AUSTRALIA AND NEW ZEALAND CLINICAL PRACTICE GUIDELINE FOR PREVENTION AND MANAGEMENT OF VENOUS LEG ULCERS
|
|
|
- Lawrence Clark
- 5 years ago
- Views:
Transcription
1 AUSTRALIA AND NEW ZEALAND CLINICAL PRACTICE GUIDELINE FOR PREVENTION AND MANAGEMENT OF VENOUS LEG ULCERS The Australian Wound Management Association Inc The New Zealand Wound Care Society
2 CONTENTS INTRODUCTION. Venous leg ulcers in the community.2 Endorsement and expiry date for the recommendations.3 Acknowledgements.4 Commonly used abbreviations.5 Glossary 2 SUMMARY OF RECOMMENDATIONS 3 BACKGROUND 3. Venous leg ulcers 3.2 The need for a guideline 3.3 Scope and target population 3.4 Focus of the guideline 3.5 Process 3.6 Limitations of the guideline 4 RECOMMENDATIONS FOR PRIMARY PREVENTION 4. Management of venous hypertension 4.2 Compression therapy 4.3 Phlebotics 5 RECOMMENDATIONS FOR ASSESSMENT, DIAGNOSIS AND REFERRAL 5. Initial and ongoing assessment 5.. Patient assessment 5..2 Wound assessment 5.2 Diagnosing a VLU 5.3 Referral 6 RECOMMENDATIONS FOR MANAGEMENT 6. Compression therapy 6.2 Dressings and topical treatments 6.2. Dressings Zinc-impregnated bandages Micellaneous topical treatments 6.3 Skin management 6.3. Skin and wound hygiene Management of venous eczema 6.4 Antimicrobial therapy 6.4. Cadexomer iodine Silver
3 6.4.3 Topical honey Other topical antimicrobials Topical antibiotics Systemic antibiotics 6.5 Wound debridement 6.6 Elevation 6.7 Exercise 6.8 Nutrition and hydration 6.9 Skin grafting 6.0 Pain management 6. Therapuetic ultrasound 6.2 Education and psychosocial support 6.2. Health professional education Patient education Psychosocial support 6.3 Pharmacological management 6.3. Nifedipine Pentoxifylline Micronised purified flavanoid fraction 7 RECOMMENDATIONS FOR PREVENTING RECURRENCE 7. Maintenance of leg care 7.2 Ongoing compression therapy 8 TREATMENTS NOT CURRENTLY RECOMMENDED 8. Electromagnetic therapy 8.2 Electrotherapy 8.3 Low level laser therapy 8.4 Topical phenytoin 8.5 Oral zinc 8.6 Horse chestnut seed extract 9 INTERVENTIONS WITH INSUFFICIENT EVIDENCE 0 EMERGING TREATMENTS 0. Protein-derived treatments 0.2 Growth factor treatments 0.3 Intravenous prostaglandin E REFERENCES APPENDIX ONE Expert Working Committee APPENDIX TWO Process report APPENDIX THREE Excluded studies APPENDIX FOUR AWMA Conflict of interest declaration form 2
4 . INTRODUCTION. Venous leg ulcers in the community In Australia, the prevalence of venous leg ulcers (VLUs) is % in the overall population and approximately 4% in adults aged over 65 years. 2 Venous leg ulcers have a high rate of recurrence (approximately 56% recur within 3 months 3 ), thereby increasing their health burden. In Australia it has been estimated that management of venous ulcers accounts for $400 million annually in health care expenditure. Aside from the direct financial burden of treating VLUs, they give rise to chronic pain, reduced participation in the workforce and social life and an overall reduced quality of life for people inflicted. 4 Within the New Zealand context, an Auckland study demonstrated the risk of developing VLUs increases dramatically with age, with people over 60 particularly at risk. 5 A capturerecapture analysis that incorporates an estimation of missed cases estimated a point prevalence of 2.48 per 000 adults. 6 Similar to Australian trends, statistics from the New Zealand Ministry of Health describe a rapid increase in the number of people over 65 years. By 2040 it is estimated the proportion of people over 65 will have risen from 2% to 24%, while the over 85 year olds will have increased fourfold from.3% to 5.5%. There is no specific published data on the incidence of VLUs in Aboriginal and Torres Strait Islander people in Australia or Maori people in New Zealand. The health of Indigenous populations differs from that of the general population in both countries. 7-9 In New Zealand, this disparity has been directly related to poor socio-economic status leading to susceptibility of disease, poorer health outcomes and a higher rate of chronic disease. 8, 9 In Australia, there is a higher prevalence of most long term health conditions in people from Aboriginal and Torres Strait Island backgrounds compared with non-indigenous populations. 7, 0 The introduction of evidence based guidelines for leg ulcer assessment and management will assist clinical decision making and may help reduce health inequalities for Australian and New Zealand Indigenous populations. The Council of Australian Governments (COAG) recognises the desire of Australians to maintain and where possible improve the quality of their lives as they age. There is significant growth in the population of adults aged over 65 years and this is projected to increase almost three fold over the next four decades. The projected cost of management of VLUs is significant. Currently one in eight Australians is aged over 65 years. By 2044 those aged over 65 years will account for one in four of the Australian population. 2 Over the next 20 years the ageing population will lead to a tripling of demand for government funded care provision for those aged over 80 years. The COAG recognises the implications of an ageing Australia including demands on infrastructure and community support; the impact of ageing in regional areas; and the availability of accessible, appropriate health and aged care services. Explicit costs include but are not limited to hospital admissions, domiciliary nursing services, nurse practitioners, consumables, pathology and radiology investigations, general practitioner 3
5 and specialist consultations, pharmaceutical costs, and additional adjuvant therapies. The financial cost to both the individual and the community is enormous. However, the implicit costs to individuals and their families are difficult to measure. Access to appropriate services for diagnosis and management of VLUs for all Australians will significantly improve health outcomes and quality of life. Statistics from the New Zealand Ministry of Health describe a trend similar to Australia, with a rapid increase in the number of people over 65 years. By 2040 the proportion of people over 65 will have risen from 2% to 24%, while the over 85 year olds will have increased fourfold from.3% to 5.5%. 3 The Australian Wound Management Association (AWMA) and the New Zealand Wound Care Society (NZWCS) aims to increase awareness of VLUs within the community. A priority is to optimise the prevention, assessment and management of VLUs via the dissemination of best available evidence and to simplify clinical decision making processes for health care professionals..2 Endorsement and expiry date for the recommendations This guideline was developed by the AWMA in conjunction with the NZWCS. The guideline presents a comprehensive review of the diagnosis, assessment, management and prevention of VLUs within the Australian and New Zealand healthcare context, based on the best available evidence available up to September Australian and New Zealand clinical practice guideline for the prevention and management of venous leg ulcers was approved by the CEO of the National Health and Medical Research Council (NHMRC) on XXXXX, under section 4A of the National Health and Medical Research Council Act 992. Approval for the guidelines by the NHMRC is granted for a period not exceeding five years, at which the date of approval expires. The NHMRC expects that the guideline will be reviewed, and revised if necessary, no less than once every five years. Readers should check with the AWMA and NZWCS websites for any reviews or updates to this guideline. The guideline is designed to provide information to assist in decision-making and is based on the best information available at the date of compilation. The guideline is not intended to have a regulatory effect. This document is a general guide to appropriate practice, to be implemented by a qualified health professional subject to his or her clinical judgment of each individual case and in consideration of the patient s personal preferences..3 Acknowledgements This project was financed by the AWMA and conducted by the AWMA experts in conjunction with NZWCS. 4
6 The following experts were involved in the appraisal of evidence and the development of the recommendations contained in the guideline as part of the Expert Working Committee: Donna Angel, RN; BN; NP; PGraddip (Clin Spec); MSc (Nur); MRCNA Judith Barker, Vice Chair; RN; NP; STN; BHlthSc (Nurs); MN(NP) Debbie Blanchfield, RN; Masters of Wound Care Keryln Carville, A/Professor; RN; STN (Cred); PhD Roy Cochrane, Consumer representative Michelle Gibb, RN; NP; Wound Care MNrsgSc(NP) Emily Haesler, BN; PGradDipAdvNsg (Ger) Cathy Hammond, RN, MN David Hardman, Chair; MBBS(Hons); LLB (Hons); GradcertHE ; FRACS; FACLM; A/Professor Susan Hillier, BappSc(Physiotherapy); PhD; NHMRC Guideline Consultant Suzanne Kapp, BN; PGDip (AdvNsg); MNSci Deane Larkman, BSci(Hons); GradDipCompStud; MInfTech Judith Manning, RN; MA; BEd. Bill McGuiness,RN; DipT; BN; MNS; PhD; A/Professor; AWMA President Robyn Rayner, RN; BSc (Nursing); Postgrad Health Admin; Master of Wound Care Jan Rice, RN; AMWA Cert. Plastic & Reconstructive Surgery; MRCNA; FAWMA Pip Rutherford, RGON; BN; GradDip CaseManage; GradCert Wound Care; MN Juliet Scott, RN; BAppSci (Prim Hlth); Grad Cert; Grad Dip DN Jill Sparks, RN; MWoundManage Sue Templeton, RN; BN; MNSc(NP) Carolina Weller, BN; MEd(Research); GradCertHlthEd Peter Wilkins, Consumer representative Michael Woodward, MB; BS; FRACP; A/Professor; Past AWMA President. The Expert Working Committee would also like to thank the following people for their advice and assistance in the development of this guideline: Julie Betts (RN, NP, MN) and Margaret Broadbent (Chronic Care & Health Promotion, Aboriginal Strategy & Consultation Unit) 5
