rupture, you may notice silicone in their lymph nodes on radiographs. This may be seen and help us detect that there is a rupture.
|
|
|
- Briana Holt
- 5 years ago
- Views:
Transcription
1 Hello. I m Melissa Crosby. I m an Associate Professor at The University of Texas MD Anderson Cancer Center in the Department of Plastic Surgery. I d like to discuss with you the Late Effects of Breast Reconstruction. On completion of this lecture, participants will be able to describe long-term sequelae of implant reconstruction; describe the long-term sequelae of autologous reconstruction; understand how adjuvant therapies may affect reconstruction long-term; determine how reconstruction may affect breast cancer recurrence. As with any surgery or where a surgical incision has been made, scarring can occur. Abnormal scarring often is the result of tension as well as patient genetics. When I find a patient that has a widened scar, we may need to revise the scar by excising the scar and re-closing it because maybe there is tension on the closure. Hypertrophic scarring means raised scars within the boundary of the original incision that was made. Again, we may want to res --- revise the scar by excising it and re-closing it under less tension. There re pressure dressings that you can place as well as silicone sheeting, massage, and scar creams. But often times, it s patients genetics that determine how they will scar, as well as technique at the time of the surgery. You can also perform steroid injections --- injections involving different steroids for decreasing the amount of scar. Keloid is a raised scar that grows beyond the boundaries of the original wound. So, your incision is not only elevated but it also goes outside of that. This is very common in darker-skinned patients. Often times, you can try to revise the scar by excising it. However, there s a high recurrence rate involved with this. Again, pressure dressings have been tried as well as silicone sheeting, massage as well as scar creams, different steroid injections as well as radiation therapy. However, this is rarely indicated and often when this is brought forward to patients, they re not too excited about having radiation therapy for a scar. However, some patients has extensive keloiding and do require radiation therapy to decrease the inflammatory response. Again, aging and weight change may affect the results from reconstruction. We know with aging that the epidermis and subcutaneous fat do thin. Our skin strength and elas - -- elasticity decrease due to decreases in the amount of connective tissue over time. And our blood vessels become more fragile. As a result, any patient that --- that has had a reconstruction may notice maybe more rippling with their implant. If they ve had an implant-based reconstruction, their breast may become more ptotic. And what I mean by that is more droopy or they may bottom out. And scars also may become more fragile over time. Also, if a patient gains weight or loses weight, they may notice changes in their reconstruction, especially those that maybe they used their own tissue. So revisional surgeries may be required. Their natural breast with an implant reconstruction may also change and there may be requirement for a symmetry procedure. Also, may be an increased risk of abdominal complications with weight gain if they ve had an abdominalbased reconstruction.
2 Looking specifically at implant reconstruction and the late effects of implant reconstruction: Some of the late --- late effects are listed here. Asymmetry, implant rippling as well as wrinkling, implant malposition, implant deflation, capsular contracture which is a scar surrounding the implant, and infection. I m going to go through each of these individually. Asymmetry: This is most common with a unilateral breast reconstruction, meaning one breast is reconstructed and the patient has their natural breast, so it s often difficult to match a natural breast over time with aging and weight changes, especially to an implanted breast. We may need to perform a symmetry procedure on the nonreconstructed breast. And again, this may involve cosmetic procedures that we perform including breast mastopexy or lifts; breast reduction, which reduces the size of the breast; or breast augmentation, which involves placing an implant to enlarge the size of a breast. Patient may request --- also, due to the differences in size, they may request surgery. Implant Rippling and Wrinkling: This is very different than an augmentation when you have the overlying breast tissue to cover the implant. So in an implant-based reconstruction we have the overlying skin and pectoralis major muscle. Over time, this does thin and some of the compliance of the implant may be transmitted through the skin. And this appears as a ripple. So, again, minimal coverage over an implant-based reconstruction; this is often seen in the upper pole of the breast because gravity will pull the majority of the implant to the lower pole of the reconstructed breast. And, therefore, the rippling will be seen on the upper pole. Sometimes, we have to overfill an implant to fill this out. Maybe use a different type of implant that has a smooth-wall rather than a textured wall. Other options include fat grafting and dermal substitutes but may add extra coverage over that implant that isn t there, with an implant-based reconstruction. Implant Malposition: This may be related to scarring around the implant or skin laxity over time. This may require revisional surgery to reposition the implant. Around each implant, there is a scar capsule so, to reposition the implant, we may need to release that capsule, or we may need to put sutures in that capsule to help position that implant in the right position. Implant Deflation and Rupture: So, saline implant rupture, the patient will know right away because the saline will be absorbed by the body. And, therefore, they will get a flattened breast. This is easily detected on physical examination. This does require replacement with a new implant. Most manufacturers report about a 1-7% over a one to three [year] period. Silicone Rupture: There re different generations of silicone implants. And the trend has been towards making more of the viscous cohesive silicone gel. Often, these ruptures are silent and may not be noticed. Patients may come to me with a notice of a change in shape or maybe some hardening of the breast. The ruptures can occur intracapsular, which means that within that scar capsule, the implant can rupture. Usually, the silicone stays within that capsule. So that makes about 80-90% of the ruptures that I see. Extracapsular means that that silicone may go outside of the scar capsule that s formed, again, very are --- rare, less common. However, in patients that have extracapsular
3 rupture, you may notice silicone in their lymph nodes on radiographs. This may be seen and help us detect that there is a rupture. Recent data over a six-year study shows that rupture rates in reconstructed patients ranges from about 4-9%, depending on each manufacturer. How do you determine if a rupture has occurred? Really, the gold standard is performing an MRI. The sensitivity and specificity are greater than 90%. There is a special linguine sign that they look for. And it allows basically radiologists to let us know that the patient does has --- have a rupture. They also may notice inverted teardrops to determine this. Capsular Contracture: Each implant that is placed, your body notices it as a foreign body. So it will form a scar around that implant. So we do have encapsulation of a breast prosthesis. At times, it can form a firm, fibrous shell. So this can be not noticeable to the patient. There are different grades of that. And, depending on the grade and the extent of scarring that forms around that implant, may cause us to perform a revisional surgery. So as you can see here, Grade IV, this is severe contracture where the patient has a very firm, visibly obvious scar capsule around that implant. It s often painful. These are more of the patients that we may move to do a revisional surgery. Some of the literature thinks that it may be related to a foreign body reaction or to an infection, or some of the bacteria got into the capsule --- or to the pocket when we were placing the implant. So, therefore, some of the studies do show that