Influence of personal characteristics of individual women on sensitivity and specificity of mammography in the Million Women Study: cohort study
|
|
|
- Matilda Samantha Davidson
- 6 years ago
- Views:
Transcription
1 Influence of personal characteristics of individual women on sensitivity and specificity of mammography in the Million Women Study: cohort study Emily Banks, Gillian Reeves, Valerie Beral, Diana Bull, Barbara Crossley, Moya Simmonds, Elizabeth Hilton, Stephen Bailey, Nigel Barrett, Peter Briers, Ruth English, Alan Jackson, Elizabeth Kutt, Janet Lavelle, Linda Rockall, Matthew G Wallis, Mary Wilson, Julietta Patnick Abstract Objectives To examine how lifestyle, hormonal, and other factors influence the sensitivity and specificity of mammography. Methods Women recruited into the Million Women Study completed a questionnaire about various personal factors before routine mammographic screening. A sample of women aged years were followed for outcome of screening and incident breast cancer in the next 12 months. Sensitivity and specificity were calculated by using standard definitions, with adjustment for potential confounding factors. Results Breast cancer was diagnosed in 726 (0.6%) women, 629 in screen positive and 97 in screen negative women; 3885 (3.2%) were screen positive but had no subsequent diagnosis of breast cancer. Overall sensitivity was 86.6% and specificity was 96.8%. Three factors had an adverse effect on both measures: use of hormone replacement therapy (sensitivity: 83.0% (95% confidence interval 77.4% to 87.6%), 84.7% (73.9% to 91.6%), and 92.1% (87.6% to 95.0%); specificity: 96.8% (96.6% to 97.0%), 97.8% (97.5% to 98.0%), and 98.1% (98.0% to 98.2%), respectively, for current, past, and never use); previous breast surgery v no previous breast surgery (sensitivity: 83.5% (75.7% to 89.1%) v 89.4% (86.5% to 91.8%); specificity: 96.2% (95.8% to 96.5%) v 97.4% (97.3% to 97.5%), respectively); and body mass index < 25 v 25 (sensitivity: 85.7% (81.2% to 89.3%) v 91.0% (87.5% to 93.6%); specificity: 97.2% (97.0% to 97.3%) v 97.4% (97.3% to 97.6%), respectively). Neither sensitivity nor specificity varied significantly according to age, family history of breast cancer, parity, past oral contraceptive use, tubal ligation, physical activity, smoking, or alcohol consumption. Conclusions The efficiency, and possibly the effectiveness, of mammographic screening is lower in users of hormone replacement therapy, in women with previous breast surgery, and in thin women compared with other women. Introduction The effectiveness of mammographic screening for breast cancer depends on its ability to detect and to exclude the presence of breast cancer, measured as the sensitivity and specificity of mammography, respectively. Reliable data on how these measures vary between women are lacking. We examined how women s personal characteristics influence the sensitivity and specificity of mammography in a large cohort of women attending the UK NHS breast screening programme. 1 2 Methods Recruitment and definitions At the time of the study, all women aged 50 to 64 years in the United Kingdom who were registered with a general practitioner were invited to attend the NHS breast screening programme for routine mammography about once every three years. Women recruited into the Million Women Study (described in detail elsewhere 3 ) who attended screening at 10 breast screening units (Avon, Gloucestershire, Hereford-Worcester, Manchester, North Lancashire, Oxfordshire, Portsmouth, Warwickshire-Solihull- Coventry, West London, and West Sussex) from June 1996 to March 1998 were selected for a special study of the effect of hormone replacement therapy (HRT) on mammographic sensitivity and specificity. The women received a study questionnaire a few weeks before their screening appointment and returned the questionnaire at screening, also giving signed consent for follow up. The questionnaire contained items on lifestyle and sociodemographic factors, reproductive factors, past health, and use of HRT (see We defined the variables for these analyses, including use of HRT, according to what was reported on the recruitment questionnaire. Women who reported not using HRT and menstruating regularly or irregularly at baseline were defined as premenopausal or perimenopausal, respectively. Women whose periods had ceased either naturally or as the result of a bilateral oophorectomy were defined as postmenopausal. As described previously, 4 we also defined women aged 53 and over who had had a hysterectomy without oophorectomy and women aged 53 and over who had begun use of HRT before their natural menopause as postmenopausal. All women were asked to give the date that they completed the questionnaire and the date of screening was taken to be seven days after this date. (In a sample of 3002 women for whom the date of screening was recorded, the mean time between the date of completing the questionnaire and being screened was 7.5 days, with an interquartile range of 0-12 days.) Women were followed up for outcome of mammography (screen positive or screen negative) and for the diagnosis of incident breast cancer in the next 12 months through records from the screening centre and the NHS central register. Women were BMJ VOLUME AUGUST 2004 bmj.com page 1 of 6
2 Table 1 Overall outcome at mammographic screening Breast cancer* Outcome of mammography Yes No Total Screen positive Screen negative Total *Diagnosed at screening or in the 12 months after screening. defined as having screen positive or screen negative results if they were recalled or not recalled for further investigation, respectively, after initial mammography, according to screening centre records. Women for whom the films were technically inadequate and needed to be repeated were classified according to the results of their repeat mammogram. Women were defined as having breast cancer if they had a histologically confirmed breast cancer (invasive cancer or carcinoma in situ, ICD-10 (international classification of diseases, 10th revision) codes C50 or D05, respectively) at screening or in the 12 months after screening. Because they were no longer subject to routine surveillance we excluded from the analyses those women who were screen positive and did not have breast cancer diagnosed at the time but were asked to return for repeat screening earlier than the usual three year interval (n = 585). Analysis We analysed data from women aged years who did not report a history of cancer (except non-melanoma skin cancer) at recruitment. Of these, 6203 (5.1%) were aged 49 or 65 when they underwent screening but were close to their 50th or 65th birthday, as women are invited to screening according to their year of birth, rather than their exact age. We classified women into one of four groups: screen positive with breast cancer (that is, breast cancer was detected at screening); screen positive and no breast cancer; screen negative with breast cancer (that is, breast cancer was diagnosed in the 12 months after screening but was not detected at screening); and screen negative and no breast cancer. A total of 726 women were diagnosed with breast cancer either at screening or in the subsequent 12 months. Of these, 596 were recorded as having breast cancer detected at screening by the collaborating screening centres, and in 565 (95%) the cancer was histologically confirmed within three months of screening. The 130 remaining women were notified to us by the NHS central register as having breast cancer histologically confirmed within 12 months after screening. A detailed investigation of all available records for 88 of these women indicated that defining women with breast cancer histologically confirmed within three months after screening as having breast cancer detected at screening correctly classified around 99% of the study population. Hence, 33 women with breast cancer histologically confirmed within three months after screening notified only through the NHS central register were defined as having cancer detected at screening. Of the women we defined as having breast cancer not detected at screening, seven had been recalled and, at assessment, were not diagnosed with breast cancer at that screening episode; however, they subsequently had breast cancer diagnosed in the 12 months after mammography. We calculated sensitivity as the number of women who were screen positive and had breast cancer detected at screening divided by the total number of women with breast cancer (that is, with cancer detected at screening plus breast cancers not detected at screening but diagnosed in the first 12 months after screening). We calculated specificity as the number of women who were screen negative and did not have breast cancer divided by the total number of women with no breast cancer. We also calculated adjusted values for sensitivity and specificity with logistic regression, adjusting where appropriate for screening centre, age (50-54, 55-59, and years), whether they were likely to have attended screening through the programme before, 1 use of HRT/menopausal status (premenopausal or perimenopausal; postmenopausal and never used HRT; postmenopausal and currently using HRT; postmenopausal and Table 2 Sensitivity and specificity of breast cancer screening mammography by menopausal status and age among women who have never used hormone replacement therapy (HRT) Characteristic and outcome at mammography Menopausal status Premenopausal: Screen positive Screen negative Perimenopausal: Screen positive Screen negative Postmenopausal: Screen positive Screen negative Age (years) : Breast cancer* Sensitivity Specificity Yes No Crude Adjusted (95% CI) P value Crude Adjusted (95% CI) P value (51.5 to 94.5) (96.4 to 97.2) 0.6 < (66.6 to 97.3) (96.8 to 97.6) (83.7 to 95.1) (97.8 to 98.1) Screen positive Screen negative (64.3 to 97.8) (97.7 to 98.3) : Screen positive (72.9 to 93.1) (97.9 to 98.4) Screen negative : Screen positive Screen negative (82.6 to 95.8) (98.1 to 98.5) *Diagnosed at screening or in the 12 months after screening. Adjusted for age, screening centre, likelihood of previous NHS breast screening programme screening, body mass index, and previous breast surgery, when appropriate For heterogeneity. Postmenopausal women only page 2 of 6 BMJ VOLUME AUGUST 2004 bmj.com
