic subtypes of breast cancer 3 Gene expression assays 3 Basis of the Prosigna test 4 Information provided by Prosigna 5 The accuracy
A new way of looking at breast cancer tumour biology Contents Intrinsic subtypes of breast cancer 3 Gene expression assays 3 Basis of the Prosigna test 4 Information provided by Prosigna 5 The accuracy
The effect of delayed adjuvant chemotherapy on relapse of triplenegative
 Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
Contemporary Classification of Breast Cancer
 Contemporary Classification of Breast Cancer Laura C. Collins, M.D. Vice Chair of Anatomic Pathology Professor of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Outline
Contemporary Classification of Breast Cancer Laura C. Collins, M.D. Vice Chair of Anatomic Pathology Professor of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Outline
EGFR as paradoxical predictor of chemosensitivity and outcome among triple-negative breast cancer
 ONCOLOGY REPORTS 21: 413-417, 2009 413 EGFR as paradoxical predictor of chemosensitivity and outcome among triple-negative breast cancer HIROKO NOGI 1, TADASHI KOBAYASHI 2, MASAFUMI SUZUKI 3, ISAO TABEI
ONCOLOGY REPORTS 21: 413-417, 2009 413 EGFR as paradoxical predictor of chemosensitivity and outcome among triple-negative breast cancer HIROKO NOGI 1, TADASHI KOBAYASHI 2, MASAFUMI SUZUKI 3, ISAO TABEI
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva
 Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Postoperative Adjuvant Chemotherapies. Stefan Aebi Luzerner Kantonsspital
 Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
Postoperative Adjuvant Chemotherapies Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Does Chemotherapy Work in Older Patients? ER : Chemotherapy vs nil Age
ANTICANCER RESEARCH 37: xxx-xxx (2017) Abstract. Background/Aim: This study investigated the
 doi:10.21873/anticanres.11xxx No: 7483-Y Please mark the appropriate section for this paper Experimental Clinical Epidemiological The Clinicopathological Factors Associated with Disease Progression in
doi:10.21873/anticanres.11xxx No: 7483-Y Please mark the appropriate section for this paper Experimental Clinical Epidemiological The Clinicopathological Factors Associated with Disease Progression in
What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland
 What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland Outline Early breast cancer Advanced breast cancer Open questions Outline Early breast cancer
What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland Outline Early breast cancer Advanced breast cancer Open questions Outline Early breast cancer
CLINICOPATHOLOGIC FEATURES AND MOLECULAR SUBTYPES OF BREAST CANCER IN FEZ-MEKNES REGION (MOROCCO): A STUDY OF 390 PATIENTS
 CLINICOPATHOLOGIC FEATURES AND MOLECULAR SUBTYPES OF BREAST CANCER IN FEZ-MEKNES REGION (MOROCCO): A STUDY OF 390 PATIENTS S. Chahbouni¹, A. Amarti 2, N. Hammas 3, L. Chbani 3, H. El fatemi 3 1 Department
CLINICOPATHOLOGIC FEATURES AND MOLECULAR SUBTYPES OF BREAST CANCER IN FEZ-MEKNES REGION (MOROCCO): A STUDY OF 390 PATIENTS S. Chahbouni¹, A. Amarti 2, N. Hammas 3, L. Chbani 3, H. El fatemi 3 1 Department
Breast cancer: Molecular STAGING classification and testing. Korourian A : AP,CP ; MD,PHD(Molecular medicine)
 Breast cancer: Molecular STAGING classification and testing Korourian A : AP,CP ; MD,PHD(Molecular medicine) Breast Cancer Theory: Halsted Operative breast cancer is a local-regional disease The positive
Breast cancer: Molecular STAGING classification and testing Korourian A : AP,CP ; MD,PHD(Molecular medicine) Breast Cancer Theory: Halsted Operative breast cancer is a local-regional disease The positive
Role of Genomic Profiling in (Minimally) Node Positive Breast Cancer
 Role of Genomic Profiling in (Minimally) Node Positive Breast Cancer Kathy S. Albain, MD, FACP Professor of Medicine Dean s Scholar Loyola University Chicago Stritch School of Medicine Cardinal Bernardin
Role of Genomic Profiling in (Minimally) Node Positive Breast Cancer Kathy S. Albain, MD, FACP Professor of Medicine Dean s Scholar Loyola University Chicago Stritch School of Medicine Cardinal Bernardin
Progesterone receptor status in determining the prognosis of estrogen receptor positive/ HER2 negative breast carcinoma patients
 JBUON 2015; 20(1): 28-34 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Progesterone receptor status in determining the prognosis of estrogen
JBUON 2015; 20(1): 28-34 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Progesterone receptor status in determining the prognosis of estrogen
Are there the specific prognostic factors for triplenegative subtype of early breast cancers (pt1-2n0m0)?
