Basal-LikeBreastCancerDefinedbyFiveBiomarkersHasSuperior Prognostic Value thantriple-negative Phenotype
|
|
|
- Phyllis Hoover
- 6 years ago
- Views:
Transcription
1 Imaging, Diagnosis, Prognosis Basal-LikeBreastCancerDefinedbyFiveBiomarkersHasSuperior Prognostic Value thantriple-negative Phenotype Maggie C.U. Cheang, 1 David Voduc, 1,3 Chris Bajdik, 2 Samuel Leung, 1 Steven McKinney, 1 Stephen K. Chia, 3 Charles M. Perou, 4 andtorsten O. Nielsen 1 Abstract Purpose: Basal-like breast cancer is associated with high grade, poor prognosis, and younger patient age. Clinically, a triple-negative phenotype definition [estrogen receptor, progesterone receptor, and human epidermal growth factor receptor (HER)-2, all negative] is commonly used to identify such cases. EGFR and cytokeratin 5/6 are readily available positive markers of basallike breast cancer applicable to standard pathology specimens. This study directly compares the prognostic significance between three- and five-biomarker surrogate panels to define intrinsic breast cancer subtypes, using a large clinically annotated series of breast tumors. Experimental Design: Four thousand forty-six invasive breast cancers were assembled into tissue microarrays. Allhad staging, pathology, treatment, andoutcomeinformation; medianfollow-up was12.5 years. Cox regression analyses and likelihood ratio tests compared the prognostic significance for breast cancer death-specific survival (BCSS) of the two immunohistochemicalpanels. Results: Among3,744interpretable cases,17% werebasalusingthetriple-negative definition(10- year BCSS, 6 7%) and 9% were basal using the five-marker method (10-year BCSS, 62%). Likelihoodratio tests of multivariable Cox models including standard clinical variables show that the fivemarker panel is significantly more prognostic than the three-marker panel. The poor prognosis of triple-negative phenotype is conferred almost entirely by those tumors positive for basal markers. Amongtriple-negativepatients treatedwithadjuvant anthracycline-basedchemotherapy, theadditionalpositive basal markers identified a cohort of patients with significantly worse outcome. Conclusions: The expanded surrogate immunopanel of estrogen receptor, progesterone receptor, human HER-2, EGFR, and cytokeratin 5/6 provides a more specific definition of basal-like breast cancer that better predicts breast cancer survival. Breast cancer is a heterogeneous disease, and by gene expression profiling has been shown to be classifiable into five major biologically distinct intrinsic subtypes: luminal A, luminal B, human epidermal growth factor receptor-2 (HER2) overexpressing, basal-like, and normal-like (1 3). These Authors Affiliations: 1 Genetic Pathology Evaluation Centre, Vancouver Coastal Health Research Institute, British Columbia Cancer Agency, and University of British Columbia; 2 Cancer Control Research Program, BC Cancer Agency; 3 BC Cancer Agency, Vancouver, British Columbia, Canada; and 4 University of North Carolina, Chapel Hill, North Carolina Received 7/5/07; revised 9/27/07; accepted11/12/07. Grant support: National Cancer Institute Strategic Partnering to Evaluate Cancer Signatures program (UO1-CA114722), National Cancer Institute Breast Specialized Programs of Research Excellence program (P50-CA A1), and a Canadian Breast Cancer Research AllianceTranslational Acceleration Grant. C. Bajdik andt.o. Nielsen are scholars of the Michael Smith Foundation for Health The Genetic Pathology Evaluation Centre is supported by an unrestricted educational grant from sanofi-aventis. The costs of publication of this article were defrayed in part by the payment of page charges. This article must therefore be hereby marked advertisement in accordance with18 U.S.C. Section1734 solely to indicate this fact. Note: Supplementary data for this article are available at Clinical Cancer Research Online ( Requests for reprints: Torsten O. Nielsen, Anatomical Pathology, JP 1401, Vancouver Hospital and Health Sciences Centre, 855 West 12th Avenue, Vancouver, BC, Canada V5Z 1M9. Phone: , ext ; Fax: ; torsten@interchange.ubc.ca. F 2008 American Association for Cancer doi: / ccr molecular subtypes have prognostic and predictive value: the HER2-overexpressing and basal-like breast cancers have poor outcomes, and within the estrogen receptor (ER) positive subtypes the luminal B cohort has a significantly worse prognosis than luminal A. Follow-up studies have shown these subtypes to be conserved across diverse patient series and array platforms (4, 5), and have shown that different gene expression based predictors are likely tracking a similar, common set of biological subtypes, with significant agreement in predicting patient outcome (6). Among the five intrinsic subtypes, basal-like breast cancers have drawn particular attention, because they express neither ER, progesterone receptor (PR), nor HER2, and therefore would not be expected to benefit from antiestrogen hormonal therapies nor from trastuzumab (7). Cost and complexity issues have to date rendered gene expression profiling impractical as a routine hospital diagnostic tool. However, there are immunohistochemistry surrogate panels proposed that can potentially identify basal-like breast cancer, including ER-PR-HER2 negative [the triple-negative phenotype (TNP); ref. 8], and negative hormone receptors and HER2 but either epidermal growth factor receptor (EGFR) or cytokeratin 5/6 (CK5/6) positive (the five-marker method ; refs. 9, 10). The TNP is convenient because it applies standard biomarkers already routinely ordered during the clinical work-up of breast cancer biopsies; however, this approach has never been formally validated by correlating to Clin Cancer Res 2008;14(5) March 1,
2 Five Biomarkers Best Define Basal Breast Cancer Table 1. Summary of clinicopathologic characteristics of 4,046 patients with invasive breast tumors included in this tissue microarray series Characteristics No. patients (%) Age at diagnosis, y V (9.4) (19) ,435 (35.5) >65 1,464 (36.2) Menstrual status at referral Premenopausal 1,188 (29.4) Postmenopausal 2,761 (68.2) Pregnant 2 (0.1) Unknown 95 (2.3) Histology Ductal 3,661 (90.5) Lobular 308 (7.6) Other 77 (1.9) Grade 1 (well differentiated) 211 (5.2) 2 (moderately well or partially differentiated) 1,582 (39.1) 3 (poorly differentiated) 2,069 (51.1) Unknown 184 (4.5) Tumor size, cm V2 2,093 (51.7) 2-5 1,697 (41.9) >5 219 (5.4) Unknown 37 (0.9) Lymphovascular invasion Positive 1,750 (43.3) Negative 2,120 (52.4) Unknown 176 (4.3) Percentage of positive/total number of examined axillary lymph nodes (%) 0 2,161 (53.4) (21.7) > (20.4) Unknown 184 (4.5) Local therapy No breast surgery 60 (1.5) Mastectomy + radiation therapy 631 (15.6) Mastectomy alone 1,557 (38.5) Lumpectomy alone 135 (3.3) Lumpectomy + radiation therapy 1,663 (41.1) Adjuvant systemic therapy (AST) None 1,689 (41.7) Tamoxifen only 1,305 (32.3) Ovarian ablation or hormone therapy other than tamoxifen 7 (0.2) Chemotherapy only, AC 148 (3.7) Chemotherapy AC + tamoxifen 125 (3.1) Chemotherapy only, CMF 429 (10.6) Chemotherapy CMF + tamoxifen 39 (1) Chemotherapy only, FAC 92 (2.3) Chemotherapy FAC + tamoxifen 68 (1.7) Chemotherapy only (other) 70 (1.7) Chemotherapy (other) + tamoxifen 69 (1.7) Ovarian ablation or hormone therapy + chemotherapy 5 (0.1) Abbreviations: AC, doxorubicin and cyclophosphamide; CMF, cyclophosphamide, methotrexate, and fluorouracil; FAC, fluorouracil, doxorubicin, and cyclophosphamide. the gold standard gene expression profiling and relies entirely on negative results to identify basal-like breast cancers, a strategy that may have an elevated risk of false assignments for technical reasons with consequent decreased specificity. On the other hand, including EGFR and CK5/6 as positive immunohistochemical markers has previously been shown to accurately identify basal-like tumors from gene microarray data with 100% specificity and 76% sensitivity (9). Approximately 15% of breast cancers are basal-like and are associated with poor relapse-free and overall survival (9 11). A recent population-based study has shown that this subtype is more prevalent in premenopausal African American women (10), which may contribute to the poor outcomes seen among these patients. Hereditary BRCA-1 breast tumors also resemble sporadic basal-like tumors (3, 12). Basal-like breast cancers are likely to be mitotically active high-grade invasive tumors and Clin Cancer Res 2008;14(5) March 1, 2008
3 Imaging, Diagnosis, Prognosis are associated with younger patient age (13, 14). A readily available prognostic immunohistochemical surrogate, easily applied on formalin-fixed, paraffin-embedded biopsy tissues, would identify a cohort of breast cancer patients who may require more aggressive systemic therapy and who would be the most appropriate subjects for clinical trials specifically targeting the basal-like subtype. This study aims to compare the prognostic value of two proposed surrogate immunohistochemical panels used to identity basal-like breast cancers: the TNP and the five-marker Core Basal definitions. Using a regional series of >4,000 primary invasive breast cancers with fully annotated clinical data, this report investigates the association of these two immunohistochemical panels with patient outcome. Materials and Methods Patients and tissue microarrays. The study cohort consists of 4,046 female primary invasive tumors. All patients had been referred to the British Columbia Cancer Agency between 1986 and 1992 and have staging, pathology, treatment, and follow-up information. The median follow-up time was 12.5 years. During the study era, f75% of breast cancer patients in the province were referred; the nonreferred were generally elderly or treated by mastectomy without indications for adjuvant systemic therapy (15). In British Columbia, most patients were treated according to provincial guidelines developed and disseminated by the British Columbia Cancer Agency (15). These guidelines were based on age, tumor size, lymphovascular invasion, nodal status, and ER levels determined by dextran charcoal ligand binding assay (16). High risk was defined as node positive, or if node negative, presence of lymphovascular invasion, or tumor >2 cm and ER negative (<10 fmol/mg). Patients considered as clinical low risk at the time of diagnosis during the study era were not given any adjuvant systemic therapy. Table 1 summarizes the tumor characteristics and treatment regimens of the breast cancer patients in this retrospective study, most of which have been previously presented (17). The Vancouver Hospital ER laboratory retained single archival blocks from each patient. Slides from these blocks were stained with H&Eand reviewed by two pathologists to identify areas of invasive breast carcinoma. Tissue microarrays were constructed as previously described (17). A total of 17 tissue array blocks were built. This study was approved by the Clinical Research Ethics Board of the University of British Columbia and the British Columbia Cancer Agency. Immunohistochemistry and fluorescent in situ hybridization. Immumunohistochemistry for ER, PR, HER2, EGFR, and CK5/6 was done on each set of 17 formalin-fixed, paraffin-embedded tissue slides using the standard streptavidin-biotin complex method with 3,3 -diaminobenzidine chromogen. ER (Clone SP1, LabVision) antibody