Malignancy-Associated Coagulopathy:
|
|
|
- Ashley Doyle
- 6 years ago
- Views:
Transcription
1 Malignancy-Associated Coagulopathy: Recognition and Laboratory Diagnosis Aneel A. Ashrani, M.D., M.S MFMER slide-1
2 Disclosures Relevant Financial Relationship -NONE Off-Label and/or Investigational Uses -NONE 2016 MFMER slide-2
3 Malignancy Associated Coagulopathy Activation of coagulation Venous and arterial thrombosis Disseminated intravascular coagulation and fibrinolysis (DIC/ICF) Hyperfibrinolysis Immune mediated FVIII inhibitor Acquired von Willebrand syndrome FV inhibitor Therapy related coagulopathy Coagulation factor depletion L-aspariginase Drug induced thrombotic microangiopathy Gemcitabine Endothelial dysfunction Thalidomide Bevacizumab Platelet activation/ dysfunction Heparin induced thrombocytopenia Ibrutinib 2016 MFMER slide-3
4 Case 1: 59 year old female 2016 MFMER slide-4
5 Case 1: 59 year old female Stage III serous adenocarcinoma of the ovary s/p total abdominal hysterectomy and bilateral salpingo-oophorectomy on paclitaxel and carboplatin 2016 MFMER slide-5
6 Case 1: 59 year old female Stage III serous adenocarcinoma of the ovary s/p total abdominal hysterectomy and bilateral salpingo-oophorectomy on paclitaxel and carboplatin Post-Influenza vaccine extensive ecchymosis No prior history of excessive bleeding or bruising Hemoglobin 8.7 g/dl 5.7 g/dl (platelets normal) 2016 MFMER slide-6
7 Case 1: 59 year old female Stage III serous adenocarcinoma of the ovary s/p total abdominal hysterectomy and bilateral salpingo-oophorectomy on paclitaxel and carboplatin Post-Influenza vaccine extensive ecchymosis No prior history of excessive bleeding or bruising Hemoglobin 8.7 g/dl 5.7 g/dl (platelets normal) PT: 11.7 sec (Ref: ) APTT: 75 sec (Ref: 25 37) 2016 MFMER slide-7
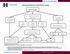
8 Prolonged PT or APTT (75 sec) Mixing study with normal plasma (39 sec) Correction (factor deficiency) No correction (inhibitor) Clotting factor assays to identify deficiency Determine type of inhibitor Drug: Heparin, IIa inhibitor, Xa inhibitor Specific factor inhibitor (FVIII: <1%) Titer: 7 BU Nonspecific inhibitor (e.g., lupus anticoagulant) Adapted from Mayo Clinic Proc.; Kamal, A.H., 2007;82(7): with permission from Elsevier MFMER slide-8
9 Acquired Factor VIII Inhibitor Neutralizing autoantibodies against factor VIII Prevalence: ~1.5 cases/million/year Most common in the elderly Median age (IQR): 73.9 yrs. ( ) Collins, P.W., et al. Blood. 2007;109: Knoebl, P., et al. J Thromb Haemost 2012; 10: MFMER slide-9
10 Acquired Factor VIII Inhibitor Neutralizing autoantibodies against factor VIII Prevalence: ~1.5 cases/million/year Most common in the elderly Median age (IQR): 73.9 yrs. ( ) Underlying disorder No. of patients Idiopathic 51.9% Malignancy 11.8% Autoimmune diseases 11.6% Pregnancy 8.5% Infections 3.8% Drug induced 3.4% MGUS 2.6% Collins, P.W., et al. Blood. 2007;109: Knoebl, P., et al. J Thromb Haemost 2012; 10: MFMER slide-10
11 Clinical Presentation Knoebl, P., et al. J Thromb Haemost 2012; 10: MFMER slide-11
12 Clinical Presentation Majority of patients bleed (95%) Spontaneous bleed: 77% Subcutaneous: 53% Deep muscle or retroperitoneal bleed: 50% Mucosal bleeding:32% Joint bleeds: 5% Severe bleed: 70% Knoebl, P., et al. J Thromb Haemost 2012; 10: MFMER slide-12
13 Clinical Presentation Majority of patients bleed (95%) Spontaneous bleed: 77% Subcutaneous: 53% Deep muscle or retroperitoneal bleed: 50% Mucosal bleeding:32% Joint bleeds: 5% Severe bleed: 70% Mortality at final follow-up: 28% Median (IRQ) time after diagnosis: 75 days (25 240) Mortality secondary to the bleed: 3% Mortality secondary to the immunosuppression: 3% Knoebl, P., et al. J Thromb Haemost 2012; 10: MFMER slide-13
14 Cancer and FVIII Inhibitors No association with specific tumor type 60% solid tumors (lung, prostate, head/neck) May be autoimmune reaction to tumor tumor antigen similar to FVIII? Standard treatment chemotherapy, radiation, & surgery do not usually eradicate inhibitors Inhibitor is not a marker of tumor recurrence Hauser and Lechner. Thromb Haemost 1999;82: MFMER slide-14
15 Treatment Strategies Dual Objectives Management Strategies Acute Management Long-term Strategy Stop the Bleeding Eradicate Inhibitor 2016 MFMER slide-15
16 Acute Management of Bleeding Bleeding controlled in 80% of patients treated with a first-line hemostatic agent Hemostatic agent No. of patients treated % Response Bypassing agent % rfviia % apcc 60 93% Replacement therapy 69 70% FVIII 55 70% DDAVP 14 64% Thrombotic events similar between rfviia (2.9%) and apcc (4.8%). Baudo, F., et al. Blood. 2012;120(1): 39-46) 2016 MFMER slide-16
17 Inhibitor Eradication: Efficacy and Safety Collins, P, et al. Blood. 2012;120(1): MFMER slide-17
18 Inhibitor Eradication: Efficacy and Safety Regimen N CR (%) Relapse (%) Any AE (%) Mortality (%) Steroids alone % 11% 25% 28% Steroids + cyclophosphamide 83 80% 10% 41% 33% Rituxan based regimens 51 61% 3% 37% 20% Collins, P, et al. Blood. 2012;120(1): MFMER slide-18
19 Inhibitor Eradication: Efficacy and Safety Regimen N CR (%) Relapse (%) Any AE (%) Mortality (%) Steroids alone % 11% 25% 28% Steroids + cyclophosphamide 83 80% 10% 41% 33% Rituxan based regimens 51 61% 3% 37% 20% Cyclophosphamide+steroids versus steroids alone OR 95% CI CR at final follow-up Alive at final follow-up: Alive and in CR Collins, P, et al. Blood. 2012;120(1): MFMER slide-19
20 Case 1: Outcome Acute bleed management: Transfused 4 units PRBCs FEIBA 75 units/kg q12 hours Inhibitor management: Prednisone 1mg/kg/day Factor VIII (%) Inhibitor titer (BU) 0 Oct Nov Dec Jan Feb Mar 2016 MFMER slide-20
21 Case 2: 51 year old female 2016 MFMER slide-21
22 Case 2: 51 year old female No prior personal or family history of bleeding Iron deficiency anemia, celiac disease and recurrent GI bleeding No improvement with gluten-free diet or small bowel resection 2016 MFMER slide-22
23 Case 2: 51 year old female No prior personal or family history of bleeding Iron deficiency anemia, celiac disease and recurrent GI bleeding No improvement with gluten-free diet or small bowel resection 3-year history of frequent epistaxis, unexplained bruises and prolonged bleeding with minor nicks/ cuts 2016 MFMER slide-23
24 Case 2: 51 year old female No prior personal or family history of bleeding Iron deficiency anemia, celiac disease and recurrent GI bleeding No improvement with gluten-free diet or small bowel resection 3-year history of frequent epistaxis, unexplained bruises and prolonged bleeding with minor nicks/ cuts APTT: 35 sec (Ref: 21 33); APTT mix: 30 sec 2016 MFMER slide-24
25 Case 2: 51 year old female No prior personal or family history of bleeding Iron deficiency anemia, celiac disease and recurrent GI bleeding No improvement with gluten-free diet or small bowel resection 3-year history of frequent epistaxis, unexplained bruises and prolonged bleeding with minor nicks/ cuts APTT: 35 sec (Ref: 21 33); APTT mix: 30 sec Von Willebrand disease profile: FVIII: 28% vwf antigen: 18% Ristocetin cofactor: <12% Normal vwf multimer distribution Ristocetin inhibitor screen: Negative 2016 MFMER slide-25
26 Case 2: 51 year old female No prior personal or family history of bleeding Iron deficiency anemia, celiac disease and recurrent GI bleeding No improvement with gluten-free diet or small bowel resection 3-year history of frequent epistaxis, unexplained bruises and prolonged bleeding with minor nicks/ cuts APTT: 35 sec (Ref: 21 33); APTT mix: 30 sec Von Willebrand disease profile: FVIII: 28% vwf antigen: 18% Ristocetin cofactor: <12% Normal vwf multimer distribution Ristocetin inhibitor screen: Negative SPEP: 0.5 g/dl IgG lambda monoclonal paraprotein; MGUS 2016 MFMER slide-26