 Are there the specific prognostic factors for triplenegative subtype of early breast cancers (pt1-2n0m0)? Department of General Surgery, Anam Hospital, Korea University, College of Medicine, 126-, Anam-dong
Are there the specific prognostic factors for triplenegative subtype of early breast cancers (pt1-2n0m0)? Department of General Surgery, Anam Hospital, Korea University, College of Medicine, 126-, Anam-dong
Breast Cancer Outcomes as Defined by the Estrogen Receptor, Progesterone Receptor, and Human Growth Factor Receptor-2 in a Multi-ethnic Asian Country
 DOI 10.1007/s00268-015-3133-2 ORIGINAL SCIENTIFIC REPORT Breast Cancer Outcomes as Defined by the Estrogen Receptor, Progesterone Receptor, and Human Growth Factor Receptor-2 in a Multi-ethnic Asian Country
DOI 10.1007/s00268-015-3133-2 ORIGINAL SCIENTIFIC REPORT Breast Cancer Outcomes as Defined by the Estrogen Receptor, Progesterone Receptor, and Human Growth Factor Receptor-2 in a Multi-ethnic Asian Country
Original Article Long term prognosis of ductal carcinoma in situ with microinvasion: a retrospective cohort study
 Int J Clin Exp Pathol 2018;11(5):2665-2674 www.ijcep.com /ISSN:1936-2625/IJCEP0072542 Original Article Long term prognosis of ductal carcinoma in situ with microinvasion: a retrospective cohort study Tianjie
Int J Clin Exp Pathol 2018;11(5):2665-2674 www.ijcep.com /ISSN:1936-2625/IJCEP0072542 Original Article Long term prognosis of ductal carcinoma in situ with microinvasion: a retrospective cohort study Tianjie
Ki-67 is a biological tumor marker that reflects tumor
 Evaluation of Ki-67 Index in Core Needle Biopsies and Matched Breast Cancer Surgical Specimens Soomin Ahn, MD; Junghye Lee, MD; Min-Sun Cho, MD, PhD; Sanghui Park, MD, PhD; Sun Hee Sung, MD, PhD Context.
Evaluation of Ki-67 Index in Core Needle Biopsies and Matched Breast Cancer Surgical Specimens Soomin Ahn, MD; Junghye Lee, MD; Min-Sun Cho, MD, PhD; Sanghui Park, MD, PhD; Sun Hee Sung, MD, PhD Context.
Prognostic implications of the intrinsic molecular subtypes in male breast cancer
 JBUON 2017; 22(2): 377-382 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic implications of the intrinsic molecular subtypes in male
JBUON 2017; 22(2): 377-382 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic implications of the intrinsic molecular subtypes in male
Long-Term Survival Analysis of Korean Breast Cancer Patients at a Single Center: Improving Outcome Over Time
 Original Article http://dx.doi.org/1.339/ymj.1.55.5.117 pissn: 513-579, eissn: 197-37 Yonsei Med J 55(5):117-1195, 1 Long-Term Survival Analysis of Korean Breast Cancer Patients at a Single Center: Improving
Original Article http://dx.doi.org/1.339/ymj.1.55.5.117 pissn: 513-579, eissn: 197-37 Yonsei Med J 55(5):117-1195, 1 Long-Term Survival Analysis of Korean Breast Cancer Patients at a Single Center: Improving
Clinical Study on Prognostic Factors and Nursing of Breast Cancer with Brain Metastases
 Clinical Study on Prognostic Factors and Nursing of Breast Cancer with Brain Metastases Ying Zhou 1#, Kefang Zhong 1#, Fang Zhou* 2 ABSTRACT This paper aims to explore the clinical features and prognostic
Clinical Study on Prognostic Factors and Nursing of Breast Cancer with Brain Metastases Ying Zhou 1#, Kefang Zhong 1#, Fang Zhou* 2 ABSTRACT This paper aims to explore the clinical features and prognostic
A Study to Evaluate the Effect of Neoadjuvant Chemotherapy on Hormonal and Her-2 Receptor Status in Carcinoma Breast
 Original Research Article A Study to Evaluate the Effect of Neoadjuvant Chemotherapy on Hormonal and Her-2 Receptor Status in Carcinoma Breast E. Rajesh Goud 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior
Original Research Article A Study to Evaluate the Effect of Neoadjuvant Chemotherapy on Hormonal and Her-2 Receptor Status in Carcinoma Breast E. Rajesh Goud 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior
Heather M. Gage, MD, Avanti Rangnekar, Robert E. Heidel, PhD, Timothy Panella, MD, John Bell, MD, and Amila Orucevic, MD, PhD
 HER2 POSITIVE BREAST CARCINOMA IN THE PRE AND POST ADJUVANT ANTI-HER-2 THERAPY ERA: A SINGLE ACADEMIC INSTITUTION EXPERIENCE IN THE SETTING OUTSIDE OF CLINICAL TRIALS Heather M. Gage, MD, Avanti Rangnekar,
