Long-term exposure to ambient ultrafine particles and respiratory disease incidence in in Toronto, Canada: a cohort study
|
|
|
- Linda Reynolds
- 6 years ago
- Views:
Transcription
1 Weichenthal et al. Environmental Health (2017) 16:64 DOI /s RESEARCH Open Access Long-term exposure to ambient ultrafine particles and respiratory disease incidence in in Toronto, Canada: a cohort study Scott Weichenthal 1,2*, Li Bai 3,4, Marianne Hatzopoulou 5, Keith Van Ryswyk 2, Jeffrey C. Kwong 3,4,6, Michael Jerrett 7, Aaron van Donkelaar 8, Randall V. Martin 8,9, Richard T. Burnett 10, Hong Lu 4 and Hong Chen 3,4,11 Abstract Background: Little is known about the long-term health effects of ambient ultrafine particles (<0.1 μm) (UFPs) including their association with respiratory disease incidence. In this study, we examined the relationship between long-term exposure to ambient UFPs and the incidence of lung cancer, adult-onset asthma, and chronic obstructive pulmonary disease (COPD). Methods: Our study cohort included approximately 1.1 million adults who resided in Toronto, Canada and who were followed for disease incidence between 1996 and UFP exposures were assigned to residential locations using a land use regression model. Random-effect Cox proportional hazard models were used to estimate hazard ratios (HRs) describing the association between ambient UFPs and respiratory disease incidence adjusting for ambient fine particulate air pollution (PM 2.5 ), NO 2, and other individual/neighbourhood-level covariates. Results: In total, 74,543 incident cases of COPD, 87,141 cases of asthma, and 12,908 cases of lung cancer were observed during follow-up period. In single pollutant models, each interquartile increase in ambient UFPs was associated with incident COPD (HR = 1.06, 95% CI: 1.05, 1.09) but not asthma (HR = 1.00, 95% CI: 1.00, 1.01) or lung cancer (HR = 1.00, 95% CI: 0.97, 1.03). Additional adjustment for NO 2 attenuated the association between UFPs and COPD and the HR was no longer elevated (HR = 1.01, 95% CI: 0.98, 1.03). PM 2.5 and NO 2 were each associated with increased incidence of all three outcomes but risk estimates for lung cancer were sensitive to indirect adjustment for smoking and body mass index. Conclusions: In general, we did not observe clear evidence of positive associations between long-term exposure to ambient UFPs and respiratory disease incidence independent of other air pollutants. Further replication is required as few studies have evaluated these relationships. Keywords: Ultrafine particles, Cohort study, Asthma, Copd, Lung cancer Background Short-term exposures to ambient ultrafine particles (UFPs) (<0.1 μm) have been associated with acute changes in physiological measures of cardiorespiratory health [1, 2] but little is known about the long-term health effects of these pollutants. Recently, Ostro et al. [3] applied a chemical transport model to estimate UFP exposures (on a * Correspondence: scott.weichenthal@mcgill.ca 1 Department of Epidemiology, Biostatistics, and Occupational Health and Gerald Bronfman Department of Oncology, McGill University, 1020 Pine Avenue, West, Montreal, QC H3A 1A2, Canada 2 Air Health Science Division, Health Canada, Ottawa, Canada Full list of author information is available at the end of the article 3 3 km scale) for women in the California Teachers Study cohort and reported a positive association between ambient UFPs and ischemic heart disease mortality. Moreover, various sources/components of ambient UFPs were independently associated with ischemic heart disease mortality including elemental/organic carbon, metals (copper and iron), and emissions from gasoline and diesel engines [3]. Ambient UFPs were not associated with all-cause mortality or respiratory mortality (including lung cancer). To our knowledge, this is the only cohort study to date to evaluate the long-term health effects of ambient UFPs and The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Weichenthal et al. Environmental Health (2017) 16:64 Page 2 of 11 studies have yet to evaluate the relationship between UFPs and the incidence of respiratory diseases. In this study, we examined the association between long-term exposure to ambient UFPs and the incidence of lung cancer, adult-onset asthma, and chronic obstructive pulmonary disease (COPD) in Toronto, Canada. Longterm ambient UFP exposures were assigned to the residential locations of cohort members using a land use regression model developed for Toronto [4]. Our primary aim in conducting this study was to determine if ambient UFPs are independently associated with respiratory disease incidence after adjusting for other air pollutants including fine particulate air pollution (PM 2.5 ) and nitrogen dioxide (NO 2 ). Methods Study population Our study was conducted using the Ontario Population Health and Environment Cohort (ONPHEC), a large population-based cohort in Ontario Canada. Details of the ONPHEC cohort are provided elsewhere [5]. Briefly, this cohort is comprised of all adults in Ontario who, on April 1, 1996 and onwards, were registered with Ontario s provincial health insurance plan, resided in Ontario for 5 years, and were Canadian-born. The cohort was created through record linkages of population-based health administrative databases developed from the Ontario universal healthcare system. Our analysis included all cohort members who, on April 1, 1996, resided in the city of Toronto, were aged between 30 and 100 years, and were free of the conditions under investigation. Cohort members were followed until December 31, 2012 to determine incident cases of asthma and chronic obstructive pulmonary disease (COPD). For lung cancer, follow-up began on April 1, 2001 to allow for a minimum 5-year time lag in exposure. Outcomes All health data (including comorbidity data for diabetes, congestive heart failure (CHF), hypertension, acute myocardial infarction (AMI) and all cancers) were obtained from databases housed at the Institute for Clinical and Evaluative Sciences (ICES). This study used the following databases: 1) Registered Persons Database (for age, sex, residential history and health insurance eligibility); 2) Ontario COPD Database (for incident COPD); 3) Ontario Asthma Surveillance Information System (for incident asthma); 4) Ontario Cancer Registry (for incident lung cancer); 5) Census at the dissemination area level (for income quintile, census tract-level unemployment rate, education and mean household income); and 6) National Population Health Survey and Canadian Community Health Survey (for smoking habits and BMI used in the indirect adjustment). The International Classification of Diseases, Ninth Revision (ICD-9) codes for COPD and asthma and the third edition of the International Classification of Diseases for Oncology (ICD-O-3) codes for lung cancer are presented in Table 1. Air pollution exposure Estimates of long-term average exposure to ambient UFP and NO 2 were derived from land use regression models developed for the city of Toronto [4, 6]. UFP exposure estimates were based on measurements collected in 2014 [4, 7] while NO 2 exposure estimates were based on measurements collected in 2004 [6]. Briefly, the UFP model was based on data collected from a mobile monitoring campaign conducted over three weeks (2 weeks in summer, 1 week in winter) including data from 405 road segments distributed across the city of Toronto. Recent evidence from Amsterdam suggests that short-term monitoring campaigns can be used to develop models to predict past spatial variations in ambient UFPs [8]. The UFP model used in this study included parameters for the natural logarithm of the distance to highways, major roads, the central business district, Pearson international airport, and bus routes as well as land use variables for park land (100-m buffer), open space (100-m buffer), on-street trees (100-m buffer), and length of bus routes (100-m buffer). The model R 2 value was 0.67; when evaluated on an external sample of 151 data points the R 2 value was 0.50 and the mean difference between measured and predicted values was 1385 particles/cm 3 (95% CI: -3754, 982) [4]. The NO 2 model was based on data collected from 94 sites across Toronto and included variables for the lengths of expressways (200-m buffer) and major roads (50-m buffer), industrial land use (750-m buffer), density of dwellings (2000-m buffer), 24-h traffic counts (500-m buffer), and being downwind of an expressway within 1500 m. The model R 2 value for the NO 2 model was Table 1 Diagnostic codes for selected outcomes and comorbidities in this study ICD-9/ICD-O-3 codes Selected outcomes Chronic obstructive pulmonary 491,492, 496 disease (COPD) Asthma 493 Lung cancer C C34.9 a Comorbid health conditions Diabetes 250 Hypertension Congestive Heart Failure (CHF) 428 Acute myocardial infarction (AMI) 410 All cancer a Malignant lung tumors (behaviour code 3)
3 Weichenthal et al. Environmental Health (2017) 16:64 Page 3 of and bias was estimated to be less than 4% in crossvalidation procedures (a cross-validation R 2 was not reported) [6]. Estimates of long-term average PM 2.5 concentrations ( ) were derived from satellite observations at a spatial resolution of approximately 1km 1kmaspreviouslydescribed[9].Theseestimates have been shown to agree closely with ground-level monitoring data across North America (R 2 =0.82)[9]. Three-year moving average exposures (based on place of residence) were used for the main analyses. Covariates Individual level covariate data are limited in the ONPHEC cohort. We compiled the following covariates at baseline: age, sex and five comorbidities including diabetes, CHF, hypertension, AMI and all cancers (ICD-9 codes in Table 1). We further created four neighbourhood-level variables using 1996, 2001, and 2006 Canadian Census Dissemination data: 1) the proportion of recent immigrants; 2) the proportion of population aged 15 years who had not completed high school; 3) unemployment rate; and 4) mean household income. Statistical methods We estimated hazard ratios (HRs) using Cox proportional hazards models stratified by sex and one-year age groups. Continuous measures of long-term exposures to UFPs, PM 2.5 and NO 2 were included in the models as time-dependent variables using a 3-year moving average. For the incidence of lung cancer, a 5-year time lag in the exposure was used (i.e. the most recent 5-years were excluded from the moving average exposure). Follow-up ended if participants died, became ineligible for provincial health insurance (i.e. movement out of province), moved outside of Toronto, or at the end of follow-up (December 31, 2012). For all three outcomes, we incrementally adjusted for a series of covariates including comorbidities and neighbourhood-level contextual variables. We also evaluated the impact of including a frailty term for neighbourhood (n = 140 in the city of Toronto) to account for any unmeasured confounding factors at the neighbourhood level that may be associated with both exposure and outcomes. Finally, we examined multi-pollutant models including UFPs, NO 2 and PM 2.5 and investigated potential effect modification by age and sex. In addition, we conducted stratified analyses to evaluate potential effect modification by NO 2 in associations between particulate air pollutants and respiratory outcomes. All HRs and 95% confidence intervals (CIs) reflect interquartile range (IQR) increases in air pollution concentrations. A series of sensitivity analyses were conducted to test the robustness of our results. Specifically, UFP concentrations (our primary exposure of interested) were additionally modelled across quintiles of exposure. In addition, we considered mean annual exposures for each pollutant over other time windows including one and two year moving averages; we restricted analyses to participants who had lived at their baseline address for more than 5 years prior to cohort entry; we adjusted for a linear term for time to account for potential changes in the risk of outcomes of interest over time; we adjusted for distance to major roadways; and we indirectly adjusted for potential confounding by smoking and BMI [10]. For lung cancer, we also tested the sensitivity of the results by repeating the analyses after taking into account 0-year (no time lag) and 2-year lags in the exposure estimates. Finally, models for asthma and