Laparoscopy and Robotics Laparoendoscopic Single-site Surgery: Initial Hundred Patients
|
|
|
- Ada Horn
- 5 years ago
- Views:
Transcription
1 Laparoscopy and Robotics Laparoendoscopic Single-site Surgery: Initial Hundred Patients Mihir M. Desai, Andre K. Berger, Ricardo Brandina, Monish Aron, Brian H. Irwin, David Canes, Mahesh R. Desai, Pradeep P. Rao, Rene Sotelo, Robert Stein, and Inderbir S. Gill OBJECTIVES To report our initial experience with laparoendoscopic single-site (LESS) surgery in 100 patients in urology. METHODS Between October 2007 and December 2008, we performed LESS urologic procedures in 100 patients for various indications. These included nephrectomy (N 34; simple 14, radical 3, donor 17), nephroureterectomy (N 2), partial nephrectomy (N 6), pyeloplasty (N 17), transvesical simple prostatectomy (N 32), and others (N 9). Data were prospectively collected in a database approved by the Institutional Review Board. All procedures were performed using a novel single-port device (r-port) and a varying combination of standard and specialized bent/articulating laparoscopic instruments. Robotic assistance was used to perform LESS pyeloplasty (N 2) and simple prostatectomy (N 1). In addition to standard perioperative data, we obtained data on postdischarge analgesia requirements, time to complete convalescence, and time to return to work. RESULTS In the study period, LESS procedures accounted for 15% of all laparoscopic cases by the authors for similar indications. Conversion to standard multiport laparoscopy was necessary in 3 cases, addition of a single 5-mm port was necessary in 3 cases, and conversion to open surgery was necessary in 4 cases. On death occurred following simple prostatectomy in a Jehovah s Witness due to patient refusal to accept transfusion following hemorrhage. Intra- and postoperative complications occurred in 5 and 9 cases, respectively. Mean operative time was 145, 230, 236, and 113 minutes and hospital stay was 2, 2.9, 2, and 3 days for simple nephrectomy, donor nephrectomy, pyeloplasty, and simple prostatectomy, respectively. CONCLUSIONS The LESS surgery is technically feasible for a variety of ablative and reconstructive applications in urology. With proper patient selection, conversion and complications rates are low. Improvement in instrumentation and technology is likely to expand the role of LESS in minimally invasive urology. UROLOGY 74: , Elsevier Inc. Laparoscopic surgery is beginning to gain acceptance as a standard of care in many intra-abdominal procedures in urology. With increasing experience in the laparoscopic environment, efforts are now directed at further minimizing morbidity and improving cosmetic outcomes. This has led to the development of techniques, multichannel single-access ports, and novel bent/articulating instruments that could allow the laparoscopic procedure to be performed through a single skin incision often hidden within the umbilicus. 1-4 Although several variants of this approach have been reported in the published data on surgery under various terminologies From the Department of Urology, Glickman Urological and Kidney Institute, Cleveland Clinic, Cleveland, Ohio; Muljibhai Patel Urological Hospital Gujarat, India; and Clinica la Floresta, Caracas, Venezuela Reprint requests: Mihir M. Desai, M.D., Stevan B. Streem Center for Endourology and Glickman Urological and Kidney Institute, Cleveland Clinic, 9500 Euclid Ave, A100, Cleveland, OH desaim1@ccf.org Submitted: January 2, 2009, accepted (with revisions): February 4, 2009 and acronyms, a recently convened international multidisciplinary consortium of experts have coined the term LESS (LaparoEndoscopic Single Site) surgery to collectively encompass laparoscopic procedures performed through a single skin incision (Gill et al, unpublished data). We have previously reported the initial developmental experiences with select LESS procedures in urology. 3,4,5-7 After considerably increasing our experience over the past year, we herein report cumulative data in the initial 100 patients undergoing ablative and reconstructive LESS surgery with a view to presenting a more mature perspective on the emerging field of single-access urologic surgery. MATERIAL AND METHODS Between October 2007 and December 2008, we performed LESS urologic procedures in 100 patients. These procedures 2009 Elsevier Inc /09/$ All Rights Reserved doi: /j.urology
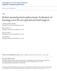
2 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Ureteral Reimplant Pyeloplasty Nephroureterectomy Kidney Cyst Excision Partial Nephrectomy Donor Nephrectomy Radical Nephrectomy Simp.Nephrectomy Standart LESS Figure 1. Graph shows the percentage of LESS cases performed using vis-à-vis standard laparoscopy by the same surgeon in the same duration. comprised 15% of the total number of laparoscopic procedures (N 67; excluding 33 transvesical LESS procedures) performed by the authors in the same duration for similar indications (Fig. 1). Data were prospectively entered in an Institutional Review Board approved database and were retrospectively reviewed. The various LESS procedures performed included nephrectomy (N 34; simple 14, radical 3, donor 17), nephroureterectomy (N 2), partial nephrectomy (N 6), pyeloplasty (N 17), simple prostatectomy (N 32), and others (N 9). The detailed list of procedures and indications are outlined in Table 1. All procedures were performed using a novel single-port device (r-port, Advanced Surgical Concepts, Wicklow, Ireland) for access. Access was obtained through the umbilicus in all 67 laparoscopic cases and through a solitary incision in the suprapubic crease in the 33 transvesical cases. The detailed description and functioning of the r-port has been described previously. Our technique for LESS nephrectomy, pyeloplasty and reconstructive procedures, donor nephrectomy, partial nephrectomy, and simple prostatectomy are detailed elsewhere. In general, we used standard laparoscopic instrumentation for most dissection and retraction maneuvers. Pre-bent instruments and specialized articulating instruments such as LaparoAngle (Cambridge Endo, Framington, MA) and RealHand (Novare Surgical Systems, Cupertino, CA) were selectively used. We used, via a skin puncture, an ancillary 2-mm Verres needle-port with needlescopic graspers to assist during suturing for all reconstructive and select ablative procedures (to facilitate retraction). A rigid 5 mm, 30, or a flexible-tip 0 digital video-laparoscope (EndoEYE, Olympus Medical, Japan) was used in all 100 cases. Three LESS procedures (1 transvesical simple prostatectomy and 2 pyeloplasty) were performed using robotic assistance (da Vinci S, Intuitive Surgical, Sunnyvale, CA). The robotic transvesical simple prostatectomy was performed using the 4-channel r-port through which the robotic camera and working trocars were inserted. For robotic LESS pyeloplasty, the robotic telescope and 15-mm working instrument were inserted through the 3-channel r-port, and the other working instrument was passed through a robotic trocar inserted through a separate fascial puncture alongside the r-port but through the same umbilical incision. All maneuvers in the 3 robotic LESS cases were performed robotically by the surgeon at the console. All data were analyzed and reported as mean SD, median (range). Analgesia scores, narcotic requirements, convalescence data, and time off work were reported for procedures involving more than 10 cases. RESULTS Demographic data are detailed in Table 2. For the entire cohort, the mean age was (10-89) years, mean BMI was 26 5 (15-41), and 15% patients had undergone abdominal surgery previously. Mean operative time was 145, 230, 236, and 113 minutes, and estimated blood loss was 109, 104, 79, and 423 ml for simple nephrectomy, donor nephrectomy, pyeloplasty, and simple prostatectomy, respectively (Table 2). Mean hospital stay was 2, 2.9, 2, and 3 days; time to return to work was 19, 17, 22, and 14 days; and time to complete convalescence was 32, 25, 31, and 15 days for simple nephrectomy, donor nephrectomy, pyeloplasty, and simple prostatectomy, respectively (Table 3). An additional 5-mm port was required in 3 cases and 3 cases were converted to standard multiport laparoscopy (Table 4). Two patients undergoing transvesical prostatectomy required extension of the suprapubic incision to facilitate digital enucleation of the adenoma to complete the procedure. Two additional patients in the transvesical prostatectomy group required open conversion for managing an inadvertent bowel injury and bleeding, respectively (vide infra). One death occurred in a Jehovah s Witness undergoing simple prostatectomy due to refusal to accept blood transfusion for hemorrhage due to coagulopathy. In this patient, the intraoperative blood loss was 50 ml and good hemostasis was secured on enucleation of adenoma; subsequently, persistent oozing was noted, and blood transfusions and clotting factors were refused by the patient. All maneuvers including open surgical suturing, packing of the prostatic fossa and bilateral internal artery embolization failed to stop the bleeding. Intraoperative complications were noted in 5 patients (bleeding 4, bowel injury 1) and postoperative complications in 9 cases (bleeding 4, corneal abrasion 1, drug-induced dyskinesia 1, urinary tract infection 1, urine leak 1). Most complications (3 intraoperative and 5 postoperative) were seen with the single-port transvesical enucleation of the prostate (STEP) procedure. There was an inadvertent bowel injury in a patient with previous laparotomy, which occurred during intravesical insertion of the r-port. The injury was recognized at the completion of the procedure and was repaired by laparotomy without further sequelae. One patient undergoing the STEP procedure had intraoperative bleeding requiring transfusion that was managed by placing sutures. Bleeding in the immediate postoperative was seen in 4 patients undergoing STEP procedure; 1 patient required open surgical exploration for securing hemostasis and 3 patients were managed conservatively with blood transfusion. Injury to the renal and gonadal vein occurred in 1 patient each undergoing LESS adrenalectomy and radical nephrectomy, respectively. There was minor oozing due to partial avulsion of the gonadal vein close to its origin 806 UROLOGY 74 (4), 2009
