Evaluation of infectious complications of the implantable venous access system in a general oncologic population
|
|
|
- Abraham Nash
- 6 years ago
- Views:
Transcription
1 Evaluation of infectious complications of the implantable venous access system in a general oncologic population Lilu Chang, RN, MSN Jir-Shiong Tsai, MD, FACP Shin-Ju Huang, RN Chiang-Ching Shih, MD Taipei, Taiwan, Republic of China Objectives: This study was conducted to evaluate the infectious morbidity associated with 2 common types of implantable port systems used in a cancer center in Taiwan. Methods: This study is retrospective and descriptive. Five hundred seventy-two patients who received implantable ports at the cancer center between January 1994 and December 1998 were included. The following 4 types of catheter-related infections were defined in this study: bloodstream, pocket, exit-site, and tunnel. Semiquantitative methods (rolling plate) were used for cultures of removed catheters. Results: The average duration for ports after placement in patients was 358 days (range, days), and the median duration was 242 days. The port-related infection rate was 5.6% in 586 ports and 0.15 per 1000 device-days. Our data indicate that when a port is in use, more frequent dressing changes of the needle exit site (every 3 days vs every 7 days) appear to have no significant impact on the catheter-related infection rate (5.2% vs 7.3%, P =.3). Our observation also indicates that if the catheter is used for total parenteral nutrition (TPN), the patient has a significantly increased chance of developing an infection from the Candida species (71% vs 8%, P =.005). Furthermore, the catheters associated with infections caused by the Candida species had a shorter catheter life (median, 44 days). Conclusions: Infection is the most common complication of venous port system use among cancer patients. According to our data, it is safe and cost-effective to change exit-site needles and transparent dressings every 7 days. It is clearly demonstrated by our study that patients with ports used for the administration of TPN had a significantly greater chance of developing infection from the Candida species. Further investigation is needed to compare the relative advantages of using ports versus other devices for the administration of TPN in cancer patients. (Am J Infect Control 2003;31:34-9.) The need for intravenous access devices for the administration of cancer therapy has increased proportionately with the increasing number of patients diagnosed with cancer. To have a reliable venous access for the delivery of therapeutic agents was particularly problematic until long-term venous devices From the Infection Control Committee, Koo-Foundation Sun,Yat-Sen Cancer Center. Reprint requests: Lilu Chang, RN, MSN, 125 Lih-Der Road, Pei-Tou District,Taipei,Taiwan, Republic of China. Copyright 2003 by the Association for Professionals in Infection Control and Epidemiology, Inc /2003/$ doi: /mic became available. 1,2 Most chemotherapy agents irritate the veins and may cause phlebitis and eventual obliteration of peripheral veins. If extravasation of vesicant agents occurs, the surrounding tissue may have a serious reaction, which may eventually lead to tissue damage and infection. The development of the implantable port has provided for a more reliable and convenient access for administering various therapeutic agents in cancer patients. 2-9 A further advantage of the implantable port is that it requires minimum care and maintenance when it is not in use. However, complications from the use of implantable ports do occur, with one of the most common being infection Numerous studies have focused on evaluating the short-term complications of the devices. However, the long-term complications, particularly 34
2 Chang et al February the infectious morbidity, have not been carefully evaluated. To prevent infections is essential in caring for cancer patients because most of them are immunocompromised during the disease course. Infections that develop during the course of treatment not only may result in longer hospital stays but also may increase health care costs. This study evaluates the infectious morbidity associated with 2 common types of implantable port systems used in our institution an established oncology center in Taiwan. PATIENTS AND METHODS This study is retrospective and descriptive. Five hundred seventy-two patients who received implantable ports for the management of cancer at the Sun Yat-Sen Cancer Center between January 1994 and December 1998 were included. Patients who were not treated or followed-up by our center were excluded. The χ 2 test was used to compare the difference between groups. The following 2 types of ports were used: (1) the Port-a-Cath (Pharmacia Implantable Access Systems, St. Paul, Minn), which is a stainless titanium portal with an internal volume of 0.5 ml that connects to a radiopaque silicone rubber catheter, and (2) the MRI port (Bard Access Systems, Salt Lake City, Utah), which is a plastic rubber portal with an internal volume of 0.5 ml and a silicone septum that is connected to a silicone Groshong catheter (a closed-system catheter with a 3-way valve that allows infusion and blood aspiration while reducing blood reflux and clotting). When ports were used, nurses adhered to our standard protocol for exit-site care, the transparent dressing of needle-insertion site, and administration set change. If ports were used at home, the home care nurse adhered to the same protocol for care and maintenance of the ports. Data, therefore, were stratified into the 2 following groups according to different protocols developed during the study period for comparing infection rate: the first group included patients whose ports were removed between January 1994 and July 1995 and whose access needles and intravenous administration sets were changed every 3 days, and the second group included patients whose ports were removed between August 1995 and December 1998 and whose access needles and intravenous administration sets were changed every 7 days. The site of needle insertion was dressed with transparent dressing (Tegaderm; 3M Health Care, St. Paul, Minn) in both groups. The dressing was changed when the needles and intravenous administration sets were replaced or whenever dressings were wet or soiled. The unused ports were flushed with 5 ml of normal saline containing 250 units of heparin (50 units/1 ml normal saline) every 4 weeks. The following 4 types of catheter-related infections were defined in our study according to Centers for Disease Control and Prevention guidelines 15 : 1. Bloodstream infection (BSI): isolation of the same organism from a blood culture drawn from the portal and from the peripheral vein of a patient with accompanying clinical symptoms of BSI and no other apparent source of infection. 2. Pocket infection: induration, erythema, and tenderness of the skin over the site of port placement or purulent exudate in the subcutaneous pocket containing the port. 3. Exit-site infection: erythema, tenderness, induration within 2 cm of port surface needle access site, or purulence at the port surface needle access site. 4. Tunnel infection: erythema, tenderness, and induration in the tissues overlying the catheter and more than 2 cm from the exit site. All catheter-related infections in our study were categorized according to these definitions. However, few infections were not proved by cultures but were a physician s clinical diagnosis. We categorized infections as BSI if patients had clinical signs of BSI and had no other sources of infections and the infectious signs subsided after removing the catheter. In our center, the indication to remove an infectious port is determined by the type, severity, and organisms of infections. Infected ports were removed immediately in the following circumstances: (1) when infections were recognized as pocket infections, tunnel infections, or exit-site infections with a large quantity of pus; (2) when infections were associated with septic emboli or infectious endocarditis; and (3) when infections were identified from blood cultures of port reservoirs as being from the Staphylococcus, Candida, Pseudomonas, Bacillus, and the Corynebacterium jeikeium. In our study, few of the catheters were removed on the basis of only the decision of the primary physicians. All catheters removed were sent to the laboratory for cultures, and semiquantitative methods (rolling plate) were used for those cultures. RESULTS Between January 1994 and December 1998, a total of 586 ports were placed in 572 patients. Among
