Lung cancer is the leading cause of cancer-related death
|
|
|
- Dylan Weaver
- 5 years ago
- Views:
Transcription
1 Molecular Diagnostics of Lung Carcinomas Sanja Dacic, MD, PhD N Context. The development of targeted therapies in the treatment of lung carcinoma is a rapidly growing area that requires a precise histologic classification of lung carcinomas and the implementation into clinical practice of testing for predictive biomarkers of therapy response. Molecular testing has added another layer of complexity in the routine workup of rather limited diagnostic tumor tissue. Objective. To review the most important lung carcinoma biomarkers predictive of response and to discuss proposed routine molecular testing in clinical practice. Data Sources. PubMed (US National Library of Medicine) available review articles, peer-reviewed original articles, and experience of the author. Conclusions. Histologic profile, clinical characteristics, and mutational profile of lung carcinoma have all been reported as predictive factors of response to epidermal growth factor receptor tyrosine kinase inhibitors (EGFR-TKIs) and other targeted therapies. Recently published results of large clinical trials indicate that mutational profiling, particularly identification of activating epidermal growth factor receptor (EGFR) mutations, is the best predictor for EGFR-TKI response. Despite all these observations, molecular profiling of lung carcinomas has not been standardized or validated in clinical practice. Rapid development of targeted therapies will probably require molecular testing for a panel of mutations to identify molecular subtypes of non small cell lung carcinomas that will benefit from new therapeutic approaches in personalized patient care. (Arch Pathol Lab Med. 2011;135: ) Lung cancer is the leading cause of cancer-related death in the world. 1 Non small cell lung carcinoma (NSCLC) accounts for 80% to 85% of all lung cancers, with lung adenocarcinoma being the most common histologic type in the United States. Most patients present with advancedstage disease and are not candidates for surgical resection but are subjected to platinum-based chemotherapy and radiation therapy alone, or in combination. Unfortunately, despite these therapies, prognosis is poor, with an overall 5-year survival rate of only 15%. Major advances in the understanding of the molecular pathogenesis of lung cancer have led to new strategies for early detection, diagnosis, staging, and therapy. 2 In recent years, the treatment options have changed from cytotoxic chemotherapies alone to single-agent and combination targeted therapies. A major accomplishment in the treatment of advanced lung cancer has been the discovery of tyrosine kinase inhibitors (TKIs) targeting the epidermal growth factor receptor (EGFR). 3 5 Patients responses to these therapies are variable, and testing for predictive biomarkers of therapeutic response is becoming an important part of the diagnostic workup. Certain clinical characteristics such as female sex, East Asian ethnicity, nonsmoking history, and adenocarcinoma histology have been shown to be associated with an increased likelihood of responsiveness to EGFR-TKI. However, molecular predictors of response, Accepted for publication January 14, From the Department of Pathology, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania. The author has no relevant financial interest in the products or companies described in this article. Reprints: Sanja Dacic, MD, PhD, Department of Pathology, Room PUH C608, University of Pittsburgh Medical Center, 200 Lothrop St, Pittsburgh, PA ( dacics@upmc.edu). such as activating mutations in the tyrosine kinase domain of EGFR, seem to be more reliable predictors of response than clinical characteristics. 6 8 Similarly, other gene alterations that play an important role in adenocarcinoma development have been identified and new targeted therapies are under development (Figure 1). The results of clinical trials with EGFR-TKI have revolutionized the first-line therapy for NSCLC, and first-line treatment with EGFR-TKI is now a standard of care for patients with an EGFR mutation. 9 Unfortunately, not much progress has been made in treatment of other subtypes of NSCLC, such as squamous cell carcinomas, which are usually nonresponsive to EGFR-TKI and may be associated with fatal complications if treated with anti vascular epithelial growth factor therapies. 10,11 Because the histologic profile is one of the predictors of response to targeted therapies, oncologists place high demands on pathologists to precisely subclassify NSCLCs. 12 At the same time, there is a pressure to facilitate and participate in the implementation of biomarker testing in clinical practice. However, as yet, clinical testing for predictive biomarkers in lung carcinoma is neither standardized nor validated in the United States. 13 Recently, the International Association for the Study of Lung Cancer (IASLC) has published the recommendations of the European workshop for EGFR mutation testing in Europe. 9 This review will address the current, most common molecular biomarker testing in lung carcinomas and the need for standardization of molecular testing in the management of patients with lung carcinoma. TUMOR TISSUE SAMPLE It is very unlikely that tumor tissue will be collected for molecular testing only. Since most of the patients with 622 Arch Pathol Lab Med Vol 135, May 2011 Molecular Diagnostics of Lung Carcinomas Dacic
2 Figure 1. Therapies targeting the epidermal growth factor receptor (EGFR) signaling pathway. Abbreviations: AKT, also known as protein kinase B; EGF, epidermal growth factor; EGFR, epidermal growth factor receptor; ERK, extracellular signal regulated kinase; HDAC, histone deacetylase; mtor, mammalian target of rapamycin; PDK1, 3- phospoinositide dependent protein kinase-1; PI3K, phosphatidylinositol 3-kinase; PTEN, phosphatase and tensin; RAS, rat sarcoma; TKIs, tyrosine kinase inhibitors; TSG, tumor suppressor gene; VEGF, vascular endothelial growth factor; VEGFR, vascular endothelial growth factor receptor. Reprinted with permission from Chirieac and Dacic. 78 lung carcinoma present at the advanced stage of the disease, no resection specimen will be available and only tissue collected at the initial diagnostic workup will be considered for molecular testing. Therefore, dilemmas regarding tumor sample remain, such as type of specimen, reliability of molecular testing on cytology specimens, biopsy technique for providing the most adequate tumor volume, and tissue processing for diagnostic and molecular workup. None of these questions presently have answers. The European EGFR Working Group has proposed some of the answers to these questions, which could be applied to any molecular assay in lung carcinoma. 9 The main initial goal in any presumable molecular testing is to obtain a high-quality, high-volume tumor specimen, which would in part depend on biopsy technique (Table). The results may be influenced also by the biopsy site, such as primary tumor versus metastatic tumor. Published studies have demonstrated discordance in results of mutational and fluorescence in situ hybridization (FISH) assays between the primary tumor and metastatic disease. Most of the time, clinicians are sampling only the most easily accessible tumor tissue. It is very hard to design a study that specifically looks into the differences in therapy responses based on molecular results obtained from different types of tumor specimens from the same patient. Therefore, we may never know the right answer to this question. For mutational assays, the ratio between malignant and normal cells within the sample is essential for the detection of specific mutations. 19 Manual or laser microdissection of tumor cells may be required to improve reliability and accuracy of the molecular results, particularly direct DNA sequencing. 20 The minimum number of tumor cells that is optimal for mutational analysis is uncertain, but empirically, 50% of tumor cells per sample is sufficient for DNA sequencing. If other, more sensitive mutation methods are used, even less than 10% of tumor cells may be adequate. 9,21 27 Although processing and fixation of lung tumors has not been standardized by experimental and clinical experiences, short fixation times (6 12 hours for biopsy specimens; 8 18 hours for larger resection specimens) in 10% neutral buffered formalin should be optimal for DNA- and RNA-based tests, as well as FISH assays. 28 In contrast, Bouin fixative should be avoided. Most lung cancers are diagnosed with cytology samples, which may be used for molecular analysis, particularly if cell blocks are made. 29,30 POSITIVE PREDICTORS OF RESPONSE TO EGFR-TKI Epidermal Growth Factor Receptor Mutational Analysis. Two treatment strategies to target EGFR have been developed: monoclonal antibodies directed against the extracellular ligand-binding domain of EGFR (eg, cetuximab [Erbitux, ImClone Systems Inc, Biopsy Technique and Volume of Diagnostic Material a 21-g Needle Aspiration 19-g Needle Aspiration Transbronchial Biopsy CT-Guided Needle Biopsy No. of cells per biopsy/ aspiration $100 $150 $300 $500 No. of biopsies Abbreviation: CT, computed tomography. a Modified with permission from Pirker et al. 9 Arch Pathol Lab Med Vol 135, May 2011 Molecular Diagnostics of Lung Carcinomas Dacic 623
