Xin Wang 1,2*, Leonid Zamdborg 3, Hong Ye 3, Inga S. Grills 3,4 and Di Yan 3,4
|
|
|
- Daniella Cross
- 5 years ago
- Views:
Transcription
1 Wang et al. BC Cancer (2018) 18:962 RESEARCH ARTICLE A matched-pair analysis of stereotactic body radiotherapy (SBRT) for oligometastatic lung tumors from colorectal cancer versus early stage nonsmall cell lung cancer Xin Wang 1,2*, Leonid Zamdborg 3, Hong Ye 3, Inga S. Grills 3,4 and Di Yan 3,4 Open Access Abstract Background: The use of stereotactic body radiotherapy (SBRT) for early-stage primary non-small cell lung cancer (NSCLC) reported excellent local control rates. But the optimal SBRT dose for oligometastatic lung tumors (OLTs) from colorectal cancer (CRC) has not yet been determined. This study aimed to evaluate whether SBRT to a dose of Gy in 4 5 fractions could result in similar local outcomes for OLTs from CRC as compared to early-stage NSCLC, and to examine potential dose-response relationships for OLTs from CRC. ethods: OLTs from CRC and primary NSCLCs treated with SBRT to Gy in 4 5 fractions at a single institution were evaluated, and a matched-pair analysis was performed. Local recurrence-free survival (LRFS) was estimated by the Kaplan-eier method. Univariate Cox regression was performed to identify significant predictors. Results: There were 72 lung lesions in 61 patients (24 OLTs from CRC in 15 patients and 48 NSCLCs in 46 patients) were analyzed with a median follow-up of 30 months. LRFS for OLTs from CRC was significantly worse than that of NSCLC when treated with Gy/4 5 fx(p = 0.006). The 1, 3 and 5-year LRFS of OLTs from CRC vs NSCLC were 80.6% vs. 100%, 68.6% vs. 97.2%, and 68.6% vs. 81.0%, respectively. On univariate analysis, OLTs from CRC treated with higher dose (BED 10 = 132 Gy) exhibited significantly better local recurrence-free survival than those treated to lower doses (BED Gy) (p = ). The 1 and 3-year LRFS rates for OLTs treated to a higher dose (BED 10 = 132 Gy) were 88.9% and 81.5%, vs 33.3%, and not achieved for lower doses (BED Gy). Conclusion: The LRFS of OLTs from CRC after SBRT of Gy/4 5 fx was significantly worse than that of primary NSCLC. Lower dose SBRT appeared to have inferior control for OLTs of CRC in this cohort. Further studies with larger sample sizes are needed. Keywords: Stereotactic ablative radiation therapy, Oligometastatic tumor, Lung metastasis, Colorectal carcinoma, Dose-response relationship * Correspondence: @qq.com Xin Wang and Leonid Zamdborg contributed equally to this work. 1 Department of Abdominal Oncology, Cancer Center, West China Hospital, Sichuan University, No. 37 of Wainan Guoxue Lane, Wuhou District, Chengdu , Sichuan Province, China 2 Department of Radiation Oncology, Cancer Center, West China Hospital, Sichuan University, Chengdu, China Full list of author information is available at the end of the article The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Wang et al. BC Cancer (2018) 18:962 Page 2 of 10 Background The term oligometastatic disease is used to describe a less-advanced state of metastatic disease, limited in the number and sites of metastases, and amenable to potentially curative local therapy [1, 2]. Local treatment may bring the disease under better control through a decrease of the tumor burden, with a consequent improvement in overall survival. Increasingly, local treatment of lung metastases has been accomplished via stereotactic body radiotherapy (SBRT)/stereotactic ablative radiation therapy (SABR) [3, 4]. SBRT/SABR has been rapidly adopted into clinical use in the last decade [5]. Studies that investigated the use of SBRT for early-stage primary non-small cell lung cancer (NSCLC) reported excellent local control rates, typically % at 3 years, with minimal acute or late toxicity [6 12]. Given these results for primary disease, and the possibility of long-term survival in some patients with oligometastases, there has also been increasing interest in using SBRT for the treatment of lung oligometastases [13 20]. Current literature likewise suggests control rates ranging from good to excellent for this application, typically % with various dose and fractionation schemes [14 23]. Worldwide, colorectal cancer (CRC) is the third-most common cancer in men, and the second-most common in women. It is also the second leading cause of cancer-related death for both sexes combined [24]. Unlike most other cancers, approximately 20% of patients with CRC have metastatic disease at the time of diagnosis, and an additional 20 30% of patients will develop metastases following initial curative resection of the primary tumor [25]. The lung is the second-most frequent site for all colorectal metastases. Nonetheless, cure is still possible for selected stage IV CRC patients, especially for those with oligometastatic liver and/or lung disease. It has been reported that patients with resectable colorectal lung oligometastases have an impressive 5-year overall survival rate of 24 56% following resection [26 30]. Given the encouraging results of SBRT for both metastatic and early stage primary lung tumors, this technique has been used as an effective alternative treatment modality for CRC patients with lung oligometastases, especially those who are not surgical candidates. While it has been reported that a biologically effective dose (BED) of greater than 100 Gy (assuming an α/β ratio of 10) was needed when performing SBRT for stage I primary NSCLC [31], the optimal dose for oligometastatic lung tumors (OLTs) from CRC has not yet been determined. Dose-fractionation schemes of Gy in 4 5 fractions are commonly used for treating stage I primary NSCLC, and result in high local control rates and low toxicities [32 35]. It remains to be seen, however, whether these dose-fractionation schemes can result in similar outcomes for OLTs from CRC. In order to answer this question, and to determine the dose-response relationship for OLTs from CRC, we performed a matched-pair analysis to compare the local recurrence-free survival (LRFS) rate of SBRT to a dose of Gy in 4 5 fractions for OLTs from CRC with that of early stage primary NSCLC. ethods Patient characteristics Records of patients in the William Beaumont Hospital with primary NSCLC treated with SBRT to a dose of Gy in 4 5 fractions on a prospective protocol, as well as those with OLTs from CRC treated with SBRT according to the same dose-fractionation schedules between November 2005 and June 2014 were evaluated. The inclusion criteria for CRC patients were as follows: primary tumor was colorectal adenocarcinoma, one to three biopsy-proven lung metastases 5 cm in size, medically inoperable or refusing surgery, and both the primary tumor and any extra-thoracic metastases con trolled. Patients with prior lung irradiation, lung surgery, and having chemotherapy, were all eligible. The inclusion criteria for patients receiving SBRT for primary NSCLC were: 1 3 stage I primary histologically-proven NSCLC, and 5 cm in size. All patients who were not treated with Gy in 4 5 fractions were excluded. This study was approved by the institutional review board of William Beaumont Hospital (HIC# ). SBRT technique The details of SBRT treatment planning and delivery have been described previously [33, 36]. Briefly, all patients were immobilized in a stereotactic body frame (Elekta Oncology, Norcross, Georgia, USA), Alpha Cradle (KGF Enterprises, Chesterfield, ichigan, USA), BodyFIX (Elekta Oncology) or a modified Alpha Cradle/ BodyFIX hybrid device. Free-breathing computed tomography (CT) and 4-dimensional CT (Philips Clinical System, adison, Wisconsin, USA) simulation were performed in all patients. After simulation, acquired CT images were transferred to the planning system (Pinnacle, Philips, ilpitas, California, USA). Pre-treatment PET scans, if available, were fused with the planning CT. The gross tumor volume (GTV) was defined using CT lung windows and fused PET imaging. The internal target volume (ITV) was composed of the union of the GTV contours on 10 4D phases of respiration. To construct the clinical target volume (CTV), a 3 5 mm margin was applied around the ITV. The planning target volume (PTV) was the CTV plus a 5 mm three-dimensional expansion. Adoseof48 60 Gy in 4 5 fractions was prescribed to the PTV, encompassing the 80% isodose volume (range 60 90%). The prescribed radiation dose must cover 95% of
3 Wang et al. BC Cancer (2018) 18:962 Page 3 of 10 the PTV. And 99% of the PTV must receive at least 90% of the prescribed radiation dose. In addition, any dose > 105% of the prescribed dose should not occur outside the PTV. The dose-fractionation schemes were prescribed by the physicians depending on the tumor volume, location, and dose constrains of normal tissues. These dose constrains have been published previously [33, 37]. SBRT plans consisted of 6 9 coplanar and non-coplanar beams with a limited number of couch angles. Intensity modulated radiation therapy was permitted in order to meet normal tissue constraints. Daily online cone-beam CT (CBCT) was performed for soft tissue target registration. Treatment was delivered every other day, with a minimum of 40 h and a maximum of 96 h between fractions. For patients who had multiple metastatic tumors, SBRT for every lesion was delivered sequentially. 