Clinical Study Clinical Study of the Relation between Mucosal Healing and Long-Term Outcomes in Ulcerative Colitis
|
|
|
- Virginia Lawrence
- 6 years ago
- Views:
Transcription
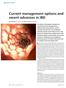
1 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2013, Article ID , 6 pages Clinical Study Clinical Study of the Relation between Mucosal Healing and Long-Term Outcomes in Ulcerative Colitis Kaoru Yokoyama, Kiyonori Kobayashi, Miyuki Mukae, Miwa Sada, and Wasaburo Koizumi Department of Gastroenterology, Kitasato University School of Medicine, Asamizodai, Minami, Sagamihara , Japan Correspondence should be addressed to Kaoru Yokoyama; kaoru.y@kitasato-u.ac.jp Received 11 February 2013; Accepted 27 February 2013 Academic Editor: Devendra Amre Copyright 2013 Kaoru Yokoyama et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Background and Objectives. Mucosal healing (MH) is considered an important therapeutic goal in ulcerative colitis (UC). We evaluate the severity of intestinal inflammation and clarify the relation between MH and long-term outcomes. Methods. The study group comprised 38 patients with UC in clinical remission on total colonoscopy who were followed up for at least 5 years. Clinical remission was defined as a Mayo score of 0 for both stool frequency and rectal bleeding. Colonoscopic findings were evaluated into 4 grades according to the Mayo endoscopic subscore (MES). Results. During clinical remission, the MES was 0 in only 24% of the patients, 1 in 40%, 2 in 26%, and 3 in 10%. Seventy-six percent of the patients thus had active disease on colonoscopy. After initial colonoscopy, the cumulative rate of remission maintenance was 100% in MES 0, 1 in 93%, 2 in 70%, and 3 in 50% at 6 months and 78%, 40%, 10%, and 0%, respectively, at 5 years (P < 0.001). Conclusion. Many patients with UC in clinical remission have active lesions. Patients with a higher MES have a higher rate of recurrence. To improve long-term outcomes, an MES of 0 should be the treatment goal. 1. Introduction The treatment response and prognosis of inflammatory bowel disease (IBD) have been evaluated on the basis of clinical remission, dose reduction of steroids, avoidance of surgery, and other factors. However, since the advent of potent drugs such as antitumor necrosis factor-α monoclonal antibody preparations, treatment response has been assessed on the basis of mucosal healing as evaluated on colonoscopy [1 3]. However, standard criteria for the evaluation of disease severity and definitions of mucosal healing on colonoscopy are currently unavailable [4]. Moreover, long-term studies examining whether mucosal healing actually contributes to remission maintenance in IBD are scant. We performed colonoscopy in patients with ulcerative colitis (UC) in clinical remission to evaluate the presence or absence of intestinal inflammation and to retrospectively analyze the relation between mucosal healing and long-term outcomes during 5 years of followup. 2. Methods 2.1. Patients. Among 46 patients with ulcerative colitis in clinical remission who underwent colonoscopy in our hospital from January 2005 through December 2006, we studied 38 patients in whom the severity of intestinal inflammation was evaluated on total endoscopy; all patients were followed up foratleast5years.eightpatientswhoreceivedcorticosteroids at the time of colonoscopy were excluded from the study because steroids can mask clinical signs and symptoms. As for the demographic characteristics of the patients, there were 18 males and 20 females. The mean age at the onset of UC was 38.8±13.0 years (range, 16 to 73). The mean disease duration at colonoscopy was 15.8 ± 9.0 years (range, 1 to 37). The disease type was flare-ups and remission in 37 patients and initial attacks in 1(Table 1). Disease extent at the onset of UC was pancolitis in 11 patients (29%), left-sided colitis in 11 (29%), proctitis in 11 (29%), and unknown in 5 patients (13%) who were initially treated at other hospitals. Overall,
2 2 Gastroenterology Research and Practice Table 1: Demographic characteristics of patients. No. of patients 38 Sex Male 18 (47%) Female 20 (53%) Age atdisease onset (range) 38.8 ± 13.0 years (16 73) Disease duration (range) 15.8 ± 9.0 years (1 37) Disease type Flare-ups and remission 37 (97%) Initial attacks 1(2%) Lesion extent at disease onset Pancolitis 11 (29%) Left-sided colitis 11 (29%) Proctitis 11 (29%) Unknown 5 (13%) History of treatment in hospital Yes 13 (34%) No 25 (66%) Drug therapy at colonoscopy Present 36 (95%) 5-Aminosalicylic acid 34 (94%) Immunomodulators 1(3%) Local therapy 7 (19%) None 2(5%) 13 patients (34%) had previously received treatment during hospitalization. At the time of colonoscopy, 36 patients (95%) were receiving drug therapy, which included 5-aminosalicylic acid (5-ASA) in 34 patients (94%), immunomodulators in 1 (3%), and local therapy such as 5-ASA and steroid suppositories and enemas in 7 (19%) (some overlap) Evaluation of UC Activity. The Mayo score [5] was used to evaluate UC activity. The Mayo score consists of 4 components: stool frequency, rectal bleeding, endoscopy findings, and physician s global assessment. Each component is assigned a score of 0 to 3; the total score ranges from 0 to 12. The higher the score, the higher is the disease severity. In the present study, clinical remission was defined as a score of 0 for both stool frequency and rectal bleeding. Flare-ups were defined as the need for additional drugs or modification of the treatment regimen because of exacerbation of clinical symptoms Colonoscopic Examination and Evaluation of Intestinal Inflammation. Before colonoscopic examination, all patients were provided with a detailed explanation of the examination objectives and gave written informed consent. An oral polyethylene glycol lavage solution was used for bowel preparation. An anticholinergic agent (scopolamine butylbromide 10mg)orglucagon(1mg)wasgivenintramuscularlyaspremedication. A small-bore, high-magnification colonoscope (PCF-Q240ZI, Olympus Co. Ltd., Tokyo, Japan) was used. All examinations were performed by 3 endoscopists specialized in the diagnosis and treatment of IBD who each had at least 15 years of experience in colonoscopy. The Mayo endoscopic subscore (MES) was used to evaluate the severity of intestinal inflammation on colonoscopy [5] as follows: MES 0, normal or inactive disease; MES 1, mild disease (erythema, decreased vascular pattern, and mild friability); MES 2, moderate disease (marked erythema, absent vascular pattern, friability, and erosions); and MES 3, severe disease (spontaneous bleeding and ulcerations) (Figures 1(a) to 1(d)). The entire colon was observed by white-light colonoscopy, and sites with the most severe inflammation were evaluated Study Variables. The severity of intestinal inflammation was evaluated on colonoscopy during clinical remission of disease. The relation between the severity of colonoscopic findings and the maintenance of clinical remission was then studied up to 5 years after initial colonoscopy. The study was approved by the ethics review committee of our hospital Statistical Analysis. Data are presented as means ± standard deviation. For statistical analysis, the chi-square test and Fisher s exact test were used to compare incidence rates. One-way factorial analysis of variance and Scheffe s test were used to compare parametric variables between multiple unpaired groups. The Kruskal-Wallis test was used to compare nonparametric variables among multiple groups. Cumulative rates of remission maintenance were calculated using the Kaplan-Meier method. Log-rank tests (Peto & Peto modification) were used to determine whether differences among multiple groups were statistically significant. P values of less than 0.05 were considered to indicate statistical significance. Statistical analyses were carried out using StatMate IV software, version 4.01 for Windows (ATMS, Tokyo, Japan). 