Caring for the Critically Ill Patient with Cerebral Palsy
|
|
|
- Oswin Bruce
- 5 years ago
- Views:
Transcription
1 Caring for the Critically Ill Patient with Cerebral Palsy Hannah Sauer, PharmD PGY1 Pediatric Pharmacy Resident Mayo Clinic Children s Center 2015 MFMER slide-1
2 Objectives Describe challenges in acute medical management of patients with cerebral palsy (CP) List special considerations for drug therapy in patients with CP Identify the optimal approach to pain and sedation in patients with CP 2015 MFMER slide-2
3 Objectives Describe challenges in acute medical management of patients with cerebral palsy (CP) List special considerations for drug therapy in patients with CP Identify the optimal approach to pain and sedation in patients with CP 2015 MFMER slide-3
4 Cerebral Palsy (CP) Occurs in 205 per 1000 live births Permanent disorder of the development of movement and posture resulting in activity limitation Caused by non-progressive disturbances that occurred in the developing fetal or infant brain Novak, I. J Child Neurol, 2914; 29(8): MFMER slide-4
5 Morbidity and Mortality Most have normal life expectancy 5-10% mortality during childhood Comorbid epilepsy and intellectual disability predictive of premature death Deterioration of function occurs due musculoskeletal impairments Medical interventions do not improve overall gross motor function Taft, LT. Pediatrics in Review, 1995; 16(11): Novak, I. J Child Neurol, 2914; 29(8): MFMER slide-5
6 Classification by Severity I - Indepdently ambulates II - Indepdently ambulates with limitations III - Ambulates with walking aids IV - Independently mobilizes with powered mobility V - Dependent for all mobility 2015 MFMER slide-6
7 Most patients with CP will walk I - Indepdently ambulates II - Indepdently ambulates with limitations III - Ambulates with walking aids IV - Independently mobilizes with powered mobility V - Dependent for all mobility 2015 MFMER slide-7
8 CP Subtypes Spastic Dyskinetic Ataxic 2015 MFMER slide-8
9 Comorbidities Neurologic/Psychiatric Intellectual disability (50%) Behavior disorder (25%) Non-verbal (25%) Epilepsy (25%) Bladder incontinence (25%) Sleep disorder (20%) Musculoskeletal Chronic pain (75%) Hip displacement (33%) Sensory Blindness (10%) Deafness (4%) Other Chronic lung disease (33%) Gastroesophageal reflux Hyper-salivation 2015 MFMER slide-9
10 Chronic Critical Illness Complex disease state with multiple comorbidities Common reasons for ICU admission Orthopedic surgeries Acute infections (pneumonia) Refractory epilepsy Novak, I. J Child Neurol, 2914; 29(8): MFMER slide-10
11 Challenges in Cerebral Palsy Low rates of confidence Consult overload Communication barriers Emotional burden Provider Factors Patient Factors Medication Factors Disease Factors Polypharmacy Medication sensitivity? Pediatric features Limited literature 2015 MFMER slide-11
12 Objectives Describe challenges in acute medical management of patients with cerebral palsy (CP) List special considerations for drug therapy in patients with CP Identify the optimal approach to pain and sedation in patients with CP 2015 MFMER slide-12
13 Common Medications Anti-epileptics Anti-spasticity Anti-spasmodics Analgesics Antacids Laxatives Anti-sialogogues Prophylactic antibiotics Bisphosphonates Assess for drug interactions. Novak, I. J Child Neurol, 2014; 29(8): MFMER slide-13
14 Drug Sensitivity May be more sensitive to dose changes Comorbid intellectual disability associated with idiosyncratic reactions Increased risk for medication withdrawal? Nolan, J, et al. Anaesthsia, 2000; 55(32-41) MFMER slide-14
15 Intrathecal Baclofen Withdrawal If pump must be removed oral baclofen should be started 2-3 days beforehand Monitor for withdrawal Tachycardia, labile pressures, hypothermia Delirium, hallucinations, seizures Muscle rigidity, paresthesis Symptom-directed treatment Ross, JC, et al. Neurocrit Care, 2011; 14: MFMER slide-15
16 Paralytic Agents Up-regulation of ACh receptors in CP patients (30%) Increased risk of hyperkalemia following succinylcholine? Increased sensitivity to non-depolarizing agents? Prosser, DP and Sharma, N. Anaesthsia, 2010; 10(3): MFMER slide-16
17 Paralytic Agents Up-regulation of ACh receptors in CP patients (30%) Increased risk of hyperkalemia following succinylcholine? Increased sensitivity to non-depolarizing agents? Clinically Succinycholine is not contraindicated Non-depolarizing agents are less potent and have shorter duration Prosser, DP and Sharma, N. Anaesthsia, 2010; 10(3): MFMER slide-17
18 Dosing Considerations Increased body surface area to body weight ratio ( giant neonates ) Low body weight relative to non-cp individuals Poor nutritional status Altered absorption Dehydration and hypovolemia common Consider appropriate assessments of renal function Taft, LT. Pediatrics in Review, 1995; 16(11): Novak, I. J Child Neurol, 2914; 29(8): MFMER slide-18
19 ASSESSMENT QUESTION 1 Which of the following represents a true statement about critically ill adult patients with CP? a) Serum creatinine is a reliable indicator of renal function b) Succinylcholine is an appropriate paralytic agent for rapid sequence intubation c) Intrathecal baclofen can be safely held for 48 hours d) Pediatric weight-based dosing should be avoided in anyone over 18 years 2015 MFMER slide-19
20 General Principles of Medication Management Use appropriate weight-based dosing, even in adult patients Keep medication withdrawal on differential Consider unpredicted responses to medications Re-start home medications as soon as possible 2015 MFMER slide-20
21 Objectives Describe challenges in acute medical management of patients with cerebral palsy (CP) List special considerations for drug therapy in patients with CP Identify the optimal approach to pain and sedation in patients with CP 2015 MFMER slide-21
22 Audience Poll: True or False Individuals with cerebral palsy are desensitized to pain and therefore have increased pain tolerance. A. True B. False 2015 MFMER slide-22
23 Pain in CP Increased sensitivity to pain stimuli due to altered excitability in the somatosensory cortex Heterogeneous pain experiences both interand intra-personally Typical and atypical physical manifestations Significant emotional and spiritual burden Riquelme I, et al. Pain Med, 2011; 12(4): Warlow and Hain. Children 2018; 5(13) MFMER slide-23
24 Baseline Pain Burden 75% of patients experience pain at least weekly 50% have episodes of pain that last >9 hours Muscle fatigue, immobility Hypertonia Constipation Musculoskeletal Pain Gastrointestinal dysmotility Warlow and Hain. Children 2018; 5(13) MFMER slide-24
25 Post-Operative Pain Management Post-operative analgesia should be continuous rather than on demand regimens Options: Continuous intravenous opioids Intermittent intravenous and oral opioids Epidural opioids Epidural opioids + local anesthetic 2015 MFMER slide-25
26 Epidural v. Systemic Analgesia Protocols Moore, et al. Study design Retrospective comparison of post-operative analgesia protocols Population Pediatric patients with cerebral palsy undergoing selective dorsal rhizotomy Efficacy Outcomes Difference in age-appropriate pain scale score Frequency of severe pain episode (pain 5) Safety Outcomes Treated nausea or pruritis Hypoxia, supplemental O2 requirements Moore, et al. Pediatric Anesthesia, 2013; 23( ) MFMER slide-26