3 Table 3 Sensitivity and specificity of breast cancer screening mammography by use of hormone replacement therapy (HRT) among postmenopausal women Use of HRT and outcome at mammography Current user: Breast cancer* Sensitivity Specificity Yes No Crude Adjusted (95% CI) P value Crude Adjusted (95% CI) P value Screen positive Screen negative (77.4 to 87.6) (96.6 to 97.0) Past user: Screen positive < (73.9 to 91.6) (97.5 to 98.0) Screen negative Never used: Screen positive Screen negative (87.6 to 95.0) (98.0 to 98.2) *Diagnosed at screening or in the 12 months after screening. Adjusted for age, likelihood of previous NHS breast screening programme screening, screening centre, body mass index, and previous breast surgery, when appropriate. For heterogeneity. previously used HRT; other or unknown), previous breast surgery (no, yes, unknown), and body mass index ( < 25, 25, unknown). The P values in the tables refer to the significance of the variable examined in the adjusted model with the likelihood ratio test. Results Overall, among women included in the analyses, 629 (0.51%) had cancer detected at screening, 97 (0.08%) were screen negative but had breast cancer diagnosed in the 12 months after screening, and 3885 (3.2%) were screen positive but did not have breast cancer (table 1). Overall sensitivity of mammography was 86.6% and specificity was 96.8%. Age, menopausal status, and use of HRT Among women who attend screening, age, menopausal status, use of HRT, and whether or not a woman has attended for screening before are closely related. Women are typically invited for their first routine screen between the age of 50 and 53 years, and they are more likely to be premenopausal at these ages than at older ages. Furthermore, the prevalence of use of HRT is higher in women in their early 50s, soon after the menopause, than at older ages. 5 To investigate the independent effects of age and menopausal status, we restricted analyses to women who had never used HRT and adjusted for screening history (table 2). 2 We found no significant effect of menopausal status on sensitivity (table 2), although specificity was significantly lower in premenopausal and perimenopausal compared with postmenopausal women (table 2). 1 We were able to examine screening outcome over a range of ages only among postmenopausal women; in these women neither sensitivity nor specificity was significantly related to age (table 2). 1 Among postmenopausal women, sensitivity varied significantly according to use of HRT (83.0% (95% confidence interval 77.4% to 87.6%), 84.7% (73.9% to 91.6%), and 92.1% (87.6% to 95.0%), respectively, for current, past, and never users, test for heterogeneity P = 0.01, table 3). Sensitivity did not vary significantly between current users of oestrogen only HRT (84.5%, 74.2% to 91.1%) and current users of oestrogenprogestogen HRT (84.1%, 76.9% to 89.4%). Specificity was significantly lower in current and past users compared with never users of HRT (96.8% (96.6% to 97.0%), 97.8% (97.5% to 98.0%), and 98.1% (98.0% to 98.2%), respectively, P < , table 3). 2 Specificity did not vary significantly between current users of oestrogen only HRT (96.9%, 96.6% to 97.2%) and current users of oestrogen-progestogen HRT (96.6%, 96.3% to 96.8%). Other personal characteristics We examined sensitivity and specificity in relation to nine additional factors: previous breast surgery for conditions other than cancer, family history of breast cancer, parity, use of oral contraceptives, tubal ligation, body mass index, exercise, smoking, and alcohol consumption. Two factors previous breast surgery and low body mass index seemed to have an adverse effect on both sensitivity and specificity. Women reporting previous breast surgery for a condition other than breast cancer had a sensitivity of 83.5% (75.7% to 89.1%) compared with 89.4% (86.5% to 91.8%) for women not reporting previous breast surgery (table 4, P = 0.06) and specificities of 96.2% (95.8% to 96.5%) v 97.4% (97.3% to 97.5%), respectively (table 4, P < ). Women with a body mass index < 25 had a sensitivity of 85.7% (81.2% to 89.3%) compared with 91.0% (87.5% to 93.6%) among women with a body mass index 25 (table 4, P = 0.03) and specificities of 97.2% (97.0% to 97.3%) and 97.4% (97.3% to 97.6%), respectively (table 4, P = 0.003). The seven other factors examined had no appreciable effect on either sensitivity or specificity (table 4). Discussion Joint consideration of the sensitivity and specificity To evaluate the impact of a particular factor on the effectiveness and efficiency of mammographic screening for breast cancer, its effect on both the proportion of cancers detected at screening (measured as sensitivity) and the proportion of women who are screen positive but do not have breast cancer (measured as 100% specificity) need to be considered together. About a tenth of the women recruited to the Million Women Study were selected for this special investigation of how characteristics of individual women influence mammographic sensitivity and specificity. The sample includes around 70% of the women screened at the 10 participating NHS breast screening centres during the recruitment period for this investigation (May 1996 to March 1998). 3 We prospectively gathered detailed data on sociodemographic, reproductive, lifestyle, and other factors immediately before screening, eliminating potential differential reporting of personal characteristics after the diagnosis of breast cancer. Questionnaire data on use of HRT have shown excellent agreement with data from general practice prescription records. 6 Our results support previous findings that current use of HRT reduces both the sensitivity and the specificity of mammography The adjusted sensitivity among current users (83.0%) is substantially lower than the value among women who have never used HRT (92.1%). Mammographic sensitivity did not differ significantly between current users of oestrogen only BMJ VOLUME AUGUST 2004 bmj.com page 3 of 6
4 Table 4 Sensitivity and specificity of breast cancer screening mammography according to various characteristics of women attending screening Characteristic and outcome of mammography Previous breast operation Breast cancer* Sensitivity Specificity Yes No Crude Adjusted (95% CI) P value Crude Adjusted 95% CI) P value Screen positive (86.5 to 91.8) (97.3 to 97.5) Screen negative < Screen positive (75.7 to 89.1) (95.8 to 96.5) Screen negative Mother or sister with breast cancer Screen positive Screen negative Screen positive Screen negative Parity Nulliparous: Screen positive Screen negative Parous: Screen positive Screen negative Previous use of oral contraceptives Screen positive Screen negative Screen positive Screen negative Tubal ligation Screen positive Screen negative Screen positive Screen negative Body mass index <25: Screen positive Screen negative : Screen positive Screen negative Regular strenuous exercise Screen positive Screen negative Screen positive Screen negative Current smoker Screen positive Screen negative Screen positive Screen negative Ever drinks alcohol Screen positive Screen negative Screen positive Screen negative (86.3 to 91.9) (97.2 to 97.4) (74.6 to 90.0) (96.9 to 97.5) (84.7 to 95.4) (96.9 to 97.4) (84.9 to 90.5) (97.2 to 97.4) (85.3 to 92.5) (97.1 to 97.4) (84.3 to 91.3) (97.2 to 97.4) (86.2 to 91.8) (97.2 to 97.4) (80.5 to 91.9) (97.1 to 97.5) (81.2 to 89.3) (97.0 to 97.3) (87.5 to 93.6) (97.3 to 97.6) (83.9 to 91.2) (97.1 to 97.4) (85.7 to 92.5) (97.2 to 97.5) (85.8 to 91.6) (97.2 to 97.4) (82.7 to 93.4) (97.0 to 97.4) (82.1 to 92.1) (97.1 to 97.5) (85.8 to 91.6) (97.2 to 97.4) *Diagnosed at screening or in the 12 months after screening. Adjusted for age, likelihood of previous NHS breast screening programme screening, screening centre, body mass index, previous breast surgery, menopausal status, and use of HRT, when appropriate. For heterogeneity. page 4 of 6 BMJ VOLUME AUGUST 2004 bmj.com