was used at 1:250 dilution with a 8-min microwave antigen retrieval in a 10 mmol/l (ph 6.0) citrate buffer. Ready-to-use PR (Clone 1E2, Ventana) antibody was used following the Ventana automated stainer standard CC1 protocol. EGFR staining was done using the EGFR pharmdx kit (DAKO) with an enzymatic antigen retrieval by proteinase K for 5 min. CK5/6 (Clone D5/ 16B4, Zymed Laboratories) antibody was used following the Ventana automated stainer mild CC1 protocol with 1:100 dilution. HER2 staining was done using HER2 (Clone SP3, LabVision) antibody at 1:100 dilution with heat-induced antigen retrieval using 0.05 mol/l Tris buffer (ph 10.0) heated to 95jC in a steamer for 30 min. For HER2 fluorescent in situ hybridization assay, slides were hybridized with probes to LSI Her-2/neu and CEP 17 with the PathVysion HER-2 DNA Probe Kit (Abbott Molecular, Inc.) according to the manufacturer s instructions, with modifications to the pretreatment and hybridization as previously described (18). Slides were counterstained with 4,6-diamidino-2-phenylindole and visualized on a Zeiss Axioplan epifluorescent microscope. Automated analysis of fluorescent in situ hybridization signals was done using a Metafer automated image acquisition and analysis system (Metasystems). The average copy number for each probe was determined and the amplification ratio was calculated as a ratio between the average copy per cell for HER2 and the average copy number for centromere 17. Biomarker expression from immunohistochemical assays were scored by two pathologists, blinded to the clinicopathologic characteristics and outcome of the breast tumors, using previously established and published criteria developed on other breast cancer cohorts. ER (17) and PR stains were considered positive if immunostaining was seen in >1% of tumor nuclei. EGFR and CK5/6 stains were considered positive if any (weak or strong) cytoplasmic and/or membranous invasive carcinoma cell staining was observed (9). For HER2 status, tumors were considered positive if scored as 3+ according to HercepTest criteria, and fluorescent in situ hybridization with amplification ratio z2.0 was used to segregate immunohistochemically equivocal (2+) results (19). All the stained tissue microarrays are digitally scanned and available for public access (username, basal4000; password, corebasal). 5 Definition of breast cancer biological subtypes by immunohistochemistry. The immunohistochemical surrogate (ER, PR, HER2, EGFR, and CK5/6) defining breast cancer subtypes has been previously published (9, 10). In this study, we use two classification schemes: the TNP and the five-biomarker method. Basal-like breast cancer is defined differently by the two schemes. Using the TNP method, basal-like is negative for all routinely tested biomarkers: ER, PR, and HER2 (ER-PR- HER2-), and this surrogate definition of basal-like is referred to as TNP in this article. Using the five-biomarker method, TNP becomes divided into two groups: (a) triple-negative cases (ER-PR-HER2-), which also positively express either EGFR or CK5/6, cases that are referred to as Core Basal in this article; and (b) five-marker negative phenotype (5NP), which is triple negative and furthermore expresses neither EGFR nor CK5/6. Thus, the 5NP cases represent those cases considered basallike by the TNP method but not by the Core Basal definition. Three other biological subtype definitions are common to both schemes: HER2+/ER-PR- subtype, luminal (ER+ and/or PR+, and HER2-), and luminal/her2+ (ER+ and/or PR+, and HER2+; Supplementary Table S1). Tumors expressing HER2 but negative for both ER and PR were defined as HER2+/ER-PR-. Tumors expressing HER2 and one of the luminal markers (ER or PR) were defined as luminal/her2+. Luminal/ HER2+ is not synonymous with the luminal B expression profile subtype because only 30% to 50% of luminal B tumors express HER2. Luminal includes all cases that expression profiling defines as luminal A, as well as those remaining luminal B tumors that do not express HER2. Biomarker information was considered uninterpretable in cases where the tissue core was lost during sectioning or processing, or contained <50 visible invasive breast carcinoma cells. Tumors missing any of ER, PR, or HER2 data are categorized as unassigned. The two classification schemes are described in Supplementary Table S1. Statistical analysis. All statistical analyses were carried out using SPSS 14.0 (SPSS, Inc.) and R Differences between breast cancer subtypes with regard to clinicopathologic characteristics were examined using m 2 tests. For survival analysis, breast cancer-specific survival (BCSS) was of primary interest. Survival time was calculated as the date of a woman s diagnosis of breast cancer until her date of death. Survival times were censored if the primary or underlying cause of death was not breast cancer, or if the patient was still alive on June 30, 2004 (the date when the outcome data were collected). Univariate survival curves were generated by the Kaplan-Meier method (20) and differences in survival among the breast cancer subtypes were assessed by the log-rank test (21). For multivariate analysis, we built Cox regression models (22) to estimate the adjusted hazard ratios of breast cancer subtypes with standard clinicopathologic variables: age at diagnosis, histologic grade, tumor size, lymphovascular invasion, and number of positive axillary lymph nodes as a percentage of the total number examined (23). Only Clin Cancer Res 2008;14(5) March 1,
4 Five Biomarkers Best Define Basal Breast Cancer Table 2. Clinicopathologic characteristics of the 4,046 breast cancer tumors Characteristic Luminal Luminal/HER2+ HER2+/ER-PR- Total n = 2,625 Total n = 222 Total n = 258 Age, y n (% within subtype) n (% within subtype) n (% within subtype) V (7.0) 21 (9.5) 37 (14.3) (18.1) 49 (22.1) 45 (17.4) (35.1) 78 (35.1) 112 (43.4) >65 1,044 (39.8) 74 (33.3) 64 (24.8) Grade n (% within subtype) n (% within subtype) n (% within subtype) (6.6) 4 (1.8) 2 (0.8) 2 1,244 (47.4) 56 (25.2) 53 (20.5) 3 1,082 (41.2) 155 (69.8) 196 (76) Unknown 125 (4.8) 7 (3.2) 7 (2.7) Tumor size, cm n (% within subtype) n (% within subtype) n (% within subtype) V2 1,455 (55.4) 90 (40.5) 105 (40.7) 2-5 1,041 (39.7) 118 (53.2) 127 (49.2) >5 106 (4.0) 13 (5.9) 20 (7.8) Unknown 23 (0.9) 1 (0.5) 6 (2.3) LVI n (% within subtype) n (% within subtype) n (% within subtype) Positive 1,100 (41.9) 133 (59.9) 137 (53.1) Negative 1,406 (53.6) 84 (37.8) 113 (43.8) Unknown 119 (4.5) 5 (2.3) 8 (3.1) Percentage of n (% within subtype) n (% within subtype) n (% within subtype) positive/total examined axillary lymph nodes (%) 0 1,412 (54.8) 90 (40.5) 109 (42.2) (22.0) 46 (20.7) 60 (23.3) > (19.5) 72 (32.4) 78 (30.2) NOTE: Subtypes are defined by the TNP and Core Basal method. Abbreviation: LVI, lymphovascular invasion. cases with information for all the covariates were included in the analysis. Smoothed plots of weighted Schoenfeld residuals were used to test proportional hazard assumptions (24). Separate Cox regression models were also built for the subsets of patients (a) receiving no adjuvant systemic therapy, to compare the prognostic values of the two basal-like subtype definitions for studying the natural history of breast cancer, and (b) receiving adjuvant chemotherapy, to estimate the additional prognostic value of EGFR and CK5/6 for defining the basallike subtype in this setting. To test the statistical significance of the additional biomarkers (EGFR and CK5/6) for defining the basal-like subtype, a likelihood ratio test (25, 26) of the differences between the nested Cox regression models was used. The null hypothesis was that the five-biomarker model did not describe BCSS differently than the three-biomarker model. Bootstrap resampling analyses (27) were carried out (10,000 iterations) to assess the adequacy of the Cox model hazard ratio confidence intervals. In this study, bootstrapping involved randomly sampling the data with replacement and repeating the Cox regression analyses to assess the hazard ratios. We found the bootstrap confidence intervals were in close agreement with the model-based estimates, yielding no evidence that the model was overfitted to the data. The purpose of this study was to validate findings from other studies and to test a relatively small number of prespecified hypotheses; accordingly, we did not perform multiple comparisons corrections. All tests were two-sided and P values <0.05 were considered statistically significant. The data were assembled to provide >80% power for testing hypotheses regarding the biomarkers in all patients combined, as well as for patient subgroups defined by the adjuvant therapies they received. Supplementary data. Supplementary Tables S1 and S2 and Supplementary Fig. S1A and S1B are available on our publication supplemental Web site. 7 Results In this series of 4,046 tumors, the percentage of positive expression among interpretable cases is 69.5% (2,791 of 4,015) for ER, 13.0% (504 of 3,865) for HER2, 51.2% (1,846 of 3,605) for PR, 13.3% (462 of 3,478) for EGFR, and 8.4% (287 of 3,400) for CK5/6. A total of 3,744 tumors with enough information for unambiguous immunohistochemical surrogate classification were defined into breast cancer biological subtypes according to the TNP and the Core Basal classification schemes, respectively. There were no statistically significant survival differences between the 302 unassigned tumors and the 3,744 classifiable tumors (log-rank P = 0.179). Among the cases with complete data for assignment by both schemes, 17% (639 of 3,744) were defined as basal-like breast cancers by the triple-negative definition, whereas 9.0% (336 of 3,744) were basal-like by the Core Basal definition (with the other 303 classified as 5NP). Clinicopathologic characteristics of breast cancer subtypes. The tumor characteristics of each breast cancer subtype are summarized in Table 2. With either classification scheme, the major breast cancer subtypes differ significantly by age, grade, tumor size, lymphovascular invasion, and percentage of positive over total dissected axillary lymph nodes. For both the TNP and the Core Basal classification, basal-like breast cancer is Clin Cancer Res 2008;14(5) March 1, 2008