irrigating the pocket when we do place that implant with antibiotics, placing it under the muscle, is helpful in preventing significant capsular contracture. More commonly, this is found, however, in reconstructed patients. And it is reported at a rate of about 80-36% [speaker intended to say 8-36%] over a one to six-year period. Oftentimes, patients that have maybe had radiation therapy, they may see a more significant contracture. This also can be a ca --- the most common cause of revisional surgery as well for these patients. Often, treatment for this involves a capsulotomy which basically means just making a hole in this fibrous capsule, so releasing that scar around that implant. It also may involve removing that entire scar, so a capsulectomy, removing that fibrous capsule. Also, may be replacing that implant if it s not underneath the muscle. However, often and most commonly in reconstructed patients, the implants are placed under the pectoralis major muscle. Some patients have such significant scarring that we may need to use their own tissue. So we do remove the implant, may be use a latissimus dorsi flap with an implant, or use their own tissue only. There is question that if a different implant is used, meaning a different saline versus silicone, or a different kind of texturing, they felt in the past that maybe textured implants cause less contracture. However, recently, this has not been shown to be true. Infection: As any kind of foreign body, this can become infected. This is usually an early complication, four to six weeks, maybe, after surgery within, you know, postoperative period. Again late infection, really a low incidence of that, may be related to bacteremia. The patient gets an infection from another cause and it seeds the implant. We do show that there s really no indication for routine antibiotic prophylaxis so many patients come
4 to me saying, I have a dental procedure. I have an implant in. Do I need to have prophylaxis with antibiotics? There re no studies to show that this is warranted. Treatment for this is based on the suspected organism. So you want to try to identify the organism that s causing the infection and focus your antibiotic therapy on this. In severe infections, removing the implant may be required to help the patient heal from this and cure the infection. With implant reconstruction, patient satisfaction is usually significantly higher in those patients that have had silicone implants, and bilateral versus unilateral reconstruction. This is most likely due to the fact that it s very difficult again to recreate a breast that mimics a natural breast, especially in an implant-based reconstruction which is more perky-looking. Satisfaction over time is diminished with both kinds of implants. Post mastectomy radiation, again, has a significant negative effect on breast satisfaction for both types of implants, mostly related to the capsular contracture. Implant reconstruction is also assodi --- associated with higher revision rates than other types of reconstruction, opting for replacement, you know, making it more symmetric, changing that pocket, as we discussed. Looking at a latissimus dorsi breast reconstruction: Some of the late effects of this reconstruction can involve scarring, asymmetry, persistent seroma, muscle contraction, fullness under the arm along the chest, implant issues, because often the implant is placed under the latissimus dorsi flap, and shoulder biomechanical changes. And I ll go through each one of these individually. Again, as mentioned with implant reconstruction, there is scarring involved in this, and the scar is often in a different location than where the mastectomy was performed. So on the back --- so, you have both a scar on the back as well as the chest. There may be required revisions of this scar once it s healed and the skin relaxes. So there may have been tension on the closure. You get a widened scar and this may need to be revised in a secondary surgery. Also, asymmetry: As with any type of reconstruction, you can have changes with aging, weight gain, effects from the implant that s underlying it, and this may require revision or symmetry procedures. Persistent seroma: this is probably the most common early complication of a latissimus dorsi flap due to the large surface area of the back where the donor site is. So placing may require serial drainage, a drain replacement if, you know, you can t remove the fluid with just serial drainage. Also, there s been use of sclerosing agents to scar down that pocket that s in the back to assist with getting rid of that seroma. Over time, there is a bursa or scar capsule in a sense, that does form when a chronic seroma exists. And, therefore, this may require surgical removal, mattress sush --- suturing and different techniques to try to close down this cavity. Also, patients notice some fullness under the arm along the chest. Again, when we perform this flap reconstruction, the flap is rotated under the arm and that muscle underlies the arm on the side of the axilla. So most of the time, we tell patients that it will atrophy over time because they aren t using it as much as they would if they had it in its normal anatomical location. So it will atrophy over time. Also, we can perform
5 liposuction of the overlying tissue to reduce the bulk. Again, because there is an implant in place, there are implant issues as discussed prior. And, these issues may result in revisional surgeries for patients having a latissimus dorsi flap. Shoulder Biomechanical Changes: So the latissimus dorsi muscle is one of 26 muscles that make up the shoulder joint. As you can see here, it involves multiple functions including medial rotation, backward extension, adduction. It helps depress a raised arm. And it s an accessory cough and squeeze muscle for us. There are six other muscles that also act in extension, adduction, and internal and external rotation. So when a patient loses the latissimus muscle, there is a synergistic action of the teres major muscle, which leads to hypertrophy and compensation. When looking at patients that have had the latissimus dorsi muscle, there s usually improvement over about a six to 12 months. They don t loo lose any range of motion, both active and passive. It s really unchanged from most studies. We do find that patients may have a faster rate of fatigue with certain activities that use extension and adduction, so ladder-climbing, swimming, or pushing up in a chair. Again, most patients don t complain of any fatigue or any problems having this procedure. Physical therapy may be necessary, however, just to increase the strength and range of motion, and assist patients with having less fatigue in certain activities if they do those activities often. When we look at reconstructions that involve autologous tissue from the abdomen, so the TRAM flaps, the DIEP, the SIE flaps, there are effects from this surgery as well. Some late effects include scarring again, asymmetry, fat necrosis, and abdominal weakness including bulges and hernias. Scarring: So when we perform this procedure, again, an incision is made in another location in the body, so the patients have a scar both on their abdomen as well as their chest. Depending on how that scar heals, we may need to revise the scar again. At the time of surgery, there is swelling so there may be more tension on closure so later we want to revise that scar when there is less tension and swelling. Patients do mak --- complain of paresthesias, so some numbness, a belt-like sensation. So I often tell my patients that if they get bloated or they eat a full meal, they may feel like they have a belt on, giving them tightness in that area. So also issues of asymmetry once again. This is their own tissue so if they have weight gain or weigh loss, then this tissue is going to change with them. So they ll gain weight in that breast reconstruction, or may lose weight in that breast reconstruction, so the size of that breast may change. In addition, if they gain weight, they may have increased pressure intra-abdominally where that tissue was closed, so leading to increased laxity and maybe risk of hernias and bulges, or that increased feeling of tightness and that belt-like sensation. So I often tell my patients to try to maintain a constant weight so that they don t have to deal with these issues.
