High Hamstring Tendinopathy: MRI and Ultrasound Imaging and Therapeutic Efficacy of Percutaneous Corticosteroid Injection
|
|
|
- Paulina Hardy
- 6 years ago
- Views:
Transcription
1 Musculoskeletal Imaging Clinical Perspective Zissen et al. Imaging of High Hamstring Tendinopathy Musculoskeletal Imaging Clinical Perspective Maurice H. Zissen 1 Grant Wallace 1 Kathryn J. Stevens 1 Michael Fredericson 2 Christopher F. Beaulieu 1 Zissen MH, Wallace G, Stevens KJ, Fredericson M, Beaulieu CF Keywords: corticosteroid, hamstring, MRI, percutaneous injection, tendinopathy, ultrasound DOI: /AJR Received September 23, 2009; accepted after revision March 17, Department of Radiology, Stanford University School of Medicine, 300 Pasteur Dr., Stanford, CA Address correspondence to C. F. Beaulieu (beaulieu@stanford.edu). 2 Department of Orthopedic Surgery, Stanford University School of Medicine, Sports Medicine Center, Redwood City, CA. AJR 2010; 195: X/10/ American Roentgen Ray Society High Hamstring Tendinopathy: MRI and Ultrasound Imaging and Therapeutic Efficacy of Percutaneous Corticosteroid Injection OBJECTIVE. The goals of this study were to review the MRI and sonographic findings in patients diagnosed clinically with high hamstring tendinopathy and to evaluate the efficacy of ultrasound-guided corticosteroid injections in providing symptomatic relief. CONCLUSION. MRI is more sensitive than ultrasound in detecting peritendinous edema and tendinopathy at the proximal hamstring origin. Fifty percent of patients had symptomatic improvement lasting longer than 1 month after percutaneous corticosteroid injection, and 24% of patients had symptom relief for more than 6 months. A cute strains of the mid and distal hamstring myotendinous complex are common athletic injuries [1 5]. Proximal hamstring tendon pathologic abnormalities, including tendon degeneration, partial tearing, and peritendinous inflammatory reaction, are less common [6]. These abnormalities are grouped clinically as high hamstring tendinopathy, and patients usually present with subacute onset of deep buttock or thigh pain that is exacerbated by repetitive activity, such as long-distance running, and often is aggravated by sitting. In many of these patients, conservative management is ineffective, and MRI is performed to confirm the diagnosis, to grade the extent of injury, or to search for alternative explanations. In cases where MRI establishes an abnormality at the hamstring origin, or where MRI findings are normal but clinical suspicion is high, we have performed ultrasound-guided injections of corticosteroids and local anesthetic at the hamstring origin. The goals of this article are to review our institution s experience with MRI and ultrasound imaging of the proximal hamstring tendons and to establish the efficacy of ultrasound-guided corticosteroid injection as an integral part of overall patient management. Materials and Methods Patient Selection Criteria This retrospective study was performed in compliance with HIPAA regulations and with approval from our institutional review board. We performed a computerized search of medical records and imaging reports at our institution, searching for the terms hamstring, MRI, ultrasound, and corticosteroid injection. Patients undergoing imaging and injection of hamstring disorders in the mid or distal thigh or about the knee were excluded. This search identified 65 patients who received ultrasound-guided proximal hamstring injections between January 2002 and December There were 28 men (43.1%) and 37 women (56.9%) with a mean age of 37.4 years (range, years). For 35 patients, MRI was performed at our facility and images were available to review. All patients had ultrasound images available for review. Image Review Two authors reviewed the MRI and ultrasound studies for all patients. MR studies included small field-of-view (~24 28 cm) T1- and T2-weighted fat-suppressed images in three planes using a phased-array coil at 1.5 T. MR images were reviewed for findings of peritendinous fluid or edema (peritendinitis), tendinopathy, partial tear, and bone marrow edema in the ischial tuberosity. Ultrasound images were reviewed for peritendinous fluid or edema, hypoechoic areas or thickening of the tendons consistent with tendinopathy, and echogenic foci consistent with calcifications. The mean (± SD) time between the MR and ultrasound studies was 90 ± 16 days (range, days). Ultrasound-Guided Peritendinous Injection All injections were performed by an experienced musculoskeletal radiologist after obtaining written informed consent. Patients were asked to identify, if possible, the site of maximum pain, either by AJR:195, October
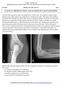
2 Zissen et al. palpation or by performing resistance maneuvers. With the patient in the prone position, a 6- to 10- MHz linear transducer was used to localize the ischial tuberosity and proximal hamstring tendons in both transverse and sagittal planes. Color Doppler was used to identify and avoid visible vascular structures. Scanning laterally to the hamstring origin in the sagittal plane, the sciatic nerve was similarly identified, and injections were performed medially to this structure. A freehand technique was used in the sagittal plane to guide the injection, first using 1% lidocaine with a 1.5-inch-long 21-gauge needle. If this needle was sufficiently long to reach the hamstring tendons, the therapeutic mixture was injected through the same needle. In larger patients, a 3-inch-long 20-gauge spinal needle was inserted after removal of the 1.5-inch needle. Two therapeutic mixtures were used in this study. The first consisted of 1 ml of triamcinolone acetonide 40 (40 mg/ml) plus 5 ml of bupivacaine. The second consisted of 1 ml of triamcinolone acetonide 40 (40 mg/ml) with 0.5 ml of dexamethasone sodium phosphate (4 mg/ml) and 5 ml of bupivacaine. The therapeutic mixture was administered using a 21- or 20-gauge needle under sterile conditions as described in the previous paragraph. After needle placement, the therapeutic mixture was injected immediately superficial to the hamstring tendons, and real-time sonography was used to monitor tracking of the fluid along the peritendinous tissues in both the sagittal and transverse directions. Repositioning was performed if fluid was not tracking over a length of tendon at least 5 cm long, to spread the medication. After injection and needle removal, the peritendinous soft tissues were massaged gently for 1 2 minutes to further spread the medication in the tissue planes. With direct ultrasound visualization of the needle, we avoided intratendinous injection. Note also that, to avoid intratendinous injection, we did not attempt to inject deeper at the tendon bone interface. On completion of the procedure, patients were asked to assess pain relief in the immediate postinjection period. Telephone Questionnaire Review of clinical records showed that only a small number of patients returned to the referring physician for a follow-up visit; thus, no useful data were available regarding efficacy of the injections from this resource. We constructed a questionnaire and attempted to contact by telephone all 65 patients who received the ultrasound-guided peritendinous injection. A total of 38 patients were reached and agreed to participate in the study. The mean time to follow-up was 4 years (range, 6 months to 8 years). Verbal informed consent was obtained before asking the patients a series of TABLE 1: Imaging Findings of Patients Receiving Ultrasound-Guided Corticosteroid Anesthetic Injection Characteristic Ultrasound findings (n = 65 patients) subjective pain assessment questions that included the degree of pain relief as well as duration of symptom resolution. The patients were also asked questions related to the mechanism of injury, prior activity level, prior treatment techniques (including medical management and physical therapy), and any complications experienced as a result of the procedure. Statistical Analysis We defined patients with significant improvement of symptoms as those who reported duration of symptomatic improvement longer than 1 month and patients with insignificant improvement as those who reported having less than 1 month of symptomatic resolution. We then used a Fisher s exact test to determine whether length of symptoms before injection, presence of tendinopathy on MRI or ultrasound, presence of peritendinitis on MRI or ultrasound or absence of imaging No. (%) of Patients