Prospective randomized comparison of three endoscopic modalities used in treatment of bladder stones
|
|
|
- Stanley Ross
- 6 years ago
- Views:
Transcription
1 UJ ISSN Urologia 2016 ; 00 ( 00): 000=000 DOI: /uro Original RESEARCH article Prospective randomized comparison of three endoscopic modalities used in treatment of bladder stones Ankur Bansal, Manoj Kumar, Satyanarayan Sankhwar, Sunny Goel, Madhusudan Patodia, Ruchir Aeron, Ved Bhaskar King George Medical University, Lucknow, Uttar Pradesh - India Abstract Introduction: The aim of this study was to compare three endoscopic modalities used in the treatment of bladder stones: transurethral use of cystoscope or nephroscope and percutaneous cystolithotripsy (PCCL). Methods: This study included 210 patients of bladder stone treated at a tertiary care centre in North India from January 2006 to July 2013 who were randomly assigned into three groups: group 1 (transurethral removal using cystoscope), group 2 (transurethral removal using nephroscope) and group 3 (PCCL). Baseline and perioperative data wererecorded and compared between three groups. Results: Baseline parameters were comparable between the three groups. Operating time in group 2 was significantly less than the other two groups. Complete clearance was achieved in all the patients. Group 2 had maximum number of urethral entries. The incidence of perioperative complications (fever, transient haematuria and persistent leakage from suprapubic site) was comparable between these three groups. Till the last follow-up, 3.2% patients (n = 2) developed urethral stricture in group 1, 7.8% (n = 5) in group 2 and no patient developed urethral stricture in group 3 (p = 0.068). Conclusions: Removal of bladder stones by the transurethral route, using a nephroscope, is the most effective treatment modality in terms of operative time with long-term urethral stricture rate similar to transurethral cystoscope technique. Comparatively, PCCL is a safe procedure with acceptable morbidity. Overall, all three techniques are equally efficacious in treating bladder stones of size 1-4 cm. Keywords: Bladder stones, cystoscope, nephroscope, percutaneous cystolithotripsy, transurethral Introduction Bladder stones account for 5% of all urinary stones in developed countries. The incidence is much higher in developing countries (1). The traditional method of treatment was open suprapubic cystolithotomy, which is still recommended for large stones (2). However, with the advances in endourology, majority of bladder stones are managed by endoscopic transurethral approach using intracorporeal lithotripters such as electrohydraulic lithotripsy, ultrasound lithotripsy, Swiss pneumatic lithoclast and holmium: yttrium-aluminium-garnet laser (Ho: YAG laser). Transurethral removal of bladder stones using a nephroscope has been recently performed and has Accepted: March 8, 2016 Published online: April 9, 2016 Corresponding author: Ankur Bansal, MS Department of Urology King George Medical College Lucknow Uttar Pradesh, India ankurbansaldmc@gmail.com proved to be fast and effective treatment modality as compared withtransurethral cystoscopic approach (3). Principles of percutaneous nephrolithomy (PCNL), that is percutaneous access and tract dilation, can also be applied to bladder stones where rapid and effective removal can be done through suprapubic percutaneous route. This study aimed at comparing three different endoscopic modalities used in the treatment of bladder stones [transurethral removal using cystoscope or nephroscope and percutaneous cystolithotripsy (PCCL)]. Materials and methods This study was conducted at a tertiary care centre in North India from January 2006 to July All patients presenting with bladder calculi who required surgery were enrolled in this study. Informed consent was taken from all the patients. Complete blood count, renal function tests, urine culture and sensitivity, X-ray kidney ureter and bladder (KUB) and ultrasound abdomen were done in all patients. Inclusion criteria were bladder stone of 1-4 cm of size, age 18 years or more and normal renal function. Patients with age less than 18 years, deranged renal function, stone size more than 4 cm, prior history of surgery for bladder stone, pelvic surgery, urinary diversion, bladder tumour or those having urethral stricture were
2 2 Comparison of three modalities used in treatment of bladder stones excluded from the study. Urodynamic study was done when indicated. Patients were randomly allotted into threegroups (using computer-generated simple randomization chart) Group 1: Transurethral removal using cystoscope Group 2: Transurethral removal using nephroscope Group 3: PCCL using nephroscope Surgical technique Prophylactic oral antibiotics were given prior to surgery in all patients. Patients presenting with urinary tract infection were managed with antibiotics preoperatively, and the surgery was postponed till the urine culture became sterile. All patients were operated under spinal anaesthesia by one of the two surgeons (SS or MK). All patients underwent cystoscopy with 19-Fr cystoscope (Karl Storz) to determine the size and number of stones and also to rule out any associated pathology. Group 1 (Transurethral removal using cystoscope) A 22-French (Fr) cystoscope with 30 telescope (KARLZ STORZ Endovision, Inc., Charlton, MA, USA ) was inserted through urethra and fragmentation of stones was done using intracorporeal pneumatic lithotripter (Swiss Lithoclast 2- Richard Wolf, Germany). Evacuation of stone fragments was done by ellik bladder evacuator (BARD, C.R. BARD, INC., New Jersey, US). At the end of procedure, a 16-Fr Foley catheter was inserted perurethrally that was removed on postoperative day 1. Group 2 (Transurethral removal using nephroscope) After inserting adequate 2% lidocaine jelly into the urethra, 22-Fr rigid nephroscope (Richard Wolf) was introduced without sheath into the bladder. The fragmentation of stones was done using intracorporeal pneumatic lithotripter. The nephroscope was then withdrawn followed by reinsertion of 22-Fr cystoscope. Removal of stone fragments was done using ellik evacuator. In case of large fragments thatcould not be evacuated by ellik evacuator, nephroscope was inserted again for further fragmentation and retrieval of fragments was done as described above. At the end of procedure, 16-Fr Foley catheter was inserted perurethrally thatwas removed on postoperative day 1. Group 3 [Percutaneous cystolithotripsy (PCCL) using nephroscope] One centimetre transverse incision was given 2 cm above the pubic symphysis. Through this incision, 18-gauge puncture needle was passed into bladder under transurethral 19-Fr cystoscope guidance. A inch guidewire was then passed through puncture needle following which dilatation of tract was done using telescopic metal dilators and 24-Fr amplatz sheath was placed. A 22-Fr nephroscope was inserted through the amplatz sheath and stone was fragmented with pneumatic lithoclast. Retrieval of fragments was done by stone-grasping forceps. Perurethral and suprapubic catheters were placed at the end of procedure. Suprapubic catheter was removed on postoperative day 1 and urethral catheter was removed on postoperative day 2. Baseline parameters were recorded thatincluded age, gender, mode of presentation, stone size and number of stones. Outcomes The primary outcomes recorded were perioperative complications (fever, transient haematuria and persistent urinary leakage from suprapubic site) and occurrence of urethral stricture. These measures were assessed perioperatively and during follow-up by an independent investigator (NK) blinded to the treatment modality received by each patient. The secondary outcomes recorded were operating time, requirement of additional procedure, type of additional procedure, number of urethral entries, pain score [calculated by visual analogue scale (VAS)], duration of hospital stay and convalescence period. The operative time required for additional procedures was not included in the operative time, which was used for statistical analysis. Pain was assessed at 6 hours postoperatively with VAS measuring 0 to 10 (0 no pain, 10 worst pain). The patients who underwent additional procedures were excluded from further analysis. Stone analysis of all patients wasdone for identification of chemical