6 Fat Necrosis: This basically means when there is inadequate blood supply to the fat that we transfer with the flap. So you can have death of the fat as well as scarring. It s basically a sterile inflammatory process that results in saponification of the fat by both blood and tissue lipases. So what results and how would you identify fat necrosis? Basically, it s a hardened area in the reconstruction so when you palpate the reconstructed breast, you feel a hardened area. Well, of course, with patients that have had a history of breast cancer, any kind of lump or bump is very concerning. So if there is a concern, an ultrasound can be performed. And often, just with an ultrasound, you can distinguish between cancer recurrence and fat necrosis. If there s any concern, then confirmation with a biopsy may be necessary. Oftentimes, I have my patients do massage, monitoring of this area, making sure it doesn t get any larger, and then confirmation with further studies. Sometimes, I may have to excise the area if it s in an area that is disturbing to the patient or aesthetically not pleasing. I can also break this up with liposuction cannulas often times as well, to make it a softer area on the breast reconstruction. Probably, more importantly, there s a risk of abdominal weakness and this is when we talk about the trend towards preserving that abdominal muscle, that rectus muscle, when we perform abdominal tissue transfer. This is why the trend towards those perforator flaps, meaning preserving that muscle, taking just the overlying skin and fat, and not taking that muscle. The important part is, is even with remee --- leaving that muscle behind, we still go through the fascia which is the strength layer of the abdomen. So as a result, there may be laxity of that abdominal fascia which is called a bulge. So it s not really a true herniation of bowel contents. It s more an aesthetic concern, so they may notice a bulge on their abdomen. And it s related to abdominal laxity. This can really occur with any type of flap that s harvested. So even if you leave muscle behind, it could get denervated so it allows laxity of the abdomen, as well as the fascia may become lax and weak, resulting in a bulge. Patients that may have had a pedicled TRAM, so mean --- leaving it on its blood supply, may see a bulge because the muscle has been transferred. So they may see a bulge kind of near their chest region where that muscle is. So similar to the latissimus flap where they see that kind of extra fullness under their arm, you may also see a bulge in muscle on their chest, or maybe some laxity in the upper abdomen where the flap is transferred. A true hernia is more concerning, and this is where the bowel contents basically strewed through that fascia layer. Again, this is more concerning. You can distinguish between a bulge and a hernia, based on CT scan. If a patient does have a hernia, then this may need surgical treatment because there can be risk of strangulation or incarceration of the bowel contents; again, pretty rare. The abdominal weakness: Basically, we worry about this more with bilateral reconstruction because we re entering two portions of the abdomen, making two incisions through the fascia and potentially taking --- weakening the muscle on both sides. The SIEA flap, which is the superficial inferior epigastric artery flap, that flap lies about the fascia so we don t have to take any fascia muscle. So it really has the lowest risk as --- of abdominal weakness as well as hernias and bulges. The rate of abdominal wall complications ranges from about 3%-48% and depends upon the type of flap,
7 unilateral versus bilateral reconstructions. That DIEP flap, the deep inferior epigastric perforator flap, so basically leaving that muscle behind and just taking the perforator, has about one-half the risk of abdominal bulge or hernia, as compared to taking a free muscle flap, so taking that entire rectus muscle with your skin and overlying fat. It does also, however, have an increased risk of the fat necrosis that we spoke about easi --- earlier because there s not as much muscle and maybe blood supply to that overlying skin and fat. However, we did find no difference in fat necrosis between what we call a muscle-sparing flap and a DIEP flap, muscle-sparing meaning that we have left some muscle behind and, again, the perforator flap. Functional Deficits: There re been studies looking at the physiotherapy and deficits caused by taking these flaps. Obviously, with a pedicled TRAM, patients may experience more deficit on a physical therapy evaluation because of removing that rectus muscle and having decreased oblique muscle function. A free TRAM, meaning taking it off its blood supply but still taking the entire muscle, has really shown no minimal deficit in rectus muscle function. However, the perforator flaps are much better in the sense of abdominal weakness, their function return to baseline. But most patients will tell you that have gone through many of these procedures, especially in unilateral reconstructions, that subjectively they don t notice any weakness in their abdominal wall because other muscles are available to help with normal daily function. So what we found is that subjective measures of abdominal wall function are pretty similar across unilateral pedicled flaps as well as free TRAM flaps and those perforator flaps, DIEP flap procedures. Muscle-sparing flaps, compared to the DIEP in a lun --- unilateral setting, again, likely no difference in abdominal wall weakness. But again, it depends on the amount of muscle taken and the denervation of the muscle when you re performing these procedures. Patient satisfaction: When you compare all reconstructive groups including implant, latissimus dorsi and abdominal-based flaps, we do know that using the patient s own tissue has basically --- has a significantly higher general, as well as aesthetic satisfaction, than implant-based reconstructions. We also know that abdominal-based flaps had significantly higher generally and aesthetic satisfaction over latissimus dorsi flaps. However, we found no difference in satisfaction between patients receiving a pedicled TRAM and those having perforator flaps. So again, using the patient s own tissue over time probably has greater patient satisfaction. When you look at reconstruction and possible interference with adjuvant therapies, when you look at chemotherapy, studies have shows that after immediate bree breast reconstruction compared to mastectomy alone, there is an increased incidence of wound complications, however, no delay in initiation of adjuvant therapy. The incidence of overall major postoperative complications are higher in the immediate breast reconstruction group. But on multivariate analysis, there were no significant relationships determined. Immediate breast reconstruction is, again, associated with a moderate increase in time to chemotherapy. However, this was not statistically
8 significant. So the data shows that patients may extend out before they start their chemotherapy, possibly about two weeks longer if they have an immediate reconstruction, only because they are possibly at higher risk for complications. When we look at radiation therapy, both pre- and post-mastectomy radiotherapy will have effects on reconstruction regardless of the method we perform. Therefore, it s very important to determine if the patient is going to need radiation therapy. And it will help us determine what type of reconstruction we perform and the timing of the reconstruction. Implant-based reconstruction have higher rates of that pathologic capsular contracture. So when I discuss the different grades of contracture, these are the patients that we may see more of that Grade III and Grade IV, where you have a firm capsule that becomes painful that may require revisional surgery. Autologous reconstructions: When they are radiated, they become contracted and tightened, and may have volume loss and contracture of that flap as well. So we see flaps that shrink in size, that become harder. We get volume loss. So it s really important to determine if a patient is going to need radiation. Reconstruction can also potentially impact the delivery of radiotherapy. So we found that radiation treatment in one study after immediate breast reconstruction were com --- was compromised and many patients, almost 52% of patients, had a compromise in their radiation treatment planning, with the largest compromise on left-sided breast cancers. So this is important to consider when a patient is going to need radiation therapy, if we should perform an immediate reconstruction because we don t want to impact their radiation therapy and their cancer care. Looking at Radiated Flaps: So, when a patient does undergo immediate reconstruction and unfortunately does have radiation to that flap, about 28% of our patients required an additional flap reconstruction for increasing the contour and volume correction. Or they may need to wear an external prosthesis to help with symmetry. So delayed reconstruction is recommended for patients who are likely to require post mastectomy radiation therapy. In certain patients, a babysitting procedure, what we mean by that is placing a tissue expander at the time of a mastectomy to kind of preserve that skin envelope, may be possible. Oftentimes, however, because of the inflated tissue expander may interfere with radiation therapy delivery, we may need to remove that expander or deflate it during radiation therapy. Again, looking at reconstruction and cancer recurrence: So many patients may come to me and ask, Well, if I have a reconstruction, how will I know if my cancer comes back? Or will it interfere with detection of breast cancer recurrence? What we found is that immediate reconstruction, even over a ten-year period, that it did not delay detection of chest wall recurrence. Most recurrences will occur within the skin or subcutaneous tissue, compared to the chest wall. Another study looked at immediate reconstruction patients with all forms of reconstruction as well as comparing those to patients that underwent mastectomy alone without reconstruction, and found that reconstruction did not adversely affect the incidence or time to detection of recurrent breast cancer. And there was no difference
9 between immediate breast reconstruction and mastectomy alone, patients and survival, time to distant metastases or local recurrence. However, the importance of physical exams and symptoms is very important because, really, we don t have any definitive screening tool to look for recurrence in patients that have had a reconstruction. So when patients come to me, examining their skin envelope, asking them for any symptoms, then we can direct our physical exam findings towards more foc --- focused exams. For example, if a patient has a nodule on their skin or subcutaneous tissue that is above our reconstruction, then we can perform an ultrasound or biopsy the area. If there re symptoms, for example, patient may be complaining of chronic pain in that area, soreness. Then, we may want to pursue that further with an ultrasound, a biopsy, or maybe CT scans or MRIs may be warranted to look at deeper structures that may be hidden by the reconstruction. If a recurrence does occur, then treatment may involve surgical excision, the patient may require further chemotherapy, and if they had not had radiation therapy from their prior breast cancer diagnosis, then patients may go on to have radiation therapy. In summary, all forms of reconstruction are associated ris ris --- with risk --- [excuse me] --- and long-term sequelae. Common implant reconstruction late effects include capsular contracture, which is that scar that forms around the implant; implant failure and malposition and rippling. Common latissimus flap reconstruction late effects include implant-related complication, --- complications because an implant is placed oftentimes under the flap, can also have scarring, seromas in the donor site in the back, and potential temporary shoulder weakness that may require physical therapy. Common abdominal flap reconstruction late effects may include abdominal weakness, scarring as well as fat necrosis. We do know that radiotherapy will impact reconstruction more than chemotherapy both in an immediate fashion and delayed. And reconstruction has been found to not interfere with detection of cancer recurrence. Thank you for your attention, and we do welcome any feedback.