Peritendinitis (fluid or edema) 13 (20) Tendinopathy 11 (16.9) Calcifications 3 (4.6) Normal 40 (61.5) MRI findings (n = 35 patients) Peritendinitis (fluid or edema) 22 (62.9) Tendinopathy 9 (25.7) Bone marrow edema 7 (20) Partial tear 7 (20) Normal 8 (22.9) findings on either MRI or ultrasound were statistically associated with improved outcomes. Results Imaging Results The imaging findings observed on retrospective review of 65 ultrasound studies and 35 MRI studies are shown in Table 1. For ultrasound, 40 (61.5%) of 65 patients showed normal tendon thickness and echogenicity without surrounding fluid or tendon calcifications. MRI findings were normal for eight (22.9%) of 35 patients. On both ultrasound (20%) and MRI (62.9%), peritendinitis, manifesting as fluid or edema adjacent to the proximal hamstring origin, was the most common abnormal imaging finding. This is illustrated in Figure 1. Findings consistent with tendinopathy were shown by ultrasound in 16.9% and by MRI in 25.7% of patients, as Fig year-old woman with proximal hamstring peritendinitis. A, Axial T2-weighted fat-suppressed image shows increased T2 signal intensity surrounding hamstring tendons at their origin (arrowhead), suggestive of peritendinitis. B, Corresponding sagittal ultrasound image shows peritendinous fluid collection (arrows) superficial to hamstring tendon (t) at its origin at ischial tuberosity (it). 994 AJR:195, October 2010
3 Imaging of High Hamstring Tendinopathy Fig year-old woman with proximal hamstring tendinopathy. A, Axial T2-weighted fat-suppressed image reveals increased T2 signal within tendon origin (arrowhead), consistent with tendinopathy. B, Corresponding ultrasound image shows hypoechogenicity and heterogeneity (arrows) of hamstring tendon (t) at its origin at ischial tuberosity (it). shown in Figure 2. Ultrasound is incapable of detecting bone marrow edema, and no discrete partial tears were evident on ultrasound on retrospective image review. MRI showed bone marrow edema and small (< 5 mm) foci of near fluid signal, suggesting partial tearing at the proximal hamstring tendon origin in 20% of the studies (Fig. 3). As indicated above, patients with MR findings consistent with discrete partial tears involving the majority of the cross-section of one of the hamstring components or greater were not believed appropriate for percutaneous steroid injection. As shown in Figure 4, ultrasound was capable of depicting echogenic intratendinous foci consistent with calcifications in 4.6% of patients. The technique of percutaneous injection is described in Materials and Methods. Figure 5 shows a frame from the real-time ultrasound images during a typical injection. Clinical Outcomes A total of 65 injections were performed, with a mean time to follow-up of 4 years (range, 6 months to 8 years). A total of 38 of the original 65 patients responded to our survey (Table 2). In terms of the degree of pain relief after injection, 11 patients who responded had complete resolution of symptoms, eight had moderate resolution, and 10 had mild resolution. Nine patients experienced no pain relief either immediately or later after the injection. The duration of symptom resolution was longer than 6 months for nine (23.7%) of the 38 patients, 1 6 months for 10 patients (26.3%), 1 week to 1 month for 9 patients (23.7%), and less than 1 week for one patient (2.6%). The same nine patients who did not experience any pain relief immediately after the injection also felt no later benefit of the injection. In addition to assessment of symptomatic relief from corticosteroid injection, we surveyed study patients regarding other treatment techniques. We found that that 26 (68.4%) of 38 patients had taken oral nonsteroidal antiinflammatory medications before the ultrasound-guided peritendinous injection. The remaining 12 patients (31.6%) took no prior medication, whereas one had a previous steroid injection without ultrasound guidance. The majority of patients (30/38 [79%]) had undergone physical therapy before the injection. In terms of the ultimate outcome, 27 (71.0%) of 38 patients reported returning to their presymptom level of activity after the injection, and three of these individuals actually described a higher level of activity. At the time of follow-up questioning, seven of the patients (18.4%) had not been able to Fig year-old man with proximal hamstring injury and bone marrow edema. Axial T2-weighted fat-suppressed image shows bone marrow edema (arrows) within ischial tuberosity adjacent to hamstring tendon origin. There is also partial undersurface irregularity of adjacent hamstring tendons. Fig year-old man with hamstring injury. Sagittal ultrasound image shows small focus of hyperechogenicity consistent with calcification (arrow). it = ischial tuberosity. Fig year-old man with proximal hamstring tendinopathy. Sagittal ultrasound image shows 22-gauge needle in place (arrowheads) for sonography-guided injection. Tip is immediately adjacent to superficial surface of hamstring tendon (t). it = ischial tuberosity. AJR:195, October
4 Zissen et al. TABLE 2: Clinical Outcomes for 38 of 65 Patients Receiving Ultrasound- Guided Corticosteroid Anesthetic Injection TABLE 3: Duration of Symptoms and Imaging Characteristics Associated With Significant Symptomatic Improvement Characteristic Duration of symptoms < 1 y 0.5 Normal MRI finding 0.39 Normal ultrasound finding 0.02 Presence of tendinopathy on MRI or ultrasound 0.55 Presence of peritendinitis on MRI or ultrasound 0.14 a Fisher s exact test. Characteristic Duration of symptoms before injection return to the level of activity they enjoyed before the onset of symptoms. None of the contacted patients experienced significant complications due to the injection. To assess for imaging features that might be predictive of a positive response to steroid injections, we tested for associations between each of the imaging features in Table 2 and the clinical outcome we defined as significant improvement. The duration of symptoms before injection, the absence of MRI findings, and the presence of tendinopathy or peritendinitis on either technique were not statistically predictive of response to therapy (Table 3). There was, however, a statistically significant association between the absence of findings on ultrasound and a significant clinical response to therapy with a p value of No. (%) of Patients < 6 m 8 (21) 6 m to 1 y 15 (39.5) > 1 y 15 (39.5) Degree of symptom resolution No resolution 9 (23.7) Mild resolution 10 (26.3) Moderate resolution 8 (21) Complete resolution 11 (28.9) Duration of symptom resolution No resolution 9 (23.7) < 1 wk 1 (2.6) 1 wk to 1 m 9 (23.7) 1 6 m 10 (26.3) > 6 m 9 (23.7) p a Discussion Proximal hamstring tendinopathy is increasingly being recognized as an important cause for chronic pain in the active population [7, 8]. This injury is distinct from the more common type of acute muscle strain that is typically limited to the myotendinous junction of the biceps femoris muscle and is routinely managed clinically with the protocol of rest, ice, compression, and elevation as the preferred first-line approach [1, 4]. For proximal hamstring tendinopathy, treatments such as antiinflammatory medications for pain control as well as rehabilitation programs involving soft-tissue mobilization, frequent stretching, and progressive strengthening can help the hamstring muscles regain flexibility and are frequently used in attempts to prevent further injury or reinjury [2, 5]. For the majority of conservatively managed patients, the time to full recovery is typically 2 6 months. However, in up to 20% of patients, symptoms can persist for more than 6 months and become recalcitrant to conservative treatment [9, 10]. With more frequent use of ultrasound and MRI in these patients, we are increasingly able to diagnose the source of the pain and focus our treatments specifically to the injured muscle. Adler et al. [11, 12] have described an effective method of ultrasound-guided anesthetic corticosteroid injections into the adjacent bursa of the iliopsoas tendon that is useful in diagnosing and treating exerciserelated iliopsoas pathology. Although peritendinous hamstring injections have been reported by other groups in limited numbers, the efficacy of this technique has not been evaluated. This work represents our institution s substantial experience with imaging of the hamstring origin and sonographically guided percutaneous treatments in the setting of a clinical diagnosis of high