Copyright 2016 Wolters Kluwer Health, Inc. Unauthorized reproduction of this article is prohibited.
|
|
|
- Arabella Banks
- 5 years ago
- Views:
Transcription
1 SPINE An International Journal for the study of the spine Publish Ahead of Print DOI : /BRS How Effective is Physical Therapy for Common Low Back Pain Diagnoses? A multivariate analysis of 4597 patients. Ananth S. Eleswarapu MD 1, Srikanth N. Divi MD 1, Douglas R. Dirschl MD 1, James M. Mok MD 1, Christopher Stout PhD 2,3, Michael J. Lee MD 1 1 University of Chicago Medical Center Chicago IL 2 ATI, Bolingbrook IL 3 University of Illinois at Chicago, College of Medicine Chicago, IL Please send all correspondence to: Ananth S. Eleswarapu, MD Department of Orthopaedic Surgery, University of Chicago Medical Center 5841 S. Maryland Avenue, MC 3079 Chicago, IL Ananth.eleswarapu@uchospitals.edu
2 Acknowledgement: October 12, 2015 Revise: January 5, 2016 Accept: January 25, 2016 The manuscript submitted does not contain information about medical device(s)/drug(s). No funds were received in support of this work. Relevant financial activities outside the submitted work: consultancy, grants, payment for development of educational presentations.
3 Structured Abstract Study Design: Retrospective review Objective: To evaluate whether the treatment of low back pain with physical therapy results in clinically significant improvements in patient-reported pain and functional outcomes. Summary of Background Data: Low back pain is a major cause of morbidity and disability in health care. Previous studies have found poor efficacy for surgery in the absence of specific indications. A variety of non-operative treatments are available, however there is scant evidence to guide the practitioner as to the efficacy of these treatments. Methods: 4597 patients who underwent physical therapy for the non-operative treatment of low back pain were included. The primary outcome measures were pre- and post-treatment scores on the Oswestry Disability Index (ODI), Numeric Pain Rating Scale (NPRS) during activity, and NPRS during rest. Previously published thresholds for minimal clinically important difference (MCID) were used to determine the proportion of patients meeting MCID for each of our outcomes. Patients with starting values below the MCID for each variable were excluded from analysis. Logistic regression analysis was used to determine patient risk factors predictive of treatment failure. Results: 28.5% of patients met the MCID for improvement in ODI. Presence of night symptoms, obesity, and smoking were predictors of treatment failure for ODI. 59% of patients met the MCID for improvement in resting NPRS, with history of venous thromboembolism, night symptoms, psychiatric disease, workers compensation status, smoking, and obesity predictive of treatment failure. 60% of patients met the MCID for improvement in activity
4 NPRS, with night symptoms, workers compensation status, and smoking predictive of treatment failure. Conclusions: We observed a substantial percentage of the population did not meet MCID for pain and function following treatment of low back pain with physical therapy. Common risk factors for treatment failure included smoking and presence of night symptoms. Key Words: low back pain; lumbago; physical therapy; outcomes; disc herniation; spinal stenosis; spondylolisthesis; numeric pain rating scale; Oswestry Disability Index; minimum clinically important difference Level of Evidence: 4
5 Introduction Low back pain continues to be a highly prevalent and challenging condition to manage. In addition, it continues to be a major cause of disability and morbidity in health care[1-5]. The etiology of back pain is multifactorial. While diagnoses including deformity, stenosis, instability, neoplasm and infection are generally thought to be amenable to surgical treatment, the management of axial low back pain in the absence of the aforementioned conditions remains challenging. There is no clear consensus on its optimal treatment. Treatment for this type of axial low back pain has included physical therapy, acupuncture, chiropractic care, injection and surgery. Numerous studies have called into question the effectiveness of these treatments, particularly surgery, for low back pain[3, 5, 6]. Furthermore, the utilization and costs of surgery have increased significantly over the past two decades[6]. Extensive discussion in the literature on the effectiveness of surgical treatment has led to increased payor oversight. In comparison, there has been relatively little discussion regarding the effectiveness of non-surgical treatments of low back pain. However, a recent systematic review reported that the while the costs of surgery accounted for 5% of expenditures on chronic low back pain, physical therapy accounted for 17% of these expenditures[7]. The Oswestry Disability Index (ODI) and Numeric Pain Rating Scales (NPRS) are commonly utilized and previously validated measures of patient reported outcome for spinal conditions[8-10]. The effectiveness for treatment of lumbar spinal conditions has been assessed by using minimal clinically important difference (MCID) thresholds in both NPRS as well as the ODI[8, 9, 11, 12]. If patients score improvements with treatment do not exceed these MCID thresholds, the treatment is considered to be not effective for the condition.
6 We hypothesized that physical therapy would result in improved ODI and NPRS scores in patients with common low back pain diagnoses. The purpose of this study was to evaluate the effectiveness of physical therapy treatment for common low back pain by assessing whether MCID thresholds for NPRS and ODI changes were met following treatment. This investigation further sought to determine if any patient factors were associated with lack of improvement in these measures. Materials and Methods Data Source Data was drawn from a registry maintained by a national commercial physical therapy organization. Consecutive patients undergoing physical therapy for low back pain-related diagnoses (lumbar sprain, lumbar disc displacement, lumbago, and lumbosacral spondylosis) from September 9, 2013 to April 22, 2015 were enrolled into a prospective database. Data was available on 40 variables comprising demographic information, comorbidities, and pre- and posttreatment outcome scores. Post-surgical patients were excluded from this dataset. In total, data was available on 4597 patients undergoing physical therapy for low back pain. Data Analysis Pre-treatment demographic and risk factors collected included age, gender, body mass index, tobacco use, payor status, duration of treatment, comorbid diagnoses (history of diabetes, hypertension, osteoporosis, stroke, venous thromboembolism, malignancy, respiratory, renal, cardiac, or psychiatric conditions), and symptomatology (sexual dysfunction, nighttime symptoms, or groin numbness). Clinical outcomes included pre- and post-treatment scores on
7 the Oswestry Disability Index (ODI) and Numeric Pain Rating Scale (NPRS). NPRS scores were recorded both at rest and during activity. For each of the three outcome scores (ODI, resting NPRS, and activity NPRS), success of treatment was defined as achievement of a minimal clinically important difference (MCID) between pre- and post-treatment scores. Previously published low back pain-specific thresholds for MCID were used. For ODI, the threshold was set at 10 points improvement from pre- to post-treatment score (on a scale of 0 to 100); for NPRS, the threshold was set at 2 points improvement (on a scale of 0 to 10)[8, 9]. Microsoft Excel (Microsoft Corp., Redmond, WA) was used for data analysis. Each of the 3 clinical outcome variables was analyzed separately. For our analysis of ODI, patients with starting scores below the 10 were excluded as by definition they could not meet the MCID for improvement. For the remaining patients, the average pre- and post-treatment scores were calculated as well as the percentage of patients meeting or exceeding the MCID for improvement. Paired two sample t test was utilized to assess the means pre and post treatment. Bivariate analysis of pre-treatment demographic and risk factors was performed to identify factors associated with failure to meet MCID. Chi-square test was used with a threshold of p < 0.1 for significance. Pre-treatment risk factors meeting this threshold of significance were then included in a logistic regression model to identify independent predictors of treatment failure. A similar analysis was performed for activity and resting NPRS.
