Pathology Consultation on Prostate-Specific Antigen Testing
|
|
|
- Barrie Day
- 5 years ago
- Views:
Transcription
1 Pathology Consultation on Prostate-Specific Antigen Testing Jaime H. Noguez, PhD, and Corinne R. Fantz, PhD From the Department of Pathology and Laboratory Medicine, Emory University School of Medicine, Atlanta, GA. Key Words: Prostate-specific antigen; Screening; Prostate cancer Am J Clin Pathol July 2014;142:7-15 DOI: /AJCPU6OOKL9JHEUR ABSTRACT Objectives: To provide clarity on the pros and cons of using prostate-specific antigen (PSA) as a screening tool for prostate cancer. Methods: Case scenarios and a literature review of recently published clinical trial data are presented to provide evidence of the controversy. Results: PSA is a sensitive biomarker for detecting diseases of the prostate, but it is limited in its ability to distinguish cancerous from noncancerous conditions or aggressive from indolent cancers and has resulted in a considerable amount of overdiagnosis and overtreatment. Conclusions: The analytical methodology for total PSA testing is both reliable and cost-effective, but patients should be encouraged to talk to their providers to understand the benefits and harms associated with this testing. Upon completion of this activity you will be able to: define the limitations of the serum prostate-specific antigen (PSA) test. describe new developments in PSA testing to improve specificity for prostate cancer. discuss the potential benefits and harms of population-based PSA screening. The ASCP is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians. The ASCP designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Credit per article. Physicians should claim only the credit commensurate with the extent of their participation in the activity. This activity qualifies as an American Board of Pathology Maintenance of Certification Part II Self-Assessment Module. The authors of this article and the planning committee members and staff have no relevant financial relationships with commercial interests to disclose. Questions appear on p 133. Exam is located at Case Scenarios Case 1 A 56-year-old man saw his primary care physician and relayed a history of lower urinary tract symptoms. A serum prostate-specific antigen (PSA) test was performed and his total PSA (tpsa) concentration was 12.8 ng/ml (12.8 mg/l; normal range <4.0 ng/ml [4 mg/l]). He was treated for presumed prostatitis with 30 days of oral antibiotics, at which time his serum PSA level had risen to 19.9 ng/ml (19.9 mg/l). He was diagnosed with benign prostatic hyperplasia (BPH) and prescribed an a-blocker. Physical examination at the time of presentation to the urologist revealed a small left varicocele and a large palpably abnormal-feeling prostate with firmness and nodularity. He was scheduled for urine cytology and a transrectal ultrasound-guided needle biopsy of the prostate. CME/SAM Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR 7
2 Noguez and Fantz / Prostate-Specific Antigen Testing Case 2 A 47-year-old man was screened for prostate cancer with a digital rectal examination (DRE) and a serum PSA test. His initial PSA concentration was 1.9 ng/ml (1.9 mg/l) and he continued to be screened annually. Over the course of 7 years, his PSA concentration gradually rose to 4.6 ng/ml (4.6 mg/l). The mildly elevated PSA level prompted several repeat measurements that year in 3-month intervals, which documented a steady rise to 5.5 ng/ml (5.5 mg/l) and then to 6.6 ng/ml (6.6 mg/l). He was scheduled for a transrectal ultrasound-guided needle biopsy of the prostate the following month at the age of 54 years. Questions 1. What is PSA? 2. What factors can increase serum levels of PSA? 3. What are the key characteristics of a population-based screening biomarker? 4. What are the risks and benefits of PSA-based screening for prostate cancer? 5. Why is screening for prostate cancer with a serum PSA test controversial? Background Prostate cancer is the second most commonly diagnosed cancer in American men, as well as the second leading cause of cancer death in the United States. 1 The American Cancer Society (ACS) estimated 238,590 new cases of prostate cancer for 2013 and projected that approximately 30,000 deaths will occur from prostate cancer. 1 The lifetime risk of a man developing prostate cancer is about 1 in 6, though the risk of dying of prostate cancer is significantly less. 1 Most prostate cancers are slow-growing and clinically insignificant, but others are aggressively metastatic and have an insidious course. Because of its widely variable clinical behavior, early detection through screening may be useful in reducing the incidence of metastatic prostate cancer and potentially save thousands of lives. However, when a biomarker lacks the specificity to discriminate between aggressive and indolent cancers, there is an inherent risk of overdiagnosis and overtreatment. PSA, also known as g-seminoprotein, is an androgenregulated serine protease secreted by the epithelial cells of the prostate gland. It is the most widely used tumor marker to date and remains the single most significant predictive factor for identifying men with increased risk of prostate cancer. 2,3 The active enzyme is formed by the sequential proteolytic cleavage of two inactive propeptides before entering the peripheral circulation Figure 1. The majority of PSA that enters the bloodstream is intact and quickly becomes bound to serum proteins, primarily to the protease inhibitors a 2 -macroglobulin Cell Figure 1 Prostate-specific antigen (PSA) formation in cells. ACT, a 1 -antichymotrypsin. (A2M) and a 1 -antichymotrypsin (ACT). 4,5 Free PSA (fpsa) and PSA bound to ACT, collectively referred to as tpsa, are the only immunoreactive forms of the protein and can be measured in blood using an immunoassay. 4-6 PSA bound to A2M is not measurable with immunoassay because all epitopes of PSA are masked due to encapsulation by A2M. 5 PSA is a sensitive biomarker for detecting pathologic conditions of the prostate, but its efficacy as a screening tool for prostate cancer has been challenged because of its lack of specificity. A low prevalence of prostate cancer in the general population, along with this lack of specificity, means that the predictive value of a positive serum PSA screening test is low. Therefore, a DRE is typically used in conjunction with a serum PSA test to screen for prostate cancer and to determine which patients will receive a prostate biopsy. This biomarker is also commonly used to monitor the treatment of men previously diagnosed with prostate cancer and to detect disease recurrence. Although the introduction and widespread use of serum PSA testing has revolutionized the diagnosis and management of prostate cancer, its use as a screening tool has recently become a topic of intense debate. History of PSA PreproPSA (inactive) ProPSA (inactive) PSA (active) Blood Free PSA PSA-ACT Total PSA PSA was discovered in the early 1970s and was initially described in the literature as a semen-specific protein that could be used as a marker for semen identification. 7 Shortly thereafter, a biochemically similar and immunologically identical antigen was isolated from both prostate tissue and human serum. 8,9 PSA was found in normal, benign, and malignant prostate tissue. Elevated serum levels were detected in men with BPH as well as in all stages of prostate cancer. In addition, serum levels of PSA were found to increase in proportion to the tumor burden, generating a considerable amount of interest in PSA as a potential marker for prostate cancer. 8 Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR
3 In 1986, the Food and Drug Administration (FDA) approved the use of the first commercial serum tpsa test, a chemiluminescent immunoassay using a monoclonal murine anti-psa antibody marketed as the Tandem PSA assay by Hybritech (San Diego, CA). The intended use was to monitor the progression of prostate cancer in men who had previously been diagnosed with the disease and to detect cancer recurrence after therapeutic interventions. Approximately 5 years after the Tandem PSA assay was introduced to the market, the age-adjusted absolute mortality rates for prostate cancer began to decline, which suggested that the PSA test was having a beneficial effect and was responsible for this reduction. 10 By the early 1990s, studies were under way to examine the clinical usefulness of serum PSA as a screening test for prostate cancer. 11 The results indicated that a serum PSA test used in conjunction with a DRE was superior for detecting prostate cancer compared with either test alone. 12 The FDA expanded the intended use of the Hybritech serum PSA test to include use as a screening tool in combination with a DRE in men older than 50 years or those with high risk. Based on the results of a large, multicenter trial, a PSA concentration of 4 ng/ml (4 mg/l) was selected as the threshold for performing prostate biopsies to confirm the presence of prostate cancer. 13 PSA screening resulted in a dramatic increase in the incidence of early-stage, organ-confined prostate cancers, and in turn, led to a rise in invasive treatments intended to cure aggressive localized tumors The ACS and the American Urological Association issued clinical guidelines supporting annual prostate cancer screening using both the serum PSA test and DRE. 17,18 However, a number of other professional societies including the National Cancer Institute, the American College of Physicians, and the US Preventive Services Task Force (USPSTF) did not find the data persuasive enough to recommend routine screening, citing a lack of conclusive evidence that PSA testing reduces disease-specific morbidity and mortality The incorporation of PSA screening recommendations into clinical guidelines in the absence of efficacy data from randomized trials ignited a 20-year debate. Amidst the controversy, a number of large manufacturers developed immunoassays to detect serum PSA on automated platforms, including Abbott Diagnostics, Beckman Coulter, Roche, Siemens, Tosoh, and Ortho Clinical Diagnostics. As the number of PSA immunoassays on the market multiplied, the need for harmonization became increasingly apparent. 22,23 Assay standards were developed to improve clinical interpretations and interchangeability of PSA results between laboratories and methodologies. Nearly every PSA assay on the market was calibrated with one of two standards: the traditional Hybritech standard used in the manual predecessor Tandem PSA assay or a more recently developed World Health Organization (WHO) standard. The concentrations of the purified PSA in the standards were measured using different methods, leading to a 23% difference in their concentrations. Ultimately, the results of assays calibrated with the Hybritech standard were found to be 10% to 25% higher than those calibrated with the more accurately determined WHO standard. 