Cascade genetic testing for mismatch repair gene mutations
|
|
|
- Georgia Carroll
- 5 years ago
- Views:
Transcription
1 Familial Cancer (2008) 7: DOI /s x Cascade genetic testing for mismatch repair gene mutations R. J. Mitchell Æ R. K. Ferguson Æ A. Macdonald Æ M. G. Dunlop Æ H. Campbell Æ M. E. Porteous Published online: 4 April 2008 Ó Springer Science+Business Media B.V Abstract Mismatch repair gene mutation carriers have a high risk of developing colorectal cancer, and can benefit from appropriate surveillance. A combined population based ascertainment cascade genetic testing approach provides a systematic and potentially effective strategy for identifying such carriers. We have developed a Markov Chain computer model system which simulates various factors influencing cascade genetic testing; including demographics, uptake, genetic epidemiology and family size. This was used to evaluate cascade genetic testing for mismatch repair gene mutations in theory and practice. Simulations focussed on the population of Scotland by way of illustration, and were based on a 20-year programme in which index cases were ascertained from colorectal cancer cases aged \55 years at onset. Results indicated that without practical barriers to cascade genetic testing, 545 R. J. Mitchell (&) H. Campbell Public Health Sciences, University of Edinburgh, Teviot Place, Edinburgh EH89AG, UK R.J.Mitchell@ed.ac.uk R. J. Mitchell M. G. Dunlop H. Campbell M. E. Porteous Colon Cancer Genetics Group, School of Molecular & Clinical Medicine, University of Edinburgh, Edinburgh, UK R. K. Ferguson Department of Computer Sciences, Heriot-Watt University, Edinburgh, UK A. Macdonald Department of Actuarial Mathematics and Statistics, The Maxwell Institute for Mathematical Sciences, Heriot-Watt University, Edinburgh, UK M. E. Porteous SE Scotland Genetic Service Western General Hospital, Edinburgh, UK (95% CI = 522, 568) carriers could be identified; 42% of the population total. This comprised approximately 140 index cases, 302 asymptomatic relatives and 104 previously affected relatives. However, when realistic ascertainment and acceptance rates were used to inform simulations, only 257 (95% CI = 246, 268) carriers, about 20% of the carrier population, were identifiable. Of these approximately 112 were index cases, 108 were asymptomatic relatives, and 37 were previously affected relatives. This contrast emphasises the importance of ascertainment and acceptance rates. Likewise the low number of index cases shows that case identification is a limiting factor. In the absence of robust data from epidemiological studies, these findings can inform decisions about the use of cascade genetic testing for mismatch repair gene mutations. Keywords Colorectal cancer Genetic screening Mismatch repair Genetic services Genetic epidemiology Abbreviations MMR Mismatch repair CRC Colorectal cancer CGTM Cascade Genetic Testing Model GPM Genetic Population Model Introduction A small but significant sub-set of colorectal cancer (CRC) cases are caused by pathogenic mutations in mismatch repair (MMR) genes [1 6], which confer an approximate lifetime risk of 80% in males and 40% in females [7]. Colonoscopic screening of carriers can have significant health benefits in terms of both reduced incidence and lifeyears saved [8]. Consequently, there is a compelling
2 294 R. J. Mitchell et al. rationale for identifying MMR gene mutation carriers before they develop disease. This presents a major challenge, however. Population prevalence is uncertain but is certainly low: the carrier frequency in Scotland has been estimated to be approximately 1:3,139 (95% CI = 1:1,247, 1:7,626) [9]. By extrapolation, this implies that there are about 1,200 carriers aged in the Scottish population of around 5 million. Population genetic testing for MMR gene mutations is not currently viable, and further information regarding the underlying genetic epidemiology and the effectiveness of intervention strategies is needed before it can even be considered [10 14]. Alternative approaches are thus required. One current strategy for finding asymptomatic mutation carriers is to offer genetic testing to close relatives of a known carrier. The specific mutation present can thus be traced through an expanded pedigree in a process known as cascade genetic testing. In practice, index cases are often selected on the basis of family history. Tests can be offered to first-degree relatives only, or to a wider group of relatives; a concept which can be referred to as depth of testing. Cascade and population screening represent opposite ends of a continuum. A further option for identifying asymptomatic MMR gene mutation carriers, which is potentially both feasible and effective, could, therefore, be to combine features of both methodologies. A systematic, population-based approach to carrier ascertainment would thus be targeted to individuals at a relatively high risk of carrying a mutation, for example those with early onset CRC. Cascade genetic testing would then be employed, using these individuals as starting points. By only testing individuals at very high risk of harbouring a pathogenic mutation, such an approach would limit the number of non-carriers tested whilst maximizing the number of carriers identified. The hypothesis that a combined population based ascertainment cascade approach may be both effective and efficient is supported by theoretical work [15]. Cascade genetic testing has also been systematically applied to other complex diseases with adult onset, notably familial hypercholesterolaemia [16, 17], for which it has been shown to be cost effective [18, 19]. However, the outcomes of cascade genetic testing are highly context specific, and this strategy remains to be thoroughly evaluated at the population level for MMR gene mutations. The overarching aim of this paper is to address this gap in current knowledge. Methods Overview The complex process of cascade genetic testing was evaluated using a computer model system, implemented using Java and the database software MySQL. Design was function driven, but in applying probabilities to events in a stochastic manner the model system is essentially an example of a Markov Chain. The model system has the flexibility to be applied to any population. Results presented here used the Scottish population for illustrative purposes. The model system comprises two integrated models, which operate sequentially: 1. Genetic Population Model (GPM) simulates demographics, family structure and genetic epidemiology in a dynamic population. 2. Cascade Genetic Testing Model (CGTM) superimposes cascade genetic testing on populations simulated by the GPM. Genetic Population Model (GPM) The GPM constitutes a flexible and powerful research tool for studying the inheritance of pathogenic mutations at the population level. A dynamic population is simulated over time, with demographics and mutation prevalence at the starting point defined by the model user. A set of variables is assigned for each individual: these include a unique identifier, year of birth, sex, mutation status, disease status and date of death. In the course of the simulation these variables are updated annually, using a series of algorithms which apply a probability for the event in question. In this manner, the occurrence of events such as births, death and disease onset over time is simulated. Obtaining input probability values from real data enables actual demographic and epidemiological trends to be simulated. Importantly, the probability of disease is determined by mutation status as well as age, sex and cohort-specific population incidence. Hence information about the prevalence and penetrance of MMR gene mutations was used to simulate their role in CRC. Another crucial feature is that partnerships are established within the population, and birth algorithms are applied to females with a current partner, with age-specific probability of birth adjusted to account for existing parity. For each birth event, mother and father identity is known and mutation status can be assigned according to Mendelian inheritance. Hence realistic family relationships and inheritance patterns evolve in the simulated population. To provide the necessary framework for simulating cascade genetic testing beginning in the present day, the GPM was used to produce a dynamic simulation of the Scottish population from the time of the 1901 census to the year In view of the uncertainty surrounding the prevalence and penetrance of MMR gene mutations (see Discussion ), these input values were considered as assumptions