3 36 Vol. 31 No. 1 Chang et al Table 1. Microbiologic isolation Total BSI Organisms No. (%) No. (%) Fig 1. Disease distribution. these patients, 12 received 2 ports, and 1 of them received 3 insertions. As shown in Fig 1, the disease most frequently encountered among patients in this study was breast cancer (195/572), followed by colorectal cancer (148/572) and other gastrointestinal tract cancer (64/572). Two hundred thirty-nine Port-a-Cath ports (Pharmacia) and 347 MRI ports (Bard) were used in patients during the study period. All of these ports were single lumen and placed in the operating room. The placement of a port was indicated in either of 2 following circumstances: when patients had poor venous access or when they needed long-term continuous intravenous infusion therapy. The average duration for a port to remain in place was 358 days (range, days), and the median duration was 242 days. The total accrued sum of device-days for the 586 ports studied was 209,694 days. In total, 205 ports (35%) remained in place until the patients died, 277 ports (47.3%) were still in use at the time the data were reviewed, and 50 ports (8.5%) were removed electively because treatment was completed during the study period. In addition, 54 ports (9.2%) were removed because of complications. Of these, 29 catheters (53.7%) were removed because of infectious complications, and 25 (46.3%) were removed because of noninfectious complications. The median interval for removing catheters because of complications was 122 days (range, days). Catheter occlusions that necessitated removal occurred in 18 of the 586 ports inserted (3%) and was the major cause of catheter removal among the noninfectious complications. However, infectious complications were the major reason for premature removal of catheters and were also the major complications associated with catheters in our study. NFGNB* 9 (.30) 6 (.20) Pseudomonas aeruginosa 4 (.13) 3 (.10) Acinetobacter baumannii 2 (.07) 1 (.03) Stenotrophomonas maltophilia 2 (.07) 1 (.03) Burkholderia cepacia 1 (.03) 1 (.03) Yeast 7 (.23) 6 (.20) Candida albicans 6 (.20) 5 (.17) Other Candida species 1 (.03) 1 (.03) Skin flora 11 (.37) 5 (.17) CoNS 6 (.2) 4 (.13) Corynebacteria 1 (.03) 0 (0) Staphylococcus aureus 3 (.10) 0 (0) Bacillus species 1 (.03) 1 (.03) Entero bactericeae 3 (.10) 2 (.07) Klebsiella pneumoniae 1 (.03) 1 (.03) Escherichia coli 1 (.03) 1 (.03) Serratia marcescens 1 (.03) 0 (0) NFGNB, Nonglucose fermentative gram-negative bacilli; CoNS, Coagulase-negative Staphylococcus. Twenty-nine of 33 catheter-related infections (94%) resulted in the removal of the catheters. Of these 33 infections, the majority were BSI (n = 21, 66%). The incidence of exit-site infections (n = 6, 19%) and pocket infections (n = 5, 15%) was lower. The estimated number of total infections per 1000 device-days was Overall, approximately 50% of infections occurred within 100 days after implantation of the catheter. The median interval from the time of port insertion to the time when device-related infection was detected was 80 days (range, days). Microbiologic data of port-related infections are summarized in Table 1. The most common micro-organism isolated from port cultures was that of the Candida species (n = 7), followed by the coagulase-negative Staphylococcus species (n = 6) and Pseudomonas aeruginosa (n = 4). Among 21 catheter-related BSI episodes, the most common micro-organism isolated from the patients also was of the Candida species (n = 6), followed by the coagulase-negative Staphylococcus species (n = 4) and P aeruginosa (n = 3). In a total of 7 infections resulting from the Candida species, 71% (n = 5) were associated with total parenteral nutrition (TPN) (Table 2). Although a higher infection rate (7.7% vs 4.5%) was noted in male groups, it was not statistically significant (P =.1). Patients with nonsolid tumors had higher infection rates compared with patients with solid tumors (10.3% vs 5.4%); however, the differ-
4 Chang et al February Table 2. Comparisons of yeast infection with and without TPN ence was not statistically significant (P =.2) and may be due to the small number of nonsolid tumors in our patient population. There was a similar infection rate between Pharmacia and Bard ports (5.4% vs 5.8%, P = 1.0). Younger patients in our study (< 40 years) appeared more likely to develop catheterrelated infection (9.9% vs 4.2%, P =.009) (Table 3). Incidences of infection were higher in the group for whom access needles and administration sets were changed every 3 days compared with the group for whom they were changed every 7 days (7.3% vs 5.2%, P =.3) (Table 4). All patients with catheter-related infections in our study responded to catheter removal and (or) antibiotic therapy. Most of the catheters (94%) were removed promptly once catheter-related infections were suspected. DISCUSSION Total With TPN Without TPN n n (%) n (%) Candida infection 7 5 (71%) 2 (29%) Bacterial infection 26 2 (8%) 24 (92%) P =.005; χ 2. Table 3. Comparisons of patients with and without infection With Without Total infection infection P Variables n n (%) n (%) value Sex Man (7.7%) 191 (92.3%).1 Woman (4.5%) 362 (95.5%) Tumor Solid (5.4%) 527 (94.6%).2 Nonsolid 29 3 (10.3%) 26 (89.7%) Port type Pharmacia (5.4%) 226 (94.6%) 1.0 Bard (5.8%) 327 (94.2%) Age (9.9%) 137 (90.1%).009 > (4.2%) 416 (95.8%) χ 2. Table 4. Infection comparison between different frequencies of port access needle change (every 3 days vs every week) Total With TPN Without TPN n n (%) n (%) Every 3 days (7.3%) 114 (92.7%) Every week (5.2%) 439 (94.8%) P =.3; χ 2 test. Infections are the most common and feared complications of long-term indwelling catheters. It was previously reported that implanted subcutaneous venous ports have a lower risk of infections and can be maintained in-site longer than other venous devices. 5-9 The infection rate of indwelling venous catheters has been reported to range between 2.4% to 16%. 1,2,4,5,8,9,11,12 It also was reported that the average infection rate in cancer patients with longterm central venous catheters is 1 to 2 per 1000 device-days. 13 The overall infection rate observed in our hospital was similar to that reported by other investigators (5.6% vs 2.4%-16%). However, among cancer patients, the infection rate is lower in our institution (0.12 vs 1-2 per 1000 device-days). The 4 major risk factors associated with catheter-related infections were identified as host factors, catheter type, duration of use, and catheter maintenance and management. 13 Although we are located in a hot and humid tropical and semitropical area, the catheter-related infection rate is similar to or even better than that of patients who live in drier geographic locations. We believe that our standards of care and maintenance are chiefly responsible for the low infection rate. In our study, the younger patients (< 40 years) were more prone to having catheter-related infections and shorter duration of the device in place. Our results are similar to Memorial Sloan-Kettering Cancer Center s report in Since this study was limited to retrospective investigation, the cause of higher infection rate in these younger patients is unclear. The gender of the patients and pathologic findings of the tumor did not relate to the incidence of infection. However, it has been reported that male patients and patients with nonsolid tumors are more likely to have port-related infections. 10 Our study has shown that the infection rate among patients with closed-end Groshong catheters (MRI port; Bard Access System) and those with open-ended catheters (Port-a-Cath; Pharmacia Implantable Access System) is similar. Thus far, there is no safety standard or consensus in practice indicating how long the access needles can be left in-site. Hempsey et al 14 compared the rate of infection between 2 groups of patients whose access
