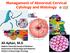
Trend of decreasing length of cervical cone excision during the last 20 years
|
|
|
- Domenic Price
- 5 years ago
- Views:
Transcription
1 European Review for Medical and Pharmacological Sciences 2017; 21: Trend of decreasing length of cervical cone excision during the last 20 years F. SOPRACORDEVOLE 1, N. CLEMENTE 1, G. DELLI CARPINI 1, G. GIORDA 1, A. DEL FABRO 1, L. MORICONI 1, G. DE PIERO 1, L. ALESSANDRINI 2, V. CANZONIERI 2, M. BUTTIGNOL 1, M. NICODEMO 1, A. CIAVATTINI 3 1 Gynecological Oncology Unit, Centro di Riferimento Oncologico, National Cancer Institute, Aviano, Italy 2 Pathology Unit, Centro di Riferimento Oncologico, National Cancer Institute, Aviano, Italy 3 Woman s Health Sciences Department, Gynecologic Section, Università Politecnica delle Marche, Ancona, Italy Francesco Sopracordevole and Nicolò Clemente contributed equally to this work Abstract. OBJECTIVE: The aim of the present investigation was to evaluate the cervical conizations performed in the last 20 years in a single institution, with a particular interest in analyzing the trend of the length of cone excisions. PATIENTS AND METHODS: A retrospective cohort study of women who underwent a CO 2 -laser cervical conization between January 1996 and December Cytological abnormalities on referral pap smear, colposcopic findings and pertinent clinical and socio-demographic characteristics of each woman were collected. In particular, the length of cone specimen was evaluated, taking into account all the factors potentially influencing the length of excision. RESULTS: A total of 1270 women who underwent cervical conization from January 1996 to December 2015 were included in the analysis. A mean cone length of 15.1 ± 5.7 mm was reported, and we observed a significant decrease in the length of cone excisions over the whole study period. Age (r partial = , p < ), see & treat procedure (r partial = , p < ) and grade II colposcopic findings (r partial = , p < ) were significantly associated with the length of cone excision on multivariate analysis. CONCLUSIONS: In the last 20 years, a significant decrease in the length of cone excision was observed. In our opinion, this can be due to the acquired awareness by the gynecologists of the potential disadvantages of wide cone excision in term of adverse obstetric outcomes in future pregnancies. Key Words: Cervical conization, CO 2 laser conization, CIN, Cervical excision. Introduction High-grade cervical intraepithelial neoplasia (CIN) and usual type adenocarcinoma in situ (AIS) are precancerous lesions of the uterine cervix, induced by persistent infection by high-risk human papilloma virus (HR-HPV) 1-3. In the last decades, the ability of the cervical cancer screening test (Pap test and HPV DNA test) to identify women at risk of precancerous lesions, and the availability of effective and relatively non-invasive treatment for these lesions has led to a reduction of incidence and mortality for cervical cancer in most industrialized countries 4. Cervical precancers can occur at any age, but the peak incidence is in women aged years 5 ; therefore, most of these lesions are diagnosed and treated in childbearing age women 6,7. Moreover, in the last decades, we have seen a continuous trend of delayed childbearing, which has resulted in an increased proportion of women being diagnosed with high-grade CIN or AIS (and subsequently treated) before their first pregnancy 8. As reported in the 2012 ASCCP guidelines for the management of abnormal cervical cancer screening tests and cancer precursors 9, and in the 2009 European guidelines for clinical management of abnormal cervical cytology 10, in the case of high-grade CIN, an excisional procedure is recommended. In the case of AIS, a total hysterectomy remains the treatment of choice; however, for women who wish to maintain fertility, a conservative approach with cervical conization Corresponding Author: Nicolò Clemente, MD; nicoclemente@alice.it 4747
2 F. Sopracordevole, N. Clemente, G. Delli Carpini, G. Giorda, A. Del Fabro, et al. can be proposed 9. Similarly, a fertility sparing approach with cervical conization can be safely proposed (in selected cases) even for women with microinvasive cervical cancer 11. Cervical conization can be performed with different techniques: cold knife, loop electrosurgical excision procedure (LEEP) and carbon dioxide laser (CO 2 laser). Regardless the technique used, the surgical removal of a portion of the cervix leads to a higher risk for obstetric complications due to the loss of cervical integrity 1,12. Indeed, in women with a history of excisional cervical surgery, an increased risk of adverse obstetric events, such as premature rupture of the membranes and preterm birth has been reported 13,14. In particular, the risk of preterm birth appears to be related to the length of cone excision 1,5,15. It is indeed reported that a cone length > 15 mm is associated with a doubled risk of preterm birth 16. For these reasons, in the last years, gynecologists have tried to be as more conservative as possible in treating cervical dysplasia. Thus, a trend of reduction in the dimension of the cone specimen should have been expected. The aim of the present work was therefore to analyze the cervical conizations performed in the last 20 years in a single institution, evaluating the trend of the length of cone excisions. Patients and Methods This was a retrospective cohort study of women who underwent a cervical excision procedure for CIN, AIS or micro-invasive cervical cancer between January 1996 and December 2015 at the Gynecological Oncology Unit, Centro di Riferimento Oncologico, National Cancer Institute, Aviano, Italy. For the present analysis, we considered only women who had undergone a cervical conization for the first time. Women with a concomitant diagnosis of vaginal dysplasia or vaginal cancer were excluded, as well as women with previous ablative treatments on the uterine cervix. Age, menopausal status, referral cytology, colposcopic findings and histological diagnosis (on colposcopy-guided biopsy) were collected for each patient. Referral cytological abnormalities were classified according to the most recent Bethesda system terminology 17. Cytology examinations performed before the introduction of the most recent Bethesda system terminology were revised accordingly. The colposcopic characteristics of each woman (visibility of the squamocolumnar junction, normal/abnormal colposcopic findings and, in particular, the definition of grade I and grade II findings) were recorded according to the 2011 revised colposcopic terminology of the International Federation for Cervical Pathology and Colposcopy (IFCPC) 18. The colposcopies performed before the introduction of the 2011 IFCPC nomenclature were revised accordingly. We have defined a two-step strategy for those cases in which the cervical conization was performed after a colposcopy-guided biopsy following an abnormal cytology. A see & treat strategy (in which the conization was performed without a prior cervical biopsy) was sometimes adopted in cases of high-grade referral cervical smear with a high-grade colposcopic impression. This approach was sometimes adopted also in the case of persistent low-grade cervical smear with a high-grade colposcopic impression or in case of high-grade cytology (or persistent low-grade cytology) in women in whom the squamocolumnar junction was not visible on colposcopy. However, the choice between the two strategies (two-step or see & treat) was made case by case, after an informed discussion between the operator and the patient, taking into account the referral cervical smear, the colposcopic impression, the clinical history and patient s preference. We have considered as high-grade preoperative diagnosis the following conditions: Cytological diagnosis of atypical squamous cells cannot exclude HSIL (ASCH), high grade squamous intraepithelial lesion (HSIL), Atypical Glandular Cells, favor neoplastic (AGC-FN) and adenocarcinoma in situ (AIS) for women with the see & treat strategy Histopathological diagnosis of CIN 2, CIN 3, AIS or invasive cancer, for women with a twostep strategy. At the histopathological examination of the cone specimen, the status of ectocervical (external margins) and endocervical (apex) cone margins and the length of the cone specimen was analyzed. The histopathological cone specimens were classified as negative, low-grade cervical intraepithelial neoplasia (CIN 1), high-grade cervical intraepithelial neoplasia (CIN 2 and CIN 3), squamous cell carcinoma (microinvasive or invasive), adenocarcinoma in situ, or adenocarcinoma (microinvasive or invasive) 19. In the cases in which 4748
3 Trend of decreasing length of cervical cone excision during the last 20 years different grades of dysplasia coexisted, the worse histopathological diagnosis was considered for the subsequent analyses. The dimensions of cone specimens were determined with a ruler by the pathologist after fixation in formalin and are expressed in millimeters. In particular, the cone length was defined as the distance from the distal to the proximal margin of the cone specimen, as otherwise described 18. All the data previously described were obtained by a review of the medical records of all the patients included in the analysis. Women with incomplete or missing data were excluded. All the procedures were performed by the same experienced operator in an outpatient setting, under local anesthesia and strict colposcopic guidance, with a hand-directed CO 2 laser (Sharplan CO 2 Laser System, Laser Ventures Inc., Woodstock, GA, USA) with a maximum power output of 40 Watts. The beam spot diameter ranged from 0.5 to 1 mm with an irradiance ranging from 2500 to 3500 W/cm 2, guided by a micromanipulator. The primary aim of the present investigation was to analyze the cervical conizations performed during the study period, with a particular interest in evaluating the trend of the length of cone excisions. As a secondary analysis, we investigated the factors related to the positivity of endocervical margins, even considering the cone length. According to a previous studies 20, we identified the following categories of cone length for the analysis: 1-9 mm, mm, mm and 20 mm. Statistical Analysis Statistical software SPSS 20 (IBM SPSS Statistics for Windows, Armonk, NY, USA) was used for data analysis. All continuous variables were tested for normality with the D Agostino-Pearson test; normally distributed variables were expressed as mean ± SD, while skewed variables were reported as median and interquartile range (IQR). The t-test or the Mann-Whitney test were used for comparison as appropriate. Qualitative variables were expressed as proportions and were compared with Chi-square or Fisher s exact test as appropriate. Correlation between continuous, normally distributed variables was determined with Pearson s correlation coefficient (r). We analyzed the trend of age and cone length as a