5 and of combined oestrogen-progestogen HRT. The specificity of mammography was also significantly lower among current users of HRT (and separately among current users of oestrogen only and of combined HRT) and among past users of HRT, compared with women who had never used HRT. Although previous studies have reported that mammographic sensitivity is lower among younger women, confounding with use of HRT and other factors can occur. After accounting for screening history, menopausal status, and use of HRT, we found that age did not have an independent effect on the sensitivity and specificity of mammography. 1 The age range examined here 50 to 64 years was, however, somewhat limited. Sensitivity did not vary significantly according to menopausal status, though specificity was significantly lower in premenopausal or perimenopausal compared with postmenopausal women. Our findings agree with previous results that showed no significant difference in mammographic sensitivity among women with and without a family history of breast cancer Previous studies have not reported on the effect of many other personal factors on overall mammographic effectiveness, and two of the nine factors examined here previous breast surgery for conditions other than cancer, and low body mass index seemed to have an adverse effect on both sensitivity and specificity. Women with a relatively high proportion of their mammograms occupied by radiologically dense tissue experience reduced sensitivity and specificity of mammographic screening for breast cancer compared with women with more radiolucent breasts Current use of HRT, having had a previous breast operation, and having a low body mass index are all associated with increased mammographic density, which is a plausible explanation for our findings Women using HRT and those who have had previous breast surgery may perhaps be under greater surveillance between screens, resulting in higher rates of breast cancer not detected at screening and hence apparently reduced mammographic sensitivity compared with other women. The relative risk of breast cancer not detected at screening among current compared with never users of HRT, however, is greater in the first year after mammography than in subsequent years. 22 This suggests that the reduced sensitivity observed here and by others is probably due to tumours being missed at mammography rather than increased surveillance in users. Implications The ultimate aim of mammographic screening is to reduce mortality from breast cancer in a cost effective way, and sensitivity and specificity are proxy measures of its effectiveness and efficiency. We measured sensitivity as the proportion of all breast cancers diagnosed either at screening or in the 12 months after screening that are detected by screening. This is a commonly used measure of mammographic sensitivity 7 and assumes that the breast cancers diagnosed in the first 12 months after a negative result at screening are present, but missed, at mammography, whereas some new breast cancers may well arise in the 12 months after mammography was performed. Nevertheless, it is generally thought that reduced mammographic sensitivity would lessen the benefit conferred by screening. Our results suggest that mammography may thus be less efficient, and possibly less effective at reducing mortality, in users of HRT, in women with previous breast surgery, and in thin women compared with other women. We thank the many women who completed questionnaires for this study. We are grateful to the staff at the collaborating breast screening units and at What is already known on this topic Evidence is limited on how the sensitivity and specificity of mammography vary between women What this study adds Sensitivity and specificity of breast cancer screening were reduced in users of hormone replacement therapy, in women who had had previous breast surgery for conditions other than breast cancer, and in thin women compared with other women Sensitivity and specificity did not vary significantly according to a woman s age, family history of breast cancer, parity, past oral contraceptive use, tubal ligation, physical activity, smoking, or alcohol consumption the Million Women Study coordinating centre for their valuable contribution to the study. Contributors: EB, GR, VB, and JP had the original idea for the study, with important input on practical aspects of study design from DB, BC, EH, and MS. EB and DB analysed the data and EB, GR, VB, and JP interpreted the data. SB, NB, PB, RE, AJ, EK, JL, LR, MGW, and MW contributed to local study design and conduct. All the authors participated in drafting the paper and gave final approval of the version to be published. EB, GR, VB, and DB are guarantors for the study Funding: The Million Women Study is supported by Cancer Research UK, the Medical Research Council, and the NHS breast screening programme. Competing interests: None declared. Ethical approval: The study was approved by the Anglia and Oxford multicentre research ethics committee. 1 Banks E, Reeves G, Beral V, Bull D, Crossley B, Simmonds M, et al. Predictors of outcome of mammography in the National Health Service breast screening programme. J Med Screen 2002;9: Banks E, Reeves G, Beral V, Bull D, Crossley B, Simmonds M, et al. Impact of use of hormone replacement therapy on false positive recall in the Million Women Study. BMJ 2004;328: Million Women Study Collaborative Group. The Million Women Study: design and characteristics of the study population. Breast Cancer Res 1999;1: Million Women Study Collaborators. Breast cancer and hormone-replacement therapy in the Million Women Study. Lancet 2003;362: Million Women Study Collaborators. Patterns of use of hormone replacement therapy in one million women in Britain, Br J Obstet Gynaecol 2002;109: Banks E, Beral V, Cameron R, Hogg A, Langley N, Barnes, et al. Agreement between general practice prescription data and self-reported use of hormone replacement therapy and treatment for various illnesses. J Epidemiol Biostatistics 2001;6: Banks E. Hormone replacement therapy and the sensitivity and specificity of breast cancer screening: a review. J Med Screen 2001;8: Chlebowski R, Hendrix S, Langer R, Stefanick ML, Gass M, Lane D, et al. Influence of estrogen plus progestin on breast cancer and mammography in healthy postmenopausal women. JAMA 2003;289: Crane CEB, Luke CG, Rogers JM, Playford PE, Roder DM. An analysis of factors associated with interval as opposed to screen-detected breast cancers, including hormone therapy and mammographic density. Breast 2002;11: Carney P, Miglioretti DL, Yankaskas BC, Kerlikowske K, Rosenberg R, Rutter CM, et al. Individual and combined effects of age, breast density and hormone replacement therapy use on the accuracy of mammography. Ann Intern Med 2003;138: Kerlikowske K, Carney P, Geller B, Mandelson MT, Taplin SH, Malvin K, et al. Performance of screening mammography among women with and without a first-degree relative with breast cancer. Ann Intern Med 2000;133: Schouten LJ, de Rijke JM, Schlangen JT, Verbeek ALM. Incidence of interval cancer. Lancet 1997;349: Rosenberg RD, Hunt WC, Williamson MR, Gilliland FD, Wiest PW, Kelsey CA, et al. Effects of age, breast density, ethnicity, and estrogen replacement therapy on screening mammographic sensitivity and cancer stage at diagnosis: review of 183,134 screening mammograms in Albuquerque, New Mexico. Radiology 1998;209: Porter P, El-Bastawissi A, Mandelson MT, Lin MG, Khalid N, Watney EA, et al. Breast cancer tumour characteristics as predictors of mammographic detection: comparison of interval and screen-detected cancers. J Natl Cancer Inst 1999;91: Ma L, Fishell E, Wright B, Hanna W, Allan S, Boyd NF. Case-control study of factors associated with failure to detect breast cancer by mammography [see comments]. JNatl Cancer Inst 1992;84: Kerlikowske K, Grady D, Barclay J, Sickles EA, Ernster V. Effect of age, breast density, and family history on the sensitivity of first screening mammography. JAMA 1996;276:33-8. BMJ VOLUME AUGUST 2004 bmj.com page 5 of 6
6 17 Wang H, Bjurstam N, Bjorndal H, Braaten A, Eriksen L, Skanne P, et al. Interval cancers in the Norwegian breast cancer screening program: frequency, characteristics and use of HRT. Int J Cancer 2001;94: Mandelson MT, Oestreicher N, Porter P, White D, Finder CA, Taplin SH, et al. Breast density as a predictor of mammographic detection: comparison of interval and screendetected cancers. J Natl Cancer Inst 2000;92: Sala E, Warren R, McCann J, Duffy S, Day N, Lucas LL. Mammographic parenchymal patterns and mode of detection: implications for the breast screening programme. J Med Screen 1998;5: Greendale GA, Reboussin BA, Sie A, Singh HR, Olson LK, Gatewood O, et al. Effects of estrogen and estrogen-progestin on mammographic parenchymal density. Ann Intern Med 1999;130: de Stavola BL, Gravelle IH, Wang DY, Allen DS, Bulbrook RD, Fentiman IS, et al. Relationship of mammographic parenchymal patterns with breast cancer risk factors and risk of breast cancer in a prospective study. Int J Epidemiol 1990;19: Beral V, Banks E, Reeves G, Green J, Gathani T, Bull D, et al. The effect of hormone replacement therapy on breast and other cancers. In: Critchley HOD, Beral V, Gebbie A, eds. Menopause and hormone replacement, proceedings of the forty seventh study group of the Royal College of Obstetricians and Gynaecologists. London: Royal College of Obstetricians and Gynaecologists (in press). (Accepted 6 July 2004) bmj.com 2004;329:477 Cancer Research UK Epidemiology Unit, Gibson Building, Radcliffe Infirmary, Oxford OX2 6HE Emily Banks deputy director Gillian Reeves statistical epidemiologist Valerie Beral director Diana Bull senior statistician Barbara Crossley chief data manager Moya Simmonds clinical coordinator Elizabeth Hilton clinical coordinator Breast Screening Service, Princess of Wales Community Hospital, Bromsgrove B61 0BB Stephen Bailey clinical director West of London Breast Screening Service, Charing Cross Hospital, London W6 8RF Nigel Barrett clinical director Gloucestershire Breast Screening Service, Linton House, Cheltenham GL53 7AS Peter Briers clinical director Breast Care Unit, Oxford Radcliffe Hospital NHS Trust, Churchill Hospital, Oxford OX3 7JH Ruth English clinical director Patricia Massey Breast Screening Unit, Queen Alexandra Hospital, Cosham, Portsmouth PO6 3LY Alan Jackson consultant radiologist Avon Breast Screening, Central Health Clinic, Tower Hill, Bristol BS2 0JD Elizabeth Kutt clinical director North Lancashire Breast Screening Service, Royal Lancaster Infirmary, Ashton Court, Lancaster LA1 4GG Janet Lavelle clinical director West Sussex Breast Screening Service, Worthing Hospital, Worthing BN11 2DH Linda Rockall clinical director Breast Screening Unit, Coventry and Warwick Hospital, Coventry CV1 4FH Matthew G Wallis clinical director Greater Manchester Breast Screening Service, Nightingale Centre, Withington Hospital, Manchester M20 0PT Mary Wilson clinical director NHS Breast Screening Programme, Manor House, Sheffield S11 9PS Julietta Patnick national coordinator Correspondence to: E Banks emily.banks@anu.edu.au page 6 of 6 BMJ VOLUME AUGUST 2004 bmj.com
General practice. Abstract. Subjects and methods. Introduction. examining the effect of use of oral contraceptives on mortality in the long term.