3 Table 1. LESS procedures (N 100): indications and patient demographics LESS Procedure No. Patients Indication Age (y) BMI Simle nephrectomy 14 Benign nonfunctioning kidney (16-78) ( ) Radical nephrectomy 3 Kidney tumor (54-86) (30-31) Donor nephrectomy 17* Renal donation (21-65) 25 (20-32) Partial nephrectomy 6 Kidney tumor Kidney cyst excision 1 Extrinsic compression and ureteropelvic junction obstruction Nephroureterectomy 2 Upper tract TCC (n 1) severe reflux recurrent pyelonephritis (n 1) Pyeloplasty 17 Primary ureteropelvic junction obstruction 62 (34-80) 25 (22-32) /55 18/ (10-79) 23 (15-35) Ureteral reimplant 2 Ureteral stricture 42, 22 25, 20 Ileal ureter 3 Ureteral stricture (23-72) 25.2 ( ) Simple prostatectomy 32 BPH ( 80 g) (57-89) 26 (19-41) Transvesical mesh sling removal 1 Erosion of sling into bladder with stone formation Adrenalectomy 1 Adrenal mass Hysterectomy 1 Fibroids and menorrhagia Total (10-89) 25 (15-41) * One patient undergoing LESS donor nephrectomy underwent concomitant adrenalectomy. Two LESS pyeloplasties were performed using robotic assistance. One patient undergoing simple prostatectomy was performed using robotic assistance. from the inferior vena cava that was adequately controlled with clips. The renal vein injury during LESS adrenalectomy was successfully suture-repaired after conversion to standard laparoscopy. The patient with renal vein injury was subsequently found to have a renal vein thrombus necessitating chronic anticoagulation. The renal vein is patent at 3-month follow-up. Addition of an extra 5-mm port was necessary in 3 cases for liver retraction (N 2), or tissue retraction (N 1). Apart from the 2 vascular complications, conversion to laparoscopy was necessary in a patient undergoing pyeloplasty for secondary ureteropelvic junction obstruction, who had significant peri-ureteropelvic junction adhesions and who ultimately required a nephrectomy, as it was a longsegment stricture and a borderline functioning kidney. Treatment efficacies for various LESS procedures were comparable to standard laparoscopic results reported in published studies and are detailed in Table 4. All patients undergoing radical nephrectomy had negative surgical margins. Median warm ischemia time for the donor nephrectomy group was 5.8 (2.5-10) minutes. One allograft (warm ischemia time 3.8 minutes, completely uneventful intraoperatively) was lost on postoperative day 1 from intrarenal vascular thrombosis of unclear etiology. All patients in the pyeloplasty group remain symptom-free. Postoperative imaging showed unobstructed drainage in 15 of the 16 patients in whom data was available. The patients undergoing ileal interposition (N 3) and ureteroneocystostomy (N 2) show unobstructed drainage at latest follow-up. Apart from the patient who died, the remaining 31 patients undergoing transvesical simple prostatectomy show improvement in flow rates and symptom scores and no patient has urinary incontinence. The patient undergoing excision of the calcified mesh developed recurrent stone formation at the previous site and is scheduled to undergo a transvesical partial cystectomy with suture reconstruction. COMMENT The last decade has witnessed an exponential increase in laparoscopic and robotic surgery for the treatment of various surgical disorders. Within urology, a significant number of reconstructive and ablative procedures for benign and oncologic indications are being performed using laparoscopic/robotic techniques with comparable efficacy and reduced morbidity vis-a-vis their open surgical counterpart. Efforts are ongoing to further decrease morbidity and visible scarring of laparoscopic surgery. Natural orifice translumenal endoscopic surgery (NOTES) is UROLOGY 74 (4),
4 Table 2. LESS urologic procedures (N 100): operative data Procedure OR Time (min) EBL (ml) Complications Additional Ports Intra Post 2 mm 5 mm Conversion Simple nephrectomy (41%) (70-300) 100 (20-300) Radical nephrectomy (100%) ( ) 200 ( ) Donor nephrectomy (100%) ( ) 50 (50-200) Partial nephrectomy (100%) 0 1 lap* 270 ( ) 525 ( ) Kidney cyst excision (100%) 0 0 Nephroureterectomy 90/200 75/ Pyeloplasty (100%) 2 1 lap* 225 ( ) 62 (10-150) Ureteral reimplant 210, , (100%) 0 0 Ileal ureter (100%) ( ) 170 (90-250) Simple prostatectomy open 90 (45-360) 250 ( ) 2 open Transvesical mesh removal Adrenalectomy (100%) 0 1 Lap Hysterectomy Total Additional 5-mm ports were required in 3 cases: Liver retraction (N 2), tissue retraction (N 1). * difficult mobilization of the ureter. 1 enterotomy, 1 bleeding. failure to progress. bleeding. Table 3. Less urologic procedures (N 100) postoperative and convalescence data Procedure Hospital Stay Median (Range) Morphine Equivalents (mg) Post-Discharge Analgesic Use (d) Return to Work (d) Complete Convalescence (d) Simple nephrectomy (1-4) 76 (0-104) 28 (1-10) 23 (6-28) 28 (28-40) Radical nephrectomy (2-5) Donor nephrectomy (1-6) 7 (0-57) 3 (0-10) 10 (10-31) 21 (14-42) Partial nephrectomy (2-22) 28 (5-50) 7 (0-7) 24.5 (14-35) 14 (14-35) Kidney cyst excision 1 Nephroureterectomy 5/1 Pyeloplasty (2-3) 29.7 (0-63) 1 (0-10) 18 (7-45) 28 (14-60) Ileal ureter 2 Re-implant 4 Simple prostatectomy (1-10) 21 (0-95) 1 (1-4) 10 (7-30) 14 (10-30) Transvesical mesh 1 removal Adrenalectomy 3 Hysterectomy 2 In-house and postoperative analgesia requirements, convalescence and return to work data are only being reported for procedures with more than 5 cases. an approach that aims at using a natural orifice to perform intra-abdominal procedures, using a combination of laparoscopic and endoscopic techniques. Despite significant interest in NOTES, its application is currently limited to the laboratory. This is primarily due to the lack of versatility and robustness of currently available instrumentation and the concern about the safety and reliability of visceral closure. As a consequence of these limitations, almost all clinical NOTES procedures performed till date has used transabdominal assistance. The LESS 808 UROLOGY 74 (4), 2009
5 Table 4. LESS urologic procedures (N 100): complications and efficacy Procedure Complications Efficacy Simple nephrectomy None Technically, feasible in all cases All cases morcellated and extracted Radical nephrectomy Gonadal vein avulsion in 1 patient that was clipped 1 transvaginal extraction Final pathology: all RCC, margins negative Donor nephrectomy Corneal abrasion Dyskinesia from antiemetics Median warm ischemia: 5.8 min Extraction: umbilicus One graft loss due to intravascular clotting on pod # 1 Partial nephrectomy Bleeding needing angioembolization Final pathology: RCC 4 patients, AML 1, oncocytoma1 Margins negative in all cases Median warm ischemia: Kidney cyst excision None Asymptomatic with unobstructed drainage Nephroureterectomy None Distal ureter management: cystoscopic resection laparoscopic EndoGIA Final pathology: T1, Low grade Pyeloplasty None All patients symptoms free Success rate: 15/16 (93.5%; image FU available for 16/19 patients) Ureteral reimplant None Both patients show unobstructed drainage on follow-up imaging Ileal ureter Simple prostatectomy Transvesical mesh removal Adrenalectomy One patient had anastomotic leak requiring nephrostomy drainage Mortality in a Jehovah s witness from hemorrhage Bleeding requiring suturing (n 1) Bowel injury requiring exploration Postoperative bleeding requiring exploration (n 1) Postoperative bleeding requiring transfusion (n 4) Postoperative UTI (n 1) None Right renal vein injury suture repaired after conversion to multiport laparoscopy. The patient developed renal vein thrombus requiring chronic anticoagulation. Renal vein patent at 3 month follow-up. All 3 patients show unobstructed drainage Bowel anastomosis performed extracorporeally through the r-port by disconnecting the valve Preoperative TRUS prostate size: 98 g Weight of the enucleated adenoma: 59 g 31 patients show unobstructed voiding with improvement in IPSS and peak flow rate. Recurrent stone formation Final pathology: hemorrhagic cyst Hysterectomy None Final pathology: myomas IPSS International Prostate Symptom Score. surgery is an alternative approach to NOTES that shares the same scarless philosophy is to perform laparoscopic surgery through a single skin incision, typically concealed within the umbilicus. The LESS procedure may use purpose-specific single-access ports that allow simultaneous passage of multiple laparoscopic instruments or use of separate standard low-profile trocars inserted through a single skin incision. A variety of terminologies have been used to describe these single-incision procedures. Recently, a consensus meeting supported the term LESS surgery to encompass the spectrum of laparoscopic procedures performed through a single skin incision (Gill et al, unpublished data). Although anecdotal reports of LESS surgery have appeared mainly in the published studies on general surgery and gynecology over the last several years, refinement of access ports, optics, and instrument technology has contributed to the recent surge in interest. 