27 Acquired von Willebrand Syndrome: Pathogenesis Autoantibodies Interfering with platelet or collagen binding Increasing VWF clearance Sequestration/adsorption of high-molecular-weight vwf Multiple myeloma Essential thrombocythemia Proteolytic cleavage of VWF Shear stress-induced vwf unfolding Aortic valve stenosis LVAD Pancreatitis, liver cirrhosis, leukemia Decreased synthesis Hypothyroidism Tiede, A., et al. Blood. 2011;117(25): MFMER slide-27
28 Diagnostic Tests Initial assays for AvWS are same as for vwd (Profile approach) Additional useful assays: vwf propeptide? Increased propeptide/ vwf:ag ratio reflects accelerated clearance of vwf Increased ratio also seen in subset of patients with type 1 vwd Autoantibodies: No standard assays Neutralizing antibodies seen in minority of AvWS Mixing studies of VWF:Activity Non-neutralizing antibodies accelerate vwf clearance ELISA assay 2016 MFMER slide-28
29 Treatment Federici AB, et al. Blood. 1998; 92 (8): Tiede, A., et al. Blood. 2011;117(25): MFMER slide-29
30 Treatment DDAVP: Overall response rate: 32% Response transient and vary by underlying disorder Low response: Cardiovascular, MPN Higher response: Autoimmune, Lymphoproliferative disorders, neoplastic, MGUS Federici AB, et al. Blood. 1998; 92 (8): Tiede, A., et al. Blood. 2011;117(25): MFMER slide-30
31 Treatment DDAVP: Overall response rate: 32% Response transient and vary by underlying disorder Low response: Cardiovascular, MPN Higher response: Autoimmune, Lymphoproliferative disorders, neoplastic, MGUS vwf containing concentrate: Half-life short, especially in patients with MGUS or inhibitors Federici AB, et al. Blood. 1998; 92 (8): Tiede, A., et al. Blood. 2011;117(25): MFMER slide-31
32 Treatment DDAVP: Overall response rate: 32% Response transient and vary by underlying disorder Low response: Cardiovascular, MPN Higher response: Autoimmune, Lymphoproliferative disorders, neoplastic, MGUS vwf containing concentrate: Half-life short, especially in patients with MGUS or inhibitors IVIG: Effective in patients with IgG-MGUS associated AVWS Peak effect in 4 days with slow return to baseline within 21 days Federici AB, et al. Blood. 1998; 92 (8): Tiede, A., et al. Blood. 2011;117(25): MFMER slide-32
33 Treatment DDAVP: Overall response rate: 32% Response transient and vary by underlying disorder Low response: Cardiovascular, MPN Higher response: Autoimmune, Lymphoproliferative disorders, neoplastic, MGUS vwf containing concentrate: Half-life short, especially in patients with MGUS or inhibitors IVIG: Effective in patients with IgG-MGUS associated AVWS Peak effect in 4 days with slow return to baseline within 21 days Plasmapheresis: Deplete autoantibodies or paraproteins Federici AB, et al. Blood. 1998; 92 (8): Tiede, A., et al. Blood. 2011;117(25): MFMER slide-33
34 Treatment DDAVP: Overall response rate: 32% Response transient and vary by underlying disorder Low response: Cardiovascular, MPN Higher response: Autoimmune, Lymphoproliferative disorders, neoplastic, MGUS vwf containing concentrate: Half-life short, especially in patients with MGUS or inhibitors IVIG: Effective in patients with IgG-MGUS associated AVWS Peak effect in 4 days with slow return to baseline within 21 days Plasmapheresis: Deplete autoantibodies or paraproteins Antifibrinolytics: Federici AB, et al. Blood. 1998; 92 (8): Tiede, A., et al. Blood. 2011;117(25): MFMER slide-34
35 What About Long-Term Management of AvWS? Treatment of the underlying disorder should be considered whenever possible Response to therapy for underlying lymphoproliferative disorders and multiple myeloma: 35-70% Response to cytoreductive therapy for underlying MPN: ~85% MGUS usually unresponsive to steroids and chemotherapy Cannot eradicate slowly proliferating plasma cell clones? Bortezomib Ojeda-Uribe M, et al. Am J Hematol. 2010;85(5): MFMER slide-35
36 Case 2: Outcome 2016 MFMER slide-36
37 Case 2: Outcome DDAVP (0.3 mcg/kg x 1) % FVIII:C vwf:ag vwf:rco Time (hours) 2016 MFMER slide-37
38 Case 2: Outcome DDAVP (0.3 mcg/kg x 1) IV IgG (1 g/kg x 1) % FVIII:C vwf:ag vwf:rco Time (hours) % vwf:rco FVIII:C vwf:ag Time (Days) 2016 MFMER slide-38
39 Case 3: 54 year old male 2016 MFMER slide-39
40 Case 3: 54 year old male Stage IV peripheral T-cell lymphoma (liver involvement) Bilirubin: 16 mg/dl 2016 MFMER slide-40
41 Case 3: 54 year old male Stage IV peripheral T-cell lymphoma (liver involvement) Bilirubin: 16 mg/dl Gemcitabine, Solu-Medrol, and cisplatin: x 2 cycles 2016 MFMER slide-41
42 Case 3: 54 year old male Stage IV peripheral T-cell lymphoma (liver involvement) Bilirubin: 16 mg/dl Gemcitabine, Solu-Medrol, and cisplatin: x 2 cycles Liver function tests improved significantly 2016 MFMER slide-42
43 Case 3: 54 year old male Stage IV peripheral T-cell lymphoma (liver involvement) Bilirubin: 16 mg/dl Gemcitabine, Solu-Medrol, and cisplatin: x 2 cycles Liver function tests improved significantly 2016 MFMER slide-43
44 Case 3: 54 year old male Stage IV peripheral T-cell lymphoma (liver involvement) Bilirubin: 16 mg/dl Gemcitabine, Solu-Medrol, and cisplatin: x 2 cycles Liver function tests improved significantly Overall significant improvement, but with new skeletal lesions 2016 MFMER slide-44
45 Case 3 (contd.) 2016 MFMER slide-45
46 Case 3 (contd.) He then received first cycle of CHOP-etoposide When due for the second cycle: Fever up to 103 o F and sweats Right arm pain and swelling (PICC line in right arm) ROS negative 2016 MFMER slide-46
47 Case 3 (contd.) He then received first cycle of CHOP-etoposide When due for the second cycle: Fever up to 103 o F and sweats Right arm pain and swelling (PICC line in right arm) ROS negative Lactate: 2.9 Uric Acid: 8.1 LDH: 324 Bilirubin: 1.6 AST 64 Alk phosphatase: 527 CXR: No infiltrate Cultures: negative 2016 MFMER slide-47
48 Case 3 (contd.) 2016 MFMER slide-48
49 Case 3 (contd.) Right UE ultrasound: Acute DVT in the right subclavian, axillary, and brachial veins Enoxaparin 1mg/kg q12h 2016 MFMER slide-49
50 Case 3 (contd.) Right UE ultrasound: Acute DVT in the right subclavian, axillary, and brachial veins Enoxaparin 1mg/kg q12h Persistent fevers, despite negative infection work up Lymphoma? 2016 MFMER slide-50
51 Case 3 (contd.) Right UE ultrasound: Acute DVT in the right subclavian, axillary, and brachial veins Enoxaparin 1mg/kg q12h Persistent fevers, despite negative infection work up Lymphoma? 2016 MFMER slide-51
52 Case 3 (contd.) Right UE ultrasound: Acute DVT in the right subclavian, axillary, and brachial veins Enoxaparin 1mg/kg q12h Persistent fevers, despite negative infection work up Lymphoma? PET-CT scan: Mixed response Increased activity in the right cardiophrenic recess but with improvement in other lesions 2016 MFMER slide-52
53 Case 3 (contd.) 2016 MFMER slide-53
54 Case 3 (contd.) Hemoglobin: 7.6 g/dl WBC: 2800/mm 3 Platelets: 68,000/mm MFMER slide-54
55 Case 3 (contd.) Hemoglobin: 7.6 g/dl WBC: 2800/mm 3 Platelets: 68,000/mm 3 PT: 18.1 sec (Ref: ) APTT: 56 sec (Ref: 28 38) 2016 MFMER slide-55
56 Case 3 (contd.) Hemoglobin: 7.6 g/dl WBC: 2800/mm 3 Platelets: 68,000/mm 3 PT: 18.1 sec (Ref: ) APTT: 56 sec (Ref: 28 38) Coagulation factors II, V, IX, X, XI, XII low; factor VII, VIII normal 2016 MFMER slide-56