7 .4 Commonly used abbreviations 4LB ABPI AWMA CEAP CI CWIP CVI CVIQ DVT EBO EMLA GIT HCSE ITT LLLT MPFF NHMRC NNT NS NSBF NZWCS QOL RCT RR SR VLU four layer bandages/ing ankle brachial pressure index Australian Wound Management Association clinical severity, (a)etiology, anatomy, pathophysiology confidence interval Cardiff Wound Impact Schedule chronic venous insufficiency Chronic Venous Insufficiency Qeustionnaire deep vein thrombosis expert based opinion eutectic mixture of local anesthetic gastrointestinal tract horse chestnut seed extract intention to treat low level laser therapy micronised purified flavanoid fraction The National Health and Medical Research Council number needed to treat not statistically significant No Sting Barrier Film New Zealand Wound Care Society quality of life randomised controlled trial relative risk systematic review venous leg ulcer 6
8 .5 Glossary antibiotic antimicrobial arterial disease atrophie blanche bioengineered grafts skin Substance or compound administered systemically or applied topically that acts selectively against bacteria. A term used to encompass antibiotics and antiseptics. A substance that non-selectively reduces the possibility of infection by inhibiting the growth of, or eradicating micro-organisms. Impaired blood flow in the arteries that generally occurs due to a build up of plaque. Plaque is made up of fat, cholesterol, calcium, fibrous tissue, and other substances found in the blood. A type of scarring that infrequently occurs on the lower leg associated with healing that occurs when blood flow is impaired. It appears ivory/white depressed atrophic plaques with prominent red blotching within the scar. Manufactured skin replacement products not derived from human or animal skin cells. chronic venous insufficiency (CVI) extensibility Indigenous lipodermatosclerosis microcirculation macrocirculation patient post-thrombotic syndrome resting pressure standard care Chronic venous insufficiency is an advanced stage of venous disease that occurs over the long term. The ability of a bandage to increase its length in response to an applied force. Australians from an Aboriginal and Torres Strait Island background and New Zealanders from a Maori background. A condition that affects the skin immediately above the ankle in patients with long-standing venous disease. Is fibrosis of the underlying sub-cutaneous tissue. The flow of blood or lymph throughout the system of smaller vessels (diameter of 00µm or less) of the body. The large blood vessels that transport blood to the organs. Any person receiving health assessment, care or treatment. Post-thrombotic syndrome is a term used to describe signs and symptoms that occur due to long-term complications of lower limb DVT. Signs and symptoms include leg aching and cramping, itching, heaviness skin discolouration and VLU. The sub-bandage pressure experienced whilst the patient is at rest The definition of standard care varied amongst the trials reported in the literature and has been described in reports of individual studies. In most instances, standard care for VLU consisted of 7
9 wound cleanse with normal saline and/or water and a nonadherent dressing, either with or without compression therapy. venous disease venous hypertension venous tone venous leg ulcer working pressure Venous disease is related to or caused by pathology or functional abnormality in the veins that leads to sluggish venous blood flow. Either superficial or deep veins may be affected. Pathology includes venous obstruction (eg. from blood clotting), swelling of the veins or stretched/weakened venous valves. Elevated blood pressure in the veins that occurs due to venous obstruction (eg due to plaque) or incompetent venous valves. Pooling of the blood in the veins leads to an increase in pressure and, in the long term, venous disease. The degree of constriction experienced by a blood vessel relative to its maximal dilated state. Full thickness defect of the skin that persists due to venous disease on the lower leg. The sub-bandage pressure experienced as the patient walks. 8
10 2. SUMMARY OF RECOMMENDATIONS RECOMMENDATIONS FOR PRIMARY PREVENTION OF VLUs Adequate prevention and management of venous hypertension includes: early detection and management of deep vein thrombosis deep vein thrombosis prophylaxis access to venous surgery and phlebology interventions. Grade EBO Applying compression therapy is effective in preventing the initial development of a VLU. There is inconsistent evidence on the effectiveness of phlebotics in preventing the development of VLUs in patients with venous disease. RECOMMENDATIONS FOR ASSESSMENT, DIAGNOSIS AND REFERRAL FOR VLUs All patients presenting with a leg ulcer should receive a comprehensive assessment by a health professional trained in the assessment and management of VLUs. A comprehensive assessment should be made of the leg ulcer on initial presentation and at regular intervals thereafter to guide ongoing management. CEAP classification could be used to evaluate and classify venous disease. Local guidelines should provide clear indication of appropriate circumstances for referral to specialist health professionals. RECOMMENDATIONS FOR TREATMENT OF VLUs There is good evidence that applying compression therapy is effective in promoting healing in VLUs. There is excellent evidence that no specific dressing product is superior for reducing healing time in VLUs. Dressings should be selected based on clinical assessment of the wound, cost, access and patient/health professional preferences. The use of dressings or bandages impregnated with water soluble zinc may provide comfort and promote epithelialisation of a healthy granulated superficial VLU. There is some evidence that topical pale sulphonated shale oil is more EBO C Grade EBO EBO EBO EBO Grade B A EBO C 9
11 effective than standard care for promoting healing in VLUs. Cleansing the leg and wound when dressings and bandages are changed is recommended. Venous eczema and impaired peri-wound skin should be treated promptly. There is weak evidence that topical barrier preparations reduce periwound erythema in patients with VLU. There is some evidence that cadexomer iodine is more effective than standard care in the treatment of VLUs. There is good evidence that silver products offer no benefit over standard care in reducing the healing time for VLUs. There is evidence that honey offers no benefits over standard care in promoting healing in VLUs. There is some evidence that other topical antimicrobial agents offer no advantage over standard care in improving VLUs healing. There may be a role for judicious use of topical antimicrobials when there is known or suspected increased microbial burden. There is a concern that the use of topical antibiotics is associated with antibiotic resistance and sensitivities. Topical antibiotics have a very limited place in management of VLUs. Their use should be judicious. There is some evidence that systemic antibiotics offer no advantage over standard care for reducing healing time of VLUs that show no clinical signs of infection. There is weak evidence that enzymatic debriding agents have no effect in promoting healing in VLUs. There is evidence that the benefits of leg elevation are related to changes in microcirculation in patients with VLUs. Elevation is recommended to reduce lower limb oedema and promote VLU healing. There is evidence that exercise improves calf muscle function and promotes venous blood flow. Exercise is recommended as part of a management plan to promote healing in VLUs. Optimising nutrition and hydration is important to the healing of VLUs. There is some evidence that bi-layered bioengineered skin grafts are more effective than standard care in promoting healing in persistent VLUs. EBO EBO D C B A C EBO EBO C D D EBO D EBO EBO B 0
12 There is excellent evidence that EMLA cream is effective in reducing pain associated with the debridement of VLUs. There is some evidence that an ibuprofen impregnated dressing reduces pain associated with VLUs. There is weak evidence that electrotherapy may have an effect in reducing pain from VLUs. There is good evidence that therapeutic ultrasound therapy is not related to an improvement in total ulcer healing but may slightly improve the percentage of healed ulcer area when used in combination with compression therapy. There is some evidence that health professionals benefit from appropriate education on VLUs and their management. Patient outcomes may be superior when ulcer care is conducted by an appropriately trained health professional. There is weak evidence that patients with VLUs benefit from appropriate education on their condition and its management. Psychosocial assessment and support is an essential component in the patient s management. There is good evidence that pentoxifylline is effective in promoting healing in VLUs. There is weak evidence that micronised purified flavanoid fraction may decrease the healing time for VLUs. RECOMMENDATIONS FOR PREVENTING RECURRENCE OF VLUs The risk of VLU recurrence is reduced through the maintenance of practices that promote the health of the legs. There is some evidence that compression systems are effective in reducing the risk of recurrence of VLUs. A C D B C D EBO B D Grade EBO C