3. Results 3.1. Mucosal Healing Rates. TheMESatinitialcolonoscopy during clinical remission was 0 in 9 patients (group A), 1 in 15 (group B), 2 in 10 (group C), and 3 in 4 (group D) (Table 2). Active intestinal lesions were found in 29 patients in clinical remission (76%), despite no diarrhea or bloody stools. Demographic characteristics such as disease duration and disease extent did not differ significantly among the 4 groups. Remission induction regimens at the time of flareups before the most recent colonoscopic examination and the duration of remission maintenance up to the time of colonoscopy also did not differ among the 4 groups. There was also no difference in drug therapy at the time of initial colonoscopy Cumulative Rates of Remission Maintenance after Colonoscopy. The cumulative rate of remission maintenance 6 months after initial colonoscopy as evaluated by the Kaplan-Meier method was 100% in group A, 93% in group B, 70% in group C, and 50% in group D. At 2 years
3 Gastroenterology Research and Practice 3 (a) (b) (c) (d) Figure 1: (a) An endoscopic image of the colonic mucosa, a Mayo endoscopic subscore of 0. The mucosal has a visible vascular pattern, and scattered white ulcer scars are evident. (b) An endoscopic image of the colonic mucosa, a Mayo endoscopic subscore of 1. The vascular pattern of the mucosa is decreased, with mild erythema. (c) An endoscopic image of the colonic mucosa, a Mayo endoscopic subscore of 2. The vascular pattern of the mucosa is decreased, with marked erythema and multiple erosions. (d) An endoscopic image of the colonic mucosa, a Mayo endoscopic subscore of 3. The mucosa shows marked erythema and ulcers. the cumulative rates of remission maintenance were 78%, 67%, 20%, and 0%, respectively, and at 5 years the rates were 78%, 40%, 10%, and 0%, respectively. The cumulative rate of remission maintenance differed significantly among the 4 groups (multiple log-rank test (Peto & Peto modification), P < 0.001) (Figure 2). Regimens during followup after colonoscopy did not differ among the 4 groups (Table 2). Adherence to drug therapy was good. At the time of flareups, 1 patient in group B and 1 in group D were admitted to receive treatment. Cumulative rate of remission maintenance (%) Followup (month) 4. Discussion UC is a chronic IBD that develops in relatively young adults and requires long-term, continuous drug therapy to stabilize disease. However, a substantial number of patients are unable to strictly comply with drug therapy during followup, increasing the risk of relapse [6]. In fact, some patients request dose reduction or treatment withdrawal soon aftertheresolutionofsymptomssuchasbloodystoolsand abdominal pain. A considerable number of patients thus do not take medication as directed. Not only patents, but Log-rank test P < Group A: endoscopy subscore of 0 Group B: endoscopy subscore of 1 Group C: endoscopy subscore of 2 Group D: endoscopy subscore of 3 Figure 2: Cumulative rates of remission maintenance according to Mayo endoscopic subscore. also some physicians instruct patients to decrease the dose or discontinue drug therapy soon after the resolution of
4 4 Gastroenterology Research and Practice Table 2: Treatment regimens according to the Mayo endoscopic subscore. Group A B C D Endoscopic subscore No. of patients (%) 9 (24%) 15 (40%) 10 (26%) 4 (10%) History of treatment in hospital Yes 4 (44%) 5 (33%) 3 (30%) 1 (25%) No 5 (56%) 10 (77%) 7 (70%) 3 (75%) Remission induction therapy before colonoscopy Present 9 (100%) 15 (100%) 10 (100%) 4 (100%) 5-Aminosalicylic acid 9 (100%) 15 (100%) 10 (100%) 3 (75%) Corticosteroid 3 (33%) 4 (27%) 2 (20%) 1 (25%) Local therapy 5 (56%) 7 (47%) 6 (60%) 3 (75%) Duration of remission maintenance before colonoscopy (months) 36.1 ± ± ± ± 9.8 Drug therapy at colonoscopy Present 8 (89%) 14 (93%) 10 (100%) 4 (100%) 5-Aminosalicylic acid 8 (89%) 13 (87%) 10 (100%) 3 (75%) Immunomodulators 1 (11%) Local therapy 1 (11%) 2 (14%) 3 (30%) 1 (25%) None 1 (11%) 1 (7%) Treatment after colonoscopy Present 8 (89%) 11 (73%) 10 (100%) 4 (100%) 5-Aminosalicylic acid 8 (89%) 10 (77%) 10 (100%) 3 (75%) Immunomodulators Local therapy 1 (7%) 2 (20%) 1 (25%) None 1 (11%) 4 (27%) symptoms, often leading to relapse. In Japan, the number of patients with UC has been increasing annually. We speculate that increasing numbers of patients with UC are being treated by not only IBD specialists, but also general internists. Even if patients with active UC are initially treated by IBD specialists, maintenance therapy after remission induction is probably often entrusted to general internists. Colonoscopy is essential for an in-depth assessment of intestinal inflammation in UC. Recent studies have reported that narrow band imaging (NBI) and magnifying endoscopy in addition to white-light endoscopy are useful for detailed assessment of the mucosa and facilitate evaluation of the severity of intestinal inflammation. These techniques are also useful for predicting outcomes, including the risk of recurrence [7, 8]. However, NBI and magnifying endoscopy can be routinely performed in only a limited number of hospitals. In general hospitals, the severity of intestinal inflammation is evaluated, and the treatment policy is decided on the basis of white-light colonoscopic findings. We therefore studied variables that can be evaluated on white-light colonoscopy. Moreover, the inclusion of many variables in the colonoscopic evaluation of the severity of intestinal inflammation in UC leads to complexity, as well as considerable variation in the results of evaluation among endoscopists [9]. In the present study, we therefore used the MES [5], a relatively straightforward evaluation system that has been widely used in clinical trials of new drugs and other clinical studies in patients with UC. To ensure that lesions were accurately diagnosed, the following precautions were taken. Because small lesions are difficult to diagnosis after inadequate intestinal lavage, all patients received pretreatment with oral intestinal lavage solution (polyethylene glycol). The same model of colonoscope was used in all patients to examine and evaluate the entire colorectum. Colonoscopy was performed byspecialistsofibdwhohadatleast15yearsexperience in colonoscopy. In addition, colonoscopic findings were evaluatedbyendoscopistswhowereblindedtothepatients outcomes. Ourresultsshowedthataboutthree-fourthsofallpatients continuedtohaveactiveintestinalinflammationevenduring clinical remission of UC. All patients received drug therapy to induce remission at the time of flare-ups before the most recent colonoscopic examination. The treatment regimens did not differ among the 4 groups. The duration of clinical remission before colonoscopy also did not differ significantly among the 4 groups. In addition, therapy being received by patients at the time of colonoscopy was similar in the 4 groups. However, the 4 groups had different severities of intestinal inflammation on colonoscopy, ranging from an MES of 0 to 3. Intestinal lesions thus did not resolve in many