4 mg of dexamethasone was administered orally before each fraction. Follow-up Patients on the prospective trial underwent CT and PET/CT imaging to assess tumor response at 6, 16, and 52 weeks following treatment. CT imaging was also performed at 26 weeks following treatment. After 1 year, patients had a chest CT performed every 6 months. Patients with CRC were followed with CT and PET/CT imaging according to a similar schedule, but PET/CT was performed at the physician s discretion. Local recurrences were documented either by CT progression consisting of tumor growth after initial shrinkage or after initial stable disease, evident by increase in glucose uptake within the PTV region on FDG-PET scan, or the combination of both, with biopsy confirmation whenever possible. Local recurrences were determined by the treating physician and confirmed with chart and imaging review. Toxicities were graded per the Common Terminology Criteria of Adverse Events Version 3.0 (CTCAE V3.0). Statistical analysis Tumors from the NSCLC and CRC patient cohorts were matched with a 1:2 ratio based on tumor size, tumor location and histology. Because OLTs from CRC typically had a smaller tumor size than NSCLC tumors, the matching criterion was defined as NSCLC tumor size less than or equal to the tumor size of the OLT plus 1 cm. The association of clinical, pathological, and treatment variables within the CRC and NSCLC groups with any given event were analyzed using Student s t test and Pearson s Chi-square/Fisher s exact test. We calculated local recurrence-free survival from the date of SBRT completion to the date of first recurrence or last contact date. For patients who did not have a recurrence but died, we calculated local recurrence-free survival from the date of SBRT completion to the date of death. Patients whodidnothavearecurrenceanddidnotdiewere censored at the last follow-up date. Survival was estimated using the Kaplan-eier method, and compared using the log-rank test. Patient characteristics associated with local recurrence-free survival were identified using univariate Cox regression. All statistical tests were two-sided. A p value of less than or equal to 0.05 was considered to be statistically significant. Statistical analyses were conducted with SPSS version 20 (IB, Somers, New York, USA). Results Tumor properties A total of 25 OLTs from CRC and 166 primary NSCLCs were retrieved from the database and met inclusion criteria to undergo matching. A total of 72 lung tumors in 61 patients were matched (Table 1). The number of lung tumors treated per patient was one to three with CRC and one to two with NSCLC. edian tumor size of OLTs from CRC was 1 cm ( cm), and was 1.55 cm ( cm) for NSCLC. All patients with NSCLC were stage I. edian follow-up was 30 months (2 69 months) for patients with OLTs from CRC, and 30 months (1 107 months) for patients with NSCLC. There were 3 dose-fractionation schemes used in this study: 60 Gy in5fractions(bed 10 = 132 Gy), 48 Gy in 4 fractions (BED 10 = Gy), and 50 Gy in 5 fractions (BED 10 = 100 Gy). The NSCLC group had a higher median age, higher percentage of smokers, higher tumor baseline SUV max, and more tumors that were treated with 48 Gy in 4 fractions. The CRC group had more patients treated with 60 Gy in 5 fractions. Local recurrence-free survival At the time of analysis, 6 OLTs (25.0%) and 2 NSCLCs (4.2%) had recurred locally. OLT recurrence was confirmed histologically for one tumor, and was confirmed by PET scan for the remaining 5. One NSCLC recurrence was confirmed by cytology, and the other diagnosed by CT imaging. Local recurrence -free survival significantly favored stage I NSCLC (p = 0.006) (Fig. 1). The 1, 3 and 5-year LRFS rates for CRC OLTs and NSCLC were 80.6% (95% confidence interval [CI] %) vs 100% (95% CI %), 68.6% (95% CI %) vs 97.2% (95% CI %), and 68.6% (95% CI %) vs 81.0% (95% CI %), respectively. In univariate analysis (Table 2), the RT dose was significantly associated with local recurrence-free survival for OLTs (p = 0.02) but not for NSCLC (p = 0.15). The 1 and 3-year LRFS rates for OLTs treated to a higher dose (BED 10 = 132 Gy) were 88.9% (95%
4 Wang et al. BC Cancer (2018) 18:962 Page 4 of 10 Table 1 Patient characteristics Characteristics OLTs from CRC Early stage NSCLC p No. lesions No. patients Age (years) edian Range Gender ale Female 5 28 Smoker Smoker 9 41 Non-smoker 6 5 Number of lesions per patient lesion lesions lesions 3 0 Location 1 Central 2 4 Peripheral Tumor size (cm) < edian Range Pathology Adenocarcinoma Dose < Gy/5 fx Gy/4 fx Gy/5 fx 18 9 Baseline SUV max < edian Range KRAS-mutation status Wild 10 utation 11 Unknown 3 CI %) and 81.5% (95% CI %), respectively. The 1-year LRFS rate for OLTs treated with lower doses (BED 10 = 100 Gy or Gy) was 33.3% (95% CI %), and none achieved 3-year LRFS. Tumor size, baseline SUV max, lesion location, and patient age were not significantly associated with local recurrence-free survival for either OLTs or NSCLCs (Table 2). In OLTs, KRAS mutation status likewise did not have a significant impact on local recurrence-free survival. No multivariate analysis was performed. Discussion There has recently been growing interest in the use of SBRT for OLTs from CRC. An increasing number of studies have demonstrated that LRFS rates following SBRT differ between OLTs from CRC and primary NSCLCs for a given does-fractionation scheme [18, 38 40]. However, the optimal dose-fractionation schemes for OLTs from CRC remain unclear. In many cases, the same dose-fractionation schemes typically used for early-stage NSCLC (48 60 Gy in 4 5 fractions), are also used for OLTs [37 44]. We thus conducted this
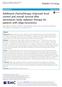
5 Wang et al. BC Cancer (2018) 18:962 Page 5 of 10 Fig. 1 Local recurrence-free survival curve for oligometastatic lung tumors from colorectal cancer and primary NSCLC retrospective matched-pair comparison of OLTs from CRC and stage I NSCLCs treated with SBRT to a dose of Gy in 4 5 fractions to better characterize LRFS of OLTs treated with these common dose-fractionation schemes. All patients with stage I NSCLCs were enrolled on a prospective trial, while all patients with CRC were identified from retrospective review of records. Our results demonstrated that LRFS for OLTs from CRC treated with SBRT to a dose of Gy in 4 5 fractions was significantly worse than that of early-stage NSCLC, despite the NSCLC group having a higher percentage of patients that were treated to a lower biologically-effective dose. On univariate analysis, RT dose (BED 10 ) was significantly associated with LRFS for OLTs from CRC (p = 0.02). A higher dose (60 Gy in 5 fractions, BED 10 = 132 Gy) resulted in significantly better LRFS of OLTs; however, a BED Gy appeared insufficient for durable LRFS of OLTs. Table 2 Univariate analysis: local control survival for OLTs from CRC and early stage NSCLC Factors CRC NSCLC p 95% CI p 95% CI Age Location Tumor size RT dose (BED 10 ) Baseline SUV max KRAS-mutation status Our study was the first matched-pair analysis to compare the outcome of SBRT to a dose of Gy in 4 5 fractions for OLTs from CRC and early stage NSCLCs. Recent reports of SBRT for metastatic lung tumors have included limited numbers of CRC patients, ranging from 7to65[27, 37, 39, 40, 43, 45 51]. These studies suggested that local control of metastatic lung tumors from CRC using SBRT was decreased compared to that of primary NSCLCs or metastatic lung tumors from other primary tumors. Kim et al. delivered SBRT to a dose of Gy in 3 fractions for 13 metastatic lung tumors from CRC, and reported a three-year local control rate of 52.7% [27]. Takeda et al. [39] analyzed the local control of OLTs resulting from various primary tumors including CRC, and compared them with the local control of primary lung cancer after SBRT to a BED 10 of 100 Gy in a non-matched fashion. The local control rate in metastatic tumors was significantly worse than that in primary lung cancer (82% vs. 93% at 2 years, p < 0.001), and the local control rate of metastases from CRC was significantly worse than that of metastatic tumors of other origins (72% vs. 94% at 2 years, p < 0.05). Oh et al. [45] delivered Gy in 4 5 fractions to OLTs, and OLTs from the colorectum and liver exhibited a lower local control rate than those from other organs of origin (85.7%, 77.8%, and 100%, p = 0.04). Additionally, it was reported in several retrospective studies that recurrent lung tumors treated by SBRT tended to be OLTs from CRC [37, 52, 53]. Baschnagel et al. reported that the 2 year actuarial local failure rate for OLTs from CRC was 20%, versus 0% for all other cases (p = 0.001) treated
6 Wang et al. BC Cancer (2018) 18:962 Page 6 of 10 with SBRT (48 60 Gy in 4 5 fractions) [37]. In another retrospective study, Hamamoto et al. [38] delivered 48 Gy in 4 fractions to both stage I primary lung cancer and metastatic lung tumors, and demonstrated 2-year local control rates of 88% and 25%, respectively. They explained that the large proportion of colorectal metastases in their study (7 out of 12, 67%) may be the reason for the poor local control rate for metastatic tumors. They also concluded that local control rates following 48 Gy in 4 fractions were significantly worse in metastatic lung tumors when compared with stage I primary lung cancer, and suggested increasing the SBRT dose for metastatic lung tumors. Several retrospective studies published recently also demonstrated colorectal cancer lung metastases are associated with a higher hazard of local failure and require higher radiation doses [42, 43, 48, 49, 54, 55]. The results of these studies are summarized in Table 3. In our study, the results of local control was similar with the data from the literature. The 1, 3 and 5-year LRFS rates for CRC OLTs in our study were 80.6%, 68. 6% and 68.6%, respectively, which were significant worse than that of NSCLC (100%, 97.2% and 81%, respectively).a number of studies analyzed the dose-response relationship of SBRT for primary lung cancer. It was previously reported that a prescription dose (BED 10 ) of 105 Gy or more was correlated with a higher rate of local control for NSCLC (96% vs 85%, p < 0.001) [34, 35]. It was also reported that tumor size was associated with the rate of local recurrence [35]. The two-year local recurrence rate of NSCLC with tumors of maximum dimension < 2.0 cm was 2% vs 8% for cm vs 10% for cm (p = 0.23) [35]. In our study, all cases of NSCLC were stage I, and our results demonstrated that there were no significant differences in the local control rates between primary NSCLC tumors treated to a higher dose (BED 10 = 132 Gy) and those treated to a lower dose (BED Gy). Unlike primary NSCLC, however, the dose-response relationship for OLTs from CRC has been unclear. Norihisa et al. [39] delivered SBRT to 43 OLTs in 34 patients, of which 9 patients had a colorectal primary. They escalated the RT dose to 60 Gy in 5 fractions after they experienced several local failures with a dose of 48 Gy in 4 fractions. Following this, no local progression was observed in tumors irradiated to a dose of 60 Gy. Rusthoven et al. conducted a phase I/II trial of SBRT for lung metastases which included 9 patients with colorectal primaries [14]. The dose schemes used in this study were Gy in 3 fractions (BED 10 ranged from Gy to 180 Gy). Local progression was observed in only one lesion, a metastasis from a sarcoma primary. All colorectal metastases achieved durable local control for the duration of the study. Yamamoto et al. reported that BED 10 (BED 10 > 105 Gy vs. BED Gy) was a significant independent predictor for local control of primary and metastatic lung tumors [56]. In our study, RT dose (BED 10 = 132 Gy vs. BED 10 = 100 Gy/105.6 Gy) was the only statistically significant factor influencing local control rate for OLTs from CRC on multivariate analysis (p = 0.028). This suggests that BED Gy is not sufficient for durable local control for OLTs from CRC. Thibault et al. delivered SBRT of 48-60Gy in 4 5 fractions to patients with primary NSCLC and metastatic lung tumors [44]. And it was concluded that covering more of the PTV with the prescription dose was also predictive of higher local control. The underlying reasons for worse outcomes in OLTs from CRC are unclear. However, based on studies of liver tumors, one may conjecture that metastases from CRC contain larger proportions of hypoxic cells than other