function of the year of the procedure and the one-way ANOVA test, along with the Tukey-Kramer test as post-hoc test, was used for comparison between mean age and mean cone length during the study period. A univariate analysis was performed with the aim of identifying factors that were significantly associated with the length of cone excision. A stepwise multivariate linear regression analysis was, then, performed including factors that were significantly associated with cone length at the univariate analysis. A similar approach (univariate stepwise multivariate logistic regression) was used to identify factors associated with positivity of endocervical margins. Local Ethic Committee approval was properly obtained for this investigation. Results From January 1996 to December 2015, 1521 women underwent a CO 2 -laser cervical conization at our institute. Among these, 103 patients with concomitant diagnosis of pre-invasive or invasive vaginal lesions, 73 women with previous cervical treatments and 75 women with incomplete or missing data on their medical charts were excluded. Therefore, 1270 patients were included in the final analysis and constituted the study population. In the entire study cohort, the mean (± SD) age was 38.7 ± 9.3 years and 123 women (9.7%) were post-menopausal. On colposcopy, the squamocolumnar junction was visible in 1235 women (97.2%). More precisely, 33 of them (2.7%) had a normal colposcopic finding; 458 (37.1%) showed grade I abnormal colposcopic findings and 744 women (60.2%) had grade II abnormal colposcopic findings. Table I shows the preoperative diagnosis (before cervical conization) according to the two different therapeutic approaches (see & treat vs. two-step). The see & treat strategy was adopted in 270 women (21.2%). A high-grade pre-operative diagnosis (as previously defined) was found in 1204 (94.8%) patients and, in particular, a pre-operative diagnosis of glandular abnormalities (cytological or histological) emerged in 82 women (6.5%). Table II reports the histopathological diagnosis on final cone specimens. The mean (± SD) cone length in the entire study population was 15.1 ± 5.7 mm. The endocervical margin was positive in 145 (11.4%) patients, while the ectocervical margin in 23 cases (1.8%). 4749
4 F. Sopracordevole, N. Clemente, G. Delli Carpini, G. Giorda, A. Del Fabro, et al. Table I. Pre-operative diagnosis according to the two different therapeutic approaches (see & treat and two-step). Approach Diagnosis No. (%) See & treat ASCUS 2 (0.7) (no. = 270) ASC-H 48 (17.8) LSIL 8 (3.0) HSIL 168 (62.2) AGC-NOS 32 (11.9) AGC-FN 10 (3.7) AIS 2 (0.7) Two-step CIN 1 24 (2.4) (no. = 1000) CIN (39.8) CIN (50.5) AIS 16 (1.6) Invasive SCC 18 (1.8) Invasive AC 39 (3.9) ASCUS: atypical squamous cells of undetermined significance; ASC-H: atypical squamous cells cannot exclude HSIL; LSIL: low-grade squamous intraepithelial lesion; HSIL: high-grade squamous intraepithelial lesion; AGC-NOS: atypical glandular cells not otherwise specified; AGC-FN: atypical glandular cells favor neoplastic; AIS: adenocarcinoma in situ; CIN: cervical intraepithelial neoplasia; SCC: squamous cell carcinoma; AC: adenocarcinoma. Figure 1 presents the trend of cone length in the period A significant decrease over the whole study period emerged (p < 0.001, one-way ANOVA) and, in particular, the mean (± SD) cone length in the period was significantly lower than the period (17.2 ± 6.0 vs ± 4.8 mm, p < ). Moreover, comparing the cervical conizations performed in 2015 with those performed in 1996, a reduction in the mean cone length of 30% was observed. Analyzing the factors potentially related to the length of the cone excision, we found a significant positive correlation with women s age (r = , p = ). Furthermore, patients with a highgrade pre-operative diagnosis on cytology or cervical biopsy had a significantly higher length of cone excision, compared to patients with a lowgrade pre-operative diagnosis (15.2 ± 5.8 vs ± 5.0 mm, p = ). Similarly, a higher length of cone excision was observed in women with grade II colposcopic findings, compared to women with grade I colposcopy (15.9 ± 6.0 vs ± 5.2 mm, p < ). The women who underwent a see & treat procedure presented instead a significantly lower length of cone excision, compared to those who underwent the two-step approach (13.0 ± 4.6 vs ± 5.9, p < ). No significant correlation emerged between the length of cone excision and the menopausal status, visibility of SCJ on colposcopy or pre-operative diagnosis of glandular lesion. Therefore, we performed a multivariate logistic regression including the following variables: age, see & treat procedure, high-grade preoperative diagnosis and grade II colposcopic appearance. On multivariate analysis, age (r partial = , p < ), see & treat (r partial = , p < ) and high-grade colposcopic appearance (r partial = , p < ) were confirmed to be significantly and independently associated with the length of the cone excision. As a secondary analysis, we investigated the factors related to the positivity of endocervical margins, even considering the cone length, in the whole study population. The mean (± SD) cone length in women with a positive endocervical margin was significantly shorter than women with a negative endocervical margin (14.2 ± 6.0 vs ± 5.7 mm, p = ) and a significantly decrease in the positivity of the endocervical margin with respect to the categories of cone length emerged (Table III). More precisely, the women with 1-9 mm cone length showed a higher positivity of the endocervical margin than women with cone length Table II. Histopathological diagnosis on final cone specimens. Whole study cohort See and treat two-step Diagnosis no. = 1270 no. = 270 no. = 1000 p Negative 75 (5.9) 17 (6.3) 58 (5.8) 0.87 CIN (12.7) 41 (15.2) 120 (12.0) 0.19 CIN (32.4) 78 (28.9) 333 (33.3) 0.19 CIN (39.6) 116 (42.9) 387 (38.7) 0.24 AIS 16 (1.2) 4 (1.5) 12 (1.2) 0.93 Invasive SCC 69 (5.4) 9 (3.3) 60 (6.0) 0.11 Invasive AC 35 (2.8) 5 (1.9) 30 (3.0) 0.44 CIN: cervical intraepithelial neoplasia; AIS: adenocarcinoma in situ; SCC: squamous cell carcinoma; AC: adenocarcinoma. Data are expressed as n (%) 4750
5 Trend of decreasing length of cervical cone excision during the last 20 years Figure 1. Length of cone excisions (expressed as mean ± SD) in the entire study cohort (n = 1270) considering the year of the procedure. 10 mm (17.9 vs. 10.7%, p = ), while no difference between women with a cone length of mm vs. 15 mm was noted (12.0 vs. 9.9%, p = ). Patients with a positive endocervical margin presented a significantly higher age at the procedure than patients with a negative endocervical margin (41.8 ± 9.6 vs ± 9.2 years, p < ). None of the other considered factors (menopausal status, visibility of SCJ, see & treat strategy, high-grade preoperative diagnosis, pre-operative diagnosis of glandular lesions or grade II colposcopic findings) was significantly associated with the positivity of the endocervical margin (Table IV). On multivariable logistic regression, age and cone length were both significantly and independently associated with the positivity of endocervical margins (age: OR = , 95% CI , p < and cone length: OR = , 95% CI , p = ). Table III. Positivity of endocervical margin according to cone length in the entire study population. Cone length No. Positive endocervical margin no. (%) p 1-9 mm (17.9) mm (12.0) mm (10.6) 20 mm (9.1) Total (11.4) CIN: cervical intraepithelial neoplasia; AIS: adenocarcinoma in situ; SCC: squamous cell carcinoma; AC: adenocarcinoma. Data are expressed as n (%) 4751
6 F. Sopracordevole, N. Clemente, G. Delli Carpini, G. Giorda, A. Del Fabro, et al. Table IV. Univariate analysis of factors potentially related to positivity of endocervical margin in the entire study population. Positive endocervical margin Negative endocervical margin Characteristics (no. = 145) (no. = 1125) p Age (yrs) 41.8 ± ± 9.2 < Menopause 21 (14.5) 102 (9.1) 0.06 Visible SCJ 137 (94.5) 1098 (97.6) 0.06 See & treat 34 (23.4) 236 (21.0) 0.58 High-grade preoperative diagnosis 136 (93.8) 1068 (94.9) 0.72 Glandular preoperative diagnosis 14 (9.7) 67 (6.0) 0.13 Abnormal grade II colposcopy 86 (59.3) 667 (59.3) 0.93 Cone length 14.2 ± ± Data are expressed as mean ± SD or no. (%) as appropriate. Discussion CIN is currently considered the precursor of invasive carcinoma of the uterine cervix, and HPV is the most important pathogenetic factor 21. Considering the growing incidence of HPV-related lesions in women of reproductive age 8, in the last few years, cervical excision procedures for treatment of high-grade cervical dysplasia have become increasingly common 9. The peak incidence of such lesions is in women aged years 5, thus, even considering the continuous trend of delayed childbearing observed over the last decades, many women with high-grade dysplasia are treated before their first pregnancy 8. For this reason, the potential impact of cervical conization on future pregnancies is a matter of increasing relevance in the literature. In the last few years, several articles have been published on this topic, and there is currently a widespread evidence suggesting an increasing occurence of adverse obstetric events in women treated with cervical conization. In particular, a high rate of miscarriage and, mostly, a significant risk of preterm delivery have been reported 1,8,13,14,22,23. The risk of preterm delivery in pregnancies following cervical conization seems to be related to the length of the cone excision 1,15,22, and a cone length > 15 mm has been found to be associated with a doubled risk of preterm birth 16. Interestingly, such a risk is not restricted to the first pregnancy post-treatment 23. Moreover, the need for a deep cone excision has been questioned by some authors who demonstrated that the average depth of the squamocolumnar junction is less than 12 mm in women in whom the upper limit of the transformation zone was not visible on colposcopy 24. Hence, considering that the cervical dysplasia usually spreads on the transformation zone, a cone excision of 12 mm or less could be considered a safe option even for women in whom the squamocolumnar junction is not visible on colposcopy. On these bases, in recent years, gynecologists have shown an increased sensitivity to the issues of conization-related adverse obstetric events, and have tried to reduce the length of cone excisions in their daily clinical practice. Through this retrospective analysis, we observed a significant decrease in the length of cone excision over the whole study period, with a 30% reduction in the length of cone specimens, from 1996 to In the multivariate analysis, age and high-grade colposcopic appearance were associated with a deeper excision on cervical conization. This was expected since in older women, with a high-grade colposcopic appearance, the attitude of the gynecologist is to obtain a complete excision of the lesion, regardless of the potential problems for future pregnancies. On the contrary, in younger women, gynecologists try to be as conservative as possible, in order to minimize the risks of adverse obstetric outcomes in future pregnancies. Women with a cone length < 10 mm showed a higher rate of positive endocervical margin compared to women with a cone length 10 mm. Furthermore, it is interesting to observe that no significant differences in the positivity of the endocervical margin of the specimen emerged in women with a cone length of mm compared to women with a cone excision of 15 mm or more. This datum is of particular clinical relevance since it demonstrates that a reduction in cone length does not influence the radicality of the surgical procedure (even if a length of excision of at least 10 mm should be reached in order to minimize the risk of positivity of the endocervical margin). This is a matter of relevance mostly 4752
