Managing lower back pain: You may be doing too much
|
|
|
- Alban Barber
- 5 years ago
- Views:
Transcription
1 William G. Elder Jr, PhD Michael King, MD Paul Dassow, MD Brian Macy, MD Family and Community Medicine, University of Kentucky College of Medicine, Lexington Managing lower back pain: You may be doing too much New guidelines call for a measured approach to imaging and medication, while emphasizing psychosocial evaluation. IN THIS ARTICLE Recommendations from the ACP/APS guidelines Page 183 Medications role in chronic lower back pain Page 185 A 32-year-old construction worker seeks treatment for the lower back pain (LBP) he s been experiencing since painting his house a few days ago. A 48-year-old man with a history of LBP comes in because he needs a refill of his hydrocodone prescription. Both patients are probably pretty typical of the back pain patients you see on a regular basis. But how would you care for each of these patients, and how does your care compare to the latest evidence? This review will help you to find out. In this article we take a look at guidelines from the American College of Physicians (ACP) and the American Pain Society (APS), 1 as well as findings from other recent studies, and apply them to these 2 patient cases. But first, a word about the ACP/APS guidelines. What s new? ACP/APS conducted a systematic review of studies of LBP epidemiology, clinical diagnosis, utility of imaging, and outcomes of pharmacologic 2 and nonpharmacologic interventions. 3 Whereas previous guidelines dealt with either acute or chronic pain, the ACP/APS guidelines synthesized the literature to apply to both. Moreover, rather than focusing mostly on pain reduction, the ACP/APS panel was interested in functional outcomes such as back-specific functioning, general health status, disability, and patient satisfaction. Finally, the panel s recommendations (TABLE) considered the unique environment of primary care (including presentations typically seen in this setting), the ability of primary care physicians to advise and counsel patients, continuity of care, and the role of the physician in coordinating care. CASE 1 Patient with acute nonspecific LBP While painting his home, a 32-year-old construction worker felt a twinge in his lower back as he stepped off a ladder. He remained active, relying on over-thecounter ibuprofen and heat packs to relieve soreness. Two days later he visits his physician because the soreness has not abated. He reports no bowel or bladder complaints, worsening of pain, radiation of symptoms, nausea, vomiting, abdominal pain, or fever. He tells his doctor that he strained his back before and that this feels the same way it did before. The last time this happened he received physical therapy (PT), which helped. He thinks he may need PT again, but wants to 180 VOL 58, NO 4 / APRIL _JFP /19/09 10:35:36 AM
2 IMAGE MAURA FLYNN discuss it with his physician. Physical exam reveals mild tenderness to palpation over the right lumbar paraspinal muscle, but no spasms are apparent. Otherwise, his musculoskeletal exam including range-of-motion testing is within normal limits. The neurologic exam also is within normal limits, including normal deep tendon reflexes of the lower extremities and negative straight-leg-raise testing. His gait is normal, with no sign of discomfort. Specific anatomic diagnoses are elusive. In the primary care setting, fewer than 15% of LBP cases have an identifiable underlying disease or spinal abnormality. 4 An exhaustive search for a specific anatomic diagnosis lacks utility in selecting initial therapy or affecting patient outcomes. Instead, when caring for a patient like the one in our case, it s important to focus on a thorough medical history and examination that assess the location and duration of symptoms, as well as uncover symptoms suggestive of radiculopathy or spinal stenosis. Of course, you ll need to rule out potentially serious conditions, such as cancer, vertebral infection, cauda equina syndrome, compression fracture, and ankylosing spondylitis. You ll also need to check for rapidly progressing or severe neurologic deficits, such as motor deficits at more than one level or a patient s report of incontinence or bladder dysfunction. Straight-leg-raise testing and neurologic assessment of the lower extremity specifically strength and reflex testing of the knee, ankle, foot, and great toe to assess nerve foot level involvement are key. With this assessment, you should categorize a patient s LBP as nonspecific, as potentially associated with radiculopathy or spinal stenosis, or as potentially associated with another specific cause (ACP/APS recommendation; strength of recommendation [SOR]: B). 1 Pursue imaging or not? While plain radiography is certainly an option if you suspect a vertebral compression fracture in a high-risk patient, it would not be necessary for a patient like the one in our case. This patient has a classic presentation of acute nonspecific LBP, for which neither routine plain radiography nor advanced imaging (CT or MRI) improves patient outcomes. Given this lack of proven benefit and the unnecessary radiation exposure with certain tests, routine imaging is not recommended for nonspecific LBP (ACP/APS recommendation; SOR: B). 1,4-6 Action steps. The evidence supports a number of steps when caring for a patient like the one in our case. Some steps are targeted to patients with nonspecific LBP and we ve labeled them as such. Others more broadly apply to patients with LBP. Explore the possible contribution of psychosocial factors and emotional distress to back pain (ACP/APS recommendation; SOR: B). 1 These factors are stronger predictors of low back pain outcomes, including chronic back pain disability, than physical exam findings and duration or severity of pain. 7,8 Predictors of poorer outcomes include depression, passive coping strategies, job dissatisfaction, For many patients with herniated discs, symptoms can improve within 4 weeks. Thus, the evidence does not support routine imaging. VOL 58, NO 4 / APRIL _JFP /19/09 10:35:40 AM
3 Evidence does not show that long-term opioid use improves functioning in patients with chronic lower back pain. somatization, higher disability levels, and disputed compensation claims. The effectiveness of specific tools for gathering such information has not been demonstrated in the primary care setting. Therefore, fully investigate psychosocial information in the patient interview. Provide patients with nonspecific LBP with evidence-based information regarding its expected course; advise them to remain active and suggest effective selfcare options (ACP/APS recommendation; SOR: B). 1 This recommendation is based on findings that the typical course and prognosis of LBP are generally favorable, on studies comparing bed rest versus remaining active, and on outcome studies for self-care interventions. Self-care includes a variety of interventions patients can implement without a clinical visit patient education, including self-care books, and patientstructured physical activities. This approach is much less expensive than and has equivalent or nearly equivalent effectiveness to costlier interventions such as physical therapy, massage, spinal manipulation, or acupuncture. Regarding work limitations, there is insufficient evidence for specific guidance. Routinely assess patient age, health, and physical demands and job tasks, and recommend restrictions based on clinical judgment. Try nonpharmacologic therapies that have proven benefits in the event that self-care fails (ACP/APS recommendation; SOR: B). 