Early Reoperations after Primary Repair of Jejunoileal Atresia in Newborns
|
|
|
- Tamsin Irene Bates
- 5 years ago
- Views:
Transcription
1 Journal of Neonatal Surgery 2016; 5(4):42 Doi: /jns.v5i4.444 ORIGINAL ARTICLE Early Reoperations after Primary Repair of Jejunoileal Atresia in Newborns Fanny Yeung, Yuk Him Tam,* Yuen Shan Wong, Siu Yan Tsui, Hei Yi Wong, Kristine Kit Yi Pang, Christopher H Houben, Jennifer Wai Cheung Mou, Kin Wai Chan, Kim Hung Lee Division of Paediatric Surgery and Paediatric Urology, Department of Surgery, Prince of Wales Hospital, The Chinese University of Hong Kong, Hong Kong, China. How to cite: Yeung F, Tam YH, Wong YS, Tsui SY, Wong HY, Pang KK, et al. Early reoperations after primary repair of jejunoileal atresia in newborns. J Neonat Surg. 2016; 5:42. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Aim: To review nine-year experience in managing jejuno-ileal atresia (JIA) by primary resection and anastomosis and identify factors associated with reoperations. Methods: From April 2006 to May 2015, all consecutive neonates who underwent bowel resection and primary anastomosis for JIA were analyzed retrospectively. Patients with temporary enterostomy were excluded. Patient demographics, types of atresia, surgical techniques, need for reoperations, and long-term outcomes were investigated. Results: A total of forty-three neonates were included, in which nineteen (44.2%) of them were preterm and fourteen (32.6%) were of low birth weight. Thirteen patients (30.2%) had jejunal atresia whereas thirty patients (69.8%) had ileal atresia. Volvulus, intussusception and meconium peritonitis were noted in 12, 8, and13 patients, respectively. Eight patients (18.6%) had short bowel syndrome after operation. Ten patients (23.3%) required reoperations from 18 days to 4 months after the initial surgery due to anastomotic stricture (n=1), adhesive intestinal obstruction (n=1), small bowel perforation (n=2) and functional obstruction (n=6). Prematurity and low birth weight were associated with functional obstruction leading to reoperation (p=0.04& 0.01 respectively). The overall long-term survival was 97.7%. All surviving patients achieved enteral autonomy and catch-up growth at a median follow-up of 4.7 years. Conclusion: Long-term survival of JIA after primary resection and anastomosis are excellent. However, patients have substantial risk of early reoperations to tackle intraabdominal complications. Key words: Jejunoileal atresia; Primary resection and anastomosis; Reoperation INTRODUCTION Jejunoileal atresia (JIA) is a major cause of neonatal intestinal obstruction, with an incidence ranging from 1.3 to 2.9 per 10,000 live births[1-3].with advancement of neonatal intensive care, anesthesia, parenteral nutrition and operative techniques, the survival figure was reported to be around 80% in 1990s [4] and further climbed to more than 90% in the 21st century [1,5]. The operative management depends on the site of the atresia, the specific anatomical findings, associated gastrointestinal tract anomalies and the length of the remaining small bowel. In contemporary practice, resection of the proximally dilated bowel along with the atretic segment and primary anastomosis is the recommended choice of operation whenever possible [4,5,6]. The frequency of temporary stoma has decreased from over 20% in the 1970s to 10% in the 1990s [6]. A temporary enterostomy, however, is necessary in less favorable conditions with doubtful vascular integrity of bowel, significant intraperitoneal contamination by meconium peritonitis, and excessive discrepancy in the diameter between the distal Correspondence*: Dr. YH Tam, Division of Paediatric Surgery & Paediatric Urology, Department of Surgery, Prince of Wales Hospital, Shatin, NT, Hong Kong, China. E mail: pyhtam@surgery.cuhk.edu.hk 2016, Journal of Neonatal Surgery Submitted: Accepted: Conflict of interest: None Source of Support: Nil
2 and the proximally dilated bowel which is too long to be resected or tapered [4,5,7,8]. Despite significant decline in mortality, infants with JIA experience substantial morbidity after primary surgery [5]. Abdominal reoperation rate varied from 14% to 25% due to postoperative complications [6,7,9]. There are few studies, however, that investigated risk factors associated with re-laparotomy following primary repair of JIA. In this study, we reviewed our experience in managing patients with congenital JIA over a 9-year period and analyzed the long-term outcomes after proximal bowel resection with primary anastomosis and the factors associated with reoperation. MATERIALS AND METHODS After obtaining the approval of the clinical research ethics committee of our institution, we conducted a retrospective analysis of all consecutive neonates who underwent primary bowel resection and anastomosis for JIA between April 2006 and May 2015 in our hospital which is a tertiary referral center. Data about gestation, birth weight, associated anomalies, antenatal diagnosis, type of JIA, possible etiology, surgical techniques and postoperative outcomes were analyzed. JIA was classified into type I to IV as described by Grosfeld et al [10]. Short bowel syndrome(sbs) was defined by residual small bowel length less than 50cm, 75cm and 100cm for premature newborns of gestation between 28 and 36 weeks, term newborns, and older children respectively [5,8]. Prematurity and lowbirth-weight (LBW) were defined by gestation of less than 37 weeks at birth and birth weight of less than 2.5kg respectively. Reoperation was defined by any re-laparotomy for complications related to previous primary repair of the JIA. Categorical data were reported in percentage as frequency. Continuous variables were expressed as median with interquartile range (IQR). Continuous and categorical data were compared by Mann-Whitney U and chi-square tests, respectively. Statistical significance was defined by p value less than RESULTS A total of 49 neonates including 28 boys and 21 girls with operation for JIA were identified. Fortythree patients (87.8%) who had primary repair by resection of proximal atretic segment with primary anastomosis were included in the study whereas six patients who underwent enterostomy were excluded. The median age at operation was 1.0 day (IQR ) Among the 43 patients with primary anastomosis, 19 patients (44.2%) were premature. Median birth weight was 2.87 kg (IQR ) and 14 patients (32.6%) had LBW. One patient had associated congenital anomaly with small ventricular septal defect. Antenatal ultrasonography was suggestive of intestinal obstruction in 19 patients (44.2%) and polyhydramnios was noted in 3 patients (7.0%). Upon laparotomy, thirteen patients (30.2%) had jejunal atresia whereas thirty patients (69.8%) had ileal atresia. Nine patients (20.9%) had type I atresia, seven patients (16.3%) had type II atresia, nineteen patients (44.2%) had type III atresia and eight patients (18.6%) had type IV multiple atresias. Volvulus and intussusception were identified in 12 and 8 patients respectively, and were believed to be the etiology for JIA. The findings of volvulus and intussusception, usually evident on the distal atretic segments, were consistent with the generally accepted belief that JIA develops after intrauterine mesenteric vascular insults leading to bowel resorption and formation of atresia [4,5]. Meconium peritonitis was present in 13 patients and reflected the occurrence of intrauterine bowel perforations. Meconium peritonitis shares the same etiology as JIA formation and its presence in some of our patients was considered to be the consequence rather than the cause of JIA [5]. The median small bowel length remaining after proximal bowel resection and primary anastomosis was 101.5cm (IQR ). Eight patients (18.6%) had SBS. The discrepancy in diameter between the proximal and the distal bowel at anastomosis was less than or equal to 3 to 1 ratio. Thirty-three patients (76.7%) recovered uneventfully from the primary surgery and achieved full enteral feeding at a median of 22 days after the initial surgery, ranging from 10 to 96 days. Ten patients (23.3%) required abdominal reoperation at a median time interval of 34.5 days, ranging from 18 days to 4 months from the first operation. Reoperation was not associated with prematurity (p=0.67), LBW (p=0.18), jejunal/ileal atresia (p=0.84), in-utero intussusception (p=0.43), inutero volvulus (p=0.53), meconium peritonitis (p=0.42) and SBS (p=0.30). The indications of reoperation were anastomotic stricture (n=1), adhesive intestinal obstruction complicated with small bowel volvulus (n=1), small bowel perforation (n=2), and functional obstruction (n=6).