tumor types [57], and this hypoxia leads to a decrease in radiosensitivity. The correlation between KRAS mutation and radiosensitivity for patients with lung metastasis is still unknown. In our study, KRAS mutation status likewise did not have a significant impact on local recurrence-free survival for OLTs from CRC (p = 0.23, 95%CI: ). In a retrospective study, It was reported that KRAS mutation had the correlation with 1-y metastasis-free survival (0% vs. 37.5%; P =.04), but not for local control [42]. The role of systematic treatment is unclear for lung OLTs. According to the literature, the most important prognostic factors for lung metastasis SBRT was tumor origin [46, 55, 56]. By ablating OLTs, oncologists might delay the need to start or change systemic treatment [55]. It was reported that the cumulative incidence of change of systemic treatment for patients with single lung metastasis and oligometastases at 12 months were 4.17% and 16.54%, respectively, which were much lower than that of patients with dominant area of progression (50.00%) [55]. It was also demonstrated that both dose escalation and adjuvant chemotherapy might improve local control of SBRT for lung metastasis form CRC [58]. In our study, systematic treatment was not analyzed for the reason of data access. This is one of the limitations of this study. But the efficacies of systematic treatment need further clarification. The other limitations of this study should also be addressed. This study, though a matched-pair analysis larger than previous series, is nonetheless a single-institution retrospective analysis of a small group of patients. In this study, the comparison were made only between two RT dose schemes, BED 10 = 132Gy and BED 10 = Gy. Therefore, we could only draw the conclusion based on these two prescription dose. Whether there was an optimal dose between BED Gy and 132Gy was still unclear. The most optimal
7 Wang et al. BC Cancer (2018) 18:962 Page 7 of 10 Table 3 Selected series of SBRT for primary NSCLC and/or metastatic lung tumors Authors P/ No. of patients Dose/fractions LC PFS/OS All P From CRC P/ CRC P/ CRC Oh et al [45] Gy/5f, 60Gy/5f, 60Gy/ 4f 3-y: 94.5% 3-y: 80.0% 2-y DFS: 59.7% Binkley et al [40] Agolli et al [42] Thibault et al [44] Qiu et al [43] Kinj et al [49] Oskan et al [50] Pasqualetti et al [54] Jung et al [48] Hamamoto et al [46] Baschnagel et al [37] Navarria et al [52] Singh et al [53] Kim et al [27] Hof et al [41] Gy/1f, 50Gy/4f 44 23Gy/1f 30Gy/1f 45Gy/3f P/ 1-y: 91.3%; 2-y: 83.8% Gy/4-5f 2-y: 96% (P) 1-y: 74.5%; 2-y: 57.8% 1-y: 68.8%; 2-y: 60.2% 3-y: 54.2% 2-y: 76% 2-y OS: 74.7%, 2-y OS: 67.7%; 3-y OS: 50.8% 2-y PFS: 20.3% 65 50Gy/5-10f 2-y: 30% 2-y OS 42.8% 2-y PFS 23.5% 53 60Gy/3f 1-y: 79.8% 2-y: 78.2% 1-y OS: 83.8%; 2-y OS: 69.3% Gy/1-8f 1-y OS: 84%; 2-y OS: 73% 5-y OS: 39% Gy/1f 27-42Gy/3f Gy/3-4f 1-y: 88.7% 3-y: 70.6% P/ Gy/4-5f 2-y: 87% (P); 2-y: 50% () Gy/4-5f 1-y: 97%, 2-y: 92%, 3-y: 85% Gy/4f, 60Gy/8f, 60Gy/3f 1-y: 95%, 3-y: 89% Gy/5f 1-y: 95%, 2-y: 88%, 3-y: 80% Gy/3f 1-y; 76.9%, 2-y: 52.7%, 3-y: 52.7% Gy/1f 1-y: 88.6%, 2-y: 73.7%, 3-y: 63.1% 2-y: 80% 1-y OS:83%, 2-y OS: 76%, 3-y OS-: 63% Recurrence in 3 of 29 patients (locally and distance) All 5 patients with local recurrences had CRC 3-y: 0% 1-y OS: 84.1%, 3-y OS: 73% 1-y OS: 78.4%, 2-y OS: 65.1%, 3-y OS: 47.8% edian PFS:13.4 m 3-y OS: 64% 3-y PFS: 24% 1-y OS: 100%, 2-y OS; 75.5%, 3-y OS: 64.7%
8 Wang et al. BC Cancer (2018) 18:962 Page 8 of 10 Table 3 Selected series of SBRT for primary NSCLC and/or metastatic lung tumors (Continued) Authors P/ No. of patients Dose/fractions LC PFS/OS All P From CRC P/ CRC P/ CRC Nagata et al [47] Takeda et al [39] Okunieff et al [17] Yamamoto et al [56] Helou et al [55] P/ P/ Gy/4f 1-y: 100% (P); 2-y: 100% (P); Gy/5f 1-y: 97% (P), 1-y: 86% () 2-y: 93% (P), 2-y: 82% () 2 mtastases from colon relapsed at 6, 7 m 1-y: 80%, 2-y: 72% Gy/10f 1-y: 83% Had an unexpected number of local failures. P/ P: primary NSCLC, : metastatic lung tumor Gy/3f, 48Gy/4f, 60Gy/ 8f, 60Gy/15f Gy/4-5f 3-y: 78%(P), 5-y: 72% (P) 3-y: 26%, 5-y: 26% 3-y OS: 60.9%, 5-y OS: 38.1% dose schemes need further investigation. And all the results would need to be confirmed in a larger study, preferably a prospective trial. Conclusions In this matched-pair study, the LRFS for OLTs from CRC after SBRT of Gy in 4 5 fractions was significantly worse than that of stage I NSCLC. A higher dose (60 Gy in 5 fractions, BED 10 = 132Gy) resulted in a significantly improved LRFS for OLTs from CRC compared with a lower dose (BED Gy). Lower dose SBRT appeared to have inferior control for OLTs from CRC in this cohort. Further studies with larger sample sizes are needed, however dose and anticipated local control rates should be considered with discussing SBRT as an option for CRC oligometastases. Abbreviations BED: Biologically effective dose; CBCT: Cone-beam CT; CI: Confidence interval; CRC: Colorectal cancer; CT: Computed tomography; CTCAE: Common Terminology Criteria of Adverse Events; CTV: Clinical target volume; GTV: Gross tumor volume; ITV: Internal target volume; LRFS: Local recurrencefree survival; NSCLC: Non-small cell lung cancer; OLTs: Oligometastatic lung tumors; PTV: Planning target volume; SABR: Stereotactic ablative radiation therapy; SBRT: Stereotactic body radiotherapy Funding This research was partially supported by grants from Elekta Corollaborative Lung Research Group. The funding agencies were not involved in the study design, data collection, analysis, or interpretation and decision to write the manuscript. Availability of data and materials The data is available upon request. Hong Ye and Xin Wang should be contacted if someone wants to request the data. Authors contributions XW and DY participated in the design of the study. XW and LZ wrote the manuscript. IG and DY supervised the study and assisted in data acquisition and interpretation. HY assisted with analysis of the data. All authors revised the manuscript and approved its content. Ethics approval and consent to participate This study was approved by the institutional review board of William Beaumont Hospital (HIC# ). All study participants provided written informed consent after careful explanation by their treating investigators. Consent for publication Not applicable Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Abdominal Oncology, Cancer Center, West China Hospital, Sichuan University, No. 37 of Wainan Guoxue Lane, Wuhou District, Chengdu , Sichuan Province, China. 2 Department of Radiation Oncology, Cancer Center, West China Hospital, Sichuan University, Chengdu, China. 3 Department of Radiation Oncology, William Beaumont Hospital, Royal Oak, ichigan, USA. 4 Department of Radiation Oncology, Oakland University William Beaumont School of edicine, Rochester, ichigan, USA. Received: 28 January 2018 Accepted: 26 September 2018 References 1. Hellman S, Weichselbaum RR. Oligometastases. J Clin Oncol. 1995;13: Weichselbaum RR, Hellman S. Oligometastases revisited. Nat Rev Clin Oncol. 2011;8: Lo SS, Fakiris AJ, Teh BS, et al. Stereotactic body radiation therapy for oligometastases. Expert Rev Anticancer Ther. 2009;9:
9 Wang et al. BC Cancer (2018) 18:962 Page 9 of Pastorino U, Buyse, Friedel G, et al. Long-term results of lung metastasectomy: prognostic analyses based on 5206 cases. J Thorac Cardiovasc Surg. 1997;113: Pan H, Simpson DR, ell LK, et al. A survey of stereotactic body radiotherapy use in the United States. Cancer. 2011;117: Fakiris AJ, cgarry RC, Yiannoutsos CT, et al. Stereotactic body radiation therapy for early-stage non-small-cell lung carcinoma: four-year results of a prospective phase II study. Int J Radiat Oncol Biol Phys. 2009;75: Timmerman R, Paulus R, Galvin J, et al. Stereotactic body radiation therapy for inoperable early stage lung cancer. JAA. 2010;303: Shibamoto Y, Hashizume C, Baba F, et al. Stereotactic body radiotherapy using a radiobiology-based regimen for stage I nonsmall cell lung cancer: a multicenter study. Cancer. 2012;118: Baumann P, Nyman J, Lax I, et al. Factors important for efficacy of stereotactic body radiotherapy of medically inoperable stage I lung cancer. A retrospective analysis of patients treated in the Nordic countries. Acta Oncol. 2006;45: Baumann P, Nyman J, Hoyer, et al. Outcome in a prospective phase II trial of medically inoperable stage I non-small-cell lung cancer patients treated with stereotactic body radiotherapy. J Clin Oncol. 2009;27: Lagerwaard FJ, Haasbeek CJ, Smit EF, et al. Outcomes of risk-adapted fractionated stereotactic radiotherapy for stage I non-small-cell lung cancer. Int J Radiat Oncol Biol Phys. 2008;70: Andratschke N, Zimmermann F, Boehm E, et al. Stereotactic radiotherapy of histologically proven inoperable stage I non-small cell lung cancer: patterns of failure. Radiother Oncol. 2011;101: Goldsmith C, Gaya A. Stereotactic ablative body radiotherapy (SABR) for primary and secondary lung tumours. Cancer Imaging. 2012;12: Rusthoven KE, Kavanagh BD, Burri SH, et al. ulti-institutional phase I/II trial of stereotactic body radiation therapy for lung metastases. J Clin Oncol. 2009;27: Yoon S, Choi EK, Lee SW, et al. Clinical results of stereotactic body frame based fractionated radiation therapy for primary or metastatic thoracic tumors. Acta Oncol. 2006;45: Brown WT, Wu X, Fowler JF, et al. Lung metastases treated by CyberKnife image-guided robotic stereotactic radiosurgery at 41 months. South ed J. 2008;101: Okunieff P, Petersen AL, Philip A, et al. Stereotactic body radiation therapy (SBRT) for lung metastases. Acta Oncol. 2006;45: Norihisa Y, Nagata Y, Takayama K, et al. Stereotactic body radiotherapy for oligometastatic lung tumors. Int J Radiat Oncol Biol Phys. 2008;72: Blackmon SH, Shah N, Roth JA, et al. Resection of pulmonary and extrapulmonary sarcomatous metastases is associated with long-term survival. Ann Thorac Surg. 2009;88: discussion Dhakal S, Corbin KS, ilano T, et al. Stereotactic body radiotherapy for pulmonary metastases from soft-tissue sarcomas: excellent local lesion control and improved patient survival. Int J Radiat Oncol Biol Phys. 2012;82: Siva S, Kron T, Bressel, et al. A randomised phase II trial of stereotactic ablative fractionated radiotherapy versus radiosurgery for Oligometastatic neoplasia to the lung (TROG SAFRON II). BC Cancer. 2016;16: Treasure T. Surgery and ablative techniques for lung metastases in the pulmonary etastasectomy in colorectal Cancer (PuliCC) trial: is there equivalence? J Thorac Dis. 2016;8:S Rieber J, Streblow J, Uhlmann L, et al. Stereotactic body radiotherapy (SBRT) for medically inoperable lung metastases a pooled analysis of the German working group stereotactic radiotherapy. Lung Cancer. 2016;97: Jemal A, Siegel R, Xu J, Ward E. Cancer statistics, CA Cancer J Clin. 2010;60: Eadens J, Grothey A. Curable metastatic colorectal cancer. Curr Oncol Rep. 2011;13: ccormack P, Burt E, Bains S, et al. Lung resection for colorectal metastases. 