 Mortality associated with oral contraceptive use: 25 year follow up of cohort of 46 000 women from Royal College of General Practitioners oral contraception study Valerie Beral, Carol Hermon, Clifford
Mortality associated with oral contraceptive use: 25 year follow up of cohort of 46 000 women from Royal College of General Practitioners oral contraception study Valerie Beral, Carol Hermon, Clifford
Mammographic breast density may be the most undervalued
 Article Individual and Combined Effects of Age, Breast Density, and Hormone Replacement Therapy Use on the Accuracy of Screening Mammography Patricia A. Carney, PhD; Diana L. Miglioretti, PhD; Bonnie C.
Article Individual and Combined Effects of Age, Breast Density, and Hormone Replacement Therapy Use on the Accuracy of Screening Mammography Patricia A. Carney, PhD; Diana L. Miglioretti, PhD; Bonnie C.
Gallbladder disease and use of transdermal versus oral hormone replacement therapy in postmenopausal women: prospective cohort study
 Gallbladder disease and use of transdermal versus oral hormone replacement therapy in postmenopausal women: prospective cohort study Bette Liu, Valerie Beral, Angela Balkwill, Jane Green, Siân Sweetland,
Gallbladder disease and use of transdermal versus oral hormone replacement therapy in postmenopausal women: prospective cohort study Bette Liu, Valerie Beral, Angela Balkwill, Jane Green, Siân Sweetland,
Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol
 Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Risk factors for breast cancer: relevance to screening
 Journal of Epidemiology and Community Health, 1983, 37, 127-131 Risk factors for breast cancer: relevance to screening S W DUFFY,1 M MAUREEN ROBERTS,2 AND R A ELTON1 From the Medical Computing and Statistics
Journal of Epidemiology and Community Health, 1983, 37, 127-131 Risk factors for breast cancer: relevance to screening S W DUFFY,1 M MAUREEN ROBERTS,2 AND R A ELTON1 From the Medical Computing and Statistics
Breast Cancer Risk in Relation to the Interval Between Menopause and Starting Hormone Therapy
 DOI: 10.1093/jnci/djq527 The Author 2011. Published by Oxford University Press. Advance Access publication on January 28, 2011 This is an Open Access article distributed under the terms of the Creative
DOI: 10.1093/jnci/djq527 The Author 2011. Published by Oxford University Press. Advance Access publication on January 28, 2011 This is an Open Access article distributed under the terms of the Creative
Breast Density. Information for Health Professionals
 Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
Supplementary Table 4. Study characteristics and association between OC use and endometrial cancer incidence
 Supplementary Table 4. characteristics and association between OC use and endometrial cancer incidence a Details OR b 95% CI Covariates Region Case-control Parslov, 2000 (1) Danish women aged 25 49 yr
Supplementary Table 4. characteristics and association between OC use and endometrial cancer incidence a Details OR b 95% CI Covariates Region Case-control Parslov, 2000 (1) Danish women aged 25 49 yr
Downloaded from:
 Ellingjord-Dale, M; Vos, L; Tretli, S; Hofvind, S; Dos-Santos-Silva, I; Ursin, G (2017) Parity, hormones and breast cancer subtypes - results from a large nested case-control study in a national screening
Ellingjord-Dale, M; Vos, L; Tretli, S; Hofvind, S; Dos-Santos-Silva, I; Ursin, G (2017) Parity, hormones and breast cancer subtypes - results from a large nested case-control study in a national screening
Relationship between body mass index and length of hospital stay for gallbladder disease
 Journal of Public Health Vol. 30, No. 2, pp. 161 166 doi:10.1093/pubmed/fdn011 Advance Access Publication 27 February 2008 Relationship between body mass index and length of hospital stay for gallbladder
Journal of Public Health Vol. 30, No. 2, pp. 161 166 doi:10.1093/pubmed/fdn011 Advance Access Publication 27 February 2008 Relationship between body mass index and length of hospital stay for gallbladder
Use of research questionnaires in the NHS Bowel Cancer Screening Programme in England: impact on screening uptake
 Original Article Use of research questionnaires in the NHS Bowel Cancer Screening Programme in England: impact on screening uptake J Med Screen 20(4) 192 197! The Author(s) 2013 Reprints and permissions:
Original Article Use of research questionnaires in the NHS Bowel Cancer Screening Programme in England: impact on screening uptake J Med Screen 20(4) 192 197! The Author(s) 2013 Reprints and permissions:
Postmenopausal hormone therapy and cancer risk
 International Congress Series 1279 (2005) 133 140 www.ics-elsevier.com Postmenopausal hormone therapy and cancer risk P. Kenemans*, R.A. Verstraeten, R.H.M. Verheijen Department of Obstetrics and Gynaecology,
International Congress Series 1279 (2005) 133 140 www.ics-elsevier.com Postmenopausal hormone therapy and cancer risk P. Kenemans*, R.A. Verstraeten, R.H.M. Verheijen Department of Obstetrics and Gynaecology,
Patterns: Value as a Predictor of
 1103 C. P. Hinton E. J. Roebuck2 M. R. Williams3 R. W. Blarney3 J. Glaves R. I. Nicholson5 K. Griffiths5 Received July 24, 1984: accepted after revision January 17, 1985. 1 Department of Surgery, Frenchay
1103 C. P. Hinton E. J. Roebuck2 M. R. Williams3 R. W. Blarney3 J. Glaves R. I. Nicholson5 K. Griffiths5 Received July 24, 1984: accepted after revision January 17, 1985. 1 Department of Surgery, Frenchay
RESEARCH. Inequalities in reported use of breast and cervical screening in Great Britain: analysis of cross sectional survey data
 Inequalities in reported use of breast and cervical screening in Great Britain: analysis of cross sectional survey data Kath Moser, senior researcher, 1 Julietta Patnick, visiting professor, 1 director,
Inequalities in reported use of breast and cervical screening in Great Britain: analysis of cross sectional survey data Kath Moser, senior researcher, 1 Julietta Patnick, visiting professor, 1 director,
RESEARCH. Cancer incidence and mortality in relation to body mass index in the Million Women Study: cohort study
 Cancer incidence and mortality in relation to body mass index in the Million Women Study: cohort study Gillian K Reeves, statistical epidemiologist, 1 Kirstin Pirie, statistician, 1 Valerie Beral, director,
Cancer incidence and mortality in relation to body mass index in the Million Women Study: cohort study Gillian K Reeves, statistical epidemiologist, 1 Kirstin Pirie, statistician, 1 Valerie Beral, director,
Mammographic Density and the Risk and Detection of Breast Cancer
 The new england journal of medicine original article Mammographic Density and the Risk and Detection of Breast Cancer Norman F. Boyd, M.D., D.Sc., Helen Guo, M.Sc., Lisa J. Martin, Ph.D., Limei Sun, M.Sc.,
The new england journal of medicine original article Mammographic Density and the Risk and Detection of Breast Cancer Norman F. Boyd, M.D., D.Sc., Helen Guo, M.Sc., Lisa J. Martin, Ph.D., Limei Sun, M.Sc.,
Tamoxifen and Breast Density in Women at Increased Risk of Breast Cancer
 Tamoxifen and Breast Density in Women at Increased Risk of Breast Cancer Jack Cuzick, Jane Warwick, Elizabeth Pinney, Ruth M. L. Warren, Stephen W. Duffy Background: Although mammographic breast density
Tamoxifen and Breast Density in Women at Increased Risk of Breast Cancer Jack Cuzick, Jane Warwick, Elizabeth Pinney, Ruth M. L. Warren, Stephen W. Duffy Background: Although mammographic breast density
// Award Number: DAMD TITLE: Markers of Breast Cancer Risk in Women with Benign Breast Disease PRINCIPAL INVESTIGATOR:
 AD Award Number: DAMD17-00-1-0623 TITLE: Markers of Breast Cancer Risk in Women with Benign Breast Disease PRINCIPAL INVESTIGATOR: Margaret Mandelson, Ph.D. CONTRACTING ORGANIZATION: Group Health Cooperative
AD Award Number: DAMD17-00-1-0623 TITLE: Markers of Breast Cancer Risk in Women with Benign Breast Disease PRINCIPAL INVESTIGATOR: Margaret Mandelson, Ph.D. CONTRACTING ORGANIZATION: Group Health Cooperative
2. Studies of Cancer in Humans
 346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
This information explains the advice about familial breast cancer (breast cancer in the family) that is set out in NICE guideline CG164.