hamstring tendinopathy. Areas of proximal hamstring tendinopathy were identified by locating the thickened and hypoechoic areas of tendon on sonography, allowing us to target our therapy to this location under direct visualization. Ultrasound is a low-cost nonionizing readily available technique for the evaluation of tendons, muscles, cysts, and other fluid collections. Ultrasound guidance for soft-tissue injections has been found to be an excellent tool for needle localization because of the real-time imaging and excellent resolution of desired structures [13 16]. In the setting of tendinopathy, it is hypothesized that the use of corticosteroids is beneficial by limiting the chronic inflammation that may lead to tendon scarring and adhesion formation [17 19]. Although there is concern that the introduction of corticosteroids to a site of injury could limit healing and subsequently weaken the underlying tendon, leading to future degeneration and rupture, there is no reliable documentation of the deleterious effects of peritendinous injections [7, 20]. It has also been suggested by multiple groups that the major benefit of performing these injections with ultrasound guidance is the accurate placement of the injection into the tendon sheath, avoiding the tendon itself and thereby minimizing adverse events [11, 16]. The immediate improvement of symptoms resulting from the injected anesthetic also serves as a clinical indicator that the medication was delivered accurately and that the hamstring tendon was indeed the cause of the patient s discomfort. The goals of imaging in the setting of hamstring pain are threefold to confirm injury, to provide a comprehensive assessment of the extent of the injury, and to identify which patients may benefit from intervention. In our study, both MRI and ultrasound were found 996 AJR:195, October 2010
5 Imaging of High Hamstring Tendinopathy to be helpful in determining the extent of the injury and detecting imaging findings suggestive of tendinopathy in patients with clinical symptoms suggestive of high hamstring tendinopathy. However, MRI was more sensitive overall in detecting both chronic and acuteon-chronic hamstring pathologic abnormalities, particularly peritendinitis. Peritendinous fluid or edema was seen in 62.9% of patients on MRI, compared with only 20% on ultrasound. As would be expected, MRI was the only technique capable of detecting associated bone marrow edema within the ischial tuberosity. At the same time, ultrasound was able to detect calcifications in the hamstring tendons in a subset of patients, findings that were not apparent on MRI. The main advantage of ultrasound is the real-time imaging capability and excellent spatial resolution, which allows targeted therapy. The ultrasound findings were compatible with the MRI findings in 13 of the 35 patients, revealing peritendinitis in three patients and tendinopathy in four patients. In six patients, the hamstring tendons appeared unremarkable on both the ultrasound and MRI studies. The imaging studies were discordant in 22 patients, with 20 studies showing abnormal findings on MRI that were not apparent on ultrasound (16 peritendinitis and four tendinopathy). In two patients, there were positive findings of peritendinous fluid on ultrasound that were not apparent on the MRI. However, these differences may be due, in part, to the time interval between the original MRI scan and subsequent ultrasound. Although MRI is quite sensitive for detecting peritendinous edema, it is possible in some cases that ultrasound might be able to detect small amounts of fluid that are not obvious on MRI. Similarly, the absence of findings on ultrasound may be due to resolution of edema during the time interval between the MRI and ultrasound. To provide rigorous comparison on the sensitivity of MRI and ultrasound, a much shorter time interval between studies would be needed. Our findings suggest that MRI is more sensitive overall than ultrasound in the diagnosis of proximal hamstring pathologic abnormalities. However, ultrasound imaging is more readily available and may be considered a reasonable alternative for initial diagnosis and treatment, reserving MRI for evaluating cases where the first attempt at therapeutic intervention is not effective. This is consistent with the study conducted by Unverferth and Olix [19], who reported that ultrasound approximates MRI in depicting acute hamstring injuries where peritendinous fluid may be the predominant imaging finding, whereas MRI is more sensitive for follow-up of chronic hamstring injuries where tendinopathy may be the predominant imaging finding. It is notable that neither MRI nor ultrasound was highly sensitive in defining an abnormality of the hamstring tendons as the responsible pain generator. Nearly 23% of MR studies and 62% of ultrasound studies were considered normal; however, a substantial number of patients with normal studies benefited from corticosteroid injection. These results underscore the importance of having a skilled clinician for patient assessment, referral to diagnostic imaging, and referral for imaging-guided injection. In general, ultrasound-guided interventions are increasingly being used as adjuvant treatment in chronic musculoskeletal pain [11, 13 17, 21]. Our study confirms that ultrasoundguided corticosteroid injections are a safe and effective treatment in patients who are recalcitrant to conservative management. All but nine of the patients in our study reported immediate symptomatic improvement after injection of the local anesthetic, confirming that the hamstring tendon was indeed the cause of their discomfort. No significant side effects or complications were reported by any of the patients undergoing injection. Furthermore, there was an excellent clinical response to corticosteroid injection, with 50% of patients reporting moderate-to-complete resolution of their symptoms for at least 1 month after the injection and 28.9% reporting complete and sustained resolution of symptoms postinjection. Even though some patients did experience complete pain resolution after the injection, an adequate treatment plan should also include physical therapy and activity modification to allow healing. In the population reported here, inciting activities such as long-distance running or sprinting were curtailed but patients were engaged in crosstraining sports or deep water pool running to maintain overall fitness. The only imaging characteristic that was associated with a statistically significant improvement in outcomes was the absence of findings on ultrasound. We hypothesize that those patients with normal ultrasound findings likely had more mild injuries that perhaps would have resolved on their own over time. In these patients, MRI would not be useful to further characterize their condition. Conversely, in patients with abnormal ultrasound examinations, further trials would be necessary to evaluate whether MRI could be useful in further characterizing their injury and possibly predict which patients would benefit from intervention. In our discussions with study participants, we also observed a trend that those patients who had longer periods of rest and physical therapy before resuming their prior activity level experienced longer lasting relief of symptoms. Subsequent studies are necessary to further evaluate the relationship of rest to overall symptom resolution. A more in-depth understanding of the pathophysiologic features of hamstring tendinopathy and associated imaging findings may help predict which patients would benefit most from intervention. A prospective study correlating imaging findings with symptoms, response to treatment, and clinical outcomes would further elucidate the mechanism of chronic tendon degeneration and repair. This knowledge may, in turn, benefit future studies looking at the potential of biologic therapies for treatment of tendon pathologic abnormalities, such as platelet-rich plasma injection [22, 23], a technique for which there are no published data on hamstring tendinopathy at this time, to our knowledge. This study has several limitations. We were unable to identify a matched control cohort of patients who did not receive corticosteroid injection. However, 79% of our patients had symptoms lasting longer than 6 months before the injection, thereby in principle serving as their own controls. The study was retrospective and relied on patient recall of symptoms dating back to 2002 in some cases. There was a variable time to follow-up for each patient, and the time difference between MRI and ultrasound studies was relatively long, owing to periods of conservative therapy undertaken between MRI diagnosis and ultrasoundguided injection. Furthermore, the subjective nature of the pain questionnaire used made it difficult to standardize the effectiveness of the procedure across the patients. Although the results were favorable, too few patients replied to the survey to allow rigorous statistical confirmation of our findings. As a result, our findings do not help refine selection criteria for patients to undergo proximal hamstring injection. Therefore, a prospective, randomized study evaluating the MRI and ultrasound imaging findings and efficacy of corticosteroid injections would be beneficial to evaluate the true potential of this procedure. In conclusion, the use of ultrasound-guided injections of corticosteroid and local anesthetic is a safe and effective technique that AJR:195, October