COPD were additional adjusted for prevalent lung cancer as a surrogate measure of smoking. Indirect adjustment analyses (to estimate the association between air pollution exposures and adjustment variables for smoking and BMI) made use of data on 3807 subjects in the city of Toronto from the Canadian Community Health Survey from the 2001, 2003, 2005 and 2007 panels who were between 30 and 100 years of age [10]. The hazard ratios between adjustment variables and respiratory disease incidence were directly calculated from the CCHS data because recent systematic reviews of the associations between our selected incidence outcomes and missing risk factors (i.e. smoking and BMI) were not identified. However, we did compare hazard ratios calculated using the CCHS respondents with those reported in previous studies, and found similar results. Specifically, lung cancer incidence was substantially higher in current (HR = 13.67, 95% CI: ) and former smokers (HR = 4.18, 95% CI ) in the CCHS respondents compared to never smokers. Similarly, the Women s Health Initiative Observational Study (WHI-OS) in the US reported that HRs for lung cancer incidence were (95% CI: ) and 4.20 (95% CI: ) in current and formers smokers, respectively, relative to never smokers [11]. The population characteristics of the CCHS cohort used for indirect adjustment were also similar to our study populations (i.e. 45% male, mean age of 58 years, and hypertension prevalence of 18.2%). Details of the indirect adjustment procedure have been describe previously [12]. Briefly, motivated by the theory of partitioned regression for linear regression models, this method allows for adjusting the HRs for these risk factors unavailable in the dataset, while simultaneously controlling for all risk factors included in the Cox models (e.g., comorbidities and neighborhood-level covariates). The method requires estimates of the spatial associations between the variables included in the Cox models and the unobserved variables. These estimated relationships were then used to indirectly adjust for smoking (never, former, or current cigarette smoker) and
4 Weichenthal et al. Environmental Health (2017) 16:64 Page 4 of 11 BMI (<25.0, , or 30 kg/m 2 ) for the entire cohort (see Additional file 1: Table S1). The Delta values reported in Table S1 refer to estimated associations between the omitted variables (i.e. smoking and BMI) and the concentrations of UFPs, PM 2.5, and NO 2. Negative values indicate inverse relationships between the prevalence of the omitted variables and levels of pollution. Results In total, 74,543 incident cases of COPD (mean follow-up 14.4 years), 87,141 cases of adult-onset asthma (mean follow-up 14.0 years), and 12,908 cases of lung cancer (mean follow-up 14.6 years) were identified over the follow-up period (Table 2). Men and women were present in our cohort in approximately equal proportions and participants had a mean age of approximately 50 years at baseline (Table 2). Approximately 22% of each baseline cohort population moved outside the city of Toronto during the follow-up period. UFP exposures varied substantially across Toronto ranging from less than 10,000/cm 3 to more than 100,000/cm 3 (Table 3). Spatial variations in ambient PM 2.5 and NO 2 concentrations were less dramatic but still covered the range of exposures typically observed across Canada (Table 3). Estimated UFP exposures were weakly correlated with PM 2.5 (r = 0.26) and NO 2 (r = 0.23); PM 2.5 and NO 2 were also weakly correlated (r = 0.22). These correlations are consistent with those previously observed in a panel study of personal air pollution exposures in Canada [13]. A scatter plot of NO2 and UFP concentrations is provided in Additional file 1: Figure S1. Hazard ratios describing the associations between ambient air pollutants and respiratory disease incidence are shown in Table 4. UFP exposures were not associated with increased lung cancer incidence. Small positive associations were observed between UFPs and asthma and COPD in single pollutant models but the magnitudes of these associations decreased when other air pollutants were included in the models (Fig. 1). The relationship between UFPs and COPD was also sensitive (and change directions) to the inclusion of a frailty term for neighbourhood suggesting an important impact of unmeasured confounding factors. When UFP exposures were modelled categorically across quintiles, COPD and asthma incidence were each increased in the four upper quintiles compared to the lowest category of Table 2 Baseline characteristics of study subjects and their neighborhoods Characteristics of the cohort COPD Asthma Lung cancer a Total cohort population Incident cases Total cohort population Incident cases Total cohort population Incident cases Number 1,105,258 74,543 1,057,722 87,141 1,039,128 12,908 % Individual risk factors at time of entry Age, years (SD) 51.4 (15.3) 62.2 (13.5) 51.8 (15.4) 51.8 (14.7) 50.7 (14.6) 60.0 (11.0) Men (%) Pre-existing comorbidity (%) Diabetes Chronic obstructive pulmonary disease (COPD) Asthma Acute myocardial infarction (AMI) Hypertension Congestive Heart Failure (CHF) Cancer Area level risk factors from Canadian Census at the census tract level at baseline Percentage of the population 15 years of age and older with less than a high school education Percentage of the population 15 years of age and older without employment Percentage of recent immigrants Average household income with all ages (in $1000 CAN) (SD) 62.1 (37.4) 57.9 (34.8) 62.2 (37.6) 58.9 (35.2) 62.0 (37.3) 57.8 (33.6) SD standard deviation a Lung cancer cohort was followed from April 1, 2001 to December 31, 2012
5 Weichenthal et al. Environmental Health (2017) 16:64 Page 5 of 11 Table 3 Descriptive statistics for estimated long-term average air pollution concentrations at baseline Pollutant IQR Mean (SD) Min 5th 25th 50th 75th 95th Max UFPs (count/cm 3 ) 10,097 28,473 (9226) ,184 22,186 26,000 32,320 58, ,759 PM 2.5 (μg/m 3 ) (2.1) NO 2 (ppb) (3.5) SD standard deviation, IQR interquartile range exposure; these risk estimates decreased (but remained elevated) when PM 2.5 and NO 2 were included in the models(table 5). Ambient PM 2.5 and NO 2 were each associated with modest increases (i.e. 1 12% in fully adjusted models) in the incidence of all three respiratory outcomes and associations were robust to adjustment for medial comorbidities, neighbourhood level covariates, and other air pollutants. However, including a frailty term in models for PM 2.5 (COPD and lung cancer models) and NO 2 (COPD model) also impacted risk estimates with hazard ratios increasing for NO 2 and decreasing for PM 2.5. For UFPs and NO 2, associations with incident COPD were strongest among younger subjects; however, other observed associations did not differ substantially by age or sex (Table 6). There was no clear evidence of effect modification by NO 2 in stratified analyses of associations between particulate air pollutants and respiratory outcomes (Additional file 1: Table S2). Additional adjustment of asthma and COD models for prevalent lung cancer did not materially change results for any of the pollutants (data not shown). Sensitivity analyses for PM 2.5 and NO 2 are shown in Tables 7 and 8. The hazard ratios for PM 2.5,NO 2, and lung cancer were sensitive to indirect adjustment for smoking and BMI and the magnitudes of these associations decreased when these parameters were included in the model. The magnitudes of associations between PM 2.5 and NO 2 and COPD/asthma were robust (i.e. changes of 1 2%) to various modeling approaches including indirect adjustment for smoking and obesity (Tables 7-8). Hazard ratios for UFPs and lung cancer Table 4 Hazard ratios (HR) and 95% CIs for the incidence of chronic obstructive pulmonary disease (COPD), adult-onset asthma and lung cancer in relation to an IQR increases in each pollutant in Toronto, Canada Exposure Model COPD ( ) Asthma ( ) Lung cancer a ( ) HR 95% CI HR 95% CI HR 95% CI UFPs UFPs only b Neighborhood-level covariates c frailty term for neighborhoods Medical comorbidities d e +PM e +NO e +PM 2.5 and NO PM 2.5 PM 2.5 only Neighborhood-level covariates d frailty term for neighborhoods Medical comorbidities e +NO NO 2 NO 2 only Neighborhood-level covariates d frailty term for neighborhoods Medical comorbidities PM 2.5 e a Cohort for lung cancer was followed up from April 1, 2001 to December 31, 2012 and a 5-year lag in exposure was used b Stratified by one-year age and sex c Neighborhood-level covariates include percentage of the population 15 years of age and older with less than a high school education, percentage of the population 15 years of age and older without employment, percentage of recent immigrants, and average household income d For COPD and asthma, we included comorbid diabetes, CHF, AMI, hypertension and all cancer; For lung cancer, we included comorbid diabetes, CHF, AMI and hypertension e Fully adjusted models
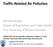
6 Weichenthal et al. Environmental Health (2017) 16:64 Page 6 of 11 Asthma COPD Lung Cancer Hazard Ratio (95% CI) NO2 PM2.5 UFP NO2 PM2.5 UFP NO2 PM2.5 UFP Fig. 1 Hazard ratios (HR) and 95% CIs for the incidence of chronic obstructive pulmonary disease (COPD), adult-onset asthma and lung cancer in relation to an IQR increases in each pollutant in Toronto, Canada. All models are stratified by one-year age and sex and are adjusted for neighborhoodlevel covariates including percentage of the population 15 years of age and older with less than a high school education, percentage of the population 15 years of age and older without employment, percentage of recent immigrants, and average household income. For COPD and asthma, comorbid diabetes, CHF, AMI, hypertension, and all cancers were included as covariates. For lung cancer, we included comorbid diabetes, CHF, AMI and hypertension. Models for UFPs are adjusted for NO 2 and PM 2.5. Models for NO 2 are adjusted for PM 2.5 ; PM 2.5 models are adjusted for NO 2 and asthma remained null in all sensitivity analyses while positive associations were generally observed between UFPs and COPD (Additional file 1: Table S3). Discussion A number of studies have observed short-term cardiovascular and respiratory health effects of ambient UFPs [1, 2] but little is known about the long-term health effects of these pollutants. We conducted a large population-based study to examine the relationship between long-term exposure to ambient UFPs and respiratory disease incidence in Toronto, Canada. In general, we did not observe clear evidence of positive associations between UFPs and respiratory disease incidence independent of other air pollutants although positive associations were observed between UFPs and incident COPD. To our knowledge, only one previous cohort study has evaluated the long-term health effects of ambient UFPs. Specifically, Ostro et al. [3] reported positive associations between UFP concentrations (and various components) and ischemic heart disease mortality but UFPs were not associated with mortality from respiratory outcomes. Our findings are consistent with this result as we did not observe clear evidence of associations between ambient UFPs and any of the respiratory outcomes examined. On the other hand, spatial variations in long-term average ambient NO 2 and PM 2.5 concentrations were positively associated with lung cancer incidence and this is consistent with existing evidence related to outdoor air pollution and lung cancer risk [14, 15]; however, these associations were sensitive to indirect adjustment for smoking and BMI in our analyses. In general, it is not clear why UFPs would not be associated with lung cancer incidence as diesel exhaust is a known carcinogen [16] and diesel vehicles are an important source of UFPs in urban areas [7, 17]. One explanation may be that the rapid condensation/ agglomeration of UFPs into larger particles tends to concentrate carcinogenic substances into larger particle size fractions and this hypothesis is supported by previous associations between PM 2.5 and lung cancer [14]. Alternatively, residential estimates of long-term average UFP concentrations may not adequately capture long-term personal exposures as other micro-environments (such as transportation) [7] likely also contribute substantially to UFP exposures. In the future, it may be interesting to incorporate mobility information (e.g. both home and workplace location) into exposure assessment in large population-based studies to see if this has an important