3 Mismatch repair gene mutations 295 rather than robust estimates. A single estimate of 0.016%, extrapolated from the study by Dunlop et al. [9], was used to represent the collective allele frequency for pathogenic mutations in hmlh1 and hmsh2. Penetrance was estimated to be 80% in males and 40% in females [3, 7]. A summary of key inputs to the GPM is shown in Appendix 1. Cascade Genetic Testing Model (CGTM) The CGTM simulates the progress of a cascade genetic testing programme over time, using weeks as time units. Initially, the population database is interrogated to identify CRC cases occurring in the current week. Ascertainment and acceptance of genetic testing is determined using probability algorithms, with test results reflecting true mutation status. Another algorithm is run to determine if mutation carriers will allow their relatives to be contacted. If the outcome is affirmative, the CGTM then retrieves relatives of the newly identified mutation carrier from the population database, beginning a new cycle of ascertainment and testing. All simulations were based on applying cascade genetic testing to a depth of all first- and second-degree relatives. To reflect the long-term nature of the strategy, the CTGM simulated cascade genetic testing over a 20-year period. Restricting genetic testing to early-onset cases is a commonly used approach to enrich for mutation carriers. For the purposes of the study, it was assumed that all CRC cases presenting under the age of 55 would be offered MMR gene mutation analysis as part of routine clinical practice. Realistic delays were also built into the model system. Uptake of cascade genetic testing, determined by both ascertainment and acceptance rates, is likely to have a significant impact on the above outcomes. To study this, two sets of input parameters were defined: (i) Optimum: assumes 100% ascertainment and acceptance and thus provides an indication of the theoretical utility of cascade genetic testing. (ii) Realistic: current best estimates of ascertainment and acceptance rates, based on published data [1, 20, 21] and the practical experience of our research group. These represent conservative assumptions about what may be achievable in practice. Table 1 provides a summary of parameters used to inform the CGTM. Strategy for evaluating cascade genetic testing using integrated model system The two models were considered as one integrated system. Each set of results was generated by running the GPM first, and then using the CGTM to model cascade genetic testing in the simulated population database. Variation is therefore the net result of variability in the entire model system. The number of repeat simulations was minimised to generate robust estimates whilst reducing computing time. Results presented here are based on mean estimates from multiple simulations (n = 25) run with identical parameters. Standard deviation and confidence intervals were calculated by standard methods. Table 1 Key parameters for Cascade Genetic Testing Model a Eligible individuals aged less than 18 years were not processed until they reached this minimum age b Practical experience suggests that ascertainment of relatives can be a prolonged process, and accordingly the realistic set of simulations modelled presentation of relatives over a period of up to 2 years Parameter type Parameter estimate applied Depth of cascade genetic testing First- and second-degree relatives Length of programme 20 years Age limit for index cases 55 years Age limit for relatives 75 years Minimum age for genetic testing 18 years a Sensitivity of genetic test 100% Specificity of genetic test 100% Realistic ascertainment rate for colorectal cancer cases 90% Realistic acceptance rate for genetic testing by colorectal cancer cases 85% Realistic proportion of index cases permitting/facilitating ascertainment 98% of relatives Realistic acceptance rate for genetic testing by relatives 50% Time required for genetic test in colorectal cancer case 52 weeks Time required for specific genetic test in relative of carrier 1 week Optimal time for ascertainment of relatives 4 12 weeks Realistic time for ascertainment of relatives 1 2 years b
4 296 R. J. Mitchell et al. Results Cascade genetic testing identifies mutations in affected individuals, or in relatives of these index cases. Inevitably, some relatives will have developed disease previously, whereas others will be asymptomatic. This latter group constitutes the key outcome against which the effectiveness of cascade genetic testing can be judged. Figures 1 and 2 illustrate the cumulative total number of carriers identified in each category, in simulations using, respectively, optimal and realistic assumptions about ascertainment and acceptance. Estimates are based on the mean value from multiple simulations, with 95% confidence intervals. Under optimum ascertainment and acceptance rates, simulations suggested that an average of 140 (95% CI = 135, 145) index cases could be identified over 20 years, at a rate of approximately seven per year. The corresponding average number of asymptomatic mutation carriers identifiable through cascade genetic testing was 302 (95% CI = 287, 317). A further 104 (95% CI = 98, 110) relatives who had previously developed CRC were predicted to be identifiable. Fig. 1 Average number of mutation carriers identified in simulations assuming optimal ascertainment and acceptance rates Fig. 2 Average number of mutation carriers identified in simulations assuming realistic ascertainment and acceptance rates
5 Mismatch repair gene mutations 297 In simulated populations generated by the GPM, the average number of mutation carriers aged years was 1,290. This value is consistent with the published estimate used to inform the model system [9], illustrating the validity of the model in this respect. The above results suggest that under optimal (i.e. 100%) ascertainment and acceptance rates, an average of 545 (95% CI = 522, 568) mutation carriers would be identified through cascade genetic testing over a 20-year period. Therefore, this implies that roughly 42% of the total number of carriers in this age group aged in Scotland could theoretically be identified through a systematic cascade genetic testing programme spanning 20 years. Results of simulations in which the CGTM was informed by more realistic estimates of ascertainment and acceptance demonstrate the major impact that these factors are likely to have on the outcomes of cascade genetic testing. These results suggest that approximately 112 (95% CI = 108, 116) index cases, 108 (95% CI = 102, 115) asymptomatic relatives, and 37 (95% CI = 34, 39) previously affected relatives would be identified when realistic ascertainment and acceptance rates applied. The total number of mutation carriers that would be identified by cascade genetic testing according to these simulated results was 257 (95% CI = 246, 268), or approximately 20% of all carriers in the population. Notably, the ratio of asymptomatic carriers identified to index cases ascertained is much lower when realistic ascertainment and acceptance rates for relatives are applied. The ratio of asymptomatic carriers identified to genetic tests performed is a key indicator of the efficiency of cascade genetic testing. The relatively complex process of searching for an unspecified MMR gene mutation in a CRC case is likely to be the most resource-intensive aspect of a cascade genetic testing programme. Simulations using the CGTM suggest that under optimal ascertainment and acceptance parameters, approximately 8,400 potential index cases need to undergo genetic testing in order to identify 302 asymptomatic relatives, a ratio of about 28:1. In the more realistic simulations, an average of 6,500 potential index cases underwent genetic testing and around 112 asymptomatic relatives were identified, an overall ratio of about 58:1 that suggests that limitations in ascertainment and acceptance rates make the process far less efficient. Extending the time period of cascade genetic testing beyond 20 years in these simulations showed that this strategy remains useful over an even longer period, although return diminishes slightly as the pool of untested mutation carriers dwindles. Simulations under optimal assumptions suggested that about 72% of carriers could be identified after 40 years. This observation implies cascade genetic testing could in theory identify the majority of carriers in the population, but is unlikely to do so within a reasonable timeframe. Discussion We have developed a robust computer model system that facilitates the study of cascade genetic testing, focussing on its theoretical and practical utility in a specific clinical context. Precise outcomes of cascade genetic testing will be population-specific due to variations in demographics and genetic epidemiology. Penetrance may vary as the specific mutations present and the proportion of hmlh1 compared to hmsh2 mutations will differ between populations. In addition, the behaviour of individuals in a cascade genetic testing programme may be influenced by social context and external factors such as the availability of free healthcare. Nonetheless, Scotland serves as a typical example of a developed country with a high incidence of CRC and low prevalence of MMR gene mutations. Hence, the methods, results and conclusions of this work have much wider relevance. Model outcomes are critically dependent on input data, so the quality of these data merits further consideration. Robust national statistics were used to simulate the demographics of the Scottish population and to simulate CRC epidemiology, although early historical data and projected estimates had less precision. In contrast, data on family size and structure was limited and relied heavily on one publication [22]. Input data relating to the genetic epidemiology of MMR gene mutations were regarded as assumptions. Published penetrance estimates vary widely [2, 3, 6], and ascertainment bias in previous studies may have led to overestimation [21]. This study considered all mutations in hmlh1 or hmsh2, although these are highly heterogenous and mutations in other MMR genes may also be clinically relevant. More detailed information could not be incorporated into the simulations because of the lack of robust input data. Due to the stochastic nature of the model and the limitations outlined above, both random variation and some minor systematic differences were evident between simulated data and the actual parameters of the Scottish population. Nonetheless, the system reliably produced simulated populations that were representative of the actual Scottish population in terms of demographics, genetic epidemiology, and family size and structure. The depth to which cascade genetic testing is applied is a crucial consideration. It is desirable to test only close relatives with a very high probability of having a mutation, but this can be rather restrictive, especially in small families. Conversely, extending cascade genetic testing to