13 3. BACKGROUND 3. Venous leg ulcers The most common causes of lower extremity ulcers are venous hypertension, arterial disease, neuropathy (usually due to diabetes), pressure injury and ischaemia. Venous leg ulceration is a debilitating, chronic condition that affects people of all ages. Venous ulceration is generally considered to result from venous occlusion, incompetent calf muscle pump function or venous valvular failure that give rise to venous hypertension. 4 Venous hypertension accounts for nearly 80% of all leg ulcers. 5 Venous ulceration is strongly related to risk factors such as family history of, or previous surgery for varicose veins; venous disease; phlebitis; deep vein thrombosis (DVT); congestive cardiac failure; obesity; immobility 6 and previous leg injury. 5 Currently VLU management is a significant burden on patients, their families and the health care system. Venous leg ulcers are the most common clinical wound problem seen in general practice and community nurses spend some 50% of their time treating leg ulcers. 7-9 Viewed in the context of an ageing Australian population, the financial and time burden of managing VLUs will remain a significant burden on the Australian health system into the future. Development of strategies to both reduce the initial development of VLUs and more effectively manage their treatment should be considered a national health priority. Australian data indicates that approximately 99% of individuals with a VLU are aged 60 years or over. 20 Treatment costs average at $AUD 2300 per individual. 20 In 996 the private hospital cost for a mean stay of 23.9 days for management of chronic leg ulceration was estimated to be $AUD In the Silver Chain study conducted in the mean cost of treating a VLU in the community was $AUD In a similar survey found the mean cost to heal any leg ulcer was $AUD 436 when comprehensive assessment was implemented. This study, which was conducted in Department of Veterans' Affairs clients predominately aged over 80 years, demonstrated that implementation of comprehensive assessment and management strategies has the potential to significantly reduce the cost of leg ulcer treatment to the health care system The need for a guideline The following points indicate there is a high degree of urgency for a guideline on management of VLUs: There is a high incidence of VLUs and recurrence within the Australian and New Zealand communities., 2 2
14 Many rural individuals, who have a high rate of hard-to-heal wounds, are disadvantaged due to inadequate access to health care diagnostic and management services. 23 No current national clinical guidelines exist for the Australian and New Zealand health care context. Clinical guidelines have been developed in other regions including New Zealand (999); Europe (2003); Canada (2004); UK (2006) and Scotland (200) There is a lack of awareness within the broader community regarding the assessment, prevention and management of VLUs. There is a need to address variability in professional knowledge and inequity in implementation of best practice in the management of leg ulcers. Venous leg ulcer research is not a funding priority. An anticipated increase in VLUs amongst the ageing population will result in a substantial increase in health costs. The guideline seeks to assist health professionals to: accurately diagnose and assess VLUs; optimise management and promote self management; prevent or delay complications associated with VLUs; optimise quality of life; and reduce the risk of recurrence. 3.3 Scope and target population The guidelines are intended for use by health professionals including but not limited to medical and surgical specialists, general practitioners, allied health professionals, nurse practitioners, nurses, pharmacists, and Aboriginal health workers. The guidelines could also be used as an informative source for consumers. Guidelines are intended to refer to people of all ages. The guidelines are intended for use in health care settings in metropolitan, regional, rural and remote areas of Australia and New Zealand. The guidelines will seek to address issues specific to special populations including: People living in rural and remote areas; People from an Aboriginal and Torres Strait Islander background; People from a Maori background; and People from ethnically, culturally and linguistically diverse (CALD) backgrounds. 3.4 Focus of the guideline The guideline focus is leg ulcers of a venous origin. Research relating to other types of leg ulcers was not included in the literature review. 3
15 The Expert Working Committee alerts the users of this guideline to the importance of accurate diagnosis of the type of ulcer being treated before implementing recommendations on the management of VLUs. 3.5 Process The Expert Working Committee (Appendix One) who has overseen the development of the guideline and supporting documents comprised of a vascular surgeon, geriatrician, nurse practitioners, registered nurses, three consumer representatives, a medical research consultant and a National Health and Medical Research Council (NHMRC) advisor. The process used to develop the guideline is outlined in full detail in the process report (Appendix Two). This guideline is based on an evidence-based literature review conducted to NHMRC requirements. Evidence statements A systematic search for literature published from 985 to 2009 was conducted and studies providing Level I evidence or Level II evidence on the NHMRC Levels of evidence scale 28 (see Appendix Two) were considered for inclusion. Individual research papers that met the inclusion criteria were critically appraised using checklists developed by SIGN 29 and given an overall descriptive quality of high, moderate or low. For areas considered important by the Expert Working Committee but for which there was limited level I or II evidence available (eg. assessment of VLUs) relevant lower level evidence, including expert opinion and consensus guidelines, was utilised. A summary of the supporting evidence used to grade the recommendation is provided with each evidence based research recommendation. Recommendations Each recommendation statement is supported by a grading from A to D (evidence based research) or EBO (expert based opinion) that reflects the strength of the recommendation and the trust or confidence health professionals can place in the recommendation when it is implemented in clinical practice. The recommendation grades are based on NHMRC additional levels of evidence and grades for recommendations for developers of guidelines (2005) 28 presented in Table one. 4
16 Table one: Recommendation grades 28 Evidence based research A Excellent evidence - body of evidence can be trusted to guide practice B C D Good evidence - body of evidence can be trusted to guide practice in most situations Some evidence - body of evidence provides some support for recommendation(s) but care should be taken in its application Weak evidence - body of evidence is weak and recommendation must be applied with caution Expert based opinion Consensus evidence there was insufficient evidence to make a graded recommendation due to insufficient or no evidence from systematic reviews or EBO RCTs or the literature search not locating research addressing the field. The EBO recommendations are supported by all members of the Expert Working Committee. The overall grade of each recommendation is based on a summation of an appraisal of individual components of the body of evidence on which the recommendation is based, including volume and consistency of the evidence. Table 3 shows the body of evidence assessment matrix, listing all the components that were considered when assessing the body of evidence, together with the grades used. 28 Expert based opinion recommendations were developed through group discussion and . The topics are those that were raised by members of the Expert Working Committee as being significant to the prevention, assessment and management of VLUs. In most instances they cover topics for which there is no high level evidence available, often because RCT designs are inappropriate for evaluation of the intervention. Discussion continued until consensus was reached. The full grading for each of the research based recommendations is available in the companion document Grading of the Australian and New Zealand research based recommendations for the prevention and management of venous leg ulcers. The Expert Working Committee supports all the recommendations and intends that they are used in conjunction with clinical judgement and clinician and patient preferences. Practice tips Most recommendations are accompanied by practice tips to assist clinicians to implement the recommendation. The practice tips were developed by the Expert Working Committee and reflect their considerable experience in assessing and managing VLUs in a range of clinical settings. 5