1 These include spinal manipulation, defined as manual therapy in which loads are applied to the spine by using short- or long-lever methods and high-velocity thrusts are applied to a spinal joint beyond its restricted range of motion. Serious adverse events are extremely rare. 3 If medication is needed for acute LBP, first-line drugs include nonopioids with proven benefits, such as acetaminophen, nonsteroidal anti-inflammatory agents, or skeletal muscle relaxants (ACP/APS recommendation; SOR: B). 2 CASE 1 The patient s course The physician carefully reviews the 32- year-old patient s psychosocial factors and finds that he is positive about his job, enjoys his work, and is not seeking compensation. He uses exercise and prayer to manage stress and is in a stable relationship. He does not smoke, use recreational drugs, or have a history of psychiatric disorders, including depression. He says he drinks 2 to 3 beers on the weekends. In discussing treatment, the patient considers PT as the optimal intervention. His doctor does not recommend it, and instead encourages him to remain active, gives him a self-care booklet on stretching and exercises, and advises him to check in again as needed, reassuring him that most cases of nonspecific acute low back pain resolve spontaneously. Initially the patient does well with self-care and he returns to activity. However, 6 weeks after his office visit, the patient returns with pain that has worsened over the last 2 weeks. He has also begun experiencing tingling sensations down his right leg, trouble standing for short intervals because of pain, and weakness in his back. On physical exam, he still has minimal tenderness to palpation over the right lumbar region. The right straightleg-raise test yields a positive result, and the right patellar reflex is diminished compared with the left. His rectal tone is normal. His gait is antalgic. When the patient requests imaging, the physician advises him of the risks associated with imaging and the unlikely prospect that it will change management despite the change in neurologic symptoms. After considering such evidence-based options as massage therapy, yoga, and spinal manipulation, they agree on a trial of PT. The patient s current level of function is reviewed, and work limitations are set. After 8 weeks of PT, the patient experiences an improvement in overall function, pain level, and weakness. His straight-leg-raise test the physical exam 182 VOL 58, NO 4 / APRIL _JFP /19/09 10:35:48 AM
4 Lower back pain TABLE Recommendations from the ACP/APS guidelines for low back pain 1 Conduct a focused history and exam to place patients into 1 of 3 broad categories: nonspecific LBP, LBP potentially associated with radiculopathy or spinal stenosis, or LBP associated with another specific cause (strength of recommendation [SOR]: B). Assess for psychosocial factors and emotional distress, as they are stronger predictors of LBP outcomes, including disability, than physical exam findings and severity of pain (SOR: B). Do not routinely obtain imaging for patients with nonspecific LBP. MRI or CT is recommended for patients with LBP associated with a specific cause, for those with severe or progressive neurologic deficits or persistent radiculopathy/spinal stenosis symptoms, and for those who are candidates for surgical interventions (SOR: B). Advise patients with nonspecific LBP to remain active and provide information on LBP s expected course and effective self-care options (SOR: B). Consider the addition of nonpharmacologic treatments, including selective alternative modalities, when self-care fails. These treatments include spinal manipulation for acute LBP and acupuncture for chronic LBP (SOR: B). Consider acetaminophen or nonsteroidal anti-inflammatory drugs as first-line medication options for most patients. Keep in mind the limited effectiveness and potential harm of others, including opioids (SOR: B). Strength of recommendation (SOR) A Good-quality patient-oriented evidence B Inconsistent or limited-quality patient-oriented evidence C Consensus, usual practice, opinion, disease-oriented evidence, case series finding with the most sensitivity for disc herniation returns to normal, as does his patellar reflex. Although frustrated with the length of recovery time, he is appreciative of his physician and therapists. Follow this physician s lead: Be prudent with imaging. Many primary care physicians caring for a patient like this one would consider imaging studies to assess the worsening signs and symptoms. The evidence, however, does not clearly support that decision. Given the potential harm of testing and varying benefit in outcomes, the ACP/APS offers different recommendations on imaging and other diagnostic tests, depending on the category of LBP. Prompt evaluation with advanced imaging (MRI or CT) is recommended for severe or progressive neurologic deficits, and with suspicion of a serious underlying condition, such as vertebral infection, cauda equine syndrome, or cancer with spinal cord compression, given that delayed treatment may lead to poor outcomes (ACP/APS recommendation; SOR: B). 1 For many patients with herniated lumbar discs, symptoms can improve within 4 weeks. 9,10 Thus, there is no compelling evidence that routine imaging changes treatment decisions or outcomes. 11 For patients with persistent symptoms of radiculopathy or spinal stenosis who have not responded to conservative therapy, invasive procedures (surgery or epidural injections) become potential treatment options, and thus imaging with MRI (preferred) or CT may be warranted. CASE 2 Patient with chronic LBP A 48-year-old man new to the practice comes in complaining of persistent pain in the lower back, which he ranks at 6 on a scale of 1 to 10. Approximately 5 years ago he underwent an L4-L5 laminectomy/fusion for herniated nucleus pulposus. The surgery relieved shooting pains Acupuncture, cognitivebehavioral therapy, physical therapy, exercise therapy, and therapeutic massage all help patients with chronic lower back pain. VOL 58, NO 4 / APRIL _JFP /19/09 10:35:52 AM
