Lower Limb Ulceration Policy. Version No 2.6. Review: February 2018
|
|
|
- Martina Banks
- 6 years ago
- Views:
Transcription
1 Livewell Southwest Lower Limb Ulceration Policy Version No 2.6 Review: February 2018 Notice to staff using a paper copy of this guidance The policies and procedures page of Intranet holds the most recent version of this guidance. Staff must ensure they are using the most recent guidance. Author: Clinical Nurse Specialist Tissue Viability Asset Number: 169 Page 1 of 29
2 Reader Information Title Lower Limb Ulceration Policy. V.2.6 Asset number 169 Rights of access Public Type of paper Policy Category Clinical Document purpose/summary Guidance for staff in promoting Tissue Integrity and Managing Lower Limb Ulceration. The policy provides staff with a framework for assessment, intervention and management of patients who have lower limb Ulceration Author Clinical Nurse Specialist Tissue Viability Ratification date and group 21 st January Policy Ratification Group. Publication date 10 th January 2017 Three years after publication, or earlier if there is a Review date and frequency change in evidence. (one, two or three years based on risk assessment) Disposal date Job title Target audience Circulation Consultation process Equality analysis checklist completed References/sources of information The Policy Ratification Group will retain an e-signed copy for the archive in accordance with the Retention and Disposal Schedule. All copies must be destroyed when replaced by a new version or withdrawn from circulation. Clinical Nurse Specialist Tissue Viability All Livewell Southwest Healthcare staff Electronic: Livewell Southwest intranet and website (if applicable) Written: Upon request to the PRG Secretary on Please contact the author if you require this document in an alternative format. This policy was produced in consultation with Managers from: Professional Lead Community Matron The District Nursing Services Vascular Consultants & Vascular Nurse Tissue Viability Specialist Nurses Plymouth Hospitals NHS Trust Yes National Institute for Clinical Excellence (2001) Wound Care- Debriding agents. Reference TA24. Ref CG National Institute of Clinical Excellence (2006) Nutrition support in adults: oral nutrition support, enteral tube feeding and parenteral nutrition Reference: CG32 Page 2 of 29
3 National Institute of Clinical Excellence (2003) Prevention of healthcare-associated infection in primary and community care Nursing and Midwifery Council The Code (2008) Guidelines for records and record keeping (2005) Guidance for the administration of medicines (2004) Royal College of Nursing Institute, Clinical Practice Guidelines: The Management of Patients with venous leg ulcers. London: RCN Institute, SIGN. The Care of Patients with Chronic Leg Ulcers, Edinburgh: SIGN Secretariat, 1998 Understanding Compression Therapy (2003) EWMA Position Document. Medical Educational Partnership Chronic Venous Insufficiency and Venous Ulceration- Aetiology and Treatment (2008) E.R Sqibb & Sons, L.L.C. Lindsey l & White R 2008 Leg Ulcers and Problems of the Lower Limb. HealthComm UK Ltd Guidelines specific to Tissue Viability European Wound Management Association (EWMA). (2006) Position Document: Management of wound infection. London: World Union of Wound Healing Societies (WUWHS) (2007) Principles of best Practice: Wound exudates and the role of dressings. A consensus document. London: MEP Ltd Identifying criteria for wound infection EWMA Position Document. (2005) Hard to heal wounds : the Holistic approach (2008) Minimising pain at wound dressing-related procedures World Union of Wound Healing Societies Initiative Published by Page 3 of 29
4 Wound exudate and the role of dressings World Union of Wound Healing Societies Initiative NHS Modernisation Agency 2003 Essence Of Care Benchmarks DOH/Skills for Health Associated documentation Livewell Southwest Competencies in Compression Bandaging and Doppler Guidelines for the assessment and management of Exudate Lower Limb Ulceration Assessment form Lower Limb Ulceration Referral Pathway Information for patients Supersedes document V.2.5 Author contact details By post: Local Care Centre Mount Gould Hospital, 200 Mount Gould Road, Plymouth, Devon, PL4 7PY. Tel: , Fax: (LCC Reception). Page 4 of 29
5 Document review history Version no. Type of change Date Originator of change Description of change 1 Published 12/03/2006 1:1 Review 10/10/2008 Clinical Nurse Specialist Tissue Viability 1.2 Amendments following PRG May Updated January 2010 Clinical Nurse Specialist Tissue Viability Clinical Nurse Specialist Tissue Viability 2:1 Review 29/03/10 Clinical Nurse Specialist Tissue Viability 2.2 Amendments following PRG 30/03/10 Clinical Nurse Specialist Tissue Viability Matron DN Treatment Clinic 2.3 Review 25/02/2012 Clinical Nurse Specialist Tissue Viability 2.4 Review 12/03/2014 Clinical Nurse Specialist Tissue Viability 2.5 Review 10/06/14 Clinical Nurse Specialists Tissue Viability Matron DN Treatment Clinic Vascular Surgeons Lead Vascular Nurse 2.6 Competencie s 02/03/16 Livewell Southwest Ratification Group Reviewed, minor changes made. Reviewed, changes made. Additions from other members of staff. Reviewed, minor changes made. Reviewed, changes made. Review of flow chart. Reviewed and major changes made. Management of Venous Leg Ulcers guidelines added. Reviewed. New competencies added. Page 5 of 29
6 Contents Page 1 Foreword 7 2 Introduction 7 3 Purpose 7 4 Duties 7 5 Definitions 8 6 Guidance 10 7 Procedures 12 8 Education 13 9 Audit Monitoring Compliance and Effectiveness 14 Appendix A Livewell Competencies 15 Appendix B Information for Patients & Carers 16 Appendix C COM151 Leg Ulcer Assessment Chart & COM152 Doppler Assessment 22 Appendix D Leg Ulcer treatment and referral pathway 23 Appendix E Clinical Guidelines for the Management of Venous Leg Ulcers. 25 Page 6 of 29
7 Lower Limb Ulceration Policy. 1 Foreword 1.1 These guidelines are not intended to be a textbook or training manual. Neither are they intended a rigid or inflexible tool. 1.2 It is strongly recommended that anyone involved in the delivery of leg ulcer care has had adequate training and developed their competencies in leg ulcer assessment, Doppler ultrasound, compression bandaging techniques and leg ulcer management. The evidence base for these guidelines is based upon systematic reviews conducted by Scottish Intercollegiate Guidelines Network (SIGN 2010). A full reference and recommended reading list will be given at the end of these guidelines. 2 Introduction 2.1 Lower limb ulceration due to venous disease is estimated to affect approximately 1% of the patient population in developed countries. Current leg ulcer care costs the NHS per year with a substantial proportion of this attributable to nursing time. (BMJ 2009). 2.2 These estimates are primarily associated with venous ulceration and yet the cost of arterial disease (and some venous ulceration) that is not managed effectively can result in lower limb amputation. The financial cost of which is 6,103 per limb and the potential personal consequence on quality of life of this surgery is or can be insurmountable. 3 Purpose 3.1 The purpose of the document is: To identify methods of assessment, intervention and treatment therapies to promote healing and reduce recurrence of lower limb ulceration. To provide health professionals with evidence linked recommendations of leg ulcer assessment and management. Assist the practitioner to identify the presence of arterial disease. Formulate and implement appropriate care and management. Reduce variations in practice and standardise care across health care settings and to facilitate appropriate and timely referral to secondary care. 3.2 Moreover, the clinician is made aware of the necessity for patient participation and involvement in their care to ensure therapeutic, non-judgemental relationships with informed patient consent (Van Hecke et al 2009). 4 Duties 4.1 The Chief Executive has overall responsibility for care and treatment of patients and the implementation of this policy. Page 7 of 29