17 3.6 Limitations of the guideline Medication information The literature search was not designed to retrieve safety trials for pharmacological interventions. The guideline does not seek to provide full safety and usage information on any medications, dressings, devices or antiseptic solutions; however commonly available safety and usage tips have been included. The selection of pharmacological interventions is complex, and should consider the specific patients clinical profile and personal preferences. The Expert Working Committee recommends consulting the National Prescribing Service ( Australian Therapeutic Guidelines ( or New Zealand Medicines and Medical Devices Safety Authority ( for detailed prescribing information including: indications and usage; drug dosage and route of administration; contraindications and interactions; supervision and monitoring requirements; and product characteristics. Wound care therapies The literature search was not designed to retrieve safety trials for wound care therapies including antimicrobials and other topical preparations. All products should be used according to manufacturer s directions. Search date The guideline is based on the best evidence published from January 985 to September Evidence published before and after these dates has not been reviewed or considered for the guideline. Interventions and types of research The search strategy was limited to specific levels of evidence. Research on interventions for managing and preventing VLUs was limited to NHMRC Level and NHMRC Level 2 evidence. Only interventions that have been investigated using a RCT design or that had been included in a systematic review or meta-analysis were considered in the grading of the recommendations addressing interventions. Lower levels of evidence have been incorporated into practice tips related to prevention, diagnosis, assessment and management of VLUs. Interventions that may have been investigated using different study designs are not represented in the guideline. The guideline is not intended to confirm or refute the 6
18 effectiveness, nor provide guidance on the use of interventions that have not been included, as the evidence has not been reviewed. The guideline does not include surgical interventions for managing venous disease. Lack of evidence For some interventions there was limited evidence from which to draw conclusions on potential effectiveness. Some interventions have received a lower grade, not due to a lack of support, but due to lack of research that has been conducted on the intervention s efficacy. In addition, some interventions may provide benefit for outcomes that have not been addressed in the research (eg. patient well being). The Expert Working Committee acknowledges that lack of evidence is not evidence of lack of effect. Some interventions were not supported or received lower grades due to lack of evidence of effect. The Expert Working Committee acknowledges that this refers to lack of evidence of effect over placebo or standard therapy, that is; patients may receive beneficial outcomes from the intervention; however, these do not exceed beneficial effects that can be expected from a placebo therapy or standard care. Cost effectiveness This guideline does not address cost effectiveness or the economic feasibility of the recommendations. 7
19 4. RECOMMENDATIONS FOR PRIMARY PREVENTION OF VLUs 4. Management of venous hypertension Prevention of VLUs requires the management of underlying venous disease. Early detection, management and prevention of deep vein thrombosis (DVT) and consideration of treatment of venous hypertension with surgery and phlebotic interventions are important in the prevention of VLUs. Surgical interventions were beyond the scope of this guideline; however, the Expert Working Committee acknowledges the role that venous surgery plays in treating venous hypertension and preventing the development of VLUs. The literature search did not identify any research related to the management of venous hypertension with the specific objective of preventing VLUs. However, the relationship between venous hypertension and VLUs is acknowledged in the literature and detection and management of the former is highlighted by the Expert Working Committee as a priority in the prevention of VLUs. Adequate prevention and management of venous hypertension includes: early detection and management of deep vein thrombosis deep vein thrombosis prophylaxis access to venous surgery and phlebology interventions. (EBO) 4.2 Compression therapy Compression therapy aims to promote venous return, reduce venous pressure and prevent venous stasis. Commencement of compression therapy in patients with signs and symptoms helps reduce the long term effects of venous disease. More information on compression therapy is provided in the recommendation for the treatment of VLUs. There was insufficient evidence to make an evidence based recommendation on the use of compression for primary prevention of VLUs because no appropriate studies were identified in the literature search, possibly due to the limitations on population types. The Expert Working Committee reached consensus that compression therapy has a demonstrated effect in improving venous return and is an effective therapy to prevent the initial development of VLUs. Applying compression therapy is effective in preventing the initial development of a VLU. (EBO) 8
20 Caution Refer to the caution statement in the recommendation for use of compression therapy in the treatment of VLUs. Practice tips Commence primary prevention compression therapy after a patient experiences DVT or severe leg trauma, or during prolonged immobility, especially when there is a past history of DVT. There is insufficient evidence on the most effective degree of compression required to prevent an initial ulcer; however the Expert Working Committee s consensus is that compression should be 8 30 mmhg at a minimum. Further practice tips can be found in the section on compression therapy for the treatment of VLUs. Evidence statement The literature search did not identify any studies specifically investigating the prevention of VLUs using compression therapy. The search may have failed to identify relevant studies if they did not list VLUs as an outcome measure in the abstract, or if they were conducted in populations without diagnosed CVI. The Expert Working Committee considered that compression therapy is effective in preventing the development of VLUs, for patients at high risk of VLU. One good quality, randomised cross over trial 30 (n=25) compared the effectiveness of low grade compression (0 to 20 mmhg) stockings in reducing painful discomfort in female patients with early stage chronic venous disease. Participants were randomised to wear either knee high low compression or placebo stockings. Results showed compression stockings were associated with significant improvement in pain (p=0.025), heavy legs (p=0.0025), cramps (p=0.0379), ankle swelling (p=0.0240), mood (p<0.0), and daily work (p<0.05), but there was no differences in ratings of paresthesia. There was no significant difference in any of the objective outcome measures; however, at commencement of the trial venous filling time and pump power were within normal limits so there was limited opportunity for significant improvement Phlebotics Phlebotics are venoactive drugs that are reported to have effects on both the macrocirculation (eg. improving venous tone) and microcirculation (eg. decreasing capillary hyperpermeability). The group of drugs known as phlebotics consists of both natural flavonoids that are manufactured from plant extracts and synthetic products. 3 There is inconsistent evidence on the effectiveness of phlebotics in preventing the development of VLUs in patients with venous disease. (Grade C) 9
21 Evidence statement A Cochrane review 3 investigated the effectiveness of oral and topical phlebotics for treating CVI. One of the primary outcomes of the SR was prevention of VLUs, which was reported in two trials. The trials, conducted in participants with moderate CVI, were of moderate to low quality and of short duration ( to 3 months) and all participants used concurrent compression therapy. The trials compared the effectiveness of diosmine, hidrosmine or rutosides (n=80 over two trials) to placebo (n=80 over two trials). Pooled findings showed no statistically significant effect for phlebotics compared to placebo (59 ulcers vs. 60 ulcers, fixed effects model RR 0.95; 95% CI 0.80 to.3, p=0.56). When analysis was restricted to the higher quality trial, the effect for phlebotics in preventing VLU bordered on significance (39 ulcers vs. 46 ulcers; RR 0.83, 95% CI 0.69 to.00, p=0.056). The safety analysis included data from all trials included within the review, most of which did not report ulcer development as an outcome measure. Pooled data from 3 studies found no significant difference in the rate of adverse events between phlebotics and placebo. The reviewers concluded that there was insufficient evidence to suggest that phlebotonics are effective in treating CVI; and the findings regarding effect in preventing VLUs were inconsistent RECOMMENDATIONS FOR ASSESSMENT, DIAGNOSIS AND REFERRAL FOR VLUs 5. Initial and ongoing assessment The optimal outcome for the patient with a VLU is facilitated by a continuous process of general, wound and environment assessment. These factors determine ulcer aetiology and wound healing and can inform the ongoing development of a treatment plan. 32 Using a formal ulcer assessment process such as the New Zealand Leg Ulcer Pathway can simplify ongoing monitoring and assessment of ulcer. The VLU pathway provides a model for national/international analysis on venous ulcer management, complications, outcomes and resources. Venous leg ulcer pathways enable clinicians to compare outcomes, based on this VLU guideline, from different practice settings, treatment options, and demographic groups. 