Effects of tibolone and continuous combined hormone therapy on mammographic breast density and breast histochemical markers in postmenopausal women
|
|
|
- Shauna Sutton
- 5 years ago
- Views:
Transcription
1 FERTILITY AND STERILITY VOL. 81, NO. 3, MARCH 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. Effects of tibolone and continuous combined hormone therapy on mammographic breast density and breast histochemical markers in postmenopausal women Isabel Valdivia, M.D., a Italo Campodónico, M.D., a Augusto Tapia, M.D., a María Capetillo, M.D., b Arturo Espinoza, M.D., b and Pablo Lavín, M.D. a School of Medicine, University of Chile, Santiago, Chile Received January 21, 2003; revised and accepted July 31, Supported in part by an unrestricted research grant from Hormoquímica de Chile, Santiago, Chile (branch of NV Organon, Oss, the Netherlands). Reprint requests: Isabel Valdivia, M.D., Vitacura 5900, Of. 412, Santiago, Chile (FAX: ; imvaldivia@ entelchile.net). a Department of Obstetrics and Gynecology. b Department of Pathology /04/$30.00 doi: /j.fertnstert Objective: To compare changes in mammographic density and the expression of markers of proliferation (Ki67) and apoptosis (Bcl-2) after 1 year of treatment with tibolone and continuous conjugated equine estrogens combined with medroxyprogesterone acetate (CEE-MPA). Design: Comparative, randomized, evaluator-blinded study. Setting: City research hospital. Patient(s): Thirty-seven postmenopausal women. Intervention(s): Tibolone (2.5 mg; n 18) or continuous conjugated estrogens (0.625 mg) combined with medroxyprogesterone acetate (5 mg; n 19) for 1 year. Main Outcome Measure(s): Mammographic density (BI-RADS density score), expression of immunohistochemical markers Ki67 and Bcl-2. Result(s): Mean breast density score decreased significantly from 2.22 to 1.67 in the tibolone group, compared with a significant increase in the CEE-MPA treated group from 1.84 to Ki67 expression decreased in 12 of 15, increased in 2 of 15, and remained unchanged in 1 of 15 subjects in the tibolone group, compared with 1 of 19, 15 of 19, and 3 of 19 subjects, respectively, in the CEE-MPA group. Bcl-2 expression decreased in 12 of 15, increased in 2 of 15, and remained unchanged in 1 of 15 subjects in the tibolone group, compared with 5 of 19, 9 of 19, and 5 of 19 subjects, respectively, in the CEE-MPA group. Conclusion(s): One-year treatment with tibolone induced a decrease in breast density, with a reduction in proliferation and a stimulation of apoptosis, whereas 1-year treatment with CEE-MPA induced an increase in breast density, with stimulation of proliferation and inhibition of apoptosis, indicating that tibolone effects on the breast are different from those of CEE-MPA. (Fertil Steril 2004;81: by American Society for Reproductive Medicine.) Key Words: Mammographic breast density, hormone therapy, tibolone, Ki67, Bcl-2, proliferation, apoptosis Postmenopausal women use various medications to relieve climacteric symptoms and to prevent osteoporosis. Continuous use of estrogens, combined with progestagens (continuous combined E P orcce P), is one of the most commonly used treatments. An alternative to this more conventional hormonal therapy (HT) is tibolone (Livial, Organon, The Netherlands), a unique tissue-specific compound (1). After oral administration, tibolone is rapidly converted by the intestine and the liver, mainly into two estrogenic metabolites (3 - and 3 OH-metabolites), which are responsible for its estrogenic effects on bone, vagina, and climacteric complaints. A third metabolite, the 4-isomer, has progestagenic and androgenic activities and is formed in the liver and intestine as well as locally in the endometrium, thereby preventing endometrial stimulation. One of the most common reasons for withdrawing from long-term use of conventional HT is fear of breast cancer. Although available data are equivocal, according to a meta-analysis of all epidemiological data, breast cancer risk increases by 2.3% for each year of estro- 617
2 gen use (2). In the Women s Health Initiative Randomized Controlled Trial, treatment for 5.2 years with conjugated estrogens medroxyprogesterone acetate (MPA) resulted in a 26% increase in risk of breast cancer compared with placebo, leading to an absolute excess risk of 8 per 10,000 person-years (3). Two recent studies suggest that combined estrogen and progestogen enhances the risk of breast cancer relative to estrogen alone (4, 5). Breast cancers diagnosed during conventional HT use, however, are smaller and less aggressive; most reports indicate no increase in breast cancer mortality (6). Conventional HT has been associated with an increase in breast density on mammography (7, 8), which is reversible after discontinuation of therapy. Increased density of the breast may complicate the detection of small tumors during mammographic screenings. Though high breast density is associated with a fourfold to sixfold increased risk of breast cancer (9, 10), there are several reasons to suspect that the increase in breast density reported with conventional HT may not be identical to the high breast density that is associated with an increased risk of breast cancer (8). The effects of tibolone on the breast differ from those observed with conventional HT. During treatment with tibolone, the incidence of breast tenderness was reported to be lower, and no relevant effect on mammographic density could be observed (7, 11, 12). Estrogens are known to enhance the rate of cell proliferation in the glandular tissue of the breast. Progestogens, which differ in structure and function, show different effects; some show breast tissue proliferation, whereas others show antiproliferation. Though an increase in proliferation per se does not necessarily mean induction of DNA mutations, stimulation of cell proliferation may increase the likelihood of a DNA replication error-escaping repair and could potentially act both as cofactor on the initiation and promotion of breast cancer. Recent studies suggest that some estrogen metabolites could act as carcinogens per se. The final stage in the life cycle of a cell is apoptosis (programmed cell death). The last step of this process is mediated by proapoptotic enzymes, which are regulated by proteins of the Bcl-2 family. Bcl-2 expression displays a strong cyclical variation and has been shown to be hormone dependent (13). A negative effect on apoptosis, for example, an increase in cell survival time, may increase the chance of inducing breast cancer. In this study, the effects of 1-year treatment with tibolone on breast density and on markers of proliferation (Ki67) and apoptosis (Bcl-2) are compared with those of continuous conjugated equine estrogens (CEE) combined with MPA therapy. Ki67 is a monoclonal antibody that reacts with a nuclear antigen that is expressed only in proliferating cells throughout the cell cycle and is absent from quiescent cells. Ki67 is the most widely used proliferation marker, whereas Bcl-2, which counteracts the occurrence of apoptosis, is one of the principal cytoplasmic apoptosis markers (14, 15). MATERIALS AND METHODS Study Design The study was designed as a randomized, single-center, assessor-blind study in postmenopausal women. It was performed at Hospital del Salvador, Santiago de Chile, between August 1998 and November 2001 and was in full compliance with the current version of the Declaration of Helsinki (Republic of South Africa, amendment October 1996) and the ICH Guideline for Good Clinical Practice. The Investigation and Education Board of the Ethical Committee of Hospital del Salvador approved the study protocol. All volunteers had given written informed consent before participating in the study. Thirty-seven volunteers were randomized to receive either tibolone (2.5 mg daily; Livial, Organon, Oss, the Netherlands) or conjugated equine estrogens (0.625 mg) medroxyprogesterone acetate (5 mg daily; Prempak plus; Wyeth-Ayerst Labs) for 12 months. Subjects To be considered for inclusion, women had to [1] have climacteric complaints, [2] be less than 65 years of age and in natural menopause (between 12 and 60 months of amenorrhea), [3] not have used hormone therapy or hormones in the past 6 months, [4] have no contraindications for hormone therapy, [5] have a negative mammography for cancer, and [6] have endometrium thickness (double layer) of 6 mm (by vaginal ultrasound). Subjects were excluded from the trial if they were overweight (body mass index 28) or had uncontrolled arterial hypertension or diabetes. Study Procedures and Methods of Evaluation Mammography was performed at baseline and after completion of 1 year of treatment with Lorad equipment (model Elite). Pretreatment and posttreatment mammographies were randomly coded and blindly assessed for density at the end of the study by a single evaluator. Mammographic density was scored according to the Breast Imaging Reporting and Data System (BI-RADS) proposed by the American College of Radiologists (16). Possible density categories were [1] entirely fatty: involutive, [2] fatty with scattered fibro-glandular tissue, [3] heterogeneously dense, and [4] extremely dense. Mean density score per treatment group was calculated. At baseline and after 1 year of treatment, a breast tissue sample (core biopsy type) was withdrawn under local anesthesia from the upper-external quadrant of the left breast using an automatic pistol system with a 1.2-mm (14G) biopsy needle. Three to five specimens of about 3 cm in length were obtained, fixed in 3.7% neutral buffered formalin, and subsequently embedded in paraffin. The samples 618 Valdivia et al. Effects of tibolone and CEE-MPA on breast tissue Vol. 81, No. 3, March 2004