5 Gastroenterology Research and Practice 5 patients, despite the clinical remission of disease. Our results support the importance of evaluating the degree of mucosal healing on colonoscopy. Frequent divergence between clinical remission and the remission of intestinal lesions in UC has also been confirmed in previous prospective studies [10, 11]. Many previous studies evaluating the effects of various types of treatment on remission maintenance in UC were relatively short (about 1 year) [10, 11]. In contrast, we analyzed long-term outcomes over the course of 5 years by assessing the severity of intestinal lesions on colonoscopy. Relapse occurred within 5 years in nearly all patients who were in clinical remission, but had erosions and ulcers with an MES of2or3oncolonoscopy.evenamongpatientswithanmes of 1 who had erythema and decreased vascular pattern on colonoscopy, the rate of remission maintenance at 5 years was only 40%. In contrast, the rate of long-term remission maintenance was 78% in patients whose condition improved to an MES of 0 with no evidence of inflammation on colonoscopy. The rate of remission maintenance in UC may be related to the remission maintenance regimens given during followup and adherence to drug therapy [6]. In our study, the regimens given after colonoscopy did not differ from those used at the time of colonoscopy, and adherence to treatment was good. Because patients with active lesions did not have symptoms atthetimeofcolonoscopy,somepatientsdidnotperceive theneedfor,oragreetoreceive,moreaggressivetherapy, but adherence with the treatment regimen being used was good.from2005through2006,wheninitialcolonoscopywas performed in this study, treatment with antitumor necrosis factor-α monoclonal antibody preparations was not covered by the National Health Insurance in Japan. In the latter half of 2006, treatment with azathioprine, an immunomodulator, finally became eligible for reimbursement by the National Health Insurance. Owing to these factors, patients continued to receive generally the same regimens during followup as those received at the time of initial colonoscopy. The differences in the remission maintenance rates among the 4 groups are therefore most likely attributed to differences in the severity of intestinal inflammation at the time of colonoscopy and not to differences in or modifications of treatment regimens. Therefore, we believe that the treatment goal should be an MES of 0. However, many previous clinical studies defined mucosal healing as an MES of 0 or 1 [10, 11]. One study evaluating the effectiveness of mesalazine for remission maintenance reported no difference in the rate of relapse at 1 year between patients with an MES of 0 and those with an MES of 1 [10]. In a prospective study assessing the effectiveness of infliximab for remission maintenance, the symptomatic remission rate after 54 weeks was 73% in patients with an MES of 0 on colonoscopy performed after remission induction and 47% in those with an MES of 1, indicating that more than half of the latter patients had relapse. However, among patients who had clinical remission 8 weeks after treatment with infliximab, there was no difference in clinical outcomes (including colectomy) at 54 weeks between patients with an MES of 0 and those with an MES of 1 at 8 weeks [11]. In the ACT 1 trial [1], the rate of steroid-free remission after 54 weeks was 63%inpatientswithanMESof0oncolonoscopyafter8 weeks of treatment, as compared with only 46% in patients with an MES of 1. Whether a difference between an MES of 0 and an MES of 1 influences clinical outcomes thus remains controversial. In addition, these findings were obtained from studieswithrelativelyshortfollow-upperiodsofabout1 year. In our study, the cumulative remission maintenance rate 6 months after colonoscopy was similar in group A (MES 0, 100%) and in group B (MES 1, 93%). However, the cumulative remission maintenance rate was 78% in group Aand67%ingroupBat2yearsand78%ingroupAand 40% in group B at 5 years, indicating that the cumulative remission maintenance rate decreased with time in patients who had an MES of 1; moreover, the divergence between group A and group B increased. These findings also support the notion that an MES of 0 should be the goal of treatment. Indeed,itmaybedifficulttoaccuratelyassesscolonoscopic findings and in particular to distinguish between an MES of 1, indicating mild disease, and an MES of 0, indicating normal or inactive disease [9]. Efforts should be made, including adequate pretreatment, to ensure that evaluations can be performed as accurately as possible. Because our study was conducted in a single hospital, differences in the conditions of endoscopic examination and in the assessment of endoscopic findings were most likely minimal. However, further multicenter, prospective studies of larger numbers of patients are needed to confirm our findings and to establish the clinical positioning of an MES of 0 and an MES of 1. As mentioned above, even patients with UC in clinical remission who have active lesions on colonoscopy have a high rate of relapse during followup. To achieve remission maintenance, the goal of therapy should be to downgrade inflammation in patients who have intestinal inflammation. Physicians should recognize that intestinal inflammation accompanied by findings such as erythema and erosions persists after the resolution of symptoms in an appreciable number of patients. Education of patients is also important. Patients should be advised not to stop drug therapy on their own initiative, even if clinical symptoms resolve. Substantial progress has been made in drug therapy for UC. Antitumor necrosis factor-α monoclonal antibody preparations, potent immunosuppressants such as tacrolimus and cyclosporine, and new treatments such as cytapheresis are now available to complement conventional preparations such as 5-ASA and steroids. Consequently, mucosal healing can now be achieved in increasing numbers of patients. Immunomodulators such as azathioprine and 6- mercaptopurine are widely known to be effective as remission maintenance therapy. Further prospective studies are needed to examine the relation between mucosal healing and longterm remission maintenance for each of these newer treatments. We evaluated the effects of mucosal healing on longterm outcomes in patients with UC. However, our study had several limitations: it was conducted in a single center and had a small sample size. Further multicenter prospective studies in larger numbers of patients are needed to confirm our findings and to further delineate the clinical significance of mucosal healing in UC.