6 298 R. J. Mitchell et al. distant relatives is more resource-intensive and may lead to reduced uptake. In reality, factors such as family history and test results in other relatives may also guide the cascade process. In this, as in any, cascade genetic testing programme, the identification of index cases is extremely important and potentially a major limiting factor [23]. Applying genetic tests to CRC cases is the simplest approach. To improve efficiency, genetic testing can be targeted to a sub-group of cases with early onset. Family history provides an alternative means of targeting testing, although use of the stringent Amsterdam criteria [24] would miss a large proportion of carriers, and high risk families may not be representative [21]. Incorporating information on tumour pathology into the genetic testing strategy could also be an effective means of targeting testing [25]. Specific approaches, such as the two-stage model described by Barnetson et al. [26] which incorporated clinical variables in stage 1 and microsatellite instability and immunohistochemistry in stage 2, may prove useful. However, data on the use of pathology features in this context is limited, and the required pathology data are not always routinely collected. Because of this, and the inherent limitations and complexity of using family history criteria, the age alone model was chosen for the current study. Although their inclusion would theoretically permit identification of additional index cases, other cancers associated with MMR gene mutations were not simulated due to lack of quality evidence to support estimates of penetrance and test uptake. Under optimum conditions, simulations suggested that approximately 140 index cases could be identified over 20 years. In reality though, ascertainment and acceptance will be sub-optimal [20, 27 29]. Results based on more realistic estimates, which suggest that 112 index cases could be identified, are thus more appropriate. Simulations suggested that cascade genetic testing could theoretically identify about 40% of MMR gene mutation carriers in Scotland, most of which were predicted to be identified at an asymptomatic stage. This is consistent with estimates of theoretical effectiveness presented by Krawczak et al. [15], although results are not directly comparable since this previous study had no chronological component, and did not relate to a specific disease or population. Published data concerning the achievable uptake for a cascade genetic testing programme is limited, and relates to large hereditary non-polyposis colorectal cancer (HNPCC) families. Figures quoted are highly variable, ranging from 33.6 [29] to 75% [27]. Low education and depression act as barriers to uptake [20], and other factors, including age, sex, and relationship to mutation carrier may also be involved [20, 27, 29]. The manner in which relatives are approached is another vital factor. Current best practice in clinical genetics, designed to comply with ethical guidelines, dictates that communication with relatives must be initiated through the index case or another family member. The onus is then on the relatives to contact a genetics clinic. For the current study, this difficulty was addressed by using an estimate of 50% to reflect the overall proportion of eligible relatives who will undergo a genetic test in realistic simulations. Based on the practical experience of our research group, we consider this to be a conservative estimate. Using realistic ascertainment and acceptance rates as input data for the CGTM produced results that are strikingly different to theoretical outcomes. These simulations suggest that a 20-year cascade genetic testing programme would identify a much smaller number of mutation carriers; approximately 260, or 20% of the population total. Less than half of these carriers are likely to be identified while asymptomatic. This may be regarded as a relatively poor return from a long-term, resource-intensive testing programme, although identifying a group of mutation carriers does offer the potential to trace mutations in future generations. The identification of asymptomatic MMR gene mutation carriers is merely the first step towards disease prevention in this population sub-group. Carriers are recommended to undergo intensive surveillance, ideally comprising biennial colonoscopy [30]. Such screening has been shown to reduce CRC incidence and mortality in MMR gene mutation carriers [8]. In practice though, incomplete compliance with surveillance is likely to constrain the potential health benefits [8, 29]. Our findings support the hypothesis that cascade genetic testing has the theoretical potential to be both effective and efficient as a means of identifying MMR gene mutation carriers from within a population. However, we have illustrated that incomplete ascertainment and acceptance has a significant impact. The practical barriers to pursuing cascade genetic testing effectively must therefore be given due consideration when deciding on the appropriateness of implementing this strategy. In summary, we provide data on the potential effectiveness and efficiency of cascade genetic testing both in theory and in practice. These data and the associated observations and conclusions that have been prompted can be used to inform decisions about the use of cascade genetic testing as part of a strategy to address the health needs of MMR gene mutation carriers. Acknowledgements This work was funded by the Chief Scientist Office of Scotland, grant no. CZH/4/145. The University of Edinburgh acted as sponsor, with vital collaboration from Heriot-Watt University. In addition to the work carried out by the authors, we acknowledge the expert input from Kenneth MacLeod regarding computer programming, and the support provided by Rosa Bisset.
7 Mismatch repair gene mutations 299 Appendix 1 Key input data to Genetic Population Model Input data Point estimate (if applicable) Source/ reference Comments on data accuracy/quality Generalisability Population size 5,094,800 (2005) GROS Robust estimate based on census data Scotland is a relatively small country but data may be extrapolated to populations with similar demographics Demographic structure GROS Robust estimate Scotland has a demographic structure that is typical of an aging population in a developed country Deaths (historical data) GROS Robust national data Scotland is broadly representative of developed countries with respect to mortality rate Deaths (projections) GAD Projections only The projected continuation of decreasing mortality rates for Scotland is typical of developed countries Births GROS Robust national data Fertility in Scotland, as with many developed countries, has decreased during the latter part of the 20th century Births (projections) GAD Projections only The projected continuation of decreasing fertility rates for Scotland is typical of developed countries Disease incidence ISD Disease incidence has been recorded with a high degree of accuracy since the 1960s; earlier data is of poor quality Disease incidence (projections) ISD Projections, based on current trends and demographic projections Penetrance of MMR gene mutations Prevalence of MMR gene mutations To age 70: males: 80% females: 40% 1:3,139 (95% CI 1:1,247, 1:7,626) Scientific literature Scientific literature Limited sources of data, various methods, wide confidence intervals One source of data only, wide confidence intervals Scotland has a relatively high incidence of colorectal cancer, but incidence is comparable with other countries in which the disease is a public health issue The increasing incidence projected for Scotland is reflected in many other populations There is currently no evidence of population variations since differences in published estimates are likely to be due to methods used and lack of statistical power. However, penetrance may vary according to the precise mutation involved and numerous other factors, and may therefore vary by population Prevalence data are scarce, and the single published estimate relates to Scotland. Prevalence is likely to vary by country, particularly when common founder mutations are present in the population (e.g. Finland), but there is no evidence to suggest that Scotland is not representative in this respect