8 4.2 The Deputy Director of Professional Practice, Quality and Safety, and Locality Managers will be responsible for ensuring that all staff follow the standards set out in this policy. 4.3 The Clinical Nurse Specialist (CNS) in Tissue Viability (TV) is responsible for providing evidence based education and training for staff within Livewell Southwest (LSW). Implementation and review of the Lower Limb (Leg Ulcer) Policy and the supporting literature to LSW. 4.4 Unit / Ward Managers / Service Managers/District Nurse Team Managers are responsible for the safe implementation of the policy. 4.5 All staff caring for patients with Lower Limb Ulceration will comply with all standards and procedures outlined in this policy. 5 Definitions Lower limb/leg Ulceration Debridement Sustained Graduated Compression Therapy Compression Hosiery A leg ulcer can be defined as an open lesion between the knee and the ankle joint which is failing to go through the normal phases of wound healing and that does not respond to treatment within 4 weeks (SIGN 2010). The removal of dead (devitalised) tissue, cell debris or foreign matter from a wound. A bandaging or hosiery system that facilitates venous return via the venous circulatory system to the heart. The graduation indicates that the sub-bandage pressure is greater at the ankle and reduced at the knee. The level of pressure achieved is determined by the use of elastic or inelastic bandages according to the ulcer aetiology, the circumference of the limb, the configuration of the bandage system being used and the level of competency of the practitioner applying the bandage system. Stockings or socks that are woven from elastic or inelastic fibres to achieve graduated compression to the lower limb in limbs that have healed, have superficial ulceration, or varicosities and associated skin changes due to early stages of venous disease. Compression hosiery also enables patients to self-care and encourages concordance with the desired treatment. Page 8 of 29
9 Reduced compression Short Stretch bandaging Sub bandage pressure Doppler Assessment Duplex ABPI Competent Reduced compression is used to treat patients who cannot tolerate full compression or who are not suitable for full compression systems so must be closely monitored. This system of bandaging provides an inelastic system for patients with lymphoedema/chronic oedema and patients who have restricted ankle movement. The interface pressure exerted between the limb and the bandages. Is an assessment using Doppler ultrasounds which measure the patient s Ankle Brachial Pressure Index (ABPI). The purpose of a Doppler assessment is to eliminate arterial disease. Compression must never be applied to treat arterial ulcers. Occasionally the vascular surgeon may request compression therapy dependant on the degree of arterial disease. On these occasions specific written instructions must be obtained from the consultant and the therapy must be closely monitored by the health care professional responsible for delivering the patient s care. A non-invasive ultrasound that provides an immediate picture of the veins and arteries to determine the strength and direction of blood flow. Duplex studies are used to identify venous incompetence and arterial disease. The ABPI (Ankle, Brachial Pressure Index) confirms or excludes the presence of arterial disease in the lower limb and is calculated via Doppler assessment. It determines the percentage of blood supply to the patient s foot/feet. A clinician that has had training in a specialised area and has achieved a level of capability that deems them competent. No form of compression therapy should be applied by practitioners who have not undertaken a recognised training program in leg ulcer management or that have not been deemed capable through a competency framework, as high compression therapy inappropriately applied can cause significant damage. Page 9 of 29
10 6 Guidance Assessment Ankle Brachial Pressure Index (ABPI) The measurement of the patient s ABPI must be undertaken by practitioners who have received adequate training in leg ulcer management and whose competencies have been updated according to local policy. Appropriate training is required due to complexities around the interpretation of the results. ABPI is carried out to substantiate the presence or absence of significant peripheral arterial disease (PAD), except in those patients with calcified vessels. For values above 1.3 (ABPI) and associated with ulceration, the vessels are likely to be incompressible and the results cannot be relied upon to make a clinical decision (SIGN 2006). 6.1 All patients to be assessed by a competent qualified nurse or an Assistant Practitioner (AP), who has received adequate training, experience and has worked through a competency framework. 6.2 Patients who have a wound to the lower limb must undergo a leg ulcer assessment including an ABPI calculation within four weeks and depending on the urgency of presenting signs and symptoms. 6.3 Aspects of past history, aetiology and patho-physiology and clinical signs and symptoms to be recorded on the assessment form with patient perceptions of the impact of their symptoms reflected in the care plan. Factors such as obesity, malnutrition, intravenous drug use and co-existing medical conditions will affect prognosis and suitability for venous surgery (SIGN 2010). 6.4 Although chronic venous insufficiency is the most common cause of leg ulceration the circulation cannot be viewed in isolation. Assessment of the patients ABPI by an experienced healthcare professional should bring together general and specific information on the following: Patient. Skin. Circulation. Limb. Ulcer. The assessment should answer the following questions: What is the cause and possible aetiology of the ulcer? What factors may delay healing? What is the most appropriate treatment for this individual patient? Are there any correctable risk factors which will speed healing and reduce recurrence? Patients presenting with risk factors, for example varicose veins and lower limb Page 10 of 29
11 ulceration. Where appropriate should be considered for intervention of underlying correctable aetiologies within a timely manner. Identification of venous or arterial disease should prompt referral. The National Institute of Clinical Excellence (NICE CQ ) recommends referral within two weeks of identifying the signs and symptoms. 6.5 The patient s mobility should be considered including joint mobility/fixed ankle joint as compression bandaging will affect the patient s mobility. Help available to the patient in the community must also be considered when prescribing compression hosiery and ease of application. 6.6 Planning of Doppler/ABPI assessment should be undertaken in negotiation with the patient to ensure the patient has an understanding of the procedure and to reduce potential anxiety. Doppler ultrasound is performed following a full clinical assessment and forms part of a holistic assessment. 6.7 Clinical Assessment of the Patient: Document:- Relevant past medical history. Associated disease and risk factors (table 2). Current ulcer history. Previous ulceration and successful/unsuccessful treatments. Current drug therapy. Allergies. Presence and type of pain Nutritional status and their build using an appropriate recognised assessment tool e.g. Pain Scale Measuring Tool and MUST if required. Sleep pattern. Social circumstances. Psychological status. 6.8 Management of Venous Ulcers. 6.9 All patients with an ABPI of <0.65 and ulceration are deemed to have significant arterial disease and should be referred to Vascular services as an urgent referral Approximately 5% of patients will have Diabetes Mellitus. All Diabetic patients with ulceration that is on the foot and below the malleolus should be referred to the Joint Diabetic Foot Clinic at Plymouth Hospitals NHS Trust. Compression therapy should not be routinely applied to diabetic patients with leg and foot ulceration due to potential micro vessel disease and neuropathy. This could increase the risk of pressure ulcers. Important note: Compression therapy should not be applied in the presence of pressure ulcers to the heels. Advice should be sought from the Tissue Viability Service. Page 11 of 29