5 Psychosocial factors are better predictors of treatment outcomes than physical findings. down his left leg, but he has since had progressive problems with lumbar pain and stiffness. Two courses of PT and a series of facet joint injections over the years have provided only temporary relief. The patient had been followed by a pain management clinic, but was discharged after exhausting his insurance benefit. A recent MRI ordered by the pain management clinic showed mild to moderate degenerative changes in L2 to S1 with a healed fusion. The reason for his visit this day is to request a refill of his hydrocodone, initiated by the pain clinic. He is worried that he will not get better and is afraid of injuring himself and has, as a result, been avoiding activities. He denies depressive symptoms except for decreased self-worth and pain-related sleep disturbance. He says that he was once more vigorous and felt competent, but is now passive and feels helpless about his pain. He is concerned that his physical capabilities will worsen even more and asks if there are any other therapies that might be helpful. No easy answers. Patients with chronic LBP pain lasting for longer than 2 months present unique challenges. They have often seen several clinicians, including pain management specialists, have undergone repeated imaging, and are frustrated by their persistent symptoms. Many have had 1 or more surgeries, and most have tried numerous medications to gain relief. This patient is seeking a refill of his opioid. Before agreeing to such a request, weigh the risks and benefits of opioids and the potential benefits of alternative therapies (SOR: B). 1 Although the chronic use of opioids is an option for a select group of patients with chronic LBP, 12 these agents can be expensive, lead to habituation and addiction, be easily redirected for monetary gain, and have untoward side effects. Evidence does not show that long-term opioid use improves functioning in patients with chronic LBP. Nonpharmacologic therapies that have proven beneficial for such patients include acupuncture, cognitive-behavioral therapy, PT, exercise therapy (defined as any supervised or formal exercise program), and therapeutic massage (SOR: B). 1 It would be preferable to start a therapeutic plan incorporating 1 or more of these modalities, based on a patient s psychosocial history, insurance status, and preferences. Suggesting these therapies with guarded optimism can lead to a decreased need for opioids and increased functioning. Again, psychosocial evaluation is important. When initially assessing a patient with chronic LBP, it is imperative to evaluate psychosocial factors. As noted earlier, psychosocial factors are better predictors of treatment outcomes than physical findings. Identifying factors related to poor outcomes (eg, anxiety, poor work history, passive attitude toward rehabilitation) can direct therapy and avoid polypharmacy. Cognitive-behavioral and educational interventions will be more effective when targeting specific psychological and social factors (SOR: C). 13,14 Fearavoidance beliefs, distress, somatization, and pain catastrophizing place patients at the highest risk for poor outcomes. Primary objectives in psychosocial intervention are providing encouragement for overcoming demoralization; helping the patient make the connection between thoughts, feelings, and behaviors; and teaching the patient coping strategies and techniques to adapt to pain and resultant problems. The ultimate goal for a patient like the one in this second case is to change his perception of chronic pain from overwhelming to manageable and to get him to see himself as resourceful and competent. 15 Physician counseling has produced small positive effects in undifferentiated primary care patients with LBP, and it may therefore be more powerful when targeted to patients with specific psychosocial issues such as fear avoidance VOL 58, NO 4 / APRIL _JFP /19/09 10:35:57 AM
6 Lower back pain Provide patients with a realistic outlook. Another key element is to direct patients expectations. Most people with chronic LBP will not become pain free, and patients need to know this fact. Aim treatment at improving function as well as reducing pain. You can assess functional status and improvement using patient questionnaires such as the Roland-Morris Disability Questionnaire ( rmdq.org/) or the Oswestry Disability Index 2.0 (ODI, resources/measurement%20tools/ Evaluative_Oswestry%20Disability% 20Index.doc). 17,18 Although these measures have not demonstrated utility in primary care practice, they have sufficient scale width to reliably detect change in most patients, and serial use can measure change clinically. These measures are used in research examining LBP functional outcomes in primary care; they are easy to use and score (SOR: C). 19 What role for medications? Because of complex trade-offs between benefits and harms, evidence is insufficient to say one medication offers a clear net advantage over others in the treatment of patients with LBP. ACP/APS has identified good evidence for tricyclic antidepressants in chronic LBP (ACP/APS recommendation; SOR: B). 2 Chronic LBP may exhibit periods of relative quiescence alternating with episodes of exacerbation. 20 You can assist your patients in preparing for these occurrences. As with exacerbations in other conditions (eg, chronic obstructive pulmonary disease), you may want to prescribe short-term use of nonpharmacologic or pharmacologic therapies that can be tapered and discontinued after the exacerbation subsides. Patients are likely to differ in how they weigh potential benefits, harms, and cost of various medications. Such a strategy should limit financial burden and potential negative side effects of chronic therapy. CASE 2 The patient s course The physician offers to partner with the patient in working toward a goal of improved functioning. The patient s spouse accompanies him on 1 visit to discuss steps the family can take to improve fitness. With the ODI, the physician establishes the patient s baseline function and tracks improvement over the period of care. The patient receives clinical massage therapy once a week, and his hydrocodone is tapered over the course of 6 visits. At the end of the period of care, the patient reports decreased pain and improved hopefulness. Correspondence William G. Elder Jr, PhD, University of Kentucky, K309 Kentucky Clinic, Lexington, KY 40536; welder@pop.uky. edu Disclosure The authors reported no potential conflicts of interest relevant to this article. Acknowledgements The authors thank Honey Elder for organizing our work on this article and for her editorial assistance. Our efforts were supported in part by Grant Number R25 AT00682 from the National Institutes of Health (NIH). Contents are solely the responsibility of the authors and do not necessarily represent the official views of NIH. References 1. Chou R, Qaseen A, Snow V, et al. Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society. Ann Intern Med. 2007;147: Chou R, Huffman LH. Medications for acute and chronic low back pain: a review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline. Ann Intern Med. 2007;147: Chou R, Huffman LH. Nonpharmacologic therapies for acute and chronic low back pain: a review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline. Ann Intern Med. 2007;147: Van Tudler MW, Assendelft WJ, Koes BW, et al. Spinal radiographic findings and nonspecific low back pain. A systematic review of observational studies. Spine. 1997;22: Kerry S, Hilton S, Dundas D, et al. Radiography for low back pain: a randomised controlled trial and observational study in primary care. Br J Gen Pract. 2002;52: Jarvik JG. Imaging of adults with low back pain in the primary care setting. Neuroimaging Clin N Am. 2003;13: Gilbert F, Grant A, Gillan M, et al. Scottish Back Trial Group. Low back pain: influence of early MR imaging or CT on treatment and outcome multicenter randomized trial. Radiology. 2004;231: CONTINUED Most people with chronic lower back pain will not become pain free, and patients need to know this fact. VOL 58, NO 4 / APRIL _JFP /19/09 10:36:01 AM