3 Branchburg, New Jersey]) and small-molecule TKIs (eg, gefitinib [Iressa, AstraZeneca, London, United Kingdom]) and erlotinib (Tarceva, F. Hoffmann-La Roche, Basel, Switzerland). 3,4,31 35 Activating somatic mutations in the exons 18 through 21 of the tyrosine kinase domain of EGFR have been shown to correlate with a high likelihood of response to EGFR-TKI, including gefitinib and erlotinib, but not to monoclonal antibodies. The status of EGFR and the patient s response to EGFR-TKI have been assessed by various methods, such as immunohistochemistry (protein expression) and FISH/chromogenic in situ hybridization (CISH) (gene copy number changes), but mutational analysis has been shown to be the best predictor of tumor response to EGFR-TKI Therefore, only EGFR mutation testing in NSCLC has been recommended in Europe. 9 Activating predictive mutations target 4 exons (18 21), which encode part of the tyrosine kinase domain of EGFR (the entire kinase domain is encoded by exons 18 24) and are clustered around the adenosine triphosphate binding pocket of the enzyme. 41 The most common are in-frame deletions in exon 19 (45%), followed by a point mutation (CTG to CGG) in exon 21 at nucleotide 2573, which results in substitution of leucine by arginine at codon 858 (L858R) (41%). Therefore, if limited DNA material is available, a reasonable approach would be to test for the most common mutations within exons 19 and 21 only. These mutations occur in approximately 10% of Western patients and up to 50% of Asian patients with lung adenocarcinomas. They also have prognostic significance, because patients with EGFR-mutant adenocarcinomas showed prolonged survival compared with those with EGFR wild-type disease, regardless of the treatment received Various mutational assays have been developed, but direct DNA sequencing is still the most commonly used method. There is no consensus on the best method, because each method has certain advantages and disadvantages. The major advantage of DNA sequencing is that it can detect all mutations, including novel variants and it identifies the exact mutation. In contrast, newer mutational methods (eg, single-strand conformation polymorphism, denaturing high-performance liquid chromatography, and amplification refractory mutation system) may miss mutations that are not assayed but are more sensitive (requiring fewer tumor cells) and are less time-consuming than DNA sequencing. The significance of low-abundance mutations detected in heterogeneous samples with these more sensitive assays is uncertain and these mutations need further evaluation, including a determination of their clinical or predictive significance. Other Methods. Until recently, the significance of EGFR copy number changes determined by FISH was an area of controversy. Initial reports 38,45 had suggested a role for EGFR-FISH results in predicting the patient s response to EGFR-TKI and antibody treatments. Similarly, chromogenic in situ hybridization was suggested as a reliable alternative to FISH in determining EGFR copy number status in NSCLC. 46 A complicating observation was the fact that EGFR-mutated tumors frequently have EGFR gene copy number changes, and until recently, it was difficult to determine which method provides better prediction of the patient s response. However, recent clinical trials have provided supporting evidence that EGFR mutation status is the most relevant marker for treatment selection, and therefore EGFR mutational analysis should be the method of choice in clinical practice. 47,48 Epidermal growth factor receptor immunohistochemistry is not recommended for EGFR testing in lung cancer. However, mutation-specific rabbit monoclonal antibodies have been shown to detect the 2 most common EGFR mutations (exon 19 deletions and exon 21 L858 mutation) (Cell Signaling Technology, Inc, Danvers, Massachusetts). 49,50 The EGFR L858R mutant antibody showed clinically acceptable performance (sensitivity 95%, positive predictive value of 99%, with a positivity cutoff of 1+). 50 The EGFR exon 19 mutant-specific antibody showed reduced sensitivity for exon 19 deletions other than 15 base pairs. 50 This simple assay should be further validated, because it may provide a rapid and cost-effective clinical test for identifying patients with lung cancer who may be responsive to EGFR-targeted therapies. NEGATIVE PREDICTORS OF RESPONSE TO EGFR-TKI Primary Resistance Genetic mutations in the genes encoding proteins involved in the EGFR signaling cascade (KRAS, HER2, BRAF, PI3K, LKB1, SHP2) exist as mutually exclusive somatic mutations with the possible exception of those in PI3K. 51 The presence of these mutations is associated with a lack of response to EGFR-TKIs in the treatment of lung cancer. Therefore, additional mutational analysis of genes other than EGFR may be necessary to improve patient selection for EGFR-targeted therapies. v-ki-ras-2 Kirsten Rat Sarcoma Viral Oncogene Homolog (KRAS). KRAS mutations are found in approximately 30% of adenocarcinomas and 5% of squamous cell carcinomas. 52,53 The EGFR-KRAS signaling cascade in lung cancer is considered a unidirectional linear outside-in signaling cascade. Therefore, KRAS mutations result in a constitutive activation of the RAS/ MAPK pathway independently of EGFR activation. KRAS point mutations, which lead to substitutions of amino acids for glycine on codons 12 and 13, are most frequently observed in former or current smokers. 42,54,55 Distinct KRAS point mutations, such as G12D, have been reported in approximately 15% of never smokers. 55 The most common method to detect KRAS codon 12 and 13 mutations is by polymerase chain reaction amplification of exon 2 and by direct sequencing of the amplicon. All of the previously discussed issues of specimen selection and quality control that affect EGFR mutational analysis apply to KRAS mutational analysis as well. The impact of KRAS mutations on the rate of recurrence of disease and patient survival has been the subject of many studies, which are difficult to interpret because of differences in tumor stage, histologic inclusion criteria, and rather small numbers of patients. Initially, KRAS was considered a poor prognostic marker, but the data have been contradictory. 56,57 59 KRAS has been also perceived as a negative predictive marker of chemotherapy benefits, on the basis of retrospective studies. With the data presently available, it is not possible to determine with certainty if KRAS mutational status is an independent prognostic marker and/or a negative predictive marker of adjuvant chemotherapy benefit. Several clinical trials 57,60,61 have reported an association between KRAS mutations and a lack of response to EGFR- TKI. In contrast to colon cancer, patients treated with anti- 624 Arch Pathol Lab Med Vol 135, May 2011 Molecular Diagnostics of Lung Carcinomas Dacic
4 EGFR monoclonal antibodies, such as cetuximab, showed no difference in response rate regardless of KRAS mutational status. 31,45,62,63 Similarly, the progression-free survival times in the cetuximab-containing arm and the chemotherapy-alone arm were similar between patients with KRAS wild-type and KRAS mutant tumors. Although many laboratories in the United States routinely perform KRAS mutational analysis of lung carcinomas, the clinical question remains whether there is clinically significant difference in the efficacy of EGFR - TKIs between KRAS mutant adenocarcinomas and KRAS wild-type/egfr wild-type adenocarcinomas. Therefore, for patients without EGFR mutations, the value of determining KRAS mutational status in selecting EGFR- TKI or anti-egfr monoclonal antibodies is uncertain. Development of new therapies targeting the downstream RAS effector pathways PI3K/AKT/mTOR and RAS/ RAF/MEK will probably require knowledge about KRAS mutational status. Secondary Resistance to EGFR Inhibitors T790M EGFR Mutation. The T790M EGFR mutation was initially considered to confer secondary resistance to TKI. 64 Using more sensitive mutation detection techniques, studies showed that this mutation may coexist with L858R mutations; this indicated that T790M might in fact confer pretreatment (primary) resistance to EGFR- TKIs. Importantly, the presence of T790M at such a low frequency did not preclude significant responses to therapy with TKI among patients with sensitivity-conferring EGFR mutations, but it was associated with a significant difference in median progression-free survival. Mesenchymal Epithelial Transition Factor. Amplification of mesenchymal epithelial transition factor (MET) proto-oncogene has been identified as a second mechanism of EGFR-TKI resistance. 65 MET amplification, which has been associated with poor prognosis in different retrospective series, is a relatively uncommon event in NSCLC, occurring in 1% to 7% of unselected cases. Nevertheless, in highly selected cohorts of patients, such as those harboring somatic mutations of EGFR, with acquired resistance to EGFR-TKI, MET amplification can be observed in up to 20% of cases (Figure 2). 66 Somatic EGFR mutations and MET amplification are not mutually exclusive events and, therefore, additional studies will be needed to clarify the role of MET in de novo and/or acquired resistance. Different methodologic approaches can be used to determine gene amplification, but for clinical laboratories using formalin-fixed, paraffin-embedded tissue, FISH assay is an optimal choice. New drugs targeting against the MET kinase receptor or its ligand are available and have shown promising results. A treatment approach, including a combination of EGFR and MET TKI, may be an effective strategy and may lead to the clinical investigation of multiple MET TKIs in combination with erlotinib. OTHER TARGETED THERAPIES Anaplastic Lymphoma Kinase Anaplastic lymphoma kinase (ALK) is a receptor tyrosine kinase originally identified as part of the t(2;5)(p23;35) translocation in a subset of anaplastic large cell lymphomas. 67,68 Subsequent studies 69,70 showed that some solid tumors (inflammatory myofibroblastic tumors, squamous cell carcinomas, and NSCLCs) activate ALK signaling by creating unique oncogenic fusions of the ALK gene (at chromosomal locus 2p23) with a variety of partners through chromosomal translocations; this results in the generation of oncogenic ALK fusion genes and their encoded proteins and leads to constitutive activation of the ALK kinase domain. ALK rearrangements were described in a subset of Asian and white patients with lung adenocarcinomas Most ALK rearrangements in lung adenocarcinoma result from an interstitial deletion and inversion in chromosome arm 2p and result in the EML4-ALK fusion gene product. The oncogenic activity of this fusion product has been effectively blocked by small-molecule inhibitors of ALK. 73,74 Early studies in unselected groups of Asian patients showed that EML4-ALK rearrangement was a relatively rare event occurring in 1% to 7% of lung adenocarcinomas. A recent report 72 has shown a similar observation in early-stage adenocarcinomas in the Western population. However, this rearrangement can be detected in up to 20% of stage IV lung adenocarcinomas, mainly in younger patients with a history of never smoking. None of the ALK-rearranged adenocarcinomas showed coexistent EGFR mutations. Several diagnostic screening tools for EML4-ALK positive tumors have been reported, including reverse transcription polymerase chain reaction (RT-PCR) assays, immunohistochemistry, and FISH. 71,75 77 Several variants that connect various exons of EML4 to ALK have been reported in the literature. Therefore, for optimal and accurate screening of ALK rearrangements, multiplex RT- PCR assays should be designed to detect all of the reported variants. It is uncertain if any clinically significant differences exist between various isoforms, and therefore, RT-PCR as a screening method in this case seems to be less optimal for clinical use. Immunohistochemical detection of EML4-ALK proteins in surgical biopsy, resection, or cytology specimens would be a convenient screening approach for pathologists. Unlike anaplastic large cell lymphoma, immunohistochemical detection of ALK translocation fusion products in lung carcinoma does not necessarily correlate with the presence of translocation. 71,77 However, a recently developed monoclonal antibody (Cell Signaling Technology) shows increased sensitivity for ALK detection, with promise for applicability in the clinical laboratory (Figure 3). 77 This novel immunohistochemical assay correctly identifies ALK-rearranged lung adenocarcinoma with high reproducibility. Because this antibody is not yet available for commercial use, many laboratories are using a FISH break-apart probe to the ALK gene (Vysis LSI ALK Dual Color, Break Apart Rearrangement Probe, Abbott Molecular Abbott Park, Illinois) (Figure 4, A and B). PRACTICAL CONSIDERATIONS FOR MOLECULAR TESTING IN LUNG CARCINOMAS It is obvious that molecular testing of lung carcinoma should be the standard of care, but there are many practical, logistic, and technical questions that need to be addressed. The first is which laboratory should be allowed to perform the testing. Only accredited, CLIA (Clinical Laboratory Improvement Amendments of 1988) certified laboratories with appropriate quality control standards should carry out this type of molecular testing. The Society Arch Pathol Lab Med Vol 135, May 2011 Molecular Diagnostics of Lung Carcinomas Dacic 625