8 300 R. J. Mitchell et al. Appendix 1 continued Input data Point estimate (if applicable) Source/reference Comments on data accuracy/quality Generalisability Disease survival ISD Robust national data In terms of survival, Scotland is representative of countries with modern health care systems Family structure ONS Data on frequency distribution of children as well as completed family size is limited to one reliable source Family structure may vary across populations according to cultural, social and demographic trends. However, Scotland has a stable population which is useful for comparisons, and the observed trend of decreasing family size leading to stabilizing or decreasing population is common GROS = General Register Office Scotland, GAD = Government Actuary s Department, ISD = Information Services Division Scotland, ONS = Office of National Statistics, CI = Confidence interval References 1. Aaltonen LA, Salovaara R, Kristo P et al (1998) Incidence of hereditary nonpolyposis colorectal cancer and the feasibility of molecular screening for the disease. N Engl J Med 338: Aarnio M, Sankila R, Pukkala E et al (1999) Cancer risk in mutation carriers of DNA-mismatch-repair genes. Int J Cancer 81: Dunlop MG, Farrington SM, Carothers AD et al (1997) Cancer risk associated with germline DNA mismatch repair gene mutations. Hum Mol Genet 6: Liu B, Farrington SM, Petersen GM et al (1995) Genetic instability occurs in the majority of young patients with colorectal cancer. Nat Med 1: Lynch HT, de la Chapelle A (1999) Genetic susceptibility to nonpolyposis colorectal cancer. J Med Genet 36: Vasen HF, Wijnen JT, Menko FH et al (1996) Cancer risk in families with hereditary nonpolyposis colorectal cancer diagnosed by mutation analysis. Gastroenterology 110: Mitchell RJ, Farrington SM, Dunlop MG et al (2002) Mismatch repair genes hmlh1 and hmsh2 and colorectal cancer: a HuGE review. Am J Epidemiol 156: Jarvinen HJ, Aarnio M, Mustonen H et al (2000) Controlled 15- year trial on screening for colorectal cancer in families with hereditary nonpolyposis colorectal cancer. Gastroenterology 118: Dunlop MG, Farrington SM, Nicholl I et al (2000) Population carrier frequency of hmsh2 and hmlh1 mutations. Br J Cancer 83: Brown ML, Kessler LG (1996) Use of gene tests to detect hereditary predisposition to cancer: what do we know about cost effectiveness? Int J Cancer 69: Coughlin SS, Miller DS (1999) Public health perspectives on testing for colorectal cancer susceptibility genes. Am J Prev Med 16: Ponder BA (1999) Costs, benefits and limitations of genetic testing for cancer risk. Br J Cancer 80 suppl 1: Terdiman JP, Conrad PG, Sleisenger MH (1999) Genetic testing in hereditary colorectal cancer: indications and procedures. Am J Gastroenterol 94: Welch HG, Burke W (1998) Uncertainties in genetic testing for chronic disease. JAMA 280: Krawczak M, Cooper DN, Schmidtke J (2001) Estimating the efficacy and efficiency of cascade genetic screening. Am J Hum Genet 69: Umans-Eckenhausen MA, Defesche JC, Sijbrands EJ et al (2001) Review of first 5 years of screening for familial hypercholesterolaemia in the Netherlands. Lancet 357: Bhatnagar D, Morgan J, Siddiq S et al (2000) Outcome of case finding among relatives of patients with known heterozygous familial hypercholesterolaemia. BMJ 321: Marks D, Wonderling D, Thorogood M et al (2002) Cost effectiveness analysis of different approaches of screening for familial hypercholesterolaemia. BMJ 324: Hadfield GS, Humphries SE (2007) Familial hypercholesterolaemia: cascade testing is tried and tested and cost effective. BMJ 335: Lerman C, Hughes C, Trock BJ et al (1999) Genetic testing in families with hereditary nonpolyposis colon cancer. JAMA 281: Quehenberger F, Vasen HF, van Houwelingen HC (2005) Risk of colorectal and endometrial cancer for carriers of mutations of the hmlh1 and hmsh2 gene: correction for ascertainment. J Med Genet 42: Chamberlain J, Smallwood S (2004) Estimates of true birth order for Scotland, Popul Trends 117: Morris JK (2004) Is cascade testing a sensible method of population screening? J Med Screen 11: Vasen HF, Mecklin JP, Khan PM et al (1991) The International Collaborative Group on hereditary non-polyposis colorectal cancer [ICG-HNPCC]. Dis Colon Rectum 34: Jenkins MA, Hayashi S, O Shea A-M et al (2007) Pathology features in Bethesda guidelines predict microsatellite instability: a population-based study. Gastroenterology 133: Barnetson RA, Tenesa A, Farrington SM et al (2006) Identification and survival of carriers of mutations in DNA mismatch-repair genes in colon cancer. N Engl J Med 354: Aktan-Collan K, Mecklin JP, Jarvinen H et al (2000) Predictive genetic testing for hereditary non-polyposis colorectal cancer: uptake and long-term satisfaction. Int J Cancer 89:44 50
9 Mismatch repair gene mutations Aktan-Collan K, Mecklin JP, de la Chapelle A, Peltomaki P, Uutela A, Kaariainen H (2000) Evaluation of a counselling protocol for predictive genetic testing for hereditary non-polyposis colorectal cancer. J Med Genet 37: Ponz de Leon M, Benatti P, Di Gregorio C et al (2004) Genetic testing among high-risk individuals in families with hereditary nonpolyposis colorectal cancer. Br J Cancer 90: Dunlop MG (2002) Guidance on gastrointestinal surveillance for hereditary non-polyposis colorectal cancer, familial adenomatous polypolis, juvenile polyposis, and Peutz-Jeghers syndrome. Gut 51 suppl 5:V21 V27
T he lifetime risk of developing colorectal cancer is 5%, with. Adenoma prevalence and cancer risk in familial non-polyposis colorectal cancer CANCER
 228 CANCER Adenoma prevalence and cancer risk in familial non-polyposis colorectal cancer G Lindgren, A Liljegren, E Jaramillo, C Rubio, A Lindblom... See end of article for authors affiliations... Correspondence
228 CANCER Adenoma prevalence and cancer risk in familial non-polyposis colorectal cancer G Lindgren, A Liljegren, E Jaramillo, C Rubio, A Lindblom... See end of article for authors affiliations... Correspondence
B Base excision repair, in MUTYH-associated polyposis and colorectal cancer, BRAF testing, for hereditary colorectal cancer, 696
 Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Risk of colorectal and endometrial cancer for carriers of mutations of the hmlh1 and hmsh2 gene: correction for ascertainment
 491 SHORT REPORT Risk of colorectal and endometrial cancer for carriers of mutations of the hmlh1 and hmsh2 gene: correction for ascertainment F Quehenberger, H F A Vasen, H C van Houwelingen... Background:
491 SHORT REPORT Risk of colorectal and endometrial cancer for carriers of mutations of the hmlh1 and hmsh2 gene: correction for ascertainment F Quehenberger, H F A Vasen, H C van Houwelingen... Background:
Hereditary nonpolyposis colorectal cancer (HNPCC)
 GASTROENTEROLOGY 2000;118:829 834 Controlled 15-Year Trial on Screening for Colorectal Cancer in Families With Hereditary Nonpolyposis Colorectal Cancer HEIKKI J. JÄRVINEN,* MARKKU AARNIO,* HARRI MUSTONEN,*
GASTROENTEROLOGY 2000;118:829 834 Controlled 15-Year Trial on Screening for Colorectal Cancer in Families With Hereditary Nonpolyposis Colorectal Cancer HEIKKI J. JÄRVINEN,* MARKKU AARNIO,* HARRI MUSTONEN,*
DIAGNOSTICS ASSESSMENT PROGRAMME Diagnostics consultation document
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE DIAGNOSTICS ASSESSMENT PROGRAMME Diagnostics consultation document Molecular testing strategies for Lynch syndrome in The National Institute for Health
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE DIAGNOSTICS ASSESSMENT PROGRAMME Diagnostics consultation document Molecular testing strategies for Lynch syndrome in The National Institute for Health
Diagnostics guidance Published: 22 February 2017 nice.org.uk/guidance/dg27
 Molecular testing strategies for Lynch syndrome in people with colorectal cancer Diagnostics guidance Published: 22 February 2017 nice.org.uk/guidance/dg27 NICE 2018. All rights reserved. Subject to Notice
Molecular testing strategies for Lynch syndrome in people with colorectal cancer Diagnostics guidance Published: 22 February 2017 nice.org.uk/guidance/dg27 NICE 2018. All rights reserved. Subject to Notice
Resource impact report: Molecular testing strategies for Lynch syndrome in people with colorectal cancer (DG27)
 Putting NICE guidance into practice Resource impact report: Molecular testing strategies for Lynch syndrome in people with colorectal cancer (DG27) Published: February 2017 Summary Molecular testing strategies
Putting NICE guidance into practice Resource impact report: Molecular testing strategies for Lynch syndrome in people with colorectal cancer (DG27) Published: February 2017 Summary Molecular testing strategies
Fourfold increased detection of Lynch syndrome by raising age limit for. tumour genetic testing from 50 to 70 years is cost-effective
 Annals of Oncology Advance Access published July 31, 2014 1 Fourfold increased detection of Lynch syndrome by raising age limit for tumour genetic testing from 50 to 70 years is cost-effective A.S. Sie
Annals of Oncology Advance Access published July 31, 2014 1 Fourfold increased detection of Lynch syndrome by raising age limit for tumour genetic testing from 50 to 70 years is cost-effective A.S. Sie
Review Article Clinicopathological Features and Management of Cancers in Lynch Syndrome
 Pathology Research International Volume 2012, Article ID 350309, 6 pages doi:10.1155/2012/350309 Review Article Clinicopathological Features and Management of Cancers in Lynch Syndrome Markku Aarnio Department
Pathology Research International Volume 2012, Article ID 350309, 6 pages doi:10.1155/2012/350309 Review Article Clinicopathological Features and Management of Cancers in Lynch Syndrome Markku Aarnio Department
ORIGINAL INVESTIGATION. Colon Cancer Screening Practices Following Genetic Testing for Hereditary Nonpolyposis Colon Cancer (HNPCC) Mutations
 ORIGINAL INVESTIGATION Colon Cancer Screening Practices Following Genetic Testing for Hereditary Nonpolyposis Colon Cancer (HNPCC) Mutations Chanita Hughes Halbert, PhD; Henry Lynch, MD; Jane Lynch, BSN;
ORIGINAL INVESTIGATION Colon Cancer Screening Practices Following Genetic Testing for Hereditary Nonpolyposis Colon Cancer (HNPCC) Mutations Chanita Hughes Halbert, PhD; Henry Lynch, MD; Jane Lynch, BSN;
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS. Family Health Clinical Genetics. Clinical Genetics department
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
Family history and molecular features of children, adolescents, and young adults with colorectal carcinoma
 1146 COLON CANCER Family history and molecular features of children, adolescents, and young adults with colorectal carcinoma C Durno, M Aronson, B Bapat, Z Cohen, S Gallinger... See end of article for
1146 COLON CANCER Family history and molecular features of children, adolescents, and young adults with colorectal carcinoma C Durno, M Aronson, B Bapat, Z Cohen, S Gallinger... See end of article for
Colorectal Cancer - Working in Partnership. David Baty Genetics, Ninewells Hospital
 Colorectal Cancer - Working in Partnership David Baty Genetics, Ninewells Hospital Genetics and Pathology National initiatives Colorectal cancer Inherited CRC Sporadic CRC The Liquid Biopsy The future?