 Familial breast cancer (breast cancer in the family) Information for the public Published: 1 June 2013 nice.org.uk About this information NICE guidelines provide advice on the care and support that should
Familial breast cancer (breast cancer in the family) Information for the public Published: 1 June 2013 nice.org.uk About this information NICE guidelines provide advice on the care and support that should
IJC International Journal of Cancer
 IJC International Journal of Cancer Changes in mammographic density over time in breast cancer cases and women at high risk for breast cancer Meghan E. Work 1, Laura L. Reimers 1, Anne S. Quante 1,2,3,
IJC International Journal of Cancer Changes in mammographic density over time in breast cancer cases and women at high risk for breast cancer Meghan E. Work 1, Laura L. Reimers 1, Anne S. Quante 1,2,3,
Copyright, 1995, by the Massachusetts Medical Society
 Copyright, 1995, by the Massachusetts Medical Society Volume 332 JUNE 15, 1995 Number 24 THE USE OF ESTROGENS AND PROGESTINS AND THE RISK OF BREAST CANCER IN POSTMENOPAUSAL WOMEN GRAHAM A. COLDITZ, M.B.,
Copyright, 1995, by the Massachusetts Medical Society Volume 332 JUNE 15, 1995 Number 24 THE USE OF ESTROGENS AND PROGESTINS AND THE RISK OF BREAST CANCER IN POSTMENOPAUSAL WOMEN GRAHAM A. COLDITZ, M.B.,
NHS Breast Cancer Screening Programme.
 NHS Breast Cancer Screening Programme. Sadie Tattersall Health Promotion Officer Breast Cancer Screening Unit. Royal Lancaster Infirmary. Breast Cancer Prevalence in the UK. Breast cancer is the most commonly
NHS Breast Cancer Screening Programme. Sadie Tattersall Health Promotion Officer Breast Cancer Screening Unit. Royal Lancaster Infirmary. Breast Cancer Prevalence in the UK. Breast cancer is the most commonly
COMMENTARY: DATA ANALYSIS METHODS AND THE RELIABILITY OF ANALYTIC EPIDEMIOLOGIC RESEARCH. Ross L. Prentice. Fred Hutchinson Cancer Research Center
 COMMENTARY: DATA ANALYSIS METHODS AND THE RELIABILITY OF ANALYTIC EPIDEMIOLOGIC RESEARCH Ross L. Prentice Fred Hutchinson Cancer Research Center 1100 Fairview Avenue North, M3-A410, POB 19024, Seattle,
COMMENTARY: DATA ANALYSIS METHODS AND THE RELIABILITY OF ANALYTIC EPIDEMIOLOGIC RESEARCH Ross L. Prentice Fred Hutchinson Cancer Research Center 1100 Fairview Avenue North, M3-A410, POB 19024, Seattle,
Association of symptoms and interval breast cancers in the mammography-screening programme: population-based matched cohort study
 www.nature.com/bjc ARTICLE Epidemiology Association of symptoms and interval breast cancers in the mammography-screening programme: population-based matched cohort study Deependra Singh 1,, Joonas Miettinen
www.nature.com/bjc ARTICLE Epidemiology Association of symptoms and interval breast cancers in the mammography-screening programme: population-based matched cohort study Deependra Singh 1,, Joonas Miettinen
Breast Carcinoma In Situ: Risk Factors and Screening Patterns
 Breast Carcinoma In Situ: Risk Factors and Screening Patterns Elizabeth B. Claus, Meredith Stowe, Darryl Carter Background: Risk factors associated with invasive breast cancer are well documented, but
Breast Carcinoma In Situ: Risk Factors and Screening Patterns Elizabeth B. Claus, Meredith Stowe, Darryl Carter Background: Risk factors associated with invasive breast cancer are well documented, but
Rate of Breast Cancer Diagnoses among Postmenopausal Women with Self-Reported Breast Symptoms
 Rate of Diagnoses among Postmenopausal Women with Self-Reported Symptoms Erin J. Aiello, MPH, Diana S. M. Buist, PhD, MPH, Emily White, PhD, Deborah Seger, and Stephen H. Taplin, MD, MPH* Background: cancer
Rate of Diagnoses among Postmenopausal Women with Self-Reported Symptoms Erin J. Aiello, MPH, Diana S. M. Buist, PhD, MPH, Emily White, PhD, Deborah Seger, and Stephen H. Taplin, MD, MPH* Background: cancer
Strategies for data analysis: case-control studies
 Strategies for data analysis: case-control studies Gilda Piaggio UNDP/UNFPA/WHO/World Bank Special Programme of Research, Development and Research Training in Human Reproduction World Health Organization
Strategies for data analysis: case-control studies Gilda Piaggio UNDP/UNFPA/WHO/World Bank Special Programme of Research, Development and Research Training in Human Reproduction World Health Organization
Dense Breasts, Get Educated
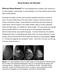 Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Information leaflet for women with a slightly increased risk of breast cancer. Breast cancer in the family
 Information leaflet for women with a slightly increased risk of breast cancer Breast cancer in the family Breast cancer in the family what does this mean? Breast cancer is the most common cancer affecting
Information leaflet for women with a slightly increased risk of breast cancer Breast cancer in the family Breast cancer in the family what does this mean? Breast cancer is the most common cancer affecting
The varying influence of socioeconomic deprivation on breast cancer screening uptake in London
 Journal of Public Health Vol. 38, No. 2, pp. 330 334 doi:10.1093/pubmed/fdv038 Advance Access Publication March 31, 2015 The varying influence of socioeconomic deprivation on breast cancer screening uptake
Journal of Public Health Vol. 38, No. 2, pp. 330 334 doi:10.1093/pubmed/fdv038 Advance Access Publication March 31, 2015 The varying influence of socioeconomic deprivation on breast cancer screening uptake
BR 1 Palpable breast lump
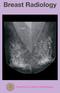 BR 1 Palpable breast lump Palpable breast lump in patient 40 years of age or above MMG +/- spot compression or digital breast tomosynthesis over palpable findings Suspicious or malignant findings (BIRADS
BR 1 Palpable breast lump Palpable breast lump in patient 40 years of age or above MMG +/- spot compression or digital breast tomosynthesis over palpable findings Suspicious or malignant findings (BIRADS
Supplementary Online Content
 Supplementary Online Content The Premenopausal Breast Cancer Collaborative Group. Association body mass index and age with premenopausal breast cancer risk in premenopausal women. JAMA Oncol. Published
Supplementary Online Content The Premenopausal Breast Cancer Collaborative Group. Association body mass index and age with premenopausal breast cancer risk in premenopausal women. JAMA Oncol. Published
Accuracy of Screening Mammography Interpretation by Characteristics of Radiologists
 Accuracy of Screening Mammography Interpretation by Characteristics of Radiologists William E. Barlow, Chen Chi, Patricia A. Carney, Stephen H. Taplin, Carl D Orsi, Gary Cutter, R. Edward Hendrick, Joann
Accuracy of Screening Mammography Interpretation by Characteristics of Radiologists William E. Barlow, Chen Chi, Patricia A. Carney, Stephen H. Taplin, Carl D Orsi, Gary Cutter, R. Edward Hendrick, Joann
Hormone replacement therapy and breast density after surgical menopause
 Hormone replacement therapy and breast density after surgical menopause Freya Schnabel*; Sarah Pivo; Esther Dubrovsky; Jennifer Chun; Shira Schwartz; Amber Guth; Deborah Axelrod Department of Surgery,
Hormone replacement therapy and breast density after surgical menopause Freya Schnabel*; Sarah Pivo; Esther Dubrovsky; Jennifer Chun; Shira Schwartz; Amber Guth; Deborah Axelrod Department of Surgery,
- The University of. - Student. Western Australia, Crawley, Western Australia
 Title: Is Step Down Assessment of Screen Detected Lesions as Safe as Workup at a Metropolitan Assessment Centre? Authors Author name Degrees/ Fellowships Position Institution Phone Email Jade P Hughes
Title: Is Step Down Assessment of Screen Detected Lesions as Safe as Workup at a Metropolitan Assessment Centre? Authors Author name Degrees/ Fellowships Position Institution Phone Email Jade P Hughes
In 1981, we published results from a case-control. study involving 881 cases and 863 controls. not associated with any substantial overall risk,
 Br. J. Cancer (1986) 54, 825-832 Menopausal oestrogens and breast cancer risk: An expanded case-control study L.A. Brinton, R. Hoover & J.F. Fraumeni, Jr Environmental Epidemiology Branch, National Cancer
Br. J. Cancer (1986) 54, 825-832 Menopausal oestrogens and breast cancer risk: An expanded case-control study L.A. Brinton, R. Hoover & J.F. Fraumeni, Jr Environmental Epidemiology Branch, National Cancer
Dietary soy intake and changes of mammographic density in premenopausal Chinese women
 Dietary soy intake and changes of mammographic density in premenopausal Chinese women 2010 WCRF International Conference, Nutrition, Physical Activity and Cancer Prevention: Current Challenges, New Horizons
Dietary soy intake and changes of mammographic density in premenopausal Chinese women 2010 WCRF International Conference, Nutrition, Physical Activity and Cancer Prevention: Current Challenges, New Horizons
Breast Density. Update 2018: Implications for Clinical Practice
 Breast Density Update 2018: Implications for Clinical Practice Matthew A. Stein, MD Assistant professor Breast Imaging Department of Radiology and Imaging Sciences University of Utah Health Disclosures
Breast Density Update 2018: Implications for Clinical Practice Matthew A. Stein, MD Assistant professor Breast Imaging Department of Radiology and Imaging Sciences University of Utah Health Disclosures
Dr Robin Wilson, The Royal Marsden
 Screening: State of the Art High risk and dense breasts Robin Wilson Smart Breast Screening? 1 in 8 women in the will get breast cancer 8 in 9 will not 55% of breast cancers are not screen detected One
Screening: State of the Art High risk and dense breasts Robin Wilson Smart Breast Screening? 1 in 8 women in the will get breast cancer 8 in 9 will not 55% of breast cancers are not screen detected One
BRCA genes and inherited breast and ovarian cancer. Information for patients
 BRCA genes and inherited breast and ovarian cancer Information for patients This booklet has been written for people who have a personal or family history of breast and/or ovarian cancer that could be
BRCA genes and inherited breast and ovarian cancer Information for patients This booklet has been written for people who have a personal or family history of breast and/or ovarian cancer that could be
Current Strategies in the Detection of Breast Cancer. Karla Kerlikowske, M.D. Professor of Medicine & Epidemiology and Biostatistics, UCSF
 Current Strategies in the Detection of Breast Cancer Karla Kerlikowske, M.D. Professor of Medicine & Epidemiology and Biostatistics, UCSF Outline ν Screening Film Mammography ν Film ν Digital ν Screening
Current Strategies in the Detection of Breast Cancer Karla Kerlikowske, M.D. Professor of Medicine & Epidemiology and Biostatistics, UCSF Outline ν Screening Film Mammography ν Film ν Digital ν Screening
Hormone Replacement Therapy (HRT) Benefits & Risks - The Facts
 Hormone Replacement Therapy (HRT) Benefits & Risks - The Facts HRT is a prescription only treatment that replaces some of the lost oestrogen and progesterone hormones which occur during menopause. It can
Hormone Replacement Therapy (HRT) Benefits & Risks - The Facts HRT is a prescription only treatment that replaces some of the lost oestrogen and progesterone hormones which occur during menopause. It can
Does Hysterectomy Lead to Weight Gain or Does Overweight Lead to Hysterectomy?