6 6 Gastroenterology Research and Practice References [1] P. Rutgeerts, W. J. Sandborn, B. G. Feagan et al., Infliximab for induction and maintenance therapy for ulcerative colitis, The New England Journal of Medicine, vol.353,no.23,pp , [2] J. F. Colombel, W. J. Sandborn, W. Reinisch et al., Infliximab, azathioprine, or combination therapy for Crohn s disease, The New England Journal of Medicine,vol.362,no.15,pp , [3] P.Rutgeerts,G.VanAssche,W.J.Sandbornetal., Adalimumab induces and maintains mucosal healing in patients with Crohn s disease: data from the EXTEND trial, Gastroenterology, vol. 142, no. 5, pp , [4] M. F. Neurath and S. P. Travis, Mucosal healing in inflammatory bowel diseases: a systematic review, Gut, vol. 61, no. 10, pp , [5] K.W.Schroeder,W.J.Tremaine,andD.M.Ilstrup, Coatedoral 5-aminosalicylic acid therapy for mildly to moderately active ulcerative colitis: a randomized study, The New England Journal of Medicine,vol.317,no.26,pp ,1987. [6] S. Kane, D. Huo, J. Aikens, and S. Hanauer, Medication nonadherence and the outcomes of patients with quiescent ulcerative colitis, American Journal of Medicine, vol.114,no.1, pp.39 43,2003. [7] T.Kudo,T.Matsumoto,M.Esaki,T.Yao,andM.Iida, Mucosal vascular pattern in ulcerative colitis: observations using narrow band imaging colonoscopy with special reference to histologic inflammation, International Journal of Colorectal Disease, vol. 24,no.5,pp ,2009. [8] M. Fujiya, Y. Saitoh, M. Nomura et al., Minute findings by magnifying colonoscopy are useful for the evaluation of ulcerative colitis., Gastrointestinal Endoscopy, vol. 56, no. 4, pp , [9]K.T.Thia,E.V.LoftusJr.,D.S.Pardietal., Measurement of disease activity in ulcerative colitis: interobserver agreement and predictors of severity, Inflammatory Bowel Diseases,vol.17, no. 6, pp , [10] G. Meucci, R. Fasoli, S. Saibeni et al., Prognostic significance of endoscopic remission in patients with active ulcerative colitis treated with oral and topical mesalazine: a prospective, multicenter study, Inflammatory Bowel Diseases, vol.18,no.6, pp , [11] J. F. Colombel, P. Rutgeerts, W. Reinisch et al., Early mucosal healing with infliximab is associated with improved long-term clinical outcomes in ulcerative colitis, Gastroenterology, vol. 141, no. 4, pp , 2011.
Moderately to severely active ulcerative colitis
 Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
Mucosal healing: does it really matter?
 Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Definitions. Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency)
 CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
Narrow band imaging efficiency in evaluation of mucosal healing/ relapse of ulcerative colitis
 Original article Narrow band imaging efficiency in evaluation of mucosal healing/ relapse of ulcerative colitis Authors Seiko Sasanuma 1, Kazuo Ohtsuka 1, 2, Shin-ei Kudo 1, Noriyuki Ogata 1, Yasuharu
Original article Narrow band imaging efficiency in evaluation of mucosal healing/ relapse of ulcerative colitis Authors Seiko Sasanuma 1, Kazuo Ohtsuka 1, 2, Shin-ei Kudo 1, Noriyuki Ogata 1, Yasuharu
Clinical Study Tacrolimus for Remission Induction and Maintenance Therapy in Patients with Ulcerative Colitis: A Retrospective Evaluation Study
 Gastroenterology Research and Practice Volume 2016, Article ID 5956316, 6 pages http://dx.doi.org/10.1155/2016/5956316 Clinical Study Tacrolimus for Remission Induction and Maintenance Therapy in Patients
Gastroenterology Research and Practice Volume 2016, Article ID 5956316, 6 pages http://dx.doi.org/10.1155/2016/5956316 Clinical Study Tacrolimus for Remission Induction and Maintenance Therapy in Patients
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 20 October 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 20 October 2010 MEZAVANT LP 1200 mg, prolonged-release gastro-resistant tablets B/60 (CIP code: 378 689-2) Applicant
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 20 October 2010 MEZAVANT LP 1200 mg, prolonged-release gastro-resistant tablets B/60 (CIP code: 378 689-2) Applicant
Title: Author: Journal:
 IMPORTANT COPYRIGHT NOTICE: This electronic article is provided to you by courtesy of Ferring Pharmaceuticals. The document is provided for personal usage only. Further reproduction and/or distribution
IMPORTANT COPYRIGHT NOTICE: This electronic article is provided to you by courtesy of Ferring Pharmaceuticals. The document is provided for personal usage only. Further reproduction and/or distribution
Evaluation of the severity of ulcerative colitis using endoscopic dual red imaging targeting deep vessels
 Evaluation of the severity of ulcerative colitis using endoscopic dual red imaging targeting deep vessels Authors Makoto Naganuma 1, 2, Naohisa Yahagi 3,RiekoBessho 1, Keiko Ohno 1, Mari Arai 1, Makoto
Evaluation of the severity of ulcerative colitis using endoscopic dual red imaging targeting deep vessels Authors Makoto Naganuma 1, 2, Naohisa Yahagi 3,RiekoBessho 1, Keiko Ohno 1, Mari Arai 1, Makoto
As clinicians we would all agree that the goal for our
 CURRENT CONTROVERSIES: PRO, CON, AND BALANCE Controversies in Mucosal Healing in Ulcerative Colitis Sunanda Kane, MD,* Frances Lu, MD, Asher Kornbluth, MD, Dahlia Awais, MD, and Peter D.R. Higgins, MD,
CURRENT CONTROVERSIES: PRO, CON, AND BALANCE Controversies in Mucosal Healing in Ulcerative Colitis Sunanda Kane, MD,* Frances Lu, MD, Asher Kornbluth, MD, Dahlia Awais, MD, and Peter D.R. Higgins, MD,
Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort
 Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Ali Keshavarzian MD Rush University Medical Center
 Treatment: Step Up or Top Down? Ali Keshavarzian MD Rush University Medical Center Questions What medication should IBD be treated with? Can we predict which patients with IBD are high risk? Is starting
Treatment: Step Up or Top Down? Ali Keshavarzian MD Rush University Medical Center Questions What medication should IBD be treated with? Can we predict which patients with IBD are high risk? Is starting
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND. Fabrizio Parente
 NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
Indications for use of Infliximab
 Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Infliximab (Remicade) for paediatric ulcerative colitis - second line
 Infliximab (Remicade) for paediatric ulcerative colitis - second line September 2011 This technology summary is based on information available at the time of research and a limited literature search. It
Infliximab (Remicade) for paediatric ulcerative colitis - second line September 2011 This technology summary is based on information available at the time of research and a limited literature search. It