1-4 This technological advance has primarily revolved around development of single-port devices such as the r-port (Advanced Surgical Concepts), UniX System (pnavel Inc.), and articulating instruments such as LaparoAngle (Cambridge Endo, Framington, MA), RealHand (Novare Surgical Systems, Cupertino, CA), and EndoRoticulate (Covidien, Norwalk, CT). The availability of small video-laparoscopes (EndoEYE, Olympus Medical, Japan) with a low external profile and in-line optics and light cables has also facilitated the development of LESS procedures. Since the initial report of LESS nephrectomy by Raman et al 1 (transumbilical, multiple ports) and Rane et al 2 (single-port device, extraumbilical incision), several investigators have demonstrated the technical feasibility UROLOGY 74 (4),
6 Figure 2. (A) External picture of the hardly visible umbilical scar in a patient undergoing LESS simple nephrectomy. The entire procedure including extraction of the morcellated kidney was performed through a 2-cm incision completely concealed within the umbilicus. The contralateral flank scar in the same patient is from a previous spine surgery. (B) External picture of an intact extracted kidney and reconstructed umbilical incision in a patient undergoing LESS radical nephrectomy for a 6-cm central renal tumor. of a variety of urologic procedures. These include advanced reconstructive procedures such as pyeloplasty, ileal interposition, ureteroneocystostomy, 5 and technically challenging procedures such as partial nephrectomy, 6 radical prostatectomy, 7 and donor nephrectomy. 8 Our report details the initial series of 100 consecutive LESS urologic procedures for various indications with very strict patient selection. In the present experience, LESS accounted for only 15% of all laparoscopic upper tract procedures performed at our institute, in the same duration for similar indications. In our opinion, LESS seems ideally suited for upper tract reconstructive procedures such as pyeloplasty and benign ablative indications such as simple nephrectomy. Laparoscopic pyeloplasty is often indicated in the younger patient population in which a good cosmetic result may be an important consideration. Treatment efficacy, in this early experience and relatively short follow-up seems to approach that of standard laparoscopic pyeloplasty. We were also able to deal with factors such as crossing vessels and concomitant renal stones during LESS pyeloplasty. Simple nephrectomy for benign disease is similarly a suitable indication for LESS as these nonfunctioning kidneys are routinely morcellated, thus restricting the skin incision to within the umbilicus, which confers an excellent cosmetic result (Fig. 2). Despite the obvious technical challenges involved in the procurement of a renal allograft in a safe and functionally optimal fashion, the obvious cosmetic advantage and potentially reduced morbidity with LESS surgery may be particularly attractive for the otherwise healthy kidney donor. After developing the technique of LESS donor nephrectomy in 4 patients, we have now expanded our experience to 17 patients. One graft was lost from intravascular clotting on postoperative day 1 after an uncomplicated LESS donor nephrectomy with a warm ischemia time of 3.8 minutes. In the entire LESS donor nephrectomy cohort, our median warm ischemia time was 5.8 minutes, and median total operative time was 240 minutes. On comparing LESS and standard laparoscopic donor nephrectomy, the LESS cohort had a longer median warm ischemia time (3 vs 6 minutes, P.001), a similar hospital stay (3 days each) but decreased analgesic requirements (80 vs 125 mg MSO 4 ; P.27), earlier return to work (17 vs 51 days; P.001) and quicker convalescence (25 vs 97 days; P.03) (Canes et al, unpublished data) Shortterm allograft function following LESS and standard laparoscopic donor nephrectomy was comparable at 1 month (serum creatinine 1.4 vs 1.2 mg/dl; P.4). Although our current experience includes select patients with cancer (N 10), LESS should be used even more selectively in this patient population. This is illustrated as that although our current experience report includes LESS partial nephrectomy (N 6) and LESS radical nephrectomy (N 3), they accounted for 3.3% and 5.5% of the overall laparoscopic partial nephrectomy and laparoscopic radical nephrectomy experience, respectively (Fig. 1). This is in contrast to simple nephrectomy, donor nephrectomy, and pyeloplasty in which LESS procedures accounted for 24%, 33%, and 25% of the procedures, respectively. We have recently published our initial experience with LESS partial nephrectomy in 5 patients with a renal tumor. Median operative time was 270 minutes, estimated blood loss was 150 ml, and warm ischemia time was 20 minutes. One patient had a postoperative bleed requiring angioembolization and all patients had negative surgical margins. The LESS partial nephrectomy at the current time should be reserved for the highly select patient with favorable tumor anatomy and performed by an experienced laparoscopic team. In the current era of nephron-sparing surgery, radical nephrectomy is generally reserved for 810 UROLOGY 74 (4), 2009
7 larger, more complex tumors that generally require a larger extraction incision. Therefore, with the exception of women in whom the en bloc intact specimen can be extracted vaginally, radical nephrectomy may not be as attractive an option for LESS surgery when compared to other upper tract procedures. A novel development made possible by LESS is the ability to perform advanced intraluminal surgical manipulations within a hollow organ, a concept hitherto not feasible. Placement of multiple ports into a hollow organ (bladder, stomach) to perform intraluminal surgery is technically cumbersome. In comparison, intraluminal entry, and secure exit, of a single port into a hollow organ appears more feasible and reliable. The unique design of the r-port allows direct percutaneous insertion of the access port into the bladder, providing an air-tight seal for establishing pneumovesicum. We reported a novel technique of STEP for large-volume BPH. 9 We have now performed the STEP procedure in 32 patients till date, and these data will be reported in a separate communication. We believe this new capability to obtain a reliable airtight single-portal multichannel access into the lumen of a hollow viscus can potentially be extended to select other surgical applications. 10 In the ultimate analysis, for LESS surgery to be more widely adopted, it has to demonstrate patient benefits beyond merely the cosmetic ones. Only 2 initial reports are available on comparison of LESS with standard laparoscopy that show conflicting trends. Early data in a limited number of patients show evidence of decreased morbidity from LESS compared to standard laparoscopic donor nephrectomy. In contrast, Raman et al 11 failed to demonstrate any difference in short-term outcomes of convalescence comparing 11 LESS to 22 standard laparoscopic nephrectomies. Specifically, the authors showed no difference in length of stay, in-house analgesia requirement, or complication rates between the 2 groups. However, the study did not report any data on complete convalescence or return to work. Both studies were retrospective reviews, with only a limited number of patients. We believe that an adequately powered prospective randomized comparison between LESS and standard laparoscopy using tools designed to detect subtle differences in morbidity and assess cosmetic satisfaction will ultimately determine the future of LESS surgery. In this regard, creation of prospective multicenter, procedure-specific registries for various LESS procedures has been identified as a top-priority at the LESS Consortium meeting. Despite gaining experience with several LESS applications, we believe that this approach remains more technically challenging compared with conventional laparoscopy. Although we have successfully performed LESS surgery with a relatively low complication and conversion rate, it is far from being a routine standard of care. In fact, in the present study, LESS accounted for only 15% of overall laparoscopic cases. As such, given that the current benefits of LESS are largely cosmetic, we recommend a very low threshold for conversion to standard laparoscopy. Robotic assistance with the da Vinci Surgical System has been used to perform LESS procedures. 