22,24 Differences in the clinical interpretation of PSA tests as a result of nonuniform assay calibration were first noted in 2003, but the impact had yet to be fully appreciated in the medical community. In recent years, the issue of metrologic traceability in the determination of PSA has received a considerable amount of interest. However, the conventional PSA threshold of 4 ng/ml (4 mg/l) continues to be a prostate biopsy decision criterion in several clinical guidelines despite being solely based on the Hybritech standard. Standardization efforts are still under way to increase interchangeability and minimize the misinterpretation of PSA results obtained with different assays and reference materials. Linking all PSA measurements to a common stable reference material will likely simplify an already challenging clinical decision. Diagnostic Dilemma Elevated serum PSA concentrations suggest the presence of prostate cancer, but increased concentrations are also found in benign conditions of the prostate such as BPH, urinary tract infections, and prostatitis Table 1. Furthermore, a normal PSA level cannot definitively rule out cancer. Although the Table 1 Benign Conditions That May Increase Serum PSA levels Noncancerous causes of elevated serum PSA Prostate disease Benign prostatic hyperplasia Prostatitis Prostate ischemia Clinical manipulations Digital rectal examination Prostate biopsy Transrectal ultrasound Indwelling urinary catheter Treatments Prostate surgery Radiation therapy Testosterone administration Luteinizing hormone/follicle-stimulating hormone administration (transient effect) Analytical interferences Heterophile antibodies Increased levels of kallikrein Antibody cross-reactivity Extra-prostate sources Parotid glands Periurethral glands Other Ejaculation Urine retention Riding a bicycle Urinary tract infections PSA, prostate-specific antigen. Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR 9
4 Noguez and Fantz / Prostate-Specific Antigen Testing risk of finding prostate cancer on biopsy increases with PSA levels higher than 4.0 ng/ml (4 mg/l), there is no PSA value at which assurance is guaranteed. In fact, one study showed that up to 15% of men with PSA levels lower than 4.0 ng/ml (4 mg/l) were found to have prostate cancer on biopsy. 25 The usefulness of PSA as a screening tool has been challenged primarily because of its poor specificity when serum PSA concentrations are only modestly elevated. PSA values between 4.0 and 10.0 ng/ml (4-10 mg/l) have often been referred to as the diagnostic gray-zone. When the serum PSA level is 10.0 ng/ml or higher, the specificity of the test for cancer is considerably higher than when the serum level is only modestly elevated ( ng/ml [4-10 mg/l]). 11,12 Because only 25% to 35% of men presenting with modest elevations in serum PSA levels are confirmed to have prostate cancer, a number of approaches have been taken to reduce the number of false positives. 12 New developments in prostate cancer testing have aided in discriminating early-stage cancer from noncancerous conditions but a great deal of focus has been placed on developing additional tests to distinguish aggressive from benign cancers. 26,27 Some of these tests are intended to be used in combination with the PSA test and others can be used independently. Improving PSA Specificity for Detecting Cancer As the limitations of PSA as a biomarker for prostate cancer screening became more apparent, a number of different strategies have been used to improve the performance characteristics of the PSA test Table 2 when the concentrations are in the diagnostic gray-zone, including PSA density, PSA velocity, percent-free PSA, prostate health index, and measurement of the different forms of PSA. 28,29 Although these new developments in PSA testing have been proven to increase the specificity of the PSA test for detecting cancer and reducing the high rate of false positives, it is important to note that they each have limitations of their own. Table 2 PSA Screening Test Characteristics at 4 ng/ml (4 mg/l) Cutoff for a Positive Test 28 Test Characteristic Sensitivity 21 Sensitivity for high grade cancer (ie, Gleason score 8) 51 Specificity 91 Positive predictive value 30 PSA, prostate-specific antigen. Percentage PSA Density Men who have larger prostates tend to have more prostate cells, which in turn, produce more PSA regardless of whether or not they have cancer. PSA levels can be normalized by measuring the prostate volume using transrectal ultrasonography then dividing the serum PSA concentration by the size of the prostate to calculate the PSA density. A high PSA density indicates that a relatively small volume of prostate tissue is making a considerable amount of PSA. Conversely, a low PSA density indicates that a large volume of prostate tissue is making relatively little PSA. There is evidence that a high PSA density indicates a higher risk of prostate cancer and, in general, men with both elevated tpsa and a high PSA density (>0.15 ng/ml [>0.15 mg/l]) should be monitored more closely for prostate cancer than those with low PSA density Although PSA density has been shown to increase the specificity of prostate cancer screening, evidence suggests that a 0.15 ng/ml (0.15 mg/l) cutoff for biopsy may be too high and may result in a large number of missed cancers. 33 PSA Velocity PSA velocity is the rate of increase in PSA concentrations over time. Enlargement of the prostate gland is a common part of aging, along with a corresponding slow increase in PSA levels. Studies have demonstrated that these levels tend to increase faster if a man has cancer and suggest that the more aggressive the cancer the steeper the rise The usefulness of PSA velocity is limited because it requires at least three serial measurements to reduce the background variability caused by short-term fluctuations in PSA. Sampling over longer intervals may decrease variation but may also prolong the screening process and increase anxiety. 37 In addition, the PSA velocity may be elevated if a man has multiple prostatic conditions that increase serum PSA values over time such as BPH, prostatitis, and cancer. fpsa:tpsa Ratio PSA circulates in the bloodstream either free or bound to serum proteins. The percent-free PSA is commonly used to help physicians decide how to further test for or treat prostate cancer. It is calculated by dividing the amount of fpsa (unbound) in the blood by the tpsa (bound + unbound). In general, benign conditions tend to increase the fpsa form, and cancerous conditions tend to increase the bound PSA-ACT (cpsa) form. 38,39 A percent-free PSA above 25% is considered normal, with an 8% probability of cancer; between 10% and 25% is considered intermediate, with a 16% to 28% probability of cancer; and below 10% is considered low, with a 56% probability of cancer. 40 When the tpsa is in the gray zone, the percent-free PSA can be used to decide whether to proceed with a prostate biopsy. It should be noted, however, that fpsa is not as stable as the 10 Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR
5 protein-bound form and requires strict specimen handling to reduce analytic variability. 41 Complexed PSA Men with prostate cancer tend to have more cpsa than those without. Measuring the proportion of cpsa has been particularly useful for risk stratification of men with tpsa levels in the range of 2 to 4 ng/ml (2-4 mg/l) because of the high incidence of prostate cancer in men without elevated tpsa values. 42 Multicenter studies have shown that cpsa outperforms the tpsa test for prostate cancer detection and can possibly replace it as the first-line screening test. 43,44 However, others have reported that cpsa alone is not helpful in reducing the rate of unnecessary biopsies. 45 Elevations in cpsa concentrations can be observed in patients with nonmalignant diseases and cpsa concentrations within the normal range can be observed in some men with confirmed prostate cancer. Because of such conflicting evidence, cpsa concentrations should not be interpreted as absolute evidence of the presence or absence of malignancy. Ratios of cpsa:tpsa and fpsa:tpsa have demonstrated similar areas under the curve at differentiating patients with BPH from those with prostate cancer when the tpsa concentration is between 2 and 10 ng/ ml (2-10 mg/l). 45 Therefore, the cpsa:tpsa ratio can be considered as an alternative to the fpsa:tpsa ratio for adding discriminatory power to the tpsa test. PSA Isoforms fpsa is composed of several different enzymatically inactive isoforms. Measuring these PSA isoforms may distinguish which men likely have prostate cancer and are candidates for a biopsy. In men with nonspecifically elevated tpsa concentrations because of BPH, the B-PSA isoform of fpsa is often increased. 46,47 In contrast, the pro-psa form and some of its truncated forms, particularly [-2]proPSA, appear to be preferentially elevated in the serum samples of men with prostate cancer Measurement of these PSA isoforms shows promise for lowering the rate of unnecessary biopsies but requires further analysis in larger multicenter studies. The Access Hybritech p2psa test is an FDA-approved assay for [-2]proPSA that is available on the Beckman Coulter Access Immunoassay system (Chaska, MN). An automated, two-site immunoassay for B-PSA has also been developed by Beckman Coulter for research use only. Prostate Health Index The Prostate Health Index (phi) is an FDA-approved test designed by Beckman Coulter that generates a composite score from the Access Hybritech tpsa, Access Hybritech fpsa, and the Access Hybritech p2psa tests. The test is available on the Beckman Coulter Access 2 and UniCel DxI immunoassay platforms and incorporates the results of the three individual tests into _ a single score using the formula: (p2psa/fpsa) tpsa. 52 Combining these three variables improves risk assessment for prostate cancer by providing clinicians with more information about the probability of prostate cancer in men 50 years and older with a nonsuspicious DRE result and a tpsa in the range of 2.0 to 10.0 ng/ml (2-10 mg/l). 52,53 A low phi result indicates a lower risk of prostate cancer, whereas an elevated phi indicates a higher risk and may suggest the need for a prostate biopsy. Although the phi has demonstrated superior clinical performance for the detection of prostate cancer in comparison to tpsa and percent-free PSA, it is yet to be clearly demonstrated whether this test can differentiate between aggressive cancers that need treatment and indolent tumors that can simply be monitored actively. 52 The Case for PSA-Based Screening Proponents of PSA-based screening argue that it enables the detection of more prostate cancers in the early stages so treatment can be initiated, thereby reducing the incidence of late-stage disease. Reducing the proportion of men presenting with high-risk, advanced disease saves lives, minimizes disease complications, and improves the quality of life. For men with an aggressive prostate cancer, the best chance for curing it is through early detection when it is localized to the prostate gland then treating it aggressively with surgery or radiation. The 5-year survival for men who have prostate cancer confined to the prostate gland (early stage) is nearly 100% and drops to 30% for men whose cancer has metastasized. 