Review Article. Evolution of Epidural Lysis of Adhesions
|
|
|
- Edward Osborne Porter
- 6 years ago
- Views:
Transcription
1 Anderson et al Epidural Adhesiolysis 262 Pain Physician, Volume 3, Number 3, pp , Association of Pain Management Anesthesiologists Review Article Evolution of Epidural Lysis of Adhesions Susan R. Anderson, MD*, Gabor B. Racz, MD W, and James Heavner, DVM, PhD** Epidural neuroplasty (lysis of epidural adhesions) is an interventional technique that has emerged over the last 10 years as part of a multidisciplinary approach to treating radiculopathy with low back pain when conservative management has failed. Neuroplasty was at one time performed as a single-catheter technique using the caudal approach. It now has many variations, including placement of the catheter tip in the anterior epidural space. This article will discuss the evolution and refinement of epidural neuroplasty at our institution. Keywords: Low back pain, radiculopathy, epidural, local anesthetic, corticosteroid, hyaluronidase, hypertonic saline, neuroplasty Epidural neuroplasty (lysis of epidural adhesions) is an interventional technique that was developed at Texas Tech Health Sciences Pain Center in It is indicated when conservative management for spinal or radicular pain has failed. Indications include failed neck/back surgery syndrome, disc disruption, vertebral compression fractures, multilevel degenerative arthritis, facet pain, epidural scarring, and pain not entirely responsive to spinal cord stimulation or intrathecal opioids. This article discusses the evolution and refinement of epidural neuroplasty at our institution over the last 10 years. ANATOMY AND PHYSIOLOGY OF LOW BACK PAIN WITH AND WITHOUT RADICULOPATHY The determination of which tissues contribute to the origin of back pain was confirmed when Kuslich and colleagues (1) performed 193 operations on the lumbar spines of patients given local anesthesia for surgery. They demonstrated that sciatica could only be produced by stimulation of a swollen, stretched, restricted, ie, scarred, or compressed nerve root. Back pain could be produced by stimulation of several lumbar tissues, but the most common From Department of Anaesthesiology Texas Tech University Health Sciences Center, Lubbock, Texas. * Dr. Susan R. Anderson is assistant professor, W Dr. Gabor B. Racz is professor and chairman emeritus, and ** Dr. James E. Heavner is professor. Address Correspondence: Susan R. Anderson, MD, Department of Anesthesiology, Texas Tech University Health Sciences Center, th Street, Room 1C-275, Lubbock, TX tissue of origin was the outer layer of the annulus fibrosus and posterior longitudinal ligament. Stimulation for pain generation of the facet-joint capsule rarely generated low back pain, and facet synovium and cartilage surfaces of the facet or muscles were never tender (2). The contribution of fibrosis as the origin of low back pain has been debated. In patients who had undergone prior laminectomies, there was always some degree of perineural fibrosis. Although scar tissue itself was never tender, the nerve root was frequently very sensitive. Kuslich (1) concluded that the presence of scar tissue compounded pain associated with the nerve root by fixing it in one position and thus increasing the susceptibility of the nerve root to tension or compression. Moreover, these researchers concluded that, Sciatica can only be reproduced by direct pressure or stretch on the inflamed, stretched, or compressed nerve root. No other tissues in the spine are capable of producing leg pain. Stolker and coworkers (3) contended that innervated structures are the only originators of pain. Mechanical factors are not the only causative factors of radicular pain. Histological injury may occur without compression, resulting in persistence of radicular symptoms. Nerve roots may be exposed to chemical irritant substances from degenerated intervertebral discs or facet joints, which can generate pain (2, 4). Structures in the ventral epidural space may become highly sensitized by chemical irritation, resulting in axial pain. These structures include (5): 1. Ventral dura, 2. Posterior longitudinal ligament, 3. Vertebral periosteum, 262
2 Anderson et al Epidural Adhesiolysis Dural attachments, and 5. Epiradicular components. Innervation to the ventral epidural space is extensive and, thus, may become highly sensitized, resulting in chronic low back pain. Histopathological studies have demonstrated sinuvertebral nerve and sympathetic innervation (6-8). Pressure induced changes in the nerves depend upon whether the compression pressures are high or low, e.g. < 200 mm Hg. High pressures exert a direct mechanical effect that can result in deformation of nerve fibers, displacement of the nodes of Ranvier, or invaginations of the paranodal myelin sheaths (2). Low pressures may lead to impairment of blood supply to tissue, decreased nutrient transport, and intraneural edema. Olmarker and colleagues (4) demonstrated that blood flow in the cauda equina ceases when applied pressure (in this case an inflated balloon fixed to the spine in animals) equals mean arterial pressure. A pressure of 5 to 10 mm Hg stopped blood flow in some venules (2, 4). An applied pressure of 10 mm Hg decreased the nutrient transport to nerve roots by 20% to 30% (4). Compression may also lead to changes in permeability or transmural pressure of endoneural capillaries. This can produce edema. It has been demonstrated that intraneural edema in chronic nerve injury is related to the formation of intraneural fibrosis (2). Chemical irritation is another factor in the origin of back pain with or without radiculopathy. The nucleus pulposus has been identified as a source of chemicals which, when leaked into the spinal canal via a rent in the annulus fibrosus, produce irritation. Nerve roots compressed by disc material often show signs of inflammation. Substances that might leak from the disc and produce inflammation of nerve roots or meninges include lactic acid, glycoprotein, cytokines, and histamine. In addition, it has been theorized that material from the nucleus pulposa might act as a foreign protein and trigger an autoimmune reaction (4). Obviously, chemically induced irritation can occur in the absence of compression by the disc (2). Fig. 1. Schematic drawing of the nerve supply of the spine. The ventral compartment of the spine is supplied by interconnected nerve plexuses