12 We used robotic assistance to perform simple prostatectomy and pyeloplasty. In our opinion, significant instrument clashing and robotic arms are limitations of incorporating the current da Vinci system to routinely perform the LESS procedure. Ongoing refinement of technology, particularly the development of novel platforms specific for LESS surgery, is critical to promote its routine widespread use. In this regard, technologies such as the magnetic anchoring and guidance system (MAGS) 13 and flexible 14 and in-vivo robotics 15 are attractive technologies on the horizon that may help circumvent some of the limitations of current LESS surgery that stem from instrument crowding and relative lack of triangulation. CONCLUSIONS The LESS urologic surgery is feasible for select indications, albeit technically challenging. With proper patient selection, complication and conversion rates are low. Outcomes in the short term appear comparable to conventional laparoscopy as reported in published data. Prospective studies comparing outcomes of LESS surgery with standard laparoscopy will determine the future direction of this approach. References 1. Raman JD, Bensalah K, Bagrodia A, et al. Laboratory and clinical development of single keyhole umbilical nephrectomy. Urology. 2007;70: Rane A, Rao P, Rao P. Laparoscopic-singleport-access nephrectomy and other urologic procedures using a novel single port device (r-port). Urology. 2008;72: Desai MM, Rao PP, Aron M, et al. Scarless single port transumbilical nephrectomy and pyeloplasty: first clinical report. BJU Int. 2008;101: Kaouk JH, Haber GP, Goel RK, et al. Single-port laparoscopic surgery in urology: initial experience. Urology. 2008;71: Desai MM, Rao PP, Stein R, et al. Embryonic natural orifice Transumbilical endoscopic Surgery (E-NOTES) for advanced reconstruction: initial experience. Urology. 2009;73: Aron M, Canes D, Desai MM, et al. Transumbilical single-port laparoscopic partial nephrectomy. BJU Int. 2009;103: Kaouk JH, Goel RK, Haber GP, et al. Single-port laparoscopic radical prostatectomy. Urology. 2008;72: Gill IS, Canes D, Aron M, et al. Single port transumbilical (E- NOTES) donor nephrectomy. J Urol. 2008;180: Desai MM, Aron M, Canes D, et al. Single-port transvesical simple prostatectomy: initial clinical report. Urology. 2008;72: Desai MM, Aron M, Berger A, et al. Transvesical robotic radical prostatectomy. BJU Int. 2008;102: Raman JD, Bagrodia A, Cadeddu JA. Single-incision, umbilical laparoscopic versus conventional laparoscopic nephrectomy: a comparison of perioperative outcomes and short-term measures of convalescence. Eur Urol (in press). 12. Kaouk JH, Goel RK, Haber GP, et al. Robotic single-port transumbilical surgery in humans: initial report. BJU Int. 2009;103: UROLOGY 74 (4),
8 13. Zeltser IS, Bergs R, Fernandez R, et al. Single trocar laparoscopic nephrectomy using magnetic anchoring and guidance system in the porcine model. J Urol. 2007;178: Desai MM, Aron M, Gill IS, et al. Flexible robotic retrograde renoscopy: description of novel robotic device and preliminary laboratory experience. Urology. 2008;72: Rentschler ME, Oleynikov D. Recent in vivo surgical robot and mechanism developments. Surg Endosc. 2007;21: EDITORIAL COMMENT We congratulate the authors for amassing the largest urologic experience with LESS procedures. They certainly demonstrate that this new laparoscopic technique is feasible and applicable to a variety of urologic pathologies. However, trying to interpret the results in this compilation of 13 different LESS surgeries is difficult the tables provided can serve as initial benchmarks for perioperative outcomes. Focusing on the higher volume procedures reported, the LESS transvesical simple prostatectomy appears to be a challenging case requiring further refinement as complications occurred in 25% of cases (most being major complications). Moreover, for LESS nephrectomy (simple or donor), it is feasible and safe, though in my opinion the advantage will remain mainly cosmetic. As such, the authors are correct in that LESS surgery should be employed selectively and comprise a small percentage of a laparoscopic urology practice. In fact, I do not believe that a yet to be determined small advantage in convalescence or cosmesis will justify routine LESS partial nephrectomy and LESS simple or radical prostatectomy. Nevertheless, the urologic community cannot overlook LESS surgery as there is a strong industry and clinical (general surgery) support for developing these procedures. It is only a matter of time before the urologic patient will develop interest in these procedures as well. Having demonstrated feasibility, we now need to investigate outcomes compared to conventional laparoscopy 1,2 to define the appropriate role of LESS surgery. Jeffrey A. Cadeddu, M.D., Department of Urology, UT Southwestern Medical Center, Dallas, Texas References 1. Zeltser IS, Bergs R, Fernandez R, et al. Single trocar laparoscopic nephrectomy using magnetic anchoring and guidance system in the porcine model. J Urol. 2007;178: Desai MM, Aron M, Gill IS, et al. Flexible robotic retrograde renoscopy: description of novel robotic device and preliminary laboratory experience. Urology. 2008;72: doi: /j.urology UROLOGY 74: 812, Elsevier Inc. EDITORIAL COMMENT We applaud the authors for their work in assessing the applicability of laparoendoscopic single-site surgery (LESS). This approach is a more practical alternative to pure natural orifice transluminal endoscopic surgery (NOTES). Several previous studies have demonstrated the feasibility of LESS in urology, for both extirpative and reconstructive surgeries. 1,2 The current series reviews to a considerable extent the safety and reproducibility of this technique. It should be pointed out, however, that in a significant proportion of these cases, the surgery described was not true single-site surgery. The authors note that all reconstructive cases (including partial nephrectomy, pyeloplasty, etc.) involved the use of an additional 2-mm trocar with accompanying instruments to complete these procedures. The use of an additional trocar, regardless of size, was needed to overcome the hurdles of retraction, triangulation, and instrument clashing. The morbidity and cosmetic effect of the additional small incision can be debated, and may be trivial, but in our view is not necessary even for reconstructive LESS procedures. 3 Is LESS a temporary stepping stone on the path to a truly scarless intervention, or is it a meaningful and lasting technique? Is it chicanery or progress? Because the internal procedure is the same as standard laparoscopy, removing and minimizing trocar sites may not have a huge effect on recovery. Indeed, previous needlescopic approaches that promised similar advantages did not progress in clinical practice. 4 In a large part, this was because of the high level of technical expertise necessary to offer this approach. Developments in instrumentation will simplify LESS and lead to wider diffusion, or a quantum leap forward in another direction will render LESS obsolete. Regardless of the role of LESS in the surgical armamentarium of the future, we embrace and validate the underlying principle that is driving this development. The modern surgeon must strive to address improved cosmesis, postoperative pain, hospital stay, and recovery time while achieving to cure patients. Lee Richstone, M.D., and Louis Kavoussi, M.D., Smith Institute for Urology, Hofstra School of Medicine, The North Shore-Long Island Jewish Health System, Long Island, NY References 1. Desai MM, Rao PP, Aron M, et al. Scarless single port transumbilical nephrectomy and pyeloplasty: first clinical report. BJU Int. 2008; 101: Raman JD, Bagrodia A, Cadeddu JA. Single-incision, umbilical laparoscopic versus conventional laparoscopic nephrectomy: a comparison of perioperative outcomes and Short-Term measures of convalescence. Eur Urol. 2008;55: Rais-Bahrami S, Montag S, Atalla M, et al. Laparoendoscopic single-site Surgery (LESS) of the kidney with no accessory trocars: an initial experience. J Endourol. 2009;23: Gill IS, Soble JJ, Sung GT, et al. Needlescopic adrenalectomy the initial series: comparison with conventional laparoscopic adrenalectomy. Urology. 1998;52: doi: /j.urology UROLOGY 74: 812, Elsevier Inc. REPLY We thank Richstone and Kavoussi for their sage comments. Clearly, the use of an adjunctive 2-mm needle-port is not always necessary, nor do we use it as such. However, in reconstructive cases, it offers a ready, morbidity-free solution to allow 812 UROLOGY 74 (4), 2009
Laparo-endoscopic single site surgery in pediatrics: Feasibility and surgical outcomes from a preliminary prospective Canadian experience
 Original research Laparo-endoscopic single site surgery in pediatrics: Feasibility and surgical outcomes from a preliminary prospective Canadian experience Aziz Khambati, MD; Elias Wehbi, MD; Walid A.
Original research Laparo-endoscopic single site surgery in pediatrics: Feasibility and surgical outcomes from a preliminary prospective Canadian experience Aziz Khambati, MD; Elias Wehbi, MD; Walid A.
Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports
 Volume 2011, Article ID 651380, 4 pages doi:10.1155/2011/651380 Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports Yasuhiro
Volume 2011, Article ID 651380, 4 pages doi:10.1155/2011/651380 Case Report Left Transperitoneal Adrenalectomy with a Laparoendoscopic Single-Site Surgery Combined Technique: Initial Case Reports Yasuhiro
Surgery without incisions; experiences in single incision laparoscopic surgery (SILS) for infants and children
 Surgery without incisions; experiences in single incision laparoscopic (SILS) for infants and children Single-incision laparoscopic is minimal access with only one small incision result in very small scar
Surgery without incisions; experiences in single incision laparoscopic (SILS) for infants and children Single-incision laparoscopic is minimal access with only one small incision result in very small scar
european urology 55 (2009)
 european urology 55 (2009) 1198 1206 available at www.sciencedirect.com journal homepage: www.europeanurology.com Endo-urology Single-Incision, Umbilical Laparoscopic versus Conventional Laparoscopic Nephrectomy:
european urology 55 (2009) 1198 1206 available at www.sciencedirect.com journal homepage: www.europeanurology.com Endo-urology Single-Incision, Umbilical Laparoscopic versus Conventional Laparoscopic Nephrectomy:
Laparoendoscopic Pfannenstiel Nephrectomy using Conventional Laparoscopic Instruments - Preliminary Experience
 Surgical Technique Laparoendoscopic Pfannenstiel Nephrectomy International Braz J Urol Vol. 36 (6): 718-723, November - December, 2010 doi: 10.1590/S1677-55382010000600010 Laparoendoscopic Pfannenstiel
Surgical Technique Laparoendoscopic Pfannenstiel Nephrectomy International Braz J Urol Vol. 36 (6): 718-723, November - December, 2010 doi: 10.1590/S1677-55382010000600010 Laparoendoscopic Pfannenstiel
Technique of Laparoscopic-Endoscopic Single-Site Surgery Radical Nephrectomy
 EUROPEAN UROLOGY 56 (2009) 644 650 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Technique of Laparoscopic-Endoscopic Single-Site Surgery Radical Nephrectomy
EUROPEAN UROLOGY 56 (2009) 644 650 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Technique of Laparoscopic-Endoscopic Single-Site Surgery Radical Nephrectomy
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments
 Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Laparoendoscopic Single-Site Nephrectomy Using Standard Laparoscopic Instruments Our Initial Experience LAPAROSCOPIC UROLOGY Alireza Aminsharifi, Bahman Goshtasbi, Firoozeh Afsar Department of Urology,
Original Article A novel approach to locate renal artery during retroperitoneal laparoendoscopic single-site radical nephrectomy
 Int J Clin Exp Med 2014;7(7):1752-1756 www.ijcem.com /ISSN:1940-5901/IJCEM0000870 Original Article during radical nephrectomy Lixin Shi, Wei Cai, Juan Dong, Jiangping Gao, Hongzhao Li, Shengkun Sun, Qiang
Int J Clin Exp Med 2014;7(7):1752-1756 www.ijcem.com /ISSN:1940-5901/IJCEM0000870 Original Article during radical nephrectomy Lixin Shi, Wei Cai, Juan Dong, Jiangping Gao, Hongzhao Li, Shengkun Sun, Qiang
Laparoendoscopic Single-Site Nephrectomy Using a Modified Umbilical Incision and a Home-Made Transumbilical Port
 Original Article DOI 10.3349/ymj.2011.52.2.307 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(2):307-313, 2011 Laparoendoscopic Single-Site Nephrectomy Using a Modified Umbilical Incision and a Home-Made
Original Article DOI 10.3349/ymj.2011.52.2.307 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(2):307-313, 2011 Laparoendoscopic Single-Site Nephrectomy Using a Modified Umbilical Incision and a Home-Made
Laparoscopic Surgery. The Da Vinci Robot. Limits of Laparoscopy. What Robotics Offers. Robotic Urologic Surgery: A New Era in Patient Care
 Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Robotic Surgery for Upper Tract Urothelial Carcinoma. Li-Ming Su, MD
 Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
PREFACE... V. CONTRIBUTORS... xiii. 1. SURGICAL INCISIONS... 3 J. Stephen Jones
 Contents PREFACE... V CONTRIBUTORS... xiii PART I: THE KIDNEY AND ADRENAL 1. SURGICAL INCISIONS... 3 2. ADRENAL DISEASE: OPEN SURGERY... 17 3. LAPAROSCOPIC ADRENALECTOMY... 23 Mihir M. Desai and Inderbir
Contents PREFACE... V CONTRIBUTORS... xiii PART I: THE KIDNEY AND ADRENAL 1. SURGICAL INCISIONS... 3 2. ADRENAL DISEASE: OPEN SURGERY... 17 3. LAPAROSCOPIC ADRENALECTOMY... 23 Mihir M. Desai and Inderbir
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
Patient-Reported Body Image and Cosmesis Outcomes Following Kidney Surgery: Comparison of Laparoendoscopic Single-Site, Laparoscopic, and Open Surgery
 EUROPEAN UROLOGY 60 (2011) 1097 1104 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Patient-Reported Body Image and Cosmesis Outcomes Following Kidney Surgery:
EUROPEAN UROLOGY 60 (2011) 1097 1104 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Patient-Reported Body Image and Cosmesis Outcomes Following Kidney Surgery:
Early Experience of Laparoendoscopic Single-Site Nephroureterectomy for Upper Urinary Tract Tumors
 www.kjurology.org DOI:10.4111/kju.2010.51.7.472 Robotics/Laparoscopy Early Experience of Laparoendoscopic Single-Site Nephroureterectomy for Upper Urinary Tract Tumors Ill Young Seo, Hye Min Hong, Il Sang
www.kjurology.org DOI:10.4111/kju.2010.51.7.472 Robotics/Laparoscopy Early Experience of Laparoendoscopic Single-Site Nephroureterectomy for Upper Urinary Tract Tumors Ill Young Seo, Hye Min Hong, Il Sang
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condition: Urinary Tract Obstruction Your urinary system produces, stores, and eliminates urine. It includes
Shape the Future of Urological Surgery
 Shape the Future of Urological Surgery THE ROLE OF LAPAROSCOPIC SURGERY IN NEW MILENNIUM Victor Chia-Hsiang Lin, MD Division of Urology, Department of Surgery Chi-Mei Medical Center MY TALK TODAY IS Minimal
Shape the Future of Urological Surgery THE ROLE OF LAPAROSCOPIC SURGERY IN NEW MILENNIUM Victor Chia-Hsiang Lin, MD Division of Urology, Department of Surgery Chi-Mei Medical Center MY TALK TODAY IS Minimal
Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA
 1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
1 Oncourology COMPLICATIONS OF PARTIAL NEPHRECTOMY AT OPERATIVE TREATMENT OF RENAL CELL CARCINOMA Address: Eduard Oleksandrovych Stakhovsky, 03022, Kyiv, Lomonosova Str., 33/43, National Cancer Institute
Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic Single-Site (R-LESS) Pyeloplasty Using a New Single-Port Platform
 EUROPEAN UROLOGY 62 (2012) 175 179 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic
EUROPEAN UROLOGY 62 (2012) 175 179 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Feasibility and Preliminary Clinical Outcomes of Robotic Laparoendoscopic
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Retroperitoneal LESS Donor Nephrectomy
 Surgical Technique Retroperitoneal LESS Donor Nephrectomy International Braz J Urol Vol. 36 (5): 602-608, September - October, 2010 doi: 10.1590/S1677-55382010000500010 Retroperitoneal LESS Donor Nephrectomy
Surgical Technique Retroperitoneal LESS Donor Nephrectomy International Braz J Urol Vol. 36 (5): 602-608, September - October, 2010 doi: 10.1590/S1677-55382010000500010 Retroperitoneal LESS Donor Nephrectomy
Identifying unrecognized collecting system entry and the integrity of repair during open partial nephrectomy: comparison of two techniques
 ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
ORIGINAL ARTICLE Vol. 40 (5): 637-643, September - October, 2014 doi: 10.1590/S1677-5538.IBJU.2014.05.08 Identifying unrecognized collecting system entry and the integrity of repair during open partial
da Vinci Prostatectomy
 da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
From laparoscopic to robo.c surgical urology 2 years of experience
 From laparoscopic to robo.c surgical urology 2 years of experience Ass. Professor V. Poulakis MD, PhD, FEBU Director of Urological Clinic Athens Medical Center Doctors Hospital Athens Laparoscopy golden
From laparoscopic to robo.c surgical urology 2 years of experience Ass. Professor V. Poulakis MD, PhD, FEBU Director of Urological Clinic Athens Medical Center Doctors Hospital Athens Laparoscopy golden
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Urologic Surgical Complications In Renal Transplantation
 Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Urologic Surgical Complications In Renal Transplantation Chris Freise, MD Professor of Surgery UCSF Transplant Division Urologic Complications Review of Bladder Anastomosis Complications and Management
Laparoscopic Radical Nephrectomy- the current gold standard
 Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Laparoscopic Radical Nephrectomy- the current gold standard Anoop M. Meraney, M.D Director, Urologic Oncology, Helen and Harry Gray Cancer Center, Hartford Hospital and Connecticut Surgical Group. Is it
Facing Surgery. for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery
 Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condit ion: Urinary Tract Obstruction Your urinary system consists of two kidneys, two ureters and the