5 Figure 2. Fluorescence in situ hybridization assay with c-met (RP11-163C9, Children s Hospital Oakland Research Institute, Oakland, California) and centromeric (CEP7) probes in lung adenocarcinoma demonstrates amplification of mesenchymal epithelial transition factor (MET) (original magnification 3200). Figure 3. Detection of anaplastic lymphoma kinase (ALK) translocation by immunohistochemistry (original magnification 340). Courtesy of Lucian Chirieac, MD, Brigham and Women s Hospital, Boston, Massachusetts. Figure 4. Break-apart fluorescence in situ hybridization probe to the anaplastic lymphoma kinase (ALK) gene (Vysis LSI ALK Dual Color, Break Apart Rearrangement Probe, Abbott Molecular, Abbott Park, Illinois). A, Normal cells. Cells without translocation show green and orange signals in juxtaposition. B, Example of lung adenocarcinoma with ALK translocation: 1 pair of fused signals (green and orange) with 1 separate green signal and 1 separate orange signal. of European Pathologists has recommended that only laboratories with an analytic success rate of 95% and an accuracy rate of more than 97% be allowed to perform KRAS mutational testing in colon cancer. At the present time, it is uncertain how many laboratories can achieve this standard. Therefore, different laboratories should share protocols and exchange positive and negative control samples to improve overall analytic performance, and they should implement a system for validation of techniques and results. Since molecular workup represents an additional step in the diagnostic workup of available tumor tissue, one of the aims should be to provide results in a timely manner. Therefore, the question is whether molecular testing should be integrated into the workflow of on site pathology laboratories or whether the tissue should be sent to commercial laboratories. The IASLC European Thoracic Oncology Platform Multidisciplinary Workshop has proposed a 626 Arch Pathol Lab Med Vol 135, May 2011 possible scenario for diagnostic and molecular workup of lung cancer cases (Figure 5). This approach has been already used by many large academic centers in the United States, but the question remains as to how lung cancer specimens will be handled by community hospitals that do not have adequate molecular laboratory support. A turnaround time of 2 weeks from diagnostic procedure to the final report has been suggested, but organizing a system that would include multiple parties, from pathology, oncology, and thoracic surgery to reference laboratories, seems to be quite challenging. Testing by outside laboratories also brings up another challenge, such as integration of all available data about the tumor (eg, histology, stage, and mutational profile) in one pathology report and in the patient s medical records, which is simple if testing is performed at a single institution. A common question is who should request the mutational profiling: a treating physician or a Molecular Diagnostics of Lung Carcinomas Dacic
6 Figure 5. Proposed workflow for lung carcinoma by the European EGFR Workshop Group. Abbreviations: EGFR, epidermal growth factor receptor; IHC, immunohistochemistry. Modified with permission from Pirker et al. 9 pathologist? This question emphasizes the importance of close communication between pathologists and treating physicians. Our institution s policy is for pathologists to order mutational profiling at the time of the diagnostic workup. This policy was implemented after discussion with thoracic oncologists and surgeons. The rationale behind reflex testing was to reduce the turnaround time for molecular testing and to provide a complete histologic/molecular profile of the tumor at the time of patient discharge or office visit. SUMMARY The diagnostic and treatment approaches to lung carcinoma, primarily adenocarcinomas, are undergoing a revolution. The classification of lung carcinoma is going beyond small cell carcinoma and NSCLC, and precise subclassification of NSCLC has a direct impact on a patient s management and prognosis. Many new targeted therapies are under development, and the molecular testing of lung carcinoma has become the standard of care in a very short period of time. EGFR mutations have emerged as a key predictive biomarker for EGFR-TKI treatment and should be the primary standard for selection of patients for first-line treatment with EGFR-TKIs. Clinical testing for EGFR mutations and other predictors of response should be optimized and standardized in regard to mutational techniques, specimen and tumor types, and result reporting. Many new drugs are on the horizon, and routine molecular diagnostics for lung cancer is going beyond EGFR mutational profiling. There is already a need for more efficient screening for multiple mutations by using high-throughput/high-sensitivity technology. References 1. Jemal A, Siegel R, Xu J, Ward E. Cancer statistics, CA Cancer J Clin. 2010;60(5): Winer E, Gralow J, Diller L, et al. Clinical cancer advances 2008: major research advances in cancer treatment, prevention, and screening a report from the American Society of Clinical Oncology. J Clin Oncol. 2009;27(5): Giaccone G, Herbst RS, Manegold C, et al. Gefitinib in combination with gemcitabine and cisplatin in advanced non-small-cell lung cancer: a phase III trial INTACT 1. J Clin Oncol. 2004;22(5): Herbst RS, Prager D, Hermann R, et al. TRIBUTE: a phase III trial of erlotinib hydrochloride (OSI-774) combined with carboplatin and paclitaxel chemotherapy in advanced non-small-cell lung cancer. J Clin Oncol. 2005;23(25): Thatcher N, Chang A, Parikh P, et al. Gefitinib plus best supportive care in previously treated patients with refractory advanced non-small-cell lung cancer: results from a randomised, placebo-controlled, multicentre study (Iressa Survival Evaluation in Lung Cancer). Lancet. 2005;366(9496): Lynch TJ, Bell DW, Sordella R, et al. Activating mutations in the epidermal growth factor receptor underlying responsiveness of non-small-cell lung cancer to gefitinib. N Engl J Med. 2004;350(21): Paez JG, Janne PA, Lee JC, et al. EGFR mutations in lung cancer: correlation with clinical response to gefitinib therapy. Science. 2004;304(5676): Pao W, Miller V, Zakowski M, et al. EGF receptor gene mutations are common in lung cancers from never smokers and are associated with sensitivity of tumors to gefitinib and erlotinib. Proc Natl Acad Sci U S A. 2004; 101(36): Pirker R, Herth FJ, Kerr KM, et al. Consensus for EGFR mutation testing in non-small cell lung cancer: results from a European workshop. J Thorac Oncol. 2010;5(10): Sandler A, Gray R, Perry MC, et al. Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med. 2006;355(24): Johnson DH, Fehrenbacher L, Novotny WF, et al. Randomized phase II trial comparing bevacizumab plus carboplatin and paclitaxel with carboplatin and paclitaxel alone in previously untreated locally advanced or metastatic nonsmall-cell lung cancer. J Clin Oncol. 2004;22(11): West H, Harpole D, Travis W. Histologic considerations for individualized systemic therapy approaches for the management of non-small cell lung cancer. Chest. 2009;136(4): Eberhard DA, Giaccone G, Johnson BE. Biomarkers of response to epidermal growth factor receptor inhibitors in Non-Small-Cell Lung Cancer Working Group: standardization for use in the clinical trial setting. J Clin Oncol. 2008;26(6): Bozzetti C, Tiseo M, Lagrasta C, et al. Comparison between epidermal growth factor receptor (EGFR) gene expression in primary non-small cell lung cancer (NSCLC) and in fine-needle aspirates from distant metastatic sites. J Thorac Oncol. 2008;3(1): Italiano A, Vandenbos FB, Otto J, et al. Comparison of the epidermal growth factor receptor gene and protein in primary non-small-cell-lung cancer and metastatic sites: implications for treatment with EGFR-inhibitors. Ann Oncol. 2006;17(6): Gallegos Ruiz MI, van Cruijsen H, Smit EF, et al. Genetic heterogeneity in patients with multiple neoplastic lung lesions: a report of three cases. J Thorac Oncol. 2007;2(1): Kalikaki A, Koutsopoulos A, Trypaki M, et al. Comparison of EGFR and K- RAS gene status between primary tumours and corresponding metastases in NSCLC. Br J Cancer. 2008;99(6): Arch Pathol Lab Med Vol 135, May 2011 Molecular Diagnostics of Lung Carcinomas Dacic 627
7 18. Monaco SE, Nikiforova MN, Cieply K, Teot LA, Khalbuss WE, Dacic S. A comparison of EGFR and KRAS status in primary lung carcinoma and matched metastases. Hum Pathol. 2010;41(1): Akbari M, Hansen MD, Halgunset J, Skorpen F, Krokan HE. Low copy number DNA template can render polymerase chain reaction error prone in a sequence-dependent manner. J Mol Diagn. 2005;7(1): Hunt JL, Finkelstein SD. Microdissection techniques for molecular testing in surgical pathology. Arch Pathol Lab Med. 2004;128(12): Pao W, Ladanyi M. Epidermal growth factor receptor mutation testing in lung cancer: searching for the ideal method. Clin Cancer Res. 2007;13(17): Hoshi K, Takakura H, Mitani Y, et al. Rapid detection of epidermal growth factor receptor mutations in lung cancer by the SMart-Amplification Process. Clin Cancer Res. 2007;13(17): Endo K, Konishi A, Sasaki H, et al. Epidermal growth factor receptor gene mutation in non-small cell lung cancer using highly sensitive and fast TaqMan PCR assay. Lung Cancer. 2005;50(3): Zhou C, Ni J, Zhao Y, Su B. Rapid detection of epidermal growth factor receptor mutations in non-small cell lung cancer using real-time polymerase chain reaction with TaqMan-MGB probes. Cancer J. 2006;12(1): Yatabe Y, Hida T, Horio Y, Kosaka T, Takahashi T, Mitsudomi T. A rapid, sensitive assay to detect EGFR mutation in small biopsy specimens from lung cancer. J Mol Diagn. 2006;8(3): Pan Q, Pao W, Ladanyi M. Rapid polymerase chain reaction-based detection of epidermal growth factor receptor gene mutations in lung adenocarcinomas. J Mol Diagn. 2005;7(3): Janne PA, Borras AM, Kuang Y, et al. A rapid and sensitive enzymatic method for epidermal growth factor receptor mutation screening. Clin Cancer Res. 2006;12: Williams C, Ponten F, Moberg C, et al. A high frequency of sequence alterations is due to formalin fixation of archival specimens. Am J Pathol. 