27 Systemic Protocol Epidural Protocol Continuous infusion fentanyl 1 mcg/kg/h x12 hours followed by 0.5 mcg/kg/h until noon POD2 Diazepam 0.1 mg/kg q4h scheduled x6 doses, then q6h x4 doses Gabapentin added D2 for kids 10 years Ropivicaine 0.2%/ hydromorphone 2.5 mcg/ml Rate of 0.2 ml/kg/h until 6 am POD3 Ketorolac 0.5 mg/kg q6h (total of 8 doses) Methocarbamol 15 mg/kg q8h prn for breakthrough spasm Moore, et al. Pediatric Anesthesia, 2013; 23( ) MFMER slide-27
28 Study Protocols Gabapentin if age-appropriate Midazolam POD1 POD2 POD3 Ropivacaine/hydromorphone epidural Ketorolac Methocarbamol as needed Systemic Protocol Epidural Protocol 2015 MFMER slide-28
29 Patient Characteristics Epidural (n=31) Systemic (n=41) Age (years) 6.06 (±3.78) 6.63 (±4.02) Weight (kg) (±9.53) 24.9 (±14.12) Male 64.5% 61% Diplegia 93.5% 92.6% Moore, et al. Pediatric Anesthesia, 2013; 23( ) MFMER slide-29
30 Post-Operative Pain Scores Epidural Systemic Moore, et al. Pediatric Anesthesia, 2013; 23( ). *p< MFMER slide-30
31 Results Epidural (n=31) Systemic (n=41) OR p-value Episodes of severe pain (POD 0-1) Episodes of severe pain (POD 0-1) Respiratory depression 9.6% 68.3% 20.1 < episodes 74 episodes NR NR 6.5% 41% 10.3 <0.001 Moore, et al. Pediatric Anesthesia, 2013; 23( ). POD=post-op day 2015 MFMER slide-31
32 Epidural v. Systemic Analgesia Protocols Study Conclusions Multimodal approach to pain control is ideal Epidural may be preferred route of analgesia in postoperative setting Study Limitations Study design Cause of improved pain control? Other medications not reported Pain assessment tools Moore, et al. Pediatric Anesthesia, 2013; 23( ) MFMER slide-32
33 Validated Pain Assessment Tools Pediatric Pain Profile (PPP) Twenty item behavioral scale (4 points each) Designed for nonverbal children with severe neurological impairment (SNI) Highly sensitive and specific Face Legs Activity Cry Consolability (FLACC) Five item behavior scale (3 points each) Quick assessment Only validated in postoperative settings for SNI Non-Communication Children s Pain Checklist Revised Thirty item behavior scale (4 points each) Two hours of observation required Highly sensitive and specific Weak correlation to parent scores Warlow and Hain. Children 2018; 5(13) MFMER slide-33
34 ASSESSMENT QUESTION 2: Which of the following may be a sign of pain in a non-verbal patient with cerebral palsy? a) Flushing and/or pallor b) Tachycardia c) Sudden stillness d) Self-harm e) All of the above 2015 MFMER slide-34
35 Procedural Sedation in CP Preferred agents Historically propofol, benzodiazepines No sedative agents contraindicated Consider co-morbidities Seizures Respiratory status Optimal doses and general approaches remain controversial 2015 MFMER slide-35
36 Sedation in Patients with CP Disability associated with risk for respiratory depression and delayed awakening Review of intravenous sedation in patients with disabilities revealed cerebral palsy: Independently associated with SpO2 <90% (OR 1.642, p=0.018) Not independently associated with delayed awakening Yoshikawa, et al. Anesth Prog, 2013; MFMER slide-36
37 General Anesthesia in CP Patients with cerebral palsy require lower doses of propofol for anesthesia induction Target bispectral index (BIS ) mg/kg versus 3.6 mg/kg (p=0.03) Decreased minimum alveolar concentration (MAC) of halothane Levels 20% lower compared to healthy controls (p<0.05) Delayed emergence? Saricaoglu F, et al. Pediatric Anesthesia, 2005; 15: Frei, FJ, et al. Anaesthesia, 1997; 52(11): MFMER slide-37
38 Optimal Propofol Dose for MRI Kim, et al. Study Population Intervention Efficacy Outcomes Cerebral palsy Age 6 months to 5 years Scheduled for brain MRI under sedation Propofol started at 2 mg/kg and modified for sequential patients If unsuccessful, dose increased by 0.5 mg/kg for next child If successful, decreased by 0.5 mg/kg for next child Successful sedation (UMSS* score 3 after 1 minute) ED50 and ED95 determined by modified up-and-down method Kim EJ, et al. Korean J Anesthesiol, 2011; 61(3): *University of Michigan Sedation Scale 2015 MFMER slide-38
39 Patient Characteristics N=20 Age 28.7 months ± 17.8 Weight 10.3 kg ± 4.6 Male 80% MRI scanning time 26.3 minutes Co-morbid behavior disturbances 16 On anti-epileptic medications 4 Kim EJ, et al. Korean J Anesthesiol, 2011; 61(3): MFMER slide-39
40 Results Successful completion of all MRI scans Ten received 2 mg/kg (50% success) Five received 1.5 mg/kg (0% success) Five received 2.5 mg/kg (80% success) Desaturation in 5 patients with successful sedation Proposed therapeutic index: ED50 = 2.07 mg/kg (CI ) ED95 = 2.69 mg/kg (CI )* Mean total dose 3.2 mg/kg ± 0.9 mg/kg Kim EJ, et al. Korean J Anesthesiol, 2011; 61(3): *Up-down method used 2015 MFMER slide-40
41 Study Summary and Conclusions Typical starting procedural sedation 1-2 mg/kg CP alone may not be a compelling indication to give lower doses of procedural sedation Lingering questions What subgroups of patients are worth exploring? Is desaturation in 25% of patients significant? What is the appropriate starting dose of propofol for procedural sedation? Kim EJ, et al. Korean J Anesthesiol, 2011; 61(3): MFMER slide-41
42 The Bottom Line for Pain and Sedation Assess and treat anxiety related to disease and hospitalization Multimodal approaches to pain are ideal (don t forget about baseline pain factors) Continuous pain control > on demand pain control Use appropriate pain assessment tools and rely on caregiver assessments Start with low end of sedative dose ranges and titrate slowly 2015 MFMER slide-42
43 ASSESSMENT QUESTION 3: A 24 yom (30 kg) with cerebral palsy s/p orthopedic surgery is being admitted to your ICU. Which of the following standard post-operative orders is your priority for re-assessment prior to his arrival to the unit? a) Morphine PCA 2 mg load, followed by (level 1) 1 mg IV every 10 minutes 20 mg LO q4h b) Ketorolac 15 mg IV q6h x 4 doses c) Cefazolin 1 g q8h x2 doses d) Senna 17.2 mg PO QHS 2015 MFMER slide-43
44 Summary A lack of published experience in managing CP patients in ICU settings makes it a challenging population Patients with CP should be assessed for appropriate weight-based dosing, drug interactions and medication withdrawal CP does not permit a one size fits all approach to optimal pain and sedation 2015 MFMER slide-44
45 Questions & Discussion 2015 MFMER slide-45
Summary of Delirium Clinical Practice Guideline Recommendations Post Operative
 Summary of Delirium Clinical Practice Guideline Recommendations Post Operative Intensive Care Unit Clinical Practice Guideline for Postoperative Clinical Practice Guidelines for the Delirium in Older Adults;
Summary of Delirium Clinical Practice Guideline Recommendations Post Operative Intensive Care Unit Clinical Practice Guideline for Postoperative Clinical Practice Guidelines for the Delirium in Older Adults;
Lumbar Fusion. Reference Guide for PACU CLINICAL PATHWAY. All patient variances to the pathway are to be circled and addressed in the progress notes.
 Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Analgesic-Sedatives Drug Dose Onset
 Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
Table 4. Commonly used medications in procedural sedation and analgesia Analgesic-Sedatives Fentanyl Morphine IV: 1-2 mcg/kg Titrate 1 mcg/kg q3-5 minutes prn IN: 2 mcg/kg Nebulized: 3 mcg/kg IV: 0.05-0.15
Cerebral Palsy. What is Cerebral Palsy? Clues to Diagnosis of Cerebral Palsy 12/30/2012
 What is Cerebral Palsy? Cerebral Palsy Hamza Alsayouf,MD American Board Of neurology with Special Qualification in Child Neurology American Board of Pediatric Neurology In 2005, a committee of the American
What is Cerebral Palsy? Cerebral Palsy Hamza Alsayouf,MD American Board Of neurology with Special Qualification in Child Neurology American Board of Pediatric Neurology In 2005, a committee of the American
Perioperative Pain Management
 Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Turlough O Hare, MD, FRCPC, MSc Assistant Clinical Professor, Department of Anesthesia, St. Joseph s Healthcare Hamilton McMaster University
 Turlough O Hare, MD, FRCPC, MSc Assistant Clinical Professor, Department of Anesthesia, St. Joseph s Healthcare Hamilton McMaster University To understand the current options available to best manage pain
Turlough O Hare, MD, FRCPC, MSc Assistant Clinical Professor, Department of Anesthesia, St. Joseph s Healthcare Hamilton McMaster University To understand the current options available to best manage pain
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intrathecal Baclofen for Spasticity. Dr. M. Mehra Dr. A. Kumar
 Intrathecal Baclofen for Spasticity Dr. M. Mehra Dr. A. Kumar Goals of Spasticity: Management Decrease spasticity Improve functional ability and independence Decrease pain associated with spasticity Prevent
Intrathecal Baclofen for Spasticity Dr. M. Mehra Dr. A. Kumar Goals of Spasticity: Management Decrease spasticity Improve functional ability and independence Decrease pain associated with spasticity Prevent
DEEP SEDATION TEST QUESTIONS
 Mailing Address: Phone: Fax: The Study Guide is provided for those physicians eligible to apply for Deep Sedation privileges. The Study Guide is approximately 41 pages, so you may consider printing only
Mailing Address: Phone: Fax: The Study Guide is provided for those physicians eligible to apply for Deep Sedation privileges. The Study Guide is approximately 41 pages, so you may consider printing only
Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe )
 PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
Improving the Management of Pain, Agitation, and Delirium (PAD) in the Intensive Care Unit: Translating Evidence Into Practice
 Improving the Management of Pain, Agitation, and Delirium (PAD) in the Intensive Care Unit: Translating Evidence Into Practice Christine M. Groth, Pharm.D., BCCCP NYS Partnership for Patients September
Improving the Management of Pain, Agitation, and Delirium (PAD) in the Intensive Care Unit: Translating Evidence Into Practice Christine M. Groth, Pharm.D., BCCCP NYS Partnership for Patients September
SEEING KETAMINE IN A NEW LIGHT
 SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
MEDICAL ADVISORY COUNCIL Position Statement PREHOSPITAL PAIN MANAGEMENT
 MEDICAL ADVISORY COUNCIL Position Statement PREHOSPITAL PAIN MANAGEMENT MAC PS 2013-002 Appropriate treatment of acute pain in the prehospital arena offers an opportunity to positively impact many patients.
MEDICAL ADVISORY COUNCIL Position Statement PREHOSPITAL PAIN MANAGEMENT MAC PS 2013-002 Appropriate treatment of acute pain in the prehospital arena offers an opportunity to positively impact many patients.