3 The patient with anastomotic stricture had resection of the stricture and bowel re-anastomosis at the reoperation. For the patient with volvulus due to adhesion band, small bowel resection and primary anastomosis was performed. The two patients with bowel perforations presented with sudden onset of distended abdomen with pneumoperitoneum on 23 and 34 days after the first operation. One of them was found to have a 2cm perforation on the anti-mesenteric side of the ileum 4cm distal to the previous anastomosis. The previous anastomosis was resected en bloc with the perforated bowel and re-anastomosis was performed. The initial pathology of this patient was type IIIb atresia with applepeel configuration of the distal small bowel. The other patient had a small punctate perforation at 25cm from the previous anastomosis and simple repair of the perforation was performed. On the other hand, six patients had reoperation for functional obstruction, in which five of them were born preterm at median gestation of 31 weeks and had LBW with median weight of 1.6 kg. Both prematurity (p=0.04) and LBW (p=0.01) were associated with functional obstruction leading to relaparotomy. These patients experienced persistent intestinal obstruction after the bowel resection and primary anastomosis. They presented with feeding intolerance, recurrent bouts of abdominal distension with dilated proximal bowel loops on abdominal radiograph when feeding was increased, and sepsis from bacterial overgrowth in dilated bowel loops. Contrast follow-through study was performed and showed patent anastomosis with transition from grossly dilated bowel on the proximal side to collapsed bowel on distal side of the anastomosis. Repeat laparotomy was performed at a median of 37 days, ranging from 18 days to 3 months after the first operation in view of persistent intestinal obstruction. Upon reoperation, patency of the previous anastomosis was confirmed in all 6 patients after adhesiolysis and bowel just proximal to the anastomosis was most dilated while bowel distal to anastomosis was collapsed. In 5 patients, the previous anastomosis was resected together with further proximal bowel resection. Immediate bowel re-anastomosis was performed in 3 patients while temporary stomas were fashioned in 2 patients. Histological examination of the resected anastomosis confirmed patency without fibrotic stricture and confirmed presence of ganglion cells in all 5 patients. The remaining one patient was treated by a side-to-side anastomosis between the dilated and collapsed bowel without resecting the original anastomosis as the primary anastomotic site was close to duodeno-jejunal flexure. For the 2 patients with temporary stomas, one recovered uneventfully after closure of stoma at her 3 months of age. The other one had recurrent functional obstruction after closure of the stoma and required another operation of side-to-side anastomosis between the dilated and collapsed bowel at his age of 4 months. His enteral feeding tolerance improved afterwards although full enteral feeding was unable to be achieved because of recurrent bowel distension. This patient, however, died at the age of 9 months because of sepsis and parenteral nutritionrelated liver failure, and was the only mortality in the whole study group. Except for the mortality case, the other 5 patients who underwent reoperation for functional obstruction eventually achieved full enteral autonomy from days after the reoperation. At a median follow-up of 4.7 years, all the surviving 42 patients achieved enteral autonomy and showed normal growth. The overall long-term survival was 97.7%. Mortality was associated with functional obstruction requiring reoperation (p=0.01), but not with prematurity (p=0.26), LBW (p=0.15), types of atresia (p=0.17), meconium peritonitis (p=0.51), abdominal reoperation (0.07) or SBS (0.63). DISCUSSION Almost 90% of our patients born with JIA were amenable to primary repair without the need of temporary enterostomy. However, almost onefourth of our patients needed an abdominal reoperation for postoperative complications after primary repair for JIA. The risk of reoperation is substantial and our finding appears to be in agreement with the impression in the existing literature although this issue has not been widely investigated. A previous study reported that 15 of 60 patients (25%) with JIA required a second abdominal operation for complications [9]. Another study recruiting 83 patients reported that 14.5% required repeat laparotomy for adhesive intestinal obstruction and another 6% for anastomotic leakage or stricture [6]. It has been known for several decades that the dilated proximal bowel should not be used to reconstruct the continuity of the gastrointestinal tract in instances of JIA as functional obstruction will result from the failure of the dilated bowel wall to generate adequate intraluminal pressure for effective peristalsis despite a patent anastomosis [11-13]. The improved neonatal care with total parenteral nutrition, and the recommended surgical principle of liberal resection of the dilated proximal bowel with primary anastomosis whenever the remaining bowel length permits, have contributed to
4 the improved long-term survival of newborns with JIA to 84% and the decline of temporary enterostomy to 10% in the 1990s[4,6]. It is, however, a clinical and subjective judgement by the operating surgeon to strike a balance between resecting adequate proximally dilated bowel to prevent leaving behind dysmotile bowel which would result in functional obstruction, and preserving as much bowel as possible to minimize the effect of short bowel syndrome. We have followed the recommendation in performing primary anastomosis that the discrepancy in diameter between the two ends of the bowel after proximal resection should not be excessive and the ratio should be less than 1 to 5 [5]. Nevertheless, we still encountered 6 cases (14%) of persistent functional obstruction after proximal resection and primary anastomosis and required reoperation. All these 6 patients did not tolerate enteral feeding at the expected pace after the initial surgery while the proximal bowel became progressively dilated and complicated with bacterial overgrowth and sepsis. Contrast follow-through study unequivocally showed patent anastomosis. Although peritoneal adhesions were found expectedly during re-laparotomy for these patients, the transition from distended to collapsed bowel was consistently at the previous anastomosis and the resected anastomosis did not show any evidence of stricture. Adhesiolysis alone does not suffice to correct functional obstruction and further proximal resection of the dysmotile bowel is necessary if the remaining bowel length permits. From our findings, prematurity and LBW were significantly associated with more functional obstruction requiring reoperation. We hypothesize that the immature intestinal motility explains this observation. Small intestinal motor activity has been found to be present at 16 weeks of gestation, but coordinated contraction and peristalsis is not established until 36 weeks [14-16]. Prematurity and LBW had also been previously shown to be significant predictors of increased mortality of JIA by Walker et al, with term infants having a 98% survival rate compared with 87% for preterm infants[1,9]. The incidence of functional obstruction requiring reoperation after primary anastomosis for JIA has not been well reported. A study in Netherlands reported that 13% of patients developed small bowel obstruction which occurred as early as within a month after the initial surgery, but the authors did not specify the cause of the obstruction nor did they report the management [5]. Kumaran et al reported 11% of prolonged adynamic ileus [6] while Piper et al reported 8% of their patients required reoperation of tapering enteroplasty [9] which presumably was indicated for the retained dilated bowel with dysmotility although the authors did not elaborate further. Notably, previous studies reported a relatively high incidence rates from 7 to 24% of adhesive intestinal obstruction requiring repeat laparotomy as early as within a month after the primary operation [4,6,7,9]. We speculate that some of the reported cases of adhesive intestinal obstruction, particularly those who had early reoperation, could be related to functional obstruction. The progressive dilatation of the dysmotile bowel on the proximal side of the anastomosis creates a funnel-shaped configuration and could result in more kinking and adhesions near the anastomotic site. In our study, there was only one patient who required reoperation due to purely adhesive intestinal obstruction. The patient had been discharged from hospital with full enteral feeding and readmitted for acute intestinal obstruction. Laparotomy found adhesion bands causing volvulus of a segment of small bowel distant from the initial anastomosis. On the other hand, two patients had isolated bowel perforations that occurred 3 to 5 weeks after the primary surgery for JIA in which the etiology of perforations was uncertain. Unnoticed injury to bowel wall or its blood supply during dissection in the initial surgery could result in delayed bowel perforation. This is possible particularly in one of the cases which the blood supply to the distal bowel with apple-peel configuration was precarious. Other findings in the present study are in agreement with the existing literature. Prenatal diagnosis of intestinal obstruction was 44.2% in our study, which was comparable to 41% in a populationbased study in Japan [2]. Like previous studies [4,5,17], we found in-utero volvulus and intussusception in 28% and 19% of our patients respectively as the etiological factors for JIA formation. After proximal bowel resection and primary anastomosis, 18% of our patients had SBS and the figure was comparable to the 15% reported in one of the largest case series among 114 neonates with JIA [5].The authors suggested higher morbidity and mortality rates among patients with SBS who were dependent on prolonged parenteral nutrition [5]. From our findings, mortality was not associated with SBS but with functional obstruction. However, the only mortality case in the present study resulted from sepsis with parenteral nutrition-related liver failure. This patient died before our introduction of fish oil-based lipid preparation in parenteral nutrition which carries a lower risk to liver injury [18]. Total parenteral nutrition was required in 47