1999; 155(5): Smouse JH, Cibas ES, Janne PA, Joshi VA, Zou KH, Lindeman NI. EGFR mutations are detected comparably in cytologic and surgical pathology specimens of nonsmall cell lung cancer. Cancer Cytopathol. 2009;117(1): Solomon SB, Zakowski MF, Pao W, et al. Core needle lung biopsy specimens: adequacy for EGFR and KRAS mutational analysis. AJR Am J Roentgenol. 2010;194(1): Pirker R, Pereira JR, Szczesna A, et al. Cetuximab plus chemotherapy in patients with advanced non-small-cell lung cancer (FLEX): an open-label randomised phase III trial. Lancet. 2009;373(9674): Robert F, Blumenschein G, Herbst RS, et al. Phase I/IIa study of cetuximab with gemcitabine plus carboplatin in patients with chemotherapy-naive advanced non-small-cell lung cancer. J Clin Oncol. 2005;23(36): Thienelt CD, Bunn PA Jr, Hanna N, et al. Multicenter phase I/II study of cetuximab with paclitaxel and carboplatin in untreated patients with stage IV non-small-cell lung cancer. J Clin Oncol. 2005;23(34): Fukuoka M, Yano S, Giaccone G, et al. Multi-institutional randomized phase II trial of gefitinib for previously treated patients with advanced nonsmall-cell lung cancer (The IDEAL 1 Trial). J Clin Oncol. 2003;21(12): Herbst RS, Giaccone G, Schiller JH, et al. Gefitinib in combination with paclitaxel and carboplatin in advanced non-small-cell lung cancer: a phase III trial INTACT 2. J Clin Oncol. 2004;22(5): Hirsch FR, Varella-Garcia M, Cappuzzo F, et al. Combination of EGFR gene copy number and protein expression predicts outcome for advanced nonsmall-cell lung cancer patients treated with gefitinib. Ann Oncol. 2007;18(4): Hirsch FR, Varella-Garcia M, McCoy J, et al. Increased epidermal growth factor receptor gene copy number detected by fluorescence in situ hybridization associates with increased sensitivity to gefitinib in patients with bronchioloalveolar carcinoma subtypes: a Southwest Oncology Group Study. J Clin Oncol. 2005;23(28): Cappuzzo F, Hirsch FR, Rossi E, et al. Epidermal growth factor receptor gene and protein and gefitinib sensitivity in non-small-cell lung cancer. J Natl Cancer Inst. 2005;97(9): Mok TS, Wu YL, Thongprasert S, et al. Gefitinib or carboplatin-paclitaxel in pulmonary adenocarcinoma. N Engl J Med. 2009;361(10): Sequist LV, Martins RG, Spigel D, et al. First-line gefitinib in patients with advanced non-small-cell lung cancer harboring somatic EGFR mutations. J Clin Oncol. 2008;26(15): Sharma SV, Bell DW, Settleman J, Haber DA. Epidermal growth factor receptor mutations in lung cancer. Nat Rev Cancer. 2007;7(3): Eberhard DA, Johnson BE, Amler LC, et al. Mutations in the epidermal growth factor receptor and in KRAS are predictive and prognostic indicators in patients with non-small-cell lung cancer treated with chemotherapy alone and in combination with erlotinib. J Clin Oncol. 2005;23(25): Jackman DM, Yeap BY, Sequist LV, et al. Exon 19 deletion mutations of epidermal growth factor receptor are associated with prolonged survival in nonsmall cell lung cancer patients treated with gefitinib or erlotinib. Clin Cancer Res. 2006;12(13): Sasaki H, Shimizu S, Endo K, et al. EGFR and erbb2 mutation status in Japanese lung cancer patients. Int J Cancer. 2006;118(1): Hirsch FR, Herbst RS, Olsen C, et al. Increased EGFR gene copy number detected by fluorescent in situ hybridization predicts outcome in non-small-cell lung cancer patients treated with cetuximab and chemotherapy. J Clin Oncol. 2008;26(20): Sholl LM, John Iafrate A, Chou Y-P, et al. Validation of chromogenic in situ hybridization for detection of EGFR copy number amplification in nonsmall cell lung carcinoma. Mod Pathol. 2007;20(10): Han SW, Kim TY, Jeon YK, et al. Optimization of patient selection for gefitinib in non-small cell lung cancer by combined analysis of epidermal growth factor receptor mutation, K-ras mutation, and Akt phosphorylation. Clin Cancer Res. 2006;12(8): Endo K, Sasaki H, Yano M, et al. Evaluation of the epidermal growth factor receptor gene mutation and copy number in non-small cell lung cancer with gefitinib therapy. Oncol Rep. 2006;16(3): Yu J, Kane S, Wu J, et al. Mutation-specific antibodies for the detection of EGFR mutations in non-small-cell lung cancer. Clin Cancer Res. 2009;15(9): Brevet M, Arcila M, Ladanyi M. Assessment of EGFR mutation status in lung adenocarcinoma by immunohistochemistry using antibodies specific to the two major forms of mutant EGFR. J Mol Diagn. 2010;12(2): Linardou H, Dahabreh IJ, Bafaloukos D, Kosmidis P, Murray S. Somatic EGFR mutations and efficacy of tyrosine kinase inhibitors in NSCLC. Nat Rev Clin Oncol. 2009;6(6): Herbst RS, Lippman SM. Molecular signatures of lung cancer toward personalized therapy. N Engl J Med. 2007;356(1): Herbst RS, Heymach JV, Lippman SM. Lung cancer. N Engl J Med. 2008; 359(13): Ahrendt SA, Decker PA, Alawi EA, et al. Cigarette smoking is strongly associated with mutation of the K-ras gene in patients with primary adenocarcinoma of the lung. Cancer. 2001;92(6): Riely GJ, Kris MG, Rosenbaum D, et al. Frequency and distinctive spectrum of KRAS mutations in never smokers with lung adenocarcinoma. Clin Cancer Res. 2008;14(18): Marks JL, Broderick S, Zhou Q, et al. Prognostic and therapeutic implications of EGFR and KRAS mutations in resected lung adenocarcinoma. J Thorac Oncol. 2008;3(2): Pao W, Wang TY, Riely GJ, et al. KRAS mutations and primary resistance of lung adenocarcinomas to gefitinib or erlotinib. PLoS Med. 2005;2(1):e17. doi: /journal.pmed Roberts PJ, Stinchcombe TE, Der CJ, Socinski MA. Personalized medicine in non-small-cell lung cancer: is KRAS a useful marker in selecting patients for epidermal growth factor receptor-targeted therapy? J Clin Oncol. 2010;28(31): Marchetti A, Milella M, Felicioni L, et al. Clinical implications of KRAS mutations in lung cancer patients treated with tyrosine kinase inhibitors: an important role for mutations in minor clones. Neoplasia. 2009;11(10): Miller VA, Riely GJ, Zakowski MF, et al. Molecular characteristics of bronchioloalveolar carcinoma and adenocarcinoma, bronchioloalveolar carcinoma subtype, predict response to erlotinib. J Clin Oncol. 2008;26(9): Zhu CQ, da Cunha Santos G, Ding K, et al. Role of KRAS and EGFR as biomarkers of response to erlotinib in National Cancer Institute of Canada Clinical Trials Group Study BR.21. J Clin Oncol. 2008;26(26): Robert F, Blumenschein G, Herbst RS, et al. Phase I/IIa study of cetuximab with gemcitabine plus carboplatin in patients with chemotherapy-naive advanced non-small-cell lung cancer. J Clin Oncol. 2005;23(36): Govindan R. Cetuximab in advanced non-small cell lung cancer. Clin Cancer Res. 2004;10:4241s 4244s. 64. Pao W, Miller VA, Politi KA, et al. Acquired resistance of lung adenocarcinomas to gefitinib or erlotinib is associated with a second mutation in the EGFR kinase domain. PLoS Med. 2005;2(3):e73. doi: / journal.pmed Engelman JA, Zejnullahu K, Mitsudomi T, et al. MET amplification leads to gefitinib resistance in lung cancer by activating ERBB3 signaling. Science. 2007; 316(5827): Bean J, Brennan C, Shih J-Y, et al. MET amplification occurs with or without T790M mutations in EGFR mutant lung tumors with acquired resistance to gefitinib or erlotinib. Proc Natl Acad Sci U S A. 2007;104(52): Lamant L, Meggetto F, al Saati T, et al. High incidence of the t(2;5)(p23;q35) translocation in anaplastic large cell lymphoma and its lack of detection in Hodgkin s disease: comparison of cytogenetic analysis, reverse transcriptase-polymerase chain reaction, and P-80 immunostaining. Blood. 1996; 87(1): Morris SW, Kirstein MN, Valentine MB, et al. Fusion of a kinase gene, ALK, to a nucleolar protein gene, NPM, in non-hodgkin s lymphoma [erratum in: Science. 1995;267(5196): ; PMID: ]. Science. 1994;263(5151): Bridge JA, Kanamori M, Ma Z, et al. Fusion of the ALK gene to the clathrin heavy chain gene, CLTC, in inflammatory myofibroblastic tumor. Am J Pathol. 2001;159(2): Soda M, Choi YL, Enomoto M, et al. Identification of the transforming EML4-ALK fusion gene in non-small-cell lung cancer. Nature. 2007;448(7153): Arch Pathol Lab Med Vol 135, May 2011 Molecular Diagnostics of Lung Carcinomas Dacic
8 71. Rodig SJ, Mino-Kenudson M, Dacic S, et al. Unique clinicopathologic features characterize ALK-rearranged lung adenocarcinoma in the western population. Clin Cancer Res. 2009;15(16): Shaw AT, Yeap BY, Mino-Kenudson M, et al. Clinical features and outcome of patients with non-small-cell lung cancer who harbor EML4-ALK. J Clin Oncol. 2009;27(26): Sasaki T, Rodig SJ, Chirieac LR, Janne PA. The biology and treatment of EML4-ALK non-small cell lung cancer. Eur J Cancer. 2010;46(10): Koivunen JP, Mermel C, Zejnullahu K, et al. EML4-ALK fusion gene and efficacy of an ALK kinase inhibitor in lung cancer. Clin Cancer Res. 2008;14(13): Takeuchi K, Choi YL, Soda M, et al. Multiplex reverse transcription-pcr screening for EML4-ALK fusion transcripts. Clin Cancer Res. 2008;14(20): Choi YL, Takeuchi K, Soda M, et al. Identification of novel isoforms of the EML4-ALK transforming gene in non-small cell lung cancer. Cancer Res. 2008; 68(13): Mino-Kenudson M, Chirieac LR, Law K, et al. A novel, highly sensitive antibody allows for the routine detection of ALK-rearranged lung adenocarcinomas by standard immunohistochemistry. Clin Cancer Res. 2010;16(5): Chirieac L, Dacic S. Targeted therapies in lung cancer. Surg Pathol Clin. 2010; 3(1):73. Arch Pathol Lab Med Vol 135, May 2011 Molecular Diagnostics of Lung Carcinomas Dacic 629
Molecular Diagnosis of Lung Cancer
 Molecular Diagnosis of Lung Cancer Lucian R. Chirieac, M.D. Assistant Professor of Pathology Harvard Medical School Staff Pathologist, Department of Pathology Brigham and Women's Hospital 75 Francis Street
Molecular Diagnosis of Lung Cancer Lucian R. Chirieac, M.D. Assistant Professor of Pathology Harvard Medical School Staff Pathologist, Department of Pathology Brigham and Women's Hospital 75 Francis Street
An ongoing research and multiple clinical
 TARGETED THERAPIES IN LUNG CANCER Lucian R. Chirieac, MD a, *, Sanja Dacic, MD, PhD b KEYWORDS Lung cancer Adenocarcinoma Squamous Tyrosine kinase inhibitors Molecular pathogenesis ABSTRACT An ongoing
TARGETED THERAPIES IN LUNG CANCER Lucian R. Chirieac, MD a, *, Sanja Dacic, MD, PhD b KEYWORDS Lung cancer Adenocarcinoma Squamous Tyrosine kinase inhibitors Molecular pathogenesis ABSTRACT An ongoing
Personalized Medicine: Lung Biopsy and Tumor
 Personalized Medicine: Lung Biopsy and Tumor Mutation Testing Elizabeth H. Moore, MD Personalized Medicine: Lung Biopsy and Tumor Mutation Testing Genomic testing has resulted in a paradigm shift in the
Personalized Medicine: Lung Biopsy and Tumor Mutation Testing Elizabeth H. Moore, MD Personalized Medicine: Lung Biopsy and Tumor Mutation Testing Genomic testing has resulted in a paradigm shift in the
EGFR, Lung Cancer and Cytology. Maureen F. Zakowski, M.D. Lung cancer is one of the most lethal cancers in Western countries and in Japan.