North Wales Critical Care Network
 North Wales Critical Care Network SEDATION GUIDELINES FOR ADULTS IN CRITICAL CARE Approved 6.9.12 1 Sedation guidelines for intensive care Betsi Cadwaladr University Health Board (Adapted from guidelines
North Wales Critical Care Network SEDATION GUIDELINES FOR ADULTS IN CRITICAL CARE Approved 6.9.12 1 Sedation guidelines for intensive care Betsi Cadwaladr University Health Board (Adapted from guidelines
Effective Postoperative Pain Management for Children. Nancy L. Glass, MD, MBA,
 Effective Postoperative Pain Management for Children Nancy L. Glass, MD, MBA, FAAP nglass@bcm.edu @DrNancyGlass1 None Disclosures Learning Objectives At the end of this presentation, participants will
Effective Postoperative Pain Management for Children Nancy L. Glass, MD, MBA, FAAP nglass@bcm.edu @DrNancyGlass1 None Disclosures Learning Objectives At the end of this presentation, participants will
May 2013 Anesthetics SLOs Page 1 of 5
 May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
DELIRIUM IN ICU: Prevention and Management. Milind Baldi
 DELIRIUM IN ICU: Prevention and Management Milind Baldi Contents Introduction Risk factors Assessment Prevention Management Introduction Delirium is a syndrome characterized by acute cerebral dysfunction
DELIRIUM IN ICU: Prevention and Management Milind Baldi Contents Introduction Risk factors Assessment Prevention Management Introduction Delirium is a syndrome characterized by acute cerebral dysfunction
MORPHINE ADMINISTRATION
 Introduction Individualised Administration Drug of Choice Route of Administration & Doses Monitoring of Neonates & high risk patients Team Management Responsibility Morphine Protocol Flow Chart Introduction
Introduction Individualised Administration Drug of Choice Route of Administration & Doses Monitoring of Neonates & high risk patients Team Management Responsibility Morphine Protocol Flow Chart Introduction
Pain Management Strategies Webinar/Teleconference
 Pain Management Strategies Webinar/Teleconference Barry K. Baines, MD April 16, 2009 Objectives Describe the principles of pain management. Identify considerations in the use of opioids. Describe the benefits
Pain Management Strategies Webinar/Teleconference Barry K. Baines, MD April 16, 2009 Objectives Describe the principles of pain management. Identify considerations in the use of opioids. Describe the benefits
Goals for sedation during mechanical ventilation
 New Uses of Old Medications Gina Riggi, PharmD, BCCCP, BCPS Clinical Pharmacist Trauma ICU Jackson Memorial Hospital Disclosure I do not have anything to disclose Objectives Describe the use of ketamine
New Uses of Old Medications Gina Riggi, PharmD, BCCCP, BCPS Clinical Pharmacist Trauma ICU Jackson Memorial Hospital Disclosure I do not have anything to disclose Objectives Describe the use of ketamine
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS)
 Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Opioid reduction strategies in an academic tertiary medical center
 Opioid reduction strategies in an academic tertiary medical center Terry Bosen, PharmD Medication Safety Program Director Vanderbilt University Medical Center Tennessee MME data per capita MME = Morphine
Opioid reduction strategies in an academic tertiary medical center Terry Bosen, PharmD Medication Safety Program Director Vanderbilt University Medical Center Tennessee MME data per capita MME = Morphine
Series 2 dexmedetomidine, tramadol, fentanyl, intellectually disabled patients:
 Series 2 dexmedetomidine, tramadol, fentanyl, intellectually disabled patients: Read the following published scientific articles and answer the questions at the end: Abstract We get a substantial number
Series 2 dexmedetomidine, tramadol, fentanyl, intellectually disabled patients: Read the following published scientific articles and answer the questions at the end: Abstract We get a substantial number
Refractory Status Epilepticus in Children: What are the Options?
 Refractory Status Epilepticus in Children: What are the Options? Weng Man Lam, PharmD, BCPS, BCPPS PICU Clinical Pharmacy Specialist Memorial Hermann Texas Medical Center November 11, 2017 Objectives 1.
Refractory Status Epilepticus in Children: What are the Options? Weng Man Lam, PharmD, BCPS, BCPPS PICU Clinical Pharmacy Specialist Memorial Hermann Texas Medical Center November 11, 2017 Objectives 1.
Gabapentin Does Not Improve Analgesia Outcomes For Total Joint Replacement. Manyat Nantha-Aree, MD
 Gabapentin Does Not Improve Analgesia Outcomes For Total Joint Replacement Manyat Nantha-Aree, MD Objective n Preliminary results of MOBILE study in total hip and knee arthroplasty Background n Gabapentin=
Gabapentin Does Not Improve Analgesia Outcomes For Total Joint Replacement Manyat Nantha-Aree, MD Objective n Preliminary results of MOBILE study in total hip and knee arthroplasty Background n Gabapentin=
Jennifer Mando-Vandrick, PharmD, BCPS Clinical Pharmacist, Emergency Department Director, PGY2 Critical Care Pharmacy Residency Duke University
 Jennifer Mando-Vandrick, PharmD, BCPS Clinical Pharmacist, Emergency Department Director, PGY2 Critical Care Pharmacy Residency Duke University Hospital Objectives Review pertinent pharmacotherapy common
Jennifer Mando-Vandrick, PharmD, BCPS Clinical Pharmacist, Emergency Department Director, PGY2 Critical Care Pharmacy Residency Duke University Hospital Objectives Review pertinent pharmacotherapy common
Acute Pain NETP: SEPTEMBER 2013 COHORT
 Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Acute Pain NETP: SEPTEMBER 2013 COHORT Pain & Suffering an unpleasant sensory & emotional experience associated with actual or potential tissue damage, or described in terms of such damage International
Opioids and Respiratory Depression
 Opioids and Respiratory Depression Clinical Committee Society of Anesthesia and Sleep Medicine https://commons.wikimedia.org/wiki/file:mu_opioid_receptor.svg Introduction Opioid-induced respiratory depression
Opioids and Respiratory Depression Clinical Committee Society of Anesthesia and Sleep Medicine https://commons.wikimedia.org/wiki/file:mu_opioid_receptor.svg Introduction Opioid-induced respiratory depression
Disclosure. Objectives 9/13/2018. NIA/NIH 1R03AG (PI-Bentov) More than Start low go slow. start low go slow
 Sedation and analgesia in geriatric trauma Sept 2018 Itay Bentov MD PhD Disclosure NIA/NIH 1R03AG042353 (PI-Bentov) More than Start low go slow start low go slow Objectives List age-related physiologic
Sedation and analgesia in geriatric trauma Sept 2018 Itay Bentov MD PhD Disclosure NIA/NIH 1R03AG042353 (PI-Bentov) More than Start low go slow start low go slow Objectives List age-related physiologic
Remifentanil PCA In Labor
 Remifentanil PCA In { Jennifer Lucero, MD Clinical Instructor UCSF Department of Anesthesia Remifentanil PCA in Discuss the Pharmokinectics of Remifentanil Review literature on the use of Remifentanil
Remifentanil PCA In { Jennifer Lucero, MD Clinical Instructor UCSF Department of Anesthesia Remifentanil PCA in Discuss the Pharmokinectics of Remifentanil Review literature on the use of Remifentanil
PAIN MANAGEMENT PGY-1. Aaron D. Storms, MD Carin van Zyl, MD Adult and Pediatric Palliative Care, LAC+USC Keck School of Medicine of USC
 PAIN MANAGEMENT PGY-1 Aaron D. Storms, MD Carin van Zyl, MD Adult and Pediatric Palliative Care, LAC+USC Keck School of Medicine of USC Perception Matters A builder aged 29 came to the accident and emergency
PAIN MANAGEMENT PGY-1 Aaron D. Storms, MD Carin van Zyl, MD Adult and Pediatric Palliative Care, LAC+USC Keck School of Medicine of USC Perception Matters A builder aged 29 came to the accident and emergency
SEDATION FOR SMALL PROCEDURES
 SEDATION FOR SMALL PROCEDURES Sinno Simons Erasmus MC Sophia Children s Hospital Rotterdam, the Netherlands s.simons@erasmusmc.nl SEDATION in newborns How and when How to evaluate How to dose Why to use
SEDATION FOR SMALL PROCEDURES Sinno Simons Erasmus MC Sophia Children s Hospital Rotterdam, the Netherlands s.simons@erasmusmc.nl SEDATION in newborns How and when How to evaluate How to dose Why to use
General Anesthesia. Mohamed A. Yaseen
 General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
What does an EEG show?