12 6.11 A high ABPI (e.g. >1.3) in the absence of clinical symptoms of arterial disease and without lower limb ulceration does not require referral to Vascular services The outcome of the assessment should be fully explained to the patient with the results of the clinician s investigation. Different treatment options must be discussed to offer the patient a choice and encourage concordance, enabling the patient and clinician to achieve an agreed plan of care that is reflective of evidenced based practice guidelines. 7 Procedures 7.1 Procedures will be undertaken that comply with universal precautions for control of infection and correct disposal of clinical waste. 7.2 Equipment used during the assessment purpose (such as Doppler or Sphygmomanometer) will be fit for purpose and the procedure carried out under optimum conditions. 7.3 For patients with active ulceration Doppler reassessment should be carried out every 24 weeks and thereafter at 24 week intervals or if there is a clinical change in the patient s symptoms which may affect the patient s arterial status. When an ulcer recurs, a full assessment should be carried out including a Doppler. Patients with healed ulcers using compression hosiery should have a reassessment of their ABPI every 6 months or sooner if there is a clinical change in presenting symptoms. 7.4 Those patients who have undergone a Duplex scan will not require a follow up Duplex or Doppler unless there are significant clinical signs of deterioration. Compression can be applied following a Deep Vein Thrombosis as long as the patient is effectively anticoagulated. 7.5 Compression therapy is the gold standard treatment for patients with venous leg ulcers. There are a variety of compression systems available to allow patient choice and participation. High compression multi component bandaging should be used in the treatment of venous leg ulcers using a multi-layer or a two layer system. 7.6 Compression therapy should only be applied by staff with the appropriate training and in accordance with the manufacturers instructions. 7.7 Primary dressings deemed necessary to address symptoms such as management of pain or exudate, or promote healing will follow the recommendations of the South and West Devon Formulary unless discussed and agreed with Specialist Tissue Viability services. Most venous ulcers can be treated with a simple low adherent primary dressing under their compression therapy dependant on the classification of the ulcer bed. There is no clinical evidence to support the use of complex wound care products under compression therapy unless there are clear clinical indications. Page 12 of 29
13 8 Education 8.1 All qualified nurses and healthcare professionals with a responsibility for caring for patients with lower limb ulceration will be updated in the treatment and management of leg ulceration particular to their level of intervention. 8.2 Registered Nurses will be deemed competent in compression bandaging and holistic Doppler assessment by an experienced clinician who has been deemed competent in leg ulcer management. Achieving competence will require practice to build upon the theoretical knowledge from education and training. The competencies will be signed off 3 yearly. They will complete yearly self assessment thereafter. Assistant Practitioners and Extended Role Health Care Assistants will have their competencies supervised and signed off by a competent Registered Nurse. 8.3 Education and training will be made available to both Livewell Southwest & PHT, via the Tissue Viability and Vascular services; and reflect the education requirements of staff. Educational study days will be designed for all Registered Nurses, Assistant Practitioners and Health Care Assistants involved in the management and treatment of leg ulcers. Consideration will be given to the level of expertise and competencies of the group receiving training and sessions will be designed specifically to meet their needs. 8.4 Staff will ensure that patents/clients and their carers are informed of the elements of and their role in maintaining tissue integrity. Patients and carers will be taught the basic principles of good skin care to maintain skin integrity. They will be shown how and when to apply compression hosiery and will be provided with information regarding hosiery applicators to encourage concordance. 9 Audit 9.1 Quality Assurance and Audit - The principles upon which this document is based are: An individual holistic assessment should be undertaken and evidenced-based treatment plans commenced. This will take into account the underlying aetiology, patient s circumstances and their choices. Working in partnership with the practitioner s clinical judgement, available resources and knowledge of more recent research findings will facilitate the overall treatment goal. Those who undertake ABPI assessment, planning, implementation and evaluation of care should be trained, educated and competent in leg ulcer care and management. They should have attended the two day in-house Leg Ulcer Management training programme and will require supervision of their practice with an experienced nurse in leg ulcer management who has had their competencies signed off. The process should be clearly documented on the leg ulcer assessment form and should be accessible to all those caring for the patient to ensure continuity of care. Monitoring of ulcer healing and recurrence rates as an indicator of quality care Page 13 of 29
14 will be undertaken regularly through a clinical audit process. Audit will be carried out to assess the efficacy of the policy and referral pathway. 9.2 All information regarding referral of patients with lower limb ulceration whether within or without the organisation will be collated and shared via the Vascular Group Meetings and using the agreed Leg Ulcer Care Pathway (Appendix E). A collaborative, multi-disciplinary approach will be taken to meet the needs of patients with or at risk of leg ulcer development. 9.3 The process of audit will be every practitioner s responsibility and reflect the philosophy from the Essence of Care (2010) document. Practice, training and procedures will be developed and amended to reflect the requirements of patients/clients and clinicians as identified from the audit process. 10 Monitoring Compliance and Effectiveness 10.1 Leg Ulcer Prevention and Management training will be delivered by the Tissue Viability Team and will be provided over the course of 2 days. The course will be available on 3 occasions annually, or according to demand Hyperlinks to relevant national guidance and best practice statements will be included on the reference list All documentation will be reviewed in response to the publication of evidence based research findings and /or National or International consensus publications that dictate essential review. All policies are required to be electronically signed by the Lead Director. Proof of the electronic signature is stored in the policies database. The Lead Director approves this document and any attached appendices. For operational policies this will be the Locality Manager. The Executive signature is subject to the understanding that the policy owner has followed the organisation process for policy Ratification. Signed: Director of Operations Date: 5 th February 2015 Page 14 of 29
15 APPENDIX A Registered Nurse and Extended HCA Competencies Bandaging competency Compression Bandaging Competencies Doppler competency Doppler Ultrasound Assessment of the Lower Limb Competency Page 15 of 29
16 APPENDIX B Patient Information Chronic Leg Ulcers 1. What is a leg ulcer? A leg ulcer is simply a break in the skin of the leg below the knee, usually caused by a minor injury. In most people such an injury will heal up without difficulty within a week or two. However, if there is an underlying cause, the wound healing may be delayed with an increased breakdown of skin, resulting in a chronic leg ulcer. Leg ulcers tend to affect older people and are more common in women. 2. What causes leg ulcers? Venous ulcers these make up about 70% of all ulcers. Each time your leg muscles move they help pump the blood up to the heart, whilst a series of one-way valves stop it from flowing backwards. If these valves become damaged, due to an injury, deep vein thrombosis (DVT), or pregnancy, the blood will flow back down the leg and cause increased pressure on the veins. After a time, the veins will become stretched and fluid will leak out causing swelling of the legs, thickening and damage to the skin. Arterial ulcers About 10% of people have this type. The arteries supply blood to the legs and feet. If the arteries become narrowed (atherosclerosis), due to smoking, high blood pressure, diabetes, rheumatoid arthritis, heart disease etc., the leg circulation will be reduced, the leg will be starved of oxygen and nutrients and the skin will begin to break down. Diabetic ulcers 5% of diabetics will suffer with ulcers, usually on the foot. Diabetes increases the likelihood of atherosclerosis. It also affects the nerves, causing a lack of sensation in the feet (sensory neuropathy) which makes ulcers more likely to appear. Diabetic ulcers can occur due to smoking, poor dietary control, incorrect medication, poor foot care or badly fitting shoes. Page 16 of 29