5 to 79% of neonates after operation for JIA, and dependency was significantly associated with the length of remaining small bowel [5-7]. Improved parenteral nutrition with less cholestasis would further decrease the morbidity and mortality after surgery for JIA. Our study was limited by its retrospective nature and the study period spanned a decade which there had been continuous improvement in neonatal intensive care with better parenteral nutrition being introduced. The operations were performed by a group of attending surgeons with variations in their experience and seniority. Nevertheless, our study provides updated data on the long-term outcomes after primary repair for JIA. We have reaffirmed the findings that vast majority of neonates born with JIA can be managed by primary repair without enterostomy. In contemporary neonatal care setting, the long-term survival after primary anastomosis can reach over 95%. However, parents should be alerted to the substantial risk of early reoperations to tackle intraabdominal complications during the informed consenting process. Despite various technical advancements in neonatal care, it remains to be a subjective judgement of the operating surgeon on how much proximally dilated bowel to be resected. It can be challenging even to experienced surgeons to strike a balance between preserving as much bowel as possible and removing adequately the bowel expected to have dysmotility. REFERENCES 1. Walker K, Badawi N, Hamid CH,Vora A, Halliday R, Taylor C, et al. A population-based study of the outcome after small bowel atresia/stenosis in New South Wales and the Australian Capital Territory, Australia, J Pediatr Surg. 2008;43: Takahashi D, Hiroma T, Takamizawa S, Nakamura T. Population-based study of esophageal and small intestinal atresia/stenosis. Pediatr Int. 2014;56: Forrester MB, Merz RD. Population-based study of small intestinal atresia and stenosis, Hawaii, Public Health. 2004;118: DallaVecchia LK, Grosfeld JL, West KW,Rescorla FJ, Scherer LR, Engum SA. Intestinal atresia and stenosis: A 25-year experience with 277 cases. Arch Surg. 1998;133: Stollman TH, de Blaauw I, Wijnen MH, van der Staak FH, Rieu PN, Draaisma JM, et al. Decreased mortality but increased morbidity in neonates with jejunoileal atresia; a study of 114 cases over a 34- year period. J Pediatr Surg. 2009;44: Kumaran N, Shankar KP, Lloyd DA, Losty PD. Trends in the management and outcome of jejunoileal atresia. Eur J Pediatr Surg. 2002;12: Calisti A, Olivieri C, Coletta R, Briganti V, Oriolo L, Giannino G. Jejunoileal atresia: factors affecting the outcome and long-term sequelae. J Clin Neonatol. 2012;1: Federici S, Sabatino MD, Domenichelli V, Straziuso S. Worst prognosis in the complex jejunoileal atresia: is it real? Eur J Pediatric Surg Rep. 2015; 3: Piper HG, Alesbury J, Waterford SD, Zurakowski D, Jaksic T. Intestinal atresias: factors affecting clinical outcomes. J Pediatr Surg. 2008;43: Grosfeld JL, Ballantine TV, Shoemaker R. Operative management of intestinal atresia and stenosis based on pathologic findings. J Pediatr Surg. 1979;14: Nixon HH, Tawes R. Etiology and treatment of small intestinal atresia: analysis of a series of 127 jejunoileal atresias and comparison with 62 duodenal atresias. Surg. 1971;69: Louw JH. Resection and end-to-end anastomosis in the management of atresia and stenosis of the small bowel. Surg. 1967;62: delorimier AA, Norman DA, Gooding CA, Preger L. A model for cinefluoroscopic and manometric study of chronic intestinal obstruction. J Pediatr Surg. 1973;8: Berseth CL. Gestational evolution of small intestine motility in preterm and term infants. J Pediatr. 1989;115: Al Tawil YS, Jadcharla SR, Berseth CL. Motor activity responses to bolus feeding differ in preterm and term infants. J Pediatr Gastroenterol Nutr. 1995;19: Berseth CL. Gastrointestinal motility in the neonate. Clin Perinatol. 1996;23: Komuro H, Hori T, Amagai T, Hirai M, Yotsumoto K, Urita Y, et al. The etiologic role of intrauterine volvulus and intussusception in jejunoileal atresia. J Pediatr Surg. 2004;39: Lam HS, Tam YH, Poon TC, Cheung HM, Yu X, Chan BP, et al. A double-blind randomised controlled trial of fish oil-based versus soy-based lipid preparations in the treatment of infants with parenteral nutrition-associated cholestasis. Neonatol. 2014;105:290-6.
Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates
 Annals of Pediatric Surgery Vol 5, No 1, January 2009, PP 31-35 Original Article Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates Almoutaz A. Eltayeb Pediatric
Annals of Pediatric Surgery Vol 5, No 1, January 2009, PP 31-35 Original Article Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates Almoutaz A. Eltayeb Pediatric
Cystic meconium peritonitis with jejunoileal atresia: Is it associated with unfavorable outcome?
 W J C P World Journal of Clinical Pediatrics Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5409/wjcp.v6.i1.40 World J Clin Pediatr 2017 February
W J C P World Journal of Clinical Pediatrics Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5409/wjcp.v6.i1.40 World J Clin Pediatr 2017 February
Imaging of Neonatal Upper Gastro-Intestinal Atresia Beyond the Esophagus in Correlation with Surgical Findings
 Med. J. Cairo Univ., Vol. 83, No. 2, March: 207-214, 2015 www.medicaljournalofcairouniversity.net Imaging of Neonatal Upper Gastro-Intestinal Atresia Beyond the Esophagus in Correlation with Surgical Findings
Med. J. Cairo Univ., Vol. 83, No. 2, March: 207-214, 2015 www.medicaljournalofcairouniversity.net Imaging of Neonatal Upper Gastro-Intestinal Atresia Beyond the Esophagus in Correlation with Surgical Findings
Gastroschisis Sequelae and Management
 Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
Case Report The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in a Newborn
 Case Reports in Pediatrics Volume 2015, Article ID 129098, 4 pages http://dx.doi.org/10.1155/2015/129098 Case Report The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in a Newborn
Case Reports in Pediatrics Volume 2015, Article ID 129098, 4 pages http://dx.doi.org/10.1155/2015/129098 Case Report The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in a Newborn
MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION
 Basrah Journal Of Surgery MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION Haithem Hussein Ali Almoamin MB, ChB, FIBMS Pediatric Surgery, Lecturer, Department of Surgery, College of Medicine,
Basrah Journal Of Surgery MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION Haithem Hussein Ali Almoamin MB, ChB, FIBMS Pediatric Surgery, Lecturer, Department of Surgery, College of Medicine,
SWISS SOCIETY OF NEONATOLOGY. Prenatal diagnosis and postnatal management of meconium pseudocysts
 SWISS SOCIETY OF NEONATOLOGY Prenatal diagnosis and postnatal management of meconium pseudocysts September 2007 2 Burch E, Caduff JH, Hodel M, Berger TM, Neonatal and Pediatric Intensive Care Unit (BE,
SWISS SOCIETY OF NEONATOLOGY Prenatal diagnosis and postnatal management of meconium pseudocysts September 2007 2 Burch E, Caduff JH, Hodel M, Berger TM, Neonatal and Pediatric Intensive Care Unit (BE,
Hirschprung s. Meconium plug R/S >1 R/S <1
 NEONATAL ABDOMINAL EMERGENCIES LOW OBSTRUCTION HIGH OBSTRUCTION INTESTINAL OBSTRUCTION High obstruction - proximal to mid-ileumileum Few dilated, air filled bowel loops Complete obstruction diagnosed by
NEONATAL ABDOMINAL EMERGENCIES LOW OBSTRUCTION HIGH OBSTRUCTION INTESTINAL OBSTRUCTION High obstruction - proximal to mid-ileumileum Few dilated, air filled bowel loops Complete obstruction diagnosed by
Takayuki; Eguchi, Susumu; Kanematsu. Citation Pediatric surgery international, 27
 NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
Atresia of the Jejunum and Ileum: What is the Difference?