 Dr Janneke BERECKI D Fitzgerald, J Berecki, R Hockey and A Dobson 1 1 School of Population Health, Faculty of Health Sciences, University of Queensland, Herston, QLD, Australia Does Hysterectomy Lead to
Dr Janneke BERECKI D Fitzgerald, J Berecki, R Hockey and A Dobson 1 1 School of Population Health, Faculty of Health Sciences, University of Queensland, Herston, QLD, Australia Does Hysterectomy Lead to
Prediction Model For Risk Of Breast Cancer Considering Interaction Between The Risk Factors
 INTERNATIONAL JOURNAL OF SCIENTIFIC & TECHNOLOGY RESEARCH VOLUME, ISSUE 0, SEPTEMBER 01 ISSN 81 Prediction Model For Risk Of Breast Cancer Considering Interaction Between The Risk Factors Nabila Al Balushi
INTERNATIONAL JOURNAL OF SCIENTIFIC & TECHNOLOGY RESEARCH VOLUME, ISSUE 0, SEPTEMBER 01 ISSN 81 Prediction Model For Risk Of Breast Cancer Considering Interaction Between The Risk Factors Nabila Al Balushi
Breast density: imaging, risks and recommendations
 Breast density: imaging, risks and recommendations Maureen Baxter, MD Radiologist Director of Ruth J. Spear Breast Center Providence St. Vincent Medical Center Alison Conlin, MD/MPH Medical Oncologist
Breast density: imaging, risks and recommendations Maureen Baxter, MD Radiologist Director of Ruth J. Spear Breast Center Providence St. Vincent Medical Center Alison Conlin, MD/MPH Medical Oncologist
Modifiers of Cancer Risk in BRCA1 and BRCA2 Mutation Carriers: A Systematic Review and Meta-Analysis
 DOI:10.1093/jnci/dju091 First published online May 14, 2014 The Author 2014. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com. Review
DOI:10.1093/jnci/dju091 First published online May 14, 2014 The Author 2014. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com. Review
RESEARCH. What is already known on this topic. What this study adds
 Risks of ovarian, breast, and corpus uteri cancer in women treated with assisted reproductive technology in Great Britain, 1991-2010: data linkage study including 2.2 million person years of observation
Risks of ovarian, breast, and corpus uteri cancer in women treated with assisted reproductive technology in Great Britain, 1991-2010: data linkage study including 2.2 million person years of observation
Effect of NHS breast screening programme on mortality from breast cancer in England and Wales, : comparison of observed with predicted mortality
 Effect of NHS breast screening programme on mortality from breast cancer in England and Wales, 1990-8: comparison of observed with predicted mortality R G Blanks, S M Moss, C E McGahan, M J Quinn, P J
Effect of NHS breast screening programme on mortality from breast cancer in England and Wales, 1990-8: comparison of observed with predicted mortality R G Blanks, S M Moss, C E McGahan, M J Quinn, P J
Factors Influencing Smoking Behavior Among Adolescents
 RESEARCH COMMUNICATION Factors Influencing Smoking Behavior Among Adolescents Urmi Sen 1, Arindam Basu 2 Abstract Objective To study the impact of tobacco advertisements and other social factors on the
RESEARCH COMMUNICATION Factors Influencing Smoking Behavior Among Adolescents Urmi Sen 1, Arindam Basu 2 Abstract Objective To study the impact of tobacco advertisements and other social factors on the
RESEARCH. Body mass index and risk of liver cirrhosis in middle aged UK women: prospective study
 Body mass index and risk of liver cirrhosis in middle aged UK women: prospective study Bette Liu, senior research fellow Angela Balkwill, statistical programmer Gillian Reeves, statistical epidemiologist
Body mass index and risk of liver cirrhosis in middle aged UK women: prospective study Bette Liu, senior research fellow Angela Balkwill, statistical programmer Gillian Reeves, statistical epidemiologist
Temporal trends in the incidence of molecular subtypes of breast cancer. Jonine D. Figueroa, Ph.D., M.P.H.
 Temporal trends in the incidence of molecular subtypes of breast cancer Jonine D. Figueroa, Ph.D., M.P.H. Epidemiology: Health data science Study of the distribution and determinants of health and disease
Temporal trends in the incidence of molecular subtypes of breast cancer Jonine D. Figueroa, Ph.D., M.P.H. Epidemiology: Health data science Study of the distribution and determinants of health and disease
A literature review examining the association between the duration of hormone replacement therapy (HRT) and the risk of breast cancer in women
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A literature review examining the association between the duration of hormone replacement therapy (HRT)
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A literature review examining the association between the duration of hormone replacement therapy (HRT)
Relationship Between Mammographic Density and Breast Cancer Death in the Breast Cancer Surveillance Consortium
 DOI:10.1093/jnci/djs327 Published by Oxford University Press 2012. Article Relationship Between Mammographic Density and Breast Cancer Death in the Breast Cancer Surveillance Consortium Gretchen L. Gierach,
DOI:10.1093/jnci/djs327 Published by Oxford University Press 2012. Article Relationship Between Mammographic Density and Breast Cancer Death in the Breast Cancer Surveillance Consortium Gretchen L. Gierach,
Reproductive and Hormonal Factors Associated with Fatty or Dense Breast Patterns among Korean Women
 breast cancer risk is thought to be increased by 2 to 5-fold in women with dense breasts [3,4]. Although controversies remain in choosing the precise method of measuring breast density in comparisons between
breast cancer risk is thought to be increased by 2 to 5-fold in women with dense breasts [3,4]. Although controversies remain in choosing the precise method of measuring breast density in comparisons between
Breast Cancer Characteristics Associated With Digital Versus Film-Screen Mammography for Screen-Detected and Interval Cancers
 Women s Imaging Original Research Henderson et al. Digital Versus Film-Screen Mammography Women s Imaging Original Research Louise M. Henderson 1 Diana L. Miglioretti 2 Karla Kerlikowske 3 Karen J. Wernli
Women s Imaging Original Research Henderson et al. Digital Versus Film-Screen Mammography Women s Imaging Original Research Louise M. Henderson 1 Diana L. Miglioretti 2 Karla Kerlikowske 3 Karen J. Wernli
Breast Cancer Risk Factors 8/3/2014
 Breast Cancer Screening: Changing Philosophies in Educating Women and Teens Courtney Benedict CNM MSN Session Objectives Explain the rationale for initiation and frequency of clinical breast exams to clients
Breast Cancer Screening: Changing Philosophies in Educating Women and Teens Courtney Benedict CNM MSN Session Objectives Explain the rationale for initiation and frequency of clinical breast exams to clients
Cite this article as: BMJ, doi: /bmj f (published 8 March 2005)
 Cite this article as: BMJ, doi:10.1136/bmj.38398.469479.8f (published 8 March 2005) Model of outcomes of screening mammography: information to support informed choices Alexandra Barratt, Kirsten Howard,
Cite this article as: BMJ, doi:10.1136/bmj.38398.469479.8f (published 8 March 2005) Model of outcomes of screening mammography: information to support informed choices Alexandra Barratt, Kirsten Howard,
ORGANISING COMMITTEE
 ORGANISING COMMITTEE Dr Anthony Maxwell (Chair) Dr Sarah Vinnicombe (Vice Chair) Dr Sheetal Sharma (Meetings Secretary) Dr Nisha Sharma (Secretary) Dr Julie Cox (Treasurer) Professor Iain Lyburn (Research)
ORGANISING COMMITTEE Dr Anthony Maxwell (Chair) Dr Sarah Vinnicombe (Vice Chair) Dr Sheetal Sharma (Meetings Secretary) Dr Nisha Sharma (Secretary) Dr Julie Cox (Treasurer) Professor Iain Lyburn (Research)
Effect ofage and Breast Density on Screening Mammograms with False-Positive Findings
 Constance Emily 23 0. Lehman1 Susan Peacock2 Mariann J. Drucker2 Nicole Urban2 4 Received April 8, 1999: accepted after revision June 2, 1999. Supported by grant ROl CA63146-04 from the National Cancer
Constance Emily 23 0. Lehman1 Susan Peacock2 Mariann J. Drucker2 Nicole Urban2 4 Received April 8, 1999: accepted after revision June 2, 1999. Supported by grant ROl CA63146-04 from the National Cancer
SURVEY OF MAMMOGRAPHY PRACTICE
 Study ID SURVEY OF MAMMOGRAPHY PRACTICE This survey takes about 10-15 minutes to complete. We realize how busy you are and greatly appreciate your time. Your input can help make a difference in mammography.