derived from branches from the sympathetic trunk and from meningeal rami of the spinal nerves, ie, the sinuvertebral nerves. The sinuvertebral nerves have their origin in the rami communicans. The dorsal compartment is supplied by the dorsal rami of the spinal nerves and contains brances from the rami communicans as well. All - anterior longitudinal ligament; BF - fibers from the communicating ramus bypassing the spinal nerve and joining the dorsal ramus; CR - communicating ramus; DR - dorsal ramus of the spinal nerve; DRG - dorsal root ganglion; FJC - facet-joint capsule; IVD - intervertebral disc; MB - medial branch of the dorsal ramus; PLL - posterior longitudinal ligament; SN - sinuvertebral nerve. (From Stolker and colleagues) (3). Structural changes in the vertebral column provide other contributing factors. In a review of the literature, Benzon (9) pointed out that abnormalities of the intervertebral disc include degeneration, bulging, and herniation. Narrowing of the disc space as a consequence of disc pathology is frequently associated with osteophyte formation, and osteoarthritis of the facet joints, which can put pressure on spinal nerves. Bulging of the intervertebral disc distends the posterior longitudinal ligament, causing localized back pain. If bulging of the disc increases, pressure may be exerted on the adjacent nerve roots, producing radicular pain (2). Innervation of the structures of the spine was reviewed by Stolker and colleagues (Fig. 1) (3). Relevant to epidural neurolysis is the fact that free nerve endings have been demonstrated in structures identified by Kuslich and coworkers (1) to be involved in low back pain, ie, the posterior longitudinal ligament and the annulus fibrosus. Interconnected neural networks supply the anterior and posterior longitudinal ligaments, and ventral dura. Perivas-
3 Anderson et al Epidural Adhesiolysis 264 cular nerves innervating the annulus fibrosus bilaterally and multisegmentally (three to five levels) contribute to formation of the neural plexus of the anterior longitudinal ligament (10). The posterior longitudinal ligament plexus consists of branches of the communicating rami, which re-enter the vertebral canal as sinuvertebral nerves. This plexus supplies, bilaterally and multisegmentally (two to four levels), the posterior part of the annulus fibrosus and the vertebral body. The anterior and posterior longitudinal ligament plexus is interconnected by branches of the communicating rami (11). Although considerable debate exists as to whether epidural fibrosis causes pain (12, 13), it is widely accepted that postoperative scar tissue renders the nerve susceptible to injury via compression phenomena, ie, stenosis, disc, etc. (14). Scar tissue is generally found in three components of the epidural space. Dorsal epidural scar tissue is formed by resorption of surgical hematoma and may be involved in pain generation (15). In the ventral epidural space, dense scar tissue is formed by ventral defects in the disc, which may persist despite surgical treatment and continue to produce chronic low back pain/radiculopathy past the surgical healing phase (16). The lateral epidural space includes epiradicular structures out of the root canals known as sleeves containing the exiting nerve root and dorsal root ganglia, susceptible to lateral disc defects, facet overgrowth, neuroforaminal stenosis, etc. (4). Based on the above discussion of possible pain generators, one or all of the following pathological changes may be present in patients with chronic low back pain with or without radiculopathy. These changes include: inflammation, edema, fibrosis, venous congestion, mechanical pressure on the posterior longitudinal ligament, reduced or absent nutrient delivery to the spinal nerve or nerve root, and central sensitization. Inflamed tissue may generate activity in nociceptors or axons that convey nociceptive information to the CNS. Inflammation may render nociceptors or nociceptor axons more sensitive to mechanical stimuli (2). EVOLUTION OF THE TECHNIQUE When the technique of epidural neuroplasty (lysis of epidural adhesions) was first developed, the catheter was inserted into the posterior epidural space. As more and more procedures were performed, it was noted that the posterior epidural space was difficult to access in some patients who had undergone surgical procedures for discogenic or radicular pain. This was most likely due to scar tissue from the previous surgery. In 1996, the technique for catheter insertion was changed to directing the catheter into the anterior epidural space. The catheter needed to be directed towards the anterior epidural space at the level of the S3 nerve root on the affected side for caudal neuroplasty. It also required the open end of the epidural needle to be directed anterolateral after insertion through the sacral hiatus. PROPOSED ALGORITHM Based on anatomy and pathological changes, an algorithm for the treatment of low back pain with and without radiculopathy may be proposed, with the rationale of local application of medications at the site of the pathology (Fig. 2). Workup of a patient begins with a thorough history, clinical exam, and diagnostic workup. The effect of failed conservative therapies should be noted. These treatment modalities include physical therapy, minor nerve blocks, transcutaneous electrical nerve stimulation, behavioral medicine, nonsteroidal anti-inflammatory medications, membrane stabilizers, and antidepressants. Also, prior to neuroplasty, all attempts should be made to eliminate nociceptive and sympathetically maintained pain. To treat the patient with back pain with and without radiculopathy, the pain-generating components must be addressed separately. The algorithmic approach can be used after all conservative therapies have failed. It is imperative that the patient has ongoing concurrent and physical therapy, functional restoration, psychotherapy, and pharmacological management. An algorithm for the treatment of back pain includes recognition and treatment of myofascial pain, facet arthropathy, and internal disc Back Pain With and Without Radiculopathy History, Clinical Exam, Diagnostic Workup Back Pain Algorithm Intrathecal Narcotics +/- Local Anesthesia Radiculopathy Algorithm Trial Dorsal Column Stimulator Permanent Dorsal Column Stimulator Fig. 2. Overall view of the algorithm for treatment of back pain with and without radiculopathy.