 Atresia of the Jejunum and Ileum: What is the Difference? Achariya Tongsin MD*, Maitree Anuntkosol MD*, Rangsan Niramis MD* * Department of Surgery, Queen Sirikit National Institute of Child Health, College
Atresia of the Jejunum and Ileum: What is the Difference? Achariya Tongsin MD*, Maitree Anuntkosol MD*, Rangsan Niramis MD* * Department of Surgery, Queen Sirikit National Institute of Child Health, College
Intestinal obstruction due to dual gastrointestinal atresia in infants: diagnosis and management of 3 cases
 Chen et al. BMC Gastroenterology 2014, 14:108 CASE REPORT Open Access Intestinal obstruction due to dual gastrointestinal atresia in infants: diagnosis and management of 3 cases Hua-dong Chen 1, Hong Jiang
Chen et al. BMC Gastroenterology 2014, 14:108 CASE REPORT Open Access Intestinal obstruction due to dual gastrointestinal atresia in infants: diagnosis and management of 3 cases Hua-dong Chen 1, Hong Jiang
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN)
 An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
Neonatal Perforated Gut: Etiology and Risk Factors
 Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Mostafa Kotb 1 * and Marwa Beyaly 2 1 Pediatric Surgery Department, Alexandria Faculty of Medicine, Egypt. 2 Human Genetics Department, Medical Research
Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Mostafa Kotb 1 * and Marwa Beyaly 2 1 Pediatric Surgery Department, Alexandria Faculty of Medicine, Egypt. 2 Human Genetics Department, Medical Research
A novel plain abdominal radiograph sign to diagnose malrotation with volvulus
 A novel plain abdominal radiograph sign to diagnose malrotation with volvulus Nataraja RM 1, Mahomed AA 1* 1. Department of Paediatric Surgery, Royal Alexandra Hospital for Sick Children, Brighton,UK *
A novel plain abdominal radiograph sign to diagnose malrotation with volvulus Nataraja RM 1, Mahomed AA 1* 1. Department of Paediatric Surgery, Royal Alexandra Hospital for Sick Children, Brighton,UK *
Original Article. Associated Anomalies and Clinical Outcomes in Infants with Omphalocele: A Single-centre 10-year Review
 HK J Paediatr (new series) 2018;23:220-224 Original Article Associated Anomalies and Clinical Outcomes in Infants with Omphalocele: A Single-centre 10-year Review YY CHEE, MSC WONG, RMS WONG, KY WONG,
HK J Paediatr (new series) 2018;23:220-224 Original Article Associated Anomalies and Clinical Outcomes in Infants with Omphalocele: A Single-centre 10-year Review YY CHEE, MSC WONG, RMS WONG, KY WONG,
OUTCOME OF BISHOP KOOP PROCEDURE IN NEONATAL JEJUNOILEAL ATRESIAS... ABSTRACT
 OUTOME OF BISHOP OOP PROEDURE IN NEONATAL JEJUNOILEAL ATRESIAS... ORIGINAL ARTILE OUTOME OF BISHOP OOP PROEDURE IN NEONATAL AL JEJUNOILEAL ATRESIAS: A RETROSPETIVE ANALYSIS Mohammad Imran, 1 Hayat Ur Rehman,
OUTOME OF BISHOP OOP PROEDURE IN NEONATAL JEJUNOILEAL ATRESIAS... ORIGINAL ARTILE OUTOME OF BISHOP OOP PROEDURE IN NEONATAL AL JEJUNOILEAL ATRESIAS: A RETROSPETIVE ANALYSIS Mohammad Imran, 1 Hayat Ur Rehman,
POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW
 CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
Management of Intestinal Strictures Post Conservative Treatment of Necrotizing Enterocolitis: The Long Term Outcome
 Journal of Neonatal Surgery 2016; 5(3):28 Doi:10.21699/j.v5i3.379 ORIGINAL ARTICLE Management of Intestinal Strictures Post Coervative Treatment of Necrotizing Enterocolitis: The Long Term Outcome Houben
Journal of Neonatal Surgery 2016; 5(3):28 Doi:10.21699/j.v5i3.379 ORIGINAL ARTICLE Management of Intestinal Strictures Post Coervative Treatment of Necrotizing Enterocolitis: The Long Term Outcome Houben
Microcolon in Neonates: Clinical and Radiographic Appearance
 icrocolon in Neonates: Clinical and Radiographic Appearance Wan-Chak Lo, Chao-Ran Wang and Kun-Eng Lim icrocolon (unused colon) is not a common problem in neonates. Radiographic contrast medium enema shows
icrocolon in Neonates: Clinical and Radiographic Appearance Wan-Chak Lo, Chao-Ran Wang and Kun-Eng Lim icrocolon (unused colon) is not a common problem in neonates. Radiographic contrast medium enema shows
Morabito A UK. -Royal Manchester Children s Hospital (PABRRU) -Intestinal Failure Unit Salford Royal Hospital
 NON-TRANSPLANT SURGERY IMPROVES OUTCOME IN SHORT BOWEL PATIENTS Morabito A UK -Royal Manchester Children s Hospital (PABRRU) -Intestinal Failure Unit Salford Royal Hospital antonino.morabito@cmft.nhs.uk
NON-TRANSPLANT SURGERY IMPROVES OUTCOME IN SHORT BOWEL PATIENTS Morabito A UK -Royal Manchester Children s Hospital (PABRRU) -Intestinal Failure Unit Salford Royal Hospital antonino.morabito@cmft.nhs.uk
Int J Clin Exp Med 2016;9(5): /ISSN: /IJCEM Shaobo Yang, Shan Zheng, Yanlei Huang, Chun Shen, Xianmin Xiao
 Int J Clin Exp Med 2016;9(5):8770-8774 www.ijcem.com /ISSN:1940-5901/IJCEM0017461 Original Article Prognostic factors in children with total colonic aganglionosis treated with the Soave procedure: the
Int J Clin Exp Med 2016;9(5):8770-8774 www.ijcem.com /ISSN:1940-5901/IJCEM0017461 Original Article Prognostic factors in children with total colonic aganglionosis treated with the Soave procedure: the
SWISS SOCIETY OF NEONATOLOGY. Neonatal gastric perforation
 SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
Perforated Necrotizing Enterocolitis: What Is The Rational Approach? Peritoneal Drainage or Laparotomy?