10-year results. Arch Surg. 1992;127: Kim S, Yoo SY, Cho CK, et al. Stereotactic body radiation therapy using three fractions for isolated lung recurrence from colorectal cancer. Oncology. 2009;76: Sakamoto T, Tsubota N, Iwanaga K, et al. Pulmonary resection for metastases from colorectal cancer. Chest. 2001;119: Watanabe I, Arai T, Ono, et al. Prognostic factors in resection of pulmonary metastasis from colorectal cancer. Br J Surg. 2003;90: Pfannschmidt J, Dienemann H, Hoffmann H. Surgical resection of pulmonary metastases from colorectal cancer: a systematic review of published series. Ann Thorac Surg. 2007;84: Onishi H, Araki T, Shirato H, et al. Stereotactic hypofractionated high-dose irradiation for stage I nonsmall cell lung carcinoma: clinical outcomes in 245 subjects in a Japanese multiinstitutional study. Cancer. 2004;101: Nagata Y, Takayama K, atsuo Y, et al. Clinical outcomes of a phase I/II study of 48 Gy of stereotactic body radiotherapy in 4 fractions for primary lung cancer using a stereotactic body frame. Int J Radiat Oncol Biol Phys. 2005;63: Grills IS, angona VS, Welsh R, et al. Outcomes after stereotactic lung radiotherapy or wedge resection for stage I non-small-cell lung cancer. J Clin Oncol. 2010;28: Grills IS, Hope AJ, Guckenberger, et al. A collaborative analysis of stereotactic lung radiotherapy outcomes for early-stage non-small-cell lung cancer using daily online cone-beam computed tomography image-guided radiotherapy. J Thorac Oncol. 2012;7: Kestin L, Grills I, Guckenberger, et al. Dose-response relationship with clinical outcome for lung stereotactic body radiotherapy (SBRT) delivered via online image guidance. Radiother Oncol. 2014;110: Grills IS, Hugo G, Kestin LL, et al. Image-guided radiotherapy via daily online cone-beam CT substantially reduces margin requirements for stereotactic lung radiotherapy. Int J Radiat Oncol Biol Phys. 2008;70: Baschnagel A, angona VS, Robertson J, et al. Lung metastases treated with image-guided stereotactic body radiation therapy. Clin Oncol (R Coll Radiol). 2013;25: Hamamoto Y, Kataoka, Yamashita, et al. Local control of metastatic lung tumors treated with SBRT of 48 Gy in four fractions: in comparison with primary lung cancer. Jpn J Clin Oncol. 2010;40: Takeda A, Kunieda E, Ohashi T, et al. Stereotactic body radiotherapy (SBRT) for oligometastatic lung tumors from colorectal cancer and other primary cancers in comparison with primary lung cancer. Radiother Oncol. 2011;101: Binkley S, Trakul N, Jacobs LR, et al. Colorectal histology is associated with an increased risk of local failure in lung metastases treated with stereotactic ablative radiation therapy. Int J Radiat Oncol Biol Phys. 2015;92: Hof H, Hoess A, Oetzel D, et al. Stereotactic single-dose radiotherapy of lung metastases. Strahlenther Onkol. 2007;183: Agolli L, Bracci S, Nicosia L, et al. Lung metastases treated with stereotactic ablative radiation therapy (SABR) in oligometastatic colorectal cancer patients: outcomes and prognostic factors after long-term follow up. Clin Colorectal Cancer. 2016;16: Qiu H, Katz AW, Chowdhry AK, et al. Stereotactic body radiotherapy for lung metastases from colorectal cancer: prognostic factors for disease control and survival. Am J Clin Oncol. 2015;93:E Thibault I, Poon I, Yeung L, et al. Predictive factors for local control in primary and metastatic lung tumours after four to five fraction stereotactic ablative body radiotherapy: a single institution's comprehensive experience. Clin Oncol (R Coll Radiol). 2014;26: Oh D, Ahn YC, Seo J, et al. Potentially curative stereotactic body radiation therapy (SBRT) for single or oligometastasis to the lung. Acta Oncol. 2012; 51: Hamamoto Y, Kataoka, Yamashita, et al. Factors affecting the local control of stereotactic body radiotherapy for lung tumors including primary lung cancer and metastatic lung tumors. Jpn J Radiol. 2012;30: Nagata Y, Negoro Y, Aoki T, et al. Clinical outcomes of 3D conformal hypofractionated single high-dose radiotherapy for one or two lung tumors using a stereotactic body frame. Int J Radiat Oncol Biol Phys. 2002;52: Jung J, Si YS, Kim JH, et al. Clinical efficacy of stereotactic ablative radiotherapy for lung metastases arising from colorectal cancer. Radiat Oncol. 2015;10: Kinj R, Bondiau PY, François E, et al. Radiosensitivity of Colon and Rectal lung Oligometastasis treated with stereotactic ablative radiotherapy. Clin Colorectal Cancer. 2017;16:e Oskan F, Dzierma Y, Wagenpfeil S, et al. Retrospective analysis of stereotactic ablative radiotherapy (SABR) for metastatic lung lesions (LLs) in comparison with a contemporaneous cohort of primary lung lesions (PLLs). J Thorac Dis. 2017;9: Siva S, Kirby K, Caine H, et al. Comparison of single-fraction and multifraction stereotactic radiotherapy for patients with 18F-fluorodeoxyglucose
10 Wang et al. BC Cancer (2018) 18:962 Page 10 of 10 positron emission tomography-staged pulmonary Oligometastases. Clin Oncol (R Coll Radiol). 2015;27: Navarria P, Ascolese A, Tomatis S, et al. Stereotactic body radiotherapy (sbrt) in lung oligometastatic patients: role of local treatments. Radiat Oncol. 2014;9: Singh D, Chen Y, Hare Z, et al. Local control rates with five-fraction stereotactic body radiotherapy for oligometastatic cancer to the lung. J Thorac Dis. 2014;6: Pasqualetti F, ontrone S. Vivaldi C al e Stereotactic Body Radiotherapy in Patients with Lung Oligometastases from Colorectal Cancer. Anticancer Res. 2017;37: Helou J, Thibault I, Poon I, et al. Stereotactic ablative radiation therapy for pulmonary metastases: istology, dose, and indication matter. Int J Radiat Oncol Biol Phys. 2017;98: Yamamoto T, Jingu K, Shirata Y, et al. Outcomes after stereotactic body radiotherapy for lung tumors, with emphasis on comparison of primary lung cancer and metastatic lung tumors. BC Cancer. 2014;14: van Laarhoven HW, Kaanders JH, Lok J, et al. Hypoxia in relation to vasculature and proliferation in liver metastases in patients with colorectal cancer. Int J Radiat Oncol Biol Phys. 2006;64: Jingu K, atsuo Y, Onishi H, et al. Dose escalation improves outcome in stereotactic body radiotherapy for pulmonary Oligometastases from colorectal Cancer. Anticancer Res. 2017;37:
Clinical Study Clinical Outcomes of Stereotactic Body Radiotherapy for Patients with Lung Tumors in the State of Oligo-Recurrence
 Pulmonary Medicine Volume 2012, Article ID 369820, 5 pages doi:10.1155/2012/369820 Clinical Study Clinical Outcomes of Stereotactic Body Radiotherapy for Patients with Lung Tumors in the State of Oligo-Recurrence
Pulmonary Medicine Volume 2012, Article ID 369820, 5 pages doi:10.1155/2012/369820 Clinical Study Clinical Outcomes of Stereotactic Body Radiotherapy for Patients with Lung Tumors in the State of Oligo-Recurrence
Clinical outcomes of patients with malignant lung lesions treated with stereotactic body radiation therapy (SBRT) in five fractions
 J Radiat Oncol (2012) 1:57 63 DOI 10.1007/s13566-012-0008-0 ORIGINAL RESEARCH Clinical outcomes of patients with malignant lung lesions treated with stereotactic body radiation therapy (SBRT) in five fractions
J Radiat Oncol (2012) 1:57 63 DOI 10.1007/s13566-012-0008-0 ORIGINAL RESEARCH Clinical outcomes of patients with malignant lung lesions treated with stereotactic body radiation therapy (SBRT) in five fractions
Radiation Therapy for Liver Malignancies
 Outline Radiation Therapy for Liver Malignancies Albert J. Chang, M.D., Ph.D. Department of Radiation Oncology, UCSF March 23, 2014 Rationale for developing liver directed therapies Liver directed therapies
Outline Radiation Therapy for Liver Malignancies Albert J. Chang, M.D., Ph.D. Department of Radiation Oncology, UCSF March 23, 2014 Rationale for developing liver directed therapies Liver directed therapies
20. Background. Oligometastases. Oligometastases: bone (including spine) and lymph nodes
 125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
SBRT & WEDGE RESECTION ARE EQUIVALENT THERAPIES FOR EARLY STAGE LUNG CANCER AND OLIGOMETASTATIC DISEASE
 & WEDGE RESECTION ARE EQUIVALENT THERAPIES FOR EARLY STAGE LUNG CANCER AND OLIGOMETASTATIC DISEASE David Rice AATS/STS GENERAL THORACIC SURGERY SYMPOSIUM, APRIL 26, 2015 Disclosure Olympus America, Inc.,
& WEDGE RESECTION ARE EQUIVALENT THERAPIES FOR EARLY STAGE LUNG CANCER AND OLIGOMETASTATIC DISEASE David Rice AATS/STS GENERAL THORACIC SURGERY SYMPOSIUM, APRIL 26, 2015 Disclosure Olympus America, Inc.,
Flattening Filter Free beam
 Dose rate effect in external radiotherapy: biology and clinic Marta Scorsetti, M.D. Radiotherapy and Radiosurgery Dep., Istituto Clinico Humanitas, Milan, Italy Brescia October 8th/9th, 2015 Flattening
Dose rate effect in external radiotherapy: biology and clinic Marta Scorsetti, M.D. Radiotherapy and Radiosurgery Dep., Istituto Clinico Humanitas, Milan, Italy Brescia October 8th/9th, 2015 Flattening
Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer
 Original Article PROGRESS in MEDICAL PHYSICS Vol. 26, No. 4, December, 2015 http://dx.doi.org/10.14316/pmp.2015.26.4.229 Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer Ji
Original Article PROGRESS in MEDICAL PHYSICS Vol. 26, No. 4, December, 2015 http://dx.doi.org/10.14316/pmp.2015.26.4.229 Response Evaluation after Stereotactic Ablative Radiotherapy for Lung Cancer Ji
4.x Oligometastases: evidence for dose-fractionation
 4.x Oligometastases: evidence for dose-fractionation Background 4.x.1. The oligometastatic state can be defined as 1-3 isolated metastatic sites, typically occurring more than six months after successful
4.x Oligometastases: evidence for dose-fractionation Background 4.x.1. The oligometastatic state can be defined as 1-3 isolated metastatic sites, typically occurring more than six months after successful
Stereotactic radiotherapy
 Stereotactic radiotherapy Influence of patient positioning and fixation on treatment planning - clinical results Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH
Stereotactic radiotherapy Influence of patient positioning and fixation on treatment planning - clinical results Frank Zimmermann Institut für Radioonkologie Universitätsspital Basel Petersgraben 4 CH
Stereotactic body radiation therapy versus surgery for patients with stage I non-small cell lung cancer
 Review Article Page 1 of 9 Stereotactic body radiation therapy versus surgery for patients with stage I non-small cell lung cancer Tomoki Kimura Department of Radiation Oncology, Hiroshima University Hospital,
Review Article Page 1 of 9 Stereotactic body radiation therapy versus surgery for patients with stage I non-small cell lung cancer Tomoki Kimura Department of Radiation Oncology, Hiroshima University Hospital,
Results of Stereotactic radiotherapy for Stage I and II NSCLC Is There a Need for Image Guidance?