can see several late effects. Asymmetry is probably the most common and the thing that patients notice the most. We can also see implant wrinkling or
 Hello, I am Summer Hanson. I m an assistant professor with the Department of Plastic and Reconstructive Surgery at the University of Texas MD Anderson Cancer Center. And today I m going to talk to you
Hello, I am Summer Hanson. I m an assistant professor with the Department of Plastic and Reconstructive Surgery at the University of Texas MD Anderson Cancer Center. And today I m going to talk to you
Breast Reconstruction. Westmead Breast Cancer Institute
 Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Goals of Care. Restore shape and function after cancer
 Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
In a second stage or a second operation that tissue expander is removed through the same incision and the implant is placed within the chest pocket.
 Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
MICHAEL R. ZENN, M.D. INFORMATION ABOUT BREAST RECONSTRUCTION
 MICHAEL R. ZENN, M.D. INFORMATION ABOUT BREAST RECONSTRUCTION The purpose of breast reconstruction is to restore body image and to enable you to wear all types of clothes without restriction. Most women
MICHAEL R. ZENN, M.D. INFORMATION ABOUT BREAST RECONSTRUCTION The purpose of breast reconstruction is to restore body image and to enable you to wear all types of clothes without restriction. Most women
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Oncoplastic and Reconstructive Surgery
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Breast Reconstruction. Breast Care
 Breast Reconstruction Breast Care We put our patients first by working as one team; leading and listening, and striving for the best. Together, we make the difference. Patient information Musgrove Park
Breast Reconstruction Breast Care We put our patients first by working as one team; leading and listening, and striving for the best. Together, we make the difference. Patient information Musgrove Park
Breast Reconstruction: Patient Information Document
 breastreconstructioncanada.ca Breast Reconstruction: Patient Information Document By Dr. Nicolas Guay Dr. Haemi Lee STANDARDIZED BREAST RECONSTRUCTION PATIENT INFORMATION TABLE OF CONTENTS Glossary...
breastreconstructioncanada.ca Breast Reconstruction: Patient Information Document By Dr. Nicolas Guay Dr. Haemi Lee STANDARDIZED BREAST RECONSTRUCTION PATIENT INFORMATION TABLE OF CONTENTS Glossary...
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons
 Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Exercise & Breast Cancer Recovery
 Exercise & Breast Cancer Recovery LEARNING OBJECTIVES Demonstrate an understanding of the diagnosis and treatment of breast cancer Demonstrate an understanding of how breast cancer surgery and treatment
Exercise & Breast Cancer Recovery LEARNING OBJECTIVES Demonstrate an understanding of the diagnosis and treatment of breast cancer Demonstrate an understanding of how breast cancer surgery and treatment
Breast Reconstruction Surgery
 Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
MISS CAROLINE PAYNE. Breast Augmentation
 MISS CAROLINE PAYNE BSc (Hons) MSc FRCS (Eng) FRCS(Plast) Consultant Plastic Reconstructive Surgeon Breast Augmentation What types of implants are available? Breast implant surgery may be referred to as
MISS CAROLINE PAYNE BSc (Hons) MSc FRCS (Eng) FRCS(Plast) Consultant Plastic Reconstructive Surgeon Breast Augmentation What types of implants are available? Breast implant surgery may be referred to as
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP
 INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
B11 Breast Reconstruction with Abdominal Tissue Flap
 B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C. Your Guide To BREAST RECONSTRUCTION
 Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
COSMETIC SURGERY: BREAST LIFT (MASTOPEXY)
 PROCEDURE FACT SHEET PLASTIC SURGERY COSMETIC SURGERY: BREAST LIFT (MASTOPEXY) This guide is for women who are considering having an operation to lift their breasts. We advise that you talk to a plastic
PROCEDURE FACT SHEET PLASTIC SURGERY COSMETIC SURGERY: BREAST LIFT (MASTOPEXY) This guide is for women who are considering having an operation to lift their breasts. We advise that you talk to a plastic
LAPAROSCOPIC HERNIA REPAIR
 LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
CONSENT FOR BREAST IMPLANT REMOVAL AND REPLACEMENT SURGERY
 CONSENT FOR BREAST IMPLANT REMOVAL AND REPLACEMENT SURGERY Breast Augmentation is a surgical procedure performed to enlarge the breasts for a number of reasons: To enhance the body contour of a woman,
CONSENT FOR BREAST IMPLANT REMOVAL AND REPLACEMENT SURGERY Breast Augmentation is a surgical procedure performed to enlarge the breasts for a number of reasons: To enhance the body contour of a woman,
BREAST AUGMENTATION TECHNIQUES
 BREAST AUGMENTATION TECHNIQUES Breast Augmentation Top Surgical Procedure in 2015 (Worldwide) Surgical Procedure : Breast Augmentation Rank : 1 Total : 1,488,992 Percent of Total Surgical Procedures :
BREAST AUGMENTATION TECHNIQUES Breast Augmentation Top Surgical Procedure in 2015 (Worldwide) Surgical Procedure : Breast Augmentation Rank : 1 Total : 1,488,992 Percent of Total Surgical Procedures :
Procedure Information Guide
 Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Medical Review Criteria Breast Surgeries
 Medical Review Criteria Breast Surgeries Subject: Breast Surgeries Authorization: Prior authorization is required for the following procedures requested for members enrolled in HPHC commercial (HMO, POS,
Medical Review Criteria Breast Surgeries Subject: Breast Surgeries Authorization: Prior authorization is required for the following procedures requested for members enrolled in HPHC commercial (HMO, POS,
Exercises After Breast Surgery
 PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massage after your breast surgery. Starting
PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massage after your breast surgery. Starting
BREAST RECONSTRUCTION ACTION PLAN
 BREAST RECONSTRUCTION ACTION PLAN CHOOSING THE PROCEDURE THAT S RIGHT FOR YOU Southern California Permanente Medical Group KPACTIONPLANS.ORG/BREASTRECON Jft KAISER PERMANENTE BREAST RECONSTRUCTION ACTION
BREAST RECONSTRUCTION ACTION PLAN CHOOSING THE PROCEDURE THAT S RIGHT FOR YOU Southern California Permanente Medical Group KPACTIONPLANS.ORG/BREASTRECON Jft KAISER PERMANENTE BREAST RECONSTRUCTION ACTION
Patient consent to investigation or treatment for: Breast augmentation/enlargement - Part 2 of 3
 Patient consent to investigation or treatment for: Breast augmentation/enlargement - Part 2 of 3 This is an informed consent document to explain the risks and alternative treatment to breast augmentation
Patient consent to investigation or treatment for: Breast augmentation/enlargement - Part 2 of 3 This is an informed consent document to explain the risks and alternative treatment to breast augmentation
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
So, we already talked about that recognition is the key to optimal treatment and outcome.