 EEG Video EEG Ambulatory EEG There s a whole lot of Shakin going on Vagus Nerve Stimulators Division of Child Neurology, Developmental Pediatrics and Genetics Intrathecal Baclofen Pumps EEG first used
EEG Video EEG Ambulatory EEG There s a whole lot of Shakin going on Vagus Nerve Stimulators Division of Child Neurology, Developmental Pediatrics and Genetics Intrathecal Baclofen Pumps EEG first used
Pain: 1-2µg/kg q30-60min prn. effects in 10 minutes. Contraindications: Morphine is preferred in. Duration of Action: minutes. renal failure.
 Procedural Sedation / Analgesia / Anaesthesia Chart - Page 1 Diazepam (Valium) Anxiolytic / Sedative Etomidate (Amidate) Hypnotic / Anesthetic Fentanyl Citrate (Sublimaze) Narcotic Analgesic Dose Pediatric:
Procedural Sedation / Analgesia / Anaesthesia Chart - Page 1 Diazepam (Valium) Anxiolytic / Sedative Etomidate (Amidate) Hypnotic / Anesthetic Fentanyl Citrate (Sublimaze) Narcotic Analgesic Dose Pediatric:
Results of a one-year, retrospective medication use evaluation. Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital
 Results of a one-year, retrospective medication use evaluation Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital Briefly review ketamine s history, mechanism of action, and unique properties
Results of a one-year, retrospective medication use evaluation Joseph Ladd, PharmD PGY-1 Pharmacy Resident BHSF Homestead Hospital Briefly review ketamine s history, mechanism of action, and unique properties
Faculty Advisors: Catherine O Brien, PharmD and Holly Maples, PharmD Location: Arkansas Children s Hospital
 Faculty Advisors: Catherine O Brien, PharmD and Holly Maples, PharmD Location: Arkansas Children s Hospital 2010 Pharmacy Practice Student Research Fellowship Title: Evaluation of Vancomycin Pharmacokinetics
Faculty Advisors: Catherine O Brien, PharmD and Holly Maples, PharmD Location: Arkansas Children s Hospital 2010 Pharmacy Practice Student Research Fellowship Title: Evaluation of Vancomycin Pharmacokinetics
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Identifying patients at risk of delirium: a project for patients undergoing elective orthopedic surgery. The next steps in orthogeriatrics
 Identifying patients at risk of delirium: a project for patients undergoing elective orthopedic surgery Dr. John Joanisse, Chantal Chabot NP The next steps in orthogeriatrics Background More than 8 years
Identifying patients at risk of delirium: a project for patients undergoing elective orthopedic surgery Dr. John Joanisse, Chantal Chabot NP The next steps in orthogeriatrics Background More than 8 years
The child with hemiplegic cerebral palsy thinking beyond the motor impairment. Dr Paul Eunson Edinburgh
 The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older)
 Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Pain Management in the Elderly. Martha Watson, MS, APRN, GCNS Christie Bowser, RN-BC, RN
 Pain Management in the Elderly Martha Watson, MS, APRN, GCNS Christie Bowser, RN-BC, RN Objectives So How Much Do You Really Know? www.geriatricpain.org Geriatric Pain Knowledge Assessment The Geriatric
Pain Management in the Elderly Martha Watson, MS, APRN, GCNS Christie Bowser, RN-BC, RN Objectives So How Much Do You Really Know? www.geriatricpain.org Geriatric Pain Knowledge Assessment The Geriatric
Care in the Last Days of Life
 Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
Delirium. Delirium. Delirium Etiology and Pathophysiology. Fall 2018
 Three most common cognitive problems in adults 1. (acute confusion) 2. Dementia 3. Depression These problems often occur together Can you think of common stimuli for each? 1 1 State of temporary but acute
Three most common cognitive problems in adults 1. (acute confusion) 2. Dementia 3. Depression These problems often occur together Can you think of common stimuli for each? 1 1 State of temporary but acute
PEDIATRIC SPINE SURGERY POST-OP PLAN - Phase:.
 - Phase:. PHYSICIAN S Diagnosis Weight Allergies DETAILS Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert IV to INT when tolerating
- Phase:. PHYSICIAN S Diagnosis Weight Allergies DETAILS Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert IV to INT when tolerating
Sedation and Analgesia in the Critically Ill
 12th Congress of the World Federation of Societies of Intensive and Critical Care Medicine August 29 (Sat.) September 1 (Tue.), 2015 COEX, Seoul, Korea ONE STEP FURTHER: THE PURSUIT OF EXCELLENCE IN CRITICAL
12th Congress of the World Federation of Societies of Intensive and Critical Care Medicine August 29 (Sat.) September 1 (Tue.), 2015 COEX, Seoul, Korea ONE STEP FURTHER: THE PURSUIT OF EXCELLENCE IN CRITICAL
James J. Mooney * and Ashley McDonell ** Introduction
 Opioid Administration as Predictor of Pediatric Epidural Failure James J. Mooney * and Ashley McDonell ** Background: Increasing use of regional analgesia in pediatric populations requires a better understanding
Opioid Administration as Predictor of Pediatric Epidural Failure James J. Mooney * and Ashley McDonell ** Background: Increasing use of regional analgesia in pediatric populations requires a better understanding
Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico
 Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico Balance is not that easy! Weaning Weaning is the liberation of a patient from
Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico Balance is not that easy! Weaning Weaning is the liberation of a patient from
The pain of it all. Rod MacLeod MNZM. Hibiscus Hospice, Auckland and University of Auckland
 The pain of it all Rod MacLeod MNZM Hibiscus Hospice, Auckland and University of Auckland Definition of PAIN An unpleasant sensory and emotional experience which we primarily associate with tissue damage
The pain of it all Rod MacLeod MNZM Hibiscus Hospice, Auckland and University of Auckland Definition of PAIN An unpleasant sensory and emotional experience which we primarily associate with tissue damage
Cerebral Palsy. By:Carrie Siders and Kelsey Hampsey. 3rd hour.