8 Results Population Averages 4597 patients were included for analysis. The average number of visits was 14. Average duration of therapy was 44.6 days (Table 1). Oswestry Disability Index Of 4597 total patients, 986 were excluded due to a starting ODI less than the MCID of 10. This left 3611 patients for analysis. The average score prior to therapy was 20.9 and following therapy was For the sample as a whole, the average ODI score improved from 20.9 to 15.3, for an average improvement of 5.6 points (SEM 0.13, p <.001). 28.5% of patients achieved the MCID of 10 points improvement (Table 2). In logistic regression analysis, night symptoms, obesity, and smoking were independent predictors of failure to meet MCID for ODI (Table 3). Resting Visual Analog Scale 1503 patients were excluded due to a starting resting NPRS less than the MCID of 2. Thus, 3094 patients were included for analysis. The average score pre-treatment was 4.4 and post-treatment was 2.3, for an average improvement of 2.1 points (SEM 0.04, p<.001). 59% of patients met the MCID for improvement (Table 2). In logistic regression analysis, history of venous thromboembolism, night symptoms, psychiatric history, workers compensation status, smoking, and obesity were all predictive of failure to meet MCID. Osteoporosis was associated with an increased rate of meeting MCID for improvement (Table 4).
9 Activity Visual Analog Scale 427 patients were excluded due to a starting activity NPRS less than the MCID of 2, leaving 4170 patients for analysis. The average score pre-treatment was 7.2 and post-treatment was 4.5, for an average improvement of 2.7 points (SEM 0.04, p <.001). 60% of patients met the MCID for improvement (Table 2). In logistic regression analysis, night symptoms, workers compensation status, and smoking were independent predictors of failure to meet MCID for improvement. History of cancer was associated with increased odds of meeting MCID for improvement (Table 5). Discussion The treatment of back pain continues to be extremely challenging. Numerous causes of back pain such as spondylolisthesis, scoliosis, neoplasm, infection, and neuro-compressive pathology are generally thought to be responsive to surgical and non-surgical treatment. However, other causes of axial back pain (such as lumbago, lumbar strain, disc degeneration, disc displacement, and spondylosis), have been suggested to be less effectively treated, particularly by surgery[3, 5]. To our knowledge, there is scant quality literature examining the effectiveness of non-surgical treatment for these common low back pain diagnoses using patient reported outcomes. We sought to examine the effectiveness of physical therapy for these LBP diagnoses. MCID thresholds for patient reported outcome measures should be regarded cautiously. There are numerous ways of creating and calculating these thresholds utilizing absolute or percentage improvement[11-14]. The outcome of the analysis and subsequent interpretation of the data may be affected by the choice of threshold. For ODI, MCID thresholds have ranged
10 from 8.2 to 19.9[11-14]. For NPRS, MCID thresholds have ranged from 1.2 to 4.5[11-14]. Based on our review of the literature, we selected MCID for ODI to be 10 and for NPRS to be 2.0. Interestingly, we observed that a substantial percentage of this population did not achieve MCID after physical therapy. For ODI, 71.5% of patients did not achieve a MCID threshold of 10 points improvement. For resting NPRS, 41% of patients did not achieve the MCID of 2 points improvement. For activity NPRS, 40% of patients did not achieve MCID of 2 points improvement. This may be a function of co-occurring comorbidities. Using multiple logistic regression analysis in a large prospective data registry, we identified statistically significant risk factors for not achieving MCID after PT for common LBP causes (Tables 3-5). Common risk factors across resting NPRS, activity NPRS and ODI included smoking and night pain. Our data suggest that patients with these risk factors are less likely to have their low back pain successfully treated with physical therapy. Rodeghero et al performed a similar analysis to the present study. In their study, they evaluated 6379 patients using a data registry compiled by Focus on Therapeutic Outcomes Inc. (FOTO) (Knoxville TN, USA.)[15] Whereas our study examines previously validated patient reported outcomes such as NPRS and ODI, they utilized Patient Inquiry, which is a computer program developed by FOTO. It is unclear how the Patient Inquiry differs from other patient reported outcome measures. In their analysis, they report age, duration of symptoms, insurance, and medication use as significant risk factors for poor outcome. The findings in our study seemingly call into question the effectiveness of PT for common LBP diagnoses, particularly as a high percentage of patients did not achieve MCID in
11 NPRS or ODI. However the decision to prescribe physical therapy for LBP should be assessed in the context of each patient s unique situation. From a safety standpoint, physical therapy is vastly superior to interventional treatments such as injections or surgery. While the likelihood of achieving MCID may be considered low, the likelihood for harm from complication is also low, at least in comparison to other treatments. Thus from a risk-benefit analysis of various treatments for common LBP diagnoses, physical therapy is still advisable in the majority of patients, particularly as a first line of treatment. The cost effectiveness of physical therapy for common LBP diagnoses, however, is unclear. Prior literature has suggested that PT for LBP may account for more than three times the cost of surgical treatment [16]. Cost effectiveness analysis was outside the scope of the present study and future study is required. There are some weaknesses of our study that should be noted. The entry of co-variate data such as co-morbidities was dependent upon the infrastructure of a nationwide physical therapy group. These data were entered by patient self-report as categorical and not continuous and thus have limited granularity for analysis. Furthermore, all potential confounding covariates may not have been recorded. For example, duration of symptoms prior to PT was not prospectively recorded. Thus, our analysis of risk factors for not achieving MCID should be interpreted cautiously. Secondly, the exact physical therapy provided may not be uniform across the patient population. While there have been several randomized controlled trials that have compared the efficacy of various PT modalities for this diagnosis, there is still a lack of consensus on a specific treatment protocol, and decisions as to which modality to employ are often made by the individual therapist. Our intention with this study was not to conduct a well-controlled trial
12 comparing the efficacy of various PT modalities, but rather to document the real-world effectiveness of PT as currently practiced, as well as identifying patient factors predictive of outcome. We believe this information will be useful to primary care physicians and spine specialists who must choose where to initially refer patients presenting with nonspecific low back pain (PT, pain clinic, advanced imaging, etc.). Finally, our follow-up ranged from one week to 35 weeks. Long-term follow-up and data are not available. It is unclear if patients continued to perform learned exercises on their own afterwards and how well they fared. However, there are strengths to this study. First, this registry prospectively recorded pre and post treatment validated patient reported outcomes data (NPRS, ODI), which allows for a direct assessment of effectiveness. Secondly, the sheer size of this sample population allows for the identification and quantification of significant risk factors using multivariate analysis. While there is likely some heterogeneity in how some risk factor data were collected, other risk factors such as payor status and obesity are likely to be collected more homogenously. A data set of this size can allow for analysis of some of these risk factors. In conclusion, physical therapy for common LBP can be effective for patients, however it would be prudent to consider risk factors for poor outcome. Though generally considered safe when compared to other treatments of common LBP diagnoses, future analyses in cost are needed to determine the true value of physical therapy in this patient population.