6 Zissen et al. can provide both immediate and long-term symptomatic relief of proximal hamstring pain in appropriately referred patients. Advances in ultrasound-guided interventional techniques allow accurate needle localization to optimize the diagnostic and therapeutic effectiveness with minimal morbidity. This procedure should be performed in conjunction with physical therapy and a progressivestrengthening program to achieve optimal results, and avoid recurrent injury leading to a more prolonged period of convalescence. This technique serves as an excellent adjuvant in the treatment of chronic hamstring injuries recalcitrant to conservative management. Acknowledgment We thank the Stanford Transactional Research Integrated Database Environment for performing the computerized search of our imaging databases. References 1. Clanton TO, Coupe KJ. Hamstring strains in athletes: diagnosis and treatment. J Am Acad Orthop Surg 1998; 6: Croisier JL. Factors associated with recurrent hamstring injuries. Sports Med 2004; 34: De Smet AA, Best TM. MR imaging of the distribution and location of acute hamstring injuries in athletes. AJR 2000; 174: Kujala UM, Orava S, Jarvinen M. Hamstring injuries: current trends in treatment and prevention. Sports Med 1997; 23: Malliaropoulos N, Papalexandris S, Papalada A, Papacostas E. The role of stretching in rehabilitation of hamstring injuries: 80 athletes follow-up. Med Sci Sports Exerc 2004; 36: Fredricson M, Moore W, Guillet M, Beaulieu C. High hamstring injuries: etiology, diagnosis, and treatment. Phys Sports Med 2005; 33: Lempainen L, Sarimo J, Mattila K, et al. Proximal hamstring tendinopathy: results of surgical management and histopathologic findings. Am J Sports Med 2009; 37: Puranen J, Orava S. The hamstring syndrome: a new diagnosis of gluteal sciatic pain. Am J Sports Med 1988; 16: Khan K, Cook J. The painful nonruptured tendon: clinical aspects. Clin Sports Med 2003; 22: Wilson JJ, Best TM. Common overuse tendon problems: a review and recommendations for treatment. Am Fam Physician 2005; 72: Adler RS, Buly R, Ambrose R, Sculco T. Diagnostic and therapeutic use of sonography-guided iliopsoas peritendinous injections. AJR 2005; 185: Adler RS, Sofka CM. Percutaneous ultrasoundguided injections in the musculoskeletal system. Ultrasound Q 2003; 19: Bentley S. The treatment of sports injuries by local injection. Br J Sports Med 1981; 15: Cardinal E, Chhem RK, Beauregard CG. Ultrasound-guided interventional procedures in the musculoskeletal system. Radiol Clin North Am 1998; 36: Kannus P, Jarvinen M, Niittymaki S. Long- or short-acting anesthetic with corticosteroid in local injections of overuse injuries? A prospective, randomized, double-blind study. Int J Sports Med 1990; 11: Sofka CM, Collins AJ, Adler RS. Use of ultrasonographic guidance in interventional musculoskeletal procedures: a review from a single institution. J Ultrasound Med 2001; 20: Fredberg U. Local corticosteroid injection in sport: review of literature and guidelines for treatment. Scand J Med Sci Sports 1997; 7: Levine WN, Bergfeld JA, Tessendorf W, Moorman CT 3rd. Intramuscular corticosteroid injection for hamstring injuries: a 13-year experience in the National Football League. Am J Sports Med 2000; 28: Unverferth LJ, Olix ML. The effect of local steroid injections on tendon. J Sports Med 1973; 1: Lin J, Jacobson JA, Fessell DP, Weadock WJ, Hayes CW. An illustrated tutorial of musculoskeletal sonography. Part 4. Musculoskeletal masses, sonographically guided interventions, and miscellaneous topics. AJR 2000; 175: Scott WA. Injection techniques and use in the treatment of sports injuries. Sports Med 1996; 22: Mishra A, Collado H, Fredericson M. Plateletrich plasma compared with corticosteroid injection for chronic lateral elbow tendinosis. PM & R, 2009; 4: Mishra A, Woodall J Jr, Vieira A. Treatment of tendon and muscle using platelet-rich plasma. Clin Sports Med 2009; 28: AJR:195, October 2010
Fluoroscopically Guided Peritendinous Corticosteroid Injection for Proximal Hamstring Tendinopathy
 Fluoroscopically Guided Peritendinous Corticosteroid Injection for Proximal Hamstring Tendinopathy A Retrospective Review Luke T. Nicholson,* MD, Steven DiSegna,* MD, Joel S. Newman,* MD, and Suzanne L.
Fluoroscopically Guided Peritendinous Corticosteroid Injection for Proximal Hamstring Tendinopathy A Retrospective Review Luke T. Nicholson,* MD, Steven DiSegna,* MD, Joel S. Newman,* MD, and Suzanne L.
Hospital NEO,Turku, Finland
 Hamstring syndrome from fibrous band to tendinosis Sakari Orava, Janne Sarimo, Lasse Lempainen, Jyrki Heinänen Hospital NEO,Turku, Finland 1 Hamstring muscles- ANATOMY over two big joints pelvic stabilizers
Hamstring syndrome from fibrous band to tendinosis Sakari Orava, Janne Sarimo, Lasse Lempainen, Jyrki Heinänen Hospital NEO,Turku, Finland 1 Hamstring muscles- ANATOMY over two big joints pelvic stabilizers
Tendon Fenestration. Disclosures. Outline: questions. Introduction: Peritendon Steroid Injections. Jon A. Jacobson, MD. Patellar Tendon: tendinosis
 Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Common Applications for Sonography and Guided Intervention: Shoulder
 Common Applications for Sonography and Guided Intervention: Shoulder Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant:
Common Applications for Sonography and Guided Intervention: Shoulder Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant:
MR Imaging of the Distribution and Location of Acute Hamstring Injuries in Athletes
 Downloaded from www.ajronline.org by 46.3.197.176 on 2/4/18 from IP address 46.3.197.176. Copyright ARRS. For personal use only; all rights reserved Arthur A. De Smet 1 Thomas M. Best 2 Received May 3,
Downloaded from www.ajronline.org by 46.3.197.176 on 2/4/18 from IP address 46.3.197.176. Copyright ARRS. For personal use only; all rights reserved Arthur A. De Smet 1 Thomas M. Best 2 Received May 3,
Musculoskeletal Imaging Review
 Musculoskeletal Imaging Review Kassarjian et al. MRI of the Quadratus Femoris Musculoskeletal Imaging Review Ara Kassarjian 1 Xavier Tomas 2 Luis Cerezal 3 Ana Canga 4,5 Eva Llopis 6 Kassarjian A, Tomas
Musculoskeletal Imaging Review Kassarjian et al. MRI of the Quadratus Femoris Musculoskeletal Imaging Review Ara Kassarjian 1 Xavier Tomas 2 Luis Cerezal 3 Ana Canga 4,5 Eva Llopis 6 Kassarjian A, Tomas
Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation
 Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
John J Christoforetti, MD Pittsburgh, Pennsylvania
 ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
tissue, Interventional non-vascular /ecr2014/C-1241
 Effectiveness of Ultrasound-guided Platelet Rich Plasma (PRP) injections after needle tenotomy in the treatment of chronic tendinopathies : A prospective study. Poster No.: C-1241 Congress: ECR 2014 Type:
Effectiveness of Ultrasound-guided Platelet Rich Plasma (PRP) injections after needle tenotomy in the treatment of chronic tendinopathies : A prospective study. Poster No.: C-1241 Congress: ECR 2014 Type:
Accuracy of Three Clinical Tests to Diagnose Hamstring Syndrome in Pa:ents with Posterior Hip Pain.
 Accuracy of Three Clinical Tests to Diagnose Hamstring Syndrome in Pa:ents with Posterior Hip Pain. Ricardo G. Schröder, PT 1 ; RobRoy L Mar8n, PT PhD 2 ; Juan Gomez-Hoyos, MD 1,3 ; Anthony Khoury M.Sc.
Accuracy of Three Clinical Tests to Diagnose Hamstring Syndrome in Pa:ents with Posterior Hip Pain. Ricardo G. Schröder, PT 1 ; RobRoy L Mar8n, PT PhD 2 ; Juan Gomez-Hoyos, MD 1,3 ; Anthony Khoury M.Sc.
