A prospective, multicentre, randomised controlled study of human fibroblast-derived dermal substitute (Dermagraft) in patients with venous leg ulcers
|
|
|
- Martin Campbell
- 5 years ago
- Views:
Transcription
1 International Wound Journal ISSN ORIGINAL ARTICLE A prospective, multicentre, randomised controlled study of human fibroblast-derived dermal substitute (Dermagraft) in patients with venous leg ulcers Keith Harding 1, Michael Sumner 2 & Matthew Cardinal 2 1 Wound Healing Research Unit, Cardiff University School of Medicine, Cardiff, UK 2 Shire Regenerative Medicine, San Diego, CA USA Key words Fibroblasts; Skin; Ulcer; Venous ulcer; Wound healing Correspondence to K Harding, CBE, MBChB Director, Wound Healing Research Unit, Institute for Translation, Innovation, Methodologies and Engagement (TIME) Cardiff University School of Medicine Upper Ground Floor, Room 18 Heath Park, Cardiff CF14 4XN, UK hardingkg@cf.ac.uk Harding K, Sumner M, Cardinal M. A prospective, multicentre, randomised controlled study of human fibroblast-derived dermal substitute (Dermagraft) in patients with venous leg ulcers. Int Wound J 2013; 10: Abstract This was an open-label, prospective, multicentre, randomised controlled study to evaluate the efficacy and safety of human fibroblast-derived dermal substitute (HFDS) plus four-layer compression compared with compression alone in the treatment of venous leg ulcers. The primary outcome variable was the proportion of patients with completely healed study ulcers by 12 weeks. The number healed was further summarised by ulcer duration and baseline ulcer size. Sixty-four (34%) of 186 patients in the HFDS group experienced healing by week 12 compared with 56 (31%) of 180 patients in the control group (P = 0 235). For ulcers 12 months duration, 49 (52%) of 94 patients in the HFDS group versus 36 (37%) of 97 patients in the control group healed at 12 weeks (P = 0 029). For ulcers 10 cm 2, complete healing at week 12 was observed in 55 (47%) of 117 patients in the HFDS group compared with 47 (39%) of 120 patients in the control group (P = 0 223). The most common adverse events (AEs) were wound infection, cellulitis and skin ulcer. The frequency of AEs did not markedly differ between the treatment and control groups. Introduction Venous leg ulcers (VLUs) have a lifetime prevalence of approximately 1% (1) and remain a challenging problem in clinical practice. In the majority of patients, the principal cause is ambulatory venous hypertension occurring as the result of valvular incompetence and venous reflux (2). Lower limb compression to counteract these effects is the standard of care for treatment (2), but, unfortunately, it often fails to achieve healing in a timely fashion. Success rates are reported to range from 30% to 65% after 24 weeks of (3). A complex series of cellular and growth factor deficiencies are present in the ulcer environment. Venous hypertension may cause blood proteins to leak in the extravascular space, trapping growth factors and cytokines needed for tissue repair. Leakage of fibrinogen from veins as well as deficiencies in fibrinolysis may also cause fibrin to build up around the vessels, preventing oxygen and nutrients from reaching cells (4). In a group of sequential biopsies taken from the margins of VLUs during their healing, a deficiency of fibronectin Key Messages chronic venous leg ulcerations are a common problem in clinical practice and the use of adjuvant therapies in combination with lower limb compression may lead to improved healing rates we investigated the proportion of patients achieving complete healing of venous ulcers using four-layer compression dressing plus applications of a human fibroblast-derived skin substitute over 12 weeks compared with compression dressing alone statistical significance was not reached for the primary efficacy endpoint of number of patients with study ulcers completely healed by 12 weeks, but a subgroup analysis of patients with ulcers < 12 months in duration showed that significantly more patients healed at week 12 in the HFDS versus control group 132 International Wound Journal 2013 Blackwell Publishing Ltd and Medicalhelplines.com Inc
2 K. Harding et al. Controlled study of human fibroblast-derived dermal substitute for venous leg ulcers has been observed in granulation tissue compared with the surrounding normal dermis (5). In another series, venous ulcers were shown to be deficient in oxygen compared with normal tissue (6). As a consequence, the conditions of the VLU wound environment may not efficiently support the epidermal migration, attachment and proliferation of regenerating cells needed for healing. Effective treatment of non healing VLUs may require, in addition to compression bandaging, the provision of a suitable substrate, specifically a dermal replacement capable of promoting epithelialisation of the wound. Dermagraft (Shire Regenerative Medicine, San Diego, CA), a human fibroblastderived dermal substitute (HFDS), consists of dermal fibroblasts derived from newborn human foreskin tissue and cultured in vitro onto a bioresorbable polyglactin mesh. The fibroblasts secrete human dermal collagen, matrix proteins, growth factors and cytokines as they proliferate throughout the threedimensional mesh and become deposited in a self-produced human dermal matrix. The result is a living, metabolically active dermal tissue. The results of pilot studies with HFDS suggested higher rates of complete wound epithelialisation with the combination of HFDS (using various application regimens) and standard compared with standard alone. On the basis of the favourable results of this and other preliminary studies, including a study in which a four-piece regimen of HFDS yielded a greater proportion of patients who achieved complete healing (38%) compared with compression alone (15%) (7), a pivotal randomised controlled study was conducted to evaluate the efficacy and safety of HFDS and standard compared with standard alone. Compression bandaging techniques vary widely from country to country. For