13 References 1. Chapman JR, Norvell DC, Hermsmeyer JT, et al. Evaluating common outcomes for measuring treatment success for chronic low back pain. Spine 2011;36(21 Suppl):S Maetzel A and Li L. The economic burden of low back pain: a review of studies published between 1996 and Best Practice & Research Clinical Rheumatology 2002;16: Mirza SK and Deyo RA. Systematic review of randomized trials comparing lumbar fusion surgery to nonoperative care for treatment of chronic back pain. Spine 2007;32: Standaert CJ, Friedly J, Erwin MW, et al. Comparative effectiveness of exercise, acupuncture, and spinal manipulation for low back pain. Spine 2011;36(21 Suppl):S Turner JA, Ersek M, Herron L, et al. Patient outcomes after lumbar spinal fusions. Journal of the American Medical Association 1992;268: Deyo RA, Gray DT, Kreuter W, et al. United States trends in lumbar fusion surgery for degenerative conditions. Spine 2005;30: Dagenais S, Caro J, and Haldeman S. A systematic review of low back pain cost of illness studies in the United States and internationally. The Spine Journal 2008;8: Childs JD, Piva SR, and Fritz JM. Responsiveness of the numeric pain rating scale in patients with low back pain. Spine 2005;30: Davidson M and Keating JL. A comparison of five low back disability questionnaires: reliability and responsiveness. Physical Therapy 2002;82: Devine J, Norvell DC, Ecker E, et al. Evaluating the correlation and responsiveness of patient-reported pain with function and quality-of-life outcomes after spine surgery. Spine 2011;36(21 Suppl):S69-74.
14 11. Parker SL, Mendenhall SK, Shau DN, et al. Minimum clinically important difference in pain, disability, and quality of life after neural decompression and fusion for same-level recurrent lumbar stenosis: understanding clinical versus statistical significance. Journal of Neurosurgery: Spine 2012;16: Paul AR, Kumar V, Roth SG, et al. 126 Determining the minimally clinical important difference in pain, quality of life, and disability for failed neck and failed back syndromes. Neurosurgery 2015;62 Suppl 1: Copay AG, Glassman SD, Subach BR, et al. Minimum clinically important difference in lumbar spine surgery patients: a choice of methods using the Oswestry Disability Index, Medical Outcomes Study questionnaire Short Form 36, and pain scales. The Spine Journal 2008;8: Van der Roer N, Ostelo RW, Bekkering GE, et al. Minimal clinically important change for pain intensity, functional status, and general health status in patients with nonspecific low back pain. Spine 2006;31: Rodeghero JR, Cook CE, Cleland JA, et al. Risk stratification of patients with low back pain seen in physical therapy practice. Manual Therapy 2015 (epub ahead of print). 16. Dagenais S, Caro J, and Haldeman S. A systematic review of low back pain cost of illness studies in the United States and internationally. The Spine Journal 2008;8:8-20.
15 Table 1: Population Averages Average Standard Deviation Number of visits Duration of therapy (days) Table 2: First vs final evaluation outcome scores Outcome Score Average First Evaluation Score Average Final Evaluation Score Average Difference 95% CI % Achieving MCID ODI ( ) 28.5% Resting NPRS ( ) 59.0% Activity NPRS ( ) 60.0% Table 3 Risk factors associated with failure to meet MCID for ODI in logistic regression analysis Risk Factor Adjusted Odds 95% CI p value Ratio Night Sweats / Night Pain 1.64 ( ) p <.001 BMI > ( ) p =.001 Smoking 1.26 ( ) p =.029
16 Table 4 Risk factors associated with failure to meet MCID for resting NPRS in logistic regression analysis Risk Factor Adjusted Odds 95% CI p value Ratio History of Blood Clot / DVT 1.84 ( ) P =.006* Night Sweats / Night Pain 1.39 ( ) p <.001* Psychological Condition 1.36 ( ) p =.029* Workers Compensation Status 1.35 ( ) p =.003* Smoking 1.30 ( ) p =.008* BMI > ( ) p =.002* Osteoporosis 0.72 ( ) p =.028* Table 5 Risk factors associated with failure to meet MCID for activity NPRS in logistic regression analysis Risk Factor Adjusted 95% CI p value Odds Ratio Night Sweats / Night Pain 1.43 ( ) p <.001* Workers Compensation Status 1.38 ( ) p =.001* Smoking 1.30 ( ) P =.003* History of Cancer 0.77 ( ) p =.049*
YOU ARE THE BEST OPTION FOR LOW BACK PAIN
 YOU ARE THE BEST OPTION FOR LOW BACK PAIN Amy Garrigues PT, DPT Orthopaedic Clinical Specialist Fellow, American Academy of Orthopaedic and Manual Physical Therapists LBP in past 3 months 25% 307% 220%
YOU ARE THE BEST OPTION FOR LOW BACK PAIN Amy Garrigues PT, DPT Orthopaedic Clinical Specialist Fellow, American Academy of Orthopaedic and Manual Physical Therapists LBP in past 3 months 25% 307% 220%
Effects of Viewing an Evidence-Based Video Decision Aid on Patients Treatment Preferences for Spine Surgery. ACCEPTED
 Spine Publish Ahead of Print DOI: 10.1097/BRS.0b013e3182055c1e Effects of Viewing an Evidence-Based Video Decision Aid on Patients Treatment Preferences for Spine Surgery. Jon D. Lurie, MD, MS; Kevin F.
Spine Publish Ahead of Print DOI: 10.1097/BRS.0b013e3182055c1e Effects of Viewing an Evidence-Based Video Decision Aid on Patients Treatment Preferences for Spine Surgery. Jon D. Lurie, MD, MS; Kevin F.
