Electromagnetic Navigation Bronchoscopy Performed by Thoracic Surgeons: One Center s Early Success
|
|
|
- Ann Holt
- 6 years ago
- Views:
Transcription
1 Electromagnetic Navigation Bronchoscopy Performed by Thoracic Surgeons: One Center s Early Success Daryl Phillip Pearlstein, MD, Curtis C. Quinn, MD, Charles C. Burtis, BS, Kwang Woo Ahn, PhD, and Aaron J. Katch, MS Divisions of Cardiothoracic Surgery, and Biostatistics, Medical College of Wisconsin, Milwaukee; Division of Cardiothoracic Surgery, Waukesha Memorial Hospital, Waukesha; and Aurora Advanced Healthcare, Milwaukee, Wisconsin Background. Multiple studies by pulmonologists have demonstrated that electromagnetic navigation bronchoscopy (ENB) can, with high diagnostic yields and low complication rates, diagnose pulmonary lesions. We believe thoracic surgeons can perform this technique with excellent early results. Methods. A retrospective analysis was conducted of the first consecutive 104 patients undergoing diagnostic ENB by 2 thoracic surgeons between April 2008 and October Procedures utilized general anesthesia and rapid on-site examination (ROSE) of cytopathology. All pulmonary lesions were suspicious for malignancy. Patients having negative biopsies subsequently underwent additional procedures or follow-up imaging. True negative biopsies were defined as lesions removed surgically and proven benign, lesions that disappeared on subsequent imaging, and lesions demonstrating stability over a 2-year period. Results. Of 104 patients, 3 were excluded due to insufficient follow-up. The remaining 101 patients had a median lesion size of 2.8 cm. Sixty-seven (82%) of the 82 lesions that were determined malignant had a positive diagnosis upon ENB. Of the 34 lesions without a positive ENB biopsy, 19 (56%) were categorized as true negatives: 8 had benign surgical biopsies, 6 disappeared, and 5 demonstrated stability. Consequently, 86 of 101 cases had an accurate ENB biopsy for a diagnostic yield of 85%. There was insufficient evidence to demonstrate an association between lesion size and diagnostic accuracy. There were 6 pneumothoraces (5.8%). Conclusions. It is possible for thoracic surgeons to perform ENB with early success. The high diagnostic yields in this study may be attributed to the routine utilization of ROSE and general anesthesia, which preserves computed tomographic-to-body divergence. (Ann Thorac Surg 2012;93:944 50) 2012 by The Society of Thoracic Surgeons Accepted for publication Nov 2, Presented at the Forty-seventh Annual Meeting of The Society of Thoracic Surgeons, San Diego, CA, Jan 31 Feb 2, Address correspondence to Dr Pearlstein, Division of Cardiothoracic Surgery Medical College of Wisconsin, Froedtert Specialty Clinics, 9200 W Wisconsin Ave, Milwaukee, WI 53226; dpearlstein@mcw.edu. Lung cancer remains the number one cancer killer in the United States [1]. While screening trials with computed tomography (CT) scans demonstrate that early detection of suspicious nodules in high-risk patients is very realistic [2 4], tissue diagnosis remains a challenge in which the algorithm is yet to be clearly defined. If lung cancer screening becomes commonplace, there will be a large volume of newly discovered pulmonary nodules, of which greater than 90% will be benign [4, 5]. Furthermore, many of these suspicious nodules will be discovered in patients with severe pulmonary disease and comorbid conditions which would make them poor operative candidates. Physicians managing these patients will need to establish effective, nonoperative ways of making accurate tissue diagnoses of these lesions to avoid unnecessary, and potentially hazardous, operations in large numbers of high-risk patients. Traditionally, nonsurgical biopsies of pulmonary nodules relied on either conventional bronchoscopy with transbronchial fine needle aspiration or percutaneous transthoracic needle aspiration with CT guidance. Conventional bronchoscopy with fine needle aspiration, while safe, has very low diagnostic yields for peripheral lesions; in some cases as low as 14% to 30% [6]. The CT-guided biopsies performed by interventional radiologists have much better diagnostic yields, but are generally applicable only to pulmonary lesions situated in the outer third of the lung and suffer from a high pneumothorax rate in patients with advanced chronic obstructive pulmonary disease (COPD); therefore, they may be considered unsuitable for this group of patients [7, 8]. Within the past several years electromagnetic navigation bronchoscopy (ENB) has proven very effective at being able to assess pulmonary nodules accurately with very low complication rates, even in patients with advanced COPD [9]. The goal of ENB is to use computer guidance to enable bronchoscopic access to pulmonary lesions deep within the lung parenchyma. In general, Dr Quinn discloses that he has a financial relationship with SuperDimension by The Society of Thoracic Surgeons /$36.00 Published by Elsevier Inc doi: /j.athoracsur
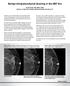
2 Ann Thorac Surg PEARLSTEIN ET AL 2012;93: ENB PERFORMED BY THORACIC SURGEONS 945 these lesions, because of their depth or small size could not be reliably biopsied by traditional bronchoscopy. The main advantage of using ENB to establish the diagnosis of a suspicious pulmonary nodule is that the visceral pleura is not violated. Consequently, patients with advanced COPD are not exposed to the risks of pneumothorax or prolonged air leak, which are inherent in percutaneous biopsy and open lung biopsy. An additional advantage of ENB is the ability to place fiducial markers within pulmonary nodules that can then be used for stereotactic body radiation therapy (SBRT) if the lesion is proven to be malignant. This advantage is especially significant for high-risk patients who may benefit from SBRT as an alternative to surgical resection. The diagnostic yields of ENB in large series of more than 40 patients range from 62% to 74% [9, 10 14]. Virtually all of these studies have been conducted and published by interventional pulmonologists who, in most cases, have subspecialty expertise and limit their practice to interventional bronchology. These highly specialized physicians, while very skilled, are limited in number and are not available in most medical centers. Another shortcoming of the published experience of ENB biopsies is that nearly all series tend to include relatively small numbers of patients, generally less than 60 cases. Below is the initial experience with ENB in a mediumsized community hospital. This 300-bed hospital has a robust and busy multidisciplinary thoracic center but does not have access to a dedicated interventional pulmonologist. Therefore, 2 thoracic surgeons were approached to see if they would be interested in learning this new technique. The thought being thoracic surgeons might posses the appropriate skill set to effectively utilize this new technology. The hope and expectation was to demonstrate that thoracic surgeons, with no previous experience in ENB, could learn this technique and have excellent early results. It was felt that this would provide a safe and valuable alternative for diagnosing and treating lung cancer in a group of