 Cerebral Palsy By:Carrie Siders and Kelsey Hampsey 3rd hour. What is Cerebral Palsy? Cerebral palsy is a physical disability It affects movement and posture It is a permanent life-long condition does not
Cerebral Palsy By:Carrie Siders and Kelsey Hampsey 3rd hour. What is Cerebral Palsy? Cerebral palsy is a physical disability It affects movement and posture It is a permanent life-long condition does not
Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1
 Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1 Fast onset of pain relief with 7% reduction in visual analog scale (VAS) scores
Effective pain management begins with OFIRMEV (acetaminophen) injection FIRST Proven efficacy with rapid reduction in pain 1 Fast onset of pain relief with 7% reduction in visual analog scale (VAS) scores
(30689) PROT Pain PCA Adult Patient Controlled Analgesia
 Diagnosis Allergies Nursing Assess and Document PCA: 1. Assess and document pain rating, sedation level and respiratory rate every 2 hours; assess and document pain rating, sedation level and respiratory
Diagnosis Allergies Nursing Assess and Document PCA: 1. Assess and document pain rating, sedation level and respiratory rate every 2 hours; assess and document pain rating, sedation level and respiratory
PATIENT CARE MANUAL. Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation
 PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
Screening - inclusion criteria
 PAIN OUT Community research EU ROP EAN COMMISSION A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Room number: Screening
PAIN OUT Community research EU ROP EAN COMMISSION A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Room number: Screening
Pain. November 1, 2006 Dr. Jana Pilkey MD, FRCP(C) Internal Medicine, Palliative Medicine
 Pain November 1, 2006 Dr. Jana Pilkey MD, FRCP(C) Internal Medicine, Palliative Medicine Objectives To be able to define pain To be able to evaluate pain To be able to classify types of pain To learn appropriate
Pain November 1, 2006 Dr. Jana Pilkey MD, FRCP(C) Internal Medicine, Palliative Medicine Objectives To be able to define pain To be able to evaluate pain To be able to classify types of pain To learn appropriate
Disclosure. Case. Objectives. Definition of Pediatric Pain. Pediatric Pain: Misunderstood. "Ow, Mommy it Hurts!" Managing Pediatric Pain 7/25/2013
 47 th Annual Meeting August 2-4, 2013 Orlando, FL "Ow, Mommy it Hurts!" Managing Pediatric Pain Tara McCabe, Pharm.D. Pediatric Hematology/Oncology Clinical Pharmacy Specialist UF Health Shands Children
47 th Annual Meeting August 2-4, 2013 Orlando, FL "Ow, Mommy it Hurts!" Managing Pediatric Pain Tara McCabe, Pharm.D. Pediatric Hematology/Oncology Clinical Pharmacy Specialist UF Health Shands Children
Status Epilepticus: Implications Outside the Neuro-ICU
 Status Epilepticus: Implications Outside the Neuro-ICU Jeffrey M Singh MD Critical Care and Neurocritical Care Toronto Western Hospital October 31 st, 2014 Disclosures I (unfortunately) have no disclosures
Status Epilepticus: Implications Outside the Neuro-ICU Jeffrey M Singh MD Critical Care and Neurocritical Care Toronto Western Hospital October 31 st, 2014 Disclosures I (unfortunately) have no disclosures
PEDIATRIC SPINE SURGERY POST-OP PLAN - Phase: Pediatric Spine Surgery General Orders
 - Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
- Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
Renal Palliative Care Last Days of Life
 Renal Palliative Care Last Days of Life Introduction This guideline is an aid to clinical decision-making and good practice for patients with stage 4-5 chronic kidney disease (egfr
Renal Palliative Care Last Days of Life Introduction This guideline is an aid to clinical decision-making and good practice for patients with stage 4-5 chronic kidney disease (egfr
Piecing the Puzzle Together: Pharmacologic Approaches to Behavioral Management in Autism Spectrum Disorder
 Piecing the Puzzle Together: Pharmacologic Approaches to Behavioral Management in Autism Spectrum Disorder Hannah Sauer, PharmD PGY1 Pediatric Pharmacy Resident Mayo Clinic 2015 MFMER slide-1 Objectives
Piecing the Puzzle Together: Pharmacologic Approaches to Behavioral Management in Autism Spectrum Disorder Hannah Sauer, PharmD PGY1 Pediatric Pharmacy Resident Mayo Clinic 2015 MFMER slide-1 Objectives
STARSHIP WITHDRAWAL OF ANALGESIA AND SEDATION
 STARSHIP WITHDRAWAL OF ANALGESIA AND SEDATION Patients receiving analgesia and/or sedation for longer than 5-7 days may suffer withdrawal if these drugs are suddenly stopped. To prevent this happening
STARSHIP WITHDRAWAL OF ANALGESIA AND SEDATION Patients receiving analgesia and/or sedation for longer than 5-7 days may suffer withdrawal if these drugs are suddenly stopped. To prevent this happening
What s New in Post-Cesarean Analgesia?
 Anesthesia & Obstetrics What s New in Post-Cesarean Analgesia? October 23rd, 2013 2013 UCSF What Does The Evidence Tell Us? Mark Rollins, MD, PhD UC SF Post-Delivery Pain (Mean pain scores for first 24
Anesthesia & Obstetrics What s New in Post-Cesarean Analgesia? October 23rd, 2013 2013 UCSF What Does The Evidence Tell Us? Mark Rollins, MD, PhD UC SF Post-Delivery Pain (Mean pain scores for first 24
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM. Is This Strictly a Pain Episode? Decision 7: Referrals
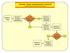 ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
Care of the dying in End Stage Kidney Disease (ESKD) - Conservative. Elizabeth Josland Renal Supportive Care CNC St George Hospital
 Care of the dying in End Stage Kidney Disease (ESKD) - Conservative Elizabeth Josland Renal Supportive Care CNC St George Hospital Introduction What does conservative management look like? How does the
Care of the dying in End Stage Kidney Disease (ESKD) - Conservative Elizabeth Josland Renal Supportive Care CNC St George Hospital Introduction What does conservative management look like? How does the
Hip Hemiarthroplasty Post Op Version 2 4/20/17
 Patient Name: Diagnosis: Allergies with reaction type: Hip Hemiarthroplasty Post Op Version 2 4/20/17 Patient Placement General Diagnosis/Procedure: Preferred Location/Unit Ortho/Neuro PCU ICU General
Patient Name: Diagnosis: Allergies with reaction type: Hip Hemiarthroplasty Post Op Version 2 4/20/17 Patient Placement General Diagnosis/Procedure: Preferred Location/Unit Ortho/Neuro PCU ICU General
Critical Care Strategic Clinical Network Provincial ICU Delirium Framework
 Pain assessed and documentation using validated tool (CPOT and NRS) Assess and document q4h and prn 100% of patients assessed for pain and documented q4h A: Assess, Prevent & Manage Pain Self Reporting
Pain assessed and documentation using validated tool (CPOT and NRS) Assess and document q4h and prn 100% of patients assessed for pain and documented q4h A: Assess, Prevent & Manage Pain Self Reporting
Satisfactory Analgesia Minimal Emesis in Day Surgeries. (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone
 Satisfactory Analgesia Minimal Emesis in Day Surgeries (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone HARSHA SHANTHANNA ASSISTANT PROFESSOR ANESTHESIOLOGY MCMASTER UNIVERSITY
Satisfactory Analgesia Minimal Emesis in Day Surgeries (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone HARSHA SHANTHANNA ASSISTANT PROFESSOR ANESTHESIOLOGY MCMASTER UNIVERSITY
Sedative-Hypnotics. Sedative Agents (General Considerations)
 Sedative Agents (General Considerations) No best sedative agent Any agent given in sufficient dosage can produce any level of sedation Intravenous dosing is more predictable then intramuscular or oral
Sedative Agents (General Considerations) No best sedative agent Any agent given in sufficient dosage can produce any level of sedation Intravenous dosing is more predictable then intramuscular or oral
Choose a category. You will be given the answer. You must give the correct question. Click to begin.
