Key words: Chronic low back pain, caudal epidural injections, disc herniation, radiculitis, lower extremity pain, local anesthetic, steroids
|
|
|
- Brice Sparks
- 5 years ago
- Views:
Transcription
1 Pain Physician 2012; 15: ISSN Randomized Trial Effect of Fluoroscopically Guided Caudal Epidural Steroid or Local Anesthetic Injections in the Treatment of Lumbar Disc Herniation and Radiculitis: A Randomized, Controlled, Double Blind Trial with a Two-Year Follow-Up Laxmaiah Manchikanti, MD 1, Vijay Singh, MD 2, Kimberly A. Cash, RT 1, Vidyasagar Pampati, MSc 1, Kim S. Damron, RN 1, and Mark V. Boswell, MD, PhD 3 From: 1 Pain Management Center of Paducah, Paducah, KY; 2 University of Louisville, Louisville, KY; and 3 Spine Pain Diagnostics Associates, Niagara, WI. Dr. Manchikanti is Medical Director of the Pain Management Center of Paducah, Paducah, Kentucky and Clinical Professor, Anesthesiology and Perioperative Medicine, University of Louisville, Louisville, Kentucky. Dr. Singh is Medical Director, Spine Pain Diagnostics Associates, Niagara, WI. Kimberly A. Cash is a Research Coordinator at the Pain Management Center of Paducah, Paducah, KY. Vidyasagar Pampati is a Statistician at the Pain Management Center of Paducah, Paducah, KY. Kim S. Damron is a Nursing Administrator at the Pain Management Center of Paducah, Paducah, KY. Dr. Boswell is Chairman, Department of Anesthesiology and Perioperative Medicine, University of Louisville, Louisville, KY Address Correspondence: Laxmaiah Manchikanti, M.D Lone Oak Road Paducah, Kentucky drlm@thepainmd.com Disclaimer: There was no external funding in the preparation of this manuscript. Conflict of interest: None. Manuscript received: 05/24/2012 Accepted for publication: 06/07/2012 Free full manuscript: Background: Lumbar disc herniation and radiculitis are common elements of low back and lower extremity pain. Among minimally invasive treatments, epidural injections are one of the most commonly performed interventions. However, the literature is mixed about their effectiveness in managing low back and lower extremity pain. In general, individual studies and systematic reviews of epidural steroid injections have been hampered by their study design, baseline differences between treatment groups, inadequate sample sizes, highly controlled settings, lack of validated outcome measures, and the inability to confirm the injectate location because fluoroscopy was not used. Study Design: A randomized, controlled, double blind, active control trial. Setting: A private, interventional pain management practice, specialty referral center in the United States. Objectives: To assess the effectiveness of fluoroscopically directed caudal epidural injections with local anesthetic with or without steroids in managing chronic low back and lower extremity pain in patients with disc herniation and radiculitis. Methods: One hundred twenty patients were randomized to two groups: Group I received 10 ml caudal epidural injections of local anesthetic, lidocaine 0.5%; Group II patients received caudal epidural injections of 0.5% lidocaine, 9 ml, mixed with 1 ml of steroid. Outcome Assessment: Multiple outcome measures were utilized. The primary outcome measures were Numeric Rating Scale (NRS) and the Oswestry Disability Index 2.0 (ODI). Secondary outcome measures were employment status and opioid intake. Significant pain relief improvement was defined as 50% or more improvement in NRS and ODI scores. Results: In the successful category, 77% of Group I had significant pain relief of 50% and functional status improvement of 50% reduction in ODI scores; in Group II it was 76%, whereas overall it was 60% and 65% in Groups I and II. Over the two years, Group I had an average number of procedures of 5.5 ± 2.8; Group II was 5.3 ± 2.4. Even though there was no significant difference in overall relief between the two groups, the average relief for each procedure was superior for steroids. Limitations: Presumed limitations of this evaluation include lack of a placebo group. Conclusion: Caudal epidural injections of local anesthetic with or without steroids might be an effective therapy for patients with disc herniation or radiculitis. The present evidence illustrates the potential superiority of steroids compared with local anesthetic at two year follow up based on average relief per procedure. Key words: Chronic low back pain, caudal epidural injections, disc herniation, radiculitis, lower extremity pain, local anesthetic, steroids Trial Registration: NCT Pain Physician 2012; 15:
2 Pain Physician: July/August 2012; 15: Over the past 77 years, voluminous literature has been written describing the epidemiology, diagnosis, and numerous treatment modalities for herniated disc pain, following the description of disc herniation by Mixter and Barr in 1934 (1-26). The estimated prevalence of lumbar radiculopathy or sciatica has been described as 9.8 per 1,000 cases (4), 5.1% in men and 3.7% in women (3). However, lumbar radiculopathy secondary to disc herniation resolves spontaneously in 23% to 48% of patients, but up to 30% to 70% will still have pronounced symptoms after one year, with 5% to 15% of patients undergoing surgery resulting in high economic impact and strain on health services (6,7,16,24-26). Among minimally invasive treatments, epidural injections are one of the most commonly performed interventions (2,17-21,24-33). However, the literature is mixed about their effectiveness in managing low back and lower extremity pain (2,17,20,21,24-32). In general, individual studies and systematic reviews of epidural steroid injections have been hampered by their study design, baseline differences between treatment groups, inadequate sample sizes, highly controlled settings, lack of validated outcome measures, and the inability to confirm the injectate location because fluoroscopy was not used (2,17,20,21,25-38). Other problems include inappropriate methodology, improper study evaluation, and evidence synthesis for systematic reviews (2,17,21,25,26,31-33). Further, the three different approaches, caudal, interlaminar, and transforaminal, are used to treat multiple pathologies including disc herniation, axial or discogenic pain, spinal stenosis, and lumbar postsurgery syndrome along with other causes of low back pain. Thus, combining patients and/or results yielded significant confusion. Incorrect needle placement has been demonstrated in 20% to 38% of patients who have caudal epidural injections without fluoroscopy (34-38). Consequently, most systematic reviews (2,20,21,25,26,31-33) have included non-fluoroscopically guided studies; some recent studies also were published without fluoroscopy (27,29). Recently, Manchikanti et al (30) published the results of fluoroscopic caudal epidural injections in the treatment of lumbar disc herniation and radiculitis in a randomized, controlled, double blind trial and showed the proportion of patients with significant pain relief of 50% or greater and/or improvement in functional status with 50% or more reduction in ODI scores to be 70% and 67% in patients receiving local anesthetic only, and 77% and 75% in patients receiving steroids with average procedures per year of 3.8. In contrast, Iversen et al (27) in a recent multicenter, blinded, randomized control trial evaluating the effect of caudal epidural steroid or saline injection for chronic lumbar radiculopathy without fluoroscopy, at 52 weeks showed no significant difference among placebo injection of 2 ml of sodium chloride solution over the sacral hiatus, 40 ml injection of sodium chloride solution into the epidural space, or 40 mg of triamcinolone mixed with 40 ml of sodium chloride solution. The multiple differences between these studies can be attributed to Iversen et al (27) using ultrasound, a technique which has not been proven to identify the caudal epidural space accurately. On the other hand, Manchikanti et al (30) used fluoroscopy. There were also multiple flaws with the design, conduct, and interpretation of the results with probable inclusion of acute pain patients, inappropriate conservative management since a significant proportion of patients improved prior to their randomization or starting treatment, using large volumes that diluted the steroid, and the lack of use of local anesthetic (27,39,40). Further, approximately 40% of the patients were excluded with neurologic problems that did not fit the inclusion criteria, including a large proportion of patients with arachnoiditis, a rare condition (27). In contrast, Manchikanti et al (30) conducted the study in a truly chronic population who had disc herniation and radiculitis for at least six months and who had failed conservative management. In this study fluoroscopy was used and injections were performed based on the return of pain and deterioration in functional status. Thus, there continues to be conflicting evidence regarding the benefit of epidural steroid injections with or without local anesthetic. Thus far, only three randomized, controlled trials have been published evaluating mid term or long term outcomes with fluoroscopically guided caudal epidural injections (28,30,41). Ackerman and Ahmed (41) only reported outcomes at 24 weeks in 30 patients. Dashfield et al (28) utilized only one injection when comparing endoscopic delivery of steroids in 27 patients and only six months of follow up. Even so, they reported positive results. The results of Manchikanti et al (30) with one year followup were positive in a practical, clinical setting. This study was undertaken to evaluate the role of caudal epidural injections in patients with chronic low back and lower extremity pain secondary to disc herniation and radiculitis. This report is a continuation 274