5 Imaging, Diagnosis, Prognosis Table 2. Clinicopathologic characteristics of the 4,046 breast cancer tumors (Cont d) TNPmethod Core Basal method Basal (TNP) Basal (Core Basal) 5NP Unassigned Total n = 639 Total n = 336 Total n =303 Total n = 302 n (% within subtype) n (% within subtype) n (% within subtype) n (% within subtype) 115 (18.0) 71 (21.1) 44 (14.5) 23 (7.6) 149 (23.3) 79 (23.5) 70 (23.1) 48 (15.9) 209 (32.7) 109 (32.4) 100 (33.0) 115 (38.1) 166 (26.0) 77 (22.9) 89 (29.4) 116 (38.4) n (% within subtype) n (% within subtype) n (% within subtype) n (% within subtype) 12 (1.9) 1 (.3) 11 (3.6) 19 (6.3) 115 (18) 35 (10.4) 80 (26.4) 114 (37.7) 488 (76.4) 293 (87.2) 195 (64.4) 148 (49) 24 (3.8) 7 (2.1) 17 (5.6) 21 (7) n (% within subtype) n (% within subtype) n (% within subtype) n (% within subtype) 284 (44.4) 152 (45.2) 132 (43.6) 159 (52.6) 300 (46.9) 155 (46.1) 145 (47.9) 111 (36.8) 53 (8.3) 28 (8.3) 25 (8.3) 27 (8.9) 2 (0.3) 1 (.3) 1 (.3) 5 (1.7) n (% within subtype) n (% within subtype) n (% within subtype) n (% within subtype) 259 (40.5) 135 (40.1) 124 (40.9) 121 (40.1) 351 (54.9) 185 (55.1) 166 (54.8) 166 (55) 29 (4.5) 16 (4.8) 13 (4.3) 15 (5) n (% within subtype) n (% within subtype) n (% within subtype) n (% within subtype) 378 (59.2) 204 (60.7) 174 (57.4) 172 (57.0) 127 (19.9) 66 (19.6) 61 (20.1) 65 (21.5) 112 (17.5) 55 (16.4) 57 (18.8) 52 (17.2) associated with younger patient age, lower rates of lymphovascular invasion, and with the lowest percentage of positive axillary lymph node involvement. However, the two schemes do differ, with an even larger fraction of Core Basal cases being high grade (87% grade 3), and <40 years old (18.8%) versus 64.4% of 5NP cases that were grade 3, and 10.2% <40 years. This suggests that the Core Basal classification is identifying a subset of particularly high-risk patients. Breast cancer specific survival by immunohistochemical subtype. The breast cancer subtypes as defined by the surrogate immunopanels differ significantly in predicting breast cancer specific survival (Fig. 1). The HER2+/ER-PR- subtype has the worst breast cancer survival among the four subtypes. Comparing the survival probabilities between basal-like definitions, the 10-year breast cancer specific survival for TNP is 67% [95% confidence interval (95% CI), 63-70; Fig. 1A], but when the basal-like subtype is segregated into Core Basal and 5NP by adding EGFR and CK5/6 immunostaining information, the Core Basal group has significantly worse outcome, with an absolute 10% lower 10-year BCSS than 5NP (Fig. 1B). The breast cancer subtypes maintain significant independent prognostic value to predict breast cancer death in the Cox model, including the established prognostic factors (Table 3). Compared with luminal, which represents the most common subtype of breast cancers, TNP has a hazard ratio of 1.39 (95% C.I ) for breast cancer specific death. On the other hand, the Core Basal group has 1.62 times greater risk for breast cancer specific death (95% CI, ), whereas the 5NP group does not have statistically or clinically significant prognostic value (HR, 1.16; 95% CI, ; Table 3). The likelihood ratio test between the two Cox models is significant (P = ; Table 3). Because the hazard ratio between luminal and 5NP is not proportional across time, Cox regression analysis may overestimate or underestimate this significance. We ran multivariate analyses in these TNP tumors to test the significance of Core Basal association with outcome in this subset. Relative to 5NP, Core Basal has an estimated hazard ratio of 1.47 (95% CI, ) for breast cancer death (Table 4A). The likelihood ratio test is also significant. Therefore, in this cohort, relying on the three-biomarker classifier (ER, PR, and HER2) to define basallike tumors loses significant information to predict breast cancer outcome, compared with the five-marker panel incorporating EGFR and CK5/6. Prognostic values of breast cancer subtypes within treatment subsets. Among the Core Basal patients, 179 received no adjuvant systemic therapy, 48 were treated with anthracyclinebased chemotherapy (32 with doxorubicin/cyclophosphamide and 16 with fluorouracil/doxorubicin/cyclophosphamide), and 55 were treated with nonanthracycline-based chemotherapy (cyclophosphamide, methotrexate, and fluorouracil). Among the 5NP patients, 141 received no adjuvant systemic therapy, 58 received anthracycline-based chemotherapy (36 doxorubicin/cyclophosphamide and 22 fluorouracil/doxorubicin/cyclophosphamide), and 31 received nonanthracycline-based chemotherapy. In the no adjuvant systemic therapy subset, although Core Basal and 5NP were ER-negative, predominantly grade 3 tumors, most had neither nodal involvement nor lymphovascular invasion and half were <2 cm (Supplementary Table S2). The Core Basal patients who received no adjuvant systemic therapy (predominantly considered clinically low risk at the time) have 9% lower 10-year BCSS than similarly treated 5NP patients (Supplementary Fig. S1A). Clin Cancer Res 2008;14(5) March 1,
6 Five Biomarkers Best Define Basal Breast Cancer Fig. 1. A, univariable breast cancer ^ specific survival analysis of breast cancer subtypes defined by thetnp method using an immunohistochemical surrogate of HER2, ER, and PR. The log-rank P value between luminal/her2+ and luminal is ; between HER2+/ER-PR- and luminal, ; and between luminal/her2+ and HER2+/ER-PR-, B, univariable breast cancer ^ specific survival analysis of breast cancer subtypes defined by the Core Basal method using an immunohistochemical surrogate of HER2, ER, PR, EGFR, and CK5/6. Core Basal has a statistically significant worse survival than 5NP (log-rank P = ); Core Basal also has a similar survival rate as HER2+/ER-PR- group for the first 3 y (log-rank P = 0.087). For patients treated with anthracycline-based adjuvant chemotherapy (Fig. 2), the Core Basal patients have a significant 26% lower 10-year BCSS than equivalently treated 5NP patients (log-rank P = ). After adjusting for age, tumor size, grade, axillary node, and lymphovascular invasion status, the Core Basal group has a significantly worse survival, with a hazard ratio of 4.26 versus the 5NP cohort (95% CI, ; Table 4B). In this patient group, Core Basal status is the most significant prognosticator in the multivariable model, ahead of nodal involvement and tumor size. The likelihood ratio test is significant (P = ). On the other hand, among tumors receiving nonanthracycline-based chemotherapy (Supplementary Fig. S1B), outcomes were relatively poor with no statistically significant survival difference between Core Basal and 5NP. The tumor characteristics between nonanthracycline (cyclophosphamide, methotrexate, and fluorouracil) versus anthracycline (doxorubicin/ cyclophosphamide or fluorouracil/doxorubicin/cyclophosphamide) treated cohorts were similar (Supplementary Table S2); tumors treated with anthracyclines were mostly diagnosed between 1990 and Discussion Using a large regional population-based cohort, this study compared two previously established immunohistochemical surrogate panels that define breast cancer subtypes. Prognostic implications of breast cancer molecular subtypes have been described in several reports (1, 3, 8 10); however, to date, no studies have been this large (>3700 patients) nor have assessed breast cancer specific survival, stratified by adjuvant treatment, using the triple-negative versus five-biomarker Core Basal methods. The molecular subtyping of breast cancer is validated and shown to be an independent prognostic factor. We show that including positive markers (EGFR and cytokeratins 5/6) for the basal subtype results in a significantly better identification of a high-risk group, whose outcome more closely matches that expected by gene expression profiling (1 3, 5) than was achieved using a triple-negative (ER-PR-HER2-) definition. Our results from the multivariable Cox regression analyses strongly suggest that among the triple-negative cases, the poor prognosis is conferred almost entirely by the subset of tumors that are positive for EGFR or basal cytokeratins. Basal-like breast cancer has been suggested to be definable by negative ER, PR, and HER2 immunostaining (8, 28 30), a TNP that can often be extracted from existing clinical records; however, this definition has never been validated with microarray data. Our results provide evidence that this definition can easily be improved upon through the use of other immunostains already commonly used in surgical pathology laboratories. The prevalence of the TNP (17%) in our study is consistent with a recent report that assigned 281 of 1,726 cases (16.3%) as TNP (31). This study found that among TNP cases, a basal phenotype (defined using Clin Cancer Res 2008;14(5) March 1, 2008
7 Imaging, Diagnosis, Prognosis CK5/6 and CK14) in a concurrent report (32) by the same group was significantly prognostic within the node-negative subset, and further suggested that triple-negative and basal definitions are associated with good response to chemotherapy (although treatments were not randomized and information on chemotherapy regimens was not given). The specific Core Basal definition used here and based on previous independent series was not presented and therefore direct comparisons are difficult to make. Another study, using 375 stage II breast tumors treated with tamoxifen but not adjuvant chemotherapy, defined 48 tumors as basal-like on the basis of cytokeratin 5 or 14 immunostaining, and reported no significant survival differences among E R- negative tumors (33). The discrepancy is likely due to limited power and the different choice of surrogate biomarkers, as cytokeratin 14 has not been found by gene expression to be a marker for basal-like tumors. In our pure prognostic group of patients receiving no adjuvant systemic therapy, Core Basal (10-year BCSS 70%) and HER2+/ER- PR- (10-year BCSS 59%) subtypes are associated with significantly distinct breast cancer specific survival in univariable Kaplan-Meier analysis (log-rank P = ), with an adjusted hazard ratio of 0.74 (95% CI, ). Our results support that basal-like phenotype breast tumors, having a different natural history than HER2+/ER-PR-, display a clinically distinct outcome, as well as distinct clinical features such as high grade, node-negative progression, and higher prevalence in young patients. By adding EGFR and CK5/6 as positive markers, a significantly worse outcome group can be identified among triplenegative cases. The Core Basal definition is associated with even poorer breast cancer survival in the whole population-based cohort, and also in the anthracycline-based chemotherapy cohort, a generally high-risk group treated with similar regimens in contemporary practice. Poor outcome despite anthracycline treatment is concordant with a recent casecontrol study (47 basal cytokeratin-expressing breast cancers and 49 stage-matched but mainly ER+ controls; ref. 34). Other studies (8, 14, 35) have reported that the basal-like subtype is a potential candidate to respond well to chemotherapy. In a neoadjuvant study, basal-like tumors (defined by TNP) had higher rates (27%) of pathologic complete response to anthracycline-based neoadjuvant chemotherapy than luminal breast cancers (36). However, those triple-negative tumors, which did not have complete response, had the highest rate of relapse, potentially explaining the poor prognosis of basal-like tumors as a group despite aggressive chemotherapy. Our findings are compatible with a recent study done analyzing 823 patients from two clinical trials randomized to receive anthracyclines versus no adjuvant chemotherapy (37). In that study, a true basal group defined as HER2 negative, ER negative, and either EGFR or CK5/6 positive exhibited less benefit from anthracyclines than the group negative for all four of these markers. One limitation of our study is that our cohort derives from a regional population base. Adjuvant! is a computer software program that predicts breast cancer outcomes based on Surveillance, Epidemiology, and End-Results data and clinical trial meta-analyses to guide treatment decisions in clinical practice (38). Almost half of our data set was used in an earlier study confirming that, in the British Columbia population, Adjuvant! predictions are comparable with observed outcomes (16), supporting extrapolation of the conclusions drawn in the present study to North American populations. Table 3. Cox regression analysis to estimate the adjusted hazard ratios of breast cancer subtypes defined by TNP and Core Basal method, respectively, on 3,558 cases with sufficient information for all of the variables Variables Univariate analysis Multivariate analysis HR (95% CI) Nested Cox model HR (95% CI) Full Cox model HR (95% CI) Age, y vs V ( ) 0.73 ( ) 0.74 ( ) vs V ( ) 0.83 ( ) 0.84 ( ) >65 vs V ( ) 0.87 ( ) 0.89 ( ) Grade 3 vs (2 and 1) 2.11 ( ) 1.49 ( ) 1.47 ( ) Lymphovascular invasion Positive vs negative 2.28 ( ) 1.31 ( ) 1.32 ( ) Tumor size, cm 2-5 vs V ( ) 1.65 ( ) 1.65 ( ) >5 vs V ( ) 1.77 ( ) 1.77 ( ) Percentage of positive/dissected axillary lymph nodes 0-25 vs ( ) 1.62 ( ) 1.62 ( ) >25 vs ( ) 2.88 ( ) 2.89 ( ) Breast cancer subtype Luminal as reference Luminal/HER ( ) 1.41 ( ) 1.41 ( ) HER2+/ER-PR ( ) 1.88 ( ) 1.89 ( ) Unassigned 1.02 ( ) 1.12 ( ) 1.13 ( ) TNP 1.50 ( ) 1.39 ( ) Core Basal 1.77 ( ) 1.62 ( ) 5NP 1.22 ( ) 1.16 ( ) NOTE: Hazard ratios above 1.0 indicate poorer outcome. Likelihood ratio test of TNP (nested model) and Core Basal (full model) methods has a P value of Hazard ratios for individual clinicopathologic variables in univariable breast cancer specific survival listed for reference. Clin Cancer Res 2008;14(5) March 1,