17 Rheumatoid ulcers- some patients have normal veins or arteries but develop ulcers because of conditions Rheumatoid Arthritis this is an inflammatory disease or Lupus this is a disease of the blood. 3. What are the symptoms? Venous ulcers The appearance of a venous leg ulcer is fairly typical. It is often located just above the ankle, on the inside of the leg. The leg is swollen and the ulcer may leak fluid. The ulcer may be tender to touch and the skin may feel dry and itchy (varicose eczema) with mottled brown or black staining. Some venous ulcers are painful, particularly if they become infected. Arterial ulcers These tend to occur on the foot and lower part of the leg. The feet and legs often feel cold and may have a whitish or bluish, shiny appearance. Arterial leg ulcers are often painful, particularly at night in bed. The pain is often relieved when the legs are lowered. 4. How are leg ulcers diagnosed? Your nurse / doctor will examine you and arrange to do some tests to assess the circulation in your lower limb to help to identify the cause of the ulcer. This should include a thorough examination, an assessment of the condition of your overall health, and a look at the appearance and site of the ulcer. These checks are important because the treatment for venous and arterial ulcers is different and they must be sure what type of ulcer you have. Routine blood and urine tests may also be done to check for other causes such as anaemia and diabetes. This usually involves a Doppler assessment, which compares the blood pressure in your ankle with the blood pressure in your arms, to give a ratio known as the Ankle Brachial Pressure Index, or ABPI. This is measured using a hand held ultrasound machine called a Doppler. The results can identify if you have poor circulation in your legs. However, you may need a more in depth vascular assessment and your GP may refer you to see a vascular surgeon. You will usually be sent an appointment to be seen in our Vascular Assessment Unit, where your ulcer will be further investigated by means of an ultrasound, or Duplex, scan. This scan will help us to find out which type of ulcer it is e.g. venous or arterial. Page 17 of 29
18 5. How will I be treated? Treatment of a venous leg ulcer is aimed firstly at controlling the high pressure in the leg veins and secondly at the ulcer itself. The mainstays of treatment are compression bandaging or stockings and elevation of the limb: Elevation of the limb. Put your legs up whenever you can and as high as you are able. The higher the leg, the lower the pressure in the leg veins. When elevating the foot above the heart the pressure in the foot will drop to a normal level. It helps to lift the lower end of your bed (6 inches or so), so that when in bed your feet are a little higher than your head. Compression bandaging or stockings. In order to keep the pressure in the leg veins at the ankle low when you are standing up, you will be treated with a compression bandaging system or compression stockings or socks. Several layers of bandages may be required to get the necessary pressure to control the veins. This may feel uncomfortable at first but if you experience severe pain, it s important to remove the bandages and contact the Nurse for a review. When the ulcer has healed, compression stockings are usually necessary to prevent the ulcer from returning. These stockings need to be specially fitted and are much stronger than ordinary "support tights". If you have difficulty putting on your stockings then you can obtain a special stocking applicator ask the nurse for details. Surgery. If your ulcer is due to varicose veins then these may be treated, by surgery or by injection of foam, usually once the ulcer has healed. A skin graft, or a procedure to correct the underlying problem with the veins, may be necessary. A small tissue sample (biopsy) may occasionally be taken if the ulcer does not respond to treatment. Good Skin care. Moisturising the skin around the ulcer is important to maintain skin integrity and prevent dry cracked skin from forming, using an emollient to add to bath water or as a soap substitute adjacent to a moisturising agent which Page 18 of 29
19 can be used to cream your leg. You need to apply the moisturiser in a gentle downward motion in the direction of the hairs, to avoid blockage of the hair follicles. If you wish to bath or shower whilst your bandages are in situ, please ask the nurse to prescribe a bandage protector (Limbo or Seal Tight). Your Doctor may prescribe Steroid creams to treat eczema but these should be sparingly applied and as instructed. These range in potency from strong (Dermovate), moderate (Elocon) to mild (Betnovate RD). Creams are used for wet eczema and ointments for dry eczema. Your Doctor may refer you to a Dermatologist for a review if symptoms persist. It is important to ensure that your leg or the area of eczema is moisturized prior to applying the Steroid ointment/cream. This will allow the Steroid to be absorbed. Steroids creams/ointments should be gradually discontinued and not stopped abruptly to avoid the eczema recurring. Antibiotics are occasionally required to treat ulcers that show clinical signs of infection and where a swab test has indicated the use of anti-biotics, particularly if there is evidence of infection in the surrounding tissues and skin (cellulitis) or lymphatic channels (lymphangitis), resulting in increased pain and a flu like illness. However, unless you are unwell with a fever, antibiotics are not needed, as they can encourage resistant bugs. The infection may be treated by antibacterial dressings. Dressings. The nurse may prescribe specific dressings under the bandages, to ease your symptoms. The ulcer will be regularly reviewed by the nurse and dressings will be prescribed according to the phases of healing. Remember the bandages will treat the cause of the ulcer. Arterial ulcers may benefit from surgery a bypass operation or balloon angioplasty (stretching an artery with a balloon), a procedure that relieves narrowing and obstruction of the arteries. 6. How long will it take the ulcer to heal? It has usually taken many years for the venous disease to cause the ulcers, so it is not surprising that the ulcers may take a fairly long time to heal. Although most venous ulcers will heal within in 12 to 16 weeks, a small proportion will take considerably longer. This may be due to other underlying health conditions and repeated infections. Even in these resistant cases, treatment is usually successful. Mixed arterial and venous ulcers are more difficult to treat and in the more severe cases it may not be possible to achieve healing. You may require further investigations to identify the most appropriate treatment. 7. Is there any risk of losing my leg? Venous ulcers - It is very rare indeed for venous ulceration of the leg to lead to the need for amputation of the leg and even the larger ulcers can usually be treated successfully. Page 19 of 29