composition of stones. Follow-up of patients in each treatment was done at 6, 12 and 24 months postoperatively, which included uroflowmetry, ultrasound abdomen and metabolic work-up of the patient. Retrograde urethrogram and urethroscopy were done if urethral stricture was suspected. Fever was defined as a temperature of more than 100 F. Haematuria that persisted for more than 6 hours and had resolved spontaneously by 48 hours was defined as transient hematuria. The return back to public life after surgery was considered as duration of convalescence. Sample size The reported cumulative incidence of perioperative and postoperative complications after endoscopic treatment for bladder stones is 7.4% (4). Assuming 80% power, 5% significance level (α = 0.05, β = 0.20), the minimum sample size per treatment arm required was 66 as per Beth and Robert (5). Statistical analysis One-way analysis of variance (ANOVA) was used to compare continuous data and Fischer exact test was used to analyse categorical data. Intergroup comparison was done to find out the groups between which the difference was statistically significant. This was done by applying post hoc comparison test. Statistical analysis was performed using SPSS, version 16 (Chicago, IL, USA). The statistical significance level used was p<0.05. Results A total of 1054 patients presented with lower urinary tract symptoms were screened for this study and 316 patients of bladder stones were enrolled in this study. One hundred six patients were excluded from the study [patients with age
3 Bansal et al 3 Fig. 1 - Flow of patients during the study period. less than 18 years (n = 23), deranged renal function (n = 9), stone size more than 4 cm (n = 29), prior history of surgery for bladder stone (n = 15), pelvic surgery (n = 6), urinary diversion (n = 3), those having urethral stricture (n = 18) or concurrent bladder tumour (n = 3)]. A total of two hundred ten patients met the inclusion criteria during the study period. These patients were randomly assigned into three groups with 70 patients in each group; 86.7% (n = 182) were male and the rest were female. Figure 1 shows the flow of patients during the study period. Baseline parameters such asage, gender, mode of presentation, stone size and number of stones were comparable between the three groups (Tab. I). Significant difference was observed in mean operating times: group 1 (51.2 ± 23.2 min), group 2 (33.6 ± 7.0 min) and group 3 (47.8 ± 17.6 min). Intergroup comparison showed that the mean operating time in group 2 was significantly lower than the other two groups (Tab. II). Complete clearance was achieved in all the patients. Nineteen patients [group 1 (n = 8), group 2 (n = 6), group 3 (n = 5)] required additional procedures,for example, bladder neck incision and transurethral resection of prostate. These patients were excluded from further analysis. When compared withother groups, group 2 had maximum number of urethral entries. VAS score of Group 3 was significantly higher than Group 2, which in turn was significantly higher than Group 1 (p = 0.001). Postoperative hospital stay and duration of convalescence were significantly more in group 3. The incidence of perioperative complications (fever, transient haematuria and persistent leakage from suprapubic site) was comparable between these three groups. Till the last follow-up, 3.2% patients (n = 2) developed urethral stricture in group 1, 7.8% (n = 5) in group 2 and no patient developed urethral stricture in group 3 (p = 0.068). All these patients had short segment, nonobliterative bulbar urethral stricture and were treated successfully with visual internal urethrotomy. Discussion Bladder stones can be classified into either primary or secondary. The stones that fall from kidney and get lodged in bladder are primary in nature, while secondary stones are formed inside the bladder due to bladder outlet obstruction, indwelling prolonged catheterization, bladder diverticulum, neurogenic bladder trauma, foreign body, etc. Struvite, uric acid and calcium stones are most common type of bladder stones in adults and older people. In our study, the most prevalent stone compositions were struvite and uric acid, which were present in 34.7% (n = 73/210) and 24.2% (n = 51/210) patients, respectively (Tab. I). The possible aetiology of bladder stones could be established in 27% (n = 56) of cases,that is prostatic enlargement (n = 19), history of
4 4 Comparison of three modalities used in treatment of bladder stones Table I - Comparison of baseline parameters and operative outcomes of three groups Parameters Group 1 Group 2 Group 3 p No. of patients Gender (n) Male Female Age (in years) 46.3 ± ± ± Mean ± SD (Range) (21-70) (19-67) (22-69) Mode of presentation Difficulty in voiding Terminal Hematuria Vague abdominal pain Urinary tract infection Acute urinary retention Incidental finding Stone size (in cm) 2.6 ± ± ± Mean ± SD (Range) ( ) ( ) ( ) Number of stones 1.13 ± ± ± Mean ± SD (Range) (1-3) (1-3) (1-3) Operating time 51.2 ± ± ± Mean ± SD (Range) (30-90) (22-48) (29-77) Additional procedures (n) BNI TURP Total Number of urethral entries 1.13 ± ± ± Mean ± SD (Range) (1-2) (2-5) (1-2) VAS score 3.1 ± ± ± Mean ± SD (Range) (1-5) (2-6) (3-7) Early complications (n) Fever Transient hematuria Persistent urinary leakage from suprapubic site Postoperative hospital stay (in days) 1.15 ± ± ± Mean ± SD (Range) (1-2) (1-2) (1-3) Duration of convalescence (in days) 5.6 ± ± ± Mean ± SD (Range) (2-7) (3-8) (4-10) Stone free rate (%) 100% 100% 100% Late complications (n) Urethral stricture Chemical composition of stone (n) Struvite Uric acid Calcium phosphate Calcium oxalate dihydrate/monohydrate Ammonium acid urate Ammonium acid urate + calcium oxalate Ammonium acid urate + uric acid
5 Bansal et al 5 Table II - Intergroup comparison of parameters (whose p value is significant in Table I) to find out the groups between which the difference was actually significant Parameters p value of intergroup comparison Group 1 vs. 2 Group 2 vs. 3 Group 1 vs. 3 Operating time Number of urethral entries VAS score Postoperative hospital stay Duration of convalescence prolonged catheterisation (n = 20), neurogenic bladder (n = 5) and cystocele in females (n = 12) in this study. Patient with bladder stones usually present with painful and intermittent voiding with or without terminal haematuria. Patient may have dull suprapubic discomfort thatis aggravated by sudden movements (6). In our study, the most common presentation was difficulty in voiding in 58.5% (n = 123) and terminal haematuria in 22.8% (n = 48) of patients, respectively. With the advancement in endourology, the majority of bladder stones are managed with endoscopic transurethral approach using intracorporeal lithotripters such as electrohydraulic lithotripsy, ultrasound lithotripsy, Swiss pneumatic lithoclast and Ho:YAG laser (2-3, 7-10). This study aimed at comparing various endoscopic modalities used in the treatment of bladder stones in our hospital. We currently use the pneumatic Swiss Lithoclast for bladder stone fragmentation, as it rapidly fragments all stones irrespective of their density. Moreover, pneumatic Lithoclast is extremely safe, with no reports of urothelial injury during its clinical use (11). Transurethral endoscopic approach is a familiar technique and favoured by most urologists. Using this technique, stones can be fragmented by either mechanical lithotrite or with one of many intracorporeal lithotripsy devices. The mechanical lithotrite is a less favourable option when the stone is more than 2 cm, hard and bladder is of small capacity. Its complication rate varies from 9 to 25% (12, 13). In our study, in group 1, bladder stones were removed using 22-Fr cystoscope combined with pneumatic lithotrite. During cystoscopic fragmentation, there was a decrease in vision quality thatprolonged the duration of fragmentation and led to longer operating time. We observed that the operative time in group 1 was more than the remaining two groups. This procedure was least painful, as VAS score was significantly low in this group. Recently, nephroscope via transurethral route has been increasingly used for removing bladder stones (3, 14). Sathaye et al (14) described the transurethral use of a nephroscope for the treatment of more than 10 cm bladder stones in four