Contribution of alternative complement pathway to delayed hemolytic transfusion reaction in sickle cell disease
|
|
|
- Alice Bryant
- 5 years ago
- Views:
Transcription
1 Published Ahead of Print on May 24, 2018, as doi: /haematol Copyright 2018 Ferrata Storti Foundation. Contribution of alternative complement pathway to delayed hemolytic transfusion reaction in sickle cell disease by Satheesh Chonat, Maa-Ohui Quarmyne, Caroline M. Bennett, Christina L. Dean, Clinton H. Joiner, Ross M. Fasano, and Sean R. Stowell Haematologica 2018 [Epub ahead of print] Citation: Satheesh Chonat, Maa-Ohui Quarmyne, Caroline M. Bennett, Christina L. Dean, Clinton H. Joiner, Ross M. Fasano, and Sean R. Stowell. Contribution of alternative complement pathway to delayed hemolytic transfusion reaction in sickle cell disease. Haematologica. 2018; 103:xxx doi: /haematol Publisher's Disclaimer. E-publishing ahead of print is increasingly important for the rapid dissemination of science. Haematologica is, therefore, E-publishing PDF files of an early version of manuscripts that have completed a regular peer review and have been accepted for publication. E-publishing of this PDF file has been approved by the authors. After having E-published Ahead of Print, manuscripts will then undergo technical and English editing, typesetting, proof correction and be presented for the authors' final approval; the final version of the manuscript will then appear in print on a regular issue of the journal. All legal disclaimers that apply to the journal also pertain to this production process.
2 Contribution of alternative complement pathway to delayed hemolytic transfusion reaction in sickle cell disease Running head: Alternative complement pathway activation in DHTR Satheesh Chonat 1,2, Maa-Ohui Quarmyne 1,2, Caroline M. Bennett 1,2, Christina L. Dean 3, Clinton H. Joiner 1,2, Ross M. Fasano 2,3* and Sean R. Stowell 3* 1 Department of Pediatrics, Emory University School of Medicine, Atlanta, USA 2 Aflac Cancer and Blood Disorders Center, Children s Healthcare of Atlanta, Atlanta, Georgia, USA 3 Center for Transfusion and Cellular Therapy, Department of Pathology and Laboratory Medicine, Emory University School of Medicine, Atlanta, Georgia, USA. *Senior authors contributed equally. Correspondence to: Satheesh Chonat, M.D., Emory University School of Medicine Children s Healthcare of Atlanta, 2015 Uppergate Drive, Emory Children s Center, Atlanta, GA schonat@emory.edu Phone: Fax: Word Count: 1369 words Figure/Table Count: 2 a) Number of Figures: 1, b) Number of Tables: 1 Reference Count: 16 d
3 Transfusion of red blood cells (RBC) remains a primary treatment modality in patients with sickle cell disease (SCD). Repeated exposure to alloantigens on transfused RBCs can lead to alloantibody formation that can increase the risk of delayed hemolytic transfusion reaction (DHTR). 1 The incidence of DHTR in transfused adult SCD patients ranged from % during a 30-month and 5-year study period, respectively. 2,3 The case fatality rate is 6%. 4 The symptoms of DHTR typically appear 7-14 days posttransfusion and include generalized pain, hemoglobinuria with/without fever, a significant drop of total hemoglobin and hemoglobin A from the post-transfusion value and suboptimal reticulocyte response. These clinical features mimic a classic vasoocclusive pain crisis (VOC), further confounding the detection of DHTR. In addition, patients can experience hyperhemolysis, evidenced by hemolysis of both native and transfused RBCs. General management of DHTR depends on the extent of hemolysis and the patient s clinical condition, from supportive care strategies to high dose erythropoietin, intravenous immunoglobulin (IVIg), and immunosuppression. 4,5 We report here comprehensive data on a 14-year-old African American female with SCD (β s β s genotype) and evidence for alternative complement pathway (ACP) activation during two of her three DHTR hyperhemolysis episodes, one of which had no new detectable allo- or autoantibody. This patient's past medical history is significant for multiple episodes of acute chest syndrome (ACS) and VOC, and an episode of acute splenic sequestration. The first episode of DHTR occurred at seven years of age, about nine days after receiving an extended phenotype-matched and crossmatch-compatible RBC transfusion for VOC and ACS (Figure 1A). A new anti-s antibody and anti-di a d