 Results of Stereotactic radiotherapy for Stage I and II NSCLC Is There a Need for Image Guidance? Frank Zimmermann Institute of Radiation Oncolgy University Clinic Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch
Results of Stereotactic radiotherapy for Stage I and II NSCLC Is There a Need for Image Guidance? Frank Zimmermann Institute of Radiation Oncolgy University Clinic Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch
SBRT in early stage NSCLC
 SBRT in early stage NSCLC Optimal technique and tumor dose Frank Zimmermann Clinic of Radiotherapy and Radiation Oncology University Hospital Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch Techniques
SBRT in early stage NSCLC Optimal technique and tumor dose Frank Zimmermann Clinic of Radiotherapy and Radiation Oncology University Hospital Basel Petersgraben 4 CH 4031 Basel radioonkologiebasel.ch Techniques
SABR. Outline. Stereotactic Radiosurgery. Stereotactic Radiosurgery. Stereotactic Ablative Radiotherapy
 CAGPO Conference October 25, 2014 Outline Stereotactic Radiation for Lung Cancer and Oligometastatic Disease What Every GPO should know Dr. David Palma, MD, MSc, PhD Radiation Oncologist, London Health
CAGPO Conference October 25, 2014 Outline Stereotactic Radiation for Lung Cancer and Oligometastatic Disease What Every GPO should know Dr. David Palma, MD, MSc, PhD Radiation Oncologist, London Health
Treatment of oligometastases: Lung
 Treatment of oligometastases: Lung Themadag Catharina ZH 30 March 2017 Max Dahele Radiation Oncologist Vumc, Amsterdam m.dahele@vumc.nl Do you all treat lung oligometastases? What is your definition of
Treatment of oligometastases: Lung Themadag Catharina ZH 30 March 2017 Max Dahele Radiation Oncologist Vumc, Amsterdam m.dahele@vumc.nl Do you all treat lung oligometastases? What is your definition of
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
Required target margins for image-guided lung SBRT: Assessment of target position intrafraction and correction residuals
 Practical Radiation Oncology (2013) 3, 67 73 www.practicalradonc.org Original Report Required target margins for image-guided lung SBRT: Assessment of target position intrafraction and correction residuals
Practical Radiation Oncology (2013) 3, 67 73 www.practicalradonc.org Original Report Required target margins for image-guided lung SBRT: Assessment of target position intrafraction and correction residuals
Lung stereotactic body radiotherapy (SBRT) delivers an
 Original Article Stereotactic Body Radiotherapy in Patients with Previous Pneumonectomy Safety and Efficacy Robert Thompson, MD,* Meredith Giuliani, MBBS,* Mei Ling Yap, MD,* Soha Atallah, MD,* Lisa W.
Original Article Stereotactic Body Radiotherapy in Patients with Previous Pneumonectomy Safety and Efficacy Robert Thompson, MD,* Meredith Giuliani, MBBS,* Mei Ling Yap, MD,* Soha Atallah, MD,* Lisa W.
Lung SBRT in a patient with poor pulmonary function
 Lung SBRT in a patient with poor pulmonary function CASE STUDY Delivered using Versa HD with High Dose Rate mode and Symmetry 4D image guidance Institution: Department of Oncology, Odense University Hospital
Lung SBRT in a patient with poor pulmonary function CASE STUDY Delivered using Versa HD with High Dose Rate mode and Symmetry 4D image guidance Institution: Department of Oncology, Odense University Hospital
Therapy of Non-Operable early stage NSCLC
 SBRT Stage I NSCLC Therapy of Non-Operable early stage NSCLC Dr. Adnan Al-Hebshi MD, FRCR(UK), FRCP(C), ABR King Faisal Specialist Hospital & Research Centre This is our territory Early Stages NSCLC Surgical
SBRT Stage I NSCLC Therapy of Non-Operable early stage NSCLC Dr. Adnan Al-Hebshi MD, FRCR(UK), FRCP(C), ABR King Faisal Specialist Hospital & Research Centre This is our territory Early Stages NSCLC Surgical
The role of Radiation Oncologist: Hi-tech treatments for liver metastases
 The role of Radiation Oncologist: Hi-tech treatments for liver metastases Icro Meattini, MD Radiotherapy-Oncology Unit AOU Careggi Hospital Florence University, Italy Liver Metastases - Background The
The role of Radiation Oncologist: Hi-tech treatments for liver metastases Icro Meattini, MD Radiotherapy-Oncology Unit AOU Careggi Hospital Florence University, Italy Liver Metastases - Background The
Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer
 Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
Radiotherapy What are our options and what is on the horizon. Dr Kevin So Specialist Radiation Oncologist Epworth Radiation Oncology
 Radiotherapy What are our options and what is on the horizon Dr Kevin So Specialist Radiation Oncologist Epworth Radiation Oncology Outline Advances in radiotherapy technique Oligo - disease Advancements
Radiotherapy What are our options and what is on the horizon Dr Kevin So Specialist Radiation Oncologist Epworth Radiation Oncology Outline Advances in radiotherapy technique Oligo - disease Advancements
Local control rates exceeding 90% have been reported using
 ORIGINAL ARTICLE Incidence and Risk Factors for Chest Wall Toxicity After Risk-Adapted Stereotactic Radiotherapy for Early-Stage Lung Cancer Eva M. Bongers, MD, Cornelis J. A. Haasbeek, MD, PhD, Frank
ORIGINAL ARTICLE Incidence and Risk Factors for Chest Wall Toxicity After Risk-Adapted Stereotactic Radiotherapy for Early-Stage Lung Cancer Eva M. Bongers, MD, Cornelis J. A. Haasbeek, MD, PhD, Frank
Stereotactic body radiotherapy (SBRT) has been increasingly
 original article Central versus Peripheral Tumor Location Influence on Survival, Local Control, and Toxicity Following Stereotactic Body Radiotherapy for Primary Non Small-Cell Lung Cancer Henry S. Park,
original article Central versus Peripheral Tumor Location Influence on Survival, Local Control, and Toxicity Following Stereotactic Body Radiotherapy for Primary Non Small-Cell Lung Cancer Henry S. Park,
Surgical treatment in non-small cell lung cancer with pulmonary oligometastasis
 He et al. World Journal of Surgical Oncology (2017) 15:36 DOI 10.1186/s12957-017-1105-8 RESEARCH Open Access Surgical treatment in non-small cell lung cancer with pulmonary oligometastasis Jinyuan He,
He et al. World Journal of Surgical Oncology (2017) 15:36 DOI 10.1186/s12957-017-1105-8 RESEARCH Open Access Surgical treatment in non-small cell lung cancer with pulmonary oligometastasis Jinyuan He,
Additional chemotherapy improved local control and overall survival after stereotactic body radiation therapy for patients with oligo-recurrence
 Nakamura et al. Radiation Oncology (2018) 13:75 https://doi.org/10.1186/s13014-018-1031-0 RESEARCH Open Access Additional chemotherapy improved local control and overall survival after stereotactic body
Nakamura et al. Radiation Oncology (2018) 13:75 https://doi.org/10.1186/s13014-018-1031-0 RESEARCH Open Access Additional chemotherapy improved local control and overall survival after stereotactic body
Imaging follow-up after stereotactic ablative radiotherapy (SABR) for lung tumors
 J Radiat Oncol (2012) 1:11 16 DOI 10.1007/s13566-012-0014-2 REVIEW Imaging follow-up after stereotactic ablative radiotherapy (SABR) for lung tumors Simon S. Lo & Bin S. Teh & Nina A. Mayr & Stephen B.
J Radiat Oncol (2012) 1:11 16 DOI 10.1007/s13566-012-0014-2 REVIEW Imaging follow-up after stereotactic ablative radiotherapy (SABR) for lung tumors Simon S. Lo & Bin S. Teh & Nina A. Mayr & Stephen B.