 EGFR, Lung Cancer and Cytology Maureen F. Zakowski, M.D. Lung cancer is one of the most lethal cancers in Western countries and in Japan. It is histopathologically divided into two major sub-groups: Small
EGFR, Lung Cancer and Cytology Maureen F. Zakowski, M.D. Lung cancer is one of the most lethal cancers in Western countries and in Japan. It is histopathologically divided into two major sub-groups: Small
Corporate Medical Policy
 Corporate Medical Policy Molecular Analysis for Targeted Therapy for Non-Small Cell Lung File Name: Origination: Last CAP Review: Next CAP Review: Last Review: molecular_analysis_for_targeted_therapy_for_non_small_cell_lung_cancer
Corporate Medical Policy Molecular Analysis for Targeted Therapy for Non-Small Cell Lung File Name: Origination: Last CAP Review: Next CAP Review: Last Review: molecular_analysis_for_targeted_therapy_for_non_small_cell_lung_cancer
SUBJECT: GENOTYPING - EPIDERMAL GROWTH
 MEDICAL POLICY SUBJECT: GENOTYPING - EPIDERMAL GROWTH Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature
MEDICAL POLICY SUBJECT: GENOTYPING - EPIDERMAL GROWTH Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature
7/6/2015. Cancer Related Deaths: United States. Management of NSCLC TODAY. Emerging mutations as predictive biomarkers in lung cancer: Overview
 Emerging mutations as predictive biomarkers in lung cancer: Overview Kirtee Raparia, MD Assistant Professor of Pathology Cancer Related Deaths: United States Men Lung and bronchus 28% Prostate 10% Colon
Emerging mutations as predictive biomarkers in lung cancer: Overview Kirtee Raparia, MD Assistant Professor of Pathology Cancer Related Deaths: United States Men Lung and bronchus 28% Prostate 10% Colon
EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence
 102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
Test Category: Prognostic and Predictive. Clinical Scenario
 Use of Epidermal Growth Factor Receptor (EGFR) Mutation Analysis in Patients with Advanced Non-Small-Cell Lung Cancer (NSCLC) to Determine Erlotinib Use as First-line Therapy Test Category: Prognostic
Use of Epidermal Growth Factor Receptor (EGFR) Mutation Analysis in Patients with Advanced Non-Small-Cell Lung Cancer (NSCLC) to Determine Erlotinib Use as First-line Therapy Test Category: Prognostic
Osamu Tetsu, MD, PhD Associate Professor Department of Otolaryngology-Head and Neck Surgery School of Medicine, University of California, San
 Osamu Tetsu, MD, PhD Associate Professor Department of Otolaryngology-Head and Neck Surgery School of Medicine, University of California, San Francisco Lung Cancer Classification Pathological Classification
Osamu Tetsu, MD, PhD Associate Professor Department of Otolaryngology-Head and Neck Surgery School of Medicine, University of California, San Francisco Lung Cancer Classification Pathological Classification
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective
 Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Frequency of EGFR Mutation and EML4-ALK fusion gene in Arab Patients with Adenocarcinoma of the Lung
 HeSMO 6(2) 2015 19 23 DOI: 10.1515/fco-2015-0009 Forum of Clinical Oncology Frequency of EGFR Mutation and EML4-ALK fusion gene in Arab Patients with Adenocarcinoma of the Lung Hanan Ezzat Shafik 1 *,
HeSMO 6(2) 2015 19 23 DOI: 10.1515/fco-2015-0009 Forum of Clinical Oncology Frequency of EGFR Mutation and EML4-ALK fusion gene in Arab Patients with Adenocarcinoma of the Lung Hanan Ezzat Shafik 1 *,
Updated Molecular Testing Guideline for the Selection of Lung Cancer Patients for Treatment with Targeted Tyrosine Kinase Inhibitors
 Q: How is the strength of recommendation determined in the new molecular testing guideline? A: The strength of recommendation is determined by the strength of the available data (evidence). Strong Recommendation:
Q: How is the strength of recommendation determined in the new molecular testing guideline? A: The strength of recommendation is determined by the strength of the available data (evidence). Strong Recommendation:
Molecular Testing in Lung Cancer
 Molecular Testing in Lung Cancer Pimpin Incharoen, M.D. Assistant Professor, Thoracic Pathology Department of Pathology, Ramathibodi Hospital Genetic alterations in lung cancer Source: Khono et al, Trans
Molecular Testing in Lung Cancer Pimpin Incharoen, M.D. Assistant Professor, Thoracic Pathology Department of Pathology, Ramathibodi Hospital Genetic alterations in lung cancer Source: Khono et al, Trans
Lung Adenocarcinoma with EGFR Amplification Has Distinct Clinicopathologic and Molecular Features in Never-Smokers
 Lung Adenocarcinoma with EGFR Amplification Has Distinct Clinicopathologic and Molecular Features in Never-Smokers The Harvard community has made this article openly available. Please share how this access
Lung Adenocarcinoma with EGFR Amplification Has Distinct Clinicopathologic and Molecular Features in Never-Smokers The Harvard community has made this article openly available. Please share how this access
Disclosures Genomic testing in lung cancer
 Disclosures Genomic testing in lung cancer No disclosures Objectives Understand how FISH and NGS provide complementary data for the evaluation of lung cancer Recognize the challenges of performing testing
Disclosures Genomic testing in lung cancer No disclosures Objectives Understand how FISH and NGS provide complementary data for the evaluation of lung cancer Recognize the challenges of performing testing
Changing demographics of smoking and its effects during therapy
 Changing demographics of smoking and its effects during therapy Egbert F. Smit MD PhD. Dept. Pulmonary Diseases, Vrije Universiteit Medical Centre, Amsterdam, The Netherlands Smoking prevalence adults
Changing demographics of smoking and its effects during therapy Egbert F. Smit MD PhD. Dept. Pulmonary Diseases, Vrije Universiteit Medical Centre, Amsterdam, The Netherlands Smoking prevalence adults
Page: 1 of 27. Molecular Analysis for Targeted Therapy of Non-Small-Cell Lung Cancer
 Last Review Status/Date: December 2014 Page: 1 of 27 Non-Small-Cell Lung Cancer Description Over half of patients with non-small-cell lung cancer (NSCLC) present with advanced and therefore incurable disease,
Last Review Status/Date: December 2014 Page: 1 of 27 Non-Small-Cell Lung Cancer Description Over half of patients with non-small-cell lung cancer (NSCLC) present with advanced and therefore incurable disease,
Refining Prognosis of Early Stage Lung Cancer by Molecular Features (Part 2): Early Steps in Molecularly Defined Prognosis
 5/17/13 Refining Prognosis of Early Stage Lung Cancer by Molecular Features (Part 2): Early Steps in Molecularly Defined Prognosis Johannes Kratz, MD Post-doctoral Fellow, Thoracic Oncology Laboratory
5/17/13 Refining Prognosis of Early Stage Lung Cancer by Molecular Features (Part 2): Early Steps in Molecularly Defined Prognosis Johannes Kratz, MD Post-doctoral Fellow, Thoracic Oncology Laboratory
Platinum-based doublets are considered to be the standard
 Blackwell Publishing Asia Review Article Recent trends in the treatment of advanced lung cancer Nagahiro Saijo 1 National Cancer Center, Hospital East, Kashiwanoha 6-5-1, Kashiwa-shi, Chiba 277-8577, Japan
Blackwell Publishing Asia Review Article Recent trends in the treatment of advanced lung cancer Nagahiro Saijo 1 National Cancer Center, Hospital East, Kashiwanoha 6-5-1, Kashiwa-shi, Chiba 277-8577, Japan
Frequency of Epidermal Growth Factor Mutation Status and Its Effect on Outcome of Patients with Adenocarcinoma of the Lung
 Journal of Cancer Therapy, 2014, 5, 1012-1020 Published Online September 2014 in SciRes. http://www.scirp.org/journal/jct http://dx.doi.org/10.4236/jct.2014.511106 Frequency of Epidermal Growth Factor
Journal of Cancer Therapy, 2014, 5, 1012-1020 Published Online September 2014 in SciRes. http://www.scirp.org/journal/jct http://dx.doi.org/10.4236/jct.2014.511106 Frequency of Epidermal Growth Factor
Joachim Aerts Erasmus MC Rotterdam, Netherlands. Drawing the map: molecular characterization of NSCLC
 Joachim Aerts Erasmus MC Rotterdam, Netherlands Drawing the map: molecular characterization of NSCLC Disclosures Honoraria for advisory board/consultancy/speakers fee Eli Lilly Roche Boehringer Ingelheim
Joachim Aerts Erasmus MC Rotterdam, Netherlands Drawing the map: molecular characterization of NSCLC Disclosures Honoraria for advisory board/consultancy/speakers fee Eli Lilly Roche Boehringer Ingelheim
RESEARCH ARTICLE. Ryosuke Hirano 1, Junji Uchino 1 *, Miho Ueno 2, Masaki Fujita 1, Kentaro Watanabe 1. Abstract. Introduction
 RESEARCH ARTICLE Low-dose Epidermal Growth Factor Receptor (EGFR)- Tyrosine Kinase Inhibition of EGFR Mutation-positive Lung Cancer: Therapeutic Benefits and Associations Between Dosage, Efficacy and Body
RESEARCH ARTICLE Low-dose Epidermal Growth Factor Receptor (EGFR)- Tyrosine Kinase Inhibition of EGFR Mutation-positive Lung Cancer: Therapeutic Benefits and Associations Between Dosage, Efficacy and Body
Quality in Control ALK-Lung Analyte Control (EML4-ALK) ALK-Lymphoma Analyte Control (NPM-ALK)
 Quality in Control ALK-Lung Analyte Control (EML4-ALK) ALK-Lymphoma Analyte Control (NPM-ALK) 10 Product Codes: HCL007, HCL008 and HCL009 HCL010, HCL011 and HCL012 Page 1 of Contents 1. What is ALK?...
Quality in Control ALK-Lung Analyte Control (EML4-ALK) ALK-Lymphoma Analyte Control (NPM-ALK) 10 Product Codes: HCL007, HCL008 and HCL009 HCL010, HCL011 and HCL012 Page 1 of Contents 1. What is ALK?...
ALK Fusion Oncogenes in Lung Adenocarcinoma
 ALK Fusion Oncogenes in Lung Adenocarcinoma Vincent A Miller, MD Associate Attending Physician, Thoracic Oncology Service Memorial Sloan-Kettering Cancer Center New York, New York The identification of
ALK Fusion Oncogenes in Lung Adenocarcinoma Vincent A Miller, MD Associate Attending Physician, Thoracic Oncology Service Memorial Sloan-Kettering Cancer Center New York, New York The identification of
Detection of Anaplastic Lymphoma Kinase (ALK) gene in Non-Small Cell lung Cancer (NSCLC) By CISH Technique
 Cancer and Clinical Oncology; Vol. 7, No. 1; 2018 ISSN 1927-4858 E-ISSN 1927-4866 Published by Canadian Center of Science and Education Detection of Anaplastic Lymphoma Kinase (ALK) gene in Non-Small Cell
Cancer and Clinical Oncology; Vol. 7, No. 1; 2018 ISSN 1927-4858 E-ISSN 1927-4866 Published by Canadian Center of Science and Education Detection of Anaplastic Lymphoma Kinase (ALK) gene in Non-Small Cell
Identification of Novel Variant of EML4-ALK Fusion Gene in NSCLC: Potential Benefits of the RT-PCR Method
 International journal of Biomedical science ORIGINAL ARTICLE Identification of Novel Variant of EML4-ALK Fusion Gene in NSCLC: Potential Benefits of the RT-PCR Method Martin K. H. Maus 1, 2, Craig Stephens
International journal of Biomedical science ORIGINAL ARTICLE Identification of Novel Variant of EML4-ALK Fusion Gene in NSCLC: Potential Benefits of the RT-PCR Method Martin K. H. Maus 1, 2, Craig Stephens
Lung adenocarcinoma: guiding EGFR-targeted therapy and beyond
 & 2008 USCAP, Inc All rights reserved 0893-3952/08 $30.00 www.modernpathology.org : guiding EGFR-targeted therapy and beyond Marc Ladanyi and William Pao Departments of Pathology and Medicine, and Human
& 2008 USCAP, Inc All rights reserved 0893-3952/08 $30.00 www.modernpathology.org : guiding EGFR-targeted therapy and beyond Marc Ladanyi and William Pao Departments of Pathology and Medicine, and Human
Role of molecular studies in the diagnosis of lung adenocarcinoma
 & 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 S11 Role of molecular studies in the diagnosis of lung adenocarcinoma Samuel A Yousem Department of Pathology, University of Pittsburgh Medical
& 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 S11 Role of molecular studies in the diagnosis of lung adenocarcinoma Samuel A Yousem Department of Pathology, University of Pittsburgh Medical
Lung cancer is the most common cause of cancer death in
 ORIGINAL ARTICLE Are There Imaging Characteristics Associated with Epidermal Growth Factor Receptor and Mutations in Patients with Adenocarcinoma of the Lung with Bronchioloalveolar Features? Catherine
ORIGINAL ARTICLE Are There Imaging Characteristics Associated with Epidermal Growth Factor Receptor and Mutations in Patients with Adenocarcinoma of the Lung with Bronchioloalveolar Features? Catherine
IRESSA (Gefitinib) The Journey. Anne De Bock Portfolio Leader, Oncology/Infection European Regulatory Affairs AstraZeneca
 IRESSA (Gefitinib) The Journey Anne De Bock Portfolio Leader, Oncology/Infection European Regulatory Affairs AstraZeneca Overview The Drug The Biomarker and Clinical Trials Sampling Lessons Learned The
IRESSA (Gefitinib) The Journey Anne De Bock Portfolio Leader, Oncology/Infection European Regulatory Affairs AstraZeneca Overview The Drug The Biomarker and Clinical Trials Sampling Lessons Learned The
Lung cancer ranks as the leading cause of cancer-related
 Review Article Reflex Testing for Epidermal Growth Factor Receptor Mutation and Anaplastic Lymphoma Kinase Fluorescence In Situ Hybridization in Non Small Cell Lung Cancer Mari Mino-Kenudson, MD; Eugene
Review Article Reflex Testing for Epidermal Growth Factor Receptor Mutation and Anaplastic Lymphoma Kinase Fluorescence In Situ Hybridization in Non Small Cell Lung Cancer Mari Mino-Kenudson, MD; Eugene
Interpretation Guide. Product Name: ALK Cell Line Analyte Control Product Codes: ALK2/CS and ALK2/CB. Page 1 of 9
 Interpretation Guide Product Name: ALK Cell Line Analyte Control Product Codes: ALK2/CS and ALK2/CB ALK2/CS/CB_IG_V_001 www.histocyte.com Page 1 of 9 Contents 1. What is ALK?... 2 2. Role of ALK in Cancer...
