Radiological changes on CT after stereotactic body radiation therapy to non-spine bone metastases: a descriptive series
|
|
|
- Jeffry French
- 6 years ago
- Views:
Transcription
1 Editor s note: Palliative Radiotherapy Column features articles emphasizing the critical role of radiotherapy in palliative care. Chairs to the columns are Dr. Edward L. W. Chow from Odette Cancer Centre, Sunnybrook Health Sciences Centre in Toronto and Dr. Stephen Lutz from Blanchard Valley Regional Cancer Center in Findlay, gathering a group of promising researchers in the field to make it an excellent column. The column includes original research manuscripts and timely review articles and perspectives relating to palliative radiotherapy, editorials and commentaries on recently published trials and studies. Palliative Radiotherapy Column (Original Article) Radiological changes on CT after stereotactic body radiation therapy to non-spine bone metastases: a descriptive series Nicholas Chiu 1, Linda Probyn 2, Srinivas Raman 1, Rachel McDonald 1, Ian Poon 1, Darby Erler 1, Drew Brotherston 1, Hany Soliman 1, Patrick Cheung 1, Hans Chung 1, William Chu 1, Andrew Loblaw 1, Nemica Thavarajah 1, Catherine Lang 2, Lee Chin 3, Edward Chow 1, Arjun Sahgal 1 1 Department of Radiation Oncology, 2 Department of Medical Imaging, 3 Department of Physics, Sunnybrook Health Sciences Centre, University of Toronto, Toronto, Ontario, Canada Contributions: (I) Conception and design: N Chiu, S Raman, E Chow; (II) Administrative support: None; (III) Provision of study materials or patients: All authors. (IV) Collection and assembly of data: R McDonald, N Thavarajah, C Lang; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Dr. Edward Chow, MBBS, MSc, PhD, FRCPC. Department of Radiation Oncology, Odette Cancer Centre, Sunnybrook Health Sciences Centre, 2075 Bayview Avenue, Toronto, ON M4N 3M5, Canada. Edward.Chow@sunnybrook.ca. Background: In recent years, stereotactic body radiation therapy (SBRT) has become increasingly used for the management of non-spine bone metastases. Few studies have examined the radiological changes in bone metastases after treatment with SBRT and there is no consensus about what constitutes radiologic response to therapy. This article describes various changes on CT after SBRT to non-spine bone metastases in eight selected cases. Methods: A retrospective review was conducted for patients treated with SBRT to non-spine bone metastases between November 2011 and April 2014 at Sunnybrook Health Sciences Centre. A musculoskeletal radiologist identified eight illustrative cases of interest and provided a description of the findings. Results: Different radiological changes following SBRT were described, including: remineralization of lytic bone metastases, demineralization of sclerotic bone metastases, pathologic fracture, size progression and response in different lesions, as well as lung fibrosis after SBRT to a rib metastasis. Conclusions: We reviewed the radiological images of eight selected cases after SBRT to nonspine bone metastases and a number of characteristic findings were highlighted. We recommend future studies to correlate radiologic changes with clinical outcomes including pain relief, toxicity and long-term local control. Keywords: Stereotactic body radiation therapy (SBRT); non-spine bone metastases; CT Submitted Nov 13, Accepted for publication Dec 25, doi: /apm View this article at:
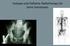
2 Annals of Palliative Medicine, Vol 5, No 2 April Introduction Bone metastases are commonly observed in patients with advanced cancer, with an approximate incidence of 70 85% (1). Single-fraction or conventionally-fractionated external beam radiation therapy (EBRT) has traditionally been used to treat non-spine bone metastases, and has been shown to decrease pain and improve quality of life (2). Stereotactic body radiation therapy (SBRT) is a more recently developed form of image-guided radiation therapy (3). SBRT allows for more precise delivery of higher biologically effective doses (BED) of radiation to smaller target volumes (4), thus minimizing the dose to surrounding organs at risk (5). In addition, with its increased precision and higher dose of radiation, SBRT may shift the aim of therapy from pain and symptom relief alone towards greater local tumor control and durable pain reduction, making it a promising treatment for patients with oligometastatic disease. SBRT is also a treatment option for patients who have been irradiated previously with low dose radiation treatment (5), and can be effective in patients with radioresistant tumors (6). For the above reasons, SBRT has become a more frequently-used option for the management of non-spine bone metastases. Few studies have examined the outcomes after SBRT to non-spine bone metastases patients (7). The use of CT imaging to analyze changes in tumors before and after SBRT may be one modality by which to predict clinical outcomes and determine response to therapy. The current report reviews the various radiological changes after SBRT in eight selected cases. Figure 1 Baseline image (Dec 7, 2011). Methods A retrospective review was conducted for patients treated with SBRT to non-spine bone metastases between November 2011 and April 2014 at Sunnybrook Health Sciences Centre. All patients underwent at least one CT scan prior to SBRT and at least one CT scan after treatment. A musculoskeletal radiologist identified eight illustrative cases of interest with CT images before and after SBRT for these patients. Results and discussion Case 1: lung cancer lytic metastasis becomes more sclerotic after SBRT Figures 1-3 are axial CT images through the chest of a Figure 2 Follow-up image (Nov 1, 2012). patient with a lytic lesion in the right lateral rib. The patient had a primary lung cancer and started SBRT (35 Gy in 5 fractions) on January 23, Ten months after radiation, the lesion decreased in size and become more sclerotic. However, follow up imaging five months later showed an increase in the size of the lesion. In the context of conventional EBRT, studies investigating CT density after radiotherapy have been published and the remineralization of osteolytic bone metastases has been well-documented (8,9). In a randomized controlled trial investigating bone remineralization published in 1999, Koswig et al. found percent bone density change following
3 118 Chiu et al. CT changes after SBRT to non-spine bone metastases Figure 3 Follow-up image (Apr 25, 2013). Figure 5 Follow-up image (Dec 14, 2013). tumor progression. Case 2: prostate cancer sclerotic bone metastasis becomes less dense after SBRT Figure 4 Baseline image (Apr 18, 2013). radiation to be 173% and 120% in the multiple and single fraction groups, respectively (9). The observation of the lesion in this case becoming more sclerotic is consistent with the response that should be expected of a typical lytic tumor following radiation. As this patient s lesion became more sclerotic 10 months after radiation, this case suggests that SBRT also causes remineralization of lytic non-spine bone metastases. However, though it seems the patient had an initial response with sclerosis of the lesion, local control was not durable, as evidenced by an increase in the size of the lesion five months later. The patient ultimately required a salvage rib rection 18 months after treatment due to Figures 4,5 are axial CT images through the pelvis of a patient with a sclerotic lesion in the right inferior pubic ramus. The patient had a primary prostate cancer and started SBRT (35 Gy in 5 fractions) on June 11, Follow-up CT imaging 6 months later demonstrated increased lucency in the lateral aspect of the lesion suggesting interval improvement. In the context of conventional EBRT, the demineralization of sclerotic metastases following radiation is less welldocumented than the remineralization of lytic metastases; however, it has been explored previously (10). In a study of 14 patients with vertebral metastases arising from breast carcinoma, Wachenfeld et al. observed a decrease in bone density following radiation for sclerotic lesions (10). The observation of the sclerotic lesion in our present prostate cancer metastasis case becoming more lucent is consistent with the response Wachenfield et al. described of a typical sclerotic tumor following radiation. Review of this patient s clinical history showed that the lesion was asymptomatic before treatment and as of September 2014, he continued to have durable local control of the lesion. This case suggests that demineralization of sclerotic non-spine bone metastases after SBRT could also be suggestive of reponse.