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Biologics in IBD. Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College
 Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
Endoscopy in Inflammatory Bowel Disease DR. REENA KHANNA
 Endoscopy in Inflammatory Bowel Disease DR. REENA KHANNA ASSISTANT PROFESSOR, UNIVERSITY OF WESTERN ONTARIO Background Clinical trials in ulcerative colitis and Crohn s disease require validated instruments
Endoscopy in Inflammatory Bowel Disease DR. REENA KHANNA ASSISTANT PROFESSOR, UNIVERSITY OF WESTERN ONTARIO Background Clinical trials in ulcerative colitis and Crohn s disease require validated instruments
Update on Biologics in Ulcerative Colitis. Scott Plevy, MD University of North Carolina Chapel Hill, NC
 Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
ENTYVIO (VEDOLIZUMAB)
 ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Community Plan Medical Benefit Drug Policy Policy Number: CS2017D0053F Effective Date: July 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Community Plan Medical Benefit Drug Policy Policy Number: CS2017D0053F Effective Date: July 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
Controversies in IBD: Resolving clinical dilemmas using Cochrane reviews
 Controversies in IBD: Resolving clinical dilemmas using Cochrane reviews DR. NILESH CHANDE COORDINATING EDITOR, IBD REVIEW GROUP; UNIVERSITY OF WESTERN ONTARIO, LONDON, ON CANADA An international organisation
Controversies in IBD: Resolving clinical dilemmas using Cochrane reviews DR. NILESH CHANDE COORDINATING EDITOR, IBD REVIEW GROUP; UNIVERSITY OF WESTERN ONTARIO, LONDON, ON CANADA An international organisation
Doncaster & Bassetlaw Medicines Formulary
 Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
PEDIATRIC INFLAMMATORY BOWEL DISEASE
 PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
Randomised clinical trial: delayed-release oral mesalazine 4.8 g day vs. 2.4 g day in endoscopic mucosal healing ASCEND I and II combined analysis
 Alimentary Pharmacology and Therapeutics Randomised clinical trial: delayed-release oral mesalazine 4.8 g day vs. 2.4 g day in endoscopic mucosal healing ASCEND I and II combined analysis G. R. Lichtenstein*,
Alimentary Pharmacology and Therapeutics Randomised clinical trial: delayed-release oral mesalazine 4.8 g day vs. 2.4 g day in endoscopic mucosal healing ASCEND I and II combined analysis G. R. Lichtenstein*,
Does Fecal Microbiota Transplantation Cause Clinical Remission in Patients with Ulcerative Colitis?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2017 Does Fecal Microbiota Transplantation
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2017 Does Fecal Microbiota Transplantation
Guideline Ulcerative colitis: management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Ulcerative colitis: management Draft for consultation, December 0 This guideline covers the care and treatment of adults, children and young
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Ulcerative colitis: management Draft for consultation, December 0 This guideline covers the care and treatment of adults, children and young
Achieving Success in Ulcerative Colitis: the Role of Infliximab
 Achieving Success in Ulcerative Colitis: the Role of Infliximab Dr Gill Watermeyer IBD clinic Groote Schuur Hospital 17 th August 2012 Inflammatory Bowel Disease Crohn s disease and ulcerative colitis
Achieving Success in Ulcerative Colitis: the Role of Infliximab Dr Gill Watermeyer IBD clinic Groote Schuur Hospital 17 th August 2012 Inflammatory Bowel Disease Crohn s disease and ulcerative colitis
Early Mucosal Healing With Infliximab Is Associated With Improved Longterm Clinical Outcomes in Ulcerative Colitis
 GASTROENTEROLOGY 2011;141:1194 1201 Early Mucosal Healing With Infliximab Is Associated With Improved Longterm Clinical Outcomes in Ulcerative Colitis JEAN FRÉDÉRIC COLOMBEL,* PAUL RUTGEERTS, WALTER REINISCH,
GASTROENTEROLOGY 2011;141:1194 1201 Early Mucosal Healing With Infliximab Is Associated With Improved Longterm Clinical Outcomes in Ulcerative Colitis JEAN FRÉDÉRIC COLOMBEL,* PAUL RUTGEERTS, WALTER REINISCH,
Mucosal Healing in Crohn s Disease. Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium
 Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
Disclosures. What Do I Do When Anti-TNF Therapy Is Not Working Anymore? Fadi Hamid, M.D. Saint Luke s GI Specialists
 What Do I Do When Anti-TNF Therapy Is Not Working Anymore? Fadi Hamid, M.D. Saint Luke s GI Specialists Disclosures No financial relationships to disclose. 1 Learning Objectives Case 24M with ileocolonic
What Do I Do When Anti-TNF Therapy Is Not Working Anymore? Fadi Hamid, M.D. Saint Luke s GI Specialists Disclosures No financial relationships to disclose. 1 Learning Objectives Case 24M with ileocolonic
September 12, 2015 Millie D. Long MD, MPH, FACG
 Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Anti tumor necrosis factor (TNF) agents have
 Achieving Clinical Response and Remission in Moderate-to-Severe Ulcerative Colitis With Golimumab Sandborn WJ, Feagan BG, Marano C, et al; PURSUIT-SC Study Group. Subcutaneous golimumab induces clinical
Achieving Clinical Response and Remission in Moderate-to-Severe Ulcerative Colitis With Golimumab Sandborn WJ, Feagan BG, Marano C, et al; PURSUIT-SC Study Group. Subcutaneous golimumab induces clinical
Clinical Policy: Vedolizumab (Entyvio) Reference Number: CP.PHAR.265
 Clinical Policy: (Entyvio) Reference Number: CP.PHAR.265 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
Clinical Policy: (Entyvio) Reference Number: CP.PHAR.265 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
CCFA. Crohns Disease vs UC: What is the best treatment for me? November
 CCFA Crohns Disease vs UC: What is the best treatment for me? November 8 2009 Ellen J. Scherl,, MD, FACP,AGAF Roberts Inflammatory Bowel Disease Center Weill Medical College Cornell University New York
CCFA Crohns Disease vs UC: What is the best treatment for me? November 8 2009 Ellen J. Scherl,, MD, FACP,AGAF Roberts Inflammatory Bowel Disease Center Weill Medical College Cornell University New York
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy
 Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
IBD Updates. Themes in IBD IBD management journey. New tools for therapeutic monitoring. First-line treatment in IBD
 IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
INFLAMMATORY BOWEL DISEASE
 1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
The Spectrum of IBD. Inflammatory Bowel Disease. Symptoms. Epidemiology. Tests for IBD. CD or UC? Inflamatory Bowel Disease. Fernando Vega, M.D.