 Hi, I m Dr. Anthony Lucci from the University of Texas MD Anderson Cancer Center in Houston. And today, I d like to talk to you about the role of surgery in inflammatory breast cancer patients. So, there
Hi, I m Dr. Anthony Lucci from the University of Texas MD Anderson Cancer Center in Houston. And today, I d like to talk to you about the role of surgery in inflammatory breast cancer patients. So, there
inding the fit that s right for you. Your Surgery Planner For Breast Augmentation or Reconstruction with NATRELLE Saline-Filled Breast Implants
 inding the fit that s right for you. Your Surgery Planner For Breast Augmentation or Reconstruction with NATRELLE Saline-Filled Breast Implants L Place Your Device Identification Card(s) Here R INTRODUCTION
inding the fit that s right for you. Your Surgery Planner For Breast Augmentation or Reconstruction with NATRELLE Saline-Filled Breast Implants L Place Your Device Identification Card(s) Here R INTRODUCTION
B10 Breast Reconstruction with Latissimus Dorsi Flap
 www.rcseng.ac.uk www.rcsed.ac.uk www.asgbi.org.uk www.pre-op.org B10 Breast Reconstruction with Latissimus Dorsi Flap Expires end of May 2016 Issued April 2015 VITALITY.CO.UK You can get more information
www.rcseng.ac.uk www.rcsed.ac.uk www.asgbi.org.uk www.pre-op.org B10 Breast Reconstruction with Latissimus Dorsi Flap Expires end of May 2016 Issued April 2015 VITALITY.CO.UK You can get more information
Radiotherapy for breast cancer. Cancer Services Information for patients
 Radiotherapy for breast cancer Cancer Services Information for patients i Introduction This booklet will tell you about radiotherapy treatment for breast cancer and the side effects that you may experience
Radiotherapy for breast cancer Cancer Services Information for patients i Introduction This booklet will tell you about radiotherapy treatment for breast cancer and the side effects that you may experience
Medical Review Criteria Breast Surgeries
 Medical Review Criteria Breast Surgeries Effective Date: November 8, 2016 Subject: Breast Surgeries Policy: HPHC covers medically necessary breast surgeries including mastectomy, breast reconstruction,
Medical Review Criteria Breast Surgeries Effective Date: November 8, 2016 Subject: Breast Surgeries Policy: HPHC covers medically necessary breast surgeries including mastectomy, breast reconstruction,
INFORMED CONSENT BREAST IMPLANT REMOVAL
 2005 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use
2005 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use
ASPS Recommended Insurance Coverage Criteria for Third- Party Payers
 ASPS Recommended Insurance Coverage Criteria for Third- Party Payers Breast Implant Associated Anaplastic Large Cell Lymphoma BACKGROUND Anaplastic Large Cell Lymphoma (ALCL) is a rare type of cancer of
ASPS Recommended Insurance Coverage Criteria for Third- Party Payers Breast Implant Associated Anaplastic Large Cell Lymphoma BACKGROUND Anaplastic Large Cell Lymphoma (ALCL) is a rare type of cancer of
NATRELLE 410 HIGHLY COHESIVE ANATOMICALLY SHAPED SILICONE-FILLED BREAST IMPLANTS
 NATRELLE 410 HIGHLY COHESIVE ANATOMICALLY SHAPED SILICONE-FILLED BREAST IMPLANTS Breast Augmentation and Reconstruction Patients Should Consider Introduction Allergan has prepared this brochure to provide
NATRELLE 410 HIGHLY COHESIVE ANATOMICALLY SHAPED SILICONE-FILLED BREAST IMPLANTS Breast Augmentation and Reconstruction Patients Should Consider Introduction Allergan has prepared this brochure to provide
BREAST AUGMENTATION. everything you ever wanted to know about. Cosmetic breast specialist Dr Michael Miroshnik uses. breasts.
 everything you ever wanted to know about BREAST AUGMENTATION Actual patient of Dr Miroshnik ACCORDING TO SYDNEY PLASTIC SURGEON DR MICHAEL MIROSHNIK, ADVANCES IN SURGICAL TECHNIQUE AND IMPLANT TECHNOLOGY
everything you ever wanted to know about BREAST AUGMENTATION Actual patient of Dr Miroshnik ACCORDING TO SYDNEY PLASTIC SURGEON DR MICHAEL MIROSHNIK, ADVANCES IN SURGICAL TECHNIQUE AND IMPLANT TECHNOLOGY
AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION
 CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
Breast reduction surgery reduction mammaplasty Is it right for me? What to expect during your consultation Be prepared to discuss:
 This guide is for women who are considering having an operation to lift their breasts. We advise that you talk to a plastic surgeon and only use this information as a guide to the procedure. Breast reduction
This guide is for women who are considering having an operation to lift their breasts. We advise that you talk to a plastic surgeon and only use this information as a guide to the procedure. Breast reduction
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
Guide to Breast Augmentation: Everything You Need to Know
 Northwestern Specialists in Plastic Surgery Dr. Neil Fine, MD, FACS Dr. Clark Schierle, MD, PhD, FACS Contents 3 Introduction 4 Implant Shell 5 Implant Fill 6 Ideal Implant 7 Implant Shape 8 Implant Placement
Northwestern Specialists in Plastic Surgery Dr. Neil Fine, MD, FACS Dr. Clark Schierle, MD, PhD, FACS Contents 3 Introduction 4 Implant Shell 5 Implant Fill 6 Ideal Implant 7 Implant Shape 8 Implant Placement
Cosmetic Surgery: Breast Reduction
 PROCEDURE FACT SHEET PLASTIC SURGERY Cosmetic Surgery: Breast Reduction This guide is for women who are considering having an operation to lift their breasts. We advise that you talk to a plastic surgeon
PROCEDURE FACT SHEET PLASTIC SURGERY Cosmetic Surgery: Breast Reduction This guide is for women who are considering having an operation to lift their breasts. We advise that you talk to a plastic surgeon
MICHAEL J. BROWN, M.D., P.L.L.C.