4 Annals of Palliative Medicine, Vol 5, No 2 April Figure 6 Baseline image (Oct 3, 2013). Figure 8 Baseline image (Oct 3, 2013). Figure 7 Follow-up image (Jun 19, 2014). Figure 9 Follow-up image (Dec 5, 2013). Case 3: lytic pelvic metastasis decreases in size after SBRT Figures 6,7 are axial CT images through the pelvis of a patient with a lytic lesion in the left ilium. The patient had a primary renal cell carcinoma and started SBRT (30 Gy in 5 fractions) on November 25, Images demonstrate that the lesion decreased in size after 7 months. This case is one example of a lesion s clear decrease in size following SBRT. Case 4: renal cell carcinoma lytic metastasis shows more lysis immediately after SBRT then becomes more sclerotic Figures 8-10 are axial CT images through the pelvis (on bone windows) of a patient with a lytic lesion in the left ilium. The patient had a primary renal cell carcinoma and started SBRT (30 Gy in 5 fractions) on November 25, 2013 Initially, 1 month after radiation, the lesion increased in size and became more lytic; it then decreased in size 4 months later with increased sclerosis. The patient's lesion has been stable as of April 24, Metastases arising from renal cancer have had a reputation of being radio-resistant (6,9,11). However, more recent studies suggest that SBRT can overcome radio-resistance with higher BED (6,11-14). The radiosensitivity of renal cancer to SBRT is believed to be due to the generation
5 120 Chiu et al. CT changes after SBRT to non-spine bone metastases Figure 10 Follow-up image (Apr 24, 2014). Figure 12 Follow-up image (Mar 9, 2012). imaging may not accurately represent a patient s long-term response to SBRT. As such, a longer follow-up period may be required to determine a patient s true response to SBRT. Case 5: bone metastasis progression after SBRT Figure 11 Baseline image (Sep 1, 2011). of ceramide, which induces endothelial apoptosis the main cause of radiation-induced cell death in renal cell carcinoma (15). However, the ceramide pathway is activated only in response to a high-dose of radiation per fraction (15). Therefore, SBRT is believed to be more effective than conventional EBRT in the renal cancer population due to its use of higher-dose radiation. With radiological evidence of increased sclerosis after SBRT, the current case suggests that SBRT can cause remineralization of lytic lesions arising from renal cell carcinoma. In addition, as illustrated by the initial increase in size and lytic activity of the lesion in Figure 11, initial changes observed in the radiological Figures 11,12 are axial CT images through the pelvis of a patient with a lytic lesion in the anterior right ilium. The patient had a primary lung cancer and started SBRT (35 Gy in 5 fractions) on November 21, Images demonstrate that the lytic lesion increased in size after 4 months. Prospective phase II studies from several centers have consistently showed very high levels of local tumor control with SBRT (16). Despite high reported levels of local tumor control with SBRT, tumor progression can still occur as in the present case. For example, in the series by Owen et al., 7 out of 74 patients treated with SBRT for non-spine bone metastases all developed local progression with a median time to failure of 2.8 months (7). The current case is an example where no initial response or control was seen, and the bone metastasis progressed shortly after SBRT. Case 6: breast cancer lytic metastasis improves after SBRT Figures 13,14 are axial CT images through the chest (on bone windows) of a patient with a lytic lesion in the left aspect of the sternal body. The patient had a primary breast cancer and started SBRT (35 Gy in 5 fractions) on April 11, Eleven months after radiation treatment, the lesion has become more lucent/lytic with decreased soft tissue
6 Annals of Palliative Medicine, Vol 5, No 2 April Figure 13 Baseline image (Mar 6, 2013). Figure 15 Baseline image (Dec 12, 2013). Figure 14 Follow-up image (Mar 21, 2014). Figure 16 Follow-up image (May 3, 2015). attenuation representing increased marrow fat at the site of the lesion. Review of the patient s clinical history shows that despite the lesion becoming more lytic initially following SBRT, the patient experienced significant pain relief and had durable local control as of January This clinical observation is consistent with the radiologic observation of decreased soft tissue in the tumor and represents an improvement in the metastasis after SBRT. Case 7: lung fibrosis after SBRT Figures 15,16 are axial CT images through the chest of a patient with a lytic lesion in the right lateral rib. The patient had a primary renal cell carcinoma and started SBRT (50 Gy in 5 fractions) on January 13, Fifteen months after SBRT, the lesion decreased in size and there were associated post-radiation fibrotic changes in the right lung with bronchiectasis, subpleural airspace opacity, and volume loss. Pulmonary fibrosis has been well documented as a possible SBRT-induced lung injury (17,18). For example, Guckenberger et al. noted that after single fraction treatment in lung SBRT, dense consolidation and retraction of pulmonary tissue indicating fibrosis were observed in 43% and 50% after 6 and 12 months, respectively (18). For
7 122 Chiu et al. CT changes after SBRT to non-spine bone metastases Table 1 Classifying late radiological changes in lung after SBRT (20) Name Description Modified Consolidation, volume loss, and bronchiectasis similar to, but usually less extensive than, conventional conventional pattern radiation fibrosis. Larger than the original tumor size. Occasionally with associated ground glass opacity Mass-like fibrosis Well-circumscribed focal consolidation limited to area surrounding the tumor. The abnormality must be larger than the original tumor Scar-like fibrosis Linear opacity in the region of the tumor associated with volume loss No evidence of No new abnormalities. Includes patients with tumors that are stable, regressing or resolved, or fibrosis in increased density the position of the original tumor that is not larger than the original tumor SBRT, stereotactic body radiation therapy. Figure 17 Baseline image (Mar 18, 2015). fractionated treatment, pulmonary fibrosis was observed in 33% and 74% after 6 and 12 months, respectively (18). Various methods have been proposed to classify radiologic changes on CT after SBRT to the lung (17,19). Broadly, radiological changes can be categorized into acute findings (within 6 months of treatment) and late findings (after 6 months) (19). Pulmonary fibrosis after SBRT is often a late finding; one proposed scoring system categorizes late SBRT changes into four groups, as described in Table 1. Although the aforementioned classification system was developed for use after SBRT to early stage lung cancers, this case illustrates that similar radiographic changes can occur after SBRT to bone metastases that are in close proximity to the lung; and consideration must be given to the possibility of lung injury following SBRT to these lesions. In this particular case, the patient did not develop any pulmonary symptoms after their SBRT treatment. Case 8: right iliac metastasis and pathologic fracture Figures 17,18 are axial and coronal CT images through the pelvis of a patient with an osseous metastasis in the lateral right ilium with a large soft tissue component. The patient had a primary NSCLC and started SBRT (30 Gy in 5 fractions) on May 28, 2015 to the right iliac lesion. She previously received two courses of radiation treatment to overlapping areas of the right pelvis in March 2015 (20 Gy in 5 fractions) and June 2014 (8 Gy in 1 fraction). Two weeks after SBRT was completed, the CT scan was repeated and showed increased sclerosis in the irradiated bone, decrease of the soft tissue mass and a new pathologic fracture. Given the short time interval between SBRT and repeat imaging, it is difficult to determine the extent of treatment response. On the radiation planning CT scan from May 19, 2015, there was no evidence of a pre-existing fracture;
8 Annals of Palliative Medicine, Vol 5, No 2 April Figure 18 Follow-up image (Jun 16, 2015). therefore the new pathologic fracture might be related to treatment effect. The development of fractures is a known complication after SBRT to spinal metastases (20). From one series, the median time to vertebral compression fractures after treatment was 3.3 months and the major predictive factors for fracture development were spine alignment, presence of lytic lesions, primary lung/ liver histologies and large SBRT dose per fraction (21). Pathologic fractures have also been infrequently observed after SBRT to non-spine bone metastases (7). However, further studies need to be performed to understand the pathophysiology and risk factors for the development of pathologic fractures after treatment to non-spine bone metastases. All patients receiving SBRT to non-spine bone metastases must routinely be informed about fracture risk as a potential complication of treatment. Conclusions Few studies have examined the clinical outcomes and radiologic changes in patients receiving SBRT for non-spine bone metastases patients. We reviewed the radiological images of eight selected cases after SBRT. Various radiological changes following SBRT are described, including: remineralization of lytic bone metastases, demineralization of sclerotic bone metastases, progression and response in different lesions, as well as lung fibrosis after SBRT to a rib metastases. We recommend future studies to correlate radiologic changes with clinical outcomes including pain relief, toxicity and long-term local control. In addition, it would be useful to perform prospective studies with larger numbers of patients with bone metastases from various primary malignancies to determine short and long term outcomes post-sbrt. Acknowledgements We thank the generous support of Bratty Family Fund, Michael and Karyn Goldstein Cancer Research Fund, Joey and Mary Furfari Cancer Research Fund, Pulenzas Cancer Research Fund, Joseph and Silvana Melara Cancer Research Fund, and Ofelia Cancer Research Fund. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Tubiana-Hulin M. Incidence, prevalence and distribution of bone metastases. Bone 1991;12 Suppl 1:S Li K, Chow E, Chiu H, et al. Effectiveness of palliative radiotherapy in the treatment of bone metastases employing the Brief Pain Inventory. J Pain Symptom Manage 2006;2: Anwar M, Weinberg V, Chang AJ, et al. Hypofractionated SBRT versus conventionally fractionated EBRT for prostate cancer: comparison of PSA slope and nadir. Radiat Oncol 2014;9:42.