7 Trend of decreasing length of cervical cone excision during the last 20 years in women of childbearing age with glandular lesions and positive endocervical margin, in which a re-excision is recommended 9. Thus, it should be advisable that the length of cone excision in women with high-grade cervical dysplasia ranges from 10 to 15 mm (except for women in whom a deeper progression of the lesion in the endocervical canal is documented), even if it is not always easy to control precisely the length of excision during the procedure of conization. The main strength of the present study is the large number of cases, included through an over 20-years clinical practice. Moreover, all the excisions were performed in the same institution, with the same techniques (CO 2 laser excision), by the same gynecologist (FS) with particular expertise in the management of cervical preinvasive lesions and cancers. As already described in previous studies, cervical conization can be performed with different techniques: LEEP and CO 2 laser are the most commonly used. No method has proved to be superior in terms of the rate of treatment failure, the disease persistence on follow-up, the adequacy of the specimen for histopathological evaluation and the risk of morbidity 25. However, in a recent systematic review and meta-analysis, Kyrgiou et al 22 reported a slightly higher relative risk for preterm birth in women treated with CO 2 laser conization compared to LEEP (2.11 vs. 1.56). Obviously, each technique of conization has strengths and weaknesses. For example, LEEP is less expensive and easy to use, with a faster learning curve for the operator, while CO 2 laser conization is more difficult technique that requires a greater expertise by the operator, and is more expensive. However, CO 2 laser conization has a great advantage: it allows the operator to customize the procedure, tailoring the extension and the depth of the excision to the characteristics of each woman (localization of the lesion, colposcopic appearance, cervical dimensions). For this reason, in our opinion, it is interesting to observe the trend of conization performed with this technique over the years, since it can be considered a real and reliable expression of the operator s tendency to reduce the depth of excision. Due to its retrospective nature, unavoidably, this work has potential limitations. Since the data collected are limited to those already reported in the medical charts, it has not been possible to analyze the obstetric outcome in these patients (e.g., the rate of preterm delivery post conization). Conclusions In the last few years, gynecologists have shown an increased sensitivity to the problems related to cervical conization and have tried to reduce the length of cone excisions in their daily clinical practice. In this study, such a trend has been demonstrated in detail, reporting a significant decrease in the length of cone excision in the last 20 years. Acknowledgements The Authors thank Anna Vallerugo, MA, for the editing. Conflict of Interest The Authors declare that they have no conflict of interests. References 1) Liverani CA, Di Giuseppe J, Clemente N, Delli Carpini G, Monti E, Fanetti F, Bolis G, Ciavattini A. Length but not transverse diameter of the excision specimen for high-grade cervical intraepithelial neoplasia (CIN 2-3) is a predictor of pregnancy outcome. Eur J Cancer Prev 2016; 25: ) Frega A, Lavini G, Guarino A, Giovanale V, Lukic A, Bianchi P, Cozza G, Marziani R, D Ambrosio A, French D, Caserta D. Cervical carcinogenesis, bacterial vaginosis, HPV-mRNA test and relapse of CIN2+ after loop electrosurgical excision procedure (LEEP). Eur Rev Med Pharmacol Sci 2017; 21: ) French D, Belleudi F, Mauro MV, Mazzetta F, Raffa S, Fabiano V, Frega A, Torrisi MR. Expression of HPV16 E5 down-modulates the TGFbeta signaling pathway. Mol Cancer 2013; 12: 38. 4) Giorgi Rossi P, Benevolo M, Vocaturo A, Caraceni D, Ciccocioppo L, Frega A, Terrenato I, Zappacosta R, French D, Rosini S. Prognostic value of HPV E6/E7 mrna assay in women with negative colposcopy or CIN1 histology result: a follow-up study. PLoS One 2013; 8: e ) Noehr B, Jensen A, Frederiksen K, Tabor A, Kjaer SK. Depth of cervical cone removed by loop electrosurgical excision procedure and subsequent risk of spontaneous preterm delivery. Obstet Gynecol 2009; 114: ) Origoni M, Salvatore S, Perino A, Cucinella G, Candiani M. Cervical Intraepithelial Neoplasia (CIN) in pregnancy: the state of the art. Eur Rev Med Pharmacol Sci 2014; 18: ) Frega A, Verrone A, Manzara F, Schimberni M, Catalano A, Milazzo GN, Marziani R, Cozza G, Bianchi P, French D, Sesti F, Caserta D. Expression of E6/ 4753
8 F. Sopracordevole, N. Clemente, G. Delli Carpini, G. Giorda, A. Del Fabro, et al. E7 HPV-DNA, HPV-mRNA and colposcopic features in management of CIN2/3 during pregnancy. Eur Rev Med Pharmacol Sci 2016; 20: ) Ciavattini A, Clemente N, Delli Carpini G, Gentili C, Di Giuseppe J, Barbadoro P, Prospero E, Liverani CA. Loop electrosurgical excision procedure and risk of miscarriage. Fertil Steril 2015; 103: ) Massad LS, Einstein MH, Huh WK, Katki HA, Kinney WK, Schiffman M, Solomon D, Wentzensen N, Lawson HW; 2012 ASCCP Consensus Guidelines Conference updated consensus guidelines for the management of abnormal cervical cancer screening tests and cancer precursors. J Low Genit Tract Dis 2013; 17(5 Suppl 1): S1-S27. 10) Jordan J, Martin-Hirsch P, Arbyn M, Schenck U, Baldauf JJ, Da Silva D, Anttila A, Nieminen P, Prendiville W. European guidelines for clinical management of abnormal cervical cytology, part 2. Cytopathology 2009; 20: ) Sopracordevole F, Chiossi G, Barbero M, Cristoforoni P, Ghiringhello B, Frega A, Tortolani F, Boselli F, Clemente N, Ciavattini A; Italian Society of Colposcopy and Cervico-Vaginal Pathology. Surgical approach and long-term clinical outcome in women with microinvasive cervical cancer. Anticancer Res 2014; 34: ) Crane JM. Pregnancy outcome after loop electrosurgical excision procedure: a systematic review. Obstet Gynecol 2003; 102: ) Kyrgiou M, Koliopoulos G, Martin-Hirsch P, Arbyn M, Prendiville W, Paraskevaidis E. Obstetric outcomes after conservative treatment for intraepithelial or early invasive cervical lesions: systematic review and meta-analysis. Lancet 2006; 367: ) Frega A, Sesti F, De Sanctis L, Pacchiarotti A, Votano S, Biamonti A, Sopracordevole F, Scirpa P, Catalano A, Caserta D, Gentile M, Schimberni M, Moscarini M. Pregnancy outcome after loop electrosurgical excision procedure for cervical intraepithelial neoplasia. Int J Gynaecol Obstet 2013; 122: ) Kyrgiou M, Valasoulis G, Stasinou SM, Founta C, Athanasiou A, Bennett P, Paraskevadis E. Proportion of cervical excision for cervical intraepithelial neoplasia as a predictor of pregnancy outcomes. Int J Gynaecol Obstet 2015; 128: ) Castanon A, Landy R, Brocklehurst P, Evans H, Peebles D, Singh N, Walker P, Patnick J, Sasieni P; PaCT Study Group. Risk of preterm delivery with increasing depth of excision for cervical intraepithelial neoplasia in England: nested case-control study. Br Med J 2014; 349: g ) Nayar R, Wilbur DC. The Pap Test and Bethesda J Low Genit Tract Dis 2015; 19: ) Bornstein J, Bentley J, Bösze P, Girardi F, Haefner H, Menton M, Perrotta M, Prendiville W, Russell P, Sideri M, Strander B, Tatti S, Torne A, Walker P colposcopic terminology of the International Federation for Cervical Pathology and Colposcopy. Obstet Gynecol 2012; 120: ) Histopathology and cytopathology of the uterine cervix: digital atlas Frappart, L; International Agency for Research on Cancer. Lyon, France: International Agency for Research on Cancer: Distributed by IARC Press, c NLM ID: [Electronic Resource]. 20) Sasieni P, Castanon A, Landy R, Kyrgiou M, Kitchener H, Quigley M, Poon L, Shennan A, Hollingworth A, Soutter WP, Freeman-Wang T, Peebles D, Prendiville W, Patnick J. Risk of preterm birth following surgical treatment for cervical disease: executive summary of a recent symposium. BJOG 2016; 123: ) Frega A, Sesti F, Lombardi D, Votano S, Sopracordevole F, Catalano A, Milazzo GN, Lombardo R, Assorgi C, Olivola S, Chiusuri V, Ricciardi E, French D, Moscarini M. Assessment of HPV-mRNA test to predict recurrent disease in patients previously treated for CIN 2/3. J Clin Virol 2014; 60: ) Kyrgiou M, Athanasiou A, Paraskevaidi M, Mitra A, Kalliala I, Martin-Hirsch P, Arbyn M, Bennett P, Paraskevaidis E. Adverse obstetric outcomes after local treatment for cervical preinvasive and early invasive disease according to cone depth: systematic review and meta-analysis. BMJ 2016; 354: i ) Castañon A, Landy R, Brocklehurst P, Evans H, Peebles D, Singh N, Walker P, Patnick J, Sasieni P; PaCT Study Group. Is the increased risk of preterm birth following excision for cervical intraepithelial neoplasia restricted to the first birth post treatment? BJOG 2015; 122: ) Saunders N, Anderson D, Sheridan E, Gilbert L, Sharp F. Endoscopic localization of the squamocolumnar junction before cervical cone biopsy in 284 patients. Cancer 1990; 65: ) Martin-Hirsch PP, Paraskevaidis E, Bryant A, Dickinson HO. Surgery for cervical intraepithelial neoplasia. Cochrane Database Syst Rev 2013; 12: CD
!"#$%&'(#)*$+&,$-&.#,$/#0()1-$ ),1')$2(%&,2#,%$%(0'#$34567$
 !"#$%&'(#)*$+&,$-&.#,$/#0()1-$ ),1')$2(%&,2#,%$%(0'#$34567$ Updated Consensus Guidelines for Managing Abnormal Cervical Cancer Screening Tests and Cancer Precursors American Society for and Cervical Pathology
!"#$%&'(#)*$+&,$-&.#,$/#0()1-$ ),1')$2(%&,2#,%$%(0'#$34567$ Updated Consensus Guidelines for Managing Abnormal Cervical Cancer Screening Tests and Cancer Precursors American Society for and Cervical Pathology
EARLY ONLINE RELEASE
 EARLY ONLINE RELEASE Note: This article was posted on the Archives Web site as an Early Online Release. Early Online Release articles have been peer reviewed, copyedited, and reviewed by the authors. Additional
EARLY ONLINE RELEASE Note: This article was posted on the Archives Web site as an Early Online Release. Early Online Release articles have been peer reviewed, copyedited, and reviewed by the authors. Additional
The society for lower genital tract disorders since 1964.