5 38 Vol. 31 No. 1 Chang et al needles were changed with different frequency (1 vs 2 weeks). Although the result of their study was inconclusive, the authors reported that leaving needles in situ for 2 weeks was just as safe as leaving them there for only 1 week. There is also no CDC recommendation for the frequency of dressings change on central catheter sites. 15 Our study suggested that when ports are in use, less frequent changes of access needles and dressings (every 7 days vs every 3 days) result in lower incidence of infection (5.2% vs 7.3%, P =.3). It is reasonable to suggest that in cancer patients with implantable ports, it is probably acceptable and safe to change access needles and dressings every 7 days. In our study, most port infections occurred after 1 month of implantation. Furthermore, 67% of the infectious organisms isolated were identified as skin flora and nonglucose fermentative gram-negative bacilli. These figures imply that rigorous care of the site of port insertion is the most important factor in preventing catheter-related infections. Establishing a centralized standard of care and maintenance has been shown to reduce catheter-related infection rates significantly. 16 Although all the care at our institution was not centralized, it was standardized. Maintenance of sterility and patency of the ports in our cancer patients was performed by well-trained nurses in accordance with standard protocols. We believe that diligent nursing care contributed to the low catheter-related infection rate among our cancer patients. Staphylococcus, the predominant species found on human skin, are the most common organisms to cause catheter-related infections. 13,16 Infection caused by the Candida species is more commonly isolated from the immunocompromised host. 17 The Staphylococcus and Candida species bind well to host protein and adhere better to silicone catheters. 13 In our study, these pathogens also were commonly isolated from the intravenous devices of patients who developed infections. Five of 7 catheters (71%) used for TPN caused infection from the Candida species. However, only 2 of 26 catheters (8%) not used for TPN were associated with Candida infections (P =.005). It should be noted that in patients who developed Candida infections, the median number of days to infection was 44. This interval, which is significantly shorter than that of infections caused by other organisms (44 days vs 126 days), indicates that ports used for TPN are prone to developing fungal infections. Several similar observations of a high incidence of fungal infections among patients receiving TPN indicate that the TPN solution may play a role in fungal infection Certain types of catheters may further increase the incidence of fungal infection when they are used for TPN. Clinicians, therefore, carefully need to select the appropriate catheter for TPN. The results of our study suggest that the intravenous line for TPN should be used with special caution and imply that the port may not be a good choice for delivering TPN in cancer patients. CONCLUSIONS Our observations are similar to those reported by the other investigators: infection is the most common complication in the use of venous port systems among cancer patients. Some catheter-related infections are difficult to prevent due to the general condition of the patient, some types of treatments, and the nature of invasive procedures. However, the infection rate can be significantly lowered by appropriate preventive strategies and by good patient care performed by a well-trained nursing staff. For debilitated and immunocompromised cancer patients, diligent aseptic care is even more important in reducing catheter-related infections. According to our data, it is safe and cost-effective to change exit-site needles and transparent dressings every 7 days. Because most of the infectious organisms are commonly colonized on the skin and in the fluids, it is most important to sterilize and maintain cleanliness of the exit-site area. Finally, our study clearly demonstrates that ports used for the administration of TPN results in the patient having a significantly greater chance of developing infection from the Candida species. The advantages of using ports for chemotherapy in cancer patients have been well documented; however, further investigation is needed to compare the relative advantages of using ports versus other devices for the administration of TPN in cancer patients. We are grateful to Cosi Long for her help and support in preparing this manuscript. References 1. Lambert ME, Chadwick GA, McMahon A, Scarffe JH. Experience with the Port-a-Cath. Hematol Oncol 1988;6: May GS, Davis C. Percutaneous catheters and totally implantable access systems: a review of reported infection rates. J Intravenous Nurs 1988;11(2): Strum B, McDermed J, Korn A, Joseph C. Improved methods for venous access: the Port-a-Cath, a totally implanted catheter system. J Clin Oncol 1986;4(4): Carde P, Cosset-Delaigue MF, Laplanche A, Chareau I. Classical external indwelling central venous catheter versus totally
6 Chang et al February implanted venous access systems for chemotherapy administration: a randomized trial in 100 patients with solid tumors. Eur J Cancer Clin Oncol 1989;25: Barrios CH, Zuke JE, Blaes B, Hirsch JD, Lyss AP. Evaluation of an implantable venous access system in a general oncology population. Oncology 1992;49: Sinoff CL, Koski T. Port-a-Cath in cancer patients. S Afr Med J 1993;83: Wesenberg F, Flaatten H, Janssen CW. Central venous catheter with subcutaneous injection port (Port-a-Cath): 8 years clinical follow up with children. Pediatr Hematol Oncol 1993;10: Poorter RL, Lauw FN, Bemelman WA, Bakker PJM, Taat CW, Veenhof CHN. Complications of an implantable venous access device (Port-a-Cath) during intermittent continuous infusion of chemotherapy. Eur J Cancer 1996;32A: Kock HJ, Pietsch M, Krause U,Wilke H, Eigler FW. Implantable vascular access systems: experience in 1500 patients with totally implanted central venous port systems.world J Surg 1998;22: Schwarz RE, Groeger JS, Coit DG. Subcutaneously implanted central venous access devices in cancer patients: a prospective analysis. Cancer 1997;79: Ballarini C, Intra M, Pisani Ceretti A, Cordovana A, Pagani M, Farina G, et al. Complications of subcutaneous infusion port in the general oncology population. Oncology 1999;56: Torramade JR, Cienfuegos JA, Hernandez JL, Pardo F, Benito C, Gonzalez J.The complications of central venous access systems: a study of 218 patients. Eur J Surg 1993;159: Raad I, Hanna H. Nosocomial infections related to use of intravascular devices inserted for long-term vascular access. In: Mayhall CG, ed. Hospital epidemiology and infection control. 2nd ed. Philadelphia: Lippincott Williams & Wilkins; p Hempsey SJ,Young JE, Alcock SR, Stack BH. Needle change preferences and rate of infection in cystic fibrosis adult with a Porta-Cath device in situ [abstract].thorax 1998;53(Suppl4):A Centers for Disease Control and Prevention, Department of Health and Human Services. Draft guideline for prevention of intravascular device-related infection. Federal Register 1994; 60:49,978-50, Maki DG. Infections causes by intravascular devices used for infusion therapy: pathogenesis, prevention and management. In: Bisno A,Waldvogel FA, eds. Infections associated with indwelling medical devices. 2nd ed.washington (DC):ASM Press; p Wheat LJ. Fungal infections in the immunocompromised host. In: Rubin RH, Young LS, eds. Clinical approach to infection in the compromised host. 3rd ed. New York: Plenum Medical Book Company; p Borzotta AP, Beardsley K. Candida infections in critically ill trauma patients: a retrospective case-control study. Arch Surg 1999;134: Chiu NC, Chung YF, Huang FY. Pediatric nosocomial fungal infections. Southeast Asian J Trop Med Public Health 1997;28(1): Dean DA, Burchard KW. Fungal infection in surgical patients.am J Surg 1996;171: Flynn PM, Marina NM, Rivera GK, Hughes WT. Candida tropicalis infections in children with leukemia. Leuk Lymphoma 1993;10:
Mary Lou Garey MSN EMT-P MedFlight of Ohio
 Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
ESPEN Congress Brussels How to take care of central venous access devices (CVAD)? Eva Johansson
 ESPEN Congress Brussels 2005 How to take care of central venous access devices (CVAD)? Eva Johansson How to take care of central venous access devices (CVAD)? Eva Johansson, RN, PhD Division of Hematology
ESPEN Congress Brussels 2005 How to take care of central venous access devices (CVAD)? Eva Johansson How to take care of central venous access devices (CVAD)? Eva Johansson, RN, PhD Division of Hematology
Central Venous Access Devices. Stephanie Cunningham Amy Waters
 Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
Vaxcel Implantable Ports Valved and Non-Valved. A Patient s Guide
 Vaxcel Implantable Ports Valved and Non-Valved A Patient s Guide Vaxcel Implantable Port This pamphlet provides some answers to questions you may have about your implantable port and how to care for it
Vaxcel Implantable Ports Valved and Non-Valved A Patient s Guide Vaxcel Implantable Port This pamphlet provides some answers to questions you may have about your implantable port and how to care for it
ORIGINAL INVESTIGATION. Single-Lumen Subcutaneous Ports Inserted by Interventional Radiologists in Patients Undergoing Chemotherapy
 ORIGINAL INVESTIGATION Single-Lumen Subcutaneous Ports Inserted by Interventional Radiologists in Patients Undergoing Chemotherapy Incidence of Infection and Outcome of Attempted Catheter Salvage Delia
ORIGINAL INVESTIGATION Single-Lumen Subcutaneous Ports Inserted by Interventional Radiologists in Patients Undergoing Chemotherapy Incidence of Infection and Outcome of Attempted Catheter Salvage Delia
The Clinical Significance of Blood Cultures. Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM
 The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
Healthcare-associated infections acquired in intensive care units
 SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy.
 Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
IV therapy. By: Susan Mberenga, RN, MSN. Copyright 2016, 2013, 2010, 2006, 2002 by Saunders, an imprint of Elsevier Inc.