3 were randomly coded to ensure blinding and assessed at the end of the study. Adjacent 3- m serial sections were placed on slides coated with APES, deparaffinized, and rinsed twice with PBS Buffer Power Block (Casein). Subsequently, the slides were evaluated for expression of Ki67 and Bcl-2 using automatic Optimax Plus equipment, by using the B-SA system method (Biogenex). The slides were placed in either a solution of monoclonal antibody Ki67 (MIB1; dilution of 1:150) for 90 minutes or in a solution of monoclonal antibody Bcl-2 (CLONE (100); dilution of 1:90) for 40 minutes. Subsequently the slides were incubated with secondary antibodies for 20 minutes (biotinylated anti-mouse, anti-rabbit, and anti-goat immunoglobulin), followed by a 20-minute incubation with streptavidin peroxidase (Biogenex) for labeling. The slides were stained using NOVARED Vector (SK 4800), followed by counterstaining with Harris Hematoxiline. The presence of both antibodies was independently quantified by two pathologists, by using an optical microscope, and was expressed as the percentage of Ki67 positive or Bcl-2 positive cells relative to the total number of cells. Statistical analysis was done using EPI-Info 2002 revision 1 software. Effects of treatment were assessed using twosided Student s t-test for mean differences and 2 test for difference in proportions. Differences in the distributions of the percentages of cells with staining for expression of Bcl-2 and Ki67 were assessed with Fisher s exact test, using Stata 7.0 software. TABLE 1 Changes in Ki67 expression from baseline to end of treatment (12 months). Type of change Tibolone, n (%) CEE-MPA, n (%) Increase 2/15 (13.3) 15/19 (78.9) Decrease 12/15 (80.0) 1/19 (5.3) No change 1/15 (6.7) 3/19 (15.8) Note: CEE-MPA conjugated equine estrogens combined with medroxyporgesterone acetate. RESULTS All 37 subjects completed the study as planned. There were no statistically significant differences between the two treatment groups with respect to demographic data. The 18 subjects in the tibolone group had the following mean (SD) values: 51.1 (3.2) years of age; 3.6 (2.2) deliveries; 28.6 (17.3) months since menopause; (6.7) cm in height; kg in weight, and body mass index of 26.2 (2.6) kg/m 2. The 19 subjects in the CEE-MPA group had mean (SD) values of 52.6 (3.9) years of age; 2.9 (2.3) deliveries; 40.3 (28.3) months since menopause; (5.4) cm in height; kg in weight; and body mass index of 26.6 (2.5) kg/m 2. There was no statistically significant difference (0.38 BI-RADS; P.27) in mean (SD) breast density at baseline between groups (2.22 [1.11] for tibolone group and 1.84 [0.96] BI-RADS for CEE-MPA group). After 12 months of treatment with tibolone, mean (SD) breast density score decreased to 1.67 (0.84) BI-RADS, whereas in the CEE- MPA treated group, an increase was observed to 2.63 (1.17) BI-RADS; this group difference of the means of 0.97 BI- RADS was statistically significant (P.007). The net mean difference of in BI-RADS change from baseline between the two groups ( [0.86] and 0789 [0.92], respectively) was statistically significant (P.00053). In the tibolone group, in only 1 (of 18; 5.5%) subject was an increase in breast density observed, whereas in 8 of 18 (45.5%) subjects, breast density score decreased, and in 9 of 18 (50.0%) subjects, no change was observed. In the CEE- MPA group, the majority of subjects (57.9%) showed an increase in breast density (11/19), whereas in only 1 of 19 (5.3%) a decrease was observed and in 7 of 19 (36.8%), breast density score remained unchanged. Of a total of 78 breast biopsies, only 3 specimens were inadequate for evaluation, leading to 15 subjects with adequate biopsies pretreatment and posttreatment in the tibolone group and 19 subjects in the CEE-MPA group. The effects of treatment with tibolone and CEE-MPA on the percentage of cells stained for expression of Ki67, expressed as the direction of change in individual subjects (increase, decrease, or no change), is presented in Table 1. In the tibolone-treated group, most women (80%) had a decrease in Ki67 expression, whereas in the CEE-MPA group, most women (78.9%) presented with an increase. The difference between the two groups in the distribution of changes was statistically significant (P.0013). The distribution of subjects presenting with a specific proportion of cells stained for Ki67 expression in the tibolone-treated group varied from baseline to after 12 months of treatment, with a shift to lower percentages of Ki67 expression (statistically significant; P.035), with, respectively, 8 and 13 cases in the 0 to 5% stained cells, 7 and 1 cases in the 6% to 10% stained cells, and 0 and 1 case in the 11% to 15% stained cells. In the CEE-MPA treated group, a nonstatistically significant shift to higher percentages could be noted (P.016), with, respectively, 13 and 6 cases in the 0 to 5% stained cells, 4 and 6 cases in the 6% to 10% stained cells, 1 to 2 cases in the 11% to 15% stained cells, 1 and 4 cases in the 16% to 20% stained cells, and 0 and 1 cases in the 21% to 25% stained cells. The absence of statistical significance in this last treatment group is probably related to the relatively small number of subjects in each treatment group. Typical examples of slides stained for Ki67 expression, FERTILITY & STERILITY 619
4 FIGURE 1 Breast cells stained for expression of cell proliferation marker Ki67 in breast biopsies taken from women before (left-hand side) and after (right-hand side) 12 months of treatment with (A and B) tibolone or with (C and D) CEE-MPA. Magnification: A, 100; B, 100; C, 100; D, 400. prepared from biopsies taken before and after 12 months of treatment with tibolone (upper quadrants, A and B, respectively) and CEE-MPA (lower quadrants, C and D, respectively), are presented in Figure 1, in which a reduction in the number of samples showing nuclear staining in the group with tibolone treatment and an increase in the number of samples showing nuclear staining in the group with CEE- MPA treatment is clearly seen after 12 months. The effects of treatment with tibolone and CEE-MPA on the percentage of cells stained for expression of Bcl-2, expressed as the direction of change in individual subjects, are presented in Table 2. In the tibolone-treated group, most women (80%) presented with a decrease in Bcl-2 expression, whereas in the CEE-MPA treated group, most women (47.4%) had an increase in Bcl-2 expression. The difference in distribution of changes between treatment groups was statistically significant (P.03). The distribution of subjects presenting with a specific proportion of cells stained for Bcl-2 expression is as follows. For the tibolone group, the number of cases with 0 10, 11 20, 21 30, 31 40, 41 50, 51 60, 61 70, and cells with positive expression before and after 12 months of treatment changed from 1 to 3, from 2 to 6, from 7 to 3, from 2 to 2, from 1 to 0, from 1 to 0, from 1 to 0, and from 0 to 1 subjects, respectively, and for the CEE-MPA treated TABLE 2 Changes in Bcl-2 expression from baseline to end of treatment (12 months). Type of change Tibolone, n (%) CEE-MPA, n (%) Increase 2/15 (13.3) 9/19 (47.4) Decrease 12/15 (80.0) 5/19 (26.3) No change 1/15 (6.7) 5/19 (26.3) Note: CEE-MPA conjugated equine estrogens combined with medroxyprogesterone acetate. 620 Valdivia et al. Effects of tibolone and CEE-MPA on breast tissue Vol. 81, No. 3, March 2004
5 FIGURE 2 Breast cells stained for expression of antiapoptotic protein Bcl-2 in breast biopsies taken from women before (left-hand side) and after (right-hand side) 12 months of treatment with (A and B) tibolone or with (C and D) CEE-MPA. Magnification: A, 400; B, 400; C, 400; D, 400. group, the distribution, respectively, was as follows: 5 to 3, 3 to 2, 5 to 7, 0 to 1, 4 to 1, 1 to 1, 0 to 1, and 1 to 3 subjects. In summary, it can be said that in the tibolone-treated group, a shift to lower percentages of antiapoptotic protein Bcl-2 expression was observed (though not statistically significant; P.248), whereas in the CEE-MPA treated group, the overall effect on the distribution is less obvious (P.612). Typical examples of slides stained for antiapoptotic protein Bcl-2 expression, prepared from biopsies taken before and after 12 months of treatment with tibolone (upper quadrants A and B, respectively) and CEE-MPA (lower quadrants C and D, respectively), are presented in Figure 2, in which a reduction of the cytoplasmic staining in the group with tibolone treatment and an increase of the cytoplasmic staining in the group with CEE-MPA treatment is clearly seen after 12 months. DISCUSSION The relative proportion of fat and fibroglandular tissue in the breast determines breast density on mammograms. High breast density is believed to represent proliferation of fibroglandular tissue. Several methods for classifying breast density are available, including Wolfe s patterns (a visual parenchymal method) (17) and estimation of the proportion (as a percentage) of the dense breast area (the percentagedensity method). In this study we used the BI-RADS density score method, which is the standard system currently used in clinical radiology practice in the United States. After 12 months of treatment with tibolone, the mean BI-RADS score decreased from 2.22 to 1.67, whereas in the CEE-MPA group, breast density increased from 1.84 to 2.63; the difference in change from baseline between the two groups was statistically significant. These results are in line with those reported in other studies. In our previous study, published in 1997 (18), using Wolfe s visual parenchymal method, breast density increased in 3.3% of the tibolone users, as compared with an increase in 66.7% to 26.7% of women using different estrogen-containing HT. The increase in the tibolone group was similar to that observed in the nontreated control group. The evaluation scores in this study FERTILITY & STERILITY 621