patients. All patients were stone free with no complications, concluding that this is an effective method with low morbidity. In group 2, 22-F nephroscope (without sheath) with pneumatic lithotrite was used to fragment the stone. Group 2 had significantly shorter operating time than the other two groups. This can be attributed partly to the better vision provided by the nephroscope and partly to the fact that this method does not require a percutaneous access. Intraoperatively, we kept a slow inflow of saline and stopped intermittently to avoid over distension of bladder. However, when bladder got distended, the bladder was emptied by removing rubber covering over the port inlet of nephroscope. Group 2 had maximum number of mean urethral entries, as 22-Fr cystoscope was inserted for the removal of fragments after removing nephroscope. In case of large fragments thatcould not be evacuated by ellik evacuator, nephroscope was inserted again for further fragmentation and retrieval of fragments. The number of entries into the urethra weremore in earlier phase of study, but as the study progressed, the number of entries were decreased,asthe fragmentation was done at the first occasion before withdrawing the nephroscope. Similar results were seen by Ener et al (3) who compared transurethrally placed nephroscope with transurethral cystoscope for the removal of large bladder stones and demonstrated that the former is a fast and effective treatment modality. PCCL is another treatment option for the removal of bladder stones. It is particularly useful in hard and large stones where transurethral route can lengthen the procedure or can lead to urethral injury. It is an effective and safe procedure in patients with artificially created urinary bladder or anatomical abnormalities of bladder (15-18). PCCL is also a better option than transurethral endoscopic approach in male children, as their urethral calibre is small (19). Recently, Salah et al (20) performed PCCL in 155 children with endemic bladder stones and concluded that it is an effective and safe procedure. Demeriel et al (21) reported the results in PCCL in 72 patients (30 children and 42 adults). The average size of stone was 3.2 cm in children and 5.5 cm in adults. All patients were stone free with no major intra or postoperative complications. In group 3, PCCL was done using 22-Fr nephroscope. Suprapubic percutaneous insertion of amplatz sheath provides excellent view and aids in better fragmentation of the stone. This also decreases prolonged urethral instrumentation. Patients in group 3 experienced more pain in postoperative period than the other two groups probably due to placement of suprapubic catheter, which increases the morbidity as well as the hospital stay of the patient. Hence, group 3 had significantly longer postoperative hospital stay and duration of convalescence. One patient had persistent urinary leakage from suprapubic site thathealed spontaneously after 1 week of catheterisation. A similar study by Kamaljeet et al (22) who also compared these three routes for removal of bladder stone in 67 patients and reported that use of nephroscope via transurethral route is an efficacious and safe method to removal for bladder stones without increase in morbidity. A potential complication of transurethral method in the treatment of bladder stones is the iatrogenic traumatic injury of the urethral lumen. Till the last follow-up, 3.2% patients (n = 2) developed urethral stricture in group 1, 7.8% (n = 5) in group 2 and none in group 3, which was statistically not significant. All these patients had short segment, nonobliterative bulbar urethral stricture and were treated with visual internal urethrotomy. The probable reason of urethral stricture was
6 6 Comparison of three modalities used in treatment of bladder stones prolonged operating time in group 1 and the more number of urethral entries in group 2 that may cause the similar insult as scope size was same in both groups. To conclude, removal of bladder stones by the transurethral route, using a nephroscope, is the most effective treatment modality in terms of operative time with long-term urethral stricture rates similar to transurethral cystoscope technique. Comparatively, PCCL is a safe procedure with acceptable morbidity. Overall, all three techniques are equally efficacious in treating bladder stones of size 1-4 cm. Acknowledgement The authors acknowledge the cooperation of residents of Urology department of King George medical university who participated in appointing the patient and following up. We also appreciate the commitment and compliance of the patient who reported the required data and attended for the regular follow-up. Disclosures Financial support: The authors declared that this study has received no financial support. Conflict of interests: No conflict of interest was declared by the authors. References 1. Zhao J, Shi L, Gao Z, Liu Q, Wang K, Zhang P. Minimally invasive surgery for patients with bulky bladder stones and large benign prostatic hyperplasia simultaneously: a novel design. Urol Int. 2013;91(1): Maheshwari PN, Oswal AT, Bansal M. Percutaneous cystolithotomy for vesical calculi: a better approach. Tech Urol. 1999;5(1): Ener K, Agras K, Aldemir M, Okulu E, Kayigil O. The randomized comparison of two different endoscopic techniques in the management of large bladder stones: transurethral use of nephroscope or cystoscope? J Endourol. 2009;23(7): Al-Marhoon MS, Sarhan OM, Awad BA, Helmy T, Ghali A, Dawaba MS. Comparison of endourological and open cystolithotomy in the management of bladder stones in children. J Urol. 2009;181(6): , discussion Dawson B, Trapp RG. Basic & clinical biostatistics. International edition, 4 th ed. New York: Mc-Graw-Hill;2004. p Papatsoris AG, Varkarakis I, Dellis A, Deliveliotis C. Bladder lithiasis: from open surgery to lithotripsy. Urol Res. 2006;34(3): Schwartz BF, Stoller ML. The vesical calculus. Urol Clin North Am. 2000;27(2): Asci R, Aybek Z, Sarikaya S. Buyukalpelli, Yilmaz A F. The management of vesical calculi with optical mechanical cystolithotripsy and transurethral prostatectomy is it safe and effective? BJU Int. 1999;84: Zhaowu Z, Xiwen W, Fenling Z. Experience with electrohydraulic shockwave lithotripsy in the treatment of vesical calculi. Br J Urol. 1988;61(6): Aron M, Goel R, Gautam G, Seth A, Gupta NP. Percutaneous versus transurethral cystolithotripsy and TURP for large prostates and large vesical calculi: refinement of technique and updated data. Int Urol Nephrol. 2007;39(1): Schulze H, Haupt G, Piergiovanni M, Wisard M, von Niederhausern W, Senge T. The Swiss Lithoclast: a new device for endoscopic stone disintegration. J Urol. 1993;149(1): Bhatia V, Biyani CS. Vesical lithiasis: open surgery versus cystolithotripsy versus extracorporeal shock wave therapy. J Urol. 1994;151(3): Razvi HA, Song TY, Denstedt JD. Management of vesical calculi: comparison of lithotripsy devices. J Endourol. 1996;10(6): Sathaye UV. Per-urethral endoscopic management of bladder stones: does size matter? J Endourol. 2003;17(7): , discussion Cain MP, Casale AJ, Kaefer M, Yerkes E, Rink RC. Percutaneous cystolithotomy in the pediatric augmented bladder. J Urol. 2002;168(4 Pt 2): Lam PN, Te CC, Wong C, Kropp BP. Percutaneous cystolithotomy of large urinary-diversion calculi using a combination of laparoscopic and endourologic techniques. J Endourol. 2007;21(2): Ikari O, Nettó NR Jr, D Ancona CA, Palma PC. Percutaneous treatment of bladder stones. J Urol. 1993;149(6): Wollin TA, Singal RK, Whelan T, Dicecco R, Razvi HA, Denstedt JD. Percutaneous suprapubic cystolithotripsy for treatment of large bladder calculi. J Endourol. 1999;13(10): Ahmadnia H, Younesi Rostami M, Yarmohammadi AA, Parizadeh SM, Esmaeili M, Movarekh M. Percutaneous treatment of bladder calculi in children: 5 years experience. Urol J. 2006; 3(1): Salah MA, Holman E, Khan AM, Toth C. Percutaneous cystolithotomy for pediatric endemic bladder stone: experience with 155 cases from 2 developing countries. J Pediatr Surg. 2005; 40(10): Demirel F, Cakan M, Yalçinkaya F, Demirel AC, Aygün A, Altuğ UU. Percutaneous suprapubic cystolithotripsy approach: for whom? Why? J Endourol. 2006;20(6): Singh KJ, Kaur J. Comparison of three different endoscopic techniques in management of bladder calculi. Indian J Urol. 2011;27(1):10-13.