 IV therapy By: Susan Mberenga, RN, MSN 1 IV Therapy Types of solutions Isotonic Hypotonic Hypertonic Caution: Too rapid or excessive infusion of any IV fluid has the potential to cause serious problems
IV therapy By: Susan Mberenga, RN, MSN 1 IV Therapy Types of solutions Isotonic Hypotonic Hypertonic Caution: Too rapid or excessive infusion of any IV fluid has the potential to cause serious problems
Determination of complication rate of PICC lines in Oncological Patients
 Original Article Determination of complication rate of PICC lines in Oncological Patients Ghulam Haider, Shiyam Kumar, Basit Salam, Nehal Masood, Asim Jamal, Yasmeen Abdul Rasheed Section Hematology, Oncology
Original Article Determination of complication rate of PICC lines in Oncological Patients Ghulam Haider, Shiyam Kumar, Basit Salam, Nehal Masood, Asim Jamal, Yasmeen Abdul Rasheed Section Hematology, Oncology
Appendix E: Overview of Vascular
 Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
Emergency clamp should always be readily available in case of accidental catheter fracture
 Note: Please see individual policies for further information. Flushing best practice: Always use a 10 diameter syringe or larger when first accessing and when flushing vascular access device (VAD) Use
Note: Please see individual policies for further information. Flushing best practice: Always use a 10 diameter syringe or larger when first accessing and when flushing vascular access device (VAD) Use
IV Drug Delivery Systems used in Cancer Care
 IV Drug Delivery Systems used in Cancer Care Cheri Constantino-Shor, RN, MSN, CRNI Seattle Cancer Care Alliance Nursing Staff Development Coordinator Presentation Objective Describe drug delivery devices
IV Drug Delivery Systems used in Cancer Care Cheri Constantino-Shor, RN, MSN, CRNI Seattle Cancer Care Alliance Nursing Staff Development Coordinator Presentation Objective Describe drug delivery devices
The High-Flow Port Designed & Indicated for Apheresis
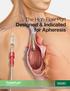 The High-Flow Port Designed & Indicated for Apheresis Advancing Lives and the Delivery of Health Care Bard is proud to introduce the first and only high-flow, power-injectable port designed and indicated
The High-Flow Port Designed & Indicated for Apheresis Advancing Lives and the Delivery of Health Care Bard is proud to introduce the first and only high-flow, power-injectable port designed and indicated
Advancing Lives and the Delivery of Health Care. The High-Flow Port Designed for Apheresis
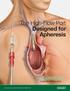 Advancing Lives and the Delivery of Health Care The High-Flow Port Designed for Apheresis Optimized for Long Device Life Bench Tested up to 1,000 Accesses 1 Bard is proud to introduce the first and only
Advancing Lives and the Delivery of Health Care The High-Flow Port Designed for Apheresis Optimized for Long Device Life Bench Tested up to 1,000 Accesses 1 Bard is proud to introduce the first and only
Central Venous Access Devices and Infection
 Central Venous Access Devices and Infection Dr Andrew Daley Microbiology & Infectious Diseases Women s & Children s Health Melbourne Background Types of infection! Local site infection! Blood stream infection!
Central Venous Access Devices and Infection Dr Andrew Daley Microbiology & Infectious Diseases Women s & Children s Health Melbourne Background Types of infection! Local site infection! Blood stream infection!
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used
 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing Description 3M Tegaderm CHG Chlorhexidine Gluconate I.V. Securement Dressing is used to cover and protect catheter sites and to secure devices
IV Fluids. Nursing B23. Objectives. Serum Osmolality
 IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
Unit 11. Objectives. Indications for IV Therapy. Intravenous Access Devices & Common IV Fluids. 3 categories. Maintenance Replacement Restoration
 Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
IV Fluids Nursing B23 Objectives Serum Osmolality 275 to 295 Isotonic
 1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
1 IV Fluids Nursing B23 2 Objectives 3 Serum Osmolality Serum osmolality solute concentration of a solution Higher osmolality means greater pulling power for water Normal serum osmolality is 275 to 295
Prevent Bloodstream Infections by Using Appropriate Devices
 37 Prevent Bloodstream Infections by Using Appropriate Devices Situation Catheter-associated infections include exit, tunnel, pocket and bloodstream infections. In the United States, when these types of
37 Prevent Bloodstream Infections by Using Appropriate Devices Situation Catheter-associated infections include exit, tunnel, pocket and bloodstream infections. In the United States, when these types of
Totally implantable venous access system (TIVAS) Complicated by Tracheo-Venous Fistula
 Totally implantable venous access system (TIVAS) Complicated by Tracheo-Venous Fistula Samer Khaled, M.D., Vladimir Gotlieb, M.D., and Arunbai Patel, M.D. Citation: Khaled S, Gotlieb V, Patel A. Totally
Totally implantable venous access system (TIVAS) Complicated by Tracheo-Venous Fistula Samer Khaled, M.D., Vladimir Gotlieb, M.D., and Arunbai Patel, M.D. Citation: Khaled S, Gotlieb V, Patel A. Totally
Totally indwelling venous access devices
 Totally indwelling venous access devices Leeds MDT. April, 2008. Totally indwelling venous access devices [online]. Department of Respiratory Medicine, St James's University Hospital, UK. Available from
Totally indwelling venous access devices Leeds MDT. April, 2008. Totally indwelling venous access devices [online]. Department of Respiratory Medicine, St James's University Hospital, UK. Available from
SPECIAL COMMUNICATION Guideline for prevention of intravascular device-related infections Part I. Intravascular device-related infections: An overview
 SPECIAL COMMUNICATION Guideline for prevention of intravascular device-related infections Part I. Intravascular device-related infections: An overview Michele L. Pearson, MD The Hospital Infection Control
SPECIAL COMMUNICATION Guideline for prevention of intravascular device-related infections Part I. Intravascular device-related infections: An overview Michele L. Pearson, MD The Hospital Infection Control
320 MBIO Microbial Diagnosis. Aljawharah F. Alabbad Noorah A. Alkubaisi 2017
 320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Blood Culture What is a blood culture? A blood culture is a laboratory test in which blood is injected into bottles with culture
320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Blood Culture What is a blood culture? A blood culture is a laboratory test in which blood is injected into bottles with culture
Intravenous Catheter Complications
 Vascular Access Device-Related Infection Inadequate skin antisepsis prior to VAD insertion Acute onset of fever, chills, and hypotension. No other apparent source of Notify Prescriber immediately Obtain
Vascular Access Device-Related Infection Inadequate skin antisepsis prior to VAD insertion Acute onset of fever, chills, and hypotension. No other apparent source of Notify Prescriber immediately Obtain
The Impact of Healthcare Associated Infection (HCAI)
 Instructions for use Save this presentation Feel free to add or delete slides as necessary, change information to suit local needs and as new guidance or evidence is published Disclaimer: Whilst the working
Instructions for use Save this presentation Feel free to add or delete slides as necessary, change information to suit local needs and as new guidance or evidence is published Disclaimer: Whilst the working
About Implanted Ports
 PATIENT & CAREGIVER EDUCATION About Your Implanted Port This information will teach you about the placement and care of your implanted port. An implanted port is a type of central venous catheter (CVC).
PATIENT & CAREGIVER EDUCATION About Your Implanted Port This information will teach you about the placement and care of your implanted port. An implanted port is a type of central venous catheter (CVC).
NOTTINGHAM CHILDREN S HOSPITAL Nursing Guideline. P07 Care and Management of Children with a Totally Implantable Venous Access Device (Portacath).