Disclosure. Pre-Procedural Considerations. Transducer Selection. Sterile Procedure. Sterile Procedure. Ultrasound Guided Foot and Ankle Injections
 Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
Ultrasound Guided Foot and Ankle Injections Disclosure No relevant financial relationships exist Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012
Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions
 APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
Stress-Related Injuries Around the Lesser Trochanter in Long-Distance Runners
 Musculoskeletal Imaging Clinical Observations Nguyen et al. Stress Injury Around Lesser Trochanter Musculoskeletal Imaging Clinical Observations Josephine T. Nguyen 1 Jeffrey S. Peterson 2 Sandip Biswal
Musculoskeletal Imaging Clinical Observations Nguyen et al. Stress Injury Around Lesser Trochanter Musculoskeletal Imaging Clinical Observations Josephine T. Nguyen 1 Jeffrey S. Peterson 2 Sandip Biswal
Endoscopic Hamstring Repair and Ischial Bursectomy. Carlos A. Guanche, MD Southern California Orthopedic Institute
 Endoscopic Hamstring Repair and Ischial Bursectomy Carlos A. Guanche, MD Southern California Orthopedic Institute cguanche@scoi.com 1 Endoscopic Hamstring Repair and Ischial Bursectomy INTRODUCTION Hamstring
Endoscopic Hamstring Repair and Ischial Bursectomy Carlos A. Guanche, MD Southern California Orthopedic Institute cguanche@scoi.com 1 Endoscopic Hamstring Repair and Ischial Bursectomy INTRODUCTION Hamstring
SEMIMEMBRANOSUS TENDINITIS
 SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Case study #11 Rt. knee
 The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
Sonographically Guided Flexor Hallucis Longus Tendon Sheath Injection
 Technical dvance Sonographically Guided Flexor Hallucis Longus Tendon Sheath Injection mir Mehdizade, MD, Ronald S. dler, PhD, MD Objective. The purpose of this study was to describe a sonographically
Technical dvance Sonographically Guided Flexor Hallucis Longus Tendon Sheath Injection mir Mehdizade, MD, Ronald S. dler, PhD, MD Objective. The purpose of this study was to describe a sonographically
Sonographically Guided Percutaneous Needle Tenotomy for the Treatment of Chronic Tendinosis
 Article Sonographically Guided Percutaneous Needle Tenotomy for the Treatment of Chronic Tendinosis Jeffrey A. Housner, MD, Jon A. Jacobson, MD, Roberta Misko, PT, PA-C Objective. Initial reports have
Article Sonographically Guided Percutaneous Needle Tenotomy for the Treatment of Chronic Tendinosis Jeffrey A. Housner, MD, Jon A. Jacobson, MD, Roberta Misko, PT, PA-C Objective. Initial reports have
Greater Trochanter: Anatomy and Pathology
 Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Greater Trochanter: Anatomy and Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties:
Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review
 Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review Poster No.: P-0127 Congress: ESSR 2015 Type: Educational Poster Authors: A. Karsandas, J. Tuckett, R. Sinha,
Ultrasound Guided Therapeutic Injections in the Treatment of Shoulder Pain: A Multimedia Review Poster No.: P-0127 Congress: ESSR 2015 Type: Educational Poster Authors: A. Karsandas, J. Tuckett, R. Sinha,
Can therapeutic ultrasound accurately detect bone stress injuries in athletes?
 Can therapeutic ultrasound accurately detect bone stress injuries in athletes? Author Beck, Belinda Ruth Published 2013 Journal Title Clinical Journal of Sport Medicine DOI https://doi.org/10.1097/jsm.0b013e3182926bda
Can therapeutic ultrasound accurately detect bone stress injuries in athletes? Author Beck, Belinda Ruth Published 2013 Journal Title Clinical Journal of Sport Medicine DOI https://doi.org/10.1097/jsm.0b013e3182926bda
Using proximal hamstring tendons as a landmark for ultrasound- and CT-guided injections of ischiofemoral impingement
 Radiology Case Reports Using proximal hamstring tendons as a landmark for ultrasound- and CT-guided injections of ischiofemoral impingement Yulia Volokhina, DO, and David Dang, MD Volume 8, Issue 1, 2013
Radiology Case Reports Using proximal hamstring tendons as a landmark for ultrasound- and CT-guided injections of ischiofemoral impingement Yulia Volokhina, DO, and David Dang, MD Volume 8, Issue 1, 2013
COMPARATIVE EFFECTIVENESS OF ULTRASOUND GUIDED INTRATENDINOUS PROLOTHERAPY INJECTION WITH CONVENTIONAL TREATMENT TO TREAT
 SCIENTIFIC ARTICLE COMPARATIVE EFFECTIVENESS OF ULTRASOUND GUIDED INTRATENDINOUS PROLOTHERAPY INJECTION WITH CONVENTIONAL TREATMENT TO TREAT FOCAL SUPRASPINATUS TENDINOSIS : RANDOMISED CONTROL STUDY 1,2
SCIENTIFIC ARTICLE COMPARATIVE EFFECTIVENESS OF ULTRASOUND GUIDED INTRATENDINOUS PROLOTHERAPY INJECTION WITH CONVENTIONAL TREATMENT TO TREAT FOCAL SUPRASPINATUS TENDINOSIS : RANDOMISED CONTROL STUDY 1,2
With the advent and further refinement of hip arthroscopy
 Endoscopic Proximal Hamstring Repair and Ischial Bursectomy Brian D. Dierckman, M.D., and Carlos A. Guanche, M.D. Abstract: With the significant increase in use of the arthroscope around the hip have come
Endoscopic Proximal Hamstring Repair and Ischial Bursectomy Brian D. Dierckman, M.D., and Carlos A. Guanche, M.D. Abstract: With the significant increase in use of the arthroscope around the hip have come
Benefits of Aspiration and Injection JOINT INJECTIONS. Injection Indications. Mechanism of Action 1/11/2016
 Benefits of Aspiration and Injection JOINT INJECTIONS Mark Niedfeldt, M.D. Medical College of Wisconsin Decrease or resolution of pain Decrease or resolution of inflammation Decrease or resolution of effusion
Benefits of Aspiration and Injection JOINT INJECTIONS Mark Niedfeldt, M.D. Medical College of Wisconsin Decrease or resolution of pain Decrease or resolution of inflammation Decrease or resolution of effusion
Musculoskeletal Ultrasound Fundamentals
 Fundamentals Benjamin D. Levine, M.D. Associate Professor of Radiology Musculoskeletal Imaging Dept. of Radiological Sciences UCLA Health System I. Image Optimization II. Image Interpretation Artifacts
Fundamentals Benjamin D. Levine, M.D. Associate Professor of Radiology Musculoskeletal Imaging Dept. of Radiological Sciences UCLA Health System I. Image Optimization II. Image Interpretation Artifacts
Ultrasound of the Knee
 Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 10/6/2012 Radiology Quiz of the Week # 93 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 10/6/2012 Radiology Quiz of the Week # 93 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
US guided treatment in calcific tendinopathy of body tendons: Techniques and follow-up
 US guided treatment in calcific tendinopathy of body tendons: Techniques and follow-up Poster No.: C-2369 Congress: ECR 2010 Type: Scientific Exhibit Topic: Musculoskeletal - Soft Tissue Authors: T. De
US guided treatment in calcific tendinopathy of body tendons: Techniques and follow-up Poster No.: C-2369 Congress: ECR 2010 Type: Scientific Exhibit Topic: Musculoskeletal - Soft Tissue Authors: T. De
BICEPS TENDON TENDINITIS (PROXIMAL) AND TENOSYNOVITIS
 BICEPS TENDON TENDINITIS (PROXIMAL) AND TENOSYNOVITIS Description Proximal biceps tendon tendinitis and tenosynovitis is characterized by pain at the front of the shoulder and upper arm caused by inflammation
BICEPS TENDON TENDINITIS (PROXIMAL) AND TENOSYNOVITIS Description Proximal biceps tendon tendinitis and tenosynovitis is characterized by pain at the front of the shoulder and upper arm caused by inflammation
Key words: Laser, sprain, strain, lameness, tendon
 MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
Original Report. Sonography of Tears of the Distal Biceps Tendon. Theodore T. Miller 1,2 Ronald S. Adler 3
 Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