57 Case 3 (contd.) Hemoglobin: 7.6 g/dl WBC: 2800/mm 3 Platelets: 68,000/mm 3 PT: 18.1 sec (Ref: ) APTT: 56 sec (Ref: 28 38) Coagulation factors II, V, IX, X, XI, XII low; factor VII, VIII normal Fibrinogen: 107 mg/dl (Ref: ) D-Dimer: 1545 ng/ml (Ref: <250) Soluble fibrin monomer complex (SFMC): 52 mcg/ml (Ref: <8) 2016 MFMER slide-57
58 Disseminated Intravascular Coagulation and Fibrinolysis (DIC/ ICF) Persistent intravascular activation of coagulation leading to fibrin formation and deposition inducing consumption of coagulation factors and platelets Can present as thrombosis or bleeding DIC is a clinical and laboratory diagnosis, based on findings of coagulopathy and/or fibrinolysis No single laboratory test can accurately confirm or eliminate the diagnosis 2016 MFMER slide-58
59 DIC Pathophysiology UNDERLYING CONDITION Activation of intravascular coagulation Platelet consumption Coagulation factor consumption Fibrin deposition fibrinolysis Endothelial damage Platelets PT APTT D-Dimer SFMC MAHA Impaired coagulation Thrombosis BLEEDING ORGAN ISCHEMIA 2016 MFMER slide-59
60 Acute versus Chronic DIC Parameter Acute (Decompensated) DIC Chronic (Compensated) DIC Underlying condition Trauma, sepsis, malignancy (esp. APL), ABO-incompatible blood transfusion Malignancy (esp. pancreatic, gastric, ovarian, brain tumors Presentation Bleeding Venous or arterial thromboembolism Platelet count Decreased Variable PT Prolonged Normal aptt Prolonged Normal Thrombin time Prolonged Normal or slightly prolonged Fibrinogen Decreased Normal or elevated Factor V Decreased Normal Factor VIII Decreased Normal D-Dimer Elevated Elevated SFMC Elevated Elevated 2016 MFMER slide-60
61 Differential Diagnosis 2016 MFMER slide-61
62 Differential Diagnosis Severe liver disease Thrombotic microangiopathy (TMA) TTP HUS Drug-induced TMA 2016 MFMER slide-62
63 Differential Diagnosis Severe liver disease Thrombotic microangiopathy (TMA) TTP HUS Drug-induced TMA Management 2016 MFMER slide-63
64 Differential Diagnosis Severe liver disease Thrombotic microangiopathy (TMA) TTP HUS Drug-induced TMA Management Treat underlying cause Supportive measures Transfusion support, if necessary PRBCs, platelets Cryoprecipitate, FFP Anticoagulation for thrombotic complications 2016 MFMER slide-64
65 Case 3: Outcome: improvement in DIC with chemotherapy Fibrinogen (mg/dl) Platelet count (x1000/mm3) Cryoprecipitate CHOP-E 2016 MFMER slide-65
66 Case 4: 63 year old female 2016 MFMER slide-66
67 Case 4: 63 year old female History of Stage IA infiltrating ductal breast cancer, s/p surgery, adjuvant chemotherapy and on aromatase inhibitor 2016 MFMER slide-67
68 Case 4: 63 year old female History of Stage IA infiltrating ductal breast cancer, s/p surgery, adjuvant chemotherapy and on aromatase inhibitor Presented with extensive spontaneous ecchymoses, hematuria and soft tissue bleeding CT of the abdomen: non-obstructing renal calculi Incidental multiple lytic and sclerotic lesions in the LS spine and pelvis 2016 MFMER slide-68
69 Case 4: 63 year old female History of Stage IA infiltrating ductal breast cancer, s/p surgery, adjuvant chemotherapy and on aromatase inhibitor Presented with extensive spontaneous ecchymoses, hematuria and soft tissue bleeding CT of the abdomen: non-obstructing renal calculi Incidental multiple lytic and sclerotic lesions in the LS spine and pelvis No prior history suggestive of a bleeding disorder 2016 MFMER slide-69
70 Case 4 (contd.) 2016 MFMER slide-70
71 Case 4 (contd.) Hemoglobin 9.4 g/dl WBC 7900/ mm 3 Platelets 192,000/mm MFMER slide-71
72 Case 4 (contd.) Hemoglobin 9.4 g/dl WBC 7900/ mm 3 Platelets 192,000/mm 3 Prothrombin time 10.5 sec (Ref: ) aptt 30 sec (Ref: 21-33) Thrombin time 24 sec (Ref: 16-25) 2016 MFMER slide-72
73 Case 4 (contd.) Hemoglobin 9.4 g/dl WBC 7900/ mm 3 Platelets 192,000/mm 3 Prothrombin time 10.5 sec (Ref: ) aptt 30 sec (Ref: 21-33) Thrombin time 24 sec (Ref: 16-25) Coagulation factors II, V, VII, VIII, IX, X, XI, XII normal 2016 MFMER slide-73
74 Case 4 (contd.) Hemoglobin 9.4 g/dl WBC 7900/ mm 3 Platelets 192,000/mm 3 Prothrombin time 10.5 sec (Ref: ) aptt 30 sec (Ref: 21-33) Thrombin time 24 sec (Ref: 16-25) Coagulation factors II, V, VII, VIII, IX, X, XI, XII normal Von Willebrand factor (vwf) antigen and vwf activity normal 2016 MFMER slide-74
75 Case 4 (contd.) Hemoglobin 9.4 g/dl WBC 7900/ mm 3 Platelets 192,000/mm 3 Prothrombin time 10.5 sec (Ref: ) aptt 30 sec (Ref: 21-33) Thrombin time 24 sec (Ref: 16-25) Coagulation factors II, V, VII, VIII, IX, X, XI, XII normal Von Willebrand factor (vwf) antigen and vwf activity normal Platelet aggregation studies and PFA100 assays normal 2016 MFMER slide-75
76 Case 4 (contd.): Now What? 2016 MFMER slide-76
77 Case 4 (contd.): Now What? Fibrinogen (Clauss) 159 mg/dl D-dimer >20000 ng/ml <250 Soluble Fibrin Monomer Negative 2016 MFMER slide-77
78 Case 4 (contd.): Now What? Fibrinogen (Clauss) 159 mg/dl D-dimer >20000 ng/ml <250 Soluble Fibrin Monomer Negative Factor XIII screen Clot dissolved before testing could be completed 2016 MFMER slide-78
79 Case 4 (contd.): Now What? Fibrinogen (Clauss) 159 mg/dl D-dimer >20000 ng/ml <250 Soluble Fibrin Monomer Negative Factor XIII screen Clot dissolved before testing could be completed Clot solubility test for XIII screen Normally, a clot is stable for 2 hours in 5M urea or 2% acetic acid, while in factor XIII deficiency the clot is unstable and dissolves in minutes 2016 MFMER slide-79
80 Case 4 (contd.): Now What? Fibrinogen (Clauss) 159 mg/dl D-dimer >20000 ng/ml <250 Soluble Fibrin Monomer Negative Factor XIII screen Clot dissolved before testing could be completed Clot solubility test for XIII screen Normally, a clot is stable for 2 hours in 5M urea or 2% acetic acid, while in factor XIII deficiency the clot is unstable and dissolves in minutes Plasminogen activity 34% Alpha-2 antiplasmin 35% MFMER slide-80
81 Fibrinolysis Tissue plasminogen activator (t-pa) Plasminogen activator inhibitor 1 and 2 Urokinase PLASMINOGEN PLASMIN Factor XIa, XIIa, Kallikrein α 2 -antiplasmin α 2 -macroglobulin FIBRINOGEN FIBRIN FIBRIN DEGRADATION PRODUCTS Thrombin Thrombin activable fibrinolysis inhibitor 2016 MFMER slide-81
82 Hyperfibrinolysis Primary Increased fibrinolytic activity independent of other factors Excess of plasminogen activators Deficiency of fibrinolysis inhibitors Secondary (e.g., DIC) Consequence of activation of coagulation and thrombin generation Stimulates the endothelium to produce increased amounts of t-pa 2016 MFMER slide-82
83 Case 4: Outcome Bone marrow biopsy: Involvement by metastatic adenocarcinoma: Immunohistochemistry for t-pa on bone marrow: t-pa expression in ER/PR positive cells (research assay) Plasma t-pa antigen: >150 ng/ml (Ref:<14.1 ng/ml) Profuse bleeding from the bone marrow biopsy site Hemoglobin 9.4 g/dl 6.4 g/dl 4 units of prbcs ε-aminocaproic acid infusion Weekly paclitaxel Bleeding and bruising improved Naina, H.V., et al. J Clin Oncol. 2010;28:e MFMER slide-83
84 Case 5: 17 year old male 2016 MFMER slide-84
85 Case 5: 17 year old male T-cell acute lymphoblastic leukemia Induction regimen included: Intrathecal cytarabine: Day 1 PEG Asparaginase: Day 4 Intrathecal methotrexate: Days 8, 29 In addition to: Vincristine; Prednisone, Daunorubicin MFMER slide-85