Facing Surgery for a Urinary Tract Condition? Learn about minimally invasive da Vinci Surgery The Condit ion: Urinary Tract Obstruction Your urinary system consists of two kidneys, two ureters and the
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
SINGLE INCISION LAPAROSCOPIC SURGERY
 SINGLE INCISION LAPAROSCOPIC SURGERY DR ADEWALE ADISA CONSULTANT MINIMAL ACCESS SURGEON & SENIOR LECTURER DEPARTMENT OF SURGERY, OBAFEMI AWOLOWO UNIVERSITY, & OBAFEMI AWOLOWO UNIVERSITY TEACHING HOSPITALS
SINGLE INCISION LAPAROSCOPIC SURGERY DR ADEWALE ADISA CONSULTANT MINIMAL ACCESS SURGEON & SENIOR LECTURER DEPARTMENT OF SURGERY, OBAFEMI AWOLOWO UNIVERSITY, & OBAFEMI AWOLOWO UNIVERSITY TEACHING HOSPITALS
RAPN. in T1b Renal Masses? A. Mottrie. G. Denaeyer, P. Schatteman, G. Novara
 RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor Thrombectomy
 EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
EUROPEAN UROLOGY 59 (2011) 652 656 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Series of the Month Initial Series of Robotic Radical Nephrectomy with Vena Caval Tumor
THE LATEST STEP FORWARD IN SURGERY. LESS Laparo-Endoscopic Single-Site Surgery
 THE LATEST STEP FORWARD IN SURGERY LESS Laparo-Endoscopic Single-Site Surgery THE ROUTE FROM OPEN SURGERY TO MINIMALLY INVASIVE SURGERY An operation is generally a radical experience for any patient. In
THE LATEST STEP FORWARD IN SURGERY LESS Laparo-Endoscopic Single-Site Surgery THE ROUTE FROM OPEN SURGERY TO MINIMALLY INVASIVE SURGERY An operation is generally a radical experience for any patient. In
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation 3D HD Vision 3D HD visualization facilitates accurate
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 8 ISSUE 1 Single Incision Laparoscopic Colectomy: A Series of Five Patients, Lessons Learned Elyssa Feinberg David O Connor Diego Camacho
World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 8 ISSUE 1 Single Incision Laparoscopic Colectomy: A Series of Five Patients, Lessons Learned Elyssa Feinberg David O Connor Diego Camacho
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches
 Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
LAPAROSCOPIC RADICAL NEPHRECTOMY FOR LARGE (GREATER THAN 7 CM, T2) RENAL TUMORS
 0022-5347/04/1726-2172/0 Vol. 172, 2172 2176, December 2004 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2004 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000140961.53335.04 LAPAROSCOPIC
0022-5347/04/1726-2172/0 Vol. 172, 2172 2176, December 2004 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2004 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000140961.53335.04 LAPAROSCOPIC
Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for Unroofing of Hepatic Cysts
 SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
Laparoendoscopic Single-Site Upper Urinary Tract Surgery: Assessment of Postoperative Complications and Analysis of Risk Factors
 EUROPEAN UROLOGY 61 (2012) 510 516 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Urothelial Cancer Editorial by Jonathan A. Coleman on pp. 517 518 of this
EUROPEAN UROLOGY 61 (2012) 510 516 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Urothelial Cancer Editorial by Jonathan A. Coleman on pp. 517 518 of this
Current status and future perspectives in laparoendoscopic single-site and natural orifice transluminal endoscopic urological surgery
 410..431 International Journal of Urology (2010) 17, 410 431 doi: 10.1111/j.1442-2042.2010.02497.x Review Articleiju_2497 Current status and future perspectives in laparoendoscopic single-site and natural
410..431 International Journal of Urology (2010) 17, 410 431 doi: 10.1111/j.1442-2042.2010.02497.x Review Articleiju_2497 Current status and future perspectives in laparoendoscopic single-site and natural
The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe Kidneys
 Thomas Jefferson University Jefferson Digital Commons Department of Urology Faculty Papers Department of Urology 1-25-2011 The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe
Thomas Jefferson University Jefferson Digital Commons Department of Urology Faculty Papers Department of Urology 1-25-2011 The Minimally Invasive Management of Ureteropelvic Junction Obstruction in Horseshoe
The benefits of minimally invasive
 Surgical techniques Applying single-incision laparoscopic surgery to gyn practice: What s involved New instrumentation and strategies have alleviated some of the challenges of performing laparoscopy through
Surgical techniques Applying single-incision laparoscopic surgery to gyn practice: What s involved New instrumentation and strategies have alleviated some of the challenges of performing laparoscopy through
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Minimally Invasive Surgery Minimised. Primary-care physicians guide to single-incision laparoscopic surgery
 Minimally Invasive Surgery Minimised Primary-care physicians guide to single-incision laparoscopic surgery The single-incision laparoscopic technique: The latest evolution in minimally invasive surgery
Minimally Invasive Surgery Minimised Primary-care physicians guide to single-incision laparoscopic surgery The single-incision laparoscopic technique: The latest evolution in minimally invasive surgery
Arieh L. Shalhav Is There a Risk in Robotic Nephroureterectomy?
 Arieh L. Shalhav Is There a Risk in Robotic Nephroureterectomy? 80 patients LNU (n = 40) or ONU (n = 40) CSS (p = 0.2), BRFS (p = 0.86), MFS (p = 0.12) similar for the entire cohort Subgroups of pt3 UTUC
Arieh L. Shalhav Is There a Risk in Robotic Nephroureterectomy? 80 patients LNU (n = 40) or ONU (n = 40) CSS (p = 0.2), BRFS (p = 0.86), MFS (p = 0.12) similar for the entire cohort Subgroups of pt3 UTUC
Laparoscopic Nephrectomy: New Standard of Care?
 Original Article Laparoscopic Nephrectomy: New Standard of Care? Hong Gee Sim, Sidney K.H. Yip, Chee Yong Ng, Yee Sze Teo, Yeh Hong Tan, Woei Yun Siow and Wai Sam Cheng, Department of Urology, Singapore
Original Article Laparoscopic Nephrectomy: New Standard of Care? Hong Gee Sim, Sidney K.H. Yip, Chee Yong Ng, Yee Sze Teo, Yeh Hong Tan, Woei Yun Siow and Wai Sam Cheng, Department of Urology, Singapore
Robot-assisted kidney transplantation pilot study
 Robot-assisted kidney transplantation pilot study This leaflet explains more about a new technique called robot-assisted kidney transplantation. This is a pilot study - this means that we are offering
Robot-assisted kidney transplantation pilot study This leaflet explains more about a new technique called robot-assisted kidney transplantation. This is a pilot study - this means that we are offering
Robotic Technology at the Service of Surgery
 Robotic Technology at the Service of Surgery -The Challenge of Robotic Urology - Vassilis Poulakis MD, PhD, FEBU Ass. Professor of Urology, University of Frankfurt, Germany Director of Urologic Clinic
Robotic Technology at the Service of Surgery -The Challenge of Robotic Urology - Vassilis Poulakis MD, PhD, FEBU Ass. Professor of Urology, University of Frankfurt, Germany Director of Urologic Clinic
ROBOTIC PRECISION. HUMAN COMPASSION.
 ROBOTIC PRECISION. HUMAN COMPASSION. Find out how robotic surgery can help you. Find a surgeon, attend a class, or learn more at adena.org/robot or by calling 877-779-7585. ADENA S NEW DA VINCI SI ROBOTIC
ROBOTIC PRECISION. HUMAN COMPASSION. Find out how robotic surgery can help you. Find a surgeon, attend a class, or learn more at adena.org/robot or by calling 877-779-7585. ADENA S NEW DA VINCI SI ROBOTIC
The 6-month course of the program is mainly dedicated to clinical experience (research time is also provided).
 Oncology Fellowship The oncology fellowship training course at Yonsei University Health System (Severance Hospital), comprising a 6-month and 1-year format, provides good quality and wide experience in
Oncology Fellowship The oncology fellowship training course at Yonsei University Health System (Severance Hospital), comprising a 6-month and 1-year format, provides good quality and wide experience in
Single-Port Laparoscopic Supracervical Hysterectomy with Transumbilical Morcellation
 Single-Port Laparoscopic Supracervical Hysterectomy with Transumbilical Morcellation Anton Langebrekke, MD, Ioannis Koutoukos, MD, PhD and Erik Qvigstad, MD, PhD From the Department of Obstetrics and Gynaecology,
Single-Port Laparoscopic Supracervical Hysterectomy with Transumbilical Morcellation Anton Langebrekke, MD, Ioannis Koutoukos, MD, PhD and Erik Qvigstad, MD, PhD From the Department of Obstetrics and Gynaecology,
GENERAL GOALS & OBJECTIVES U-1. U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES
 GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
Research Article Transvesicoscopic Repair of Vesicovaginal Fistula
 Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
Diagnostic and Therapeutic Endoscopy Volume 2010, Article ID 760348, 4 pages doi:10.1155/2010/760348 Research Article Transvesicoscopic Repair of Vesicovaginal Fistula R. B. Nerli and Mallikarjun Reddy
Complications in robotic surgery!! Review of the literature! RALP, RAPN and RARC!