Study Design: Prospective observational study of cervical transforaminal epidural steroid injections in patients with cervical radicular pain
 Study Design: Prospective observational study of cervical transforaminal epidural steroid injections in patients with cervical radicular pain Background and Significance To be completed by the project
Study Design: Prospective observational study of cervical transforaminal epidural steroid injections in patients with cervical radicular pain Background and Significance To be completed by the project
Study Design: Prospective observational study of cervical interlaminar injection of steroid in patients with cervical radicular pain
 Study Design: Prospective observational study of cervical interlaminar injection of steroid in patients with cervical radicular pain Background and Significance To be completed by the project s Principal
Study Design: Prospective observational study of cervical interlaminar injection of steroid in patients with cervical radicular pain Background and Significance To be completed by the project s Principal
2016 OPAM Mid-Year Educational Conference, sponsored by AOCOPM Thursday, March 10, 2016 C-1
 Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
Does obesity affect outcomes after decompressive surgery for lumbar spinal stenosis? A multicenter observational registry-based study
 Does obesity affect outcomes after decompressive surgery for lumbar spinal stenosis? A multicenter observational registry-based study Charalampis Giannadakis, Ulf S. Nerland, Ole Solheim, Asgeir S. Jakola,
Does obesity affect outcomes after decompressive surgery for lumbar spinal stenosis? A multicenter observational registry-based study Charalampis Giannadakis, Ulf S. Nerland, Ole Solheim, Asgeir S. Jakola,
SWESPINE THE SWEDISH SPINE REGISTER 2010 REPORT
 SWESPINE THE SWEDISH SPINE REGISTER 21 REPORT SEPTEMBER 21 SWEDISH SOCIETY OF SPINAL SURGEONS Björn Strömqvist Peter Fritzell Olle Hägg Bo Jönsson ISBN 978-91-978553-8-9 Table of Contents 2 Introduction
SWESPINE THE SWEDISH SPINE REGISTER 21 REPORT SEPTEMBER 21 SWEDISH SOCIETY OF SPINAL SURGEONS Björn Strömqvist Peter Fritzell Olle Hägg Bo Jönsson ISBN 978-91-978553-8-9 Table of Contents 2 Introduction
Disability and health-related quality of life in patients undergoing spinal fusion: a comparison with a general population sample
 Pekkanen et al. BMC Musculoskeletal Disorders 13, 14:211 RESEARCH ARTICLE Open Access Disability and health-related quality of life in patients undergoing spinal fusion: a comparison with a general population
Pekkanen et al. BMC Musculoskeletal Disorders 13, 14:211 RESEARCH ARTICLE Open Access Disability and health-related quality of life in patients undergoing spinal fusion: a comparison with a general population
Alan H Daniels, MD. Spine Division, Department of Orthopaedics Warren Alpert School of Medicine of Brown University
 Spinal and Orthopaedic Surgery in the Elderly Alan H Daniels, MD Spine Division, Department of Orthopaedics Warren Alpert School of Medicine of Brown University As the population ages, and patients remain
Spinal and Orthopaedic Surgery in the Elderly Alan H Daniels, MD Spine Division, Department of Orthopaedics Warren Alpert School of Medicine of Brown University As the population ages, and patients remain
KEY WORDS lumbar spine; spinal surgery; surgical effectiveness; surgical outcomes; effective measures; long-term outcomes
 clinical article J Neurosurg Spine 25:689 696, 2016 Do measures of surgical effectiveness at 1 year after lumbar spine surgery accurately predict 2-year outcomes? Owoicho Adogwa, MD, MPH, 1 Aladine A.
clinical article J Neurosurg Spine 25:689 696, 2016 Do measures of surgical effectiveness at 1 year after lumbar spine surgery accurately predict 2-year outcomes? Owoicho Adogwa, MD, MPH, 1 Aladine A.
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Sigita Burneikiene, MD; Alan T. Villavicencio, MD; Alexander Mason, MD; Sharad Rajpal, MD
 The Timing of Surgery and Symptom Resolu6on in Pa6ents Undergoing Transforaminal Lumbar Interbody Fusion for Lumbar Degenera6ve Disc Disease and Radiculopathy Sigita Burneikiene, MD; Alan T. Villavicencio,
The Timing of Surgery and Symptom Resolu6on in Pa6ents Undergoing Transforaminal Lumbar Interbody Fusion for Lumbar Degenera6ve Disc Disease and Radiculopathy Sigita Burneikiene, MD; Alan T. Villavicencio,
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Top spine papers of 2016
 Top spine papers of 2016 Ai Mukai, MD Texas Orthopedics, Sports & Rehabilitation University of Texas-Austin, PM&R Residency October 21, 2016 Top papers in spine? Top papers in Spine How do you define top?
Top spine papers of 2016 Ai Mukai, MD Texas Orthopedics, Sports & Rehabilitation University of Texas-Austin, PM&R Residency October 21, 2016 Top papers in spine? Top papers in Spine How do you define top?
Original Article Clinics in Orthopedic Surgery 2017;9: https://doi.org/ /cios
 Original Article Clinics in Orthopedic Surgery 2017;9:177-183 https://doi.org/10.4055/cios.2017.9.2.177 The Effect of Anxiety, Depression, and Optimism on Postoperative Satisfaction and Clinical Outcomes
Original Article Clinics in Orthopedic Surgery 2017;9:177-183 https://doi.org/10.4055/cios.2017.9.2.177 The Effect of Anxiety, Depression, and Optimism on Postoperative Satisfaction and Clinical Outcomes
Template 1 for summarising studies addressing prognostic questions
 Template 1 for summarising studies addressing prognostic questions Instructions to fill the table: When no element can be added under one or more heading, include the mention: O Not applicable when an
Template 1 for summarising studies addressing prognostic questions Instructions to fill the table: When no element can be added under one or more heading, include the mention: O Not applicable when an
Disclosures. The Value Agenda in Spine Care Steven D. Glassman, M.D. 10/14/16. AllinaHealthSystems 1. Introduction. Introduction.