Colorectal Cancer - Working in Partnership David Baty Genetics, Ninewells Hospital Genetics and Pathology National initiatives Colorectal cancer Inherited CRC Sporadic CRC The Liquid Biopsy The future?
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial colorectal adenocarcinoma and hereditary nonpolyposis colorectal cancer: a nationwide epidemiological study from Sweden
 doi: 10.1054/ bjoc.2001.1718, available online at http://www.idealibrary.com on http://www.bjcancer.com Familial colorectal adenocarcinoma and hereditary nonpolyposis colorectal cancer: a nationwide epidemiological
doi: 10.1054/ bjoc.2001.1718, available online at http://www.idealibrary.com on http://www.bjcancer.com Familial colorectal adenocarcinoma and hereditary nonpolyposis colorectal cancer: a nationwide epidemiological
Risk of Colorectal Cancer (CRC) Hereditary Syndromes in GI Cancer GENETIC MALPRACTICE
 Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Content. Diagnostic approach and clinical management of Lynch Syndrome: guidelines. Terminology. Identification of Lynch Syndrome
 of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
Hereditary nonpolyposis colorectal cancer and familial colorectal cancer. in Central part of Iran, Isfahan
 Received: 30.1.2011 Accepted: 6.1.2012 Original Article Hereditary nonpolyposis colorectal cancer and familial colorectal cancer in Central part of Iran, Isfahan Amin Nemati 1, Zahra Kazemi Rahmatabadi
Received: 30.1.2011 Accepted: 6.1.2012 Original Article Hereditary nonpolyposis colorectal cancer and familial colorectal cancer in Central part of Iran, Isfahan Amin Nemati 1, Zahra Kazemi Rahmatabadi
COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University
 COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University 1. I am a surgeon; of course I have nothing to disclose.
COLON CANCER GENETICS (FOR SURGEONS) Mark W. Arnold MD Chief, Division of Colon and Rectal Surgery Professor of Surgery The Ohio State University 1. I am a surgeon; of course I have nothing to disclose.
MRC-Holland MLPA. Description version 29;
 SALSA MLPA KIT P003-B1 MLH1/MSH2 Lot 1209, 0109. As compared to the previous lots 0307 and 1006, one MLH1 probe (exon 19) and four MSH2 probes have been replaced. In addition, one extra MSH2 exon 1 probe,
SALSA MLPA KIT P003-B1 MLH1/MSH2 Lot 1209, 0109. As compared to the previous lots 0307 and 1006, one MLH1 probe (exon 19) and four MSH2 probes have been replaced. In addition, one extra MSH2 exon 1 probe,
PENETRANCE ACTIONABILITY SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above) YES (Proceed to Stage II)
 Stage I: Binning Dashboard GENE/GENE PANEL: APC ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition? 2. Does the practice guideline
Stage I: Binning Dashboard GENE/GENE PANEL: APC ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition? 2. Does the practice guideline
The Whys OAP Annual Meeting CCO Symposium September 20. Immunohistochemical Assessment Dr. Terence Colgan Mount Sinai Hospital, Toronto
 Immunohistochemical Assessment of Mismatch Repair Proteins in Endometrial Cancer: The Whys and How Terence J. Colgan, MD Head of Gynaecological Pathology, Mount Sinai Hospital, University of Toronto, Toronto.
Immunohistochemical Assessment of Mismatch Repair Proteins in Endometrial Cancer: The Whys and How Terence J. Colgan, MD Head of Gynaecological Pathology, Mount Sinai Hospital, University of Toronto, Toronto.
FACT SHEET 49. What is meant by a family history of bowel cancer? What is bowel cancer? What causes bowel cancer?
 Important points The most important factors that can influence an individual s chance of developing bowel cancer are getting older and having a family history of bowel cancer A family history of bowel
Important points The most important factors that can influence an individual s chance of developing bowel cancer are getting older and having a family history of bowel cancer A family history of bowel
Mr Chris Wakeman. General Surgeon University of Otago, Christchurch. 12:15-12:40 Management of Colorectal Cancer
 Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
journal of medicine The new england Identification and Survival of Carriers of Mutations in DNA Mismatch-Repair Genes in Colon Cancer ABSTRACT
 The new england journal of medicine established in 1812 june 29, 2006 vol. 354 no. 26 Identification and Survival of Carriers of Mutations in DNA Mismatch-Repair Genes in Colon Cancer Rebecca A. Barnetson,
The new england journal of medicine established in 1812 june 29, 2006 vol. 354 no. 26 Identification and Survival of Carriers of Mutations in DNA Mismatch-Repair Genes in Colon Cancer Rebecca A. Barnetson,
TumorNext-Lynch. genetic testing for hereditary colorectal or uterine cancer
 TumorNet-Lynch genetic testing for hereditary colorectal or uterine cancer What Are the Causes of Hereditary Colorectal Cancer? sporadic 70% familial 20% hereditary 10% Lynch syndrome, up to 4% Familial
TumorNet-Lynch genetic testing for hereditary colorectal or uterine cancer What Are the Causes of Hereditary Colorectal Cancer? sporadic 70% familial 20% hereditary 10% Lynch syndrome, up to 4% Familial
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014
 COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
COLON CANCER & GENETICS VERMONT COLORECTAL CANCER SUMMIT NOVEMBER 15, 2014 WENDY MCKINNON, MS, CGC CERTIFIED GENETIC COUNSELOR FAMILIAL CANCER PROGRAM UNIVERSIT Y OF VERMONT MEDICAL CENTER 1 CHARACTERISTICS
A positive family history has been shown to be an important
 335 LETTER TO JMG Hereditary non-polyposis colorectal cancer: current s of colorectal cancer largely overestimated J Carayol, M Khlat, J Maccario, C Bonaïti-Pellié... A positive family history has been
335 LETTER TO JMG Hereditary non-polyposis colorectal cancer: current s of colorectal cancer largely overestimated J Carayol, M Khlat, J Maccario, C Bonaïti-Pellié... A positive family history has been
How common are mutations in the MSH2 gene? 1. Mutations that cause Lynch syndrome are rare found in approximately 1 in 370 individuals.
 The gene is a tumor suppressor gene. Tumor suppressor genes slow down cell division, repair DNA mistakes, or tell cells when to die. When they don't work properly, cells can grow out of control, which
The gene is a tumor suppressor gene. Tumor suppressor genes slow down cell division, repair DNA mistakes, or tell cells when to die. When they don't work properly, cells can grow out of control, which
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2019 Origination: 1/2004 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2019 Origination: 1/2004 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2018 Origination: 1/2004 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: 2.04.08 Last Review: 1/2018 Origination: 1/2004 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
Management of higher risk of colorectal cancer. Huw Thomas
 Management of higher risk of colorectal cancer Huw Thomas Colorectal Cancer 41,000 new cases pa in UK 16,000 deaths pa 60% 5 year survival Adenoma-carcinoma sequence (Morson) Survival vs stage (Dukes)
Management of higher risk of colorectal cancer Huw Thomas Colorectal Cancer 41,000 new cases pa in UK 16,000 deaths pa 60% 5 year survival Adenoma-carcinoma sequence (Morson) Survival vs stage (Dukes)
MSI test to distinguish between HNPCC and other predisposing syndromes of value in tailored surveillance 1
 Disease Markers 20 (2004) 259 267 259 IOS Press MSI test to distinguish between HNPCC and other predisposing syndromes of value in tailored surveillance 1 Annelie Liljegren a,c, Louise Olsson b and Annika
Disease Markers 20 (2004) 259 267 259 IOS Press MSI test to distinguish between HNPCC and other predisposing syndromes of value in tailored surveillance 1 Annelie Liljegren a,c, Louise Olsson b and Annika
A636P testing in Ashkenazi Jews
 Familial Cancer 3: 223 227, 2004. Ó 2004 Kluwer Academic Publishers. Printed in the Netherlands. A636P testing in Ashkenazi Jews Jose G. Guillem 1, Harvey G. Moore 1, Crystal Palmer 2, Emily Glogowski
Familial Cancer 3: 223 227, 2004. Ó 2004 Kluwer Academic Publishers. Printed in the Netherlands. A636P testing in Ashkenazi Jews Jose G. Guillem 1, Harvey G. Moore 1, Crystal Palmer 2, Emily Glogowski
M. M. Blokhuis G. E. Pietersen P. A. Goldberg U. Algar L. Van der Merwe N. Mbatani A. A. Vorster R. S. Ramesar
 Familial Cancer (2010) 9:357 363 DOI 10.1007/s10689-010-9334-9 Lynch syndrome: the influence of environmental factors on extracolonic cancer risk in hmlh1 c.c1528t mutation carriers and their mutation-negative
Familial Cancer (2010) 9:357 363 DOI 10.1007/s10689-010-9334-9 Lynch syndrome: the influence of environmental factors on extracolonic cancer risk in hmlh1 c.c1528t mutation carriers and their mutation-negative
YES NO UNKNOWN. Stage I: Rule-Out Dashboard ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
P eople who have relatives affected by colorectal cancer
 291 COLON CANCER Accuracy of reporting of family history of colorectal cancer R J Mitchell, D Brewster, H Campbell, M E M Porteous, A H Wyllie, C C Bird, M G Dunlop... See end of article for authors affiliations...