86 Case 5: 17 year old male T-cell acute lymphoblastic leukemia Induction regimen included: Intrathecal cytarabine: Day 1 PEG Asparaginase: Day 4 Intrathecal methotrexate: Days 8, 29 In addition to: Vincristine; Prednisone, Daunorubicin. Day 8: Post-intrathecal methotrexate Progressive back pain and lower extremity weakness 2016 MFMER slide-86
87 Case 5: 17 year old male T-cell acute lymphoblastic leukemia Induction regimen included: Intrathecal cytarabine: Day 1 PEG Asparaginase: Day 4 Intrathecal methotrexate: Days 8, 29 In addition to: Vincristine; Prednisone, Daunorubicin. Day 8: Post-intrathecal methotrexate Progressive back pain and lower extremity weakness 2016 MFMER slide-87
88 Case 5 (contd.) 2016 MFMER slide-88
89 Case 5 (contd.) Lab Prechemo Pre-LP Post-LP Post-cryo + FFP Ref. range Hemoglobin (g/dl) Platelets (x1000/mm3) PT (sec) APTT (sec) Fibrinogen (mg/dl) 326 < MFMER slide-89
90 Case 5 (contd.) Lab Prechemo Pre-LP Post-LP Post-cryo + FFP Ref. range Hemoglobin (g/dl) Platelets (x1000/mm3) PT (sec) APTT (sec) Fibrinogen (mg/dl) 326 < Patient underwent laminoforaminotomies with decompression of T11 through S1 and evacuation of hematoma 2016 MFMER slide-90
91 Case 5 (contd.) Fibrinogen (mg/dl) 200 Cryoprecipitate PEG-Asparaginase MFMER slide-91
92 L-Asparaginase Catalyzes the hydrolysis of L-asparagine (ASN) to L-aspartic acid and ammonia Depletion of the circulating pool of ASN Lymphoblasts typically have low levels of ASN synthetase activity and are dependent on extracellular sources of ASN for protein synthesis Depletion of ASN is associated with cell-cycle arrest in the G1 phase L-Asparaginase also catalyzes the hydrolysis of glutamine (GLU) to glutamic acid, resulting in depletion of circulating levels of GLU Three product types: Native E. coli asparaginase Pegylated form of the E. coli asparaginase (long half life) Erwinia asparaginase (Erwinase) 2016 MFMER slide-92
93 L-Asparaginase: Adverse Effect Profile Allergy/Hypersensitivity Hyperbilirubinemia Elevated liver enzymes Hyperglycemia Pancreatitis Nausea/vomiting Fatigue Neuropathy Pediatric (n=1274) Adult (n=76) Hypofibrinogenemia CNS ischemia Thrombosis Bleeding Stock, W et al. Leukemia & Lymphoma.2011; 52(12): MFMER slide-93
94 Thrombosis and Bleeding L-Asparaginase leads to asparagine depletion Decreased synthesis of: Fibrinogen Plasminogen Antithrombin (AT), protein C, and protein S AT and fibrinogen are particularly affected Reduction in AT and protein C leads to thrombosis Patients with AT <70% are at high risk for thrombosis Depletion of fibrinogen is associated with increased bleeding Patients with fibrinogen <100 mg/dl are at high risk of hemorrhage Stock, W et al. Leukemia & Lymphoma.2011; 52(12): MFMER slide-94
95 Risk Factors for Thrombosis Increasing age Pediatric patients: 5% Adult patients: 34% Adults > 30 years: 42% Presence of indwelling venous catheters Oral contraceptives Prednisone versus dexamethasone therapy Lower thrombosis rates reported for dexamethasone Inherited thrombotic diathesis e.g., factor V Leiden, protein S deficiency, protein C deficiency Stock, W et al. Leukemia & Lymphoma.2011; 52(12): MFMER slide-95
96 Suggested Monitoring During L- Asparaginase Rx 2016 MFMER slide-96
97 Suggested Monitoring During L- Asparaginase Rx Baseline (before first dose) 2016 MFMER slide-97
98 Suggested Monitoring During L- Asparaginase Rx Baseline (before first dose) APTT, PT, AT and fibrinogen Prolonged APTT: r/o LAC or heparin or factor deficiency Prolonged PT: r/o Vitamin K deficiency, liver disease, DIC 2016 MFMER slide-98
99 Suggested Monitoring During L- Asparaginase Rx Baseline (before first dose) Serially (after administration) APTT, PT, AT and fibrinogen Prolonged APTT: r/o LAC or heparin or factor deficiency Prolonged PT: r/o Vitamin K deficiency, liver disease, DIC 2016 MFMER slide-99
100 Suggested Monitoring During L- Asparaginase Rx Baseline (before first dose) Serially (after administration) APTT, PT, AT and fibrinogen Prolonged APTT: r/o LAC or heparin or factor deficiency Prolonged PT: r/o Vitamin K deficiency, liver disease, DIC APTT, PT, AT and fibrinogen Twice weekly after last dose of L-asparaginase until there is no evidence of ongoing coagulation factor depletion. This is typically one week after L-asparaginase but may be up to 3 or more weeks after the pegylated form 2016 MFMER slide-100
101 Suggested Monitoring During L- Asparaginase Rx Baseline (before first dose) Serially (after administration) APTT, PT, AT and fibrinogen Prolonged APTT: r/o LAC or heparin or factor deficiency Prolonged PT: r/o Vitamin K deficiency, liver disease, DIC APTT, PT, AT and fibrinogen Twice weekly after last dose of L-asparaginase until there is no evidence of ongoing coagulation factor depletion. This is typically one week after L-asparaginase but may be up to 3 or more weeks after the pegylated form Suggested replacement triggers during and after L-asparaginase therapy: Fibrinogen < 100 mg/dl AT < 60% (normal: %) 2016 MFMER slide-101
102 Summary 2016 MFMER slide-102
103 Summary Multiple presentations of cancer coagulopathy Asymptomatic laboratory abnormality Bleeding disorder Thrombotic disorder 2016 MFMER slide-103
104 Summary Multiple presentations of cancer coagulopathy Asymptomatic laboratory abnormality Bleeding disorder Thrombotic disorder Variable mechanisms of cancer coagulopathy Activation of coagulation and fibrinolysis Immune mediated Endothelial damage Therapy related Platelet dysfunction 2016 MFMER slide-104
105 Summary Multiple presentations of cancer coagulopathy Asymptomatic laboratory abnormality Bleeding disorder Thrombotic disorder Variable mechanisms of cancer coagulopathy Activation of coagulation and fibrinolysis Immune mediated Endothelial damage Therapy related Platelet dysfunction Recognition and appropriate laboratory testing critical for optimal management of the patient 2016 MFMER slide-105
106 Questions & Discussion 2016 MFMER slide-106
Acquired Inhibitors of Coagulation
 Acquired Inhibitors of Coagulation Christine L Kempton, MD, MSc Emory University Disclosures for In compliance with COI policy, ISTH requires the following disclosures to the session audience: Research
Acquired Inhibitors of Coagulation Christine L Kempton, MD, MSc Emory University Disclosures for In compliance with COI policy, ISTH requires the following disclosures to the session audience: Research
ACQUIRED COAGULATION ABNORMALITIES
 ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
Approach to bleeding disorders &treatment. by RAJESH.N General medicine post graduate
 Approach to bleeding disorders &treatment by RAJESH.N General medicine post graduate 2 Approach to a patient of bleeding diathesis 1. Clinical evaluation: History, Clinical features 2. Laboratory approach:
Approach to bleeding disorders &treatment by RAJESH.N General medicine post graduate 2 Approach to a patient of bleeding diathesis 1. Clinical evaluation: History, Clinical features 2. Laboratory approach:
Coagulation Disorders. Dr. Muhammad Shamim Assistant Professor, BMU
 Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
INHERITED COAGULOPATHY
 Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Hemostasis. PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures
 Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Hematologic Disorders. Assistant professor of anesthesia
 Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Bleeding Disorders. Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph
 Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
Bleeding and Thrombotic Disorders. Kristine Krafts, M.D.
 Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13
 Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
DIC. Bert Vandewiele Fellow Critical Care 23 May 2011
 DIC Bert Vandewiele Fellow Critical Care 23 May 2011 Dissiminated Intravascular Coagulopathie 11/3/2011 Dr. Bert Vandewiele 2 Dissiminated Intravascular Coagulopathie = Consumption coagulopathie = Defibrination
DIC Bert Vandewiele Fellow Critical Care 23 May 2011 Dissiminated Intravascular Coagulopathie 11/3/2011 Dr. Bert Vandewiele 2 Dissiminated Intravascular Coagulopathie = Consumption coagulopathie = Defibrination
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College
 Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Haemostasis & Coagulation disorders Objectives:
 Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche
 L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
John Davidson Consultant in Intensive Care Medicine Freeman Hospital, Newcastle upon Tyne
 John Davidson Consultant in Intensive Care Medicine Freeman Hospital, Newcastle upon Tyne Overview of coagulation Testing coagulation Coagulopathy in ICU Incidence Causes Evaluation Management Coagulation
John Davidson Consultant in Intensive Care Medicine Freeman Hospital, Newcastle upon Tyne Overview of coagulation Testing coagulation Coagulopathy in ICU Incidence Causes Evaluation Management Coagulation
Disseminated Intravascular Coagulation. M.Bahmanpour MD Assistant professor IUMS
 به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
به نام خدا Disseminated Intravascular Coagulation M.Bahmanpour MD Assistant professor IUMS Algorithm for Diagnosis of DIC DIC Score factor score Presence of known underlying disorder No= 0 yes=2 Coagolation
Disseminated intravascular coagulation (DIC) Dr. Klara Vezendi Szeged University Transfusiology Department
 Disseminated intravascular coagulation (DIC) Dr. Klara Vezendi Szeged University Transfusiology Department Disseminated intravascular coagulation (DIC, consumptive coagulopathy) is a clinicopathologic
Disseminated intravascular coagulation (DIC) Dr. Klara Vezendi Szeged University Transfusiology Department Disseminated intravascular coagulation (DIC, consumptive coagulopathy) is a clinicopathologic
A 60 year old woman with altered mental status and thrombotic microangiopathy. Josh Veatch
 A 60 year old woman with altered mental status and thrombotic microangiopathy Josh Veatch Previously healthy 60 year old woman 2 3 months of fatigue following a URI, transient episodes being out of it
A 60 year old woman with altered mental status and thrombotic microangiopathy Josh Veatch Previously healthy 60 year old woman 2 3 months of fatigue following a URI, transient episodes being out of it
Manejo del paciente con Enfermedad de Von Willebrand y Hemofilias Adquiridas
 Manejo del paciente con Enfermedad de Von Willebrand y Hemofilias Adquiridas Management of patients with Acquired von Willebrand Syndrome and Acquired Haemophilia A Enfermedad de Von Willebrand Augusto
Manejo del paciente con Enfermedad de Von Willebrand y Hemofilias Adquiridas Management of patients with Acquired von Willebrand Syndrome and Acquired Haemophilia A Enfermedad de Von Willebrand Augusto
Rip roaring hematologic dysfunction from solid organ malignancies
 Rip roaring hematologic dysfunction from solid organ malignancies A tale from UWMC hematology consult service in 4/2017 Lindsay Hannan, MD MSPH Discussant: Dr. Sioban Keel. Main objectives 1) DIC scoring
Rip roaring hematologic dysfunction from solid organ malignancies A tale from UWMC hematology consult service in 4/2017 Lindsay Hannan, MD MSPH Discussant: Dr. Sioban Keel. Main objectives 1) DIC scoring
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
DISSEMINATED INTRAVASCULAR COAGULATION (DIC) Pichika Chantrathammachart MD Division of Hematology, Department of Medicine Ramathibodi Hospital
 DISSEMINATED INTRAVASCULAR COAGULATION (DIC) Pichika Chantrathammachart MD Division of Hematology, Department of Medicine Ramathibodi Hospital Disseminated intravascular coagulation (DIC) Disseminated
DISSEMINATED INTRAVASCULAR COAGULATION (DIC) Pichika Chantrathammachart MD Division of Hematology, Department of Medicine Ramathibodi Hospital Disseminated intravascular coagulation (DIC) Disseminated
Platelet Disorders. By : Saja Al-Oran
 Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
Pathology note 8 BLEEDING DISORDER
 Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
MANAGEMENT OF COMMON BLEEDING DISORDERS. Auro Viswabandya Department of Haematology, CMC, Vellore
 MANAGEMENT OF COMMON BLEEDING DISORDERS Auro Viswabandya Department of Haematology, CMC, Vellore BLOOD CLOT : PRIMARY HAEMOSTASIS (Platelets) + SECONDARY HAEMOSTASIS (Coagulation Factors) HAEMOSTATIC DISORDERS
MANAGEMENT OF COMMON BLEEDING DISORDERS Auro Viswabandya Department of Haematology, CMC, Vellore BLOOD CLOT : PRIMARY HAEMOSTASIS (Platelets) + SECONDARY HAEMOSTASIS (Coagulation Factors) HAEMOSTATIC DISORDERS
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN
 Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
Haematological Emergencies (Part 1) Ray Mun Koo Haematology Advanced Trainee Canberra Hospital
 Haematological Emergencies (Part 1) Ray Mun Koo Haematology Advanced Trainee Canberra Hospital Case Number 1 43 year old male presenting with fevers, abdominal distension and weight gain over 2 weeks.
Haematological Emergencies (Part 1) Ray Mun Koo Haematology Advanced Trainee Canberra Hospital Case Number 1 43 year old male presenting with fevers, abdominal distension and weight gain over 2 weeks.