8 Five Biomarkers Best Define Basal Breast Cancer Table 4. Cox regression analyses on basal (TNP) tumors A. Cox regression analysis on 575 basal (TNP) tumors with sufficient information for the clinicopathologic covariates: age, tumor size, grade, lymphovascular invasion, and percentage positive among total examined axillary lymph nodes. Likelihood ratio test, P = , df =1 Variables Hazard ratio (95% CI) Age, y vs V ( ) vs V ( ) >65 vs V ( ) Grade 3 vs (2 and 1) 1.31 ( ) Lymphovascular invasion Positive vs negative 1.72 ( ) Tumor size, cm 2-5 vs V ( ) >5 vs V ( ) Percentage of positive/total number of dissected axillary lymph nodes 0-25 vs ( ) >25 vs ( ) Breast cancer subtype Basal (Core Basal) vs 5NP 1.47 ( ) B. Cox regression analysis on the 95 basal (TNP) tumors treated with anthracycline-based (AC or FAC) adjuvant chemotherapy with sufficient information for the clinicopathologic covariates: age, tumor size, grade, lymphovascular invasion, and percentage positive among total examined axillary lymph nodes. Likelihood ratio test, P = , df =1 Variables Hazard ratio (95% CI) Age, y z50 vs < ( ) Grade 3 vs (2 and 1) 0.38 ( ) Lymphovascular invasion Positive vs negative 1.19 ( ) Tumor size, cm >2 vs V ( ) Percentage of positive/total number of dissected axillary lymph nodes 0-25 vs ( ) >25 vs ( ) Breast cancer subtype Basal (Core Basal) vs 5NP 4.26 ( ) In British Columbia, most patients were treated according to provincial guidelines developed and disseminated by the British Columbia Cancer Agency. Associations relying on nonrandomized treatment regimens (such as the apparent Fig. 2. Univariable breast cancer ^ specific analysis among106 TNP tumors receivinganthracycline-basedadjuvantchemotherapy regimen. Solidline, CoreBasal cases expressing EGFRor CK5/6. Dashedline, 5NP cases expressingnone of these markers. poor outcomes of Core Basal over 5NP tumors in the adjuvant anthracycline subset) are best considered hypothesis generating. Thus, our finding that the Core Basal definition may predict response of anthracycline-based adjuvant chemotherapies needs validation. Prospective clinical trial designs are clearly needed to investigate the benefit of different chemotherapy regimens in basal-like breast cancer. Use of a triple-negative definition is attractive in the design of such studies as it does not necessitate additional biomarker information. However, a major implication of our current study is that relying on a TNP definition of basal-like breast cancer will still identify a heterogeneous group with significant differences in survival, potentially obscuring important findings. In North American and European populations, f12% to 20% of breast cancer patients have basal-like gene expression profiles and/or a triple-negative immunophenotype (1, 3, 30, 31). Our results provide strong evidence to support the use of a five-biomarker surrogate (ER, PR, HER2, EGFR, and CK5/6) to define the basal-like subtype, a finding of immediate relevance to prognostication and clinical trial design. Drawing on readily available inexpensive diagnostic tools already in clinical use, this immunopanel provides a more specific definition of this aggressive form of breast cancer for which there is a particular need to improve therapeutic options. References 1. Perou CM, Sorlie T, Eisen MB, et al. Molecular portraits of human breast tumours. Nature 2000;406: 747 ^ SorlieT, Perou CM, Tibshirani R, et al. Gene expression patterns of breast carcinomas distinguish tumor subclasses with clinical implications. Proc Natl Acad Sci U S A 2001;98:10869^ SorlieT,Tibshirani R, Parker J, et al. Repeated observation of breast tumor subtypes in independent gene expression data sets. Proc Natl Acad Sci U S A 2003; 100:8418 ^ Hu Z, Fan C, Oh DS, et al. The molecular portraits of breast tumors are conserved across microarray platforms. BMC Genomics 2006;7: Sorlie T, Wang Y, Xiao C, et al. Distinct molecular mechanisms underlying clinically relevant subtypes of breast cancer: gene expression analyses across three different platforms. BMC Genomics 2006;7: Fan C, Oh DS,Wessels L, et al. Concordance among gene-expression-based predictors for breast cancer. N Engl JMed 2006;355:560^ Clin Cancer Res 2008;14(5) March 1, 2008
9 Imaging, Diagnosis, Prognosis 7. Slamon DJ, Leyland-Jones B, Shak S, et al. Use of chemotherapy plus a monoclonal antibody against HER2 for metastatic breast cancer that overexpresses HER2. N Engl JMed 2001;344:783^ Haffty BG, Yang Q, Reiss M, et al. Locoregional relapse and distant metastasis in conservatively managed triple negative early-stage breast cancer. J Clin Oncol 2006;24:5652^7. 9. NielsenTO, Hsu FD, Jensen K, et al. Immunohistochemical and clinical characterization of the basal-like subtype of invasive breast carcinoma. Clin Cancer Res 2004;10:5367 ^ Carey LA, Perou CM, Livasy CA, et al. Race, breast cancer subtypes, and survival in the Carolina Breast Cancer Study. JAMA 2006;295:2492^ Abd El-Rehim DM, Pinder SE, Paish CE, et al. Expression of luminal and basal cytokeratins in human breast carcinoma. JPathol 2004;203:661^ TurnerN,Tutt A, AshworthA. Hallmarksof BRCAness insporadic cancers. Nat Rev Cancer 2004;4:814^ Livasy CA, Karaca G, Nanda R, et al. Phenotypic evaluation of the basal-like subtype of invasive breast carcinoma. Mod Pathol 2006;19:264^ Rodriguez-Pinilla SM, Sarrio D, Honrado E, et al. Prognostic significance of basal-like phenotype and fascin expression in node-negative invasive breast carcinomas. Clin Cancer Res 2006;12:1533 ^ Olivotto A, Coldman AJ, Hislop TG, et al. Compliance with practice guidelines for node-negative breast cancer. J Clin Oncol 1997;15:216^ Olivotto IA, Bajdik CD, Ravdin PM, et al. Populationbased validation of the prognostic model ADJU- VANT! for early breast cancer. J Clin Oncol 2005;23: 2716 ^ Cheang MC,Treaba DO, Speers CH, et al. Immunohistochemical detection using the new rabbit monoclonal antibody SP1 of estrogen receptor in breast cancer is superior to mouse monoclonal antibody 1D5 in predicting survival. J Clin Oncol 2006;24: 5637^ Brown LA, Irving J, Parker R, et al. Amplification of EMSY, a novel oncogene on 11q13, in high grade ovarian surface epithelial carcinomas. Gynecol Oncol 2006;100:264 ^ Yaziji H, Goldstein LC, BarryTS, et al. HER-2 testing in breast cancer using parallel tissue-based methods. JAMA 2004;291:1972^ Bland JM, Altman DG. Survival probabilities (the Kaplan-Meier method). BMJ1998;317: Bland JM, Altman DG. The logrank test. BMJ 2004; 328: Cox DR, Oakes D. Analysis of survival data. London (England): Chapman & Hall; Truong PT, Berthelet E, LeeJ, Kader HA, Olivotto IA. The prognostic significance of the percentage of positive/dissected axillary lymph nodes in breast cancer recurrence and survival in patients with one to three positive axillary lymph nodes. Cancer 2005;103: 2006 ^ Grambsch P,TherneauT. Proportional hazards tests and diagnostics based on weighted residuals. Biometrika 1994;81:515^ Hosmer DW, Lemeshow S. Applied logistic regression. NewYork (NY): Wiley & Sons; Tableman M, KimJS. Survival analysis using S: analysis of time-to-event data. Boca Raton: Chapman & Hall/CRC; Efron B,Tibshirani RJ. An introduction to the bootstrap.chapman&hall; Brenton JD, Carey LA, Ahmed AA, Caldas C. Molecular classification and molecular forecasting of breast cancer: ready for clinical application? J Clin Oncol 2005;23:7350^ Jacquemier J, Padovani L, Rabayrol L, et al. Typical medullary breast carcinomas have a basal/myoepithelial phenotype. JPathol 2005;207:260^ Bauer KR, Brown M, Cress RD, Parise CA, Caggiano V. Descriptive analysis of estrogen receptor (ER)- negative, progesterone receptor (PR)-negative, and HER2-negative invasive breast cancer, the socalled triple-negative phenotype: a population-based study from the California cancer Registry. Cancer 2007;109:1721 ^ Rakha EA, El-Sayed ME, Green AR, LeeAH, Robertson JF, Ellis IO. Prognostic markers in triple-negative breast cancer. Cancer 2007;109:25^ Rakha EA, El-Rehim DA, Paish C, et al. Basal phenotype identifies a poor prognostic subgroup of breast cancer of clinical importance. Eur J Cancer 2006;42:3149 ^ Jumppanen M, Gruvberger-Saal S, Kauraniemi P, et al. Basal-like phenotype is not associated with patient survival in estrogen receptor negative breast cancers. Breast Cancer Res 2007;9:R Banerjee S, Reis-Filho JS, Ashley S, et al. Basal-like breast carcinomas: clinical outcome and response to chemotherapy. J Clin Pathol 2006;59:729^ Rouzier R, Perou CM, Symmans WF, et al. Breast cancer molecular subtypes respond differently to preoperative chemotherapy. Clin Cancer Res 2005;11: 5678^ Carey LA, Dees EC, Sawyer L, et al. The triple negative paradox: primary tumor chemosensitivity of breast cancer subtypes. Clin Cancer Res 2007;13: 2329 ^ Conforti R, BouletT,Tomasic G, et al. Breast cancer molecular subclassification and estrogen receptor expression to predict efficacy of adjuvant anthracyclines-based chemotherapy: a biomarker study from two randomized trials. Ann Oncol 2007;18:1477^ RavdinPM,SiminoffLA,DavisGJ,etal.Computer program to assist in making decisions about adjuvant therapy for women with early breast cancer. J Clin Oncol 2001;19:980^91. Clin Cancer Res 2008;14(5) March 1,
10 Basal-Like Breast Cancer Defined by Five Biomarkers Has Superior Prognostic Value than Triple-Negative Phenotype Maggie C.U. Cheang, David Voduc, Chris Bajdik, et al. Clin Cancer Res 2008;14: Updated version Access the most recent version of this article at: Cited articles Citing articles This article cites 34 articles, 15 of which you can access for free at: This article has been cited by 64 HighWire-hosted articles. Access the articles at: alerts Sign up to receive free -alerts related to this article or journal. Reprints and Subscriptions Permissions To order reprints of this article or to subscribe to the journal, contact the AACR Publications Department at To request permission to re-use all or part of this article, use this link Click on "Request Permissions" which will take you to the Copyright Clearance Center's (CCC) Rightslink site.