20 Arterial ulcers/ulcers associated with Diabetes Mellitus - Occasionally it is not possible to perform a bypass operation or an angioplasty and if you have a very large painful ulcer on your leg it may be better for you to consider an amputation. Your doctor will discuss this with you in detail. He or she will be aware that this is a very difficult decision for you and will not proceed with an amputation unless you are happy that this is the appropriate option for you. 8. How can I help myself? Stop smoking. This is one of the major risk factors for vascular (circulatory) disease. It is difficult to give up but help is available. Speak to your doctor or further help is available locally from the Livewell Stop Smoking Service Tel: Take regular exercise. Using your foot and leg muscles encourages the circulation. By flexing and rotating your ankles and flexing your toes will significantly improve your circulation. Avoid standing or sitting in one position for a long time. Eat a healthy well balanced diet and include protein, oily fish, fresh fruit and vegetables. Lose weight if you are overweight. Your Nurse / Doctor can give advice and refer you to a dietician if appropriate. If you are advised to put your legs up, ideally rest with your ankles above waist height. Don t cross your legs when sitting or allow the edge of the chair to press into the back of your legs. Wear support stockings if these have been advised. If you have a problem with your dressings or bandages, or if your stockings become loose, tell your nurse straight away. Avoid tight clothing on your legs and wear comfortable, well-fitting shoes & socks. See a podiatrist (chiropodist) regularly (at least every 3 months) and take care when cutting toe nails. Take care not to bang your feet or legs on sharp corners or objects. If you injure your feet or toes, keep the wound clean and seek advice from your Nurse regarding dressings. Protect your skin and legs. Keep your feet and legs warm but avoid extremes of temperature, e.g. hot baths, sunburn, sitting too close to the fire. Use mild soap, or soap substitute, to keep your skin clean and keep it supple with a bland moisturiser. Your doctor or nurse can advise you about products to use. Inspect your feet and legs regularly. Look for sores or changes in colour use a mirror to help. Do not delay in seeking help if you think you are developing an ulcer. Please contact your GP if it has been some time since you have had contact with your nurse. He/She will direct you to the appropriate clinician and service. 9. How can I stop the ulcer coming back? Ulcers do have a tendency to recur, especially in elderly people or people who have advanced venous disease where intervention is not appropriate. Although the skin is intact the underlying problem with the veins remains and you must take precautions to Page 20 of 29
21 prevent the ulcer recurring. If you have been advised to wear support stockings, you will need to wear these indefinitely. These should be replaced according to the manufacturer s instructions to maintain adequate compression and should be re measured and checked. Your nurse will advise you specific to your requirements. If your ulcer reoccurs, you must inform the nurse immediately. Vascular Surgical Unit Surgical Directorate Derriford Hospital Lead Clinician Consultant Vascular Surgeon Consultant Vascular Surgeon Plymouth PL6 8DH Consultant Vascular and transplant Surgeon Vascular Scientists Vascular Nurse Specialist Livewell Southwest District Nurse team G.P Tissue Viability Specialist Nurse Page 21 of 29
22 APPENDIX C COM151 Leg Ulcer Assessment Chart COM151 Leg Ulcer Assessment Chart COM152 Doppler Assessment COM152 Leg Ulcer Doppler Assessment Chart Page 22 of 29
23 APPENDIX D Directions for the use of the Vascular Pathway Flow Chart The Vascular Pathway requires the user to have performed both a clinical and Doppler Assessment to determine the presentation, symptoms and the blood supply of the affected limb/limbs. ABPI Measurements and referral criteria need to be considered to facilitate a correct referral. If ABPI cannot be undertaken then the reasons should documented on the referral. The flow chart is an aide memoir for Clinicians on the appropriate intervention and referral criteria required for patients with lower limb ulceration.it aims to reduce inappropriate referrals to the wrong specialities, streamline patient care and ensure safe and effective leg ulcer management. Lower Limb ulceration is defined as a wound that is below the knee and above the malleolus (ankle) that has been present for 4 weeks or more. Foot ulceration is a wound that is below the malleolus. It s important to consider the clinical presentation and patient history to establish whether there is Ischemic disease or Neuropathy and whether they have a familial history or a diagnosis of Diabetes. Arterial Ulcers The Vascular Consultants recommend that a referral is required for all patients with leg ulceration whose ABPI 0.65 mmhg and below. Signs & Symptoms of Arterial ulcers include: Resting pain to the toes/foot. Discolouration of the toes or extremities (dependent rubor). Increased pain not relieved on elevation. Loss of sensation. Atrophic shiny skin. Increased depth of ulceration. Diabetic foot ulcers All patients with Diabetes (Type I & II) with an ulcer on or below the malleolus should be referred to the diabetic foot clinic at Plymouth Hospitals NHS Trust, for a more in-depth assessment. Page 23 of 29
24 Mixed Venous / Arterial Ulcers Patients with mixed Venous / Arterial ulcers with ABPI of , should be routinely referred for a vascular assessment. Reduced compression may be commenced if clinically indicated and decisions documented. Close monitoring and observation is essential and compression must be discontinued if not tolerated. Uncomplicated Venous leg Ulcers These are often the end stage result of a chronic disease process, namely chronic venous insufficiency. Compression should be commenced in Patients with ABPI of 0.8 and above. NICE recommends that patients with active venous ulcers that have not healed within two weeks should now be referred to see a vascular specialist for consider treatment of the underlying venous disease to help prevent recurrence (NICE CQ ). A routine vascular referral should be made, as the Patient may benefit from surgical intervention, such as Foam Sclerotherapy. Healed leg ulcers The referral of healed ulcers is for those patients with signs of venous disease who may benefit from an endovenous intervention such as Ultrasound guided foam Sclerotherapy; to treat underlying venous disease and prevent ulcer recurrence. NICE recommends that patients with active venous ulcers that have not healed within two weeks should now be referred to see a vascular specialist for consider treatment of the underlying venous disease to help prevent recurrence (NICE CQ ). Calcified arteries Patients with an ABPI of > 1.3 do not routinely need a vascular assessment in the absence of arterial symptoms and/ or ulceration or tissue loss. It is the local consensus that the patient s arteries are already calcified and that compression CANNOT do any untoward damage, as the vessels will not be squeezed. Compression may be commenced if clinically indicated and no signs of arterial disease are present, but the Patient should be observed and closely monitored for further ischemic changes, when a referral for vascular assessment should be made. Any concerns or queries can be directed via your Tissue Viability Service by telephoning:- (01752) Livewell Southwest (01752) Plymouth Hospital Trust or (01752) Vascular Specialist Nurse Plymouth Hospital Trust Page 24 of 29
25 Joint LIVEWELL SOUTHWEST & PHNT Leg Ulceration: Vascular Treatment Pathway Pathway PRESENTATION: Patient presents with a Leg Ulcer, a wound below the knee that has been present for 4 weeks or more. ASSESSMENT: Undertake full clinical history and holistic patient assessment. DIAGNOSIS: Arterial Ulcer ABPI of < 0.65 TREATMENT: Nil Compression. Simple dressings as per Plymouth Area Joint Formulary recommendations. Perform a Doppler Assessment to gain an ABPI (Ankle Brachial Pressure Index) Mixed Venous/Arterial Ulcer/ Diabetic Leg Ulcer (ON OR ABOVE MALLEOLUS) ABPI OF 0.65 TO 0.8 Reduced compression bandages at mmhgs should only be applied under the instructions of the vascular surgeon, vascular nurse or tissue viability nurse and must be closely monitored. If pain is present or evidence of compression damage DO NOT apply Compression. Where Doppler Ultrasound cannot be heard refer to Tissue Viability Service Toe Pressure Measurement Once Diagnosis confirmed, commence Treatment and consider Specialist Referral (See Referral Pathway overleaf). Refer to Joint Lower Formulary Limb Ulceration for Dressing Policy. V. 2.6 Choices. Reference; EWMA Position Document 2003 Understanding compression therapy pp 12 Diabetic Foot Ulcer (Below the Malleolus) Uncomplicated Venous Ulcer ABPI of > Healed Venous Leg Ulceration ABPI of >0.8 Dressings as per Plymouth Area Joint Formulary Recommendations Compression Therapy: To aim for 40 mm Hgs with Elastic (4 layer) or Inelastic bandaging (Short Stretch) or Hosiery Kits. Prevention of recurrence: Page 25 - of Long 29 Term compression hosiery, Skin Care & Education.