JMSCR Vol 04 Issue 10 Page October 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i10.40 Combined Bladder Stones Removal: In
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i10.40 Combined Bladder Stones Removal: In
Kemal Ener, M.D., Koray Agras, M.D., Mustafa Aldemir, M.D., Emrah Okulu, M.D., and Onder Kayigil, M.D.
 JOURNAL OF ENDOUROLOGY Volume 23, Number 7, July 2009 ª Mary Ann Liebert, Inc. Pp. 1151 1155 DOI: 10.1089=end.2008.0647 The Randomized Comparison of Two Different Endoscopic Techniques in the Management
JOURNAL OF ENDOUROLOGY Volume 23, Number 7, July 2009 ª Mary Ann Liebert, Inc. Pp. 1151 1155 DOI: 10.1089=end.2008.0647 The Randomized Comparison of Two Different Endoscopic Techniques in the Management
Shock Wave Lithotripsy for Bladder Stones
 Human Journals Research Article February 2018 Vol.:11, Issue:3 All rights are reserved by Haider A. AbuAlmaali et al. Shock Wave Lithotripsy for Bladder Stones Keywords: Shock Wave Lithotripsy, Bladder
Human Journals Research Article February 2018 Vol.:11, Issue:3 All rights are reserved by Haider A. AbuAlmaali et al. Shock Wave Lithotripsy for Bladder Stones Keywords: Shock Wave Lithotripsy, Bladder
Lec-8 جراحة بولية د.نعمان
 4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size
 Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Author's response to reviews Title:Transurethral Cystolitholapaxy with the AH -1 Stone Removal System for the Treatment of Bladder Stones of Variable Size Authors: Aihua Li (Li121288@aliyun.com) Chengdong
Percutaneous Nephrolithotomy and Laparoscopic Management of Urinary Tract Calculi
 16 Percutaneous Nephrolithotomy and Laparoscopic Management of Urinary Tract Calculi Pedro-José López, Michael J. Kellett, and Patrick G. Duffy Urinary calculus in childhood is not common. The incidence
16 Percutaneous Nephrolithotomy and Laparoscopic Management of Urinary Tract Calculi Pedro-José López, Michael J. Kellett, and Patrick G. Duffy Urinary calculus in childhood is not common. The incidence
traced in Hippocratic oath stating that I will not cut for bladder stone, even for patients in whom the disease is manifest
 ORIGINAL ARTICLE ROLE OF PNEUMATIC LITHOTRIPSY IN PAEDIATRIC BLADDER STONES I WILL NOT CUT UPON STONE! ABSTRACT Liaqat Ali 1, Saima Ali 2, Shafieullah 3, Nasir Orakzai 4 OBJECTIVE: To study the effectiveness
ORIGINAL ARTICLE ROLE OF PNEUMATIC LITHOTRIPSY IN PAEDIATRIC BLADDER STONES I WILL NOT CUT UPON STONE! ABSTRACT Liaqat Ali 1, Saima Ali 2, Shafieullah 3, Nasir Orakzai 4 OBJECTIVE: To study the effectiveness
Research Article Effect of Amplatz Sheath on Cystolithotripsy for Women with Large Bladder Stone
 Hindawi BioMed Research International Volume 2017, Article ID 9341042, 4 pages https://doi.org/10.1155/2017/9341042 Research Article Effect of Amplatz Sheath on Cystolithotripsy for Women with Large Bladder
Hindawi BioMed Research International Volume 2017, Article ID 9341042, 4 pages https://doi.org/10.1155/2017/9341042 Research Article Effect of Amplatz Sheath on Cystolithotripsy for Women with Large Bladder
Preface. Prasad P. Godbole. vii
 Preface Pediatric urology has rapidly developed as a separate subspeciality in the last decade. During this time, significant advances in technology and instrumentation have meant that more procedures
Preface Pediatric urology has rapidly developed as a separate subspeciality in the last decade. During this time, significant advances in technology and instrumentation have meant that more procedures
RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES
 1110-5712 Vol. 20, No. 3, 2014 Egyptian Journal of Urology 121-125 RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES AHMED EL-FEEL, AHMED SAMIR, HESHAM FATHY, OMAR M
1110-5712 Vol. 20, No. 3, 2014 Egyptian Journal of Urology 121-125 RETROGRADE URETEROSCOPIC HOLMIUM: YAG LASER LITHOTRIPSY FOR URETERAL AND RENAL STONES AHMED EL-FEEL, AHMED SAMIR, HESHAM FATHY, OMAR M
Transurethral cystolitholapaxy with the AH-1 stone removal system for the treatment of bladder stones of variable size
 Li et al. BMC Urology (2015) 15:9 DOI 10.1186/s12894-015-0003-z TECHNICAL ADVANCE Open Access Transurethral cystolitholapaxy with the AH-1 stone removal system for the treatment of bladder stones of variable
Li et al. BMC Urology (2015) 15:9 DOI 10.1186/s12894-015-0003-z TECHNICAL ADVANCE Open Access Transurethral cystolitholapaxy with the AH-1 stone removal system for the treatment of bladder stones of variable
Research Paper. Zhenlong Wang #, Li Xue #, Ziming Wang, Weimin Gan, Haiwen Chen, Hecheng Li, Peng Zhang, Hongliang Li, Tie Chong* 1.
 Adjuvant U100-plus laser cystolithotripsy is therapeutically effective and safe for benign prostate hyperplasia patients with complicating bladder lithiasis: a prospective, randomized, controlled study
Adjuvant U100-plus laser cystolithotripsy is therapeutically effective and safe for benign prostate hyperplasia patients with complicating bladder lithiasis: a prospective, randomized, controlled study
URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 9 (58) No. 2-2016 URETERORENOSCOPY: INDICATIONS AND COMPLICATIONS - A RETROSPECTIVE STUDY L. MAXIM 1,2 I.A. BĂNUŢĂ 2 I.
Original Article - Lasers in Urology. Min Ho Lee, Hee Jo Yang, Doo Sang Kim, Chang Ho Lee, Youn Soo Jeon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report
 198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
198) Prague Medical Report / Vol. 117 (2016) No. 4, p. 198 203 Percutaneous Nephrolithotomy in a Patient with Mainz Pouch II Urinary Diversion: A Case Report Stavros Sfoungaristos 1, Ioannis Mykoniatis
ISSN East Cent. Afr. J. surg. (Online)
 87 Ureteroscopy in a Resource Limited Setting: The Tikur Anbessa General Specialized Hospital Experience in Addis Ababa, Ethiopia. D. Andualem, L. Be-ede, T. Mulat, L. Samodi Addis Ababa University-School
87 Ureteroscopy in a Resource Limited Setting: The Tikur Anbessa General Specialized Hospital Experience in Addis Ababa, Ethiopia. D. Andualem, L. Be-ede, T. Mulat, L. Samodi Addis Ababa University-School
Hong Kong College of Surgical Nursing
 Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
Hong Kong College of Surgical Nursing Higher Surgical Nursing Training: Part B Specialty - Urological Nursing Curriculum TABLE OF CONTENTS No. Contents Page. Introduction. Aims. Learning Objectives 4.