54 Although many early-stage cancers are not aggressive and may never cause a health problem, there is currently no way to discern aggressive from indolent cancers at detection. In addition, no existing tests are known to accurately predict which men with prostate cancer detected on PSA screening are most likely to benefit from aggressive treatment. Experts in favor of prostate cancer screening cite that the mortality rate of prostate cancer has declined by 40% since widespread implementation of PSA screening in the 1990s. 1 According to projection models, PSA screening has attributed to as much as 70% of the observed decline in mortality, which is most likely because of a stage shift. 10 The preliminary results of the large European Randomized Study of Screening for Prostate Cancer (ERSPC) trial found that through 11 years of follow-up men who underwent PSA testing had a 21% reduction in their chance of dying of prostate cancer compared with men who did not undergo PSA screening. 55,56 Similarly, the Göteborg trial observed a substantial benefit of PSA screening with a 44% reduction in cancer death when followed up after 14 years. 57 The results of a randomized, multicenter Scandinavian study found that even among low-risk men, prostatectomy offered a survival advantage Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR 11
6 Noguez and Fantz / Prostate-Specific Antigen Testing over watchful waiting. 58 Advocates of PSA-based screening contend that it has substantially reduced the incidence of metastatic prostate cancer. New evidence suggests that it saves thousands of lives and should be used despite the risk of overdiagnosis and overtreatment. 56 of serious surgical complications or death. Even the initial biopsy taken as a result of an elevated total serum PSA test can potentially cause pain, bleeding, and infection. 61 The Case Against PSA-Based Screening Although PSA screening may account for much of the observed reduction in prostate cancer mortality over the years, other factors such as changing treatment practices most certainly contributed to improving prostate cancer outcomes. Those against PSA-based screening acknowledge that it has saved many lives but contend that the absolute impact of the observed decline in prostate cancer mortality is overinterpreted for an individual man. Further, critics maintain that the well-documented problems associated with this kind of population screening are being overlooked. A number of recently published reports provide convincing evidence that PSAbased prostate cancer screening programs result in considerable overdiagnosis and overtreatment. The preliminary data from the large, randomized Prostate, Lung, Colon and Ovarian (PLCO) trial was published at the same time as the data from the ERSPC trial and highlighted the high rate of overdiagnosis associated with PSA-based prostate cancer screening programs. The PLCO trial found no significant reduction in prostate cancer related deaths after 13 years of follow-up; however, it is difficult to draw any conclusions because of the extremely high rate of PSA testing in the control arm before study entry. 59 The results of the Prostate Cancer Intervention Versus Observation Trial (PIVOT) found no benefit in prostate cancer specific mortality associated with surgery compared with watchful waiting for patients with low-risk disease, even though the benefits in those with higher-risk disease were substantial. 60 The data from this large, randomized trial were contrary to those found by the multicenter Scandinavian study showing a considerable benefit to surgery over watchful waiting in men with prostate cancer in general. Those who recommend against PSA-based screening state that the potential benefits of screening are not greater than the expected harms. This screening ultimately puts individuals at risk of potential treatment complications by detecting and unnecessarily treating many cases of asymptomatic, slow-growing prostate cancers that may not cause health problems during a man s lifetime. Because of the high degree of uncertainty about which cancers are life-threatening and need to be treated aggressively, almost all men diagnosed with prostate cancer detected with the PSA test get treatment with surgery, radiation, or hormone therapy. These treatments may result in lasting harms such as erectile dysfunction, urinary incontinence, bowel control issues, and even a small risk Conclusions In addition to having sufficient analytic performance characteristics, a valuable screening biomarker should be cost effective and influence disease outcomes. Ideally, it should be able to detect disease at an earlier stage and guide treatment decisions that lead to a better outcome. 62 Although PSA has become the most widely used biomarker for cancer screening over the past 20 years, there has been a lack of evidence supporting the ability of the serum PSA test to reduce metastasis and cancer-specific mortality as a population-based screening tool. PSA-based prostate cancer screening was a controversial issue from the onset because decisions had been made and incorporated into clinical guidelines by some professional associations in the absence of efficacy data from randomized trials or even consensus within the field. Although PSA screening promised earlier detection and treatment of prostate cancer, evidence-based discussions of the benefits and harms of PSA-based screening were not possible until recently. In 2009, the initial results of two high-powered, prospective randomized clinical trials for PSA-based screening for prostate cancer were published. It was anticipated that the data would put an end to the 20-year debate. Unfortunately the contrasting results of these studies created more confusion than clarity. In the ERSPC trial, PSA-based screening was associated with a 21% relative reduction in prostate cancer specific mortality after a median follow-up time of 11 years, albeit at the cost of a considerable amount of overdiagnosis. 55,56 Conversely, the PLCO trial showed a higher incidence of prostate cancer in the screening group than the control group but no significant reduction in prostate cancer related deaths after 13 years of follow-up. 59 The designs of both studies were found to be flawed and the contamination rates were found to be 25% for the ERSPC trial and 77% in the PLCO trial for previous PSA testing in the control group before study entry. 55,56,59,63 Even though these studies have several limitations, they have provided some of the strongest evidence to date regarding the efficacy of PSA-based screening in reducing cancer-related mortality. Several professional societies have updated their recommendations for PSA-based prostate cancer screening to encourage shared decision making between the physician and patient. Recommendations focus on the necessity of providing appropriate patient education on the benefits and limitations of screening, so that patients will be equipped to make informed decisions regarding their health. The final recommendation of the USPSTF regarding the use of PSA for prostate cancer 12 Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR
7 screening is perhaps the most controversial aspect of the entire PSA debate. In 2012, the USPSTF amended its 2008 recommendation against screening for prostate cancer in men 75 years or older. The new statement now recommends against routine PSA screening for cancer in men of all ages who do not have symptoms highly suspicious for prostate cancer. The task force concluded that there is convincing evidence that the potential benefits of PSA-based screening are not greater than the expected harms. It has subsequently been criticized for drawing such definitive conclusions on the basis of incomplete evidence with notable limitations. Many believe that the USPSTF has a narrow view of the value of PSA, raising concerns about the potential consequences of taking a one size fits all approach by recommending against PSA screening altogether. 64 Until the final results of these trials are published, it is important that the benefits of PSA-based screening not be overinterpreted or the risks associated with overtreatment discounted. Using a shared decision-making strategy between the physician and patient is the most practical approach moving forward, given the lack of definitive screening outcome data and the considerable trade-offs of PSA-based screening. It is also of utmost importance for physicians and their patients to understand that the debate surrounding PSA testing is not about the analytic performance of the test, but rather the challenging clinical decisions made based on the test results. Case Summaries Case 1 The urine cytology findings were positive for PSA malignant cells consistent with prostate cancer and the needle biopsy showed Gleason = 7 prostatic adenocarcinoma in 12/12 cores with extensive perineural invasion. The prostatic volume was estimated at 31.2 ml on transrectal ultrasonography. Bone scan was negative for metastatic disease but computed tomography (CT) of the abdomen and pelvis revealed several rounded liver lesions and several subcentimeter lung nodules, both organs suspicious for metastasis. At this time he was started on hormonal treatment for prostate cancer including antiandrogens and luteinizing hormonereleasing hormone agonists. The serum PSA fell from 40.8 ng/ml (40.8 mg/l) to 4.9 ng/ml (4.9 mg/l) with androgen deprivation. Biopsy of the liver revealed metastatic adenocarcinoma consistent with a prostatic primary lesion. A repeat CT scan demonstrated a decrease in size of all metastatic lesions while taking androgen deprivation therapy, thus confirming the prostatic origin of these metastases. However, the cancer became androgen independent and within 3 months of the PSA nadir it had risen to ng/ml (102.2 mg/l). The patient began combination chemotherapy and demonstrated a positive response with a second PSA nadir of 35.9 ng/ml (35.9 mg/l). While the patient completed multiple additional courses of chemotherapy, his disease continued to progress, with rising PSA levels and new metastasis evident on imaging. He died at the age of 58 years just under 2 years after the initial diagnosis of prostate cancer, with a final PSA level of 2,095 ng/ml (2.095 mg/l) obtained 2 weeks before his death. Case 2 The patient underwent a transrectal ultrasound-guided needle biopsy of the prostate at the age of 54 years, which revealed Gleason = 7 adenocarcinoma in 30% of the right-sided cores and Gleason = 6 disease in 5% of the left-sided cores. The prostatic volume was estimated at 34.0 ml on transrectal ultrasonography. At this