Ki67 Index, HER2 Status, and Prognosis of Patients With Luminal B Breast Cancer
 ARTICLE Ki67 Index, HER2 Status, and Prognosis of Patients With Breast Cancer Maggie C. U. Cheang, Stephen K. Chia, David Voduc, Dongxia Gao, Samuel Leung, Jacqueline Snider, Mark Watson, Sherri Davies,
ARTICLE Ki67 Index, HER2 Status, and Prognosis of Patients With Breast Cancer Maggie C. U. Cheang, Stephen K. Chia, David Voduc, Dongxia Gao, Samuel Leung, Jacqueline Snider, Mark Watson, Sherri Davies,
EGFR as paradoxical predictor of chemosensitivity and outcome among triple-negative breast cancer
 ONCOLOGY REPORTS 21: 413-417, 2009 413 EGFR as paradoxical predictor of chemosensitivity and outcome among triple-negative breast cancer HIROKO NOGI 1, TADASHI KOBAYASHI 2, MASAFUMI SUZUKI 3, ISAO TABEI
ONCOLOGY REPORTS 21: 413-417, 2009 413 EGFR as paradoxical predictor of chemosensitivity and outcome among triple-negative breast cancer HIROKO NOGI 1, TADASHI KOBAYASHI 2, MASAFUMI SUZUKI 3, ISAO TABEI
RNA preparation from extracted paraffin cores:
 Supplementary methods, Nielsen et al., A comparison of PAM50 intrinsic subtyping with immunohistochemistry and clinical prognostic factors in tamoxifen-treated estrogen receptor positive breast cancer.
Supplementary methods, Nielsen et al., A comparison of PAM50 intrinsic subtyping with immunohistochemistry and clinical prognostic factors in tamoxifen-treated estrogen receptor positive breast cancer.
J Clin Oncol 24: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 24 NUMBER 36 DECEMBER 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Locoregional Relapse and Distant Metastasis in Conservatively Managed Triple Negative Early-Stage Breast Cancer
VOLUME 24 NUMBER 36 DECEMBER 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Locoregional Relapse and Distant Metastasis in Conservatively Managed Triple Negative Early-Stage Breast Cancer
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Breast Cancer Subtypes and the Risk of Local and Regional Relapse
 VOLUME 28 NUMBER 10 APRIL 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Breast Cancer s and the Risk of Local and Regional Relapse K. David Voduc, Maggie C.U. Cheang, Scott Tyldesley,
VOLUME 28 NUMBER 10 APRIL 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Breast Cancer s and the Risk of Local and Regional Relapse K. David Voduc, Maggie C.U. Cheang, Scott Tyldesley,
Hormone receptor and Her2 neu (Her2) analysis
 ORIGINAL ARTICLE Impact of Triple Negative Phenotype on Breast Cancer Prognosis Henry G. Kaplan, MD* and Judith A. Malmgren, PhD à *Swedish Cancer Institute at Swedish Medical Center; HealthStat Consulting
ORIGINAL ARTICLE Impact of Triple Negative Phenotype on Breast Cancer Prognosis Henry G. Kaplan, MD* and Judith A. Malmgren, PhD à *Swedish Cancer Institute at Swedish Medical Center; HealthStat Consulting
The effect of delayed adjuvant chemotherapy on relapse of triplenegative
 Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
Immunohistochemical classification of breast tumours
 Immunohistochemical classification of breast tumours Workshop in Diagnostic Immunohistochemistry September 19 th - 21 th 2018 Anne-Vibeke Lænkholm Department of Surgical Pathology, Zealand University Hospital,
Immunohistochemical classification of breast tumours Workshop in Diagnostic Immunohistochemistry September 19 th - 21 th 2018 Anne-Vibeke Lænkholm Department of Surgical Pathology, Zealand University Hospital,
Triple Negative Breast Cancer
 Triple Negative Breast Cancer Prof. Dr. Pornchai O-charoenrat Division of Head-Neck & Breast Surgery Department of Surgery Faculty of Medicine Siriraj Hospital Breast Cancer Classification Traditional
Triple Negative Breast Cancer Prof. Dr. Pornchai O-charoenrat Division of Head-Neck & Breast Surgery Department of Surgery Faculty of Medicine Siriraj Hospital Breast Cancer Classification Traditional
J Clin Oncol 24: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 24 NUMBER 36 DECEMBER 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Immunohistochemical Detection Using the New Rabbit Monoclonal Antibody SP1 of Estrogen Receptor in Breast Cancer
VOLUME 24 NUMBER 36 DECEMBER 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Immunohistochemical Detection Using the New Rabbit Monoclonal Antibody SP1 of Estrogen Receptor in Breast Cancer
Basal phenotype: a powerful prognostic factor in small screen-detected invasive breast cancer with long-term follow-up ...
 21 ORIGINAL ARTICLE Basal phenotype: a powerful prognostic factor in small screen-detected invasive breast cancer with long-term follow-up A J Evans, E A Rakha, S E Pinder, A R Green, C Paish and I O Ellis...
21 ORIGINAL ARTICLE Basal phenotype: a powerful prognostic factor in small screen-detected invasive breast cancer with long-term follow-up A J Evans, E A Rakha, S E Pinder, A R Green, C Paish and I O Ellis...
Prevalence of molecular subtypes and prognosis of invasive breast cancer in north-east of Morocco: retrospective study
 BMC Research Notes This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Prevalence of molecular
BMC Research Notes This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Prevalence of molecular
Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer. Cheol Min Kang 2018/04/05
 Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer
 Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer Dr. HassanAli Al-Khirsani, MBChB, CABM, F.I.C.M.S AL-Sadder teaching hospital, oncology unit Dr. Nasser Ghaly Yousif, MBChB,G.P.
Clinico- Pathological Features And Out Come Of Triple Negative Breast Cancer Dr. HassanAli Al-Khirsani, MBChB, CABM, F.I.C.M.S AL-Sadder teaching hospital, oncology unit Dr. Nasser Ghaly Yousif, MBChB,G.P.
UK Interdisciplinary Breast Cancer Symposium. Should lobular phenotype be considered when deciding treatment? Michael J Kerin
 UK Interdisciplinary Breast Cancer Symposium Should lobular phenotype be considered when deciding treatment? Michael J Kerin Professor of Surgery National University of Ireland, Galway and Galway University
UK Interdisciplinary Breast Cancer Symposium Should lobular phenotype be considered when deciding treatment? Michael J Kerin Professor of Surgery National University of Ireland, Galway and Galway University
Clinical pathological and epidemiological study of triple negative breast cancer
 International Journal of Research in Medical Sciences Ajay A et al. Int J Res Med Sci. 217 Jun;5(6):2657-2661 www.msjonline.org pissn 232-71 eissn 232-12 Original Research Article DOI: http://dx.doi.org/1.1823/232-12.ijrms2172465
International Journal of Research in Medical Sciences Ajay A et al. Int J Res Med Sci. 217 Jun;5(6):2657-2661 www.msjonline.org pissn 232-71 eissn 232-12 Original Research Article DOI: http://dx.doi.org/1.1823/232-12.ijrms2172465
Question 1 A. ER-, PR-, HER+ B. ER+, PR+, HER2- C. ER-, PR+, HER2- D. ER-, PR-, HER2- E. ER-, PR+, HER2+
 Triple Negative Breast Cancer Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Question 1 The tumor depicted on the next slide
Triple Negative Breast Cancer Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Question 1 The tumor depicted on the next slide
Concordance among Gene-Expression Based Predictors for Breast Cancer
 The new england journal of medicine original article Concordance among Gene-Expression Based Predictors for Breast Cancer Cheng Fan, M.S., Daniel S. Oh, Ph.D., Lodewyk Wessels, Ph.D., Britta Weigelt, Ph.D.,
The new england journal of medicine original article Concordance among Gene-Expression Based Predictors for Breast Cancer Cheng Fan, M.S., Daniel S. Oh, Ph.D., Lodewyk Wessels, Ph.D., Britta Weigelt, Ph.D.,
Breast cancer Molecular subtypes and their clinicopathological characteristics amongst patients at the Aga Khan University hospital (Nairobi)
 The ANNALS of AFRICAN SURGERY www.sskenya.org Breast cancer Molecular subtypes and their clinicopathological characteristics amongst patients at the Aga Khan University hospital (Nairobi) Gakinya S.M.
The ANNALS of AFRICAN SURGERY www.sskenya.org Breast cancer Molecular subtypes and their clinicopathological characteristics amongst patients at the Aga Khan University hospital (Nairobi) Gakinya S.M.