Note: Page numbers of article titles are in boldface type. A ACJ. See Acromioclavicular joint (ACJ) Acromioclavicular joint (ACJ) procedures of, 557 559 Ankle and foot procedures of, 649 671 (See also
Hamstring Injury: When to Consider Surgical Treatment
 Hamstring Injury: When to Consider Surgical Treatment Prof. dr. Gino Kerkhoffs Orthopaedic Surgery www.acesamsterdam.nl Gino Kerkhoffs Hans Tol Guus Reurink Mario Maas Pau Golanó Rolf Peters Maarten Moen
Hamstring Injury: When to Consider Surgical Treatment Prof. dr. Gino Kerkhoffs Orthopaedic Surgery www.acesamsterdam.nl Gino Kerkhoffs Hans Tol Guus Reurink Mario Maas Pau Golanó Rolf Peters Maarten Moen
Case study #12 Left knee
 The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
Ultrasound-Guided Biceps Peritendinous Injections in the Absence of a Distended Tendon Sheath
 TECHNICAL INNOVATION Ultrasound-Guided Biceps Peritendinous Injections in the Absence of a Distended Tendon Sheath A Novel Rotator Interval Approach Taylor J. Stone, MD, Ronald S. Adler, MD, PhD This retrospective
TECHNICAL INNOVATION Ultrasound-Guided Biceps Peritendinous Injections in the Absence of a Distended Tendon Sheath A Novel Rotator Interval Approach Taylor J. Stone, MD, Ronald S. Adler, MD, PhD This retrospective
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation. Disclosures. Outline. Joint Effusion. Suprapatellar recess
 Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Management of Chronic Plantar Fasciitis using Hyperosmolar Dextrose Injection Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Management of Chronic Plantar Fasciitis using Hyperosmolar Dextrose Injection Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid
Dominic Carreira M.D. Matt Kruchten, B.S. Fort Lauderdale, FL
 Dominic Carreira M.D. Matt Kruchten, B.S Fort Lauderdale, FL Disclosures ConMed Linvatec: Consulting and Education Zimmer Biomet Consulting and Education Royalties for Product Development The hamstring
Dominic Carreira M.D. Matt Kruchten, B.S Fort Lauderdale, FL Disclosures ConMed Linvatec: Consulting and Education Zimmer Biomet Consulting and Education Royalties for Product Development The hamstring
Original Report. Sonography of Ankle Tendon Impingement with Surgical Correlation
 Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Ultrasound-Guided Tendon Fenestration
 85 Mary M. Chiavaras, MD, PhD 1 Jon A. Jacobson, MD 2 1 Department of Radiology, McMaster University, Hamilton General Hospital, Hamilton, Ontario, Canada 2 Department of Radiology, University of Michigan,
85 Mary M. Chiavaras, MD, PhD 1 Jon A. Jacobson, MD 2 1 Department of Radiology, McMaster University, Hamilton General Hospital, Hamilton, Ontario, Canada 2 Department of Radiology, University of Michigan,
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
Rotator Cuff and Biceps Pathology
 Rotator Cuff and Biceps Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board:
Rotator Cuff and Biceps Pathology Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board:
MRI of Quadratus Femoris Muscle Tear: Another Cause of Hip Pain
 MRI of Quadratus Femoris Muscle Tear Musculoskeletal Imaging Clinical Observations Seth D. O Brien 1 Liem T. Bui-Mansfield 1,2,3 O Brien SD, Bui-Mansfield LT Keywords: hip pain, MRI, muscle tear, quadratus
MRI of Quadratus Femoris Muscle Tear Musculoskeletal Imaging Clinical Observations Seth D. O Brien 1 Liem T. Bui-Mansfield 1,2,3 O Brien SD, Bui-Mansfield LT Keywords: hip pain, MRI, muscle tear, quadratus
Servers Disease (Calcaneal Apophysitis ) 101
 Servers Disease (Calcaneal Apophysitis ) 101 Servers Disease Causes a disturbance to the growing area at the back of the heel bone (calcaneus) where the strong Achilles tendon attaches to it. It is most
Servers Disease (Calcaneal Apophysitis ) 101 Servers Disease Causes a disturbance to the growing area at the back of the heel bone (calcaneus) where the strong Achilles tendon attaches to it. It is most
3/20/2017. Disclosures. Ultrasound Fundamentals. Ultrasound Fundamentals. Bone Anatomy. Tissue Characteristics
 Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
Sonographic Target Sign in Neurofibromas
 Sonographic Target Sign in Neurofibromas John Lin, MD, Jon A. Jacobson, MD, Curtis W. Hayes, MD Neurofibromas are the most common tumors of the peripheral nerves. They may be solitary lesions, multiple
Sonographic Target Sign in Neurofibromas John Lin, MD, Jon A. Jacobson, MD, Curtis W. Hayes, MD Neurofibromas are the most common tumors of the peripheral nerves. They may be solitary lesions, multiple
Achilles Tendon Anatomy. Achilles Tendon Anatomy. Acute Achilles Rupture. Acute Achilles Rupture 8/19/14. Primary plantarflexor
 Disclosure Conditions of the Achilles Tendon Brian Clowers, M.D. I have no financial relationships that would influence the content of this presentation Oklahoma Sports and Orthopedic Institute September
Disclosure Conditions of the Achilles Tendon Brian Clowers, M.D. I have no financial relationships that would influence the content of this presentation Oklahoma Sports and Orthopedic Institute September
Sonographic Evaluation of Tears of the Gastrocnemius Medial Head ( Tennis Leg )
 Sonographic Evaluation of Tears of the Gastrocnemius Medial Head ( Tennis Leg ) Stefano Bianchi, MD, Carlo Martinoli, MD, Ibrahim Fikry Abdelwahab, MD, Lorenzo E. Derchi, MD, Sandro Damiani, MD Rupture
Sonographic Evaluation of Tears of the Gastrocnemius Medial Head ( Tennis Leg ) Stefano Bianchi, MD, Carlo Martinoli, MD, Ibrahim Fikry Abdelwahab, MD, Lorenzo E. Derchi, MD, Sandro Damiani, MD Rupture
The Role of Sonography in Differentiating Full Versus Partial Distal Biceps Tendon Tears: Correlation With Surgical Findings
 Musculoskeletal Imaging Original Research Da Gama Lobo et al. Sonography in Biceps Tendon Tears Musculoskeletal Imaging Original Research Lucas Da Gama Lobo 1,2 David P. Fessell 1 Bruce S. Miller 1,3 Aine
Musculoskeletal Imaging Original Research Da Gama Lobo et al. Sonography in Biceps Tendon Tears Musculoskeletal Imaging Original Research Lucas Da Gama Lobo 1,2 David P. Fessell 1 Bruce S. Miller 1,3 Aine
ELENI ANDIPA General Hospital of Athens G. Gennimatas
 ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
Tendinopathy from Overuse: Overview and a New(er) Treatment Option
 Tendinopathy from Overuse: Overview and a New(er) Treatment Option Robert Flannery MD Assistant Professor, Division of Sports Medicine Department of Orthopedic Surgery, Case Western Reserve University
Tendinopathy from Overuse: Overview and a New(er) Treatment Option Robert Flannery MD Assistant Professor, Division of Sports Medicine Department of Orthopedic Surgery, Case Western Reserve University
Proximal Hamstring Tendinosis and Partial Ruptures
 Proximal Hamstring Tendinosis and Partial Ruptures Ashley N. Startzman, DO; Oliver Fowler, BS; Dominic Carreira, MD abstract Proximal hamstring tendinosis and partial hamstring origin ruptures are painful
Proximal Hamstring Tendinosis and Partial Ruptures Ashley N. Startzman, DO; Oliver Fowler, BS; Dominic Carreira, MD abstract Proximal hamstring tendinosis and partial hamstring origin ruptures are painful
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Ultrasound assessment of Achilles tendon tear
 Ultrasound assessment of Achilles tendon tear Poster No.: C-1955 Congress: ECR 2015 Type: Educational Exhibit Authors: S. Stefurac, E. O. Arhire, D. Negru; Iasi/RO Keywords: Trauma, Inflammation, Acute,
Ultrasound assessment of Achilles tendon tear Poster No.: C-1955 Congress: ECR 2015 Type: Educational Exhibit Authors: S. Stefurac, E. O. Arhire, D. Negru; Iasi/RO Keywords: Trauma, Inflammation, Acute,
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology?
 Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
MR imaging of the quadratus femoris: Anatomic considerations and pathologic lesions
 MR imaging of the quadratus femoris: Anatomic considerations and pathologic lesions Poster No.: C-2355 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: A. Kassarjian, X. Tomás,
MR imaging of the quadratus femoris: Anatomic considerations and pathologic lesions Poster No.: C-2355 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: A. Kassarjian, X. Tomás,
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
Platelet-Rich Plasma Compared With Other Common Injection Therapies in the Treatment of Chronic Lateral Epicondylitis
 Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
Alex Garcia, MD Affinity Orthopedics and Sports Medicine
 Alex Garcia, MD Affinity Orthopedics and Sports Medicine Intact Tendon Reactive Inflammatory Tendinopathy Degenerative Chronic Tendinopathy INSULT Neurovascular Mediation Reparative Process? Healed 3
Alex Garcia, MD Affinity Orthopedics and Sports Medicine Intact Tendon Reactive Inflammatory Tendinopathy Degenerative Chronic Tendinopathy INSULT Neurovascular Mediation Reparative Process? Healed 3
Sonography of the Acetabular Labrum
 Case Series Visualization of Labral Injuries During Intra-Articular Injections Carolyn M. Sofka, MD, Ronald S. Adler, PhD, MD, Martha A. Danon, MD Objective. The purpose of this series was to describe
Case Series Visualization of Labral Injuries During Intra-Articular Injections Carolyn M. Sofka, MD, Ronald S. Adler, PhD, MD, Martha A. Danon, MD Objective. The purpose of this series was to describe
Practical Reporting of Musculoskeletal Imaging Studies: MRI Elbow
 Practical Reporting of Musculoskeletal Imaging Studies: MRI Elbow James F Griffith History Where is pain located? For how long? Trauma if so, what and when Radiographers can get this info Grade. Don t
Practical Reporting of Musculoskeletal Imaging Studies: MRI Elbow James F Griffith History Where is pain located? For how long? Trauma if so, what and when Radiographers can get this info Grade. Don t
Principles of Ultrasound. Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012
 Principles of Ultrasound Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012 None Disclosures Outline Introduction Benefits and Limitations of US Ultrasound (US) Physics
Principles of Ultrasound Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012 None Disclosures Outline Introduction Benefits and Limitations of US Ultrasound (US) Physics
Plantar fasciopathy (PFs)
 Plantar fasciopathy (PFs) 2016. 04. 30. Jung-Soo Lee, M.D., Ph.D. Department of Rehabilitation Medicine, Uijeongbu St. Mary's Hospital, College of Medicine, The Catholic University of Korea Anatomy of
Plantar fasciopathy (PFs) 2016. 04. 30. Jung-Soo Lee, M.D., Ph.D. Department of Rehabilitation Medicine, Uijeongbu St. Mary's Hospital, College of Medicine, The Catholic University of Korea Anatomy of
Ultrasound of Shoulder Pathology and Intervention 서울대학교병원재활의학과 김기원
 Ultrasound of Shoulder Pathology and Intervention 서울대학교병원재활의학과 김기원 Ultrasound for Shoulder Disorder Advantage Dynamic evaluation Immediate clinical correlation + Intervention Weakness Diagnostic accuracy?
Ultrasound of Shoulder Pathology and Intervention 서울대학교병원재활의학과 김기원 Ultrasound for Shoulder Disorder Advantage Dynamic evaluation Immediate clinical correlation + Intervention Weakness Diagnostic accuracy?
Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications
 Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications Andrew Lavigne, MD, FRCPC Physical Medicine and Rehabilitation CSCN Diplomat (EMG) Dip Sport Medicine Eugene Maida, MD, PGY-4 Resident
Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications Andrew Lavigne, MD, FRCPC Physical Medicine and Rehabilitation CSCN Diplomat (EMG) Dip Sport Medicine Eugene Maida, MD, PGY-4 Resident
Intratendinous tears of the Achilles tendon - a new pathology? Analysis of a large 4 year cohort.
 Intratendinous tears of the Achilles tendon - a new pathology? Analysis of a large 4 year cohort. Poster No.: C-1680 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Morton, T. Parkes, O. Chan,
Intratendinous tears of the Achilles tendon - a new pathology? Analysis of a large 4 year cohort. Poster No.: C-1680 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Morton, T. Parkes, O. Chan,
A Patient s Guide to Posterior Tibial Tendon Problems
 A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Posterior Tibial Tendon Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Doc, I've done my groin. Groin Pain. Peter Brukner. Doc, I've done my groin 1. acute chronic
 Doc, I've done my groin Peter Brukner Associate Professor in Sports Medicine Centre for Sports Medicine Research and Education School of Physiotherapy 9/22/2006 The University of Melbourne Groin Pain acute
Doc, I've done my groin Peter Brukner Associate Professor in Sports Medicine Centre for Sports Medicine Research and Education School of Physiotherapy 9/22/2006 The University of Melbourne Groin Pain acute
A Patient s Guide to Trochanteric Bursitis of the Hip
 A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
Interesting Case Series. Morel-Lavallée Lesion
 Interesting Case Series Morel-Lavallée Lesion Jonathan Miller, BS, a Justin Daggett, MD, a RajAmbay,MD, b and WyattG.Payne,MD c a Division of Plastic Surgery, Department of Surgery, University of South
Interesting Case Series Morel-Lavallée Lesion Jonathan Miller, BS, a Justin Daggett, MD, a RajAmbay,MD, b and WyattG.Payne,MD c a Division of Plastic Surgery, Department of Surgery, University of South
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
Case study # 6 Sharon P
 Patient is a morbidly obese 70 year old female presenting with left shoulder pain after a severe fall. Patient is in moderate to severe pain with extremely limited range of motion due to extensive shoulder
Patient is a morbidly obese 70 year old female presenting with left shoulder pain after a severe fall. Patient is in moderate to severe pain with extremely limited range of motion due to extensive shoulder
HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY
 HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY EDMONTON BREWERY DISTRICT DOWNTOWN Edmonton s First Boutique Physiotherapy Clinic WHAT SETS US APART? NO ATHLETE IS TRULY TESTED UNTIL THEY VE STARED INJURY
HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY EDMONTON BREWERY DISTRICT DOWNTOWN Edmonton s First Boutique Physiotherapy Clinic WHAT SETS US APART? NO ATHLETE IS TRULY TESTED UNTIL THEY VE STARED INJURY
Normal Anatomy and Strains of the Deep Musculotendinous Junction of the Proximal Rectus Femoris: MRI Features
 Musculoskeletal Imaging Clinical Observations Gyftopoulos et al. MRI of the Proximal Rectus Femoris Musculotendinous Junction Musculoskeletal Imaging Clinical Observations Soterios Gyftopoulos 1 Zehava
Musculoskeletal Imaging Clinical Observations Gyftopoulos et al. MRI of the Proximal Rectus Femoris Musculotendinous Junction Musculoskeletal Imaging Clinical Observations Soterios Gyftopoulos 1 Zehava
Spondylolisthesis DESCRIPTION EXPECTED OUTCOME POSSIBLE COMPLICATIONS COMMON SIGNS AND SYMPTOMS GENERAL TREATMENT CONSIDERATIONS CAUSES
 DESCRIPTION is the slippage of one or more vertebrae, the bones of the spine. Many causes of slippage of the vertebra are possible; these include stress fracture (spondylolysis), which is often seen in
DESCRIPTION is the slippage of one or more vertebrae, the bones of the spine. Many causes of slippage of the vertebra are possible; these include stress fracture (spondylolysis), which is often seen in