6 were highly reliable, with between-radiologist agreement ranging from 70% to 90%. In a recent study published by Lundström etal.(7), the effects of tibolone on breast density were compared with those of continuous combined hormone therapy (E 2 with norethisterone acetate) and placebo. In the women treated with estrogen-progestogen, breast density was increased in 46% 50%, as compared with an increase in 2% 6% in the group receiving tibolone and with an increase of 0 in the placebo group. An increase in breast density with estrogen-containing HT and the absence of a relevant effect with tibolone was also reported by Erel et al. (19, 20), Colacurci et al. (21), Egarter et al. (22), and Sendag et al. (23). In addition to the effect on breast density, we also investigated the effects of tibolone and CEE-MPA on cell proliferation (assessed as expression of Ki67) and apoptosis (assessed as expression of Bcl-2). In the present study, tibolone treatment showed a strong antiproliferative activity; most of the subjects presented decreased Ki67 expression, whereas in the CEE-MPA group, an increase in proliferation was observed. An HT-induced increase in proliferation was also observed in a cross-sectional observational study by Hofseth et al. (15). Compared with no HT, the breast epithelium of women who had received estrogen either alone or combined with progestogen had significantly higher proliferation (as assessed by determination of Ki67 expression and anti-proliferative cell nuclear antigen, anti-pcna), the effect of the combined treatment being greater than that of estrogen alone. Furthermore, with the combined therapy, breast proliferation was localized to the terminal duct-lobular unit of the breast, which is the site of development of most breast cancers. In a recent study by von Schoultz (24), the effects of 6 months treatment with E 2 (2 mg) combined with norethisterone acetate (1 mg), with tibolone, or with placebo on breast cell proliferation in cytological specimens obtained by fine needle aspiration, by using the Ki67 antibody technique, were compared. Treatment with E 2 norethisterone acetate induced an almost threefold increase in proliferation, whereas the effects of tibolone did not differ from those of placebo. The effects of treatment with tibolone and CEE-MPA on Bcl-2 expression differed significantly in the present study. In the tibolone group, the expression of Bcl-2 diminished in 80% of the subjects, whereas in only 13.3% of the subjects was an increase observed. In the CEE-MPA group, a decrease was observed in only 26.3% of the subjects, compared with an increase in 47% of the subjects. There are no published data on the effects of HT on markers of apoptosis (such as Bcl-2) in clinical studies. In cell cultures of normal and transformed breast epithelial cells, E 2 was shown to have an anti-apoptotic effect, whereas progestagens were found to be proapoptotic; tibolone was also found to stimulate apoptosis (15, 25 27). It is interesting to speculate on the causes of the differences in effects observed with tibolone and estrogen-progestogen treatment. Normal breast tissue contains high concentrations of estrogens. Tibolone and its 4 -isomer have been shown to lower estrogen concentrations in breast tissue by inhibiting sulfatases (inhibition of estrone formation from sulfated precursors), with a concomitant stimulation of sulfotransferase enzymes (stimulation of formation of biologically inactive sulfated forms of estrogen). Moreover, tibolone and its 4 - isomer block the 17 -hydroxysteroid dehydrogenase type I and stimulate the 17 -hydroxysteroid dehydrogenase type II, resulting in reduced local levels of E 2. The overall effect is a reduction of estrogenic exposure in the breast (28). The above effects have been observed in normal breast tissue and breast cancer lines (29, 30) but have not been found in other tissues such as bones (31). Estrogens are also synthesized from androgens via the aromatase pathway. However, tibolone and its main metabolites do not act as substrates for aromatase enzymes (32). A consequence of conventional HT treatment is that breast tissue is exposed to far higher concentrations of estrogen than before. Estrogens are known to enhance the rate of cell proliferation in the glandular tissue of the breast. The observation that conventional HT leads to an increase in tissue concentrations of estrogen in the breast, whereas tibolone treatment induces a reduction of such, may explain the differences in effects on breast density, cell proliferation, and apoptosis. An additional explanation of the difference in effect may be the effects of tibolone on free T levels and sex hormone binding globulin. In a study by Dören et al. (33), tibolone treatment was found to increase free T levels and decrease sex hormone binding globulin concentrations, whereas treatment with E 2 norethindrone acetate induced the opposite pattern. Breast cell proliferation has been described to be negatively correlated with free T in women who are using oral contraceptives (34) and to inhibit estrogen-induced breast epithelial proliferation and estrogen receptor expression in rhesus monkeys (35). Increased T levels may add to local actions in the breast to explain the different effects on breast proliferation during treatment with tibolone, as compared with conventional HT. In conclusion, 1-year treatment with tibolone induced a decrease in breast density, with a reduction in proliferation (reduction of Ki67 expression) and a stimulation of apoptosis (decrease in anti-apoptotic protein Bcl-2), whereas 1-year treatment with CEE-MPA induced an increase in breast density, with an increase in proliferation and inhibition of 622 Valdivia et al. Effects of tibolone and CEE-MPA on breast tissue Vol. 81, No. 3, March 2004
7 apoptosis; the differences between the two groups were statistically significant. Our results clearly indicate that the effects of tibolone on the breast are different from those of conventional HT. References 1. Kloosterboer HJ. Tibolone: a steroid with a tissue-specific mode of action. J Steroid Biochem Mol Biol 2001;76: Beral V, Bull D, Doll R, Key T, Peto R, Reeves G. Breast cancer and hormone replacement therapy; collaborative reanalysis of data from 51 epidemiological studies of women with breast cancer and women without breast cancer. Lancet 1997;350: Writing Group for the Women s Health Initiative Investigators. Risks and benefits of estrogen plus progestin in healthy postmenopausal women. Principal results from the Women s Health Initiative Randomized Controlled Trial. JAMA 2002;288: Schairer C, Lubin J, Troisi R, Sturgeon S, Brinton L, Hoover R. Menopausal estrogen and estrogen-progestin replacement therapy and breast cancer risk. J Am Med Assoc 2000;283: Ross RK, Paganini-Hill A, Wan PC, Pike MC. Effect of hormone replacement therapy on breast cancer risk: estrogen versus estrogen plus progestin. J Natl Cancer Inst 2000;92: Schairer C, Gail M, Byrne C, Rosenberg PS, Sturgeon SR, Brinton LA, et al. Estrogen replacement therapy and breast cancer survival in a large screening study. J Natl Cancer Inst 1999;91: Lundström E, Christow A, Kersemaekers W, Svane G, Azavedo E, Söderqvist G, et al. Effects of tibolone and continuous combined hormone replacement therapy on mammographic breast density. Am J Obstet Gynecol 2002;186: Speroff L. The meaning of mammographic breast density in users of postmenopausal hormone therapy. Maturitas 2002;41: Byrne C, Schairer C, Wolfe J, Parekh N, Salane M, Brinton LA, et al. Mammographic features and breast cancer risk: effects with time, age and menopause status. J Natl Cancer Inst 1995;87: Byng JW, Yaffe MJ, Jong RA, Shumak RS, Lockwood GA, Tritchler DL, et al. Analysis of mammographic density and breast cancer risk from digitized mammograms. Radiographics 1998;18: Hammar M, Christau S, Nathorst-Böös J, Rud T, Garre K. A doubleblind randomized trial comparing the effects of tibolone and continuous combined hormone replacement therapy in postmenopausal women with menopausal complaints. Br J Obstet Gynaecol 1998;105: Valdivia I, Ortega D. Mammographic density in postmenopausal women treated with tibolone, estriol or conventional hormone replacement therapy. Clin Drug Invest 2000;20: Gompel A, Somai S, Chaouat M, Kazem A, Kloosterboer HJ, Beusman I, et al. Hormonal regulation of apoptosis in breast cells and tissues. Steroids 2000;65: Van Dierendonck JH, Keijzer R, van de Velde CHJ, Cornelisse CJ. Nuclear distribution of the Ki67 antigen during the cell cycle: comparison with growth fraction in human breast cancer cells. Cancer Res 1989;49: Hofseth L, Raafat AM, Osuch JR, Pathak DR, Slomski CA, Haslam SZ. Hormone replacement therapy with estrogen plus medroxyprogesterone acetate is associated with increased epithelial proliferation in the normal postmenopausal breast. J Clin Endocrinol Metab 1999;84: American College of Radiology. Breast imaging reporting and data system (BI-RADS), 2nd ed. Reston, VA: American College of Radiology, Wolfe JN. Breast patterns as an index of risk for developing breast cancer. Am J Roentgenol 1976;126: Valdivia I, Ortega D. A one-year evaluation of mammary radiographic density (MxDx) changes with different HRTs regimens in climacteric women. Acta Obstet Gynecol Scand 1997;167(Suppl 76): Erel CT, Elter K, Akman C, Ersavasti G, Altug A, Seyisoglu H, et al. Mammographic changes in women receiving tibolone therapy. Fertil Steril 1998;69: Erel CT, Esen G, Seyisoglu H, Elter K, Uras C, Ertungealp E, et al. Mammographic density increase in women receiving different hormone replacement regimens. Maturitas 2001;40: Colacurci N, Fornaro F, de Franciscis P, Palermo M, del Vecchio W. Effects of different types of hormone replacement therapy on mammographic density. Maturitas 2001;40: Egarter C, Eppel W, Vogel S, Wolf G. A pilot study of hormone replacement therapy with tibolone in women with mastopathic breasts. Maturitas 2001;40: Sendag F, Terek MC, Özsener S, Öztekin K. Mammographic density changes in postmenopausal women using tibolone therapy. Int J Gynecol Obstet 2001;74: von Schoultz B. The effects of tibolone and conventional HRT on breast cell proliferation and mammographic density. Climacteric 2002; 5(Suppl 1): Gompel A, Kandouz M, Siromachkova M, Lombet A, Thevenin D, Mimoun M, et al. The effect of tibolone on proliferation, differentiation and apoptosis in normal breast cells. Gynecol Endocrinol 1997; 11(Suppl 1): Kloosterboer HJ, Schoonen WGEJ, Deckers GH, Klijn JGM. Effects of progestagens and Org OD14 in vitro and in vivo tumor models. J Steroid Biochem Mol Biol 1994;49: Gompel A, Chaouat M, Jacob D, et al. In vitro studies of tibolone in breast cells. Fertil Steril 2002;78: Kloosterboer HJ. New mechanisms of action for tibolone in breast cancer. In: Menopause. Hormones and cancer. Proceedings of the 2nd International Symposium of the Portuguese Menopause Society. 2002: Chetrite GS, Kloosterboer HJ, Philippe J-C, Pasqualini JP. Effect of Org OD 14 (Livial) and its metabolites on human estrogen sulfotransferase activity in the hormone-dependent MCF-7 and T-47D, and the hormone-independent MDA-MB-231, breast cancer cell lines. Anticancer Res 1999;19: Chetrite GS, Kloosterboer HJ, Philippe J-C, Pasqualini JR. Effect of Org OD 14 (Livial) and its metabolites on 17 -hydroxysteroid dehydrogenase activity in hormone-dependent MCF-7 and T-47D breast cancer cells. Anticancer Res 1999;19: de Gooyer ME, Overklift Vaupel Kleyn GT, Smits KC, Ederveen AGH, Verheul HAM, Kloosterboer HJ. Tibolone: a compound with tissue specific inhibitory effects on sulfatase. Mol Cell Endocrinol 2001;183: de Gooyer ME, Oppers-Tiemissen HM, Leysen D, Verheul HAM, Kloosterboer HJ. Tibolone is not converted by human aromatase to 7 -methyl-17 -ethynylestradiol (7 -MEE): analyses with sensitive bioassays for estrogens and androgens and with LC-MSMS. Steroids 2003;68: Dören M, Röbig A, Coelingh Bennink HJT, Holzgreve W. Differential effects on the androgen status of postmenopausal women treated with tibolone and continuous combined estradiol and norethindrone acetate replacement therapy. Fertil Steril 2001;75: Isaksson E, von Schoultz E, Odlind V, Söderqvist G, Csemiczky G, Calström K, et al. Effects of oral contraceptives on breast epithelial proliferation. Breast Cancer Res Treat 2001;65: Zhou J, Ng S. Testosterone inhibits estrogen-induced mammary epithelial proliferation and suppresses estrogen receptor expression. FASEB J 2000;14: FERTILITY & STERILITY 623