5.. Patient assessment Only one trial investigating methods of assessing patients with VLUs was identified in the literature search. The trial provided low quality evidence on the efficacy of pulse oximetry that was insufficient to make a research based recommendation. The Expert Working Committee concurs with other expert groups 25, that patient assessment is crucial to the appropriate management of VLUs. All patients presenting with a leg ulcer should receive a comprehensive assessment by a health professional trained in the assessment and management of VLUs. (EBO) CEAP classification could be used to evaluate and classify venous disease. (EBO) 20
22 Essential in comprehensive assessment is the identification of the aetiology of the leg ulcer. Specifically, the use of compression therapy the most effective treatment for VLU can result in damage to the lower limb if applied incorrectly or to a non-venous leg ulcer. 34, 35 Assessment should seek to identify co-morbidities that may influence treatment of the VLU and/or require concurrent management. Co-morbidities that require further investigation and management include peripheral arterial disease, rheumatoid arthritis, vasculitis, a past history of multiple skin cancers(lesions)and diabetes mellitus. 34, 35 Assessment should be conducted and documented by a health professional with education and experience in the management of VLUs. 25, Assessment should include a patient history, examination of the leg, vascular assessment, biochemical analysis, microbiology, nutritional assessment, psychological and social assessments and past treatments for the ulceration Patient history A clinical history indicative of a leg ulcer of venous origin includes: 35 confirmed venous disease family history of leg ulceration varicose veins previous or current DVT phlebitis surgery or trauma of the affected leg chest pain, haemoptysis or pulmonary embolism occupations of prolonged standing or sitting The patient s leg ulcer history helps develop a comprehensive picture of the disease history. Information that can assist in diagnosis and development of a treatment plan includes: 35 the duration of the current ulcer, previous ulcers and the time they have taken to heal, time spent free of ulcers strategies used to manage previous ulcers Examination of the leg A bilateral limb assessment 25, 33, 35 and gait assessment should be conducted. Signs and symptoms that are indicators of VLUs are outlined in Table two. 2
23 Table two: Clinical indicators of venous leg ulcers 36 Signs or symptoms in isolation may not be clinical indicators of VLUs. A grouping of the following signs and symptoms is indicative of an ulcer of venous origin. Predisposing factors Associated changes in the leg Ulcer location History of deep vein thrombosis (DVT) Valvular incompetence in the perforating veins Obesity Familial history of venous ulcers Trauma or surgery to the leg/s Decrease in calf muscle pump function Firm ( brawny ) oedema Haemosiderin deposition (reddish brown pigmentation) lipodermatosclerosis Evidence of healed ulcers Dilated and torturous superficial veins Limb may be warm Atrophie blanche Eczema Altered shape -Inverted champagne bottle Ankle flare Anterior to medial malleolus Pretibial area Generally lower third of leg Ulcer characteristics Pain Surrounding area Pulses Irregular shaped edges Ruddy granulation tissue Absence of non-viable tissue Pain varying from nil, to mild or extreme Pain may be relieved by elevation of leg Leaking oedema may result in maceration, pruritis and scale Hot itchiness of the leg Normal foot/leg pulses Vascular assessment The aim of vascular assessment is to distinguish arterial aetiologies from venous and other aetiologies and assess the extent of venous insufficiency. Table three describes investigations that can assist in the diagnosis of ulcer aetiology. 22
24 Table three: Investigations Blood pressure (BP) 25, 33, 35, 37 Blood Ankle brachial pressure index (ABPI) 25, 32-35, 37 pressure measures th pressure of the blood on the vessel walls using a spyphgmomanometer. It provides an indication of possible presence of a range or cardiovascular diseases. The systolic BP is used in calculation ABPI. Non invasive vascular test which identifies large vessel peripheral arterial disease in the leg. It provides evidence of adequate arterial blood flow in the leg before use of compression therapy. Systolic BP is measured at the brachial artery and also at the ankle level. Using these two measurements ABPI is calculated as the the highest systolic blood pressure in both ankles (either dorsalis pedis or posterior tibial pressures) divided by the higher brachial systolic pressure in both arms, which is the best estimate of central systolic blood pressure. 38 Patients with a leg ulcer and an ABPI less than.0 or greater do not have evidence of arterial disease. 38 Duplex ultrasound 32 A non invasive test that combines ultrasound with Doppler ultrasonography in which the blood flow through arteries and veins can be investigated to reveal obstructions. 39 An ABPI can be performed at the same time. Photoplethysmography (PPG) 32 Pulse oximetry34, 37 Non Toe brachial pressure index (TBPI) Transcutaneous oxygen (TcpO2) 32 A non invasive test that measures venous refill time by using a small light probe that is placed on the surface of the skin just above the ankle. The test required the patient to perform calf muscle pump exercises for brief periods followed by rest. 40 The PPG probe measures the reduction in skin blood content following exercise. This determines the efficiency of the musculovenous pump and the presence of abnormal venous reflux. Patients with problems with the superficial or deep veins usually have poor emptying of the skin and abnormally rapid refilling usually less than 25 seconds invasive test that measures the red and infrared light absorption of oxygenated and deoxygenated haemoglobin in the digit. Oxygenated hemoglobin absorbs more infrared light and allows more red light to pass through a digit. Deoxygenated hemoglobin absorbs more red light and allows more infrared light to pass through the digit. There is insufficient evidence to recommend this investigation as the primary diagnostic tool. 34, 37 A non invasive test which measures arterial perfusion in the toes and feet. A toe cuff is applied to the hallux (or second toe if amputated) and the pressure is divided by the higher brachial systolic pressure in both arms, which is the best estimate of central systolic blood pressure. The TBPI is used to measure arterial perfusion in the feet and toes of patients with incompressible arteries due to calcification as seen in patients with diabetes and renal disease or with an ABPI of greater than.3 mmhg.{wound Ostomy Continence Nurses Society, 2008 #2} Measures the amount of oxygen reaching the skin through blood circulation. There is insufficient evidence to recommend this investigation as the primary diagnostic test. 34, 37 23
25 The CEAP classification is an international consensus method of assessing venous disease. It incorporates clinical, (a)aetiological, anatomical and pathophysical evaluation. The scale consists of seven classifications from C0 to C6 that describe the severity of the patient s venous disease. Patients presenting with one of more active VLU would be classified as C6, which describes the most severe venous disease. Patients with evidence of healed VLUs are categorised as C5 due to the high risk of recurrent ulceration. Doppler ultrasound measurement of ankle brachial pressure index (ABPI) is the investigation most frequently used to identify arterial aetiology. 25, 33-35, 37 However, results can be unreliable when ABPI is conducted by untrained health professionals and in patients with calcification or diabetes. 35 It may also be difficult to perform accurately in patients with severe oedema, lymphoedema, very painful ulcers or extensive ulceration. 37 Toe brachial pressure index (TBPI) may prove more accurate for identifying arterial perfusion the in feet and toes of patients with diabetes and renal disease with an ABPI of greater than.3 mmhg.{wound Ostomy Continence Nurses Society, 2008 #2} Pulse oximetry could be considered to support the diagnosis of a venous ulcer; however there is insufficient evidence to recommend this investigation as the primary diagnostic tool. 34, Biochemical analysis Appropriate biochemical analysis may include: blood glucose25, 32, 33, 35 haemoglobin 32 urea and electrolytes 32 plasma albumin 32 lipids 32 rheumatoid factor 32 auto antibodies 32 white blood cell count 32 erythroctye sedimentation rate 32 C-reactive protein 32 liver function tests Microbiology and histopathology Microbiology assists in the identification of infection and histopathology can identify malignant or other aetiologies. Investigations may include: bacterial wound swab or biopsy for bacterial status 32 wound biopsy if malignancy or other aetiology is suspected32, 34, Nutritional assessment A nutritional assessment should be conducted. 25, 33 This may include: weight and/or body mass index (BMI) 25, 33, 35, 37 24