9 124 Chiu et al. CT changes after SBRT to non-spine bone metastases 4. Farnia B, Louis CU, Teh BS, et al. Stereotactic body radiation therapy (SBRT) for an isolated bone metastasis in an adolescent male with nasopharyngeal carcinoma. Pediatr Blood Cancer 2014;61: Sahgal A, Roberge D, Schellenberg D, et al. The Canadian Association of Radiation Oncology scope of practice guidelines for lung, liver and spine stereotactic body radiotherapy. Clin Oncol (R Coll Radiol) 2012;24: Balagamwala EH, Angelov L, Koyfman SA, et al. Single-fraction stereotactic body radiotherapy for spinal metastases from renal cell carcinoma: Clinical article. J Neurosurg Spine 2012;17: Owen D, Laack NN, Mayo CS, et al. Outcomes and toxicities of stereotactic body radiation therapy for non-spine bone oligometastases. Pract Radiat Oncol 2014;4:e Chow E, Holden L, Rubenstein J, et al. Computed tomography (CT) evaluation of breast cancer patients with osteolytic bone metastases undergoing palliative radiotherapy a feasibility study. Radiother Oncol 2014;70: Blanco AI, Teh BS, Amato RJ. Role of radiation therapy in the management of renal cell cancer. Cancers (Basel) 2011;3: Wachenfeld I, Sanner G, Bottcher HD, et al. The remineralization of the vertebral metastases of breast carcinoma after radiotherapy. Strahlenther Onkol 1996;172: Weber K, Doucet M, Kominsky S. Renal cell carcinoma bone metastasis elucidating the molecular targets. Cancer Metastasis Rev 2007;26: Jhaveri PM, Teh BS, Paulino AC, et al. A doseresponse relationship for time to bone pain resolution after stereotactic body radiotherapy (SBRT) for renal cell carcinoma (RCC) bony metastases. Acta Oncol 2012;51: Ranck MC, Golden DW, Corbin KS, et al. Stereotactic body radiotherapy for the treatment of oligometastatic renal cell carcinoma. Am J Clin Oncol 2013;36: Stinauer MA, Kavanagh BD, Schefter TE, et al. Stereotactic body radiation therapy for melanoma and renal cell carcinoma: impact of single fraction equivalent dose on local control. Radiat Oncol 2011;6: De Meerleer G, Khoo V, Escudier B, et al. Radiotherapy for renal-cell carcinoma. Lancet Oncol 2014;15:e Timmerman RD, Kavanagh BD, Cho LC, et al. Stereotactic body radiation therapy in multiple organ sites. J Clin Oncol 2007;25: Trovo M, Linda A, El Naqa I, et al. Early and late lung radiographic injury following stereotactic body radiation therapy (SBRT). Lung Cancer 2010;69: Guckenberger M, Heilman K, Wulf J, et al. Pulmonary injury and tumor response after stereotactic body radiotherapy (SBRT): results of a serial follow-up CT study. Radiother Oncol 2007;85: Dahele M, Palma D, Lagerwaard F, et al. Radiological changes after stereotactic radiotherapy for stage I lung cancer. J Thorac Oncol 2011;6: Sahgal A, Whyne CM, Ma L, et al. Vertebral compression fracture after stereotactic body radiotherapy for spinal metastases. Lancet Oncol 2013;14:e Cunha MV, Al-Omair A, Atenafu EG, et al. Vertebral compression fracture (VCF) after spine stereotactic body radiation therapy (SBRT): analysis of predictive factors. Int J Radiat Oncol Biol Phys 2012;84:e Cite this article as: Chiu N, Probyn L, Raman S, McDonald R, Poon I, Erler D, Brotherston D, Soliman H, Cheung P, Chung H, Chu W, Loblaw A, Thavarajah N, Lang C, Chin L, Chow E, Sahgal A. Radiological changes on CT after stereotactic body radiation therapy to non-spine bone metastases: a descriptive series. Ann Palliat Med 2016;5(2): doi: /apm
Computed Tomography Evaluation of Density Following Stereotactic Body Radiation Therapy of Nonspine Bone Metastases
 Stereotactic Radiotherapy Computed Tomography Evaluation of Density Following Stereotactic Body Radiation Therapy of Nonspine Bone Metastases Technology in Cancer Research & Treatment 2016, Vol. 15(5)
Stereotactic Radiotherapy Computed Tomography Evaluation of Density Following Stereotactic Body Radiation Therapy of Nonspine Bone Metastases Technology in Cancer Research & Treatment 2016, Vol. 15(5)
Spinal cord compression as a first presentation of cancer: A case report
 J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
Re-irradiation for painful bone metastases: evidence-based approach
 Editor s note: Palliative Radiotherapy Column features articles emphasizing the critical role of radiotherapy in palliative care. Chairs to the columns are Dr. Edward L.W. Chow from Odette Cancer Centre,
Editor s note: Palliative Radiotherapy Column features articles emphasizing the critical role of radiotherapy in palliative care. Chairs to the columns are Dr. Edward L.W. Chow from Odette Cancer Centre,
4.x Oligometastases: evidence for dose-fractionation
 4.x Oligometastases: evidence for dose-fractionation Background 4.x.1. The oligometastatic state can be defined as 1-3 isolated metastatic sites, typically occurring more than six months after successful
4.x Oligometastases: evidence for dose-fractionation Background 4.x.1. The oligometastatic state can be defined as 1-3 isolated metastatic sites, typically occurring more than six months after successful
8/3/2017. Spine SBRT: A Clinician's Update On Techniques and Outcomes. Disclosures. Outline
 Spine SBRT: A Clinician's Update On Techniques and Outcomes Chia-Lin (Eric) Tseng, MD FRCPC Radiation Oncologist Sunnybrook Health Sciences Centre University of Toronto August 3, 2017 Disclosures I have
Spine SBRT: A Clinician's Update On Techniques and Outcomes Chia-Lin (Eric) Tseng, MD FRCPC Radiation Oncologist Sunnybrook Health Sciences Centre University of Toronto August 3, 2017 Disclosures I have
Pelvic insufficiency fractures in women following radiation treatment: a case series
 Case Report Pelvic insufficiency fractures in women following radiation treatment: a case series Stephanie Chan, Leigha Rowbottom, Rachel McDonald, Elizabeth David, Hans Chung, Albert Yee, Angela Turner,
Case Report Pelvic insufficiency fractures in women following radiation treatment: a case series Stephanie Chan, Leigha Rowbottom, Rachel McDonald, Elizabeth David, Hans Chung, Albert Yee, Angela Turner,
Disclosure SBRT. SBRT for Spinal Metastases 5/2/2010. No conflicts of interest. Overview
 Stereotactic Body Radiotherapy (SBRT) for Recurrent Spine Tumors Arjun Sahgal M.D., F.R.C.P.C. Assistant Professor Princess Margaret Hospital Sunnybrook Health Sciences Center University of Toronto Department
Stereotactic Body Radiotherapy (SBRT) for Recurrent Spine Tumors Arjun Sahgal M.D., F.R.C.P.C. Assistant Professor Princess Margaret Hospital Sunnybrook Health Sciences Center University of Toronto Department
20. Background. Oligometastases. Oligometastases: bone (including spine) and lymph nodes
 125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
Radiological changes following stereotactic radiotherapy for stage I lung cancer. M. Dahele, D. Palma, F. Lagerwaard, B. Slotman, S.