 The society for lower genital tract disorders since 1964. Updated Consensus Guidelines for Managing Abnormal Cervical Cancer Screening Tests and Cancer Precursors American Society for and Cervical Pathology
The society for lower genital tract disorders since 1964. Updated Consensus Guidelines for Managing Abnormal Cervical Cancer Screening Tests and Cancer Precursors American Society for and Cervical Pathology
Treatment of Cervical Intraepithelial Neoplasia. Case. How would you manage this woman?
 Treatment of Cervical Intraepithelial Neoplasia Karen Smith-McCune Professor, Department of Obstetrics, Gynecology and Reproductive Sciences I have no conflicts of interest Case How would you manage this
Treatment of Cervical Intraepithelial Neoplasia Karen Smith-McCune Professor, Department of Obstetrics, Gynecology and Reproductive Sciences I have no conflicts of interest Case How would you manage this
Clinical Guidance: Recommended Best Practices for Delivery of Colposcopy Services in Ontario Best Practice Pathway Summary
 Clinical Guidance: Recommended Best Practices for Delivery of Colposcopy Services in Ontario Best Practice Pathway Summary Glossary of Terms Colposcopy is the examination of the cervix, vagina and, in
Clinical Guidance: Recommended Best Practices for Delivery of Colposcopy Services in Ontario Best Practice Pathway Summary Glossary of Terms Colposcopy is the examination of the cervix, vagina and, in
Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two
 Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two Seshu P. Sarma, MD, FAAP Emory University Regional Training Center Atlanta, Georgia Produced by the Alabama Department of Public Health
Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two Seshu P. Sarma, MD, FAAP Emory University Regional Training Center Atlanta, Georgia Produced by the Alabama Department of Public Health
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines
 Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Understanding Your Pap Test Results
 Understanding Your Pap Test Results Most laboratories in the United States use a standard set of terms called the Bethesda System to report pap test results. Normal: Pap samples that have no cell abnormalities
Understanding Your Pap Test Results Most laboratories in the United States use a standard set of terms called the Bethesda System to report pap test results. Normal: Pap samples that have no cell abnormalities
What is being excised and why? Professor Henry Kitchener Institute of Cancer Sciences The University of Manchester
 What is being excised and why? Professor Henry Kitchener Institute of Cancer Sciences The University of Manchester Qu. What is being excised? A. Colposcopic lesions which should contain CIN2+ Qu. Why is
What is being excised and why? Professor Henry Kitchener Institute of Cancer Sciences The University of Manchester Qu. What is being excised? A. Colposcopic lesions which should contain CIN2+ Qu. Why is
Making Sense of Cervical Cancer Screening
 Making Sense of Cervical Cancer Screening New Guidelines published November 2012 Tammie Koehler DO, FACOG The incidence of cervical cancer in the US has decreased more than 50% in the past 30 years because
Making Sense of Cervical Cancer Screening New Guidelines published November 2012 Tammie Koehler DO, FACOG The incidence of cervical cancer in the US has decreased more than 50% in the past 30 years because
Prof. Silvio Tatti MD, MSc, Phd, FACOG Past President IFCPC Hospital de Clínicas José de San Martín University of Buenos Aires
 Prof. Silvio Tatti MD, MSc, Phd, FACOG Past President IFCPC Hospital de Clínicas José de San Martín University of Buenos Aires Introduction and Update of the new IFCPC nomenclature Professor Silvio Tatti
Prof. Silvio Tatti MD, MSc, Phd, FACOG Past President IFCPC Hospital de Clínicas José de San Martín University of Buenos Aires Introduction and Update of the new IFCPC nomenclature Professor Silvio Tatti
Running head: EVIDENCE-BASED MEDICINE TWO-STEP DISCREPANCY
 Evidence-Based Medicine Two-Step Discrepancy 1 Running head: EVIDENCE-BASED MEDICINE TWO-STEP DISCREPANCY Evidence-Based Medicine Two-Step Discrepancy Julie Nelson Texas Woman s University Philosophy of
Evidence-Based Medicine Two-Step Discrepancy 1 Running head: EVIDENCE-BASED MEDICINE TWO-STEP DISCREPANCY Evidence-Based Medicine Two-Step Discrepancy Julie Nelson Texas Woman s University Philosophy of
Cervical Cancer Screening for the Primary Care Physician for Average Risk Individuals Clinical Practice Guidelines. June 2013
 Cervical Cancer Screening for the Primary Care Physician for Average Risk Individuals Clinical Practice Guidelines General Principles: Since its introduction in 1943, Papanicolaou (Pap) smear is widely
Cervical Cancer Screening for the Primary Care Physician for Average Risk Individuals Clinical Practice Guidelines General Principles: Since its introduction in 1943, Papanicolaou (Pap) smear is widely
Cervical Conization. 1
 Cervical Conization www.zohrehyousefi.com 1 Cone Biopsy is a surgical procedure with removal of a cone shaped portion of the cervix The extent of involvement of epithelium on the ectocervix has been clearly
Cervical Conization www.zohrehyousefi.com 1 Cone Biopsy is a surgical procedure with removal of a cone shaped portion of the cervix The extent of involvement of epithelium on the ectocervix has been clearly
Management Algorithms for Abnormal Cervical Cytology and Colposcopy
 Management Algorithms for Abnormal Cervical Cytology and Colposcopy Table of Contents Standard Colposcopic Definitions... 1 Guidelines for the Assessment of Abnormal Cervical Cytology... 2 Ia: Persistent
Management Algorithms for Abnormal Cervical Cytology and Colposcopy Table of Contents Standard Colposcopic Definitions... 1 Guidelines for the Assessment of Abnormal Cervical Cytology... 2 Ia: Persistent
Cryotherapy has No Place in Colposcopy Practice
 Cryotherapy has No Place in Colposcopy Practice No financial disclosures No conflicts of interest ? Precision? Personalized Medicine? Best Evidence Based Practice Prinicipals of Surgical Management CIN1
Cryotherapy has No Place in Colposcopy Practice No financial disclosures No conflicts of interest ? Precision? Personalized Medicine? Best Evidence Based Practice Prinicipals of Surgical Management CIN1
Molecular markers for diagnosis and prognosis in cervical neoplasia Eijsink, Jasper Johannes Hendrikus
 University of Groningen Molecular markers for diagnosis and prognosis in cervical neoplasia Eijsink, Jasper Johannes Hendrikus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Molecular markers for diagnosis and prognosis in cervical neoplasia Eijsink, Jasper Johannes Hendrikus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Cervical Screening Results Leading to Detection of Adenocarcinoma in Situ of the Uterine Cervix
 DOI:10.31557/APJCP.2019.20.2.377 Cervical Screening Results Leading to Detecting Cervical AIS RESEARCH ARTICLE Editorial Process: Submission:09/27/2018 Acceptance:01/18/2019 Cervical Screening Results
DOI:10.31557/APJCP.2019.20.2.377 Cervical Screening Results Leading to Detecting Cervical AIS RESEARCH ARTICLE Editorial Process: Submission:09/27/2018 Acceptance:01/18/2019 Cervical Screening Results
ASCCP 2013 Guidelines for Managing Abnormal Cervical Cancer Screening Tests
 ASCCP 2013 Guidelines for Managing Abnormal Cervical Cancer Screening Tests www.treatmentok.com Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Ann Arbor, Michigan Disclosures
ASCCP 2013 Guidelines for Managing Abnormal Cervical Cancer Screening Tests www.treatmentok.com Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Ann Arbor, Michigan Disclosures
Management of Abnormal Cervical Cytology and Histology
 Management of Abnormal Cervical Cytology and Histology Assoc. Prof. Gökhan Tulunay Etlik Zübeyde Hanım Women s Diseases Teaching & Research Hospital Gynecologic Oncology Clinic Universally accepted guideline
Management of Abnormal Cervical Cytology and Histology Assoc. Prof. Gökhan Tulunay Etlik Zübeyde Hanım Women s Diseases Teaching & Research Hospital Gynecologic Oncology Clinic Universally accepted guideline
Cervical Screening for Dysplasia and Cancer in Patients with HIV
 Cervical Screening for Dysplasia and Cancer in Patients with HIV Adult Clinical Guideline from the New York State Department of Health AIDS Institute w w w.hivg uidelines.org Purpose of the Guideline Increase
Cervical Screening for Dysplasia and Cancer in Patients with HIV Adult Clinical Guideline from the New York State Department of Health AIDS Institute w w w.hivg uidelines.org Purpose of the Guideline Increase
Updated ASCCP Consensus Guidelines For Managing Diagnosed Cervical Cancer Precursors Michael A. Gold, M.D.