7 Recommend Zucol to to treat URTI s with with the the proven effective, safe, safe, natural choice. FAST, FAST, EFFECTIVE RELIEF of upper of upper respiratory tract tract infections related related to the to the common common cold. cold. NATURALLY SAFE SAFE NO NO DRUG DRUG INTERACTIONS CLINICALLY PROVEN MEDICINE Reduce Reduce duration and and severity of URTI s of URTI s More More than than studies Proven Proven effective for: for: Bronchitis Bronchitis Sinusitis Sinusitis Tonsillitis Tonsillitis Leading medicine in Europe in Europe widely widely prescribed prescribed by physicians by physicians and and pharmacists Clinically Clinically Proven Proven Naturally Naturally Safe Safe STOPS THE THE COLD BEFORE IT IT TAKES HOLD 8. Pengel LH, Herbert RD, Maher CG, et al. Acute low back pain: systematic review of its prognosis. BMJ. 2003;327: Fayad F, Lefevre-Colau MM, Poiraudeau S, et al. Chronicity, recurrence, and return to work in low back pain: common prognostic factors. Ann Readapt Med Phys. 2004;47: [In French] 10. Vroomen PC, de Krom MC, Knottnerus JA. Predicting the outcome of sciatica at short-term follow-up. Br J Gen Pract. 2002;52: Weber H. Lumbar disc herniation. A controlled, prospective study with ten years of observation. Spine. 1983;8: Modic MT, Obuchowski NA, Ross JS, et al. Acute low back pain and radiculopathy: MR imaging findings and their prognostic role and effect on outcome. Radiology. 2005;237: Dillie KS, Fleming MF, Mundt MP, et al. Quality of life associated with daily opioid therapy in a primary care chronic pain sample. J Am Board Fam Med. 2008;21: Dance KA, Neufeld RW. Aptitude treatment interaction research in the clinical setting: a review of attempts to dispel the patient uniformity myth. Psychol Bull. 1988;104: Jellema P, Van der Horst HE, Vlaeyen JW, et al. Predictors of outcome in patients with (sub) acute low back pain differ across treatment groups. Spine. 2006;31: Main CJ, Sullivan MJ, Watson PJ, eds. Pain Management: Practical Applications of the Biopsychosocial Perspective in Clinical and Occupational Settings. 2nd ed. Edinburgh, Scotland: Churchill Livingstone; Van der Windt D, Hay E, Jellema P, et al. Psychosocial interventions for low back pain in primary care: Lessons learned from recent trials. Spine. 2008;33: Roland M, Fairbank J. The Roland-Morris Disability Questionnaire and the Oswestry Disability Questionnaire. Spine. 2000;25: Lauridsen HH, Hartvigsen J, Manniche C, et al. Responsiveness and minimal clinically important difference for pain and disability instruments in low back pain patients. BMC Musculoskelet Disord. 2006;7: Resnik L, Dobrykowski E. Outcomes measurement for patients with low back pain. Orthop Nurs. 2005;24: Please take a moment to share your opinion! We want to hear from you! Have a comment? Drop us a line and let us know what you think. You can send a letter 1 of 3 ways. 1 jfp@fammed.uc.edu 2 Fax Mail The Journal of Family Practice 110 Summit Ave. Montvale, NJ Letters should be addressed to the Editor, The Journal of Family Practice, and be 200 words or less. They may be edited prior to publication. c 2008 c Abkit, 2008 Abkit, Inc. Inc. 186_JFP /19/09 10:36:05 AM
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society
 Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
A Patient s Guide to Treatment Guidelines for Low Back Pain
 A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Treatment Guidelines for Low Back Pain 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled
Critical Appraisal of a Clinical Practice Guideline
 Critical Appraisal of a Clinical Practice Guideline Goal: To critically evaluate a guideline, using the Users Guides (reference below). Objectives: 1. Assess the validity of a guideline 2. Understand the
Critical Appraisal of a Clinical Practice Guideline Goal: To critically evaluate a guideline, using the Users Guides (reference below). Objectives: 1. Assess the validity of a guideline 2. Understand the
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
CLINICAL GUIDELINES. Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision
 CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
Disclosure Statement of Financial Interest. Evidence Based Evaluation and. Learning Objectives. What is Low Back Pain?
 Disclosure Statement of Financial Interest Evidence Based Evaluation and Management of Low Back Pain June 28, 2013 St. Charles Medical Center Summer Boslaugh and Alison Little DO NOT have a financial interest/arrangement
Disclosure Statement of Financial Interest Evidence Based Evaluation and Management of Low Back Pain June 28, 2013 St. Charles Medical Center Summer Boslaugh and Alison Little DO NOT have a financial interest/arrangement
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Chiropractic Health Plan - Diagnosis of Low Back Pain
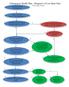 Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
What Is Back Pain? Fast Facts: An Easy-to-Read Series of Publications for the Public. Who Gets Back Pain? What Are the Causes of Back Pain?
 Back pain can range from a dull, constant ache to a sudden, sharp pain that makes it hard to move. It can start quickly if you fall or lift something too heavy, or it can get worse slowly. Who Gets Back
Back pain can range from a dull, constant ache to a sudden, sharp pain that makes it hard to move. It can start quickly if you fall or lift something too heavy, or it can get worse slowly. Who Gets Back
Hailee Gibson, CCPA Neurosurgery Physician Assistant. Windsor Neurosurgery & Spine Associates. Windsor Regional Hospital Ouellette Campus
 Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
What Is Back Pain? Can Back Pain Be Prevented? When Should I See a Doctor for Pain? How Is Back Pain Diagnosed?
 What Is Back Pain? Back pain can also occur with some conditions and diseases, such as: Scoliosis Spondylolisthesis Arthritis Spinal stenosis Pregnancy Kidney stones Infections Endometriosis Fibromyalgia.
What Is Back Pain? Back pain can also occur with some conditions and diseases, such as: Scoliosis Spondylolisthesis Arthritis Spinal stenosis Pregnancy Kidney stones Infections Endometriosis Fibromyalgia.
COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C. Dr. John Kirkpatrick
 COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C Dr. John Kirkpatrick Investigation Committee C of the College of Physicians and Surgeons of Nova Scotia
COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C Dr. John Kirkpatrick Investigation Committee C of the College of Physicians and Surgeons of Nova Scotia
LOTHIAN LUMBAR SPINE PATHWAYS
 LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY. Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group
 IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
LOW BACK PAIN EPIDEMIOLOGY:
 LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Are you getting the best treatment for your low back pain?
 Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
The evidence for SMT in CLBP
 The evidence for SMT in CLBP Peter Tuchin BSc, GradDipChiro, DipOHS PhD FACC Associate Professor, MU (1991 - ) Past President, COCA 1 Peter Tuchin Peter Tuchin 2 WCA 2007 Peter Tuchin 3 Number of injuries
The evidence for SMT in CLBP Peter Tuchin BSc, GradDipChiro, DipOHS PhD FACC Associate Professor, MU (1991 - ) Past President, COCA 1 Peter Tuchin Peter Tuchin 2 WCA 2007 Peter Tuchin 3 Number of injuries
YOU ARE THE BEST OPTION FOR LOW BACK PAIN
 YOU ARE THE BEST OPTION FOR LOW BACK PAIN Amy Garrigues PT, DPT Orthopaedic Clinical Specialist Fellow, American Academy of Orthopaedic and Manual Physical Therapists LBP in past 3 months 25% 307% 220%
YOU ARE THE BEST OPTION FOR LOW BACK PAIN Amy Garrigues PT, DPT Orthopaedic Clinical Specialist Fellow, American Academy of Orthopaedic and Manual Physical Therapists LBP in past 3 months 25% 307% 220%
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia
 Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Regional Pain Syndromes: Neck and Low Back
 Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Managing back pain a new approach
 Managing back pain a new approach David Rogers Clinical Lead Functional Restoration Service Extended Scope Physiotherapist Royal Orthopaedic Hospital Setting the scene Back pain is one of the most common
Managing back pain a new approach David Rogers Clinical Lead Functional Restoration Service Extended Scope Physiotherapist Royal Orthopaedic Hospital Setting the scene Back pain is one of the most common
Back Pain Update. Steven Andersen, MD Providence Physiatry Clinic 2016
 Back Pain Update Steven Andersen, MD Providence Physiatry Clinic 2016 Back Pain is Very Common Lifetime prevalence 80% 12 month prevalence 40% Point prevalence 20% Centers for Disease Control and Prevention.
Back Pain Update Steven Andersen, MD Providence Physiatry Clinic 2016 Back Pain is Very Common Lifetime prevalence 80% 12 month prevalence 40% Point prevalence 20% Centers for Disease Control and Prevention.
Wendy Field Advanced Physiotherapy Practitioner June 2018
 Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers
 In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
Thoracolumbar Spine Conditions: Treatment and Return to Play
 Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
MUSCULOSKELETAL PROGRAM OF CARE
 MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
MEMORANDUM 377/87. DATE: April 5, 1988 TO: ALL WCAT STAFF SUBJECT: DECISION NO. 377/87
 MEMORANDUM 377/87 DATE: April 5, 1988 TYPE: A TO: ALL WCAT STAFF SUBJECT: DECISION NO. 377/87 Aggravation (preexisting condition) (degenerative disc disease) - Disc, herniated (L4-5). - Bricklayer not
MEMORANDUM 377/87 DATE: April 5, 1988 TYPE: A TO: ALL WCAT STAFF SUBJECT: DECISION NO. 377/87 Aggravation (preexisting condition) (degenerative disc disease) - Disc, herniated (L4-5). - Bricklayer not
Back Pain and Emotional Distress
 Back Pain and Emotional Distress North American Spine Society Public Education Series Common Reactions to Back Pain Four out of five adults will experience an episode of significant back pain sometime
Back Pain and Emotional Distress North American Spine Society Public Education Series Common Reactions to Back Pain Four out of five adults will experience an episode of significant back pain sometime
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 111/07
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 111/07 BEFORE: S. Ryan: Vice-Chair HEARING: January 15, 2007 at Toronto Written DATE OF DECISION: January 17, 2007 NEUTRAL CITATION: 2007 ONWSIAT
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 111/07 BEFORE: S. Ryan: Vice-Chair HEARING: January 15, 2007 at Toronto Written DATE OF DECISION: January 17, 2007 NEUTRAL CITATION: 2007 ONWSIAT
Cox Technic Case Report #126 published at (sent December 2013 ) 1
 Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
Emergency Triage System for Back Pain
 Emergency Triage System for Back Pain Andrew J. Haig, M.D. Haig et al., Consulting The University of Michigan Physical Medicine and Rehabilitation Haig Disclosures Haig et al., Consulting helps hospitals,
Emergency Triage System for Back Pain Andrew J. Haig, M.D. Haig et al., Consulting The University of Michigan Physical Medicine and Rehabilitation Haig Disclosures Haig et al., Consulting helps hospitals,
Herniated Disk in the Lower Back
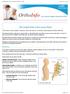 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Mr. LBP: Case Presentation
 CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
CLINICAL CASES Case: Mr. LBP Mr. LBP: Case Presentation Mr. LBP is a 35-year-old male He fell down while participating in a recreational sports activity He subsequently developed low back pain Upon arrival
An Osteopathic Approach to Low Back Pain. Ryan Seals DO Interim Chair of Family Medicine and OMM
 An Osteopathic Approach to Low Back Pain Ryan Seals DO Interim Chair of Family Medicine and OMM Objectives Review Osteopathic Philosophy and Principles Discuss how somatic dysfunction influences low back
An Osteopathic Approach to Low Back Pain Ryan Seals DO Interim Chair of Family Medicine and OMM Objectives Review Osteopathic Philosophy and Principles Discuss how somatic dysfunction influences low back
What guidelines are available for sciatica and radicular pain?
 Chapter 5 What guidelines are available for sciatica and radicular pain? Paolo Marchettini Guidelines for the management of low back pain (LBP) and lumbar or cervical radiculopathy resulting from sciatica
Chapter 5 What guidelines are available for sciatica and radicular pain? Paolo Marchettini Guidelines for the management of low back pain (LBP) and lumbar or cervical radiculopathy resulting from sciatica
DOCTOR DISCUSSION GUIDE
 DOCTOR DISCUSSION GUIDE BE PREPARED For the best outcome from a visit with your doctor, it s important to be prepared. The more completely and clearly you describe the pain you re experiencing, the easier
DOCTOR DISCUSSION GUIDE BE PREPARED For the best outcome from a visit with your doctor, it s important to be prepared. The more completely and clearly you describe the pain you re experiencing, the easier
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice
 The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
What is the role of imaging in acute low back pain?