26 food and fluid intake 32 hair and skin changes 32 mini nutritional assessment Pain assessment A pain assessment that investigates pain intensity with a validated pain scale should be conducted. 25, 32, 33, Psychosocial, quality of life and social assessments Conduct psychosocial and social assessments using appropriate assessment tools. 25, 33 Appropriate assessments include: Mini mental examination 32 Hospital anxiety and depression scale 32 Hamilton scale 32 Quality of life scales for specific health populations, 4, 32 for example the the Cardiff Wound Impact Schedule (CWIS) and Chronic Venous Insufficiency Questionnaire (CVIQ) that have both been validated in patients with venous disease. 4 Practice tips Bacterial swabs should only be taken when the ulcer shows clinical signs of infection. 34, 35 A structured, systematic leg ulcer assessment tool can assist in accurate and comprehensive assessment that is clearly documented. Evidence statement A low quality observational cohort trial 37 investigated the reliability of pulse oximetry in assessing patients prior to commencing treatment of leg ulcers. Pulse oximetry was compared with the gold standard, Doppler ABPI. Participants (n=39) were attending a leg ulcer clinic; however their specific selection for inclusion in the trial was not reported. Pulse oximetry and ABPI were both measured after the patient had reclined at a 40 angle for 5 minutes. Pulse oximetry was conducted on the patient s toe and finger to determine a toe finger oximetry index (TFOI) that was reported to be analogous to an ABPI measurement. Analysis of the ratio of TFOI and Doppler ABPI showed only fair agreement (kappa 0.29, weighted kappa 0.39). The researchers suggested pulse oximetry could be used to determine whether compression therapy is appropriate for patients presenting with leg ulcers. 37 A low quality SR 4 reported on the life impact of VLUs. Participants in the research included in the review were primarily older females. The review reports that two psychosocial assessment tools are particularly relevant to populations with VLU the Cardiff Wound Impact Schedule (CWIS) and Chronic Venous Insufficiency Questionnaire (CVIQ). The CWIS is specific to, and has been validated in VLU populations. It includes sections on physical symptoms and daily living, social life, well being and overall health related QOL. The CVIQ has been validation in populations with venous insufficiency and for people with a VLU, offers the advantage of being able to compare scores to pre-ulceration psychosocial status. The review concluded that patients with VLU have a 25
VENOUS LEG ULCERS (VLU)
 VENOUS LEG ULERS (VLU) REOMMENDTION S Evidence-based gradings Excellent evidence ody of evidence can be trusted to guide practice. Good evidence ody of evidence can be trusted to guide practice in most
VENOUS LEG ULERS (VLU) REOMMENDTION S Evidence-based gradings Excellent evidence ody of evidence can be trusted to guide practice. Good evidence ody of evidence can be trusted to guide practice in most
Australian and New Zealand Clinical Practice Guideline for Prevention and Management of Venous Leg Ulcers. Abridged version
 Australian and New Zealand Clinical Practice Guideline for Prevention and Management of Venous Leg Ulcers Abridged version October 2011 Printed publication This work is copyright. You may reproduce the
Australian and New Zealand Clinical Practice Guideline for Prevention and Management of Venous Leg Ulcers Abridged version October 2011 Printed publication This work is copyright. You may reproduce the
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Dr Paul Thibault. Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology
 Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
AWMA MODULE ACCREDITATION. Module Three: Assessment and Management of Lower Leg Ulceration
 AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Three: Assessment and Management of Lower Leg Ulceration Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Lower Leg Ulceration. Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network;
 Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
Lower Leg Ulceration Wendy McInnes Vascular Nurse Practitioner; Northern Adelaide Local Health Network; wendy.mcinnes@sa.gov.au 0447 051 036 1 Lower Leg Ulceration A manifestation of underlying pathology/disease
Arterial & Venous Ulcers. A Comprehensive Review Assessment & Management
 Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Lower Extremity Venous Disease (LEVD)
 Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND
 GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
GUIDELINES FOR THE MEASUREMENT OF ANKLE BRACHIAL PRESSURE INDEX USING DOPPLER ULTRASOUND AIM To provide evidence based principles for the measurement of Ankle Brachial Pressure Index (ABPI) using a BACKGROUND/EVIDENCE
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS
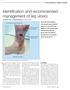 Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
How to manage leg ulcers in the elderly
 How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
OHTAC Recommendation. Endovascular Laser Treatment for Varicose Veins. Presented to the Ontario Health Technology Advisory Committee in November 2009
 OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
Chronic Venous Insufficiency Compression and Beyond
 Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Independent evaluation of BEMER physical vascular regulation therapy
 of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
All WALES LYMPHOEDEMA GUIDANCE:
 All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
Leg ulcers. Causes and management. OBJECTIVE This article outlines the assessment and management of patients with leg ulceration.
 THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
THEME Wounds Leg ulcers Causes and management BACKGROUND A leg ulcer is not a disease but the manifestation of an underlying problem that requires a clear diagnosis. Sandra Dean RN, is nurse consultant
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options
 Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Improving customer care in compression hosiery
 Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Improving customer care in compression hosiery Introduction Within the modern NHS, the Pharmacy Team provides the front line service that most patients have contact with. Compression hosiery has a key
Management of Post-Thrombotic Syndrome
 Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Promoting best practice in leg ulcer management
 Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Vascular dysfunction and vulnerable skin
 Vascular dysfunction and vulnerable skin Professor Peter Vowden Honorary Consultant Vascular Surgeon Clinical Director WoundTec HTC Bradford, UK 1 Exploring the clinical problem associated with the application
Vascular dysfunction and vulnerable skin Professor Peter Vowden Honorary Consultant Vascular Surgeon Clinical Director WoundTec HTC Bradford, UK 1 Exploring the clinical problem associated with the application
Leg ulcers are non-healing
 Clinical Chronic REVIEW WOUNDS Doppler assessment: getting it right Full leg ulcer assessments are important in order to identify the aetiology of patients leg ulcer and Doppler ultrasounds form a part
Clinical Chronic REVIEW WOUNDS Doppler assessment: getting it right Full leg ulcer assessments are important in order to identify the aetiology of patients leg ulcer and Doppler ultrasounds form a part
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Leg Ulcer Case Study
 Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT. SCOPE: Western Australia. Clinical Protocol for Venous Leg Ulcer Management
 CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
CLINICAL PROTOCOL - VENOUS LEG ULCER MANAGEMENT SCOPE: Western Australia Clinical Protocol for Venous Leg Ulcer The following protocol outlines the sequence of events in the assessment and management of
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES
 ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
New Guideline in venous ulcer treatment: dressing, medication, intervention
 New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
Interactive Learning Session
 Chronic Venous Disease - Part I Interactive Learning Session 2011 Ali Sabbour Prof of Vascular Surgery http://mic.shams.edu.eg/moodle6 Login as a guest Surgery 2 Ali Sabbour - Chronic Venous Disease Intended
Chronic Venous Disease - Part I Interactive Learning Session 2011 Ali Sabbour Prof of Vascular Surgery http://mic.shams.edu.eg/moodle6 Login as a guest Surgery 2 Ali Sabbour - Chronic Venous Disease Intended
Determine the patients relative risk of thrombosis. Be confident that you have had a meaningful discussion with the patient.
 Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Dr Peter Chapman-Smith
 Dr Peter Chapman-Smith Phlebologist NZ Stem Cell Treatment Centre, Whangarei 12:00-12:30 Healing Those Heartsink Leg Ulcers Healing Those Heartsink Leg Ulcers Practice Nurses Presentation GPCME Christchurch
Dr Peter Chapman-Smith Phlebologist NZ Stem Cell Treatment Centre, Whangarei 12:00-12:30 Healing Those Heartsink Leg Ulcers Healing Those Heartsink Leg Ulcers Practice Nurses Presentation GPCME Christchurch
RADIOFREQUENCY ABLATION. Professor M Baguneid MB ChB MD FRCS
 RADIOFREQUENCY ABLATION This minimally invasive treatment involves closing the faulty veins using a keyhole approach thereby avoiding the larger cuts and avoiding stripping of the veins. Professor M Baguneid
RADIOFREQUENCY ABLATION This minimally invasive treatment involves closing the faulty veins using a keyhole approach thereby avoiding the larger cuts and avoiding stripping of the veins. Professor M Baguneid
Priorities Forum Statement
 Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Additional Information S-55
 Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Address: Left Leg. other: Nails: thick yellow brittle fungus abnormal thick yellow brittle fungus abnormal
 South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
South West Regional Wound Care Toolkit: Interdisciplinary Lower Leg Assessment Form Instructions for use: Competent/ Proficient/ Expert level HCP to complete if lower leg ulcer present or risk of ulcer
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device
 VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
Managing venous leg ulcers and oedema using compression hosiery
 Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
Managing venous leg ulcers and oedema using compression hosiery Tickle J (2015) Managing venous leg ulcers and oedema using compression hosiery. Nursing Standard. 30, 8, 57-63. Date of submission: July
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Arterial Studies And The Diabetic Foot Patient
 Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Post-Thrombotic Syndrome Prevention and Management. Dr. Ashwini Bennett
 Post-Thrombotic Syndrome Prevention and Management Dr. Ashwini Bennett Disclosures No disclosures relevant to this presentation Outline Importance of VTE and PTS Aetiology of PTS PTS risk factors PTS clinical
Post-Thrombotic Syndrome Prevention and Management Dr. Ashwini Bennett Disclosures No disclosures relevant to this presentation Outline Importance of VTE and PTS Aetiology of PTS PTS risk factors PTS clinical
COMMISSIONING POLICY
 Ref No. 1a7.5 COMMISSIONING POLICY Surgery for venous disease of the leg (Varicosities of the Long Saphenous Vein) April 2011 CONTENTS Section Page Summary 2 1. Background 2 2. Criteria for eligibility
Ref No. 1a7.5 COMMISSIONING POLICY Surgery for venous disease of the leg (Varicosities of the Long Saphenous Vein) April 2011 CONTENTS Section Page Summary 2 1. Background 2 2. Criteria for eligibility
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
How to prevent blood clots whilst in hospital and after your return home
 How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
How to prevent blood clots whilst in hospital and after your return home Patient information WHAT What IS is DEEP deep VEIN vein THROMBOSIS? thrombosis? Deep Vein Thrombosis DVT is a blood clot within
Alberta Health. Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual
 Alberta Health Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual March 7, 2016 Revision History Description Date N-03, N 05 and N-07:
Alberta Health Alberta Aids to Daily Living Compression Stockings and Lymphedema Sleeves Ready Made Benefits Policy & Procedures Manual March 7, 2016 Revision History Description Date N-03, N 05 and N-07:
Venous leg ulcers: importance of early assessment and intervention for long-term success
 Venous leg ulcers: importance of early assessment and intervention for long-term success Introduction A venous leg ulcer (VLU) can be defined as: an open lesion between the knee and ankle joint that occurs
Venous leg ulcers: importance of early assessment and intervention for long-term success Introduction A venous leg ulcer (VLU) can be defined as: an open lesion between the knee and ankle joint that occurs
VTE Prophylaxis. NICE guidance. Providing venous thromboembolism (VTE) prophylaxis to all at risk hospital patients
 NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
JoyTickle, Tissue Viability Nurse Specialist, Shropshire Community Health NHS Trust
 Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Lower limb Ulceration Pathway: Leanne Atkin, Lecturer practitioner/vascular Nurse Specialist, School of Human and Health Sciences, University of Huddersfield and Mid Yorkshire NHS Trust, E mail: l.atkin@hud.ac.uk
Treating your leg ulcer
 Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Page 1 of 7 Treating your leg ulcer Introduction The information in this leaflet will answer many questions you may have about your leg ulcer. If you have any further questions about your condition or
Venous Insufficiency Ulcer
 Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
Efficacy of Velcro Band Devices in Venous and. Mixed Arterio-Venous Patients
 Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
Recurrent varicose veins. Information for patients Sheffield Vascular Institute
 Recurrent varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins that have recurred (come back). This leaflet explains more about recurrent
Recurrent varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins that have recurred (come back). This leaflet explains more about recurrent
Due to Perimed s commitment to continuous improvement of our products, all specifications are subject to change without notice.
 A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
First Coast Service Options (FCSO) Medicare Policy Primer
 First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
Wound Management Capital Health Network Practice Nurses 20 Feb 2018
 Wound Management Capital Health Network Practice Nurses 20 Feb 2018 ) MNP Judith Barker RN; NP; STN; B Hlth Sc (Nurs); MN (NP) Nurse Practitioner Wound Management Rehabilitation, Aged & Community Care
Wound Management Capital Health Network Practice Nurses 20 Feb 2018 ) MNP Judith Barker RN; NP; STN; B Hlth Sc (Nurs); MN (NP) Nurse Practitioner Wound Management Rehabilitation, Aged & Community Care
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Housekeeping 15/03/2016 URGO MEDICAL, HEALING PEOPLE. Tissue Viability information. Tissue Viability Intranet page
 TO REPAIR TO HEAL TO REPAIR TO HEAL TO LOVE TO TOUCH TO LOVE TO TOUCH TO LIVE TO MOVE TO LIVE TO MOVE TO SHARE TO CURE TO SHARE TO CURE URGO MEDICAL, HEALING PEOPLE Leg Ulcer Assessment 2016 Tissue Viability
TO REPAIR TO HEAL TO REPAIR TO HEAL TO LOVE TO TOUCH TO LOVE TO TOUCH TO LIVE TO MOVE TO LIVE TO MOVE TO SHARE TO CURE TO SHARE TO CURE URGO MEDICAL, HEALING PEOPLE Leg Ulcer Assessment 2016 Tissue Viability
Varicose veins. Information for patients Sheffield Vascular Institute
 Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
Varicose veins Information for patients Sheffield Vascular Institute You have been diagnosed as having varicose veins. This leaflet explains more about varicose veins and answers some of the most frequently
Chronic Venous Insufficiency
 Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND
 PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND (to achieve Ankle Brachial Pressure Index) First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To enable nurses
PROCEDURE FOR VASCULAR ASSESSMENT BY DOPPLER ULTRASOUND (to achieve Ankle Brachial Pressure Index) First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One To enable nurses
Varicose Veins are a Symptom of Vein Disease. Now you can treat the source of your varicose veins with non-surgical endovenous laser treatment.