 Instructions for using this template. Remember this is Jeopardy, so where I have written Answer this is the prompt the students will see, and where I have Question should be the student s response. To
Instructions for using this template. Remember this is Jeopardy, so where I have written Answer this is the prompt the students will see, and where I have Question should be the student s response. To
General anesthesia. No single drug capable of achieving these effects both safely and effectively.
 General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
Long Term Care Formulary HCD - 08
 1 of 5 PREAMBLE Opioids are an important component of the pharmaceutical armamentarium for management of chronic pain. The superiority of analgesic effect of one narcotic over another is not generally
1 of 5 PREAMBLE Opioids are an important component of the pharmaceutical armamentarium for management of chronic pain. The superiority of analgesic effect of one narcotic over another is not generally
Post-caesarean analgesia. Genevieve Goulding Royal Brisbane & Women's Hospital 1
 Post-caesarean analgesia Genevieve Goulding Royal Brisbane & Women's Hospital 1 Contemporary challenges & barriers to providing optimal post-caesarean analgesia Genevieve Goulding Royal Brisbane & Women's
Post-caesarean analgesia Genevieve Goulding Royal Brisbane & Women's Hospital 1 Contemporary challenges & barriers to providing optimal post-caesarean analgesia Genevieve Goulding Royal Brisbane & Women's
Post-op Care and Pain. Dr. Karima
 Post-op Care and Pain Management Dr. Karima Post-op monitoring 1. Hand-off from operation Who is the patient? (premature, underlying problems or medical conditions, what was the problem/ reason for surgery,
Post-op Care and Pain Management Dr. Karima Post-op monitoring 1. Hand-off from operation Who is the patient? (premature, underlying problems or medical conditions, what was the problem/ reason for surgery,
Screening - inclusion criteria
 A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Patient code (local): Room number: Screening - inclusion criteria
A Date of data collection: B Time of data collection: C Ward where data is collected: 2 0 1 Y M M D D H H M M D Research assistant Code: Patient code (local): Room number: Screening - inclusion criteria
Effects of Home Antipsychotic Reinitiation in ICU Patients with a History of Mental Illness
 Effects of Home Antipsychotic Reinitiation in ICU Patients with a History of Mental Illness Gary Sweet, PharmD PGY-1 Pharmacy Practice Resident St. John Medical Center, Tulsa, OK Conflict of Interest Nothing
Effects of Home Antipsychotic Reinitiation in ICU Patients with a History of Mental Illness Gary Sweet, PharmD PGY-1 Pharmacy Practice Resident St. John Medical Center, Tulsa, OK Conflict of Interest Nothing
Chapter 25. General Anesthetics
 Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
5 th ERAS UK Conference. Advances in Pain Management. Jayne Balson Advanced Nurse Specialist Pain Management Western General Hospital Edinburgh
 5 th ERAS UK Conference Advances in Pain Management Jayne Balson Advanced Nurse Specialist Pain Management Western General Hospital Edinburgh Pre-op information Optimised organ function No nutritional
5 th ERAS UK Conference Advances in Pain Management Jayne Balson Advanced Nurse Specialist Pain Management Western General Hospital Edinburgh Pre-op information Optimised organ function No nutritional
Using methadone alongside other opioids. Dr. Jo Murrell BVSc. (hons), PhD, DiplECVAA, MRCVS
 Using methadone alongside other opioids Dr. Jo Murrell BVSc. (hons), PhD, DiplECVAA, MRCVS Why might we want to use methadone alongside other opioids? 1. Multi-modal analgesia strategies e.g. using methadone
Using methadone alongside other opioids Dr. Jo Murrell BVSc. (hons), PhD, DiplECVAA, MRCVS Why might we want to use methadone alongside other opioids? 1. Multi-modal analgesia strategies e.g. using methadone
Opioid Case Studies. Thomas P. Pittelkow, D.O., M.P.H. Mayo Clinic College of Medicine Rochester, MN. September 29, MFMER slide-1
 Opioid Case Studies Thomas P. Pittelkow, D.O., M.P.H. Mayo Clinic College of Medicine Rochester, MN September 29, 2016 2015 MFMER slide-1 Disclosures Relevant Financial Relationship(s) None Off Label and/or
Opioid Case Studies Thomas P. Pittelkow, D.O., M.P.H. Mayo Clinic College of Medicine Rochester, MN September 29, 2016 2015 MFMER slide-1 Disclosures Relevant Financial Relationship(s) None Off Label and/or
Overview of Essentials of Pain Management. Updated 11/2016
 0 Overview of Essentials of Pain Management Updated 11/2016 1 Overview of Essentials of Pain Management 1. Assess pain intensity on a 0 10 scale in which 0 = no pain at all and 10 = the worst pain imaginable.
0 Overview of Essentials of Pain Management Updated 11/2016 1 Overview of Essentials of Pain Management 1. Assess pain intensity on a 0 10 scale in which 0 = no pain at all and 10 = the worst pain imaginable.