Interpretation Guide Product Name: ALK Cell Line Analyte Control Product Codes: ALK2/CS and ALK2/CB ALK2/CS/CB_IG_V_001 www.histocyte.com Page 1 of 9 Contents 1. What is ALK?... 2 2. Role of ALK in Cancer...
1. Q: What has changed from the draft recommendations posted for public comment in November/December 2011?
 Frequently Asked Questions (FAQs) in regard to Molecular Testing Guideline for Selection of Lung Cancer Patients for EGFR and ALK Tyrosine Kinase Inhibitors 1. Q: What has changed from the draft recommendations
Frequently Asked Questions (FAQs) in regard to Molecular Testing Guideline for Selection of Lung Cancer Patients for EGFR and ALK Tyrosine Kinase Inhibitors 1. Q: What has changed from the draft recommendations
AHFS Final. line. Criteria Used in. combined. cisplatin. Strength. established was. Non-small Cell Lung. Cancer: of carboplatin and
 Drug/Drug Combination: Cetuximab Off-label Use: First-line treatment of advanced non-small Use for Review: cell lung cancer Criteria Used in Selection of Off-labell AHFS Final Determination of Medical
Drug/Drug Combination: Cetuximab Off-label Use: First-line treatment of advanced non-small Use for Review: cell lung cancer Criteria Used in Selection of Off-labell AHFS Final Determination of Medical
Virtual Journal Club: Front-Line Therapy and Beyond Recent Perspectives on ALK-Positive Non-Small Cell Lung Cancer.
 Virtual Journal Club: Front-Line Therapy and Beyond Recent Perspectives on ALK-Positive Non-Small Cell Lung Cancer Reference Slides ALK Rearrangement in NSCLC ALK (anaplastic lymphoma kinase) is a receptor
Virtual Journal Club: Front-Line Therapy and Beyond Recent Perspectives on ALK-Positive Non-Small Cell Lung Cancer Reference Slides ALK Rearrangement in NSCLC ALK (anaplastic lymphoma kinase) is a receptor
Prognosis of recurrent non small cell lung cancer following complete resection
 1300 Prognosis of recurrent non small cell lung cancer following complete resection HIDEFUMI SASAKI, AYUMI SUZUKI, TSUTOMU TATEMATSU, MASAYUKI SHITARA, YU HIKOSAKA, KATSUHIRO OKUDA, SATORU MORIYAMA, MOTOKI
1300 Prognosis of recurrent non small cell lung cancer following complete resection HIDEFUMI SASAKI, AYUMI SUZUKI, TSUTOMU TATEMATSU, MASAYUKI SHITARA, YU HIKOSAKA, KATSUHIRO OKUDA, SATORU MORIYAMA, MOTOKI
Original Articles. Implications for Optimal Clinical Testing
 Original Articles Comparison of Reverse Transcription-Polymerase Chain Reaction, Immunohistochemistry, and Fluorescence In Situ Hybridization Methodologies for Detection of Echinoderm Microtubule-Associated
Original Articles Comparison of Reverse Transcription-Polymerase Chain Reaction, Immunohistochemistry, and Fluorescence In Situ Hybridization Methodologies for Detection of Echinoderm Microtubule-Associated
Molecular Analysis for Targeted Therapy for Non- Small-Cell Lung Cancer Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory
 2.04.45 Molecular Analysis for Targeted Therapy for Non- Small-Cell Lung Cancer Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory Effective Date November 26, 2014 Original Policy Date November
2.04.45 Molecular Analysis for Targeted Therapy for Non- Small-Cell Lung Cancer Section 2.0 Medicine Subsection 2.04 Pathology/Laboratory Effective Date November 26, 2014 Original Policy Date November
Personalized cancer therapy has attracted much attention
 ORIGINAL ARTICLE EML4-ALK Translocation Predicts Better Outcome in Lung Adenocarcinoma Patients with Wild-Type EGFR Shang-Gin Wu, MD,* Yao-Wen Kuo, MD,* Yih-Leong Chang, MD, Jin-Yuan Shih, MD, PhD, Ya-Hui
ORIGINAL ARTICLE EML4-ALK Translocation Predicts Better Outcome in Lung Adenocarcinoma Patients with Wild-Type EGFR Shang-Gin Wu, MD,* Yao-Wen Kuo, MD,* Yih-Leong Chang, MD, Jin-Yuan Shih, MD, PhD, Ya-Hui
The Human Epidermal growth factor Receptor (HER) family: structure and function
 Chapter 2 The Human Epidermal growth factor Receptor (HER) family: structure and function Epidermal growth factor receptor (EGFR) belongs to a family of four different receptors, including EGFR (ErbB-1;
Chapter 2 The Human Epidermal growth factor Receptor (HER) family: structure and function Epidermal growth factor receptor (EGFR) belongs to a family of four different receptors, including EGFR (ErbB-1;
The effi cacy of therapy targeted to a specifi c. Personalized targeted therapy in advanced non small cell lung cancer
 PATRICK C. MA, MD, MS Director, Aerodigestive Oncology Translational Research, Department of Translational Hematology and Oncology Research and Department of Solid Tumor Oncology, Taussig Cancer Institute,
PATRICK C. MA, MD, MS Director, Aerodigestive Oncology Translational Research, Department of Translational Hematology and Oncology Research and Department of Solid Tumor Oncology, Taussig Cancer Institute,
Biomarkers of Response to EGFR-TKIs EORTC-NCI-ASCO Meeting on Molecular Markers in Cancer November 17, 2007
 Biomarkers of Response to EGFR-TKIs EORTC-NCI-ASCO Meeting on Molecular Markers in Cancer November 17, 2007 Bruce E. Johnson, MD Dana-Farber Cancer Institute, Brigham and Women s Hospital, and Harvard
Biomarkers of Response to EGFR-TKIs EORTC-NCI-ASCO Meeting on Molecular Markers in Cancer November 17, 2007 Bruce E. Johnson, MD Dana-Farber Cancer Institute, Brigham and Women s Hospital, and Harvard
8/22/2016. Major risk factors for the development of lung cancer are: Outline
 Carcinomas of the Lung: Changes in Staging, Adenocarcinoma Classification and Genetics Grace Y. Lin, M.D., Ph.D. Outline Background Staging of Lung Cancer: Review of the 2010 7 th Edition of the AJCC Cancer
Carcinomas of the Lung: Changes in Staging, Adenocarcinoma Classification and Genetics Grace Y. Lin, M.D., Ph.D. Outline Background Staging of Lung Cancer: Review of the 2010 7 th Edition of the AJCC Cancer
Evolution of Pathology
 1 Traditional pathology Molecular pathology 2 Evolution of Pathology Gross Pathology Cellular Pathology Morphologic Pathology Molecular/Predictive Pathology Antonio Benivieni (1443-1502): First autopsy
1 Traditional pathology Molecular pathology 2 Evolution of Pathology Gross Pathology Cellular Pathology Morphologic Pathology Molecular/Predictive Pathology Antonio Benivieni (1443-1502): First autopsy
GENETIC TESTING FOR TARGETED THERAPY FOR NON-SMALL CELL LUNG CANCER (NSCLC)
 CANCER (NSCLC) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
CANCER (NSCLC) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
DM Seminar. ALK gene rearrangements & ALK targeted therapy in NSCLC Dr Sarat
 DM Seminar ALK gene rearrangements & ALK targeted therapy in NSCLC Dr Sarat Introduction Discovery of activating mutations in kinase domain of epidermal growth factor receptor (EGFR) opened a new era of
DM Seminar ALK gene rearrangements & ALK targeted therapy in NSCLC Dr Sarat Introduction Discovery of activating mutations in kinase domain of epidermal growth factor receptor (EGFR) opened a new era of
PRACTICE GUIDELINE SERIES
 ELLIS et al. PRACTICE GUIDELINE SERIES The role of the epidermal growth factor receptor tyrosine kinase inhibitors as therapy for advanced, metastatic, and recurrent nonsmall-cell lung cancer: a Canadian
ELLIS et al. PRACTICE GUIDELINE SERIES The role of the epidermal growth factor receptor tyrosine kinase inhibitors as therapy for advanced, metastatic, and recurrent nonsmall-cell lung cancer: a Canadian
REVIEWS. Personalized medicine in lung cancer: what we need to know. Tony S. K. Mok
 Personalized medicine in lung cancer: what we need to know Tony S. K. Mok Abstract Lung cancer is a complex and often fatal disease. The recent discovery of activating mutations in EGFR and fusion genes
Personalized medicine in lung cancer: what we need to know Tony S. K. Mok Abstract Lung cancer is a complex and often fatal disease. The recent discovery of activating mutations in EGFR and fusion genes
Personalised Healthcare (PHC) with Foundation Medicine (FMI) Fatma Elçin KINIKLI, FMI Turkey, Science Leader
 Personalised Healthcare (PHC) with Foundation Medicine (FMI) Fatma Elçin KINIKLI, FMI Turkey, Science Leader Agenda PHC Approach Provides Better Patient Outcome FMI offers Comprehensive Genomic Profiling,
Personalised Healthcare (PHC) with Foundation Medicine (FMI) Fatma Elçin KINIKLI, FMI Turkey, Science Leader Agenda PHC Approach Provides Better Patient Outcome FMI offers Comprehensive Genomic Profiling,
Introduction: Overview of Current Status of Lung Cancer Predictive Biomarkers
 Introduction: Overview of Current Status of Lung Cancer Predictive Biomarkers Program 7:15 7:40 Translocations as predictive biomarkers in lung cancer: Overview Mari Mino Kenudson, MD 7:40 8:05 Translocation
Introduction: Overview of Current Status of Lung Cancer Predictive Biomarkers Program 7:15 7:40 Translocations as predictive biomarkers in lung cancer: Overview Mari Mino Kenudson, MD 7:40 8:05 Translocation
EGFR-directed monoclonal antibodies in non-small cell lung cancer: how to predict efficacy?