 The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
ENTYVIO (VEDOLIZUMAB)
 ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 285.8 T2 Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Oxford Clinical Policy Policy Number: PHARMACY 285.8 T2 Effective Date: November 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
National Institute for Health and Care Excellence
 National Institute for Health and Care Excellence 4-year surveillance (2017) Ulcerative colitis: management (2013) NICE guideline CG166 Appendix A.2: Summary of new evidence from surveillance Patient information
National Institute for Health and Care Excellence 4-year surveillance (2017) Ulcerative colitis: management (2013) NICE guideline CG166 Appendix A.2: Summary of new evidence from surveillance Patient information
Op#mizing)Management)in)IBD:) Mucosal)Healing)
 Op#mizing)Management)in)IBD:) Mucosal)Healing) Vipul&Jairath&MD&PhD& Associate&Professor&of&Medicine,&Epidemiology&and& Biosta=s=cs& Western&University&&& Division&of&Gastroenterology,&& London&Health&Sciences&Network&
Op#mizing)Management)in)IBD:) Mucosal)Healing) Vipul&Jairath&MD&PhD& Associate&Professor&of&Medicine,&Epidemiology&and& Biosta=s=cs& Western&University&&& Division&of&Gastroenterology,&& London&Health&Sciences&Network&
ENTYVIO (VEDOLIZUMAB)
 ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Commercial Medical Benefit Drug Policy Policy Number: 2017D0053F Effective Date: July 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Commercial Medical Benefit Drug Policy Policy Number: 2017D0053F Effective Date: July 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
Once Daily Dosing for Induction and Maintenance of Remission in Ulcerative Colitis
 Once Daily Dosing for Induction and Maintenance of Remission in Ulcerative Colitis John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University JKM 2014 Svartz N. Acta Med Scand
Once Daily Dosing for Induction and Maintenance of Remission in Ulcerative Colitis John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University JKM 2014 Svartz N. Acta Med Scand
Mucosal Healing in Ulcerative Colitis When Zero is Better
 Journal of Crohn's and Colitis, 2016, 20 25 doi:10.1093/ecco-jcc/jjv180 Advance Access publication October 5, 2015 Original Article Original Article Mucosal Healing in Ulcerative Colitis When Zero is Better
Journal of Crohn's and Colitis, 2016, 20 25 doi:10.1093/ecco-jcc/jjv180 Advance Access publication October 5, 2015 Original Article Original Article Mucosal Healing in Ulcerative Colitis When Zero is Better
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 1-5 Effectiveness of adalimumab for ambulatory ulcerative colitis patients after failure of infliximab treatment: a first real-life experience in
ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 1-5 Effectiveness of adalimumab for ambulatory ulcerative colitis patients after failure of infliximab treatment: a first real-life experience in
Until recently, treatment of active ulcerative colitis
 ORIGINAL ARTICLE Prognostic Significance of Endoscopic Remission in Patients with Active Ulcerative Colitis Treated with Oral and Topical Mesalazine: A Prospective, Multicenter Study Gianmichele Meucci,
ORIGINAL ARTICLE Prognostic Significance of Endoscopic Remission in Patients with Active Ulcerative Colitis Treated with Oral and Topical Mesalazine: A Prospective, Multicenter Study Gianmichele Meucci,
DENOMINATOR: All patients aged 18 and older with a diagnosis of inflammatory bowel disease
 Measure #270: Inflammatory Bowel Disease (IBD): Preventive Care: Corticosteroid Sparing Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Measure #270: Inflammatory Bowel Disease (IBD): Preventive Care: Corticosteroid Sparing Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
New treatment options in UC. Rob Bryant IBD Consultant Royal Adelaide Hospital
 New treatment options in UC Rob Bryant IBD Consultant Royal Adelaide Hospital Talk Outline 1. Raising expectations 2. Optimising UC therapy 3. Clinical trials 4. What s new on the PBS? 5. Questions 1.
New treatment options in UC Rob Bryant IBD Consultant Royal Adelaide Hospital Talk Outline 1. Raising expectations 2. Optimising UC therapy 3. Clinical trials 4. What s new on the PBS? 5. Questions 1.
-2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine. -June 2008: Recurrence of rectal blood loss and urgency
 SD, male 40 yrs. old. (680718M467.) -2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine -June 2008: Recurrence of rectal blood loss and urgency Total colonoscopy: ulcerative rectitis,
SD, male 40 yrs. old. (680718M467.) -2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine -June 2008: Recurrence of rectal blood loss and urgency Total colonoscopy: ulcerative rectitis,
Northern Treatment Advisory Group. Biologic drugs for treatment-refractory moderately to severely active ulcerative colitis
 Northern Treatment Advisory Group Biologic drugs for treatment-refractory moderately to severely active ulcerative colitis Lead author: Dominic McDermott Regional Drug & Therapeutics Centre (Newcastle)
Northern Treatment Advisory Group Biologic drugs for treatment-refractory moderately to severely active ulcerative colitis Lead author: Dominic McDermott Regional Drug & Therapeutics Centre (Newcastle)
Positioning Biologics in Ulcerative Colitis
 Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Treating to Achieve a Target and Disease Monitoring in 2015: State of the Art
 Treating to Achieve a Target and Disease Monitoring in 2015: State of the Art David T. Rubin, MD The Joseph B. Kirsner Professor of Medicine Chief, Section of Gastroenterology, Hepatology and Nutrition
Treating to Achieve a Target and Disease Monitoring in 2015: State of the Art David T. Rubin, MD The Joseph B. Kirsner Professor of Medicine Chief, Section of Gastroenterology, Hepatology and Nutrition
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Ulcerative colitis: the management of ulcerative colitis Quality standard title: Ulcerative
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Ulcerative colitis: the management of ulcerative colitis Quality standard title: Ulcerative
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital
 IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
ULCERATIVE COLITIS. Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC
 ULCERATIVE COLITIS Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC What is Ulcerative Colitis? Ulcerative colitis (UC) is a disease marked by inflammation
ULCERATIVE COLITIS Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC What is Ulcerative Colitis? Ulcerative colitis (UC) is a disease marked by inflammation
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals
 Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
Research Article Temporary Fecal Diversion in the Management of Colorectal and Perianal Crohn s Disease
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2015, Article ID 286315, 5 pages http://dx.doi.org/10.1155/2015/286315 Research Article Temporary Fecal Diversion in the Management
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2015, Article ID 286315, 5 pages http://dx.doi.org/10.1155/2015/286315 Research Article Temporary Fecal Diversion in the Management
Clinical Course of Infliximab Treatment in Korean Pediatric Ulcerative Colitis Patients: A Single Center Experience
 pissn: 2234-8646 eissn: 2234-8840 http://dx.doi.org/10.5223/pghn.2014.17.1.31 Pediatric Gastroenterology, Hepatology & Nutrition 2014 March 17(1):31-36 Original Article PGHN Clinical Course of Infliximab
pissn: 2234-8646 eissn: 2234-8840 http://dx.doi.org/10.5223/pghn.2014.17.1.31 Pediatric Gastroenterology, Hepatology & Nutrition 2014 March 17(1):31-36 Original Article PGHN Clinical Course of Infliximab
Primary & Secondary Care Inflammatory Bowel Disease Pathway February 2018
 South East London Area Prescribing Committee: Primary & Secondary Care Inflammatory Bowel Disease Pathway February 2018 Developed by: South East London IBD Pathway Development Group Approved: February
South East London Area Prescribing Committee: Primary & Secondary Care Inflammatory Bowel Disease Pathway February 2018 Developed by: South East London IBD Pathway Development Group Approved: February
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases
 Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