4 Anderson et al Epidural Adhesiolysis 265 Back Pain Radiculopathy Myofascial Pain Facet Arthropathy Internal Disc Disruption Epidural Fibrosis, Spinal Fibrosis and 1 or 2 Discogenic Pain Diagnostic Injection Therapeutic Injection Diagnostic Block Therapeutic Block Discography Epidural Steroid Algorithm Diagnostic Selective Root Sleeve Injection with Small Volume Botox Injection Radiofrequency Thermal Coagulation Disco Lesioning Therapeutic Root Sleeve Injection RFTC of Dorsal Root Ganglion Pulsed RF of DRG Surgery Radiofrequency Thermal Coagulation Fig. 3. Algorithm for treatment of back pain. IDET Other disruption (Fig. 3). The approach for radiculopathy includes treatment for epidural fibrosis, spinal fibrosis, and primary or secondary discogenic pain with epidural steroid injections or selective nerve-root-sleeve injections (Figs. 4 and 5). It should be noted that neuroplasty is appropriate after a failed single-shot epidural steroid injection trial. Often this is due to accumulation of fibrotic tissue in the epidural space that prevents spread of the medication to the site of pathology (Fig. 4). Further, if a significant filling defect is evident with placement of the caudal catheter for neuroplasty, a second catheter should be placed transforaminally. Finally, a single-catheter technique with epiduroscopy is being developed that will include neurophysiologic mapping. It should be noted that implantable techniques such as intrathecal narcotic pumps and dorsal column stimulators are considered after all Epidural Steroid Injection x 1 Epidural Steroid Injection Series Radiculopathy Epidural Fibrosis, Spinal Fibrosis and 1 or 2 Discogenic Pain Neuroplasty Single-catheter Technique Diagnostic Selective Root Algorithm Double-catheter Technique + Transforaminal Single-catheter Technique with Epiduroscopy and Neurophysiologic Mapping Fig. 4. Algorithm for treatment of radiculopathy with epidural steroids. Selective Neuroplasty Fig. 5. Algorithm for treatment of radiculopathy with selective root-sleeve injections. other therapies have failed. PREPARATION OF THE PATIENT The history and physical exam should be thorough and note failed conservative therapies. It is important to delineate chronic low back pain with or without radiculopathy as seen secondary to failed spinal surgery or chronic low back pain secondary to internal disc disruption. The physical exam should include neural tension tests, neurological changes, and maneuvers that provoke axial pain. Specific neural tension tests are the straight-leg raise from 30 to 60 degrees and the slump test. The slump should note provocation with proximal and/or distal initiation. The neurological testing should reveal dermatomal or myotomal loss, reflex changes, and motion changes. The diagnostic workup includes radiographic and physiologic exams. Xrays of the lumbar spine in flexion and extension may reveal a hypermobility problem. A magnetic resonance imaging scan with gadolinium is necessary to demonstrate epidural fibrosis. Discography may reveal an internal disc disruption. Physiologic studies might include electromyograph/nerve conduction studies or somatosensory-evoked potentials. Prior to an invasive procedure such as neuroplasty, other issues must be addressed. The patient must be willing to participate in a multidisciplinary rehabilitation program. Significant psychopathology must be ruled out with psychological testing and evaluation. Secondary gain issues, be they monetary, related to medication, or psychological, must be addressed. Finally, detoxification from narcotics, if an issue, must be accomplished.
5 Anderson et al Epidural Adhesiolysis 266 COMPLICATIONS A number of complications may be encountered when performing neuroplasty, whether it be by the caudal, thoracic, cervical, or transforaminal route. These include subarachnoid or subdural injection of local anesthetic or hypertonic saline, paralysis, bowel and/or bladder dysfunction, spinal cord compression from loculation of the injected fluids or hematoma, infection, sensitivity to hyaluronidase, and catheter shearing. DRUGS USED FOR NEUROPLASTY The medications used in neuroplasty are directed at the origination of pain generators (7). Iohexol, the nonionic, water-soluble contrast dye, is used to identify filling defects for placement of the catheter. It is low in osmolarity for decreased toxicity. Iohexol is renally excreted in unmetabolized form (88% intrathecal dose detectable in urine within 24 hours) (17). Chemotoxic reactions are 1/ 100,000 in occurrence. The dose-dependent reaction includes sudden hypotension, organ failure, cardiac arrest, and loss of consciousness. Idiosyncratic reactions include headache (18%) (17), myalgias, nausea, vomiting, dizziness, aseptic meningitis, and allergic, or anaphylactoid reactions (18). The risk for injection into the epidural space is considered no more significant than with diagnostic lumbar puncture (19). Ropivacaine is the local anesthetic used to block nerve axons. It is an amide similar to lidocaine, mepivacaine, or bupivacaine. Advantages of ropivacaine as compared to bupivacaine are: shorter time to onset, shorter duration of motor block, a less cardiotoxic profile, and more selective action on A- delta and C fibers (20). Corticosteroids are injected as an anti-inflammatory agent and for reduction of edema. Triamcinolone diacetate has high glucocorticoid activity (21) with related side effects, e.g., muscle wasting, peptic