 Updated ASCCP Consensus Guidelines For Managing Diagnosed Cervical Cancer Precursors Michael A. Gold, M.D. 27 May, 2014 London, England Faculty Disclosure X No, nothing to disclose Yes, please specify
Updated ASCCP Consensus Guidelines For Managing Diagnosed Cervical Cancer Precursors Michael A. Gold, M.D. 27 May, 2014 London, England Faculty Disclosure X No, nothing to disclose Yes, please specify
Managament of Abnormal Cervical Cytology and Histology
 Managament of Abnormal Cervical Cytology and Histology Ali Ayhan, M.D Başkent University Faculty of Medicine Department of Gynecology and Obstetrics Division of Gynecologic Oncology Abnormal Cytologic
Managament of Abnormal Cervical Cytology and Histology Ali Ayhan, M.D Başkent University Faculty of Medicine Department of Gynecology and Obstetrics Division of Gynecologic Oncology Abnormal Cytologic
Woo Dae Kang, Ho Sun Choi, Seok Mo Kim
 Is vaccination with quadrivalent HPV vaccine after Loop Electrosurgical Excision Procedure effective in preventing recurrence in patients with High-grade Cervical Intraepithelial Neoplasia (CIN2-3)? Chonnam
Is vaccination with quadrivalent HPV vaccine after Loop Electrosurgical Excision Procedure effective in preventing recurrence in patients with High-grade Cervical Intraepithelial Neoplasia (CIN2-3)? Chonnam
BRITISH COLUMBIA S CERVICAL CANCER SCREENING PROGRAM
 BRITISH COLUMBIA S CERVICAL CANCER SCREENING PROGRAM DATE: NOVEMBER 19, 2016 PRESENTER: DR. DIRK VAN NIEKERK 1 Conflict of Interest Disclosure Nothing to disclose 2 ..in the beginning of the malady it
BRITISH COLUMBIA S CERVICAL CANCER SCREENING PROGRAM DATE: NOVEMBER 19, 2016 PRESENTER: DR. DIRK VAN NIEKERK 1 Conflict of Interest Disclosure Nothing to disclose 2 ..in the beginning of the malady it
I have no financial interests in any product I will discuss today.
 Cervical Cancer Screening Update and Implications for Annual Exams George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics
Cervical Cancer Screening Update and Implications for Annual Exams George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics
SOGC / SCC Clinical Practice Guideline
 SOGC / SCC Clinical Practice Guideline Colposcopic Management of Abnormal Cervical Cancer Screening and Histology These Clinical Practice Guidelines have been prepared and approved by the Executive and
SOGC / SCC Clinical Practice Guideline Colposcopic Management of Abnormal Cervical Cancer Screening and Histology These Clinical Practice Guidelines have been prepared and approved by the Executive and
Eradicating Mortality from Cervical Cancer
 Eradicating Mortality from Cervical Cancer Michelle Berlin, MD, MPH Vice Chair, Obstetrics & Gynecology Associate Director, Center for Women s Health June 2, 2009 Overview Prevention Human Papilloma Virus
Eradicating Mortality from Cervical Cancer Michelle Berlin, MD, MPH Vice Chair, Obstetrics & Gynecology Associate Director, Center for Women s Health June 2, 2009 Overview Prevention Human Papilloma Virus
Gynecological Oncology Unit, Centro di Riferimento Oncologico National Cancer Institute, Aviano, Italy 2
 European Review for Medical and Pharmacological Sciences 2016; 20: 818-824 High-grade vaginal intraepithelial neoplasia and risk of progression to vaginal cancer: a multicentre study of the Italian Society
European Review for Medical and Pharmacological Sciences 2016; 20: 818-824 High-grade vaginal intraepithelial neoplasia and risk of progression to vaginal cancer: a multicentre study of the Italian Society
HPV and Cervical Cancer, Screening and Prevention. John Ragsdale, MD July 12, 2018 CME Lecture Series
 HPV and Cervical Cancer, Screening and Prevention John Ragsdale, MD July 12, 2018 CME Lecture Series We have come a long Way Prevalence HPV in Young Adults in U.S HPV genotypes 55-60% of All cancers 20%
HPV and Cervical Cancer, Screening and Prevention John Ragsdale, MD July 12, 2018 CME Lecture Series We have come a long Way Prevalence HPV in Young Adults in U.S HPV genotypes 55-60% of All cancers 20%
CERVICAL INTRAEPITHELIAL NEOPLASIA (CIN)
 CERVICAL INTRAEPITHELIAL NEOPLASIA (CIN) The cervix constitutes the lower third of the uterus. It is in two parts, the endocervix and the ectocervix. Ectocervix is covered with squamous epithelium. Endocervix
CERVICAL INTRAEPITHELIAL NEOPLASIA (CIN) The cervix constitutes the lower third of the uterus. It is in two parts, the endocervix and the ectocervix. Ectocervix is covered with squamous epithelium. Endocervix
Management that provides continuity of care for women
 Management that provides continuity of care for women If women are diagnosed with reproductive tract infection, prompt treatment should be instituted according to the WHO guidelines. Though it may be preferred
Management that provides continuity of care for women If women are diagnosed with reproductive tract infection, prompt treatment should be instituted according to the WHO guidelines. Though it may be preferred
Cervical Dysplasia and HPV
 Cervical Dysplasia and HPV J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse HPV Double stranded DNA virus The HPV infect epithelial cells of the skin and mucous membranes Highest risk
Cervical Dysplasia and HPV J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse HPV Double stranded DNA virus The HPV infect epithelial cells of the skin and mucous membranes Highest risk
Colposcopy. Attila L Major, MD, PhD
 Colposcopy Attila L Major, MD, PhD Histology Colposcopy Cytology It has been estimated that annual Pap smear testing reduces a woman s chance of dying of cervical cancer from 4 in 1000 to about 5 in 10,000
Colposcopy Attila L Major, MD, PhD Histology Colposcopy Cytology It has been estimated that annual Pap smear testing reduces a woman s chance of dying of cervical cancer from 4 in 1000 to about 5 in 10,000
Clinical outcomes after conservative management of CIN1/2, CIN2, and CIN2/3 in women ages years
 Clinical outcomes after conservative management of CIN1/2, CIN2, and CIN2/3 in women ages 21-39 years Michelle I. Silver, PhD, ScM Cancer Prevention Fellow National Cancer Institute Division of Cancer
Clinical outcomes after conservative management of CIN1/2, CIN2, and CIN2/3 in women ages 21-39 years Michelle I. Silver, PhD, ScM Cancer Prevention Fellow National Cancer Institute Division of Cancer
BC Cancer Cervix Screening 2015 Program Results. February 2018
 BC Cancer Cervix Screening 2015 Program Results BC Cancer Cervix Screening 2015 Program Results 2 Table of Contents BC Cancer Cervix Screening 2015 Program Results... 1 Table of Contents... 2 Program Overview...
BC Cancer Cervix Screening 2015 Program Results BC Cancer Cervix Screening 2015 Program Results 2 Table of Contents BC Cancer Cervix Screening 2015 Program Results... 1 Table of Contents... 2 Program Overview...
Dysplasia: layer of the cervical CIN. Intraepithelial Neoplasia. p16 immunostaining. 1, Cervical. Higher-risk, requires CIN.
 CLINICAL PRACTICE GUIDELINE Guideline Number: DHMP_DHMC_PG1015 Guideline Subject: Routine Cervical Cancer Screening Effective Date: 9/2018 Revision Date: 9/2019 Pages: 2 of 2 Quality Management Committee
CLINICAL PRACTICE GUIDELINE Guideline Number: DHMP_DHMC_PG1015 Guideline Subject: Routine Cervical Cancer Screening Effective Date: 9/2018 Revision Date: 9/2019 Pages: 2 of 2 Quality Management Committee
Study Number: Title: Rationale: Phase: Study Period Study Design: Centres: Indication Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Samuel B. Wolf, D.O., F.A.C.O.G. Emerald Coast Obstetrics and Gynecology Panama City Florida
 Making sense of the new Pap smear screening guidelines. Samuel B. Wolf, D.O., F.A.C.O.G. Emerald Coast Obstetrics and Gynecology Panama City Florida Case 17 year old G1P0010 with first sexual encounter
Making sense of the new Pap smear screening guidelines. Samuel B. Wolf, D.O., F.A.C.O.G. Emerald Coast Obstetrics and Gynecology Panama City Florida Case 17 year old G1P0010 with first sexual encounter
Objectives. I have no financial interests in any product I will discuss today. Cervical Cancer Screening Guidelines: Updates and Controversies
 Cervical Cancer Screening Guidelines: Updates and Controversies I have no financial interests in any product I will discuss today. Jody Steinauer, MD, MAS University of California, San Francisco Objectives
Cervical Cancer Screening Guidelines: Updates and Controversies I have no financial interests in any product I will discuss today. Jody Steinauer, MD, MAS University of California, San Francisco Objectives
Vasile Goldiş Western University of Arad, Faculty of Medicine, Obstetrics- Gynecology Department, Romania b
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Cervical Intraepithelial Neoplasia in the Dr. Salvator Vuia Clinical Obstetrics and Gynecology Hospital - Arad During the 2000-2009 Period Voicu
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Cervical Intraepithelial Neoplasia in the Dr. Salvator Vuia Clinical Obstetrics and Gynecology Hospital - Arad During the 2000-2009 Period Voicu
I have no financial interests to disclose.