 Curr Rev Musculoskelet Med (2009) 2:69 73 DOI 10.1007/s12178-008-9037-0 What is the role of imaging in acute low back pain? Humaira Lateef Æ Deepak Patel Published online: 28 April 2009 Ó The Author(s)
Curr Rev Musculoskelet Med (2009) 2:69 73 DOI 10.1007/s12178-008-9037-0 What is the role of imaging in acute low back pain? Humaira Lateef Æ Deepak Patel Published online: 28 April 2009 Ó The Author(s)
North American Spine Society Public Education Series
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Piriformis Syndrome. Midwest Bone & Joint Institute 2350 Royal Boulevard Suite 200 Elgin, IL Phone: Fax:
 A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Chapter 35 Back Pain. Episode overview: Wisecracks: Crack Cast Show Notes Back Pain July 2016
 Chapter 35 Back Pain Episode overview: 1) List 10 historical red flags for back pain 2) List 6 Emergent Diagnosis for back pain Wisecracks: 1) Describe the most common sites of disc protrusion with their
Chapter 35 Back Pain Episode overview: 1) List 10 historical red flags for back pain 2) List 6 Emergent Diagnosis for back pain Wisecracks: 1) Describe the most common sites of disc protrusion with their
Adult Isthmic Spondylolisthesis
 Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
Session Objectives. Why We Need to Diagnose 4/2/18. Diagnosis: Defining the Patient Problem A prerequisite for treatment
 Diagnosis: Defining the Patient Problem A prerequisite for treatment Marcia Spoto PT, DC, OCS Nazareth College of Rochester Session Objectives 1. Appreciate the role of Physical Therapist (PT) diagnosis
Diagnosis: Defining the Patient Problem A prerequisite for treatment Marcia Spoto PT, DC, OCS Nazareth College of Rochester Session Objectives 1. Appreciate the role of Physical Therapist (PT) diagnosis
DECISION Keith G. Barry Review Commissioner
 WORKPLACE HEALTH, SAFETY & COMPENSATION REVIEW DIVISION 6 Mt. Carson Ave., Dorset Building Mt. Pearl, NL A1N 3K4 DECISION 13213 Keith G. Barry Review Commissioner October 2013 WORKPLACE HEALTH, SAFETY
WORKPLACE HEALTH, SAFETY & COMPENSATION REVIEW DIVISION 6 Mt. Carson Ave., Dorset Building Mt. Pearl, NL A1N 3K4 DECISION 13213 Keith G. Barry Review Commissioner October 2013 WORKPLACE HEALTH, SAFETY
A M E R I C A N A R B I T R A T I O N A S S O C I A T I O N NO-FAULT/ACCIDENT CLAIMS AWARD OF DISPUTE RESOLUTION PROFESSIONAL
 CASE NO. 18 Z 600 17449 03 2 A M E R I C A N A R B I T R A T I O N A S S O C I A T I O N NO-FAULT/ACCIDENT CLAIMS In the Matter of the Arbitration between (Claimant) AAA CASE NO.: 18 Z 600 17449 03 v.
CASE NO. 18 Z 600 17449 03 2 A M E R I C A N A R B I T R A T I O N A S S O C I A T I O N NO-FAULT/ACCIDENT CLAIMS In the Matter of the Arbitration between (Claimant) AAA CASE NO.: 18 Z 600 17449 03 v.
What is a Chiropractic Treatment?
 What is a Chiropractic Treatment? Have you ever been to the Chiropractor? Do you know exactly what to expect when you visit one? Well, here is a complete and thorough guide for you to understand exactly
What is a Chiropractic Treatment? Have you ever been to the Chiropractor? Do you know exactly what to expect when you visit one? Well, here is a complete and thorough guide for you to understand exactly
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F GNB TECHNOLOGIES (EXIDE) ZURICH AMERICAN INS. CO.
 BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F011769 JOE GILL GNB TECHNOLOGIES (EXIDE) ZURICH AMERICAN INS. CO. INSURANCE CARRIER CLAIMANT RESPONDENT RESPONDENT OPINION FILED OCTOBER
BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. F011769 JOE GILL GNB TECHNOLOGIES (EXIDE) ZURICH AMERICAN INS. CO. INSURANCE CARRIER CLAIMANT RESPONDENT RESPONDENT OPINION FILED OCTOBER
Corporate Medical Policy
 Corporate Medical Policy Spinal Manipulation under Anesthesia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_manipulation_under_anesthesia 5/1998 10/2018 10/2019 10/2018
Corporate Medical Policy Spinal Manipulation under Anesthesia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_manipulation_under_anesthesia 5/1998 10/2018 10/2019 10/2018
Studies in Pain Management JAMES HUDSON, MD
 Studies in Pain Management JAMES HUDSON, MD Basics: How do I do this? What providers ask most: How do I get patients off opioids? Two Groups 1. Most chronic pain patients aren t on opioids. The ones that
Studies in Pain Management JAMES HUDSON, MD Basics: How do I do this? What providers ask most: How do I get patients off opioids? Two Groups 1. Most chronic pain patients aren t on opioids. The ones that
Agenda. Oregon Health Plan Back Pain Coverage Changes
 Oregon Health Plan Back Pain Coverage Changes Effective July 1, 2016 Alison Little, MD, MPH Medical Director, Medicaid, PacificSource Community Solutions PR3755_06202016 Agenda History Evidence on treatment
Oregon Health Plan Back Pain Coverage Changes Effective July 1, 2016 Alison Little, MD, MPH Medical Director, Medicaid, PacificSource Community Solutions PR3755_06202016 Agenda History Evidence on treatment
BACK PAIN. Disclaimer. Integrated web marketing. Multimedia Health Education
 BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
BACK PAIN Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or a licensed healthcare
Objectives. Identify and differentiate appropriate surgical cases. Good Surgical Outcomes
 ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
CERVICAL STRAIN AND SPRAIN
 CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN (Whiplash)
 CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
Quality Standards. Low Back Pain Care for Adults With Acute Low Back Pain. April 2018
 Quality Standards Low Back Pain Care for Adults With Acute Low Back Pain April 2018 Draft do not cite. Report is a work in progress and could change following public consultation. Summary This quality
Quality Standards Low Back Pain Care for Adults With Acute Low Back Pain April 2018 Draft do not cite. Report is a work in progress and could change following public consultation. Summary This quality
NOT DESIGNATED FOR PUBLICATION BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. G ROBERT D. MILLER, EMPLOYEE
 NOT DESIGNATED FOR PUBLICATION BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. G009055 ROBERT D. MILLER, EMPLOYEE NORTH ARKANSAS REGIONAL MEDICAL CENTER, EMPLOYER CENTRAL ADJUSTMENT COMPANY,
NOT DESIGNATED FOR PUBLICATION BEFORE THE ARKANSAS WORKERS' COMPENSATION COMMISSION CLAIM NO. G009055 ROBERT D. MILLER, EMPLOYEE NORTH ARKANSAS REGIONAL MEDICAL CENTER, EMPLOYER CENTRAL ADJUSTMENT COMPANY,
Corporate Medical Policy
 Corporate Medical Policy Spinal Manipulation under Anesthesia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_manipulation_under_anesthesia 5/1998 11/2017 11/2018 11/2017
Corporate Medical Policy Spinal Manipulation under Anesthesia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: spinal_manipulation_under_anesthesia 5/1998 11/2017 11/2018 11/2017
SUMMARY DECISION NO. 529/97. Recurrences (compensable injury).