Selby Inflamm Bowel Dis. 2008:14:
 Medical Management of Inflammatory Bowel Disease Freddy Caldera D.O. Assistant Professor Division of Gastroenterology Objectives Discuss Crohn s disease and Ulcerative Colitis Discuss Medications for Inflammatory
Medical Management of Inflammatory Bowel Disease Freddy Caldera D.O. Assistant Professor Division of Gastroenterology Objectives Discuss Crohn s disease and Ulcerative Colitis Discuss Medications for Inflammatory
Treatment Goals. Current Therapeutic Pyramids Crohn s Disease Ulcerative Colitis 11/14/10
 Current Management of IBD: From Conventional Agents to Biologics Stephen B. Hanauer, M.D. University of Chicago Treatment Goals Induce and maintain response/ remission Prevent complications Improve quality
Current Management of IBD: From Conventional Agents to Biologics Stephen B. Hanauer, M.D. University of Chicago Treatment Goals Induce and maintain response/ remission Prevent complications Improve quality
FERRING PHARMACEUTICALS. Enjoy The simple COR/939/2014/CH3
 Enjoy The simple pleasures of life COR/939/2014/CH3 Ulcerative colitis disrupts the simple pleasures in life Patients with ulcerative colitis may live with a considerable symptom burden despite medical
Enjoy The simple pleasures of life COR/939/2014/CH3 Ulcerative colitis disrupts the simple pleasures in life Patients with ulcerative colitis may live with a considerable symptom burden despite medical
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel diseases: a real life experience
 Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
How do I choose amongst medicines for inflammatory bowel disease. Maria T. Abreu, MD
 How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
5-ASA Therapy, Steroids and Antibiotics in Inflammatory Bowel Disease
 5-ASA Therapy, Steroids and Antibiotics in Inflammatory Bowel Disease David T. Rubin, MD Associate Professor of Medicine Co-Director, Inflammatory Bowel Disease Center University it of Chicago Medical
5-ASA Therapy, Steroids and Antibiotics in Inflammatory Bowel Disease David T. Rubin, MD Associate Professor of Medicine Co-Director, Inflammatory Bowel Disease Center University it of Chicago Medical
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Biologic Therapy for Ulcerative Colitis in 2015
 5/6/215 Biologic Therapy for Ulcerative Colitis in 215 John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University Bressler B, Marshall JK, et al. Gastroenterology 215;148: 135-58
5/6/215 Biologic Therapy for Ulcerative Colitis in 215 John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University Bressler B, Marshall JK, et al. Gastroenterology 215;148: 135-58
Patho Basic Chronic Inflammatory Bowel Diseases. Jürg Vosbeck Pathology
 Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Review article: induction therapy for patients with active ulcerative colitis
 Alimentary Pharmacology & Therapeutics Review article: induction therapy for patients with active ulcerative colitis S. P. L. TRAVIS John Radcliffe Hospital and Linacre College, Oxford, UK Correspondence
Alimentary Pharmacology & Therapeutics Review article: induction therapy for patients with active ulcerative colitis S. P. L. TRAVIS John Radcliffe Hospital and Linacre College, Oxford, UK Correspondence
Perianal and Fistulizing Crohn s Disease: Tough Management Decisions. Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic
 Perianal and Fistulizing Crohn s Disease: Tough Management Decisions Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic Talk Overview Background Assessment and Classification
Perianal and Fistulizing Crohn s Disease: Tough Management Decisions Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic Talk Overview Background Assessment and Classification
SER-287 Phase 1b topline study results in patients with mild-to-moderate Ulcerative Colitis October 2, 2017
 SER-287 Phase 1b topline study results in patients with mild-to-moderate Ulcerative Colitis October 2, 2017 Leading the Microbiome Revolution Forward Looking Statements Some of the statements in this presentation
SER-287 Phase 1b topline study results in patients with mild-to-moderate Ulcerative Colitis October 2, 2017 Leading the Microbiome Revolution Forward Looking Statements Some of the statements in this presentation
5-aminosalicylic acid (5-ASA) is the mainstay of first-line therapy
 MMX Mesalamine for Induction and Maintenance Therapy in Mild-to-Moderate Ulcerative Colitis Stephen B. Hanauer, MD 1 ; Gary R. Lichtenstein, MD 2 ; Michael A. Kamm, MD 3 ; William J. Sandborn, MD 4 ; Kirstin
MMX Mesalamine for Induction and Maintenance Therapy in Mild-to-Moderate Ulcerative Colitis Stephen B. Hanauer, MD 1 ; Gary R. Lichtenstein, MD 2 ; Michael A. Kamm, MD 3 ; William J. Sandborn, MD 4 ; Kirstin
Ulcerative Colitis: Refining our Management and Incorporating Newer Concepts
 Ulcerative Colitis: Refining our Management and Incorporating Newer Concepts Asher Kornbluth, MD Clinical Professor of Medicine The Henry D. Janowitz The Mt. Sinai School of Medicine Refining our Management
Ulcerative Colitis: Refining our Management and Incorporating Newer Concepts Asher Kornbluth, MD Clinical Professor of Medicine The Henry D. Janowitz The Mt. Sinai School of Medicine Refining our Management
Gionata Fiorino VEDOLIZUMAB E IBD. Un nuovo target terapeutico
 Gionata Fiorino VEDOLIZUMAB E IBD Un nuovo target terapeutico Anti cell adhesion molecules Danese S, NEJM 2011 6 Steps leukocyte recruitment Fiorino G. et al. 2010 Vedolizumab Blocks Fewer Biological Pathways
Gionata Fiorino VEDOLIZUMAB E IBD Un nuovo target terapeutico Anti cell adhesion molecules Danese S, NEJM 2011 6 Steps leukocyte recruitment Fiorino G. et al. 2010 Vedolizumab Blocks Fewer Biological Pathways
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 3 October 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis
 doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
Tumor necrosis factor-alpha antibody for maintenace of remission in Crohn s disease (Review)
 Tumor necrosis factor-alpha antibody for maintenace of remission in Crohn s disease (Review) Behm BW, Bickston SJ This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Tumor necrosis factor-alpha antibody for maintenace of remission in Crohn s disease (Review) Behm BW, Bickston SJ This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Medicine OPEN. Observational Study. 1. Introduction
 Observational Study Medicine OPEN Prospective comparison of preference and efficacy of adalimumab and infliximab for treating ulcerative colitis naive to antitumor necrosis factor therapy Tsutomu Mizoshita,
Observational Study Medicine OPEN Prospective comparison of preference and efficacy of adalimumab and infliximab for treating ulcerative colitis naive to antitumor necrosis factor therapy Tsutomu Mizoshita,
Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R.
 UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger
 ORIGINAL ARTICLE: GASTROENTEROLOGY Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger Judith R. Kelsen, Andrew B. Grossman, Helen Pauly-Hubbard, Kernika Gupta, Robert N. Baldassano, and
ORIGINAL ARTICLE: GASTROENTEROLOGY Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger Judith R. Kelsen, Andrew B. Grossman, Helen Pauly-Hubbard, Kernika Gupta, Robert N. Baldassano, and
Clinical Trials in IBD. Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases
 Clinical Trials in IBD Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases Objectives Today s discussion will address the following topics: Similarities and differences between Crohn
Clinical Trials in IBD Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases Objectives Today s discussion will address the following topics: Similarities and differences between Crohn
INFLAMMATORY BOWEL DISEASE. Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic
 INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
Clinical guideline Published: 10 October 2012 nice.org.uk/guidance/cg152
 Crohn's disease: management Clinical guideline Published: 10 October 2012 nice.org.uk/guidance/cg152 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Crohn's disease: management Clinical guideline Published: 10 October 2012 nice.org.uk/guidance/cg152 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
This information explains the advice about Crohn's disease that is set out in NICE guideline CG152.