the purposes of standardisation, all patients received compression using the Profore four-layer compression system (Smith & Nephew, Hull, UK). This fourlayer system consists of a layer of orthopaedic padding to absorb wound exudate and protect bony prominences, a light conformable bandage, an elastic compression bandage and an elastic cohesive bandage to apply additional compression and hold all bandages in place. Four-layer compression has demonstrated effectiveness in healing some chronic wound ulcerations (8). Methods Patients or participants Patients at least 18 years of age who were referred to participating hospital or community-based VLU clinics in the UK, the USA or Canada were eligible for the study. Patients were required to have a VLU located between the knee and ankle (at the level of, and including, the lateral and medial malleolus) that was present for at least 2 months and no more than 5 years prior to screening. The patient s ulcer had to (i) be 3 25 cm 2 in size; (ii) have a typical appearance of a VLU without exposure of muscle, tendon or bone and (iii) have clean, granulating base with minimal adherent slough, suitable to receive a skin graft. Ulcers that reduced in size (cm 2 ) by less than 50% while under compression during the 2-week screening period of the study were eligible for randomisation into the study. Sufficient circulation to the study leg to make wound healing possible was required. To be included in the study, patients had to have an ankle brachial pressure index between 0 8 and 1 2 and venous disease had to be confirmed by duplex ultrasonography to demonstrate reflux of >0 5 seconds in saphenous, calf perforator or popliteal veins. Patients whose ulcers were deemed by the investigator to be caused by a medical condition other than venous insufficiency were excluded. Patients who had evidence of sinus tracts within their ulcer or evidence of a wound infection (purulence and/or odour), cellulitis and/or confirmed osteomyelitis were not enrolled. Other key exclusion criteria included morbid obesity, skin diseases near study ulcer, malignant disease within 5 years, severe peripheral vascular disease or renal disease, congestive heart failure, cell anaemia, thalassemia or uncontrolled diabetes. Patients who had received immune suppressants, systemic corticosteroids, cytotoxic chemo or topical steroids for more than 2 weeks and within 1 month of initial screening or who had a history of radiation at the ulcer site were not included in the study. Patients with a known allergy to bovine products or components of the compression bandage, or who could not tolerate compression bandage, had received an investigational drug within 30 days of randomisation or had been previously treated with HFDS and/or other tissue-engineered materials were also excluded. Study design and treatment This was an open-label, prospective, multicentre, randomised controlled study that evaluated HFDS plus four-layer compression compared with conventional (compression alone) in the treatment of VLUs. The patients gave informed consent. This study was conducted under independent Ethics Committees and Institutional Review Boards, and it was performed in accordance with the guidelines of the Declaration of Helsinki (1964) and subsequent revisions. During a 2-week screening period, a study ulcer was identified for each patient. Only one ulcer was selected for the study; if a patient had more than one ulcer, the largest ulcer that met the inclusion criteria was selected. Wound tracing and ulcer area grid evaluations were performed to determine percentage of healing between screening and randomisation. During the screening period, all subjects were treated with a standard dressing regimen including four-layer compression bandaging. Each wound was covered with a layer of non adherent dressing (Dermanet, DeRoyal, Powell, TN) followed by the appropriately sized compression bandage, which was determined by measuring the circumference of the patient s ankle 1 inch above the tibial malleolus. For deeper ulcers, extra light packing (gauze) could be used on top of the non adherent dressing to ensure adequate contact with the base of the ulcer. For heavily exuding ulcers, a further absorbent dressing could be applied at the discretion of the investigator. During the 2-week screening period, the wound was observed weekly to determine that the ulcer was free of necrotic tissue, clear of infection and had a vascular bed. If clinically indicated, the dressing could be changed earlier. International Wound Journal 2013 Blackwell Publishing Ltd and Medicalhelplines.com Inc 133
3 Controlled study of human fibroblast-derived dermal substitute for venous leg ulcers K. Harding et al. Prior to randomisation, surgical debridement of the study ulcer could be performed at the discretion of the investigator. After confirming the absence of clinical infection or necrotic tissue, the wound was rinsed with normal saline, the ulcer was traced and the area of the ulcer was calculated using planimetry analysis. Randomisation was conducted in blocks of either two or four to ensure that study personnel could not predict treatment allocation. Randomisation was stratified by study centre and by study ulcer area. The two strata for ulcer size were ulcers from 3 to 10 cm 2 and from >10 to 25 cm 2. Patients were randomised to receive HFDS plus the four-layer compression bandage (active) or the four-layer compression bandage alone (control). Patients randomised to the active treatment group received HFDS applied to the wound at weeks 0, 1, 4 and 8. Before implantation, HFDS was thawed, rinsed and prepared according to directions for use. The prepared HFDS was cut to fit the shape of the ulcer and to accommodate any epithelial islands, placed into the wound bed with no overlap onto the intact skin surrounding the ulcer and smoothed gently to ensure that the entire piece of HFDS was in contact with the wound surface. The wound-dressing regimen was identical for both treatment groups and was identical to that used