 MICHAEL J. BROWN, M.D., P.L.L.C. Aesthetic Cosmetic Plastic Surgery INFORMED-CONSENT OPEN CAPSULECTOMY WITH BREAST IMPLANT EXCHANGE INSTRUCTIONS This is an informed-consent document that has been prepared
MICHAEL J. BROWN, M.D., P.L.L.C. Aesthetic Cosmetic Plastic Surgery INFORMED-CONSENT OPEN CAPSULECTOMY WITH BREAST IMPLANT EXCHANGE INSTRUCTIONS This is an informed-consent document that has been prepared
Considering Breast Enhancement
 Consent Form While every effort has been made by Allergan to ensure the accuracy of the information contained in this booklet, Allergan accepts no responsibility and/or liability for errors or omissions.
Consent Form While every effort has been made by Allergan to ensure the accuracy of the information contained in this booklet, Allergan accepts no responsibility and/or liability for errors or omissions.
Breast Augmentation - Silicone Implants
 Breast Augmentation - Silicone Implants Breast augmentation, or augmentation mammoplasty, is one of the most common plastic surgery procedures performed today. Over time, factors such as age, genetics,
Breast Augmentation - Silicone Implants Breast augmentation, or augmentation mammoplasty, is one of the most common plastic surgery procedures performed today. Over time, factors such as age, genetics,
INFORMED CONSENT BREAST IMPLANT EXPLORATION
 . Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
Informed consent Breast implant removal
 Informed consent Breast implant removal Instructions This is an informed-consent document that has been prepared to help inform you about the removal of breast implant(s), its risks, and alternative treatment(s).
Informed consent Breast implant removal Instructions This is an informed-consent document that has been prepared to help inform you about the removal of breast implant(s), its risks, and alternative treatment(s).
Surgery Choices for Breast Cancer
 Surgery Choices for Breast Cancer Surgery Choices for Women with DCIS or Breast Cancer As a woman with DCIS (ductal carcinoma in situ) or breast cancer that can be removed with surgery, you may be able
Surgery Choices for Breast Cancer Surgery Choices for Women with DCIS or Breast Cancer As a woman with DCIS (ductal carcinoma in situ) or breast cancer that can be removed with surgery, you may be able
Individual Women. Individual Choices. onsidering Breast CEnhancement
 While every effort has been made to ensure the accuracy of the information contained in this booklet, Allergan accepts no responsibility and/or liability for errors or omissions. The information contained
While every effort has been made to ensure the accuracy of the information contained in this booklet, Allergan accepts no responsibility and/or liability for errors or omissions. The information contained
INFORMED-CONSENT- AUGMENTATION MAMMOPLASTY
 INFORMED-CONSENT- AUGMENTATION MAMMOPLASTY Instructions This is an informed-consent document that has been prepared to help inform you about augmentation mammoplasty, its risks, and alternative treatments.
INFORMED-CONSENT- AUGMENTATION MAMMOPLASTY Instructions This is an informed-consent document that has been prepared to help inform you about augmentation mammoplasty, its risks, and alternative treatments.
Important Information. about Mentor MemoryGel Silicone Gel-Filled Breast Implants
 Important Information for Augmentation Patients about Mentor MemoryGel Silicone Gel-Filled Breast Implants 1 Important Information for Augmentation Patients about Mentor MemoryGel Silicone gel-filled
Important Information for Augmentation Patients about Mentor MemoryGel Silicone Gel-Filled Breast Implants 1 Important Information for Augmentation Patients about Mentor MemoryGel Silicone gel-filled
Prophylactic Mastectomy & Reconstructive Implications
 Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
it is normal to show up on the morning of surgery and still be unsure of the fi nal size implant we will choose with you.
 BREAST AUGMENTATION When most people hear the words breast augmentation they usually think of Playboy playmates, Dolly Parton or Pamela Anderson types. There is another group of less visible patients who
BREAST AUGMENTATION When most people hear the words breast augmentation they usually think of Playboy playmates, Dolly Parton or Pamela Anderson types. There is another group of less visible patients who
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Medical Policy Original Effective Date: Revised Date: Page 1 of 8
 Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Breast implants What types of implants are available Under or On top of muscle placement of breast implants Miss Anita Hazari MBBS, MD, FRCS (Plast)
 Breast implants What types of implants are available Breast implants may be referred to as Breast Augmentation. There are two types of implants that are commonly used in the UK - Silicone and Saline. Both
Breast implants What types of implants are available Breast implants may be referred to as Breast Augmentation. There are two types of implants that are commonly used in the UK - Silicone and Saline. Both
COSMETIC SURGERY: BREAST REDUCTION FOR MEN (GYNAECOMASTIA)
 PROCEDURE FACT SHEET PLASTIC SURGERY COSMETIC SURGERY: BREAST REDUCTION FOR MEN (GYNAECOMASTIA) This is a guide for men who are considering having a breast reduction operation. We advise that you talk
PROCEDURE FACT SHEET PLASTIC SURGERY COSMETIC SURGERY: BREAST REDUCTION FOR MEN (GYNAECOMASTIA) This is a guide for men who are considering having a breast reduction operation. We advise that you talk
INFORMED- CONSENT- BREAST IMPLANT REMOVAL SURGERY
 INFORMED- CONSENT- BREAST IMPLANT REMOVAL SURGERY INSTRUCTIONS This is an informed- consent document that has been prepared to help your plastic surgeon inform you concerning breast implant removal, its
INFORMED- CONSENT- BREAST IMPLANT REMOVAL SURGERY INSTRUCTIONS This is an informed- consent document that has been prepared to help your plastic surgeon inform you concerning breast implant removal, its
No Drain Abdominoplasty: No More Excuses. Karol A Gutowski, MD, FACS
 No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Disclosures NO financial interests in any suture company Will use brand names due to lack of distinguishing generic names Objectives
No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Disclosures NO financial interests in any suture company Will use brand names due to lack of distinguishing generic names Objectives
Patient Educational Brochure RECONSTRUCTION. Breast Reconstruction with MENTOR MemoryGel Silicone Gel Breast Implants
 Patient Educational Brochure RECONSTRUCTION Breast Reconstruction with MENTOR MemoryGel Silicone Gel Breast Implants 1 PATIENT EDUCATIONAL BROCHURE RECONSTRUCTION BREAST RECONSTRUCTION WITH MENTOR MEMORYGEL
Patient Educational Brochure RECONSTRUCTION Breast Reconstruction with MENTOR MemoryGel Silicone Gel Breast Implants 1 PATIENT EDUCATIONAL BROCHURE RECONSTRUCTION BREAST RECONSTRUCTION WITH MENTOR MEMORYGEL
Mommy Makeover
 Mommy Makeover Many women experience significant physical changes following pregnancy and breast-feeding, many of which can be persistent and difficult to correct with diet and exercise alone. Changes
Mommy Makeover Many women experience significant physical changes following pregnancy and breast-feeding, many of which can be persistent and difficult to correct with diet and exercise alone. Changes
Breast Reconstruction
 Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Barbed Sutures in Progressive Tension Suture Technique Abdominoplasty. Karol A Gutowski, MD
 Barbed Sutures in Progressive Tension Suture Technique Abdominoplasty Karol A Gutowski, MD 1 Disclosures Speakers Bureau for AngioTech since April 2011 (Makers of Quill bi-directional barbed sutures) Technique
Barbed Sutures in Progressive Tension Suture Technique Abdominoplasty Karol A Gutowski, MD 1 Disclosures Speakers Bureau for AngioTech since April 2011 (Makers of Quill bi-directional barbed sutures) Technique
INFORMED CONSENT BREAST IMPLANT REMOVAL & BREAST LIFT
 . Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein and reproduce the modified version for use in the Purchaser's own practice only.