 Complications in robotic surgery Review of the literature RALP, RAPN and RARC Anna Wallerstedt, MD Karolinska University Hospital Stockholm, Sweden Agenda The importance of reporting surgical complications
Complications in robotic surgery Review of the literature RALP, RAPN and RARC Anna Wallerstedt, MD Karolinska University Hospital Stockholm, Sweden Agenda The importance of reporting surgical complications
BJUI. Robotic nephrectomy for the treatment of benign and malignant disease
 . JOURNAL COMPILATION 2008 BJU INTERNATIONAL Laparoscopic and Robotic Urology ROGERS et al. BJUI BJU INTERNATIONAL Robotic nephrectomy for the treatment of benign and malignant disease Craig Rogers, Rajesh
. JOURNAL COMPILATION 2008 BJU INTERNATIONAL Laparoscopic and Robotic Urology ROGERS et al. BJUI BJU INTERNATIONAL Robotic nephrectomy for the treatment of benign and malignant disease Craig Rogers, Rajesh
Goals & Objectives by Year in Training: U-1
 Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
Minimally invasive surgery in urology oncology. Dr. Tongchai Nakamont 23 Jan 2014
 Minimally invasive surgery in urology oncology Dr. Tongchai Nakamont 23 Jan 2014 Urology oncology Renal cell carcinoma ( RCC) Transitional cell carcinoma (TCC) Kidney Ureter Bladder Prostate cancer Urological
Minimally invasive surgery in urology oncology Dr. Tongchai Nakamont 23 Jan 2014 Urology oncology Renal cell carcinoma ( RCC) Transitional cell carcinoma (TCC) Kidney Ureter Bladder Prostate cancer Urological
Robot-assisted partial nephrectomy: Evaluation of learning curve for an experienced renal surgeon
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2010 Robot-assisted partial nephrectomy: Evaluation of learning curve for an experienced renal surgeon Mohammed
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2010 Robot-assisted partial nephrectomy: Evaluation of learning curve for an experienced renal surgeon Mohammed
Videoforum Videosurgery
 Videoforum Videosurgery Laparoscopic nephroureterectomy with transvesical single-port distal ureter and bladder cuff dissection: points of technique and initial surgical outcomes with five patients Marek
Videoforum Videosurgery Laparoscopic nephroureterectomy with transvesical single-port distal ureter and bladder cuff dissection: points of technique and initial surgical outcomes with five patients Marek
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE. Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham
 SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
Laparoendoscopic Single-Site Radical Nephrectomy for Renal Cancer: Technique and Surgical Outcomes
 EUROPEAN UROLOGY 62 (2012) 168 174 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Laparoendoscopic Single-Site Radical Nephrectomy for Renal Cancer: Technique
EUROPEAN UROLOGY 62 (2012) 168 174 available at www.sciencedirect.com journal homepage: www.europeanurology.com Surgery in Motion Laparoendoscopic Single-Site Radical Nephrectomy for Renal Cancer: Technique
Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit Urinary Diversion
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
available at www.sciencedirect.com journal homepage: www.europeanurology.com Case Study of the Month Retroperitoneoscopic Transureteroureterostomy with Cutaneous Ureterostomy to Salvage Failed Ileal Conduit
SINGLE INCISION ENDOSCOPIC SURGERY (SIES)
 EAES CONSENSUS CONFERENCE SINGLE INCISION ENDOSCOPIC SURGERY (SIES) STATEMENTS AND RECOMMENDATIONS EAES appreciates your input! Please give your opinion on the below statements and recommendations of the
EAES CONSENSUS CONFERENCE SINGLE INCISION ENDOSCOPIC SURGERY (SIES) STATEMENTS AND RECOMMENDATIONS EAES appreciates your input! Please give your opinion on the below statements and recommendations of the
Contents SECTION I: ESSENTIALS OF LAPAROSCOPY. Chapter 1: Chronological advances in Minimal Access Surgery
 Contents SECTION I: ESSENTIALS OF LAPAROSCOPY Chapter 1: Chronological advances in Minimal Access Surgery Chapter 2: Laparoscopic Equipments a. Laparoscopic Trolley b. Light cable c. Light source d. Telescope
Contents SECTION I: ESSENTIALS OF LAPAROSCOPY Chapter 1: Chronological advances in Minimal Access Surgery Chapter 2: Laparoscopic Equipments a. Laparoscopic Trolley b. Light cable c. Light source d. Telescope
Setting Department of Gynecology and Obstetrics, Cleveland Clinic Foundation (tertiary care academic centre), USA.
 Prospective randomized clinical trial of laparoscopically assisted vaginal hysterectomy versus total abdominal hysterectomy Falcone T, Paraiso M F, Mascha E Record Status This is a critical abstract of
Prospective randomized clinical trial of laparoscopically assisted vaginal hysterectomy versus total abdominal hysterectomy Falcone T, Paraiso M F, Mascha E Record Status This is a critical abstract of
Transumbilical Single-Port Surgery: Evolution and Current Status
 european urology 54 (2008) 1020 1030 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review Laparoscopy Transumbilical Single-Port Surgery: Evolution and Current Status David
european urology 54 (2008) 1020 1030 available at www.sciencedirect.com journal homepage: www.europeanurology.com Review Laparoscopy Transumbilical Single-Port Surgery: Evolution and Current Status David
Pancreatic pseudocysts (PP) are chronic collections of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 9, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2009.0421 Hand-Sewn Cystogastrostomy Using the Novel Single-Incision Laparoscopy
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 9, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2009.0421 Hand-Sewn Cystogastrostomy Using the Novel Single-Incision Laparoscopy
Facing Gynecologic Surgery?
 Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
Feasibility of Laparoendoscopic Single-Site Partial Nephrectomy in a Porcine Model
 www.kjurology.org DOI:10.4111/kju.2011.52.1.44 Endourology/Urolithiasis Feasibility of Laparoendoscopic Single-Site Partial Nephrectomy in a Porcine Model Dong-Hun Koo, Yong Hyun Park, Chang Wook Jeong
www.kjurology.org DOI:10.4111/kju.2011.52.1.44 Endourology/Urolithiasis Feasibility of Laparoendoscopic Single-Site Partial Nephrectomy in a Porcine Model Dong-Hun Koo, Yong Hyun Park, Chang Wook Jeong
Outcomes. Glickman Urological & Kidney Institute
 Outcomes 28 Glickman Urological & Kidney Institute Prostate Cryotherapy Cryotherapy has recently been used for treatment of prostate cancer as primary treatment and after failure of radiation treatment.
Outcomes 28 Glickman Urological & Kidney Institute Prostate Cryotherapy Cryotherapy has recently been used for treatment of prostate cancer as primary treatment and after failure of radiation treatment.