patients who were felt to be at increased risk for surgery. The following is a summary of the first 104 patients who underwent ENB for the purpose of diagnosing pulmonary lesions suspicious for malignancy. Patients and Methods A retrospective analysis was conducted of the first consecutive 104 patients undergoing diagnostic ENB by 2 thoracic surgeons at a single center (Waukesha Memorial Hospital) between April 2008 and October Of the 104 patients there were 64 males and 40 females. Their ages ranged from 44 to 92 years (mean 69). All patients had pulmonary lesions suspicious for malignancy. Of note, the Institutional Review Board at Waukesha Memorial Hospital reviewed this study in its planning phase. The Institutional Review Board approved the study and decided that, although this study involves human subjects, there was no need for individual patient consent because the study is retrospective and no patient identifiers are included. All high-risk patients with pulmonary nodules suspicious for malignancy were presented at a weekly multidisciplinary thoracic oncology conference. In regular attendance at this conference were thoracic surgeons, medical oncologists, radiation oncologists, pulmonologists, interventional radiologists, and pathologists. When discussing these patients the following clinical material was reviewed and discussed: (1) chest CT showing 1 or more suspicious nodules; (2) positron emission tomography (PET) scan; and (3) pulmonary function studies. The group reviewed each patient s information and a consensus opinion was reached regarding whether to proceed with ENB as opposed to some other diagnostic method or follow-up imaging. Although no rigid criteria were used, the factors which led the group to recommend ENB were the following: (1) a nodule highly suspicious for malignancy based on CT morphology and increased metabolic activity on PET scan; (2) nodule felt by interventional radiologists to be unsuitable for CTguided biopsy either because of its depth, small size, or the patient s severe COPD; (3) patient felt to be at high risk for surgical resection due to comorbidities or advanced pulmonary disease; and (4) the absence of other suspicious lesions or mediastinal adenopathy which might be approachable by standard interventional means, mediastinoscopy, or endobronchial ultrasound. Although both thoracic surgeons involved had a rich experience in conventional bronchoscopy, the ENB training regimen for both surgeons was limited to a weekend course provided by the manufacturer of the system (SuperDimension, Minneapolis, MN). Each procedure was done using the first generation SuperDimension system and software (inreach system Version 4.3.4). The procedures were performed in a bronchoscopy suite in a room that was set up and mapped according to the SuperDimension specifications. When the surgeons initially planned the conduct of the procedures it was decided that each case would utilize general endotracheal anesthesia (GA) with muscle relaxation and rapid on-site evaluation of the cytopathology (ROSE). These decisions were made with the intention of maximizing the early yields for this procedure. The technical details of ENB consist of 4 basic elements. (1) Computer software that utilizes a thin-slice CT to create a three-dimensional rendering of the lung and tracheobronchial tree, which can then be used for virtual bronchoscopy. (2) An electromagnetic field encompassing the patients thorax so that the real anatomy, as viewed with a flexible bronchoscope, can be merged with the computer-generated (virtual) anatomy by the use of standard, easily recognizable landmarks in the tracheobronchial tree (eg, carina, takeoff of the right upper lobe bronchus, bifurcation between the left upper and lower lobes; Fig 1). Usually, between 5 and 7 of these easily recognized structures are marked in the computer planning phase and are known as registration points. Once these registration points are identified during the actual bronchoscopy, the computer software correlates how closely the real anatomy matches the three-dimensional computer-generated (virtual) anatomy. This correlation is known as the CT-to-body divergence (CTBD) and, in general, a CTBD less than 5 mm is considered acceptable.
3 946 PEARLSTEIN ET AL Ann Thorac Surg ENB PERFORMED BY THORACIC SURGEONS 2012;93: Fig 1. Registration points (purple) merging computer-generated anatomy (A) with patient s real anatomy (B). (Reproduced with permission from SuperDimension, Inc.) (3) A locatable guide catheter that fits through the working or suction channel of a bronchoscope with a steering mechanism. Because the locatable guide catheter is recognizable within the electromagnetic field, it can be navigated through the small airways of the lung toward peripheral lesions not reachable by conventional bronchoscopy. (4) A hollow, extended working channel that fits tightly around the locatable guide catheter like a sleeve and can be secured (or wedged) in a small peripheral airway. Once the working channel is secured in an airway the guidance catheter slides out and the channel can be used for the passing of diagnostic instruments such as brushes, aspirating needles, and biopsy forceps (Fig 2). During each ENB procedure, slides were prepared and reviewed on site by a cytopathologist. Although some specimens were considered very likely to be malignant, these assessments were always considered preliminary and were mainly used by the operator to decide whether or not to continue to pursue more biopsies. To add credence to this study, all specimens that were categorized as positive for malignancy or true positives were processed, analyzed, and reviewed by multiple pathologists within their department and felt to be clearly diagnostic of carcinoma. We assumed there were no false positives. Any specimens that were felt to be equivocal by this group of pathologists were labeled suspicious, but not diagnostic of carcinoma and, for the purposes of our study, were placed in the negative for malignancy group. Patients having biopsies negative for malignancy subsequently underwent additional diagnostic procedures (either percutaneous biopsy with CT guidance or surgical biopsy) or were followed closely with imaging. Again, all of these cases were discussed at the weekly multidisciplinary thoracic oncology conference. A consensus decision was reached about whether to recommend a highrisk percutaneous biopsy or surgical resection versus following closely with serial CT or PET scans. This recommendation was based on many variables (including the patient s wishes) but strongly considered the patient s overall lung function and performance status. True negative biopsies were defined as lesions that were removed surgically and found to be benign, lesions which disappeared on subsequent imaging, and lesions that demonstrated stability over a 2-year period of follow-up imaging. False negative biopsies were defined as lesions that were initially biopsied by ENB and were not diagnostic of malignancy but were subsequently found to be malignant by percutaneous or surgical biopsy. Fig 2. Electromagnetic navigation bronchoscopy setup. (Reproduced with permission from SuperDimension, Inc.)