7 Weichenthal et al. Environmental Health (2017) 16:64 Page 7 of 11 Table 5 Hazard ratios (HR) and 95% CIs for the incidence of chronic obstructive pulmonary disease (COPD), adult-onset asthma, and lung cancer across quintiles of ambient UFP concentrations in Toronto, Canada Exposure COPD Asthma Lung cancer HR 95%CI HR 95%CI HR 95%CI Single Pollutant Model UFPs (by quintiles) a Q Q Q Q Q Adjusted for NO 2 and PM 2.5 UFPs a Q Q Q Q Q a Hazard ratios by quintiles of distributions were estimated in the single-pollutant models stratified by age and sex and adjusted for medical comorbidities and neighborhood-level variables. For COPD, quintiles of UFPs: Q1, 21,473; Q2, 21,473 24,349; Q3, 24,349 27,813; Q4, 27,813 34,763; Q5, > 34,763 count/cm 3. For asthma, quintiles of UFPs: Q1, 21,459; Q2, 21,459 24,325; Q3, 24,325 27,788; Q4, 27,788 34,726; Q5, > 34,726 count/cm 3. For lung cancer, quintiles of UFPs: Q1, 21,464; Q2, 21,464 24,329; Q3, 24,329 27,793; Q4, 27,793 34,758; Q5, > 34,758 count/cm 3 Table 6 Hazard ratios and 95% CI for the associations of incident COPD, adult-onset asthma, and lung cancer with an IQR increase in each pollutant by age and sex in Toronto, Canada Covariates No. of cases UFPs PM 2.5 NO 2 HR 95% CI HR 95% CI HR 95% CI COPD Age <60 28, , > = 75 13, Sex Men 39, Women 35, Asthma Age <60 58, , Sex > = Men 35, Women 52, Lung Cancer Age < Sex > = Men Women All models are stratified by age and sex, include a frailty term for neighborhoods, and are adjusted for neighborhood-level covariates
8 Weichenthal et al. Environmental Health (2017) 16:64 Page 8 of 11 Table 7 Sensitivity analyses for the associations of respiratory disease incidence with PM 2.5 Sensitivity analysis COPD Asthma Lung cancer a HR 95% CI HR 95% CI HR 95% CI Results from the Main Analyses (Table 4) Two different time windows of exposure 1 year before event NA NA NA 2 year before event NA NA NA Two different lags in the exposure 0-year lag b NA NA NA NA NA NA year lag c NA NA NA NA NA NA Restricted to subjects who lived at their baseline addresses for 5 years prior to cohort entry Adjusted for a linear term for time Adjusted for the distance to roadways Indirect adjustment (with HRs directly calculated from the CCHS cohort) + Smoking only Smoking and BMI a The cohort was followed up from April 1, 2001 to December 31, 2012 b The cohort was followed up from April 1, 1996 to December 31, 2012 c The cohort was followed up from April 1, 1998 to December 31, All models are stratified by age and sex, include a frailty term for neighborhoods, and are adjusted for neighborhood-level covariates impact on effect estimates for pollutants with high spatial variability. A previous review of epidemiological studies related to air pollution and adult-onset asthma found inconsistent evidence in support of a causal relationship and identified the need for large-scale cohort studies and the inclusion of local-scale traffic pollutants like UFPs [18]. Our investigation addressed both of these needs and our results indicate that NO 2 and PM 2.5 may each contribute to increases in the incidence of adult-onset asthma independent of other potential risk factors. The results of two other large cohort studies also support these Table 8 Sensitivity analyses for the associations of respiratory disease incidence with NO 2 in fully adjusted models Sensitivity analysis COPD Asthma Lung cancer a HR 95% CI HR 95% CI HR 95% CI Results from the Main Analyses (Table 4) Two different time windows of exposure 1 year before event NA NA NA 2 year before event NA NA NA Two different lags in the exposure 0-year lag b NA NA NA NA NA NA year lag c NA NA NA NA NA NA Restricted to subjects who lived at their baseline addresses for 5 years prior to cohort entry Adjusted for a linear term for time Adjusted for the distance to roadways Indirect adjustment (with HRs directly calculated from the CCHS cohort) + Smoking only Smoking and BMI a The cohort was followed up from April 1, 2001 to December 31, 2012 b The cohort was followed up from April 1, 1996 to December 31, 2012 c The cohort was followed up from April 1, 1998 to December 31, All models are stratified by age and sex, include a frailty term for neighborhoods, and are adjusted for neighborhood-level covariates
9 Weichenthal et al. Environmental Health (2017) 16:64 Page 9 of 11 findings. Specifically, Young et al. [19] reported positive associations between incident adult-onset asthma/ wheeze and ambient PM 2.5 and NO 2 concentrations among approximately 50,000 women followed over a 4- year period as part of the United States Sister Study cohort. Moreover, a combined analysis of six European cohorts including approximately 24,000 subjects reported positive associations between ambient PM 2.5 /NO 2 and the development of adult onset asthma [20]. Collectively, evidence from these recent large prospective cohort studies suggests that ambient air pollutants including NO 2 and PM 2.5 may contribute to a modest increase in the incidence of adult-onset asthma. Epidemiological evidence related long-term air pollution exposures and COPD incidence is somewhat limited and remains inconclusive [21]. In particular, two recent cohort studies found little evidence of important relationships between PM 2.5, NO 2, and COPD incidence. Specifically, Gan et al. [22] reported weak associations between PM 2.5,NO 2, and COPD hospitalizations/mortality in a cohort of approximately 500,000 subjects in Vancouver, Canada followed over a 4-year period. Similarly, a large national cohort study in England including more than 800,000 subjects found little evidence of an important association between PM 2.5, NO 2 and COPD incidence [23]. Conversely, Andersen et al. [24] reported a positive association between long-term exposure to NO 2 and incident COPD in a Danish cohort study of approximately 57,000 subjects followed between 1993 and While our findings support modest association between PM 2.5,NO 2 and COPD incidence (and possibly UFPs), collective evidence remains limited. This study had a number of important advantages including large numbers of incident cases and detailed exposure information for multiple air pollutants accounting for subject mobility; however, it is important to note several limitations. First, it is difficult to compare the magnitude of associations across pollutants as different exposure models were used for each air pollutant. Therefore, differences in exposure measurement error might have resulted in more/ less bias in associations for a given air pollutant depending on the degree to which residential exposure estimates (assigned to postal code centroids) reflected true long-term personal exposures. This measurement error likely contains components of both Classical (i.e. estimated ambient concentrations distribute around true ambient concentrations) and Berkson type measurement error (true personal exposures distributed around estimated mean ambient concentrations). As this error is likely non-differential with respect to survival time, the Classical measurement error component would tend to bias risk estimates toward the null in proportion to the correlation between measured exposures and true long-term personal exposures(which is unknown and is not provided by the model evaluation R 2 values). The Berkson component of measurement error would not bias risk estimates but would decrease the precision of risk estimates. Therefore, the hazard ratios presented in this study likely underestimate the true magnitudes of associations between long-term exposure to air pollution and respiratory disease incidence. For UFPs, the exposure model was based on spatial monitoring data collected after the follow-up period and this may have contributed to the null associations observed in our analyses. While analysis of long-term trends would help to clarify this question, the data required to support such an analysis do not exist. Moreover, UFPs are only weakly correlated with ambient NO 2 and PM 2.5 and thus trends in these pollutants cannot be used to infer trends in UFPs. What seems likely is that our model may underestimate true long-term exposure levels owing to decreases in vehicle emissions over time. However, spatial differences in UFP concentrations are likely more stable over time because spatial differences are primarily impacted by changes in the spatial patterns of diesel traffic (primarily large diesel vehicles). Since large diesel vehicles remain concentrated on major roadways, contrasts between high-traffic and low-traffic areas are likely preserved over time. Therefore, our model likely provides useful estimates of the relationship between health outcomes and changes in UFP exposure but may not be appropriate for determining absolute concentrations at which health effects occur (i.e. some minimum exposure threshold). Another limitation is that we did not have individual level data on smoking behavior which is an important risk factor for all of the outcomes examined. To address this limitation, we used an indirect method of confounder adjustment based on pollutant-outcome associations in a second cohort available in the Toronto area and observed important changes in our effect estimates when this method was applied. However, we cannot rule out residual confounding by smoking. Conclusions We did not observe clear evidence of positive associations between long-term exposure to ambient UFPs and the incidence of lung cancer, COPD, or adult onset asthma. Our findings do suggest a possible association between UFPs and COPD but this association was sensitive to other air pollutants. In general, our findings require further replication in future cohort analyses as few studies have examined the chronic health effects of ambient UFPs to date. Additional files Additional file 1: Table S1. Linear associations between smoking and BMI and concentrations of UFPs, PM2.5, and NO 2. Table S2. Hazard ratios (HR) and 95% CIs for the incidence of chronic obstructive pulmonary
10 Weichenthal et al. Environmental Health (2017) 16:64 Page 10 of 11 disease (COPD), adult-onset asthma and lung cancer in relation to an IQR increases in UFPs and PM 2.5 across tertiles of NO 2. Table S3. Sensitivity analyses for the associations of respiratory disease incidence with UFPs. Figure S1. A scatter plot of ultrafine particles (count/cm 3 ) and NO 2 (ppb) concentrations at baseline. (DOCX 77 kb) Abbreviations AMI: Acute myocardial infarction; BMI: Body mass index; CCHS: Canadian community health survey; CHF: Congestive heart failure; COPD: Chronic obstructive pulmonary disease; HR: Hazard ratio; ICD: International classification of diseases; ICES: Institute for clinical and evaluative sciences; ONPHEC: Ontario population health and environment cohort; UFPs: Ultrafine particles Acknowledgements The authors would like to thank Dr. Eric Lavigne for his comments in reviewing the paper. Funding This study was funded by Health Canada and supported by Public Health Ontario (PHO) and the Institute for Clinical Evaluative Sciences (ICES), which is funded by an annual grant from the Ontario Ministry of Health and Long-Term Care (MOHLTC). Parts of this material are based on data and information compiled and provided by the Canadian Information Health Institute (CIHI). Dr. Weichenthal also received financial support from a GRePEC salary award funded by the Cancer Research Society, the Quebec Ministry of Economy, Science and Innovation, and FRSQ (Fonds de recherche du Québec- Santé). Availability of data and materials The exposure models/data used in this study are available upon request to support future investigations and are described in the references [4, 6, 9]. The cohort data are housed at the Institute for Clinical Evaluative Sciences and cannot be distributed and must be analyzed on site. Author s contributions SW was the lead author and developed the UFP exposure model with MH and KVR. LB and HC conducted all statistical analyses with input from RB. MJ developed the NO 2 exposure model and RM and AD provided the PM 2.5 exposure data. All author read and approved the final manuscript, provided comments, and contributed to preparing the final document. Competing interests The authors declare that they have no competing interests. Consent for publication Not applicable. Ethics approval and consent to participate The Research Ethics Board of Sunnybrook Health Sciences Centre, Toronto approved the study. Disclaimer Not applicable. Author details 1 Department of Epidemiology, Biostatistics, and Occupational Health and Gerald Bronfman Department of Oncology, McGill University, 1020 Pine Avenue, West, Montreal, QC H3A 1A2, Canada. 