during the screening period. Assessments Efficacy assessment The primary outcome variable was the proportion of patients with completely healed study ulcers by 12 weeks. Complete healing was defined by having a closed wound for two consecutive weekly visits. A closed wound was defined as full epithelialisation of the wound with the absence of drainage (i.e. no exudate or scab). The primary outcome of complete healing was ascertained by the primary investigator by visual inspection. The primary outcome variable was also summarised by duration of current ulceration and baseline ulcer size ( 10 and >10 cm 2 ). Secondary outcome variables included time to healing, complete healing by week 24 (follow-up endpoint) and percent reduction in ulcer area. The area of the study ulcer was calculated using planimetry analysis. After debridement (if required) and cleansing, ulcer tracings were obtained by placing a clear plastic bag over the patient s wound and making a direct tracing at the edge of the intact epithelium and around epithelial islands, if present. Whenever possible, the same person performed the tracing at every visit. Once the bag was removed from the wound and directionally marked, planimetry was performed on each tracing to calculate the ulcer area. Safety assessment Adverse events (AEs) were identified and grouped by system organ class using the Dictionary for Medical Drug Regulatory Activities (MedDRA) Version 7. The AEs were reported according to guidelines specific to the country where the treatment centres were located. Patients exhibiting serious and/or unexpected adverse drug reactions were withdrawn from the study at the discretion of the investigator. Statistical analysis Sample size analysis called for 166 patients in each treatment group to detect a 15% difference in the proportion of patients who achieve complete healing at week 12. The sample size calculation was based on a χ 2 test for the comparison of proportions of healing using a healing rate of 32% for control and 47% for HFDS with a 0 05 two-sided significance level and at least 80% power. The intent-to-treat (ITT) population was defined as all patients receiving study treatment at baseline and having a follow-up visit post-baseline. The safety population was defined as all patients with a baseline visit. Descriptive statistics were used to report baseline demographics and characteristics. The primary outcome variable, a binary measure of healed or not healed by 12 weeks, was assessed for the ITT population after adjusting for covariates including treatment, ulcer area at baseline and duration of current ulceration using an initial logistical regression model. A forward selection procedure was used for the addition of other baseline covariates with an F of 0 1. The 95% confidence interval (CI) (unadjusted for all covariates) for the difference between treatments in the percent healed by 12 weeks was generated along with the χ 2 test P value. The percent reduction in ulcer area per week was compared between treatment groups using the Mann Whitney test. No multiplicity testing across secondary endpoints was performed to control for type 1 error. The number of patients with an AE was compared between treatment groups using a two-sided Fisher s exact test. A P value of 0 05 was considered significant. Results Patients Of the 573 patients screened, 207 failed screening (36% screen failure rate). The most common reasons for screen failure were study ulcers reducing in size by more than 50% during screening, study ulcers less than 3 cm 2 at randomisation and subjects without evidence of venous reflux. The remaining 366 patients were randomised to receive treatment at a total of25centres:19intheuk,1incanadaand5intheusa. The ITT population included 186 patients in the HFDS group and 180 patients in the control group. A total of 10% (19 of 186) of patients in the HFDS group discontinued the study early compared with 23% (41 of 180) of patients in the control group. The reasons for early discontinuation were AE (3% in the HFDS group versus 6% in the control group), patient s own request (2% versus 9%), patient lost to follow-up (2% versus 3%) and other (4% from each group). The mean age of the ITT population was 68 5 years, 46% of patients were male, 54% were female and most were Caucasian (92%). The mean body mass index was 30 1 kg/m 2 (Table 1). The treatment groups were generally well balanced with regard to baseline characteristics, including key study ulcer characteristics known to be associated with ulcer healing. The median duration of the current ulcer was 49 7weeks in the HFDS group and 45 3 weeks in the control group; the median 134 International Wound Journal 2013 Blackwell Publishing Ltd and Medicalhelplines.com Inc
4 K. Harding et al. Controlled study of human fibroblast-derived dermal substitute for venous leg ulcers Table 1 Baseline demographics and characteristics Parameter HFDS plus compression (N = 186) Compression (N = 180) Mean age, years (SD) 67 9 (13 8) 69 1 (12 4) Sex, n (%) Female 100 (53 8) 97 (53 9) Male 86 (46 2) 83 (46 1) Race, n (%) White 173 (93 0) 164 (91 1) Black 5 (2 7) 8 (4 4) Asian 3 (1 6) 1 (0 6) Other 5 (2 7) 7 (3 9) Mean body mass index, 30 0 (6 4) 30 1 (6 8) kg/m 2 (SD) Median duration of current 49 7 ( ) 45 3 ( ) study ulcer, weeks (range) Median ulcer size, cm ( ) 7 2 ( ) (range) Study ulcer has healed and 104 (56) 86 (48) recurred, n (%) Median duration since the ulceration first appeared at the study site, weeks (range) ( ) ( ) Figure 1 Percent of patients with complete healing of study ulcer by week 12 (overall intent-to-treat population). HFDS, human fibroblastderived dermal substitute. HFDS, human fibroblast-derived dermal substitute; SD, standard deviation. study ulcer area was 7 4cm 2 in the HFDS group and 7 2cm 2 in the control group. The groups were also well balanced with regard to gender, height, study ulcer health state, percentage of unhealthy tissue and ankle circumference. Assessments Efficacy assessments Primary endpoint. Sixty-four (34%) of 186 patients