 Chapter 9 Radiological changes following stereotactic radiotherapy for stage I lung cancer M. Dahele, D. Palma, F. Lagerwaard, B. Slotman, S. Senan Department of Radiation Oncology, VU University Medical
Chapter 9 Radiological changes following stereotactic radiotherapy for stage I lung cancer M. Dahele, D. Palma, F. Lagerwaard, B. Slotman, S. Senan Department of Radiation Oncology, VU University Medical
Pulmonary changes induced by radiotherapy. HRCT findings
 Pulmonary changes induced by radiotherapy. HRCT findings Poster No.: C-2299 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. Albert Antequera, K. Müller Campos, D. 1 2 4 3 1
Pulmonary changes induced by radiotherapy. HRCT findings Poster No.: C-2299 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. Albert Antequera, K. Müller Campos, D. 1 2 4 3 1
Radiotherapy for patients with unresected locally advanced breast cancer
 Original Article Radiotherapy for patients with unresected locally advanced breast cancer Caitlin Yee, Yasir Alayed, Leah Drost, Irene Karam, Danny Vesprini, Claire McCann, Hany Soliman, Liying Zhang,
Original Article Radiotherapy for patients with unresected locally advanced breast cancer Caitlin Yee, Yasir Alayed, Leah Drost, Irene Karam, Danny Vesprini, Claire McCann, Hany Soliman, Liying Zhang,
SBRT for lung metastases: Case report
 SBRT for lung metastases: Case report Guillermo de Velasco MD, PhD University Hospital 12 de Octubre @H12O_GUCancer @g_develasco Case report 71 years old man Smoker DM 2005 Right radical nephrectomy Histology:
SBRT for lung metastases: Case report Guillermo de Velasco MD, PhD University Hospital 12 de Octubre @H12O_GUCancer @g_develasco Case report 71 years old man Smoker DM 2005 Right radical nephrectomy Histology:
Thoracic complications post stereotactic body radiotherapy (SBRT) for lung cancer - what the radiologist needs to know
 Thoracic complications post stereotactic body radiotherapy (SBRT) for lung cancer - what the radiologist needs to know Poster No.: C-1700 Congress: ECR 2014 Type: Educational Exhibit Authors: G. E. Khanda,
Thoracic complications post stereotactic body radiotherapy (SBRT) for lung cancer - what the radiologist needs to know Poster No.: C-1700 Congress: ECR 2014 Type: Educational Exhibit Authors: G. E. Khanda,
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2
 Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
Minimally Invasive Radiofrequency Ablation Treatment of Metastatic Spinal Tumors
 Minimally Invasive Radiofrequency Ablation Treatment of Metastatic Spinal Tumors 1 Objectives Demographics of spinal tumors Treatment options and goals Adoption of RF ablation for pain palliation by NCCN
Minimally Invasive Radiofrequency Ablation Treatment of Metastatic Spinal Tumors 1 Objectives Demographics of spinal tumors Treatment options and goals Adoption of RF ablation for pain palliation by NCCN
Imaging follow-up after stereotactic ablative radiotherapy (SABR) for lung tumors
 J Radiat Oncol (2012) 1:11 16 DOI 10.1007/s13566-012-0014-2 REVIEW Imaging follow-up after stereotactic ablative radiotherapy (SABR) for lung tumors Simon S. Lo & Bin S. Teh & Nina A. Mayr & Stephen B.
J Radiat Oncol (2012) 1:11 16 DOI 10.1007/s13566-012-0014-2 REVIEW Imaging follow-up after stereotactic ablative radiotherapy (SABR) for lung tumors Simon S. Lo & Bin S. Teh & Nina A. Mayr & Stephen B.
Symptom clusters using the Brief Pain Inventory in patients with breast cancer
 Original Article Symptom clusters using the Brief Pain Inventory in patients with breast cancer Vithusha Ganesh, Leah Drost, Nicholas Chiu, Liying Zhang, Leonard Chiu, Ronald Chow, Nicholas Lao, Bo Angela
Original Article Symptom clusters using the Brief Pain Inventory in patients with breast cancer Vithusha Ganesh, Leah Drost, Nicholas Chiu, Liying Zhang, Leonard Chiu, Ronald Chow, Nicholas Lao, Bo Angela
8/2/2018. Acknowlegements: TCP SPINE. Disclosures
 A Presentation for the AAPM Annual meeting, Aug 2, 2018 Nashville, TN Stereotactic Radiosurgery for Spinal Metastases: Tumor Control Probability Analyses and Recommended Reporting Standards for Future
A Presentation for the AAPM Annual meeting, Aug 2, 2018 Nashville, TN Stereotactic Radiosurgery for Spinal Metastases: Tumor Control Probability Analyses and Recommended Reporting Standards for Future
CT appearance of radiation injury of the lung after stereotactic body radiation therapy (SBRT) for lung cancers: a pictorial review
 CT appearance of radiation injury of the lung after stereotactic body radiation therapy (SBRT) for lung cancers: a pictorial review Award: Certificate of Merit Poster No.: C-210 Congress: ECR 2009 Type:
CT appearance of radiation injury of the lung after stereotactic body radiation therapy (SBRT) for lung cancers: a pictorial review Award: Certificate of Merit Poster No.: C-210 Congress: ECR 2009 Type:
Imaging of bone metastases
 Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
Should dexamethasone be standard in the prophylaxis of pain flare after palliative radiotherapy for bone metastases? a debate
 Perspective Should dexamethasone be standard in the prophylaxis of pain flare after palliative radiotherapy for bone metastases? a debate Mark Niglas, Srinivas Raman, Danielle Rodin, Jay Detsky, Carlo
Perspective Should dexamethasone be standard in the prophylaxis of pain flare after palliative radiotherapy for bone metastases? a debate Mark Niglas, Srinivas Raman, Danielle Rodin, Jay Detsky, Carlo
Original Article. Keywords: Pain; quality of life; radiation oncology
 Original Article Impact of a dedicated palliative radiation oncology service on the use of single fraction and hypofractionated radiation therapy among patients with bone metastases Sonia Skamene 1 *,
Original Article Impact of a dedicated palliative radiation oncology service on the use of single fraction and hypofractionated radiation therapy among patients with bone metastases Sonia Skamene 1 *,
Radiotherapy symptoms control in bone mets. Francesco Cellini GemelliART. Ernesto Maranzano,MD. Session 5: Symptoms management
 Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.15 Single Institutional Comparative
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.15 Single Institutional Comparative
Managing Bone Pain in Metastatic Disease. Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018
 Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
External beam radiotherapy and bone metastases
 Review Article External beam radiotherapy and bone metastases Candice Johnstone 1, Stephen T. Lutz 2 1 Department of Radiation Oncology, Medical College of Wisconsin, Milwaukee, Wisconsin, USA; 2 Department
Review Article External beam radiotherapy and bone metastases Candice Johnstone 1, Stephen T. Lutz 2 1 Department of Radiation Oncology, Medical College of Wisconsin, Milwaukee, Wisconsin, USA; 2 Department
Superior target delineation for stereotactic body radiotherapy of bone metastases from renal cell carcinoma on MRI compared to CT
 Original Article Superior target delineation for stereotactic body radiotherapy of bone metastases from renal cell carcinoma on MRI compared to CT Fieke M. Prins 1, Joanne M. van der Velden 1, Anne S.