 NOTTINGHAM CHILDREN S HOSPITAL Nursing Guideline P07 Care and Management of Children with a Totally Implantable Venous Access Device (Portacath). Introduction A Portacath is a central venous access device
NOTTINGHAM CHILDREN S HOSPITAL Nursing Guideline P07 Care and Management of Children with a Totally Implantable Venous Access Device (Portacath). Introduction A Portacath is a central venous access device
Port Design. Page 1. Port Placement, Removal, and Management. Selecting a Vascular Access Device. Thomas M. Vesely, MD
 Non-Dialysis Procedures Port Placement, Removal, and Management Thomas M. Vesely, MD Saint Louis, Missouri Selecting a Vascular Access Device Duration of use Number of lumens Frequency used Blood flow
Non-Dialysis Procedures Port Placement, Removal, and Management Thomas M. Vesely, MD Saint Louis, Missouri Selecting a Vascular Access Device Duration of use Number of lumens Frequency used Blood flow
Venenkatheter-assoziierte Infektionen
 Update Infektionen in der Hämatologie und Onkologie Venenkatheter-assoziierte Infektionen Georg Maschmeyer Potsdam www.dghoinfektionen.de Aktuelle Leitlinie der AGIHO...unter Berücksichtigung von: Ann
Update Infektionen in der Hämatologie und Onkologie Venenkatheter-assoziierte Infektionen Georg Maschmeyer Potsdam www.dghoinfektionen.de Aktuelle Leitlinie der AGIHO...unter Berücksichtigung von: Ann
SURVEILLANCE BLOODSTREAM INFECTIONS IN BELGIAN HOPITALS ( SEP ) RESULTS ANNUAL REPORT data
 SURVEILLANCE BLOODSTREAM INFECTIONS IN BELGIAN HOPITALS ( SEP ) RESULTS ANNUAL REPORT data 2000-2014 SEP Workgroup Meeting 24 June 2015 Dr. Naïma Hammami Dr. Marie-Laurence Lambert naima.hammami@wiv-isp.be
SURVEILLANCE BLOODSTREAM INFECTIONS IN BELGIAN HOPITALS ( SEP ) RESULTS ANNUAL REPORT data 2000-2014 SEP Workgroup Meeting 24 June 2015 Dr. Naïma Hammami Dr. Marie-Laurence Lambert naima.hammami@wiv-isp.be
Consideration of some other specific indications: Bacteremia
 European Medicines Agency Workshop on Antibacterials, London 7-8 February 2011 Consideration of some other specific indications: Bacteremia Harald Seifert Institut für Medizinische Mikrobiologie, Immunologie
European Medicines Agency Workshop on Antibacterials, London 7-8 February 2011 Consideration of some other specific indications: Bacteremia Harald Seifert Institut für Medizinische Mikrobiologie, Immunologie
MANAGEMENT OF INTRAVASCULAR (IV) LINES AND THERAPY. All GCC Countries
 TITLE/DESCRIPTION: MANAGEMENT OF INTRAVASCULAR (IV) LINES AND THERAPY INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL CENTRE
TITLE/DESCRIPTION: MANAGEMENT OF INTRAVASCULAR (IV) LINES AND THERAPY INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL CENTRE
PORTS SETTING THE STANDARD WITH A COMPREHENSIVE FAMILY OF PORTS
 PORTS SETTING THE STANDARD WITH A COMPREHENSIVE FAMILY OF PORTS As a single-source provider, Bard Access Systems sets the standard for implanted ports and vascular access devices. We make it possible for
PORTS SETTING THE STANDARD WITH A COMPREHENSIVE FAMILY OF PORTS As a single-source provider, Bard Access Systems sets the standard for implanted ports and vascular access devices. We make it possible for
Key words: Bacteremia, Catheter
 Key words: Bacteremia, Catheter 1. ID No.: 2. Name: 3. Date of Birth: 4. Ward: Table 1 Recordings Inspection Card on Central Venous Catheter [To be filled out by physicians] 5. Type of catheter A: central
Key words: Bacteremia, Catheter 1. ID No.: 2. Name: 3. Date of Birth: 4. Ward: Table 1 Recordings Inspection Card on Central Venous Catheter [To be filled out by physicians] 5. Type of catheter A: central
Per-Q-Cath* PICC Catheters with Excalibur Introducer* System
 Bard Access Systems Per-Q-Cath* PICC and Catheters with Excalibur Introducer* System Instructions For Use Table of Contents Table of Contents Page Contents 1 Product Description, Indications & Contraindications
Bard Access Systems Per-Q-Cath* PICC and Catheters with Excalibur Introducer* System Instructions For Use Table of Contents Table of Contents Page Contents 1 Product Description, Indications & Contraindications
External Ref: Andres, D.A., et al. Catheter Pinch-Off Syndrome: Recognition and Management.
 Department Policy Code: D: PC-5530 Entity: Fairview Pharmacy Services Department: Fairview Home Infusion Manual: Policy and Procedure Manual Category: Home Infusion Subject: Complications With Intravenous
Department Policy Code: D: PC-5530 Entity: Fairview Pharmacy Services Department: Fairview Home Infusion Manual: Policy and Procedure Manual Category: Home Infusion Subject: Complications With Intravenous
Surveillance of Healthcare Associated Infections in Scottish Intensive Care Units
 Surveillance of Healthcare Associated Infections in Scottish Intensive Care Units Annual report of data from January 2010 to December 2010 Scottish Intensive Care Society Audit Group 1 Health Protection
Surveillance of Healthcare Associated Infections in Scottish Intensive Care Units Annual report of data from January 2010 to December 2010 Scottish Intensive Care Society Audit Group 1 Health Protection
Insertion of a totally implantable vascular access device (TIVAD)
 Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
ISF criteria (International sepsis forum consensus conference of infection in the ICU) Secondary peritonitis
 Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
The Impact of Catheter Occlusion in Central Line Associated Bloodstream Infections M A R C H 15, 2017
 The Impact of Catheter Occlusion in Central Line Associated Bloodstream Infections D A R C Y DOELLMAN M S N, RN, CRNI, VA - BC M A R C H 15, 2017 LOUISVILLE, KENTUCKY Cincinnati Children s Hospital 642
The Impact of Catheter Occlusion in Central Line Associated Bloodstream Infections D A R C Y DOELLMAN M S N, RN, CRNI, VA - BC M A R C H 15, 2017 LOUISVILLE, KENTUCKY Cincinnati Children s Hospital 642
Central Line Care and Management
 Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
If viewing a printed copy of this policy, please note it could be expired. Got to to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5530 Entity: Fairview Pharmacy Services
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5530 Entity: Fairview Pharmacy Services
REVIEW Safety of Central Venous Catheter Placement at Diagnosis of Acute Lymphoblastic Leukemia in Children
 Pediatr Blood Cancer 2012;58:498 502 REVIEW Safety of Central Venous Catheter Placement at Diagnosis of Acute Lymphoblastic Leukemia in Children G. Gonzalez, MD, 1 A.M. Davidoff, MD, 1,2 S.C. Howard, MD,
Pediatr Blood Cancer 2012;58:498 502 REVIEW Safety of Central Venous Catheter Placement at Diagnosis of Acute Lymphoblastic Leukemia in Children G. Gonzalez, MD, 1 A.M. Davidoff, MD, 1,2 S.C. Howard, MD,
Venous Access and Ports. Helen Starosta
 Venous Access and Ports Helen Starosta Venous access and ports Peripheral IV access Arterio-Venous Fistula Central venous access Peripherally Inserted Central Catheter (PICC) Non Tunnelled Central Venous
Venous Access and Ports Helen Starosta Venous access and ports Peripheral IV access Arterio-Venous Fistula Central venous access Peripherally Inserted Central Catheter (PICC) Non Tunnelled Central Venous
High Impact Intervention Peripheral intravenous cannula care bundle
 High Impact Intervention Peripheral intravenous cannula care bundle Aim To reduce the incidence of peripheral intravenous cannula infections. Introduction The aim of the care bundle, as set out in this
High Impact Intervention Peripheral intravenous cannula care bundle Aim To reduce the incidence of peripheral intravenous cannula infections. Introduction The aim of the care bundle, as set out in this
ESPEN Congress Florence 2008
 ESPEN Congress Florence 2008 Complications of Central Venous Catheters EPIDEMIOLOGY & DIAGNOSIS & PREVENTION Federico Bozzetti (Italy) CVC COMPLICATIONS EPIDEMIOLOGY & DIAGNOSIS & PREVENTION Federico Bozzetti
ESPEN Congress Florence 2008 Complications of Central Venous Catheters EPIDEMIOLOGY & DIAGNOSIS & PREVENTION Federico Bozzetti (Italy) CVC COMPLICATIONS EPIDEMIOLOGY & DIAGNOSIS & PREVENTION Federico Bozzetti
Nosocomial infections surveillance in RIPAS Hospital
 Original Article Brunei Int Med J. 212; 8 (6): 32-333 Nosocomial infections surveillance in RIPAS Hospital Muppidi SATYAVANI, 1, 2 Junita MOMIN, ² and Samuel Kai San YAPP 2, 3 ¹ Department of Microbiology,
Original Article Brunei Int Med J. 212; 8 (6): 32-333 Nosocomial infections surveillance in RIPAS Hospital Muppidi SATYAVANI, 1, 2 Junita MOMIN, ² and Samuel Kai San YAPP 2, 3 ¹ Department of Microbiology,
Lab 4. Blood Culture (Media) MIC AMAL-NORA-ALJAWHARA 1
 Lab 4. Blood Culture (Media) 2018 320 MIC AMAL-NORA-ALJAWHARA 1 Blood Culture 2018 320 MIC AMAL-NORA-ALJAWHARA 2 What is a blood culture? A blood culture is a laboratory test in which blood is injected
Lab 4. Blood Culture (Media) 2018 320 MIC AMAL-NORA-ALJAWHARA 1 Blood Culture 2018 320 MIC AMAL-NORA-ALJAWHARA 2 What is a blood culture? A blood culture is a laboratory test in which blood is injected
Fungi GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 53: Author Moi Lin Ling, MBBS, FRCPA, CPHQ, MBA
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 53: Fungi Author Moi Lin Ling, MBBS, FRCPA, CPHQ, MBA Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Cover heading - Topic Outline Topic outline
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 53: Fungi Author Moi Lin Ling, MBBS, FRCPA, CPHQ, MBA Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Cover heading - Topic Outline Topic outline
Preserving sites and protecting veins
 Reduces complications 1 * Dwells longer 1 * Preserves sites 1-7 Preserving sites and protecting veins The BD Nexiva closed peripheral IV catheter system, shown to preserve sites for longer and designed
Reduces complications 1 * Dwells longer 1 * Preserves sites 1-7 Preserving sites and protecting veins The BD Nexiva closed peripheral IV catheter system, shown to preserve sites for longer and designed
Alberta Health Services Infection Prevention and Control - Initiatives and Services. Surveillance Protocol January 12, 2010 Rev.