in the HFDS group experienced healing by week 12 compared with 56 (31%) of 180 patients in the control group (P = 0 235, odds ratio = 1 40, 95% CI = 0 80, 2 41) (Figure 1). Evidence of a treatment by duration of the current study ulcer interaction was observed (odds ratio, ulcer duration HFDS: ulcer duration control = 0 99, 95% CI = 0 98, 1 00). Because the primary analysis assumed a consistent treatment effect across the baseline duration of the current study ulcer, rather than the inconsistent effect that was observed, the primary analysis did not hold. After identification of the treatment-by-ulcer interaction, a pre-specified subgroup analysis evaluating complete healing by ulcer duration was performed. For the subgroup of patients with ulcer duration of 12 months or less, healing by week 12 was observed in significantly more patients in the HFDS group compared with the control group, 49 (52%) of 94 patients versus 36 (37%) of 97 patients, respectively (P = 0 029, odds ratio 2 37, 95% CI = 1 08, 5 14) (Figure 2). In the subgroup of patients with ulcers 10 cm 2 or less, complete healing at week 12 was observed in 55 (47%) of 117 patients in the HFDS group compared with 47 (39%) of 120 patients in the control group, but this difference did not reach statistical significance (Figure 3). Figure 2 Effect of ulcer duration on percent of patients with complete healing of study ulcer by week 12 (intent-to-treat population). HFDS, human fibroblast-derived dermal substitute. Secondary analyses. For the full ITT population, 96 (52%) of 186 patients in the HFDS group and 88 (49%) of 180 patients in the control group achieved complete healing by week 24. No significant difference between treatment groups was observed in the time to healing (P = 0 660, hazard ratio = 1 07, 95% CI = 0 80, 1 43). At week 12, the median percentage reduction in ulcer area was 83 7% in the HFDS group compared with 73 0% in the control group. Safety assessments The overall incidence and type of AEs were comparable between the HFDS and control groups. One hundred forty-six (78%) of 187 patients in the HFDS group reported 444 AEs and 138 (77%) of 179 patients in the control group reported 472 AEs (P = 0 900). The most common treatment-emergent AEs were wound infection, cellulitis and skin ulcer (Table 2). These events were expected in this population and their frequencies did not markedly differ between the treatment and control group. A total of 39 AEs were reported in 21 patients (11% of all patients) assessed by the investigator as probably (4 patients) International Wound Journal 2013 Blackwell Publishing Ltd and Medicalhelplines.com Inc 135
5 Controlled study of human fibroblast-derived dermal substitute for venous leg ulcers K. Harding et al. Table 2 Most commonly reported treatment-emergent adverse events (safety population)* Adverse event, n (%) HFDS plus compression (N = 187) Compression (N = 179) Figure 3 Effect of initial ulcer area on percent of patients with complete healing of study ulcer by week 12 (intent-to-treat population). HFDS, human fibroblast-derived dermal substitute. or possibly (35 patients) related to HFDS; none of which was serious. There were 24 serious/severe AEs in the HFDS group and 33 serious/severe AEs in the control group. There was no evidence of a difference between treatment groups in the numbers of patients experiencing a study site infection. During the course of the study, a study site infection was observed in 43 (23%) of 187 patients in the HFDS group and 46 (26%) of 179 patients in the control group (P = 0 62). Of the study ulcers that healed, 15% recurred in the HFDS group and 23% recurred in the control group during the 24-week study period. Discussion We compared HFDS plus compression to compression alone for the treatment of VLUs. Statistical significance was not reached for the primary efficacy endpoint of number of patients with study ulcers completely healed by 12 weeks. As a result of an observed treatment by duration of study ulcer interaction, a subanalysis was conducted for patients with duration of study ulcer < 12 months, which showed more patients healed at week 12 in the HFDS versus control group. Other advanced therapies combined with compression have been investigated for the treatment of VLU. Studies of pentoxifylline and Apligraf (Organogenesis, Canton, MA), another tissue-engineered product, have both demonstrated a benefit when used in addition to standard compression to treat leg ulcer populations with median or mean ulcer sizes less than 5 cm 2 (9,10). Baseline ulcer area is a significant predictor of time to heal (3,8,11,12). In one multicentre study conducted by Phillips et al., healing was observed in 72% of patients with a baseline ulcer area of <5cm 2 compared with 40% of subjects with a baseline area of >5cm 2 (11). In a study of Apligraf, a benefit was observed in treating ulcers older than 12 months (10). However, the mean ulcer sizes in both the active and standard care groups of this study were smaller than 2 cm 2. By contrast, the ulcers in the current HFDS study were larger and thus harder to heal, having a mean area of 6 6cm 2 in the subgroup of patients with ulcers of 12-month duration or less (10). Ulcer duration is a well-established marker predicting the likelihood of healing (3,8,11,12). In the study by Infections and infestations Wound infection 55 (29 4) 43 (24 0) Study site infection 43 (23) 46 (26) Cellulitis 12 (6 4) 18 (10 1) Nasopharyngitis 12 (6 4) 6 (3 4) Skin and subcutaneous tissue disorders Skin ulcer 25 (13 4) 39 (21 8) Pruritus 13 (7 0) 6 (3 4) Venous ulcer pain 10 (5 3) 9 (5 0) Stasis dermatitis 10 (5 3) 6 (3 4) Skin disorder 8 (4 3) 15 (8 4) Injury, poisoning and procedural complications Fall 6 (3 2) 11 (6 1) General disorders and administration site conditions Peripheral oedema 13 (7 0) 5 (2 8) Musculoskeletal and connective tissue disorders Pain in extremity 9 (4 8) 10 (5 6) HFDS, human fibroblast-derived dermal substitute. *Adverse events reported in 5% in either treatment group. Phillips et al., a