26 Joint LIVEWELL SOUTHWEST & PHNT Leg Ulceration: Vascular Referral Pathway Assessment: Patient presents with lower limb ulceration. Undertake full clinical history and holistic patient assessment including Ankle Brachial Pressure Index (ABPI). DIAGNOSIS: Arterial Ulcer ABPI of < 0.65 REFERRAL: URGENT fast track referral to a Vascular Consultant via DRSS ( ) OUTCOME: Priority outpatient appointment to investigate, diagnose and to treat underlying condition Mixed Venous/ Arterial Ulcer/ Diabetic leg ulcer (ON OR ABOVE MALLEOLUS) ABPI of 0.65 to 0.8 Routine Vascular Consultant referral via DRSS Outpatient appointment to investigate, diagnose and treat underlying condition Diabetic Foot Ulcer (BELOW THE MALLEOLUS) Uncomplicated Venous Ulcer ABPI of >0.8 Healed Venous Leg Ulceration ABPI of >0.8 Reference; EWMA Position Document 2003 Understanding compression therapy pp 12 All patients with diabetic foot ulcers are to be referred to the Joint Diabetes Foot Clinic in PHT Refer Routine to Referral Nurse Specialist to Vascular led Venous Specialist Leg Venous Ulcer Clinic Leg Ulcer via Sentinel Clinic if not healed within two weeks via DRSS Routine vascular nurse specialist Routine Vascular referral Specialist via Sentinel referral via DRSS Effective management of diabetic foot ulcers within a specialist multi- disciplinary outpatients setting Duplex assessment of underlying venous insufficiency and assessment of suitability for compression therapy and possible treatment of venous disease Page 26 of 29
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS
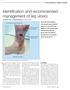 Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Varicose veins. Information for patients Sheffield Vascular Institute
 Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
Endovenous Laser Treatment (EVLT)
 Endovenous Laser Treatment (EVLT) Day Surgery Unit Patient information leaflet What is Endovenous Laser Treatment (EVLT)? Endovenous laser therapy is a treatment for varicose veins which seals the vein
Endovenous Laser Treatment (EVLT) Day Surgery Unit Patient information leaflet What is Endovenous Laser Treatment (EVLT)? Endovenous laser therapy is a treatment for varicose veins which seals the vein
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Leg ulcers Vascular Surgery Patient Information Leaflet
 Leg ulcers Vascular Surgery Patient Information Leaflet What is a leg ulcer? A leg ulcer is simply a break in the skin of the leg which allows air and bacteria to get into the underlying tissue. This is
Leg ulcers Vascular Surgery Patient Information Leaflet What is a leg ulcer? A leg ulcer is simply a break in the skin of the leg which allows air and bacteria to get into the underlying tissue. This is
Injection sclerotherapy. Information for patients Sheffield Vascular Institute
 Injection sclerotherapy Information for patients Sheffield Vascular Institute page 2 of 8 You have been diagnosed as having varicose veins that are suitable for injection sclerotherapy. This leaflet explains
Injection sclerotherapy Information for patients Sheffield Vascular Institute page 2 of 8 You have been diagnosed as having varicose veins that are suitable for injection sclerotherapy. This leaflet explains
Arterial Leg Ulcers. Tissue Viability
 Arterial Leg Ulcers Tissue Viability 01270 275315 Leaflet Ref: 15031 Published: 12/15 Review: 12/18 Page 1 Problems that can occur Skin problems When you have an arterial leg ulcer, the surrounding skin
Arterial Leg Ulcers Tissue Viability 01270 275315 Leaflet Ref: 15031 Published: 12/15 Review: 12/18 Page 1 Problems that can occur Skin problems When you have an arterial leg ulcer, the surrounding skin
Recurrent varicose veins. Information for patients Sheffield Vascular Institute
 Recurrent varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins that have recurred (come back). This leaflet explains more about recurrent
Recurrent varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins that have recurred (come back). This leaflet explains more about recurrent
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING
 HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
HOW TO APPLY EFFECTIVE MULTILAYER COMPRESSION BANDAGING Alison Hopkins is Clinical Nurse Specialist, East London Wound Healing Centre, Tower Hamlets Primary Care Trust Compression therapy is essential
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND
 GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
Advice for rheumatoid patients at risk of developing foot related problems
 Advice for rheumatoid patients at risk of developing foot related problems Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Advice for rheumatoid patients at risk of developing foot related problems Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Varicose Vein Cyanoacrylate Glue treatment
 The South West s premier independent healthcare and cosmetic clinic Varicose Vein Cyanoacrylate Glue treatment Varicose veins are a sign of underlying venous insufficiency and affect 20 30% of adults.
The South West s premier independent healthcare and cosmetic clinic Varicose Vein Cyanoacrylate Glue treatment Varicose veins are a sign of underlying venous insufficiency and affect 20 30% of adults.
You have high risk feet
 You have high risk feet diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY. Emergency Department
You have high risk feet diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY. Emergency Department
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Intermittent claudication exercise programme
 Intermittent claudication programme This leaflet explains about an programme that is offered to patients with intermittent claudication. If you have any questions or concerns, please ask a member of staff
Intermittent claudication programme This leaflet explains about an programme that is offered to patients with intermittent claudication. If you have any questions or concerns, please ask a member of staff
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Endovenous ablation treatment of varicose veins under local anaesthetic
 Patient information: Endovenous varicose vein treatment (LA) Endovenous ablation treatment of varicose veins under local anaesthetic Introduction The vascular consultant (doctor specialising in veins and
Patient information: Endovenous varicose vein treatment (LA) Endovenous ablation treatment of varicose veins under local anaesthetic Introduction The vascular consultant (doctor specialising in veins and
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Promoting best practice in leg ulcer management
 Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Pressure Ulcers Patient Information Leaflet
 Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet
 Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
LOOKING AFTER YOUR FEET
 LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy.
 Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Managing venous leg ulcers and oedema using compression hosiery
 Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
PATIENT STUDY INFORMATION LEAFLET
 PATIENT STUDY INFORMATION LEAFLET BOOKLET 1 You are invited to take part in this research study. Before you decide, it is important for you to understand why the research is being done and what it will
PATIENT STUDY INFORMATION LEAFLET BOOKLET 1 You are invited to take part in this research study. Before you decide, it is important for you to understand why the research is being done and what it will
JoyTickle, Tissue Viability Nurse Specialist, Shropshire Community Health NHS Trust
 Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
ARTERIAL BYPASS GRAFTS IN THE LEG
 The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation
 Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Intermittent Claudication
 Intermittent Claudication Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us what is important to
Intermittent Claudication Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us what is important to
Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders
 Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders Oedema, sometimes known as Lymphoedema or fluid retention is the build up of fluid and other elements
Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders Oedema, sometimes known as Lymphoedema or fluid retention is the build up of fluid and other elements
Improving customer care in compression hosiery
 Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Vascular malformations and their management
 Information for patients Vascular malformations and their management Introduction This leaflet tells you about the condition known as vascular malformation, including venous malformation, arteriovenous
Information for patients Vascular malformations and their management Introduction This leaflet tells you about the condition known as vascular malformation, including venous malformation, arteriovenous
Looking after your diabetic foot ulcer
 Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY.
Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY.
Foot Care. Taking steps towards good FOR AT-RISK FEET. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a LOW RISK of developing serious problems,
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a LOW RISK of developing serious problems,
How is 1st MTP joint fusion carried out? Patient Information: Big Toe Fusion Metatarsophalangeal (MTP)
 Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Deep Vein Thrombosis and Pulmonary Embolism: Risks, Prevention & Treatment
 Deep Vein Thrombosis and Pulmonary Embolism: Risks, Prevention & Treatment Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Deep Vein Thrombosis and Pulmonary Embolism: Risks, Prevention & Treatment Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Excision of Morton s Neuroma
 Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Looking after your diabetic foot ulcer
 Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have breaks in the skin PHONE 07786250788 IMMEDIATELY.
Looking after your diabetic foot ulcer diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have breaks in the skin PHONE 07786250788 IMMEDIATELY.
PDP SELF-TEST QUESTIONNAIRE LEG ULCERS. Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring.
 Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS UPDATED PDP SELF-TEST QUESTIONNAIRE SEPTEMBER 2013 Ulcer Full thickness loss of
Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS UPDATED PDP SELF-TEST QUESTIONNAIRE SEPTEMBER 2013 Ulcer Full thickness loss of
Compression Bandaging Formulary 2017
 Area Drugs Therapeutics Committee Compression Bandaging Formulary 2017 Compression Bandaging Formulary 2017 Developed by the NHS Fife Wound and Skin Care Forum (WSCF) Group Approved: October 2017 Review:
Area Drugs Therapeutics Committee Compression Bandaging Formulary 2017 Compression Bandaging Formulary 2017 Developed by the NHS Fife Wound and Skin Care Forum (WSCF) Group Approved: October 2017 Review:
Diabetes - Foot Care
 Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
PATIENT STUDY INFORMATION LEAFLET
 PATIENT STUDY INFORMATION LEAFLET BOOKLET 1 You are invited to take part in this research study. Before you decide, it is important for you to understand why the research is being done and what it will
PATIENT STUDY INFORMATION LEAFLET BOOKLET 1 You are invited to take part in this research study. Before you decide, it is important for you to understand why the research is being done and what it will
Patient Information. Preventing and treating blood clots
 Patient Information Preventing and treating blood clots 1_Clexane_Patient_Booklet_AW05.indd 1 8/04/2016 11:26 a The information provided in this document is for patients prescribed CLEXANE, and should
Patient Information Preventing and treating blood clots 1_Clexane_Patient_Booklet_AW05.indd 1 8/04/2016 11:26 a The information provided in this document is for patients prescribed CLEXANE, and should
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Priorities Forum Statement
 Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Level 2 Leg Ulcer Management Service. Service Level Agreement Background. Contents:
 Level 2 Leg Ulcer Management Service Service Level Agreement 2016-2019 Contents: 1. Background to Leg Ulcer Management Service 2. Service Details 3. Accreditation 4. Service Standards 5. Finance Details
Level 2 Leg Ulcer Management Service Service Level Agreement 2016-2019 Contents: 1. Background to Leg Ulcer Management Service 2. Service Details 3. Accreditation 4. Service Standards 5. Finance Details
West Gloucestershire Primary Care Trust Community Nursing Service. Leg Ulcer Audit. Gloucestershire Primary & Community Care Audit Group
 West Gloucestershire Primary Care Trust Community Nursing Service Leg Ulcer Audit 2006 Gloucestershire Primary & Community Care Audit Group Contents Page number Background 3 Audit Aims 4 Methodology 4
West Gloucestershire Primary Care Trust Community Nursing Service Leg Ulcer Audit 2006 Gloucestershire Primary & Community Care Audit Group Contents Page number Background 3 Audit Aims 4 Methodology 4
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
In line with the professional requirements of the Nursing and Midwifery Council
 STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
DIABETIC FOOT BOOK THE. A guide to keeping it simple and preventing complications. Practice genii. the Diabetic Foot Book
 DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
DIABETIC THE FOOT BOOK A guide to keeping it simple and preventing complications Understanding how diabetes can affect foot health and the measures that are taken to prevent diabetic foot complications
EDUCATION. Peripheral Artery Disease
 EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Our Vision NADA BoD Strategic Planning Session -
 Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
4-layer compression bandaging system (includes microbe binding wound contact layer) Latex-free, 4-layer compression bandaging system
 JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
JOBST Comprifore JOBST Comprifore at a glance: provides effective levels of sustained graduated compression provides built in safety and ease of application Insures compliance and maximum healing for cost
Juxta CURES Compression Ulcer Recovery System
 medi UK Ltd. Plough Lane Hereford HR4 OEL United Kingdom T 01432 37 35 00 F 01432 37 35 10 enquiries@mediuk.co.uk www.mediuk.co.uk 97C28/01.2013 Juxta CURES Compression Ulcer Recovery System Patient Information
medi UK Ltd. Plough Lane Hereford HR4 OEL United Kingdom T 01432 37 35 00 F 01432 37 35 10 enquiries@mediuk.co.uk www.mediuk.co.uk 97C28/01.2013 Juxta CURES Compression Ulcer Recovery System Patient Information
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
AWMA MODULE ACCREDITATION. Module Three: Assessment and Management of Lower Leg Ulceration
 AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Prevention and management of pressure ulcers
 The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
Toe and forefoot amputation. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Toe and forefoot amputation Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Toe and forefoot amputation Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
PRACTICAL TIPS FOR LOOKING AFTER YOUR SKIN
 Being an active partner in your care www.veteransmates.net.au PRACTICAL TIPS FOR LOOKING AFTER YOUR SKIN As we get older, our skin becomes more delicate and dry, and skin tears are common. However, the
Being an active partner in your care www.veteransmates.net.au PRACTICAL TIPS FOR LOOKING AFTER YOUR SKIN As we get older, our skin becomes more delicate and dry, and skin tears are common. However, the
Varicose Vein Surgery
 What are varicose veins? Varicose veins are enlarged and twisted veins in your leg. Varicose veins are common, affecting up to 3 in 10 people. Varicose veins tend to run in families and are made worse
What are varicose veins? Varicose veins are enlarged and twisted veins in your leg. Varicose veins are common, affecting up to 3 in 10 people. Varicose veins tend to run in families and are made worse
Deep Vein Thrombosis
 Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
Deep Vein Thrombosis from NHS (UK) guidelines Introduction Deep vein thrombosis (DVT) is a blood clot in one of the deep veins in the body. Blood clots that develop in a vein are also known as venous thrombosis.