 Information for the public Published: 1 October 2012 nice.org.uk About this information NICE guidelines provide advice on the care and support that should be offered to people who use health and care services.
Information for the public Published: 1 October 2012 nice.org.uk About this information NICE guidelines provide advice on the care and support that should be offered to people who use health and care services.
Understanding Inflammatory Bowel Diseases (IBD):
 Understanding Inflammatory Bowel Diseases (IBD): What Every Patient Needs to Know William H Holderman, MD Digestive Health Specialists Tacoma, WA Today s Objectives Define IBD, its potential causes and
Understanding Inflammatory Bowel Diseases (IBD): What Every Patient Needs to Know William H Holderman, MD Digestive Health Specialists Tacoma, WA Today s Objectives Define IBD, its potential causes and
Current management options and recent advances in IBD
 n DRUG REVIEW Current management options and recent advances in IBD Ben Warner BSc, MRCP and Peter Irving MA, MD, FRCP SPL The advent of biological therapies has revolutionised the management of inflammatory
n DRUG REVIEW Current management options and recent advances in IBD Ben Warner BSc, MRCP and Peter Irving MA, MD, FRCP SPL The advent of biological therapies has revolutionised the management of inflammatory
Pharmacotherapy of Inflammatory Bowel Disorder
 PHARMACY / MEDICAL POLICY 5.01.563 Pharmacotherapy of Inflammatory Bowel Disorder Effective Date: May 1, 2018 Last Revised: April 18, 2018 Replaces: Extracted from 5.01.550 RELATED MEDICAL POLICIES: 11.01.523
PHARMACY / MEDICAL POLICY 5.01.563 Pharmacotherapy of Inflammatory Bowel Disorder Effective Date: May 1, 2018 Last Revised: April 18, 2018 Replaces: Extracted from 5.01.550 RELATED MEDICAL POLICIES: 11.01.523
To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture,
 To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture, click Options in the Message Bar, and then click Enable
To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture, click Options in the Message Bar, and then click Enable
Review article: the long-term management of ulcerative colitis
 Aliment Pharmacol Ther 2004; 20 (Suppl. 4): 97 101. Review article: the long-term management of ulcerative colitis S. B. HANAUER Section of Gastroenterology, University of Chicago, Chicago, IL, USA SUMMARY
Aliment Pharmacol Ther 2004; 20 (Suppl. 4): 97 101. Review article: the long-term management of ulcerative colitis S. B. HANAUER Section of Gastroenterology, University of Chicago, Chicago, IL, USA SUMMARY
 Tacrolimus therapy as an alternativ Titlemaintaining remission in patients w colitis. Author(s) Yamamoto, Shuji; Nakase, Hiroshi; M Masuda, Satohiro; Inui, Ken-ichi; C Citation Journal of clinical gastroenterolog
Tacrolimus therapy as an alternativ Titlemaintaining remission in patients w colitis. Author(s) Yamamoto, Shuji; Nakase, Hiroshi; M Masuda, Satohiro; Inui, Ken-ichi; C Citation Journal of clinical gastroenterolog
Title: Accuracy of calprotectin in evaluating sub- clinical inflammation in Ulcerative
 PROTOCOL ACERTIVE STUDY Title: Accuracy of calprotectin in evaluating sub- clinical inflammation in Ulcerative colitis (ACERTIVE) Sponsor: Portuguese IBD Study Group (Grupo de Estudos da Doença Inflamatória
PROTOCOL ACERTIVE STUDY Title: Accuracy of calprotectin in evaluating sub- clinical inflammation in Ulcerative colitis (ACERTIVE) Sponsor: Portuguese IBD Study Group (Grupo de Estudos da Doença Inflamatória
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease. David A. Schwartz, MD
 An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
Treatment of Pediatric IBD: What is Different?
 Treatment of Pediatric IBD: What is Different? January 13, 2017 Michael Kappelman MD, MPH University of North Carolina at Chapel Hill Overview Is Pediatric IBD the same disease? Treatment considerations
Treatment of Pediatric IBD: What is Different? January 13, 2017 Michael Kappelman MD, MPH University of North Carolina at Chapel Hill Overview Is Pediatric IBD the same disease? Treatment considerations
IBD Understanding Your Medications. Thomas V. Aguirre, MD Santa Barbara GI Consultants
 IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
Predicting the natural history of IBD. Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium
 Predicting the natural history of IBD Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium Patient 1 Patient 2 Age 22 Frequent cramps and diarrhea for 6 months Weight
Predicting the natural history of IBD Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium Patient 1 Patient 2 Age 22 Frequent cramps and diarrhea for 6 months Weight
Mucosal Healing in Ulcerative Colitis: A Comprehensive Review
 Drugs DOI 10.1007/s40265-016-0676-y REVIEW ARTICLE Mucosal Healing in Ulcerative Colitis: A Comprehensive Review Pedro Boal Carvalho 1 José Cotter 1,2,3 Springer International Publishing Switzerland 2017
Drugs DOI 10.1007/s40265-016-0676-y REVIEW ARTICLE Mucosal Healing in Ulcerative Colitis: A Comprehensive Review Pedro Boal Carvalho 1 José Cotter 1,2,3 Springer International Publishing Switzerland 2017
Introduction. Toshifumi Hibi 1 Yuya Imai
 J Gastroenterol (2017) 52:1101 1111 DOI 10.1007/s00535-017-1326-1 ORIGINAL ARTICLE ALIMENTARY TRACT Efficacy and safety of golimumab 52-week maintenance therapy in Japanese patients with moderate to severely
J Gastroenterol (2017) 52:1101 1111 DOI 10.1007/s00535-017-1326-1 ORIGINAL ARTICLE ALIMENTARY TRACT Efficacy and safety of golimumab 52-week maintenance therapy in Japanese patients with moderate to severely
Rectal Lymphoid Follicle Aphthous Lesions Frequently Progress to Ulcerative Colitis with Proximal Extension
 doi: 10.2169/internalmedicine.1635-18 Intern Med Advance Publication http://internmed.jp ORIGINAL ARTICLE Rectal Lymphoid Follicle Aphthous Lesions Frequently Progress to Ulcerative Colitis with Proximal
doi: 10.2169/internalmedicine.1635-18 Intern Med Advance Publication http://internmed.jp ORIGINAL ARTICLE Rectal Lymphoid Follicle Aphthous Lesions Frequently Progress to Ulcerative Colitis with Proximal