 The Value Agenda in Spine Care Steven D. Glassman, M.D. Professor of Orthopedic Surgery University of Louisville Norton Leatherman Spine Center Past-President, Scoliosis Research Society Medtronic Disclosures
The Value Agenda in Spine Care Steven D. Glassman, M.D. Professor of Orthopedic Surgery University of Louisville Norton Leatherman Spine Center Past-President, Scoliosis Research Society Medtronic Disclosures
ProDisc-L Total Disc Replacement. IDE Clinical Study
 Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Lumbar total disc replacement
 The Norwegian TDR Study Lumbar total disc replacement Predictors for long-term outcome Background Lumbar total disc replacement (TDR) is a surgical option for selected patients with chronic low back pain
The Norwegian TDR Study Lumbar total disc replacement Predictors for long-term outcome Background Lumbar total disc replacement (TDR) is a surgical option for selected patients with chronic low back pain
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Patient Reported Outcome High Priority
 Quality ID #460: Average Change in Back Pain Following Lumbar Fusion National Quality Strategy Domain: Person and Caregiver-Centered Experience and Outcomes Meaningful Measure Area: Patient Reported Functional
Quality ID #460: Average Change in Back Pain Following Lumbar Fusion National Quality Strategy Domain: Person and Caregiver-Centered Experience and Outcomes Meaningful Measure Area: Patient Reported Functional
focus Neurosurg Focus 39 (6):E13, 2015
 neurosurgical focus Neurosurg Focus 39 (6):E13, 2015 Prediction model for outcome after low-back surgery: individualized likelihood of complication, hospital readmission, return to work, and 12-month improvement
neurosurgical focus Neurosurg Focus 39 (6):E13, 2015 Prediction model for outcome after low-back surgery: individualized likelihood of complication, hospital readmission, return to work, and 12-month improvement
ACO #44 Use of Imaging Studies for Low Back Pain
 Measure Information Form (MIF) DATA SOURCE Medicare Claims Medicare beneficiary enrollment data MEASURE SET ID ACO #44 VERSION NUMBER AND EFFECTIVE DATE Version 1, effective 01/01/18 CMS APPROVAL DATE
Measure Information Form (MIF) DATA SOURCE Medicare Claims Medicare beneficiary enrollment data MEASURE SET ID ACO #44 VERSION NUMBER AND EFFECTIVE DATE Version 1, effective 01/01/18 CMS APPROVAL DATE
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis
 Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN Disclosures
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN Disclosures
A Surgeon s Perspective for the Primary Care Physician Stephen Curtin M.D. Tucson Orthopeadic Institute
 A Surgeon s Perspective for the Primary Care Physician Stephen Curtin M.D. Tucson Orthopeadic Institute 26th Annual Southwestern Conference on Medicine AXIAL MUSCULO- SKELETAL PACK PAIN: Common Self-limited
A Surgeon s Perspective for the Primary Care Physician Stephen Curtin M.D. Tucson Orthopeadic Institute 26th Annual Southwestern Conference on Medicine AXIAL MUSCULO- SKELETAL PACK PAIN: Common Self-limited
Clinical Study. Overview
 Clinical Study David A. Mayer, MD, JD, FICS Associate Professor of Clinical Surgery New York Medical College Chairman of Surgery Emeritus Overview A practice based prospective study of 31 consecutive patients
Clinical Study David A. Mayer, MD, JD, FICS Associate Professor of Clinical Surgery New York Medical College Chairman of Surgery Emeritus Overview A practice based prospective study of 31 consecutive patients
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis
 Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Surgery has long been an accepted treatment for. Patient-specific factors affecting hospital costs in lumbar spine surgery
 clinical article J Neurosurg Spine 24:1 6, 2016 Patient-specific factors affecting hospital costs in lumbar spine surgery Ross C. Puffer, MD, Ryan Planchard, BE, Grant W. Mallory, MD, and Michelle J. Clarke,
clinical article J Neurosurg Spine 24:1 6, 2016 Patient-specific factors affecting hospital costs in lumbar spine surgery Ross C. Puffer, MD, Ryan Planchard, BE, Grant W. Mallory, MD, and Michelle J. Clarke,
Dingjun Hao, Baorong He, Liang Yan. Hong Hui Hospital, Xi an Jiaotong University College. of Medicine, Xi an, Shaanxi , China
 Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
Xi an Hong Hui Hospital Xi an, Shaanxi, China The difference of occurring superior adjacent segment pathology after lumbar posterolateral fusion by using two different pedicle screw insertion techniques
MEDICAL POLICY Acupuncture
 POLICY: PG0382 ORIGINAL EFFECTIVE: 12/13/16 LAST REVIEW: 06/12/18 MEDICAL POLICY Acupuncture GUIDELINES This policy does not certify benefits or authorization of benefits, which is designated by each individual
POLICY: PG0382 ORIGINAL EFFECTIVE: 12/13/16 LAST REVIEW: 06/12/18 MEDICAL POLICY Acupuncture GUIDELINES This policy does not certify benefits or authorization of benefits, which is designated by each individual
NUHS Evidence Based Practice I Journal Club. Date:
 Topic NUHS Evidence Based Practice I Journal Club Team Members: Date: Featured Research Article: Vancouver format example: Weinstein JN, Tosteson TD, Lurie JD, Tosteson AN, Hanscom B, Skinner JS, Abdu
Topic NUHS Evidence Based Practice I Journal Club Team Members: Date: Featured Research Article: Vancouver format example: Weinstein JN, Tosteson TD, Lurie JD, Tosteson AN, Hanscom B, Skinner JS, Abdu
Supplementary Online Content
 Supplementary Online Content Fritz JM, Magel JS, McFadden M, et al. Early physical therapy vs usual care in patients with recent onset low back pain: a randomized clinical trial. JAMA. doi:10.1001/jama.2015.11648.
Supplementary Online Content Fritz JM, Magel JS, McFadden M, et al. Early physical therapy vs usual care in patients with recent onset low back pain: a randomized clinical trial. JAMA. doi:10.1001/jama.2015.11648.
Background Information
 Background Information Age plays an important role in patients selection for spinal surgeries as it is associated with increased morbidity and mortality Consequences of suffering postoperative complications
Background Information Age plays an important role in patients selection for spinal surgeries as it is associated with increased morbidity and mortality Consequences of suffering postoperative complications
Patient Preferences and Expectations for Care
 SPINE Volume 33, Number 24, pp 2663 2668 2008, Lippincott Williams & Wilkins Patient Preferences and Expectations for Care Determinants in Patients With Lumbar Intervertebral Disc Herniation Jon D. Lurie,
SPINE Volume 33, Number 24, pp 2663 2668 2008, Lippincott Williams & Wilkins Patient Preferences and Expectations for Care Determinants in Patients With Lumbar Intervertebral Disc Herniation Jon D. Lurie,
Natural Evolution of Lumbar Spinal Stenosis
 Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Dethroning the Clinical Prediction Rule WPTA Fall Conference 2017
 Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
Relationship between depression and clinical outcome following anterior cervical discectomy and fusion
 Original Study Relationship between depression and clinical outcome following anterior cervical discectomy and fusion Kevin Phan 1,2, Dane Moran 1, Thomas Kostowski 1, Risheng Xu 1, Rory Goodwin 1, Benjamin
Original Study Relationship between depression and clinical outcome following anterior cervical discectomy and fusion Kevin Phan 1,2, Dane Moran 1, Thomas Kostowski 1, Risheng Xu 1, Rory Goodwin 1, Benjamin
Wendy Field Advanced Physiotherapy Practitioner June 2018
 Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Patient-reported outcome questionnaires have become
 J Neurosurg Spine 16:61 67, 2012 Determination of minimum clinically important difference in pain, disability, and quality of life after extension of fusion for adjacent-segment disease Clinical article
J Neurosurg Spine 16:61 67, 2012 Determination of minimum clinically important difference in pain, disability, and quality of life after extension of fusion for adjacent-segment disease Clinical article
Patient-reported outcome questionnaires have become
 J Neurosurg Spine 16:471 478, 2012 Minimum clinically important difference in pain, disability, and quality of life after neural decompression and fusion for same-level recurrent lumbar stenosis: understanding
J Neurosurg Spine 16:471 478, 2012 Minimum clinically important difference in pain, disability, and quality of life after neural decompression and fusion for same-level recurrent lumbar stenosis: understanding
Innovative Spine Care Technology
 Extentrac Elite Innovative Spine Care Technology US FDA 510(k) K031996, K980021 China FDA Kazakhstan FDA #C3 2009/05629 United States Patents 6,905,508 6,923,825 7,309,347 Additional United States and
Extentrac Elite Innovative Spine Care Technology US FDA 510(k) K031996, K980021 China FDA Kazakhstan FDA #C3 2009/05629 United States Patents 6,905,508 6,923,825 7,309,347 Additional United States and
A COMPARATIVE STUDY OF THE
 A COMPARATIVE STUDY OF THE OUTCOMES OF PRIMARY AND REVISION DISCECTOMY SURGERY MS Patel, J Braybrooke, M Newey, P Sell BACKGROUND Following primary discectomy, a recurrent lumbar disc herniation at the
A COMPARATIVE STUDY OF THE OUTCOMES OF PRIMARY AND REVISION DISCECTOMY SURGERY MS Patel, J Braybrooke, M Newey, P Sell BACKGROUND Following primary discectomy, a recurrent lumbar disc herniation at the
J Neurosurg Spine 21:
 See the corresponding editorial in this issue, pp 141 142. J Neurosurg Spine 21:143 149, 2014 AANS, 2014 Two-year comprehensive medical management of degenerative lumbar spine disease (lumbar spondylolisthesis,
See the corresponding editorial in this issue, pp 141 142. J Neurosurg Spine 21:143 149, 2014 AANS, 2014 Two-year comprehensive medical management of degenerative lumbar spine disease (lumbar spondylolisthesis,
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Clinical Reference Guide
 Clinical Reference Guide Table of Clinical References PREVALENCE Bernard, 1987 Cohen, 2005 Weksler, 2007 Sembrano, 2009 POST LUMBAR FUSION Maigne, 2005 Ha, 2008 Ivanov, 2009 Liliang, 2011 DePalma, 2011
Clinical Reference Guide Table of Clinical References PREVALENCE Bernard, 1987 Cohen, 2005 Weksler, 2007 Sembrano, 2009 POST LUMBAR FUSION Maigne, 2005 Ha, 2008 Ivanov, 2009 Liliang, 2011 DePalma, 2011
What Improvement in Function and Pain Intensity is Meaningful to Patients Recovering from Low-Risk Arm Fractures?