HER2 POSITIVE BREAST CARCINOMA IN THE PRE AND POST ADJUVANT ANTI-HER-2 THERAPY ERA: A SINGLE ACADEMIC INSTITUTION EXPERIENCE IN THE SETTING OUTSIDE OF CLINICAL TRIALS Heather M. Gage, MD, Avanti Rangnekar,
The Clinical Significance of. Triple-negative Phenotype on. Cancer Patients
 The Clinical Significance of Triple-negative Phenotype on Prognosis of Young Age( 35) Breast Cancer Patients IM-KYUNG KIM Department of Medicine The Graduate School, Yonsei University The Clinical Significance
The Clinical Significance of Triple-negative Phenotype on Prognosis of Young Age( 35) Breast Cancer Patients IM-KYUNG KIM Department of Medicine The Graduate School, Yonsei University The Clinical Significance
Author(s) Emi; Hatanaka, Yutaka; Matsuno, Yoshihiro; Yamashita. The final publication is available at link.springer. Instructions for use
 Title Prognostic significance of pathologic complete respo cancer Yoshioka, Tatsuya; Hosoda, Mitsuchika; Yamamoto, Mit Author(s) Emi; Hatanaka, Yutaka; Matsuno, Yoshihiro; Yamashita CitationBreast Cancer,
Title Prognostic significance of pathologic complete respo cancer Yoshioka, Tatsuya; Hosoda, Mitsuchika; Yamamoto, Mit Author(s) Emi; Hatanaka, Yutaka; Matsuno, Yoshihiro; Yamashita CitationBreast Cancer,
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Clinical activity of fulvestrant in metastatic breast cancer previously treated with endocrine therapy and/or chemotherapy
 ORIGINAL ARTICLE 2018 Mar 16. [Epub ahead of print] Clinical activity of fulvestrant in metastatic breast cancer previously treated with endocrine therapy and/or chemotherapy Mi Hwa Heo, Hee Kyung Kim,
ORIGINAL ARTICLE 2018 Mar 16. [Epub ahead of print] Clinical activity of fulvestrant in metastatic breast cancer previously treated with endocrine therapy and/or chemotherapy Mi Hwa Heo, Hee Kyung Kim,
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY
 Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY Methodology The test is based on the reported 50-gene classifier algorithm originally named PAM50 and is performed on the ncounter Dx Analysis System
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY Methodology The test is based on the reported 50-gene classifier algorithm originally named PAM50 and is performed on the ncounter Dx Analysis System
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY
 Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY GENE EXPRESSION PROFILING WITH PROSIGNA What is Prosigna? Prosigna Breast Cancer Prognostic Gene Signature Assay is an FDA-approved assay which provides
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY GENE EXPRESSION PROFILING WITH PROSIGNA What is Prosigna? Prosigna Breast Cancer Prognostic Gene Signature Assay is an FDA-approved assay which provides
Kazuhiro Araki, Yasuo Miyoshi
 Editorial Abundant options to avoid toxicity and alternative strategies for human epidermal growth factor receptor 2-positive and hormone receptor-positive advanced breast cancer Kazuhiro Araki, Yasuo
Editorial Abundant options to avoid toxicity and alternative strategies for human epidermal growth factor receptor 2-positive and hormone receptor-positive advanced breast cancer Kazuhiro Araki, Yasuo
UK Interdisciplinary Breast Cancer Symposium. Should lobular phenotype be considered when deciding treatment? Michael J Kerin
 UK Interdisciplinary Breast Cancer Symposium Should lobular phenotype be considered when deciding treatment? Michael J Kerin Professor of Surgery National University of Ireland, Galway and Galway University
UK Interdisciplinary Breast Cancer Symposium Should lobular phenotype be considered when deciding treatment? Michael J Kerin Professor of Surgery National University of Ireland, Galway and Galway University
Adjuvan Chemotherapy in Breast Cancer
 Adjuvan Chemotherapy in Breast Cancer Prof Dr Adnan Aydıner Istanbul University, Oncology Institute aa1 Slide 1 aa1 adnan aydiner; 17.02.2008 15-Year Reductions in Recurrence and Disease-Specific Mortality
Adjuvan Chemotherapy in Breast Cancer Prof Dr Adnan Aydıner Istanbul University, Oncology Institute aa1 Slide 1 aa1 adnan aydiner; 17.02.2008 15-Year Reductions in Recurrence and Disease-Specific Mortality
Correlation between estrogen receptor β expression and the curative effect of endocrine therapy in breast cancer patients