Original Article Superior target delineation for stereotactic body radiotherapy of bone metastases from renal cell carcinoma on MRI compared to CT Fieke M. Prins 1, Joanne M. van der Velden 1, Anne S.
A Guide to Ewing Sarcoma
 A Guide to Ewing Sarcoma Written By Physicians For Physicians WHAT IS EWING SARCOMA (ES) ES is a malignant bone tumor that can evolve from any bone in the body (and occasionally soft tissue) and mostly
A Guide to Ewing Sarcoma Written By Physicians For Physicians WHAT IS EWING SARCOMA (ES) ES is a malignant bone tumor that can evolve from any bone in the body (and occasionally soft tissue) and mostly
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Renal cell cancer (RCC) metastases have been traditionally
 J Neurosurg Spine 21:711 718, 2014 AANS, 2014 Spine stereotactic body radiotherapy for renal cell cancer spinal metastases: analysis of outcomes and risk of vertebral compression fracture Clinical article
J Neurosurg Spine 21:711 718, 2014 AANS, 2014 Spine stereotactic body radiotherapy for renal cell cancer spinal metastases: analysis of outcomes and risk of vertebral compression fracture Clinical article
Disclosure. Paul Medin teaches radiosurgery courses sponsored by BrainLAB Many animals (and humans) were harmed to make this presentation possible!
 Disclosure The tolerance of the nervous system to SBRT: dogma, data and recommendations Paul Medin, PhD Paul Medin teaches radiosurgery courses sponsored by BrainLAB Many animals (and humans) were harmed
Disclosure The tolerance of the nervous system to SBRT: dogma, data and recommendations Paul Medin, PhD Paul Medin teaches radiosurgery courses sponsored by BrainLAB Many animals (and humans) were harmed
Marco Trovò CRO-Aviano
 From pre-clinical research to clinical practice in radiation therapy: new predictive factors and biological markers to predict normal tissue toxicity after radiation therapy of the lung. Marco Trovò CRO-Aviano
From pre-clinical research to clinical practice in radiation therapy: new predictive factors and biological markers to predict normal tissue toxicity after radiation therapy of the lung. Marco Trovò CRO-Aviano
Vertebral Body Compression Fracture Following Spine SBRT
 RADIATION ONCOLOGY & MOLECULAR RADIATION SCIENCES Vertebral Body Compression Fracture Following Spine SBRT Kristin J. Redmond, MD, MPH Disclosure & Disclaimer An honorarium is provided by Accuray for this
RADIATION ONCOLOGY & MOLECULAR RADIATION SCIENCES Vertebral Body Compression Fracture Following Spine SBRT Kristin J. Redmond, MD, MPH Disclosure & Disclaimer An honorarium is provided by Accuray for this
Role of SBRT in the management of lung and liver metastases. Ronan TANGUY, M.D. Radiation Oncologist
 Role of SBRT in the management of lung and liver metastases Ronan TANGUY, M.D. Radiation Oncologist Oligometastatic RCC mrcc: Lung, Bone, Liver, Brain (Schlesinger-Raab, EJC2008) Targeted therapies Objective
Role of SBRT in the management of lung and liver metastases Ronan TANGUY, M.D. Radiation Oncologist Oligometastatic RCC mrcc: Lung, Bone, Liver, Brain (Schlesinger-Raab, EJC2008) Targeted therapies Objective
Clinical Case Conference
 Clinical Case Conference Palliative radiation therapy for bone metastasis Jeff Burkeen, MD, PGY2 7/20/2015 1 Overview Epidemiology Pathophysiology Common presentations and symptoms Imaging Surgery Radiation
Clinical Case Conference Palliative radiation therapy for bone metastasis Jeff Burkeen, MD, PGY2 7/20/2015 1 Overview Epidemiology Pathophysiology Common presentations and symptoms Imaging Surgery Radiation
Stereotactic Ablative Radiotherapy for Prostate Cancer
 Stereotactic Ablative Radiotherapy for Prostate Cancer Laurie Cuttino, MD Associate Professor of Radiation Oncology VCU Massey Cancer Center Director of Radiation Oncology Sarah Cannon Cancer Center at
Stereotactic Ablative Radiotherapy for Prostate Cancer Laurie Cuttino, MD Associate Professor of Radiation Oncology VCU Massey Cancer Center Director of Radiation Oncology Sarah Cannon Cancer Center at
Palliative radiotherapy in lung cancer
 New concepts and insights regarding the role of radiation therapy in metastatic disease Umberto Ricardi University of Turin Department of Oncology Radiation Oncology Palliative radiotherapy in lung cancer
New concepts and insights regarding the role of radiation therapy in metastatic disease Umberto Ricardi University of Turin Department of Oncology Radiation Oncology Palliative radiotherapy in lung cancer
Effects of circadian rhythms and treatment times on the response of radiotherapy for painful bone metastases
 Original Article Effects of circadian rhythms and treatment times on the response of radiotherapy for painful bone metastases Stephanie Chan, Liying Zhang, Leigha Rowbottom, Rachel McDonald, Georg A. Bjarnason,
Original Article Effects of circadian rhythms and treatment times on the response of radiotherapy for painful bone metastases Stephanie Chan, Liying Zhang, Leigha Rowbottom, Rachel McDonald, Georg A. Bjarnason,
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Conference Schedule / Thursday May 3, 2012
 Conference Schedule / Thursday May 3, 2012 7:30-8:30 Breakfast and Registration (2nd Level, Grand Banking Hall) 8:30-8:45 Welcome and Introduction Michael Sherar, President & CEO, Cancer Care Ontario David
Conference Schedule / Thursday May 3, 2012 7:30-8:30 Breakfast and Registration (2nd Level, Grand Banking Hall) 8:30-8:45 Welcome and Introduction Michael Sherar, President & CEO, Cancer Care Ontario David
Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery
 Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation I: Patient ER 74 y/o male with A1A
Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation I: Patient ER 74 y/o male with A1A
Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer
 Original Article PROGRESS in MEDICAL PHYSICS Vol. 26, No. 4, December, 2015 http://dx.doi.org/10.14316/pmp.2015.26.4.229 Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer Ji
Original Article PROGRESS in MEDICAL PHYSICS Vol. 26, No. 4, December, 2015 http://dx.doi.org/10.14316/pmp.2015.26.4.229 Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer Ji
Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases
 Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases CASE STUDY Institution: Odette Cancer Centre Location: Sunnybrook
Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases CASE STUDY Institution: Odette Cancer Centre Location: Sunnybrook
Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience.
 Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience. Elisabetta Ponti MD, Gianluca Ingrosso MD, Alessandra Carosi PhD, Luana
Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience. Elisabetta Ponti MD, Gianluca Ingrosso MD, Alessandra Carosi PhD, Luana
Clinical outcomes of patients treated with accelerated partial breast irradiation with high-dose rate brachytherapy: Scripps Clinic experience
 Original Article Clinical outcomes of patients treated with accelerated partial breast irradiation with high-dose rate brachytherapy: Scripps Clinic experience Rachel Murray 1, Fantine Giap 2, Ray Lin
Original Article Clinical outcomes of patients treated with accelerated partial breast irradiation with high-dose rate brachytherapy: Scripps Clinic experience Rachel Murray 1, Fantine Giap 2, Ray Lin
Symptom clusters using the EORTC QLQ-C15-PAL in palliative radiotherapy
 Original Article Symptom clusters using the EORTC QLQ-C15-PAL in palliative radiotherapy Vithusha Ganesh, Liying Zhang, Bo Angela Wan, Leah Drost, May Tsao, Elizabeth Barnes, Carlo DeAngelis, Hans Chung,
Original Article Symptom clusters using the EORTC QLQ-C15-PAL in palliative radiotherapy Vithusha Ganesh, Liying Zhang, Bo Angela Wan, Leah Drost, May Tsao, Elizabeth Barnes, Carlo DeAngelis, Hans Chung,
Flattening Filter Free beam
 Dose rate effect in external radiotherapy: biology and clinic Marta Scorsetti, M.D. Radiotherapy and Radiosurgery Dep., Istituto Clinico Humanitas, Milan, Italy Brescia October 8th/9th, 2015 Flattening
Dose rate effect in external radiotherapy: biology and clinic Marta Scorsetti, M.D. Radiotherapy and Radiosurgery Dep., Istituto Clinico Humanitas, Milan, Italy Brescia October 8th/9th, 2015 Flattening
Disclosures. Overview 8/3/2016. SRS: Cranial and Spine
 SRS: Cranial and Spine Brian Winey, Ph.D. Department of Radiation Oncology Massachusetts General Hospital Harvard Medical School Disclosures Travel and research funds from Elekta Travel funds from IBA
SRS: Cranial and Spine Brian Winey, Ph.D. Department of Radiation Oncology Massachusetts General Hospital Harvard Medical School Disclosures Travel and research funds from Elekta Travel funds from IBA
a Phase II Randomised Controlled Trial Matthias Guckenberger
 Dose-intensified Image-guided Fractionated Stereotactic Body Radiation Therapy for Painful Spinal Metastases (DOSIS) versus Conventional Radiation Therapy: a Phase II Randomised Controlled Matthias Guckenberger
Dose-intensified Image-guided Fractionated Stereotactic Body Radiation Therapy for Painful Spinal Metastases (DOSIS) versus Conventional Radiation Therapy: a Phase II Randomised Controlled Matthias Guckenberger
Tecniche Radioterapiche U. Ricardi
 Tecniche Radioterapiche U. Ricardi UNIVERSITA DEGLI STUDI DI TORINO Should we always rely on stage? T4N0M0 Stage IIIB T2N3M0 Early stage NSCLC The treatment of choice for early-stage NSCLC is anatomic
Tecniche Radioterapiche U. Ricardi UNIVERSITA DEGLI STUDI DI TORINO Should we always rely on stage? T4N0M0 Stage IIIB T2N3M0 Early stage NSCLC The treatment of choice for early-stage NSCLC is anatomic
Clinical Aspects of SBRT in Abdominal Regions Brian D. Kavanagh, MD, MPH University of Colorado Department of Radiation Oncology
 Clinical Aspects of SBRT in Abdominal Regions Brian D. Kavanagh, MD, MPH University of Colorado Department of Radiation Oncology Abdominal SBRT: Clinical Aspects Rationales for liver and pancreas SBRT
Clinical Aspects of SBRT in Abdominal Regions Brian D. Kavanagh, MD, MPH University of Colorado Department of Radiation Oncology Abdominal SBRT: Clinical Aspects Rationales for liver and pancreas SBRT
Nothing to disclose. Disclosures
 Low Dose-Rate Brachytherapy vs. Standard External Beam Radiotherapy vs. Stereotactic Body Radiotherapy for Low Risk Prostate Cancer: A Cost-Utility Analysis Joelle Helou, Sofia Torres, Hima Bindu Musunuru,
Low Dose-Rate Brachytherapy vs. Standard External Beam Radiotherapy vs. Stereotactic Body Radiotherapy for Low Risk Prostate Cancer: A Cost-Utility Analysis Joelle Helou, Sofia Torres, Hima Bindu Musunuru,
Local radiotherapy for palliation in multiple myeloma patients with symptomatic bone lesions
 Original Article Radiat Oncol J 2016;34(1):59-63 pissn 2234-1900 eissn 2234-3156 Local radiotherapy for palliation in multiple myeloma patients with symptomatic bone lesions Jeong Won Lee, MD, Jeong Eun
Original Article Radiat Oncol J 2016;34(1):59-63 pissn 2234-1900 eissn 2234-3156 Local radiotherapy for palliation in multiple myeloma patients with symptomatic bone lesions Jeong Won Lee, MD, Jeong Eun
Treatment of oligometastases: Lung
 Treatment of oligometastases: Lung Themadag Catharina ZH 30 March 2017 Max Dahele Radiation Oncologist Vumc, Amsterdam m.dahele@vumc.nl Do you all treat lung oligometastases? What is your definition of
Treatment of oligometastases: Lung Themadag Catharina ZH 30 March 2017 Max Dahele Radiation Oncologist Vumc, Amsterdam m.dahele@vumc.nl Do you all treat lung oligometastases? What is your definition of
Prospective Assessment of Patient-Rated Symptoms Following Whole Brain Radiotherapy for Brain Metastases
 18 Journal of Pain and Symptom Management Vol. 30 No. 1 July 2005 Original Article Prospective Assessment of Patient-Rated Symptoms Following Whole Brain Radiotherapy for Brain Metastases Edward Chow,
18 Journal of Pain and Symptom Management Vol. 30 No. 1 July 2005 Original Article Prospective Assessment of Patient-Rated Symptoms Following Whole Brain Radiotherapy for Brain Metastases Edward Chow,
The Role of Radiotherapy in Metastatic Breast Cancer. Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health
 The Role of Radiotherapy in Metastatic Breast Cancer Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health Indications for Palliative Pain Control Radiation Bone
The Role of Radiotherapy in Metastatic Breast Cancer Shilpen Patel MD, FACRO Associate Professor Departments of Radiation Oncology and Global Health Indications for Palliative Pain Control Radiation Bone
Stereotactic radiotherapy
 Stereotactic radiotherapy Influence of patient positioning and fixation on treatment planning - clinical results Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH
Stereotactic radiotherapy Influence of patient positioning and fixation on treatment planning - clinical results Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH
The accuracy of clinicians predictions of survival in advanced cancer: a review
 Review Article The accuracy of clinicians predictions of survival in advanced cancer: a review Stephanie Cheon, Arnav Agarwal, Marko Popovic, Milica Milakovic, Michael Lam, Wayne Fu, Julia DiGiovanni,
Review Article The accuracy of clinicians predictions of survival in advanced cancer: a review Stephanie Cheon, Arnav Agarwal, Marko Popovic, Milica Milakovic, Michael Lam, Wayne Fu, Julia DiGiovanni,
CLINICAL APPLICATION OF LINEAR-QUADRATIC MODEL IN REIRRADIATION OF SYMPTOMATIC BONE METASTASES
 MEDICAL PHYSICS CLINICAL APPLICATION OF LINEAR-QUADRATIC MODEL IN REIRRADIATION OF SYMPTOMATIC BONE METASTASES L. REBEGEA 1,2, M. DUMITRU 1, D. FIRESCU 2,3 1 Sf. Ap. Andrei Emergency Clinical Hospital,
MEDICAL PHYSICS CLINICAL APPLICATION OF LINEAR-QUADRATIC MODEL IN REIRRADIATION OF SYMPTOMATIC BONE METASTASES L. REBEGEA 1,2, M. DUMITRU 1, D. FIRESCU 2,3 1 Sf. Ap. Andrei Emergency Clinical Hospital,
SBRT in early stage NSCLC
 SBRT in early stage NSCLC Optimal technique and tumor dose Frank Zimmermann Clinic of Radiotherapy and Radiation Oncology University Hospital Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch Techniques
SBRT in early stage NSCLC Optimal technique and tumor dose Frank Zimmermann Clinic of Radiotherapy and Radiation Oncology University Hospital Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch Techniques
Local Therapy for Ewing Sarcoma: Current Concepts and Opportunities for Improvement