291 COLON CANCER Accuracy of reporting of family history of colorectal cancer R J Mitchell, D Brewster, H Campbell, M E M Porteous, A H Wyllie, C C Bird, M G Dunlop... See end of article for authors affiliations...
CANCER GENETICS PROVIDER SURVEY
 Dear Participant, Previously you agreed to participate in an evaluation of an education program we developed for primary care providers on the topic of cancer genetics. This is an IRB-approved, CDCfunded
Dear Participant, Previously you agreed to participate in an evaluation of an education program we developed for primary care providers on the topic of cancer genetics. This is an IRB-approved, CDCfunded
New Strategy For Treatment Of Hereditary Colorectal Cancer By Shozo Baba
 New Strategy For Treatment Of Hereditary Colorectal Cancer By Shozo Baba If you are looking for a book by Shozo Baba New Strategy for Treatment of Hereditary Colorectal Cancer in pdf form, then you have
New Strategy For Treatment Of Hereditary Colorectal Cancer By Shozo Baba If you are looking for a book by Shozo Baba New Strategy for Treatment of Hereditary Colorectal Cancer in pdf form, then you have
Cascade Genetic Testing in Families with Lynch Syndrome. Elena M. Stoffel MD MPH University of Michigan January 26, 2016
 Cascade Genetic Testing in Families with Lynch Syndrome Elena M. Stoffel MD MPH University of Michigan January 26, 2016 Cascade Genetic Screening An active process to find relatives of patients affected
Cascade Genetic Testing in Families with Lynch Syndrome Elena M. Stoffel MD MPH University of Michigan January 26, 2016 Cascade Genetic Screening An active process to find relatives of patients affected
Universal Screening for Lynch Syndrome in Women with Newly Diagnosed Endometrial Cancer
 Universal Screening for Lynch Syndrome in Women with Newly Diagnosed Endometrial Cancer Sarah E. Ferguson, MD FRCSC; Divisions of Gynecologic Oncology UHN/MSH, Department of Obstetrics and Gynecology,
Universal Screening for Lynch Syndrome in Women with Newly Diagnosed Endometrial Cancer Sarah E. Ferguson, MD FRCSC; Divisions of Gynecologic Oncology UHN/MSH, Department of Obstetrics and Gynecology,
Colonic polyps and colon cancer. Andrew Macpherson Director of Gastroentology University of Bern
 Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Colonic polyps and colon cancer Andrew Macpherson Director of Gastroentology University of Bern Improtance of the problem of colon cancers - Epidemiology Lifetime risk 5% Incidence/10 5 /annum (US Detroit
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
ORIGINAL INVESTIGATION. Association Between Colorectal Cancer and Urologic Cancers
 ORIGINAL INVESTIGATION Association Between Colorectal and Urologic s Audrey H. Calderwood, MD; Dezheng Huo, hd; David T. Rubin, MD Background: Different types of urologic cancers have been associated with
ORIGINAL INVESTIGATION Association Between Colorectal and Urologic s Audrey H. Calderwood, MD; Dezheng Huo, hd; David T. Rubin, MD Background: Different types of urologic cancers have been associated with
Clinicopathological Features and Type of Surgery for Lynch Syndrome: Changes during the Past Two Decades
 pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2016;48(2):605-611 Original Article http://dx.doi.org/10.4143/crt.2015.092 Open Access Clinicopathological Features and Type of Surgery for Lynch Syndrome:
pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2016;48(2):605-611 Original Article http://dx.doi.org/10.4143/crt.2015.092 Open Access Clinicopathological Features and Type of Surgery for Lynch Syndrome:
2018 National Academy of Medicine Annual Meeting
 2018 National Academy of Medicine Annual Meeting October 15, 2018 Targeting Cancer with Precision Prevention Ernest Hawk, M.D., M.P.H. What is Precision Prevention? The concept of precision medicine prevention
2018 National Academy of Medicine Annual Meeting October 15, 2018 Targeting Cancer with Precision Prevention Ernest Hawk, M.D., M.P.H. What is Precision Prevention? The concept of precision medicine prevention
PMS2 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table
 PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
GI EMERGENCIES Acute Abdominal Pain
 GI EMERGENCIES Acute Abdominal Pain Marcia Cruz-Correa, MD, PhD, AGAF. FASGE Associate Professor of Medicine, Biochemistry, Surgery Director Translational Research University of Puerto Rico Comprehensive
GI EMERGENCIES Acute Abdominal Pain Marcia Cruz-Correa, MD, PhD, AGAF. FASGE Associate Professor of Medicine, Biochemistry, Surgery Director Translational Research University of Puerto Rico Comprehensive
MSH6 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table
 MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
Nuclear Pedigree Criteria of Suspected HNPCC
 pp. 34-38 Nuclear Pedigree Criteria of Suspected HNPCC Józef K³adny 1, Gabriela Möslein 2, Torben Myrhøj 3, Grzegorz Kurzawski 4, Anna Jakubowska 4, Tadeusz Dêbniak 4, Wojciech Petriczko 1, Micha³ Koz³owski
pp. 34-38 Nuclear Pedigree Criteria of Suspected HNPCC Józef K³adny 1, Gabriela Möslein 2, Torben Myrhøj 3, Grzegorz Kurzawski 4, Anna Jakubowska 4, Tadeusz Dêbniak 4, Wojciech Petriczko 1, Micha³ Koz³owski
Analysis of current testing practices
 Clin Genet 2015: 87: 368 372 Printed in Singapore. All rights reserved Short Report Analysis of current testing practices for biallelic MUTYH mutations in MUTYH-associated polyposis 2014 John Wiley & Sons
Clin Genet 2015: 87: 368 372 Printed in Singapore. All rights reserved Short Report Analysis of current testing practices for biallelic MUTYH mutations in MUTYH-associated polyposis 2014 John Wiley & Sons
Supporting people at higher risk of bowel cancer
 #never2young Never too young: Supporting people at higher risk of bowel cancer Campaign briefing Supporting people at higher risk of bowel cancer Bowel cancer is the second most common cause of cancer
#never2young Never too young: Supporting people at higher risk of bowel cancer Campaign briefing Supporting people at higher risk of bowel cancer Bowel cancer is the second most common cause of cancer
Caring for Patients at Risk for Hereditary Colorectal Cancer
 February 05, 2007 By Karen Greco, PhD, RN, ANP [1] About 6% of colorectal cancers are caused by genetic mutations associated with hereditary colorectal cancer syndromes. The most common hereditary cancer
February 05, 2007 By Karen Greco, PhD, RN, ANP [1] About 6% of colorectal cancers are caused by genetic mutations associated with hereditary colorectal cancer syndromes. The most common hereditary cancer