Editorial Process: Submission:11/30/2017 Acceptance:01/04/2019
 RESEARCH ARTICLE Editorial Process: Submission:11/30/2017 Acceptance:01/04/2019 in Non-Metastatic Triple-Negative Breast Cancer O Al jarroudi*, A Zaimi, S A Brahmi, S Afqir Abstract Introduction: Triple-negative
RESEARCH ARTICLE Editorial Process: Submission:11/30/2017 Acceptance:01/04/2019 in Non-Metastatic Triple-Negative Breast Cancer O Al jarroudi*, A Zaimi, S A Brahmi, S Afqir Abstract Introduction: Triple-negative
CME. CK5 Is More Sensitive Than CK5/6 in Identifying the Basal-like Phenotype of Breast Carcinoma
 Anatomic Pathology / CK5 vs CK5/6 in Breast Carcinoma CK5 Is More Sensitive Than CK5/6 in Identifying the Basal-like Phenotype of Breast Carcinoma Rohit Bhargava, MD, 1 Sushil Beriwal, MD, 2 Kim McManus,
Anatomic Pathology / CK5 vs CK5/6 in Breast Carcinoma CK5 Is More Sensitive Than CK5/6 in Identifying the Basal-like Phenotype of Breast Carcinoma Rohit Bhargava, MD, 1 Sushil Beriwal, MD, 2 Kim McManus,
4/13/2010. Silverman, Buchanan Breast, 2003
 Tailoring Breast Cancer Treatment: Has Personalized Medicine Arrived? Judith Luce, M.D. San Francisco General Hospital Avon Comprehensive Breast Care Center Outline First, treatment of DCIS Sorting risk
Tailoring Breast Cancer Treatment: Has Personalized Medicine Arrived? Judith Luce, M.D. San Francisco General Hospital Avon Comprehensive Breast Care Center Outline First, treatment of DCIS Sorting risk
Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer
 Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Response to Paclitaxel in Node-positive Triple Negative Breast Cancer
 J Korean Surg Soc 2010;79:173-179 DOI: 10.4174/jkss.2010.79.3.173 원 저 Response to Paclitaxel in Node-positive Triple Negative Breast Cancer Department of Surgery, Kosin University College of Medicine,
J Korean Surg Soc 2010;79:173-179 DOI: 10.4174/jkss.2010.79.3.173 원 저 Response to Paclitaxel in Node-positive Triple Negative Breast Cancer Department of Surgery, Kosin University College of Medicine,
Breast cancer in elderly patients (70 years and older): The University of Tennessee Medical Center at Knoxville 10 year experience
 Breast cancer in elderly patients (70 years and older): The University of Tennessee Medical Center at Knoxville 10 year experience Curzon M, Curzon C, Heidel RE, Desai P, McLoughlin J, Panella T, Bell
Breast cancer in elderly patients (70 years and older): The University of Tennessee Medical Center at Knoxville 10 year experience Curzon M, Curzon C, Heidel RE, Desai P, McLoughlin J, Panella T, Bell
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva
 Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/55957 holds various files of this Leiden University dissertation Author: Dekker T.J.A. Title: Optimizing breast cancer survival models based on conventional
Cover Page The handle http://hdl.handle.net/1887/55957 holds various files of this Leiden University dissertation Author: Dekker T.J.A. Title: Optimizing breast cancer survival models based on conventional
RESEARCH ARTICLE. Abstract. Introduction
 DOI:http://dx.doi.org/10.7314/APJCP.2014.15.3.1187 Molecular Subtype of Breast Cancer, MVD and VEGF Expression RESEARCH ARTICLE Clinicopathologic Features of Breast Carcinomas Classified by Biomarkers
DOI:http://dx.doi.org/10.7314/APJCP.2014.15.3.1187 Molecular Subtype of Breast Cancer, MVD and VEGF Expression RESEARCH ARTICLE Clinicopathologic Features of Breast Carcinomas Classified by Biomarkers
Breast Cancer Outcomes as Defined by the Estrogen Receptor, Progesterone Receptor, and Human Growth Factor Receptor-2 in a Multi-ethnic Asian Country
 DOI 10.1007/s00268-015-3133-2 ORIGINAL SCIENTIFIC REPORT Breast Cancer Outcomes as Defined by the Estrogen Receptor, Progesterone Receptor, and Human Growth Factor Receptor-2 in a Multi-ethnic Asian Country
DOI 10.1007/s00268-015-3133-2 ORIGINAL SCIENTIFIC REPORT Breast Cancer Outcomes as Defined by the Estrogen Receptor, Progesterone Receptor, and Human Growth Factor Receptor-2 in a Multi-ethnic Asian Country
Table S2. Expression of PRMT7 in clinical breast carcinoma samples
 Table S2. Expression of PRMT7 in clinical breast carcinoma samples (All data were obtained from cancer microarray database Oncomine.) Analysis type* Analysis Class(number sampels) 1 2 3 4 Correlation (up/down)#
Table S2. Expression of PRMT7 in clinical breast carcinoma samples (All data were obtained from cancer microarray database Oncomine.) Analysis type* Analysis Class(number sampels) 1 2 3 4 Correlation (up/down)#
Contemporary Classification of Breast Cancer
 Contemporary Classification of Breast Cancer Laura C. Collins, M.D. Vice Chair of Anatomic Pathology Professor of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Outline
Contemporary Classification of Breast Cancer Laura C. Collins, M.D. Vice Chair of Anatomic Pathology Professor of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Outline
Local Recurrence and Distant Metastases after Breast Conservation Treatment in Women with Triple Negative Breast Cancer Subtype
 Local Recurrence and Distant Metastases after Breast Conservation Treatment in Women with Triple Negative Breast Cancer Subtype Amr Ghannam 1, Omnia Abd el-fattah 1 and Ayman El-Nemr 2 1 Clinical Oncology
Local Recurrence and Distant Metastases after Breast Conservation Treatment in Women with Triple Negative Breast Cancer Subtype Amr Ghannam 1, Omnia Abd el-fattah 1 and Ayman El-Nemr 2 1 Clinical Oncology
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY
 Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY Methodology The test is based on the reported 50-gene classifier algorithm originally named PAM50 and is performed on the ncounter Dx Analysis System
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY Methodology The test is based on the reported 50-gene classifier algorithm originally named PAM50 and is performed on the ncounter Dx Analysis System
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY
 Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY GENE EXPRESSION PROFILING WITH PROSIGNA What is Prosigna? Prosigna Breast Cancer Prognostic Gene Signature Assay is an FDA-approved assay which provides
Prosigna BREAST CANCER PROGNOSTIC GENE SIGNATURE ASSAY GENE EXPRESSION PROFILING WITH PROSIGNA What is Prosigna? Prosigna Breast Cancer Prognostic Gene Signature Assay is an FDA-approved assay which provides
CHARLES M. PEROU. The University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA
 The Oncologist Molecular Stratification of Triple-Negative Breast Cancers CHARLES M. PEROU The University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA Key Words. Triple-negative breast
The Oncologist Molecular Stratification of Triple-Negative Breast Cancers CHARLES M. PEROU The University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA Key Words. Triple-negative breast
Low ER+ Breast Cancer. Is This a Distinct Group? Nika C. Gloyeske, MD, David J. Dabbs, MD, and Rohit Bhargava, MD ABSTRACT
 Low ER+ Breast Cancer Is This a Distinct Group? Nika C. Gloyeske, MD, David J. Dabbs, MD, and Rohit Bhargava, MD From the Magee-Womens Hospital of University of Pittsburgh Medical Center, Pittsburgh, PA.
Low ER+ Breast Cancer Is This a Distinct Group? Nika C. Gloyeske, MD, David J. Dabbs, MD, and Rohit Bhargava, MD From the Magee-Womens Hospital of University of Pittsburgh Medical Center, Pittsburgh, PA.
SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER
 SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER Sunil Shrestha 1*, Ji Yuan Yang, Li Shuang and Deepika Dhakal Clinical School of Medicine, Yangtze University, Jingzhou, Hubei Province, PR. China Department
SYSTEMIC TREATMENT OF TRIPLE NEGATIVE BREAST CANCER Sunil Shrestha 1*, Ji Yuan Yang, Li Shuang and Deepika Dhakal Clinical School of Medicine, Yangtze University, Jingzhou, Hubei Province, PR. China Department
Immunohistochemical Analysis of ER, PR, Her2 and CK5/6 in Infiltrative Breast Carcinomas in Indian Patients
 Immunohistochemical Analysis of Infiltrative Breast Carcinomas in Indian Patients RESEARCH COMMUNICATION Immunohistochemical Analysis of ER, PR, Her2 and CK5/6 in Infiltrative Breast Carcinomas in Indian
Immunohistochemical Analysis of Infiltrative Breast Carcinomas in Indian Patients RESEARCH COMMUNICATION Immunohistochemical Analysis of ER, PR, Her2 and CK5/6 in Infiltrative Breast Carcinomas in Indian
SCIENCE CHINA Life Sciences
 SCIENCE CHINA Life Sciences RESEARCH PAPER April 2013 Vol.56 No.4: 335 340 doi: 10.1007/s11427-013-4435-y Risk factors of recurrence in small-sized, node negative breast cancer in young women: a retrospective
SCIENCE CHINA Life Sciences RESEARCH PAPER April 2013 Vol.56 No.4: 335 340 doi: 10.1007/s11427-013-4435-y Risk factors of recurrence in small-sized, node negative breast cancer in young women: a retrospective
Morphological and Molecular Typing of breast Cancer
 Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological
Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological
Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol
 Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
It is a malignancy originating from breast tissue
 59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
The Expression of Basal Cytokeratins in Breast Cancers
 Global Journal of Medical Research: C Microbiology and Pathology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: C Microbiology and Pathology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Characterization of immunohistochemical markers in triple negative breast carcinomas
 JBUON 2013; 18(4): 886-890 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Characterization of immunohistochemical markers in triple negative breast
JBUON 2013; 18(4): 886-890 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Characterization of immunohistochemical markers in triple negative breast
Breast cancer presents a major risk to American. Cancer recurrence and survival in patients with early-stage triple-negative breast cancer
 Original Research Cancer recurrence and survival in patients with early-stage triple-negative breast cancer Neal P. Christiansen, MD, 1 Lei Chen, MD, PhD, 2 James Gilmore, DPharm, 3 and Stephen Szabo,
Original Research Cancer recurrence and survival in patients with early-stage triple-negative breast cancer Neal P. Christiansen, MD, 1 Lei Chen, MD, PhD, 2 James Gilmore, DPharm, 3 and Stephen Szabo,
PMRT for N1 breast cancer :CONS. Won Park, M.D., Ph.D Department of Radiation Oncology Samsung Medical Center
 PMRT for N1 breast cancer :CONS Won Park, M.D., Ph.D Department of Radiation Oncology Samsung Medical Center DBCG 82 b & c Overgaard et al Radiot Oncol 2007 1152 pln(+), 8 or more nodes removed Systemic
PMRT for N1 breast cancer :CONS Won Park, M.D., Ph.D Department of Radiation Oncology Samsung Medical Center DBCG 82 b & c Overgaard et al Radiot Oncol 2007 1152 pln(+), 8 or more nodes removed Systemic
Dr. dr. Primariadewi R, SpPA(K)
 Curriculum Vitae Dr. dr. Primariadewi R, SpPA(K) Education : Medical Doctor from UKRIDA Doctoral Degree from Faculty of Medicine University of Indonesia Pathologist Specialist and Consultant from Faculty
Curriculum Vitae Dr. dr. Primariadewi R, SpPA(K) Education : Medical Doctor from UKRIDA Doctoral Degree from Faculty of Medicine University of Indonesia Pathologist Specialist and Consultant from Faculty
Health Disparities Advances in Breast Cancer Treatment. Jo Anne Zujewski April 27, 2009
 Health Disparities Advances in Breast Cancer Treatment Jo Anne Zujewski April 27, 2009 Disclaimer Breast Cancer Incidence 1994-2003 Breast Cancer Mortality 1994-2003 Access to Care Comorbidity Biology
Health Disparities Advances in Breast Cancer Treatment Jo Anne Zujewski April 27, 2009 Disclaimer Breast Cancer Incidence 1994-2003 Breast Cancer Mortality 1994-2003 Access to Care Comorbidity Biology
CLINICOPATHOLOGIC FEATURES AND MOLECULAR SUBTYPES OF BREAST CANCER IN FEZ-MEKNES REGION (MOROCCO): A STUDY OF 390 PATIENTS
 CLINICOPATHOLOGIC FEATURES AND MOLECULAR SUBTYPES OF BREAST CANCER IN FEZ-MEKNES REGION (MOROCCO): A STUDY OF 390 PATIENTS S. Chahbouni¹, A. Amarti 2, N. Hammas 3, L. Chbani 3, H. El fatemi 3 1 Department
CLINICOPATHOLOGIC FEATURES AND MOLECULAR SUBTYPES OF BREAST CANCER IN FEZ-MEKNES REGION (MOROCCO): A STUDY OF 390 PATIENTS S. Chahbouni¹, A. Amarti 2, N. Hammas 3, L. Chbani 3, H. El fatemi 3 1 Department
Risk Factors for Triple-Negative Breast Cancer in Women Under the Age of 45 Years
 1157 Risk Factors for Triple-Negative Breast Cancer in Women Under the Age of 45 Years Jessica M. Dolle, 1 Janet R. Daling, 1 Emily White, 1,3 Louise A. Brinton, 4 David R. Doody, 1 Peggy L. Porter, 2
1157 Risk Factors for Triple-Negative Breast Cancer in Women Under the Age of 45 Years Jessica M. Dolle, 1 Janet R. Daling, 1 Emily White, 1,3 Louise A. Brinton, 4 David R. Doody, 1 Peggy L. Porter, 2
Androgen Receptor Expression in Estrogen Receptor Negative Breast Cancer Immunohistochemical, Clinical, and Prognostic Associations
 Anatomic Pathology / ANDROGEN RECEPTOR IN BREAST CANCER Androgen Receptor Expression in Estrogen Receptor Negative Breast Cancer Immunohistochemical, Clinical, and Prognostic Associations S. Nicholas Agoff,
Anatomic Pathology / ANDROGEN RECEPTOR IN BREAST CANCER Androgen Receptor Expression in Estrogen Receptor Negative Breast Cancer Immunohistochemical, Clinical, and Prognostic Associations S. Nicholas Agoff,
Breast cancer: Molecular STAGING classification and testing. Korourian A : AP,CP ; MD,PHD(Molecular medicine)
 Breast cancer: Molecular STAGING classification and testing Korourian A : AP,CP ; MD,PHD(Molecular medicine) Breast Cancer Theory: Halsted Operative breast cancer is a local-regional disease The positive
Breast cancer: Molecular STAGING classification and testing Korourian A : AP,CP ; MD,PHD(Molecular medicine) Breast Cancer Theory: Halsted Operative breast cancer is a local-regional disease The positive
NIH Public Access Author Manuscript Cancer Epidemiol Biomarkers Prev. Author manuscript; available in PMC 2011 January 1.