3 Caudal Epidural Steroid Injectiions in the Treatment of Lumbar Disc Herniation and Radiculits of the results of a previous publication (30) reflecting the results of the comparative effectiveness of caudal epidural injections of local anesthetic with or without steroids. This report contains data from the long term followup of two years. Methods This randomized, double blind, controlled trial was conducted based on the Consolidated Standards of Reporting Trials (CONSORT) (42). The study was approved by the Institutional Review Board (IRB) and was registered with the U.S. Clinical Trial Registry. It was conducted in an interventional pain management practice in the United States. Patients were recruited from new patients presenting to a single pain management center. Interventions All patients were provided with the approved protocol and informed consent that described the study and withdrawal process. Patients were assigned into two groups. Group I patients received caudal epidural injections under fluoroscopy of local anesthetic (lidocaine 0.5%), while Group II patients received caudal epidural injections of lidocaine mixed with steroids. Pre-Enrollment Evaluation The preenrollment evaluation consisted of specific data and outcome parameters. Outcome parameters included numeric rating scale (NRS), Oswestry Disability Index 2.0 (ODI), work status, and opioid intake. Demographic data included medical and surgical history with coexisting disease(s), radiologic investigations, and physical examination findings. Inclusion Criteria For patients to be included in the study, essential requirements were demonstrated disc herniation with radiculitis; age over 18 years; function limiting low back and lower extremity pain of at least six months; and, finally, patients who were competent and willing to participate in the study protocol and who could provide voluntary, written informed consent. Exclusion criteria were: patients with a previous history of lumbar surgery; radiculitis secondary to either central or foraminal stenosis; no disc herniation; uncontrollable or unstable opioid use; uncontrollable psychiatric disorders; uncontrolled medical illness, either acute or chronic; pregnant or lactating women; a history or potential for adverse reactions from local anesthetic or steroid; and any conditions that could interfere with the interpretation of the outcome measurements. Description of Interventions All caudal epidural procedures were performed by one physician in an ambulatory surgery setting, in a sterile operating room, under fluoroscopy, with an #18 gauge Tuohy needle, with the patient in the prone position. Appropriate monitoring with intravenous access and sedation with midazolam and fentanyl were provided as needed. Access to the epidural space was confirmed by injection of non-ionic contrast medium, followed by injection of 10 ml of lidocaine hydrochloride 0.5% preservative free into 60 Group I patients, and in Group II 9 ml of lidocaine mixed with 6 mg of betamethasone (either brand name or non-particulate) or 40 mg of methylprednisolone was injected. Twenty patients in Group II each received one of the three steroids. Additional Interventions Additional or repeat caudal epidural injections were provided on the basis of the patient s response, either after unblinding or without unblinding. All unblinded patients were considered to be withdrawn from the study. Non-responsive patients who did not receive further interventions were followed without unblinding. Cointerventions There were no specific cointerventions or additional interventions. However, all patients continued previous exercise programs, drug therapy, and work. Objectives The design of the study was a randomized, double blind, active control to evaluate the effectiveness of caudal epidural injections with or without steroids in managing chronic low back and lower extremity pain secondary to disc herniation or radiculitis. Outcomes The primary outcomes were pain relief and functional status improvement based on NRS pain scales and ODI disability scale. The secondary outcomes were employment and opioid intake. The NRS pain scale (0-10), the ODI disability scale on a 0 to 50 scale, employment status, and opioid intake in terms of morphine equivalents were assessed at 3, 6, 12, 18, and 24 months posttreatment. The reliability of the NRS and ODI have been reported (43,44)
4 Pain Physician: July/August 2012; 15: Significant pain relief and functional improvement of 50% or more reduction in NRS or ODI from baseline have been deemed appropriate (45-50). The opioid intake was converted into morphine equivalents on the basis of the dosage frequency and schedule of the drug (51). Employment and work status were classified into multiple categories based on present employment, unemployment due to pain, housewife with no desire to work outside the home, retirement, or over the age of 65 years. Patients who were unemployed because of pain or employed but on sick leave or laid off were considered as employable. Patient response was considered successful if a patient obtained consistent relief lasting at least a total of three weeks with the first two procedures. Patients with less than three weeks of relief were considered as failures. Sample Size Sample size was calculated on the basis of significant pain relief and improvement in functional status. Considering a 0.05 two sided significance level, a power of 80%, and an allocation ratio of 1:1, 55 patients in each group were estimated (52). Allowing for a 10% attrition/non-compliance rate, 60 patients were required. A previous Cochrane systematic review of epidural injections (33), and multiple other studies (45-50) identified 50 to 60 patients as acceptable; others have identified even smaller samples (27,53). Randomization Sixty patients were randomly assigned into each group, for a total of 120 patients. Sequence Generation A computer generated random allocations sequence by simple randomization was used for randomization. Allocation Concealment Based on randomization, drugs were prepared by the operating room nurse assisting with the procedure. Implementation Patients meeting inclusion criteria were invited to enroll in the study. One of the three nurse coordinators of the study enrolled the participants and assigned participants to their Blinding (Masking) Participants, those administering the interventions, and all others involved in patient care were blinded to the group assignments. The blinding was also assured by mixing the patients with other patients receiving routine treatment and not informing the physician performing the procedure of the inclusion of the patients in the study or their group assignment. Statistical Methods Data analyses were carried out using the Statistical Package for Social Sciences version 9.01 (SPSS Inc, Chicago, IL). For categorical and continuous data comparison, Chi-square (Fisher test where necessary) and t test were used respectively. Because the outcome measures of the participants were measured at 4 points in time, repeated measures analysis of variance were performed with the post hoc analysis. A P value of less than 0.05 was considered significant. There were no significant differences noted among the three subgroups receiving steroids in any outcome parameters or the frequency of interventions. Thus, the three subgroups receiving steroids were considered as one group (group II). Intent-to-Treat Analysis An intent-to-treat analysis was performed. A sensitivity analysis with changes in the NRS was performed utilizing the last follow-up score, best case scenario, and worst case scenario if there were no significant differences; the intent-to-treat analysis with last follow-up visit was used. Results Patient Flow Figure 1 illustrates the participant flow. Recruitment The recruitment period started in January 2007 and ended in October Baseline Characteristics Table 1 illustrates the baseline demographic and clinical characteristics of each group. There were differences in the demographic characteristics with respect to age, weight, and mode of pain onset
5 Caudal Epidural Steroid Injectiions in the Treatment of Lumbar Disc Herniation and Radiculits Eligible Patients Assessed 178 Patients Excluded Patients Not Meeting Inclusion Criteria = 46 Patients Refusing to Participate = 12 Patients randomized 120 Patients included in this evaluation 120 Group I (60) Group II (60) Caudal epidural injections with local anesthetics Caudal epidural injections with local anesthetics and one of the steroids Patients included in analysis = 60 Patients included in analysis = 60 Patients withdrawn and unblinded = 1 Patients withdrawn and unblinded = 1 All participants received local anesthetic All patients received local anesthetic plus 20 patients each received one of the steroids brand name Betamethasone (6 mg) non-particulate betamethasone (6 mg), or depomethylprednisolone (40 mg) 12 months 80% (48) participants available for follow-up 100% (60) participants included in analysis 12 months 85% (51) participants available for follow-up 100% (60) participants included in analysis 24 months 80% (48) participants available for follow-up 100% (60) participants included in analysis 24 months 80% (48) participants available for follow-up 100% (60) participants included in analysis Fig. 1. Schematic presentation of patient flow at 2 year follow-up of 60 patients
6 Pain Physician: July/August 2012; 15: Table 1. Baseline demographic characteristics. Sex *Multiple patients presented with disc herniation at more than one level. Group 1 (60) Group II (60) Male 32% (19) 38% (23) Female 68% (41) 62% (37) P value Age Mean ± SD 48.7 ± ± Weight Mean ± SD ± ± Height Mean ± SD 66.2 ± ± Duration of Pain (Months) Mean ± SD 93.4 ± ± Onset of Pain Gradual 72% (43) 52% (31) Injury 28% (17) 48% (29) Numeric Rating Score Mean ± SD 8.1 ± ± Oswestry Disability Index Mean ± SD 29.2 ± ± Disc Herniation * (levels) L3/4 8% (5) 5% (3) L4/5 67% (40) 70% (42) L5/S1 58% (35) 50% (30) NS Analysis of Outcomes Pain Relief & Functional Assessment Table 2 presents the results of repeated measures analysis. There were significant differences in participants average pain scores within group by time (P < ), and no significant differences between two groups (P = 0.802). In the Oswestry Disability Index for functional status, there were significant differences in summary scores within group by time (P = 0.001) and no significant differences between two groups (P = 0.705). Paired samples t-test analysis indicates that mean differences baseline and the other five time points within the group were significant at the 0.05 level. Employment Characteristics Table 3 illustrates employment characteristics. Opioid Intake Table 4 illustrates opioid intake converted to morphine equivalents. Therapeutic Procedural Characteristics Therapeutic procedural characteristics and average pain relief data are illustrated in Table 5. The relief at- tained was significantly higher in Group II, the group that received steroids, compared with Group I for the first two procedures; the average relief per procedure over two years was also higher in Group II. When patients were separated into successful and failed groups, the total number of injections per year was 4.3 ± 1.0 and 6.5 ± 2.4 for two years in Group I and 3.8 ± 1.0 per year and 5.8 ± 2.2 for two years in Group II in the successful group. Total relief was 70.1 ± 30.8 weeks in Group I and 76.5 ± 27.7 weeks in Group II for two years in successful category. Figure 2 illustrates outcome data percentages of all participants, failed participants, and successful participants. Changes in Weight There were no differences in change (gain or loss) in body weight from baseline within the groups (Table 6). Adverse Events There were no major adverse events reported over a period of two years in all 120 patients
7 Caudal Epidural Steroid Injectiions in the Treatment of Lumbar Disc Herniation and Radiculits Table 2. Comparison of Numeric Rating Scale for pain and Oswestry Disability Index score summaries at 4 time points. Time Points Numeric Pain Rating scale Oswestry Disability Index Group I (60) Group II (60) Group I (60) Group II (60) Mean ± SD Mean ± SD Mean ± SD Mean ± SD Baseline 8.1 ± ± ± ± months 6 months 12 months 18 months 24 months 4.1* ± 1.8 (77%) 3.9* ± 1.8 (77%) 4.1* ± 1.8 (70%) 4.1* ± 1.8 (65%) 4.2* ± 1.8 (63%) 3.4* ± 1.7 (80%) 3.5* ± 1.7 (82%) 3.5* ± 1.9 (77%) 3.5* ± 1.8 (75%) 3.6* ± 1.8 (68%) 16.5* ± 7.2 (62%) 15.5* ± 7.3 (72%) 15.5* ± 7.74 (67%) 15.5* ± 7.4 (62%) 15.6* ± 7.3 (60%) Group Difference Time Difference Group by Time Interaction Lower the value indicates better condition * significant difference with baseline values within the group (P < 0.05) ( ) illustrates proportion with significant pain relief ( 50%) from baseline 13.6* ± 6.5 (73%) 13.7* ± 7.0 (73%) 13.1* ± 7.0 (75%) 13.2* ± 6.7 (77%) 13.5* ± 7.2 (70%) Table 3. Employment characteristics. Employment status Group I Group II Baseline 12 Months 24 Months Baseline 12 Months 24 Months Employed Part-time Employed Full-time Unemployed Total Employed Eligible for Employment Housewife Disabled Over 65 Years Old Total Number of Patients Discussion This randomized, active control trial of 120 patients with chronic persistent low back and lower extremity pain secondary to disc herniation and radiculitis, assessing caudal epidural injections with or without steroids, showed clinically meaningful and significant improvement in all parameters at the end of a two year period. The results of this study illustrate that in carefully selected patients, judged as successful participants who responded to the first two initial procedures, combined pain relief and improvement in functional status was observed in 77% in Group I and 76% in Group II at two year follow up. However, overall improvement was also significant with 60% of the patients showing improvement in Group I and 65% of the patients in Group II. Consequently, this study confirms the failure of the null hypothesis that treatment of chronic lumbar radiculopathy with caudal epidural injections of 279