 Alberta Health Services Infection Prevention and Control - Initiatives and Services Hospital Acquired Bloodstream Infections (HABSI) Hospital Wide- in Acute Care and Acute Rehabilitation Facilities Surveillance
Alberta Health Services Infection Prevention and Control - Initiatives and Services Hospital Acquired Bloodstream Infections (HABSI) Hospital Wide- in Acute Care and Acute Rehabilitation Facilities Surveillance
Foundations in Microbiology
 Foundations in Microbiology Fifth Edition Talaro Chapter 13 Microbe Human Interactions: Infection and Disease Chapter 13 2 3 Infection a condition in which pathogenic microbes penetrate host defenses,
Foundations in Microbiology Fifth Edition Talaro Chapter 13 Microbe Human Interactions: Infection and Disease Chapter 13 2 3 Infection a condition in which pathogenic microbes penetrate host defenses,
CENTRAL VENOUS ACCESS DEVICES. BETHANY COLTON
 CENTRAL VENOUS ACCESS DEVICES. BETHANY COLTON Aims and Objectives To know what central venous access devices (CVAD) are. Types of CVADS used in haematology. To understand why we use them To know the complications
CENTRAL VENOUS ACCESS DEVICES. BETHANY COLTON Aims and Objectives To know what central venous access devices (CVAD) are. Types of CVADS used in haematology. To understand why we use them To know the complications
Central Venous Catheter (CVC) Care for the Patient with Cancer. Clinical Practice Guideline
 Central Venous Catheter (CVC) Care for the Patient with Cancer Clinical Practice Guideline Introduction & Context Stable venous access is used for a wide range of indications including chemotherapy, blood
Central Venous Catheter (CVC) Care for the Patient with Cancer Clinical Practice Guideline Introduction & Context Stable venous access is used for a wide range of indications including chemotherapy, blood
The University of Toledo Medical Center and its Medical Staff
 Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
2016:26: % [1] Frederick Foley 9,600 25% [2,3] DOI: /ICJ
![2016:26: % [1] Frederick Foley 9,600 25% [2,3] DOI: /ICJ 2016:26: % [1] Frederick Foley 9,600 25% [2,3] DOI: /ICJ](/thumbs/93/114528525.jpg) 203 1,3 1,2,3 1 2 3 2016:26:203-209 Frederick Foley 4 95% [1] 9,600 25% [2,3] 105 6 15 105 8 31 201 02-28757462 DOI: 10.6526/ICJ.2016.503 105 10 204 [4-6] ( ) (extraluminal infection) (endogenous) 70%
203 1,3 1,2,3 1 2 3 2016:26:203-209 Frederick Foley 4 95% [1] 9,600 25% [2,3] 105 6 15 105 8 31 201 02-28757462 DOI: 10.6526/ICJ.2016.503 105 10 204 [4-6] ( ) (extraluminal infection) (endogenous) 70%
TYPES AND USES OF VENOUS ACCESS DEVICES
 FOR HEALTHCARE PROVIDER USE ONLY. THIS INFORMATION IS FOR REFERENCE PURPOSES ONLY AND DOES NOT TYPES AND USES OF VENOUS ACCESS DEVICES PERIPHERAL DEVICES 1 Typically inserted in the hand, arm, or foot
FOR HEALTHCARE PROVIDER USE ONLY. THIS INFORMATION IS FOR REFERENCE PURPOSES ONLY AND DOES NOT TYPES AND USES OF VENOUS ACCESS DEVICES PERIPHERAL DEVICES 1 Typically inserted in the hand, arm, or foot
Vascular Catheter Related Infections in a Tertiary Care Hospital A Microbiological Study
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 592-599 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.072
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 592-599 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.072
EXECUTIVE SUMMARY. General
 I D S A G U I D E L I N E S Clinical Practice Guidelines for the Diagnosis and Management of Intravascular Catheter-Related Infection: 2009 Update by the Infectious Diseases Society of America Leonard
I D S A G U I D E L I N E S Clinical Practice Guidelines for the Diagnosis and Management of Intravascular Catheter-Related Infection: 2009 Update by the Infectious Diseases Society of America Leonard
Is it Necessary to Verify Blood Return in Monthly Port Flushes?