Chapter 3. Haemostatic abnormalities in patients with liver disease
 Chapter 3 Haemostatic abnormalities in patients with liver disease Ton Lisman, Frank W.G. Leebeek 1, and Philip G. de Groot Thrombosis and Haemostasis Laboratory, Department of Haematology, University
Chapter 3 Haemostatic abnormalities in patients with liver disease Ton Lisman, Frank W.G. Leebeek 1, and Philip G. de Groot Thrombosis and Haemostasis Laboratory, Department of Haematology, University
Haemorrhagic Disorders. Dr. Bashar Department of Pathology Mosul Medical College
 Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion
 This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
Acquired Von Willebrand Syndrome and Heyde s Syndrome. Debra L. Smith, MD, PhD Hematology Fellows Conference April 8, 2016
 Acquired Von Willebrand Syndrome and Heyde s Syndrome Debra L. Smith, MD, PhD Hematology Fellows Conference April 8, 2016 Objectives Describe acquired von Willebrand syndrome (AVWS) clinical presentation
Acquired Von Willebrand Syndrome and Heyde s Syndrome Debra L. Smith, MD, PhD Hematology Fellows Conference April 8, 2016 Objectives Describe acquired von Willebrand syndrome (AVWS) clinical presentation
Introduction to coagulation and laboratory tests
 Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
BLEEDING DISORDERS Simple complement:
 BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
Optimal Utilization of Thrombophilia Testing
 Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
Heme (Bleeding and Coagulopathies) in the ICU
 Heme (Bleeding and Coagulopathies) in the ICU General Topics To Discuss Transfusions DIC Thrombocytopenia Liver and renal disease related bleeding Lack of evidence in managing critical illness related
Heme (Bleeding and Coagulopathies) in the ICU General Topics To Discuss Transfusions DIC Thrombocytopenia Liver and renal disease related bleeding Lack of evidence in managing critical illness related
Effective Date: Approved by: Laboratory Director, Jerry Barker (electronic signature)
 1 of 5 Policy #: 702 (PHL-702-05) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 Subject: TRANSFUSION GUIDELINES Approved by: Laboratory Director, Jerry Barker (electronic signature) Approved by: Laboratory
1 of 5 Policy #: 702 (PHL-702-05) Effective Date: 9/30/2004 Reviewed Date: 8/1/2016 Subject: TRANSFUSION GUIDELINES Approved by: Laboratory Director, Jerry Barker (electronic signature) Approved by: Laboratory
Approach To A Bleeding Patient
 ABDUL MAJEED, RAHUL RAJEEV REVIEW ARTICLE INTRODUCTION Hemostasis is the process of forming clots in the walls of damaged blood vessels and preventing blood loss while maintaining blood in a fluid state
ABDUL MAJEED, RAHUL RAJEEV REVIEW ARTICLE INTRODUCTION Hemostasis is the process of forming clots in the walls of damaged blood vessels and preventing blood loss while maintaining blood in a fluid state
Prothrombin Complex Concentrate- Octaplex. Octaplex
 Prothrombin Complex Concentrate- Concentrated Factors Prothrombin Complex Concentrate (PCC) 3- factor (factor II, IX, X) 4-factor (factors II, VII, IX, X) Activated 4-factor (factors II, VIIa, IX, X) Coagulation
Prothrombin Complex Concentrate- Concentrated Factors Prothrombin Complex Concentrate (PCC) 3- factor (factor II, IX, X) 4-factor (factors II, VII, IX, X) Activated 4-factor (factors II, VIIa, IX, X) Coagulation
Blood clotting. Subsequent covalent cross-linking of fibrin by a transglutaminase (factor XIII) further stabilizes the thrombus.
 Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Coagulation, Haemostasis and interpretation of Coagulation tests
 Coagulation, Haemostasis and interpretation of Coagulation tests Learning Outcomes Indicate the normal ranges for routine clotting screen and explain what each measurement means Recognise how to detect
Coagulation, Haemostasis and interpretation of Coagulation tests Learning Outcomes Indicate the normal ranges for routine clotting screen and explain what each measurement means Recognise how to detect
PCCN Review Hematology
 PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
Easy bruising vs Coagulopathy
 Easy bruising vs Coagulopathy Sept. 19, 2015 Lakehead Summer School Chris Hillis, MD MSc FRCPC hillis@hhsc.ca @HemeHillis Aim & Objectives Aim: To increase comfort in detecting non-pathologic bleeding
Easy bruising vs Coagulopathy Sept. 19, 2015 Lakehead Summer School Chris Hillis, MD MSc FRCPC hillis@hhsc.ca @HemeHillis Aim & Objectives Aim: To increase comfort in detecting non-pathologic bleeding
Document Title: Hemostasis: Platelet and Coagulation Disorders. Author(s): Joseph H. Hartmann (University of Michigan), DO 2012
 Project: Ghana Emergency Medicine Collaborative Document Title: Hemostasis: Platelet and Coagulation Disorders Author(s): Joseph H. Hartmann (University of Michigan), DO 2012 License: Unless otherwise
Project: Ghana Emergency Medicine Collaborative Document Title: Hemostasis: Platelet and Coagulation Disorders Author(s): Joseph H. Hartmann (University of Michigan), DO 2012 License: Unless otherwise
Part IV Antithrombotics, Anticoagulants and Fibrinolytics
 Part IV Antithrombotics, Anticoagulants and Fibrinolytics "The meaning of good and bad, of better and worse, is simply helping or hurting" Emerson Chapter 16: Blood Coagulation and Fibrinolytic System
Part IV Antithrombotics, Anticoagulants and Fibrinolytics "The meaning of good and bad, of better and worse, is simply helping or hurting" Emerson Chapter 16: Blood Coagulation and Fibrinolytic System
Blood Transfusion Guidelines in Clinical Practice
 Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
HEMOSTASIS/THROMBOSIS II
 HEMOSTASIS/THROMBOSIS II Congenital/Acquired Hemorrhagic Disorders & Their Treatment COAGULATION TESTING!Bleeding time primary screening test for platelet function!if bleeding time abnormal!platelet Aggregation
HEMOSTASIS/THROMBOSIS II Congenital/Acquired Hemorrhagic Disorders & Their Treatment COAGULATION TESTING!Bleeding time primary screening test for platelet function!if bleeding time abnormal!platelet Aggregation
3/19/2012. What is the indication for anticoagulation? Has the patient previously been on warfarin? If so, what % of the time was the INR therapeutic?
 Abigail E. Miller, PharmD, BCPS Clinical Specialist, Cardiology University of North Carolina Hospitals I have no personal financial relationships with the manufacturers of the products to disclose. Boehringer
Abigail E. Miller, PharmD, BCPS Clinical Specialist, Cardiology University of North Carolina Hospitals I have no personal financial relationships with the manufacturers of the products to disclose. Boehringer
Hematology Review. CCRN exam. The Coagulation Cascade. The Coagulation Cascade. Components include: Intrinsic pathway Extrinsic pathway Common pathway
 CCRN exam Hematology Review CCRN Review October 2013 Department of Critical Care Nursing Hematology is 2% of the exam Focus on coagulation cascade, DIC, and HIT Anatomy of the hematologic system Bone marrow
CCRN exam Hematology Review CCRN Review October 2013 Department of Critical Care Nursing Hematology is 2% of the exam Focus on coagulation cascade, DIC, and HIT Anatomy of the hematologic system Bone marrow
Blood coagulation and fibrinolysis. Blood clotting (HAP unit 5 th )
 Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Bleeding Disorders HOPE Maram Al-anbar
 Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
Primary Exam Physiology lecture 5. Haemostasis
 Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura
 Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura Kristen Knoph, PharmD, BCPS PGY2 Pharmacotherapy Resident Pharmacy Grand Rounds April 25, 2017 2016 MFMER slide-1 Objectives
Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura Kristen Knoph, PharmD, BCPS PGY2 Pharmacotherapy Resident Pharmacy Grand Rounds April 25, 2017 2016 MFMER slide-1 Objectives
COAGULATIONS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin)
 COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
Approach to disseminated intravascular coagulation
 Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Disseminated Intravascular Coagulation (DIC) Seminar. Ron Kopilov 4 th year Medical Student, Tel Aviv University Internal Medicine A 8.3.