healing rate of 64% was observed with ulcers of less than 1-year duration compared with 48% with ulcers of 1- to 3-year duration (11). Similarly, in our study, a significant effect of HFDS was observed in ulcers of 12-month duration or less, but not in those of over 12-month duration. The failure to demonstrate a significant benefit in older ulcers (i.e. >12-month duration) in this study may be attributed to changes over time in the biological environment of the wound that may make older ulcers more resistant to healing. Older ulcers may have higher levels of cellular senescence (13), matrix impairment (14) and bacterial burden that interfere with healing (15). Older ulcers may also require additional applications of HFDS over a longer period of time to achieve significant improvement in the rates of healing. However, further investigation is needed. In conclusion, HFDS did not show a statistically significant improvement over compression alone for overall healing by week 12. However, efficacy appears to improve as ulcer duration decreases, suggesting clinical merit for earlier use of adjuvant. There were no differences between the groups in reported AEs. The safety profile of HFDS in the treatment of venous ulcers is comparable to that of standard. Acknowledgements The authors take full responsibility for the contents of this manuscript and verify that they have met all of the journal s requirements for authorship. The authors thank The JB Ashtin Group, Inc., for assistance in preparing this manuscript for publication based on the authors input and direction. Financial support for editorial assistance was provided by Smith & Nephew Wound Management, Hull, UK, and Shire Regenerative Medicine, San Diego, California, USA. Prof. KH 136 International Wound Journal 2013 Blackwell Publishing Ltd and Medicalhelplines.com Inc
6 K. Harding et al. Controlled study of human fibroblast-derived dermal substitute for venous leg ulcers discloses that the Wound Healing Research Unit is a selffunded group in Cardiff University that receives funding from a variety of academic and commercial concerns. These include 3M, Convatec, Covidien, Frontier Therapeutics, KCI, Photopharmica, Shire Regenerative Medicine (formally Advanced BioHealing), Smith & Nephew and Tissue Therapies. Dr MS and Mr MC are full-time employees of Shire Regenerative Medicine in San Diego, California, USA. References 1. Nelzen O. Prevalence of venous leg ulcer: the importance of the data collection method. Phlebolymphology 2008;15: Kunimoto B, Cooling M, Gulliver W, Houghton P, Orsted H, Sibbald RG. Best practices for the prevention and treatment of venous leg ulcers. Ostomy Wound Manage 2001;47: Margolis DJ, Berlin JA, Strom BL. Risk factors associated with the failure of a venous leg ulcer to heal. Arch Dermatol 1999;135: Brem H, Kirsner RS, Falanga V. Protocol for the successful treatment of venous ulcers. Am J Surg 2004;188(1A Suppl): Herrick SE, Sloan P, McGurk M, Freak L, McCollum CN, Ferguson MW. Sequential changes in histologic pattern and extracellular matrix deposition during the healing of chronic venous ulcers. Am J Pathol 1992;141: Falanga V, Moosa HH, Nemeth AJ, Alstadt SP, Eaglstein WH. Dermal pericapillary fibrin in venous disease and venous ulceration. Arch Dermatol 1987;123: Krishnamoorthy L, Harding K, Griffiths D, Moore K, Leaper D, Poskitt K, Sibbald RG, Brassard A, Dolynchuk K, Adams J, Whyman M. The clinical and histological effects of Dermagraft in the healing of chronic venous leg ulcers. Phlebology 2003;18: Moffatt CJ, Franks PJ, Oldroyd M, Bosanquet N, Brown P, Greenhalgh RM, McCollum CN. Community clinics for leg ulcers and impact on healing. Br Med J 1992;305: Falanga V, Fujitani RM, Diaz C, Hunter G, Jorizzo J, Lawrence PF, Lee BY, Menzoian JO, Tretbar LL, Holloway GA, Hoballah J, Seabrook GR, McMillan DE, Wolf W. Systemic treatment of venous leg ulcers with high doses of pentoxifylline: efficacy in a randomized, placebo-controlled trial. Wound Repair Regen 1999;7: Falanga V, Sabolinski M. A bilayered living skin construct (APLIGRAF) accelerates complete closure of hard-to-heal venous ulcers. Wound Repair Regen 1999;7: Phillips TJ, Machado F, Trout R, Porter J, Olin J, Falanga V. Prognostic indicators in venous ulcers. J Am Acad Dermatol 2000;43: Margolis DJ, Allen-Taylor L, Hoffstad O, Berlin JA. The accuracy of venous leg ulcer prognostic models in a wound care system. Wound Repair Regen 2004;12: Agren MS, Steenfos HH, Dabelsteen S, Hansen JB, Dabelsteen E. Proliferation and mitogenic response to PDGF-BB of fibroblasts isolated from chronic venous leg ulcers is ulcer-age dependent. J Invest Dermatol 1999;112: Loots MA, Lamme EN, Zeegelaar J, Mekkes JR, Bos JD, Middelkoop E. Differences in cellular infiltrate and extracellular matrix of chronic diabetic and venous ulcers versus acute wounds. J Invest Dermatol 1998;111: Tuttle MS, Mostow E, Mukherjee P, Hu FZ, Melton-Kreft R, Ehrlich GD, Dowd SE, Ghannoum MA. Characterization of bacterial communities in venous insufficiency wounds by use of conventional culture and molecular diagnostic methods. J Clin Microbiol 2011;49: International Wound Journal 2013 Blackwell Publishing Ltd and Medicalhelplines.com Inc 137
Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU)
 Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU) Sami Khan, MD FACS Associate Professor of Surgery Division of Plastic and Reconstructive Surgery SUNY-Stony
Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU) Sami Khan, MD FACS Associate Professor of Surgery Division of Plastic and Reconstructive Surgery SUNY-Stony
The Georgetown Team Approach to Diabetic Limb Salvage: 2013
 The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Use of Non-Contact Low Frequency Ultrasound in Wound Care
 Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
P. P.2-7 P R A C T I C A L
 P R A T I A L O U R S E The use of hyaluronic acid derivatives in the treatment of long-term non-healing wounds Systematic review and meta-analysis of RSs (randomized controlled studies) J. Voigt and V.