4 Ann Thorac Surg PEARLSTEIN ET AL 2012;93: ENB PERFORMED BY THORACIC SURGEONS 947 Results Of the 104 patients, 3 were excluded due to insufficient follow-up. The remaining 101 patients had a median lesion size of 2.8 cm (range 0.8 to 10 cm). The mean number of registration points was 6.8. After registration the mean CTBD was 4.0 mm (range 2.4 to 7.0 mm). Once navigation toward the target lesion was optimized, the average measured distance to the lesion was 7.4 mm (range 0.3 to 25 mm). The average length of the procedure was 1 hour 10 minutes (range 0:25 to 2:37). Eighty-two of 101 suspicious lesions were ultimately determined to be malignant. Sixty-seven (82%) of these 82 malignancies had a positive diagnosis upon ENB. Of the 34 lesions without a positive ENB biopsy, 19 (56%) were categorized as true negatives; 8 had benign surgical biopsies (7 granulomas, 1 intralobar pulmonary sequestration), 6 disappeared on subsequent imaging, and 5 demonstrated stability over serial CT scans performed for 2 years. Of the 15 false negative biopsies, 4 were demonstrated to be malignant with open surgical biopsy or removal and 8 were determined malignant by CTguided percutaneous biopsy. There were 3 lesions that were defined as false negative because, even though the ENB biopsy was negative, upon subsequent imaging the lesions grew and showed metastases indicative of a malignancy. Consequently, 86 of 101 cases had an accurate ENB biopsy for a diagnostic yield of 85%. An extensive statistical evaluation was conducted to determine whether diagnostic yield could be correlated with the size of targeted lesions. The assumption was that larger lesions would have greater diagnostic yield compared with small lesions. Positive predictive value, negative predictive value, sensitivity, specificity, and accuracy were investigated for the following 3 groups of lesions based on size: less than 1.5 cm; 1.5 to 2 cm; and greater than 2 cm. While most ENB studies divide lesions into those greater or less than 2 cm (ie, large and small lesions), we chose to subdivide our small lesions into those greater or less than 1.5 cm. Our reason for doing this was to further clarify how the size of the lesion affected our diagnostic yield. As there were assumed to be no false positives, positive predictive value and specificity are always 100%. Table 1 shows negative predictive value and sensitivity based on lesion size and Tables 2 and 3 show details. The Fisher exact test was performed to see whether there is any difference in negative predictive value or sensitivity among the 3 groups, but all p values are greater than Table 1. Negative Predictive Value and Sensitivity Based on Lesion Size Lesion Size (cm) Overall Negative predictive 78% 20% 55% 56% value Sensitivity 78% 69% 85% 82% Fisher exact test p value for negative predictive value: 0.141; Fisher exact test p value for sensitivity: Table 2. Actual Counts for Negative Predictive Value Lesion Size (cm) Total True negative (TN) False negative (FN) Total Negative predictive value TN/(TN FN). Thus, no differences were found in negative predictive value or sensitivity based on size of lesion. For diagnostic accuracy, true and false results were investigated and the Fisher exact test was used to determine if accuracy is different among the 3 groups of lesions ( 1.5, 1.5 to 2, 2 cm; see Tables 4 and 5). The Fisher exact test p value is which is much greater than Thus, statistically speaking, there is insufficient evidence for association between the size of lesion and diagnostic accuracy. A multinomial logistic regression was performed to analyze the relationship between CTBD and outcomes (true positive, true negative, false negative), and between distance from lesion and outcomes (see Table 6). But, again, p values for CTBD and distances from lesion are and , which are greater than Therefore no strong relationship was found between CTBD or distance from lesion and diagnostic yield. In terms of complications, there were 6 pneumothoraces (5.8%), all of which required chest-tube placement and admission. The average length of stay after chesttube placement was 3.8 days (range 2 to 6 days). There were no long-term sequelae as a result of the pneumothoraces. Although all patients were able to be extubated after the procedure, 4 (3.9%) were admitted overnight for observation secondary to tenuous respiratory status. There were no mortalities. Comment Based upon these results it appears that it is possible for thoracic surgeons, with no prior experience in ENB, to learn the technique and succeed immediately with high diagnostic yields and low complication rates. In fact, our diagnostic yield of 85% is higher than any large study published to date. Our early success may be attributed to several factors. First, we utilized ROSE in each case, which allowed us to continue to take samples and, in some cases, reposition our working channel until the pathologists were satisfied that we had obtained diagnostic material. Second, each procedure was performed with Table 3. Actual Counts for Sensitivity Lesion Size (cm) Total True positive (TP) False negative (FN) Total Sensitivity TP/(TP FN).
5 948 PEARLSTEIN ET AL Ann Thorac Surg ENB PERFORMED BY THORACIC SURGEONS 2012;93: Table 4. Accuracy Lesion Size (cm) Overall True result 88% 71% 87% 85% False result 12% 29% 13% 15% Fisher exact test p value: the patient under GA and paralyzed, whereas most of the previous studies by pulmonologists used only conscious sedation for their procedures. Because the calibration between the virtual and real anatomy takes place at the beginning of the case, any movement the patient exhibits after this calibration will likely decrease the diagnostic accuracy. Performing the procedure with the patient under GA therefore may improve diagnostic yield by preserving the CTBD. Certainly, a fair criticism of this study might be that the routine use of ROSE and GA for every procedure adds to the overall cost. One may wonder whether this added cost is truly necessary. While there has been no study to date comparing diagnostic yields in patients undergoing ENB procedures with or without GA and ROSE, our data suggest that yields are improved when these adjunctive measures are utilized. The financial analysts of the institution in which these procedures were performed were asked to evaluate the added cost per procedure when GA and ROSE were utilized. They claimed that using GA, as opposed to conscious sedation, adds roughly $215 to the organization s direct cost per procedure (excluding the onsite pathology cost). Onsite pathology was a global service utilized by the institution and was difficult to examine on a procedural level. While the routine use of GA and ROSE generate higher charges (most notably the charges related to the anesthesiologist and pathologist), reimbursement on the higher charges allows the institution to recoup some, if not all, of the additional costs. As of now, the institution has not had difficulty being reimbursed for the utilization of anesthesiologists and pathologists in ENB procedures. An interesting, and somewhat surprising finding of this study was that diagnostic yields did not improve for larger lesions. Statistically speaking, the yields were the same for lesions of all sizes (except for when the lesions were greater than 4.5 cm, in which case the diagnostic yield was 100%). This finding, while not the norm, is certainly not unique to our study. Gildea and colleagues [10] and Makris and colleagues [9] published studies in which they were unable to demonstrate a definite relationship between larger lesion size and improved diagnostic yield. Two theories come to mind when trying to Table 5. Actual Counts For Accuracy Lesion Size (cm) Total True result False result Total Table 6. Summary of Means, Medians, and Standard Deviations for Full Data Variable Mean Median Standard Deviation Size of lesion (cm) CT-to-body divergence (mm) Distance from lesion (mm) CT computed tomography. explain this phenomenon. First, it is possible that our sample size of 101 cases was too small to demonstrate a statistical significance of improved diagnostic yield based on larger lesion size. Second, the diagnosis of lesions may be dependent on anatomic factors other than sheer size. Some studies have shown that the selection of lesions with airways seen going right into them on CT [13] and choosing lesions in reachable locations probably has a major impact on the success of the procedure. At least 1 study suggests that a crucial aspect of diagnostic success seems to be establishing a CTBD of 4 mm or less [9].Ifso, the new I-Logic generation of SuperDimension software should correct for this variable (further discussion below). Our average CTBD was 4.0 mm, which, of course, suggests that half of the time CTBD was greater than this distance. Yet, a statistical analysis was not able to demonstrate a correlation between CTBD and diagnostic yield in our study. One potential explanation is that once registration is established within an acceptable range ( 5 to 6 mm), and assuming an appropriate target lesion was selected, the diagnostic accuracy mainly necessitates preserving the initial CTDB and having the cytology of the biopsy specimens evaluated during the procedure. It is possible, then, that our fine results are related, at least in part, to our use of GA with muscle relaxant and ROSE in each case. One of the major benefits of ENB in the management of these patients was that many individuals who were considered high risk for percutaneous biopsy and surgery had their diagnosis of lung cancer established safely and then went on to be treated with SBRT. Of the 67 patients in our study who had a diagnosis of malignancy established by ENB, a large portion (46) had fiducial markers placed bronchoscopically and then had their lesion treated by SBRT, thus avoiding high-risk surgery. One additional point the authors would like to make is that all of these results were obtained using the first generation of SuperDimension software (inreach system Version 4.3.4). The new I-Logic software, which has many improvements over the older version, is now available. The most notable improvements are related to the fact that the I-Logic system uses sophisticated software to create an automatic registration, thus eliminating the need for registration points and creating a CTBD between 3 and 4 mm in virtually every case. Furthermore, the software will scan the airways, recommend an optimal pathway to the lesion, and allow additional computerized three-dimensional viewing screens for improved navigation of the small, nonvisualized airways toward