 NIH Public Access Author Manuscript Published in final edited form as: Cancer Epidemiol Biomarkers Prev. 2010 January ; 19(1): 144 147. doi:10.1158/1055-9965.epi-09-0807. Feasibility Study for Collection
NIH Public Access Author Manuscript Published in final edited form as: Cancer Epidemiol Biomarkers Prev. 2010 January ; 19(1): 144 147. doi:10.1158/1055-9965.epi-09-0807. Feasibility Study for Collection
Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target?
 Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target? New Frontiers in Urologic Oncology Juan Chipollini, MD Clinical Fellow Department of Genitourinary Oncology Moffitt Cancer
Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target? New Frontiers in Urologic Oncology Juan Chipollini, MD Clinical Fellow Department of Genitourinary Oncology Moffitt Cancer
RESEARCH ARTICLE. Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India
 APJCP.2016.17.6.2995 RESEARCH ARTICLE Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India Dinesh Chandra Doval 1,2 *, P Suresh 1, Rupal Sinha 2, Saud Azam 2, Ullas Batra
APJCP.2016.17.6.2995 RESEARCH ARTICLE Eight Year Survival Analysis of Patients with Triple Negative Breast Cancer in India Dinesh Chandra Doval 1,2 *, P Suresh 1, Rupal Sinha 2, Saud Azam 2, Ullas Batra
Breast Cancer: Basic and Clinical Research
 Breast Cancer: Basic and Clinical Research Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Clinico-Pathological Characteristics of Triple
Breast Cancer: Basic and Clinical Research Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Clinico-Pathological Characteristics of Triple
Molecular classification of breast cancer implications for pathologists. Sarah E Pinder
 Molecular classification of breast cancer implications for pathologists Sarah E Pinder Courtesy of CW Elston Histological types Breast Cancer Special Types 17 morphological special types 25-30% of all
Molecular classification of breast cancer implications for pathologists Sarah E Pinder Courtesy of CW Elston Histological types Breast Cancer Special Types 17 morphological special types 25-30% of all
A new way of looking at breast cancer tumour biology
 A new way of looking at breast cancer tumour biology Contents Intrinsic subtypes of breast cancer 3 Gene expression assays 3 Basis of the Prosigna test 4 Information provided by Prosigna 5 The accuracy
A new way of looking at breast cancer tumour biology Contents Intrinsic subtypes of breast cancer 3 Gene expression assays 3 Basis of the Prosigna test 4 Information provided by Prosigna 5 The accuracy
Residual cancer burden in locally advanced breast cancer: a superior tool
 ABSTRACT Objectives Locally advanced breast cancer (LABC) poses a difficult clinical challenge with an overall poor long-term prognosis. The strength of the association between tumour characteristics,
ABSTRACT Objectives Locally advanced breast cancer (LABC) poses a difficult clinical challenge with an overall poor long-term prognosis. The strength of the association between tumour characteristics,
CLINICOPATHOLOGICAL FEATURES OF NONSPECIFIC INVASIVE BREAST CANCER ACCORDING TO ITS MOLECULAR SUBTYPES
 122 Experimental Oncology 38, 122 127, 16 (June) Exp Oncol 16 38, 2, 122 127 CLINICOPATHOLOGICAL FEATURES OF NONSPECIFIC INVASIVE BREAST CANCER ACCORDING TO ITS MOLECULAR SUBTYPES M. Zavyalova 1, 2, 3,
122 Experimental Oncology 38, 122 127, 16 (June) Exp Oncol 16 38, 2, 122 127 CLINICOPATHOLOGICAL FEATURES OF NONSPECIFIC INVASIVE BREAST CANCER ACCORDING TO ITS MOLECULAR SUBTYPES M. Zavyalova 1, 2, 3,
HEALTH CARE DISPARITIES. Bhuvana Ramaswamy MD MRCP The Ohio State University Comprehensive Cancer Center
 HEALTH CARE DISPARITIES Bhuvana Ramaswamy MD MRCP The Ohio State University Comprehensive Cancer Center Goals Understand the epidemiology of breast cancer Understand the broad management of breast cancer
HEALTH CARE DISPARITIES Bhuvana Ramaswamy MD MRCP The Ohio State University Comprehensive Cancer Center Goals Understand the epidemiology of breast cancer Understand the broad management of breast cancer
Molecular Characterization of Breast Cancer: The Clinical Significance
 Molecular Characterization of : The Clinical Significance Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine-Jacksonville
Molecular Characterization of : The Clinical Significance Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine-Jacksonville
Histological Type. Morphological and Molecular Typing of breast Cancer. Nottingham Tenovus Primary Breast Cancer Study. Survival (%) Ian Ellis
 Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Breast-Conserving Therapy for Triple-Negative Breast Cancer
 Research Original Investigation PACIFIC COAST SURGICAL ASSOCIATION Breast-Conserving Therapy for Triple-Negative Breast Cancer Alexandra Gangi, MD; Alice Chung, MD; James Mirocha, MS; Douglas Z. Liou,
Research Original Investigation PACIFIC COAST SURGICAL ASSOCIATION Breast-Conserving Therapy for Triple-Negative Breast Cancer Alexandra Gangi, MD; Alice Chung, MD; James Mirocha, MS; Douglas Z. Liou,
A Study to Evaluate the Effect of Neoadjuvant Chemotherapy on Hormonal and Her-2 Receptor Status in Carcinoma Breast
 Original Research Article A Study to Evaluate the Effect of Neoadjuvant Chemotherapy on Hormonal and Her-2 Receptor Status in Carcinoma Breast E. Rajesh Goud 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior
Original Research Article A Study to Evaluate the Effect of Neoadjuvant Chemotherapy on Hormonal and Her-2 Receptor Status in Carcinoma Breast E. Rajesh Goud 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior
Oncotype DX testing in node-positive disease
 Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
Estrogen Receptor, Progesterone Receptor, and Her-2/neu Oncogene Expression in Breast Cancers Among Bangladeshi Women
 Journal of Bangladesh College of Physicians and Surgeons Vol. 28, No. 3, September 2010 Estrogen Receptor, Progesterone Receptor, and Her-2/neu Oncogene Expression in Breast Cancers Among Bangladeshi Women
Journal of Bangladesh College of Physicians and Surgeons Vol. 28, No. 3, September 2010 Estrogen Receptor, Progesterone Receptor, and Her-2/neu Oncogene Expression in Breast Cancers Among Bangladeshi Women
FISH mcgh Karyotyping ISH RT-PCR. Expression arrays RNA. Tissue microarrays Protein arrays MS. Protein IHC
 Classification of Breast Cancer in the Molecular Era Susan J. Done University Health Network, Toronto Why classify? Prognosis Prediction of response to therapy Pathogenesis Invasive breast cancer can have
Classification of Breast Cancer in the Molecular Era Susan J. Done University Health Network, Toronto Why classify? Prognosis Prediction of response to therapy Pathogenesis Invasive breast cancer can have
Modern classification of breast cancer-should we stick with morphology or convert to molecular profiles?
 Modern classification of breast cancer-should we stick with morphology or convert to molecular profiles? Ian Ellis Professor of Cancer Pathology Molecular Medical Sciences University of Nottingham Dept
Modern classification of breast cancer-should we stick with morphology or convert to molecular profiles? Ian Ellis Professor of Cancer Pathology Molecular Medical Sciences University of Nottingham Dept
Retrospective analysis to determine the use of tissue genomic analysis to predict the risk of recurrence in early stage invasive breast cancer.
 Retrospective analysis to determine the use of tissue genomic analysis to predict the risk of recurrence in early stage invasive breast cancer. Goal of the study: 1.To assess whether patients at Truman
Retrospective analysis to determine the use of tissue genomic analysis to predict the risk of recurrence in early stage invasive breast cancer. Goal of the study: 1.To assess whether patients at Truman
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Supplementary Fig. 1: ATM is phosphorylated in HER2 breast cancer cell lines. (A) ATM is phosphorylated in SKBR3 cells depending on ATM and HER2
 Supplementary Fig. 1: ATM is phosphorylated in HER2 breast cancer cell lines. (A) ATM is phosphorylated in SKBR3 cells depending on ATM and HER2 activity. Upper panel: Representative histograms for FACS
Supplementary Fig. 1: ATM is phosphorylated in HER2 breast cancer cell lines. (A) ATM is phosphorylated in SKBR3 cells depending on ATM and HER2 activity. Upper panel: Representative histograms for FACS
Does HER2/neu overexpression in breast cancer influence adjuvant chemotherapy and hormonal therapy choices by Ontario physicians? A physician survey
 MYERS et al. ORIGINAL ARTICLE Does HER2/neu overexpression in breast cancer influence adjuvant chemotherapy and hormonal therapy choices by Ontario physicians? A physician survey J.A. Myers MD FRCPC, G.
MYERS et al. ORIGINAL ARTICLE Does HER2/neu overexpression in breast cancer influence adjuvant chemotherapy and hormonal therapy choices by Ontario physicians? A physician survey J.A. Myers MD FRCPC, G.
What to do after pcr in different subtypes?