8 Pain Physician: July/August 2012; 15: Table 4. Opioid intake (morphine equivalents in mg). Opioid Intake (Morphine Equivalents in mg) Group I (60) Group II (60) Mean ± SD Mean ± SD Baseline 51.8 ± ± Months 32.8* ± ± Months 32.9* ± ± Months 32.8* ± ± Months 32.8* ± ± Months 32.8* ± ± 37.5 Group Difference Time Difference Group by Time Interaction * significant difference with baseline values (P < 0.05) Table 5. Therapeutic procedural characteristics with procedural frequency, average relief per procedure, and average total relief in weeks over a period of one and two years. Successful Patients Failed Patients Overall Results Group I (47) Group II (50) Group I (13) Group II (10) Group I (60) Group II (60) Average Number of Procedures First Year 4.3# ± ± ± ± ± ± 1.1 Average Number of Procedures Over 2 Years 6.5 ± ± ± ± ± ± 2.4 Average Relief per Procedure for Initial 2 Procedures in Weeks (Maximum) Average Relief per Procedure After Initial 2 Procedures (Maximum) 6.6* ± 3.8 (17 weeks) 12.7* ± 3.5 (36 weeks) 11.3 ± 14.6 (100 weeks) 14.4 ± 9.2 (94 weeks) 1.4 ± 2.2 ( 8 weeks) 4.8 ± 5.4 (13 weeks) 1.3 ± 2.6 (11 weeks) 7.3 ± 9.4 (26 weeks) 5.6* ± 4.1 (17 weeks) 12.5* ± 3.7 (36 weeks) 9.7 ± 13.9 (100 weeks) 14.1 ± 9.2 (94 weeks) Average Relief per Procedure 10.8* ± ± ± ± * ± ± 11.4 Average Total Relief First Year (Weeks) 40.7 ± ± ± ± ± ± 17.2 Average Total Relief Over 2 Years (Weeks) 70.1 ± ± ± ± ± ± 36.5 * significant difference Group II (P < 0.05) Successful group - At least three weeks of relief with first 2 procedures Group I Group II 100% 80% 60% 72% 73% 67% 72% 60% 65% 87% 86% 85% 84% 77% 76% 40% 20% 0% 15% 10% 10% 10% 0% 0% 6 months 12 months 24 months 6 months 12 months 24 months 6 months 12 months 24 months All participants Failed participants Successful participants Fig. 2. Proportion of patients with significant reduction in Numeric Rating Score and Oswestry Disability Index ( 50% reduction from baseline)
9 Caudal Epidural Steroid Injectiions in the Treatment of Lumbar Disc Herniation and Radiculits Table 6. Characteristics of weight monitoring. Weight (lbs) Group I (60) Group II (60) Mean ± SD Mean ± SD P value Weight at Beginning ± ± Weight at One Year ± ± Change 5.3 ± ± Lost Weight 27% (16) 37% (22) No Change 18% (11) 15% (9) Gained Weight 55% (33) 48% (29) Weight at Two Years ± ± Change -5.9 ± ± Lost Weight 53% (32) 50% (30) No Change 22% (13) 8% (5) Gained Weight 25% (15) 42% (25) steroids or local anesthetic has no clinically important effect. Instead, it confirms that the treatment of lumbar disc herniation with radiculopathy with caudal epidural injection of steroids or local anesthetics has clinically important effects, irrespective of the steroid utilized, whether it is methylprednisolone, brand name betamethasone, or non-particulate betamethasone mixed with local anesthetic. While the average total relief over two years was not significantly different 70.1 ± 30.8 weeks in Group I and 76.5 ± 27.7 weeks in Group II in the successful group the average relief per procedure for the initial two procedures, as well as subsequent procedures and overall procedures over the period of two years, was significantly higher in Group II, not only in the successful patients, but also with reference to overall results. Thus, steroids indicate a potential superiority on a long term basis over a two year period, requiring approximately six procedures over two years, whereas it was slightly higher for Group I without steroids at 6.5 procedures for two years. We also observed a significant decrease in opioid intake from the baseline in Group I and an insignificant decrease in opioid intake in Group II along with an insignificant increase in employment in both groups at two years. At the end of two years, almost all of the patients eligible for employment in both groups were employed. We expected significant weight gains in the steroid group, however, there was no change noted in patients gaining weight at the end of one year. There was a significant proportion of patients gaining weight at the end of two years. This is significant since baseline weights were significantly higher in Group I, thus this finding may indicate that over a long-term period steroids may contribute to weight gain even though this change was absent at the end of one-year. The literature is replete with multiple studies and systematic reviews in favor of and against epidural injections in general (2,17,20,21,25-33). Multiple studies have been criticized, most importantly for their design and their inability to confirm the location of the injectate by not using fluoroscopy. Systematic reviews have been criticized for their methodology by evaluating the studies inappropriately; consequently their evidence synthesis has led to inaccurate conclusions. In a systematic review by Conn et al (17) of randomized trials of caudal epidural injections for managing chronic low back pain of various origins, including disc herniation, only two trials met the inclusion criteria of long term follow up of at least six months and the use of fluoroscopic visualization (28,54). They concluded that patients receiving caudal epidural injections with or without steroids had better results when the injections were performed under fluoroscopy. The authors did not include one study because of a 24 week follow up, which also showed positive results (41). Other systematic reviews (20,21,33) have combined multiple approaches into one category; the majority of them did not use fluoroscopy. Since the publication of these systematic reviews, new studies were published (27,29,30) confirming the effectiveness of epidural injections (29,30), even without fluoroscopy in one study (29), and showing nega
10 Pain Physician: July/August 2012; 15: tive results in one study (27). Iversen et al (27) published a placebo controlled study under ultrasound without fluoroscopy showing negative results, however the study has been criticized for multiple flaws with design, conduct, patient selection, lack of fluoroscopy, and interpretation of the results (39,40). Further, Cohen (55) in an editorial accompanying Iversen et al (27), commented that overall epidural steroid injections seem to be beneficial, but only provide modest improvement in carefully selected patients with predominantly radicular symptoms. Cohen believed that there was no definitive answer and postulated multiple reasons for the failure of epidural steroid injections in Iversen et al s study (27). Despite the negative findings, Cohen believed that Iversen et al s study should not be misinterpreted as suggesting that epidural steroid injections are of no use in neuropathic back pain. He also commented that if only a small proportion of people return to work or can avoid surgery, epidural steroid injections may be considered as an effective adjunct when used judiciously. Thus, in the era of comparative effective research (31,32,56-58), the evidence from comparative effectiveness or active controlled trials such as the present study are crucial in selecting a clinical intervention. In recent years, comparative effectiveness research has been considered pivotal to evidence based medicine (31,32,56-58). Even though the current study is limited to a single center, it is randomized, active controlled, and double blind, designed to determine whether fluoroscopically directed epidural injections with or without steroids with usual volumes injected in practice are helpful. Consequently, the results of this trial are applicable to interventional pain management in practical settings. Patient selection was not only practical but also was met with great sensitivity and included only patients with chronic persistent pain due to disc herniation and radiculitis. Consequently, this study meets the criteria for pragmatic or practical clinical trials with an active control group instead of a placebo group, and measures effectiveness, which is considered more appropriate than explanatory trials measuring efficacy (43,59-62). In addition, the current study was made as practical as possible by utilizing injection therapy with repeat caudal epidural injections based on the requirement that there be an increase in pain and deterioration in functional status prior to repeating the injection, rather than following a routine of a certain number of procedures, inappropriate assessment, and expecting one or two years of positive outcomes with one procedure. Further, as seen in contemporary specialized practices, this study demonstrated that the first or the initial two procedures do not provide long term relief, and if the initial relief does not last more than three weeks, the procedures may not provide relief in patients on a long term basis as was observed in failed patients, and that it may be futile to continue to repeat these procedures in these patients, unless there are compelling reasons. Further, this study may be criticized by not focusing on clinical aspects and as deficient because of the lack of a placebo group. However, most studies have utilized inappropriate methodology of placebo groups (27,63-68). The appropriate placebo design by Ghahreman et al (67) showed no significant effect with sodium chloride solution when injected into an inactive structure. Further, these concepts, including local anesthetic transformed into placebo, are not only methodologically and conceptually inaccurate, they also result in misleading conclusions since inactive substances injected into active structures have been shown to result in various types of effects (69-72) and local anesthetics have been shown to provide long term improvement in patients both in clinical as well as experimental settings (45-50,73-85). Further, an Institute of Medicine (IOM) report states that the effectiveness of pain treatments depends greatly on the strength of the clinician-patient relationship: Pain treatment is never about the clinician s intervention alone, but about the clinician and the patient (and family) working together (86). Finally, other weaknesses include differences in baseline demographic characteristics with respect to weight, age, and the pain s mode of onset. However, these differences may be considered minor and have not shown to have any effect on the final results. Even though the mechanism of action of steroids and local anesthetics continues to be debated and multiple hypothesis are emerging, the evidence shows that steroids as well as local anesthetics have significant effects on the modulation of noxious stimulation by various mechanisms (73-78,87-90) with no significant difference whether local anesthetics are injected alone or with steroids (45-50,79-85). Implications of this trial are enormous in an era of evidence based medicine, comparative effectiveness research, and exploding health care costs. Studies with proper methodology in practical settings are crucial. Proper application of the interventions will improve patient s pain function, reduce drug use, and may return them to the work force a great benefit for society