ulcer, impaired wound healing, and impaired immunologic function (22). It is preservative free and, more importantly, does not flocculate with lidocaine as methylprednisolone does (Antal EG. Pharmacia, and Upjohn, Inc., Kalamazoo, MI, written communication, July 3, 1997). It does suppress the hypothalamic-pituitary-adrenal axis for 21 days (23). Triamcinolone also has nonglucocorticoid-related side effects such as allergic reactions, arachnoiditis from intrathecal injections (24), meningitis (aseptic and bacterial), and epidural abscess (25, 26). Hyaluronidase is injected to disrupt the ground substance in epidural adhesions. This leads to accelerated diffusion (27) and increased absorption by increasing capillary permeability (28, 29). It is noted to preserve the dura and provides improved efficacy of decompressive neuroplasty (3). Hypertonic saline decreases tissue edema and increases the fluid volume within the epidural space, causing microdissection. Hypertonic saline is also noted to have some local anesthetic action (30, 31) and C-fiber selectivity (32). A possible complication from injection of hypertonic saline is arachnoiditis (33). TECHNIQUE Epidural neuroplasty is performed in the caudal region for low back pain. It can also be performed in the cervical and thoracic areas with modifications, ie, the technique for catheter insertion and the different dosages of medications used. When the procedure is chosen, it should be thoroughly explained to the patient, including all benefits and risks. Informed consent should be obtained. A preoperative complete blood cell count, prothrombin time, partial thromboplastin time, bleeding time, and urinalysis are required. Laboratory values should be optimal. Caudal Approach PROTOCOL In the operating room: 1. Routine intraoperative monitors are placed, an intravenous drip is started, and appropriate sedation is given. Place the patient in the prone position. Place sterile drapes in position. 2. Place a 15- or 16-gauge RK TM epidural needle via the sacral hiatus on the side opposite the suspected pathology after local anesthetic infiltration of the skin on the top of the buttock. 3. With confirmation of the correct placement of the needle in the epidural space, inject 10 ml iohexol (Omnipaque 240 TM ) after negative aspiration and visualize spread of the contrast medium (epidurogram). 4. If a filling defect corresponding to the area of pain is present, thread a Racz Tun-L-Kath TM or Racz Tun-L-XL TM (stiffer) catheter towards the filling defect (scarring or fibrosis). Prior to insertion, place a 30-degree bend approximately 2.5 cm from the catheter tip to aid in placement of the catheter towards the side and anteriorly. Confirm ven-
6 Anderson et al Epidural Adhesiolysis 267 tral placement of the catheter with a lateral fluoroscopic view. 5. After correct placement, inject 10 ml of preservative-free normal saline with 1500 U of hyaluronidase into the filling defect. 6. Inject an additional 2 to 3 ml of iohexol to visualize opening of the scarred area and spread of the injectate within the epidural space. 7. Inject 9 ml of 0.2% ropivacaine with 1 ml of 40 mg/ml triamcinolone diacetate. First inject a 3-mL test dose, followed 5 minutes later by the remaining 7 ml if there is no evidence of intravascular or intrathecal injection. 8. Remove the needle and secure the catheter to the skin with 3.0 nylon suture. Apply triple-antibiotic ointment to the skin entry site and place a sterile dressing. 9. Attach a bacteriostatic filter to the catheter. In the postanesthesia care unit (PACU) 30 minutes later: 1. If there is no evidence of a subarachnoid block, infuse 10 ml of 10% saline via the catheter over 30 minutes. If the patient complains of pain, stop the infusion and inject an additional 2 to 3 ml of 0.2% ropivacaine via the catheter, wait 5 minutes and restart the infusion. 2. At the end of the infusion, flush the catheter with 2 ml of preservative-free normal saline. In the PACU (or designated procedure area) after 18 to 24 hours: 1. On the following 2 days, inject 10 ml of 0.2% ropivacaine; wait 25 minutes, infuse 10 ml of 10% saline over 30 minutes. 2. Flush catheter with 2 ml of preservative-free normal saline. 3. On day 3, repeat the above process, remove the catheter, and place sterile dressing. Three D Technique For epidural neuroplasty in the cervical and thoracic region, the approach to accessing the epidural space utilizes the Three D technique. This involves using fluoroscopic views to ascertain Direction, Depth, and Direction of the epidural needle as one approaches the epidural space. The synopsis of the technique for cervical and thoracic neuroplasty follows. In the operating room: 1. Position the patient in the left lateral decubitus position. 2. Use the paramedian approach 1 cm from midline, one interspace below the intended epidural space entry. 3. Obtain epidural access with a 16-gauge RK epidural needle. 4. Use anteroposterior fluoroscopy to assess direction. 5. Use lateral fluoroscopy to assess depth. 6. Use anteroposterior fluoroscopy to reassess direction and correct if necessary. 7. Advance the needle to the base of the spinous process that corresponds to the level of the lamina near the posterior aspect of the epidural space. The tip of the needle should be midline. Remove the stylet. Fig. 6. Anteroposterior view of placement of the transforaminal catheter (top arrow) and caudal catheter (bottom arrow) for the double-catheter technique.