 Varicose Veins are a Symptom of Vein Disease. Now you can treat the source of your varicose veins with non-surgical endovenous laser treatment. Approximately 1 in 5 adult Americans suffer from superficial
Varicose Veins are a Symptom of Vein Disease. Now you can treat the source of your varicose veins with non-surgical endovenous laser treatment. Approximately 1 in 5 adult Americans suffer from superficial
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
AWMA MODULE ACCREDITATION. Module Seven: Conservative Sharp Wound Debridement
 AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
In line with the professional requirements of the Nursing and Midwifery Council
 STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
STANDARDS OF PRACTICE FOR LEG CLUB STAFF October 2010 Foreword In line with the professional requirements of the Nursing and Midwifery Council Code: Standards of conduct, performance and ethics for nurses
VTE Prophylaxis. NEW NICE guidance. Providing venous thromboembolism (VTE) prophylaxis to all at risk hospital patients
 NEW NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
NEW NICE guidance NICE guidance (MTG19) supports the use of the geko device for people who have a high risk of VTE and for whom pharmacological or other mechanical methods of VTE prevention are impractical
Jackie Stephen-Haynes. Compression therapies- Does. Jackie Stephen-Haynes 2011
 Jackie Stephen-Haynes Compression therapies- Does compression meet the patients needs? 2011 Aims For practitioner to be able to consider compression options and the impact for the patient Leg Ulcer Definition
Jackie Stephen-Haynes Compression therapies- Does compression meet the patients needs? 2011 Aims For practitioner to be able to consider compression options and the impact for the patient Leg Ulcer Definition
Inferior Vena Cava Filter for DVT
 Inferior Vena Cava Filter for DVT Deep Vein Thrombosis A deep vein thrombosis (DVT) is a blood clot that forms in a deep vein. This is a serious condition that occurs more often than you might think. If
Inferior Vena Cava Filter for DVT Deep Vein Thrombosis A deep vein thrombosis (DVT) is a blood clot that forms in a deep vein. This is a serious condition that occurs more often than you might think. If
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
PROF S.R.SUBRAMMANIYAN INSTITUTE OF VASCULAR SURGERY MADRAS MEDICAL COLLEGE
 PROF S.R.SUBRAMMANIYAN INSTITUTE OF VASCULAR SURGERY MADRAS MEDICAL COLLEGE VARICOSE VEINS OF SUPERFICIAL VENOUS SYSTEM OF LOWER LIMBS A SYMPTOM NOT A DISEASE INITIAL,MILD CASES and severe cases with contraindication
PROF S.R.SUBRAMMANIYAN INSTITUTE OF VASCULAR SURGERY MADRAS MEDICAL COLLEGE VARICOSE VEINS OF SUPERFICIAL VENOUS SYSTEM OF LOWER LIMBS A SYMPTOM NOT A DISEASE INITIAL,MILD CASES and severe cases with contraindication
Varicose Vein Cyanoacrylate Glue treatment
 The South West s premier independent healthcare and cosmetic clinic Varicose Vein Cyanoacrylate Glue treatment Varicose veins are a sign of underlying venous insufficiency and affect 20 30% of adults.
The South West s premier independent healthcare and cosmetic clinic Varicose Vein Cyanoacrylate Glue treatment Varicose veins are a sign of underlying venous insufficiency and affect 20 30% of adults.
Elizabeth Frost District Nurse Capital and Coast DHB
 Elizabeth Frost District Nurse Capital and Coast DHB Holistic Assessment No progress Tenacity Lateral thinking Results Population base of 301,510 people live within the Capital & Coast district, with two
Elizabeth Frost District Nurse Capital and Coast DHB Holistic Assessment No progress Tenacity Lateral thinking Results Population base of 301,510 people live within the Capital & Coast district, with two
LEG ULCERATION. BY Helen Langthorne And Emma Rayner
 LEG ULCERATION BY Helen Langthorne And Emma Rayner Definition A leg ulcer is a loss of skin below the knee on the leg or foot which takes more than six weeks to heal (CKS 2012). Venous ulcer account for
LEG ULCERATION BY Helen Langthorne And Emma Rayner Definition A leg ulcer is a loss of skin below the knee on the leg or foot which takes more than six weeks to heal (CKS 2012). Venous ulcer account for
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
Occasional pain or other discomfort (ie, not restricting regular daily activity)
 Revised Venous Clinical Severity Score Pain : 0 Mild: 1 or other discomfort (ie, aching, heaviness, fatigue, soreness, burning) Occasional pain or other discomfort (ie, not restricting regular daily activity)
Revised Venous Clinical Severity Score Pain : 0 Mild: 1 or other discomfort (ie, aching, heaviness, fatigue, soreness, burning) Occasional pain or other discomfort (ie, not restricting regular daily activity)
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound
 Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU)
 Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU) Sami Khan, MD FACS Associate Professor of Surgery Division of Plastic and Reconstructive Surgery SUNY-Stony
Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU) Sami Khan, MD FACS Associate Professor of Surgery Division of Plastic and Reconstructive Surgery SUNY-Stony
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
Medical Policy Original Effective Date: 01/23/2019
 Page 1 of 12 Disclaimer Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans or the plan may have broader or more limited benefits
Page 1 of 12 Disclaimer Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans or the plan may have broader or more limited benefits
Clinical Examination of VASCULAR PATIENTS. Stephanie Hirst & Alexander Sunde
 Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) GUIDELINES FOR THE USE OF COMPRESSION HOSIERY Do not include made to measure on the prescription; the community pharmacy/dispensing practice will endorse
Lower Extremity Venous Insufficiency Evaluation
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
FIND RELIEF FROM VARICOSE VEINS. VenaSeal Closure System
 FIND RELIEF FROM VARICOSE VEINS VenaSeal Closure System UNDERSTAND Varicose veins may be a sign of something more severe venous reflux disease Your doctor can help you understand if you have this condition.
FIND RELIEF FROM VARICOSE VEINS VenaSeal Closure System UNDERSTAND Varicose veins may be a sign of something more severe venous reflux disease Your doctor can help you understand if you have this condition.
Appendix 1 to Direct Vision Sclerotherapy AUSTRALASIAN COLLEGE OF PHLEBOLOGY CLINICAL PROCEDURES. CP Direct Vision Sclerotherapy Clinical procedure
 Appendix 1 to Direct Vision Sclerotherapy AUSTRALASIAN COLLEGE OF PHLEBOLOGY CLINICAL PROCEDURES CP Direct Vision Sclerotherapy Clinical procedure 1 PURPOSE This procedure summarises the actions required
Appendix 1 to Direct Vision Sclerotherapy AUSTRALASIAN COLLEGE OF PHLEBOLOGY CLINICAL PROCEDURES CP Direct Vision Sclerotherapy Clinical procedure 1 PURPOSE This procedure summarises the actions required
PDP SELF-TEST QUESTIONNAIRE
 Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Number 5 CORE TUTORIALS IN DERMATOLOGY FOR PRIMARY CARE PDP SELF-TEST QUESTIONNAIRE METEOR CRATER, ARIZONA, USA LEG ULCERS Ulcer Full thickness loss of epidermis and some dermis, which will heal with scarring
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
lipodermatosclerosis standards of medical practitioners and the quality of patient care related to the treatment of venous disorders.
 Chattanooga s premiere VEIN CENTER Update on Venous Insufficiency, Varicose and Spider Veins 2016 Vincent W. Gardner, MD, FACS, RPVI Fellow, American College of Surgeons Board Certified, American Board
Chattanooga s premiere VEIN CENTER Update on Venous Insufficiency, Varicose and Spider Veins 2016 Vincent W. Gardner, MD, FACS, RPVI Fellow, American College of Surgeons Board Certified, American Board