P R A T I A L O U R S E The use of hyaluronic acid derivatives in the treatment of long-term non-healing wounds Systematic review and meta-analysis of RSs (randomized controlled studies) J. Voigt and V.
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Health technology The use of four-layer compression bandaging (4LB) versus alternative dressings for the treatment of venous ulcers.
 Randomized clinical trial and economic analysis of four-layer compression bandaging for venous ulcers O'Brien J F, Grace P A, Perry I J, Hannigan A, Clarke Moloney M, Burke P E Record Status This is a
Randomized clinical trial and economic analysis of four-layer compression bandaging for venous ulcers O'Brien J F, Grace P A, Perry I J, Hannigan A, Clarke Moloney M, Burke P E Record Status This is a
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Interesting Case Series. Skin Grafting in Pyoderma Gangrenosum
 Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Ray Norris, Rachel Henchy
 Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer
 Original Research Article A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer S Vijayalakshmi * Associate Professor, Department of General Surgery, Govt.
Original Research Article A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer S Vijayalakshmi * Associate Professor, Department of General Surgery, Govt.
Arterial & Venous Ulcers. A Comprehensive Review Assessment & Management
 Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Accelerate wound healing of acute and chronic wounds in patients with Diabetes: Experience from Mexico using supplementary haemoglobin spray.
 Accelerate wound healing of acute and chronic wounds in patients with Diabetes: Experience from Mexico using supplementary haemoglobin spray. Obdulia Lopez Lopez 1, Fredrik Elg 2 Peter Engels 3, 1 Universidad
Accelerate wound healing of acute and chronic wounds in patients with Diabetes: Experience from Mexico using supplementary haemoglobin spray. Obdulia Lopez Lopez 1, Fredrik Elg 2 Peter Engels 3, 1 Universidad
Hemostasis Inflammatory Phase Proliferative/rebuilding Phase Maturation Phase
 The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
Clinical Policy: EpiFix Wound Treatment
 Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
WOUND CARE UPDATE. -Commonly Used Skin Substitute Products For Wound. -Total Contact Casting. Jack W. Hutter DPM, FACFAS, C. ped.
 WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude
 Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks
 A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks Robert J. Snyder, DPM, CWS; Matthew Cardinal, ME; Damien M. Dauphinée, DPM, FACFAS, CWS; and
A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks Robert J. Snyder, DPM, CWS; Matthew Cardinal, ME; Damien M. Dauphinée, DPM, FACFAS, CWS; and
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Four Layer Versus Actico Cohesive Short Stretch Bandage Background
 Four Layer Versus Actico Cohesive Short Stretch Bandage Background Cochrane Systematic Review 6/2/01 "Five small studies found no difference in healing between multi-layer high compression (4-layer bandage
Four Layer Versus Actico Cohesive Short Stretch Bandage Background Cochrane Systematic Review 6/2/01 "Five small studies found no difference in healing between multi-layer high compression (4-layer bandage
Venous Insufficiency Ulcer
 Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers
 A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
JOURNAL OF WOUND CARE. VOLUME 8. NUMBER 9. October A comparison of sub-bandage pressures produced with two multi-layer bandaging systems
 JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
JOURNAL OF WOUND CARE VOLUME 8. NUMBER 9. October 1999 A comparison of sub-bandage pressures produced with two multi-layer bandaging systems A.D. Taylor, MSc, RGN, SCM, DN, Clinical Nurse Specialist, Salford
versus short stretch compression bandages for the treatment of venous leg ulcers
 Ann R Coll Surg Engl 1998; 80: 215-220 A prospective randomised trial of four-layer versus short stretch compression bandages for the treatment of venous leg ulcers J M Scriven BSc FRCS* Clinical Research
Ann R Coll Surg Engl 1998; 80: 215-220 A prospective randomised trial of four-layer versus short stretch compression bandages for the treatment of venous leg ulcers J M Scriven BSc FRCS* Clinical Research
NovoSorb BTM. A unique synthetic biodegradable wound scaffold. Regenerating tissue. Changing lives.
 NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
A comprehensive study on effect of collagen dressing in diabetic foot ulcer
 Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Application Guide for Full-Thickness Wounds
 Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Prediction of healing for post-operative diabetic foot wounds based on early wound area progression
 Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds
 Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Do all foam dressings have the same efficacy in the treatment of chronic wounds? Janice Bianchi, David Gray, John Timmons, Sylvie Meaume
 Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Buy full version here - for $ 6.00
 This is a Sample version of the Leg and Foot Ulcer Questionnaire (LFUQ) The full version of Leg and Foot Ulcer Questionnaire (LFUQ) comes without sample watermark.. The full complete version includes LFUQ
This is a Sample version of the Leg and Foot Ulcer Questionnaire (LFUQ) The full version of Leg and Foot Ulcer Questionnaire (LFUQ) comes without sample watermark.. The full complete version includes LFUQ
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
STUDY. complication of diabetes, affecting 12% to 15% of patients. during their lifetime. 1,2 Diabetic foot ulcers (DFUs) impair quality
 STUDY Advanced Biological Therapies for Diabetic Foot Ulcers Robert S. Kirsner, MD, PhD; Robert Warriner, MD; Michelle Michela, MS; Laure Stasik, BA; Katherine Freeman, PhD Objective: To assess the clinical
STUDY Advanced Biological Therapies for Diabetic Foot Ulcers Robert S. Kirsner, MD, PhD; Robert Warriner, MD; Michelle Michela, MS; Laure Stasik, BA; Katherine Freeman, PhD Objective: To assess the clinical
First Coast Service Options (FCSO) Medicare Policy Primer
 First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL. of the infection risk in chronic wound
 Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Topical Oxygen Wound Therapy (MEDICAID)
 Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Clinical. Summaries. 3M Tegaderm Matrix Matrix Dressing. Delayed wound healing: A major clinical problem
 3M Tegaderm Matrix Matrix Dressing Clinical Summaries Delayed wound healing: A major clinical problem Chronic wounds have been defined as those that fail to progress through a normal, orderly, and timely
3M Tegaderm Matrix Matrix Dressing Clinical Summaries Delayed wound healing: A major clinical problem Chronic wounds have been defined as those that fail to progress through a normal, orderly, and timely
Treatment of Chronic Venous Ulcers Using New Four Layers Compressive Bandage Dressing
 ORIGINAL ARTICLE J Nepal Med Assoc 215;53(199):156-61 CC S BY NC OPEN ACCESS Treatment of Chronic Venous Ulcers Using New Four Layers Compressive Bandage Dressing Kaushal K Tiwari, 1 Krishna G Shrestha,
ORIGINAL ARTICLE J Nepal Med Assoc 215;53(199):156-61 CC S BY NC OPEN ACCESS Treatment of Chronic Venous Ulcers Using New Four Layers Compressive Bandage Dressing Kaushal K Tiwari, 1 Krishna G Shrestha,
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
CASE 1: TYPE-II DIABETIC FOOT ULCER
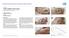 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Tdressing, cross-linked hydrogels, biological dressings, platelet-derived. Sepaderm for the Management of Acute and Chronic Wounds CASE SERIES
 CASE SERIES Sepaderm for the Management of Acute and Chronic Wounds Kerry Thibodeaux, MD, FACS; 1 S. William Tam, PhD 2 WOUNDS 2010;22(10):251 255 Abstract: The following case series includes a surgical
CASE SERIES Sepaderm for the Management of Acute and Chronic Wounds Kerry Thibodeaux, MD, FACS; 1 S. William Tam, PhD 2 WOUNDS 2010;22(10):251 255 Abstract: The following case series includes a surgical
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
SAMPLE. HLTEN406A Undertake basic wound care. Learner resource. HLT07 Health Training Package. Version 2
 HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
Compression bandaging remains the basis of venous
 CLINICAL EVALUATION Evaluation of Urgotul plus K-Four compression for venous leg ulcers J Smith, J Hill, S Barrett, W Hayes, P Kirby, S Walsh, E Gittins, F Whitehurst, R Cooper Compression bandaging remains
CLINICAL EVALUATION Evaluation of Urgotul plus K-Four compression for venous leg ulcers J Smith, J Hill, S Barrett, W Hayes, P Kirby, S Walsh, E Gittins, F Whitehurst, R Cooper Compression bandaging remains
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING
 HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
CHAPTER 1 HOW COMPRESSION WORKS
 CHAPTER 1 HOW COMPRESSION WORKS The impact that compression has had on leg ulcer healing over the last two decades has been enormous. Although it is frequently reported that compression has been in use
CHAPTER 1 HOW COMPRESSION WORKS The impact that compression has had on leg ulcer healing over the last two decades has been enormous. Although it is frequently reported that compression has been in use
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
New Guideline in venous ulcer treatment: dressing, medication, intervention
 New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
1/5. Introduction. Primary endpoint Time to reach readiness for closure by surgical intervention or left for closure by secondary intention
 1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
Clinical Review Criteria
 Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
Leg ulcers. Causes and management. OBJECTIVE This article outlines the assessment and management of patients with leg ulceration.
 THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
4-layer compression bandaging system (includes microbe binding wound contact layer) Latex-free, 4-layer compression bandaging system
 JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
The Influence of Dressings on Venous Ulcer Healing--A Randomised Trial
 Eur J Vasc Endovasc Surg 13, 174-179 (1997) The Influence of Dressings on Venous Ulcer Healing--A Randomised Trial M. C. Stacey*, A. G. Jopp-Mckay, P. Rashid, S. E. Hoskin and P. J. Thompson University
Eur J Vasc Endovasc Surg 13, 174-179 (1997) The Influence of Dressings on Venous Ulcer Healing--A Randomised Trial M. C. Stacey*, A. G. Jopp-Mckay, P. Rashid, S. E. Hoskin and P. J. Thompson University
The influence of wound geometry on the measurement of wound healing rates in clinical trials
 The influence of wound geometry on the measurement of wound healing rates in clinical trials Daniel R. Gorin, MD, Paul R. Cordts, MD, Wayne W. LaMorte, MD, PhD, MPH, and James O. Menzoian, MD, Boston,
The influence of wound geometry on the measurement of wound healing rates in clinical trials Daniel R. Gorin, MD, Paul R. Cordts, MD, Wayne W. LaMorte, MD, PhD, MPH, and James O. Menzoian, MD, Boston,
QUICK GUIDE SNAP THERAPY SYSTEM
 QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
 PATCH Analysis Plan v1.2.doc Prophylactic Antibiotics for the Treatment of Cellulitis at Home: PATCH Analysis Plan for PATCH I and PATCH II Authors: Angela Crook, Andrew Nunn, James Mason and Kim Thomas,
PATCH Analysis Plan v1.2.doc Prophylactic Antibiotics for the Treatment of Cellulitis at Home: PATCH Analysis Plan for PATCH I and PATCH II Authors: Angela Crook, Andrew Nunn, James Mason and Kim Thomas,
If both a standardized, validated screening tool and an evaluation of clinical factors are utilized, select Response 2.