Study ID SURVEY OF MAMMOGRAPHY PRACTICE This survey takes about 10-15 minutes to complete. We realize how busy you are and greatly appreciate your time. Your input can help make a difference in mammography.
Clinical guideline Published: 25 June 2013 nice.org.uk/guidance/cg164
 Familial breast cancer: classification, care and managing breast cancer and related risks in people with a family history of breast cancer Clinical guideline Published: 25 June 2013 nice.org.uk/guidance/cg164
Familial breast cancer: classification, care and managing breast cancer and related risks in people with a family history of breast cancer Clinical guideline Published: 25 June 2013 nice.org.uk/guidance/cg164
Localization of Breast Lesion Using Mammographic-Basic Views
 Research Article imedpub Journals www.imedpub.com Vol. 2 No. 1: 2 Localization of Breast Lesion Using Mammographic-Basic Views Nikki Mishra*, Meena Chakradhar, Ranjit Jha and Rauniyar RK Department of
Research Article imedpub Journals www.imedpub.com Vol. 2 No. 1: 2 Localization of Breast Lesion Using Mammographic-Basic Views Nikki Mishra*, Meena Chakradhar, Ranjit Jha and Rauniyar RK Department of
Tissue Breast Density
 Tissue Breast Density Reporting breast density within the letter to the patient is now mandated by VA law. Therefore, this website has been established by Peninsula Radiological Associates (PRA), the radiologists
Tissue Breast Density Reporting breast density within the letter to the patient is now mandated by VA law. Therefore, this website has been established by Peninsula Radiological Associates (PRA), the radiologists
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 336 J UNE 19, 1997 NUMBER 25 POSTMENOPAUSAL HORMONE THERAPY AND MORTALITY FRANCINE GRODSTEIN, SC.D., MEIR
The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 336 J UNE 19, 1997 NUMBER 25 POSTMENOPAUSAL HORMONE THERAPY AND MORTALITY FRANCINE GRODSTEIN, SC.D., MEIR
The best way of detection of and screening for breast cancer in women with genetic or hereditary risk
 The best way of detection of and screening for breast cancer in women with genetic or hereditary risk Ingrid Vogelaar Introduction Each year almost 1.2 million women are diagnosed with breast cancer worldwide.
The best way of detection of and screening for breast cancer in women with genetic or hereditary risk Ingrid Vogelaar Introduction Each year almost 1.2 million women are diagnosed with breast cancer worldwide.
The relationship between mammographic density and duration of hormone therapy: effects of estrogen and estrogen progestin
 Human Reproduction Vol.20, No.6 pp. 1741 1745, 2005 Advance Access publication April 21, 2005 doi:10.1093/humrep/deh820 The relationship between mammographic density and duration of hormone therapy: effects
Human Reproduction Vol.20, No.6 pp. 1741 1745, 2005 Advance Access publication April 21, 2005 doi:10.1093/humrep/deh820 The relationship between mammographic density and duration of hormone therapy: effects
Audit. Public Health Monitoring Report on 2006 Data. National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons.
 National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons Audit Public Health Monitoring Report on 2006 Data November 2009 Prepared by: Australian Safety & Efficacy Register of
National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons Audit Public Health Monitoring Report on 2006 Data November 2009 Prepared by: Australian Safety & Efficacy Register of
Breast Cancer Screening: Changing Philosophies in Educating Women and Teens
 Breast Cancer Screening: Changing Philosophies in Educating Women and Teens Courtney Benedict CNM MSN Disclosures Merck Nexplanon trainer Session Objectives Explain the rationale for initiation and frequency
Breast Cancer Screening: Changing Philosophies in Educating Women and Teens Courtney Benedict CNM MSN Disclosures Merck Nexplanon trainer Session Objectives Explain the rationale for initiation and frequency
Interval Cancers in BreastScreen Aotearoa
 Interval Cancers in BreastScreen Aotearoa 2008 2009 Released 2018 nsu.govt.nz Citation: National Screening Unit. 2018. Interval Cancers in BreastScreen Aotearoa 2008 2009. Wellington: Ministry of Health.
Interval Cancers in BreastScreen Aotearoa 2008 2009 Released 2018 nsu.govt.nz Citation: National Screening Unit. 2018. Interval Cancers in BreastScreen Aotearoa 2008 2009. Wellington: Ministry of Health.
The Decrease in Breast-Cancer Incidence in 2003 in the United States
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e s p e c i a l r e p o r t The Decrease in Breast-Cancer Incidence in 23 in the United States Peter M. Ravdin, Ph.D., M.D., Kathleen A. Cronin, Ph.D.,
T h e n e w e ng l a nd j o u r na l o f m e dic i n e s p e c i a l r e p o r t The Decrease in Breast-Cancer Incidence in 23 in the United States Peter M. Ravdin, Ph.D., M.D., Kathleen A. Cronin, Ph.D.,
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
BREAST CANCER SCREENING:
 BREAST CANCER SCREENING: controversies D David Dershaw Memorial Sloan Kettering Cancer Center New York, NY Areas of general agreement about mammographic screening Screening mammography has been demonstrated
BREAST CANCER SCREENING: controversies D David Dershaw Memorial Sloan Kettering Cancer Center New York, NY Areas of general agreement about mammographic screening Screening mammography has been demonstrated
Please read the following instructions carefully
 Grand River Regional Cancer Centre 835 King Street West, PO Box 9056 Kitchener, ON N2G 1G3 Tel: (519) 749-4370 x2832 Fax: (519) 749-4394 Dear: You have been referred to the High Risk Ontario Breast Screening
Grand River Regional Cancer Centre 835 King Street West, PO Box 9056 Kitchener, ON N2G 1G3 Tel: (519) 749-4370 x2832 Fax: (519) 749-4394 Dear: You have been referred to the High Risk Ontario Breast Screening
Breast Cancer Screening Database Reference Guide For Years
 Breast Cancer Screening Database Reference Guide For Years 1996-2014 Compiled by: Edna Kalu, Zikuan Liu HOW TO OBTAIN MORE INFORMATION For more information about this guide or other services and data available
Breast Cancer Screening Database Reference Guide For Years 1996-2014 Compiled by: Edna Kalu, Zikuan Liu HOW TO OBTAIN MORE INFORMATION For more information about this guide or other services and data available
Correlates of Hysterectomy among African-American Women
 American Journal of Epidemiology Copyright O 99 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 150, Printed In USA. Correlates of Hysterectomy among African-American
American Journal of Epidemiology Copyright O 99 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 150, Printed In USA. Correlates of Hysterectomy among African-American
Breast Cancer Screening Factsheet
 Breast Cancer Screening What does breast cancer screening entail? The National Breast Cancer Screening Programme is designed for women between 50 and 75 years of age. Once every 2 years, women in this
Breast Cancer Screening What does breast cancer screening entail? The National Breast Cancer Screening Programme is designed for women between 50 and 75 years of age. Once every 2 years, women in this
CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY
 Biomed. Papers 147(2), 211 219 (2003) D. Houserková, J. Matlochová, M. Hartlová 211 CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY Dana Houserková
Biomed. Papers 147(2), 211 219 (2003) D. Houserková, J. Matlochová, M. Hartlová 211 CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY Dana Houserková
Effects of a short-term suspension of hormone replacement therapy on mammographic density
 FERTILITY AND STERILITY VOL. 76, NO. 3, SEPTEMBER 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Effects of a short-term
FERTILITY AND STERILITY VOL. 76, NO. 3, SEPTEMBER 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Effects of a short-term
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report CONTENTS FIGURES AND TABLES... Figures... Tables... 3 INTRODUCTION... 5 SECTION MAXIMISING PARTICIPATION... 6 Program acceptance... 6 Eligibility... 6 Inviting
BreastScreen Victoria Annual Statistical Report CONTENTS FIGURES AND TABLES... Figures... Tables... 3 INTRODUCTION... 5 SECTION MAXIMISING PARTICIPATION... 6 Program acceptance... 6 Eligibility... 6 Inviting