6 Ann Thorac Surg PEARLSTEIN ET AL 2012;93: ENB PERFORMED BY THORACIC SURGEONS 949 the target lesion [15]. Although there are no objective data yet about how these improvements will impact diagnostic yields, anecdotally the new system seems to decrease the learning curve and increase early success. While the technology of ENB continues to evolve and improve, making the analysis of optimal procedural strategies somewhat of a moving target, we believe our methods can serve as a model for physicians hoping to have excellent early results in ENB. If screening for lung cancer with CT scans becomes commonplace, the volume of suspicious pulmonary nodules likely will grow markedly in the near future. Certainly many of the patients who are discovered to have suspicious pulmonary nodules will be at high risk for surgery or poor candidates for percutaneous biopsy. In such a scenario, it will be imperative that a strategy is developed to obtain tissue diagnosis that is accurate, safe, and widely available. By all accounts, ENB seems to be a very useful diagnostic procedure. Because subspecialty-trained interventional pulmonologists are in short supply, if ENB is to be utilized widely it will be incumbent on physicians from other disciplines to perform this procedure well. We believe that thoracic surgeons have the skill set to master this technique quickly and perform it with excellent early results. Furthermore, there seems to be the suggestion that the use of GA and ROSE improves diagnostic accuracy. Of course the utilization of GA and ROSE adds to the overall cost of the procedure, but when factoring in the cost of follow-up imaging and procedures incurred after nondiagnostic tests the additional up-front cost may not be significant. While further analysis is needed, our early results suggest that thoracic surgeons utilizing ENB may, in the future, play an important role in the early diagnosis of lung cancer. References 1. Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ. Cancer statistics, CA Cancer J Clin 2009;59: International Early Lung Cancer Action Program Investigators, Henschke C, Yankelevitz DF, et al. Survival of patients with stage I lung cancer detected on CT screening. N Engl J Med 2006;355: National Lung Screening Trial, 2010 Updates. National Cancer Institute website. Available at clinicaltrials/noteworthy-trials/nlst/updates. Accessed December 5, The National Lung Screening Trial Research Team. Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med 2011;365: Radke JR, Conway WA, Eyler WR, Kvale PA. Diagnostic accuracy in peripheral lung lesions: factors predicting success with flexible fiberoptic bronchoscopy. Chest 1979;76: Baaklini WA, Reinoso MA, Gorin AB, Sharafkaneh A, Manian P. Diagnostic yield of fiberoptic bronchoscopy in evaluating solitary pulmonary nodules. Chest 2000;117: Li H, Boiselle PM, Shepard JO, Trotman-Dickenson B, McLoud TC. Diagnostic accuracy and safety of CT-guided percutaneous needle aspiration biopsy of the lung: comparison of small and large pulmonary nodules. Am J Roentgenol 1996;167: Shulman L, Ost D. Advances in bronchoscopic diagnosis of lung cancer. Curr Opin Pulm Med 2007;13: Makris D, Scherpereel A, Leroy S, et al. Electromagnetic navigation diagnostic bronchoscopy for small peripheral lung lesions. Eur Respir J 2007;29: Gildea TR, Mazzone PJ, Karnak D, Meziane M, Mehta AC. Electromagnetic navigation diagnostic bronchoscopy: a prospective study. Am J Respir Crit Care Med 2006;174: Eberhardt R, Anantham D, Herth F, Feller-Kopman D, Ernst A. Electromagnetic navigation diagnostic bronchoscopy in peripheral lung lesions. Chest 2007;131: Bertoletti L, Robert A, Cottier M, Chambonniere ML, Vergnon JM. Accuracy and feasibility of electromagnetic navigated bronchoscopy under nitrous oxide sedation for pulmonary peripheral opacities: an outpatient study. Respiration 2009;78: Seijo LM, de Torres JP, Lozano MD, et al. Diagnostic yield of electromagnetic navigation bronchoscopy is highly dependent on the presence of a bronchus sign on CT imaging: results from a prospective study. Chest 2010;138: Wilson DS, Bartlett RJ. Improved diagnostic yield of bronchoscopy in a community practice: combination of electromagnetic navigation system and rapid on-site evaluation. J Bronchol 2007;14: SuperDimension physician education and outreach materials. Available at cfm/go/enb.materials. Accessed January 24, DISCUSSION DR HUMBERTO R. RAVELO (Long Beach, CA): Dr Pearlstein, as a Medical College of Wisconsin graduate, I especially enjoyed your expert presentation. I have been in practice for thirty years in a tertiary referral center where the Electromagnetic Navigation Diagnostic Bronchoscopy equipment has just been acquired and is being used. At this point, the institution is supporting and subsidizing the performance of this procedure by Pulmonary Medicine. How do you propose to best persuade and prepare thoracic surgeons to incorporate this technique as part of their valuable, operating room diagnostic armamentarium? DR PEARLSTEIN: Well, I think there are two answers to your question. First of all, I think in the future, a lot of these procedures are not going to be specialty limited. I think they re going to be ability limited. Secondly, I think a surgeon is in a unique position if they understand this technique as well as endobronchial ultrasound. They can set it up in an operating room and perform these interventions. And with the patient asleep, they can maybe do a mediastinoscopy if they don t have diagnostic material, or you can flip them on the side and do a VATS [video-assisted thoracic surgery]. So I think a surgeon is in a unique position to utilize a lot of different tools to establish a diagnosis. DR RAFAEL S. ANDRADE (Minneapolis, MN): This is a very nice presentation, very impressive results. I have two questions for you. We have started doing this, although we ve encountered a fairly steep learning curve, and I think we ve not been very selective about which nodules. We just see a nodule and say, well, let s try, and with the back-up plan, we can do a thoracoscopy or whatever.
7 950 PEARLSTEIN ET AL Ann Thorac Surg ENB PERFORMED BY THORACIC SURGEONS 2012;93: Can you clarify how you selected your patients? Were you selective in doing these or did you just start with all comers? DR PEARLSTEIN: Well, we were. And I can tell you that all of our pulmonary nodules are presented at a multidisciplinary thoracic oncology conference every week, and interventional radiologists are part of that. We are fortunate to have a very good interventional radiology department and we cross-refer to each other. Generally the lesions we went after with electromagnetic navigation bronchoscopy early in our experience were lesions that were greater than 2 cm. They were in high-risk patients who really couldn t tolerate a pneumothorax if the radiologist was doing multiple passes. And I think you have to look at whether there is an airway going directly to the lesion on the CT [computer tomographic] scan. If there s an airway going to the lesion, your chances of making that diagnosis are much greater, and there s been a recent paper that s shown that. And I d say pick lesions that you think you can get good results with up front. Encourage yourself and the team, build a little confidence, and then go after the small peripheral lesions. DR DAVID P. MASON (Cleveland, OH): Just a quick question. The lesion size, median size 2.8 cm, how did that compare to some of these other studies? That seems like a pretty big lesion. DR PEARLSTEIN: Essentially it was identical statistically to the other large studies. Once you get below 1-1/2 cm, the lesions do get tricky to hit. Certainly below 1 cm they re very difficult to hit if there isn t an airway leading right into it. DR MASON: I mean, I think what you said in terms of the selection is important to note because actually what you did is you selected the patients that you thought you had a good chance of getting positive results on, and those were the ones that you did the procedure on. And you sorted those out already as the high-yield patients as opposed to, for example, everyone who comes in with a lesion that s 2.8 cm sitting anywhere. DR PEARLSTEIN: Right. DR ELISABETH U. DEXTER (Buffalo, NY): Very nice results. I was just wondering, have you done any analysis of how many times you had to pass an instrument through the extended working channel once you got it in position? DR PEARLSTEIN: That is a great question. DR DEXTER: And whether it was the fine needle aspiration or the brush or the forceps or the lavage that got you the most yields? DR PEARLSTEIN: Right. It s two questions. So the first one, we should have kept track of that, and we didn t. We thought about it later on. I can tell you that when you have the on-site pathologist and they re looking at the slides as you re making them, we d usually do one or two passes, and sometimes we d get our diagnosis right away and we d be done. There are instances where we would do five, six, seven passes, especially when we thought it really was going to be a lung cancer, and we just sort of hung in there with it and our pathologist did as well. I d say on average it s about three passes per instrument. We do a Wang needle, a biopsy forceps, and a brush on each patient, and I d say, in answering your second question, that we got the diagnosis with the brushes more often than the other two instruments, but it varied. It could have been any of them. DR DEXTER: Thank you.
Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions
 Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions Original Effective Date: 8/25/14 Policy Number: MCP-206 Revision Date(s): Review
Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions Original Effective Date: 8/25/14 Policy Number: MCP-206 Revision Date(s): Review
Owing to the recent attention given to lung cancer
 Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules
 Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Corporate Medical Policy Electromagnetic Navigation Bronchoscopy
 Corporate Medical Policy Electromagnetic Navigation Bronchoscopy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: electromagnetic_navigation_bronchoscopy 1/2010 3/2017 3/2018 9/2017
Corporate Medical Policy Electromagnetic Navigation Bronchoscopy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: electromagnetic_navigation_bronchoscopy 1/2010 3/2017 3/2018 9/2017
Electromagnetic Navigation Bronchoscopy
 Medical Policy Manual Surgery, Policy No. 179 Electromagnetic Navigation Bronchoscopy Next Review: March 2018 Last Review: March 2017 Effective: May 1, 2017 IMPORTANT REMINDER Medical Policies are developed
Medical Policy Manual Surgery, Policy No. 179 Electromagnetic Navigation Bronchoscopy Next Review: March 2018 Last Review: March 2017 Effective: May 1, 2017 IMPORTANT REMINDER Medical Policies are developed
Erica Giblin, MD Holy Family Hospital
 Erica Giblin, MD Holy Family Hospital Electromagnetic Navigation Bronchoscopy A New Treatment for Patients with Peripheral Lung Lesions Lung Cancer: An Epidemic? In the U.S.: #1 cause of cancer-related
Erica Giblin, MD Holy Family Hospital Electromagnetic Navigation Bronchoscopy A New Treatment for Patients with Peripheral Lung Lesions Lung Cancer: An Epidemic? In the U.S.: #1 cause of cancer-related
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT POLICY GUIDELINES DESCRIPTION. Page: 1 of 6
 Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title ELECTROMAGNETIC NAVIGATION BRONCHOSCOPY Policy Number 6.01.40 Category Technology Assessment Effective Date 04/21/11 Revised Date
Page: 1 of 6 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title ELECTROMAGNETIC NAVIGATION BRONCHOSCOPY Policy Number 6.01.40 Category Technology Assessment Effective Date 04/21/11 Revised Date
The Effect of Respiratory Motion on Pulmonary Nodule Location During Electromagnetic Navigation Bronchoscopy
 [ Original Research Pulmonary Procedures ] The Effect of Respiratory Motion on Pulmonary Nodule Location During Electromagnetic Navigation Bronchoscopy Alexander Chen, MD ; Nicholas Pastis, MD, FCCP ;
[ Original Research Pulmonary Procedures ] The Effect of Respiratory Motion on Pulmonary Nodule Location During Electromagnetic Navigation Bronchoscopy Alexander Chen, MD ; Nicholas Pastis, MD, FCCP ;
May-Lin Wilgus. A. Study Purpose and Rationale
 Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
Utility of a Computer-Aided Diagnosis Program in the Evaluation of Solitary Pulmonary Nodules Detected on Computed Tomography Scans: A Prospective Observational Study May-Lin Wilgus A. Study Purpose and
UNDERSTANDING SERIES LUNG CANCER BIOPSIES LungCancerAlliance.org
 UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Electromagnetic Navigation Bronchoscopy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Electromagnetic Navigation Bronchoscopy
 Electromagnetic Navigation Bronchoscopy Policy Number: 7.01.122 Last Review: 9/2018 Origination: 1/2010 Next Review: 9/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Electromagnetic Navigation Bronchoscopy Policy Number: 7.01.122 Last Review: 9/2018 Origination: 1/2010 Next Review: 9/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Electromagnetic Navigation Bronchoscopy. Populations Interventions Comparators Outcomes Individuals: With suspicious pulmonary lesion(s)
 Protocol Electromagnetic Navigation Bronchoscopy Medical Benefit Effective Date: 04/01/13 Next Review Date: 01/20 Preauthorization No Review Dates: 09/10, 09/11, 01/12, 01/13, 01/14, 01/15, 01/16, 01/17,
Protocol Electromagnetic Navigation Bronchoscopy Medical Benefit Effective Date: 04/01/13 Next Review Date: 01/20 Preauthorization No Review Dates: 09/10, 09/11, 01/12, 01/13, 01/14, 01/15, 01/16, 01/17,
Policy #: 400 Latest Review Date: June 2016
 Name of Policy: Electromagnetic Navigational Bronchoscopy Policy #: 400 Latest Review Date: June 2016 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under
Name of Policy: Electromagnetic Navigational Bronchoscopy Policy #: 400 Latest Review Date: June 2016 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under
Electromagnetic Navigation Bronchoscopy
 Electromagnetic Navigation Bronchoscopy Policy Number: 7.01.122 Last Review: 9/2017 Origination: 1/2010 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Electromagnetic Navigation Bronchoscopy Policy Number: 7.01.122 Last Review: 9/2017 Origination: 1/2010 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Electromagnetic Navigation Bronchoscopy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Introduction to Interventional Pulmonology
 Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Thoracoscopy for Lung Cancer
 Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Information for. Patients with an Abnormal Lung X-ray
 Information for Patients with an Abnormal Lung X-ray Some of the materials in this resource were adapted with permission from: Understanding Lung Cancer, Juravinski Cancer Centre, Hamilton Health Sciences,
Information for Patients with an Abnormal Lung X-ray Some of the materials in this resource were adapted with permission from: Understanding Lung Cancer, Juravinski Cancer Centre, Hamilton Health Sciences,
Innovations in Lung Cancer Diagnosis and Surgical Treatment
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Bronchoscopy and endobronchial ultrasound for diagnosis and staging of lung cancer
 FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
Lung Cancer Resection
 Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
The Maine Lung Cancer Coalition. Working Together to Reduce Lung Cancer in Maine
 The Maine Lung Cancer Coalition Working Together to Reduce Lung Cancer in Maine funding Maine Lung Cancer Coalition (MLCC) Webinar Lung Cancer Screening: Following Up On Abnormal Low Dose CT Scans with
The Maine Lung Cancer Coalition Working Together to Reduce Lung Cancer in Maine funding Maine Lung Cancer Coalition (MLCC) Webinar Lung Cancer Screening: Following Up On Abnormal Low Dose CT Scans with
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center
 Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Thoracic Diagnostic Assessment Program. Patient information for. Last revised: November