time he underwent a bone scan that was negative for metastasis. The patient was offered radical prostatectomy, radiation therapy, and watchful waiting as treatment options. He chose watchful waiting because he did not have any symptoms related to the prostate. The patient ultimately decided to self-medicate with herbal remedies for his cancer. Over the 11 years since diagnosis, the serum PSA level continued to rise to the most recent determination of 76.1 ng/ml (76.1 mg/l) without additional treatment. It can be difficult for physicians to decide how to treat individual patients because there is currently no way of determining the aggressiveness of early-stage cancers or to predict which men will respond well to treatment. The heterogeneous presentation of prostate cancer renders both diagnosis and prognosis a challenge. Risk stratification is complex though tools exist such as the serum PSA test, cancer staging by Gleason score, and multifactorial nomograms to help guide crucial decisions regarding treatment. Despite these advances, the ability to accurately predict the outcome for each patient remains severely limited as demonstrated by these two case scenarios. Although an elevated serum PSA test assisted the clinician in making the diagnosis of prostate cancer in both of these cases, it provided little information regarding the aggressiveness of the disease or the how these men would respond to treatment. Address reprint requests to Dr Noguez: Dept of Pathology and Laboratory Medicine, Emory University School of Medicine, 1364 Clifton Rd, Room G163, Atlanta, GA 30322; jaime.noguez@ emory.edu. Acknowledgment: We thank John A. Petros, MD, Department of Urology, Emory University School of Medicine, for providing case histories. References 1. Siegel R, Naishadham D, Jemal A. Cancer statistics, CA Cancer J Clin. 2013;63: Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR 13
8 Noguez and Fantz / Prostate-Specific Antigen Testing 2. Fleshner N, Lawrentschuk N. Risk of developing prostate cancer in the future: overview of prognostic biomarkers. Urology. 2009;73(suppl):S21-S Schroder F, Roobol M, Andriole G, et al. Defining increased future risk for prostate cancer: evidence from a population based screening cohort. J Urol. 2009;181: Lilja H, Christensson A, Dahlen U, et al. Prostate-specific antigen in serum occurs predominantly in complex with alpha 1-antichymotrypsin. Clin Chem. 1991;37: Stenman UH, Leinonen J, Alfthan H, et al. A complex between prostate-specific antigen and alpha 1-antichymotrypsin is the major form of prostate-specific antigen in serum of patients with prostatic cancer: assay of the complex improves clinical sensitivity for cancer. Cancer Res. 1991;51: Zhou AM, Tewari PC, Bluestein BI, et al. Multiple forms of prostate-specific antigen in serum: differences in immunorecognition by monoclonal and polyclonal assays. Clin Chem. 1993;39: Sensabaugh GF. Isolation and characterization of a semenspecific protein from human seminal plasma: a potential new marker for semen identification. J Forensic Sci. 1978;23: Wang MC, Valenzuela LA, Murphy GP, et al. Purification of a human prostate specific antigen. Invest Urol. 1979;17: Papsidero LD, Wang MC, Valenzuela LA, et al. A prostate antigen in sera of prostatic cancer patients. Cancer Res. 1980;40: Etzioni R, Tsodikov A, Mariotto A, et al. Quantifying the role of PSA screening in the US prostate cancer mortality decline. Cancer Causes Control. 2008;19: Catalona WJ, Smith DS, Ratliff TL, et al. Measurement of prostate-specific antigen in serum as a screening test for prostate cancer. N Engl J Med. 1991;324: Catalona WJ, Richie JP, Ahmann FR, et al. Comparison of digital rectal examination and serum prostate specific antigen in the early detection of prostate cancer: results of a multicenter clinical trial of 6,630 men. J Urol. 1994;151: Catalona WJ, Hudson MA, Scardino PT, et al. Selection of optimal prostate specific antigen cutoffs for early detection of prostate cancer: receiver operating characteristic curves. J Urol. 1994;152: Lu-Yao GL, Friedman M, Yao SL. Use of radical prostatectomy among Medicare beneficiaries before and after the introduction of prostate specific antigen testing. J Urol. 1997;157: Lu-Yao GL, Greenberg ER. Changes in prostate cancer incidence and treatment in USA. Lancet. 1994;343: Potosky AL, Miller BA, Albertsen PC, et al. The role of increasing detection in the rising incidence of prostate cancer. JAMA. 1995;273: Mettlin C, Jones G, Averette H, et al. Defining and updating the American Cancer Society guidelines for the cancerrelated checkup: prostate and endometrial cancers. CA Cancer J Clin. 1993;43: American Urological Association. Early detection of prostate cancer and use of transrectal ultrasound. American Urological Association 1992 Policy Statement Book. Baltimore, MD: Williams & Wilkins; American College of Physicians. Screening for prostate cancer. Ann Intern Med. 1997;126: United States Preventive Services Task Force. Guide to Clinical Preventive Services. 2nd ed. Baltimore, MD: Williams & Wilkins; National Cancer Institute. PDQ prostate cancer screening [database on the Internet]. Available at: cancertopics/pdq/screening/prostate/healthprofessional. Accessed March 20, Slev PR, La ulu SL, Roberts WL. Intermethod differences in results for total PSA, free PSA, and percentage of free PSA. Am J Clin Pathol. 2008;129: Puustinen J, Lahteenmaki R, Polo-Kantola P, et al. Effect of withdrawal from long-term use of temazepam, zopiclone or zolpidem as hypnotic agents on cognition in older adults. Eur J Clin Pharmacol. 2013;70: Stenman UH, Koivunen E, Itkonen O. Biology and function of tumor-associated trypsin inhibitor, TATI. Scand J Clin Lab Invest Suppl. 1991;207: Thompson IM, Pauler DK, Goodman PJ, et al. Prevalence of prostate cancer among men with a prostate-specific antigen level < or =4.0 ng per milliliter. N Engl J Med. 2004;350: Prensner JR, Rubin MA, Wei JT, et al. Beyond PSA: the next generation of prostate cancer biomarkers. Sci Transl Med. 2012;4:127rv Killick E, Bancroft E, Kote-Jarai Z, et al. Beyond prostatespecific antigen - future biomarkers for the early detection and management of prostate cancer. Clin Oncol (R Coll Radiol). 2012;24: Wolf AM, Wender RC, Etzioni RB, et al. American Cancer Society guideline for the early detection of prostate cancer: update CA Cancer J Clin. 2010;60: Partin MR, Powell AA, Burgess DJ, et al. Adding postal follow-up to a web-based survey of primary care and gastroenterology clinic physician chiefs improved response rates but not response quality or representativeness [published online ahead of print December 5, 2013]. Eval Health Prof Benson MC, Whang IS, Olsson CA, et al. The use of prostate specific antigen density to enhance the predictive value of intermediate levels of serum prostate specific antigen. J Urol. 1992;147: Andriole GL, Telle WB, Coplen DE, et al. PSA index (PSAI) as a predictor of prostate cancer in men with persistent serum PSA elevation. J Urol. 1992;147:387A. 32. Benson MC, Whang IS, Pantuck A, et al. Prostate specific antigen density: a means of distinguishing benign prostatic hypertrophy and prostate cancer. J Urol. 1992;147: Catalona WJ, Richie JP, dekernion JB, et al. Comparison of prostate specific antigen concentration versus prostate specific antigen density in the early detection of prostate cancer: receiver operating characteristic curves. J Urol. 1994;152: Smith DS, Catalona WJ. Rate of change in serum prostate specific antigen levels as a method for prostate cancer detection. J Urol. 1994;152: Carter HB, Ferrucci L, Kettermann A, et al. Detection of life-threatening prostate cancer with prostate-specific antigen velocity during a window of curability. J Natl Cancer Inst. 2006;98: Carter HB, Pearson JD, Metter EJ, et al. Longitudinal evaluation of prostate-specific antigen levels in men with and without prostate disease. JAMA. 1992;267: Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR
9 37. Riehmann M, Rhodes PR, Cook TD, et al. Analysis of variation in prostate-specific antigen values. Urology. 1993;42: Carter HB, Partin AW, Luderer AA, et al. Percentage of free prostate-specific antigen in sera predicts aggressiveness of prostate cancer a decade before diagnosis. Urology. 1997;49: Hoffman RM, Clanon DL, Littenberg B, et al. Using the free-to-total prostate-specific antigen ratio to detect prostate cancer in men with nonspecific elevations of prostate-specific antigen levels. J Gen Intern Med. 2000;15: Catalona WJ, Partin AW, Slawin KM, et al. Use of the percentage of free prostate-specific antigen to enhance differentiation of prostate cancer from benign prostatic disease: a prospective multicenter clinical trial. JAMA. 1998;279: Piironen T, Pettersson K, Suonpaa M, et al. In vitro stability of free prostate-specific antigen (PSA) and prostate-specific antigen (PSA) complexed to alpha 1-antichymotrypsin in blood samples. Urology. 1996;48: Horninger W, Cheli CD, Babaian RJ, et al. Complexed prostate-specific antigen for early detection of prostate cancer in men with serum prostate-specific antigen levels of 2 to 4 nanograms per milliliter. Urology. 2002;60: Khan SK, Malviya A, Muller SD, et al. Reduced short-term complications and mortality following enhanced recovery primary hip and knee arthroplasty: results from 6,000 consecutive procedures. Acta Orthop. 2013;85: Partin AW, Brawer MK, Bartsch G, et al. Complexed prostate specific antigen improves specificity for prostate cancer detection: results of a prospective multicenter clinical trial. J Urol. 2003;170: Jung K, Elgeti U, Lein M, et al. Ratio of free or complexed prostate-specific antigen (PSA) to total PSA: which ratio improves differentiation between benign prostatic hyperplasia and prostate cancer? Clin Chem. 2000;46: Mikolajczyk SD, Marks LS, Partin AW, et al. Free prostatespecific antigen in serum is becoming more complex. Urology. 2002;59: Canto EI, Singh H, Shariat SF, et al. Serum BPSA outperforms both total PSA and free PSA as a predictor of prostatic enlargement in men without prostate cancer. Urology. 2004;63: ; discussion Sokoll LJ, Sanda MG, Feng Z, et al. A prospective, multicenter, National Cancer Institute Early Detection Research Network study of [-2]proPSA: improving prostate cancer detection and correlating with cancer aggressiveness. Cancer Epidemiol Biomarkers Prev. 2010;19: Sokoll LJ, Wang Y, Feng Z, et al. [-2]proenzyme prostate specific antigen for prostate cancer detection: a national cancer institute early detection research network validation study. J Urol. 2008;180: ; discussion Catalona WJ, Partin AW, Sanda MG, et al. A multicenter study of [-2]pro-prostate specific antigen combined with prostate specific antigen and free prostate specific antigen for prostate cancer detection in the 2.0 to 10.0 ng/ml prostate specific antigen range. J Urol. 2011;185: Le BV, Griffin CR, Loeb S, et al. [-2]Proenzyme prostate specific antigen is more accurate than total and free prostate specific antigen in differentiating prostate cancer from benign disease in a prospective prostate cancer screening study. J Urol. 2010;183: Stenman G, Sahlin P, Mark J, et al. Structural alterations of the c-mos locus in benign pleomorphic adenomas with chromosome abnormalities of 8q12. Oncogene. 