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
The technology described in this briefing is minimally invasive percutaneous nephrolitholapaxy medium (MIP-M). It is used to remove kidney stones.
 pat hways Minimally invasive percutaneous nephrolitholapaxy medium (MIP-M) for removing kidney stones Medtech innovation briefing Published: 26 January 2018 nice.org.uk/guidance/mib8 Summary The technology
pat hways Minimally invasive percutaneous nephrolitholapaxy medium (MIP-M) for removing kidney stones Medtech innovation briefing Published: 26 January 2018 nice.org.uk/guidance/mib8 Summary The technology
Pneumatic Lithotripsy: A New Modality for Treatment of Ureteric Stones
 Pneumatic Lithotripsy: A New Modality for Treatment of Ureteric Stones Pages with reference to book, From 9 To 11 A.A. Naqvi, M. Khaliq, M.N. Zafar, S.A.H. Rizvi ( Institute of Urology and Transplantation,
Pneumatic Lithotripsy: A New Modality for Treatment of Ureteric Stones Pages with reference to book, From 9 To 11 A.A. Naqvi, M. Khaliq, M.N. Zafar, S.A.H. Rizvi ( Institute of Urology and Transplantation,
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 54/Oct 20, 2014 Page 12411
 SAFETY AND EFFICACY OF PAEDIATRIC PCNL T. Jagadeeshwar 1, Ravi Jahagirdhar 2, A. Bhagawan 3, N. Rama Murthy 4, G. Ravichandar 5, G. Mallikarjun 6, B. Santosh 7, K. V. Narendra 8 HOW TO CITE THIS ARTICLE:
SAFETY AND EFFICACY OF PAEDIATRIC PCNL T. Jagadeeshwar 1, Ravi Jahagirdhar 2, A. Bhagawan 3, N. Rama Murthy 4, G. Ravichandar 5, G. Mallikarjun 6, B. Santosh 7, K. V. Narendra 8 HOW TO CITE THIS ARTICLE:
3. Urinary Catheters. Indications. Methods of Bladder Catheterization. Hashim Hashim
 3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
3. Urinary Catheters Hashim Hashim Indications Urinary catheters are used to drain urine from the bladder. The main indications are: A. Diagnostic Measure post-void residual in the absence of ultrasound
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study
 Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
Ureteral Stenting after Flexible Ureterorenoscopy with Ureteral Access Sheath; Is It Really Needed?: A Prospective Randomized Study J Med Assoc Thai 2017; 100 (Suppl. 3): S174-S178 Full text. e-journal:
Corresponding Author : Dr.P.Gunaseelan
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 10 (May. 2018), PP 68-72 www.iosrjournals.org Comparison of outcomes of Percutaneous
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 10 (May. 2018), PP 68-72 www.iosrjournals.org Comparison of outcomes of Percutaneous
Complication of long indwelling urinary catheter and stent COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT
 151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
151 COMPLICATION OF LONG INDWELLING URINARY CATHETER AND STENT Jain A 1 *, Srivastava R 1, Prasad A 1, Marwah K 1 1. Department of surgery, Subharti medical college, Meerut U.P. India Correspondence: Dr.
The Evaluation of not Stenting after Uncomplicated Ureteroscopy: A Randomized Prospective Study
 Bahrain Medical Bulletin, Vol.26, No. 1, Mach 2004 The Evaluation of not Stenting after Uncomplicated Ureteroscopy: A Randomized Prospective Study Waleed Ali, FRCS* Mohammed Al-Durazi, FRCS** Reem Al-Bareeq,
Bahrain Medical Bulletin, Vol.26, No. 1, Mach 2004 The Evaluation of not Stenting after Uncomplicated Ureteroscopy: A Randomized Prospective Study Waleed Ali, FRCS* Mohammed Al-Durazi, FRCS** Reem Al-Bareeq,
ENDOSCOPY INSTRUMENTS. - / Web:- Maryland, USA : +1(202) /
 ENDOSCOPY INSTRUMENTS Email:- sales@addler.com / sales.addler@gmail.com Web:- Maryland, USA : +1(202)2302130 / 2478875 CYSTOSCOPY ACCESSORIES We are leading manufacturer of Cystoscope Sheaths which design
ENDOSCOPY INSTRUMENTS Email:- sales@addler.com / sales.addler@gmail.com Web:- Maryland, USA : +1(202)2302130 / 2478875 CYSTOSCOPY ACCESSORIES We are leading manufacturer of Cystoscope Sheaths which design
Treatment of pediatric renal calculi between 1990 and 2006 in Henan province
 Treatment of pediatric renal calculi between 1990 and 2006 in Henan province Bingqian Liu *, Yudong Wu, Jinxing Wei, Jianguang Gao Department of Urology, the First Affiliated Hospital of Zhengzhou University,
Treatment of pediatric renal calculi between 1990 and 2006 in Henan province Bingqian Liu *, Yudong Wu, Jinxing Wei, Jianguang Gao Department of Urology, the First Affiliated Hospital of Zhengzhou University,
Percutaneous nephrolithotomy for staghorn kidney stones in elderly patients
 Int Urol Nephrol (2011) 43:639 643 DOI 10.1007/s11255-010-9885-6 UROLOGY ORIGINAL PAPER Percutaneous nephrolithotomy for staghorn kidney stones in elderly patients Baris Kuzgunbay Tahsin Turunc Ozgur Yaycioglu
Int Urol Nephrol (2011) 43:639 643 DOI 10.1007/s11255-010-9885-6 UROLOGY ORIGINAL PAPER Percutaneous nephrolithotomy for staghorn kidney stones in elderly patients Baris Kuzgunbay Tahsin Turunc Ozgur Yaycioglu
Tubeless Percutaneous Nephrolithotomy: Spinal versus General Anesthesia
 Tubeless Percutaneous Nephrolithotomy: Spinal versus General Anesthesia Murat Gonen, 1 Betul Basaran 2 ENDOUROLOGY AND STONE DISEASE 1 Department of Urology, Baskent University, Konya, Turkey. 2 Department
Tubeless Percutaneous Nephrolithotomy: Spinal versus General Anesthesia Murat Gonen, 1 Betul Basaran 2 ENDOUROLOGY AND STONE DISEASE 1 Department of Urology, Baskent University, Konya, Turkey. 2 Department
Clinical Study Ureteral Stenting after Uncomplicated Ureteroscopy for Distal Ureteral Stones: A Randomized, Controlled Trial
 Minimally Invasive Surgery, Article ID 892890, 4 pages http://dx.doi.org/10.1155/2014/892890 Clinical Study Ureteral Stenting after Uncomplicated Ureteroscopy for Distal Ureteral Stones: A Randomized,
Minimally Invasive Surgery, Article ID 892890, 4 pages http://dx.doi.org/10.1155/2014/892890 Clinical Study Ureteral Stenting after Uncomplicated Ureteroscopy for Distal Ureteral Stones: A Randomized,
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Urology ENDOSCOPIC LOWER URINARY TRACT
 ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
ENDOSCOPIC LOWER URINARY TRACT Cystolitholapaxy Cystoscopic removal of foreign body from bladder Cystoscopic removal of ureteric stent Cystoscopy and cystodiathermy Cystoscopy and transurethral biopsy
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
Urological Procedure Coding
 Urological Procedure Coding AAPC Annual Conference April 6, 2011 Long Beach, California Objectives Understand anatomy and CPT procedural terminology related to urological procedures Recognize and code
Urological Procedure Coding AAPC Annual Conference April 6, 2011 Long Beach, California Objectives Understand anatomy and CPT procedural terminology related to urological procedures Recognize and code
Urology Department Percutaneous Nephrolithotomy (PCNL)
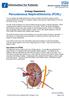 Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
In Situ Extracorporeal Shock Wave Lithotripsy (ESWL) and ESWL after Push Back For Upper Ureteric Calculi: A Comparative Study
 ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Original Article Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 6, Number 1, Issue 10, January-June
ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Original Article Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 6, Number 1, Issue 10, January-June
Combined Antegrade And Retrograde Endoscopic Realignment Of Traumatic Urethral Disruption
 ISPUB.COM The Internet Journal of Urology Volume 7 Number 1 Combined Antegrade And Retrograde Endoscopic Realignment Of Traumatic Urethral Disruption I SO, O OA, E JO, B BO, A RA Citation I SO, O OA, E
ISPUB.COM The Internet Journal of Urology Volume 7 Number 1 Combined Antegrade And Retrograde Endoscopic Realignment Of Traumatic Urethral Disruption I SO, O OA, E JO, B BO, A RA Citation I SO, O OA, E
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA. A Minimally Invasive Innovative Treatment
 PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
PROSTATIC ARTERY EMBOLISATION (PAE) FOR BENIGN PROSTATIC HYPERPLASIA A Minimally Invasive Innovative Treatment What is the prostate? The prostate is an accessory organ of the male reproductive system.