 1568 Correlation between estrogen receptor β expression and the curative effect of endocrine therapy in breast cancer patients LIYING GUO 1, YU ZHANG 2, WEI ZHANG 3 and DILIMINA YILAMU 1 1 Department of
1568 Correlation between estrogen receptor β expression and the curative effect of endocrine therapy in breast cancer patients LIYING GUO 1, YU ZHANG 2, WEI ZHANG 3 and DILIMINA YILAMU 1 1 Department of
Introduction. Wilfred Truin 1 Rudi M. H. Roumen. Vivianne C. G. Tjan-Heijnen 2 Adri C. Voogd
 Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/55957 holds various files of this Leiden University dissertation Author: Dekker T.J.A. Title: Optimizing breast cancer survival models based on conventional
Cover Page The handle http://hdl.handle.net/1887/55957 holds various files of this Leiden University dissertation Author: Dekker T.J.A. Title: Optimizing breast cancer survival models based on conventional
Editorial Process: Submission:11/30/2017 Acceptance:01/04/2019
 RESEARCH ARTICLE Editorial Process: Submission:11/30/2017 Acceptance:01/04/2019 in Non-Metastatic Triple-Negative Breast Cancer O Al jarroudi*, A Zaimi, S A Brahmi, S Afqir Abstract Introduction: Triple-negative
RESEARCH ARTICLE Editorial Process: Submission:11/30/2017 Acceptance:01/04/2019 in Non-Metastatic Triple-Negative Breast Cancer O Al jarroudi*, A Zaimi, S A Brahmi, S Afqir Abstract Introduction: Triple-negative
SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER
 SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER Sunil Shrestha 1*, Ji Yuan Yang, Li Shuang and Deepika Dhakal Clinical School of Medicine, Yangtze University, Jingzhou, Hubei Province, PR. China Department
SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER Sunil Shrestha 1*, Ji Yuan Yang, Li Shuang and Deepika Dhakal Clinical School of Medicine, Yangtze University, Jingzhou, Hubei Province, PR. China Department
Background: Case Report: Conclusions: Neoplasm Metastasis Breast Neoplasms therapy Aromatase Inhibitors. MeSH Keywords:
 ISSN 1941-5923 DOI: 10.12659/AJCR.890023 Received: 2013.11.11 Accepted: 2013.12.08 Published: 2014.02.24 Long-term complete remission of metastatic breast cancer, induced by a steroidal aromatase inhibitor
ISSN 1941-5923 DOI: 10.12659/AJCR.890023 Received: 2013.11.11 Accepted: 2013.12.08 Published: 2014.02.24 Long-term complete remission of metastatic breast cancer, induced by a steroidal aromatase inhibitor
J Clin Oncol 24: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 24 NUMBER 36 DECEMBER 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Locoregional Relapse and Distant Metastasis in Conservatively Managed Triple Negative Early-Stage Breast Cancer
VOLUME 24 NUMBER 36 DECEMBER 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Locoregional Relapse and Distant Metastasis in Conservatively Managed Triple Negative Early-Stage Breast Cancer
The Oncotype DX Assay A Genomic Approach to Breast Cancer
 The Oncotype DX Assay A Genomic Approach to Breast Cancer Pathology: 20 th and 21 st Century Size Age Phenotype Nodal status Protein/Gene Genomic Profiling Prognostic & Predictive Markers Used in Breast
The Oncotype DX Assay A Genomic Approach to Breast Cancer Pathology: 20 th and 21 st Century Size Age Phenotype Nodal status Protein/Gene Genomic Profiling Prognostic & Predictive Markers Used in Breast
Evaluation the Correlation between Ki67 and 5 Years Disease Free Survival of Breast Cancer Patients
 BIOSCIENCES BIOTECHNOLOGY RESEARCH ASIA, December 2015. Vol. 12(3), 2221-2225 Evaluation the Correlation between Ki67 and 5 Years Disease Free Survival of Breast Cancer Patients S.M. Hosseini¹, H. Shahbaziyan
BIOSCIENCES BIOTECHNOLOGY RESEARCH ASIA, December 2015. Vol. 12(3), 2221-2225 Evaluation the Correlation between Ki67 and 5 Years Disease Free Survival of Breast Cancer Patients S.M. Hosseini¹, H. Shahbaziyan
Giuseppe Viale for the BIG 1 98 Collaborative and International Breast Cancer Study Groups
 Central Review of ER, PgR and HER2 in BIG 1 98 Evaluating Letrozole vs. Letrozole Tamoxifen vs. Tamoxifen Letrozole as Adjuvant Endocrine Therapy for Postmenopausal Women with Hormone Receptor Positive