2 Air Health Science Division, Health Canada, Ottawa, Canada. 3 Public Health Ontario, Toronto, Canada. 4 Institute for Clinical Evaluative Sciences, Toronto, ON, Canada. 5 Department of Civil Engineering, University of Toronto, Toronto, Canada. 6 Department of Family and Community Medicine, University of Toronto, Toronto, ON, Canada. 7 School of Public Health, University of California, Los Angeles, CA, USA. 8 Dalhousie University, Halifax, Nova Scotia, Canada. 9 Harvard-Smithsonian Center for Astrophysics, Cambridge, MA, USA. 10 Population Studies Division, Health Canada, Ottawa, Canada. 11 Dalla Lana School of Public Health, University of Toronto, Toronto, ON, Canada. Received: 12 January 2017 Accepted: 11 June 2017 References 1. Weichenthal S. Selected physiological effects of ultrafine particles in acute cardiovascular morbidity. Environ Res. 2012;115: Evans KA, Halterman JS, Hopke PK, Fagnano M, Rich DQ. Increased ultrafine particles and carbon monoxide concentrations are associated with asthma exacerbation among urban children. Environ Res. 2014;129: Ostro B, Hu J, Goldberg D, Reynolds P, Hertz A, Bernstein L, et al. Associations of mortality with long-term exposures to fine and ultrafine particles, species and sources: Results from the California teachers study cohort. Environ Health Perspect. 2015;123(6): Weichenthal S, Van Ryswyk K, Goldstein A, Shekarrizfard M, Hatzopoulou M. Characterizing the spatial distribution of ambient ultrafine particles in Toronto, Canada: A land use regression model. Environ Pollut. 2016;208(Pt A): Chen H, Kwong JC, Copes R, Villeneuve PJ, Goldberg MS, Weichenthal S, van Donkelaar A, Jerrett M, Martin RV, Brook JR, Kopp A, Burnett RT. Cohort profile: The Ontario Population Health and Environment Cohort (ONPHEC). Int J Epidemiol 2016; Epub ahead of print Apr. 20. doi: /ije/dyw Jerrett M, Arain MA, Kanaroglou P, Beckerman B, Crouse D, Gilbert NL, et al. Modeling the intraurban variability of ambient pollution in Toronto, Canada. J Toxicol Environ Health A. 2007;70(3 4): Weichenthal S, Van Ryswyk K, Kulka R, Sun L, Wallace L, Joseph L. In-vehicle exposures to particulate air pollution in Canadian metropolitan areas: The urban transportation exposure study. Environ Sci Technol. 2015;49(1): Montagne DR, Hoek G, Klompmaker JO, Wang M, Meliefste K, Brunekreef B. Land use regression models for ultrafine particles and black carbon based on short-term monitoring predict past spatial variation. Environ Sci Technol. 2015;49(14): van Donkelaar A, Martin RV, Spurr RJ, Burnett RT. High-resolution satellitederived PM2.5 from optimal estimation and geographically weighted regression over North America. Environ Sci Technol. 2015;49(17): Shin HH, Cakmak S, Brion O, Villeneuve P, Turner MC, Goldberg MS, et al. Indirect adjustment for multiple missing variables applicable to environmental epidemiology. Environ Res. 2014;134: Wang A, Kubo J, Luo J, Desai M, Hedlin H, Henderson M, et al. Active and passive smoking in relation to lung cancer incidence in the Women s health initiative observational study prospective cohort. Ann Oncol. 2015;26: Crouse DL, Peters PA, Hystad P, Brook JR, van Donkelaar A, Martin RV, et al. Ambient PM2.5, O3, and NO2 exposures and associations with mortality over 16 years of follow-up in the Canadian census health and environment cohort (CanCHEC). Environ Health Perspect. 2015;123(11): Weichenthal S, Hatzopoulou M, Goldberg M. Exposure to traffic-related air pollution during physical activity and acute changes in blood pressure, autonomic and micro-vascular function in women: A cross-over study. Part Fibre Toxicol. 2014;11: Hamra GB, Guha N, Cohen AJ, Laden F, Raaschou-Nielsen O, Samet JM, et al. Outdoor particulate matter exposure and lung cancer: A systematic review and meta-analysis. Environ Health Perspect. 2014;122(9): Hamra GB, Laden F, Cohen AJ, Raaschou-Nielsen O, Brauer M, Loomis D. Lung cancer and exposure to nitrogen dioxide and traffic: A systematic review and meta-analysis. Environ Health Persepct. 2015;123(11): Benbrahim-Tallaa L, Baan RA, Grosee Y, Lauby-Secretan B, El Ghissassi F, Bouvard V, et al. Carcinogenicity of diesel-engine and gasoline-engine exhausts and some nitroarenes. Lancet Oncology ;13(7): Wang Y, Zhu Y, Salinas R, Ramirez D, Karnae S, John K. Roadside measurements of ultrafine particles at a busy urban intersection. J Air Waste Manage Assoc. 2008;58(11): Jacquemin B, Schikowski T, Carsin AE, Hansell A, Kramer U, Sunyer J, et al. The role of air pollution in adult-onset asthma: A review of the current evidence. Semin Respir Crit Care Med. 2012;33(6): Young MT, Sandler DP, DeRoo LA, Vedal S, Kaufmann JD, London SJ. Ambient air pollution exposure and incident adult asthma in a nationwide cohort of U.S. women. Am J Respir Crit Care Med. 2014;190(8): Jacuemin B, Siroux V, Sanchez M, Carsin AE, Schikowski T, et al. Ambient air pollution and adult asthma incidence in six European cohorts (ESCAPE). Environ Health Perspect. 2015;123(6): Schikowski T, Mills IC, Anderson HR, Cohen A, Hansell A, Kauffmann F, et al. Ambient air pollution: A cause of COPD? Eur Respir J. 2014;43(1):
11 Weichenthal et al. Environmental Health (2017) 16:64 Page 11 of Gan WQ, FitzGerald JM, Carlsten C, Sadatsafavi M, Brauer M. Associations of ambient air pollution with chronic obstructive pulmonary disease hospitalization and mortality. Am J Respir Crit Care Med. 2013;187(7): Atkinson RW, Carey IM, Kent AJ, van Staa TP, Anderson HR, Cook DG. Longterm exposure to outdoor air pollution and the incidence of chronic obstructive pulmonary disease in a national English cohort. Occup Environ Med. 2015;72(1): Andersen ZJ, Hvidberg M, Jensen SS, Ketzel M, Loft S, Sorensen M, et al. Chronic obstructive pulmonary disease and long-term exposure to trafficrelated air pollution. Am J Respir Crit Care Med. 2011;183(4): Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Chen H, Kwong JC, Copes R, et al. Living near
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Chen H, Kwong JC, Copes R, et al. Living near
Traffic-Related Air Pollution
 Traffic-Related Air Pollution Michael Brauer School of Population and Public Health The University of British Columbia OEMAC 30 th Annual Scientific Conference, October 1-2, 2012 Sheraton Vancouver Wall
Traffic-Related Air Pollution Michael Brauer School of Population and Public Health The University of British Columbia OEMAC 30 th Annual Scientific Conference, October 1-2, 2012 Sheraton Vancouver Wall
Considerations About Exposure and Health Effects of Traffic Pollution
 Considerations About Exposure and Health Effects of Traffic Pollution Northern Transportation and Air Quality Summit 2010 August 24, 2010 Maria Costantini Health Effects Institute What Is HEI HEI is a
Considerations About Exposure and Health Effects of Traffic Pollution Northern Transportation and Air Quality Summit 2010 August 24, 2010 Maria Costantini Health Effects Institute What Is HEI HEI is a
Traffic Air Pollution and Mortality Rate Advancement Periods
 American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 160, No. 2 Printed in U.S.A. DOI: 10.1093/aje/kwh181 Traffic Air Pollution
American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 160, No. 2 Printed in U.S.A. DOI: 10.1093/aje/kwh181 Traffic Air Pollution
Alexeeff et al. Environmental Health (2018) 17:38 https://doi.org/ /s
 Alexeeff et al. Environmental Health (2018) 17:38 https://doi.org/10.1186/s12940-018-0382-1 RESEARCH High-resolution mapping of traffic related air pollution with Google street view cars and incidence
Alexeeff et al. Environmental Health (2018) 17:38 https://doi.org/10.1186/s12940-018-0382-1 RESEARCH High-resolution mapping of traffic related air pollution with Google street view cars and incidence
AIR POLLUTION AND EMERGENCY DEPARTMENT VISITS FOR DEPRESSION IN EDMONTON, CANADA
 International Journal of Occupational Medicine and Environmental Health 2007;20(3):241 245 DOI 10.2478/v10001-007-0024-2 AIR POLLUTION AND EMERGENCY DEPARTMENT VISITS FOR DEPRESSION IN EDMONTON, CANADA
International Journal of Occupational Medicine and Environmental Health 2007;20(3):241 245 DOI 10.2478/v10001-007-0024-2 AIR POLLUTION AND EMERGENCY DEPARTMENT VISITS FOR DEPRESSION IN EDMONTON, CANADA
Impact of fine particles in ambient air on lung cancer
 Chinese Journal of Cancer Review Impact of fine particles in ambient air on lung cancer Gerard Hoek 1 and Ole Raaschou-Nielsen 2 Abstract Recently, the International Agency for Research on Cancer (IARC)
Chinese Journal of Cancer Review Impact of fine particles in ambient air on lung cancer Gerard Hoek 1 and Ole Raaschou-Nielsen 2 Abstract Recently, the International Agency for Research on Cancer (IARC)
Long-Term Exposure to Air Pollution and Type 2 Diabetes in Adults. Robin Puett, PhD, Associate Professor, University of Maryland
 Long-Term Exposure to Air Pollution and Type 2 Diabetes in Adults Robin Puett, PhD, Associate Professor, University of Maryland Background Diabetes modified effect of air pollution exposure on cardiovascular
Long-Term Exposure to Air Pollution and Type 2 Diabetes in Adults Robin Puett, PhD, Associate Professor, University of Maryland Background Diabetes modified effect of air pollution exposure on cardiovascular
Health effects of (particulate) air pollution
 Health effects of (particulate) air pollution Peter Hoet Ben Nemery Jan Emmerechts Katrien Luyts Ernesto Alfaro-Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution and Health Introduction
Health effects of (particulate) air pollution Peter Hoet Ben Nemery Jan Emmerechts Katrien Luyts Ernesto Alfaro-Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution and Health Introduction
Long-term exposure to air pollution and diabetes risk in Danish Nurse Cohort study
 Long-term exposure to air pollution and diabetes risk in Danish Nurse Cohort study Anne Busch Hansen a, Line Ravnskjær b, Steffen Loft c, Klaus Kaae Andersen b, Elvira Bräuner d, Rikke Baastrup e, Claire
Long-term exposure to air pollution and diabetes risk in Danish Nurse Cohort study Anne Busch Hansen a, Line Ravnskjær b, Steffen Loft c, Klaus Kaae Andersen b, Elvira Bräuner d, Rikke Baastrup e, Claire
APPENDIX AVAILABLE ON THE HEI WEB SITE
 APPENDIX AVAILABLE ON THE HEI WEB SITE Research Report 178 National Particle Component Toxicity (NPACT) Initiative Report on Cardiovascular Effects Sverre Vedal et al. Section 1: NPACT Epidemiologic Study
APPENDIX AVAILABLE ON THE HEI WEB SITE Research Report 178 National Particle Component Toxicity (NPACT) Initiative Report on Cardiovascular Effects Sverre Vedal et al. Section 1: NPACT Epidemiologic Study
t air pollution Peter Hoet Ben Nemery
 Health effects of (particulate) t air pollution Peter Hoet Ben Nemery Tim Nawrot Jan Emmerechts Katrien Luyts Ernesto Alfaro Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution
Health effects of (particulate) t air pollution Peter Hoet Ben Nemery Tim Nawrot Jan Emmerechts Katrien Luyts Ernesto Alfaro Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution
Overview of Key Ozone Epidemiology Literature
 Overview of Key Ozone Epidemiology Literature Julie E. Goodman, Ph.D., DABT, ACE, ATS Ozone Webinar Texas Commission on Environmental Quality March 20, 2015 Epidemiology The study of the causes, distribution,
Overview of Key Ozone Epidemiology Literature Julie E. Goodman, Ph.D., DABT, ACE, ATS Ozone Webinar Texas Commission on Environmental Quality March 20, 2015 Epidemiology The study of the causes, distribution,
Air Quality: What an internist needs to know
 Air Quality: What an internist needs to know Robert Paine, M.D. Pulmonary and Critical Care Medicine University of Utah School of Medicine Program for Air Quality, Health and Society February, 2017 October
Air Quality: What an internist needs to know Robert Paine, M.D. Pulmonary and Critical Care Medicine University of Utah School of Medicine Program for Air Quality, Health and Society February, 2017 October
What are the Human Health Effects of Air Pollution?