Ultrasound assessment of most frequent shoulder disorders
 Ultrasound assessment of most frequent shoulder disorders Poster No.: C-2026 Congress: ECR 2014 Type: Educational Exhibit Authors: S. P. Ivanoski; Ohrid/MK Keywords: Trauma, Athletic injuries, Arthritides,
Ultrasound assessment of most frequent shoulder disorders Poster No.: C-2026 Congress: ECR 2014 Type: Educational Exhibit Authors: S. P. Ivanoski; Ohrid/MK Keywords: Trauma, Athletic injuries, Arthritides,
Piriformis Syndrome. Midwest Bone & Joint Institute 2350 Royal Boulevard Suite 200 Elgin, IL Phone: Fax:
 A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Piriformis Syndrome 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
The Essentials Tissue Characterization and Knobology
 The Essentials Tissue Characterization and Knobology Randy E. Moore, DC, RDMS RMSK No relevant financial relationships Ultrasound The New Standard of Care Musculoskeletal sonography has become the standard
The Essentials Tissue Characterization and Knobology Randy E. Moore, DC, RDMS RMSK No relevant financial relationships Ultrasound The New Standard of Care Musculoskeletal sonography has become the standard
ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW
 PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
PRACTICAL ADVICE ULTRASOUND- GUIDED INJECTIONS A TECHNICAL REVIEW Written by Akira M. Murakami, USA Ultrasound is a powerful modality for guiding the intra-articular injection of both therapeutic medication
Ultrasound of the Hip: Anatomy, Pathology, and Procedures
 Ultrasound of the Hip: Anatomy, Pathology, and Procedures Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Outline Hip Joint Native hip
Ultrasound of the Hip: Anatomy, Pathology, and Procedures Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Outline Hip Joint Native hip
A Patient s Guide to Tendonitis. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Tendonitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Tendonitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Sonography of Knee and Calf Pain: the differential considerations
 Sonography of Knee and Calf Pain: the differential considerations Dr. Lisa L. S.Wong Consultant Radiologist St Paul s Hospital Outline Ultrasound techniques Common pathologies in calf and posterior knee
Sonography of Knee and Calf Pain: the differential considerations Dr. Lisa L. S.Wong Consultant Radiologist St Paul s Hospital Outline Ultrasound techniques Common pathologies in calf and posterior knee
MSK Radiology Interesting Case Presentation
 MSK Radiology Interesting Case Presentation Sitt Ching Man Jacqueline 27 th Feb 2015 Patient 1: YPY F/27 Professional badminton player C/o sudden onset of right shoulder pain after a very vigorous match
MSK Radiology Interesting Case Presentation Sitt Ching Man Jacqueline 27 th Feb 2015 Patient 1: YPY F/27 Professional badminton player C/o sudden onset of right shoulder pain after a very vigorous match
Hamstring injuries in professional football players: magnetic resonance imaging correlation with return to play.
 Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 9-1-2011 Hamstring injuries in professional football players: magnetic resonance imaging correlation with return
Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 9-1-2011 Hamstring injuries in professional football players: magnetic resonance imaging correlation with return
Introduction. Anatomy
 the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
Ultrasound of the Shoulder
 Ultrasound of the Shoulder Patrick Battaglia, DC, DACBR Logan University, Department of Radiology Outline Review ultrasound appearance of NMSK tissues Present indications for ultrasound of the shoulder.
Ultrasound of the Shoulder Patrick Battaglia, DC, DACBR Logan University, Department of Radiology Outline Review ultrasound appearance of NMSK tissues Present indications for ultrasound of the shoulder.
A Patient s Guide to Pes Anserine Bursitis
 A Patient s Guide to Pes Anserine Bursitis 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Pes Anserine Bursitis 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet is compiled
Effectiveness of Ultrasound-Guided Corticosteroid Injection for the Treatment of Gluteus Medius Tendinopathy
 Musculoskeletal Imaging Original Research Labrosse et al. Ultrasound-Guided Corticosteroid Injection for Tendinopathy Musculoskeletal Imaging Original Research Julie M. Labrosse 1 Étienne Cardinal 1 Bernard
Musculoskeletal Imaging Original Research Labrosse et al. Ultrasound-Guided Corticosteroid Injection for Tendinopathy Musculoskeletal Imaging Original Research Julie M. Labrosse 1 Étienne Cardinal 1 Bernard
Imaging Diagnosis and Prognostication of Hamstring Injuries
 Musculoskeletal Imaging Review Rubin Hamstring Injuries Musculoskeletal Imaging Review David. Rubin 1 Rubin D FOCUS ON: Keywords: avulsion, hamstring, injury, muscle, strain DOI:10.2214/JR.12.8784 Received
Musculoskeletal Imaging Review Rubin Hamstring Injuries Musculoskeletal Imaging Review David. Rubin 1 Rubin D FOCUS ON: Keywords: avulsion, hamstring, injury, muscle, strain DOI:10.2214/JR.12.8784 Received
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers
 Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
HIP CASESTUDY 3. Body Chart-Initial Hypothesis: Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1
 Body Chart-Initial Hypothesis: HIP CASESTUDY 3 Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT OCS FAAOMPT Hamstring Strain HS Tendinopathy Lumbar Radiculopathy Lumbar
Body Chart-Initial Hypothesis: HIP CASESTUDY 3 Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Eric Magrum DPT OCS FAAOMPT Hamstring Strain HS Tendinopathy Lumbar Radiculopathy Lumbar
Ultrasound of soft-tissue vascular anomalies
 Ultrasound of soft-tissue vascular anomalies Oscar M. Navarro Associate Professor, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Toronto, Canada Declaration of Disclosure
Ultrasound of soft-tissue vascular anomalies Oscar M. Navarro Associate Professor, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Toronto, Canada Declaration of Disclosure
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
Common Injuries. Hamstring Injuries. by Dr. Ben Benjamin
 Common Injuries Assessing and Treating the Most Common Injuries Assessment and Treatment of Hamstring Injuries by Dr. Ben Benjamin The Benjamin Institute 175 Richdale Ave Suite 106 Cambridge, MA 02140
Common Injuries Assessing and Treating the Most Common Injuries Assessment and Treatment of Hamstring Injuries by Dr. Ben Benjamin The Benjamin Institute 175 Richdale Ave Suite 106 Cambridge, MA 02140
NIH Public Access Author Manuscript J Orthop Sports Phys Ther. Author manuscript; available in PMC 2010 May 11.
 NIH Public Access Author Manuscript Published in final edited form as: J Orthop Sports Phys Ther. 2010 February ; 40(2): 67 81. doi:10.2519/jospt.2010.3047. Hamstring Strain Injuries: Recommendations for
NIH Public Access Author Manuscript Published in final edited form as: J Orthop Sports Phys Ther. 2010 February ; 40(2): 67 81. doi:10.2519/jospt.2010.3047. Hamstring Strain Injuries: Recommendations for
Lateral Elbow Pathology
 Lateral Elbow Pathology Jon A. Jacobson, M.D. Professor of adiology Director, Division of Musculoskeletal adiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board: GE, Philips
Lateral Elbow Pathology Jon A. Jacobson, M.D. Professor of adiology Director, Division of Musculoskeletal adiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Board: GE, Philips
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