Leg Ulcer Clinic Audit
 Gloucestershire PCT Community Nursing Service Leg Ulcer Clinic Audit 2007 Contents Page number Background 3 Audit Aims 4 Methodology 4 Results 5-11 Discussion 13-15 Action Plan References 2 Background
Gloucestershire PCT Community Nursing Service Leg Ulcer Clinic Audit 2007 Contents Page number Background 3 Audit Aims 4 Methodology 4 Results 5-11 Discussion 13-15 Action Plan References 2 Background
Varicose Veins Operation. Patient Information Leaflet
 Varicose Veins Operation Patient Information Leaflet April 2017 1 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the leaky
Varicose Veins Operation Patient Information Leaflet April 2017 1 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the leaky
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Compression therapy can
 What are the benefits of using cohesive inelastic compression bandages in the community? Compression therapy can play a vital role in improving the quality of life for those with chronic venous insufficiency,
What are the benefits of using cohesive inelastic compression bandages in the community? Compression therapy can play a vital role in improving the quality of life for those with chronic venous insufficiency,
Varicose Veins. These are abnormal veins in the legs that appear as unsightly or cause other problems.
 Varicose Veins What are varicose veins? These are abnormal veins in the legs that appear as unsightly or cause other problems. They develop due to abnormal valve function that allows the blood to travel
Varicose Veins What are varicose veins? These are abnormal veins in the legs that appear as unsightly or cause other problems. They develop due to abnormal valve function that allows the blood to travel
Varicose Veins: A guide for patients
 Varicose Veins: A guide for patients Varicose Veins: A guide for patients What are varicose veins? Varicose veins are swollen, twisted and unsightly veins (usually on the legs) that look lumpy and bluish
Varicose Veins: A guide for patients Varicose Veins: A guide for patients What are varicose veins? Varicose veins are swollen, twisted and unsightly veins (usually on the legs) that look lumpy and bluish
Reducing the Risk of Deep Vein Thrombosis (DVT) whilst in hospital and following your discharge home
 Reducing the Risk of Deep Vein Thrombosis (DVT) whilst in hospital and following your discharge home 1 Part of: South Tyneside and Sunderland Healthcare Group Introduction This leaflet explains what Deep
Reducing the Risk of Deep Vein Thrombosis (DVT) whilst in hospital and following your discharge home 1 Part of: South Tyneside and Sunderland Healthcare Group Introduction This leaflet explains what Deep
Big toe fusion. If you have any further questions, please speak to a doctor or nurse caring for you.
 Big toe fusion This leaflet aims to answer your questions about having big toe fusion surgery. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Big toe fusion This leaflet aims to answer your questions about having big toe fusion surgery. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
National Aboriginal Diabetes Association
 National Aboriginal Diabetes Association 2015 To increase awareness of diabetes and foot care management Disclaimer: This presentation is offered as educational information and shall not be used as a substitute
National Aboriginal Diabetes Association 2015 To increase awareness of diabetes and foot care management Disclaimer: This presentation is offered as educational information and shall not be used as a substitute
Understanding compression stockings (hosiery) Leg Ulcer Management Team Patient Information Leaflet
 Understanding compression stockings (hosiery) Leg Ulcer Management Team Patient Information Leaflet Introduction Your leg ulcer clinic coordinator, nurse or health professional has recommended that you
Understanding compression stockings (hosiery) Leg Ulcer Management Team Patient Information Leaflet Introduction Your leg ulcer clinic coordinator, nurse or health professional has recommended that you
Complex Limb Injury. Exceptional healthcare, personally delivered
 Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
a health care guide Care of your high-risk feet
 a health care guide Care of your high-risk feet Why is it important? Certain medical conditions for example, diabetes, rheumatoid arthritis and circulation disorders can place your feet at high risk of
a health care guide Care of your high-risk feet Why is it important? Certain medical conditions for example, diabetes, rheumatoid arthritis and circulation disorders can place your feet at high risk of
The Clatterbridge Cancer Centre. NHS Foundation Trust. Lymphoedema Advice. Rehabilitation and Support. A guide for patients and carers
 The Clatterbridge Cancer Centre NHS Foundation Trust Lymphoedema Advice Rehabilitation and Support A guide for patients and carers Contents Lymphatic system... 1 Causes of lymphoedema after cancer treatment...
The Clatterbridge Cancer Centre NHS Foundation Trust Lymphoedema Advice Rehabilitation and Support A guide for patients and carers Contents Lymphatic system... 1 Causes of lymphoedema after cancer treatment...
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS
 Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
Shropshire s Continence Advisory Service INDWELLING URINARY CATHETERS Information for Patients and Carers F:\CONTINENCE\Acute Urianary Retention\04-12\005- Indwelling Urinary Cathter Leaflet - A4-13-02-09.doc
How can DIABETES affect my FEET? Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL. of the infection risk in chronic wound
 Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Lymphoedema Network Northern Ireland. Advice for patients at risk of developing lymphoedema
 Lymphoedema Network Northern Ireland Advice for patients at risk of developing lymphoedema Conditions related to increased risk of developing lymphoedema: High risk referral criteria Do you have any of
Lymphoedema Network Northern Ireland Advice for patients at risk of developing lymphoedema Conditions related to increased risk of developing lymphoedema: High risk referral criteria Do you have any of
Femoropopliteal/distal. bypass grafts. Vascular Surgery Patient Information Leaflet
 Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
V11 Endovenous Ablation
 For the personal patients of Bruce Braithwaite V11 Endovenous Ablation What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common, affecting up to 3 in 10 people.
For the personal patients of Bruce Braithwaite V11 Endovenous Ablation What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common, affecting up to 3 in 10 people.
A Patient s guide to. Shoulder Spica
 A Patient s guide to Shoulder Spica Plaster Theatre Helpline Telephone: 0208 909 5467 Monday to Friday 7:45am - 5pm Out of hours Contact your local emergency services and inform the above number ASAP.
A Patient s guide to Shoulder Spica Plaster Theatre Helpline Telephone: 0208 909 5467 Monday to Friday 7:45am - 5pm Out of hours Contact your local emergency services and inform the above number ASAP.
Transperineal Biopsy of the Prostate
 Transperineal Biopsy of the Prostate Department of Urology Patient Information What What is a is Prostate? a Prostate? The Prostate is an organ forming part of the male reproductive system. It is located
Transperineal Biopsy of the Prostate Department of Urology Patient Information What What is a is Prostate? a Prostate? The Prostate is an organ forming part of the male reproductive system. It is located
Sclerotherapy for Venous Vascular and Lymphatic Malformations
 Service: Imaging Sclerotherapy for Venous Vascular and Lymphatic Malformations Exceptional healthcare, personally delivered Your doctor has requested that you have sclerotherapy. We hope that the following
Service: Imaging Sclerotherapy for Venous Vascular and Lymphatic Malformations Exceptional healthcare, personally delivered Your doctor has requested that you have sclerotherapy. We hope that the following