Overcoming Opioid-Induced Oversedation: More Than Meets the Eye
 Overcoming Opioid-Induced Oversedation: More Than Meets the Eye ANCC National Magnet Conference 2013 Jeannine M. Brant, PhD, APRN, AOCN Lisa Peterson, RN-BC, BSN Health Care, Education and Research www.billingsclinic.com
Overcoming Opioid-Induced Oversedation: More Than Meets the Eye ANCC National Magnet Conference 2013 Jeannine M. Brant, PhD, APRN, AOCN Lisa Peterson, RN-BC, BSN Health Care, Education and Research www.billingsclinic.com
Delirium and Dementia
 Delirium and Dementia Elder Friendly Care in Acute Care Seniors Health Strategic Clinical Network Acute Care Stress Blender Poor Poor sleep At-Risk Older Adult TREAT CAUSE immediately & aggressively. Increased
Delirium and Dementia Elder Friendly Care in Acute Care Seniors Health Strategic Clinical Network Acute Care Stress Blender Poor Poor sleep At-Risk Older Adult TREAT CAUSE immediately & aggressively. Increased
INTRATHECAL THERAPY TREATMENT OF PAIN AND SPASTICITY. Christopher S. Rumana, M.D. Tallahassee Neurological Clinic Department of Neurosurgery
 INTRATHECAL THERAPY TREATMENT OF PAIN AND SPASTICITY Christopher S. Rumana, M.D. Tallahassee Neurological Clinic Department of Neurosurgery Intrathecal Therapy Insertion of a drug into CSF space, commonly
INTRATHECAL THERAPY TREATMENT OF PAIN AND SPASTICITY Christopher S. Rumana, M.D. Tallahassee Neurological Clinic Department of Neurosurgery Intrathecal Therapy Insertion of a drug into CSF space, commonly
Assessment. Consults & Referrals
 University of Virginia Health System Clinical Pathway: Whipple Enhanced Recovery After () LOS: 4-5 days Date of Origin/Revision: June 29, 2016/September 6, 2017/January 31, 2018 : SAS : : : D1 D2 D 3/
University of Virginia Health System Clinical Pathway: Whipple Enhanced Recovery After () LOS: 4-5 days Date of Origin/Revision: June 29, 2016/September 6, 2017/January 31, 2018 : SAS : : : D1 D2 D 3/
PEDIATRIC ANALGESIA AND SEDATION DRUG MANUAL
 PEDIATRIC ANALGESIA AND SEDATION DRUG MANUAL HARBOR-UCLA MEDICAL CENTER PEDIATRIC ANALGESIA AND SEDATION DRUG MANUAL SECTION Preface Disclaimer Nonpharmacologic Methods Table of Contents PAGE i ii iii
PEDIATRIC ANALGESIA AND SEDATION DRUG MANUAL HARBOR-UCLA MEDICAL CENTER PEDIATRIC ANALGESIA AND SEDATION DRUG MANUAL SECTION Preface Disclaimer Nonpharmacologic Methods Table of Contents PAGE i ii iii
Sedation and Delirium Questions
 Sedation and Delirium Questions TLC Curriculum William J. Ehlenbach, MD MSc Assistant Professor of Medicine Pulmonary & Critical Care Medicine Question 1 Deep sedation in ventilated critically patients
Sedation and Delirium Questions TLC Curriculum William J. Ehlenbach, MD MSc Assistant Professor of Medicine Pulmonary & Critical Care Medicine Question 1 Deep sedation in ventilated critically patients
Appendix A: Pharmacologic approaches to pain management during MVA
 Pain medication Though the medications shown below are commonly used for pain management during uterine evacuation, many other options exist. This table does not cover general anesthetic agents. Both anxiolytics
Pain medication Though the medications shown below are commonly used for pain management during uterine evacuation, many other options exist. This table does not cover general anesthetic agents. Both anxiolytics
Equianalgesic Dosing: Making Opioid Interchange Easier. Joseph Bubalo PharmD, BCPS, BCOP Oncology Clinical Pharmacist Assistant Professor Of Medicine
 Equianalgesic Dosing: Making Opioid Interchange Easier Joseph Bubalo PharmD, BCPS, BCOP Oncology Clinical Pharmacist Assistant Professor Of Medicine 1 Why Change Opioids? Side Effects Insufficient Pain
Equianalgesic Dosing: Making Opioid Interchange Easier Joseph Bubalo PharmD, BCPS, BCOP Oncology Clinical Pharmacist Assistant Professor Of Medicine 1 Why Change Opioids? Side Effects Insufficient Pain
Palliative Care for Primary Care Providers QUYNH BUI, MD MPH DECEMBER 2015
 Palliative Care for Primary Care Providers QUYNH BUI, MD MPH DECEMBER 2015 Objectives Define palliative care and primary palliative care Describe the rationale for providing primary palliative care in
Palliative Care for Primary Care Providers QUYNH BUI, MD MPH DECEMBER 2015 Objectives Define palliative care and primary palliative care Describe the rationale for providing primary palliative care in
PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE
 1 PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE 2 Table of Contents page# Learning Objectives 3 Concepts of Pain Relief 4 Introduction to PCA 4 Definition of terms used with IV PCA 6 Opioids used with
1 PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE 2 Table of Contents page# Learning Objectives 3 Concepts of Pain Relief 4 Introduction to PCA 4 Definition of terms used with IV PCA 6 Opioids used with
How Low Should You Go? Management of Blood Pressure in Intracranial Hemorrhage
 How Low Should You Go? Management of Blood Pressure in Intracranial Hemorrhage Rachael Scott, Pharm.D. PGY2 Critical Care Pharmacy Resident Pharmacy Grand Rounds August 21, 2018 2018 MFMER slide-1 Patient
How Low Should You Go? Management of Blood Pressure in Intracranial Hemorrhage Rachael Scott, Pharm.D. PGY2 Critical Care Pharmacy Resident Pharmacy Grand Rounds August 21, 2018 2018 MFMER slide-1 Patient
Balanced Analgesia With NSAIDS and Coxibs. Raymond S. Sinatra MD, Ph.D
 Balanced Analgesia With NSAIDS and Coxibs Raymond S. Sinatra MD, Ph.D Prostaglandins and Pain The primary noxious mediator released from damaged tissue is prostaglandin (PG) PG is responsible for nociceptor
Balanced Analgesia With NSAIDS and Coxibs Raymond S. Sinatra MD, Ph.D Prostaglandins and Pain The primary noxious mediator released from damaged tissue is prostaglandin (PG) PG is responsible for nociceptor
Baptist Health Lexington. ERAS Protocols
 Baptist Health Lexington ERAS Protocols Enhanced Recovery After Surgery BHLex Colorectal ERAS Protocol Preoperative Patient/Family Education: PAT and office, ERAS brochure & educational flyer/checklist
Baptist Health Lexington ERAS Protocols Enhanced Recovery After Surgery BHLex Colorectal ERAS Protocol Preoperative Patient/Family Education: PAT and office, ERAS brochure & educational flyer/checklist
Practical Management of the Delirious Patient with Mental Retardation by the Nurse Anesthetist
 Practical Management of the Delirious Patient with Mental Retardation by the Nurse Anesthetist 1. Basic Facts on Delirium The nurse anesthetist plays an important role in prevention of delirium among surgical
Practical Management of the Delirious Patient with Mental Retardation by the Nurse Anesthetist 1. Basic Facts on Delirium The nurse anesthetist plays an important role in prevention of delirium among surgical
Pain & Sedation Management in PICU. Marut Chantra, M.D.
 Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Digital RIC. Rhode Island College. Linda M. Green Rhode Island College
 Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2013 The Relationship
Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 1-1-2013 The Relationship
Delirium. Assessment and Management
 Delirium Assessment and Management Goals and Objectives Participants will: 1. be able to recognize and diagnose the syndrome of delirium. 2. understand the causes of delirium. 3. become knowledgeable about
Delirium Assessment and Management Goals and Objectives Participants will: 1. be able to recognize and diagnose the syndrome of delirium. 2. understand the causes of delirium. 3. become knowledgeable about
01/07/2018 ISCHAEMIC PAIN IN NON-RECONSTRUCTABLE CRITICAL LIMB ISCHAEMIA PRESENTATION OUTLINE
 ISCHAEMIC PAIN IN NON-RECONSTRUCTABLE CRITICAL LIMB ISCHAEMIA Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE A Typical Case Background
ISCHAEMIC PAIN IN NON-RECONSTRUCTABLE CRITICAL LIMB ISCHAEMIA Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE A Typical Case Background