 ORIGINAL ARTICLE What Improvement in Function and Pain Intensity is Meaningful to Patients Recovering from Low-Risk Arm Fractures? ABSTRACT Background Small, statistically significant differences in patient-reported
ORIGINAL ARTICLE What Improvement in Function and Pain Intensity is Meaningful to Patients Recovering from Low-Risk Arm Fractures? ABSTRACT Background Small, statistically significant differences in patient-reported
LONG-TERM EFFECT ANALYSIS OF IDD THERAPY IN LOW BACK PAIN: A RETROSPECTIVE CLINICAL PILOT STUDY
 Preliminary Findings LONG-TERM EFFECT ANALYSIS OF IDD THERAPY IN LOW BACK PAIN: A RETROSPECTIVE CLINICAL PILOT STUDY C. Norman Shealy, MD, PhD, Nirman Koladia, MD, and Merrill M. Wesemann, MD Abstract.
Preliminary Findings LONG-TERM EFFECT ANALYSIS OF IDD THERAPY IN LOW BACK PAIN: A RETROSPECTIVE CLINICAL PILOT STUDY C. Norman Shealy, MD, PhD, Nirman Koladia, MD, and Merrill M. Wesemann, MD Abstract.
National Imaging Associates, Inc. Clinical guidelines CHIROPRACTIC SERVICES. Original Date: Page 1 of FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines CHIROPRACTIC SERVICES CPT4 Codes: Please refer to pages 2-10 LCD ID Number: L35424 Novitas: J-H: DC, DE, MD, NJ, PA J-L: AR, CO, LA, MS, NM, OK, TX
National Imaging Associates, Inc. Clinical guidelines CHIROPRACTIC SERVICES CPT4 Codes: Please refer to pages 2-10 LCD ID Number: L35424 Novitas: J-H: DC, DE, MD, NJ, PA J-L: AR, CO, LA, MS, NM, OK, TX
Usage of Outcomes Measurements in Chiropractic Care
 2013 Usage of Outcomes Measurements in Chiropractic Care Table of Contents I. Executive Summary II. Overview of Chiropractic Care of Minnesota, Inc. III. Planning the Outcomes Program IV. Background; Chiropractic
2013 Usage of Outcomes Measurements in Chiropractic Care Table of Contents I. Executive Summary II. Overview of Chiropractic Care of Minnesota, Inc. III. Planning the Outcomes Program IV. Background; Chiropractic
Jeremy Fairbank MD FRCS Professor of Spine Surgery NDORMS University of Oxford
 Towards a paradigm shift in chronic low back pain? Identification of patient profiles to guide treatment Surgery and combined physical and psychological treatment as competitive treatment options for all
Towards a paradigm shift in chronic low back pain? Identification of patient profiles to guide treatment Surgery and combined physical and psychological treatment as competitive treatment options for all
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Friedly JL, Comstock BA, Turner JA, et al. A randomized trial
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Friedly JL, Comstock BA, Turner JA, et al. A randomized trial
Vertebral Axial Decompression
 Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2017 Origination: 11/2005 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2017 Origination: 11/2005 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS
 THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
THRESHOLD POLICY T17 SPINAL SURGERY FOR ACUTE LUMBAR CONDITIONS Policy author: Ipswich and East Suffolk and West Suffolk CCGs with support from Public Health Suffolk Policy start date: September 2014 Subsequent
2015 Part 3 Cox Certification in Chicago, IL
 Cox Technic Case Report #166 published at www.coxtechnic.com 2015 Part 3 Cox Certification in Chicago, IL Multi-level cervical disc displacement with stenosis and adjacent levels retrolistethesis, 16 years
Cox Technic Case Report #166 published at www.coxtechnic.com 2015 Part 3 Cox Certification in Chicago, IL Multi-level cervical disc displacement with stenosis and adjacent levels retrolistethesis, 16 years
Patient Selection and Lumbar Operative Interventions
 Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Pasquale Donnarumma 1, Roberto Tarantino 1, Lorenzo Nigro 1, Marika Rullo 2, Domenico Messina 3, Daniele Diacinti 4, Roberto Delfini 1.
 Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
Original Study Decompression versus decompression and fusion for degenerative lumbar stenosis: analysis of the factors influencing the outcome of back pain and disability Pasquale Donnarumma 1, Roberto
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis
 Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN The following
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN The following
MAKING THE NSQIP PARTICIPANT USE DATA FILE (PUF) WORK FOR YOU
 MAKING THE NSQIP PARTICIPANT USE DATA FILE (PUF) WORK FOR YOU Hani Tamim, PhD Clinical Research Institute Department of Internal Medicine American University of Beirut Medical Center Beirut - Lebanon Participant
MAKING THE NSQIP PARTICIPANT USE DATA FILE (PUF) WORK FOR YOU Hani Tamim, PhD Clinical Research Institute Department of Internal Medicine American University of Beirut Medical Center Beirut - Lebanon Participant
Vertebral Axial Decompression
 Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
2013 UCSF SPINE SYMPOSIUM RICHARD DEYO, MD MPH MICHAEL GROFF, MD
 2013 UCSF SPINE SYMPOSIUM RICHARD DEYO, MD MPH MICHAEL GROFF, MD OHSU Professor and the Kaiser- Permanente Endowed Professor of Evidence-Based Medicine in the Department of Family Medicine at Oregon Health
2013 UCSF SPINE SYMPOSIUM RICHARD DEYO, MD MPH MICHAEL GROFF, MD OHSU Professor and the Kaiser- Permanente Endowed Professor of Evidence-Based Medicine in the Department of Family Medicine at Oregon Health
GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE. A Guide for Patients
 GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE A Guide for Patients Your Spine Deserves Special Care Your spine is at the center of a delicately balanced system that controls all of your body s movements.
GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE A Guide for Patients Your Spine Deserves Special Care Your spine is at the center of a delicately balanced system that controls all of your body s movements.
Spine Center. Spine Center at Miami Valley Hospital. Our Approach to Care. Why Come to MVH
 The Region s Leader Spine Center Spine Center at Miami Valley Hospital The Spine Center at Miami Valley Hospital (MVH) is the only Spine Center of Excellence in the Dayton region that offers comprehensive
The Region s Leader Spine Center Spine Center at Miami Valley Hospital The Spine Center at Miami Valley Hospital (MVH) is the only Spine Center of Excellence in the Dayton region that offers comprehensive
External validation of a prediction model for surgical site infection after thoracolumbar spine surgery in a Western European cohort
 Janssen et al. Journal of Orthopaedic Surgery and Research (2018) 13:114 https://doi.org/10.1186/s13018-018-0821-2 RESEARCH ARTICLE Open Access External validation of a prediction model for surgical site
Janssen et al. Journal of Orthopaedic Surgery and Research (2018) 13:114 https://doi.org/10.1186/s13018-018-0821-2 RESEARCH ARTICLE Open Access External validation of a prediction model for surgical site
Interlaminar Decompression For Lumbar Stenosis: When is Less More?
 Interlaminar Decompression For Lumbar Stenosis: When is Less More? Kris Radcliff, MD Associate Professor Department of Orthopedic Surgery Associate Professor of Neurosurgery and Hospitals The Rothman Institute
Interlaminar Decompression For Lumbar Stenosis: When is Less More? Kris Radcliff, MD Associate Professor Department of Orthopedic Surgery Associate Professor of Neurosurgery and Hospitals The Rothman Institute
JOSS. original article ABSTRACT INTRODUCTION. Data Source
 original article Anterior Cervical 10.5005/jp-journals-10039-1053 Surgery: Drain Needed or Not? 1 Shivalingegouda Rayagouda Patil, 2 Anantha Kishan, 3 Anantha Gabbita, 4 DN Varadharaju, 5 PM Jagannath
original article Anterior Cervical 10.5005/jp-journals-10039-1053 Surgery: Drain Needed or Not? 1 Shivalingegouda Rayagouda Patil, 2 Anantha Kishan, 3 Anantha Gabbita, 4 DN Varadharaju, 5 PM Jagannath
Related Policies None
 Medical Policy MP 7.01.541 BCBSA Ref. Policy: 7.01.141 Last Review: 06/27/2018 Effective Date: 06/27/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Medical Policy MP 7.01.541 BCBSA Ref. Policy: 7.01.141 Last Review: 06/27/2018 Effective Date: 06/27/2018 Section: Surgery Related Policies None DISCLAIMER Our medical policies are designed for informational
Chiropractic Health Plan - Diagnosis of Low Back Pain
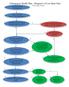 Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
CAN WE PREDICT SURGERY FOR SCIATICA?
 7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
1 Does Maintained Spinal Manipulation Therapy for Chronic Nonspecific Low Back Pain Result in Better Long-Term Outcome?
 1 Does Maintained Spinal Manipulation Therapy for Chronic Nonspecific Low Back Pain Result in Better Long-Term Outcome? Randomized Trial SPINE August 1, 2011; Volume 36, Number 18, pp. 1427 1437 Mohammed
1 Does Maintained Spinal Manipulation Therapy for Chronic Nonspecific Low Back Pain Result in Better Long-Term Outcome? Randomized Trial SPINE August 1, 2011; Volume 36, Number 18, pp. 1427 1437 Mohammed
When Clinical Reasoning Overrules the Evidence
 When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
Completing the Circle: Novel Methods for using PRO Scores in Shared Decision- Making and Patient Self-Management.
 Completing the Circle: Novel Methods for using PRO Scores in Shared Decision- Making and Patient Self-Management. Karon Cook, PhD, Northwestern University Chicago, IL Thursday, September 28, 2017 Relevant
Completing the Circle: Novel Methods for using PRO Scores in Shared Decision- Making and Patient Self-Management. Karon Cook, PhD, Northwestern University Chicago, IL Thursday, September 28, 2017 Relevant
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
The Cochrane Library Impact Factor Data Pack
 The Cochrane Library Impact Factor Data Pack When considering the data presented below, please be aware of the following: The dataset we have used to generate impact factors for individual review groups
The Cochrane Library Impact Factor Data Pack When considering the data presented below, please be aware of the following: The dataset we have used to generate impact factors for individual review groups
Manual Therapy Interventions For Patients With Lumbar Spinal Stenosis A Systematic Review
 Manual Therapy Interventions For Patients With Lumbar Spinal Stenosis A Systematic Review symptomatic lumbar spinal stenosis have difficulty walking for extended periods. Physical Therapy Treatment Programs
Manual Therapy Interventions For Patients With Lumbar Spinal Stenosis A Systematic Review symptomatic lumbar spinal stenosis have difficulty walking for extended periods. Physical Therapy Treatment Programs
Department of Neurosurgery, University of Virginia, Charlottesville, Virginia
 J Neurosurg Spine 9:000 000, 9:326 331, 2008 Neurological symptoms and deficits in adults with scoliosis who present to a surgical clinic: incidence and association with the choice of operative versus
J Neurosurg Spine 9:000 000, 9:326 331, 2008 Neurological symptoms and deficits in adults with scoliosis who present to a surgical clinic: incidence and association with the choice of operative versus
Low back pain in a Nutshell Paul Manjaly. Paul Manjaly
 Low back pain in a Nutshell Paul Manjaly Paul Manjaly Pain: An unpleasant sensory and emotional experience which follows actual or potential tissue damage or is described in terms of such damage Unpleasant
Low back pain in a Nutshell Paul Manjaly Paul Manjaly Pain: An unpleasant sensory and emotional experience which follows actual or potential tissue damage or is described in terms of such damage Unpleasant
Prospective Data Collection Provider Perspective
 Prospective Data Collection Provider Perspective Zoher Ghogawala, M.D. Chairman and Associate Professor Department of Neurosurgery Lahey Clinic Tufts University School of Medicine Science of Clinical Practice
Prospective Data Collection Provider Perspective Zoher Ghogawala, M.D. Chairman and Associate Professor Department of Neurosurgery Lahey Clinic Tufts University School of Medicine Science of Clinical Practice
Spine Tango, utility and results from real life. Emin Aghayev Institute for Social and Preventive Medicine University of Bern
 Spine Tango, utility and results from real life Emin Aghayev Institute for Social and Preventive Medicine University of Bern Table of content What is Spine Tango History and key figures Why do we need
Spine Tango, utility and results from real life Emin Aghayev Institute for Social and Preventive Medicine University of Bern Table of content What is Spine Tango History and key figures Why do we need
We look forward to reviewing your report when completed and offering our comments again. Sincerely, John
 ICER Chronic Low Back and Neck Pain Draft Scoping Document Open Input Period Commentary from United States Bone and Joint Initiative www.usbji.org April 25, 2017 Dear Sirs, We, the United States Bone and
ICER Chronic Low Back and Neck Pain Draft Scoping Document Open Input Period Commentary from United States Bone and Joint Initiative www.usbji.org April 25, 2017 Dear Sirs, We, the United States Bone and
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Are you getting the best treatment for your low back pain?
 Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Research Report. Which Prognostic Factors for Low Back Pain Are Generic Predictors of Outcome Across a Range of Recovery Domains?
 Research Report C.E. Cook, PT, PhD, MBA, OCS, FAAOMPT, Division of Physical Therapy, Walsh University, 2020 East Maple, North Canton, OH 44720 (USA). Address all correspondence to Dr Cook at: ccook@walsh.edu.
Research Report C.E. Cook, PT, PhD, MBA, OCS, FAAOMPT, Division of Physical Therapy, Walsh University, 2020 East Maple, North Canton, OH 44720 (USA). Address all correspondence to Dr Cook at: ccook@walsh.edu.
Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries
 Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries Victoria L. Tseng, MD, Fei Yu, PhD, Flora Lum, MD, Anne L. Coleman, MD, PhD JAMA. 2012;308(5):493-501 Background Visual impairment
Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries Victoria L. Tseng, MD, Fei Yu, PhD, Flora Lum, MD, Anne L. Coleman, MD, PhD JAMA. 2012;308(5):493-501 Background Visual impairment
Adult Spinal Deformity: Principles of Surgical Correction
 Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
FirstCarolinaCare Spinal Surgery Prior authorization Guidelines
 FirstCarolinaCare Spinal Surgery Prior authorization Guidelines Subject LUMBAR FUSION (arthrodesis) Next Review 06/2014 General Requirements for Lumbar Spinal Fusion: 1. Prior authorization is required
FirstCarolinaCare Spinal Surgery Prior authorization Guidelines Subject LUMBAR FUSION (arthrodesis) Next Review 06/2014 General Requirements for Lumbar Spinal Fusion: 1. Prior authorization is required
Interlaminar Decompression & Stabilization. Reginald Davis, M.D., FAANS, FACS Director of Clinical Research
 Interlaminar Decompression & Stabilization Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Background Device meant to stabilize the spine without fusion following decompression
Interlaminar Decompression & Stabilization Reginald Davis, M.D., FAANS, FACS Director of Clinical Research Disclosures Background Device meant to stabilize the spine without fusion following decompression
Transforaminal Lumbar Interbody Fusion: Prognostic Factors Related to Retention in an Active Duty Military Population
 MILITARY MEDICINE, 178, 2:228, 2013 Transforaminal Lumbar Interbody Fusion: Prognostic Factors Related to Retention in an Active Duty Military Population MAJ Andrew J. Schoenfeld, MC USA*; CPT Dimitri
MILITARY MEDICINE, 178, 2:228, 2013 Transforaminal Lumbar Interbody Fusion: Prognostic Factors Related to Retention in an Active Duty Military Population MAJ Andrew J. Schoenfeld, MC USA*; CPT Dimitri
FOCUS Neurosurg Focus 44 (1):E2, 2018
 NEUROSURGICAL» This article has been updated from its originally published version to correct an author s name. See the corresponding erratum notice, DOI: 10.3171/2018.1.FOCUS17554a. «FOCUS Neurosurg Focus
NEUROSURGICAL» This article has been updated from its originally published version to correct an author s name. See the corresponding erratum notice, DOI: 10.3171/2018.1.FOCUS17554a. «FOCUS Neurosurg Focus
Jurisdiction New Mexico. Retirement Date N/A
 Local Coverage Determination (LCD): Chiropractic Services (L34816) Contractor Information Contractor Name Novitas Solutions, Inc. opens in new Contract Number 04212 Contract Type A and B MAC J - H LCD
Local Coverage Determination (LCD): Chiropractic Services (L34816) Contractor Information Contractor Name Novitas Solutions, Inc. opens in new Contract Number 04212 Contract Type A and B MAC J - H LCD
Low back pain is common among adults of all ages, but
 SPINE Volume 40, Number 17, pp 1352-1362 2015, Wolters Kluwer Health, Inc. All rights reserved. HEALTH SERVICES RESEARCH Trajectories of Symptoms and Function in Older Adults With Low Back Disorders Richard
SPINE Volume 40, Number 17, pp 1352-1362 2015, Wolters Kluwer Health, Inc. All rights reserved. HEALTH SERVICES RESEARCH Trajectories of Symptoms and Function in Older Adults With Low Back Disorders Richard
Is Pilates an Effective Treatment for Improving Functional Disability and Pain in Patients with Nonspecific Low Back Pain?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is Pilates an Effective Treatment for
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is Pilates an Effective Treatment for
Setting The setting was primary care (general medical practice). The economic study was carried out in Germany.
 Pragmatic randomized trial evaluating the clinical and economic effectiveness of acupuncture for chronic low back pain Witt C M, Jena S, Selim D, Brinkhaus B, Reinhold T, Wruck K, Liecker B, Linde K, Wegscheider
Pragmatic randomized trial evaluating the clinical and economic effectiveness of acupuncture for chronic low back pain Witt C M, Jena S, Selim D, Brinkhaus B, Reinhold T, Wruck K, Liecker B, Linde K, Wegscheider
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
Self-Directed Structured Spine Care. David Hanscom, MD Swedish Neuroscience Specialists Seattle, WA
 Self-Directed Structured Spine Care David Hanscom, MD Swedish Neuroscience Specialists Seattle, WA Two Years Later David, She has made remarkable changes. She is motivated and has developed a strong
Self-Directed Structured Spine Care David Hanscom, MD Swedish Neuroscience Specialists Seattle, WA Two Years Later David, She has made remarkable changes. She is motivated and has developed a strong
Adverse events in adult spinal deformity procedures.
 Adverse events in adult spinal deformity procedures. Evalina L BURGER*, Michael S CHANG**, Sean MOLLOY*** Vincent FIERE**** * Department of Orthopedic Surgery, University of Colorado,Aurora, USA ** Department
Adverse events in adult spinal deformity procedures. Evalina L BURGER*, Michael S CHANG**, Sean MOLLOY*** Vincent FIERE**** * Department of Orthopedic Surgery, University of Colorado,Aurora, USA ** Department
Supplementary Online Content
 Supplementary Online Content Goertz CM, Long CR, Vining RD, Pohlman KA, Walter J, Coulter I. Effect of usual medical care plus chiropractic care vs usual medical care alone on pain and disability among
Supplementary Online Content Goertz CM, Long CR, Vining RD, Pohlman KA, Walter J, Coulter I. Effect of usual medical care plus chiropractic care vs usual medical care alone on pain and disability among