 Thoracic Diagnostic Assessment Program Patient information for Last revised: November 2016 1 A list of your tests and appointments Diagnostic tests 2 3 4 Specialist appointments Doctor: Specialty: Notes:
Thoracic Diagnostic Assessment Program Patient information for Last revised: November 2016 1 A list of your tests and appointments Diagnostic tests 2 3 4 Specialist appointments Doctor: Specialty: Notes:
Larry Tan, MD Thoracic Surgery, HSC. Community Cancer Care Educational Conference October 27, 2017
 Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
ADVANCED LUNG DIAGNOSTICS
 ADVANCED LUNG DIAGNOSTICS SAMIR S. MAKANI, MD, FCCP DIRECTOR INTERVENTIONAL PULMONARY AND BROCHOSCOPY UNIVERSITY OF CALIFORNIA SAN DIEGO MEDICAL CENTER SAN DIEGO, CA Dr. Samir Makani is an Associate professor
ADVANCED LUNG DIAGNOSTICS SAMIR S. MAKANI, MD, FCCP DIRECTOR INTERVENTIONAL PULMONARY AND BROCHOSCOPY UNIVERSITY OF CALIFORNIA SAN DIEGO MEDICAL CENTER SAN DIEGO, CA Dr. Samir Makani is an Associate professor
Update on Navigational Bronchoscopy: Electromagnetic Navigation Bronchoscopy
 Update on Navigational Bronchoscopy: Electromagnetic Navigation Bronchoscopy and Lung Point 28.02.15 The Prince Charles Hospital University of Queensland Thoracic Research Center AUSTRALIA The Prince Charles
Update on Navigational Bronchoscopy: Electromagnetic Navigation Bronchoscopy and Lung Point 28.02.15 The Prince Charles Hospital University of Queensland Thoracic Research Center AUSTRALIA The Prince Charles
Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer
 Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Role of electromagnetic navigational bronchoscopy in pulmonary nodule management
 Review Article Role of electromagnetic navigational bronchoscopy in pulmonary nodule management Aditya Goud 1, Chanukya Dahagam 1, David P. Breen 2, Saiyad Sarkar 3 1 Department of Internal Medicine, MedStar
Review Article Role of electromagnetic navigational bronchoscopy in pulmonary nodule management Aditya Goud 1, Chanukya Dahagam 1, David P. Breen 2, Saiyad Sarkar 3 1 Department of Internal Medicine, MedStar
Improved Diagnostic Efficacy by Rapid Cytology Test in Fluoroscopy-Guided Bronchoscopy
 ORIGINAL ARTICLE Improved Diagnostic Efficacy by Rapid Cytology Test in Fluoroscopy-Guided Bronchoscopy Junji Uchida, MD, Fumio Imamura, MD, Akemi Takenaka, CT, Mana Yoshimura, MD, Kiyonobu Ueno, MD, Kazuyuki
ORIGINAL ARTICLE Improved Diagnostic Efficacy by Rapid Cytology Test in Fluoroscopy-Guided Bronchoscopy Junji Uchida, MD, Fumio Imamura, MD, Akemi Takenaka, CT, Mana Yoshimura, MD, Kiyonobu Ueno, MD, Kazuyuki
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
CT Screening for Lung Cancer for High Risk Patients
 CT Screening for Lung Cancer for High Risk Patients The recently published National Lung Cancer Screening Trial (NLST) showed that low-dose CT screening for lung cancer reduces mortality in high-risk patients
CT Screening for Lung Cancer for High Risk Patients The recently published National Lung Cancer Screening Trial (NLST) showed that low-dose CT screening for lung cancer reduces mortality in high-risk patients
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer
 Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Small Cell Lung Cancer
 Small Cell Lung Cancer Small cell lung cancer (SCLC) affects 15% of all lung cancer patients. SCLC is the most aggressive type of lung cancer. It may be treated with chemotherapy and radiation. SCLC has
Small Cell Lung Cancer Small cell lung cancer (SCLC) affects 15% of all lung cancer patients. SCLC is the most aggressive type of lung cancer. It may be treated with chemotherapy and radiation. SCLC has
Electromagnetic navigation transthoracic needle aspiration for the diagnosis of pulmonary nodules: A safety and feasibility pilot study
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Electromagnetic navigation transthoracic needle aspiration for the diagnosis of pulmonary nodules: A safety
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Electromagnetic navigation transthoracic needle aspiration for the diagnosis of pulmonary nodules: A safety
Fiducial Marker Placement Using Endobronchial Ultrasound and Navigational Bronchoscopy for Stereotactic Radiosurgery: An Alternative Strategy
 Fiducial Marker Placement Using Endobronchial Ultrasound and Navigational Bronchoscopy for Stereotactic Radiosurgery: An Alternative Strategy Daniel P. Harley, MD, William S. Krimsky, MD, Saiyad Sarkar,
Fiducial Marker Placement Using Endobronchial Ultrasound and Navigational Bronchoscopy for Stereotactic Radiosurgery: An Alternative Strategy Daniel P. Harley, MD, William S. Krimsky, MD, Saiyad Sarkar,
Effect of Electromagnetic Navigation on CT-Guided Percutaneous Thermal Ablation or Biopsy of Lung Tumors
 Effect of Electromagnetic Navigation on CT-Guided Percutaneous Thermal Ablation or Biopsy of Lung Tumors Chaitan K. Narsule 1, Avneesh Gupta 2, Michael I. Ebright 1, Ricardo Sales dos Santos 3, Roberto
Effect of Electromagnetic Navigation on CT-Guided Percutaneous Thermal Ablation or Biopsy of Lung Tumors Chaitan K. Narsule 1, Avneesh Gupta 2, Michael I. Ebright 1, Ricardo Sales dos Santos 3, Roberto
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC)
 Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
Living With Lung Cancer. Patient Education Guide
 Living With Lung Cancer Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Your doctor has just told you that you have lung cancer. Even if you thought that you might
Living With Lung Cancer Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Your doctor has just told you that you have lung cancer. Even if you thought that you might
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times
 Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
CT Fluoroscopy-Guided vs Multislice CT Biopsy ModeGuided Lung Biopies:a preliminary experience
 CT Fluoroscopy-Guided vs Multislice CT Biopsy ModeGuided Lung Biopies:a preliminary experience Poster No.: C-0097 Congress: ECR 2016 Type: Scientific Exhibit Authors: A. Casarin, G. Rech, C. Cicero, A.
CT Fluoroscopy-Guided vs Multislice CT Biopsy ModeGuided Lung Biopies:a preliminary experience Poster No.: C-0097 Congress: ECR 2016 Type: Scientific Exhibit Authors: A. Casarin, G. Rech, C. Cicero, A.
Since central airway stenosis is often a lifethreatening. Double Y-stenting for tracheobronchial stenosis. Masahide Oki and Hideo Saka
 Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Accurate mediastinal staging is a critical component
 Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Less Invasive Options for Pulmonary Testing
 Less Invasive Options for Pulmonary Testing Guest Expert: Jonathan, MD www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with doctors Francine Foss and Lynn. I am Bruce Barber.