Outline. WBRT field. Brain Metastases. Whole Brain RT Prophylactic WBRT Stereotactic radiosurgery (SRS) 1 fraction Stereotactic frame
 Radiation Therapy for Advanced NSC Lung Ca Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of California San Francisco
Radiation Therapy for Advanced NSC Lung Ca Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of California San Francisco
Stereotactic ablative radiotherapy in early NSCLC and metastases
 Stereotactic ablative radiotherapy in early NSCLC and metastases Scheduled: 0810-0830 hrs, 10 March 2012 Professor Suresh Senan Department of Radiation Oncology SABR in stage I NSCLC A major treatment
Stereotactic ablative radiotherapy in early NSCLC and metastases Scheduled: 0810-0830 hrs, 10 March 2012 Professor Suresh Senan Department of Radiation Oncology SABR in stage I NSCLC A major treatment
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部
 肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
Stereotactic Body Radiation Therapy for Primary Lung Cancers >3 Centimeters
 Original Article Stereotactic Body Radiation Therapy for Primary Lung Cancers >3 Centimeters John J. Cuaron, MD,* Ellen D. Yorke, PhD,* Amanda Foster, BA,* Meier Hsu, MS,* Zhigang Zhang, PhD,* Fan Liu,
Original Article Stereotactic Body Radiation Therapy for Primary Lung Cancers >3 Centimeters John J. Cuaron, MD,* Ellen D. Yorke, PhD,* Amanda Foster, BA,* Meier Hsu, MS,* Zhigang Zhang, PhD,* Fan Liu,
Tecniche Radioterapiche U. Ricardi
 Tecniche Radioterapiche U. Ricardi UNIVERSITA DEGLI STUDI DI TORINO Should we always rely on stage? T4N0M0 Stage IIIB T2N3M0 Early stage NSCLC The treatment of choice for early-stage NSCLC is anatomic
Tecniche Radioterapiche U. Ricardi UNIVERSITA DEGLI STUDI DI TORINO Should we always rely on stage? T4N0M0 Stage IIIB T2N3M0 Early stage NSCLC The treatment of choice for early-stage NSCLC is anatomic
Role of SBRT in the management of lung and liver metastases. Ronan TANGUY, M.D. Radiation Oncologist
 Role of SBRT in the management of lung and liver metastases Ronan TANGUY, M.D. Radiation Oncologist Oligometastatic RCC mrcc: Lung, Bone, Liver, Brain (Schlesinger-Raab, EJC2008) Targeted therapies Objective
Role of SBRT in the management of lung and liver metastases Ronan TANGUY, M.D. Radiation Oncologist Oligometastatic RCC mrcc: Lung, Bone, Liver, Brain (Schlesinger-Raab, EJC2008) Targeted therapies Objective
Rob Glynne-Jones Mount Vernon Cancer Centre
 ESMO Preceptorship Programme Colorectal Cancer Barcelona October 2017 Interventional radiology and stereotactic radiotherapy Rob Glynne-Jones Mount Vernon Cancer Centre My Disclosures: last 5 years Speaker:
ESMO Preceptorship Programme Colorectal Cancer Barcelona October 2017 Interventional radiology and stereotactic radiotherapy Rob Glynne-Jones Mount Vernon Cancer Centre My Disclosures: last 5 years Speaker:
Racial Disparities In The Treatment Of Non-Surgical Patients With Lung Cancer. S Annangi, M G Foreman, H P Ravipati, S Nutakki, E Flenaugh
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 18 Number 1 Racial Disparities In The Treatment Of Non-Surgical Patients With Lung Cancer S Annangi, M G Foreman, H P Ravipati, S Nutakki, E
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 18 Number 1 Racial Disparities In The Treatment Of Non-Surgical Patients With Lung Cancer S Annangi, M G Foreman, H P Ravipati, S Nutakki, E
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR
 Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease
 Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease Reference: NHS England: 16032/P 2 NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease Reference: NHS England: 16032/P 2 NHS England INFORMATION READER BOX Directorate
Treatment of oligometastatic NSCLC
 Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
Radiotherapy and Conservative Surgery For Merkel Cell Carcinoma - The British Columbia Cancer Agency Experience
 Radiotherapy and Conservative Surgery For Merkel Cell Carcinoma - The British Columbia Cancer Agency Experience Poster No.: RO-0003 Congress: RANZCR FRO 2012 Type: Scientific Exhibit Authors: C. Harrington,
Radiotherapy and Conservative Surgery For Merkel Cell Carcinoma - The British Columbia Cancer Agency Experience Poster No.: RO-0003 Congress: RANZCR FRO 2012 Type: Scientific Exhibit Authors: C. Harrington,
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Reirradiazione. La radioterapia stereotassica ablativa: torace. Pierluigi Bonomo Firenze
 Reirradiazione La radioterapia stereotassica ablativa: torace Pierluigi Bonomo Firenze Background Stage III NSCLC isolated locoregional recurrence in 25% of pts mostly unresectable; low RR with 2 nd line
Reirradiazione La radioterapia stereotassica ablativa: torace Pierluigi Bonomo Firenze Background Stage III NSCLC isolated locoregional recurrence in 25% of pts mostly unresectable; low RR with 2 nd line
Radiological changes following stereotactic radiotherapy for stage I lung cancer. M. Dahele, D. Palma, F. Lagerwaard, B. Slotman, S.
 Chapter 9 Radiological changes following stereotactic radiotherapy for stage I lung cancer M. Dahele, D. Palma, F. Lagerwaard, B. Slotman, S. Senan Department of Radiation Oncology, VU University Medical
Chapter 9 Radiological changes following stereotactic radiotherapy for stage I lung cancer M. Dahele, D. Palma, F. Lagerwaard, B. Slotman, S. Senan Department of Radiation Oncology, VU University Medical
Clinical Commissioning Policy: Stereotactic Body Radiotherapy / Stereotactic Ablative Radiotherapy. December Reference : NHSCB/B1a
 Clinical Commissioning Policy: Stereotactic Body Radiotherapy / Stereotactic Ablative Radiotherapy December 2012 Reference : NHSCB/B1a NHS Commissioning Board Clinical Commissioning Policy: Stereotactic
Clinical Commissioning Policy: Stereotactic Body Radiotherapy / Stereotactic Ablative Radiotherapy December 2012 Reference : NHSCB/B1a NHS Commissioning Board Clinical Commissioning Policy: Stereotactic
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia
 A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
Protocol of Radiotherapy for Small Cell Lung Cancer
 107 年 12 月修訂 Protocol of Radiotherapy for Small Cell Lung Cancer Indication of radiotherapy Limited stage: AJCC (8th edition) stage I-III (T any, N any, M0) that can be safely treated with definitive RT
107 年 12 月修訂 Protocol of Radiotherapy for Small Cell Lung Cancer Indication of radiotherapy Limited stage: AJCC (8th edition) stage I-III (T any, N any, M0) that can be safely treated with definitive RT
Thoracic Recurrences. Soft tissue recurrence
 Stereotactic body radiotherapy for thoracic and soft malignancies Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of
Stereotactic body radiotherapy for thoracic and soft malignancies Alexander Gottschalk, M.D., Ph.D. Associate Professor Director of CyberKnife Radiosurgery Department of Radiation Oncology University of
Stereotactic Ablative Radiotherapy for Non Small Cell Lung Cancer: Rationale and Outcomes
 1514 Original Article Stereotactic Ablative Radiotherapy for Non Small Cell Lung Cancer: Rationale and Outcomes Puneeth Iyengar, MD, PhD, a and Robert D. Timmerman, MD a,b Abstract Stereotactic ablative
1514 Original Article Stereotactic Ablative Radiotherapy for Non Small Cell Lung Cancer: Rationale and Outcomes Puneeth Iyengar, MD, PhD, a and Robert D. Timmerman, MD a,b Abstract Stereotactic ablative
stereotactic body radiation therapy Citation Journal of radiation research (2013 original work is properly cited
 Differences in the dose-volume metr Titlecorrection status and its influence stereotactic body radiation therapy Ueki, Nami; Matsuo, Yukinori; Shibu Author(s) Mitsuhiro; Narabayashi, Masaru; Sak Norihisa,
Differences in the dose-volume metr Titlecorrection status and its influence stereotactic body radiation therapy Ueki, Nami; Matsuo, Yukinori; Shibu Author(s) Mitsuhiro; Narabayashi, Masaru; Sak Norihisa,
Where are we with radiotherapy for biliary tract cancers?
 Where are we with radiotherapy for biliary tract cancers? Professor Maria A. Hawkins Associate Professor in Clinical Oncology MRC Group Leader/Honorary Consultant Clinical Oncologist CRUK MRC Oxford Institute
Where are we with radiotherapy for biliary tract cancers? Professor Maria A. Hawkins Associate Professor in Clinical Oncology MRC Group Leader/Honorary Consultant Clinical Oncologist CRUK MRC Oxford Institute
The Evolution of SBRT and Hypofractionation in Thoracic Radiation Oncology
 The Evolution of SBRT and Hypofractionation in Thoracic Radiation Oncology (specifically, lung cancer) 2/10/18 Jeffrey Kittel, MD Radiation Oncology, Aurora St. Luke s Medical Center Outline The history
The Evolution of SBRT and Hypofractionation in Thoracic Radiation Oncology (specifically, lung cancer) 2/10/18 Jeffrey Kittel, MD Radiation Oncology, Aurora St. Luke s Medical Center Outline The history
NRG Oncology Lung Cancer Portfolio 2016
 NRG Oncology Lung Cancer Portfolio 2016 Roy Decker, MD PhD Yale Cancer Center Walter J Curran, Jr, MD Winship Cancer Institute of Emory University NRG Oncology Lung Cancer Selected Discussion Stage III
NRG Oncology Lung Cancer Portfolio 2016 Roy Decker, MD PhD Yale Cancer Center Walter J Curran, Jr, MD Winship Cancer Institute of Emory University NRG Oncology Lung Cancer Selected Discussion Stage III
Applicazione Clinica: Polmone
 Applicazione Clinica: Polmone Andrea Riccardo Filippi Dipar5mento di Oncologia Università di Torino A technique for delivering external beam radiotherapy i. with a high degree of accuracy to an extra-cranial
Applicazione Clinica: Polmone Andrea Riccardo Filippi Dipar5mento di Oncologia Università di Torino A technique for delivering external beam radiotherapy i. with a high degree of accuracy to an extra-cranial
UNIVERSITY OF WISCONSIN-LA CROSSE Graduate Studies USE OF STEREOTACTIC BODY RADIATION THERAPY FOR INOPERABLE NON- SMALL CELL LUNG TUMORS
 UNIVERSITY OF WISCONSIN-LA CROSSE Graduate Studies USE OF STEREOTACTIC BODY RADIATION THERAPY FOR INOPERABLE NON- SMALL CELL LUNG TUMORS A Research Project Report Submitted in Partial Fulfillment of the
UNIVERSITY OF WISCONSIN-LA CROSSE Graduate Studies USE OF STEREOTACTIC BODY RADIATION THERAPY FOR INOPERABLE NON- SMALL CELL LUNG TUMORS A Research Project Report Submitted in Partial Fulfillment of the
Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience.
 Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience. Elisabetta Ponti MD, Gianluca Ingrosso MD, Alessandra Carosi PhD, Luana
Stereotactic body radiation therapy in oligometastatic patient with lymph node recurrent prostate cancer: a single centre experience. Elisabetta Ponti MD, Gianluca Ingrosso MD, Alessandra Carosi PhD, Luana
Aytul OZGEN 1, *, Mutlu HAYRAN 2 and Fatih KAHRAMAN 3 INTRODUCTION
 Journal of Radiation Research, 2012, 53, 916 922 doi: 10.1093/jrr/rrs056 Advance Access Publication 21 August 2012 Mean esophageal radiation dose is predictive of the grade of acute esophagitis in lung
Journal of Radiation Research, 2012, 53, 916 922 doi: 10.1093/jrr/rrs056 Advance Access Publication 21 August 2012 Mean esophageal radiation dose is predictive of the grade of acute esophagitis in lung
Radiation Therapy for Soft Tissue Sarcomas
 Radiation Therapy for Soft Tissue Sarcomas Alexander R. Gottschalk, MD, PhD Assistant Professor, Radiation Oncology University of California, San Francisco 1/25/08 NCI: limb salvage vs. amputation 43 patients
Radiation Therapy for Soft Tissue Sarcomas Alexander R. Gottschalk, MD, PhD Assistant Professor, Radiation Oncology University of California, San Francisco 1/25/08 NCI: limb salvage vs. amputation 43 patients
Although surgical resection with a lobectomy remains the
 Original Article Changes in Pulmonary Function Following Image-Guided Stereotactic Lung Radiotherapy Neither Lower Baseline Nor Post-SBRT Pulmonary Function Are Associated with Worse Overall Survival Brandon
Original Article Changes in Pulmonary Function Following Image-Guided Stereotactic Lung Radiotherapy Neither Lower Baseline Nor Post-SBRT Pulmonary Function Are Associated with Worse Overall Survival Brandon
Might Adaptive Radiotherapy in NSCLC be feasible in clinical practice?
 Might Adaptive Radiotherapy in NSCLC be feasible in clinical practice? E.Molfese, P.Matteucci, A.Iurato, L.E.Trodella, A.Sicilia, B.Floreno, S.Ramella, L.Trodella Radioterapia Oncologica, Università Campus
Might Adaptive Radiotherapy in NSCLC be feasible in clinical practice? E.Molfese, P.Matteucci, A.Iurato, L.E.Trodella, A.Sicilia, B.Floreno, S.Ramella, L.Trodella Radioterapia Oncologica, Università Campus
Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed tomography for non-operative lung cancer during adaptive
 Oncology and Translational Medicine October 2015, Vol. 1, No. 5, P195 200 DOI 10.1007/s10330-015-0054-3 ORIGINAL ARTICLE Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed
Oncology and Translational Medicine October 2015, Vol. 1, No. 5, P195 200 DOI 10.1007/s10330-015-0054-3 ORIGINAL ARTICLE Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed
Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery
 Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation I: Patient ER 74 y/o male with A1A
Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation I: Patient ER 74 y/o male with A1A
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Clinical Implications Of Dose Summation And Adaptation
 Clinical Implications Of Dose Summation And Adaptation Patrick Kupelian, M.D. Professor and Vice Chair University of California Los Angeles Department of Radiation Oncology pkupelian@mednet.ucla.edu August
Clinical Implications Of Dose Summation And Adaptation Patrick Kupelian, M.D. Professor and Vice Chair University of California Los Angeles Department of Radiation Oncology pkupelian@mednet.ucla.edu August
4D Radiotherapy in early ca Lung. Prof. Manoj Gupta Dept of Radiotherapy & oncology I.G.Medical College Shimla
 4D Radiotherapy in early ca Lung Prof. Manoj Gupta Dept of Radiotherapy & oncology I.G.Medical College Shimla Presentation focus on ---- Limitation of Conventional RT Why Interest in early lung cancer
4D Radiotherapy in early ca Lung Prof. Manoj Gupta Dept of Radiotherapy & oncology I.G.Medical College Shimla Presentation focus on ---- Limitation of Conventional RT Why Interest in early lung cancer
Radioterapia nella malattia oligometastatica. Fiorenza De Rose, M.D., Radiotherapy and Radiosurgery Dep. Humanitas Clinical and Research Hospital
 Radioterapia nella malattia oligometastatica Fiorenza De Rose, M.D., Radiotherapy and Radiosurgery Dep. Humanitas Clinical and Research Hospital OUTLINE Definition of oligometastatic state Local ablative
Radioterapia nella malattia oligometastatica Fiorenza De Rose, M.D., Radiotherapy and Radiosurgery Dep. Humanitas Clinical and Research Hospital OUTLINE Definition of oligometastatic state Local ablative
Jefferson Digital Commons. Thomas Jefferson University. Maria Werner-Wasik Thomas Jefferson University,
 Thomas Jefferson University Jefferson Digital Commons Department of Radiation Oncology Faculty Papers Department of Radiation Oncology May 2008 Increasing tumor volume is predictive of poor overall and
Thomas Jefferson University Jefferson Digital Commons Department of Radiation Oncology Faculty Papers Department of Radiation Oncology May 2008 Increasing tumor volume is predictive of poor overall and
Metastasis is the leading cause of cancer death in patients
 ORIGINAL ARTICLE Hypofractionated Image-Guided Radiation Therapy for Patients with Limited Volume Metastatic Non-small Cell Lung Cancer Michael D. Hasselle, MD,* Daniel J. Haraf, MD,* Kyle E. Rusthoven,
ORIGINAL ARTICLE Hypofractionated Image-Guided Radiation Therapy for Patients with Limited Volume Metastatic Non-small Cell Lung Cancer Michael D. Hasselle, MD,* Daniel J. Haraf, MD,* Kyle E. Rusthoven,
Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer
 1 Charles Poole April Case Study April 30, 2012 Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer Abstract: Introduction: This study
1 Charles Poole April Case Study April 30, 2012 Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer Abstract: Introduction: This study
A Prospective Pilot Study of Curative-intent Stereotactic Body Radiation Therapy in Patients With 5 or Fewer Oligometastatic Lesions
 650 A Prospective Pilot Study of Curative-intent Stereotactic Body Radiation Therapy in Patients With 5 or Fewer Oligometastatic Lesions Michael T. Milano, MD, PhD 1 Alan W. Katz, MD, MPH 1 Ann G. Muhs,
650 A Prospective Pilot Study of Curative-intent Stereotactic Body Radiation Therapy in Patients With 5 or Fewer Oligometastatic Lesions Michael T. Milano, MD, PhD 1 Alan W. Katz, MD, MPH 1 Ann G. Muhs,
SBRT I: Overview of Simulation, Planning, and Delivery
 Disclosure SBRT I: Overview of Simulation, Planning, and Delivery I have received research funding from NIH, the Golfers Against Cancer (GAC) foundation, and Philips Health System. Jing Cai, PhD Duke University
Disclosure SBRT I: Overview of Simulation, Planning, and Delivery I have received research funding from NIH, the Golfers Against Cancer (GAC) foundation, and Philips Health System. Jing Cai, PhD Duke University
SBRT for lung metastases: Case report
 SBRT for lung metastases: Case report Guillermo de Velasco MD, PhD University Hospital 12 de Octubre @H12O_GUCancer @g_develasco Case report 71 years old man Smoker DM 2005 Right radical nephrectomy Histology:
SBRT for lung metastases: Case report Guillermo de Velasco MD, PhD University Hospital 12 de Octubre @H12O_GUCancer @g_develasco Case report 71 years old man Smoker DM 2005 Right radical nephrectomy Histology:
Pancreatic Cancer and Radiation Therapy
 Pancreatic Cancer and Radiation Therapy Why? Is there a role for local therapy with radiation in a disease with such a high rate of distant metastases? When? Resectable Disease Is there a role for post-op
Pancreatic Cancer and Radiation Therapy Why? Is there a role for local therapy with radiation in a disease with such a high rate of distant metastases? When? Resectable Disease Is there a role for post-op
Clinical outcomes of CyberKnife stereotactic radiosurgery for elderly patients with presumed primary stage I lung cancer
 Original Article Clinical outcomes of CyberKnife stereotactic radiosurgery for elderly patients with presumed primary stage I lung cancer Zhen Wang 1, Ao-Mei Li 1, Jie Gao 1, Jing Li 1, Bing Li 1, Percy
Original Article Clinical outcomes of CyberKnife stereotactic radiosurgery for elderly patients with presumed primary stage I lung cancer Zhen Wang 1, Ao-Mei Li 1, Jie Gao 1, Jing Li 1, Bing Li 1, Percy
N.E. Verstegen A.P.W.M. Maat F.J. Lagerwaard M.A. Paul M.I. Versteegh J.J. Joosten. W. Lastdrager E.F. Smit B.J. Slotman J.J.M.E. Nuyttens S.