 What are the Human Health Effects of Air Pollution? Dr. Judy Guernsey Department of Community Health and Epidemiology Dalhousie University Nova Scotia Department of Environment and Labour Outdoor Air Quality
What are the Human Health Effects of Air Pollution? Dr. Judy Guernsey Department of Community Health and Epidemiology Dalhousie University Nova Scotia Department of Environment and Labour Outdoor Air Quality
The prevalence of type 2 diabetes mellitus is increasing CMAJ OPEN. Research
 Hospital admission rates and emergency department use in relation to glycated hemoglobin in people with diabetes mellitus: a linkage study using electronic medical record and administrative data in Ontario
Hospital admission rates and emergency department use in relation to glycated hemoglobin in people with diabetes mellitus: a linkage study using electronic medical record and administrative data in Ontario
The updated incidences and mortalities of major cancers in China, 2011
 DOI 10.1186/s40880-015-0042-6 REVIEW Open Access The updated incidences and mortalities of major cancers in China, 2011 Wanqing Chen *, Rongshou Zheng, Hongmei Zeng and Siwei Zhang Abstract Introduction:
DOI 10.1186/s40880-015-0042-6 REVIEW Open Access The updated incidences and mortalities of major cancers in China, 2011 Wanqing Chen *, Rongshou Zheng, Hongmei Zeng and Siwei Zhang Abstract Introduction:
Air Pollution and Heart Health
 Air Pollution and Heart Health Wayne E. Cascio, MD, FACC, FAHA Director, Environmental Public Health Division National Health and Environmental Effects Research Laboratory Disclosure of Conflicts of Interest
Air Pollution and Heart Health Wayne E. Cascio, MD, FACC, FAHA Director, Environmental Public Health Division National Health and Environmental Effects Research Laboratory Disclosure of Conflicts of Interest
Author s response to reviews
 Author s response to reviews Title: Short-term effects of ambient fine particulate matter pollution on hospital visits for chronic obstructive pulmonary disease in Beijing, China Authors: Yaohua Tian (yaohua_tian@bjmu.edu.com)
Author s response to reviews Title: Short-term effects of ambient fine particulate matter pollution on hospital visits for chronic obstructive pulmonary disease in Beijing, China Authors: Yaohua Tian (yaohua_tian@bjmu.edu.com)
Groupe d Analyse Économique An Analysis Group Company
 Groupe d Analyse Économique To: From: Canadian Council for Tobacco Control Groupe d Analyse Économique Date: April 9, 2002 Re: Impact of an anti-tobacco campaign on direct health care costs in Canada 1.
Groupe d Analyse Économique To: From: Canadian Council for Tobacco Control Groupe d Analyse Économique Date: April 9, 2002 Re: Impact of an anti-tobacco campaign on direct health care costs in Canada 1.
Finland and Sweden and UK GP-HOSP datasets
 Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
GUIDANCE ON METHODOLOGY FOR ASSESSMENT OF FOREST FIRE INDUCED HEALTH EFFECTS
 GUIDANCE ON METHODOLOGY FOR ASSESSMENT OF FOREST FIRE INDUCED HEALTH EFFECTS David M. Mannino Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center
GUIDANCE ON METHODOLOGY FOR ASSESSMENT OF FOREST FIRE INDUCED HEALTH EFFECTS David M. Mannino Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center
Diesel Exhaust: Health Effects. Research Needs
 Diesel Exhaust: Health Effects and Research Needs Eric Garshick, MD, MOH Assistant Professor of Medicine VA Boston Healthcare System Channing Laboratory, Brigham and Womens Hospital Harvard Medical School
Diesel Exhaust: Health Effects and Research Needs Eric Garshick, MD, MOH Assistant Professor of Medicine VA Boston Healthcare System Channing Laboratory, Brigham and Womens Hospital Harvard Medical School
Air pollution as a major risk factor for cancer
 Air pollution as a major risk factor for cancer Dr Elisabete Weiderpass, MD, PHD Director-elect International Agency for Research on Cancer, Lyon, France IARC Hazard Assessment Volume 109 (2016) Outdoor
Air pollution as a major risk factor for cancer Dr Elisabete Weiderpass, MD, PHD Director-elect International Agency for Research on Cancer, Lyon, France IARC Hazard Assessment Volume 109 (2016) Outdoor
Asthma and air pollution: health effects and prevention
 Asthma and air pollution: health effects and prevention FuyuenYip PhD, MPH Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center for Environmental
Asthma and air pollution: health effects and prevention FuyuenYip PhD, MPH Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center for Environmental
Estimates and predictors of health care costs of esophageal adenocarcinoma: a population-based cohort study
 Thein et al. BMC Cancer (2018) 18:694 https://doi.org/10.1186/s12885-018-4620-2 RESEARCH ARTICLE Estimates and predictors of health care costs of esophageal adenocarcinoma: a population-based cohort study
Thein et al. BMC Cancer (2018) 18:694 https://doi.org/10.1186/s12885-018-4620-2 RESEARCH ARTICLE Estimates and predictors of health care costs of esophageal adenocarcinoma: a population-based cohort study
Ambient Air Pollution and Lung Cancer Risk in the Women s Health Initiative Observational Study. Shilpa N Gowda. A thesis
 Ambient Air Pollution and Lung Cancer Risk in the Women s Health Initiative Observational Study Shilpa N Gowda A thesis submitted in partial fulfillment of the requirements for the degree of Master of
Ambient Air Pollution and Lung Cancer Risk in the Women s Health Initiative Observational Study Shilpa N Gowda A thesis submitted in partial fulfillment of the requirements for the degree of Master of
Composition of PM 2.5 in the Urban Atmosphere Overall Episode PM 10>50μg/m 3
 Why worry about PM 2.5 and Black Carbon? Dr Ian S Mudway MRC-PHE Centre for Environment & Health, King s College London Composition of PM 2.5 in the Urban Atmosphere Overall Episode PM 10>50μg/m 3 Yin
Why worry about PM 2.5 and Black Carbon? Dr Ian S Mudway MRC-PHE Centre for Environment & Health, King s College London Composition of PM 2.5 in the Urban Atmosphere Overall Episode PM 10>50μg/m 3 Yin
Public health approaches to measuring the urban built environment and its effects on health: A focus on diabetes.