 Review Article EGFR-directed monoclonal antibodies in non-small cell lung cancer: how to predict efficacy? Robert Pirker Department of Medicine I, Medical University of Vienna, 1090 Vienna, Austria Corresponding
Review Article EGFR-directed monoclonal antibodies in non-small cell lung cancer: how to predict efficacy? Robert Pirker Department of Medicine I, Medical University of Vienna, 1090 Vienna, Austria Corresponding
Molecular Targets in Lung Cancer
 Molecular Targets in Lung Cancer Robert Ramirez, DO, FACP Thoracic and Neuroendocrine Oncology November 18 th, 2016 Disclosures Consulting and speaker fees for Ipsen Pharmaceuticals, AstraZeneca and Merck
Molecular Targets in Lung Cancer Robert Ramirez, DO, FACP Thoracic and Neuroendocrine Oncology November 18 th, 2016 Disclosures Consulting and speaker fees for Ipsen Pharmaceuticals, AstraZeneca and Merck
MET skipping mutation, EGFR
 New NSCLC biomarkers in clinical research: detection of MET skipping mutation, EGFR T790M, and other important biomarkers Fernando López-Ríos Laboratorio de Dianas Terapéuticas Hospital Universitario HM
New NSCLC biomarkers in clinical research: detection of MET skipping mutation, EGFR T790M, and other important biomarkers Fernando López-Ríos Laboratorio de Dianas Terapéuticas Hospital Universitario HM
May 9, Dr. James Almas Medical Director MolDX 17 Technology Circle AG-315 Columbia, SC Dear Dr. Almas:
 May 9, 2018 Dr. James Almas Medical Director MolDX 17 Technology Circle AG-315 Columbia, SC 29202 Dear Dr. Almas: On behalf of LUNGevity Foundation, the nation s preeminent lung cancer nonprofit that funds
May 9, 2018 Dr. James Almas Medical Director MolDX 17 Technology Circle AG-315 Columbia, SC 29202 Dear Dr. Almas: On behalf of LUNGevity Foundation, the nation s preeminent lung cancer nonprofit that funds
Molecular Testing Updates. Karen Rasmussen, PhD, FACMG Clinical Molecular Genetics Spectrum Medical Group, Pathology Division Portland, Maine
 Molecular Testing Updates Karen Rasmussen, PhD, FACMG Clinical Molecular Genetics Spectrum Medical Group, Pathology Division Portland, Maine Keeping Up with Predictive Molecular Testing in Oncology: Technical
Molecular Testing Updates Karen Rasmussen, PhD, FACMG Clinical Molecular Genetics Spectrum Medical Group, Pathology Division Portland, Maine Keeping Up with Predictive Molecular Testing in Oncology: Technical
Personalized maintenance therapy in advanced non-small cell lung cancer
 China Lung Cancer Research Highlight Personalized maintenance therapy in advanced non-small cell lung cancer Kazuhiro Asami, Kyoichi Okishio, Tomoya Kawaguchi, Shinji Atagi Department of Clinical Oncology,
China Lung Cancer Research Highlight Personalized maintenance therapy in advanced non-small cell lung cancer Kazuhiro Asami, Kyoichi Okishio, Tomoya Kawaguchi, Shinji Atagi Department of Clinical Oncology,
Updated Molecular Testing Guideline for the Selection of Lung Cancer Patients for Treatment with Targeted Tyrosine Kinase Inhibitors
 Updated Molecular Testing Guideline for the Selection of Lung Cancer Patients for Treatment with Targeted Tyrosine Kinase Inhibitors Guideline from the College of American Pathologists, the International
Updated Molecular Testing Guideline for the Selection of Lung Cancer Patients for Treatment with Targeted Tyrosine Kinase Inhibitors Guideline from the College of American Pathologists, the International
Rearrangement of the anaplastic lymphoma kinase (ALK)
 Brief Report Clinical Implications of Variant ALK FISH Rearrangement Patterns Xin Gao, MD,* Lynette M. Sholl, MD,* Mizuki Nishino, MD,* Jennifer C. Heng, BS, Pasi A. Jänne, MD, PhD,* and Geoffrey R. Oxnard,
Brief Report Clinical Implications of Variant ALK FISH Rearrangement Patterns Xin Gao, MD,* Lynette M. Sholl, MD,* Mizuki Nishino, MD,* Jennifer C. Heng, BS, Pasi A. Jänne, MD, PhD,* and Geoffrey R. Oxnard,
Key Words. Lung cancer EGFR Mutation Genetic screening
 The Oncologist Lung Cancer Response to Treatment and Survival of Patients with Non-Small Cell Lung Cancer Undergoing Somatic EGFR Mutation Testing LECIA V. SEQUIST, VICTORIA A. JOSHI, PASI A. JÄNNE, ALONA
The Oncologist Lung Cancer Response to Treatment and Survival of Patients with Non-Small Cell Lung Cancer Undergoing Somatic EGFR Mutation Testing LECIA V. SEQUIST, VICTORIA A. JOSHI, PASI A. JÄNNE, ALONA
A case of different EGFR mutations in surgically resected synchronous triple lung cancer
 Case Report A case of different EGFR mutations in surgically resected synchronous triple lung cancer Naoki Haratake 1, Mitsuhiro Takenoyama 1, Makoto Edagawa 1, Shinichiro Shimamatsu 1, Ryo Toyozawa 1,
Case Report A case of different EGFR mutations in surgically resected synchronous triple lung cancer Naoki Haratake 1, Mitsuhiro Takenoyama 1, Makoto Edagawa 1, Shinichiro Shimamatsu 1, Ryo Toyozawa 1,
CAP Laboratory Improvement Programs. Worldwide Frequency of Commonly Detected EGFR Mutations
 CAP Laboratory Improvement Programs Worldwide Frequency of Commonly Detected EGFR Mutations Rondell P. Graham, MBBS; Amanda L. Treece, MD; Neal I. Lindeman, MD; Patricia Vasalos, BS; Mu Shan, BS; Lawrence
CAP Laboratory Improvement Programs Worldwide Frequency of Commonly Detected EGFR Mutations Rondell P. Graham, MBBS; Amanda L. Treece, MD; Neal I. Lindeman, MD; Patricia Vasalos, BS; Mu Shan, BS; Lawrence
Personalized Genetics
 Personalized Genetics Understanding Your Genetic Test Results Tracey Evans, MD September 29, 2017 Genetics 101 Punnett Square Genetic Pedigree 2 Genetics 101 Punnett Square Genetic Pedigree 3 It s not
Personalized Genetics Understanding Your Genetic Test Results Tracey Evans, MD September 29, 2017 Genetics 101 Punnett Square Genetic Pedigree 2 Genetics 101 Punnett Square Genetic Pedigree 3 It s not
and management of lung cancer Maureen F. Zakowski, M.D. Memorial Sloan-Kettering Cancer Center
 The new role of cytology in the diagnosis and management of lung cancer Maureen F. Zakowski, M.D. Memorial Sloan-Kettering Cancer Center Outline Role of cytology in the diagnosis of lung cancer Non-small
The new role of cytology in the diagnosis and management of lung cancer Maureen F. Zakowski, M.D. Memorial Sloan-Kettering Cancer Center Outline Role of cytology in the diagnosis of lung cancer Non-small
Lihong Ma 1 *, Zhengbo Song 2 *, Yong Song 1, Yiping Zhang 2. Original Article
 Original Article MET overexpression coexisting with epidermal growth factor receptor mutation influence clinical efficacy of EGFR-tyrosine kinase inhibitors in lung adenocarcinoma patients Lihong Ma 1
Original Article MET overexpression coexisting with epidermal growth factor receptor mutation influence clinical efficacy of EGFR-tyrosine kinase inhibitors in lung adenocarcinoma patients Lihong Ma 1
EGFR. Pathway and biomarkers. Alex Soltermann
 EGFR Pathway and biomarkers Alex Soltermann EGFR = HER1 signaling pathway EGFR Cheng Mod Pathol 2012 Chromosome 7p11.2, spans 200kb, 28 exons, 464 aa, 170 kda protein 2 Signal transduction pathways controlled
EGFR Pathway and biomarkers Alex Soltermann EGFR = HER1 signaling pathway EGFR Cheng Mod Pathol 2012 Chromosome 7p11.2, spans 200kb, 28 exons, 464 aa, 170 kda protein 2 Signal transduction pathways controlled
Research Article Mutated KRAS is an Independent Negative Prognostic Factor for Survival in NSCLC Stage III Disease Treated with High-Dose Radiotherapy
 Lung Cancer International Volume 2012, Article ID 587424, 6 pages doi:10.1155/2012/587424 Research Article Mutated KRAS is an Independent Negative Prognostic Factor for Survival in NSCLC Stage III Disease
Lung Cancer International Volume 2012, Article ID 587424, 6 pages doi:10.1155/2012/587424 Research Article Mutated KRAS is an Independent Negative Prognostic Factor for Survival in NSCLC Stage III Disease
Additional clinical features of this patient include:
 *Not an actual patient. Challenge your knowledge of biomarker testing in advanced NSCLC. Consider this case study of disease progression following chemotherapy, with insightful commentary from Dr Edward
*Not an actual patient. Challenge your knowledge of biomarker testing in advanced NSCLC. Consider this case study of disease progression following chemotherapy, with insightful commentary from Dr Edward
Do You Think Like the Experts? Refining the Management of Advanced NSCLC With ALK Rearrangement. Reference Slides Introduction
 Do You Think Like the Experts? Refining the Management of Advanced NSCLC With ALK Rearrangement Reference Slides Introduction EML4-ALK Fusion Oncogene Key Driver in 3% to 7% NSCLC Inversion or Translocation
Do You Think Like the Experts? Refining the Management of Advanced NSCLC With ALK Rearrangement Reference Slides Introduction EML4-ALK Fusion Oncogene Key Driver in 3% to 7% NSCLC Inversion or Translocation
Transform genomic data into real-life results
 CLINICAL SUMMARY Transform genomic data into real-life results Biomarker testing and targeted therapies can drive improved outcomes in clinical practice New FDA-Approved Broad Companion Diagnostic for
CLINICAL SUMMARY Transform genomic data into real-life results Biomarker testing and targeted therapies can drive improved outcomes in clinical practice New FDA-Approved Broad Companion Diagnostic for
Template for Reporting Results of Biomarker Testing of Specimens From Patients With Non-Small Cell Carcinoma of the Lung
 Template for Reporting Results of Biomarker Testing of Specimens From Patients With Non-Small Cell Carcinoma of the Lung Authors Philip T. Cagle, MD, FCAP Department of Pathology and Genomic Medicine,
Template for Reporting Results of Biomarker Testing of Specimens From Patients With Non-Small Cell Carcinoma of the Lung Authors Philip T. Cagle, MD, FCAP Department of Pathology and Genomic Medicine,
ALCHEMIST. Adjuvant Lung Cancer Enrichment Marker Identification And Sequencing Trials
 ALCHEMIST Adjuvant Lung Cancer Enrichment Marker Identification And Sequencing Trials What is ALCHEMIST? ALCHEMIST is 3 integrated trials testing targeted therapy in early stage lung cancer: l A151216:
ALCHEMIST Adjuvant Lung Cancer Enrichment Marker Identification And Sequencing Trials What is ALCHEMIST? ALCHEMIST is 3 integrated trials testing targeted therapy in early stage lung cancer: l A151216:
The estimation of tumor cell percentage for molecular testing by pathologists is not accurate
 168 & 2014 USCAP, Inc All rights reserved 0893-3952/14 $32.00 The estimation of tumor cell percentage for molecular testing by pathologists is not accurate Alexander JJ Smits 1,2, J Alain Kummer 1, Peter
168 & 2014 USCAP, Inc All rights reserved 0893-3952/14 $32.00 The estimation of tumor cell percentage for molecular testing by pathologists is not accurate Alexander JJ Smits 1,2, J Alain Kummer 1, Peter
Non-small cell lung cancer (NSCLC) has been the leading
 ORIGINAL ARTICLE EGFR and HER2 Gene Copy Number and Response to First-Line Chemotherapy in Patients with Advanced Non-small Cell Lung Cancer (NSCLC) Federico Cappuzzo, MD,* Claudio Ligorio, PhD, Luca Toschi,
ORIGINAL ARTICLE EGFR and HER2 Gene Copy Number and Response to First-Line Chemotherapy in Patients with Advanced Non-small Cell Lung Cancer (NSCLC) Federico Cappuzzo, MD,* Claudio Ligorio, PhD, Luca Toschi,
Molecular Diagnostics in Lung Cancer
 Molecular Diagnostics in Lung Cancer Mutations in lung carcinomas and their impact on diagnosis and treatment With special thanks to: Barbara Chaitin, MD Medical Director, Esoteric Services AmeriPath Orlando,