A Review from the Genetic Counselor s Perspective
 : A Review from the Genetic Counselor s Perspective Erin Sutcliffe, MS, CGC Certified Genetic Counselor Cancer Risk Evaluation Program INTRODUCTION Errors in base pair matching that occur during DNA replication,
: A Review from the Genetic Counselor s Perspective Erin Sutcliffe, MS, CGC Certified Genetic Counselor Cancer Risk Evaluation Program INTRODUCTION Errors in base pair matching that occur during DNA replication,
Nationwide Study of Clinical and Molecular Features of Hereditary Non-polyposis Colorectal Cancer (HNPCC) in Latvia
 Nationwide Study of Clinical and Molecular Features of Hereditary Non-polyposis Colorectal Cancer (HNPCC) in Latvia ARVIDS IRMEJS 1, VIKTORS BOROSENKO 1, INGA MELBARDE-GORKUSA 1, ANDRIS GARDOVSKIS 1, MARIANNA
Nationwide Study of Clinical and Molecular Features of Hereditary Non-polyposis Colorectal Cancer (HNPCC) in Latvia ARVIDS IRMEJS 1, VIKTORS BOROSENKO 1, INGA MELBARDE-GORKUSA 1, ANDRIS GARDOVSKIS 1, MARIANNA
CAP Laboratory Improvement Programs. Summary of Microsatellite Instability Test Results From Laboratories Participating in Proficiency Surveys
 CAP Laboratory Improvement Programs Summary of Microsatellite Instability Test Results From Laboratories Participating in Proficiency Surveys Proficiency Survey Results From 2005 to 2012 Theresa A. Boyle,
CAP Laboratory Improvement Programs Summary of Microsatellite Instability Test Results From Laboratories Participating in Proficiency Surveys Proficiency Survey Results From 2005 to 2012 Theresa A. Boyle,
Tilburg University. Document version: Publisher's PDF, also known as Version of record. DOI: /s Publication date: 2016
 Tilburg University Hereditary cancer registries improve the care of patients with a genetic predisposition to cancer Vasen, Hans F A; Velthuizen, Mary E; Kleibeuker, Jan H; Menko, Fred H; Nagengast, Fokke
Tilburg University Hereditary cancer registries improve the care of patients with a genetic predisposition to cancer Vasen, Hans F A; Velthuizen, Mary E; Kleibeuker, Jan H; Menko, Fred H; Nagengast, Fokke
Cancer Genomics 101. BCCCP 2015 Annual Meeting
 Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Cancer Genomics 101 BCCCP 2015 Annual Meeting Objectives Identify red flags in a person s personal and family medical history that indicate a potential inherited susceptibility to cancer Develop a systematic
Measure Description. Denominator Statement
 CMS ID/CMS QCDR ID: CAP 18 Title: Mismatch Repair (MMR) or Microsatellite Instability (MSI) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Primary or Metastatic
CMS ID/CMS QCDR ID: CAP 18 Title: Mismatch Repair (MMR) or Microsatellite Instability (MSI) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Primary or Metastatic
THE LIKELY IMPACT OF EARLIER DIAGNOSIS OF CANCER ON COSTS AND BENEFITS TO THE NHS
 Policy Research Unit in Economic Evaluation of Health & Care Interventions (EEPRU) THE LIKELY IMPACT OF EARLIER DIAGNOSIS OF CANCER ON COSTS AND BENEFITS TO THE NHS November 2013 Report 015 Authors: Tappenden
Policy Research Unit in Economic Evaluation of Health & Care Interventions (EEPRU) THE LIKELY IMPACT OF EARLIER DIAGNOSIS OF CANCER ON COSTS AND BENEFITS TO THE NHS November 2013 Report 015 Authors: Tappenden
Why Test for Hereditary Cancer in Preventive Care?
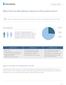 Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Why Test for Hereditary Cancer in Preventive Care? Millions of people are sidelined by cancer. Wouldn't it be worth it for your patients to know their risk? background HEREDITARY (5-10%) More than 1 in
Review Article Relationship between DNA Mismatch Repair Deficiency and Endometrial Cancer
 SAGE-Hindawi Access to Research Molecular Biology International Volume 2011, Article ID 256063, 6 pages doi:10.4061/2011/256063 Review Article Relationship between DNA Mismatch Repair Deficiency and Kenta
SAGE-Hindawi Access to Research Molecular Biology International Volume 2011, Article ID 256063, 6 pages doi:10.4061/2011/256063 Review Article Relationship between DNA Mismatch Repair Deficiency and Kenta
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions. South Island Cancer Nurses Network September 2013
 For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
ACG Clinical Guideline: Colorectal Cancer Screening
 ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Genetic Testing for Lynch Syndrome and Other Inherited Page 1 of 34 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Genetic Testing for Lynch Syndrome and Other
Genetic Testing for Lynch Syndrome and Other Inherited Page 1 of 34 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Genetic Testing for Lynch Syndrome and Other
Subject: Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 05-82000-31 Original Effective Date: 10/15/01 Reviewed: 10/25/18 Revised: 11/15/18 Subject: Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes THIS MEDICAL COVERAGE GUIDELINE
05-82000-31 Original Effective Date: 10/15/01 Reviewed: 10/25/18 Revised: 11/15/18 Subject: Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes THIS MEDICAL COVERAGE GUIDELINE
Clinicopathologic Characteristics of Left-Sided Colon Cancers with High Microsatellite Instability
 The Korean Journal of Pathology 29; 43: 428-34 DOI: 1.4132/KoreanJPathol.29.43.5.428 Clinicopathologic Characteristics of Left-Sided Colon Cancers with High Microsatellite Instability Sang Kyum Kim Junjeong
The Korean Journal of Pathology 29; 43: 428-34 DOI: 1.4132/KoreanJPathol.29.43.5.428 Clinicopathologic Characteristics of Left-Sided Colon Cancers with High Microsatellite Instability Sang Kyum Kim Junjeong
HEREDITARY NONPOLYPOSIS
 ORIGINAL CONTRIBUTION Genetic Testing in Families With Hereditary Nonpolyposis Colon Cancer Caryn Lerman, PhD Chanita Hughes, PhD Bruce J. Trock, PhD Ronald E. Myers, PhD, DSW David Main, MA, MS Aba Bonney,
ORIGINAL CONTRIBUTION Genetic Testing in Families With Hereditary Nonpolyposis Colon Cancer Caryn Lerman, PhD Chanita Hughes, PhD Bruce J. Trock, PhD Ronald E. Myers, PhD, DSW David Main, MA, MS Aba Bonney,
Colorectal Neoplasia. Dr. Smita Devani MBChB, MRCP. Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi
 Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Assessment of Universal Mismatch repair (MMR) or Microsatellite Instability (MSI) testing in colorectal cancers.