11 Caudal Epidural Steroid Injectiions in the Treatment of Lumbar Disc Herniation and Radiculits However, inappropriate provision of any type of intervention, specifically one which incurs substantial expenses, will not provide any benefit, harm the patient, and deplete resources, thus reducing access. Similarly, inappropriately performed evaluations that lead to inaccurate conclusions may reduce health care expenditures, but will also increase patient suffering, reduce function, increase drug use, and finally impede access to medical care. Conclusion This randomized double blind, active controlled trial of 120 patients treated with fluoroscopically guided caudal epidural injections of local anesthetic with or without steroids for chronic low back and lower extremity pain secondary to disc herniation and radiculitis, illustrated effectiveness in more than 75% of the patients with improvement in functional status, requiring an average of six procedures over two years and providing over 70 weeks of pain relief and function status improvement during the two year period in appropriately selected patients. Acknowledgments The authors wish to thank Sekar Edem for assistance in the search of the literature, Bert Fellows, MA, and Tom Prigge, MA, for manuscript review, and Tonie M. Hatton and Diane E. Neihoff, transcriptionists, for their assistance in preparation of this manuscript. We would like to thank the editorial board of Pain Physician for review and criticism in improving the manuscript. References 1. Mixter WJ, Barr JS. Rupture of the intervertebral disc with involvement of the spinal canal. N Eng J Med 1934; 211: Manchikanti L, Boswell MV, Singh V, Benyamin RM, Fellows B, Abdi S, Buenaventura RM, Conn A, Datta S, Derby R, Falco FJE, Erhart S, Diwan S, Hayek SM, Helm S, Parr AT, Schultz DM, Smith HS, Wolfer LR, Hirsch JA. Comprehensive evidence-based guidelines for interventional techniques in the management of chronic spinal pain. Pain Physician 2009; 12: Konstantinou K, Dunn KM. Sciatica: Review of epidemiological studies and prevalence estimates. Spine (Phila Pa 1976) 2008; 33: Savettieri G, Salemi G, Rocca WA, Meneghini F, D Arpa A, Morgante L, ci MA, Reggio A, Grigoletto F, Di Perri R. Prevalence of lumbosacral radiculopathy in two Sicilian municipalities. Sicilian Neuro-Epidemiologic Study (SNES) Group. Acta Neurol Scand 1996; 93: Martin BI, Turner JA, Mirza SK, Lee MJ, Comstock BA, Deyo RA. Trends in health care expenditures, utilization, and health status among US adults with spine problems, Spine (Phila Pa 1976) 2009; 34: Hoy D, Brooks P, Blyth F, Buchbinder R. The epidemiology of low back pain. Best Pract Res Clin Rheumatol 2010; 24: Tosteson AN, Tosteson TD, Lurie JD, Abdu W, Herkowitz H, Andersson G, Albert T, Bridwell K, Zhao W, Grove MR, Weinstein MC, Weinstein JN. Comparative effectiveness evidence from the spine patient outcomes research trial: Surgical versus nonoperative care for spinal stenosis, degenerative spondylolisthesis, and intervertebral disc herniation. Spine (Phila Pa 1976) 2011; 36: Ivanova JI, Birnbaum HG, Schiller M, Kantor E, Johnstone BM, Swindle RW. Real-world practice patterns, health-care utilization, and costs in patients with low back pain: The long road to guidelineconcordant care. Spine J 2011; 11: Freburger JK, Holmes GM, Agans RP, Jackman AM, Darter JD, Wallace AS, Castel LD, Kalsbeek WD, Carey TS. The rising prevalence of chronic low back pain. Arch Intern Med 2009; 169: Luo X, Pietrobon R, Sun SX, Liu GG, Hey L. Estimates and patterns of direct health care expenditures among individuals with back pain in the United States. Spine (Phila Pa 1976) 2004; 29: Rubinstein SM, van Middelkoop M, Assendelft WJ, de Boer MR, van Tulder MW. Spinal manipulative therapy for chronic low-back pain: An update of a Cochrane review. Spine (Phila Pa 1976) 2011; 36:E825 E Chou R, Qaseem A, Owens DK, Shekelle P; Clinical Guidelines Committee of the American College of Physicians. Diagnostic imaging for low back pain: Advice for high-value health care from the American College of Physicians. Ann Intern Med 2011; 154: Baras JD, Baker LC. Magnetic resonance imaging and low back pain care for Medicare patients. Health Aff (Millwood) 2009; 28:w1133 w Hahne AJ, Ford JJ, McMeeken JM. Conservative management of lumbar disc herniation with associated radiculopathy: A systematic review. Spine (Phila Pa 1976) 2010; 35:E488-E van Middelkoop M, Rubinstein SM, Kuijpers T, Verhagen AP, Ostelo R, Koes BW, van Tulder MW. A systematic review on the effectiveness of physical and rehabilitation interventions for chronic nonspecific low back pain. Eur Spine J 2011; 20: Jacobs WC, van Tulder M, Arts M, Rubinstein SM, van Middelkoop M, Ostelo R, Verhagen A, Koes B, Peul WC. Surgery versus conservative management of sciatica due to a lumbar herniated disc: A systematic review. Eur Spine J 2011;20: Conn A, Buenaventura R, Datta S, Abdi S, Diwan S. Systematic review of caudal epidural injections in the management of chronic low back pain. Pain Physician 2009; 12: Manchikanti L, Pampati V, Boswell MV, Smith HS, Hirsch JA. Analysis of the growth of epidural injections and costs 283
12 Pain Physician: July/August 2012; 15: in the Medicare population: A comparative evaluation of 1997, 2002, and 2006 data. Pain Physician 2010; 13: Abbott ZI, Nair KV, Allen RR, Akuthota VR. Utilization characteristics of spinal interventions. Spine J 2012; 1: Staal JB, de Bie RA, de Vet HC, Hildebrandt J, Nelemans P. Injection therapy for subacute and chronic low back pain: An updated Cochrane review. Spine (Phila Pa 1976) 2009; 34: Chou R, Huffman L. Guideline for the Evaluation and Management of Low Back Pain: Evidence Review. American Pain Society, Glenview, IL, Manchikanti L, Fellows B, Ailinani H, Pampati V. Therapeutic use, abuse, and nonmedical use of opioids: A ten-year perspective. Pain Physician 2010; 13: Manchikanti L, Ailinani H, Koyyalagunta D, Datta S, Singh V, Eriator I, Sehgal N, Shah R, Benyamin R, Vallejo R, Fellows B, Christo PJ. A systematic review of randomized trials of long-term opioid management for chronic non-cancer pain. Pain Physician 2011; 14: Deyo RA, Mirza SK, Turner JA, Martin BI. Overtreating chronic back pain: Time to back off? J Am Board Fam Med 2009; 22: Manchikanti L, Singh V, Boswell MV. Interventional pain management at crossroads: The perfect storm brewing for a new decade of challenges. Pain Physician 2010; 13:E111 E Benyamin RM, Datta S, Falco FJE. A perfect storm in interventional pain management: Regulated, but unbalanced. Pain Physician 2010;13: Iversen T, Solberg T, Romner B, Wilsgaard T, Twisk J, Anke A, Nygaard O, Hasvold T, Ingebrigtsen T. Effect of caudal epidural steroid or saline injection in chronic lumbar radiculopathy: Multicentre, blinded, randomised controlled trial. BMJ 2011; 343:d Dashfield AK, Taylor MB, Cleaver JS, Farrow D. Comparison of caudal steroid epidural with targeted steroid placement during spinal endoscopy for chronic sciatica: A prospective, randomized, double-blind trial. Br J Anaesth 2005; 94: Sayegh FE, Kenanidis EI, Papavasiliou KA, Potoupnis ME, Kirkos JM, Kapetanos GA. Efficacy of steroid and nonsteroid caudal epidural injections for low back pain and sciatica: A prospective, randomized, double-blind clinical trial. Spine (Phila Pa 1976) 2009; 34: Manchikanti L, Singh V, Cash K, Vidyasagar P, Damron K, Boswell M. A randomized, controlled, double-blind trial of fluoroscopic caudal epidural injections in the treatment of lumbar disc herniation and radiculitis. Spine (Phila Pa 1976) 2011; 36: Manchikanti L, Datta S, Gupta S, Munglani R, Bryce DA, Ward SP, Benyamin RM, Sharma ML, Helm S 2nd, Fellows B, Hirsch JA. A critical review of the American Pain Society clinical practice guidelines for interventional techniques: Part 2. Therapeutic interventions. Pain Physician 2010; 13:E215 E Manchikanti L, Falco FJE, Boswell MV, Hirsch JA. Facts, fallacies, and politics of comparative effectiveness research: Part 2. Implications for interventional pain management. Pain Physician 2010; 13:E55-E Koes BW, Scholten RJ, Mens JM, Bouter LM. Efficacy of epidural steroid injections for low-back pain and sciatica: A systematic review of randomized clinical trials. Pain 1995; 63: Manchikanti L, Cash KA, Pampati V, Mc- Manus CD, Damron KS. Evaluation of fluoroscopically guided caudal epidural injections. Pain Physician 2004; 7: Cleary M, Keating C, Poynton AR. The flow patterns of caudal epidural in upper lumbar spinal pathology. Eur Spine J 2011; 20: Stitz MY, Sommer HM. Accuracy of blind versus fluoroscopically guided caudal epidural injection. Spine (Phila Pa 1976) 1999; 24: White AH, Derby R, Wynne G. Epidural injections for the treatment of low back pain. Spine (Phila Pa 1976) 1980; 5: Manchikanti L, Bakhit CE, Pampati V. The role of epidurography in caudal neuroplasty. Pain Digest 1998; 8: Gupta S, Ward S, Munglani R, Sharma M. Letter to the Editor re: Iversen T, et al. Effect of caudal epidural steroid or saline injection in chronic lumbar radiculopathy: multicentre, blinded, randomised controlled trial. BMJ 2011; 343:d5278. Careful patient selection, fluoroscopy and contrast injection are needed for effective spinal injections. Published online 9/26/2011. Author s reply: Published online 9/29/ Norman. Letter to the Editor re: Iversen T, et al. Effect of caudal epidural steroid or saline injection in chronic lumbar radiculopathy: multicentre, blinded, randomised controlled trial. BMJ 2011; 343:d5278. The effect of caudal epidural in chronic lumbar radiculopathy remains unclear. Published online 9/23/2011. Author s reply: Published online 9/24/ Ackerman WE 3rd, Ahmad M. The efficacy of lumbar epidural steroid injections in patients with lumbar disc herniations. Anesth Analg 2007; 104: Altman DG, Schulz KF, Moher D, Egger M, Davidoff F, Elbourne D, et al; CON- SORT GROUP (Consolidated Standards of Reporting Trials). The revised CON- SORT statement for reporting randomized trials: Explanation and elaboration. Ann Intern Med 2001;134: Manchikanti L, Benyamin RM, Helm S, Hirsch JA. Evidence-based medicine, systematic reviews, and guidelines in interventional pain management: Part 3: Systematic reviews and meta-analyses of randomized trials. Pain Physician 2009; 12: Fairbank JC, Pynsent PB. The Oswestry Disability Index. Spine (Phila Pa 1976) 2000; 25: Manchikanti L, Cash KA, McManus CD, Pampati V, Smith HS. One year results of a randomized, double-blind, active controlled trial of fluoroscopic caudal epidural injections with or without steroids in managing chronic discogenic low back pain without disc herniation or radiculitis. Pain Physician 2011; 14: Manchikanti L, Singh V, Cash KA, Pampati V, Datta S. Management of pain of post lumbar surgery syndrome: Oneyear results of a randomized, double double-blind, active controlled trial of fluoroscopic caudal epidural injections. Pain Physician 2010; 13: Manchikanti L, Cash RA, McManus CD, Pampati V, Fellows B. Fluoroscopic caudal epidural injections with or without steroids in managing pain of lumbar spinal stenosis: One year results of randomized, double-blind, active-controlled trial. J Spinal Disord 2012; 25: Manchikanti L, Singh V, Falco FJE, Cash KA, Pampati V. Evaluation of lumbar facet joint nerve blocks in managing chronic low back pain: A randomized, doubleblind, controlled trial with a 2-year follow-up. Int J Med Sci 2010; 7:
13 Caudal Epidural Steroid Injectiions in the Treatment of Lumbar Disc Herniation and Radiculits 49. Manchikanti L, Singh V, Falco FJE, Cash KA, Fellows B. Comparative outcomes of a 2-year follow-up of cervical medial branch blocks in management of chronic neck pain: A randomized, double-blind controlled trial. Pain Physician 2010; 13: Manchikanti L, Singh V, Falco FJ, Cash KA, Pampati V, Fellows B. Comparative effectiveness of a one-year follow-up of thoracic medial branch blocks in management of chronic thoracic pain: A randomized, double-blind active controlled trial. Pain Physician 2010; 13: Pereira J, Lawlor P, Vigano A, Dorgan M, Bruera E. Equianalgesic dose ratios for opioids. A critical review and proposals for long-term dosing. J Pain Symptom Manage 2001; 22: Narcotic analgesic converter, GlobalRPh Inc. Accessed April 7, Browner WS, Newman TB, Cummings SR, Hulley SB. Estimating sample size and power. In Hulley SB, Cummings SR, Browner WS, et al (eds). Designing Clinical Research: An Epidemiologic Approach, 2nd ed. Philadelphia, PA: Lippincott, Williams & Wilkins, 2001, pp Gharibo C, Varlotta G, Rhame E, Liu ECJ, Bendo J, Perloff M. Interlaminar versus transforaminal epidural steroids for the treatment of sub-acute lumbar radicular pain: A randomized, blinded, prospective outcome study. Pain Physician 2011; 14: Manchikanti L, Singh V, Cash KA, Pampati V, Damron KS, Boswell MV. Preliminary results of randomized, equivalence trial of fluoroscopic caudal epidural injections in managing chronic low back pain: Part 2. Disc herniation and radiculitis. Pain Physician 2008; 11: Cohen SP. Epidural steroid injections for low back pain. BMJ 2011; 343:d Manchikanti L, Falco FJ, Benyamin RM, Helm S 2nd, Parr AT, Hirsch JA. The impact of comparative effectiveness research on interventional pain management: Evolution from Medicare Modernization Act to Patient Protection and Affordable Care Act and the Patient- Centered Outcomes Research Institute. Pain Physician 2011; 14:E249 E Manchikanti L, Falco FJE, Boswell MV, Hirsch JA. Facts, fallacies, and politics of comparative effectiveness research: Part I. Basic considerations. Pain Physician 2010; 13:E23 E Manchikanti L, Datta S, Derby R, Wolfer LR, Benyamin RM, Hirsch JA. A critical review of the American Pain Society clinical practice guidelines for interventional techniques: Part 1. Diagnostic interventions. Pain Physician 2010; 13:E141 E Hotopf M. The pragmatic randomized controlled trial. Adv Psychiatr Treat 2002; 8: Tunis SR, Stryer DB, Clancy CM. Practical clinical trials. Increasing the value of clinical research for decision making in clinical and health policy. JAMA 2003; 290: Roland M, Torgerson DJ. What are pragmatic trials? BMJ 1998; 316: International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for Human Use. ICH Harmonised Tripartite Guideline. Choice of Control Group and Related Issues in Clinical Trials E10. July 20, Carette S, Leclaire R, Marcoux S, Morin F, Blaise GA, St-Pierre A, Truchon R, Parent F, Levésque J, Bergeron V, Montminy P, Blanchette C. Epidural corticosteroid injections for sciatica due to herniated nucleus pulposus. N Engl J Med 1997; 336: Karppinen J, Malmivaara A, Kurunlahti M, Kyllönen E, Pienimäki T, Nieminen P, Ohinmaa A, Tervonen O, Vanharanta H. Periradicular infiltration for sciatica: A randomized controlled trial. Spine (Phila Pa 1976) 2001; 26: Manchikanti L, Giordano J, Fellows B, Hirsch JA. Placebo and nocebo in interventional pain management: A friend or a foe - or simply foes? Pain Physician 2011; 14:E157 E Smuck M, Levin JH. RE: Manchikanti L, Singh V, Falco FJE, Cash KA, Fellows B. Cervical medial branch blocks for chronic cervical facet joint pain: A randomized double-blind, controlled trial with one-year follow-up. Spine (Phila Pa 1976) 2008; 33: Spine (Phila Pa 1976) 2009; 34: Ghahreman A, Ferch R, Bogduk N. The efficacy of transforaminal injection of steroids for the treatment of lumbar radicular pain. Pain Med 2010; 11: Chou R, Atlas SJ, Loeser JD, Rosenquist RW, Stanos SP. Guideline warfare over interventional therapies for low back pain: Can we raise the level of discourse? J Pain 2011; 12: Indahl A, Kaigle AM, Reikeräs O, Holm SH. Interaction between the porcine lumbar intervertebral disc, zygapophysial joints, and paraspinal muscles. Spine (Phila Pa 1976) 1997; 22: Indahl A, Kaigle A, Reikeräs O, Holm S. Electromyographic response of the porcine multifidus musculature after nerve stimulation. Spine (Phila Pa 1976) 1995; 20: Pham Dang C, Lelong A, Guilley J, Nguyen JM, Volteau C, Venet G, Perrier C, Lejus C, Blanloeil Y. Effect on neurostimulation of injectates used for perineural space expansion before placement of a stimulating catheter: Normal saline versus dextrose 5% in water. Reg Anesth Pain Med 2009; 34: Tsui BC, Kropelin B, Ganapathy S, Finucane B. Dextrose 5% in water: Fluid medium maintaining electrical stimulation of peripheral nerve during stimulating catheter placement. Acta Anaesthesiol Scand 2005; 49: Pasqualucci A, Varrassi G, Braschi A, Peduto VA, Brunelli A, Marinangeli F, Gori F, Colò F, Paladini A, Mojoli F. Epidural local anesthetic plus corticosteroid for the treatment of cervical brachial radicular pain: Single injection verus continuous infusion. Clin J Pain 2007; 23: Mao J, Chen LL. Systemic lidocaine for neuropathic pain relief. Pain 2000; 87: Pasqualucci A. Experimental and clinical studies about the preemptive analgesia with local anesthetics. Possible reasons of the failure. Minerva Anestesiol 1998; 64: Arner S, Lindblom U, Meyerson BA, Molander C. Prolonged relief of neuralgia after regional anesthetic block. A call for further experimental and systematic clinical studies. Pain 1990; 43: Lavoie PA, Khazen T, Filion PR. Mechanisms of the inhibition of fast axonal transport by local anesthetics. Neuropharmacology 1989; 28: Bisby MA. Inhibition of axonal transport in nerves chronically treated with local anesthetics. Exp Neurol 1975; 47: Manchikanti L, Singh V, Falco FJE, Cash KA, Pampati V. Evaluation of the effectiveness of lumbar interlaminar epidural injections in managing chronic pain of lumbar disc herniation or radiculitis: A randomized, double-blind, controlled trial. Pain Physician 2010; 13:
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
 Comparison of the Efficacy of Caudal, Interlaminar, and Transforaminal Epidural Injections in Managing Lumbar Disc Herniation: Is One Method Superior to the Other? The Harvard community has made this article
Comparison of the Efficacy of Caudal, Interlaminar, and Transforaminal Epidural Injections in Managing Lumbar Disc Herniation: Is One Method Superior to the Other? The Harvard community has made this article
Randomized Trial. Pain Physician 2011; 14:25-36 ISSN
 Pain Physician 2011; 14:25-36 ISSN 1533-3159 Randomized Trial One-Year Results of a Randomized, Double-Blind, Active Controlled Trial of Fluoroscopic Caudal Epidural Injections With or Without Steroids
Pain Physician 2011; 14:25-36 ISSN 1533-3159 Randomized Trial One-Year Results of a Randomized, Double-Blind, Active Controlled Trial of Fluoroscopic Caudal Epidural Injections With or Without Steroids
Laxmaiah Manchikanti, MD, Kimberly A. Cash, RT, Vidyasagar Pampati, MSc, Bradley W. Wargo, DO, and Yogesh Malla, MD
 Pain Physician 2010; 13:223-236 ISSN 1533-3159 Randomized Trial The Effectiveness of Fluoroscopic Cervical Interlaminar Epidural Injections in Managing Chronic Cervical Disc Herniation and Radiculitis:
Pain Physician 2010; 13:223-236 ISSN 1533-3159 Randomized Trial The Effectiveness of Fluoroscopic Cervical Interlaminar Epidural Injections in Managing Chronic Cervical Disc Herniation and Radiculitis:
A Randomized, Double-Blind, Active-Control Trial of the Effectiveness of Lumbar Interlaminar Epidural Injections in Disc Herniation
 Pain Physician 2014; 17:E61-E74 ISSN 2150-1149 Randomized Trial A Randomized, Double-Blind, Active-Control Trial of the Effectiveness of Lumbar Interlaminar Epidural Injections in Disc Herniation Laxmaiah
Pain Physician 2014; 17:E61-E74 ISSN 2150-1149 Randomized Trial A Randomized, Double-Blind, Active-Control Trial of the Effectiveness of Lumbar Interlaminar Epidural Injections in Disc Herniation Laxmaiah
Laxmaiah Manchikanti, MD, Kimberly A. Cash, RT, Vidyasagar Pampati, MSc, Bradley W. Wargo, DO, and Yogesh Malla, MD
 Pain Physician 2010; 13:E265-E278 ISSN 2150-1149 Randomized Trial Cervical Epidural Injections in Chronic Discogenic Neck Pain Without Disc Herniation or Radiculitis: Preliminary Results of a Randomized,
Pain Physician 2010; 13:E265-E278 ISSN 2150-1149 Randomized Trial Cervical Epidural Injections in Chronic Discogenic Neck Pain Without Disc Herniation or Radiculitis: Preliminary Results of a Randomized,
Randomized Trial. Pain Physician 2010; 13: ISSN
 Pain Physician 2010; 13:437-450 ISSN 1533-3159 Randomized Trial Comparative Outcomes of a 2-Year Follow-Up of Cervical Medial Branch Blocks in Management of Chronic Neck Pain: A Randomized, Double-Blind
Pain Physician 2010; 13:437-450 ISSN 1533-3159 Randomized Trial Comparative Outcomes of a 2-Year Follow-Up of Cervical Medial Branch Blocks in Management of Chronic Neck Pain: A Randomized, Double-Blind
Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: Preliminary Results of a Randomized, Double-Blind, Active Control Trial
 Pain Physician 2012; 15:51-63 ISSN 1533-3159 Randomized Trial Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: Preliminary Results of a Randomized, Double-Blind, Active Control Trial
Pain Physician 2012; 15:51-63 ISSN 1533-3159 Randomized Trial Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: Preliminary Results of a Randomized, Double-Blind, Active Control Trial
Transforaminal Epidural Injections in Chronic Lumbar Disc Herniation: A Randomized, Double-Blind, Active-Control Trial
 Pain Physician 2014; 17:E489-E501 ISSN 2150-1149 Randomized Trial Transforaminal Epidural Injections in Chronic Lumbar Disc Herniation: A Randomized, Double-Blind, Active-Control Trial Laxmaiah Manchikanti,
Pain Physician 2014; 17:E489-E501 ISSN 2150-1149 Randomized Trial Transforaminal Epidural Injections in Chronic Lumbar Disc Herniation: A Randomized, Double-Blind, Active-Control Trial Laxmaiah Manchikanti,
Results of 2-Year Follow-Up of a Randomized, Double-Blind, Controlled Trial of Fluoroscopic Caudal Epidural Injections In Central Spinal Stenosis
 Pain Physician 2012; 15:371-384 ISSN 1533-3159 Randomized Controlled Trial Results of 2-Year Follow-Up of a Randomized, Double-Blind, Controlled Trial of Fluoroscopic Caudal Epidural Injections In Central
Pain Physician 2012; 15:371-384 ISSN 1533-3159 Randomized Controlled Trial Results of 2-Year Follow-Up of a Randomized, Double-Blind, Controlled Trial of Fluoroscopic Caudal Epidural Injections In Central
Setting: An interventional pain management practice, a specialty referral center, a private practice setting in the United States.