 Local Therapy for Ewing Sarcoma: Current Concepts and Opportunities for Improvement Safia K. Ahmed, MD Department of Radiation Oncology Washington University August 25, 2017 2017 MFMER slide-1 Outline
Local Therapy for Ewing Sarcoma: Current Concepts and Opportunities for Improvement Safia K. Ahmed, MD Department of Radiation Oncology Washington University August 25, 2017 2017 MFMER slide-1 Outline
Efficacy of single fraction conventional radiation therapy for painful uncomplicated bone metastases: a systematic review and meta-analysis
 Original Article Efficacy of single fraction conventional radiation therapy for painful uncomplicated bone metastases: a systematic review and meta-analysis Ronald Chow 1, Peter Hoskin 2, Drew Hollenberg
Original Article Efficacy of single fraction conventional radiation therapy for painful uncomplicated bone metastases: a systematic review and meta-analysis Ronald Chow 1, Peter Hoskin 2, Drew Hollenberg
The Evolution of SBRT and Hypofractionation in Thoracic Radiation Oncology
 The Evolution of SBRT and Hypofractionation in Thoracic Radiation Oncology (specifically, lung cancer) 2/10/18 Jeffrey Kittel, MD Radiation Oncology, Aurora St. Luke s Medical Center Outline The history
The Evolution of SBRT and Hypofractionation in Thoracic Radiation Oncology (specifically, lung cancer) 2/10/18 Jeffrey Kittel, MD Radiation Oncology, Aurora St. Luke s Medical Center Outline The history
Thoracic Recurrences. Soft tissue recurrence
 Stereotactic body radiotherapy for thoracic and soft malignancies Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of
Stereotactic body radiotherapy for thoracic and soft malignancies Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of
Osseous Metastases Missed by Bone Scan in Hepatocellular Carcinoma: A Retrospective Analysis
 Osseous Metastases Missed by Bone Scan in Hepatocellular Carcinoma: A Retrospective Analysis Lauren Ferrante, MD ICCR rotation: IRB protocol November 26, 2008 A. Study Background, Rationale, and Objectives
Osseous Metastases Missed by Bone Scan in Hepatocellular Carcinoma: A Retrospective Analysis Lauren Ferrante, MD ICCR rotation: IRB protocol November 26, 2008 A. Study Background, Rationale, and Objectives
Vertebral compression fractures after stereotactic body radiation therapy: a large, multi-institutional, multinational evaluation
 clinical article J Neurosurg Spine 24:928 936, 2016 Vertebral compression fractures after stereotactic body radiation therapy: a large, multi-institutional, multinational evaluation Maha Saada Jawad, MD,
clinical article J Neurosurg Spine 24:928 936, 2016 Vertebral compression fractures after stereotactic body radiation therapy: a large, multi-institutional, multinational evaluation Maha Saada Jawad, MD,
Reirradiation spine stereotactic body radiation therapy for spinal metastases: systematic review
 LITERATURE REVIEW Reirradiation spine stereotactic body radiation therapy for spinal metastases: systematic review International Stereotactic Radiosurgery Society practice guidelines Sten Myrehaug, MD,
LITERATURE REVIEW Reirradiation spine stereotactic body radiation therapy for spinal metastases: systematic review International Stereotactic Radiosurgery Society practice guidelines Sten Myrehaug, MD,
Intraoperative Radiation Therapy for
 Frontiers ofradiation Therapy and Oncology Reprint Editors: J.M. Vaeth, J.L. Meyer, San Francisco, Calif. ~' Publishers: S.Karger, Basel Printed in Switzerland Vaeth JM, Meyer JL (eds): The Role of High
Frontiers ofradiation Therapy and Oncology Reprint Editors: J.M. Vaeth, J.L. Meyer, San Francisco, Calif. ~' Publishers: S.Karger, Basel Printed in Switzerland Vaeth JM, Meyer JL (eds): The Role of High
Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C.
 Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Role of Whole-body Diffusion MR in Detection of Metastatic lesions Prof. Dr. NAGUI M. ABDELWAHAB,M.D.; MARYSE Y. AWADALLAH, M.D. AYA M. BASSAM, Ms.C. Cancer is a potentially life-threatening disease,
Stereotactic radiosurgery/stereotactic body radiation therapy reflection on the last decade s achievements and future directions
 Editor s note: Palliative Radiotherapy Column features articles emphasizing the critical role of radiotherapy in palliative care. Chairs to the columns are Dr. Edward L. W. Chow from Odette Cancer Centre,
Editor s note: Palliative Radiotherapy Column features articles emphasizing the critical role of radiotherapy in palliative care. Chairs to the columns are Dr. Edward L. W. Chow from Odette Cancer Centre,
Clinical outcomes of patients with malignant lung lesions treated with stereotactic body radiation therapy (SBRT) in five fractions
 J Radiat Oncol (2012) 1:57 63 DOI 10.1007/s13566-012-0008-0 ORIGINAL RESEARCH Clinical outcomes of patients with malignant lung lesions treated with stereotactic body radiation therapy (SBRT) in five fractions
J Radiat Oncol (2012) 1:57 63 DOI 10.1007/s13566-012-0008-0 ORIGINAL RESEARCH Clinical outcomes of patients with malignant lung lesions treated with stereotactic body radiation therapy (SBRT) in five fractions
Original Article on Palliative Radiotherapy
 Original Article on Palliative Radiotherapy Quality of life in responders after palliative radiation therapy for painful bone metastases using EORTC QLQ-C30 and EORTC QLQ- BM22: results of a Brazilian
Original Article on Palliative Radiotherapy Quality of life in responders after palliative radiation therapy for painful bone metastases using EORTC QLQ-C30 and EORTC QLQ- BM22: results of a Brazilian
Spinal metastases will develop in 40% of patients
 clinical article J Neurosurg Spine 25:646 653, 2016 Re-irradiation stereotactic body radiotherapy for spinal metastases: a multi-institutional outcome analysis Ahmed Hashmi, MD, 1 Matthias Guckenberger,
clinical article J Neurosurg Spine 25:646 653, 2016 Re-irradiation stereotactic body radiotherapy for spinal metastases: a multi-institutional outcome analysis Ahmed Hashmi, MD, 1 Matthias Guckenberger,
Painful vertebral metastases are a frequent manifestation of malignancies
 2892 COMMUNICATION Palliative Radiation Therapy for Painful Vertebral Metastases A Practice Survey Tejpal Gupta, M.D., D.N.B. Rajiv Sarin, M.D. Department of Radiation Oncology, Tata Memorial Hospital,
2892 COMMUNICATION Palliative Radiation Therapy for Painful Vertebral Metastases A Practice Survey Tejpal Gupta, M.D., D.N.B. Rajiv Sarin, M.D. Department of Radiation Oncology, Tata Memorial Hospital,
Persistence of Myeloma Protein for More than One Year after Radiotherapy Is an Adverse Prognostic Factor in Solitary Plasmacytoma of Bone
 1532 Persistence of Myeloma Protein for More than One Year after Radiotherapy Is an Adverse Prognostic Factor in Solitary Plasmacytoma of Bone Richard B. Wilder, M.D. 1 Chul S. Ha, M.D. 1 James D. Cox,
1532 Persistence of Myeloma Protein for More than One Year after Radiotherapy Is an Adverse Prognostic Factor in Solitary Plasmacytoma of Bone Richard B. Wilder, M.D. 1 Chul S. Ha, M.D. 1 James D. Cox,
Palliative RT. Jiraporn Setakornnukul, M.D. Radiation Oncology Division Siriraj Hospital, Mahidol University
 Palliative RT Jiraporn Setakornnukul, M.D. Radiation Oncology Division Siriraj Hospital, Mahidol University Scope Brain metastasis Metastasis epidural spinal cord compression SVC obstruction Bone pain
Palliative RT Jiraporn Setakornnukul, M.D. Radiation Oncology Division Siriraj Hospital, Mahidol University Scope Brain metastasis Metastasis epidural spinal cord compression SVC obstruction Bone pain
Elizabeth David 1, Sagi Kaduri 1, Albert Yee 2, Edward Chow 3, Arjun Sahgal 3, Stephanie Chan 3, Ramez Hanna 1. Original Article
 Original Article Initial single center experience: radiofrequency ablation assisted vertebroplasty and osteoplasty using a bipolar device in the palliation of bone metastases Elizabeth David 1, Sagi Kaduri