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 17, Issue 5 Ver. 12(May. 218), PP 19-23 www.iosrjournals.org Perforated Necrotizing Enterocolitis: What
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 17, Issue 5 Ver. 12(May. 218), PP 19-23 www.iosrjournals.org Perforated Necrotizing Enterocolitis: What
A novel and simple method using a transanal intestinal long tube for protecting intestinal anastomosis and decompressing the small bowel
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.93.3.137 Annals of Surgical Treatment and Research A novel and simple method using a transanal intestinal long tube for
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.93.3.137 Annals of Surgical Treatment and Research A novel and simple method using a transanal intestinal long tube for
Resuscitating neonatal and infant organs and preserving function. GI Tract and Kidneys
 Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
Improved survival in a multidisciplinary short bowel syndrome program
 Journal of Pediatric Surgery (2008) 43, 20 24 www.elsevier.com/locate/jpedsurg Improved survival in a multidisciplinary short bowel syndrome program Biren P. Modi a,b, Monica Langer a,b, Y. Avery Ching
Journal of Pediatric Surgery (2008) 43, 20 24 www.elsevier.com/locate/jpedsurg Improved survival in a multidisciplinary short bowel syndrome program Biren P. Modi a,b, Monica Langer a,b, Y. Avery Ching
Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help. Print this Page Add to my Bookmarks Page 3 of 10
 Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS
 Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of
Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of Pediatrics UMDNJ RWJMS Daniel Hirsch, MD Director of Neonatology Somerset Medical Center Assistant Professor of
Neonatal intestinal obstruction: how to make etiological diagnosis?
 Neonatal intestinal obstruction: how to make etiological diagnosis? Poster No.: C-1414 Congress: ECR 2013 Type: Educational Exhibit Authors: W. Mnari, M. Zguidi, A. Zrig, M. Maatouk, B. Hmida, R. Salem,
Neonatal intestinal obstruction: how to make etiological diagnosis? Poster No.: C-1414 Congress: ECR 2013 Type: Educational Exhibit Authors: W. Mnari, M. Zguidi, A. Zrig, M. Maatouk, B. Hmida, R. Salem,
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN
 PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
PARENTERAL NUTRITION- ASSOCIATED LIVER DISEASE IN CHILDREN Praveen Goday MBBS CNSC Associate Professor Pediatric Gastroenterology Medical College of Wisconsin Milwaukee, WI Parenteral Nutrition-Associated
Strategies for preventing and treating IFALD
 Strategies for preventing and treating IFALD Dr Sue Beath The Liver Unit (including small bowel transplantation) sue.beath@nhs.net Birmingham Children s Hospital Intestinal failure associated liver disease
Strategies for preventing and treating IFALD Dr Sue Beath The Liver Unit (including small bowel transplantation) sue.beath@nhs.net Birmingham Children s Hospital Intestinal failure associated liver disease
1 p-issn: ,e-issn: Original Article. Neonatal Intestinal Obstruction-Four Year Experience. BJKines-NJBAS Volume-7(1), June
 Neonatal Intestinal Obstruction-Four Year Experience D. Rathore 1, J. Ramji 2*, R. Joshi 3, A. Shah 4, T. Dihare 5, M. Bachani 6 1 Pediatric Surgeon, 2 Associate Professor, 3 Professor & Head, 4,5 Resident,
Neonatal Intestinal Obstruction-Four Year Experience D. Rathore 1, J. Ramji 2*, R. Joshi 3, A. Shah 4, T. Dihare 5, M. Bachani 6 1 Pediatric Surgeon, 2 Associate Professor, 3 Professor & Head, 4,5 Resident,
Advanced Necrotizing Enterocolitis Part 1: Mortality
 8 Original Article Advanced Necrotizing Enterocolitis Part 1: Mortality M. Thyoka 1 P. de Coppi 1 S. Eaton 1 K. Khoo 1 N.J. Hall 1 J. Curry 1 E. Kiely 1 D. Drake 1 K. Cross 1 A. Pierro 1 1 Department of
8 Original Article Advanced Necrotizing Enterocolitis Part 1: Mortality M. Thyoka 1 P. de Coppi 1 S. Eaton 1 K. Khoo 1 N.J. Hall 1 J. Curry 1 E. Kiely 1 D. Drake 1 K. Cross 1 A. Pierro 1 1 Department of
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
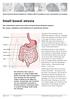 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Minimal Enteral Nutrition
 Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Abstract Minimal Enteral Nutrition Although parenteral nutrition has been used widely in the management of sick very low birth weight infants, a smooth transition to the enteral route is most desirable.
Neonatal intestinal obstruction: how to make etiological diagnosis?
 Neonatal intestinal obstruction: how to make etiological diagnosis? Poster No.: C-1414 Congress: ECR 2013 Type: Educational Exhibit Authors: W. MNARI, M. Zguidi, A. Zrig, M. MAATOUK, B. Hmida, R. Salem,
Neonatal intestinal obstruction: how to make etiological diagnosis? Poster No.: C-1414 Congress: ECR 2013 Type: Educational Exhibit Authors: W. MNARI, M. Zguidi, A. Zrig, M. MAATOUK, B. Hmida, R. Salem,
Anorectal malformations include a wide spectrum of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
Gastrointestinal tract
 Chapter 7 Gastrointestinal tract NORMAL SONOGRAPHIC ANATOMY Sonographically, the fetal stomach is visible from 9 weeks of gestation as a sonolucent cystic structure in the upper left quadrant of the abdomen.
Chapter 7 Gastrointestinal tract NORMAL SONOGRAPHIC ANATOMY Sonographically, the fetal stomach is visible from 9 weeks of gestation as a sonolucent cystic structure in the upper left quadrant of the abdomen.