Molecular Diagnostics in Lung Cancer Mutations in lung carcinomas and their impact on diagnosis and treatment With special thanks to: Barbara Chaitin, MD Medical Director, Esoteric Services AmeriPath Orlando,
Protocol. Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC)
 Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) (20445) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization
Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) (20445) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization
When Policy Topic is covered Crizotinib may be considered medically necessary in patients 18 years or older when the following criteria are met:
 Xalkori (crizotinib) Policy Number: 5.01.539 Last Review: 6/2018 Origination: 7/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for crizotinib
Xalkori (crizotinib) Policy Number: 5.01.539 Last Review: 6/2018 Origination: 7/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for crizotinib
Personalized Medicine in Oncology and the Implication for Clinical Development
 THE POWER OFx Experts. Experienc e. Execution. Personalized Medicine in Oncology and the Implication for Clinical Development Jamal Gasmi MD, PhD, Medical Director, Medpace Introduction The notable success
THE POWER OFx Experts. Experienc e. Execution. Personalized Medicine in Oncology and the Implication for Clinical Development Jamal Gasmi MD, PhD, Medical Director, Medpace Introduction The notable success
Exploring Personalized Therapy for First Line Treatment of Advanced Non-Small Cell Lung Cancer (NSCLC)
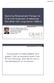 Exploring Personalized Therapy for First Line Treatment of Advanced Non-Small Cell Lung Cancer (NSCLC) Suresh S. Ramalingam, MD Director of Thoracic Oncology Associate Professor Emory University Atlanta,
Exploring Personalized Therapy for First Line Treatment of Advanced Non-Small Cell Lung Cancer (NSCLC) Suresh S. Ramalingam, MD Director of Thoracic Oncology Associate Professor Emory University Atlanta,
GTS. Earn CME credits at
 Reflex testing of resected stage I through III lung adenocarcinomas for EGFR and KRAS mutation: Report on initial experience and clinical utility at a single center Sandra P. D Angelo, MD, Bernard Park,
Reflex testing of resected stage I through III lung adenocarcinomas for EGFR and KRAS mutation: Report on initial experience and clinical utility at a single center Sandra P. D Angelo, MD, Bernard Park,
Management Strategies for Lung Cancer Sensitive or Resistant to EGRF Inhibitors
 Management Strategies for Lung Cancer Sensitive or Resistant to EGRF Inhibitors Conor E. Steuer, MD Assistant Professor The Winship Cancer Institute of Emory University July 27, 2017 1 Lung Cancer One
Management Strategies for Lung Cancer Sensitive or Resistant to EGRF Inhibitors Conor E. Steuer, MD Assistant Professor The Winship Cancer Institute of Emory University July 27, 2017 1 Lung Cancer One
THE IASLC/ERS/ATS ADENOCARCINOMA CLASSIFICATION RATIONALE AND STRENGTHS
 THE IASLC/ERS/ATS ADENOCARCINOMA CLASSIFICATION RATIONALE AND STRENGTHS PULMONARY PATHOLOGY SOCIETY USCAP, BALTIMORE, March 2, 2013 William D. Travis, M.D. Dept of Pathology, Memorial Sloan-Kettering Cancer
THE IASLC/ERS/ATS ADENOCARCINOMA CLASSIFICATION RATIONALE AND STRENGTHS PULMONARY PATHOLOGY SOCIETY USCAP, BALTIMORE, March 2, 2013 William D. Travis, M.D. Dept of Pathology, Memorial Sloan-Kettering Cancer
ONCOLOGY LETTERS 8: , 2014
 ONCOLOGY LETTERS 8: 813-818, 2014 Investigation of the epidermal growth factor receptor mutation rate in non small cell lung cancer patients and the analysis of associated risk factors using logistic regression
ONCOLOGY LETTERS 8: 813-818, 2014 Investigation of the epidermal growth factor receptor mutation rate in non small cell lung cancer patients and the analysis of associated risk factors using logistic regression
HOW TO GET THE MOST INFORMATION FROM A TUMOR BIOPSY
 HOW TO GET THE MOST INFORMATION FROM A TUMOR BIOPSY 7 TH Annual New York Lung Cancer Symposium Saturday, November 10, 2012 William D. Travis, M.D. Attending Thoracic Pathologist Memorial Sloan Kettering
HOW TO GET THE MOST INFORMATION FROM A TUMOR BIOPSY 7 TH Annual New York Lung Cancer Symposium Saturday, November 10, 2012 William D. Travis, M.D. Attending Thoracic Pathologist Memorial Sloan Kettering
CHAPTER 8A. High-dose, pulsatile erlotinib in two NSCLC patients with leptomeningeal metastases one with a remarkable thoracic response as well
 CHAPTER 8A High-dose, pulsatile erlotinib in two NSCLC patients with leptomeningeal metastases one with a remarkable thoracic response as well J.L. Kuiper, E.F. Smit Lung Cancer 2013 Apr;80(1):102-5 Chapter
CHAPTER 8A High-dose, pulsatile erlotinib in two NSCLC patients with leptomeningeal metastases one with a remarkable thoracic response as well J.L. Kuiper, E.F. Smit Lung Cancer 2013 Apr;80(1):102-5 Chapter
An Interactive Guide to ALK+ Lymphoma. Our understanding of lung cancer has changed From one disease to many subtypes LCD
 An Interactive Guide to ALK+ Anaplastic Lymphoma Kinase Non-Small Cell Lung (NSCLC) Our understanding of lung cancer has changed From one disease to many subtypes Click to get started Learning about Lung
An Interactive Guide to ALK+ Anaplastic Lymphoma Kinase Non-Small Cell Lung (NSCLC) Our understanding of lung cancer has changed From one disease to many subtypes Click to get started Learning about Lung
Lung cancer is the leading cause of cancer-related
 Original Articles Correlation of Mutation Status With Predominant Histologic Subtype of Adenocarcinoma According to the New Lung Adenocarcinoma Classification of the International Association for the Study
Original Articles Correlation of Mutation Status With Predominant Histologic Subtype of Adenocarcinoma According to the New Lung Adenocarcinoma Classification of the International Association for the Study
Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) Original Policy Date
 MP 2.04.34 Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last
MP 2.04.34 Epidermal Growth Factor Receptor (EGFR) Mutation Analysis for Patients with Non-Small Cell Lung Cancer (NSCLC) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last
VENTANA ALK (D5F3) Rabbit Monoclonal Primary Antibody. ALK IHC Biomarker Testing Aiding in patient diagnosis
 VENTANA (D5F3) Rabbit Monoclonal Primary Antibody IHC Biomarker Testing Aiding in patient diagnosis 2 IHC Biomarker Testing Lung cancer is the leading cause of death Lung cancer is the most prevalent form
VENTANA (D5F3) Rabbit Monoclonal Primary Antibody IHC Biomarker Testing Aiding in patient diagnosis 2 IHC Biomarker Testing Lung cancer is the leading cause of death Lung cancer is the most prevalent form
LUNG CANCER. pathology & molecular biology. Izidor Kern University Clinic Golnik, Slovenia
 LUNG CANCER pathology & molecular biology Izidor Kern University Clinic Golnik, Slovenia 1 Pathology and epidemiology Small biopsy & cytology SCLC 14% NSCC NOS 4% 70% 60% 50% 63% 62% 61% 62% 59% 54% 51%
LUNG CANCER pathology & molecular biology Izidor Kern University Clinic Golnik, Slovenia 1 Pathology and epidemiology Small biopsy & cytology SCLC 14% NSCC NOS 4% 70% 60% 50% 63% 62% 61% 62% 59% 54% 51%
Identifying ALK+ NSCLC patients for targeted treatment
 VENTANA (D5F3) CDx Assay Identifying + NSCLC patients for targeted treatment VENTANA (D5F3) CDx Assay Identify + NSCLC patients eligible for treatment with XORI, ZYKADIA or ALECENSA NSCLC tissue samples
VENTANA (D5F3) CDx Assay Identifying + NSCLC patients for targeted treatment VENTANA (D5F3) CDx Assay Identify + NSCLC patients eligible for treatment with XORI, ZYKADIA or ALECENSA NSCLC tissue samples
Advances in Pathology and molecular biology of lung cancer. Lukas Bubendorf Pathologie
 Advances in Pathology and molecular biology of lung cancer Lukas Bubendorf Pathologie Agenda The revolution of predictive markers Liquid biopsies PD-L1 Molecular subtypes (non-squamous NSCLC) Tsao AS et
Advances in Pathology and molecular biology of lung cancer Lukas Bubendorf Pathologie Agenda The revolution of predictive markers Liquid biopsies PD-L1 Molecular subtypes (non-squamous NSCLC) Tsao AS et
D Ross Camidge, MD, PhD
 i n t e r v i e w D Ross Camidge, MD, PhD Dr Camidge is Director of the Thoracic Oncology Clinical Program and Associate Director for Clinical Research at the University of Colorado Cancer Center in Aurora,
i n t e r v i e w D Ross Camidge, MD, PhD Dr Camidge is Director of the Thoracic Oncology Clinical Program and Associate Director for Clinical Research at the University of Colorado Cancer Center in Aurora,
Respiratory Department of Peking Union Medical College Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College, Peking, China
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Efficacy of bronchoscopic biopsy for the detection of epidermal growth factor receptor mutations and anaplastic lymphoma kinase gene rearrangement in lung
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Efficacy of bronchoscopic biopsy for the detection of epidermal growth factor receptor mutations and anaplastic lymphoma kinase gene rearrangement in lung
PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC. Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy
 PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy Prognostic versus predictive Prognostic: In presence of the biomarker patient outcome
PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy Prognostic versus predictive Prognostic: In presence of the biomarker patient outcome
Non-Small Cell Lung Carcinoma - Myers
 Role of Routine Histology and Special Testing in Managing Patients with Non- Small Cell Lung Carcinoma Jeffrey L. Myers, M.D. A. James French Professor Director, Anatomic Pathology & MLabs University of
Role of Routine Histology and Special Testing in Managing Patients with Non- Small Cell Lung Carcinoma Jeffrey L. Myers, M.D. A. James French Professor Director, Anatomic Pathology & MLabs University of
Biomedical Research 2017; 28 (14): ISSN X
 Biomedical Research 2017; 28 (14): ISSN 0970-938X www.biomedres.info Study of the relationship between EGFR mutation status and bone metastasis in advanced lung adenocarcinoma. Xiaoye Ai, Adalati Yasheng,
Biomedical Research 2017; 28 (14): ISSN 0970-938X www.biomedres.info Study of the relationship between EGFR mutation status and bone metastasis in advanced lung adenocarcinoma. Xiaoye Ai, Adalati Yasheng,
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW. Erlotinib for the third or fourth-line treatment of NSCLC January 2012
 Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
MEDICAL POLICY. SUBJECT: GENOTYPING - RAS MUTATION ANALYSIS IN METASTATIC COLORECTAL CANCER (KRAS/NRAS) POLICY NUMBER: CATEGORY: Laboratory
 MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
Approximately one third of all cancer-related deaths in
 ORIGINAL ARTICLE Comparison Between Epidermal Growth Factor Receptor (EGFR) Gene Expression in Primary Non-small Cell Lung Cancer (NSCLC) and in Fine-Needle Aspirates from Distant Metastatic Sites Cecilia
ORIGINAL ARTICLE Comparison Between Epidermal Growth Factor Receptor (EGFR) Gene Expression in Primary Non-small Cell Lung Cancer (NSCLC) and in Fine-Needle Aspirates from Distant Metastatic Sites Cecilia