Long-term effects of tibolone on mammographic density. Key Words: Tibolone, mammographic density, long-term use
 FERTILITY AND STERILITY VOL. 82, NO. 5, NOVEMBER 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. MENOPAUSE Long-term effects
FERTILITY AND STERILITY VOL. 82, NO. 5, NOVEMBER 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. MENOPAUSE Long-term effects
Mammographic density increase in women receiving different hormone replacement regimens
 Maturitas 40 (2001) 151 157 www.elsevier.com/locate/maturitas Mammographic density increase in women receiving different hormone replacement regimens Cemal Tamer Erel a, *, Gul Esen b, Hakan Seyisoglu
Maturitas 40 (2001) 151 157 www.elsevier.com/locate/maturitas Mammographic density increase in women receiving different hormone replacement regimens Cemal Tamer Erel a, *, Gul Esen b, Hakan Seyisoglu
NEW SELECTIVE TISSUE ESTROGENIC ACTIVITY REGULATOR (STEAR) IN MENOPAUSAL THERAPY IN TAIWAN
 ORIGINAL ARTICLE Tibolone Compliance and Efficacy in Women Living in Taiwan NEW SELECTIVE TISSUE ESTROGENIC ACTIVITY REGULATOR (STEAR) IN MENOPAUSAL THERAPY IN TAIWAN Kuan-Chong Chao*, Peng-Hui Wang, Ming-Shyen
ORIGINAL ARTICLE Tibolone Compliance and Efficacy in Women Living in Taiwan NEW SELECTIVE TISSUE ESTROGENIC ACTIVITY REGULATOR (STEAR) IN MENOPAUSAL THERAPY IN TAIWAN Kuan-Chong Chao*, Peng-Hui Wang, Ming-Shyen
The relationship between mammographic density and duration of hormone therapy: effects of estrogen and estrogen progestin
 Human Reproduction Vol.20, No.6 pp. 1741 1745, 2005 Advance Access publication April 21, 2005 doi:10.1093/humrep/deh820 The relationship between mammographic density and duration of hormone therapy: effects
Human Reproduction Vol.20, No.6 pp. 1741 1745, 2005 Advance Access publication April 21, 2005 doi:10.1093/humrep/deh820 The relationship between mammographic density and duration of hormone therapy: effects
CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY
 Biomed. Papers 147(2), 211 219 (2003) D. Houserková, J. Matlochová, M. Hartlová 211 CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY Dana Houserková
Biomed. Papers 147(2), 211 219 (2003) D. Houserková, J. Matlochová, M. Hartlová 211 CHANGES IN MAMMOGRAPHIC AND ULTRASOUND IMAGE OF THE BREAST OF WOMEN UNDERGOING ESTROGEN REPLACEMENT THERAPY Dana Houserková
Effects of a short-term suspension of hormone replacement therapy on mammographic density
 FERTILITY AND STERILITY VOL. 76, NO. 3, SEPTEMBER 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Effects of a short-term
FERTILITY AND STERILITY VOL. 76, NO. 3, SEPTEMBER 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Effects of a short-term
Received for publication October 19, 2005; revised March 8, 2006; accepted March 8, 2006
 American Journal of Obstetrics and Gynecology (2006) 195, 1320 7 www.ajog.org Effects of Tibolone and Continuous Combined Conjugated Equine Estrogen/Medroxyprogesterone Acetate on the Endometrium and Vaginal
American Journal of Obstetrics and Gynecology (2006) 195, 1320 7 www.ajog.org Effects of Tibolone and Continuous Combined Conjugated Equine Estrogen/Medroxyprogesterone Acetate on the Endometrium and Vaginal
Postmenopausal hormone therapy and cancer risk
 International Congress Series 1279 (2005) 133 140 www.ics-elsevier.com Postmenopausal hormone therapy and cancer risk P. Kenemans*, R.A. Verstraeten, R.H.M. Verheijen Department of Obstetrics and Gynaecology,
International Congress Series 1279 (2005) 133 140 www.ics-elsevier.com Postmenopausal hormone therapy and cancer risk P. Kenemans*, R.A. Verstraeten, R.H.M. Verheijen Department of Obstetrics and Gynaecology,
In vitro studies of tibolone in breast cells
 FERTILITY AND STERILITY VOL. 78, NO. 2, AUGUST 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. In vitro studies of
FERTILITY AND STERILITY VOL. 78, NO. 2, AUGUST 2002 Copyright 2002 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. In vitro studies of
Department of Obstetrics and Gynecology, Karolinska Hospital, Stockholm, Sweden
 FERTILITY AND STERILITY VOL. 81, NO. 6, JUNE 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. MENOPAUSE Mammographic breast
FERTILITY AND STERILITY VOL. 81, NO. 6, JUNE 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. MENOPAUSE Mammographic breast
Influence of different HRT regimens on mammographic density
 Maturitas 50 (2005) 105 110 Influence of different HRT regimens on mammographic density Hans Junkermann a,, Thomas von Holst b, Eva Lang c, Viatcheslav Rakov c a Ruprecht-Karls-Universität Heidelberg,
Maturitas 50 (2005) 105 110 Influence of different HRT regimens on mammographic density Hans Junkermann a,, Thomas von Holst b, Eva Lang c, Viatcheslav Rakov c a Ruprecht-Karls-Universität Heidelberg,
5. Summary of Data Reported and Evaluation
 326 5. Summary of Data Reported and Evaluation 5.1 Exposure data Combined estrogen progestogen menopausal therapy involves the co-administration of an estrogen and a progestogen to peri- or postmenopausal
326 5. Summary of Data Reported and Evaluation 5.1 Exposure data Combined estrogen progestogen menopausal therapy involves the co-administration of an estrogen and a progestogen to peri- or postmenopausal
Preventing Breast Cancer in HT users by Manuel Neves-e-Castro Portuguese Menopause Society September 2004
 Preventing Breast Cancer in HT users by Manuel Neves-e-Castro Portuguese Menopause Society September 2004 I am also PRO!... because HT does not increase breast cancer, and overall, its benefits out weight
Preventing Breast Cancer in HT users by Manuel Neves-e-Castro Portuguese Menopause Society September 2004 I am also PRO!... because HT does not increase breast cancer, and overall, its benefits out weight
4. Other Data Relevant to an Evaluation of Carcinogenicity and its Mechanisms
 550 4. Other Data Relevant to an Evaluation of Carcinogenicity and its Mechanisms 4.1 Absorption, distribution, metabolism and excretion 4.1.1 Humans The pharmacokinetics of the newer progestogens, desogestrel,
550 4. Other Data Relevant to an Evaluation of Carcinogenicity and its Mechanisms 4.1 Absorption, distribution, metabolism and excretion 4.1.1 Humans The pharmacokinetics of the newer progestogens, desogestrel,
Tibolone: Clinical recommendations and practical guidelines A report of the International Tibolone Consensus Group
 Maturitas 51 (2005) 21 28 Tibolone: Clinical recommendations and practical guidelines A report of the International Tibolone Consensus Group P. Kenemans a,, L. Speroff b for the International Tibolone
Maturitas 51 (2005) 21 28 Tibolone: Clinical recommendations and practical guidelines A report of the International Tibolone Consensus Group P. Kenemans a,, L. Speroff b for the International Tibolone
ARTICLES. Postmenopausal Hormone Therapy and Change in Mammographic Density
 ARTICLES Postmenopausal Hormone Therapy and Change in Mammographic Density Gail A. Greendale, Beth A. Reboussin, Stacey Slone, Carol Wasilauskas, Malcolm C. Pike, Giske Ursin Background: Mammographic density
ARTICLES Postmenopausal Hormone Therapy and Change in Mammographic Density Gail A. Greendale, Beth A. Reboussin, Stacey Slone, Carol Wasilauskas, Malcolm C. Pike, Giske Ursin Background: Mammographic density
Postmenopausal hormone therapy before and after breast cancer: clinical experiences
 Maturitas 49 (2004) S22 S31 Postmenopausal hormone therapy before and after breast cancer: clinical experiences N.J. Bundred, L.E. Turner Education and Research Centre, South Manchester University Hospital,
Maturitas 49 (2004) S22 S31 Postmenopausal hormone therapy before and after breast cancer: clinical experiences N.J. Bundred, L.E. Turner Education and Research Centre, South Manchester University Hospital,
Learning Objectives. Peri menopause. Menopause Overview. Recommendation grading categories
 Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
Mammographic Density a Risk Factor for Breast Cancer
 Prague Medical Report / Vol. 108 (2007) No. 3, p. 205 214 205) Mammographic Density a Risk Factor for Breast Cancer Fait T., Žižka Z. Department of Gynaecology and Obstetrics, Charles University in Prague,
Prague Medical Report / Vol. 108 (2007) No. 3, p. 205 214 205) Mammographic Density a Risk Factor for Breast Cancer Fait T., Žižka Z. Department of Gynaecology and Obstetrics, Charles University in Prague,
During the last few years, serious concerns
 Menopause: The Journal of The North American Menopause Society Vol. 14, No. 1, pp. 89-96 DOI: 10.1097/01.gme.0000230346.20992.34 * 2007 by The North American Menopause Society 5 Text printed on acid-free
Menopause: The Journal of The North American Menopause Society Vol. 14, No. 1, pp. 89-96 DOI: 10.1097/01.gme.0000230346.20992.34 * 2007 by The North American Menopause Society 5 Text printed on acid-free