Less Invasive Options for Pulmonary Testing Guest Expert: Jonathan, MD www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with doctors Francine Foss and Lynn. I am Bruce Barber.
Radial endobronchial ultrasound (EBUS), performed during
 Original Article Can Computed Tomography Characteristics Predict Outcomes in Patients Undergoing Radial Endobronchial Ultrasound-Guided Biopsy of Peripheral Lung Lesions? Matthew Evison,* Philip A.J. Crosbie,*
Original Article Can Computed Tomography Characteristics Predict Outcomes in Patients Undergoing Radial Endobronchial Ultrasound-Guided Biopsy of Peripheral Lung Lesions? Matthew Evison,* Philip A.J. Crosbie,*
In 1982 Pearson and colleagues [1] from Toronto published
![In 1982 Pearson and colleagues [1] from Toronto published In 1982 Pearson and colleagues [1] from Toronto published](/thumbs/95/124110746.jpg) Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
Subject: Computer Assisted Surgical Navigation
 02-99221-14 Original Effective Date: 03/15/09 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Computer Assisted Surgical Navigation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
02-99221-14 Original Effective Date: 03/15/09 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Computer Assisted Surgical Navigation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
DENOMINATOR: All final reports for CT imaging studies with a finding of an incidental pulmonary nodule for patients aged 35 years and older
 Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Percutaneous Lung Biopsy in the Molecular Profiling Era: A Survey of Current Practices
 Percutaneous Lung Biopsy in the Molecular Profiling Era: A Survey of Current Practices PHILLIP GUICHET, B.A. 1, FEREIDOUN ABTIN, M.D. 2, CHRISTOPHER LEE, M.D. 1 1 KECK SCHOOL OF MEDICINE OF USC, DEPT OF
Percutaneous Lung Biopsy in the Molecular Profiling Era: A Survey of Current Practices PHILLIP GUICHET, B.A. 1, FEREIDOUN ABTIN, M.D. 2, CHRISTOPHER LEE, M.D. 1 1 KECK SCHOOL OF MEDICINE OF USC, DEPT OF
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
American College Of Radiology ACR Appropriateness Criteria WORK-UP OF THE SOLITARY PULMONARY NODULE
 This document is provided to you by the American College of Radiology. We strive to deliver this information in a convenient and effective manner. After you finish reviewing the criteria, please provide
This document is provided to you by the American College of Radiology. We strive to deliver this information in a convenient and effective manner. After you finish reviewing the criteria, please provide
Benign Intraparenchymal Scarring in the DBT Era
 Benign Intraparenchymal Scarring in the DBT Era David Gruen, MD, MBA, FACR Director of Women s Imaging, Stamford Health, Stamford, CT With the advent of Digital Breast Tomosynthesis (DBT or 3D mammography),
Benign Intraparenchymal Scarring in the DBT Era David Gruen, MD, MBA, FACR Director of Women s Imaging, Stamford Health, Stamford, CT With the advent of Digital Breast Tomosynthesis (DBT or 3D mammography),
National Optimal Lung Cancer Pathway
 National Optimal Lung Cancer Pathway This document was produced by the Lung Clinical Expert Group 2017 Document Title: National Optimal Lung Cancer Pathway and Implementation Guide Date of issue: August
National Optimal Lung Cancer Pathway This document was produced by the Lung Clinical Expert Group 2017 Document Title: National Optimal Lung Cancer Pathway and Implementation Guide Date of issue: August
The Itracacies of Staging Patients with Suspected Lung Cancer
 The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Virtual Bronchoscopic Navigation Improves the Diagnostic Yield of Radial-Endobronchial Ultrasound for Peripheral Pulmonary Lesions with Involved Bronchi on CT Fumihiro Asano 1, Naofumi
ORIGINAL ARTICLE Virtual Bronchoscopic Navigation Improves the Diagnostic Yield of Radial-Endobronchial Ultrasound for Peripheral Pulmonary Lesions with Involved Bronchi on CT Fumihiro Asano 1, Naofumi
Charlton Campus Map Information Handbook
 Charlton Campus Map Information Handbook 50 Charlton Avenue East Hamilton, Ontario, L8N 4A6 S Parking Garage Public Parking W N Walkway to Hospital Fontbonne for patients and families Staff Only Parking
Charlton Campus Map Information Handbook 50 Charlton Avenue East Hamilton, Ontario, L8N 4A6 S Parking Garage Public Parking W N Walkway to Hospital Fontbonne for patients and families Staff Only Parking
MATERIALS AND METHODS. We retrospectively reviewed a consecutive series
 Huanqi Li1 Phillip M. Boiselle1 2 Jo-Anne 0. Shepard1 Beatrice Trotman-Dickenson1 Theresa C. McLoud1 Received January 2, 1996; accepted after revision Febru ary 19, 1996. tchest Division, Department of
Huanqi Li1 Phillip M. Boiselle1 2 Jo-Anne 0. Shepard1 Beatrice Trotman-Dickenson1 Theresa C. McLoud1 Received January 2, 1996; accepted after revision Febru ary 19, 1996. tchest Division, Department of
In 1995, American physicians investigated an estimated 150,000 patients
 Lacasse et al General Thoracic Surgery Transthoracic needle biopsy in the diagnosis of solitary pulmonary nodules: A survey of Canadian physicians Yves Lacasse, MD, MSc Julie Plante, MD Simon Martel, MD
Lacasse et al General Thoracic Surgery Transthoracic needle biopsy in the diagnosis of solitary pulmonary nodules: A survey of Canadian physicians Yves Lacasse, MD, MSc Julie Plante, MD Simon Martel, MD
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Expert Round Table with Drs. Anne Tsao and Alex Farivar Part 1: Elderly Man with Indolent Bronchioloalveolar Carcinoma
 Expert Round Table with Drs. Anne Tsao and Alex Farivar Part 1: Elderly Man with Indolent Bronchioloalveolar Carcinoma February 2010 I d like to welcome everyone, thanks for coming out to our lunch with
Expert Round Table with Drs. Anne Tsao and Alex Farivar Part 1: Elderly Man with Indolent Bronchioloalveolar Carcinoma February 2010 I d like to welcome everyone, thanks for coming out to our lunch with
Slide 1. Slide 2. Slide 3. Investigation and management of lung cancer Robert Rintoul. Epidemiology. Risk factors/aetiology
 Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Lung Surgery: Thoracoscopy
 Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Fiberoptic Bronchoscopy: Correlation of Cytology and Biopsy Results
 ORIGINAL ARTICLE Tanaffos (2007) 6(2), 46-50 2007 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Fiberoptic Bronchoscopy: Correlation of Cytology and Biopsy Results Zohreh Mohammad
ORIGINAL ARTICLE Tanaffos (2007) 6(2), 46-50 2007 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran Fiberoptic Bronchoscopy: Correlation of Cytology and Biopsy Results Zohreh Mohammad
Breast Cancer Imaging Webcast October 21, 2009 Peter Eby, M.D. Introduction
 Breast Cancer Imaging Webcast October 21, 2009 Peter Eby, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff or
Breast Cancer Imaging Webcast October 21, 2009 Peter Eby, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle Cancer Care Alliance, its medical staff or
Blood path technique to reduce pneumothorax after CT guided lung biopsy