Central Review of ER, PgR and HER2 in BIG 1 98 Evaluating Letrozole vs. Letrozole Tamoxifen vs. Tamoxifen Letrozole as Adjuvant Endocrine Therapy for Postmenopausal Women with Hormone Receptor Positive
Breast cancer classification: beyond the intrinsic molecular subtypes
 Breast cancer classification: beyond the intrinsic molecular subtypes Britta Weigelt, PhD Signal Transduction Laboratory CRUK London Research Institute Summary Breast cancer heterogeneity Molecular classification
Breast cancer classification: beyond the intrinsic molecular subtypes Britta Weigelt, PhD Signal Transduction Laboratory CRUK London Research Institute Summary Breast cancer heterogeneity Molecular classification
Response to Paclitaxel in Node-positive Triple Negative Breast Cancer
 J Korean Surg Soc 2010;79:173-179 DOI: 10.4174/jkss.2010.79.3.173 원 저 Response to Paclitaxel in Node-positive Triple Negative Breast Cancer Department of Surgery, Kosin University College of Medicine,
J Korean Surg Soc 2010;79:173-179 DOI: 10.4174/jkss.2010.79.3.173 원 저 Response to Paclitaxel in Node-positive Triple Negative Breast Cancer Department of Surgery, Kosin University College of Medicine,
The Oncotype DX Assay in the Contemporary Management of Invasive Early-stage Breast Cancer
 The Oncotype DX Assay in the Contemporary Management of Invasive Early-stage Breast Cancer Cancer The Biology Century Understanding and treating the underlying tumor biology Cancer genetic studies demonstrate
The Oncotype DX Assay in the Contemporary Management of Invasive Early-stage Breast Cancer Cancer The Biology Century Understanding and treating the underlying tumor biology Cancer genetic studies demonstrate
Reporting of Breast Cancer Do s and Don ts
 Reporting of Breast Cancer Do s and Don ts 7 th SGH Annual Breast Pathology Course Professor Michael Bilous Conjoint Professor Western Sydney University Consultant Pathologist, Australian Clinical Labs,
Reporting of Breast Cancer Do s and Don ts 7 th SGH Annual Breast Pathology Course Professor Michael Bilous Conjoint Professor Western Sydney University Consultant Pathologist, Australian Clinical Labs,
Outcomes of Trastuzumab Therapy for 6 and 12 Months in Indonesian National Health Insurance System Clients with Operable HER2-Positive Breast Cancer
 DOI:10.22034/APJCP.2017.18.4.1151 Trastuzumab RESEARCH ARTICLE Outcomes of Trastuzumab Therapy for 6 and 12 Months in Indonesian National Health Insurance System Clients with Operable HER2-Positive Breast
DOI:10.22034/APJCP.2017.18.4.1151 Trastuzumab RESEARCH ARTICLE Outcomes of Trastuzumab Therapy for 6 and 12 Months in Indonesian National Health Insurance System Clients with Operable HER2-Positive Breast
Gene Signatures in Breast Cancer: Moving Beyond ER, PR, and HER2? Lisa A. Carey, M.D. University of North Carolina USA
 Gene Signatures in Breast Cancer: Moving Beyond ER, PR, and HER2? Lisa A. Carey, M.D. University of North Carolina USA When Are Biomarkers Ready To Use? Same Rules for Gene Expression Panels Key elements
Gene Signatures in Breast Cancer: Moving Beyond ER, PR, and HER2? Lisa A. Carey, M.D. University of North Carolina USA When Are Biomarkers Ready To Use? Same Rules for Gene Expression Panels Key elements
Clinicopathologic characteristics and prognostic factors for HER2-positive patients with metastatic breast cancer in southern China
 Clinical research Clinicopathologic characteristics and prognostic factors for HER2-positive patients with metastatic breast cancer in southern China Tao Qin 1, Zhong-Yu Yuan 1, Rou-Jun Peng 1, Bing Bai
Clinical research Clinicopathologic characteristics and prognostic factors for HER2-positive patients with metastatic breast cancer in southern China Tao Qin 1, Zhong-Yu Yuan 1, Rou-Jun Peng 1, Bing Bai
Prognosis in women with small (T1mic,T1a,T1b) node-negative operable breast cancer by immunohistochemically selected subtypes
 Prognosis in women with small (T1mic,T1a,T1b) node-negative operable breast cancer by immunohistochemically selected subtypes G. Cancello, P. Maisonneuve, N. Rotmensz, G. Viale, M. G. Mastropasqua, G.
Prognosis in women with small (T1mic,T1a,T1b) node-negative operable breast cancer by immunohistochemically selected subtypes G. Cancello, P. Maisonneuve, N. Rotmensz, G. Viale, M. G. Mastropasqua, G.