 Workshop: Case Management of Abnormal Pap Smears and Colposcopies Rebecca Jackson, MD Professor Obstetrics, Gynecology & Reproductive Sciences and Epidemiology & Biostatistics I have no financial interests
Workshop: Case Management of Abnormal Pap Smears and Colposcopies Rebecca Jackson, MD Professor Obstetrics, Gynecology & Reproductive Sciences and Epidemiology & Biostatistics I have no financial interests
Case Based Problems. Recommended Guidelines. Workshop: Case Management of Abnormal Pap Smears and Colposcopies. Disclosure
 Disclosure Workshop: Case Management of Abnormal Pap Smears and Colposcopies Rebecca Jackson, MD Associate Professor Obstetrics, Gynecology & Reproductive Sciences and Epidemiology & Biostatistics This
Disclosure Workshop: Case Management of Abnormal Pap Smears and Colposcopies Rebecca Jackson, MD Associate Professor Obstetrics, Gynecology & Reproductive Sciences and Epidemiology & Biostatistics This
Adverse Reproductive Outcomes After CIN Treatment. Similar results from other publications
 Adverse Reproductive Outcomes After CIN Treatment Similar results from other publications Maria Kyrgiou Senior Lecturer Consultant Gynaecologic Oncology Queen Charlotte s & Chelsea Hammersmith Hospital
Adverse Reproductive Outcomes After CIN Treatment Similar results from other publications Maria Kyrgiou Senior Lecturer Consultant Gynaecologic Oncology Queen Charlotte s & Chelsea Hammersmith Hospital
POST-CONIZATION FOLLOW-UP OF PATIENTS WITH HIGH GRADE SQUAMOUS INTRAEPITHELIAL LESION TREATED BY LEEP PROCEDURE: A LITERATURE REVIEW
 POST-CONIZATION FOLLOW-UP OF PATIENTS WITH HIGH GRADE SQUAMOUS INTRAEPITHELIAL LESION TREATED BY LEEP PROCEDURE: A LITERATURE REVIEW Boureima Ali Nafissatou and Dong zhao * Department of Gynecology, Shanghai
POST-CONIZATION FOLLOW-UP OF PATIENTS WITH HIGH GRADE SQUAMOUS INTRAEPITHELIAL LESION TREATED BY LEEP PROCEDURE: A LITERATURE REVIEW Boureima Ali Nafissatou and Dong zhao * Department of Gynecology, Shanghai
Although rare, a significant increase in incidence
 Original Research Concurrent Anal Human Papillomavirus and Abnormal Anal Cytology in Women With Known Cervical Dysplasia Jacqueline Lammé, MD, Tina Pattaratornkosohn, MD, Joselyn Mercado-Abadie, MD, Addie
Original Research Concurrent Anal Human Papillomavirus and Abnormal Anal Cytology in Women With Known Cervical Dysplasia Jacqueline Lammé, MD, Tina Pattaratornkosohn, MD, Joselyn Mercado-Abadie, MD, Addie
Cytology/Biopsy/Leep Gynecologic Correlation: Practical Considerations and Approaches.
 Cytology/Biopsy/Leep Gynecologic Correlation: Practical Considerations and Approaches. Fadi W. Abdul-Karim MD MEd. Professor of Pathology. Vice chair for education. Robert Tomsich Pathology and Lab Med
Cytology/Biopsy/Leep Gynecologic Correlation: Practical Considerations and Approaches. Fadi W. Abdul-Karim MD MEd. Professor of Pathology. Vice chair for education. Robert Tomsich Pathology and Lab Med
Acceptable predictive accuracy of histopathology results by colposcopy done by Gynecology residents using Reid index
 DOI 10.1007/s00404-012-2569-y GYNECOLOGIC ONCOLOGY Acceptable predictive accuracy of histopathology results by colposcopy done by Gynecology residents using Reid index Hadi Shojaei Fariba Yarandi Leila
DOI 10.1007/s00404-012-2569-y GYNECOLOGIC ONCOLOGY Acceptable predictive accuracy of histopathology results by colposcopy done by Gynecology residents using Reid index Hadi Shojaei Fariba Yarandi Leila
EFC and European Standards for Colposcopic Evaluation
 EFC and European Standards for Colposcopic Evaluation Cagatay Taskiran, MD. Koc University School of Medicine, and VKF American Hospital Department of Obstetrics and Gynecology Division of Gynecologic
EFC and European Standards for Colposcopic Evaluation Cagatay Taskiran, MD. Koc University School of Medicine, and VKF American Hospital Department of Obstetrics and Gynecology Division of Gynecologic
Cervical Precancer: Evaluation and Management
 TAJ June 2002; Volume 15 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Review fam Cervical Precancer: Evaluation and Management SM Khodeza Nahar Begum 1 Abstract Carcinoma of
TAJ June 2002; Volume 15 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Review fam Cervical Precancer: Evaluation and Management SM Khodeza Nahar Begum 1 Abstract Carcinoma of
I have no financial interests in any product I will discuss today.
 Cervical Cancer Prevention: 2012 and Beyond George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics University of California,
Cervical Cancer Prevention: 2012 and Beyond George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics University of California,
GLANDULAR LESIONS PITFALLS IN MANAGEMENT. Dr Li Wai Hon HKSCCP The 15 th Anniversary Symposium 10 December 2016
 GLANDULAR LESIONS PITFALLS IN MANAGEMENT Dr Li Wai Hon HKSCCP The 15 th Anniversary Symposium 10 December 2016 Introduction Cervical glandular lesions are much less common than squamous lesion Incidence
GLANDULAR LESIONS PITFALLS IN MANAGEMENT Dr Li Wai Hon HKSCCP The 15 th Anniversary Symposium 10 December 2016 Introduction Cervical glandular lesions are much less common than squamous lesion Incidence
Human Papillomavirus
 Human Papillomavirus Dawn Palaszewski, MD Assistant Professor of Obstetrics and Gynecology University of February 18, 2018 9:40 am Dawn Palaszewski, MD Assistant Professor Department of Obstetrics and
Human Papillomavirus Dawn Palaszewski, MD Assistant Professor of Obstetrics and Gynecology University of February 18, 2018 9:40 am Dawn Palaszewski, MD Assistant Professor Department of Obstetrics and
Cervical Cancer Screening Update. Melissa Hartman, DO Women s Health
 Cervical Cancer Screening Update Melissa Hartman, DO Women s Health Previous Cervical Cancer Screening Organization Recommendation ACS (2011) ACP (2008) NCI (2003) Age 21 or 3 years after first intercourse
Cervical Cancer Screening Update Melissa Hartman, DO Women s Health Previous Cervical Cancer Screening Organization Recommendation ACS (2011) ACP (2008) NCI (2003) Age 21 or 3 years after first intercourse
Chapter 10: Pap Test Results
 Chapter 10: Pap Test Results On completion of this section, the learner will be able to: 1. Identify how Pap test results are interpreted and the reasons for normal and abnormal results. 2. Describe the
Chapter 10: Pap Test Results On completion of this section, the learner will be able to: 1. Identify how Pap test results are interpreted and the reasons for normal and abnormal results. 2. Describe the
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics Treatment of Cervical Precancerous Lesions using Thermocoagulation(Cold Coagulation) and Cryotherapy General Principles All high grade CIN should be
International Federation of Gynecology and Obstetrics Treatment of Cervical Precancerous Lesions using Thermocoagulation(Cold Coagulation) and Cryotherapy General Principles All high grade CIN should be
I have no financial interests in any product I will discuss today.