 N.E. Verstegen A.P.W.M. Maat F.J. Lagerwaard M.A. Paul M.I. Versteegh J.J. Joosten W. Lastdrager E.F. Smit B.J. Slotman J.J.M.E. Nuyttens S.Senan Submitted 10 Salvage surgery for local failures after stereotactic
N.E. Verstegen A.P.W.M. Maat F.J. Lagerwaard M.A. Paul M.I. Versteegh J.J. Joosten W. Lastdrager E.F. Smit B.J. Slotman J.J.M.E. Nuyttens S.Senan Submitted 10 Salvage surgery for local failures after stereotactic
Stereotactic body radiotherapy (SBRT) is increasingly used
 ORIGINAL ARTICLE A Comparison of Two Stereotactic Body Radiation Fractionation Schedules for Medically Inoperable Stage I Non-small Cell Lung Cancer The Cleveland Clinic Experience Kevin L. Stephans, MD,*
ORIGINAL ARTICLE A Comparison of Two Stereotactic Body Radiation Fractionation Schedules for Medically Inoperable Stage I Non-small Cell Lung Cancer The Cleveland Clinic Experience Kevin L. Stephans, MD,*
Defining Target Volumes and Organs at Risk: a common language
 Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
Clinical Aspects of SBRT in Abdominal Regions Brian D. Kavanagh, MD, MPH University of Colorado Department of Radiation Oncology
 Clinical Aspects of SBRT in Abdominal Regions Brian D. Kavanagh, MD, MPH University of Colorado Department of Radiation Oncology Abdominal SBRT: Clinical Aspects Rationales for liver and pancreas SBRT
Clinical Aspects of SBRT in Abdominal Regions Brian D. Kavanagh, MD, MPH University of Colorado Department of Radiation Oncology Abdominal SBRT: Clinical Aspects Rationales for liver and pancreas SBRT
Survey of the Patterns of Using Stereotactic Ablative Radiotherapy for Early-Stage Non-small Cell Lung Cancer in Korea
 pissn 1598-2998, eissn 2005-9256 Original Article https://doi.org/10.4143/crt.2016.219 Open Access Survey of the Patterns of Using Stereotactic Ablative Radiotherapy for Early-Stage Non-small Cell Lung
pissn 1598-2998, eissn 2005-9256 Original Article https://doi.org/10.4143/crt.2016.219 Open Access Survey of the Patterns of Using Stereotactic Ablative Radiotherapy for Early-Stage Non-small Cell Lung
Stereotactic Body Radiotherapy (SBRT) For HCC T A R E K S H O U M A N P R O F. R A D I A T I O N O N C O L O G Y N C I, C A I R O U N I V.
 Stereotactic Body Radiotherapy (SBRT) For HCC T A R E K S H O U M A N P R O F. R A D I A T I O N O N C O L O G Y N C I, C A I R O U N I V. Hepatocellular carcinoma (HCC), is a major health problem worldwide.
Stereotactic Body Radiotherapy (SBRT) For HCC T A R E K S H O U M A N P R O F. R A D I A T I O N O N C O L O G Y N C I, C A I R O U N I V. Hepatocellular carcinoma (HCC), is a major health problem worldwide.
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer
 Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Aoki et al. Radiation Oncology (2016) 11:5 DOI /s
 Aoki et al. Radiation Oncology (2016) 11:5 DOI 10.1186/s13014-016-0581-2 RESEARCH Open Access Clinical outcome of stereotactic body radiotherapy for primary and oligometastatic lung tumors: a single institutional
Aoki et al. Radiation Oncology (2016) 11:5 DOI 10.1186/s13014-016-0581-2 RESEARCH Open Access Clinical outcome of stereotactic body radiotherapy for primary and oligometastatic lung tumors: a single institutional
Additional radiation boost to whole brain radiation therapy may improve the survival of patients with brain metastases in small cell lung cancer
 Sun et al. Radiation Oncology (2018) 13:250 https://doi.org/10.1186/s13014-018-1198-4 RESEARCH Open Access Additional radiation boost to whole brain radiation therapy may improve the survival of patients
Sun et al. Radiation Oncology (2018) 13:250 https://doi.org/10.1186/s13014-018-1198-4 RESEARCH Open Access Additional radiation boost to whole brain radiation therapy may improve the survival of patients
Uncertainties and Quality Assurance of Localization and Treatment in Lung SBRT Jing Cai, PhD Duke University Medical Center
 Uncertainties and Quality Assurance of Localization and Treatment in Lung SBRT Jing Cai, PhD Duke University Medical Center 2013 AAPM 55 th Annual Meeting, Educational Course, Therapy Track, MOC SAM Program
Uncertainties and Quality Assurance of Localization and Treatment in Lung SBRT Jing Cai, PhD Duke University Medical Center 2013 AAPM 55 th Annual Meeting, Educational Course, Therapy Track, MOC SAM Program
Institute of Oncology & Radiobiology. Havana, Cuba. INOR
 Institute of Oncology & Radiobiology. Havana, Cuba. INOR 1 Transition from 2-D 2 D to 3-D 3 D conformal radiotherapy in high grade gliomas: : our experience in Cuba Chon. I, MD - Chi. D, MD - Alert.J,
Institute of Oncology & Radiobiology. Havana, Cuba. INOR 1 Transition from 2-D 2 D to 3-D 3 D conformal radiotherapy in high grade gliomas: : our experience in Cuba Chon. I, MD - Chi. D, MD - Alert.J,
Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer
 Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer Gabriela M. Vargas, MD Kristin M. Sheffield, PhD, Abhishek Parmar, MD, Yimei Han, MS, Kimberly M. Brown,
Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer Gabriela M. Vargas, MD Kristin M. Sheffield, PhD, Abhishek Parmar, MD, Yimei Han, MS, Kimberly M. Brown,
LONG-TERM SURGICAL OUTCOMES OF 1018 PATIENTS WITH EARLY STAGE NSCLC IN ACOSOG Z0030 (ALLIANCE) TRIAL
 LONG-TERM SURGICAL OUTCOMES OF 1018 PATIENTS WITH EARLY STAGE NSCLC IN ACOSOG Z0030 (ALLIANCE) TRIAL Stacey Su, MD; Walter J. Scott, MD; Mark S. Allen, MD; Gail E. Darling, MD; Paul A. Decker, MS; Robert
LONG-TERM SURGICAL OUTCOMES OF 1018 PATIENTS WITH EARLY STAGE NSCLC IN ACOSOG Z0030 (ALLIANCE) TRIAL Stacey Su, MD; Walter J. Scott, MD; Mark S. Allen, MD; Gail E. Darling, MD; Paul A. Decker, MS; Robert
Prostate Cancer Appraisal Addendum: Stereotactic Body Radiation Therapy (SBRT)
 Prostate Cancer Appraisal Addendum: Stereotactic Body Radiation Therapy (SBRT) The Institute for Clinical and Economic Review (ICER) has published appraisals on multiple management options for clinically-localized,
Prostate Cancer Appraisal Addendum: Stereotactic Body Radiation Therapy (SBRT) The Institute for Clinical and Economic Review (ICER) has published appraisals on multiple management options for clinically-localized,
SBRT fundamentals. Outline 8/2/2012. Stereotactic Body Radiation Therapy Quality Assurance Educational Session
 Stereotactic Body Radiation Therapy Quality Assurance Educational Session J Perks PhD, UC Davis Medical Center, Sacramento CA SBRT fundamentals Extra-cranial treatments Single or small number (2-5) of
Stereotactic Body Radiation Therapy Quality Assurance Educational Session J Perks PhD, UC Davis Medical Center, Sacramento CA SBRT fundamentals Extra-cranial treatments Single or small number (2-5) of
Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery
 ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
The Physics of Oesophageal Cancer Radiotherapy
 The Physics of Oesophageal Cancer Radiotherapy Dr. Philip Wai Radiotherapy Physics Royal Marsden Hospital 1 Contents Brief clinical introduction Imaging and Target definition Dose prescription & patient
The Physics of Oesophageal Cancer Radiotherapy Dr. Philip Wai Radiotherapy Physics Royal Marsden Hospital 1 Contents Brief clinical introduction Imaging and Target definition Dose prescription & patient
Pattern of recurrence after CyberKnife stereotactic body radiotherapy for peripheral early non-small cell lung cancer
 Original Article Pattern of recurrence after CyberKnife stereotactic body radiotherapy for peripheral early non-small cell lung cancer Masaki Nakamura 1,2, Ryo Nishikawa 1,3, Hiroshi Mayahara 1, Haruka
Original Article Pattern of recurrence after CyberKnife stereotactic body radiotherapy for peripheral early non-small cell lung cancer Masaki Nakamura 1,2, Ryo Nishikawa 1,3, Hiroshi Mayahara 1, Haruka
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer
 Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer
 Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication for Repeat Metastasectomy
 Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Stereotaxy. Outlines. Establishing SBRT Program: Physics & Dosimetry. SBRT - Simulation. Body Localizer. Sim. Sim. Sim. Stereotaxy?
 Establishing SBRT Program: Physics & Dosimetry Lu Wang, Ph.D. Radiation Oncology Department Fox Chase Cancer Center Outlines Illustrate the difference between SBRT vs. CRT Introduce the major procedures
Establishing SBRT Program: Physics & Dosimetry Lu Wang, Ph.D. Radiation Oncology Department Fox Chase Cancer Center Outlines Illustrate the difference between SBRT vs. CRT Introduce the major procedures
IAEA RTC. PET/CT and Planning of Radiation Therapy 20/08/2014. Sarajevo (Bosnia & Hercegovina) Tuesday, June :40-12:20 a.
 IAEA RTC PET/CT and Planning of Radiation Therapy Sarajevo (Bosnia & Hercegovina) Tuesday, June 17 2014 11:40-12:20 a.m María José García Velloso Servicio de Medicina Nuclear Clínica Universidad de Navarra
IAEA RTC PET/CT and Planning of Radiation Therapy Sarajevo (Bosnia & Hercegovina) Tuesday, June 17 2014 11:40-12:20 a.m María José García Velloso Servicio de Medicina Nuclear Clínica Universidad de Navarra
IGRT Protocol Design and Informed Margins. Conflict of Interest. Outline 7/7/2017. DJ Vile, PhD. I have no conflict of interest to disclose
 IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
Comparison of Interfacility Implementation of Essential SBRT Components. Keith Neiderer B.S. CMD RT(T) VCU Health System
 Comparison of Interfacility Implementation of Essential SBRT Components Keith Neiderer B.S. CMD RT(T) VCU Health System Disclosures None Objectives Review essential components that characterize SBRT Compare
Comparison of Interfacility Implementation of Essential SBRT Components Keith Neiderer B.S. CMD RT(T) VCU Health System Disclosures None Objectives Review essential components that characterize SBRT Compare
brain SPINE 2 SRS Matures into breast lung spine LUNG Dr. Robert Timmerman Discusses SBRT for Inoperable Lung Cancer BRAIN
 NEWS AND ADVANCES IN THE MANAGEMENT AND TREATMENT OF SERIOUS DISEASE brain SPINE 2 SRS Matures into Mainstream Extracranial Technique lung spine breast LUNG Dr. Robert Timmerman Discusses SBRT for Inoperable
NEWS AND ADVANCES IN THE MANAGEMENT AND TREATMENT OF SERIOUS DISEASE brain SPINE 2 SRS Matures into Mainstream Extracranial Technique lung spine breast LUNG Dr. Robert Timmerman Discusses SBRT for Inoperable