 Pain Physician 2010; 13:509-521 ISSN 1533-3159 Randomized Trial Management of Pain of Post Lumbar Surgery Syndrome: One-Year Results of a Randomized, Double-Blind, Active Controlled Trial of Fluoroscopic
Pain Physician 2010; 13:509-521 ISSN 1533-3159 Randomized Trial Management of Pain of Post Lumbar Surgery Syndrome: One-Year Results of a Randomized, Double-Blind, Active Controlled Trial of Fluoroscopic
Randomized Trial. Pain Physician 2012; 15:13-26 ISSN
 Pain Physician 2012; 15:13-26 ISSN 1533-3159 Randomized Trial Fluoroscopic Cervical Interlaminar Epidural Injections in Managing Chronic Pain of Cervical Postsurgery Syndrome: Preliminary Results of a
Pain Physician 2012; 15:13-26 ISSN 1533-3159 Randomized Trial Fluoroscopic Cervical Interlaminar Epidural Injections in Managing Chronic Pain of Cervical Postsurgery Syndrome: Preliminary Results of a
Follow this and additional works at: Part of the Musculoskeletal Diseases Commons
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Do Epidural Injections With Local Anesthetic
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Do Epidural Injections With Local Anesthetic
Comments on Washington State Health Care Authority, HTA Program Key Questions for Spinal Injections
 American Society of Interventional ain hysicians " The Voice of Interventional ain Management " 81 Lakeview Drive, aducah, KY 42001 Tel.: (270) 554-9412; Fax : (270) 554-8987 E-mail:asipp@asipp.org August
American Society of Interventional ain hysicians " The Voice of Interventional ain Management " 81 Lakeview Drive, aducah, KY 42001 Tel.: (270) 554-9412; Fax : (270) 554-8987 E-mail:asipp@asipp.org August
d EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Vijay Singh, M.D Roosevelt Rd., Niagara, WI 54151
 Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Is Dexamethasone Epidural Injection Effective in Relieving Radicular Pain in an Adult Population?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Dexamethasone Epidural Injection Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Dexamethasone Epidural Injection Effective
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 7/1/2018 Section: MED Policy No: 123 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 12/15 Medical Policy Committee Approved Date: 8/94; 7/96; 8/97; 4/98;
Effective Date: 7/1/2018 Section: MED Policy No: 123 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 12/15 Medical Policy Committee Approved Date: 8/94; 7/96; 8/97; 4/98;
Behnam Hosseini, Mohammad Hossein Ataei, Sirous Momenzadeh, Reza Jalili Khoshnood, Davood Ommi
 Original Article The comparison between steroid and hypertonic saline 10% with steroid in transforaminal epidural injection in patients with unilateral foraminal stenosis Behnam Hosseini, Mohammad Hossein
Original Article The comparison between steroid and hypertonic saline 10% with steroid in transforaminal epidural injection in patients with unilateral foraminal stenosis Behnam Hosseini, Mohammad Hossein
CLINICAL GUIDELINES. CMM-207: Epidural Adhesiolysis. Version Effective February 15, 2019
 CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14 SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
Fluoroscopic Epidural Injections in Cervical Spinal Stenosis: Preliminary Results of a Randomized, Double-Blind, Active Control Trial
 Pain Physician 2012; 15:E59-E70 ISSN 2150-1149 Randomized Trial Fluoroscopic Epidural Injections in Cervical Spinal Stenosis: Preliminary Results of a Randomized, Double-Blind, Active Control Trial Laxmaiah
Pain Physician 2012; 15:E59-E70 ISSN 2150-1149 Randomized Trial Fluoroscopic Epidural Injections in Cervical Spinal Stenosis: Preliminary Results of a Randomized, Double-Blind, Active Control Trial Laxmaiah
Randomized Trial. Pain Physician 2008; 11: ISSN
 Pain Physician 2008; 11:801-815 ISSN 1533-3159 Randomized Trial Preliminary Results of a Randomized, Equivalence Trial of Fluoroscopic Caudal Epidural Injections in Managing Chronic Low Back Pain: Part
Pain Physician 2008; 11:801-815 ISSN 1533-3159 Randomized Trial Preliminary Results of a Randomized, Equivalence Trial of Fluoroscopic Caudal Epidural Injections in Managing Chronic Low Back Pain: Part
Outcome Measures: Numeric Rating Scale (NRS) pain scale, the Oswestry Disability Index 2.0 (ODI), employment status, and opioid intake.
 Pain Physician 2007; 10:425-440 ISSN 1533-3159 Randomized Trial Evaluation of Lumbar Facet Joint Nerve Blocks in the Management of Chronic Low Back Pain: Preliminary Report of A Randomized, Double-Blind
Pain Physician 2007; 10:425-440 ISSN 1533-3159 Randomized Trial Evaluation of Lumbar Facet Joint Nerve Blocks in the Management of Chronic Low Back Pain: Preliminary Report of A Randomized, Double-Blind
Outcome of Caudal Epidural Steroid. Injection in Chronic Low Back Pain. {Original Article (Orthopedic) Gulzar Saeed Ahmed
 Outcome of Caudal Epidural Steroid Injection in Chronic Low Back Pain {Original Article (Orthopedic) Gulzar Saeed Ahmed Assoc. Prof. of Orthopedic Surgery and traumatology, Liaquat University of Medical
Outcome of Caudal Epidural Steroid Injection in Chronic Low Back Pain {Original Article (Orthopedic) Gulzar Saeed Ahmed Assoc. Prof. of Orthopedic Surgery and traumatology, Liaquat University of Medical
Clinical Policy: Caudal or Interlaminar Epidural Steroid Injections
 Clinical Policy: Reference Number: PA.CP.MP.164 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log Description Epidural steroid injections have been used for pain control in
Clinical Policy: Reference Number: PA.CP.MP.164 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log Description Epidural steroid injections have been used for pain control in
Variation In The Method Of Caudal Epidural Injection- A Regional Survey
 ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 2 Variation In The Method Of Caudal Epidural Injection- A Regional Survey S Haque., J Gaskin., A Uguwoke, S Karmani Citation S Haque., J
ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 2 Variation In The Method Of Caudal Epidural Injection- A Regional Survey S Haque., J Gaskin., A Uguwoke, S Karmani Citation S Haque., J
Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
 Pain Physician 2009; 12:855-866 ISSN 1533-3159 Original Contribution Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
Pain Physician 2009; 12:855-866 ISSN 1533-3159 Original Contribution Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: A 2-Year Follow-Up of 152 Patients Diagnosed with Controlled Diagnostic Blocks
DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL
 Subject: Percutaneous Epidural Adhesiolysis for Chronic Low Back Pain (RACZ Procedure) Original Effective Date: 10/12/15 Policy Number: MCP-257 Revision Date(s): Review Date: 12/16/15, 12/14/16, 6/22/17
Subject: Percutaneous Epidural Adhesiolysis for Chronic Low Back Pain (RACZ Procedure) Original Effective Date: 10/12/15 Policy Number: MCP-257 Revision Date(s): Review Date: 12/16/15, 12/14/16, 6/22/17
A Systematic Evaluation of Thoracic Interlaminar Epidural Injections
 Pain Physician 2012; 15:E497-E514 ISSN 2150-1149 Systematic Review A Systematic Evaluation of Thoracic Interlaminar Epidural Injections Ramsin M. Benyamin, MD 1, Victor Wang, MD, PhD 2, Ricardo Vallejo,
Pain Physician 2012; 15:E497-E514 ISSN 2150-1149 Systematic Review A Systematic Evaluation of Thoracic Interlaminar Epidural Injections Ramsin M. Benyamin, MD 1, Victor Wang, MD, PhD 2, Ricardo Vallejo,
Guideline Number: NIA_CG_301 Last Revised Date: March 2018 Responsible Department: Clinical Operations
 Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Lysis of Epidural Adhesions
 Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
Medical Policy Manual Surgery, Policy No. 94 Lysis of Epidural Adhesions Next Review: September 2019 Last Review: October 2018 Effective: November 1, 2018 IMPORTANT REMINDER Medical Policies are developed
Randomized Trial. Pain Physician 2008; 11: ISSN
 Pain Physician 2008; 11:491-504 ISSN 1533-3159 Randomized Trial Effectiveness of Thoracic Medial Branch Blocks in Managing Chronic Pain: A Preliminary Report of a Randomized, Double-Blind Controlled Trial;
Pain Physician 2008; 11:491-504 ISSN 1533-3159 Randomized Trial Effectiveness of Thoracic Medial Branch Blocks in Managing Chronic Pain: A Preliminary Report of a Randomized, Double-Blind Controlled Trial;
Laxmaiah Manchikanti, MD, Sneha Pampati, and Kimberly A. Cash, RT
 Pain Physician 2010; 13:133-143 ISSN 1533-3159 Diagnostic Accuracy Study Making Sense of the Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: An Assessment of the Implications of 50% Relief, 80%
Pain Physician 2010; 13:133-143 ISSN 1533-3159 Diagnostic Accuracy Study Making Sense of the Accuracy of Diagnostic Lumbar Facet Joint Nerve Blocks: An Assessment of the Implications of 50% Relief, 80%
Epidural Steroid Injections for Back Pain
 Epidural Steroid Injections for Back Pain Policy Number: 2.01.94 Last Review: 12/2018 Origination: 12/2014 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Epidural Steroid Injections for Back Pain Policy Number: 2.01.94 Last Review: 12/2018 Origination: 12/2014 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
An Update of Evaluation of Therapeutic Thoracic Facet Joint Interventions
 Pain Physician 2012; 15:E463-E481 ISSN 2150-1149 Systematic Review An Update of Evaluation of Therapeutic Thoracic Facet Joint Interventions Kavita N. Manchikanti, MD 1, Sairam Atluri, MD 2, Vijay Singh,
Pain Physician 2012; 15:E463-E481 ISSN 2150-1149 Systematic Review An Update of Evaluation of Therapeutic Thoracic Facet Joint Interventions Kavita N. Manchikanti, MD 1, Sairam Atluri, MD 2, Vijay Singh,
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14, 06/18/15, 05/25/16, 05/18/17
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product,
Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain Caused by Spinal Stenosis
 Journal of Basic & Clinical Medicine http://www.sspublications.org/index.php/jbcm/index Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain
Journal of Basic & Clinical Medicine http://www.sspublications.org/index.php/jbcm/index Comparing the Efficacy of Caudal Injection of Triamcinolone with Dexamethasone in Patients with Chronic Back Pain
MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/ /01/ /17/2017
 MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/2017 11/01/2018 12/17/2017 Policy Name Policy Number Policy Type MEDICAL Administrative Pharmacy Reimbursement
MEDICAL POLICY STATEMENT INDIANA MEDICAID Original Issue Date Next Annual Review Effective Date 11/01/2017 11/01/2018 12/17/2017 Policy Name Policy Number Policy Type MEDICAL Administrative Pharmacy Reimbursement
Medical Policy. MP Epidural Steroid Injections for Neck or Back Pain
 Medical Policy BCBSA Ref. Policy: 2.01.94 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 7.01.87 Artificial Intervertebral Disc: Lumbar Spine 7.01.108 Artificial
Medical Policy BCBSA Ref. Policy: 2.01.94 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 7.01.87 Artificial Intervertebral Disc: Lumbar Spine 7.01.108 Artificial
CLINICAL GUIDELINES. CMM-201 ~ Facet Joint Injections. Version 19.0 Effective August 11, 2017