 Public health approaches to measuring the urban built environment and its effects on health: A focus on diabetes. Gillian Booth Marisa Creatore Li Ka Shing Knowledge Institute, St. Michael s Hospital Institute
Public health approaches to measuring the urban built environment and its effects on health: A focus on diabetes. Gillian Booth Marisa Creatore Li Ka Shing Knowledge Institute, St. Michael s Hospital Institute
Exposure to outdoor particulate air pollution is believed to
 ORIGINAL ARTICLE Long-Term Exposure to Outdoor Air Pollution and Incidence of Cardiovascular Diseases Richard W. Atkinson, a Iain M. Carey, a Andrew J. Kent, b Tjeerd P. van Staa, c H. Ross Anderson, d
ORIGINAL ARTICLE Long-Term Exposure to Outdoor Air Pollution and Incidence of Cardiovascular Diseases Richard W. Atkinson, a Iain M. Carey, a Andrew J. Kent, b Tjeerd P. van Staa, c H. Ross Anderson, d
Hotspot Analysis For Examining The Association Between Spatial Air Pollutants And Asthma In New York State, USA Using Kernel Density Estimation (KDE)
 Hotspot Analysis For Examining The Association Between Spatial Air Pollutants And Asthma In New York State, USA Using Kernel Density Estimation (KDE) Francis Tuluri 1, Amit Kr. Gorai 2, Aaron James 1 1
Hotspot Analysis For Examining The Association Between Spatial Air Pollutants And Asthma In New York State, USA Using Kernel Density Estimation (KDE) Francis Tuluri 1, Amit Kr. Gorai 2, Aaron James 1 1
Lucia Cea Soriano 1, Saga Johansson 2, Bergur Stefansson 2 and Luis A García Rodríguez 1*
 Cea Soriano et al. Cardiovascular Diabetology (2015) 14:38 DOI 10.1186/s12933-015-0204-5 CARDIO VASCULAR DIABETOLOGY ORIGINAL INVESTIGATION Open Access Cardiovascular events and all-cause mortality in
Cea Soriano et al. Cardiovascular Diabetology (2015) 14:38 DOI 10.1186/s12933-015-0204-5 CARDIO VASCULAR DIABETOLOGY ORIGINAL INVESTIGATION Open Access Cardiovascular events and all-cause mortality in
Linking Environment and Health Data
 Linking Environment and Health Data Experiences from the Netherlands Oscar Breugelmans Brigit Staatsen Contents 1. Developments in Environmental Public Health policy and research 2. Examples of recent
Linking Environment and Health Data Experiences from the Netherlands Oscar Breugelmans Brigit Staatsen Contents 1. Developments in Environmental Public Health policy and research 2. Examples of recent
Cardiovascular. Mathew Mercuri PhD(C), Sonia S Anand MD PhD FRCP(C)
 Cardiovascular Disease IN THE MÉTIS NATION OF ONTARIO Clinical Significance report March 2012 Mathew Mercuri PhD(C), Sonia S Anand MD PhD FRCP(C) Abstract Cardiovascular disease (CVD) is the leading cause
Cardiovascular Disease IN THE MÉTIS NATION OF ONTARIO Clinical Significance report March 2012 Mathew Mercuri PhD(C), Sonia S Anand MD PhD FRCP(C) Abstract Cardiovascular disease (CVD) is the leading cause
Canadian census mortality and cancer cohort: A linked cohort for the surveillance of occupational exposure and cancer
 1991 2010 Canadian census mortality and cancer cohort: A linked cohort for the surveillance of occupational exposure and cancer Jill Hardt Occupational Cancer Research Centre Cancer Care Ontario November
1991 2010 Canadian census mortality and cancer cohort: A linked cohort for the surveillance of occupational exposure and cancer Jill Hardt Occupational Cancer Research Centre Cancer Care Ontario November
Burden of Illness. Chapter 3 -- Highlights Document ONTARIO WOMEN'S HEALTH EQUITY REPORT
 Burden of Illness Chapter 3 -- Highlights Document A primary objective of the POWER (Project for an Ontario Women's Health Report) Study is to develop a tool that can be used to improve the health and
Burden of Illness Chapter 3 -- Highlights Document A primary objective of the POWER (Project for an Ontario Women's Health Report) Study is to develop a tool that can be used to improve the health and
Epidemiologic studies on health effects of air pollution in Japan
 Epidemiologic studies on health effects of air pollution in Japan Masayuki Shima 島正之 Hyogo College of Medicine, Japan 兵庫医科大学 Outlines Air pollution and its health effects in the past Pollution control
Epidemiologic studies on health effects of air pollution in Japan Masayuki Shima 島正之 Hyogo College of Medicine, Japan 兵庫医科大学 Outlines Air pollution and its health effects in the past Pollution control
EFFECTS OF BUFFER SIZE AND SHAPE ON ASSOCIATIONS BETWEEN THE BUILT ENVIRONMENT AND ENERGY BALANCE
 EFFECTS OF BUFFER SIZE AND SHAPE ON ASSOCIATIONS BETWEEN THE BUILT ENVIRONMENT AND ENERGY BALANCE PETER JAMES (HARVARD SCHOOL OF PUBLIC HEALTH) DAVID BERRIGAN (NATIONAL CANCER INSTITUTE) JAIME E HART (HARVARD
EFFECTS OF BUFFER SIZE AND SHAPE ON ASSOCIATIONS BETWEEN THE BUILT ENVIRONMENT AND ENERGY BALANCE PETER JAMES (HARVARD SCHOOL OF PUBLIC HEALTH) DAVID BERRIGAN (NATIONAL CANCER INSTITUTE) JAIME E HART (HARVARD
Analysis of lung cancer incidence relating to air pollution levels adjusting for cigarette smoking: a case-control study
 Air Pollution XIX 445 Analysis of lung cancer incidence relating to air pollution levels adjusting for cigarette smoking: a case-control study P. R. Band, H. Jiang & J. M. Zielinski Population Studies
Air Pollution XIX 445 Analysis of lung cancer incidence relating to air pollution levels adjusting for cigarette smoking: a case-control study P. R. Band, H. Jiang & J. M. Zielinski Population Studies
Long-term exposure to traffic-related air pollution and progression of carotid artery atherosclerosis: a prospective cohort study
 To cite: Gan WQ, Allen RW, Brauer M, et al. Long-term exposure to traffic-related air pollution and progression of carotid artery atherosclerosis: a prospective cohort study. BMJ Open 2014;4:e004743. doi:10.1136/bmjopen-2013-004743
To cite: Gan WQ, Allen RW, Brauer M, et al. Long-term exposure to traffic-related air pollution and progression of carotid artery atherosclerosis: a prospective cohort study. BMJ Open 2014;4:e004743. doi:10.1136/bmjopen-2013-004743
DIABETES MORTALITY IN NOVA SCOTIA FROM 1998 TO 2005: A DESCRIPTIVE ANALYSIS USING BOTH UNDERLYING AND MULTIPLE CAUSES OF DEATH
 DIABETES MORTALITY IN NOVA SCOTIA FROM 1998 TO 2005: A DESCRIPTIVE ANALYSIS USING BOTH UNDERLYING AND MULTIPLE CAUSES OF DEATH Alison Zwaagstra Health Information Analyst Network for End of Life Studies
DIABETES MORTALITY IN NOVA SCOTIA FROM 1998 TO 2005: A DESCRIPTIVE ANALYSIS USING BOTH UNDERLYING AND MULTIPLE CAUSES OF DEATH Alison Zwaagstra Health Information Analyst Network for End of Life Studies
Supplementary Online Content
 Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
New York State Department of Health Center for Environmental Health
 New York State Department of Health Center for Environmental Health March 2002 Evaluation of Asthma and Other Respiratory Hospital Admissions among Residents of ZIP Codes 14043 and 14227, Cheektowaga,
New York State Department of Health Center for Environmental Health March 2002 Evaluation of Asthma and Other Respiratory Hospital Admissions among Residents of ZIP Codes 14043 and 14227, Cheektowaga,
Relation between income, air pollution and mortality: a cohort study
 Research Recherche Relation between income, air pollution and mortality: a cohort study Murray M. Finkelstein, Michael Jerrett, Patrick DeLuca, Norm Finkelstein, Dave K. Verma, Kenneth Chapman, Malcolm
Research Recherche Relation between income, air pollution and mortality: a cohort study Murray M. Finkelstein, Michael Jerrett, Patrick DeLuca, Norm Finkelstein, Dave K. Verma, Kenneth Chapman, Malcolm
REPORT FROM THE CANADIAN CHRONIC DISEASE SURVEILLANCE SYSTEM: ASTHMA AND CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) IN CANADA, 2018
 REPORT FROM THE CANADIAN CHRONIC DISEASE SURVEILLANCE SYSTEM: ASTHMA AND CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) IN CANADA, 2018 P R O T E C T I N G A N D E M P O W E R I N G C A N A D I A N S T O
REPORT FROM THE CANADIAN CHRONIC DISEASE SURVEILLANCE SYSTEM: ASTHMA AND CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) IN CANADA, 2018 P R O T E C T I N G A N D E M P O W E R I N G C A N A D I A N S T O
The Effect of Patient Neighbourhood Income Level on the Purchase of Continuous Positive Airway
 Online Data Supplement The Effect of Patient Neighbourhood Income Level on the Purchase of Continuous Positive Airway Pressure Treatment among Sleep Apnea Patients Tetyana Kendzerska, MD, PhD, Andrea S.
Online Data Supplement The Effect of Patient Neighbourhood Income Level on the Purchase of Continuous Positive Airway Pressure Treatment among Sleep Apnea Patients Tetyana Kendzerska, MD, PhD, Andrea S.
ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study
 ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study Statistical modelling details We used Cox proportional-hazards
ESM1 for Glucose, blood pressure and cholesterol levels and their relationships to clinical outcomes in type 2 diabetes: a retrospective cohort study Statistical modelling details We used Cox proportional-hazards
Air Pollution and the Development of Posttransplant Chronic Lung Allograft Dysfunction
 American Journal of Transplantation 2014; 14: 2749 2757 Wiley Periodicals Inc. C Copyright 2014 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12909
American Journal of Transplantation 2014; 14: 2749 2757 Wiley Periodicals Inc. C Copyright 2014 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12909
Health Effects of Ambient Air Pollution
 Health Effects of Ambient Air Pollution Jennifer L. Peel, PhD, MPH jennifer.peel@colostate.edu Department of Environmental and Radiological Health Sciences Colorado State University Fort Collins, CO 5/18/2010
Health Effects of Ambient Air Pollution Jennifer L. Peel, PhD, MPH jennifer.peel@colostate.edu Department of Environmental and Radiological Health Sciences Colorado State University Fort Collins, CO 5/18/2010
Trends in adult obesity
 53 by Margot Shields and Michael Tjepkema Keywords: body mass index, body weight, income, smoking In recent years, the percentage of Canadian adults with excess weight has increased considerably, part
53 by Margot Shields and Michael Tjepkema Keywords: body mass index, body weight, income, smoking In recent years, the percentage of Canadian adults with excess weight has increased considerably, part
Effect modification of perinatal exposure to air pollution and childhood asthma incidence