7 Anderson et al Epidural Adhesiolysis 268 Fig. 7. Lateral view of correct placement of the transforaminal catheter with confirmation by dye spread. 8. Using loss-of-bounce technique with a pulsator syringe containing 4 ml of normal saline and 2 ml of air, enter the epidural space. 9. Perform an epidurogram by injecting 2 to 5 ml of iohexol through the needle. 10. Thread the Racz Tun-L-Kath TM through the needle toward the targeted nerve root in the lateral epidural space; lateral placement is optimal. 11. Inject 1 to 2 ml of iohexol through the catheter to verify that there are no loculations and that the catheter is not in a blood vessel. 12. Inject 6 ml of preservative-free normal saline containing 1500 U hyaluronidase if in the cervical region, 8 ml if in the thoracic region. 13. If in the cervical region, inject 5 ml of 0.2% ropivacaine with 1 ml of 40 mg/ ml triamcinolone diacetate (6 ml total volume) in 2 to 3 ml incremental doses to verify that the catheter is not subdural or subarachnoid. If in the tho- racic region, the total volume is 8 ml, including the steroid. 14. Remove the needle under fluoroscopic guidance and suture the catheter in place with 3.0 nylon suture. 15. Attach the connector to the catheter with a bacteriostatic filter. 16. Apply triple-antibiotic ointment and cover catheter with split 2 x 2s and a transparent dressing. Place a half loop in the catheter prior to applying the transparent dressing. Tape the catheter to the patient s skin. In the PACU: 1. If there is no evidence of subdural or subarachnoid spread, infuse the catheter with 4 to 5 ml of 10% saline for the cervical region and 8 ml if in the thoracic region. The infusion should run in over 30 minutes. 2. Flush the catheter with 2 ml of preservative-free normal saline. In the PACU or designated procedure area: 1. On days two and three, aspirate the catheter and inject 6 ml (cervical) or 8 ml (thoracic) of 0.2% ropivacaine over 25 minutes. First give a 2-mL test bolus, wait 5 minutes as a precaution against subarachnoid or subdural spread, and then give the remaining amount over 20 minutes. 2. Infuse 4 to 5 or 8 ml (cervical or thoracic, respectively) of 10% saline over 30 minutes. 3. Flush with 2 ml of preservative-free normal saline. 4. On day three, remove the catheter at the end of the infusion and apply a sterile dressing. Transforaminal Approach Recently a lumbar transforaminal technique has been advocated for patients for whom the area of scarring is above the L5/S1 nerve root, making it difficult to access via the caudal approach. Using a 15-degree oblique and a 15- degree caudocephalad fluoroscopic view, a curved RK TM epidural needle is directed using gun-barrel technique towards a point just lateral to the superior pars of the vertebrae that comprises the caudad portion of the neural foramen. The tip of the needle should be 2 to 3 mm within
8 Anderson et al Epidural Adhesiolysis 269 the neural foramen. Two to three milliliters of contrast is injected to confirm epidural spread. The Tun-L-Kath or Tun-L-XL TM is inserted through the needle into the epidural space. If resistance is met, advance the needle 1 to 2 mm more and reinsert the catheter. (A guidewire or a stiff probe with a flexible, blunt or atraumatic tip may be inserted through the needle to facilitate opening of the anterior epidural space.) Once inside the epidural space, the catheter is advanced to the midline and the epidural needle is removed (Figs. 6 and 7). The injection of medications follows the same guidelines as those for caudal neuroplasty. This approach may be used in conjunction with a caudal catheter for a double-catheter technique, when deemed necessary. OUTCOMES The first report of this procedure was by Racz and Holubec in 1989 (34). The results were based on a survey of 72 patients who were randomly selected from a pool of approximately 200 patients who underwent caudal neuroplasty. There were slight variations in the protocol, namely the dose of bupivacaine used (25 ml instead of 10 ml) and the omission of hyaluronidase. Approximately 72.2% of the patients reported pain relief on discharge, while 37.5% had pain relief of < 1 month, 30.0% reported pain relief of 1 to 3 months duration, and 12.5% had relief for 3 to 6 months. Arthur, Racz, Heinrich and colleagues (35) presented another retrospective study that used the same technique, except only 50 of the 100 patients received hyaluronidase. In the hyaluronidase group, 81.6% of the patients had persistent pain relief at the time of interview (in some up to 3 years postprocedure). In the no-hyaluronidase group, 68% of the patients had varying degrees and durations of pain relief, and 15% had persistent pain relief. Most recently, Racz, Raj, and Heavner (36) performed a prospective evaluation of 0.9% sodium chloride versus 10% sodium chloride with or without hyaluronidase. Results from this study show that 49% of the patients had pain relief in the body area targeted for lesion-specific therapy at 1-year follow-up. Hammer and coworkers performed a study on the double catheter (caudal and transforaminal) technique with findings in agreement with Texas Tech University (Hammer. M, Transforaminal Lumbar Epidural Neuroplasty, unpublished data, 2000). After 2 weeks, patients reported a 50% or greater relief of pain. At 6 months follow-up, 86% of patients would repeat the procedure, 60% attained more than 50% pain relief, 10% achieved 100% pain relief, 20% achieved less than 50% pain relief, and 10% of patients had no change in their pain severity (12). Manchikanti and colleagues, in a retrospective study, (37) report that a 1-day injection series is as effective as the 3- day injection series per Racz and coworkers. Hence, a prospective study for the 1-day injection series should be done. SUMMARY Percutaneous epidural neuroplasty has been proven to be safe and effective in selected patients with epidural adhesions. It must be performed by a technically competent, trained pain physician. Recent information on the innervation of the ventral epidural space emphasizes the need for ventral, site-specific catheter placement for delivery of medications (2). It is imperative to adhere to the technique (including the placement of the catheter tip into the scar) without modification for maximizing benefits. The prospective studies indicate improved and cost-effective results (2, 37, 38). REFERENCES 1. Kuslich SD, Ulstrom CL, Michael CJ. The tissue origin of low back pain and sciatica. Orthopaedic Clin NA 1991; 22: Racz GB, Noe C, Heavner JE. Selective spinal injections for lower back pain. Current Review of Pain 1999; 3: Stolker RJ, Vervest ACM, Groen GJ. The management of chronic spinal pain by blockades: A review. Pain 1994; 58: Olmarker K, Rydevik B. Pathophysiology of sciatica. Orthopedic Clin NA 1991; 22: Cautico W, Parker JC, Pappert E et al. An anatomical and clinical investigation of spinal meningeal nerves. Aeta Neurochir (Wien) 1988; 90: Imai S, Hukuda S, Maeda T. Dually nnervating nociceptive networks in the rat lumbar posterior longitudinal ligaments. Spine 1995; 19: Lewandowski EM. The efficacy of solutions used in caudal neuroplasty. Pain Digest 1997; 7: Olmarker K, Rydevik B, Nordburg C. Autologous nucleus pulposus induces neurophysiologic and histologic changes in porcine cauda equina nerve roots. Spine 1993; 11: Benzon HT. Epidural steroid injection for low back pain and lumbosacral radiculopathy. Pain 1986; 24: Groen GJ. De innervatie van de wervelkolom bij de mens. Ned Tijdschr Man Ther 1991; 10: Groen GJ, Baljet B, Rdukker J. Nerves and nerve plexus of the human vertebral column. Am J Anat 1990; 188: Gaughan E, Nikon A, Krooh L et al. Effect of sodium
9 Anderson et al Epidural Adhesiolysis 270 hyaluronate on tendon healing and adhesion formation in the horse. Am J Vet Res 1991; 52: Annertz M, Jonsson B, Stromqvist B et al. No relationship between epidural fibrosis and sciatica in the lumbar postdiscectomy syndrome. A study with contrast-enhanced magnetic resonance imaging in symptomatic and asymptomatic patients. Spine 1995; 4: Cervellini P, Curri D, Volpin L et al. Computed tomography of epidural fibrosis after discectomy. A comparison between symptomatic and asymptomatic patients. Neurosurgery 1988; 6: Songer M, Ghosh L, Spencer D. Effects of sodium hyaluronate on peridural fibrosis after lumbar laminectomy and discectomy. Spine 1990; 15: Key JA, Ford LT. Experimental intervertebral disc lesions. Journal Bone Joint Surgery (AM) 1948; 30: Omnipaque TM product insert. Princeton, NJ, Nycomed, Inc., Lasser EC, Lyon SG, Berry CB. Reports on contrast media reactions: Analysis of data from reports to the U.S. Food and Drug Administration. Radiology 1997; 203: Ndosi BN, Ndosi NK, Kazema RR. Myelography with Omnipaque TM (Iohexol) using basic radiographic facilities: The main adverse effects. Cent Afr J Med 1996; 42: Kerkkemp HEM, Gielen MJM. Cardiovascular effects of epidural local anesthetics: Comparison of 0.75% bupivacaine and 0.75% ropivacaine, both with adrenaline. Anaesthesia 1991; 46: Aristocort TM Forte Product Insert. Deerfield, IL, Fujisawa USA, Inc., Abram SE, O Connor TC. Complications associated with epidural steroid injections. Reg Anesth 1996; 21: Jacobs S, Pullan PT, Potter JM et al. Adrenal suppression following extradural steroids. Anaesthesia 1983; 38: Nelson DA, Vates TS, Thomas RB. Complications from intrathecal steroid therapy in patients with multiple sclerosis. Acta Neurol Scand 1973; 49: Dougherty JH, Fraser RAR. Complications following intraspinal injections of steroids. J Neurosurg 1978; 48: Shealy CN. Dangers of spinal injection without proper diagnosis. JAMA 1966; 197: Watson D. Hyaluronidase. Br J Anaesth 1993; 71: Szabo G, Magyar S. Effect of hyaluronidase on capillary permeability, lymph flow, and passage of dyelabelled protein from plasma to lymph. Nature 1958; 182: Hechter O, Dopkeen SK, Yudell MH. Clinical use of hyaluronidase in hypodermoclysis. J Pediat 1947; 30: Hodgkin AL, Katz B. The effect of sodium ions on the electrical activity of the giant axon of the squid. J Physiol (London) 1949; 108: Hubbard JL, Jones SF, Landau EM. An examination of the effects of osmotic pressure changes upon transmitter release from mammalian motor nerve terminals. J Physiol (London) 1968; 197: King JS, Jewett DL, Sundberg HR. Differential blockade of cat dorsal root C fibers by various chloride solutions. J Neurosurg 1972; 36: Aldrete JA, Zapata JC, Ghaly R. Arachnoiditis following epidural adhesiolysis with hypertonic saline. Report of two cases. Pain Digest 1996; 6: Racz GB, Holubec JT. Lysis of adhesions in the epidural space. In Racz GB (ed). Techniques of Neurolysis. Boston, Kluwer Academic Publishers 1989, pp Arthur J, Racz GB, Heinrich R et al. Epidural space: Identification of filling defects and lysis of adhesions in the treatment of chronic painful conditions. Abstracts of the 7 th World Congress on Pain, Paris, IASP Punlications, 1993, Racz GB, Heavner JE, Raj PP. Percutaneous epidural neuroplasty: Prospective one-year follow-up. Pain Digest 1999; 9: Manchikanti L, Pakanati RR, Bakhit CE et al. Role of adhesiolysis and hypertonic saline neurolysis in management of low back pain: Evaluation of modification of the Racz protocol. Pain Digest 1999; 9: Heavner JE, Racz GB, Raj PP. Percutaneous epidural neuroplasty: Prospective evaluation of 0.9% NaCl vs 10% NaCl with or without hyaluronidase. Reg Anesth Pain Med 1999; 24:
Outcomes of Epidural Neuroplasty to Treat Lumbar Discogenic Pain- One-Year Follow-Up
 Chinese J. Pain 2009;19(1):08~16 Outcomes of Epidural Neuroplasty to Treat Lumbar Discogenic Pain- One-Year Follow-Up 1,4 3 2 2 1,4 Li Wei, Kung-Shing Lee, Man-Kit Siu, Yu-Ting Tai, Jia-Wei Lin, 1,4 1,4
Chinese J. Pain 2009;19(1):08~16 Outcomes of Epidural Neuroplasty to Treat Lumbar Discogenic Pain- One-Year Follow-Up 1,4 3 2 2 1,4 Li Wei, Kung-Shing Lee, Man-Kit Siu, Yu-Ting Tai, Jia-Wei Lin, 1,4 1,4
Neuroplasty or Epidural Adhesiolysis / Neurolysis
 Epidural injections are a very common treatment for neck, back and extremity pain. Back problems have become one of the most common medical conditions in our society today. Approximately 80 percent of
Epidural injections are a very common treatment for neck, back and extremity pain. Back problems have become one of the most common medical conditions in our society today. Approximately 80 percent of
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Pathophysiology of lumbar disc degeneration: a review of the literature. Neurosurg Focus 13 (2): August, 2002
 Pathophysiology of lumbar disc degeneration: a review of the literature Neurosurg Focus 13 (2): August, 2002 MICHAEL D. MARTIN, M.D., CHRISTOPHER M. BOXELL, M.D., F.A.C.S., AND DAVID G. MALONE, M.D. FROM
Pathophysiology of lumbar disc degeneration: a review of the literature Neurosurg Focus 13 (2): August, 2002 MICHAEL D. MARTIN, M.D., CHRISTOPHER M. BOXELL, M.D., F.A.C.S., AND DAVID G. MALONE, M.D. FROM
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Discussion Points 10/17/16. Spine Pain is Ubiquitous. Interventional Pain Management
 Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Outline. Introduction / Epidemiology. Anatomy / Pain generators. Diagnosis. Treatment. Most Important lecture!!
 Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
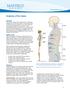 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for
 Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
Central Nervous System: Part 2
 Central Nervous System: Part 2 1. Meninges 2. CSF 3. Spinal Cord and Spinal Nerves Explain spinal cord anatomy, including gray and white matter and meninges (give the general functions of this organ).
Central Nervous System: Part 2 1. Meninges 2. CSF 3. Spinal Cord and Spinal Nerves Explain spinal cord anatomy, including gray and white matter and meninges (give the general functions of this organ).
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
INDEX. Cancerpain alcohol neurolysis for, 5, 20, 53-54
 INDEX Alcohol advantages of, 54 celiac plexus block with, 19-20, 165 chemical hypophysectomy with, 20 complications and side effects of, 18, 19, 45-46, 54-55 contraindications for, 54 doses with, 52 drug
INDEX Alcohol advantages of, 54 celiac plexus block with, 19-20, 165 chemical hypophysectomy with, 20 complications and side effects of, 18, 19, 45-46, 54-55 contraindications for, 54 doses with, 52 drug
Pain Management Clinic ISIC
 Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Chapter 13. The Spinal Cord & Spinal Nerves. Spinal Cord. Spinal Cord Protection. Meninges. Together with brain forms the CNS Functions
 Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Back Pain Policies Summary
 Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
PRECISE DIAGNOSIS AND TREATMENT OF NECK AND BACK PAIN
 PRECISE DIAGNOSIS AND TREATMENT OF NECK AND BACK PAIN MEDICAL DIRECTOR Elgin, Itasca, Lake Barrington, McHenry, Libertyville, Huntley, Elmhurst John V. Prunskis M.D. FIPP JOHN V. PRUNSKIS Illinois M.D.
PRECISE DIAGNOSIS AND TREATMENT OF NECK AND BACK PAIN MEDICAL DIRECTOR Elgin, Itasca, Lake Barrington, McHenry, Libertyville, Huntley, Elmhurst John V. Prunskis M.D. FIPP JOHN V. PRUNSKIS Illinois M.D.
nvt Transforaminal Lumbar Interbody Fusion System
 nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13)
 Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
CLINICAL GUIDELINES. CMM-207: Epidural Adhesiolysis. Version Effective February 15, 2019
 CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
CLINICAL GUIDELINES CMM-207: Version 1.0.2019 Effective February 15, 2019 Clinical guidelines for medical necessity review of speech therapy services. CMM-207: CMM-207.1: Definition 3 CMM-207.2: General
Bony framework of the vertebral column Structure of the vertebral column
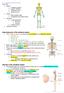 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
Epidural Analgesia in Labor - Whats s New
 Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
nva Anterior Lumbar Interbody Fusion System
 nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
nvp Posterior Lumbar Interbody Fusion System
 nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
Clinical Policy: Lysis of Epidural Lesions Reference Number: CP.MP.116
 Clinical Policy: Reference Number: CP.MP.116 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.116 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18
 Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lysis of Epidural Adhesions Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Lysis of Epidural Adhesions Professional Institutional Original Effective
Lysis of Epidural Adhesions Page 1 of 11 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Lysis of Epidural Adhesions Professional Institutional Original Effective
RADICULOPATHY AN INTRODUCTION TO
 AN INTRODUCTION TO RADICULOPATHY This booklet provides general information on radiculopathy. It is not meant to replace any personal conversations that you might wish to have with your physician or other
AN INTRODUCTION TO RADICULOPATHY This booklet provides general information on radiculopathy. It is not meant to replace any personal conversations that you might wish to have with your physician or other
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Table of Contents: Part 1 General principles. Section 1: Introduction. 1. Past, present and future of interventional physiatry 2.
 Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
Systematic Review of Effectiveness and Complications of Adhesiolysis in the Management of Chronic Spinal Pain: An Update
 Pain Physician 2007; 10:129-146 ISSN 1533-3159 Review Systematic Review of Effectiveness and Complications of Adhesiolysis in the Management of Chronic Spinal Pain: An Update Andrea M. Trescot, MD 1, Pradeep
Pain Physician 2007; 10:129-146 ISSN 1533-3159 Review Systematic Review of Effectiveness and Complications of Adhesiolysis in the Management of Chronic Spinal Pain: An Update Andrea M. Trescot, MD 1, Pradeep
Spinal Pain Experienced as a Visceral Referral
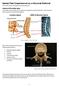 Spinal Pain Experienced as a Visceral Referral The lumbar spine is a frequent site of low back pain. Anatomy of the lumbar spine The lumbar spine is made up of 5 vertebrae, separated by intervertebral
Spinal Pain Experienced as a Visceral Referral The lumbar spine is a frequent site of low back pain. Anatomy of the lumbar spine The lumbar spine is made up of 5 vertebrae, separated by intervertebral
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Orthopedic Coding Changes for 2012
 Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Placename CCG. Policies for the Commissioning of Healthcare. Policy for Managing Back Pain- Spinal Injections
 Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Lysis of Epidural Adhesions
 Lysis of Epidural Adhesions Policy Number: 8.01.18 Last Review: 6/2018 Origination: 8/2007 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for lysis
Lysis of Epidural Adhesions Policy Number: 8.01.18 Last Review: 6/2018 Origination: 8/2007 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for lysis
Coventry Pain Clinic - Spianl Pain - Sciatica and Brachalgia
 Coventry Pain Clinic - Spianl Pain - Sciatica and Brachalgia Copyright 2002-2005 Dr. Richard S. Walker Introduction Spinal Nerve Root Pain (Radiculopathy) can arise from the problems affecting the:- C4
Coventry Pain Clinic - Spianl Pain - Sciatica and Brachalgia Copyright 2002-2005 Dr. Richard S. Walker Introduction Spinal Nerve Root Pain (Radiculopathy) can arise from the problems affecting the:- C4
Kevin S. Ladin, M.D. Board Certified in Physical Medicine & Rehabilitation ABMS Subspecialty Board Certified in Pain Medicine
 Kevin S. Ladin, M.D. Board Certified in Physical Medicine & Rehabilitation ABMS Subspecialty Board Certified in Pain Medicine kslmd@cox.net EBM in Pain Medicine Evidence-based medicine (EBM) is a form
Kevin S. Ladin, M.D. Board Certified in Physical Medicine & Rehabilitation ABMS Subspecialty Board Certified in Pain Medicine kslmd@cox.net EBM in Pain Medicine Evidence-based medicine (EBM) is a form
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Confirmation with Epidurogram Necessary?
 Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Interventional Pain Management
 Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Lumbar Retrodiscal Transforaminal Injection
 Pain Physician 2007; 10:501-510 ISSN 1533-3159 Technical Update Lumbar Retrodiscal Transforaminal Injection Joseph F. Jasper, MD From: Advanced Pain Medicine Physicians, Tacoma, WA. Dr. Jasper is Medical
Pain Physician 2007; 10:501-510 ISSN 1533-3159 Technical Update Lumbar Retrodiscal Transforaminal Injection Joseph F. Jasper, MD From: Advanced Pain Medicine Physicians, Tacoma, WA. Dr. Jasper is Medical
Comprehensive Centers for Pain Management. Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain
 Comprehensive Centers for Pain Management Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain There are many different treatments for back pain. Taking lots of drugs
Comprehensive Centers for Pain Management Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain There are many different treatments for back pain. Taking lots of drugs
Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
Lecture 14: The Spinal Cord
 Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
PERCUTANEOUS FACET JOINT DENERVATION
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
Jessica Jameson MD Post Falls, ID
 Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Epidural Steroid Injection
 Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
A Patient s Guide to Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 2778 N. Webb Rd. Wichita, KS 67226 Phone: (316) 631-1600 Fax: (316) 631-1617 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Epidural Steroid Injections 2778 N. Webb Rd. Wichita, KS 67226 Phone: (316) 631-1600 Fax: (316) 631-1617 DISCLAIMER: The information in this booklet is compiled from
Vijay Singh, M.D Roosevelt Rd., Niagara, WI 54151
 Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Overview. Spinal Anatomy Spaces & Meninges Spinal Cord. Anatomy of the dura. Anatomy of the arachnoid. Anatomy of the spinal meninges
 European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
DRAFT as posted for public comment 11/8/2016 to 8 a.m. 12/9/2016. HERC Coverage Guidance
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
Wake me when this makes sense. Today s Objectives. Quote from Maitland. Quote from Maitland 8/4/2012
 Wake me when this makes sense Today s Objectives Selection of techniques Order of efficacy of techniques Ground the theory in reality Application of techniques How do you do what you should do Quote from
Wake me when this makes sense Today s Objectives Selection of techniques Order of efficacy of techniques Ground the theory in reality Application of techniques How do you do what you should do Quote from
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
SPINAL PAIN. Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon
 SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
SPINAL PAIN Mr. Yagnesh Vellore FRACS Neurosurgeon and Spine Surgeon PAIN GENERATORS IN THE SPINE Ligaments: ALL,PLL Muscle Periosteum bone Outer 1/3 annulus disc Facet joints Sacro-iliac joint sinuvertebral
Facet Joint Syndrome / Arthritis
 Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Fluoroscopically-Guided Injections to Treat Kissing Spine Disease
 Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
Pain Physician 2008; 11:549-554 ISSN 1533-3159 Case Report Fluoroscopically-Guided Injections to Treat Kissing Spine Disease Timothy J. Lamer, MD 1, Jeffrey M. Tiede, MD 2 and Douglas S. Fenton, MD 3 From:
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Medical Policy. MP Lysis of Epidural Adhesions
 Medical Policy MP 8.01.18 BCBSA Ref. Policy: 8.01.18 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Radiology Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our
Medical Policy MP 8.01.18 BCBSA Ref. Policy: 8.01.18 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Radiology Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our
HERNIATED DISCS AN INTRODUCTION TO
 AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Alamo T Transforaminal Lumbar Interbody System Surgical Technique
 Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Beyond Epidurals Management of Back Pain
 Beyond Epidurals Management of Back Pain Muhammad A. Munir, MD Diplomat American Board of Anesthesiology and Pain Management Present Practice of Pain Medicine Pain Management vs Pain Medicine Palliative
Beyond Epidurals Management of Back Pain Muhammad A. Munir, MD Diplomat American Board of Anesthesiology and Pain Management Present Practice of Pain Medicine Pain Management vs Pain Medicine Palliative
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
2013 FINAL - Physician Payment Rates
 ASC/Hospital) Injection, therapeutic (eg, local anesthetic; corticosteroid), 20526 carpal tunnel $74.88 $56.50 $76.55 $56.48 2.2% 0.0% tendon sheath, ligament injection 20550 $57.18 $40.85 $58.52 $41.17
ASC/Hospital) Injection, therapeutic (eg, local anesthetic; corticosteroid), 20526 carpal tunnel $74.88 $56.50 $76.55 $56.48 2.2% 0.0% tendon sheath, ligament injection 20550 $57.18 $40.85 $58.52 $41.17
 The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON INTRADISCAL PRESSURE
 EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande Regional Hospital,
EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande Regional Hospital,