Information For Women AMERICAN SOCIETYOF PLASTIC SURGEONS
 Information For Women AMERICAN SOCIETYOF PLASTIC SURGEONS CONTENTS What are silicone implants?.............................................................4 Risks related to silicone gel-filled implants.................................................5
Information For Women AMERICAN SOCIETYOF PLASTIC SURGEONS CONTENTS What are silicone implants?.............................................................4 Risks related to silicone gel-filled implants.................................................5
Information on breast reconstruction (Tissue expansion)
 Information on breast reconstruction (Tissue expansion) This information sheet explains the implications of breast reconstruction surgery and should be read in addition to the Breast Cancer Care booklet
Information on breast reconstruction (Tissue expansion) This information sheet explains the implications of breast reconstruction surgery and should be read in addition to the Breast Cancer Care booklet
Mastectomy. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Mastectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this brochure
Mastectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this brochure
IMPORTANT INFORMATION FOR AUGMENTATION PATIENTS ABOUT MENTOR MEMORYGEL SILICONE GEL-FILLED BREAST IMPLANTS August 2006
 1 Canadian IMPORTANT INFORMATION FOR AUGMENTATION PATIENTS ABOUT MENTOR MEMORYGEL SILICONE GEL-FILLED BREAST IMPLANTS August 2006 2 11859-00 1 Important Information for Augmentation Patients About Mentor
1 Canadian IMPORTANT INFORMATION FOR AUGMENTATION PATIENTS ABOUT MENTOR MEMORYGEL SILICONE GEL-FILLED BREAST IMPLANTS August 2006 2 11859-00 1 Important Information for Augmentation Patients About Mentor
A Combined Practice. Why Its Worked. Barriers to Breast Reconstruction. As a breast oncologist the patient gets seemless care
 A Combined Practice A Combined Breast Oncology and Plastic Surgery Practice Why It Works Anne M. Wallace, MD, FACS Director, Comprehensive Breast Health Center Professor of Clinical Surgery, Surgical Oncology
A Combined Practice A Combined Breast Oncology and Plastic Surgery Practice Why It Works Anne M. Wallace, MD, FACS Director, Comprehensive Breast Health Center Professor of Clinical Surgery, Surgical Oncology
inding the fit that s right for you. Your Surgery Planner For Augmentation Surgery with NATRELLE Silicone-Filled Breast Implants
 inding the fit that s right for you. Your Surgery Planner For Augmentation Surgery with NATRELLE Silicone-Filled Breast Implants L Place Your Device Identification Card(s) Here R ACCEPTANCE OF RISK AND
inding the fit that s right for you. Your Surgery Planner For Augmentation Surgery with NATRELLE Silicone-Filled Breast Implants L Place Your Device Identification Card(s) Here R ACCEPTANCE OF RISK AND
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
B02 Mastectomy. Expires end of November Write questions or notes here:
 Practice Locations: St John of God Consulting Suites, 117 Anstruther Road, Mandurah Suite 50, Murdoch Medical Centre, 100 Murdoch Drive, Murdoch Tel: 08 6333 2800 Web: saudhamza.com.au B02 Mastectomy Expires
Practice Locations: St John of God Consulting Suites, 117 Anstruther Road, Mandurah Suite 50, Murdoch Medical Centre, 100 Murdoch Drive, Murdoch Tel: 08 6333 2800 Web: saudhamza.com.au B02 Mastectomy Expires
Augmentation BREAST AUGMENTATION WITH NATRELLE SILICONE-FILLED BREAST IMPLANTS AND NATRELLE INSPIRA BREAST IMPLANTS
 Augmentation BREAST AUGMENTATION WITH NATRELLE SILICONE-FILLED BREAST IMPLANTS AND NATRELLE INSPIRA BREAST IMPLANTS Table of Contents Glossary... 2 1. Considering Silicone Gel-Filled Breast Implant Surgery...11
Augmentation BREAST AUGMENTATION WITH NATRELLE SILICONE-FILLED BREAST IMPLANTS AND NATRELLE INSPIRA BREAST IMPLANTS Table of Contents Glossary... 2 1. Considering Silicone Gel-Filled Breast Implant Surgery...11
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
IMPORTANT INFORMATION FOR RECONSTRUCTION PATIENTS ABOUT MENTOR MEMORYGEL SILICONE GEL-FILLED BREAST IMPLANTS August 2006
 11859-00 1 Canadian IMPORTANT INFORMATION FOR RECONSTRUCTION PATIENTS ABOUT MENTOR MEMORYGEL SILICONE GEL-FILLED BREAST IMPLANTS August 2006 2 11859-00 11860-00 1 IMPORTANT INFORMATION FOR RECONSTRUCTION
11859-00 1 Canadian IMPORTANT INFORMATION FOR RECONSTRUCTION PATIENTS ABOUT MENTOR MEMORYGEL SILICONE GEL-FILLED BREAST IMPLANTS August 2006 2 11859-00 11860-00 1 IMPORTANT INFORMATION FOR RECONSTRUCTION
Post-mastectomy breast reconstruction
 Follow the link from the online version of this article to obtain certified continuing medical education credits Post-mastectomy breast reconstruction Paul T R Thiruchelvam, 1 Fiona McNeill, 2 Navid Jallali,
Follow the link from the online version of this article to obtain certified continuing medical education credits Post-mastectomy breast reconstruction Paul T R Thiruchelvam, 1 Fiona McNeill, 2 Navid Jallali,
Breast Augmentation with NATRELLE Silicone-Filled Breast Implants
 Breast Augmentation with NATRELLE Silicone-Filled Breast Implants AUG Patient Labeling Rev 4/6/09 page 1 TABLE OF CONTENTS Page GLOSSARY... 3 1.0 CONSIDERING SILICONE GEL-FILLED BREAST IMPLANT SURGERY...