1991;6: Stenman G, Sandros J, Nordkvist A, et al. Expression of the ERBB2 protein in benign and malignant salivary gland tumors. Genes Chromosomes Cancer. 1991;3: Howlander N, Noone AM, Krapcho M, et al, eds. SEER Cancer Statistics Review, Bethesda, MD: National Cancer Institute. Available at gov/csr/1975_2010/, based on November 2012 SEER data submission posted to the SEER website, April Accessed March 20, Schroder FH, Hugosson J, Roobol MJ, et al. Screening and prostate-cancer mortality in a randomized European study. N Engl J Med. 2009;360: Schroder FH, Hugosson J, Roobol MJ, et al. Prostatecancer mortality at 11 years of follow-up. N Engl J Med. 2012;366: Hugosson J, Carlsson S, Aus G, et al. Mortality results from the Goteborg randomised population-based prostate-cancer screening trial. Lancet Oncol. 2010;11: Bill-Axelson A, Holmberg L, Ruutu M, et al. Radical prostatectomy versus watchful waiting in early prostate cancer. N Engl J Med. 2011;364: Andriole GL, Crawford ED, Grubb RL, 3rd, et al. Mortality results from a randomized prostate-cancer screening trial. N Engl J Med. 2009;360: Wilt TJ, Brawer MK, Jones KM, et al. Radical prostatectomy versus observation for localized prostate cancer. N Engl J Med. 2012;367: Loeb S, Vellekoop A, Ahmed HU, et al. Systematic review of complications of prostate biopsy. Eur Urol Duffy MJ. Use of biomarkers in screening for cancer. J Int Fed Clin Chem Lab Med Available at ejifcc/vol21. Accessed March 20, Pinsky PF, Blacka A, Kramer BS, et al. Assessing contamination and compliance in the prostate component of the Prostate, Lung, Colorectal, and Ovarian (PLCO) Cancer Screening Trial. Clin Trials. 2010;7: Aleksic I, Mouraviev V, Albala D. Recent developments in prostate cancer screening guidelines. J Cancer Sci Ther. 2013;S7:005. Am J Clin Pathol 2014;142: DOI: /AJCPU6OOKL9JHEUR 15
Prostate-Specific Antigen (PSA) Test
 Prostate-Specific Antigen (PSA) Test What is the PSA test? Prostate-specific antigen, or PSA, is a protein produced by normal, as well as malignant, cells of the prostate gland. The PSA test measures the
Prostate-Specific Antigen (PSA) Test What is the PSA test? Prostate-specific antigen, or PSA, is a protein produced by normal, as well as malignant, cells of the prostate gland. The PSA test measures the
Elevated PSA. Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017
 Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
10/2/2018 OBJECTIVES PROSTATE HEALTH BACKGROUND THE PROSTATE HEALTH INDEX PHI*: BETTER PROSTATE CANCER DETECTION
 THE PROSTATE HEALTH INDEX PHI*: BETTER PROSTATE CANCER DETECTION Lenette Walters, MS, MT(ASCP) Medical Affairs Manager Beckman Coulter, Inc. *phi is a calculation using the values from PSA, fpsa and p2psa
THE PROSTATE HEALTH INDEX PHI*: BETTER PROSTATE CANCER DETECTION Lenette Walters, MS, MT(ASCP) Medical Affairs Manager Beckman Coulter, Inc. *phi is a calculation using the values from PSA, fpsa and p2psa
Prostate Cancer Screening Guidelines in 2017
 Prostate Cancer Screening Guidelines in 2017 Pocharapong Jenjitranant, M.D. Division of Urology, Department of Surgery, Faculty of Medicine, Ramathibodi Hospital Prostate Specific Antigen (PSA) Prostate
Prostate Cancer Screening Guidelines in 2017 Pocharapong Jenjitranant, M.D. Division of Urology, Department of Surgery, Faculty of Medicine, Ramathibodi Hospital Prostate Specific Antigen (PSA) Prostate
Although the test that measures total prostate-specific antigen (PSA) has been
 ORIGINAL ARTICLE STEPHEN LIEBERMAN, MD Chief of Urology Kaiser Permanente Northwest Region Clackamas, OR Effective Clinical Practice. 1999;2:266 271 Can Percent Free Prostate-Specific Antigen Reduce the
ORIGINAL ARTICLE STEPHEN LIEBERMAN, MD Chief of Urology Kaiser Permanente Northwest Region Clackamas, OR Effective Clinical Practice. 1999;2:266 271 Can Percent Free Prostate-Specific Antigen Reduce the
Urological Society of Australia and New Zealand PSA Testing Policy 2009
 Executive summary Urological Society of Australia and New Zealand PSA Testing Policy 2009 1. Prostate cancer is a major health problem and is the second leading cause of male cancer deaths in Australia
Executive summary Urological Society of Australia and New Zealand PSA Testing Policy 2009 1. Prostate cancer is a major health problem and is the second leading cause of male cancer deaths in Australia
Focus on... Prostate Health Index (PHI) Proven To Outperform Traditional PSA Screening In Predicting Clinically Significant Prostate Cancer
 Focus on... Prostate Health Index (PHI) Proven To Outperform Traditional PSA Screening In Predicting Clinically Significant Prostate Cancer Prostate Cancer in Ireland & Worldwide In Ireland, prostate cancer
Focus on... Prostate Health Index (PHI) Proven To Outperform Traditional PSA Screening In Predicting Clinically Significant Prostate Cancer Prostate Cancer in Ireland & Worldwide In Ireland, prostate cancer
PSA screening. To screen or not to screen, that s the question Walid Shahrour FRCSC, MDCM, BSc Assistant professor Northern Ontario School of Medicine
 PSA screening To screen or not to screen, that s the question Walid Shahrour FRCSC, MDCM, BSc Assistant professor Northern Ontario School of Medicine Conflict of Interest Declaration: Nothing to Disclose
PSA screening To screen or not to screen, that s the question Walid Shahrour FRCSC, MDCM, BSc Assistant professor Northern Ontario School of Medicine Conflict of Interest Declaration: Nothing to Disclose
Controversies in Prostate Cancer Screening
 Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
BPH AND BEYOND. BPSA: A Novel Serum Marker for Benign Prostatic Hyperplasia Kevin M. Slawin, MD, Shahrokh Shariat, MD, Eduardo Canto, MD
 BPH AND BEYOND B: A Novel Serum Marker for Benign Prostatic Hyperplasia Kevin M. Slawin, MD, Shahrokh Shariat, MD, Eduardo Canto, MD Baylor Prostate Center, The Scott Department of Urology, Baylor College
BPH AND BEYOND B: A Novel Serum Marker for Benign Prostatic Hyperplasia Kevin M. Slawin, MD, Shahrokh Shariat, MD, Eduardo Canto, MD Baylor Prostate Center, The Scott Department of Urology, Baylor College
Intermethod Differences in Results for Total PSA, Free PSA, and Percentage of Free PSA
 Clinical Chemistry / PSA and Free PSA Method Differences Intermethod Differences in Results for Total PSA, Free PSA, and Percentage of Free PSA Patricia R. Slev, PhD, Sonia L. La ulu, and William L. Roberts,
Clinical Chemistry / PSA and Free PSA Method Differences Intermethod Differences in Results for Total PSA, Free PSA, and Percentage of Free PSA Patricia R. Slev, PhD, Sonia L. La ulu, and William L. Roberts,
PSA Screening and Prostate Cancer. Rishi Modh, MD
 PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
Cigna Medical Coverage Policy
 Cigna Medical Coverage Policy Subject Prostate-Specific Antigen (PSA) Screening for Prostate Cancer Table of Contents Coverage Policy... 1 General Background... 1 Coding/Billing Information... 12 References...
Cigna Medical Coverage Policy Subject Prostate-Specific Antigen (PSA) Screening for Prostate Cancer Table of Contents Coverage Policy... 1 General Background... 1 Coding/Billing Information... 12 References...
Health Screening Update: Prostate Cancer Zamip Patel, MD FSACOFP Convention August 1 st, 2015
 Health Screening Update: Prostate Cancer Zamip Patel, MD FSACOFP Convention August 1 st, 2015 Outline Epidemiology of prostate cancer Purpose of screening Method of screening Contemporary screening trials
Health Screening Update: Prostate Cancer Zamip Patel, MD FSACOFP Convention August 1 st, 2015 Outline Epidemiology of prostate cancer Purpose of screening Method of screening Contemporary screening trials
Prostate Cancer Incidence
 Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement
 Clinical Review & Education JAMA US Preventive Services Task Force RECOMMENDATION STATEMENT Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement US Preventive Services
Clinical Review & Education JAMA US Preventive Services Task Force RECOMMENDATION STATEMENT Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement US Preventive Services
Questions and Answers About the Prostate-Specific Antigen (PSA) Test
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Questions and Answers
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Questions and Answers
Screening and Risk Stratification of Men for Prostate Cancer Metastasis and Mortality
 Screening and Risk Stratification of Men for Prostate Cancer Metastasis and Mortality Sanoj Punnen, MD, MAS Assistant Professor of Urologic Oncology University of Miami, Miller School of Medicine and Sylvester
Screening and Risk Stratification of Men for Prostate Cancer Metastasis and Mortality Sanoj Punnen, MD, MAS Assistant Professor of Urologic Oncology University of Miami, Miller School of Medicine and Sylvester
PROSTATE CANCER SCREENING: AN UPDATE
 PROSTATE CANCER SCREENING: AN UPDATE William G. Nelson, M.D., Ph.D. Sidney Kimmel Comprehensive Cancer Center at Johns Hopkins American Association for Cancer Research William G. Nelson, M.D., Ph.D. Disclosures
PROSTATE CANCER SCREENING: AN UPDATE William G. Nelson, M.D., Ph.D. Sidney Kimmel Comprehensive Cancer Center at Johns Hopkins American Association for Cancer Research William G. Nelson, M.D., Ph.D. Disclosures
Prostate Cancer Screening: Risks and Benefits across the Ages
 Prostate Cancer Screening: Risks and Benefits across the Ages 7 th Annual Symposium on Men s Health Continuing Progress: New Gains, New Challenges June 10, 2009 Michael J. Barry, MD General Medicine Unit
Prostate Cancer Screening: Risks and Benefits across the Ages 7 th Annual Symposium on Men s Health Continuing Progress: New Gains, New Challenges June 10, 2009 Michael J. Barry, MD General Medicine Unit
Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate volume matter?
 ORIGINAL ARTICLE Gulhane Med J 2018;60: 14-18 Gülhane Faculty of Medicine 2018 doi: 10.26657/gulhane.00010 Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate
ORIGINAL ARTICLE Gulhane Med J 2018;60: 14-18 Gülhane Faculty of Medicine 2018 doi: 10.26657/gulhane.00010 Contribution of prostate-specific antigen density in the prediction of prostate cancer: Does prostate
Response to United States Preventative Services Task Force draft PSA Screening recommendation: Donald B. Fuller, M.D. Genesis Healthcare Partners
 Response to United States Preventative Services Task Force draft PSA Screening recommendation: Donald B. Fuller, M.D. Genesis Healthcare Partners October 2011 Cancer Incidence Statistics, 2011 CA: A Cancer
Response to United States Preventative Services Task Force draft PSA Screening recommendation: Donald B. Fuller, M.D. Genesis Healthcare Partners October 2011 Cancer Incidence Statistics, 2011 CA: A Cancer