Safety of tibolone in the treatment of vasomotor symptoms in breast cancer patients Design and baseline data 'LIBERATE' trial
 Safety of tibolone in the treatment of vasomotor symptoms in breast cancer patients Design and baseline data 'LIBERATE' trial E. Kubista a, P. Kenemans b, J.M. Foidart c, C.H. Yip d, B. von Schoultz e,
Safety of tibolone in the treatment of vasomotor symptoms in breast cancer patients Design and baseline data 'LIBERATE' trial E. Kubista a, P. Kenemans b, J.M. Foidart c, C.H. Yip d, B. von Schoultz e,
Melatonin and its Role in the Inhibition of Breast Cancer Ciara Nicol Ross Copyright 2014 by Ciara Ross and Koni Stone
 1 Melatonin and its Role in the Inhibition of Breast Cancer Ciara Nicol Ross Copyright 2014 by Ciara Ross and Koni Stone Cancer is a disease caused by out of control division of abnormal cells within a
1 Melatonin and its Role in the Inhibition of Breast Cancer Ciara Nicol Ross Copyright 2014 by Ciara Ross and Koni Stone Cancer is a disease caused by out of control division of abnormal cells within a
Correlation of Estrogen Sulfotransferase Activity and Proliferation in Normal and Carcinomatous Human Breast. A Hypothesis
 Correlation of Estrogen Sulfotransferase Activity and Proliferation in Normal and Carcinomatous Human Breast. A Hypothesis JORGE RAUL PASQUALINI 1 and GERARD SAMUEL CHETRITE 2 1 Hormones and Cancer Research
Correlation of Estrogen Sulfotransferase Activity and Proliferation in Normal and Carcinomatous Human Breast. A Hypothesis JORGE RAUL PASQUALINI 1 and GERARD SAMUEL CHETRITE 2 1 Hormones and Cancer Research
5. Summary of Data Reported and Evaluation
 168 IARC MONOGRAPHS VOLUME 91 5. Summary of Data Reported and Evaluation 5.1 Exposure data The first oral hormonal contraceptives that were found to inhibit both ovulation and implantation were developed
168 IARC MONOGRAPHS VOLUME 91 5. Summary of Data Reported and Evaluation 5.1 Exposure data The first oral hormonal contraceptives that were found to inhibit both ovulation and implantation were developed
Serum estrogen level after hormone replacement therapy and body mass index in postmenopausal and bilaterally ovariectomized women
 Maturitas 50 (2005) 19 29 Serum estrogen level after hormone replacement therapy and body mass index in postmenopausal and bilaterally ovariectomized women Toshiyuki Yasui a,, Hirokazu Uemura a, Yuka Umino
Maturitas 50 (2005) 19 29 Serum estrogen level after hormone replacement therapy and body mass index in postmenopausal and bilaterally ovariectomized women Toshiyuki Yasui a,, Hirokazu Uemura a, Yuka Umino
Management of Perimenopausal symptoms
 Management of Perimenopausal symptoms Serge Rozenberg CHU St Pierre Université libre de Bruxelles Belgium serge_rozenberg@stpierre-bru.be serge.rozenberg@skynet.be Conflict of interest & Disclosure Conflicts
Management of Perimenopausal symptoms Serge Rozenberg CHU St Pierre Université libre de Bruxelles Belgium serge_rozenberg@stpierre-bru.be serge.rozenberg@skynet.be Conflict of interest & Disclosure Conflicts
d Pathology and Cytology, and e Oncology, Radiumhemmet,
 Digitized assessment of mammographic breast density in patients who received low-dose intrauterine levonorgestrel in continuous combination with oral estradiol valerate: a pilot study Eva Lundström, M.D.,
Digitized assessment of mammographic breast density in patients who received low-dose intrauterine levonorgestrel in continuous combination with oral estradiol valerate: a pilot study Eva Lundström, M.D.,
Hormone replacement therapy after breast cancer: 10 year follow up of the Stockholm randomised trial
 European Journal of Cancer (2013) 49, 52 59 Available at www.sciencedirect.com journalhomepage:www.ejcancer.info Hormone replacement therapy after breast cancer: 10 year follow up of the Stockholm randomised
European Journal of Cancer (2013) 49, 52 59 Available at www.sciencedirect.com journalhomepage:www.ejcancer.info Hormone replacement therapy after breast cancer: 10 year follow up of the Stockholm randomised
Appendix: Reference Table of HT Brand Names
 Appendix: Reference Table of HT Brand Names This is a full reference table in alphabetical order, of Brand Name drugs used in HT. It is the basis for prescription advice throughout this handbook. Drug
Appendix: Reference Table of HT Brand Names This is a full reference table in alphabetical order, of Brand Name drugs used in HT. It is the basis for prescription advice throughout this handbook. Drug
Effects of TX-001HR on Uterine Bleeding Rates in Menopausal Women with Vasomotor Symptoms
 Effects of TX-001HR on Uterine Bleeding Rates in Menopausal Women with Vasomotor Symptoms Photo (compulsory) Steven R Goldstein, MD 1 ; Ginger D Constantine, MD 2 ; David F Archer, MD 3 ; James H Pickar,
Effects of TX-001HR on Uterine Bleeding Rates in Menopausal Women with Vasomotor Symptoms Photo (compulsory) Steven R Goldstein, MD 1 ; Ginger D Constantine, MD 2 ; David F Archer, MD 3 ; James H Pickar,
Bioidentical Hormones: Just the Facts
 Bioidentical Hormones: Just the Facts Melissa McNeil, MD, MPH Professor of Medicine and Obstetrics, Gynecology and Reproductive Sciences Chief, Section of Women s Health University of Pittsburgh Disclosures!
Bioidentical Hormones: Just the Facts Melissa McNeil, MD, MPH Professor of Medicine and Obstetrics, Gynecology and Reproductive Sciences Chief, Section of Women s Health University of Pittsburgh Disclosures!
Hormones friend or foe? Undertreatment and quality of life. No conflicts of interest to declare
 Hormones friend or foe? Undertreatment and quality of life Anette Tønnes Pedersen MD, Ph.D. Consultant, Associate professor Dept. Of Gynecology / Fertility Clinic Rigshospitalet No conflicts of interest
Hormones friend or foe? Undertreatment and quality of life Anette Tønnes Pedersen MD, Ph.D. Consultant, Associate professor Dept. Of Gynecology / Fertility Clinic Rigshospitalet No conflicts of interest
Safety of tibolone in the treatment of vasomotor symptoms in breast cancer patients Design and baseline data LIBERATE trial
 THE BREAST The Breast 16 (27) S182 S189 Original Article www.elsevier.com/locate/breast Safety of tibolone in the treatment of vasomotor symptoms in breast cancer patients Design and baseline data LIBERATE
THE BREAST The Breast 16 (27) S182 S189 Original Article www.elsevier.com/locate/breast Safety of tibolone in the treatment of vasomotor symptoms in breast cancer patients Design and baseline data LIBERATE
Amammography report is a key component of the breast
 Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
Hormone. Free Androgen Index. 2-Hydroxyestrone. Reference Range. Hormone. Estrone Ratio. Free Androgen Index
 Hormonal Health PATIENT: Sample Report TEST REF: TST-12345 Hormonal Health 0.61 0.30-1.13 ng/ml DHEA-S 91 35-430 mcg/dl tient: SAMPLE TIENT e: x: N: Sex Binding Globulin 80 18-114 nmol/l Testosterone 0.34
Hormonal Health PATIENT: Sample Report TEST REF: TST-12345 Hormonal Health 0.61 0.30-1.13 ng/ml DHEA-S 91 35-430 mcg/dl tient: SAMPLE TIENT e: x: N: Sex Binding Globulin 80 18-114 nmol/l Testosterone 0.34
HRT, breast and endometrial cancers: strategies and intervention options
 Maturitas 32 (1999) 131 139 www.elsevier.com/locate/maturitas HRT, breast and endometrial cancers: strategies and intervention options Piero Sismondi a, *, Nicoletta Biglia a, Maurizia Giai a, Riccardo
Maturitas 32 (1999) 131 139 www.elsevier.com/locate/maturitas HRT, breast and endometrial cancers: strategies and intervention options Piero Sismondi a, *, Nicoletta Biglia a, Maurizia Giai a, Riccardo
Estrone EIA kit. For the quantitative determination of estrone in dried fecal extracts, urine and tissue culture media. Cat. No.
 K-ASSAY KAMIYA BIOMEDICAL COMPANY KAMIYA BIOMEDICAL COMPANY Estrone EIA kit For the quantitative determination of estrone in dried fecal extracts, urine and tissue culture media Cat. No. KT-720 For Research
K-ASSAY KAMIYA BIOMEDICAL COMPANY KAMIYA BIOMEDICAL COMPANY Estrone EIA kit For the quantitative determination of estrone in dried fecal extracts, urine and tissue culture media Cat. No. KT-720 For Research
HT: Where do we stand after WHI?
 HT: Where do we stand after WHI? Hormone therapy and cardiovascular disease risk Experimental and clinical evidence indicate that hormone therapy (HT) reduces the risk of cardiovascular disease (CVD) Women
HT: Where do we stand after WHI? Hormone therapy and cardiovascular disease risk Experimental and clinical evidence indicate that hormone therapy (HT) reduces the risk of cardiovascular disease (CVD) Women
SPRMs, androgens and breast cancer
 SPRMs, androgens and breast cancer Dr Joëlle Desreux BMS 04/06/2016 WHI : the nuclear explosion Looking for the perfect menopause treatment Hot flushes relieve Osteoporosis prevention Cardio-vascular health
SPRMs, androgens and breast cancer Dr Joëlle Desreux BMS 04/06/2016 WHI : the nuclear explosion Looking for the perfect menopause treatment Hot flushes relieve Osteoporosis prevention Cardio-vascular health
Postmenopausal hormone therapy - cardiac disease risks and benefits
 Postmenopausal hormone therapy - cardiac disease risks and benefits Tomi S. Mikkola, MD Helsinki University Central Hospital Department of Obstetrics and Gynecology Helsinki, Finland Disclosures Speaker/consulting
Postmenopausal hormone therapy - cardiac disease risks and benefits Tomi S. Mikkola, MD Helsinki University Central Hospital Department of Obstetrics and Gynecology Helsinki, Finland Disclosures Speaker/consulting
HKCOG Guidelines. Guidelines for the Administration of Hormone Replacement Therapy. Number 2 revised January 2003
 HKCOG Guidelines Guidelines for the Administration of Hormone Replacement Therapy Number 2 revised January 2003 published by The Hong Kong College of Obstetricians and Gynaecologists A Foundation College
HKCOG Guidelines Guidelines for the Administration of Hormone Replacement Therapy Number 2 revised January 2003 published by The Hong Kong College of Obstetricians and Gynaecologists A Foundation College
LOBULAR CARCINOMA IN SITU: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE
 : WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
MENOPAUSE. I have no disclosures 10/11/18 OBJECTIVES WHAT S NEW? WHAT S SAFE?