 CLINICAL GUIDELINES CMM-201 ~ Facet Joint Injections Version 19.0 Effective August 11, 2017 evicore healthcare Clinical Decision Support Tool Diagnostic Strategies:This tool addresses common symptoms and
CLINICAL GUIDELINES CMM-201 ~ Facet Joint Injections Version 19.0 Effective August 11, 2017 evicore healthcare Clinical Decision Support Tool Diagnostic Strategies:This tool addresses common symptoms and
Contractor Information. LCD Information. FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836)
 FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836) Please note: Future Effective Date. Contractor Information Contractor Name Noridian Healthcare Solutions, LLC opens in new
FUTURE Local Coverage Determination (LCD): Lumbar Epidural Injections (L33836) Please note: Future Effective Date. Contractor Information Contractor Name Noridian Healthcare Solutions, LLC opens in new
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections
 Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
Clinical Policy: Selective Nerve Root Blocks and Transforaminal Epidural Steroid Injections Reference Number: PA.CP.MP.165 Effective Date: 09/18 Last Review Date: 09/18 Coding Implications Revision Log
What is the Role of Epidural Injections in the Treatment of Lumbar Discogenic Pain: A Systematic Review of Comparative Analysis with Fusion
 Review Article Korean J Pain 2015 April; Vol. 28, No. 2: 75-87 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2015.28.2.75 What is the Role of Epidural Injections in the Treatment of Lumbar
Review Article Korean J Pain 2015 April; Vol. 28, No. 2: 75-87 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2015.28.2.75 What is the Role of Epidural Injections in the Treatment of Lumbar
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lysis of Epidural Adhesions Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Lysis of Epidural Adhesions Professional Institutional Original Effective
Lysis of Epidural Adhesions Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Lysis of Epidural Adhesions Professional Institutional Original Effective
Efficacy of Epidural Injections in Managing Chronic Spinal Pain: A Best Evidence Synthesis
 Pain Physician 2015; 18:E939-E1004 ISSN 2150-1149 Systematic Review Efficacy of Epidural Injections in Managing Chronic Spinal Pain: A Best Evidence Synthesis Alan D. Kaye, MD, PhD 1, Laxmaiah Manchikanti,
Pain Physician 2015; 18:E939-E1004 ISSN 2150-1149 Systematic Review Efficacy of Epidural Injections in Managing Chronic Spinal Pain: A Best Evidence Synthesis Alan D. Kaye, MD, PhD 1, Laxmaiah Manchikanti,
FACET JOINT INJECTIONS Version 18.0; Effective
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
Effect of Spinal Exercises and Epidural Injections in Chronic Low Back Pain
 Effect of Spinal Exercises and Epidural Injections in Chronic Low Back Pain Sargun Singh Walia, Jaswinder Pal Singh, Harshita Yadav and Anuradha Lehri Abstract Aim: Effect of Spinal Exercises and Epidural
Effect of Spinal Exercises and Epidural Injections in Chronic Low Back Pain Sargun Singh Walia, Jaswinder Pal Singh, Harshita Yadav and Anuradha Lehri Abstract Aim: Effect of Spinal Exercises and Epidural
A Randomized, Double-Blind Controlled Trial of Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: 2-Year Follow-Up
 Pain Physician 2015; 18:79-92 ISSN 1533-3159 Randomized Trial A Randomized, Double-Blind Controlled Trial of Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: 2-Year Follow-Up Laxmaiah
Pain Physician 2015; 18:79-92 ISSN 1533-3159 Randomized Trial A Randomized, Double-Blind Controlled Trial of Lumbar Interlaminar Epidural Injections in Central Spinal Stenosis: 2-Year Follow-Up Laxmaiah
Comparison of effectiveness for fluoroscopic cervical interlaminar epidural injections with or without steroid in cervical post-surgery syndrome
 Original Article Korean J Pain 2018 October; Vol. 31, No. 4: 277-288 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2018.31.4.277 Comparison of effectiveness for fluoroscopic cervical interlaminar
Original Article Korean J Pain 2018 October; Vol. 31, No. 4: 277-288 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2018.31.4.277 Comparison of effectiveness for fluoroscopic cervical interlaminar
Medical Policy. MP Lysis of Epidural Adhesions
 Medical Policy MP 8.01.18 BCBSA Ref. Policy: 8.01.18 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Radiology Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our
Medical Policy MP 8.01.18 BCBSA Ref. Policy: 8.01.18 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Radiology Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our
Lysis of Epidural Adhesions
 Lysis of Epidural Adhesions Policy Number: 8.01.18 Last Review: 6/2018 Origination: 8/2007 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for lysis
Lysis of Epidural Adhesions Policy Number: 8.01.18 Last Review: 6/2018 Origination: 8/2007 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for lysis
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA Mailstop: CA
 To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
Cervical Medial Branch Blocks for Chronic Cervical Facet Joint Pain
 Cervical Medial Branch Blocks for Chronic Cervical Facet Joint Pain A Randomized, Double-Blind, Controlled Trial With One-Year Follow-up Laxmaiah Manchikanti, MD,* Vijay Singh, MD, Frank J. E. Falco, MD,
Cervical Medial Branch Blocks for Chronic Cervical Facet Joint Pain A Randomized, Double-Blind, Controlled Trial With One-Year Follow-up Laxmaiah Manchikanti, MD,* Vijay Singh, MD, Frank J. E. Falco, MD,
Concordant Provocation as a Prognostic Indicator During Interlaminar Lumbosacral Epidural Steroid Injections
 Pain Physician 2014; 17:247-253 ISSN 1533-3159 Randomized Trial Concordant Provocation as a Prognostic Indicator During Interlaminar Lumbosacral Epidural Steroid Injections Alexander H. Sinofsky, MD 1,
Pain Physician 2014; 17:247-253 ISSN 1533-3159 Randomized Trial Concordant Provocation as a Prognostic Indicator During Interlaminar Lumbosacral Epidural Steroid Injections Alexander H. Sinofsky, MD 1,
Randomized Trial. Pain Physician 2013; 16: ISSN
 Pain Physician 2013; 16:465-478 ISSN 1533-3159 Randomized Trial A Randomized, Double-Blind, Active Control Trial of Fluoroscopic Cervical Interlaminar Epidural Injections in Chronic Pain of Cervical Disc
Pain Physician 2013; 16:465-478 ISSN 1533-3159 Randomized Trial A Randomized, Double-Blind, Active Control Trial of Fluoroscopic Cervical Interlaminar Epidural Injections in Chronic Pain of Cervical Disc
Limitations: A single center study, lack of documentation of adjuvant therapies like individual analgesic medication, and lack of placebo group.
 Pain Physician 2015; 18:237-248 ISSN 1533-3159 Randomized Trial Effectiveness of Parasagittal Interlaminar Epidural Local Anesthetic with or without Steroid in Chronic Lumbosacral Pain: A Randomized, Double-Blind
Pain Physician 2015; 18:237-248 ISSN 1533-3159 Randomized Trial Effectiveness of Parasagittal Interlaminar Epidural Local Anesthetic with or without Steroid in Chronic Lumbosacral Pain: A Randomized, Double-Blind
Efficacy of Epidural Injections in the Treatment of Lumbar Central Spinal Stenosis: A Systematic Review
 Efficacy of Epidural Injections in the Treatment of Lumbar Central Spinal Stenosis: A Systematic Review The Harvard community has made this article openly available. Please share how this access benefits
Efficacy of Epidural Injections in the Treatment of Lumbar Central Spinal Stenosis: A Systematic Review The Harvard community has made this article openly available. Please share how this access benefits
Effect of Addition of Epidural Ketamine to Steroid in Lumbar Radiculitis: One-Year Follow-Up
 Pain Physician 2011; 14:475-481 ISSN 1533-3159 Randomized Trial Effect of Addition of Epidural Ketamine to Steroid in Lumbar Radiculitis: One-Year Follow-Up Yasser Mohamed Amr, MD From: Tanta University
Pain Physician 2011; 14:475-481 ISSN 1533-3159 Randomized Trial Effect of Addition of Epidural Ketamine to Steroid in Lumbar Radiculitis: One-Year Follow-Up Yasser Mohamed Amr, MD From: Tanta University
A Medical-Legal Review Regarding the Standard of Care for Epidural Injections, with Particular Reference to a Closed Case
 Pain Physician 2010; 13:145-150 ISSN 1533-3159 Medical-Legal Review A Medical-Legal Review Regarding the Standard of Care for Epidural Injections, with Particular Reference to a Closed Case Standiford
Pain Physician 2010; 13:145-150 ISSN 1533-3159 Medical-Legal Review A Medical-Legal Review Regarding the Standard of Care for Epidural Injections, with Particular Reference to a Closed Case Standiford
DRAFT as posted for public comment 11/8/2016 to 8 a.m. 12/9/2016. HERC Coverage Guidance
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of Follow-up
 Pain Physician 2014; 17:E599-E608 ISSN 2150-1149 Retrospective Analysis The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of
Pain Physician 2014; 17:E599-E608 ISSN 2150-1149 Retrospective Analysis The Catheter Tip Position and Effects of Percutaneous Epidural Neuroplasty in Patients with Lumbar Disc Disease During 6-Months of
Management of lumbar zygapophysial (facet) joint pain
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i5.315 World J Orthop 2016 May 18; 7(5): 315-337 ISSN 2218-5836 (online) 2016 Baishideng
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5312/wjo.v7.i5.315 World J Orthop 2016 May 18; 7(5): 315-337 ISSN 2218-5836 (online) 2016 Baishideng
Effect of Cervical Interlaminar Epidural Steroid Injection: Analysis According to the Neck Pain Patterns and MRI Findings
 Original Article Korean J Pain 2016 April; Vol. 29, No. 2: 96-102 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.2.96 Effect of Cervical Interlaminar Epidural Steroid Injection:
Original Article Korean J Pain 2016 April; Vol. 29, No. 2: 96-102 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.2.96 Effect of Cervical Interlaminar Epidural Steroid Injection:
A Randomized, Prospective, Double-Blind, Placebo-Controlled Evaluation of the Effect of Sedation on Diagnostic Validity of Cervical Facet Joint Pain
 Manchikanti et al Effect of Sedation on Diagnostic Validity of Cervical Facet Joint Pain 301 Pain Physician. 2004;7:301-309, ISSN 1533-3159 A Randomized Evaluation A Randomized, Prospective, Double-Blind,
Manchikanti et al Effect of Sedation on Diagnostic Validity of Cervical Facet Joint Pain 301 Pain Physician. 2004;7:301-309, ISSN 1533-3159 A Randomized Evaluation A Randomized, Prospective, Double-Blind,
A Best-Evidence Systematic Appraisal of the Diagnostic Accuracy and Utility of Facet (Zygapophysial) Joint Injections in Chronic Spinal Pain
 Pain Physician 2015; 18:E497-E533 ISSN 2150-1149 Systematic Review From: 1 Department of Anesthesiology and Perioperative Medicine, University of Louisville, Louisville, KY; 2 Pain Management Center of
Pain Physician 2015; 18:E497-E533 ISSN 2150-1149 Systematic Review From: 1 Department of Anesthesiology and Perioperative Medicine, University of Louisville, Louisville, KY; 2 Pain Management Center of
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
UnitedHealthcare Commercial Medical Policy EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAI001 Effective Date: May 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
SPINE SECTION. Design. Prospective clinical study.