Untangling the Confusion: Multiple Breast Cancer Screening Guidelines and the Ones We Should Follow
 Untangling the Confusion: Multiple Breast Cancer Screening Guidelines and the Ones We Should Follow Debra A. Walz, RN, MS, AOCNP, WHNP-BC, RNFA Advanced Oncology & Women s Health Nurse Practitioner Oneida
Untangling the Confusion: Multiple Breast Cancer Screening Guidelines and the Ones We Should Follow Debra A. Walz, RN, MS, AOCNP, WHNP-BC, RNFA Advanced Oncology & Women s Health Nurse Practitioner Oneida
Introduction to Breast Density
 Introduction to Breast Density A/Prof Wendy Ingman Breast Biology & Cancer Unit Ethical and Legal Considerations in Breast Density Workshop 2018 In this presentation My interest in breast density What
Introduction to Breast Density A/Prof Wendy Ingman Breast Biology & Cancer Unit Ethical and Legal Considerations in Breast Density Workshop 2018 In this presentation My interest in breast density What
Research Article An Estrogen Model: The Relationship between Body Mass Index, Menopausal Status, Estrogen Replacement Therapy, and Breast Cancer Risk
 Hindawi Publishing Corporation Computational and Mathematical Methods in Medicine Volume 202, Article ID 792375, 8 pages doi:0.55/202/792375 Research Article An Estrogen Model: The Relationship between
Hindawi Publishing Corporation Computational and Mathematical Methods in Medicine Volume 202, Article ID 792375, 8 pages doi:0.55/202/792375 Research Article An Estrogen Model: The Relationship between
Computer-aided Detection in the United Kingdom National Breast Screening Programme: Prospective Study 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Lisanne A. L. Khoo,
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Lisanne A. L. Khoo,
Scenarios for Clinicians
 Breast Density, Breast Cancer Risk and Wisconsin Breast Density Notification Law (2017 Wisconsin Act 201) Scenarios for Clinicians Content adapted from the California Breast Density Information Group,
Breast Density, Breast Cancer Risk and Wisconsin Breast Density Notification Law (2017 Wisconsin Act 201) Scenarios for Clinicians Content adapted from the California Breast Density Information Group,
REPRODUCTIVE ENDOCRINOLOGY
 FERTILITY AND STERILITY VOL. 70, NO. 6, DECEMBER 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. REPRODUCTIVE ENDOCRINOLOGY
FERTILITY AND STERILITY VOL. 70, NO. 6, DECEMBER 1998 Copyright 1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. REPRODUCTIVE ENDOCRINOLOGY
Contraception and cancerepidemiological
 Contraception and cancerepidemiological evidence Hormonal contraception Combined Progestogen-only Philip C Hannaford University of Aberdeen Breast cancer and combined oral Re-analysis of individual data
Contraception and cancerepidemiological evidence Hormonal contraception Combined Progestogen-only Philip C Hannaford University of Aberdeen Breast cancer and combined oral Re-analysis of individual data
Stopping oral contraceptives: an effective blood pressure-lowering intervention in women with hypertension
 (2005) 19, 451 455 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Stopping oral contraceptives: an effective blood pressure-lowering intervention
(2005) 19, 451 455 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Stopping oral contraceptives: an effective blood pressure-lowering intervention
Breast Cancer Risk Assessment and Prevention
 Breast Cancer Risk Assessment and Prevention Katherine B. Lee, MD, FACP October 4, 2017 STATISTICS More than 252,000 cases of breast cancer will be diagnosed this year alone. About 40,000 women will die
Breast Cancer Risk Assessment and Prevention Katherine B. Lee, MD, FACP October 4, 2017 STATISTICS More than 252,000 cases of breast cancer will be diagnosed this year alone. About 40,000 women will die
Drug Use in Relation to Outcome of Mammography Screening
 Research Article imedpub Journals www.imedpub.com Drug Use in Relation to Outcome of Mammography Screening von Euler-Chelpin M 1, Wu W 1, Vejborg I 2 and Lynge E 1 1 Department of Public Health, University
Research Article imedpub Journals www.imedpub.com Drug Use in Relation to Outcome of Mammography Screening von Euler-Chelpin M 1, Wu W 1, Vejborg I 2 and Lynge E 1 1 Department of Public Health, University
Menopausal hormone therapy currently has no evidence-based role for
 IN PERSPECTIVE HT and CVD Prevention: From Myth to Reality Nanette K. Wenger, M.D. What the studies show, in a nutshell The impact on coronary prevention Alternative solutions Professor of Medicine (Cardiology),
IN PERSPECTIVE HT and CVD Prevention: From Myth to Reality Nanette K. Wenger, M.D. What the studies show, in a nutshell The impact on coronary prevention Alternative solutions Professor of Medicine (Cardiology),
Frequently Asked Questions about Breast Density, Breast Cancer Risk, and the Breast Density Notification Law in California: A Consensus Document
 RSNA, 2013 Appendix E1 Frequently Asked Questions about Breast Density, Breast Cancer Risk, and the Breast Density Notification Law in California: A Consensus Document 1. I have been getting more questions
RSNA, 2013 Appendix E1 Frequently Asked Questions about Breast Density, Breast Cancer Risk, and the Breast Density Notification Law in California: A Consensus Document 1. I have been getting more questions
THE POSSIBLE ASSOCIATION BEtween
 ORIGINAL CONTRIBUTION Hormone Replacement Therapy in Relation to Breast Cancer Chi-Ling Chen, PhD Noel S. Weiss, MD, DrPH Polly Newcomb, PhD William Barlow, PhD Emily White, PhD THE POSSIBLE ASSOCIATION
ORIGINAL CONTRIBUTION Hormone Replacement Therapy in Relation to Breast Cancer Chi-Ling Chen, PhD Noel S. Weiss, MD, DrPH Polly Newcomb, PhD William Barlow, PhD Emily White, PhD THE POSSIBLE ASSOCIATION
Women s Health: Breast Cancer Screening. K. Rast, MD and E. McNany, MD
 Women s Health: Breast Cancer Screening K. Rast, MD and E. McNany, MD 2013 2017 Update: Who? How? When? Cases and Practice Questions Question 1 A 40 year old female comes to your office for a well woman
Women s Health: Breast Cancer Screening K. Rast, MD and E. McNany, MD 2013 2017 Update: Who? How? When? Cases and Practice Questions Question 1 A 40 year old female comes to your office for a well woman
Breast Thermography A radiation-free breast health assessment suitable for young women By Janet van Dam Medical Thermographer/ Member ACCT
 Breast Thermography A radiation-free breast health assessment suitable for young women By Janet van Dam Medical Thermographer/ Member ACCT I often get the question: at what age should I start worrying
Breast Thermography A radiation-free breast health assessment suitable for young women By Janet van Dam Medical Thermographer/ Member ACCT I often get the question: at what age should I start worrying
Screening Mammograms: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Screening Mammograms:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Screening Mammograms:
ORGANISING COMMITTEE
 ORGANISING COMMITTEE Dr Anthony Maxwell (Chair) Dr Sarah Vinnicombe (Vice Chair) Dr Sheetal Sharma (Meetings Secretary) Dr Nisha Sharma (Secretary) Dr Julie Cox (Treasurer) Professor Iain Lyburn (Research)
ORGANISING COMMITTEE Dr Anthony Maxwell (Chair) Dr Sarah Vinnicombe (Vice Chair) Dr Sheetal Sharma (Meetings Secretary) Dr Nisha Sharma (Secretary) Dr Julie Cox (Treasurer) Professor Iain Lyburn (Research)
Improving Screening Mammography Outcomes Through Comparison With Multiple Prior Mammograms
 Women s Imaging Original Research Hayward et al. Comparing Screening Mammograms With Multiple Prior Mammograms Women s Imaging Original Research Jessica H. Hayward 1 Kimberly M. Ray 1 Dorota J. Wisner
Women s Imaging Original Research Hayward et al. Comparing Screening Mammograms With Multiple Prior Mammograms Women s Imaging Original Research Jessica H. Hayward 1 Kimberly M. Ray 1 Dorota J. Wisner
PRESS RELEASE. NICE issues first guideline on menopause to stop women suffering in silence
 EMBARGOED UNTIL: 00.01hrs, THURSDAY 12 NOVEMBER 2015 PRESS RELEASE NICE issues first guideline on menopause to stop women suffering in silence More than a million women could benefit from the first NICE
EMBARGOED UNTIL: 00.01hrs, THURSDAY 12 NOVEMBER 2015 PRESS RELEASE NICE issues first guideline on menopause to stop women suffering in silence More than a million women could benefit from the first NICE