 MENOPAUSE WHAT S NEW? WHAT S SAFE? I have no disclosures Sara Whetstone, MD, MHS OBJECTIVES To describe risks of HT by age and menopause onset To recommend specific HT regimen for women who undergo early
MENOPAUSE WHAT S NEW? WHAT S SAFE? I have no disclosures Sara Whetstone, MD, MHS OBJECTIVES To describe risks of HT by age and menopause onset To recommend specific HT regimen for women who undergo early
A literature review examining the association between the duration of hormone replacement therapy (HRT) and the risk of breast cancer in women
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A literature review examining the association between the duration of hormone replacement therapy (HRT)
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects A literature review examining the association between the duration of hormone replacement therapy (HRT)
Hormones and Healthy Bones Joint Project of National Osteoporosis Foundation and Association of Reproductive Health Professionals
 Hormones and Healthy Bones Joint Project of National Osteoporosis Foundation and Association of Reproductive Health Professionals Literature Review (January 2009) Hormone Therapy for Women Women's Health
Hormones and Healthy Bones Joint Project of National Osteoporosis Foundation and Association of Reproductive Health Professionals Literature Review (January 2009) Hormone Therapy for Women Women's Health
LOCAL INFLAMMATION IN BREAST TISSUE AND MAMMOGRAPHIC DENSITY AMONG PREMENOPAUSAL AND POSTMENOPAUSAL WOMEN
 LOCAL INFLAMMATION IN BREAST TISSUE AND MAMMOGRAPHIC DENSITY AMONG PREMENOPAUSAL AND POSTMENOPAUSAL WOMEN Mirette Hanna MD Clinical pathology PhD (candidate) Experimental medicine MSc Clinical and chemical
LOCAL INFLAMMATION IN BREAST TISSUE AND MAMMOGRAPHIC DENSITY AMONG PREMENOPAUSAL AND POSTMENOPAUSAL WOMEN Mirette Hanna MD Clinical pathology PhD (candidate) Experimental medicine MSc Clinical and chemical
Hormone replacement therapy and breast density after surgical menopause
 Hormone replacement therapy and breast density after surgical menopause Freya Schnabel*; Sarah Pivo; Esther Dubrovsky; Jennifer Chun; Shira Schwartz; Amber Guth; Deborah Axelrod Department of Surgery,
Hormone replacement therapy and breast density after surgical menopause Freya Schnabel*; Sarah Pivo; Esther Dubrovsky; Jennifer Chun; Shira Schwartz; Amber Guth; Deborah Axelrod Department of Surgery,
Effects of hormone treatment on sexual functioning in postmenopausal women Nijland, Esmé Aurelia
 University of Groningen Effects of hormone treatment on sexual functioning in postmenopausal women Nijland, Esmé Aurelia IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Effects of hormone treatment on sexual functioning in postmenopausal women Nijland, Esmé Aurelia IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
CORRELATION OF CLINICAL PARAMETERS WITH GLUCOSE TOLERANCE TESTS IN WOMEN TAKING ORAL CONTRACEPTIVES
 FERTIUTY AND STERILITY Copyright 1974 The American Fertility Society Vol. 25, No.7, July 1974 Printed in U.S.A. CORRELATION OF CLINICAL PARAMETERS WITH GLUCOSE TOLERANCE TESTS IN WOMEN TAKING ORAL CONTRACEPTIVES
FERTIUTY AND STERILITY Copyright 1974 The American Fertility Society Vol. 25, No.7, July 1974 Printed in U.S.A. CORRELATION OF CLINICAL PARAMETERS WITH GLUCOSE TOLERANCE TESTS IN WOMEN TAKING ORAL CONTRACEPTIVES
Virtual Mentor Ethics Journal of the American Medical Association November 2005, Volume 7, Number 11
 Virtual Mentor Ethics Journal of the American Medical Association November 2005, Volume 7, Number 11 Clinical Pearl Post Women's Health Initiative Menopausal Women and Hormone Therapy by JoAnn V. Pinkerton,
Virtual Mentor Ethics Journal of the American Medical Association November 2005, Volume 7, Number 11 Clinical Pearl Post Women's Health Initiative Menopausal Women and Hormone Therapy by JoAnn V. Pinkerton,
Low & Ultra Low Dose HRT The Cardiovascular Impact
 Low & Ultra Low Dose HRT The Cardiovascular Impact Wyeth Symposium, Turin 29 th Sept 2007 Nick Panay Consultant Gynaecologist Queen Charlotte s & Chelsea and Chelsea & Westminster Hospitals Honorary Senior
Low & Ultra Low Dose HRT The Cardiovascular Impact Wyeth Symposium, Turin 29 th Sept 2007 Nick Panay Consultant Gynaecologist Queen Charlotte s & Chelsea and Chelsea & Westminster Hospitals Honorary Senior
The selective estrogen enzyme modulators in breast cancer: a review
 Biochimica et Biophysica Acta 1654 (2004) 123 143 www.bba-direct.com Review The selective estrogen enzyme modulators in breast cancer: a review Jorge R. Pasqualini* Hormones and Cancer Research Unit, Institut
Biochimica et Biophysica Acta 1654 (2004) 123 143 www.bba-direct.com Review The selective estrogen enzyme modulators in breast cancer: a review Jorge R. Pasqualini* Hormones and Cancer Research Unit, Institut
Disclosure Information Relationships Relevant to this Session
 Disclosure Information Relationships Relevant to this Session DeCensi, Andrea No relevant relationships to disclose. Please note, all disclosures are reported as submitted to ASCO, and are always available
Disclosure Information Relationships Relevant to this Session DeCensi, Andrea No relevant relationships to disclose. Please note, all disclosures are reported as submitted to ASCO, and are always available
SAMPLE REPORT. Order Number: PATIENT. Age: 40 Sex: F MRN:
 Patient: Age: 40 Sex: F MRN: SAMPLE PATIENT Order Number: Completed: Received: Collected: SAMPLE REPORT Progesterone ng/ml 0.34 0.95 21.00 DHEA-S mcg/dl Testosterone ng/ml 48 35 0.10 0.54 0.80 430 Sex
Patient: Age: 40 Sex: F MRN: SAMPLE PATIENT Order Number: Completed: Received: Collected: SAMPLE REPORT Progesterone ng/ml 0.34 0.95 21.00 DHEA-S mcg/dl Testosterone ng/ml 48 35 0.10 0.54 0.80 430 Sex
HKCOG Guidelines. Guidelines for the Administration of Hormone Replacement Therapy. Number 2 Revised November BENEFITS OF HRT
 HKCOG Guidelines Guidelines for the Administration of Hormone Replacement Therapy Number 2 Revised November 2006 Published by The Hong Kong College of Obstetricians and Gynaecologists A Foundation College
HKCOG Guidelines Guidelines for the Administration of Hormone Replacement Therapy Number 2 Revised November 2006 Published by The Hong Kong College of Obstetricians and Gynaecologists A Foundation College
Prevention of endometrial hyperplasia by progesterone during long-term estradiol replacement: influence of bleeding pattern and secretory changes*
 FERTILITY AND STERILITY Vol. 59, No.5, May 1993 Copyright e 1993 The American Fertility Society Printed on acid-free paper in U.S.A. Prevention of endometrial hyperplasia by progesterone during long-term
FERTILITY AND STERILITY Vol. 59, No.5, May 1993 Copyright e 1993 The American Fertility Society Printed on acid-free paper in U.S.A. Prevention of endometrial hyperplasia by progesterone during long-term
Table of Contents. 1. Overview. 2. Interpretation Guide. 3. Staining Gallery Cases Negative for CINtec PLUS
 Staining Atlas Table of Contents 1. Overview 1.1 Introduction 1.2 Role of p16 INK4a 1.3 Role of Ki-67 1.4 Molecular Pathogenesis 1.5 p16 INK4a Expression in Cervical Dysplasia 1.6 The Concept of CINtec
Staining Atlas Table of Contents 1. Overview 1.1 Introduction 1.2 Role of p16 INK4a 1.3 Role of Ki-67 1.4 Molecular Pathogenesis 1.5 p16 INK4a Expression in Cervical Dysplasia 1.6 The Concept of CINtec
the cumulative rates of persistence with estrogen replacement therapy, CEE/MPA and tibolone;
 Economic impact of tibolone compared with continuous-combined hormone replacement therapy in the management of climacteric symptoms in postmenopausal women Diaby V, Perreault S, Lachaine J Record Status
Economic impact of tibolone compared with continuous-combined hormone replacement therapy in the management of climacteric symptoms in postmenopausal women Diaby V, Perreault S, Lachaine J Record Status
Outline. Estrogens and SERMS The forgotten few! How Does Estrogen Work in Bone? Its Complex!!! 6/14/2013
 Outline Estrogens and SERMS The forgotten few! Clifford J Rosen MD rosenc@mmc.org Physiology of Estrogen and estrogen receptors Actions of estrogen on bone BMD, fracture, other off target effects Cohort
Outline Estrogens and SERMS The forgotten few! Clifford J Rosen MD rosenc@mmc.org Physiology of Estrogen and estrogen receptors Actions of estrogen on bone BMD, fracture, other off target effects Cohort
A cost-utility analysis of low-dose hormone replacement therapy in postmenopausal women with an intact uterus Swift J A, Conway P, Purdie D W
 A cost-utility analysis of low-dose hormone replacement therapy in postmenopausal women with an intact uterus Swift J A, Conway P, Purdie D W Record Status This is a critical abstract of an economic evaluation
A cost-utility analysis of low-dose hormone replacement therapy in postmenopausal women with an intact uterus Swift J A, Conway P, Purdie D W Record Status This is a critical abstract of an economic evaluation
Copyright, 1995, by the Massachusetts Medical Society
 Copyright, 1995, by the Massachusetts Medical Society Volume 332 JUNE 15, 1995 Number 24 THE USE OF ESTROGENS AND PROGESTINS AND THE RISK OF BREAST CANCER IN POSTMENOPAUSAL WOMEN GRAHAM A. COLDITZ, M.B.,
Copyright, 1995, by the Massachusetts Medical Society Volume 332 JUNE 15, 1995 Number 24 THE USE OF ESTROGENS AND PROGESTINS AND THE RISK OF BREAST CANCER IN POSTMENOPAUSAL WOMEN GRAHAM A. COLDITZ, M.B.,
Southern California Center for Sexual Health and Survivorship Medicine Inc, Newport Beach, CA 3
 The WISDOM survey: Physicians Level of Comfort Prescribing Treatment for Vulvar and Vaginal Atrophy (VVA) Symptoms in Women with a Predisposition or History of Breast Cancer Lisa Larkin, MD 1 ; Michael
The WISDOM survey: Physicians Level of Comfort Prescribing Treatment for Vulvar and Vaginal Atrophy (VVA) Symptoms in Women with a Predisposition or History of Breast Cancer Lisa Larkin, MD 1 ; Michael
OBSTETRICS & GYNECOLOGY
 AUGUST 2011 NORLAND AVENUE PHARMACY PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: BHRT for Menopause
AUGUST 2011 NORLAND AVENUE PHARMACY PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: BHRT for Menopause
How Neurosteroids Modulate Seizures in Children and Adults November 30, 2012
 How Neurosteroids Modulate Seizures in Children and Adults November 30, 2012 Page B. Pennell, MD Brigham and Women s Hospital Harvard Medical School Boston, MA American Epilepsy Society Annual Meeting
How Neurosteroids Modulate Seizures in Children and Adults November 30, 2012 Page B. Pennell, MD Brigham and Women s Hospital Harvard Medical School Boston, MA American Epilepsy Society Annual Meeting
25 mg oestradiol implants--the dosage of first choice for subcutaneous oestrogen replacement therapy?
 Research Subcutaneous estrogen replacement therapy. Jones SC. Journal of Reproductive Medicine March, 2004; 49(3):139-142. Department of Obstetrics and Gynecology, Keesler Medical Center, Keesler Air Force
Research Subcutaneous estrogen replacement therapy. Jones SC. Journal of Reproductive Medicine March, 2004; 49(3):139-142. Department of Obstetrics and Gynecology, Keesler Medical Center, Keesler Air Force
1. Collaborative Group on Epidemiological Studies of Ovarian Cancer. Ovarian cancer and oral contraceptives: collaborative reanalysis of data from 45
 1 2 3 1. Collaborative Group on Epidemiological Studies of Ovarian Cancer. Ovarian cancer and oral contraceptives: collaborative reanalysis of data from 45 epidemiological studies including 23,257 women
1 2 3 1. Collaborative Group on Epidemiological Studies of Ovarian Cancer. Ovarian cancer and oral contraceptives: collaborative reanalysis of data from 45 epidemiological studies including 23,257 women
New products and regimens (since 2003)
 CLIMACTERIC 2007;10(Suppl 2):109 114 New products and regimens (since 2003) N. West London Menopause & PMS Centre, London, UK Key words: HORMONE REPLACEMENT THERAPY, ULTRA-LOW-DOSE THERAPY, TRANSDERMAL
CLIMACTERIC 2007;10(Suppl 2):109 114 New products and regimens (since 2003) N. West London Menopause & PMS Centre, London, UK Key words: HORMONE REPLACEMENT THERAPY, ULTRA-LOW-DOSE THERAPY, TRANSDERMAL
Natural Hormones Replacement An Evidence and Practice Based Approach
 Natural Hormones Replacement An Evidence and Practice Based Approach Andres Ruiz, PharmD, MSc, FACA President/Partner Stonegate Pharmacy PRESENTED BY THE AMERICAN COLLEGE OF APOTHECARIES 2830 SUMMER OAKS
Natural Hormones Replacement An Evidence and Practice Based Approach Andres Ruiz, PharmD, MSc, FACA President/Partner Stonegate Pharmacy PRESENTED BY THE AMERICAN COLLEGE OF APOTHECARIES 2830 SUMMER OAKS
Discussing breast cancer and hormone replacement therapy with women
 INTERPRETING KEY TRIALS PELIN BATUR, MD Section of Women s Health, Department of General Internal Medicine, Gault Women s Health and Breast Pavilion, The Cleveland Clinic HOLLY L. THACKER, MD, FACP Departments
INTERPRETING KEY TRIALS PELIN BATUR, MD Section of Women s Health, Department of General Internal Medicine, Gault Women s Health and Breast Pavilion, The Cleveland Clinic HOLLY L. THACKER, MD, FACP Departments
Estrogens & Antiestrogens
 Estrogens & Antiestrogens Menstrual cycle... Changes and hormonal events Natural estrogens: Estadiol >> Estrone > Estriol Ineffective orally Synthesis: From cholesterol ; role of aromatase enzyme in converting
Estrogens & Antiestrogens Menstrual cycle... Changes and hormonal events Natural estrogens: Estadiol >> Estrone > Estriol Ineffective orally Synthesis: From cholesterol ; role of aromatase enzyme in converting
Said Saleh. Department of Obstetrics and Gynecology, Faculty of Medicine, Menoufia University, Menoufia, Egypt
 ARC Journal of Gynecology and Obstetrics Volume 1, Issue 2, 2016, PP 7-12 ISSN No. (Online) 2456-0561 http://dx.doi.org/10.20431/2456-0561.0102003 www.arcjournals.org Efficacy and Acceptability of two
ARC Journal of Gynecology and Obstetrics Volume 1, Issue 2, 2016, PP 7-12 ISSN No. (Online) 2456-0561 http://dx.doi.org/10.20431/2456-0561.0102003 www.arcjournals.org Efficacy and Acceptability of two
9/27/2017. Disclosure. Selecting Progestogens: Breast, Cardiovascular, and Cognitive Outcomes. James H Liu, MD. Overview
 Disclosure Selecting Progestogens: Breast, Cardiovascular, and Cognitive utcomes James H Liu, MD Arthur H Bill Professor and Chair Departments of Reproductive Biology and bstetrics and Gynecology UH Cleveland
Disclosure Selecting Progestogens: Breast, Cardiovascular, and Cognitive utcomes James H Liu, MD Arthur H Bill Professor and Chair Departments of Reproductive Biology and bstetrics and Gynecology UH Cleveland
Disease Test Result Present Absent Total Positive A B N 1 = A+B Negative C D N 2 =C+D Total M 1 =A+C M 2 =B+D N 1 +N 2 =M 1 +M 2
 Basic Definitions and Concepts Disease Test Result Present Absent Total Positive A B N 1 = A+B Negative C D N 2 =C+D Total M 1 =A+C M 2 =B+D N 1 +N 2 =M 1 +M 2 Examples The following example was extracted
Basic Definitions and Concepts Disease Test Result Present Absent Total Positive A B N 1 = A+B Negative C D N 2 =C+D Total M 1 =A+C M 2 =B+D N 1 +N 2 =M 1 +M 2 Examples The following example was extracted
Intrauterine delivery of progestogen in the peri- and postmenopausal women. Outline of the presentation. Levonorgestrel releasing IUS - Mirena
 QuickTime ja Valokuva - JPEG pakkauksen purkuohjelma tarvitaan elokuvan katselemiseen. Intrauterine delivery of progestogen in the peri- and postmenopausal women ESHRE Campus meeting 6.-7.10.2008 Oskari
QuickTime ja Valokuva - JPEG pakkauksen purkuohjelma tarvitaan elokuvan katselemiseen. Intrauterine delivery of progestogen in the peri- and postmenopausal women ESHRE Campus meeting 6.-7.10.2008 Oskari
Research. Breast cancer represents a major
 Research GENERAL GYNECOLOGY Gynecologic conditions in participants in the NSABP breast cancer prevention study of tamoxifen and raloxifene (STAR) Carolyn D. Runowicz, MD; Joseph P. Costantino, DrPH; D.
Research GENERAL GYNECOLOGY Gynecologic conditions in participants in the NSABP breast cancer prevention study of tamoxifen and raloxifene (STAR) Carolyn D. Runowicz, MD; Joseph P. Costantino, DrPH; D.
Mammographic Density Estimation by Volpara software: Comparison with Radiologists' visual assessment and relationship with BI-RADS category
 Mammographic Density Estimation by Volpara software: Comparison with Radiologists' visual assessment and relationship with BI-RADS category Poster No.: C-1957 Congress: ECR 2014 Type: Authors: Keywords:
Mammographic Density Estimation by Volpara software: Comparison with Radiologists' visual assessment and relationship with BI-RADS category Poster No.: C-1957 Congress: ECR 2014 Type: Authors: Keywords:
Women s Health: Managing Menopause. Jane S. Sillman, MD Assistant Professor of Medicine Harvard Medical School
 Women s Health: Managing Menopause Jane S. Sillman, MD Assistant Professor of Medicine Harvard Medical School Disclosures I have no conflicts of interest. Learning Objectives 1. Apply strategies to help
Women s Health: Managing Menopause Jane S. Sillman, MD Assistant Professor of Medicine Harvard Medical School Disclosures I have no conflicts of interest. Learning Objectives 1. Apply strategies to help
Department of Obstetrics and Gynecology, Osaka Medical College, Takatsuki-city, Osaka , Japan. Pituitary gonadotropin, Clinical managament
 Original Article Adequate Reduction Degree of Pituitary Gonadotropin Level in the Clinical Management of Short-Term Hormone Replacement Therapy of Women with Menopausal Symptoms Department of Obstetrics
Original Article Adequate Reduction Degree of Pituitary Gonadotropin Level in the Clinical Management of Short-Term Hormone Replacement Therapy of Women with Menopausal Symptoms Department of Obstetrics
Mammary Nodular Hyperplasia in Intact R hesus Monkeys
 Vet. Path. 10: 130-134 (1973) Mammary Nodular Hyperplasia in Intact R hesus Monkeys L. W NELSON and L. D. SHOTT Department of Pathology and Toxicology, Mead Johnson Research Center, Evansville, Ind., and
Vet. Path. 10: 130-134 (1973) Mammary Nodular Hyperplasia in Intact R hesus Monkeys L. W NELSON and L. D. SHOTT Department of Pathology and Toxicology, Mead Johnson Research Center, Evansville, Ind., and
WHI Estrogen--Progestin vs. Placebo (Women with intact uterus)
 HORMONE REPLACEMENT THERAPY In the historical period it was commonly held that estrogen had two principal benefits to postmenopausal women: 1) To alleviate the constitutional symptoms related to the climacteric
HORMONE REPLACEMENT THERAPY In the historical period it was commonly held that estrogen had two principal benefits to postmenopausal women: 1) To alleviate the constitutional symptoms related to the climacteric
Tamoxifen and Mammographic Breast Densities 1
 Vol. 9, 911 915, September 2000 Cancer Epidemiology, Biomarkers & Prevention 911 Tamoxifen and Mammographic Breast Densities 1 Jacques Brisson, 2 Benoit Brisson, Gary Coté, Elizabeth Maunsell, Sylvie Bérubé,
Vol. 9, 911 915, September 2000 Cancer Epidemiology, Biomarkers & Prevention 911 Tamoxifen and Mammographic Breast Densities 1 Jacques Brisson, 2 Benoit Brisson, Gary Coté, Elizabeth Maunsell, Sylvie Bérubé,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
CPC 4 Breast Cancer. Rochelle Harwood, a 35 year old sales assistant, presents to her GP because she has noticed a painless lump in her left breast.
 CPC 4 Breast Cancer Rochelle Harwood, a 35 year old sales assistant, presents to her GP because she has noticed a painless lump in her left breast. 1. What are the most likely diagnoses of this lump? Fibroadenoma
CPC 4 Breast Cancer Rochelle Harwood, a 35 year old sales assistant, presents to her GP because she has noticed a painless lump in her left breast. 1. What are the most likely diagnoses of this lump? Fibroadenoma
LET S START WITH (AND REMEMBER WE ARE TALKING ABOUT LOCAL E2) THERAPUTIC AGENTS: ARE THEY SAFE? Systemic HT/ET. Ospemifene. Local Estrogen Therapy
 THERAPUTIC AGENTS: ARE THEY SAFE? Steven R. Goldstein, M.D. Professor of Obstetrics & Gynecology New York University School of Medicine Director of Gynecologic Ultrasound Co-Director of Bone Densitometry
THERAPUTIC AGENTS: ARE THEY SAFE? Steven R. Goldstein, M.D. Professor of Obstetrics & Gynecology New York University School of Medicine Director of Gynecologic Ultrasound Co-Director of Bone Densitometry
Menopausal Symptoms. Hormone Therapy Products Available in Canada for the Treatment of. Physician Desk Reference - 3rd Edition
 Hormone Therapy Products Available in Canada for the Treatment of Menopausal Symptoms Physician Desk Reference - 3rd Edition A clinical resource provided to you by: The Society of Obstetricians and Gynaecologists
Hormone Therapy Products Available in Canada for the Treatment of Menopausal Symptoms Physician Desk Reference - 3rd Edition A clinical resource provided to you by: The Society of Obstetricians and Gynaecologists
Sexual dysfunction: Is it all about hormones?
 Sexual dysfunction: Is it all about hormones? Angelica Lindén Hirschberg, MD, PhD, Professor Department of Women s and Children s Health, Karolinska Institutet and Karolinska University Hospital, Stockholm,
Sexual dysfunction: Is it all about hormones? Angelica Lindén Hirschberg, MD, PhD, Professor Department of Women s and Children s Health, Karolinska Institutet and Karolinska University Hospital, Stockholm,
Breast Density. Information for Health Professionals
 Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
Tissue Breast Density
 Tissue Breast Density Reporting breast density within the letter to the patient is now mandated by VA law. Therefore, this website has been established by Peninsula Radiological Associates (PRA), the radiologists
Tissue Breast Density Reporting breast density within the letter to the patient is now mandated by VA law. Therefore, this website has been established by Peninsula Radiological Associates (PRA), the radiologists
PERIMENOPAUSE. Objectives. Disclosure. The Perimenopause Perimenopause Menopause. Definitions of Menopausal Transition: STRAW.
 PERIMENOPAUSE Patricia J. Sulak, MD Founder, Living WELL Aware LLC Author, Should I Fire My Doctor? Author, Living WELL Aware: Eleven Essential Elements to Health and Happiness Endowed Professor Texas
PERIMENOPAUSE Patricia J. Sulak, MD Founder, Living WELL Aware LLC Author, Should I Fire My Doctor? Author, Living WELL Aware: Eleven Essential Elements to Health and Happiness Endowed Professor Texas
The Radiology Aspects
 REQUIREMENTS FOR INTERNATIONAL ACCREDITATION OF BREAST CENTERS/UNITS The Radiology Aspects Miri Sklair-Levy, Israel RADIOLOGY GUIDELINES FOR QUALITY ASSURANCE IN BREAST CANCER SCREENING AND DIAGNOSIS Radiologists
REQUIREMENTS FOR INTERNATIONAL ACCREDITATION OF BREAST CENTERS/UNITS The Radiology Aspects Miri Sklair-Levy, Israel RADIOLOGY GUIDELINES FOR QUALITY ASSURANCE IN BREAST CANCER SCREENING AND DIAGNOSIS Radiologists
Sex Hormones in Postmenopausal Women Receiving Low-Dose Hormone Therapy: The Effect of BMI
 nature publishing group Sex Hormones in Postmenopausal Women Receiving Low-Dose Hormone Therapy: The Effect of BMI Irene Lambrinoudaki 1, Eleni Armeni 1, Demetrios Rizos 2, Eythimios Deligeoroglou 1, Panagiotis
nature publishing group Sex Hormones in Postmenopausal Women Receiving Low-Dose Hormone Therapy: The Effect of BMI Irene Lambrinoudaki 1, Eleni Armeni 1, Demetrios Rizos 2, Eythimios Deligeoroglou 1, Panagiotis
Potential Value of Hormone Receptor Assay in Carcinoma In Situ of Breast
 Potential Value of Hormone Receptor Assay in Carcinoma In Situ of Breast ROBERT BARNES, M.D. AND SHAHLA MASOOD, M.D. The estrogen receptor (ER) expression of invasive breast cancer has been extensively
Potential Value of Hormone Receptor Assay in Carcinoma In Situ of Breast ROBERT BARNES, M.D. AND SHAHLA MASOOD, M.D. The estrogen receptor (ER) expression of invasive breast cancer has been extensively
Imaging in breast cancer. Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since
 Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Dense Breasts, Get Educated
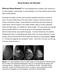 Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
The Practice Committee of the American Society for Reproductive Medicine,
 FERTILITY AND STERILITY VOL. 81, NO. 1, JANUARY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. PRACTICE COMMITTEE Estrogen
FERTILITY AND STERILITY VOL. 81, NO. 1, JANUARY 2004 Copyright 2004 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. PRACTICE COMMITTEE Estrogen
Menopausal hormone therapy currently has no evidence-based role for
 IN PERSPECTIVE HT and CVD Prevention: From Myth to Reality Nanette K. Wenger, M.D. What the studies show, in a nutshell The impact on coronary prevention Alternative solutions Professor of Medicine (Cardiology),
IN PERSPECTIVE HT and CVD Prevention: From Myth to Reality Nanette K. Wenger, M.D. What the studies show, in a nutshell The impact on coronary prevention Alternative solutions Professor of Medicine (Cardiology),
HRT in Perimenopausal Women. Dr. Rubina Yasmin Asst. Prof. Medicine Dhaka Dental College
 HRT in Perimenopausal Women Dr. Rubina Yasmin Asst. Prof. Medicine Dhaka Dental College 1 This is the Change But the CHANGE is not a disease 2 Introduction With a marked increase in longevity, women now
HRT in Perimenopausal Women Dr. Rubina Yasmin Asst. Prof. Medicine Dhaka Dental College 1 This is the Change But the CHANGE is not a disease 2 Introduction With a marked increase in longevity, women now
RCD24, B7-H4 and PCNA expression and clinical significance in ovarian cancer
 JBUON 2019; 24(2): 715-719 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE RCD24, B7-H4 and PCNA expression and clinical significance in ovarian
JBUON 2019; 24(2): 715-719 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE RCD24, B7-H4 and PCNA expression and clinical significance in ovarian
S. Murgo, MD. Chr St-Joseph, Mons Erasme Hospital, Brussels
 S. Murgo, MD Chr St-Joseph, Mons Erasme Hospital, Brussels? Introduction Mammography reports are sometimes ambiguous and indecisive. ACR has developped the BIRADS. BIRADS consists of a lexicon in order
S. Murgo, MD Chr St-Joseph, Mons Erasme Hospital, Brussels? Introduction Mammography reports are sometimes ambiguous and indecisive. ACR has developped the BIRADS. BIRADS consists of a lexicon in order
Breast Cancer Risk in Patients Using Hormonal Contraception
 Breast Cancer Risk in Patients Using Hormonal Contraception Bradley L. Smith, Pharm.D. Smith.bradley1@mayo.edu Pharmacy Ground Rounds Mayo Clinic Rochester April 3 rd, 2018 2017 MFMER slide-1 Presentation
Breast Cancer Risk in Patients Using Hormonal Contraception Bradley L. Smith, Pharm.D. Smith.bradley1@mayo.edu Pharmacy Ground Rounds Mayo Clinic Rochester April 3 rd, 2018 2017 MFMER slide-1 Presentation