MOLECULAR AND CLINICAL ONCOLOGY 2: JIA YI WU *, WEI GUO CHEN *, XIAO SONG CHEN, OU HUANG, JIAN RONG HE, LI ZHU, YAFEN LI and KUN WEI SHEN
 MOLECULAR AND CLINICAL ONCOLOGY 2: 997-1002 Long term outcomes following adjuvant endocrine therapy in breast cancer patients with a positive to negative change of hormone receptor status following neoadjuvant
MOLECULAR AND CLINICAL ONCOLOGY 2: 997-1002 Long term outcomes following adjuvant endocrine therapy in breast cancer patients with a positive to negative change of hormone receptor status following neoadjuvant
Multimedia Appendix 6 Educational Materials Table of Contents. Intervention Educational Materials Audio Script (version 1)
 Multimedia Appendix 6 Educational Materials Table of Contents Intervention Educational Materials... 1 Audio Script (version 1)... 1 Text (version 1)... 5 Slides (version 1)... 17 Audio Script (version
Multimedia Appendix 6 Educational Materials Table of Contents Intervention Educational Materials... 1 Audio Script (version 1)... 1 Text (version 1)... 5 Slides (version 1)... 17 Audio Script (version
Clinical significance and prognostic value of receptor conversion in hormone receptor positive breast cancers after neoadjuvant chemotherapy
 Yang et al. World Journal of Surgical Oncology (2018) 16:51 https://doi.org/10.1186/s12957-018-1332-7 RESEARCH Open Access Clinical significance and prognostic value of receptor conversion in hormone receptor
Yang et al. World Journal of Surgical Oncology (2018) 16:51 https://doi.org/10.1186/s12957-018-1332-7 RESEARCH Open Access Clinical significance and prognostic value of receptor conversion in hormone receptor
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection
 Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
J Clin Oncol 23: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 23 NUMBER 30 OCTOBER 20 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Retrospective Analysis of Time to Recurrence in the ATAC Trial According to Hormone Receptor Status: An Hypothesis-Generating
VOLUME 23 NUMBER 30 OCTOBER 20 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Retrospective Analysis of Time to Recurrence in the ATAC Trial According to Hormone Receptor Status: An Hypothesis-Generating
Radiation Therapy for the Oncologist in Breast Cancer
 REVIEW ARTICLE Chonnam National University Medical School Sung-Ja Ahn, M.D. Adjuvant Tamoxifen with or without in Patients 70 Years of Age with Stage I ER-Positive Breast Cancer: Efficacy Outcomes (10
REVIEW ARTICLE Chonnam National University Medical School Sung-Ja Ahn, M.D. Adjuvant Tamoxifen with or without in Patients 70 Years of Age with Stage I ER-Positive Breast Cancer: Efficacy Outcomes (10
Published Ahead of Print on October 11, 2011 as /JCO J Clin Oncol by American Society of Clinical Oncology INTRODUCTION
 Published Ahead of Print on October 11, 2011 as 10.1200/JCO.2010.31.2835 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2010.31.2835 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R
Published Ahead of Print on October 11, 2011 as 10.1200/JCO.2010.31.2835 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2010.31.2835 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R
Alternate Gene Signatures, or Not
 Charles M. Perou, Ph.D. Departments of Genetics and Pathology Lineberger Comprehensive Cancer Center University of North Carolina Chapel Hill, North Carolina, USA Alternate Gene Signatures, or Not Charles
Charles M. Perou, Ph.D. Departments of Genetics and Pathology Lineberger Comprehensive Cancer Center University of North Carolina Chapel Hill, North Carolina, USA Alternate Gene Signatures, or Not Charles
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Overview of breast cancerpatients and their prognostic factors treated in Baghdad teaching hospital/ oncology department in the year 2010
 Original Article Overview of breast cancerpatients and their prognostic factors treated in Baghdad teaching hospital/ oncology department in the year 21 * DMRT clinical oncology, MSc. pathology. Summary:
Original Article Overview of breast cancerpatients and their prognostic factors treated in Baghdad teaching hospital/ oncology department in the year 21 * DMRT clinical oncology, MSc. pathology. Summary:
Surgical Pathology Issues of Practical Importance
 Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Molecular subtypes in patients with inflammatory breast cancer; A single center experience
 JBUON 05; 0(): 35-3 ISSN: 0-065, online ISSN: 4-63 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Molecular subtypes in patients with inflammatory breast cancer; A single center experience
JBUON 05; 0(): 35-3 ISSN: 0-065, online ISSN: 4-63 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Molecular subtypes in patients with inflammatory breast cancer; A single center experience
The role of p95her2 in trastuzumab resistance in breast cancer
 JBUON 2016; 21(2): 382-389 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE The role of p95her2 in trastuzumab resistance in breast cancer Nuket
JBUON 2016; 21(2): 382-389 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE The role of p95her2 in trastuzumab resistance in breast cancer Nuket
Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer
 Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer Dr. HassanAli Al-Khirsani, MBChB, CABM, F.I.C.M.S AL-Sadder teaching hospital, oncology unit Dr. Nasser Ghaly Yousif, MBChB,G.P.
Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer Dr. HassanAli Al-Khirsani, MBChB, CABM, F.I.C.M.S AL-Sadder teaching hospital, oncology unit Dr. Nasser Ghaly Yousif, MBChB,G.P.
Dr. dr. Primariadewi R, SpPA(K)
 Curriculum Vitae Dr. dr. Primariadewi R, SpPA(K) Education : Medical Doctor from UKRIDA Doctoral Degree from Faculty of Medicine University of Indonesia Pathologist Specialist and Consultant from Faculty
Curriculum Vitae Dr. dr. Primariadewi R, SpPA(K) Education : Medical Doctor from UKRIDA Doctoral Degree from Faculty of Medicine University of Indonesia Pathologist Specialist and Consultant from Faculty
Biomarkers for HER2-directed Therapies : Past Failures and Future Perspectives
 Biomarkers for HER2-directed Therapies : Past Failures and Future Perspectives Ian Krop Dana-Farber Cancer Institute Harvard Medical School Inchon 2018 Adjuvant Trastuzumab Improves Outcomes in HER2+ Breast
Biomarkers for HER2-directed Therapies : Past Failures and Future Perspectives Ian Krop Dana-Farber Cancer Institute Harvard Medical School Inchon 2018 Adjuvant Trastuzumab Improves Outcomes in HER2+ Breast
Journal of Breast Cancer
 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2017 June; 20(2): 160-169 Prognostic Impact of Progesterone Receptor Status in Chinese Estrogen Receptor Positive Invasive Breast Cancer Patients
Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2017 June; 20(2): 160-169 Prognostic Impact of Progesterone Receptor Status in Chinese Estrogen Receptor Positive Invasive Breast Cancer Patients
Life Science Journal 2014;11(7)
 Life Science Journal 4;(7) http://www.lifesciencesite.com Impact of primary tumor resection on response and survival in metastatic breast cancer patients Enas. A. Elkhouly¹, Eman. A. Tawfik ¹, Alaa. A.
Life Science Journal 4;(7) http://www.lifesciencesite.com Impact of primary tumor resection on response and survival in metastatic breast cancer patients Enas. A. Elkhouly¹, Eman. A. Tawfik ¹, Alaa. A.
Lecture 5. Primary systemic therapy: clinical and biological endpoints
 Lecture 5 Primary systemic therapy: clinical and biological endpoints Valentina Guarneri, M.D., Ph.D. Primary systemic therapy in breast cancer Firstly introduced d into clinical i l practice in 70s for
Lecture 5 Primary systemic therapy: clinical and biological endpoints Valentina Guarneri, M.D., Ph.D. Primary systemic therapy in breast cancer Firstly introduced d into clinical i l practice in 70s for
Mechanisms of Resistance to. Lisa A. Carey, M.D. University of North Carolina at Chapel Hill Lineberger Comprehensive Cancer Center
 Mechanisms of Resistance to Hormonal Therapy Lisa A. Carey, M.D. University of North Carolina at Chapel Hill Lineberger Comprehensive Cancer Center Antagonizing Estrogen Dependent Growth Premenopausal
Mechanisms of Resistance to Hormonal Therapy Lisa A. Carey, M.D. University of North Carolina at Chapel Hill Lineberger Comprehensive Cancer Center Antagonizing Estrogen Dependent Growth Premenopausal
It is a malignancy originating from breast tissue
 59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
Oncotype DX testing in node-positive disease
 Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
J Clin Oncol 31: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 31 NUMBER 2 SEPTEMBER 1 213 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Patterns of Recurrence and Outcome According to Breast Cancer Subtypes in Lymph Node Negative Disease: Results
VOLUME 31 NUMBER 2 SEPTEMBER 1 213 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Patterns of Recurrence and Outcome According to Breast Cancer Subtypes in Lymph Node Negative Disease: Results
She counts on your breast cancer expertise at the most vulnerable time of her life.
 HOME She counts on your breast cancer expertise at the most vulnerable time of her life. Empowering the right treatment choice for better patient outcomes. The comprehensive genomic assay experts trust.
HOME She counts on your breast cancer expertise at the most vulnerable time of her life. Empowering the right treatment choice for better patient outcomes. The comprehensive genomic assay experts trust.