 (M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
(M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
Original Article Tissue engineered skin for diabetic foot ulcers: a meta-analysis
 Int J Clin Exp Med 2015;8(10):18191-18196 www.ijcem.com /ISSN:1940-5901/IJCEM0014309 Original Article Tissue engineered skin for diabetic foot ulcers: a meta-analysis Xuedong Li 1, Geliang Xu 2, Jianqiu
Int J Clin Exp Med 2015;8(10):18191-18196 www.ijcem.com /ISSN:1940-5901/IJCEM0014309 Original Article Tissue engineered skin for diabetic foot ulcers: a meta-analysis Xuedong Li 1, Geliang Xu 2, Jianqiu
Leg ulceration is a chronic condition affecting
 Effect of super-absorbent dressings on compression sub-bandage pressure Leanne Cook Leanne Cook, Vascular Nurse Specialist, Mid Yorkshire NHS Trust Email: Leanne.cook@midyorks.nhs.uk Leg ulceration is
Effect of super-absorbent dressings on compression sub-bandage pressure Leanne Cook Leanne Cook, Vascular Nurse Specialist, Mid Yorkshire NHS Trust Email: Leanne.cook@midyorks.nhs.uk Leg ulceration is
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Discussion Topics. Calcium Alginates. DME For the Diabetic Foot 1/25/2017. Jeffrey D. Lehrman, DPM, FASPS, FACFAS, MAPWCA
 DME For the Diabetic Foot Jeffrey D. Lehrman, DPM, FASPS, FACFAS, MAPWCA Editorial Advisory Board, WOUNDS Board of Directors, American Society of Podiatric Surgeons Board of Directors, American Professional
DME For the Diabetic Foot Jeffrey D. Lehrman, DPM, FASPS, FACFAS, MAPWCA Editorial Advisory Board, WOUNDS Board of Directors, American Society of Podiatric Surgeons Board of Directors, American Professional
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study
 The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study Woundmanagement Summary In the treatment of patients with chronic
The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study Woundmanagement Summary In the treatment of patients with chronic
1. Device Description
 DIRECTIONS FOR USE Caution: Federal (U.S.) law restricts this device to sale by or on the order of a physician (or properly licensed practitioner). 1. Device Description Dermagraft is a cryopreserved human
DIRECTIONS FOR USE Caution: Federal (U.S.) law restricts this device to sale by or on the order of a physician (or properly licensed practitioner). 1. Device Description Dermagraft is a cryopreserved human
CATRIX WOUND DRESSING CARTILAGE POWDER
 CATRIX WOUND DRESSING CARTILAGE POWDER Distributed By: Lescarden Inc. NY, NY (USA) Customer Relations: Toll Free (USA) (888) 581-2076. (212) 687-1050 Internet: www.catrix.com E-mail: info@catrix.com CATRIX
CATRIX WOUND DRESSING CARTILAGE POWDER Distributed By: Lescarden Inc. NY, NY (USA) Customer Relations: Toll Free (USA) (888) 581-2076. (212) 687-1050 Internet: www.catrix.com E-mail: info@catrix.com CATRIX
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Defining Outcomes for Clinical Wound Research in Older Adults February 21, 2014
 Defining Outcomes for Clinical Wound Research in Older Adults February 21, 214 Harold Brem, MD Professor of Surgery Stony Brook University School of Medicine Chief, Division of Wound Healing and Regenerative
Defining Outcomes for Clinical Wound Research in Older Adults February 21, 214 Harold Brem, MD Professor of Surgery Stony Brook University School of Medicine Chief, Division of Wound Healing and Regenerative
Consider the impact of Venous Disease Review elements in the workup and diagnosis of Venous Disease Review treatment considerations
 Gregory Bohn, MD FACS Clinical Symposium on Advances in Skin and Wound Care September 9-12, 2011 Gaylord National Washington, DC Consider the impact of Venous Disease Review elements in the workup and
Gregory Bohn, MD FACS Clinical Symposium on Advances in Skin and Wound Care September 9-12, 2011 Gaylord National Washington, DC Consider the impact of Venous Disease Review elements in the workup and
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options
 Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Prevalence of leg ulceration in a London population
 Q J Med 2004; 97:431 437 doi:10.1093/qjmed/hch075 Prevalence of leg ulceration in a London population C.J. MOFFATT 1, P.J. FRANKS 1, D.C. DOHERTY 1, R. MARTIN 2, R. BLEWETT 2 and F. ROSS 3 From the 1 Centre
Q J Med 2004; 97:431 437 doi:10.1093/qjmed/hch075 Prevalence of leg ulceration in a London population C.J. MOFFATT 1, P.J. FRANKS 1, D.C. DOHERTY 1, R. MARTIN 2, R. BLEWETT 2 and F. ROSS 3 From the 1 Centre
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
The primary function of low-adherence wound contact
 S35 Product focus S35 A multicentre clinical evaluation of silicone wound contact layer in daily practice Abstract Objective To evaluate clinically the performance of, a silicone-based primary contact
S35 Product focus S35 A multicentre clinical evaluation of silicone wound contact layer in daily practice Abstract Objective To evaluate clinically the performance of, a silicone-based primary contact
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
Setting The setting was a hospital. The economic study was carried out in the USA.
 A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
Wound Healing Basic Concept
 Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
2017 Florida Vascular Society
 Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Assisted Living Resident Assessment (To be used when yes is indicated for skin issues under Section 5 of Assisted Living Resident Assessment)
 Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
Hyperbarics in Diabetic Wound Care. Aurel Mihai, MD & Brian Kline, MD
 Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