Pre-test. Prostate Cancer The Good News: Prostate Cancer Screening 2012: Putting the PSA Controversy to Rest
 Pre-test Matthew R. Cooperberg, MD, MPH UCSF 40 th Annual Advances in Internal Medicine Prostate Cancer Screening 2012: Putting the PSA Controversy to Rest 1. I do not offer routine PSA screening, and
Pre-test Matthew R. Cooperberg, MD, MPH UCSF 40 th Annual Advances in Internal Medicine Prostate Cancer Screening 2012: Putting the PSA Controversy to Rest 1. I do not offer routine PSA screening, and
Section Editors Robert H Fletcher, MD, MSc Michael P O'Leary, MD, MPH
 1 de 32 04-05-2013 19:24 Official reprint from UpToDate www.uptodate.com 2013 UpToDate Author Richard M Hoffman, MD, MPH Disclosures Section Editors Robert H Fletcher, MD, MSc Michael P O'Leary, MD, MPH
1 de 32 04-05-2013 19:24 Official reprint from UpToDate www.uptodate.com 2013 UpToDate Author Richard M Hoffman, MD, MPH Disclosures Section Editors Robert H Fletcher, MD, MSc Michael P O'Leary, MD, MPH
The Evolving Role of PSA for Prostate Cancer. The Evolving Role of PSA for Prostate Cancer: 10/30/2017
 The Evolving Role of PSA for Prostate Cancer Adele Marie Caruso, DNP, CRNP Adult Nurse Practitioner Perelman School of Medicine at the University of Pennsylvania November 4, 2017 The Evolving Role of PSA
The Evolving Role of PSA for Prostate Cancer Adele Marie Caruso, DNP, CRNP Adult Nurse Practitioner Perelman School of Medicine at the University of Pennsylvania November 4, 2017 The Evolving Role of PSA
Overview. What is Cancer? Prostate Cancer 3/2/2014. Davis A Romney, MD Ironwood Cancer and Research Centers Feb 18, 2014
 Prostate Cancer Davis A Romney, MD Ironwood Cancer and Research Centers Feb 18, 2014 Overview Start with the basics: Definition of cancer Most common cancers in men Prostate, lung, and colon cancers Cancer
Prostate Cancer Davis A Romney, MD Ironwood Cancer and Research Centers Feb 18, 2014 Overview Start with the basics: Definition of cancer Most common cancers in men Prostate, lung, and colon cancers Cancer
Prostate-Specific Antigen (PSA) Screening for Prostate Cancer
 Medical Coverage Policy Effective Date... 4/15/2018 Next Review Date... 4/15/2019 Coverage Policy Number... 0215 Prostate-Specific Antigen (PSA) Screening for Prostate Cancer Table of Contents Related
Medical Coverage Policy Effective Date... 4/15/2018 Next Review Date... 4/15/2019 Coverage Policy Number... 0215 Prostate-Specific Antigen (PSA) Screening for Prostate Cancer Table of Contents Related
PROSTATE CANCER SURVEILLANCE
 PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
Annual Report on Prostate Diseases
 An except from the HMS 2010 Annual Report on Prostate Diseases. To purchase the full report, visit www.health.harvard.edu/special_health_reports/prostate_disease Harvard Medical School 2010 Annual Report
An except from the HMS 2010 Annual Report on Prostate Diseases. To purchase the full report, visit www.health.harvard.edu/special_health_reports/prostate_disease Harvard Medical School 2010 Annual Report
Association of [ 2]proPSA with Biopsy Reclassification During Active Surveillance for Prostate Cancer
![Association of [ 2]proPSA with Biopsy Reclassification During Active Surveillance for Prostate Cancer Association of [ 2]proPSA with Biopsy Reclassification During Active Surveillance for Prostate Cancer](/thumbs/91/105963370.jpg) Association of [ 2]proPSA with Biopsy Reclassification During Active Surveillance for Prostate Cancer Jeffrey J. Tosoian,*, Stacy Loeb,*, Zhaoyong Feng, Sumit Isharwal, Patricia Landis, Debra J. Elliot,
Association of [ 2]proPSA with Biopsy Reclassification During Active Surveillance for Prostate Cancer Jeffrey J. Tosoian,*, Stacy Loeb,*, Zhaoyong Feng, Sumit Isharwal, Patricia Landis, Debra J. Elliot,
PSA and the Future. Axel Heidenreich, Department of Urology
 PSA and the Future Axel Heidenreich, Department of Urology PSA and Prostate Cancer EAU Guideline 2011 PSA is a continuous variable PSA value (ng/ml) risk of PCa, % 0 0.5 6.6 0.6 1 10.1 1.1 2 17.0 2.1 3
PSA and the Future Axel Heidenreich, Department of Urology PSA and Prostate Cancer EAU Guideline 2011 PSA is a continuous variable PSA value (ng/ml) risk of PCa, % 0 0.5 6.6 0.6 1 10.1 1.1 2 17.0 2.1 3
What to Do with an Abnormal PSA Test. Feinberg School of Medicine, Chicago, Illinois, USA
 The Oncologist Genitourinary Cancer What to Do with an Abnormal PSA Test STACY LOEB, a WILLIAM J. CATALONA b a Department of Urology, Johns Hopkins School of Medicine, Baltimore, Maryland, USA; b The Northwestern
The Oncologist Genitourinary Cancer What to Do with an Abnormal PSA Test STACY LOEB, a WILLIAM J. CATALONA b a Department of Urology, Johns Hopkins School of Medicine, Baltimore, Maryland, USA; b The Northwestern
Questions and Answers about Prostate Cancer Screening with the Prostate-Specific Antigen Test
 Questions and Answers about Prostate Cancer Screening with the Prostate-Specific Antigen Test About Cancer Care Ontario s recommendations for prostate-specific antigen (PSA) screening 1. What does Cancer
Questions and Answers about Prostate Cancer Screening with the Prostate-Specific Antigen Test About Cancer Care Ontario s recommendations for prostate-specific antigen (PSA) screening 1. What does Cancer
Consensus and Controversies in Cancer of Prostate BASIS FOR FURHTER STUDIES. Luis A. Linares MD FACRO Medical Director
 BASIS FOR FURHTER STUDIES Main controversies In prostate Cancer: 1-Screening 2-Management Observation Surgery Standard Laparoscopic Robotic Radiation: (no discussion on Cryosurgery-RF etc.) Standard SBRT
BASIS FOR FURHTER STUDIES Main controversies In prostate Cancer: 1-Screening 2-Management Observation Surgery Standard Laparoscopic Robotic Radiation: (no discussion on Cryosurgery-RF etc.) Standard SBRT
PSA Isoforms in Prostate Cancer Detection
 european urology supplements 5 (2006) 495 499 available at www.sciencedirect.com journal homepage: www.europeanurology.com PSA Isoforms in Prostate Cancer Detection Haluk Özen a, *, Sinan Sözen b a Department
european urology supplements 5 (2006) 495 499 available at www.sciencedirect.com journal homepage: www.europeanurology.com PSA Isoforms in Prostate Cancer Detection Haluk Özen a, *, Sinan Sözen b a Department
Pro PSA: a more cancer specific form of prostate specific antigen for the early detection of prostate cancer
 REVIEW Pro PSA: a more cancer specific form of prostate specific antigen for the early detection of prostate cancer Stephen D. Mikolajczyk and Harry G. Rittenhouse Beckman Coulter, Inc., San Diego, CA,
REVIEW Pro PSA: a more cancer specific form of prostate specific antigen for the early detection of prostate cancer Stephen D. Mikolajczyk and Harry G. Rittenhouse Beckman Coulter, Inc., San Diego, CA,
Prostate Cancer: from Beginning to End
 Prostate Cancer: from Beginning to End Matthew D. Katz, M.D. Assistant Professor Urologic Oncology Robotic and Laparoscopic Surgery University of Arkansas for Medical Sciences Winthrop P. Rockefeller Cancer
Prostate Cancer: from Beginning to End Matthew D. Katz, M.D. Assistant Professor Urologic Oncology Robotic and Laparoscopic Surgery University of Arkansas for Medical Sciences Winthrop P. Rockefeller Cancer
Screening for Prostate Cancer with the Prostate Specific Antigen (PSA) Test: Recommendations 2014
 Screening for Prostate Cancer with the Prostate Specific Antigen (PSA) Test: Recommendations 2014 Canadian Task Force on Preventive Health Care October 2014 Putting Prevention into Practice Canadian Task
Screening for Prostate Cancer with the Prostate Specific Antigen (PSA) Test: Recommendations 2014 Canadian Task Force on Preventive Health Care October 2014 Putting Prevention into Practice Canadian Task
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
Since the beginning of the prostate-specific antigen (PSA) era in the. Characteristics of Insignificant Clinical T1c Prostate Tumors
 2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
PSA Screening for Prostate Cancer at Western Medical Clinic Kardy Fedorowich University of Manitoba Max Rady College of Medicine
 PSA Screening for Prostate Cancer at Western Medical Clinic Kardy Fedorowich University of Manitoba Max Rady College of Medicine Abstract While PSA screening for prostate cancer remains a widely used tool
PSA Screening for Prostate Cancer at Western Medical Clinic Kardy Fedorowich University of Manitoba Max Rady College of Medicine Abstract While PSA screening for prostate cancer remains a widely used tool
Prostate Cancer Screening. Eric Shreve, MD Bend Urology Associates
 Prostate Cancer Screening Eric Shreve, MD Bend Urology Associates University of Cincinnati Medical Center University of Iowa Hospitals and Clinics PSA Human kallikrein 3 Semenogelin is substrate Concentration
Prostate Cancer Screening Eric Shreve, MD Bend Urology Associates University of Cincinnati Medical Center University of Iowa Hospitals and Clinics PSA Human kallikrein 3 Semenogelin is substrate Concentration
Fellow GU Lecture Series, Prostate Cancer. Asit Paul, MD, PhD 02/20/2018
 Fellow GU Lecture Series, 2018 Prostate Cancer Asit Paul, MD, PhD 02/20/2018 Disease Burden Screening Risk assessment Treatment Global Burden of Prostate Cancer Prostate cancer ranked 13 th among cancer
Fellow GU Lecture Series, 2018 Prostate Cancer Asit Paul, MD, PhD 02/20/2018 Disease Burden Screening Risk assessment Treatment Global Burden of Prostate Cancer Prostate cancer ranked 13 th among cancer
Prostate Cancer Screening: Con. Laurence Klotz Professor of Surgery, Sunnybrook HSC University of Toronto
 Prostate Cancer Screening: Con Laurence Klotz Professor of Surgery, Sunnybrook HSC University of Toronto / Why not PSA screening? Overdiagnosis Overtreatment Risk benefit ratio unfavorable Flaws of PSA
Prostate Cancer Screening: Con Laurence Klotz Professor of Surgery, Sunnybrook HSC University of Toronto / Why not PSA screening? Overdiagnosis Overtreatment Risk benefit ratio unfavorable Flaws of PSA
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT
 MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
Complexed Prostate-specific Antigen for the Detection of Prostate Cancer
 Complexed Prostate-specific Antigen for the Detection of Prostate Cancer XAVIER FILELLA 1, DAVID TRUAN 2, JOAN ALCOVER 2, RAFAEL GUTIERREZ 2, RAFAEL MOLINA 1, FRANCISCA COCA 1 and ANTONIO M. BALLESTA 1
Complexed Prostate-specific Antigen for the Detection of Prostate Cancer XAVIER FILELLA 1, DAVID TRUAN 2, JOAN ALCOVER 2, RAFAEL GUTIERREZ 2, RAFAEL MOLINA 1, FRANCISCA COCA 1 and ANTONIO M. BALLESTA 1
Prostate-Specific Antigen (PSA)
 Prostate-Specific Antigen (PSA) The diagnosis of prostate cancer hinges on three primary factors: digital rectal exam, or DRE, (to be discussed) PSA testing, (discussed here) and ultrasound-guided biopsy.
Prostate-Specific Antigen (PSA) The diagnosis of prostate cancer hinges on three primary factors: digital rectal exam, or DRE, (to be discussed) PSA testing, (discussed here) and ultrasound-guided biopsy.