PMRT for N1 breast cancer :CONS. Won Park, M.D., Ph.D Department of Radiation Oncology Samsung Medical Center
 PMRT for N1 breast cancer :CONS Won Park, M.D., Ph.D Department of Radiation Oncology Samsung Medical Center DBCG 82 b & c Overgaard et al Radiot Oncol 2007 1152 pln(+), 8 or more nodes removed Systemic
PMRT for N1 breast cancer :CONS Won Park, M.D., Ph.D Department of Radiation Oncology Samsung Medical Center DBCG 82 b & c Overgaard et al Radiot Oncol 2007 1152 pln(+), 8 or more nodes removed Systemic
P atients with primary breast cancer have an increased risk of developing contralateral breast cancer1. When
 OPEN SUBJECT AREAS: BONE METASTASES BREAST CANCER Received 23 July 2013 Accepted 19 August 2013 Published 5 September 2013 Correspondence and requests for materials should be addressed to C.W.D. (ducaiwen@
OPEN SUBJECT AREAS: BONE METASTASES BREAST CANCER Received 23 July 2013 Accepted 19 August 2013 Published 5 September 2013 Correspondence and requests for materials should be addressed to C.W.D. (ducaiwen@
Molecular characterization of breast cancer cell lines by clinical immunohistochemical markers
 4708 Molecular characterization of breast cancer cell lines by clinical immunohistochemical markers ANDRÉ DE LIMA MOTA 1, ADRIANE FEIJO EVANGELISTA 1, TACIANE MACEDO 1, RENATO OLIVEIRA 1, CRISTOVAM SCAPULATEMPO
4708 Molecular characterization of breast cancer cell lines by clinical immunohistochemical markers ANDRÉ DE LIMA MOTA 1, ADRIANE FEIJO EVANGELISTA 1, TACIANE MACEDO 1, RENATO OLIVEIRA 1, CRISTOVAM SCAPULATEMPO
When is Chemotherapy indicated in Advanced Luminal Breast Cancer?
 When is Chemotherapy indicated in Advanced Luminal Breast Cancer? Soo-Chin Lee Head & Senior Consultant Department of Haematology-Oncology Clinical Care National University Cancer Institute, Singapore
When is Chemotherapy indicated in Advanced Luminal Breast Cancer? Soo-Chin Lee Head & Senior Consultant Department of Haematology-Oncology Clinical Care National University Cancer Institute, Singapore
Molecular Classification of Iraqi Breast Cancer Patients and Its Correlation with Patients Profile
 Original Article Molecular Classification of Iraqi Breast Cancer Patients and Its Correlation * Manwar A Al-Naqqash* Mustafa K Jassim** MBChB, DMRT MBChB, DMRT, MSc Pathology MBChB Fac Med Baghdad 2016;
Original Article Molecular Classification of Iraqi Breast Cancer Patients and Its Correlation * Manwar A Al-Naqqash* Mustafa K Jassim** MBChB, DMRT MBChB, DMRT, MSc Pathology MBChB Fac Med Baghdad 2016;
Emerging Approaches for (Neo)Adjuvant Therapy for ER+ Breast Cancer
 Emerging Approaches for (Neo)Adjuvant Therapy for E+ Breast Cancer Cynthia X. Ma, M.D., Ph.D. Associate Professor of Medicine Washington University in St. Louis Outline Current status of adjuvant endocrine
Emerging Approaches for (Neo)Adjuvant Therapy for E+ Breast Cancer Cynthia X. Ma, M.D., Ph.D. Associate Professor of Medicine Washington University in St. Louis Outline Current status of adjuvant endocrine
Genomic Profiling of Tumors and Loco-Regional Recurrence
 1 Genomic Profiling of Tumors and Loco-Regional Recurrence Terry Mamounas, M.D., M.P.H., F.A.C.S. Medical Director, Comprehensive Breast Program UF Health Cancer Center at Orlando Health Professor of Surgery,
1 Genomic Profiling of Tumors and Loco-Regional Recurrence Terry Mamounas, M.D., M.P.H., F.A.C.S. Medical Director, Comprehensive Breast Program UF Health Cancer Center at Orlando Health Professor of Surgery,
Claudin-4 Expression in Triple Negative Breast Cancer: Correlation with Androgen Receptors and Ki-67 Expression
 Claudin-4 Expression in Triple Negative Breast Cancer: Correlation with Androgen Receptors and Ki-67 Expression Mona A. Abd-Elazeem, Marwa A. Abd- Elazeem Pathology department, Faculty of Medicine, Tanta
Claudin-4 Expression in Triple Negative Breast Cancer: Correlation with Androgen Receptors and Ki-67 Expression Mona A. Abd-Elazeem, Marwa A. Abd- Elazeem Pathology department, Faculty of Medicine, Tanta
Predictors of pathological complete response to neoadjuvant chemotherapy in stage II and III breast cancer: The impact of chemotherapeutic regimen
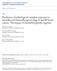 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Predictors of pathological complete response to neoadjuvant chemotherapy in stage II and III breast cancer:
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Predictors of pathological complete response to neoadjuvant chemotherapy in stage II and III breast cancer:
