DO NOT DUPLICATE. A Comparison of Collagenase to Hydrogel Dressings in Maintenance Debridement and Wound Closure.
|
|
|
- Ada Moody
- 5 years ago
- Views:
Transcription
1 Original research WOUNDS 2012;24(11): From 1 Connecticut Clinical Nursing Associates, LLC, Plymouth, CT; 2 Federal Hill Plastic Surgery, Bristol, CT Address correspondence to: Catherine T. Milne, APRN Connecticut Clinical Nursing Associates, LLC P.O. Box 1535 Bristol, CT ccna2@juno.com A Comparison of Collagenase to Hydrogel Dressings in Maintenance Debridement and Wound Closure Catherine T. Milne, APRN, MSN, CWOCN 1 ; Armann Ciccarelli, MD, FACS 2 ; Mandie Lassy, BSN 1 Abstract: The role of maintenance debridement in wound healing has been well described, yet little is known regarding comparative methods and associated outcomes with this process when using collagenase or hydrogel. Objective. Evaluation of maintenance debridement and wound closure with collagenase compared to hydrogel in institutionalized adults with pressure ulcers from time of necrotic tissue removal up to 84 days from enrollment. Methods. This second phase of a rollover evaluation enrolled only subjects who successfully completed phase 1 (previously reported) from time of necrotic tissue debridement. Subjects received daily dressing changes with either hydrogel or collagenase followed by a standard semiocclusive dressing to evaluate wound-healing parameters and wound closure from initial enrollment to day 84. Investigators blinded to randomization evaluated weekly wound photographs using a digital planimetry software package for wound-healing parameters. Additionally, Pressure Ulcer Scale for Healing (PUSH) Tool and wound bed scores (WBS) were monitored. Results. Eleven of 13 subjects from the collagenase group entered into phase 2, with 4 of the 14 subjects from the hydrogel group. One subject from each group was eliminated within the first week of phase 2. All subjects (n = 3) in the hydrogel group reached complete epithelialization with a mean of 32.6 days. Nine of 10 subjects in the collagenase group reached completed epithelialization with a mean of 45 days. An independent samples t test showed no statistical significance between the 2 groups (P = 0.121) in days to healing. A Fisher s exact test performed on the primary endpoint of complete epithelialization also demonstrated no significant difference in outcomes between the groups (P = 0.99). Mean WBS at the onset of phase 2 was 13.7 (range 12-16), and the PUSH Tool mean score was 1.0 (range 0-3). In aggregating phase 1 and phase 2 data, a difference in the closure rates at the end of the study, 69% (collagenase) vs 21% (hydrogel), was statically significant (P = ) using a Fisher s exact test. Conclusion. Facilitating maintenance debridement by either collagenase or hydrogel can be used to complete wound closure when used in conjunction with a validated predictive wound-healing tool that closely monitors therapy. This study showed statistical significance in favor of collagenase when evaluating closure rates from the onset of the pressure ulcer. Vol. 24, No. 11 November
2 318 WOUNDS Wound bed preparation (WBP) is an established concept in chronic wound management. Addressing the relationship between necrotic tissue, exudate, and bacterial and cellular dysfunction 1 leads to optimal outcomes. Execution of WBP includes eliminating necrotic tissue, bacterial burden, biofilms, edema, and exudate, while promoting the formation of granulation tissue. Debridement is one essential step in accomplishing these goals. Concepts related to debridement have evolved with increased understanding of WBP. Initially considered the removal of visible, nonviable tissue, debridement is further elucidated into 2 distinct phases: initial debridement and maintenance debridement. Initial debridement is defined as the removal of necrotic, damaged, and/or infected tissue. 2 However, despite removal of visibly necrotic tissue, phenotypically altered senescent fibroblasts and keratinocytes, coupled with accumulating extracellular matrix materials and substrates that may contribute to bioburden, need ongoing removal from the wound bed. 2-4 Maintenance debridement offers a continuous removal of cellular burden not visible to the naked eye and frees the wound bed from these obstacles to healing. Falanga s review of in vitro studies suggest that maintenance debridement may recruit functional cells to the chronic wound. 5 Maintenance debridement can be achieved via mechanical, enzymatic, or autolytic means; though there is little literature that associates these concepts in vivo. Regardless, incorporating this key concept in clinical practice is paramount to optimizing wound outcomes. The clinical setting in which maintenance debridement occurs often influences decision-making regarding treatment, as resources, patient populations, and expertise in wound management may differ. Clinicians often change from one therapeutic modality to another when the wound appears to be free from necrotic debris upon visual assessment. A less-skilled clinician often equates the absence of necrotic tissue with wound health, 4 failing to appreciate the pathophysiological processes occurring at the cellular level. Many skilled nursing facilities have adopted predetermined wound protocols, as standardization has been shown to improve wound healing outcomes. 6,7 Many protocols provided by wound care vendors strongly encourage changing from an active debridement process, such as an enzymatic agent, to a product that provides corrective moisture balance when visible, non-viable tissue has been removed. Collagenase has not been traditionally accepted in clinical practice for use beyond the removal of necrotic tissue, though in vitro work suggests collagenase may play a role in reducing formation of biofilms and bacterial proliferation, 8,9 and enhance keratinocyte proliferation and migration. 10,11 While comparison of hydrogel dressings and enzymatic debriding agents on wound healing have been done using swine, 12 there are no reports in the clinical area, or, specifically, the long-term care setting, where these agents are extensively used. The aim of this 2-phase study was to evaluate the outcomes of both hydrogel and collagenase on initial debridement of nonviable tissue and impact on the maintenance debridement phase of wound bed preparation. The results of phase 1, examining initial debridement, have been published. 13 This manuscript reports the time from complete debridement of visible, nonviable tissue to epithelialization from phase 2. Execution of wound bed preparation includes eliminating necrotic tissue, bacterial burden, biofilms, edema, and exudate, while promoting the formation of granulation tissue. Debridement is one essential step in accomplishing these goals. Collagenase has not been traditionally accepted in clinical practice for use beyond the removal of necrotic tissue, though in vitro work suggests collagenase may play a role in reducing formation of biofilms and bacterial proliferation, 8,9 and enhance keratinocyte proliferation and migration. 10,11 While comparison of hydrogel dressings and enzymatic debriding agents on wound healing have been done using swine, 12 there are no reports in the clinical area, or, specifically, the long-term care setting, where these agents are extensively used. Methods The study protocol was approved by the local Institutional Review Boards of the long-term care facilities from which patients were recruited. Patients or their legal representatives were asked to sign a written informed consent prior to entering phase 1. Inclusion and exclusion criteria for phase 1 have been reported, 13 and salient details have been reproduced (Table 1). Subjects were rolled over to phase 2 if complete debridement of all visible, nonviable tissue was complete by day 42, with continuance of pressure redistribution or offloading recommendations, and adherence to dietary intake recommendations. The primary outcome of this evaluation was to determine the number of days needed to achieve epithelialization, capped at 84 days. Secondary outcomes in-
3 Table 1. Inclusion/Exclusion Criteria Inclusion Criteria Age > 18 years Presence of at least 85% necrotic nonviable tissue on a pressure ulcer between 1 cm 2 and 64 cm 2 Hydrogel or collagenase dressing naïve on study pressure ulcer No current use of parenteral or oral antibiotics except for urinary tract suppressive therapy Hemoglobin A1C (HbA1c) < 7.9% Currently receiving adequate pressure redistribution to the affected area via devices such as a group 2 or group 3 specialty bed, and a static air wheelchair cushion if out of bed, and/or an offloading device if the pressure ulcer was located on the lower extremity Compliance with nutritional interventions per registered dietician No allergies to collagenase or hydrogel No allergies to semiocclusive secondary dressing Written informed consent Exclusion Criteria Steroid use > 5 mg daily Inability to cooperate with offloading recommendations Ankle-brachial index < 0.85 if the pressure ulcer was located on the lower extremity Presence of callus requiring sharp or surgical debridement within 3 days prior to enrollment Medical instability as deemed by the investigator Pregnancy Participation in another clinical trial or wound dressing evaluation in the 30 days prior to enrollment cluded the portion of patients with complete wound closure by 84 days, and the evaluation of changes in wound measurements on a weekly basis. Randomization occurred after informed consent was obtained to reduce selection bias. Subjects were assigned to either collagenase (Santyl Ointment, Healthpoint, LTD, Fort Worth, TX) or hydrogel (SoloSite Gel, Smith & Nephew, Largo, FL). Successful completion of phase 1 was determined by visual assessment by 1 investigator, and confirmed by wound photography using calibrated digital wound measurement software (PictZar, BioVisual Technologies, Elmwood Park, NJ) by investigators blinded to randomization category. Subjects remained on the same assigned agent when rolling over into phase 2. Each dressing change consisted of the following: normal saline irrigation with a device providing 4-15 psi (Irri- Max, Weston, FL) followed by application of the assigned therapeutic agent, nickel thick, to the entire wound bed. In the presence of wound depth, after application of the assigned agent, the wound was then filled to the depth equal to that of the surrounding wound tissue with gauze dampened with normal saline, so that there was no excess moisture noted when pressure from the clinician s hand was applied. The wound was then covered with a semi-occlusive dressing (CoverSite, Smith and Nephew, Largo, FL). Dressing changes, performed by the nursing staff at the long-term care facility, occurred on a daily basis and as needed if the dressing integrity was lost due to dislodgement or incontinence. Weekly subject evaluations, including subject and wound assessment, as well as wound photographs, were conducted by the same investigator. Wound photos were evaluated for wound healing parameters using calibrated digital wound measurement software (Pictzar, Biovisual Technologies, Elmwood Park, NJ) by 2 designated investigators blinded to randomization. In addition, each weekly photograph was assigned a wound bed score (WBS) 14 or a Pressure Ulcer Scale for Healing (PUSH) Tool score, as each of these tools has shown reliability and validity in monitoring and predicting wound healing. Nursing staff at each facility were trained by one investigator in the wound dressing procedure. Other methods of debridement were not performed during phase 2. Subjects were assigned to either collagenase or hydrogel. Successful completion of phase 1 was determined by visual assessment by 1 investigator, and confirmed by wound photography using calibrated digital wound measurement software by investigators blinded to randomization category. Subjects remained on the same assigned agent when rolling over into phase 2. Dressing changes, performed by the nursing staff at the long-term care facility, occurred on a daily basis and as needed if the dressing integrity was lost due to dislodgement or incontinence. Results Twenty-seven subjects consented to participate over an enrollment period of 1 year. Thirteen subjects were randomized to the collagenase group; 14 were randomized to the hydrogel group. Data analysis was performed by SPSS. Using Student s t test, there were no significant differences in groups for age, gender, age of wound, or percentage of nonviable tissue at the time of enrollment (P < Vol. 24, No. 11 November
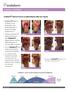
4 Milne et al E leven of the 13 subjects from the collagenase group, and 4 of the 14 subjects from the hydrogel group, entered the portion of the study reported in this paper. One subject from each group was eliminated within the first week of phase 2. All subjects (n=3) in the hydrogel group reached complete epithelialization with a mean of 32.6 days. Nine of the 10 subjects in the collagenase group reached completed epithelialization with a mean of 45 days. An independent samples t test showed no statistical significance between the 2 groups (P = 0.121) in days to healing. Hydrogel group N = 14 Wound Closed 3(21%) Figure 1. Intent-to-treat wound closure rates. U Wound Closed 9(69%) D O N O T D 0.03). More than half of the pressure ulcers (55.5%) were related to devices such as splints, braces, ill-fitting wheelchair arm rests, or prostheses.wound size was statistically different; overall the collagenase group presented with larger wounds (P < 0.004) when entering phase 1. Eleven of the 13 subjects from the collagenase group, and 4 of the 14 subjects from the hydrogel group, entered the portion of the study reported in this paper. One subject from each group was eliminated within the first week of phase 2: 1 collagenase subject was lost to follow-up when transferred to an acute care facility for treatment of pneumonia; and 1 hydrogel subject was discontinued from the study after developing cellulitis at the wound site. Data analysis occurred on 10 of the collagenase and 3 of the hydrogel subjects using SPSS. There were no significant differences using a Student s t test in groups for age, gender, age of wound,wbs, or PUSH Tool score.there were no differences (P = 0.26) in wound size between the 2 groups at the onset of the rollover into phase 2, despite a statistical significance between groups at the onset of the entire study showing greater wound size in the collagenase group than in the hydrogel group (P = 0.04). At the time of complete debridement, 7 patients had stage 3 pressure ulcers (4 collagenase; 3 hydrogel) with the remaining 6 patients having stage 4 pressure ulcers (6 collagenase; 0 hydrogel). Significance in wound pressure 320 WOUNDS ulcer stage was noted using Chi-Squared analysis, with the collagenase group having greater severity (P = 0.03). All subjects (n=3) in the hydrogel group reached complete epithelialization with a mean of 32.6 days. Nine of the 10 subjects in the collagenase group reached completed epithelialization with a mean of 45 days. An independent samples t test showed no statistical significance between the 2 groups (P = 0.121) in days to healing. A Fisher s exact test performed on the primary endpoint of complete epithelialization also demonstrated no significant difference in outcomes between the groups (P = 0.99). The WBS mean at the onset of phase 2 was 13.7 (range 12-16) and the PUSH Tool mean score was 1.0 (range 0-3). Intent-to-treat closure rates were statistically significant (P = ) at the end of the study: 69% (collagenase) vs 21% (hydrogel) using a Fisher s exact test. (Figure 1). Weekly reductions in wound sizes occurred at a greater rate in the collagenase group (P = 0.009) as compared to subjects receiving hydrogel using a Fisher s exact test. PL 84 Days IC Collagenase group N = 13 A TE Patients N = 27 Discussion Hydrogels, which are composed of hydrophilic polymers in a dimensional matrix, are frequently used after the removal of visible necrotic material to provide moisture to the wound bed. By providing an exogenous source of moisture, the body s own physiological mechanisms to achieve wound repair can occur in the optimized environment. Maintenance debridement is achieved via moisture-facilitated cell migration in the absence of dessication18 and thermal insulation.19 Intrinsic enzymes recruited by the moist wound bed environment provided by hydrogel are selective in the protein degradation. This passive method of debridement has been shown to be slow and associated with anaerobic bacteria.18 Hydrophilic components and water content of hydrogels vary,
5 making general comparisons between this class of topical wound treatment and other, nonhydrogel treatments difficult. However, hydrogels have been shown to be superior to moist saline gauze dressings. 20 Hydrogels have shown efficacy in wound healing and now have replaced wet-to-dry dressings as the product category for which to compare outcomes. 21 Bale et al 23 compared 2 amorphous hydrogels and found little difference in time to debridement between them. Eisenbud et al 22 in their review of physiological interaction of hydrogels with the wound bed suggested that one particular hydrogel offered no clinical benefit over any other hydrogel. Collagenase ointment, a metalloproteinase made from the bacteria Clostridium histolyticum, has been studied extensively with regards to its ability to degrade eschar in the clinical setting, though not for maintenance debridement. Herman 10 and Shi et al 11 have shown in vitro ability of collagenase to promote fibroblast proliferation, keratinocyte migration, and growth factor preservation. Falanga first suggested the clinical utility of collagenase in performing maintenance debridement. 3 The ability of collagenase to debride eschar from the edge of the wound while simultaneously promoting angiogenesis and reepithelialization, thus allowing a smaller wound to be managed at the time of complete eschar removal, was postulated. This may be considered a beneficial edge effect of collagenase. The results of this study suggest maintenance debridement begins at the time of initial application of collagenase, lending support to the findings of Margolis et al 24 for predictive significance of wound healing with edge migration. At day 84, there was complete epithelialization in 9 of the 13 intent-to-treat subjects assigned to the collagenase group, which clinically supports previous works by Riley and Herman 12, Herman 10 and Shi et al. 11 As collagenase in vitro avoids nondenatured collagen and other protein degradation, growth factors are preserved. Accumulation of nonviable cellular debris and remaining denatured collagen in the wound bed, invisible to the naked eye, promotes the prolongation of the chronic wound state. This study suggests collagenase may impact this accumulation. Additional studies with larger subject numbers are warranted. In the intent-to-treat hydrogel group, slower closure rates suggest that no edge effect with fibroblast proliferation and keratinocyte migration occurred. As hydrogel success is related to the host s ability to mount the physiological response for wound healing, the quick epithelialization time in the study suggests this group may have improved regardless. This may have influenced the nonstatistical significance between the primary outcome comparing days to healing. Further studies with larger subject numbers should be performed to confirm these findings. The prognostic ability of both the WBS and PUSH Tool to predict complete wound closure supports the previous works in this area. 14, Upper quartiles of the WBS favor wound closure in pressure ulcers with a score of less than 14, as do PUSH Tool scores. Until biological markers that correlate with wound health are routinely available at the bedside, the use of these instruments can provide reliable objectivity to the clinician in guiding treatment decisions. Given cost considerations in the current health care economic climate, changing therapies without objective measurements that support prognostic capability based on wound visualization may not be cost-effective. Of the patients in the rollover analysis reported here, it is important to recognize that the continuum of data from phase 1 and phase 2 provides information on the clinical management of pressure ulcers in long term care. This was addressed by assigning these patients to identical clinical pathways with the only difference being the choice of debridement, enzymatic vs autolytic. In this case, the proportions healed (9 of 13 for collagenase; 3 of 4 for hydrogel) in this intent-to-treat group, encompassing both phases of the evaluation, were assessed at 84 days after the initiation of therapy (Figure 1). In this study, there is a statistically significant difference in the healing rates of 48 percentage points between the collagenase and hydrogel groups. Limitations of this study include the small number of enrolled patients that entered into phase 2. Further exploration into the area of maintenance debridement with Falanga first suggested the clinical utility of collagenase in performing maintenance debridement. 3 The ability of collagenase to debride eschar from the edge of the wound while simultaneously promoting angiogenesis and reepithelialization thus allowing a smaller wound to be managed at the time of complete eschar removal was postulated. This may be considered a beneficial edge effect of collagenase. In the intent-to-treat hydrogel group, slower closure rates suggest that no edge effect with fibroblast proliferation and keratinocyte migration occurred. As hydrogel success is related to the host s ability to mount the physiological response for wound healing, the quick epithelialization time in the study suggests this group may have improved regardless. Vol. 24, No. 11 November
6 these and other agents is required. These results cannot be generalized to all hydrogels owing to their different chemical compositions. Generalizations cannot be made in populations with wounds caused by other etiologies or outside the long-term care setting. Conclusion Pressure ulcer healing continues to be a challenging issue for clinicians in the long-term care setting. In a frail population within a financially stressed health system, this study adds to the evidence base that facilitating maintenance debridement, either by collagenase or hydrogel, can be used to complete wound closure when utilized in conjunction with a validated predictive wound healing tool that closely monitors therapy. References 322 WOUNDS 1. Vowden K, Vowden R. Wound bed preparation. World Wide Wounds. Vowden/Wound-Bed-Preparation.html. Published March Accessed February 23, Falanga V, Brem H, Ennis WJ, Wolcott R, Lisa JG, Ayello EA. Maintenance debridement in the treatment of difficult-to-heal chronic wounds. Ostomy Wound Manage. 2008;54(6)(suppl-1):S1-S Falanga V. Wound bed preparation and the role of enzymes: a case for multiple actions of therapeutic agents. WOUNDS. 2002;14(2): Panuncialman J, Falanga V. The science of wound bed preparation. Clin Plast Surg. 2007;34(4): Falanga V. The chronic wound: impaired healing and solutions in the context of wound bed preparation. Blood Cells Mol Dis. 2004;32(1): Bolton L, McNees P, van Rijswijk L, et al. Wound healing outcomes using standardized assessment and care in clinical practice. J Wound Ostomy Continence Nurs. 2004;31(2): Baier R, Gifford D, Lyder C, Schall M, Funston-Dillin D, Ordin D. Quality improvement for pressure ulcer care in the nursing home setting: the northeast pressure ulcer project. J Am Med Dir Assoc. 2003;4(6): Knox KR, Dariashvili RO, Granick MS. Surgical wound bed preparation of chronic and acute wounds. Clin Plas Surg. 2007;34: Smith RG. Enzymatic debriding agents: an evaluation of the medical literature. Ostomy Wound Manage. 2008;54(8): Herman IM. Stimulation of human keratinocyte migration and proliferation in vitro: insights into the cellular responses to injury and wound healing. WOUNDS. 1996;8(2): Shi L, Ermis R, Garcia A, Telgenhoff D, Aust D. Degradation of human collagen isoforms by clostridium collagenase and the effects of degradation products on cell migration. Int Wound J. 2010;7(2): Riley KN, Herman IM. Collagenase promotes the cellular responses to injury and wound healing in vivo. J Burns Wounds. 2005;4:e8. Epub May 17, Accessed March 3, Milne CT, Ciccarelli A, Lassy M. A comparison of collagenase to hydrogel dressings in wound debridement. WOUNDS. 2010; 22(11): Falanga V, Saap LJ, Ozonoff A. Wound bed score and its correlation with healing of chronic wounds. Dermatol Ther. 2006; 19(6): National Pressure Ulcer Advisory Panel (NPUAP). PUSH tool 3.0. Available at: Accessed February 23, Gardner SE, Hillis SL, Frantz RA. A prospective study of the PUSH tool in diabetic foot ulcers. J Wound Ostomy Continence Nurs. 2011;38(4): Hon J, Lagden K, McLaren AM, et al. A prospective, multicenter study to validate use of the PUSH in patients with diabetic, venous, and pressure ulcers. Ostomy Wound Manage. 2010;56(2): Turner TD. The development of wound management products. In: Krasner DI, Rodeheaver GT, Sibbald RG, eds. Chronic Wound Care: A Clinical Source Book for Healthcare Professionals, 3rd ed. Wayne, PA: HMP Communications; 2001: Morin RJ, Tomaselli NL. Interactive dressings and topical agents. Clin Plastic Surg. 2007; 34(4): Edwards J, Stapley S. Debridement of diabetic foot ulcers. Cochrane Database of Syst Rev. 2010;1:CD Sussman C, Bates-Jensen B. Wound Care: A Collaborative Practice Manual for Health Professionals. 4th Ed. Philadelphia, PA: Lippincott, Williams and Wilkins; Eisenbud D, Hunter H, Kessler L, Zulkowski K. Hydrogel wound dressings: where do we stand in 2003? Ostomy Wound Manage. 2003;49(10): Bale S, Banks V, Haglestein S, Harding KG. A comparison of two amorphous hydrogels in the debridement of pressure sores. J Wound Care. 1998;7(2): Margolis DJ, Allen-Taylor L, Hoffstad O, Berlin JA. The accuracy of venous leg ulcer prognostic models in a wound care system. Wound Repair Regen. 2004;12(2):
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Use of Non-Contact Low Frequency Ultrasound in Wound Care
 Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Prepares wounds to allow natural healing
 ADVANCED CARE OF ACUTE AND CHRONIC WOUNDS Prepares wounds to allow natural healing 0373 Medical Device Hyaluronic Acid and Collagenase COMBINED ACTION IN WOUND REPAIR Hyaluronic acid and collagenase promote
ADVANCED CARE OF ACUTE AND CHRONIC WOUNDS Prepares wounds to allow natural healing 0373 Medical Device Hyaluronic Acid and Collagenase COMBINED ACTION IN WOUND REPAIR Hyaluronic acid and collagenase promote
Use of an outside force to remove nonviable. Wound Debridement Guide South West Regional Wound Care Program Last Updated March 12,
 Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
Worsening Tissue Damage Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term
ACOFP 55th Annual Convention & Scientific Seminars. New Physicians and Residents: Introduction to Wound Care. Katherine Lincoln, DO, FAAFP
 8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
Wound and Ostomy Care: Basics and Troubleshooting
 Wound and Ostomy Care: Basics and Troubleshooting Catherine Clarey-Sanford, PhD, RN, CWOCN Conflict of Interest No conflict of interest exists No commercial interest No financial benefits Specific wound
Wound and Ostomy Care: Basics and Troubleshooting Catherine Clarey-Sanford, PhD, RN, CWOCN Conflict of Interest No conflict of interest exists No commercial interest No financial benefits Specific wound
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
CASE REPORT Use of a Hydroconductive Dressing to Treat a Traumatic Avulsive Injury of the Face
 CASE REPORT Use of a Hydroconductive Dressing to Treat a Traumatic Avulsive Injury of the Face Colin Jerome Perumal, BDS, a and Martin Robson, MD b a Department of Maxillofacial and Oral Surgery, Medical
CASE REPORT Use of a Hydroconductive Dressing to Treat a Traumatic Avulsive Injury of the Face Colin Jerome Perumal, BDS, a and Martin Robson, MD b a Department of Maxillofacial and Oral Surgery, Medical
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Clinical Policy Title: Debridement of diabetic foot ulcers
 Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
A Reprint from Surgical Technology International XXVI
 A Reprint from Surgical Technology International XXVI GENTIAN VIOLET AND METHYLENE BLUE POLYVINYL ALCOHOL FOAM ANTIBACTERIAL DRESSING AS A VIABLE FORM OF AUTOLYTIC DEBRIDEMENT IN THE WOUND BED ANDREW JOSEPH
A Reprint from Surgical Technology International XXVI GENTIAN VIOLET AND METHYLENE BLUE POLYVINYL ALCOHOL FOAM ANTIBACTERIAL DRESSING AS A VIABLE FORM OF AUTOLYTIC DEBRIDEMENT IN THE WOUND BED ANDREW JOSEPH
Palliative Care. EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for. Treatment. Improving Quality of Care Based on CMS Guidelines 39
 Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Pressure Ulcers: 3 Keys to Pressure Ulcer Management. Evidence Based Prevention & Management. I have no financial conflicts of interest
 Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
The VERSAJET II Hydrosurgery System
 Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
CLINICAL EVIDENCE Partial and Deep Partial Burns
 CLINICAL EVIDENCE Partial and Deep Partial Burns Endoform helps to improve re-epithelialization after burn injuries Endoform helps to facilitate tissue granulation and epithelialization in partial and
CLINICAL EVIDENCE Partial and Deep Partial Burns Endoform helps to improve re-epithelialization after burn injuries Endoform helps to facilitate tissue granulation and epithelialization in partial and
DEBRIDEMENT. In This Chapter. Chapter 8. Necrotic Tissue Eschar Slough Types of Debridement When Not to Debride...
 Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Clinical Policy: EpiFix Wound Treatment
 Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
The Proven Multifunctional Dressing
 The Proven Multifunctional Dressing belongs to an innovative class of multifunctional wound care dressings. dressings effectively cleanse, fill, absorb and moisten wounds throughout the healing continuum.
The Proven Multifunctional Dressing belongs to an innovative class of multifunctional wound care dressings. dressings effectively cleanse, fill, absorb and moisten wounds throughout the healing continuum.
Disclosures. Outpatient NPWT Options Free up Hospital Beds, but Do They Work? Objectives. Clinically Effective: Does it Work?
 4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Sarah Medrano, RN, BSN, WOCN; and Mary Jo Beneke, RN, BS, CWOCN Yuma Regional Medical Center, Yuma, Arizona
 Sound Evidence coustic Pressure Wound Therapy to ebride Unstageable Pressure Ulcers in the cute Care Setting: Case Series Sarah Medrano, RN, BSN, WCN; and Mary Jo Beneke, RN, BS, CWCN Yuma Regional Medical
Sound Evidence coustic Pressure Wound Therapy to ebride Unstageable Pressure Ulcers in the cute Care Setting: Case Series Sarah Medrano, RN, BSN, WCN; and Mary Jo Beneke, RN, BS, CWCN Yuma Regional Medical
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Prontosan. Clean. Easy Wound Healing. Wound Cleansing
 Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
NPUAP Mission. Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries. npuap.org
 Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
Pressure Injury Assessment Guide South West Regional Wound Care Program Last Updated October 31,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Precise excision. Preserve viable tissue and reduce time to closure (1,2)
 Precise excision Preserve viable tissue and reduce time to closure (1,2) Precision to preserve Conventional surgical excision Non-viable tissue VERSAJET II excision More precise tissue removal Non-viable
Precise excision Preserve viable tissue and reduce time to closure (1,2) Precision to preserve Conventional surgical excision Non-viable tissue VERSAJET II excision More precise tissue removal Non-viable
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude
 Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
The Risk. Background / Bias. Integrating Wound Care into a Limb Preservation Initiative 4/24/2009
 Stimulating Wound Granulation: Advances in NPWT and other Measures (Wound Bed Preparation) Charles Andersen MD, FACS, FAPWCA Clinical Prof of Surgery UW, USUHS Chief Vascular/Endovascular/ Limb Preservation
Stimulating Wound Granulation: Advances in NPWT and other Measures (Wound Bed Preparation) Charles Andersen MD, FACS, FAPWCA Clinical Prof of Surgery UW, USUHS Chief Vascular/Endovascular/ Limb Preservation
A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer
 Original Research Article A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer S Vijayalakshmi * Associate Professor, Department of General Surgery, Govt.
Original Research Article A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer S Vijayalakshmi * Associate Professor, Department of General Surgery, Govt.
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Topical Oxygen Wound Therapy (MEDICAID)
 Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Comparative cost and clinical effectiveness of clostridial collagenase ointment for chronic dermal ulcers
 For reprint orders, please contact: reprints@futuremedicine.com Comparative cost and clinical effectiveness of clostridial collagenase ointment for chronic dermal ulcers Curtis Waycaster*,1, Marissa J
For reprint orders, please contact: reprints@futuremedicine.com Comparative cost and clinical effectiveness of clostridial collagenase ointment for chronic dermal ulcers Curtis Waycaster*,1, Marissa J
The Georgetown Team Approach to Diabetic Limb Salvage: 2013
 The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
The word debridement derives from the
 Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Wound bed preparation: TIME in practice
 Wound bed preparation: TIME in practice Wound bed preparation is now a well established concept and the TIME framework has been developed as a practical tool to assist practitioners when assessing and
Wound bed preparation: TIME in practice Wound bed preparation is now a well established concept and the TIME framework has been developed as a practical tool to assist practitioners when assessing and
1/5. Introduction. Primary endpoint Time to reach readiness for closure by surgical intervention or left for closure by secondary intention
 1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
Surgical Wounds & Incisions
 Surgical Wounds & Incisions A Comprehensive Review Assessment & Management Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist www.woundcarenurses.org 1
Surgical Wounds & Incisions A Comprehensive Review Assessment & Management Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist www.woundcarenurses.org 1
Ira M. Herman, PhD, FAPWCA Jeffrey D. Lehrman, DPM, FASPS, MAPWCA Lee C. Ruotsi, MD, CWS, UHM Dr. Herman: Dr. Lehrman: Dr. Ruotsi:
 Faculty Ira M. Herman, PhD, FAPWCA Professor and Director Program in Cell, Molecular and Developmental Biology Center for Innovations in Wound Healing Research Tufts University School of Medicine Boston,
Faculty Ira M. Herman, PhD, FAPWCA Professor and Director Program in Cell, Molecular and Developmental Biology Center for Innovations in Wound Healing Research Tufts University School of Medicine Boston,
DEBRIDEMENT. Four Methods of Debridement
 Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
A comprehensive study on effect of collagen dressing in diabetic foot ulcer
 Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Overview. Holistic Approach 07/04/2014. My Resident Has a Chronic Wound. Wound Causes Factors that impair wound healing Wound Assessment
 My Resident Has a Chronic Wound Now What??? Jolene Heil RN ET MClScWH April 8, 2014 Overview Wound Causes Factors that impair wound healing Wound Assessment Holistic Approach What is the cause of the wound?
My Resident Has a Chronic Wound Now What??? Jolene Heil RN ET MClScWH April 8, 2014 Overview Wound Causes Factors that impair wound healing Wound Assessment Holistic Approach What is the cause of the wound?
Understanding and Managing
 Understanding and Managing MM s in Wound Bed Brock Liden DM, ABM, FAWCA Learning Objectives Review the four sequential phases of normal wound healing and recognize the BENEFICIAL effects of CONTROLLED
Understanding and Managing MM s in Wound Bed Brock Liden DM, ABM, FAWCA Learning Objectives Review the four sequential phases of normal wound healing and recognize the BENEFICIAL effects of CONTROLLED
Prediction of healing for post-operative diabetic foot wounds based on early wound area progression
 Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Many patients with chronic wounds. Case reports. The use of Prontosan in combination with Askina Calgitrol : an independent case series
 Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Wound Assessment and Measurement
 Wound Assessment and Measurement Content Creators: Members of the s Clinical Practice and Knowledge Translation Learning Collaborative Learning Objectives 1. Explain the importance and frequency of accurate
Wound Assessment and Measurement Content Creators: Members of the s Clinical Practice and Knowledge Translation Learning Collaborative Learning Objectives 1. Explain the importance and frequency of accurate
o Venous edema o Stasis ulcers o Varicose veins (not including spider veins) o Lipodermatosclerosis
 Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Debridement within the context of the EWMA s debridement guidelines. Emil Schmidt WCNS SDHB - Otago
 Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
BIS TIME management by medicinal larvae Dr. Wilhelm Jung
 Infoservice Larval Therapy up-to-date BIS TIME management Dr. Wilhelm Jung Making healing possible BIS TIME management Original publication: TIME management Pritchard D.I., Cerovsky V., Nigam Y., Pickles
Infoservice Larval Therapy up-to-date BIS TIME management Dr. Wilhelm Jung Making healing possible BIS TIME management Original publication: TIME management Pritchard D.I., Cerovsky V., Nigam Y., Pickles
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
Minor Pediatric Burns
 F E A T U R E Minor Pediatric Burns BY Doug Baron Doug Baron, BScPT (IIWCC), is the burn clinic co-ordinator and team leader for the outpatient musculoskeletal physiotherapy services at the Alberta Children
F E A T U R E Minor Pediatric Burns BY Doug Baron Doug Baron, BScPT (IIWCC), is the burn clinic co-ordinator and team leader for the outpatient musculoskeletal physiotherapy services at the Alberta Children
Basic Dressing Categories
 Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
Category of Dressing Examples Advantages/Indications Disadvantages/Contraindications Hydrofiber Aquacel AG - ConvaTec Aquacel - Convatec Excellent for absorbing excess exudate These dressings form a gel
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Wound care has come a long
 Caring for chronic wounds: A knowledge update Wound care is a lot more sophisticated than it used to be. Here s what you should know about assessing and managing chronic wounds. By Patricia A. Slachta,
Caring for chronic wounds: A knowledge update Wound care is a lot more sophisticated than it used to be. Here s what you should know about assessing and managing chronic wounds. By Patricia A. Slachta,
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
DO NOT DUPLICATE. Negative pressure wound therapy (NPWT) has revolutionized the
 Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Wound Healing: General Principles. Mansour Dib MD
 Wound Healing: General Principles Mansour Dib MD Normal Wound Healing Chronic Wounds: Stuck Where does it get stuck? Mostly Proliferation Sometimes Remodeling Why? Systemic factors Local factors How do
Wound Healing: General Principles Mansour Dib MD Normal Wound Healing Chronic Wounds: Stuck Where does it get stuck? Mostly Proliferation Sometimes Remodeling Why? Systemic factors Local factors How do
Wound Management in the Elderly
 Wound Management in the Elderly Stephanie Yates, MSN, ANP, ANP-BC, CWOCN Nurse Practitioner/CNS Duke University Medical Center Durham, NC stephanie.yates@duke.edu Skin Condition Key quality indicator To
Wound Management in the Elderly Stephanie Yates, MSN, ANP, ANP-BC, CWOCN Nurse Practitioner/CNS Duke University Medical Center Durham, NC stephanie.yates@duke.edu Skin Condition Key quality indicator To
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers
 A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
Debridement: D.E.B.R.I.D.E. Clinician s Resource Guide. *smith&nephew
 *smith&nephew Debridement: Clinician s Resource Guide D.E.B.R.I.D.E. A guide to assist you in selecting or recommending a debridement method for your patient PDQWC mission PDQWC elevates the importance
*smith&nephew Debridement: Clinician s Resource Guide D.E.B.R.I.D.E. A guide to assist you in selecting or recommending a debridement method for your patient PDQWC mission PDQWC elevates the importance
Wound Care for Hospice Patients
 Wound Care for Hospice Patients Kristen Lyn Brodrick, RN, BSN, CHPN,CWCN No financial disclosures. Unique Population Patients needing hospice/palliative care are often at risk for developing multiple skin
Wound Care for Hospice Patients Kristen Lyn Brodrick, RN, BSN, CHPN,CWCN No financial disclosures. Unique Population Patients needing hospice/palliative care are often at risk for developing multiple skin
TIME CONCEPT AND LOCAL WOUND MANAGEMENT
 TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
Description. Section: Medicine Effective Date: April 15, 2015 Subsection: Medicine Original Policy Date: September 13, 2012 Subject:
 Last Review Status/Date: March 2015 Description Page: 1 of 6 Low-frequency ultrasound (US) in the kilohertz (KHz) range may improve wound healing. Several noncontact devices have received regulatory approval
Last Review Status/Date: March 2015 Description Page: 1 of 6 Low-frequency ultrasound (US) in the kilohertz (KHz) range may improve wound healing. Several noncontact devices have received regulatory approval
Teaming Together to Understand Pressure Injuries / (Ulcers): NPUAP Terminology and Staging Clarification
 Teaming Together to Understand Pressure Injuries / (Ulcers): NPUAP Terminology and Staging Clarification We encourage you to share this information with your staff and colleagues by facilitating clinician
Teaming Together to Understand Pressure Injuries / (Ulcers): NPUAP Terminology and Staging Clarification We encourage you to share this information with your staff and colleagues by facilitating clinician
TOO MANY DRESSING CHOICES!!!! WOUND CARE MANAGEMENT AND PRODUCTS. Should Your Practice Dispense Wound Care Supplies? Pros:
 WOUND CARE MANAGEMENT AND PRODUCTS Animesh Bhatia DPM, CWS, FAPWCA Board Certified Wound Specialist Diplomate, American Academy of Wound Management Fellow, American Professional Wound Care Association
WOUND CARE MANAGEMENT AND PRODUCTS Animesh Bhatia DPM, CWS, FAPWCA Board Certified Wound Specialist Diplomate, American Academy of Wound Management Fellow, American Professional Wound Care Association
This article is based on a symposium held
 Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
CONNECTIVE ISSUES 2014 Pressure Injury Case Study
 CONNECTIVE ISSUES 2014 Pressure Injury Case Study r1 Outline Medical History Social History Patient Assessment Lower Limb Assessment Factor affecting healing and goals setting Progress of the wound and
CONNECTIVE ISSUES 2014 Pressure Injury Case Study r1 Outline Medical History Social History Patient Assessment Lower Limb Assessment Factor affecting healing and goals setting Progress of the wound and
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
If both a standardized, validated screening tool and an evaluation of clinical factors are utilized, select Response 2.
 (M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
(M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
Hemostasis Inflammatory Phase Proliferative/rebuilding Phase Maturation Phase
 The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
Wound Management for Nurses/Technicians What do we need to know?
 Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
Pressure Ulcers. A global health concern 1,2,3,4
 Pressure Ulcers A global health concern 1,2,3,4 Among chronic wounds, pressure ulcers heal the slowest 1 and are most costly to treat. Prevention programs have resulted in a reduction in incidence as well
Pressure Ulcers A global health concern 1,2,3,4 Among chronic wounds, pressure ulcers heal the slowest 1 and are most costly to treat. Prevention programs have resulted in a reduction in incidence as well