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic partial nephrectomy 308 Introduction This overview has been
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of laparoscopic partial nephrectomy 308 Introduction This overview has been
LAPAROSCOPIC NEPHRON-SPARING SURGERY IN THE PRESENCE OF RENAL ARTERY DISEASE
 SURGICAL TECHNIQUES IN UROLOGY LAPAROSCOPIC NEPHRON-SPARING SURGERY IN THE PRESENCE OF RENAL ARTERY DISEASE ANDREW P. STEINBERG, SIDNEY C. ABREU, MIHIR M. DESAI, ANUP P. RAMANI, JIHAD H. KAOUK, AND INDERBIR
SURGICAL TECHNIQUES IN UROLOGY LAPAROSCOPIC NEPHRON-SPARING SURGERY IN THE PRESENCE OF RENAL ARTERY DISEASE ANDREW P. STEINBERG, SIDNEY C. ABREU, MIHIR M. DESAI, ANUP P. RAMANI, JIHAD H. KAOUK, AND INDERBIR
DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT OF URETERAL STENT: SIMPLIFICATION OF THE TECHNIQUE
 Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Take Home Messages A. Najmaldin - H. Reusens
 Take Home Messages A. Najmaldin - H. Reusens - In complicated appendicitis (localized or diffuse peritonitis): don t be afraid to use an (expensive) stapler, if available less postop abscesses, ileus,
Take Home Messages A. Najmaldin - H. Reusens - In complicated appendicitis (localized or diffuse peritonitis): don t be afraid to use an (expensive) stapler, if available less postop abscesses, ileus,
Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors
 Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors Kyung Hwa Choi, Cheol Kyu Oh, Wooju Jeong, Enrique Ian S. Lorenzo, Woong Kyu Han, Koon Ho Rha From
Initial Clinical Experience with Robot-Assisted Laparoscopic Partial Nephrectomy for Complex Renal Tumors Kyung Hwa Choi, Cheol Kyu Oh, Wooju Jeong, Enrique Ian S. Lorenzo, Woong Kyu Han, Koon Ho Rha From
Laparoscopic Radical Nephrectomy for Renal Masses 7 Centimeters or Larger
 SCIENTIFIC PAPER Laparoscopic Radical Nephrectomy for Renal Masses 7 Centimeters or Larger James S. Rosoff, MD, Jay D. Raman, MD, R. Ernest Sosa, MD, Joseph J. Del Pizzo, MD ABSTRACT Objective: To report
SCIENTIFIC PAPER Laparoscopic Radical Nephrectomy for Renal Masses 7 Centimeters or Larger James S. Rosoff, MD, Jay D. Raman, MD, R. Ernest Sosa, MD, Joseph J. Del Pizzo, MD ABSTRACT Objective: To report
PRACTICAL Urology. USC Institute of Urology 4 th Annual Conference: Guest Faculty. Thursday January 31, January 31, February 1 2, 2019
 USC Institute of Urology 4 th Annual Conference: PRACTICAL Urology January 31, February 1 2, 2019 Guest Faculty Jeffrey Cadeddu, MD University of Texas Southwestern University of Michigan University of
USC Institute of Urology 4 th Annual Conference: PRACTICAL Urology January 31, February 1 2, 2019 Guest Faculty Jeffrey Cadeddu, MD University of Texas Southwestern University of Michigan University of
Financial and Other Disclosures
 Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Critical Analysis of Laparoscopic Donor Nephrectomy in the Setting of Complex Renal Vasculature: Initial Experience and Intermediate Outcomes
 JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 451 455 DOI: 10.1089=end.2008.0242 Critical Analysis of Laparoscopic Donor Nephrectomy in the Setting of Complex Renal
JOURNAL OF ENDOUROLOGY Volume 23, Number 3, March 2009 ª Mary Ann Liebert, Inc. Pp. 451 455 DOI: 10.1089=end.2008.0242 Critical Analysis of Laparoscopic Donor Nephrectomy in the Setting of Complex Renal
Pure transumbilical approach for oncologic surgeries of the male pelvis is now closer to become a reality
 Editorial Pure transumbilical approach for oncologic surgeries of the male pelvis is now closer to become a reality Cristina Esquinas, Javier C. Angulo Clinical Department, Universidad Europea de Madrid,
Editorial Pure transumbilical approach for oncologic surgeries of the male pelvis is now closer to become a reality Cristina Esquinas, Javier C. Angulo Clinical Department, Universidad Europea de Madrid,
LAPAROSCOPIC RADICAL PROSTATECTOMY IN THE ERA OF ROBOT-ASSISTED TECHNOLOGY
 LAPAROSCOPIC RADICAL PROSTATECTOMY IN THE ERA OF ROBOT-ASSISTED TECHNOLOGY *Iason Kyriazis, 1 Marinos Vasilas, 1 Panagiotis Kallidonis, 2 Vasilis Panagopoulos, 1 Evangelos Liatsikos 3 1. Resident in Urology,
LAPAROSCOPIC RADICAL PROSTATECTOMY IN THE ERA OF ROBOT-ASSISTED TECHNOLOGY *Iason Kyriazis, 1 Marinos Vasilas, 1 Panagiotis Kallidonis, 2 Vasilis Panagopoulos, 1 Evangelos Liatsikos 3 1. Resident in Urology,
First Transumbilical Transabdominal Preperitoneal Inguinal Hernia Repair in the Middle East
 ISPUB.COM The Internet Journal of Surgery Volume 25 Number 1 First Transumbilical Transabdominal Preperitoneal Inguinal Hernia Repair in the Middle East A Al-Dowais Citation A Al-Dowais. First Transumbilical
ISPUB.COM The Internet Journal of Surgery Volume 25 Number 1 First Transumbilical Transabdominal Preperitoneal Inguinal Hernia Repair in the Middle East A Al-Dowais Citation A Al-Dowais. First Transumbilical
Gregory Eads MD Women s Centre for Well Being
 Gregory Eads MD Women s Centre for Well Being 1 Program Gynecologic Conditions Surgical Options da Vinci Gynecologic Surgery da Vinci Hysterectomy da Vinci Hysterectomy for Cancer da Vinci Myomectomy (fibroids)
Gregory Eads MD Women s Centre for Well Being 1 Program Gynecologic Conditions Surgical Options da Vinci Gynecologic Surgery da Vinci Hysterectomy da Vinci Hysterectomy for Cancer da Vinci Myomectomy (fibroids)
An analysis of the impact of previous laparoscopic hysterectomy experience on the learning curve for robotic hysterectomy
 J Robotic Surg (2013) 7:295 299 DOI 10.1007/s11701-012-0388-6 ORIGINAL ARTICLE An analysis of the impact of previous laparoscopic hysterectomy experience on the learning curve for robotic hysterectomy
J Robotic Surg (2013) 7:295 299 DOI 10.1007/s11701-012-0388-6 ORIGINAL ARTICLE An analysis of the impact of previous laparoscopic hysterectomy experience on the learning curve for robotic hysterectomy
Clinical Study Single-Port Access Laparoscopy-Assisted Vaginal Hysterectomy: Our Initial Experiences with 100 Cases
 Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2012, Article ID 543627, 5 pages doi:10.1155/2012/543627 Clinical Study Single-Port Access Laparoscopy-Assisted Vaginal Hysterectomy: Our
Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2012, Article ID 543627, 5 pages doi:10.1155/2012/543627 Clinical Study Single-Port Access Laparoscopy-Assisted Vaginal Hysterectomy: Our
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Challenges in RCC surgery. Treatment Goals. Surgical challenges. Management options in VHL associated RCCs
 Management options in VHL associated RCCs Challenges in RCC surgery JJ PATARD, MD, PhD Paris XI University Observation, Radical nephrectomy, Renal parenchymal sparing surgery, Open, laparoscopic, robotic
Management options in VHL associated RCCs Challenges in RCC surgery JJ PATARD, MD, PhD Paris XI University Observation, Radical nephrectomy, Renal parenchymal sparing surgery, Open, laparoscopic, robotic
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET
 LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
LAPAROSCOPIC PYELOPLASTY INFORMATION LEAFLET Laparoscopic Pyeloplasty Page 1 of 8 LAPAROSCOPIC PYELOPLASTY This leaflet has been written to answers questions that you may have about your operation. If
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh)
 A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
Single-stage laparoscopic surgery for bilateral organ tumors using a transumbilical approach with a zigzag incision: a report of two cases
 Kato et al. BMC Urology (2018) 18:28 https://doi.org/10.1186/s12894-018-0343-6 CASE REPORT Single-stage laparoscopic surgery for bilateral organ tumors using a transumbilical approach with a zigzag incision:
Kato et al. BMC Urology (2018) 18:28 https://doi.org/10.1186/s12894-018-0343-6 CASE REPORT Single-stage laparoscopic surgery for bilateral organ tumors using a transumbilical approach with a zigzag incision:
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Clinical Policy: Robotic Surgery Reference Number: CP.MP. 207
 Clinical Policy: Robotic Surgery Reference Number: CP.MP. 207 Effective Date: 03/05 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: Robotic Surgery Reference Number: CP.MP. 207 Effective Date: 03/05 Last Review Date: 10/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important
Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor
 Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
 Surgical Technique Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (1): 71-75, January - February, 2000 TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
Surgical Technique Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (1): 71-75, January - February, 2000 TECHNIQUE OF ENDOPYELOTOMY WITH THE ACUCISE CUTTING BALLOON
Laparoscopic Nephrectomy For Benign and Inflammatory Conditions* T. MANOHAR, M.D., MIHIR DESAI, M.D., and MAHESH DESAI, M.S., FRCS, FRCS ABSTRACT
 JOURNAL OF ENDOUROLOGY Volume 21, Number 11, November 2007 Mary Ann Liebert, Inc. DOI: 10.1089/end.2007.9883 Laparoscopic Nephrectomy For Benign and Inflammatory Conditions* T. MANOHAR, M.D., MIHIR DESAI,
JOURNAL OF ENDOUROLOGY Volume 21, Number 11, November 2007 Mary Ann Liebert, Inc. DOI: 10.1089/end.2007.9883 Laparoscopic Nephrectomy For Benign and Inflammatory Conditions* T. MANOHAR, M.D., MIHIR DESAI,
Indications and effectiveness of the open surgery in vesicoureteral reflux
 Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
Indications and effectiveness of the open surgery in vesicoureteral reflux Suzi DEMIRBAG, MD Department of Pediatric Surgery, Gulhane Military Medical Academy, Ankara, TURKEY Vesicoureteral reflux (VUR)