 ORIGINAL ARTICLE ASTHMA Effect of perinatal exposure to air pollution and childhood asthma incidence Éric Lavigne 1,2, Marc-André Bélair 3, Daniel Rodriguez Duque 3, Minh T. Do 4, David M. Stieb 2,5, Perry
ORIGINAL ARTICLE ASTHMA Effect of perinatal exposure to air pollution and childhood asthma incidence Éric Lavigne 1,2, Marc-André Bélair 3, Daniel Rodriguez Duque 3, Minh T. Do 4, David M. Stieb 2,5, Perry
Air Pollution and Stroke Risk in the WHI. Gregory A. Wellenius, ScD Department of Epidemiology Brown University
 Air Pollution and Stroke Risk in the WHI Gregory A. Wellenius, ScD Department of Epidemiology Brown University London Smog, 1952 In central London the visibility remained below 500 meters continuously
Air Pollution and Stroke Risk in the WHI Gregory A. Wellenius, ScD Department of Epidemiology Brown University London Smog, 1952 In central London the visibility remained below 500 meters continuously
etable 3.1: DIABETES Name Objective/Purpose
 Appendix 3: Updating CVD risks Cardiovascular disease risks were updated yearly through prediction algorithms that were generated using the longitudinal National Population Health Survey, the Canadian
Appendix 3: Updating CVD risks Cardiovascular disease risks were updated yearly through prediction algorithms that were generated using the longitudinal National Population Health Survey, the Canadian
Health impact assessment in the framework of global and regional AQ modelling
 Health impact assessment in the framework of global and regional AQ modelling Rita Van Dingenen European Commission, Joint Research Centre Air pollution and health Ambient air pollution (individual) risk
Health impact assessment in the framework of global and regional AQ modelling Rita Van Dingenen European Commission, Joint Research Centre Air pollution and health Ambient air pollution (individual) risk
Traffic pollution and the incidence of cardio-respiratory outcomes in an adult cohort in London
 Traffic pollution and the incidence of cardio-respiratory outcomes in an adult cohort in London IM Carey 1, HR Anderson 2, RW Atkinson 1, S Beevers 2, DG Cook 1, D Dajnak 2, J Gulliver 3, FJ Kelly 2. 1
Traffic pollution and the incidence of cardio-respiratory outcomes in an adult cohort in London IM Carey 1, HR Anderson 2, RW Atkinson 1, S Beevers 2, DG Cook 1, D Dajnak 2, J Gulliver 3, FJ Kelly 2. 1
Outdoor environment. Introduction. Pollution: composition/sources. Key points
 6 Outdoor environment Introduction i Key points A large proportion of the European population lives in areas with unhealthy outdoor air quality, and is thus unable to avoid exposure to the harmful effects
6 Outdoor environment Introduction i Key points A large proportion of the European population lives in areas with unhealthy outdoor air quality, and is thus unable to avoid exposure to the harmful effects
Acute and chronic exposure to urban air
 Eur Respir J 2009; 34: 316 323 DOI: 10.1183/09031936.00138908 CopyrightßERS Journals Ltd 2009 Acute effects of outdoor air pollution on forced expiratory volume in 1 s: a panel study of schoolchildren
Eur Respir J 2009; 34: 316 323 DOI: 10.1183/09031936.00138908 CopyrightßERS Journals Ltd 2009 Acute effects of outdoor air pollution on forced expiratory volume in 1 s: a panel study of schoolchildren
Health impacts of diesel emissions
 Health impacts of diesel emissions 13 June 2014 Christine Cowie www.smh.com.au Diesel exhaust particles DEP consist of a carbon core surrounded by trace metals, quinones, VOCs The solid particulate fraction
Health impacts of diesel emissions 13 June 2014 Christine Cowie www.smh.com.au Diesel exhaust particles DEP consist of a carbon core surrounded by trace metals, quinones, VOCs The solid particulate fraction
Health effects of wood burning. Dr. M.E. Gerlofs-Nijland RIVM, The Netherlands
 Health effects of wood burning Dr. M.E. Gerlofs-Nijland RIVM, The Netherlands 1 Outline Introduction wood smoke and particulate matter In vitro cell culture studies In vivo animal studies Comparison effects
Health effects of wood burning Dr. M.E. Gerlofs-Nijland RIVM, The Netherlands 1 Outline Introduction wood smoke and particulate matter In vitro cell culture studies In vivo animal studies Comparison effects
RESEARCH. Dagfinn Aune, 1,2 Abhijit Sen, 1 Manya Prasad, 3 Teresa Norat, 2 Imre Janszky, 1 Serena Tonstad, 3 Pål Romundstad, 1 Lars J Vatten 1
 open access BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants Dagfinn Aune, 1,2 Abhijit
open access BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants Dagfinn Aune, 1,2 Abhijit
Ultrafine particles around Amsterdam Schipol airport and potential implications for human health. Dr. Miriam E Gerlofs-Nijland
 Ultrafine particles around Amsterdam Schipol airport and potential implications for human health Dr. Miriam E Gerlofs-Nijland 1 Disclaimer The contents of this presentation does not necessarily reflect
Ultrafine particles around Amsterdam Schipol airport and potential implications for human health Dr. Miriam E Gerlofs-Nijland 1 Disclaimer The contents of this presentation does not necessarily reflect
The Burden of Kidney Disease in Rural & Northern Ontario
 Ontario Branch The Burden of Kidney Disease in Rural & Northern Ontario Contact: Janet Bick Director, Policy & Programs The Kidney Foundation of Canada Ontario Branch Tel: 905-278-3003/1.800-387-4474 ext.4970
Ontario Branch The Burden of Kidney Disease in Rural & Northern Ontario Contact: Janet Bick Director, Policy & Programs The Kidney Foundation of Canada Ontario Branch Tel: 905-278-3003/1.800-387-4474 ext.4970
Associations of Ambient Air Pollution with Chronic Obstructive Pulmonary Disease Hospitalization and Mortality
 Associations of Ambient Air Pollution with Chronic Obstructive Pulmonary Disease Hospitalization and Mortality Wen Qi Gan 1,2, J. Mark FitzGerald 3,4, Chris Carlsten 3,4,5, Mohsen Sadatsafavi 3,4, and
Associations of Ambient Air Pollution with Chronic Obstructive Pulmonary Disease Hospitalization and Mortality Wen Qi Gan 1,2, J. Mark FitzGerald 3,4, Chris Carlsten 3,4,5, Mohsen Sadatsafavi 3,4, and
Atmospheric particulate matter and hospital admission due to lower respiratory tract infection: a
 Med J Chin PLA, Vol. 41, No. 2, February 1, 2016 123 (PM 10 /PM 2.5 ) [ ] Pearson logistic Pearson PM 2.5 PM 10 SO 2 NO 2 CO O 3 PM 2.5 5d PM 10 10 g/m 3 OR (95%CI) 1.010(1.005~1.015) 1.006(1.003~1.009)
Med J Chin PLA, Vol. 41, No. 2, February 1, 2016 123 (PM 10 /PM 2.5 ) [ ] Pearson logistic Pearson PM 2.5 PM 10 SO 2 NO 2 CO O 3 PM 2.5 5d PM 10 10 g/m 3 OR (95%CI) 1.010(1.005~1.015) 1.006(1.003~1.009)
Income-related inequalities for injury hospitalizations in Canada: trends and policy approaches
 Income-related inequalities for injury hospitalizations in Canada: trends and policy approaches 1 Income-related inequalities for injury hospitalizations in Canada: trends and policy approaches 2014 CAHSPR
Income-related inequalities for injury hospitalizations in Canada: trends and policy approaches 1 Income-related inequalities for injury hospitalizations in Canada: trends and policy approaches 2014 CAHSPR
Association between Long-term Exposure to Outdoor Air Pollution and Mortality in China: a Cohort Study
 Association between Long-term Exposure to Outdoor Air Pollution and Mortality in China: a Cohort Study Haidong Kan ( 阚海东 ), PhD Fudan University ( 复旦大学 ) A&WMA International Specialty Conference Xi an,
Association between Long-term Exposure to Outdoor Air Pollution and Mortality in China: a Cohort Study Haidong Kan ( 阚海东 ), PhD Fudan University ( 复旦大学 ) A&WMA International Specialty Conference Xi an,
SMOKING STAGES OF CHANGE KEY MESSAGES
 KEY MESSAGES In Peel among current daily or occasional smokers: o 19% are not thinking are not thinking about quitting (pre-contemplation stage) in the next six months; o 21% are thinking about quitting
KEY MESSAGES In Peel among current daily or occasional smokers: o 19% are not thinking are not thinking about quitting (pre-contemplation stage) in the next six months; o 21% are thinking about quitting
APPENDIX J Health Studies
 APPENDIX J Health Studies Air Quality and Human Health Assessment - i - January 2005 TABLE OF CONTENTS 1.0 INTRODUCTION... 1 2.0 STRUCTURE OF THE REVIEW... 1 3.0 CANADA GENERAL POPULATON... 2 3.1 HEALTH
APPENDIX J Health Studies Air Quality and Human Health Assessment - i - January 2005 TABLE OF CONTENTS 1.0 INTRODUCTION... 1 2.0 STRUCTURE OF THE REVIEW... 1 3.0 CANADA GENERAL POPULATON... 2 3.1 HEALTH
Nitrogen dioxide and mortality: review and meta-analysis of long-term studies
 ERJ Express. Published on February 20, 2014 as doi: 10.1183/09031936.00114713 REVIEW IN PRESS CORRECTED PROOF Nitrogen dioxide and mortality: review and meta-analysis of long-term studies Annunziata Faustini
ERJ Express. Published on February 20, 2014 as doi: 10.1183/09031936.00114713 REVIEW IN PRESS CORRECTED PROOF Nitrogen dioxide and mortality: review and meta-analysis of long-term studies Annunziata Faustini
ParkScore. Youth Physical Activity. Outdoor Spaces & Buildings
 ParkScore Borrowed from the Trust for Public Land's framework, this index measures how well cities are meeting the community s park needs. Higher scores indicate better availability of and access to quality
ParkScore Borrowed from the Trust for Public Land's framework, this index measures how well cities are meeting the community s park needs. Higher scores indicate better availability of and access to quality
Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009
 Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
Western University Scholarship@Western Electronic Thesis and Dissertation Repository June 2015 Secular Trends in Cardiovascular Disease in Kidney Transplant Recipients: 1994 to 2009 Ngan Lam The University
CIHI Trends in Health Inequalities in Canada. APHEO September 15, 2014
 CIHI Trends in Health Inequalities in Canada APHEO September 15, 2014 1 Outline and Objectives Introduction to CIHI and CPHI Work in Health Inequality Trends in Health Inequalities Project Questions /
CIHI Trends in Health Inequalities in Canada APHEO September 15, 2014 1 Outline and Objectives Introduction to CIHI and CPHI Work in Health Inequality Trends in Health Inequalities Project Questions /
Quantification of increase in Blood pressure due to Urban Air Pollution in terms of AQI with reduction in Forced vital capacity of Lungs.