 SUMMARY DECISION NO. 529/97 Recurrences (compensable injury). The worker suffered a low back injury in 1984. The worker appealed a decision of the Appeals Officer denying entitlement for recurrences in
SUMMARY DECISION NO. 529/97 Recurrences (compensable injury). The worker suffered a low back injury in 1984. The worker appealed a decision of the Appeals Officer denying entitlement for recurrences in
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 776/15
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 776/15 BEFORE: S. Netten: Vice-Chair HEARING: April 21, 2015 at Toronto Written DATE OF DECISION: May 1, 2015 NEUTRAL CITATION: 2015 ONWSIAT
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 776/15 BEFORE: S. Netten: Vice-Chair HEARING: April 21, 2015 at Toronto Written DATE OF DECISION: May 1, 2015 NEUTRAL CITATION: 2015 ONWSIAT
A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT
 LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
If you have a condition that compresses your nerves, causing debilitating back pain or numbness along the back of your leg.
 Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
Below, we have provided some basic information for your benefit. Please use this information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk
REVIEW OF LITERATURE BMJ 2007; 334(7607): Diagnosis and treatment of sciatica. Bart W. Koes Maurits W. van Tulder Wilco C.
 2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
2 REVIEW OF LITERATURE Diagnosis and treatment of sciatica Bart W. Koes Maurits W. van Tulder Wilco C. Peul BMJ 2007; 334(7607):1313-1317 22 CHAPTER 2 DIAGNOSIS AND TREATMENT OF SCIATICA 23 INTRODUCTION
CLEVELAND CLINIC BACK AND NECK CENTERS. Comprehensive Care for Back and Neck Problems Tips to Help You Maintain a Healthy Back
 CLEVELAND CLINIC BACK AND NECK CENTERS Comprehensive Care for Back and Neck Problems Tips to Help You Maintain a Healthy Back Back to normal Nearly everyone experiences back or neck pain at some time during
CLEVELAND CLINIC BACK AND NECK CENTERS Comprehensive Care for Back and Neck Problems Tips to Help You Maintain a Healthy Back Back to normal Nearly everyone experiences back or neck pain at some time during
NICE guideline Published: 30 November 2016 nice.org.uk/guidance/ng59
 Low back pain and sciatica in over 16s: assessment and management NICE guideline Published: 30 November 2016 nice.org.uk/guidance/ng59 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Low back pain and sciatica in over 16s: assessment and management NICE guideline Published: 30 November 2016 nice.org.uk/guidance/ng59 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Hiroyuki Hayashi The benefit of Manual Osteopath treatment effect for lower back pain
 The benefit of Manual Osteopath treatment effect for lower back pain 1. What is the Manual Osteopath? Osteopathy is a type of alternative medicine and is a form of drug-free non-invasive manual medicine
The benefit of Manual Osteopath treatment effect for lower back pain 1. What is the Manual Osteopath? Osteopathy is a type of alternative medicine and is a form of drug-free non-invasive manual medicine
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY
 Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
Scoliosis. This leaflet gives you information on scoliosis and what you can do to help manage the symptoms you are experiencing.
 Scoliosis This leaflet gives you information on scoliosis and what you can do to help manage the symptoms you are experiencing. What is Scoliosis? The term scoliosis refers to the abnormal twisting and
Scoliosis This leaflet gives you information on scoliosis and what you can do to help manage the symptoms you are experiencing. What is Scoliosis? The term scoliosis refers to the abnormal twisting and
History of Present Condition
 Name: Date: Address: City: Province: Postal Code: Home Phone: Cell Phone: Work Phone: Email: Marital Status: Name Of Family Physician (MD): Age: Occupation: Employer: Extended Health Care Company: Policy
Name: Date: Address: City: Province: Postal Code: Home Phone: Cell Phone: Work Phone: Email: Marital Status: Name Of Family Physician (MD): Age: Occupation: Employer: Extended Health Care Company: Policy
LUMBAR SPINE CASE 3. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1. L4-5, 5-S1 disc, facet (somatic)
 LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
The Psychology of Pain within the Biological Model. Michael Coupland, CPsych, CRC Integrated Medical Case Solutions (IMCS Group)
 The Psychology of Pain within the Biological Model Michael Coupland, CPsych, CRC Integrated Medical Case Solutions (IMCS Group) Integrated Medical Case Solutions National Panel of Psychologists Biopsychosocial
The Psychology of Pain within the Biological Model Michael Coupland, CPsych, CRC Integrated Medical Case Solutions (IMCS Group) Integrated Medical Case Solutions National Panel of Psychologists Biopsychosocial
Chiropractic Healthcare. What, How, & Why
 Chiropractic Healthcare What, How, & Why Table of Contents Introduction 3 Topics Why Should Anyone go to a Chiropractor? 4 What to Expect on Your First Visit 7 Chiropractic and Exercise: Better than Drugs
Chiropractic Healthcare What, How, & Why Table of Contents Introduction 3 Topics Why Should Anyone go to a Chiropractor? 4 What to Expect on Your First Visit 7 Chiropractic and Exercise: Better than Drugs
Low Back Pain Optimal Management in General Practice
 Low Back Pain Optimal Management in General Practice Dr Neil Hearnden Musculoskeletal Physician M.B. B.S. FRACGP. Grad Dip Musculoskeletal.Med. (Otago) MAFMM Arana Hills Medical Centre Brisbane Outcome
Low Back Pain Optimal Management in General Practice Dr Neil Hearnden Musculoskeletal Physician M.B. B.S. FRACGP. Grad Dip Musculoskeletal.Med. (Otago) MAFMM Arana Hills Medical Centre Brisbane Outcome
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Interventional Pain Management
 Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Why Focus on Low Back Pain? Care Pathway Roles and Responsibilities. The following table describes general role and responsibilities.