Original Article Initial single center experience: radiofrequency ablation assisted vertebroplasty and osteoplasty using a bipolar device in the palliation of bone metastases Elizabeth David 1, Sagi Kaduri
Imaging of cardio-pulmonary treatment related damage. Radiotheraphy and Lung
 Imaging of cardio-pulmonary treatment related damage Dr. Andrea Borghesi Dr. Emanuele Gavazzi Department of Radiology 2 University of Brescia Radiotheraphy and Lung The goal of radiation therapy (RT) is
Imaging of cardio-pulmonary treatment related damage Dr. Andrea Borghesi Dr. Emanuele Gavazzi Department of Radiology 2 University of Brescia Radiotheraphy and Lung The goal of radiation therapy (RT) is
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
MRI XR, CT, NM. Principal Modality (2): Case Report # 2. Date accepted: 15 March 2013
 Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting
 Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Isotopes and Palliative Radiotherapy for bone metastases
 Isotopes and Palliative Radiotherapy for bone metastases Rationale for Bone-seeking Isotope Therapies in Prostate Cancer > 90% of patients with advanced prostate cancer have bone metastases which can be
Isotopes and Palliative Radiotherapy for bone metastases Rationale for Bone-seeking Isotope Therapies in Prostate Cancer > 90% of patients with advanced prostate cancer have bone metastases which can be
Predictors of Radiotherapy Induced Bone Injury (RIBI) after stereotactic lung radiotherapy
 Taremi et al. Radiation Oncology 2012, 7:159 RESEARCH Open Access Predictors of Radiotherapy Induced Bone Injury (RIBI) after stereotactic lung radiotherapy Mojgan Taremi 1,2,5*, Andrew Hope 1,2, Patricia
Taremi et al. Radiation Oncology 2012, 7:159 RESEARCH Open Access Predictors of Radiotherapy Induced Bone Injury (RIBI) after stereotactic lung radiotherapy Mojgan Taremi 1,2,5*, Andrew Hope 1,2, Patricia
Bone metastases of solid tumors Diagnosis and management by
 Bone metastases of solid tumors Diagnosis and management by Dr/RASHA M Abd el Motagaly oncology consultant Nasser institute adult oncology unit 3/27/2010 1 Goals 1- Know the multitude of problem of bone
Bone metastases of solid tumors Diagnosis and management by Dr/RASHA M Abd el Motagaly oncology consultant Nasser institute adult oncology unit 3/27/2010 1 Goals 1- Know the multitude of problem of bone
Digital tomosynthesis (DT) has been well described as a
 Case Report The Usefulness of Digital Tomosynthesis (DT) in Assisting in Cases of Doubtful Routine Radiography and/or Computed Tomography (CT) Image. Abstract Digital tomosynthesis is useful in assisting
Case Report The Usefulness of Digital Tomosynthesis (DT) in Assisting in Cases of Doubtful Routine Radiography and/or Computed Tomography (CT) Image. Abstract Digital tomosynthesis is useful in assisting
Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer
 Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes
Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes
Outline. WBRT field. Brain Metastases. Whole Brain RT Prophylactic WBRT Stereotactic radiosurgery (SRS) 1 fraction Stereotactic frame
 Radiation Therapy for Advanced NSC Lung Ca Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of California San Francisco
Radiation Therapy for Advanced NSC Lung Ca Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of California San Francisco
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Orthopedics and Rheumatology Type of Article: Case Report Title:
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Orthopedics and Rheumatology Type of Article: Case Report Title:
Winston Tan MD FACP Associate Professor of Medicine Mayo Clinic Florida
 Winston Tan MD FACP Associate Professor of Medicine Mayo Clinic Florida } none } To develop an understanding of the management of bone metastasis through a multidisciplinary approach } Enable the learner
Winston Tan MD FACP Associate Professor of Medicine Mayo Clinic Florida } none } To develop an understanding of the management of bone metastasis through a multidisciplinary approach } Enable the learner
ACR Appropriateness Criteria Metastatic Epidural Spinal Cord Compression and Recurrent Spinal Metastasis EVIDENCE TABLE
 . Cole JS, Patchell RA. Metastatic epidural spinal cord compression. Lancet Neurol. 2008;7(5):59-66. 2. Loblaw DA, Mitera G, Ford M, Laperriere NJ. A 20 updated systematic review and clinical practice
. Cole JS, Patchell RA. Metastatic epidural spinal cord compression. Lancet Neurol. 2008;7(5):59-66. 2. Loblaw DA, Mitera G, Ford M, Laperriere NJ. A 20 updated systematic review and clinical practice
Treatment Planning & IGRT Credentialing for NRG SBRT Trials
 Treatment Planning & IGRT Credentialing for NRG SBRT Trials Hania Al Hallaq, Ph.D. Department of Radiation & Cellular Oncology The University of Chicago Learning Objectives Explain rationale behind credentialing
Treatment Planning & IGRT Credentialing for NRG SBRT Trials Hania Al Hallaq, Ph.D. Department of Radiation & Cellular Oncology The University of Chicago Learning Objectives Explain rationale behind credentialing
Radiotherapy physics & Equipments
 Radiotherapy physics & Equipments RAD 481 Lecture s Title: An Overview of Radiation Therapy for Health Care Professionals Dr. Mohammed Emam Vision :IMC aspires to be a leader in applied medical sciences,
Radiotherapy physics & Equipments RAD 481 Lecture s Title: An Overview of Radiation Therapy for Health Care Professionals Dr. Mohammed Emam Vision :IMC aspires to be a leader in applied medical sciences,
Lung Cancer Radiotherapy
 Lung Cancer Radiotherapy Indications, Outcomes, and Impact on Survivorship Care Malcolm Mattes, MD Assistant Professor WVU Department of Radiation Oncology When people think about radiation, they think
Lung Cancer Radiotherapy Indications, Outcomes, and Impact on Survivorship Care Malcolm Mattes, MD Assistant Professor WVU Department of Radiation Oncology When people think about radiation, they think
Original Date: April 2016 Page 1 of 7 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care
 Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care Institution: San Raffaele Hospital Milan, Italy By Nadia Di Muzio, M.D., Radiotherapy Department (collaborators: Berardi
Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care Institution: San Raffaele Hospital Milan, Italy By Nadia Di Muzio, M.D., Radiotherapy Department (collaborators: Berardi
The Paul Evans Memorial Lecture Functional radiotherapy targeting using focused dose escalation. Roberto Alonzi Mount Vernon Cancer Centre
 The Paul Evans Memorial Lecture Functional radiotherapy targeting using focused dose escalation Roberto Alonzi Mount Vernon Cancer Centre Overview Introduction and rationale for focused dose escalation
The Paul Evans Memorial Lecture Functional radiotherapy targeting using focused dose escalation Roberto Alonzi Mount Vernon Cancer Centre Overview Introduction and rationale for focused dose escalation
J Neurosurg Spine 18:
 See the corresponding editorial in this issue, pp 48 49. J Neurosurg Spine 8:4 45, AANS, Radiation-induced vertebral compression fracture following spine stereotactic radiosurgery: clinicopathological
See the corresponding editorial in this issue, pp 48 49. J Neurosurg Spine 8:4 45, AANS, Radiation-induced vertebral compression fracture following spine stereotactic radiosurgery: clinicopathological
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
National Cancer Institute of Canada Clinical Trials Group (NCIC CTG) Trial design:
 Open clinical uro-oncology trials in Canada Eric Winquist, MD, Mary J. Mackenzie, MD, George Rodrigues, MD London Health Sciences Centre, London, Ontario, Canada BLADDER CANCER A PHASE III STUDY OF IRESSA
Open clinical uro-oncology trials in Canada Eric Winquist, MD, Mary J. Mackenzie, MD, George Rodrigues, MD London Health Sciences Centre, London, Ontario, Canada BLADDER CANCER A PHASE III STUDY OF IRESSA