 What to do after pcr in different subtypes? Luca Moscetti Breast Unit Università degli Studi di Modena e Reggio Emilia Policlinico di Modena, Italy Aims of neoadjuvant therapy in breast cancer Primary
What to do after pcr in different subtypes? Luca Moscetti Breast Unit Università degli Studi di Modena e Reggio Emilia Policlinico di Modena, Italy Aims of neoadjuvant therapy in breast cancer Primary
Breast Cancer Earlier Disease. Stefan Aebi Luzerner Kantonsspital
 Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Breast Cancer Earlier Disease Stefan Aebi Luzerner Kantonsspital stefan.aebi@onkologie.ch Switzerland Breast Cancer Earlier Disease Diagnosis and Prognosis Local Therapy Surgery Radiation therapy Adjuvant
Pathology Report Patient Companion Guide
 Pathology Report Patient Companion Guide Breast Cancer - Understanding Your Pathology Report Pathology Reports can be overwhelming. They contain scientific terms that are unfamiliar and might be a bit
Pathology Report Patient Companion Guide Breast Cancer - Understanding Your Pathology Report Pathology Reports can be overwhelming. They contain scientific terms that are unfamiliar and might be a bit
Introduction. Wilfred Truin 1 Rudi M. H. Roumen. Vivianne C. G. Tjan-Heijnen 2 Adri C. Voogd
 Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
Race is not a factor in overall survival in patients with triple negative breast cancer: a retrospective review
 Starlard-Davenport et al. SpringerPlus 2013, 2:516 a SpringerOpen Journal RESEARCH Open Access Race is not a factor in overall survival in patients with triple negative breast cancer: a retrospective review
Starlard-Davenport et al. SpringerPlus 2013, 2:516 a SpringerOpen Journal RESEARCH Open Access Race is not a factor in overall survival in patients with triple negative breast cancer: a retrospective review
Breast Cancer? Breast cancer is the most common. What s New in. Janet s Case
 Focus on CME at The University of Calgary What s New in Breast Cancer? Theresa Trotter, MD, FRCPC Breast cancer is the most common malignancy affecting women in Canada, accounting for almost a third of
Focus on CME at The University of Calgary What s New in Breast Cancer? Theresa Trotter, MD, FRCPC Breast cancer is the most common malignancy affecting women in Canada, accounting for almost a third of
30 years of progress in cancer research
 Breast Cancer Molecular Knowledge Integrated in Clinical Practice Personalized Medicine Laura J. Esserman UCSF Comprehensive Cancer Center Retreat Breast Cancer Management Advances 80-90s 1) Screening
Breast Cancer Molecular Knowledge Integrated in Clinical Practice Personalized Medicine Laura J. Esserman UCSF Comprehensive Cancer Center Retreat Breast Cancer Management Advances 80-90s 1) Screening
Immunohistochemical and Clinical Characterization of the Basal- Like Subtype of Invasive Breast Carcinoma
 Vol. 10, 5367 5374, August 15, 2004 Clinical Cancer Research 5367 Featured Article Immunohistochemical and Clinical Characterization of the Basal- Like Subtype of Invasive Breast Carcinoma Torsten O. Nielsen,
Vol. 10, 5367 5374, August 15, 2004 Clinical Cancer Research 5367 Featured Article Immunohistochemical and Clinical Characterization of the Basal- Like Subtype of Invasive Breast Carcinoma Torsten O. Nielsen,
Poly ADP-ribose Polymerase PARP Staining for Immunohistological Investigation of Primary Breast Cancer
 Showa Univ J Med Sci 25 2, 83 91, June 2013 Original Poly ADP-ribose Polymerase PARP Staining for Immunohistological Investigation of Primary Breast Cancer Genki TSUKUDA 1 2, Yuko DATE 1, Kunio ASONUMA
Showa Univ J Med Sci 25 2, 83 91, June 2013 Original Poly ADP-ribose Polymerase PARP Staining for Immunohistological Investigation of Primary Breast Cancer Genki TSUKUDA 1 2, Yuko DATE 1, Kunio ASONUMA
Identification of a basal-like subtype of breast ductal carcinoma in situ B
 Human Pathology (2007) 38, 197 204 www.elsevier.com/locate/humpath Original contribution Identification of a basal-like subtype of breast ductal carcinoma in situ B Chad A. Livasy MD a,d, *, Charles M.
Human Pathology (2007) 38, 197 204 www.elsevier.com/locate/humpath Original contribution Identification of a basal-like subtype of breast ductal carcinoma in situ B Chad A. Livasy MD a,d, *, Charles M.
Post Neoadjuvant therapy: issues in interpretation
 Post Neoadjuvant therapy: issues in interpretation Disclosure: Overview D Prognostic features in assessment of post treatment specimens: Tumor size Cellularity Grade Receptors LN Neoadjuvant chemotherapy:
Post Neoadjuvant therapy: issues in interpretation Disclosure: Overview D Prognostic features in assessment of post treatment specimens: Tumor size Cellularity Grade Receptors LN Neoadjuvant chemotherapy:
Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
 JBUON 2018; 23(4): 877-882 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
JBUON 2018; 23(4): 877-882 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Is adjuvant chemotherapy necessary for Luminal A-like breast cancer?
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine
 Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Key Words. Adjuvant therapy Breast cancer Taxanes Anthracyclines
 The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
The Oncologist Mayo Clinic Hematology/Oncology Reviews Adjuvant Therapy for Breast Cancer: Recommendations for Management Based on Consensus Review and Recent Clinical Trials BETTY A. MINCEY, a,b FRANCES
Neoadjuvant therapy a new pathway to registration?
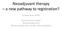 Neoadjuvant therapy a new pathway to registration? Graham Ross, FFPM Clinical Science Leader Roche Products Ltd Welwyn Garden City, UK (full time employee) Themes Neoadjuvant therapy Pathological Complete
Neoadjuvant therapy a new pathway to registration? Graham Ross, FFPM Clinical Science Leader Roche Products Ltd Welwyn Garden City, UK (full time employee) Themes Neoadjuvant therapy Pathological Complete
Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer
 Original Articles Jpn J Clin Oncol 2012;42(6)471 476 doi:10.1093/jjco/hys046 Advance Access Publication 3 April 2012 Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer Junnan Li,
Original Articles Jpn J Clin Oncol 2012;42(6)471 476 doi:10.1093/jjco/hys046 Advance Access Publication 3 April 2012 Clinical Features and Survival Analysis of T1mic, a, bn0m0 Breast Cancer Junnan Li,
Correspondence should be addressed to Alicia McMaster;
 Cancer Research Volume 2013, Article ID 308236, 5 pages http://dx.doi.org/10.1155/2013/308236 Research Article Taxpas: Epidemiological and Survival Data in Breast Cancer Patients Treated with a Docetaxel-Based
Cancer Research Volume 2013, Article ID 308236, 5 pages http://dx.doi.org/10.1155/2013/308236 Research Article Taxpas: Epidemiological and Survival Data in Breast Cancer Patients Treated with a Docetaxel-Based
Radiation Therapy for the Oncologist in Breast Cancer
 REVIEW ARTICLE Chonnam National University Medical School Sung-Ja Ahn, M.D. Adjuvant Tamoxifen with or without in Patients 70 Years of Age with Stage I ER-Positive Breast Cancer: Efficacy Outcomes (10
REVIEW ARTICLE Chonnam National University Medical School Sung-Ja Ahn, M.D. Adjuvant Tamoxifen with or without in Patients 70 Years of Age with Stage I ER-Positive Breast Cancer: Efficacy Outcomes (10
Prognostic implications of the intrinsic molecular subtypes in male breast cancer
 JBUON 2017; 22(2): 377-382 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic implications of the intrinsic molecular subtypes in male
JBUON 2017; 22(2): 377-382 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Prognostic implications of the intrinsic molecular subtypes in male
Prediction of Lymph Node Involvement in Patients with Breast Tumors Measuring 3 5 cm in a Middle-Income Setting: the Role of CancerMath
 DOI 10.1007/s00268-014-2752-3 BRIEF ORIGINAL SCIENTIFIC REPORT Prediction of Lymph Node Involvement in Patients with Breast Tumors Measuring 3 5 cm in a Middle-Income Setting: the Role of CancerMath E.
DOI 10.1007/s00268-014-2752-3 BRIEF ORIGINAL SCIENTIFIC REPORT Prediction of Lymph Node Involvement in Patients with Breast Tumors Measuring 3 5 cm in a Middle-Income Setting: the Role of CancerMath E.
Claudin-4 Expression in Triple Negative Breast Cancer: Correlation with Androgen Receptors and Ki-67 Expression
 Claudin-4 Expression in Triple Negative Breast Cancer: Correlation with Androgen Receptors and Ki-67 Expression Mona A. Abd-Elazeem, Marwa A. Abd- Elazeem Pathology department, Faculty of Medicine, Tanta
Claudin-4 Expression in Triple Negative Breast Cancer: Correlation with Androgen Receptors and Ki-67 Expression Mona A. Abd-Elazeem, Marwa A. Abd- Elazeem Pathology department, Faculty of Medicine, Tanta
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Comparison of Triple Negative Breast Cancer between Asian and Western Data Sets
 2010 IEEE International Conference on Bioinformatics and Biomedicine Workshops Comparison of Triple Negative Breast Cancer between Asian and Western Data Sets Lee H. Chen Bioinformatics and Biostatistics
2010 IEEE International Conference on Bioinformatics and Biomedicine Workshops Comparison of Triple Negative Breast Cancer between Asian and Western Data Sets Lee H. Chen Bioinformatics and Biostatistics
Radiotherapy and Conservative Surgery For Merkel Cell Carcinoma - The British Columbia Cancer Agency Experience
 Radiotherapy and Conservative Surgery For Merkel Cell Carcinoma - The British Columbia Cancer Agency Experience Poster No.: RO-0003 Congress: RANZCR FRO 2012 Type: Scientific Exhibit Authors: C. Harrington,
Radiotherapy and Conservative Surgery For Merkel Cell Carcinoma - The British Columbia Cancer Agency Experience Poster No.: RO-0003 Congress: RANZCR FRO 2012 Type: Scientific Exhibit Authors: C. Harrington,
Prognostic significance of stroma tumorinfiltrating lymphocytes according to molecular subtypes of breast cancer
 Prognostic significance of stroma tumorinfiltrating lymphocytes according to molecular subtypes of breast cancer Hee Jung Kwon, Nuri Jang, Min Hui Park, Young Kyung Bae Department of Pathology, Yeungnam
Prognostic significance of stroma tumorinfiltrating lymphocytes according to molecular subtypes of breast cancer Hee Jung Kwon, Nuri Jang, Min Hui Park, Young Kyung Bae Department of Pathology, Yeungnam
Priti Lal, MD, 1 Paulo A. Salazar, 1 Clifford A. Hudis, MD, 2 Marc Ladanyi, MD, 1 and Beiyun Chen, MD, PhD 1. Abstract
 Anatomic Pathology / DUAL- VS SINGLE-COLOR SCORING IN IMMUNOHISTOCHEMICAL AND FISH HER-2 TESTING HER-2 Testing in Breast Cancer Using Immunohistochemical Analysis and Fluorescence In Situ Hybridization
Anatomic Pathology / DUAL- VS SINGLE-COLOR SCORING IN IMMUNOHISTOCHEMICAL AND FISH HER-2 TESTING HER-2 Testing in Breast Cancer Using Immunohistochemical Analysis and Fluorescence In Situ Hybridization