 Blood path technique to reduce pneumothorax after CT guided lung biopsy Poster No.: C-0753 Congress: ECR 2011 Type: Scientific Paper Authors: G. J. Mallarajapatna, N. Ramanna; Bangalore/IN Keywords: Interventional
Blood path technique to reduce pneumothorax after CT guided lung biopsy Poster No.: C-0753 Congress: ECR 2011 Type: Scientific Paper Authors: G. J. Mallarajapatna, N. Ramanna; Bangalore/IN Keywords: Interventional
Prevalence of Benign Disease in Patients Undergoing Resection for Suspected Lung Cancer
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Lung Cancer Screening
 Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Modernizing the Mitral Valve: Advances in Robotic and Minimally Invasive Cardiac Repair
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/modernizing-mitral-valveadvances-robotic-minimally-invasive-cardiac-repair/7686/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/modernizing-mitral-valveadvances-robotic-minimally-invasive-cardiac-repair/7686/
Gold Anchor enables safe reach to inner organs
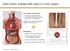 Gold Anchor enables safe reach to inner organs Fine needles for cytology have been used >50 years in all parts of the human body with no to very little harm Gold Anchor comes pre-loaded in needles of the
Gold Anchor enables safe reach to inner organs Fine needles for cytology have been used >50 years in all parts of the human body with no to very little harm Gold Anchor comes pre-loaded in needles of the
Accuracy and safety of CT guided transthoracic needle biopsy
 Original Article Accuracy and safety of CT guided transthoracic needle biopsy * Atheer A. Fadhil** FICMS-CABMS-FICMS (Pulm.), DMRD, FIBMS (Rad.), Fac Med Baghdad 2012; Vol. 54, No. 1 Received Dec.2011
Original Article Accuracy and safety of CT guided transthoracic needle biopsy * Atheer A. Fadhil** FICMS-CABMS-FICMS (Pulm.), DMRD, FIBMS (Rad.), Fac Med Baghdad 2012; Vol. 54, No. 1 Received Dec.2011
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Quality ID #364: Optimizing Patient Exposure to Ionizing Radiation: Appropriateness: Follow-up CT Imaging for Incidentally Detected Pulmonary Nodules According to Recommended Guidelines National Quality
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Dr. Coakley, so virtual colonoscopy, what is it? Is it a CT exam exactly?
 Virtual Colonoscopy Webcast January 26, 2009 Fergus Coakley, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Virtual Colonoscopy Webcast January 26, 2009 Fergus Coakley, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
ENDOBRONCHIAL ABLATIVE THERAPIES. Christopher Cortes, MD, FPCCP
 ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
Lung Cancer Screening. Eric S. Papierniak, DO NF/SG VHA UF Health
 Lung Cancer Screening Eric S. Papierniak, DO NF/SG VHA UF Health Overview Background Supporting evidence Guidelines Practical considerations Patient selection What to do with abnormal results Billing/coding
Lung Cancer Screening Eric S. Papierniak, DO NF/SG VHA UF Health Overview Background Supporting evidence Guidelines Practical considerations Patient selection What to do with abnormal results Billing/coding
Lung Cancer Screening
 Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Scan for mobile link. Lung Cancer Screening What is lung cancer screening? Screening examinations are tests performed to find disease before symptoms begin. The goal of screening is to detect disease at
Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule
 Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
The Virtual Lung Nodule Clinic
 The Virtual Lung Nodule Clinic Poster No.: C-1023 Congress: ECR 2016 Type: Educational Exhibit Authors: S. Higgins, F. C. Lyall, J. Taylor, J. goldman, S. Rolin, B. 1 2 1 2 2 3 2 2 3 Soar ; Torbay/UK,
The Virtual Lung Nodule Clinic Poster No.: C-1023 Congress: ECR 2016 Type: Educational Exhibit Authors: S. Higgins, F. C. Lyall, J. Taylor, J. goldman, S. Rolin, B. 1 2 1 2 2 3 2 2 3 Soar ; Torbay/UK,
ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM
 ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM This competency-based curriculum has been designed by a task force of interventional pulmonology specialists to underline the learning outcomes
ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM This competency-based curriculum has been designed by a task force of interventional pulmonology specialists to underline the learning outcomes
Pancreatic Cancer: Associated Signs, Symptoms, Risk Factors and Treatment Approaches
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/pancreatic-cancerassociated-signs-symptoms-and-risk-factors-and-treatment-approaches/9552/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/pancreatic-cancerassociated-signs-symptoms-and-risk-factors-and-treatment-approaches/9552/
Lung Isolation: Clinical Challenges and Strategies for Success
 Lung Isolation: Clinical Challenges and Strategies for Success 2017 Dr. Alan Jay Schwartz: Hello. This is Alan Jay Schwartz, Editor-in-Chief of the American Society of Anesthesiologists 2017 Refresher
Lung Isolation: Clinical Challenges and Strategies for Success 2017 Dr. Alan Jay Schwartz: Hello. This is Alan Jay Schwartz, Editor-in-Chief of the American Society of Anesthesiologists 2017 Refresher
CT-Guided Transthoracic Needle Aspiration Biopsy of Small ( 20 mm) Solitary Pulmonary Nodules
 Yoshiharu Ohno 1 Hiroto Hatabu 2 Daisuke Takenaka 1 Takanori Higashino 1 Hirokazu Watanabe 1 Chiho Ohbayashi 3 Kazuro Sugimura 1 Received May 16, 2002; accepted after revision October 30, 2002. 1 Department
Yoshiharu Ohno 1 Hiroto Hatabu 2 Daisuke Takenaka 1 Takanori Higashino 1 Hirokazu Watanabe 1 Chiho Ohbayashi 3 Kazuro Sugimura 1 Received May 16, 2002; accepted after revision October 30, 2002. 1 Department
The Challenge of Lung Cancer
 The Challenge of Lung Cancer Despite important advances in the treatment of lung cancer, it continues to account for more cancer deaths than colon, prostate, breast, and pancreas cancer combined. In 2012,
The Challenge of Lung Cancer Despite important advances in the treatment of lung cancer, it continues to account for more cancer deaths than colon, prostate, breast, and pancreas cancer combined. In 2012,
Screening for Lung Cancer: New Guidelines, Old Problems
 Screening for Lung Cancer: New Guidelines, Old Problems Robert Schilz DO, PhD Associate Professor of Medicine Interim Chief of the Division of Pulmonary, Critical Care and Sleep Medicine University Hospitals
Screening for Lung Cancer: New Guidelines, Old Problems Robert Schilz DO, PhD Associate Professor of Medicine Interim Chief of the Division of Pulmonary, Critical Care and Sleep Medicine University Hospitals
BREAST CANCER PATHOLOGY
 BREAST CANCER PATHOLOGY FACT SHEET Version 4, Aug 2013 This fact sheet was produced by Breast Cancer Network Australia with input from The Royal College of Pathologists of Australasia I m a nurse and know
BREAST CANCER PATHOLOGY FACT SHEET Version 4, Aug 2013 This fact sheet was produced by Breast Cancer Network Australia with input from The Royal College of Pathologists of Australasia I m a nurse and know