Prostate cancer screening: a wobble Balance. Elias NAOUM PGY-4 Urology Hotel-Dieu de France Universite Saint Joseph
 Prostate cancer screening: a wobble Balance Elias NAOUM PGY-4 Urology Hotel-Dieu de France Universite Saint Joseph Epidemiology Most common non skin malignancy in men in developed countries Third leading
Prostate cancer screening: a wobble Balance Elias NAOUM PGY-4 Urology Hotel-Dieu de France Universite Saint Joseph Epidemiology Most common non skin malignancy in men in developed countries Third leading
Enzyme Immunoassay for the Quantitative Determination of Free Prostate Specific Antigen (f-psa) in Human Serum
 Enzyme Immunoassay for the Quantitative Determination of Free Prostate Specific Antigen (f-psa) in Human Serum FOR RESEARCH USE ONLY Store at 2 to 8 C. PROPRIETARY AND COMMON NAMES f-psa Enzyme Immunoassay
Enzyme Immunoassay for the Quantitative Determination of Free Prostate Specific Antigen (f-psa) in Human Serum FOR RESEARCH USE ONLY Store at 2 to 8 C. PROPRIETARY AND COMMON NAMES f-psa Enzyme Immunoassay
Use of the Percentage of Free Prostate-Specific Antigen to Enhance Differentiation of Prostate Cancer From Benign Prostatic Disease
 Use of the Percentage of Free Prostate-Specific Antigen to Enhance Differentiation of Prostate From Benign Prostatic Disease A Prospective Multicenter Clinical Trial William J. Catalona, MD; Alan W. Partin,
Use of the Percentage of Free Prostate-Specific Antigen to Enhance Differentiation of Prostate From Benign Prostatic Disease A Prospective Multicenter Clinical Trial William J. Catalona, MD; Alan W. Partin,
The U.S. Preventive Services Task Force (USPSTF) makes
 Annals of Internal Medicine Clinical Guideline Screening for Prostate Cancer: U.S. Preventive Services Task Force Recommendation Statement Virginia A. Moyer, MD, MPH, on behalf of the U.S. Preventive Services
Annals of Internal Medicine Clinical Guideline Screening for Prostate Cancer: U.S. Preventive Services Task Force Recommendation Statement Virginia A. Moyer, MD, MPH, on behalf of the U.S. Preventive Services
Prostate cancer screening: Attitudes and practices of family physicians in Ontario
 Original research Prostate cancer screening: Attitudes and practices of family physicians in Ontario Christopher B. Allard, MD; * Shawn Dason; * Janis Lusis, MD; Anil Kapoor, MD, FRCSC * *McMaster Institute
Original research Prostate cancer screening: Attitudes and practices of family physicians in Ontario Christopher B. Allard, MD; * Shawn Dason; * Janis Lusis, MD; Anil Kapoor, MD, FRCSC * *McMaster Institute
Contact: Linda Aagard Huntsman Cancer Institute
 Contact: Linda Aagard Huntsman Cancer Institute 801-587-7639 linda.aagard@hci.utah.edu U.S. Cancer Screening Trial Reports More Diagnoses, but No Fewer Deaths from Annual Prostate Cancer Screening Huntsman
Contact: Linda Aagard Huntsman Cancer Institute 801-587-7639 linda.aagard@hci.utah.edu U.S. Cancer Screening Trial Reports More Diagnoses, but No Fewer Deaths from Annual Prostate Cancer Screening Huntsman
PSA To screen or not to screen? Darrel Drachenberg, MD, FRCSC
 PSA To screen or not to screen? Darrel Drachenberg, MD, FRCSC Disclosures Faculty / Speaker s name: Darrel Drachenberg Relationships with commercial interests: Grants/Research Support: None Speakers Bureau/Honoraria:
PSA To screen or not to screen? Darrel Drachenberg, MD, FRCSC Disclosures Faculty / Speaker s name: Darrel Drachenberg Relationships with commercial interests: Grants/Research Support: None Speakers Bureau/Honoraria:
Screening for Prostate Cancer
 clinical practice Screening for Prostate Cancer Richard M. Hoffman, M.D., M.P.H. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies
clinical practice Screening for Prostate Cancer Richard M. Hoffman, M.D., M.P.H. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies
Otis W. Brawley, MD, MACP, FASCO, FACE
 Otis W. Brawley, MD, MACP, FASCO, FACE Chief Medical and Scientific Officer American Cancer Society Professor of Hematology, Medical Oncology, Medicine and Epidemiology Emory University Atlanta, Georgia
Otis W. Brawley, MD, MACP, FASCO, FACE Chief Medical and Scientific Officer American Cancer Society Professor of Hematology, Medical Oncology, Medicine and Epidemiology Emory University Atlanta, Georgia
SERUM PROSTATE SPECIFIC ANTIGEN LEVELS IN MEN WITH BENIGN PROSTATIC HYPERPLASIA AND CANCER OF PROSTATE. A. AMAYO and W.
 22 EAST AFRICAN MEDICAL JOURNAL January 2004 The East African Medical Journal Vol. 81 No. 1 January 2004 SERUM PROSTATE SPECIFIC ANTIGEN LEVELS IN MEN WITH BENIGN PROSTATIC HYPERPLASIA AND CANCER OF PROSTATE.
22 EAST AFRICAN MEDICAL JOURNAL January 2004 The East African Medical Journal Vol. 81 No. 1 January 2004 SERUM PROSTATE SPECIFIC ANTIGEN LEVELS IN MEN WITH BENIGN PROSTATIC HYPERPLASIA AND CANCER OF PROSTATE.
Contemporary Approaches to Screening for Prostate Cancer
 Contemporary Approaches to Screening for Prostate Cancer Gerald L. Andriole, MD Robert K. Royce Distinguished Professor Chief of Urologic Surgery Siteman Cancer Center Washington University School of Medicine
Contemporary Approaches to Screening for Prostate Cancer Gerald L. Andriole, MD Robert K. Royce Distinguished Professor Chief of Urologic Surgery Siteman Cancer Center Washington University School of Medicine
Prostate Cancer. Axiom. Overdetection Is A Small Issue. Reducing Morbidity and Mortality
 Overdetection Is A Small Issue (in the context of decreasing prostate cancer mortality rates and with appropriate, effective, and high-quality treatment) Prostate Cancer Arises silently Dwells in a curable
Overdetection Is A Small Issue (in the context of decreasing prostate cancer mortality rates and with appropriate, effective, and high-quality treatment) Prostate Cancer Arises silently Dwells in a curable
Prostate Biopsy. Prostate Biopsy. We canʼt go backwards: Screening has helped!
 We canʼt go backwards: Screening has helped! Robert E. Donohue M.D. Denver V.A. Medical Center University of Colorado Prostate Biopsy Is cure necessary; when it is possible? Is cure possible; when it is
We canʼt go backwards: Screening has helped! Robert E. Donohue M.D. Denver V.A. Medical Center University of Colorado Prostate Biopsy Is cure necessary; when it is possible? Is cure possible; when it is
Objectives. Prostate Cancer Screening and Surgical Management
 Prostate Cancer Screening and Surgical Management Dr. Ken Jacobsohn Director, Minimally Invasive Urologic Surgery Assistant Professor, Department of Urology Medical College of Wisconsin Objectives Update
Prostate Cancer Screening and Surgical Management Dr. Ken Jacobsohn Director, Minimally Invasive Urologic Surgery Assistant Professor, Department of Urology Medical College of Wisconsin Objectives Update
OBJECTIVE. significantly different classification rates of patients. These differences were even larger when using fixed %fpsa thresholds.
 Original Article CLINICAL IMPACT OF DIFFERENT PSA ASSAYS STEPHAN et al. Different prostate-specific antigen assays give different results on the same blood sample: an obstacle to recommending uniform limits
Original Article CLINICAL IMPACT OF DIFFERENT PSA ASSAYS STEPHAN et al. Different prostate-specific antigen assays give different results on the same blood sample: an obstacle to recommending uniform limits
Prostate-Specific Antigen in 2006: Effective Use in Benign Prostatic Hyperplasia and Prostate Cancer
 Volume 1, Number 3 ISSN: 1932-9245 Weill Medical College of Cornell University Reports on Men s Urologic Health 1 Editor: Steven A. Kaplan, MD, Professor of Urology, and Chief, Institute for Bladder and
Volume 1, Number 3 ISSN: 1932-9245 Weill Medical College of Cornell University Reports on Men s Urologic Health 1 Editor: Steven A. Kaplan, MD, Professor of Urology, and Chief, Institute for Bladder and
AllinaHealthSystems 1
 2018 Dimensions in Oncology Genitourinary Cancer Disclosures I have no financial or commercial relationships relevant to this presentation. Matthew O Shaughnessy, MD, PhD Director of Urologic Oncology
2018 Dimensions in Oncology Genitourinary Cancer Disclosures I have no financial or commercial relationships relevant to this presentation. Matthew O Shaughnessy, MD, PhD Director of Urologic Oncology
4/20/2015. Serum Protein Tumor Marker Assays: A Need for Constant Vigilance. Learning Objectives. Estimated Cancer Deaths in the US in 2015
 Serum Protein Tumor Marker Assays: A Need for Constant Vigilance Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning Objectives Describe what comprises an ideal
Serum Protein Tumor Marker Assays: A Need for Constant Vigilance Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning Objectives Describe what comprises an ideal
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
#1 cancer. #2 killer. Boulder has higher rate of prostate cancer compared to other areas surrounding Rocky Flats
 Prostate cancer is a VERY COMMON DISEASE BREAKTHROUGHS IN THE DETECTION OF PROSTATE CANCER Carolyn M. Fronczak M.D., M.S.P.H. Urologic Surgery 303-647-9129 #1 cancer #2 killer Ca Cancer J Clin 2018;68:7
Prostate cancer is a VERY COMMON DISEASE BREAKTHROUGHS IN THE DETECTION OF PROSTATE CANCER Carolyn M. Fronczak M.D., M.S.P.H. Urologic Surgery 303-647-9129 #1 cancer #2 killer Ca Cancer J Clin 2018;68:7
Age-specific reference ranges for prostate-specific antigen (PSA) in Jordanian patients
 (2003) 6, 256 260 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Age-specific reference ranges for prostate-specific antigen (PSA) in Jordanian patients 1, *
(2003) 6, 256 260 & 2003 Nature Publishing Group All rights reserved 1365-7852/03 $25.00 www.nature.com/pcan Age-specific reference ranges for prostate-specific antigen (PSA) in Jordanian patients 1, *
Determination of An Optimum Cut-off Point for % fpsa/tpsa to Improve Detection of Prostate Cancer
 Original Article DOI: 10.21276/APALM.1254 Determination of An Optimum Cut-off Point for % fpsa/tpsa to Improve Detection of Prostate Cancer Vineeth* G Nair and M. H. Shariff Department of Pathology, Yenepoya
Original Article DOI: 10.21276/APALM.1254 Determination of An Optimum Cut-off Point for % fpsa/tpsa to Improve Detection of Prostate Cancer Vineeth* G Nair and M. H. Shariff Department of Pathology, Yenepoya
european urology 55 (2009)
 european urology 55 (2009) 385 393 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Is Prostate-Specific Antigen Velocity Selective for Clinically Significant
european urology 55 (2009) 385 393 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Is Prostate-Specific Antigen Velocity Selective for Clinically Significant
BLADDER PROSTATE PENIS TESTICLES BE YO ND YO UR CA NC ER
 BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen).