 Is it Necessary to Verify Blood Return in Monthly Port Flushes? Gloria B. Ascoli, RN, CRNI, Amy C. Brown, BSN, RN, Jessica L. Cooper, BSN, RN, Allison N. Crawford, BSN, RN, CRNI Background Research Aims
Is it Necessary to Verify Blood Return in Monthly Port Flushes? Gloria B. Ascoli, RN, CRNI, Amy C. Brown, BSN, RN, Jessica L. Cooper, BSN, RN, Allison N. Crawford, BSN, RN, CRNI Background Research Aims
CAUTI CONFERENCE CAUTI Prevention and Appropriate Use of Indwelling Urinary Catheters in the Hospital Setting
 CAUTI CONFERENCE CAUTI Prevention and Appropriate Use of Indwelling Urinary Catheters in the Hospital Setting James T. Fields, MD Carolinas Center for Medical Excellence Columbia, South Carolina February
CAUTI CONFERENCE CAUTI Prevention and Appropriate Use of Indwelling Urinary Catheters in the Hospital Setting James T. Fields, MD Carolinas Center for Medical Excellence Columbia, South Carolina February
Blood cultures in ED. Dr Sebastian Chang MBBS FACEM
 Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
A Multicentre Study about Pattern and Organisms Isolated in Follow-up Blood Cultures
 Ann Clin Microbiol Vol., No., March, 0 http://dx.doi.org/0./acm.0... ISSN -0 A Multicentre Study about Pattern and Organisms Isolated in Follow-up Blood Cultures Jeong Hwan Shin, Eui Chong Kim, Sunjoo
Ann Clin Microbiol Vol., No., March, 0 http://dx.doi.org/0./acm.0... ISSN -0 A Multicentre Study about Pattern and Organisms Isolated in Follow-up Blood Cultures Jeong Hwan Shin, Eui Chong Kim, Sunjoo
Choosing the right access for long term parenteral nutrition: PICC lines or tunnelled catheters G. Goossens (BE)
 ESPEN Congress Lisbon 2015 HOW TO MAKE HOME PARENTERAL NUTRITION SAFER Choosing the right access for long term parenteral nutrition: PICC lines or tunnelled catheters G. Goossens (BE) Choosing the right
ESPEN Congress Lisbon 2015 HOW TO MAKE HOME PARENTERAL NUTRITION SAFER Choosing the right access for long term parenteral nutrition: PICC lines or tunnelled catheters G. Goossens (BE) Choosing the right
Catheter tip cultures on open-heart surgery patients: associations with site of catheter and age of patients
 Catheter tip cultures on open-heart surgery patients: associations with site of catheter and age of patients R FREEMAN, N HJERSING, AND ANITA BURRIDGE From the Department of Microbiology, Freman Hospital,
Catheter tip cultures on open-heart surgery patients: associations with site of catheter and age of patients R FREEMAN, N HJERSING, AND ANITA BURRIDGE From the Department of Microbiology, Freman Hospital,
URINARY TRACT INFECTIONS: Focus on CA UTIs
 URINARY TRACT INFECTIONS: Focus on CA UTIs William A. Rutala, Ph.D., M.P.H. Director, Statewide Program for Infection Control and Epidemiology and Research Professor of Medicine, University of North Carolina
URINARY TRACT INFECTIONS: Focus on CA UTIs William A. Rutala, Ph.D., M.P.H. Director, Statewide Program for Infection Control and Epidemiology and Research Professor of Medicine, University of North Carolina
Comparison of blood stream infection rate between conventional peripherally inserted central line (PICC) and tunneled PICC.
 Comparison of blood stream infection rate between conventional peripherally inserted central line (PICC) and tunneled PICC. Poster No.: C-1015 Congress: ECR 2013 Type: Scientific Exhibit Authors: O. Nawawi,
Comparison of blood stream infection rate between conventional peripherally inserted central line (PICC) and tunneled PICC. Poster No.: C-1015 Congress: ECR 2013 Type: Scientific Exhibit Authors: O. Nawawi,
Arglaes provides a seven-day, non-cytotoxic barrier against infection
 Arglaes provides a seven-day, non-cytotoxic barrier against infection Arglaes Controlled-Release Silver Technology Reduce bioburden with Arglaes Silver Barrier Dressings Antimicrobial Arglaes began the
Arglaes provides a seven-day, non-cytotoxic barrier against infection Arglaes Controlled-Release Silver Technology Reduce bioburden with Arglaes Silver Barrier Dressings Antimicrobial Arglaes began the
NEOSPORIN G.U. Irrigant Sterile (neomycin sulfate polymyxin B sulfate solution for irrigation)
 NEOSPORIN G.U. Irrigant Sterile (neomycin sulfate polymyxin B sulfate solution for irrigation) NEOSPORIN G.U.SOLUTION NOT FOR INJECTION DESCRIPTION NEOSPORIN G.U. Irrigant is a concentrated sterile antibiotic
NEOSPORIN G.U. Irrigant Sterile (neomycin sulfate polymyxin B sulfate solution for irrigation) NEOSPORIN G.U.SOLUTION NOT FOR INJECTION DESCRIPTION NEOSPORIN G.U. Irrigant is a concentrated sterile antibiotic
Sterility Testing of Peripheral Blood Stem cell (PBSC) harvests in a Tertiary Oncology Setup
 Sterility Testing of Peripheral Blood Stem cell (PBSC) harvests in a Tertiary Oncology Setup Bankar S 1, Tirlotkar A 1, Ojha S 1, Bhat V 2,Kannan S 3, Rajadhyaksha S 1 1. Department of Transfusion Medicine,
Sterility Testing of Peripheral Blood Stem cell (PBSC) harvests in a Tertiary Oncology Setup Bankar S 1, Tirlotkar A 1, Ojha S 1, Bhat V 2,Kannan S 3, Rajadhyaksha S 1 1. Department of Transfusion Medicine,
Identification and Management of Central Vascular Access Device Complications
 Identification and Management of Central Vascular Access Device Complications David Hahn, MD Interventional Radiology NorthShore University HealthSystem Evanston, Illinois Disclosures Consultant, AngioDynamics,
Identification and Management of Central Vascular Access Device Complications David Hahn, MD Interventional Radiology NorthShore University HealthSystem Evanston, Illinois Disclosures Consultant, AngioDynamics,
Bloodstream Infections
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 30: Bloodstream Infections Authors Larry Lutwick MD Gonzalo Bearman MD, MPH Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Topic Outline Definition
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 30: Bloodstream Infections Authors Larry Lutwick MD Gonzalo Bearman MD, MPH Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Topic Outline Definition
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任
 Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure
 ORIGINAL ARTICLE Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure Yi-Ching Tung, Yen-Hsuan Ni, Hong-Shiee Lai, 1 Der-Yirng Hsieh, 2 Mei-Hwei Chang*
ORIGINAL ARTICLE Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure Yi-Ching Tung, Yen-Hsuan Ni, Hong-Shiee Lai, 1 Der-Yirng Hsieh, 2 Mei-Hwei Chang*
open-heart surgery patients
 Thorax (1975), 30, 26. Analysis of results of catheter tip cultures in open-heart surgery patients R. FREEMAN and B. KING Department of Microbiology, University of Leeds Freeman, R. and King, B. (1975).
Thorax (1975), 30, 26. Analysis of results of catheter tip cultures in open-heart surgery patients R. FREEMAN and B. KING Department of Microbiology, University of Leeds Freeman, R. and King, B. (1975).