 bs_bs_banner Pain Medicine 2014; 15: 379 385 Wiley Periodicals, Inc. SPINE SECTION Original Research Article Caudal vs Transforaminal Epidural Steroid Injections as Short-Term (6 Months) Pain Relief in
bs_bs_banner Pain Medicine 2014; 15: 379 385 Wiley Periodicals, Inc. SPINE SECTION Original Research Article Caudal vs Transforaminal Epidural Steroid Injections as Short-Term (6 Months) Pain Relief in
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product
Assessment of the Growth of Epidural Injections in the Medicare Population from 2000 to 2011
 Pain Physician 2013; 16:E349-E364 ISSN 2150-1149 Health Policy Review Assessment of the Growth of Epidural Injections in the Medicare Population from 2000 to 2011 Laxmaiah Manchikanti, MD 1,2, Vidyasagar
Pain Physician 2013; 16:E349-E364 ISSN 2150-1149 Health Policy Review Assessment of the Growth of Epidural Injections in the Medicare Population from 2000 to 2011 Laxmaiah Manchikanti, MD 1,2, Vidyasagar
Effectiveness of Cervical Epidural Injections in the Management of Chronic Neck and Upper Extremity Pain
 Pain Physician 2012; 15:E405-E434 ISSN 2150-1149 Systematic Review Effectiveness of Cervical Epidural Injections in the Management of Chronic Neck and Upper Extremity Pain Sudhir A. Diwan, MD 1, Laxmaiah
Pain Physician 2012; 15:E405-E434 ISSN 2150-1149 Systematic Review Effectiveness of Cervical Epidural Injections in the Management of Chronic Neck and Upper Extremity Pain Sudhir A. Diwan, MD 1, Laxmaiah
In Response: From Manchikanti et al
 Letters to the Editor In Response: From Manchikanti et al We appreciate the lengthy letter by Chou entitled Critiquing the Critiques. At the outset, the letter reminded us of an exchange between Bogduk
Letters to the Editor In Response: From Manchikanti et al We appreciate the lengthy letter by Chou entitled Critiquing the Critiques. At the outset, the letter reminded us of an exchange between Bogduk
Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up
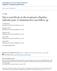 Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Retrospective cohort study of usage patterns of epidural injections for spinal pain in the US fee-for-service Medicare population from 2000 to 2014
 Retrospective cohort study of usage patterns of epidural injections for spinal pain in the US fee-for-service Medicare population from 2000 to 2014 The Harvard community has made this article openly available.
Retrospective cohort study of usage patterns of epidural injections for spinal pain in the US fee-for-service Medicare population from 2000 to 2014 The Harvard community has made this article openly available.
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Medical Affairs Policy
 Medical Affairs Policy Service: Back and Nerve Pain Procedures - Radiofrequency Ablation, Facet and Other Injections PUM 250-0035-1706 Cryoablation Medial Branch Neuroablation Radiofrequency Neuroablation
Medical Affairs Policy Service: Back and Nerve Pain Procedures - Radiofrequency Ablation, Facet and Other Injections PUM 250-0035-1706 Cryoablation Medial Branch Neuroablation Radiofrequency Neuroablation
CLINICAL GUIDELINES. CMM-201: Facet Joint Injections/Medial Branch Blocks. Version Effective October 22, 2018
 CLINICAL GUIDELINES CMM-201: Facet Joint Injections/Medial Branch Blocks Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-201:
CLINICAL GUIDELINES CMM-201: Facet Joint Injections/Medial Branch Blocks Version 20.0.2018 Effective October 22, 2018 Clinical guidelines for medical necessity review of speech therapy services. CMM-201:
Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Thoracic Facet Joint Interventions
 Pain Physician 2008; 11:611-629 ISSN 1533-3159 Systematic Review Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Thoracic Facet Joint Interventions Sairam Atluri, MD 1, Sukdeb
Pain Physician 2008; 11:611-629 ISSN 1533-3159 Systematic Review Systematic Review of Diagnostic Utility and Therapeutic Effectiveness of Thoracic Facet Joint Interventions Sairam Atluri, MD 1, Sukdeb
Clinical Policy: Lysis of Epidural Lesions Reference Number: CP.MP.116
 Clinical Policy: Reference Number: CP.MP.116 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.116 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Systematic Review of Effectiveness and Complications of Adhesiolysis in the Management of Chronic Spinal Pain: An Update
 Pain Physician 2007; 10:129-146 ISSN 1533-3159 Review Systematic Review of Effectiveness and Complications of Adhesiolysis in the Management of Chronic Spinal Pain: An Update Andrea M. Trescot, MD 1, Pradeep
Pain Physician 2007; 10:129-146 ISSN 1533-3159 Review Systematic Review of Effectiveness and Complications of Adhesiolysis in the Management of Chronic Spinal Pain: An Update Andrea M. Trescot, MD 1, Pradeep
Lysis of Epidural Adhesions
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Clinical Policy: Caudal or Interlaminar Epidural Steroid Injections
 Clinical Policy: Reference Number: CP.MP.164 Last Review Date: 04/18 See Important Reminder at the end of this policy for important regulatory and legal information. Coding Implications Revision Log Description
Clinical Policy: Reference Number: CP.MP.164 Last Review Date: 04/18 See Important Reminder at the end of this policy for important regulatory and legal information. Coding Implications Revision Log Description
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
5/31/2013. Disclosures. Lumbar Facet Joint Pain: Evidence. I have nothing to disclose
 Disclosures : Evidence I have nothing to disclose David J. Lee, MD Professor Pain Management Center Department of Anesthesia Facet Joint Pain Prevalence Spinal pain 54-80% lifetime 80-90% resolve in 6
Disclosures : Evidence I have nothing to disclose David J. Lee, MD Professor Pain Management Center Department of Anesthesia Facet Joint Pain Prevalence Spinal pain 54-80% lifetime 80-90% resolve in 6
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 6.01.23 Diagnosis and Treatment of Sacroiliac Joint Pain 7.01.120 Facet Arthroplasty Facet Joint Denervation Description Percutaneous
FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 6.01.23 Diagnosis and Treatment of Sacroiliac Joint Pain 7.01.120 Facet Arthroplasty Facet Joint Denervation Description Percutaneous
Evidence based Practice Changes Spinal Injections
 Evidence based Practice Changes Spinal Injections Kathryn Mueller, MD, MPH, FACOEM Professor, School of Public Health & Department of Physiatry - University of Colorado President - American College of
Evidence based Practice Changes Spinal Injections Kathryn Mueller, MD, MPH, FACOEM Professor, School of Public Health & Department of Physiatry - University of Colorado President - American College of
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Assessment of Efficacy of Fluoroscopy Guided Steroid Injection By Transforaminal Approach in Patients with Chronic Lumbosacral Radiculopathy.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. X (July. 2017), PP 95-99 www.iosrjournals.org Assessment of Efficacy of Fluoroscopy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. X (July. 2017), PP 95-99 www.iosrjournals.org Assessment of Efficacy of Fluoroscopy
Percutaneous Adhesiolysis Procedures in the Medicare Population: Analysis of Utilization and Growth Patterns from 2000 to 2011
 Pain Physician 2014; 17:E129-E139 ISSN 2150-1149 Health Policy Review Percutaneous Adhesiolysis Procedures in the Medicare Population: Analysis of Utilization and Growth Patterns from 2000 to 2011 Laxmaiah
Pain Physician 2014; 17:E129-E139 ISSN 2150-1149 Health Policy Review Percutaneous Adhesiolysis Procedures in the Medicare Population: Analysis of Utilization and Growth Patterns from 2000 to 2011 Laxmaiah
Facet Joint Injections and Facet Joint Nerve Blocks Effective Date December 15, 2014 Original Policy Date March 16, 1988
 BSC6.03 Section 7.0 Surgery Subsection 7.01 Surgery Facet Joint Injections and Facet Joint Nerve Blocks Effective Date December 15, 2014 Original Policy Date March 16, 1988 Next Review Date December 2015
BSC6.03 Section 7.0 Surgery Subsection 7.01 Surgery Facet Joint Injections and Facet Joint Nerve Blocks Effective Date December 15, 2014 Original Policy Date March 16, 1988 Next Review Date December 2015
MEDICAL POLICY SUBJECT: RADIOFREQUENCY FACET DENERVATION
 MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Cigna Medical Coverage Policies Musculoskeletal Facet Joint Injections/Medial Branch Blocks
 Cigna Medical Coverage Policies Musculoskeletal January 15, 2018 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
Cigna Medical Coverage Policies Musculoskeletal January 15, 2018 Instructions for use The following coverage policy applies to health benefit plans administered by Cigna. Coverage policies are intended
Original Policy Date
 MP 7.01.96 Facet Joint Denervation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 7.01.96 Facet Joint Denervation Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
Facet Joint Denervation. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Facet Joint Denervation Page: 1 of 16 Last Review Status/Date: March 2014 Facet Joint Denervation Description Facet joint denervation is performed
Section: Surgery Effective Date: April 15, 2014 Subject: Facet Joint Denervation Page: 1 of 16 Last Review Status/Date: March 2014 Facet Joint Denervation Description Facet joint denervation is performed
Facet Joint Denervation. Description
 Section: Surgery Effective Date: April 15, 2015 Subject: Facet Joint Denervation Page: 1 of 14 Last Review Status/Date: March 2015 Facet Joint Denervation Description Facet joint denervation is performed
Section: Surgery Effective Date: April 15, 2015 Subject: Facet Joint Denervation Page: 1 of 14 Last Review Status/Date: March 2015 Facet Joint Denervation Description Facet joint denervation is performed
Comparison of Epidural Methylprednisolone, Bupivacaine and Normal Saline Injection in Chronic Low Back Pain Due to Discal Hernia
 http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 5, No., January 8, 57 6 eissn 48-9696 Comparison of Epidural Methylprednisolone, Bupivacaine and
http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 5, No., January 8, 57 6 eissn 48-9696 Comparison of Epidural Methylprednisolone, Bupivacaine and
Randomized Trial. Pain Physician 2014; 17: ISSN
 Pain Physician 2014; 17:277-290 ISSN 1533-3159 Randomized Trial Transforaminal Versus Parasagittal Interlaminar Epidural Steroid Injection in Low Back Pain with Radicular Pain: A Randomized, Double-Blind,
Pain Physician 2014; 17:277-290 ISSN 1533-3159 Randomized Trial Transforaminal Versus Parasagittal Interlaminar Epidural Steroid Injection in Low Back Pain with Radicular Pain: A Randomized, Double-Blind,
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18
 Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Survey of European Pain Medicine Practice
 Pain Physician 2012; 15:E983-E994 ISSN 2150-1149 Survey Survey of European Pain Medicine Practice Sanjeeva Gupta, MD, FRCA, FFPMRCA 1, Manish Gupta, FRCA 2, Sherdil Nath, MD, FRCA 3, and G. Michael Hess,
Pain Physician 2012; 15:E983-E994 ISSN 2150-1149 Survey Survey of European Pain Medicine Practice Sanjeeva Gupta, MD, FRCA, FFPMRCA 1, Manish Gupta, FRCA 2, Sherdil Nath, MD, FRCA 3, and G. Michael Hess,
A Novel Application of an Adjustable Catheter in Acute Radicular Pain Management
 https://doi.org/10.1007/s40122-018-0110-0 BRIEF REPORT A Novel Application of an Adjustable Catheter in Acute Radicular Pain Management Maria Clemente. Carla Roero. Veronica Perlo. Elena Peila. Anna De
https://doi.org/10.1007/s40122-018-0110-0 BRIEF REPORT A Novel Application of an Adjustable Catheter in Acute Radicular Pain Management Maria Clemente. Carla Roero. Veronica Perlo. Elena Peila. Anna De