INTESTINAL OBSTRUCTION ESCAPED SURGERY: MECONIUM PLUG
 7 INTESTINAL OBSTRUCTION ESCAPED SURGERY: MECONIUM PLUG Oluwayemi IO 1 *, Ade-Ojo IP 2, Olofinbiyi BA 2 1. Department of Paediatrics, Ekiti State University Teaching Hospital, Ado-Ekiti, Ekiti State, Nigeria
7 INTESTINAL OBSTRUCTION ESCAPED SURGERY: MECONIUM PLUG Oluwayemi IO 1 *, Ade-Ojo IP 2, Olofinbiyi BA 2 1. Department of Paediatrics, Ekiti State University Teaching Hospital, Ado-Ekiti, Ekiti State, Nigeria
Vacuum-Assisted Closure: A Novel Method of Managing Surgical Necrotizing Enterocolitis
 Original Article 41 Vacuum-Assisted Closure: A Novel Method of Managing Surgical Necrotizing Enterocolitis Stephanie Sea 1 Teerin Meckmongkol 1 Matthew L. Moront 1 Shaheen Timmapuri 1 Rajeev Prasad 1 Marshall
Original Article 41 Vacuum-Assisted Closure: A Novel Method of Managing Surgical Necrotizing Enterocolitis Stephanie Sea 1 Teerin Meckmongkol 1 Matthew L. Moront 1 Shaheen Timmapuri 1 Rajeev Prasad 1 Marshall
Intestinal Obstruction Clinical Presentation & Causes
 Intestinal Obstruction Clinical Presentation & Causes V Chidambaram-Nathan Consultant Transplant and General Surgeon Sheffield Kidney Institute Northern General Hospital Intestinal Obstruction One of the
Intestinal Obstruction Clinical Presentation & Causes V Chidambaram-Nathan Consultant Transplant and General Surgeon Sheffield Kidney Institute Northern General Hospital Intestinal Obstruction One of the
PAPER. High Morbidity of Enterostomy and Its Closure in Premature Infants With Necrotizing Enterocolitis
 High Morbidity of Enterostomy and Its Closure in Premature Infants With Necrotizing Enterocolitis Ann O Connor, MD; Robert S. Sawin, MD PAPER Objective: To review the morbidity and mortality among 68 premature
High Morbidity of Enterostomy and Its Closure in Premature Infants With Necrotizing Enterocolitis Ann O Connor, MD; Robert S. Sawin, MD PAPER Objective: To review the morbidity and mortality among 68 premature
Topics for discussion. Pediatric General Surgery. Physiology. Surgical Newborns. Neonatal Intestinal Obstruction
 Topics for discussion Pediatric General Surgery Professor General & Thoracic Surgery What makes Pediatric Surgery unique? Neonatal intestinal obstruction Abdominal wall defects Inguinal hernias Appendicitis
Topics for discussion Pediatric General Surgery Professor General & Thoracic Surgery What makes Pediatric Surgery unique? Neonatal intestinal obstruction Abdominal wall defects Inguinal hernias Appendicitis
Management of Short Bowel Syndrome in the Era of Teduglutide. Charlene Compher, PhD, RD University of Pennsylvania
 Management of Short Bowel Syndrome in the Era of Teduglutide Charlene Compher, PhD, RD University of Pennsylvania compherc@nursing.upenn.edu Disclosures Research funding for clinical trials by NPS Pharmaceuticals
Management of Short Bowel Syndrome in the Era of Teduglutide Charlene Compher, PhD, RD University of Pennsylvania compherc@nursing.upenn.edu Disclosures Research funding for clinical trials by NPS Pharmaceuticals
Surgery for Intestinal Failure
 Surgery for Intestinal Failure Kishore Iyer, MBBS, FRCS (Eng), FACS Director, Adult & Pediatric Intestinal Transplantation Associate Professor of Surgery & Pediatrics Mount Sinai School of Medicine New
Surgery for Intestinal Failure Kishore Iyer, MBBS, FRCS (Eng), FACS Director, Adult & Pediatric Intestinal Transplantation Associate Professor of Surgery & Pediatrics Mount Sinai School of Medicine New
ISSN East Cent. Afr. J. surg. (Online)
 143 Barium enema with reference to rectal biopsy for the diagnosis and exclusion of Hirschsprung disease W. Esayias 1, Y. Hawaz 1, B. Dejene 2, W. Ergete 3 Department of Radiology, School of Medicine,
143 Barium enema with reference to rectal biopsy for the diagnosis and exclusion of Hirschsprung disease W. Esayias 1, Y. Hawaz 1, B. Dejene 2, W. Ergete 3 Department of Radiology, School of Medicine,
Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai
 Original Research Article Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai S. Vijayalakshmi 1, Sriramchristopher M 2* 1 Associate
Original Research Article Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai S. Vijayalakshmi 1, Sriramchristopher M 2* 1 Associate
SWISS SOCIETY OF NEONATOLOGY. Congenital omphalo-mesenteric fistula in a newborn
 SWISS SOCIETY OF NEONATOLOGY Congenital omphalo-mesenteric fistula in a newborn NOVEMBER 2011 2 Dommange SJ, Lhermitte B, de Buys Roessingh A, Cachat F, Panchard MA, Department of Pediatrics (DSJ, CF,
SWISS SOCIETY OF NEONATOLOGY Congenital omphalo-mesenteric fistula in a newborn NOVEMBER 2011 2 Dommange SJ, Lhermitte B, de Buys Roessingh A, Cachat F, Panchard MA, Department of Pediatrics (DSJ, CF,
Vomiting in children: The good coordination between radiologists and pediatricians is the key to success
 Vomiting in children: The good coordination between radiologists and pediatricians is the key to success C. Santos Montón 1, M. T. Garzon Guiteria 2, A. Hortal Benito-Sendín 1, K. El Karzazi 1, P. Sanchez
Vomiting in children: The good coordination between radiologists and pediatricians is the key to success C. Santos Montón 1, M. T. Garzon Guiteria 2, A. Hortal Benito-Sendín 1, K. El Karzazi 1, P. Sanchez
Introduction. Cir Cir 2013;81: Abstract
 Cir Cir 2013;81:490-495. Description of morbidity and mortality of intestinal atresia in the neonatal period María Petra Gutiérrez-Carrillo, 1 José Manuel Zertuche-Coindreau, 1 Carmen Leticia Santana-
Cir Cir 2013;81:490-495. Description of morbidity and mortality of intestinal atresia in the neonatal period María Petra Gutiérrez-Carrillo, 1 José Manuel Zertuche-Coindreau, 1 Carmen Leticia Santana-
Chapter I 7. Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial
 Chapter I 7 Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial Bastiaan R. Klarenbeek Roberto Bergamaschi Alexander
Chapter I 7 Laparoscopic versus open elective sigmoid resection in diverticular disease: six months follow-up of the randomized control Sigma-trial Bastiaan R. Klarenbeek Roberto Bergamaschi Alexander
A simple technique of oblique anastomosis can prevent stricture formation in primary repair of esophageal atresia
 Journal of Pediatric Surgery (2012) 47, 1767 1771 www.elsevier.com/locate/jpedsurg Operative Techniques A simple technique of oblique anastomosis can prevent stricture formation in primary repair of esophageal
Journal of Pediatric Surgery (2012) 47, 1767 1771 www.elsevier.com/locate/jpedsurg Operative Techniques A simple technique of oblique anastomosis can prevent stricture formation in primary repair of esophageal
Pathology of Intestinal Obstruction. Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College
 Pathology of Intestinal Obstruction Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College Pathology of Intestinal Obstruction Objectives list the causes of intestinal obstruction
Pathology of Intestinal Obstruction Dr. M. Madhavan, MBBS., MD., MIAC, Professor of Pathology Saveetha Medical College Pathology of Intestinal Obstruction Objectives list the causes of intestinal obstruction
Colostomy & Ileostomy
 Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
A Rare Cause of Sub-Acute Proximal Intestinal Obstruction Due to Annular Pancreas Weledji EP, Ngowe M, Mokake M
 Case report A Rare Cause of Sub-Acute Proximal Intestinal Obstruction Due to Annular Pancreas Weledji EP, Ngowe M, Mokake M Department of Surgery, Regional Hospital Buea, Cameroon Correspondence to: E
Case report A Rare Cause of Sub-Acute Proximal Intestinal Obstruction Due to Annular Pancreas Weledji EP, Ngowe M, Mokake M Department of Surgery, Regional Hospital Buea, Cameroon Correspondence to: E
Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of Conservative Treatment
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 645104, 4 pages doi:10.5402/2011/645104 Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 645104, 4 pages doi:10.5402/2011/645104 Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction
 Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
Posterior Rectus Sheath Hernia Causing Intermittent Small Bowel Obstruction Scott Lenobel 1*, Robert Lenobel 2, Joseph Yu 1 1. Department of Radiology, The Ohio State University Wexner Medical Center,
Gastroschisis in the United States : analysis and risk categorization of 4344 patients