CVAD Flushing Literature
 CVAD Flushing Literature Aquino, V. M., E. S. Sandler, et al. (2002). "A prospective double-blind randomized trial of urokinase flushes to prevent bacteremia resulting from luminal colonization of subcutaneous
CVAD Flushing Literature Aquino, V. M., E. S. Sandler, et al. (2002). "A prospective double-blind randomized trial of urokinase flushes to prevent bacteremia resulting from luminal colonization of subcutaneous
Totally implantable venous access devices in children with cystic fibrosis: incidence and type of complications
 Thorax 1998;53:285 289 285 Thoracic Medicine J Deerojanawong SMSawyer C F Robertson Radiology A M Fink Surgery K B Stokes Royal Children s Hospital, Parkville, Melbourne, Victoria 3052, Australia Correspondence
Thorax 1998;53:285 289 285 Thoracic Medicine J Deerojanawong SMSawyer C F Robertson Radiology A M Fink Surgery K B Stokes Royal Children s Hospital, Parkville, Melbourne, Victoria 3052, Australia Correspondence
Incidence of Infectious Complications in Central Venous Catheterization: Internal Jugular versus Subclavian Route
 Original Article DOI: 0.7354/ijss/206/60 Incidence of Infectious Complications in Central Venous Catheterization: Internal Jugular versus Ashita Mowar, H S Nanda 2, R K Goyal 3 Post-graduate Student, Department
Original Article DOI: 0.7354/ijss/206/60 Incidence of Infectious Complications in Central Venous Catheterization: Internal Jugular versus Ashita Mowar, H S Nanda 2, R K Goyal 3 Post-graduate Student, Department
Clinical Practice Guideline on Central Venous Catheter Care for the Patient with Cancer
 Clinical Practice Guideline on Central Venous Catheter Care for the Patient with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER
Clinical Practice Guideline on Central Venous Catheter Care for the Patient with Cancer COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive Care Endorsed Guidelines. DISCLAIMER
Section: 2. Introduction
 Section: 2 Introduction Associated Infection; Indian Society of Critical Care Medicine. How to cite this article: Associated Infection; Indian Society of Critical Care Medicine.. Introduction. Indian J
Section: 2 Introduction Associated Infection; Indian Society of Critical Care Medicine. How to cite this article: Associated Infection; Indian Society of Critical Care Medicine.. Introduction. Indian J
Jo Kuehn, RN, MSN, CPHQ Jenell Westhoven, RN, BSN
 Jo Kuehn, RN, MSN, CPHQ Jenell Westhoven, RN, BSN Disclosure Information Intravenous Therapy and Parenteral Nutrition Administration: Nursing In- Focus Jo Kuehn, RN, MSN, CPHQ and Jenell Westhoven, RN,
Jo Kuehn, RN, MSN, CPHQ Jenell Westhoven, RN, BSN Disclosure Information Intravenous Therapy and Parenteral Nutrition Administration: Nursing In- Focus Jo Kuehn, RN, MSN, CPHQ and Jenell Westhoven, RN,
Central venous catheters
 Follow the link from the online version of this article to obtain certified continuing medical education credits Central venous catheters Reston N Smith, 1 Jerry P Nolan 2 1 North Bristol NHS Trust, Bristol,
Follow the link from the online version of this article to obtain certified continuing medical education credits Central venous catheters Reston N Smith, 1 Jerry P Nolan 2 1 North Bristol NHS Trust, Bristol,
Successful IV Starts Revised February 2014
 Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
Successful IV Starts Revised February 2014 Why Intravenous Therapy? Used for access to the body s circulation Indications: Administer fluids, blood, medications, and nutrition Obtain laboratory specimens
IR Central Venous Access [ ] Pre Procedure
![IR Central Venous Access [ ] Pre Procedure IR Central Venous Access [ ] Pre Procedure](/thumbs/90/104119758.jpg) IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
Relationship between climate conditions and nosocomial infection rates
 Relationship between climate conditions and nosocomial infection rates Chen Y 1, Xu X 2, Liang J 3, *Lin H 1 1. Department of Prevention and Health-care 2. Department of Stomatology, The Second Affiliated
Relationship between climate conditions and nosocomial infection rates Chen Y 1, Xu X 2, Liang J 3, *Lin H 1 1. Department of Prevention and Health-care 2. Department of Stomatology, The Second Affiliated
RESTORING PATENCY TO CENTRAL VENOUS ACCESS DEVICES
 RESTORING PATENCY TO CENTRAL VENOUS ACCESS DEVICES Indications Venous access is poor Intravenous therapy involves venous sclerosants Ambulatory chemotherapy given as an outpatient Repeated sampling, or
RESTORING PATENCY TO CENTRAL VENOUS ACCESS DEVICES Indications Venous access is poor Intravenous therapy involves venous sclerosants Ambulatory chemotherapy given as an outpatient Repeated sampling, or
Enhanced EARS-Net Surveillance 2017 First Half
 1 Enhanced EARS-Net Surveillance 2017 First Half In this report Main results for 2017, first half Breakdown of factors by organism and resistance subtype Device-association Data quality assessment Key
1 Enhanced EARS-Net Surveillance 2017 First Half In this report Main results for 2017, first half Breakdown of factors by organism and resistance subtype Device-association Data quality assessment Key
A Primer on Central Venous Access: Peripherally-Inserted Central Catheters, Tunneled Catheters, and Subcutaneous Ports
 Disclosures A Primer on Central Venous Access: Peripherally-Inserted Central Catheters, Tunneled Catheters, and Subcutaneous Ports No conflicts of interest relevant to this presentation Jason W. Pinchot,
Disclosures A Primer on Central Venous Access: Peripherally-Inserted Central Catheters, Tunneled Catheters, and Subcutaneous Ports No conflicts of interest relevant to this presentation Jason W. Pinchot,
Home Health Foundation, Inc. To create more permanent IV access for patients undergoing long term IV therapy.
 PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
Ailyn T. Isais-Agdeppa, MD*, Lulu Bravo, MD*
 A FIVE-YEAR RETROSPECTIVE STUDY ON THE COMMON MICROBIAL ISOLATES AND SENSITIVITY PATTERN ON BLOOD CULTURE OF PEDIATRIC CANCER PATIENTS ADMITTED AT THE PHILIPPINE GENERAL HOSPITAL FOR FEBRILE NEUTROPENIA
A FIVE-YEAR RETROSPECTIVE STUDY ON THE COMMON MICROBIAL ISOLATES AND SENSITIVITY PATTERN ON BLOOD CULTURE OF PEDIATRIC CANCER PATIENTS ADMITTED AT THE PHILIPPINE GENERAL HOSPITAL FOR FEBRILE NEUTROPENIA
International Journal of Medical Science and Education pissn eissn
 CATHETER ASSOCIATED URINARY TRACT INFECTION (CAUTI) INDUCED NOSOCOMIAL INFECTION WITH REFERENCE TO INCIDENCE, DURATION AND ORGANISM IN A TERTIARY CARE TEACHING HOSPITAL Dr.Trilok Patil* Associate Professor,
CATHETER ASSOCIATED URINARY TRACT INFECTION (CAUTI) INDUCED NOSOCOMIAL INFECTION WITH REFERENCE TO INCIDENCE, DURATION AND ORGANISM IN A TERTIARY CARE TEACHING HOSPITAL Dr.Trilok Patil* Associate Professor,
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Outpatient parenteral antimicrobial therapy (OPAT) in patients with cystic fibrosis
 Pedersen et al. BMC Infectious Diseases (2015) 15:290 DOI 10.1186/s12879-015-1019-4 RESEARCH ARTICLE Open Access Outpatient parenteral antimicrobial therapy (OPAT) in patients with cystic fibrosis Maya
Pedersen et al. BMC Infectious Diseases (2015) 15:290 DOI 10.1186/s12879-015-1019-4 RESEARCH ARTICLE Open Access Outpatient parenteral antimicrobial therapy (OPAT) in patients with cystic fibrosis Maya
Nephrology. ABC Fax Marie Philipneri Ziyad Al Aly Kamal Amin Mary E. Gellens Bahar Bastani
 American Journal of Nephrology Original Article: Patient-Oriented, Translational Research Am J Nephrol 2003;23:202 207 DOI: 10.1159/000071479 Received: April 1, 2003 Accepted: April 9, 2003 Published online:
American Journal of Nephrology Original Article: Patient-Oriented, Translational Research Am J Nephrol 2003;23:202 207 DOI: 10.1159/000071479 Received: April 1, 2003 Accepted: April 9, 2003 Published online:
A study on common pathogens associated with nosocomial infections and their antibiotic sensitivity
 International Journal of Contemporary Pediatrics Ahirrao VS et al. Int J Contemp Pediatr. 2017 Mar;4(2):365-369 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Ahirrao VS et al. Int J Contemp Pediatr. 2017 Mar;4(2):365-369 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
Impact of a National Shortage of Sterile Ethanol on a Home Parenteral Nutrition Practice: A Case Series
 Case Report Impact of a National Shortage of Sterile Ethanol on a Home Parenteral Nutrition Practice: A Case Series Mandy Corrigan, MPH, RD, LD, CNSC 1, and Donald F. Kirby, MD, FACP, FACN, FACG, AGAF,
Case Report Impact of a National Shortage of Sterile Ethanol on a Home Parenteral Nutrition Practice: A Case Series Mandy Corrigan, MPH, RD, LD, CNSC 1, and Donald F. Kirby, MD, FACP, FACN, FACG, AGAF,
Prevention of dialysis catheter-related sepsis with a citrate taurolidine-containing lock solution
 Nephrol Dial Transplant (2004) 19: 1546 1551 DOI: 10.1093/ndt/gfh014 Advance Access publication 19 February 2004 Original Article Prevention of dialysis catheter-related sepsis with a citrate taurolidine-containing
Nephrol Dial Transplant (2004) 19: 1546 1551 DOI: 10.1093/ndt/gfh014 Advance Access publication 19 February 2004 Original Article Prevention of dialysis catheter-related sepsis with a citrate taurolidine-containing
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