Objectives: To analyze various factors predicting success of retrograde ureteric stenting in managing patients with ureteric obstruction.
 ISPUB.COM The Internet Journal of Urology Volume 14 Number 1 Factors Predicting Success Rate Of Retrograde Ureteric Stenting In Managing Patients With Ureteric Obstruction- Our Experiences In A South Indian
ISPUB.COM The Internet Journal of Urology Volume 14 Number 1 Factors Predicting Success Rate Of Retrograde Ureteric Stenting In Managing Patients With Ureteric Obstruction- Our Experiences In A South Indian
Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP)
 JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
JRural Med 2007 ; 2 : 93 97 Original article Early-Stage Clinical Experiences of Holmium Laser Enucleation of the Prostate (HoLEP) Shuzo Hamamoto 1,TakehikoOkamura 1,HideyukiKamisawa 1,KentaroMizuno 1,
Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi
 Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
The use of Amplatz renal dilators in the minimally invasive management of complex urethral strictures
 301 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY The use of Amplatz renal dilators in the minimally invasive management of complex urethral strictures Michael Nomikos 1, Sarantis Papanikolaou
301 O R I G I N A L P A P E R TRAUMA AND RECONSTRUCTIVE UROLOGY The use of Amplatz renal dilators in the minimally invasive management of complex urethral strictures Michael Nomikos 1, Sarantis Papanikolaou
Authors KC Cheng, LF Lee, KW Wong, HC Chan, CL Cho, H Chau, KM Lam, HS So. Division of Urology, Department of Surgery, United Christian Hospital
 Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Efficacy of Routine Screening of Urine Culture before Transurethral Prostatectomy on the Improvement of the Post Operative Outcome - a Single Centre Experience Authors KC Cheng, LF Lee, KW Wong, HC Chan,
Long-term results of permanent memotherm urethral stent in the treatment of recurrent bulbar urethral strictures
 ORIGINAL Article Vol. 40 (1): 80-86, January - February, 2014 doi: 10.1590/S1677-5538.IBJU.2014.01.12 Long-term results of permanent memotherm urethral stent in the treatment of recurrent bulbar urethral
ORIGINAL Article Vol. 40 (1): 80-86, January - February, 2014 doi: 10.1590/S1677-5538.IBJU.2014.01.12 Long-term results of permanent memotherm urethral stent in the treatment of recurrent bulbar urethral
Clinical Study Comparison of Ultrasonic and Pneumatic Intracorporeal Lithotripsy Techniques during Percutaneous Nephrolithotomy
 The Scientific World Journal Volume 2013, Article ID 604361, 4 pages http://dx.doi.org/10.1155/2013/604361 Clinical Study Comparison of Ultrasonic and Pneumatic Intracorporeal Lithotripsy Techniques during
The Scientific World Journal Volume 2013, Article ID 604361, 4 pages http://dx.doi.org/10.1155/2013/604361 Clinical Study Comparison of Ultrasonic and Pneumatic Intracorporeal Lithotripsy Techniques during
Keywords: laparatomy, pyelolithotomy, laparoscopic.
 bü z ÇtÄ TÜà väx Large calculi within malpositioned and malformed kidneys, is percutaneous nephrolithotomy (PCNL) feasible? A Single Center s Experience over 10 Years. Awad Ka`abneh and Firas Al-Hammouri
bü z ÇtÄ TÜà väx Large calculi within malpositioned and malformed kidneys, is percutaneous nephrolithotomy (PCNL) feasible? A Single Center s Experience over 10 Years. Awad Ka`abneh and Firas Al-Hammouri
CASE REVIEW. Risk Factor Analysis and Management of Ureteral Double-J Stent Complications
 CASE REVIEW Risk Factor Analysis and Management of Ureteral Double-J Stent Complications Youness Ahallal, MD, Abdelhak Khallouk, PhD, Mohammed Jamal El Fassi, PhD, Moulay Hassan Farih, PhD Department of
CASE REVIEW Risk Factor Analysis and Management of Ureteral Double-J Stent Complications Youness Ahallal, MD, Abdelhak Khallouk, PhD, Mohammed Jamal El Fassi, PhD, Moulay Hassan Farih, PhD Department of
Treatment of Kidney and Ureteral Stones
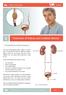 Patient Information English 3 Treatment of Kidney and Ureteral Stones The underlined terms are listed in the glossary. You have been diagnosed with a kidney or ureteral stone. This leaflet describes the
Patient Information English 3 Treatment of Kidney and Ureteral Stones The underlined terms are listed in the glossary. You have been diagnosed with a kidney or ureteral stone. This leaflet describes the
INJINTERNATIONAL. Foreign Bodies in the Urinary Bladder and Their Management: A Single-Centre Experience From North India.
 Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Official Journal of Korean Continence Society / Korean Society of Urological Research / The Korean Children s Continence and Enuresis Society / The Korean Association of Urogenital Tract Infection and
Surgical Treatment of LUTS in Men with BPE
 Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Patient Information English 35 Surgical Treatment of LUTS in Men with BPE The underlined terms are listed in the glossary. You have been diagnosed with benign prostatic enlargement (BPE) and your doctor
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Recanalisation of urethral strictures with new-generation temporary covered biocompatible metal endoprostheses
 Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
Introduction/Learning Objectives. Incontinence: Natural History. Course Outline 10/14/2016. Urinary Incontinence: Conservative Measures
 Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
The number following the procedure code is the TRICARE payment group. KIDNEY
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M JUNE 25, 1999 S POLICY CHAPTER 13 SECTION 9.1 ADDENDUM 1, SECTION 8 TRICARE-APPROVED AMBULATORY SURGERY S - URINARY SYSTEM The number following the procedure code
Fractured retained Double-J stents presenting as urethral foreign body
 Case Series Fractured retained Double-J stents presenting as urethral foreign body J. Sasi Kumar 1, P. Rahul Tej 1, A. Sri Balram 1, B. Srinivas 1, Y. Anil Reddy 1, B. Swapnil 1, N. Rama Murthy 1* 1 Mamata
Case Series Fractured retained Double-J stents presenting as urethral foreign body J. Sasi Kumar 1, P. Rahul Tej 1, A. Sri Balram 1, B. Srinivas 1, Y. Anil Reddy 1, B. Swapnil 1, N. Rama Murthy 1* 1 Mamata
Outcomes in a Large Series of Minipercs: Analysis of Consecutive 318 Patients
 JOURNAL OF ENDOUROLOGY Volume 00, Number 00, XXXXXX 2014 ª Mary Ann Liebert, Inc. Pp. --- --- DOI: 10.1089/end.2014.0290 Original Research Outcomes in a Large Series of Minipercs: Analysis of Consecutive
JOURNAL OF ENDOUROLOGY Volume 00, Number 00, XXXXXX 2014 ª Mary Ann Liebert, Inc. Pp. --- --- DOI: 10.1089/end.2014.0290 Original Research Outcomes in a Large Series of Minipercs: Analysis of Consecutive
Two cases of retained ureteral stents presenting with breakage and encrustations
 Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 10:208-212 Two cases of retained ureteral stents presenting with breakage and
Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 10:208-212 Two cases of retained ureteral stents presenting with breakage and
2017 Coding and Reimbursement Survival Guide
 2017 Coding and Reimbursement Survival Guide Chapter 20: Urology CPT Changes: Key Into Guideline Updates for Successful Procedure Coding in 2017 Plus: New coding tips also will help keep you on track.