Breast Augmentation with NATRELLE Silicone-Filled Breast Implants AUG Patient Labeling Rev 4/6/09 page 1 TABLE OF CONTENTS Page GLOSSARY... 3 1.0 CONSIDERING SILICONE GEL-FILLED BREAST IMPLANT SURGERY...
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Strattice Reconstructive Tissue Matrix used in the repair of rippling
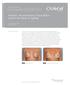 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
No Drain Abdominoplasty: No More Excuses. Karol A Gutowski, MD, FACS Instructional Course
 No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Instructional Course Disclosures Angiotech/Surgical Specialties - Advisory Board AxcelRx Pharmacuticals - Advisory Board Suneva Medical
No Drain Abdominoplasty: No More Excuses Karol A Gutowski, MD, FACS Instructional Course Disclosures Angiotech/Surgical Specialties - Advisory Board AxcelRx Pharmacuticals - Advisory Board Suneva Medical
INFORMED-CONSENT-AUGMENTATION MAMMAPLASTY
 INFORMED-CONSENT-AUGMENTATION MAMMAPLASTY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein
INFORMED-CONSENT-AUGMENTATION MAMMAPLASTY 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify documents contained herein
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read this
Functional rehab after breast reconstruction surgery A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read this
Breast augmentation (enlargement)
 Breast augmentation is a surgical procedure that uses breast implants to enhance shape or increase the size of a woman s breast after body changes such as pregnancy, weight loss or from natural ageing.
Breast augmentation is a surgical procedure that uses breast implants to enhance shape or increase the size of a woman s breast after body changes such as pregnancy, weight loss or from natural ageing.
Delayed implant based breast reconstruction
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient Delayed implant based breast reconstruction affix patient label What is a delayed implant breast reconstruction?
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient Delayed implant based breast reconstruction affix patient label What is a delayed implant breast reconstruction?
National Mastectomy & Breast Reconstruction Audit Datasheet - Mastectomy +/- Immediate Reconstruction
 Patient Registration data Surname Forename NHS/Private Hospital Number Date of birth Postcode Ethnicity Patient-reported outcomes consent Has this patient consented to being sent outcome questionnaires?
Patient Registration data Surname Forename NHS/Private Hospital Number Date of birth Postcode Ethnicity Patient-reported outcomes consent Has this patient consented to being sent outcome questionnaires?
-AESTETICA- Plastic Surgery Clinic JACEK JARLINSKI, MD, PhD plastic surgeon
 -AESTETICA- Plastic Surgery Clinic JACEK JARLINSKI, MD, PhD plastic surgeon www.aestetica.pl Contact: Jacek Jarlinski, MD, PhD tel. +48 600 208 208 jarlinski@aestetica.pl Piotr Jarlinski, MD tel. +48 601
-AESTETICA- Plastic Surgery Clinic JACEK JARLINSKI, MD, PhD plastic surgeon www.aestetica.pl Contact: Jacek Jarlinski, MD, PhD tel. +48 600 208 208 jarlinski@aestetica.pl Piotr Jarlinski, MD tel. +48 601
Breast Augmentation - Saline Implants
 Breast Augmentation - Saline Implants Breast augmentation, or augmentation mammoplasty, is one of the most common plastic surgery procedures performed today. Over time, factors such as age, genetics, pregnancy,
Breast Augmentation - Saline Implants Breast augmentation, or augmentation mammoplasty, is one of the most common plastic surgery procedures performed today. Over time, factors such as age, genetics, pregnancy,
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
ONCOPLASTIC SURGERY. Dr. Sadir Alrawi Director of Surgical Oncology Services. Dr. Humaa Darr Surgical Oncology Fellow
 Hessa St ONCOPLASTIC SURGERY Dr. Sadir Alrawi Director of Surgical Oncology Services Dr. Humaa Darr Surgical Oncology Fellow Al Sufouh Rd AL SUFOUH AL SUFOUH Sharaf DG Mall of the Emirates Mall Of the
Hessa St ONCOPLASTIC SURGERY Dr. Sadir Alrawi Director of Surgical Oncology Services Dr. Humaa Darr Surgical Oncology Fellow Al Sufouh Rd AL SUFOUH AL SUFOUH Sharaf DG Mall of the Emirates Mall Of the
All surgery carries some uncertainty and risk
 Dr Mi chel s on@mi chel s onmd. com All surgery carries some uncertainty and risk While scar revision is normally safe, there is always the possibility of complications. These may include infection, bleeding,
Dr Mi chel s on@mi chel s onmd. com All surgery carries some uncertainty and risk While scar revision is normally safe, there is always the possibility of complications. These may include infection, bleeding,
Exercises After Breast Surgery
 PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massag e after your breast surg ery. Starting
PATIENT & CAREGIVER EDUCATION Exercises After Breast Surgery This information describes how to do arm and shoulder exercises, a breathing exercise, and scar massag e after your breast surg ery. Starting
Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position
 Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
What are the different techniques used for chest surgery?
 Chest Surgery Chest surgery is a gender-affirming, masculinizing, top surgery that removes breast* tissue and forms remaining tissue into a shape that is typically considered to be more masculine. What
Chest Surgery Chest surgery is a gender-affirming, masculinizing, top surgery that removes breast* tissue and forms remaining tissue into a shape that is typically considered to be more masculine. What
INFORMATION SHEET MODIFIED (MINI) ABDOMINOPLASTY
 INFORMATION SHEET MODIFIED (MINI) ABDOMINOPLASTY INTRODUCTION There is not much which is mini about a mini-abdominoplasty because it can take as long and can be as complicated as a standard abdominoplasty
INFORMATION SHEET MODIFIED (MINI) ABDOMINOPLASTY INTRODUCTION There is not much which is mini about a mini-abdominoplasty because it can take as long and can be as complicated as a standard abdominoplasty
Your comprehensive guide to BREAST LIFT SURGERY. (07) cosmedic.com.au
 Your comprehensive guide to BREAST LIFT SURGERY (07) 5588 4777 cosmedic.com.au Breast Lift Surgery Breast lift, or Mastopexy, is designed to recreate the appearance of firm and more youthful breasts. Whether
Your comprehensive guide to BREAST LIFT SURGERY (07) 5588 4777 cosmedic.com.au Breast Lift Surgery Breast lift, or Mastopexy, is designed to recreate the appearance of firm and more youthful breasts. Whether
Breast Surgery. for Reconstructive. Center of Excellence. city center of Düsseldorf. You will find us in the
 You will find us in the city center of Düsseldorf Rathaus Rhein Steinstraße Berger Allee Poststraße Bastionstraße Kasernenstraße Breite Straße Königsallee Grünstraße Berliner Allee Königsallee 88 Graf-Adolf-Platz
You will find us in the city center of Düsseldorf Rathaus Rhein Steinstraße Berger Allee Poststraße Bastionstraße Kasernenstraße Breite Straße Königsallee Grünstraße Berliner Allee Königsallee 88 Graf-Adolf-Platz
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