 Assessment of Universal Mismatch repair (MMR) or Microsatellite Instability (MSI) testing in colorectal cancers. Soheila Hamidpour MD, Madhusudhana S MD. MMR deficient colorectal tumors can be present
Assessment of Universal Mismatch repair (MMR) or Microsatellite Instability (MSI) testing in colorectal cancers. Soheila Hamidpour MD, Madhusudhana S MD. MMR deficient colorectal tumors can be present
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_colon_cancer 5/2004 8/2017 8/2018 8/2017 Description of Procedure or Service Genetic
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_colon_cancer 5/2004 8/2017 8/2018 8/2017 Description of Procedure or Service Genetic
A Patient s Guide to risk assessment. Hereditary Colorectal Cancer
 A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
A Patient s Guide to risk assessment Hereditary Colorectal Cancer Hereditary Cancer Testing: Is it Right for You? Overview of Syndromes This workbook is designed to help you decide if hereditary cancer
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By. Magnitude of the Problem. Magnitude of the Problem. Cardinal Features of Lynch Syndrome
 GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By HENRY T. LYNCH, M.D. 1 Could this be hereditary Colon Cancer 4 Creighton University School of Medicine Omaha, Nebraska Magnitude of the Problem Annual
GENETICS OF COLORECTAL CANCER: HEREDITARY ASPECTS By HENRY T. LYNCH, M.D. 1 Could this be hereditary Colon Cancer 4 Creighton University School of Medicine Omaha, Nebraska Magnitude of the Problem Annual
Genetic testing all you need to know
 Genetic testing all you need to know Sue Clark Consultant Colorectal Surgeon, St Mark s Hospital, London, UK. Colorectal cancer Familial 33% Polyposis syndromes
Genetic testing all you need to know Sue Clark Consultant Colorectal Surgeon, St Mark s Hospital, London, UK. Colorectal cancer Familial 33% Polyposis syndromes
The Next Generation of Hereditary Cancer Testing
 The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
The Next Generation of Hereditary Cancer Testing Why Genetic Testing? Cancers can appear to run in families. Often this is due to shared environmental or lifestyle patterns, such as tobacco use. However,
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Health and economic consequences of HCV lookback Pereira A
 Health and economic consequences of HCV lookback Pereira A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract contains a
Health and economic consequences of HCV lookback Pereira A Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract contains a
Policy Specific Section: March 1, 2005 January 30, 2015
 Medical Policy Fecal DNA Analysis for Colorectal Cancer Screening Type: Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date: Effective Date: March 1, 2005
Medical Policy Fecal DNA Analysis for Colorectal Cancer Screening Type: Investigational / Experimental Policy Specific Section: Laboratory/Pathology Original Policy Date: Effective Date: March 1, 2005
Chapter 9 Hereditary Nonpolyposis Colorectal Cancer
 Chapter 9 Hereditary Nonpolyposis Colorectal Cancer W. Donald Buie and Anthony R. MacLean Hereditary nonpolyposis colorectal cancer (HNPCC) is one of two distinct inherited colorectal cancer syndromes
Chapter 9 Hereditary Nonpolyposis Colorectal Cancer W. Donald Buie and Anthony R. MacLean Hereditary nonpolyposis colorectal cancer (HNPCC) is one of two distinct inherited colorectal cancer syndromes
Genetic Testing for Lynch Syndrome and Inherited Intestinal Polyposis Syndromes
 Genetic Testing for Lynch Syndrome and Inherited Intestinal Polyposis Syndromes Policy Number: 2.04.08 Last Review: 1/2014 Origination: 1/2004 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas
Genetic Testing for Lynch Syndrome and Inherited Intestinal Polyposis Syndromes Policy Number: 2.04.08 Last Review: 1/2014 Origination: 1/2004 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas
Data briefing: Reflex testing for Lynch syndrome in people diagnosed with bowel cancer under the age of 50
 Data briefing: Reflex testing for Lynch syndrome in people diagnosed with bowel cancer under the age of 50 Introduction Lynch syndrome is an inherited condition that predisposes individuals to bowel and
Data briefing: Reflex testing for Lynch syndrome in people diagnosed with bowel cancer under the age of 50 Introduction Lynch syndrome is an inherited condition that predisposes individuals to bowel and
FAMILIAL COLORECTAL CANCER. Lyn Schofield Manager Familial Cancer Registry
 FAMILIAL COLORECTAL CANCER Lyn Schofield Manager Familial Cancer Registry Cancer in WA 2004 4000 3500 ASPR, rate per 100,000 3000 2500 2000 1500 1000 Male incidence Female incidence Male mortality Female
FAMILIAL COLORECTAL CANCER Lyn Schofield Manager Familial Cancer Registry Cancer in WA 2004 4000 3500 ASPR, rate per 100,000 3000 2500 2000 1500 1000 Male incidence Female incidence Male mortality Female
Endometrial Cancer and Lynch Syndrome: Clinical and Pathologic Considerations
 Lynch syndrome is associated with early onset of cancer, particularly colon and endometrial cancer, and thus warrants careful screening and prevention practices to decrease the likelihood of developing
Lynch syndrome is associated with early onset of cancer, particularly colon and endometrial cancer, and thus warrants careful screening and prevention practices to decrease the likelihood of developing
Detecting and managing hereditary colorectal cancer syndromes in your practice
 PERSONALIZING PATIENT CARE CME CREDIT EDUCATIONAL OBJECTIVE: Readers will assess their patients personal and family histories and suspect hereditary colorectal cancer syndromes if red flags are present
PERSONALIZING PATIENT CARE CME CREDIT EDUCATIONAL OBJECTIVE: Readers will assess their patients personal and family histories and suspect hereditary colorectal cancer syndromes if red flags are present
MLH1 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MLH1 Summary Cancer Risk Table
 MLH1 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Cancer (HNPCC) MLH1 Summary Cancer Risk Table CANCER GENETIC CANCER RISK Endometrial Other MLH1 gene Overview Lynch syndrome 1,
MLH1 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Cancer (HNPCC) MLH1 Summary Cancer Risk Table CANCER GENETIC CANCER RISK Endometrial Other MLH1 gene Overview Lynch syndrome 1,
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Extensive Surgery in LS factoring in gene and gender. Gabriela Möslein
 Extensive Surgery in LS factoring in gene and gender Gabriela Möslein Where we are coming from. Non polyposis colon cancer Recommend subtotal colectomy at the time of the first colon cancer Recommend prophylactic
Extensive Surgery in LS factoring in gene and gender Gabriela Möslein Where we are coming from. Non polyposis colon cancer Recommend subtotal colectomy at the time of the first colon cancer Recommend prophylactic
Hereditary Non Polyposis Colorectal Cancer(HNPCC) From clinic to genetics
 From clinic to genetics Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Autosomal dominant Question 2) Incidence of
From clinic to genetics Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Question 1) Clinical pattern of inheritance of the HNPCC-Syndrome? Autosomal dominant Question 2) Incidence of
Serrated Polyps and a Classification of Colorectal Cancer
 Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Genetic Testing for Lynch Syndrome and Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Mismatch Repair Deficiency Testing for Patients with Colorectal Cancer: A Clinical and Cost-Effectiveness Evaluation
 CADTH Optimal Use Report Mismatch Repair Deficiency Testing for Patients with Colorectal Cancer: A Clinical and Cost-Effectiveness Evaluation September 2015 Volume 5, Issue 3a PROSPERO Registration Number:
CADTH Optimal Use Report Mismatch Repair Deficiency Testing for Patients with Colorectal Cancer: A Clinical and Cost-Effectiveness Evaluation September 2015 Volume 5, Issue 3a PROSPERO Registration Number:
Uptake of genetic testing by the children of Lynch syndrome variant carriers across three generations
 https://helda.helsinki.fi Uptake of genetic testing by the children of Lynch syndrome variant carriers across three generations Seppala, Toni T. 2017-11 Seppala, T T, Pylvanainen, K & Mecklin, J-P 2017,
https://helda.helsinki.fi Uptake of genetic testing by the children of Lynch syndrome variant carriers across three generations Seppala, Toni T. 2017-11 Seppala, T T, Pylvanainen, K & Mecklin, J-P 2017,
Microsatellite instability in colorectal-cancer patients with suspected genetic predisposition.
 Chapter 3 Microsatellite instability in colorectal-cancer patients with suspected genetic predisposition. Calistri D, Presciuttini S, Buonsanti G, Radice P, Gazzoli I, Pensotti V, Sala P, Eboli M, Andreola
Chapter 3 Microsatellite instability in colorectal-cancer patients with suspected genetic predisposition. Calistri D, Presciuttini S, Buonsanti G, Radice P, Gazzoli I, Pensotti V, Sala P, Eboli M, Andreola
A missense germline mutation in exon 7 of the MSH2 gene in a HNPCC family from center-italy
 DOI 10.1007/s10689-006-9110-z ORIGINAL PAPER A missense germline mutation in exon 7 of the MSH2 gene in a HNPCC family from center-italy Francesca Bianchi Æ Eva Galizia Æ Emilio Porfiri Æ Laura Belvederesi
DOI 10.1007/s10689-006-9110-z ORIGINAL PAPER A missense germline mutation in exon 7 of the MSH2 gene in a HNPCC family from center-italy Francesca Bianchi Æ Eva Galizia Æ Emilio Porfiri Æ Laura Belvederesi
Predictive Genetic Testing and Counselling for Hereditary Non-Polyposis Colorectal Cancer (HNPCC)
 Department of Medical Genetics, The Family Federation of Finland and Department of Medical Genetics, Haartman Institute University of Helsinki Predictive Genetic Testing and Counselling for Hereditary
Department of Medical Genetics, The Family Federation of Finland and Department of Medical Genetics, Haartman Institute University of Helsinki Predictive Genetic Testing and Counselling for Hereditary
Genetic Testing for Lynch Syndrome And Other Inherited Colon Cancer Syndromes
 Genetic Testing for Lynch Syndrome And Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Genetic Testing for Lynch Syndrome And Other Inherited Colon Cancer Syndromes Policy Number: Original Effective Date: MM.02.007 09/01/2011 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Genetic Determinants, Risk Assessment and Management
 Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
Genetic Determinants, Risk Assessment and Management Rachel Rando, MS, CGC Genetic Counselor Hunterdon Regional Cancer Center Flemington, NJ I have no disclosures. Acknowledgements: Staff of Hunterdon