2017 Coding and Reimbursement Survival Guide Chapter 20: Urology CPT Changes: Key Into Guideline Updates for Successful Procedure Coding in 2017 Plus: New coding tips also will help keep you on track.
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Hydronephrosis. What is hydronephrosis?
 What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
BIOPSY GUN. Delivered in sterile peel-open package. Device is made of Stainless Steel and PP material.
 BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
URINARY SYSTEM. MEDICAL TERMINOLOGY Chapter Six HIT #141. Anatomy
 URINARY SYSTEM MEDICAL TERMINOLOGY Chapter Six HIT #141 Anatomy Kidneys = bean-shaped organs, located on each side of the spinal column, removal of waste from the blood. Nephron = microscopic located in
URINARY SYSTEM MEDICAL TERMINOLOGY Chapter Six HIT #141 Anatomy Kidneys = bean-shaped organs, located on each side of the spinal column, removal of waste from the blood. Nephron = microscopic located in
urethral stricture recurrence after internal urethrotomy.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 9-, p-issn: 9-.Volume, Issue Ver. II (Nov. ), PP - www.iosrjournals.org Effects of Intralesional Triamcinalone injection following Internal
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 9-, p-issn: 9-.Volume, Issue Ver. II (Nov. ), PP - www.iosrjournals.org Effects of Intralesional Triamcinalone injection following Internal
Should we say farewell to ESWL?
 Should we say farewell to ESWL? HARRY WINKLER Director, section of Endo-urology Kidney stone center Dept. of Urology Sheba medical center Financial and Other Disclosures Off-label use of drugs, devices,
Should we say farewell to ESWL? HARRY WINKLER Director, section of Endo-urology Kidney stone center Dept. of Urology Sheba medical center Financial and Other Disclosures Off-label use of drugs, devices,
Rezūm procedure for the Prostate
 Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Rezūm procedure for the Prostate Mr Jas Kalsi Consultant Urological Surgeon This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm
Ureteroscopic and Extracorporeal Shock Wave Lithotripsy for Rather Large Renal Pelvis Calculi
 Endourology and Stone Disease Ureteroscopic and Extracorporeal Shock Wave Lithotripsy for Rather Large Renal Pelvis Calculi Kamyar Tavakkoli Tabasi, Mehri Baghban Haghighi Introduction: The aim of this
Endourology and Stone Disease Ureteroscopic and Extracorporeal Shock Wave Lithotripsy for Rather Large Renal Pelvis Calculi Kamyar Tavakkoli Tabasi, Mehri Baghban Haghighi Introduction: The aim of this
Can the complicated forgotten indwelling ureteric stents be lethal?
 International Urology and Nephrology (2005) 37:541 546 Ó Springer 2005 DOI 10.1007/s11255-004-4704-6 Can the complicated forgotten indwelling ureteric stents be lethal? V. Singh, A. Srinivastava, R. Kapoor
International Urology and Nephrology (2005) 37:541 546 Ó Springer 2005 DOI 10.1007/s11255-004-4704-6 Can the complicated forgotten indwelling ureteric stents be lethal? V. Singh, A. Srinivastava, R. Kapoor
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
A Review of Day Care Ureteroscopy of a Teaching Hospital in Malaysia
 A Review of Day Care Ureteroscopy of a Teaching Hospital in Malaysia K Y Chan, MRCSEd, M Z Zulkifli, MS, M J Nazri, MS, M O Rashid, MS Division of Urology, Department of Surgery, Hospital Universiti Kebangsaan
A Review of Day Care Ureteroscopy of a Teaching Hospital in Malaysia K Y Chan, MRCSEd, M Z Zulkifli, MS, M J Nazri, MS, M O Rashid, MS Division of Urology, Department of Surgery, Hospital Universiti Kebangsaan
HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION.
 IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT LASER AT YOUR SIDE IN YOUR HANDS is a high power holmium laser
IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT LASER AT YOUR SIDE IN YOUR HANDS is a high power holmium laser
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007)
 4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
4 th Year Urology Core Objectives Keith Rourke (Revised June 1, 2007) I. Genitourinary Trauma: 1. Goal: The student will be able to demonstrate a basic clinical approach to the management & diagnosis of
COMPRARISON OF TREATMENT METHODS FOR UROLITHIASIS IN CHILDREN WITH THE APPLICATION OF ESWL AND URSL METHODS
 Adam Haliński, Andrzej Haliński Provincial Hospital, Zielona Góra, Poland, Department of Paediatric Surgery and Paediatric Urology Specialized Medical Centre UROLOG, Zielona Góra, Poland COMPRARISON OF
Adam Haliński, Andrzej Haliński Provincial Hospital, Zielona Góra, Poland, Department of Paediatric Surgery and Paediatric Urology Specialized Medical Centre UROLOG, Zielona Góra, Poland COMPRARISON OF
Lasers in Urology. Laser Tissue Interaction, November 28 th, Qureshi, Muhammad Mohsin. Biomedical in vivo Opto-scopy Laboratory
 Laser Tissue Interaction, November 28 th, 2016 Lasers in Urology Qureshi, Muhammad Mohsin Gwangju Institute of Science and Technology Biomedical in vivo Opto-scopy Laboratory 2 Content Introduction to
Laser Tissue Interaction, November 28 th, 2016 Lasers in Urology Qureshi, Muhammad Mohsin Gwangju Institute of Science and Technology Biomedical in vivo Opto-scopy Laboratory 2 Content Introduction to
GENERAL GOALS & OBJECTIVES U-1. U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES
 GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
GENERAL GOALS & OBJECTIVES U-1 U-1 (PGY-2, 3) GENERAL GOALS and OBJECTIVES In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base by participating actively in conferences,
You have been booked for a. Flexible Cystoscopy. Under Local Anaesthetic
 You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
You have been booked for a Flexible Cystoscopy Under Local Anaesthetic 1 WHAT IS A FLEXIBLE CYSTOSCOPY A flexible cystoscopy is a test to examine the uretha (waterpipe) and bladder using a thin, lighted
Urinary lithiasis affects about 5% of the Western
 227 Tratamento cirúrgico da litíase vesical: revisão de literatura Review FABIO CESAR MIRANDA TORRICELLI 1 ; EDUARDO MAZZUCCHI 2 ; ALEXANDRE DANILOVIC 1 ; RAFAEL FERREIRA COELHO 1 ; MIGUEL SROUGI, TCBC-SP
227 Tratamento cirúrgico da litíase vesical: revisão de literatura Review FABIO CESAR MIRANDA TORRICELLI 1 ; EDUARDO MAZZUCCHI 2 ; ALEXANDRE DANILOVIC 1 ; RAFAEL FERREIRA COELHO 1 ; MIGUEL SROUGI, TCBC-SP
Renal Stone Disease 1
 Renal Stone Disease 1 What is a Stone? A Precipitation of secretions within an excretory organ Four sites: Renal, Prostatic, Biliary, Salivary Stone Formation needs Supersaturation of urine with solute
Renal Stone Disease 1 What is a Stone? A Precipitation of secretions within an excretory organ Four sites: Renal, Prostatic, Biliary, Salivary Stone Formation needs Supersaturation of urine with solute
Find Medical Solutions to Your Problems HYDRONEPHROSIS. (Distension of Renal Calyces & Pelvis)
 HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
HYDRONEPHROSIS (Distension of Renal Calyces & Pelvis) Hydronephrosis is the distension of the renal calyces and pelvis due to accumulation of the urine as a result of the obstruction to the outflow of
Goals & Objectives by Year in Training: U-1
 Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
Goals & Objectives by Year in Training: U-1 U-1 (PGY-2, 3) Resident Responsibilities, Goals and Objectives In addition to the goals listed for PGY-1, the U-1 resident will add to his/her knowledge base
for Virus Studies and Research WHETHER POST-URETEROSCOPY STENTING IS NECESSARY OR NOT?