 American International Journal of Research in Formal, Applied & Natural Sciences Available online at http://www.iasir.net ISSN (Print): 8-777, ISSN (Online): 8-78, ISSN (CD-ROM): 8-79 AIJRFANS is a refereed,
American International Journal of Research in Formal, Applied & Natural Sciences Available online at http://www.iasir.net ISSN (Print): 8-777, ISSN (Online): 8-78, ISSN (CD-ROM): 8-79 AIJRFANS is a refereed,
AHA Clinical Science Special Report: November 10, 2015
 www.canheart.ca High-density lipoprotein cholesterol and cause-specific mortality: A population-based study of more than 630,000 individuals without prior cardiovascular conditions Dennis T. Ko, MD, MSc;
www.canheart.ca High-density lipoprotein cholesterol and cause-specific mortality: A population-based study of more than 630,000 individuals without prior cardiovascular conditions Dennis T. Ko, MD, MSc;
Canada: Equitable Cancer Care Access and Outcomes? Historic Observational Evidence: Incidence Versus Survival, Canada Versus the United States
 Canada: Equitable Cancer Care Access and Outcomes? Historic Observational Evidence: Incidence Versus Survival, Canada Versus the United States This work is funded by the: Canadian Institutes of Health
Canada: Equitable Cancer Care Access and Outcomes? Historic Observational Evidence: Incidence Versus Survival, Canada Versus the United States This work is funded by the: Canadian Institutes of Health
Immigrant Density, Sense of Community Belonging, and Suicidal Ideation among Racial Minority and White Immigrants in Canada
 Immigrant Density, Sense of Community Belonging, and Suicidal Ideation among Racial Minority and White Immigrants in Canada Stephen W. Pan 1 & Richard M. Carpiano 2 1 University of British Columbia School
Immigrant Density, Sense of Community Belonging, and Suicidal Ideation among Racial Minority and White Immigrants in Canada Stephen W. Pan 1 & Richard M. Carpiano 2 1 University of British Columbia School
TRANSPHORM. Deliverable D3.2, type 2
 TRANSPHORM Transport related Air Pollution and Health impacts Integrated Methodologies for Assessing Particulate Matter Collaborative Project, Large-scale Integrating Project SEVENTH FRAMEWORK PROGRAMME
TRANSPHORM Transport related Air Pollution and Health impacts Integrated Methodologies for Assessing Particulate Matter Collaborative Project, Large-scale Integrating Project SEVENTH FRAMEWORK PROGRAMME
US power plant carbon standards and clean air and health co-benefits
 US power plant carbon standards and clean air and health co-benefits Emissions Modeling For each scenario, we used emissions output from ICF International s Integrated Planning Model (IPM) conducted by
US power plant carbon standards and clean air and health co-benefits Emissions Modeling For each scenario, we used emissions output from ICF International s Integrated Planning Model (IPM) conducted by
DAILY SMOKERS - AVERAGE NUMBER OF CIGARETTES SMOKED DAILY KEY MESSAGES
 DAILY SMOKERS - AVERAGE KEY MESSAGES On average, daily smokers in Peel smoke 12 cigarettes per day (2011/2012) and this has remained stable over time. Daily smokers in Ontario smoke slightly more per day
DAILY SMOKERS - AVERAGE KEY MESSAGES On average, daily smokers in Peel smoke 12 cigarettes per day (2011/2012) and this has remained stable over time. Daily smokers in Ontario smoke slightly more per day
REMINGTON PARK CANCER CLUSTER INVESTIGATION REPORT TOWN HALL MEETING
 REMINGTON PARK CANCER CLUSTER INVESTIGATION REPORT TOWN HALL MEETING Dr. Gary Kirk, Windsor-Essex County Health Unit Dr. Elaina MacIntyre, Public Health Ontario Thursday, September 8, 2016 INTRODUCTION
REMINGTON PARK CANCER CLUSTER INVESTIGATION REPORT TOWN HALL MEETING Dr. Gary Kirk, Windsor-Essex County Health Unit Dr. Elaina MacIntyre, Public Health Ontario Thursday, September 8, 2016 INTRODUCTION
Annette Peters. Research Needs for Aerosols and Health
 Research Needs for Aerosols and Health Annette Peters Helmholtz Zentrum München, Institute of Epidemiology, Neuherberg, Germany Harvard School of Public Health, Department of Environmental Health, Boston,
Research Needs for Aerosols and Health Annette Peters Helmholtz Zentrum München, Institute of Epidemiology, Neuherberg, Germany Harvard School of Public Health, Department of Environmental Health, Boston,
Objective: To describe a new approach to neighborhood effects studies based on residential mobility and demonstrate this approach in the context of
 Objective: To describe a new approach to neighborhood effects studies based on residential mobility and demonstrate this approach in the context of neighborhood deprivation and preterm birth. Key Points:
Objective: To describe a new approach to neighborhood effects studies based on residential mobility and demonstrate this approach in the context of neighborhood deprivation and preterm birth. Key Points:
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH
 Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Understanding the Potential Ultrafine Particle Pollution Problem and its Impact on California s Air Quality
 South Coast Air Quality Management District Ultrafine Particle Conference April 30 May 2, 2006 Understanding the Potential Ultrafine Particle Pollution Problem and its Impact on California s Air Quality
South Coast Air Quality Management District Ultrafine Particle Conference April 30 May 2, 2006 Understanding the Potential Ultrafine Particle Pollution Problem and its Impact on California s Air Quality
Takashi Yagisawa 1,2*, Makiko Mieno 1,3, Norio Yoshimura 1,4, Kenji Yuzawa 1,5 and Shiro Takahara 1,6
 Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Clinical Track. Relationships Between Fine Particulate Air Pollution, Cardiometabolic Disorders, and Cardiovascular Mortality
 Clinical Track Relationships Between Fine Particulate Air Pollution, Cardiometabolic Disorders, and Cardiovascular Mortality C. Arden Pope III, Michelle C. Turner, Richard T. Burnett, Michael Jerrett,
Clinical Track Relationships Between Fine Particulate Air Pollution, Cardiometabolic Disorders, and Cardiovascular Mortality C. Arden Pope III, Michelle C. Turner, Richard T. Burnett, Michael Jerrett,
Adult overweight and obesity
 Facts on Adult overweight and obesity March 2017 in Durham Region Highlights In 2013/2014, 57 per cent of Durham Region adults 18 and older were overweight or obese. Rates for both Durham Region and Ontario
Facts on Adult overweight and obesity March 2017 in Durham Region Highlights In 2013/2014, 57 per cent of Durham Region adults 18 and older were overweight or obese. Rates for both Durham Region and Ontario
Data Brief. Exploring Urban Environments and Inequalities in Health
 Data Brief Exploring Urban Environments and Inequalities in Health Halifax Census Metropolitan Area In 008, the Canadian Population Health Initiative (CPHI), a part of the Canadian Institute for Health
Data Brief Exploring Urban Environments and Inequalities in Health Halifax Census Metropolitan Area In 008, the Canadian Population Health Initiative (CPHI), a part of the Canadian Institute for Health
Cigarette smoking is the number one cause of preventable death and disease in Ontario. Smoking kills half of its long-term users.
 HEALTH SURVEILLANCE INDICATORS: SMOKING Public Health Relevance Cigarette smoking is the number one cause of preventable death and disease in Ontario. Smoking kills half of its long-term users. Smoking
HEALTH SURVEILLANCE INDICATORS: SMOKING Public Health Relevance Cigarette smoking is the number one cause of preventable death and disease in Ontario. Smoking kills half of its long-term users. Smoking
Online supplementary material
 Online supplementary material Add-on long-acting β2-agonist (LABA) in a separate inhaler as asthma step-up therapy versus increased dose of inhaled corticosteroid (ICS) or ICS/LABA combination inhaler
Online supplementary material Add-on long-acting β2-agonist (LABA) in a separate inhaler as asthma step-up therapy versus increased dose of inhaled corticosteroid (ICS) or ICS/LABA combination inhaler
Disability in long-term care residents explained by prevalent geriatric syndromes, not long-term care home characteristics: a cross-sectional study
 Lane et al. BMC Geriatrics (2017) 17:49 DOI 10.1186/s12877-017-0444-1 RESEARCH ARTICLE Open Access Disability in long-term care residents explained by prevalent geriatric syndromes, not long-term care
Lane et al. BMC Geriatrics (2017) 17:49 DOI 10.1186/s12877-017-0444-1 RESEARCH ARTICLE Open Access Disability in long-term care residents explained by prevalent geriatric syndromes, not long-term care
Measuring health care inequalities using the Census- DAD data linkage
 Measuring health care inequalities using the Census- DAD data linkage Erin Pichora, Program Lead Canadian Population Health Initiative Canadian Institute for Health Information November 14, 2017 Epichora@cihi.ca
Measuring health care inequalities using the Census- DAD data linkage Erin Pichora, Program Lead Canadian Population Health Initiative Canadian Institute for Health Information November 14, 2017 Epichora@cihi.ca
HEALTH SURVEILLANCE INDICATORS: COLORECTAL CANCER. Public Health Relevance. Highlights
 HEALTH SURVEILLANCE INDICATORS: COLORECTAL CANCER Public Health Relevance Colorectal cancer is the third most diagnosed cancer in Ontario. It is the second leading cause of cancer mortality in Ontario
HEALTH SURVEILLANCE INDICATORS: COLORECTAL CANCER Public Health Relevance Colorectal cancer is the third most diagnosed cancer in Ontario. It is the second leading cause of cancer mortality in Ontario
8/10/2012. Education level and diabetes risk: The EPIC-InterAct study AIM. Background. Case-cohort design. Int J Epidemiol 2012 (in press)
 Education level and diabetes risk: The EPIC-InterAct study 50 authors from European countries Int J Epidemiol 2012 (in press) Background Type 2 diabetes mellitus (T2DM) is one of the most common chronic
Education level and diabetes risk: The EPIC-InterAct study 50 authors from European countries Int J Epidemiol 2012 (in press) Background Type 2 diabetes mellitus (T2DM) is one of the most common chronic
Asthma and Chronic Obstructive Pulmonary Disease (COPD) Prevalence and Health Services Use in Ontario Métis: A Population-Based Cohort Study
 Asthma and Chronic Obstructive Pulmonary Disease (COPD) Prevalence and Health Services Use in Ontario Métis: A Population-Based Cohort Study Andrea S. Gershon 1,2,3,4 *, Saba Khan 2, Julie Klein-Geltink
Asthma and Chronic Obstructive Pulmonary Disease (COPD) Prevalence and Health Services Use in Ontario Métis: A Population-Based Cohort Study Andrea S. Gershon 1,2,3,4 *, Saba Khan 2, Julie Klein-Geltink
REGULATORY REGISTRY FEEDBACK FORM. Proposed Places of Use Regulations under the Cannabis Act, 2017
 REGULATORY REGISTRY FEEDBACK FORM Proposed Places of Use Regulations under the Cannabis Act, 2017 The Ontario government would like your feedback on regulatory proposals related to where cannabis can be
REGULATORY REGISTRY FEEDBACK FORM Proposed Places of Use Regulations under the Cannabis Act, 2017 The Ontario government would like your feedback on regulatory proposals related to where cannabis can be
HEALTH SURVEILLANCE INDICATORS: LUNG CANCER. Public Health Relevance. Highlights.
 HEALTH SURVEILLANCE INDICATORS: LUNG CANCER Public Health Relevance Lung cancer is one of the top three most commonly diagnosed cancers among both males and females. Lung cancer has a very low survival
HEALTH SURVEILLANCE INDICATORS: LUNG CANCER Public Health Relevance Lung cancer is one of the top three most commonly diagnosed cancers among both males and females. Lung cancer has a very low survival
Influenza Vaccination Coverage in British Columbia Canadian Community Health Survey 2011 & 2012
 Background The Canadian Community Health Survey (CCHS) is a cross-sectional survey that collects information related to the health status, health care utilization and health determinants of the Canadian
Background The Canadian Community Health Survey (CCHS) is a cross-sectional survey that collects information related to the health status, health care utilization and health determinants of the Canadian
Incidence of diabetes among postmenopausal breast cancer survivors
 Diabetologia (2013) 56:476 483 DOI 10.1007/s00125-012-2793-9 ARTICLE Incidence of diabetes among postmenopausal breast cancer survivors L. L. Lipscombe & W. W. Chan & L. Yun & P. C. Austin & G. M. Anderson
Diabetologia (2013) 56:476 483 DOI 10.1007/s00125-012-2793-9 ARTICLE Incidence of diabetes among postmenopausal breast cancer survivors L. L. Lipscombe & W. W. Chan & L. Yun & P. C. Austin & G. M. Anderson
The Association of Air Pollution With the Patients Visits to the Department of Respiratory Diseases
 Elmer ress Original Article J Clin Med Res. 2015;7(7):551-555 The Association of Air Pollution With the Patients Visits to the Department of Respiratory Diseases Yanran Cai a, Yumeng Shao a, Chenggang
Elmer ress Original Article J Clin Med Res. 2015;7(7):551-555 The Association of Air Pollution With the Patients Visits to the Department of Respiratory Diseases Yanran Cai a, Yumeng Shao a, Chenggang