 (2007) 27, 50 55 r 2007 Nature Publishing Group All rights reserved. 0743-8346/07 $30 www.nature.com/jp ORIGINAL ARTICLE Gastroschisis in the United States 1988 2003: analysis and risk categorization of
(2007) 27, 50 55 r 2007 Nature Publishing Group All rights reserved. 0743-8346/07 $30 www.nature.com/jp ORIGINAL ARTICLE Gastroschisis in the United States 1988 2003: analysis and risk categorization of
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
PediatlJC Surgery International Springer-Verlag 1987
 Pediatr Surg Int (1987) 2:27-32 PediatlJC Surgery International Springer-Verlag 1987 An international survey of gastroschisis and omphalocele (490 cases) III. Factors influencing outcome of surgical management
Pediatr Surg Int (1987) 2:27-32 PediatlJC Surgery International Springer-Verlag 1987 An international survey of gastroschisis and omphalocele (490 cases) III. Factors influencing outcome of surgical management
Heterotaxia syndrome: The role of screening for intestinal rotation. abnormalities
 ADC Online First, published on May 12, 2005 as 10.1136/adc.2004.067504 Heterotaxia syndrome: The role of screening for intestinal rotation abnormalities Matthew Choi, Steven H Borenstein, Lisa Hornberger
ADC Online First, published on May 12, 2005 as 10.1136/adc.2004.067504 Heterotaxia syndrome: The role of screening for intestinal rotation abnormalities Matthew Choi, Steven H Borenstein, Lisa Hornberger
Impact of Suture Choice on Stricture Formation Following Repair of Esophageal Atresia
 Annals of Pediatric Surgery, Vol 3, No 2, April 2007 PP 75-79 Original Article Impact of Suture Choice on Stricture Formation Following Repair of Esophageal Atresia Shawn D. St. Peter, Patricia A. Valusek,
Annals of Pediatric Surgery, Vol 3, No 2, April 2007 PP 75-79 Original Article Impact of Suture Choice on Stricture Formation Following Repair of Esophageal Atresia Shawn D. St. Peter, Patricia A. Valusek,
BOWEL LENGTHENING procedures may be beneficial
 Serial Transverse Enteroplasty (STEP): A Novel Bowel Lengthening Procedure By Heung Bae Kim, Dario Fauza, Jennifer Garza, Jung-Tak Oh, Samuel Nurko, and Tom Jaksic Boston, Massachusetts Background/Purpose:
Serial Transverse Enteroplasty (STEP): A Novel Bowel Lengthening Procedure By Heung Bae Kim, Dario Fauza, Jennifer Garza, Jung-Tak Oh, Samuel Nurko, and Tom Jaksic Boston, Massachusetts Background/Purpose:
Non-Neonatal Intestinal Obstruction in children: 3 Years Experience and review of literature.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 52-57 www.iosrjournals.org Non-Neonatal Intestinal Obstruction in
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 52-57 www.iosrjournals.org Non-Neonatal Intestinal Obstruction in
ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM
 ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM DATA COLLECTION FORM Most Australian hospitals contribute data
ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM DATA COLLECTION FORM Most Australian hospitals contribute data
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications
 Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
DIGESTIVE SYSTEM SURGICAL PROCEDURES December 22, 2015 (effective March 1, 2016) INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
NEC. cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine
 NEC cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine Necrotizing enterocolitis (NEC) the most common and most lethal disease
NEC cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine Necrotizing enterocolitis (NEC) the most common and most lethal disease
Dysphagia after EA repair. Disclosure. Learning objectives 9/17/2013
 Dysphagia after EA repair Christophe Faure, M.D. Professor of Pediatrics, Division of Pediatric Gastroenterology, Sainte-Justine University Health Center, Université de Montréal, Montréal, QC, Canada christophe.faure@umontreal.ca
Dysphagia after EA repair Christophe Faure, M.D. Professor of Pediatrics, Division of Pediatric Gastroenterology, Sainte-Justine University Health Center, Université de Montréal, Montréal, QC, Canada christophe.faure@umontreal.ca
Alyssa Brzenski MD May 2, 2012
 Alyssa Brzenski MD May 2, 2012 Overview Background Pre repair bronchoscopy Thorascopic repair To extubate or not? Esophageal atresia treatment of long gap esophageal atresia Complications following TEF/EA
Alyssa Brzenski MD May 2, 2012 Overview Background Pre repair bronchoscopy Thorascopic repair To extubate or not? Esophageal atresia treatment of long gap esophageal atresia Complications following TEF/EA
1 University of Kansas School of Medicine-Wichita, Department of Pediatrics 2 Wesley Medical Center, Department of Neonatology
 Impact of on Very Low Birth Weight Infants Siddharthan Sivamurthy, M.D. 1, Carolyn R. Ahlers-Schmidt, Ph.D. 1, Katherine S. Williams, M.Ed. 1, Jared Shaw 2, Paula Delmore, M.S.N. 2, Barry T. Bloom, M.D.
Impact of on Very Low Birth Weight Infants Siddharthan Sivamurthy, M.D. 1, Carolyn R. Ahlers-Schmidt, Ph.D. 1, Katherine S. Williams, M.Ed. 1, Jared Shaw 2, Paula Delmore, M.S.N. 2, Barry T. Bloom, M.D.
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Intussusception Secondary to a Meckel Diverticulum in an Adolescent
 48) Intussusception Secondary to a Meckel Diverticulum in an Adolescent Yener O., Demir M., Yigitbaşı R. Department of Surgery, Göztepe Training and Research Hospital, Istanbul, Turkey Received March 28,
48) Intussusception Secondary to a Meckel Diverticulum in an Adolescent Yener O., Demir M., Yigitbaşı R. Department of Surgery, Göztepe Training and Research Hospital, Istanbul, Turkey Received March 28,
SWISS SOCIETY OF NEONATOLOGY. Unusual cause of pneumoperitoneum in a spontaneously breathing 1-day-old term infant
 SWISS SOCIETY OF NEONATOLOGY Unusual cause of pneumoperitoneum in a spontaneously breathing 1-day-old term infant March 2012 2 Berger TM, Winiker H, Neonatal and Pediatric Intensive Care Unit (BTM), Pediatric
SWISS SOCIETY OF NEONATOLOGY Unusual cause of pneumoperitoneum in a spontaneously breathing 1-day-old term infant March 2012 2 Berger TM, Winiker H, Neonatal and Pediatric Intensive Care Unit (BTM), Pediatric
Clinical Characteristics and Management of Benign Transient Non-Organic Ileus of Neonates: A Single-Center Experience
 Original Article http://dx.doi.org/10.3349/ymj.2014.55.1.157 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(1):157-161, 2014 Clinical Characteristics and Management of Benign Transient Non-Organic
Original Article http://dx.doi.org/10.3349/ymj.2014.55.1.157 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(1):157-161, 2014 Clinical Characteristics and Management of Benign Transient Non-Organic
Computed tomography (CT) imaging review of small bowel obstruction
 Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract - Small Bowel Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK,
Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract - Small Bowel Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK,
Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure
 ORIGINAL ARTICLE Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure Yi-Ching Tung, Yen-Hsuan Ni, Hong-Shiee Lai, 1 Der-Yirng Hsieh, 2 Mei-Hwei Chang*
ORIGINAL ARTICLE Clinical Improvement Following Home Parenteral Nutrition in Pediatric Patients with Intestinal Failure Yi-Ching Tung, Yen-Hsuan Ni, Hong-Shiee Lai, 1 Der-Yirng Hsieh, 2 Mei-Hwei Chang*
Pediatric Bowel Obstruction
 Pediatric Bowel Obstruction Matt Zerden, Harvard Medical School III Patient 1 16 year old presents with severe, episodic abdominal pain, nausea and vomiting. Questionable abdominal mass in RLQ Previous
Pediatric Bowel Obstruction Matt Zerden, Harvard Medical School III Patient 1 16 year old presents with severe, episodic abdominal pain, nausea and vomiting. Questionable abdominal mass in RLQ Previous
FACE THE EXAMINER. Hirschsprung s Disease in Newborns. (This section is meant for residents to check their understanding regarding a particular topic)
 Journal of Neonatal Surgery 2013;2(4):51 FACE THE EXAMINER Hirschsprung s Disease in Newborns (This section is meant for residents to check their understanding regarding a particular topic) QUESTIONS 1.
Journal of Neonatal Surgery 2013;2(4):51 FACE THE EXAMINER Hirschsprung s Disease in Newborns (This section is meant for residents to check their understanding regarding a particular topic) QUESTIONS 1.
Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations
 Original paper Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations Paweł Nachulewicz 1, Kamila Zaborowska 1, Błażej Rogowski 1, Anita Kalińska 1, Marzena
Original paper Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations Paweł Nachulewicz 1, Kamila Zaborowska 1, Błażej Rogowski 1, Anita Kalińska 1, Marzena
Index. Note: Page numbers of article title are in boldface type.
 Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Physical Exam. Vitals stable on room air Abdomen soft, non-distented Normal external genitalia Patent anus No limb anomalies
 Case Presentation 1 day-old full-term baby girl noted to have drooling of saliva and increased secretions at birth Fetal US @32wks had shown polyhydramnios Birth weight 3515g Apgar 7@1min and 8@5min Unable
Case Presentation 1 day-old full-term baby girl noted to have drooling of saliva and increased secretions at birth Fetal US @32wks had shown polyhydramnios Birth weight 3515g Apgar 7@1min and 8@5min Unable
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Mehmet Melek 1 and Ufuk Cobanoglu Introduction. 2. Material and Method
 Gastroenterology Research and Practice Volume 2011, Article ID 527323, 4 pages doi:10.1155/2011/527323 Methodology Report A New Technique in Primary Repair of Congenital Esophageal Atresia Preventing Anastomotic
Gastroenterology Research and Practice Volume 2011, Article ID 527323, 4 pages doi:10.1155/2011/527323 Methodology Report A New Technique in Primary Repair of Congenital Esophageal Atresia Preventing Anastomotic
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
Health Center Krusevac, Department of Surgery, Krusevac, Serbia
 Health Center Krusevac, Department of Surgery, Krusevac, Serbia SURGICAL TREATMENT OF MECKEL S DIVERTICULUM Milan Jovanovic, R. Zdravkovic, S. Zajic, M. Smiljkovic, V. Kulic, A. Kitanovic, G. Filipovic,
Health Center Krusevac, Department of Surgery, Krusevac, Serbia SURGICAL TREATMENT OF MECKEL S DIVERTICULUM Milan Jovanovic, R. Zdravkovic, S. Zajic, M. Smiljkovic, V. Kulic, A. Kitanovic, G. Filipovic,
NEONATAL GASTROINTESTINAL PERFORATIONS: A 7-YEAR SINGLE CENTER EXPERIENCE AT A TERTIARY NEONATAL INTENSIVE CARE UNIT IN TURKEY
 NEONATAL GASTROINTESTINAL PERFORATIONS: A 7-YEAR SINGLE CENTER EXPERIENCE AT A TERTIARY NEONATAL INTENSIVE CARE UNIT IN TURKEY *Nilay Hakan 1, Mustafa Aydin 1, Derya Erdogan 2, Yusuf Hakan Cavusoglu 2,
NEONATAL GASTROINTESTINAL PERFORATIONS: A 7-YEAR SINGLE CENTER EXPERIENCE AT A TERTIARY NEONATAL INTENSIVE CARE UNIT IN TURKEY *Nilay Hakan 1, Mustafa Aydin 1, Derya Erdogan 2, Yusuf Hakan Cavusoglu 2,
4/15/2014. Nurses Take the Lead to Improve Overall Infant Growth. Improving early nutrition. Problem Identification
 Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
Nurses Take the Lead to Improve Overall Infant Growth Cathy Lee Leon, RN, BSN, MBA, NE-BC California Pacific Medical Center-San Francisco Improving early nutrition Standardized feeding protocol Problem
Nordic Forum - Trauma & Emergency Radiology. Bowel Obstruction: Imaging Update
 Nordic Forum - Trauma & Emergency Radiology Bowel Obstruction: Imaging Update Borut Marincek Institute of Diagnostic Radiology University Hospital Zurich, Switzerland Acute Abdomen Bowel Obstruction Bowel
Nordic Forum - Trauma & Emergency Radiology Bowel Obstruction: Imaging Update Borut Marincek Institute of Diagnostic Radiology University Hospital Zurich, Switzerland Acute Abdomen Bowel Obstruction Bowel
Prognosis of Patients With Gastric Cancer Who Underwent Proximal Gastrectomy
 Int Surg 2012;97:275 279 Prognosis of Patients With Gastric Cancer Who Underwent Proximal Gastrectomy Masahide Ikeguchi, Abdul Kader, Seigo Takaya, Youji Fukumoto, Tomohiro Osaki, Hiroaki Saito, Shigeru
Int Surg 2012;97:275 279 Prognosis of Patients With Gastric Cancer Who Underwent Proximal Gastrectomy Masahide Ikeguchi, Abdul Kader, Seigo Takaya, Youji Fukumoto, Tomohiro Osaki, Hiroaki Saito, Shigeru
University of Groningen. Colorectal Anastomoses Bakker, Ilsalien
 University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Relationship Between Small Bowel Obstruction and Small Bowel Feces Sign: Four Cases Report
 Case Report Elmer Press Relationship Between Small Bowel Obstruction and Small Bowel Feces Sign: Four Cases Report Altintoprak Fatih a, e, Gunduz Yasemin b, Yalkin Omer c, Gundugdu Kemal c, Serbulent Gokhan
Case Report Elmer Press Relationship Between Small Bowel Obstruction and Small Bowel Feces Sign: Four Cases Report Altintoprak Fatih a, e, Gunduz Yasemin b, Yalkin Omer c, Gundugdu Kemal c, Serbulent Gokhan
Management of gastroschisis using standard urobag as silo
 Journal of Pediatric Diseases www.jpediatrdis.com CASE REPORT Management of gastroschisis using standard urobag as silo Rajesh Gupta 1*, Aradhana Singh 2 1 Department of Surgery, Division of Pediatric
Journal of Pediatric Diseases www.jpediatrdis.com CASE REPORT Management of gastroschisis using standard urobag as silo Rajesh Gupta 1*, Aradhana Singh 2 1 Department of Surgery, Division of Pediatric
Case Whirlpool sign in midgut volvulus
 Case 11454 Whirlpool sign in midgut volvulus Emad El-din Althamer 1, Shagufta Jabeen 2, Nada Al-Assaf 1, Akram Jawad 1, Muhammad Hassan 1, Muhammad Fatani 1, Rumayan Al-Rumyan 1, A Aziz Mosabihi 1, Ahmeduddin
Case 11454 Whirlpool sign in midgut volvulus Emad El-din Althamer 1, Shagufta Jabeen 2, Nada Al-Assaf 1, Akram Jawad 1, Muhammad Hassan 1, Muhammad Fatani 1, Rumayan Al-Rumyan 1, A Aziz Mosabihi 1, Ahmeduddin
Computed tomography (CT) imaging review of small bowel obstruction
 Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK, Leeds/UK
Computed tomography (CT) imaging review of small bowel obstruction Poster No.: C-1602 Congress: ECR 2010 Type: Educational Exhibit Topic: GI Tract Authors: A. Vousough, D. S. Prasad ; Aberdeen/UK, Leeds/UK
Unusual presentations of late onset diaphragmatic hernia: a six year study
 International Surgery Journal Aggarwal S et al. Int Surg J. 2017 Apr;4(4):1180-1184 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170895
International Surgery Journal Aggarwal S et al. Int Surg J. 2017 Apr;4(4):1180-1184 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170895
Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience
 Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
Atypical use of button gastrostomy tube for children with complex colorectal malformations (ileostomy, vesicostomy, vaginostomy)
 Atypical use of button gastrostomy tube for children with complex colorectal malformations (ileostomy, vesicostomy, vaginostomy) Christian PIOLAT, Yohann Robert, Pierre-Yves Rabattu, Youssef Teklali, Catherine
Atypical use of button gastrostomy tube for children with complex colorectal malformations (ileostomy, vesicostomy, vaginostomy) Christian PIOLAT, Yohann Robert, Pierre-Yves Rabattu, Youssef Teklali, Catherine