 Al - Azhar Un. Center for virus studies and Research. Vol 1(1) Dec.2007 1 Al - Azhar University Center for Virus Studies and Research WHETHER POST-URETEROSCOPY STENTING IS NECESSARY OR NOT? Hashem Hafez,
Al - Azhar Un. Center for virus studies and Research. Vol 1(1) Dec.2007 1 Al - Azhar University Center for Virus Studies and Research WHETHER POST-URETEROSCOPY STENTING IS NECESSARY OR NOT? Hashem Hafez,
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Combined Transurethral Prostatectomy And Inguinal Hernioplasty
 ISPUB.COM The Internet Journal of Surgery Volume 20 Number 1 Combined Transurethral Prostatectomy And Inguinal Hernioplasty I Othman, A Abdel-Maguid Citation I Othman, A Abdel-Maguid. Combined Transurethral
ISPUB.COM The Internet Journal of Surgery Volume 20 Number 1 Combined Transurethral Prostatectomy And Inguinal Hernioplasty I Othman, A Abdel-Maguid Citation I Othman, A Abdel-Maguid. Combined Transurethral
PROGRESS IN ENDOSCOPIC. Olivier Traxer.
 PROGRESS IN ENDOSCOPIC TREATMENT OF UROLITHIASIS Olivier Traxer Tenon Hospital, Paris, France Université Pierre & Marie CURIE (PARIS VI) Université Pierre & Marie CURIE (PARIS VI) olivier.traxer@tnn.aphp.fr
PROGRESS IN ENDOSCOPIC TREATMENT OF UROLITHIASIS Olivier Traxer Tenon Hospital, Paris, France Université Pierre & Marie CURIE (PARIS VI) Université Pierre & Marie CURIE (PARIS VI) olivier.traxer@tnn.aphp.fr
Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011
 Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Urologic AMPUTATION OF PENIS Table 1 BIOPSY BLADDER Table 1 BIOPSY PENILE Table 1 BIOPSY URETERAL LESION Table 1 BLADDER DIVERTICULECTOMY
Indiana Regional Medical Center Procedures to Labs/Tests June 1, 2011 Urologic AMPUTATION OF PENIS Table 1 BIOPSY BLADDER Table 1 BIOPSY PENILE Table 1 BIOPSY URETERAL LESION Table 1 BLADDER DIVERTICULECTOMY
Multi-tract percutaneous nephrolithotomy combined with EMS lithotripsy for bilateral complex renal stones: our experience
 Liang et al. BMC Urology (2017) 17:15 DOI 10.1186/s12894-017-0205-7 RESEARCH ARTICLE Open Access Multi-tract percutaneous nephrolithotomy combined with EMS lithotripsy for bilateral complex renal stones:
Liang et al. BMC Urology (2017) 17:15 DOI 10.1186/s12894-017-0205-7 RESEARCH ARTICLE Open Access Multi-tract percutaneous nephrolithotomy combined with EMS lithotripsy for bilateral complex renal stones:
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (10), Page
 The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (10), Page 1778-1783 Comparison between the Efficacy of Transureteral Lithotripsy and Extracorporeal Shock Wave Lithotripsy in the Treatment
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (10), Page 1778-1783 Comparison between the Efficacy of Transureteral Lithotripsy and Extracorporeal Shock Wave Lithotripsy in the Treatment
SURGICAL PROCEDURES OPERATIONS ON THE UROGENITAL SYSTEM
 KIDNEYS AND PERINEPHRUM 1. No additional claim should be made for nephroscopy when done at the time of pyelolithotomy or nephrolithotomy. 2. In a routine surgical approach to the kidney and related procedures,
KIDNEYS AND PERINEPHRUM 1. No additional claim should be made for nephroscopy when done at the time of pyelolithotomy or nephrolithotomy. 2. In a routine surgical approach to the kidney and related procedures,
LOWER POLE STONE DR.NOOR ASHANI MD YUSOFF DEPT. OF UROLOGY HOSP.KUALA LUMPUR
 DR.NOOR ASHANI MD YUSOFF DEPT. OF UROLOGY HOSP.KUALA LUMPUR ! The appropriate treatment of lower pole calculi is controversial:! Shock wave lithotripsy! Retrograde ureteroscopy! Percutaneous lithotripsy
DR.NOOR ASHANI MD YUSOFF DEPT. OF UROLOGY HOSP.KUALA LUMPUR ! The appropriate treatment of lower pole calculi is controversial:! Shock wave lithotripsy! Retrograde ureteroscopy! Percutaneous lithotripsy
HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT
 IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT Manufactured by Asclepion Laser Technologies GmbH LASER AT
IN YOUR HANDS HOLMIUM:YAG LASER WHEN POWERFUL VERSATILITY INTEGRATES UNMATCHED PRECISION. Main Application Fields UROLOGY GENERAL SURGERY ENT Manufactured by Asclepion Laser Technologies GmbH LASER AT
ORIGINAL ARTICLES Endourology and Stone Diseases
 Urology Journal UNRC/IUA Vol. 3, No. 1, 15-19 Winter 2006 Printed in IRAN ORIGINAL ARTICLES Endourology and Stone Diseases Retrograde Flexible Ureteroscopic Approach for Pyelocaliceal Calculi Petrisor
Urology Journal UNRC/IUA Vol. 3, No. 1, 15-19 Winter 2006 Printed in IRAN ORIGINAL ARTICLES Endourology and Stone Diseases Retrograde Flexible Ureteroscopic Approach for Pyelocaliceal Calculi Petrisor
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use
 Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Holmium:YAG Laser for Treatment of Strictures of Vesicourethral Anastomosis after Radical Prostatectomy
 JOURNAL OF ENDOUROLOGY Volume 19, Number 4, May 2005 Mary Ann Liebert, Inc. Holmium:YAG Laser for Treatment of Strictures of Vesicourethral Anastomosis after Radical Prostatectomy BRUNOLF W. LAGERVELD,
JOURNAL OF ENDOUROLOGY Volume 19, Number 4, May 2005 Mary Ann Liebert, Inc. Holmium:YAG Laser for Treatment of Strictures of Vesicourethral Anastomosis after Radical Prostatectomy BRUNOLF W. LAGERVELD,
Forgotten JJ stent: A rare case report
 Ped Urol Case Rep 2015; 2(2):6-10 DOI: 10.14534/PUCR.201529390 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Forgotten
Ped Urol Case Rep 2015; 2(2):6-10 DOI: 10.14534/PUCR.201529390 PUCR Ped Urol Case Rep PEDIATRIC UROLOGY CASE REPORTS ISSN: 2148 2969 Journal homepage: http://www.pediatricurologycasereports.com Forgotten
Mrs Maya Harris Consultant Urologist INDWELLING CATHETERS: COMPLICATIONS AND SOLUTIONS
 Mrs Maya Harris Consultant Urologist INDWELLING CATHETERS: COMPLICATIONS AND SOLUTIONS AIMS OF PRESENTATION Discuss what can go wrong Discuss reducing risks Discuss managing troublesome problems and when
Mrs Maya Harris Consultant Urologist INDWELLING CATHETERS: COMPLICATIONS AND SOLUTIONS AIMS OF PRESENTATION Discuss what can go wrong Discuss reducing risks Discuss managing troublesome problems and when
ISSN X (Print) Original Research Article. *Corresponding author Avinash Barfa
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(5D):1706-1710 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(5D):1706-1710 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