 Cervical Cancer Screening Update and Implications for Annual Exams George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics
Cervical Cancer Screening Update and Implications for Annual Exams George F. Sawaya, MD Professor Department of Obstetrics, Gynecology and Reproductive Sciences Department of Epidemiology and Biostatistics
Expression of E6/E7 HPV-DNA, HPV-mRNA and colposcopic features in management of CIN2/3 during pregnancy
 European Review for Medical and Pharmacological Sciences Expression of E6/E7 HPV-DNA, HPV-mRNA and colposcopic features in management of CIN2/3 during pregnancy A. FREGA 1, A. VERRONE 1, F. MANZARA 1,
European Review for Medical and Pharmacological Sciences Expression of E6/E7 HPV-DNA, HPV-mRNA and colposcopic features in management of CIN2/3 during pregnancy A. FREGA 1, A. VERRONE 1, F. MANZARA 1,
Cervical cancer screening in vaccinated population
 Cervical cancer screening in vaccinated population Cytology and molecular testing Prof. Dr. Fuat Demirkıran I.U Cerrahpaşa School of Medicine. Department of OB&GYN Division Of Gynocol Oncol Izmir, November
Cervical cancer screening in vaccinated population Cytology and molecular testing Prof. Dr. Fuat Demirkıran I.U Cerrahpaşa School of Medicine. Department of OB&GYN Division Of Gynocol Oncol Izmir, November
HKCOG GUIDELINES NUMBER 3 (revised November 2002) published by The Hong Kong College of Obstetricians and Gynaecologists
 HKCOG Guidelines Guidelines on the Management of An Abnormal Cervical Smear Number 3 revised November 2002 published by The Hong Kong College of Obstetricians and Gynaecologists A Foundation College of
HKCOG Guidelines Guidelines on the Management of An Abnormal Cervical Smear Number 3 revised November 2002 published by The Hong Kong College of Obstetricians and Gynaecologists A Foundation College of
The LAST Guidelines in Clinical Practice. Implementing Recommendations for p16 Use
 AJCP / Original Article The LAST Guidelines in Clinical Practice Implementing Recommendations for p16 Use Lani K. Clinton, MD, PhD, 1,2 Kyle Miyazaki, 1 Asia Ayabe, 1 James Davis, PhD, 2 Pamela Tauchi-Nishi,
AJCP / Original Article The LAST Guidelines in Clinical Practice Implementing Recommendations for p16 Use Lani K. Clinton, MD, PhD, 1,2 Kyle Miyazaki, 1 Asia Ayabe, 1 James Davis, PhD, 2 Pamela Tauchi-Nishi,
Gynaecological surgery. Introduction. MJ Camargo, a FB Russomano, a MA Trist~ao, a G Huf, b W Prendiville c
 DOI: 10.1111/1471-0528.13200 www.bjog.org Gynaecological surgery Large loop versus straight-wire excision of the transformation zone for treatment of cervical intraepithelial neoplasia: a randomised controlled
DOI: 10.1111/1471-0528.13200 www.bjog.org Gynaecological surgery Large loop versus straight-wire excision of the transformation zone for treatment of cervical intraepithelial neoplasia: a randomised controlled
News. Laboratory NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING TIMOTHY UPHOFF, PHD, DABMG, MLS (ASCP) CM
 Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Lessons From Cases of Screened Women Who Developed Cervical Carcinoma
 Lessons From Cases of Screened Women Who Developed Cervical Carcinoma R. Marshall Austin MD,PhD Magee-Womens Hospital of University of Pittsburgh Medical Center raustin@magee.edu Why Focus Study On Cases
Lessons From Cases of Screened Women Who Developed Cervical Carcinoma R. Marshall Austin MD,PhD Magee-Womens Hospital of University of Pittsburgh Medical Center raustin@magee.edu Why Focus Study On Cases
PAP SMEAR WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE
 Arch Iranian Med 2005; 8 (3): 192 196 Original Article PAP SMEAR WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE Fatemeh Ghaemmaghami MD *, Fereshteh Ensani MD**, Nadereh Behtash MD* Ebrahim
Arch Iranian Med 2005; 8 (3): 192 196 Original Article PAP SMEAR WITH ATYPICAL SQUAMOUS CELLS OF UNDETERMINED SIGNIFICANCE Fatemeh Ghaemmaghami MD *, Fereshteh Ensani MD**, Nadereh Behtash MD* Ebrahim
Medicine OPEN. Diagnostic Accuracy Study. 1. Introduction
 Diagnostic Accuracy Study Medicine OPEN Clinical analysis of cervical intraepithelial neoplasia with vaginal intraepithelial neoplasia Yue He, MD, Qun Zhao, PhD, Yu-Ning Geng, MD, Shu-Li Yang, MD, Cheng-Hong
Diagnostic Accuracy Study Medicine OPEN Clinical analysis of cervical intraepithelial neoplasia with vaginal intraepithelial neoplasia Yue He, MD, Qun Zhao, PhD, Yu-Ning Geng, MD, Shu-Li Yang, MD, Cheng-Hong
Clinical Practice Guidelines June 2013
 Clinical Practice Guidelines June 2013 General Principles: The Papanicolaou (Pap) smear is widely credited with reducing mortality from cervical cancer, and remains the single best method for the early
Clinical Practice Guidelines June 2013 General Principles: The Papanicolaou (Pap) smear is widely credited with reducing mortality from cervical cancer, and remains the single best method for the early
The routine use of ZedScan within one colposcopy service in England. MC Macdonald, R Lyon, JE Palmer, JA Tidy
 The routine use of ZedScan within one colposcopy service in England MC Macdonald, R Lyon, JE Palmer, JA Tidy Introduction Colposcopic impression alone has been shown to be subjective with variable rates
The routine use of ZedScan within one colposcopy service in England MC Macdonald, R Lyon, JE Palmer, JA Tidy Introduction Colposcopic impression alone has been shown to be subjective with variable rates
Long Term Outcomes of Laser Conization for High Grade Cervical Intraepithelial Neoplasia in Thai Women
 RESEARCH ARTICLE Long Term Outcomes of Laser Conization for High Grade Cervical Intraepithelial Neoplasia in Thai Women Weerasak Wongtiraporn, Somsak Laiwejpithaya*, Suthi Sangkarat, Mongkol Benjapibal,
RESEARCH ARTICLE Long Term Outcomes of Laser Conization for High Grade Cervical Intraepithelial Neoplasia in Thai Women Weerasak Wongtiraporn, Somsak Laiwejpithaya*, Suthi Sangkarat, Mongkol Benjapibal,
Cervical Cancer 4/27/2016
 Guidelines for Cervical Cancer Screening and Prevention Management of Abnormal Results Kathy A. King, MD Assistant Professor of OB/GYN Medical College of Wisconsin May 6, 2016 Cervical Cancer In US about
Guidelines for Cervical Cancer Screening and Prevention Management of Abnormal Results Kathy A. King, MD Assistant Professor of OB/GYN Medical College of Wisconsin May 6, 2016 Cervical Cancer In US about
Who Should Have a Pap Test and How Frequently? 1
 Chapter 3: Screening On completion of this section, the learner will be able to: 1. Describe who should have a Pap test and how frequently. 2. Identify who should be excluded from Pap tests and who should
Chapter 3: Screening On completion of this section, the learner will be able to: 1. Describe who should have a Pap test and how frequently. 2. Identify who should be excluded from Pap tests and who should
European Union survey on organization and quality control of cervical cancer screening and HPV vaccination programs
 European Union survey on organization and quality control of cervical cancer screening and HPV vaccination programs Introduction to the Survey The purpose of this project is to collect information regarding
European Union survey on organization and quality control of cervical cancer screening and HPV vaccination programs Introduction to the Survey The purpose of this project is to collect information regarding
A retrospective study of cytology, high-risk HPV and colposcopy results of vaginal intraepithelial neoplasia patients
 A retrospective study of cytology, high-risk HPV and colposcopy results of vaginal intraepithelial neoplasia patients Qing Cong* 1, 2,3, Yu Song* 1, 2,3, Qing Wang 1, 2,3, Hongwei Zhang 1, 2,3,Shujun Gao
A retrospective study of cytology, high-risk HPV and colposcopy results of vaginal intraepithelial neoplasia patients Qing Cong* 1, 2,3, Yu Song* 1, 2,3, Qing Wang 1, 2,3, Hongwei Zhang 1, 2,3,Shujun Gao
Your Colposcopy Visit
 Introduction Welcome to the colposcopy clinic. This booklet tells you about. The colposcopy examination.. Tests that are done in the colposcopy clinic.. What these tests look for Take a few minutes to
Introduction Welcome to the colposcopy clinic. This booklet tells you about. The colposcopy examination.. Tests that are done in the colposcopy clinic.. What these tests look for Take a few minutes to
Sydney Gynaecology Oncology Group, Sydney Cancer Centre, Royal Prince Alfred Hospital, Camperdown, New South Wales, Australia
 bs_bs_banner doi:10.1111/jog.12545 J. Obstet. Gynaecol. Res. Vol. 41, No. 3: 440 444, March 2015 Abnormal cervicovaginal cytology, unsatisfactory colposcopy and the use of vaginal estrogen cream: An observational
bs_bs_banner doi:10.1111/jog.12545 J. Obstet. Gynaecol. Res. Vol. 41, No. 3: 440 444, March 2015 Abnormal cervicovaginal cytology, unsatisfactory colposcopy and the use of vaginal estrogen cream: An observational
Cervicovaginal Cytology: Normal and Abnormal Cells and Adequacy of Specimens
 Cervicovaginal Cytology: Normal and Abnormal Cells and Adequacy of Specimens 3 Christine Bergeron, MD, PhD Introduction Carcinoma of the cervix is a slow growing cancer, which is preceded by precancerous
Cervicovaginal Cytology: Normal and Abnormal Cells and Adequacy of Specimens 3 Christine Bergeron, MD, PhD Introduction Carcinoma of the cervix is a slow growing cancer, which is preceded by precancerous
Chapter 8 Adenocarcinoma
 Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Human Papillomaviruses and Cancer: Questions and Answers. Key Points. 1. What are human papillomaviruses, and how are they transmitted?