 Disseminated Intravascular Coagulation (DIC) Seminar Ron Kopilov 4 th year Medical Student, Tel Aviv University Internal Medicine A 8.3.2012 1 Our plan: Understand the pathophysiology Identify risk factors
Disseminated Intravascular Coagulation (DIC) Seminar Ron Kopilov 4 th year Medical Student, Tel Aviv University Internal Medicine A 8.3.2012 1 Our plan: Understand the pathophysiology Identify risk factors
Disseminated Intravascular Coagulation: A Case-Based Approach
 Disseminated Intravascular Coagulation: A Case-Based Approach Thursday, May 17 9:45 11 am Note one action you ll take after attending this session: Rebecca Martin, BSN, RN, OCN, BMTCN Staff RN/Educator
Disseminated Intravascular Coagulation: A Case-Based Approach Thursday, May 17 9:45 11 am Note one action you ll take after attending this session: Rebecca Martin, BSN, RN, OCN, BMTCN Staff RN/Educator
Anticoagulants. Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT
 Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
LAMA SHATAT TTP, ITP, DIC
 TTP, ITP, DIC Reduction in platelet number (thrombocytopenia) constitutes an important cause of generalized bleeding. A count less than 100,000 platelets/μl is generally considered to constitute thrombocytopenia.
TTP, ITP, DIC Reduction in platelet number (thrombocytopenia) constitutes an important cause of generalized bleeding. A count less than 100,000 platelets/μl is generally considered to constitute thrombocytopenia.
Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma
 Chapt. 45 Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma Inheritance of X-linked gene for Factor VIII hemophilia A Explain the
Chapt. 45 Ch. 45 Blood Plasma proteins, Coagulation and Fibrinolysis Student Learning Outcomes: Describe basic components of plasma Inheritance of X-linked gene for Factor VIII hemophilia A Explain the
What is meant by Thrombotic Microangiopathy (TMA)?
 What is meant by Thrombotic Microangiopathy (TMA)? Thrombotic Microangiopathy (TMA) is a group of disorders characterized by injured endothelial cells, microangiopathic hemolytic anemia (MAHA), with its
What is meant by Thrombotic Microangiopathy (TMA)? Thrombotic Microangiopathy (TMA) is a group of disorders characterized by injured endothelial cells, microangiopathic hemolytic anemia (MAHA), with its
Epidemiology of Thrombosis in Patients with Malignancy. Cancer and Venous Thromboembolism. Chew HK, Arch Int Med, Feb Blom et al, JAMA, Feb 2005
 Cancer and Venous Thromboembolism Objectives 1. Epidemiology of thrombosis in patients with malignancy 2. Anticancer agents and thrombosis 3. Current treatment protocols at UHN 4. Prevention of DVT 5.
Cancer and Venous Thromboembolism Objectives 1. Epidemiology of thrombosis in patients with malignancy 2. Anticancer agents and thrombosis 3. Current treatment protocols at UHN 4. Prevention of DVT 5.
Thrombotic Thrombocytopenic
 The Treatment of TTP and the Prevention of Relapses GERALD APPEL, MD Professor of Clinical Medicine Columbia University College of Physicians and Surgeons NY-Presbyterian Hospital New York, New York Thrombotic
The Treatment of TTP and the Prevention of Relapses GERALD APPEL, MD Professor of Clinical Medicine Columbia University College of Physicians and Surgeons NY-Presbyterian Hospital New York, New York Thrombotic
Moath Darweesh. Omar Sami. Saleem Khreisha. 1 P a g e
 7 Moath Darweesh Omar Sami Saleem Khreisha 1 P a g e -First of all, I want to give a quick revision to simplify the whole hemostasis mechanism, it will be much easier here with me. Enjoy (you can skip
7 Moath Darweesh Omar Sami Saleem Khreisha 1 P a g e -First of all, I want to give a quick revision to simplify the whole hemostasis mechanism, it will be much easier here with me. Enjoy (you can skip
Bleeding, Coagulopathy, and Thrombosis in the Injured Patient
 Bleeding, Coagulopathy, and Thrombosis in the Injured Patient June 7, 2008 Kristan Staudenmayer, MD Trauma Fellow UCSF/SFGH Trauma deaths Sauaia A, et al. J Trauma. Feb 1995;38(2):185 Coagulopathy is Multi-factorial
Bleeding, Coagulopathy, and Thrombosis in the Injured Patient June 7, 2008 Kristan Staudenmayer, MD Trauma Fellow UCSF/SFGH Trauma deaths Sauaia A, et al. J Trauma. Feb 1995;38(2):185 Coagulopathy is Multi-factorial
, Malcolm Tait, Barry Frank Jacobson, Evashin Pillay and Susan J. Louw. Elizabeth Sarah Mayne *
 Mayne et al. Thrombosis Journal (2018) 16:30 https://doi.org/10.1186/s12959-018-0184-2 CASE REPORT Open Access Combination of acquired von Willebrand syndrome (AVWS) and Glanzmann thrombasthenia in monoclonal
Mayne et al. Thrombosis Journal (2018) 16:30 https://doi.org/10.1186/s12959-018-0184-2 CASE REPORT Open Access Combination of acquired von Willebrand syndrome (AVWS) and Glanzmann thrombasthenia in monoclonal
Sysmex Educational Enhancement and Development No
 SEED Coagulation Sysmex Educational Enhancement and Development No 2 2016 An approach to the bleeding patient The purpose of this newsletter is to provide an overview of the approach to the bleeding patient
SEED Coagulation Sysmex Educational Enhancement and Development No 2 2016 An approach to the bleeding patient The purpose of this newsletter is to provide an overview of the approach to the bleeding patient
Introduction to von Willebrand Disease Mary Lesh RN, MS, CPNP
 Introduction to von Willebrand Disease Mary Lesh RN, MS, CPNP OVERVIEW Von Willebrand Disease (VWD) is the most common hereditary bleeding disorder in humans, with an estimated prevalence ranging upward
Introduction to von Willebrand Disease Mary Lesh RN, MS, CPNP OVERVIEW Von Willebrand Disease (VWD) is the most common hereditary bleeding disorder in humans, with an estimated prevalence ranging upward
von Willebrand Disease
 von Willebrand Disease Jeremy Robertson Paediatric Haematologist Royal Children s s Hospital & Pathology Queensland Foglo,, April 1924: the journey begins Oskar and Augusta sail to Helsinki... ...to o
von Willebrand Disease Jeremy Robertson Paediatric Haematologist Royal Children s s Hospital & Pathology Queensland Foglo,, April 1924: the journey begins Oskar and Augusta sail to Helsinki... ...to o
Important Considera/ons for Coagula/on Tests on Children and Neonates
 Important Considera/ons for Coagula/on Tests on Children and Neonates Cindy Neunert, MD MSCS Associate Professor Pediatric Hematology/Oncology/Bone Marrow Transplant Columbia University Medical Center
Important Considera/ons for Coagula/on Tests on Children and Neonates Cindy Neunert, MD MSCS Associate Professor Pediatric Hematology/Oncology/Bone Marrow Transplant Columbia University Medical Center
Hemostasis and thrombosis in patients with liver disease. Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands
 Hemostasis and thrombosis in patients with liver disease Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands Importance of the liver in hemostasis Synthesis of Coagulation factors Fibrinolytic proteins
Hemostasis and thrombosis in patients with liver disease Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands Importance of the liver in hemostasis Synthesis of Coagulation factors Fibrinolytic proteins
Adult Reversal of Anticoagulation and Anti-platelet Agents for Life- Threatening Bleeding or Emergency Surgery Protocol
 Adult Reversal of Anticoagulation and Anti-platelet Agents for Life- Threatening Bleeding or Emergency Surgery Protocol Page Platelet Inhibitors 2 Aspirin, Clopidogrel (Plavix), Prasugrel (Effient) & Ticagrelor
Adult Reversal of Anticoagulation and Anti-platelet Agents for Life- Threatening Bleeding or Emergency Surgery Protocol Page Platelet Inhibitors 2 Aspirin, Clopidogrel (Plavix), Prasugrel (Effient) & Ticagrelor
Topics of today lectures: Hemostasis
 Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms of hemostasis - Vascular contraction - Platelets plug - Blood coagulation (clotting) - Structure and functions of platelets - Blood
Agent Dose MoA/PK/Admin Adverse events Disadvantages Protamine Heparin: 1mg neutralizes ~ 100 units Heparin neutralization in ~ 5 min
 Nanik (Nayri) Hatsakorzian Pharm.D/MPH candidate 2014 Touro University College of Pharmacy CA Bleeding Reversal Agents Agent Dose MoA/PK/Admin Adverse events Disadvantages Protamine Heparin: 1mg neutralizes
Nanik (Nayri) Hatsakorzian Pharm.D/MPH candidate 2014 Touro University College of Pharmacy CA Bleeding Reversal Agents Agent Dose MoA/PK/Admin Adverse events Disadvantages Protamine Heparin: 1mg neutralizes
Chapter 46. Care of the Patient with a Blood or Lymphatic Disorder
 Chapter 46 Care of the Patient with a Blood or Lymphatic Disorder All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Components of the Blood Red
Chapter 46 Care of the Patient with a Blood or Lymphatic Disorder All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Components of the Blood Red
Recommendations for Celiac Disease Testing. IgA & ttg IgA
 Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Hemostatic derangement in Dengue infection
 Hemostatic derangement in Dengue infection By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University
Hemostatic derangement in Dengue infection By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University
What are blood clots?