 What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
Clinical Policy Title: Prostate-specific antigen screening
 Clinical Policy Title: Prostate-specific antigen screening Clinical Policy Number: 13.01.06 Effective Date: May 1, 2017 Initial Review Date: April 19, 2017 Most Recent Review Date: April 19, 2017 Next
Clinical Policy Title: Prostate-specific antigen screening Clinical Policy Number: 13.01.06 Effective Date: May 1, 2017 Initial Review Date: April 19, 2017 Most Recent Review Date: April 19, 2017 Next
Mr PHIP No. 1 Prostate cancer: Should I be tested?
 Mr PHIP No. 1 cancer: Should I be tested? Having a large prostate doesn t increase your chances of having prostate cancer. No. 1 / 1 Key points cancer is the most common male cancer after skin cancer.
Mr PHIP No. 1 cancer: Should I be tested? Having a large prostate doesn t increase your chances of having prostate cancer. No. 1 / 1 Key points cancer is the most common male cancer after skin cancer.
When PSA fails. Urology Grand Rounds Alexandra Perks. Rising PSA after Radical Prostatectomy
 When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
When PSA fails Urology Grand Rounds Alexandra Perks Rising PSA after Radical Prostatectomy Issues Natural History Local vs Metastatic Treatment options 1 10 000 men / year in Canada 4000 RRP 15-year PSA
USA Preventive Services Task Force PSA Screening Recommendations- May 2018
 GPGU - NOTÍCIAS USA Preventive Services Task Force PSA Screening Recommendations- May 2018 Rationale Importance Prostate cancer is one of the most common types of cancer that affects men. In the United
GPGU - NOTÍCIAS USA Preventive Services Task Force PSA Screening Recommendations- May 2018 Rationale Importance Prostate cancer is one of the most common types of cancer that affects men. In the United
THE UROLOGY GROUP
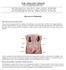 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
Use of early PSA velocity to predict eventual abnormal PSA values in men at risk for prostate cancer {
 Use of early PSA velocity to predict eventual abnormal PSA values in men at risk for prostate cancer { (2003) 6, 39 44 ß 2003 Nature Publishing Group All rights reserved 1365 7852/03 $25.00 www.nature.com/pcan
Use of early PSA velocity to predict eventual abnormal PSA values in men at risk for prostate cancer { (2003) 6, 39 44 ß 2003 Nature Publishing Group All rights reserved 1365 7852/03 $25.00 www.nature.com/pcan
Chapter 2. Understanding My Diagnosis
 Chapter 2. Understanding My Diagnosis With contributions from Nancy L. Brown, Ph.D.,Palo Alto Medical Foundation Research Institute; and Patrick Swift, M.D., Alta Bates Comprehensive Cancer Program o Facts
Chapter 2. Understanding My Diagnosis With contributions from Nancy L. Brown, Ph.D.,Palo Alto Medical Foundation Research Institute; and Patrick Swift, M.D., Alta Bates Comprehensive Cancer Program o Facts
PROSTATE CANCER Amit Gupta MD MPH
 PROSTATE CANCER Amit Gupta MD MPH Depts. of Urology and Epidemiology Amit-Gupta-1@uiowa.edu dramitgupta@gmail.com Tel: 319-384-5251 OUTLINE PSA screening controversy How to use PSA more effectively Treatment
PROSTATE CANCER Amit Gupta MD MPH Depts. of Urology and Epidemiology Amit-Gupta-1@uiowa.edu dramitgupta@gmail.com Tel: 319-384-5251 OUTLINE PSA screening controversy How to use PSA more effectively Treatment
Where are we with PSA screening?
 Where are we with PSA screening? Faculty/Presenter Disclosure Rela%onships with commercial interests: None Disclosure of Commercial Support This program has received no financial support. This program
Where are we with PSA screening? Faculty/Presenter Disclosure Rela%onships with commercial interests: None Disclosure of Commercial Support This program has received no financial support. This program
Understanding the risk of recurrence after primary treatment for prostate cancer. Aditya Bagrodia, MD
 Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Financial Disclosures. Prostate Cancer Screening and Surgical Management
 Prostate Cancer Screening and Surgical Management Dr. Ken Jacobsohn Director, Minimally Invasive Urologic Surgery Assistant Professor, Department of Urology Medical College of Wisconsin Financial Disclosures
Prostate Cancer Screening and Surgical Management Dr. Ken Jacobsohn Director, Minimally Invasive Urologic Surgery Assistant Professor, Department of Urology Medical College of Wisconsin Financial Disclosures
A pilot study evaluating serum pro-prostate-specific antigen in patients with rising PSA following radical prostatectomy
 ONCOLOGY LETTERS 3: 819-824, 2012 A pilot study evaluating serum pro-prostate-specific antigen in patients with rising PSA following radical prostatectomy ANTONINO SOTTILE 1, CINZIA ORTEGA 2, ALFREDO BERRUTI
ONCOLOGY LETTERS 3: 819-824, 2012 A pilot study evaluating serum pro-prostate-specific antigen in patients with rising PSA following radical prostatectomy ANTONINO SOTTILE 1, CINZIA ORTEGA 2, ALFREDO BERRUTI
Prostate Cancer. Biomedical Engineering for Global Health. Lecture Fourteen. Early Detection. Prostate Cancer: Statistics
 Biomedical Engineering for Global Health Lecture Fourteen Prostate Cancer Early Detection Prostate Cancer: Statistics Prostate gland contributes enzymes, nutrients and other secretions to semen. United
Biomedical Engineering for Global Health Lecture Fourteen Prostate Cancer Early Detection Prostate Cancer: Statistics Prostate gland contributes enzymes, nutrients and other secretions to semen. United
Quality-of-Life Effects of Prostate-Specific Antigen Screening
 Quality-of-Life Effects of Prostate-Specific Antigen Screening Eveline A.M. Heijnsdijk, Ph.D., Elisabeth M. Wever, M.Sc., Anssi Auvinen, M.D., Jonas Hugosson, M.D., Stefano Ciatto, M.D., Vera Nelen, M.D.,
Quality-of-Life Effects of Prostate-Specific Antigen Screening Eveline A.M. Heijnsdijk, Ph.D., Elisabeth M. Wever, M.Sc., Anssi Auvinen, M.D., Jonas Hugosson, M.D., Stefano Ciatto, M.D., Vera Nelen, M.D.,
NIH Public Access Author Manuscript Can J Urol. Author manuscript; available in PMC 2009 September 14.
 NIH Public Access Author Manuscript Published in final edited form as: Can J Urol. 2008 December ; 15(6): 4363 4374. Screening for Prostate Cancer: An Update Shahrokh F. Shariat 1, Peter T. Scardino 1,
NIH Public Access Author Manuscript Published in final edited form as: Can J Urol. 2008 December ; 15(6): 4363 4374. Screening for Prostate Cancer: An Update Shahrokh F. Shariat 1, Peter T. Scardino 1,
Screening for Prostate Cancer
 Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
Table 1. Descriptive characteristics, total prostate-specific antigen, and percentage of free/total prostate-specific antigen distribution Age Groups
 Oncology Population-based Analysis of Normal Total PSA and Percentage of Free/Total PSA Values: Results From Screening Cohort Umberto Capitanio, Paul Perrotte, Laurent Zini, Nazareno Suardi, Elie Antebi,
Oncology Population-based Analysis of Normal Total PSA and Percentage of Free/Total PSA Values: Results From Screening Cohort Umberto Capitanio, Paul Perrotte, Laurent Zini, Nazareno Suardi, Elie Antebi,
PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS
 ADULT UROLOGY PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS ABRAHAM MORGENTALER AND ERNANI LUIS RHODEN ABSTRACT Objectives. To determine
ADULT UROLOGY PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS ABRAHAM MORGENTALER AND ERNANI LUIS RHODEN ABSTRACT Objectives. To determine
When to worry, when to test?
 Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Repeating an abnormal prostate-specific antigen (PSA) level: how relevant is a decrease in PSA?
 Repeating an abnormal prostate-specific antigen (PSA) level: how relevant is a decrease in PSA? Connolly, D., Black, A., Murray, L., Nambirajan, T., Keane, P. F., & Gavin, A. (2009). Repeating an abnormal
Repeating an abnormal prostate-specific antigen (PSA) level: how relevant is a decrease in PSA? Connolly, D., Black, A., Murray, L., Nambirajan, T., Keane, P. F., & Gavin, A. (2009). Repeating an abnormal
Definition Prostate cancer
 Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Prostate cancer 61 Definition Prostate cancer is a malignant neoplasm that arises from the prostate gland and the most common form of cancer in men. localized prostate cancer is curable by surgery or radiation
Distribution of prostate specific antigen (PSA) and percentage free PSA in a contemporary screening cohort with no evidence of prostate cancer
 Urological Oncology CHUN et al. Distribution of prostate specific antigen (PSA) and percentage free PSA in a contemporary screening cohort with no evidence of prostate cancer Felix K.-H. Chun, Georg C.
Urological Oncology CHUN et al. Distribution of prostate specific antigen (PSA) and percentage free PSA in a contemporary screening cohort with no evidence of prostate cancer Felix K.-H. Chun, Georg C.
Reducing overtreatment of prostate cancer by radical prostatectomy in Eastern Ontario: a population-based cohort study
 Reducing overtreatment of prostate cancer by radical prostatectomy in Eastern Ontario: a population-based cohort study Luke Witherspoon MD MSc, Johnathan L. Lau BSc, Rodney H. Breau MD MSc, Christopher
Reducing overtreatment of prostate cancer by radical prostatectomy in Eastern Ontario: a population-based cohort study Luke Witherspoon MD MSc, Johnathan L. Lau BSc, Rodney H. Breau MD MSc, Christopher
Prostate Overview Quiz
 Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
Prostate Overview Quiz 1. The path report reads: Gleason 3 + 4 = 7. The Gleason s score is a. 3 b. 4 c. 7 d. None of the above 2. The path report reads: Moderately differentiated adenocarcinoma of the
Implications of Prostate Specific Antigen and its Molecular Derivatives in the Management of Carcinoma Prostate
 Review Article DOI: 10.17354/ijss/2015/327 Implications of Prostate Specific Antigen and its Molecular Derivatives in the Management of Carcinoma Prostate Sujan Narayan Agrawal 1, Chanjiv Singh 2, Sanwal
Review Article DOI: 10.17354/ijss/2015/327 Implications of Prostate Specific Antigen and its Molecular Derivatives in the Management of Carcinoma Prostate Sujan Narayan Agrawal 1, Chanjiv Singh 2, Sanwal