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Human Papillomaviruses
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Human Papillomaviruses
Cervical Cancer Screening. David Quinlan December 2013
 Cervical Cancer Screening David Quinlan December 2013 Cervix Cervical Cancer Screening Modest variation provincially WHO and UK begin at 25 stop at 60 Finland begin at 30 stop at 60 Rationale for
Cervical Cancer Screening David Quinlan December 2013 Cervix Cervical Cancer Screening Modest variation provincially WHO and UK begin at 25 stop at 60 Finland begin at 30 stop at 60 Rationale for
HPV Genotyping: A New Dimension in Cervical Cancer Screening Tests
 HPV Genotyping: A New Dimension in Cervical Cancer Screening Tests Lee P. Shulman MD The Anna Ross Lapham Professor in Obstetrics and Gynecology and Chief, Division of Clinical Genetics Feinberg School
HPV Genotyping: A New Dimension in Cervical Cancer Screening Tests Lee P. Shulman MD The Anna Ross Lapham Professor in Obstetrics and Gynecology and Chief, Division of Clinical Genetics Feinberg School
cle Modern management of abnormal cervical smear Tint Tint Wai and Dilip Patil BJMP 2008:1(2) 18-22
 BJMP 2008:1(2) 18-22 Review Articl cle Modern management of abnormal cervical smear Tint Tint Wai and Dilip Patil Abbreviations BSCCP British Society of Colposcopy and Cervical Pathology CIN Cervical intraepithelial
BJMP 2008:1(2) 18-22 Review Articl cle Modern management of abnormal cervical smear Tint Tint Wai and Dilip Patil Abbreviations BSCCP British Society of Colposcopy and Cervical Pathology CIN Cervical intraepithelial
Associate Professor of Gyn. & Obs., Department of Gynecology and Obstetrics, Tehran University of Medical Sciences, Iran.
 Assessment of Visual Inspection with Acetic Acid (VIA) as a Screening Test for Cervical Neoplasia in Comparison with Cytologic Screening in Imam Khomeini Hospital F. Ghaemmaghami, MD Associate Professor
Assessment of Visual Inspection with Acetic Acid (VIA) as a Screening Test for Cervical Neoplasia in Comparison with Cytologic Screening in Imam Khomeini Hospital F. Ghaemmaghami, MD Associate Professor
Triage of Women with Minor Cervical Lesions: Data Suggesting a Test and Treat Approach for HPV E6/E7 mrna Testing
 Triage of Women with Minor Cervical Lesions: Data Suggesting a Test and Treat Approach for HPV E6/E7 mrna Testing Sveinung Wergeland Sørbye 1 *, Silje Fismen 1, Tore Gutteberg 2,3, Elin Synnøve Mortensen
Triage of Women with Minor Cervical Lesions: Data Suggesting a Test and Treat Approach for HPV E6/E7 mrna Testing Sveinung Wergeland Sørbye 1 *, Silje Fismen 1, Tore Gutteberg 2,3, Elin Synnøve Mortensen
Department of Obstetrics and Gynecology, Faculty of Medicine, The University of Tokyo, Tokyo, Japan
 bs_bs_banner doi:10.1111/jog.12196 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 554 560, February 2014 High-risk human papillomavirus correlates with recurrence after laser ablation for treatment of patients
bs_bs_banner doi:10.1111/jog.12196 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 554 560, February 2014 High-risk human papillomavirus correlates with recurrence after laser ablation for treatment of patients
Cervical Testing and Results Management. An Evidenced-Based Approach April 22nd, Debora Bear, MSN, MPH
 Cervical Testing and Results Management An Evidenced-Based Approach April 22nd, 2010 Debora Bear, MSN, MPH Assistant Medical Director for Planned Parenthood of New Mexico, Inc. Burden of cervical cancer
Cervical Testing and Results Management An Evidenced-Based Approach April 22nd, 2010 Debora Bear, MSN, MPH Assistant Medical Director for Planned Parenthood of New Mexico, Inc. Burden of cervical cancer
CPC on Cervical Pathology
 CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
Original Policy Date
 MP 2.04.03 Cervicography Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index Disclaimer
MP 2.04.03 Cervicography Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index Disclaimer
Reduction of the risk of cervical intraepithelial neoplasia in HIV-infected women treated with highly active antiretroviral therapy
 ACTA BIOMED 2007; 78: 36-40 Mattioli 1885 O R I G I N A L A R T I C L E Reduction of the risk of cervical intraepithelial neoplasia in HIV-infected women treated with highly active antiretroviral therapy
ACTA BIOMED 2007; 78: 36-40 Mattioli 1885 O R I G I N A L A R T I C L E Reduction of the risk of cervical intraepithelial neoplasia in HIV-infected women treated with highly active antiretroviral therapy
Becoming a colposcopist: Colposcope case studies
 Becoming a colposcopist: Colposcope case studies Seon-Kyung Lee, M.D. Department of Obstetrics and Gynecology College of Medicine, Kyung Hee University Value of Colposcopy Cytology is an effective screening
Becoming a colposcopist: Colposcope case studies Seon-Kyung Lee, M.D. Department of Obstetrics and Gynecology College of Medicine, Kyung Hee University Value of Colposcopy Cytology is an effective screening
THE NEW ZEALAND MEDICAL JOURNAL
 THE NEW ZEALAND MEDICAL JOURNAL Vol 8 No ISSN 75 876 Findings and outcome of teenage women referred for colposcopy at Christchurch Women s Hospital, New Zealand Peter Sykes, Dianne Harker, David Peddie
THE NEW ZEALAND MEDICAL JOURNAL Vol 8 No ISSN 75 876 Findings and outcome of teenage women referred for colposcopy at Christchurch Women s Hospital, New Zealand Peter Sykes, Dianne Harker, David Peddie
WELL WOMAN CLINIC-SCREENING PROGRAM FOR CERVICAL CARCINOMAS G. J. Vani Padmaja 1
 WELL WOMAN CLINIC-SCREENING PROGRAM FOR CERVICAL CARCINOMAS G. J. Vani Padmaja 1 HOW TO CITE THIS ARTICLE: G. J. Vani Padmaja. Well Woman Clinic-Screening Program for Cervical Carcinomas. Journal of Evolution
WELL WOMAN CLINIC-SCREENING PROGRAM FOR CERVICAL CARCINOMAS G. J. Vani Padmaja 1 HOW TO CITE THIS ARTICLE: G. J. Vani Padmaja. Well Woman Clinic-Screening Program for Cervical Carcinomas. Journal of Evolution
An Update on Cervical Cancer Screening Recommendations and on the DOH BCC Program
 An Update on Cervical Cancer Screening Recommendations and on the DOH BCC Program Susan Baum, MD, MPH NM Nurse Practitioner Council Annual Conference April 20, 2012 I have no commercial relationships related
An Update on Cervical Cancer Screening Recommendations and on the DOH BCC Program Susan Baum, MD, MPH NM Nurse Practitioner Council Annual Conference April 20, 2012 I have no commercial relationships related
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening
 Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
Northern Ireland cervical screening programme. Information for primary care and smear takers
 Northern Ireland cervical screening programme Information for primary care and smear takers From January 2011, the Northern Ireland cervical screening programme will no longer invite women aged under 25
Northern Ireland cervical screening programme Information for primary care and smear takers From January 2011, the Northern Ireland cervical screening programme will no longer invite women aged under 25
Cuid d Fheidhmeannacht na Seirbhíse Sláinte. Part of the Health Service Executive. CS/PR/PM-20 Rev 2 ISBN Programme Report 2014/2015
 Programme Report 2014/2015 Contents Summary points 2 Introduction to the statistics 2014/2015 3 Part 1 Cervical screening activity 3 Programme coverage 4 Laboratory turnaround time 7 Notification of results
Programme Report 2014/2015 Contents Summary points 2 Introduction to the statistics 2014/2015 3 Part 1 Cervical screening activity 3 Programme coverage 4 Laboratory turnaround time 7 Notification of results
No Disclosures. Updated Guidelines for Cervical Cancer Screening and Prevention Management of Abnormal Results. Objectives 5/9/2016
 Updated Guidelines for Cervical Cancer Screening and Prevention Management of Abnormal Results Kathy A. King, MD Assistant Professor of OB/GYN Medical Director, PPWI Medical College of Wisconsin May 6,
Updated Guidelines for Cervical Cancer Screening and Prevention Management of Abnormal Results Kathy A. King, MD Assistant Professor of OB/GYN Medical Director, PPWI Medical College of Wisconsin May 6,
What Causes Cervical Cancer? Symptoms of Cervical Cancer
 Cervical Health Awareness Month is a chance to raise awareness about how women can protect themselves from HPV (human papillomavirus) and cervical cancer. HPV is a very common infection that spreads through
Cervical Health Awareness Month is a chance to raise awareness about how women can protect themselves from HPV (human papillomavirus) and cervical cancer. HPV is a very common infection that spreads through
LESION AT PACIFIC MEDICAL COLLEGE, UDAIPUR. 1. Assistant Professor, Department of Pathology, Pacific Medical college and hospital, Udaipur.
 International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original Research Article HISTOPATHOLOGICAL AND CYTOLOGICAL ANALYSIS
International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original Research Article HISTOPATHOLOGICAL AND CYTOLOGICAL ANALYSIS
Pap Smears Pelvic Examinations Well Woman Examinations. When should you have them performed???
 Pap Smears Pelvic Examinations Well Woman Examinations. When should you have them performed??? Arlene Evans-DeBeverly, PA-C Copyright 2012 There are always ongoing changes in gynecology, including the
Pap Smears Pelvic Examinations Well Woman Examinations. When should you have them performed??? Arlene Evans-DeBeverly, PA-C Copyright 2012 There are always ongoing changes in gynecology, including the
Over-diagnoses in Cytopathology: Is histology the gold standard?
 Over-diagnoses in Cytopathology: Is histology the gold standard? Teresa M. Darragh, MD UCSF Departments of Pathology and Obstetrics, Gynecology & Reproductive Sciences Faculty Disclosures: Teresa M. Darragh,
Over-diagnoses in Cytopathology: Is histology the gold standard? Teresa M. Darragh, MD UCSF Departments of Pathology and Obstetrics, Gynecology & Reproductive Sciences Faculty Disclosures: Teresa M. Darragh,