 What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
What are blood clots? Dr Matthew Fay GP Principal The Willows Medical Practice- Queensbury GPwSI and Co-Founder Westcliffe Cardiology Service GP Partner Westcliffe Medical Group Created 5/31/18 Dr. Matthew
Approach to bleeding
 Approach to bleeding By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University The mechanism of
Approach to bleeding By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University The mechanism of
Medical Surgical Review Handout- Hematology/Oncology 2016
 Medical Surgical Review Handout- Hematology/Oncology 2016 Overview Blood circulates in the cardiovascular system o Carries oxygen to the cells o Carries waste away from the cells Functions of blood o Transportation:
Medical Surgical Review Handout- Hematology/Oncology 2016 Overview Blood circulates in the cardiovascular system o Carries oxygen to the cells o Carries waste away from the cells Functions of blood o Transportation:
UNIT VI. Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav. Copyright 2011 by Saunders, an imprint of Elsevier Inc.
 UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
Hemostatic System - general information
 PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
Blood Components & Indications for Transfusion. Neda Kalhor
 Blood Components & Indications for Transfusion Neda Kalhor Blood products Cellular Components: Red blood cells - Leukocyte-reduced RBCs - Washed RBCs - Irradiated RBCs Platelets - Random-donor platelets
Blood Components & Indications for Transfusion Neda Kalhor Blood products Cellular Components: Red blood cells - Leukocyte-reduced RBCs - Washed RBCs - Irradiated RBCs Platelets - Random-donor platelets
Hematologic changes in systemic diseases. Chittima Sirijerachai
 Hematologic changes in systemic diseases Chittima Sirijerachai Systemic diseases Infection Renal diseases Liver diseases Connective tissue diseases Malignancy Anemia of chronic disease (ACD) Chronic infections:
Hematologic changes in systemic diseases Chittima Sirijerachai Systemic diseases Infection Renal diseases Liver diseases Connective tissue diseases Malignancy Anemia of chronic disease (ACD) Chronic infections:
Challenges in Coagulation
 Challenges in Coagulation Michael H. Rosove, MD Clinical Professor of Medicine UCLA Division of Hematology-Oncology April 30, 2016 Vitamin K Deficiency Vitamin K1 source from diet Vitamin K2 source from
Challenges in Coagulation Michael H. Rosove, MD Clinical Professor of Medicine UCLA Division of Hematology-Oncology April 30, 2016 Vitamin K Deficiency Vitamin K1 source from diet Vitamin K2 source from
11. An acute leukemia causing. 12. An adult patient presents with acute. 13. Anemia due to renal failure may be
 Hematology Study online at 1. A 23 year old white female has weakness, fatigue and has developed a habit of chewing ice. What are the expected findings in regard to TIBC and Ferritin? 2. A 25 year old
Hematology Study online at 1. A 23 year old white female has weakness, fatigue and has developed a habit of chewing ice. What are the expected findings in regard to TIBC and Ferritin? 2. A 25 year old
Bleeding disorders. Hemostatic failure: Inappropriate and excessive bleeding either spontaneous or in response to injury.
 1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
Hematological Issues in Critically Ill Patients with Cancer
 Hematological Issues in Critically Ill Patients with Cancer Karen S. Carlson, MD, PhD a, Maria T. DeSancho, MD, MSc b, * KEYWORDS Cancer Thrombosis Hemostasis Critical illness Patients with solid and hematologic
Hematological Issues in Critically Ill Patients with Cancer Karen S. Carlson, MD, PhD a, Maria T. DeSancho, MD, MSc b, * KEYWORDS Cancer Thrombosis Hemostasis Critical illness Patients with solid and hematologic
A CASE OF ECCHYMOSIS IN AN ELDERLY LADY
 A CASE OF ECCHYMOSIS IN AN ELDERLY LADY Inter-hospital Geriatrics Meeting 28 Oct 2011 Speaker: Cheng Jen Ngai Chairperson: Dr. CS Leung Caritas Medical Centre Background Information F/ 85 years old, widow,
A CASE OF ECCHYMOSIS IN AN ELDERLY LADY Inter-hospital Geriatrics Meeting 28 Oct 2011 Speaker: Cheng Jen Ngai Chairperson: Dr. CS Leung Caritas Medical Centre Background Information F/ 85 years old, widow,
Things to never miss in the office. Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC
 Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute lung injury (ALI) transfusion-related, 363 372. See also Transfusion-related acute lung injury (TRALI) ALI. See Acute lung injury
Index Note: Page numbers of article titles are in boldface type. A Acute lung injury (ALI) transfusion-related, 363 372. See also Transfusion-related acute lung injury (TRALI) ALI. See Acute lung injury
THROMBOSIS AND BLEEDING
 THROMBOSIS AND BLEEDING Klara Gadó MD. PhD. Senior Professor of Internal Medicine Semmelweis University, Budapest What is thrombosis? formation of a blood clot in a blood vessel Blood can not flow Organ
THROMBOSIS AND BLEEDING Klara Gadó MD. PhD. Senior Professor of Internal Medicine Semmelweis University, Budapest What is thrombosis? formation of a blood clot in a blood vessel Blood can not flow Organ
Thrombosis. By Dr. Sara Mohamed Abuelgasim
 Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
Thrombosis By Dr. Sara Mohamed Abuelgasim 1 Thrombosis Unchecked, blood coagulation would lead to dangerous occlusion of blood vessels if the protective mechanisms of coagulation factor inhibitors, blood
Hemostasis. Clo)ng factors and Coagula4on NORMAL COAGULATION. Overview of blood coagula4on. The Cascade Theory 5/1/12. Clot
 Hemostasis Clo)ng factors and Coagula4on Dr Badri Paudel www.badripaudel.com Hemostasis is defined as a property of circula4on whereby blood is maintained within a vessel and the ability of the system
Hemostasis Clo)ng factors and Coagula4on Dr Badri Paudel www.badripaudel.com Hemostasis is defined as a property of circula4on whereby blood is maintained within a vessel and the ability of the system
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89
 Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
There are two main causes of a low platelet count
 Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Bleeding and Haemostasis. Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon
 Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Bleeding and Haemostasis Saman W.Boskani HDD, FIBMS Maxillofacial Surgeon 1 Beeding Its escaping or extravasation of blood contents from blood vessels Types: - Arterial - Venous - Capillary Differences
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
CrackCast Episode 7 Blood and Blood Components
 CrackCast Episode 7 Blood and Blood Components Episode Overview: 1) Describe the 3 categories of blood antigens 2) Who is the universal donor and why? 3) Define massive transfusion 4) List 5 physiologic
CrackCast Episode 7 Blood and Blood Components Episode Overview: 1) Describe the 3 categories of blood antigens 2) Who is the universal donor and why? 3) Define massive transfusion 4) List 5 physiologic