 Low Back Pain This CPM presents a model of care based on scientific evidence available at the time of publication. It is not a prescription for every physician or every patient, nor does it replace clinical
Low Back Pain This CPM presents a model of care based on scientific evidence available at the time of publication. It is not a prescription for every physician or every patient, nor does it replace clinical
Low Back Pain in the Athlete Steven E. Mayer, MD Northwestern Medicine Physical Medicine and Rehabilitation Sports Medicine
 Low Back Pain in the Athlete Steven E. Mayer, MD Northwestern Medicine Physical Medicine and Rehabilitation Sports Medicine When to Play and When to Sit Controversial Based on clinical/expert opinion Current
Low Back Pain in the Athlete Steven E. Mayer, MD Northwestern Medicine Physical Medicine and Rehabilitation Sports Medicine When to Play and When to Sit Controversial Based on clinical/expert opinion Current
Common neuromusculoskeletal disorders in the workplace W. Shane Journeay, PhD, MD, MPH, FRCPC, BC-OEM
 Common neuromusculoskeletal disorders in the workplace W. Shane Journeay, PhD, MD, MPH, FRCPC, BC-OEM OEMAC Calgary September 23, 2018 OBJECTIVES 1. To name key diagnoses of neuromusculoskeletal conditions
Common neuromusculoskeletal disorders in the workplace W. Shane Journeay, PhD, MD, MPH, FRCPC, BC-OEM OEMAC Calgary September 23, 2018 OBJECTIVES 1. To name key diagnoses of neuromusculoskeletal conditions
Paul Allan Regional Clinical Lead - South. Lumbar Spine. Assessment & Differential Diagnosis
 Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1041/16
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1041/16 BEFORE: K. Iima: Vice-Chair HEARING: April 20, 2016 at Toronto Written DATE OF DECISION: July 8, 2016 NEUTRAL CITATION: 2016 ONWSIAT
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1041/16 BEFORE: K. Iima: Vice-Chair HEARING: April 20, 2016 at Toronto Written DATE OF DECISION: July 8, 2016 NEUTRAL CITATION: 2016 ONWSIAT
Post-op / Pre-op Page (ALREADY DONE)
 Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment
 ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment This booklet was created to help you learn about tapering. You probably have lots
ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment This booklet was created to help you learn about tapering. You probably have lots
HealthPartners Inspire Special Needs Basic Care Clinical Care Planning and Resource Guide CHRONIC PAIN
 The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Neurological Disorders and Stroke), Mount Sinai Beth Israel
The following evidence based guideline was used in developing this clinical care guide: National Institute of Health (NIH National Institute of Neurological Disorders and Stroke), Mount Sinai Beth Israel
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis
 Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
DECISION Lloyd Piercey. Review Commissioner
 WORKPLACE HEALTH, SAFETY & COMPENSATION REVIEW DIVISION 6 Mt. Carson Ave., Dorset Building Mt. Pearl, NL A1N 3K4 DECISION 13028 Lloyd Piercey Review Commissioner February 2013 WORKPLACE HEALTH, SAFETY
WORKPLACE HEALTH, SAFETY & COMPENSATION REVIEW DIVISION 6 Mt. Carson Ave., Dorset Building Mt. Pearl, NL A1N 3K4 DECISION 13028 Lloyd Piercey Review Commissioner February 2013 WORKPLACE HEALTH, SAFETY
Understanding your spine and how it works can help you better understand low back pain.
 Low Back Pain Almost everyone will experience low back pain at some point in their lives. This pain can vary from mild to severe. It can be short-lived or long-lasting. However it happens, low back pain
Low Back Pain Almost everyone will experience low back pain at some point in their lives. This pain can vary from mild to severe. It can be short-lived or long-lasting. However it happens, low back pain
VacuPractor Technique for Low Back Pain Relief
 VacuPractor Technique for Low Back Pain Relief Protocol for Using the VacuPractor General Information Lower back pain is a common condition that affects 84% of adults at some point in their lives (1).
VacuPractor Technique for Low Back Pain Relief Protocol for Using the VacuPractor General Information Lower back pain is a common condition that affects 84% of adults at some point in their lives (1).
Approaches to Low Back Pain
 Approaches to Low Back Pain NECOM/MaAOHN Annual Conference December 4, 2014 Moderator: John W. Burress, MD, MPH, FACOEM Panelists: Mark Crislip, MD Kathryn Mueller, MD, MPH, FACOEM Tony Tannoury, MD Donald
Approaches to Low Back Pain NECOM/MaAOHN Annual Conference December 4, 2014 Moderator: John W. Burress, MD, MPH, FACOEM Panelists: Mark Crislip, MD Kathryn Mueller, MD, MPH, FACOEM Tony Tannoury, MD Donald
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS
 THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center
 Oh My Aching Back! Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center Epidemiology 90% of episodes of LBP resolves
Oh My Aching Back! Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center Epidemiology 90% of episodes of LBP resolves
Where is your pain located? Please use the diagram below to indicate where most of your pain is located.
 Name: Address: Social Security Number: Email Address: Emergency Contact: Primary Care Physician: Name: Address: Phone Number: Date of Birth: Today's date: Cell Phone Number: Phone #: Referring Physician:
Name: Address: Social Security Number: Email Address: Emergency Contact: Primary Care Physician: Name: Address: Phone Number: Date of Birth: Today's date: Cell Phone Number: Phone #: Referring Physician:
Managing Chronic Pain
 Managing Chronic Pain What Is Chronic Pain? Everyone feels pain sometimes the sharp stab of a twisted ankle, the throb of a headache, the muscle soreness that comes from too much activity. This type of
Managing Chronic Pain What Is Chronic Pain? Everyone feels pain sometimes the sharp stab of a twisted ankle, the throb of a headache, the muscle soreness that comes from too much activity. This type of