4 antibody were detected in the serum, with a negative direct antiglobulin test (DAT). She was treated with corticosteroids and made a complete recovery. The patient s second episode of DHTR was at 13.5 years-of-age. She was initially transfused with extended phenotype-matched and crossmatch-compatible RBCs for VOC and hemoglobin (HGB) of 4.4 g/dl (Figure 1B; day -9). Nine days after this transfusion, she presented with generalized pain and HGB of 7.2 g/dl. Within 24 hours of presentation, she progressed to having fevers, profound hemolysis (HGB 3.1 g/dl), thrombocytopenia (120 x10 3 /μl), and absolute reticulocytopenia 75% below her baseline. Also, there was evidence for marked hemoglobinuria, liver dysfunction and acute kidney injury (creatinine 0.9 mg/dl; baseline 0.5 mg/dl). Immunohematology testing revealed a new anti-sd a antibody, a cold agglutinin in the serum, and a negative DAT. Mycoplasma IgM in serum was positive, suggestive of acute mycoplasma infection. The patient responded well to 150 IU/kg of erythropoietin, corticosteroids and additional extended phenotype-matched and crossmatch-compatible RBC transfusions on days 2 and 4 to mitigate the ongoing effects of hemolysis from antibody-mediated DHTR and cold agglutinin syndrome (CAS). Hyperhemolysis and multi-organ involvement prompted analysis of complement proteins, which subsequently revealed elevated anaphylatoxin, C5a and terminal complex, C5b-9; both support the evidence for complement activation (Table 1 DHTR#2). Complement activation could have been caused either by DHTR, mycoplasma infection, or from a combination of the two in this case. Given her rapid improvement, eculizumab was not used during this episode. d
5 Eight months later, the patient again presented with significant VOC pain and a HGB of 5.6 g/dl (Figure 1C), which dropped to 3.9 g/dl within 24 hours of admission (Figure 1C) in the absence of preceding RBC transfusion. Immunohematology testing reconfirmed the previous anti-sd a, but did not detect the previous anti-di a, anti-s, or cold agglutinin. The DAT was negative. The patient received three units of extended phenotype-matched, crossmatch-compatible RBC units and was discharged home with a HGB of 9.5 g/dl. The patient presented again eight days later with generalized pain, fever, hemoglobinuria, and total hyperbilirubinemia of 7.3 mg/dl. Although her HGB was 11.0 g/dl on admission, it declined sharply (Figure 1C) with worsening of intravascular hemolysis reflected by elevated free plasma hemoglobin of 100 mg/dl, worsening hemoglobinuria, and LDH peak of 1753 U/L, along with elevated transaminases. DAT and antibody testing were again negative. A combination of immunosuppressive medications was initiated, including high dose steroids, IVIg and anti-cd20 antibody rituximab, as these along with erythropoietin have been previously used to help manage DHTR with life threatening hyperhemolysis. 4 We completed 4- doses regimen of Rituximab, to ensure adequate suppression of B lymphocytes and minimize the risk for relapse. In spite of these treatments, on day 14, the HGB declined to a nadir of 1.9 g/dl, creatinine doubled (Figure 1D), with worsening symptoms of pain, altered mental status, and development of new diffuse pulmonary edema requiring positive airway pressure support. The blood smear was notable for occasional schistocytes. This episode of antibody-negative DHTR hyperhemolysis and multi-organ dysfunction prompted the administration of eculizumab 600mg intravenously along with transfusion of one unit (4 ml/kg) extended phenotype-matched and crossmatch- d
6 compatible RBCs. Within 48 hours, the patient's mental status improved remarkably, she reported less pain, hemolysis declined, and the patient was weaned off respiratory support. Concurrent complement analyses revealed increased levels of Bb, C5a, and C5b-9 (DHTR#3 day 13, Table 1), reflecting complement activation. On day 20, the patient was discharged and closely followed up in the clinic. On day 39, a second dose of eculizumab 600mg was administered for downward drift in HGB (nadir: 5.4 g/dl). Following this, the patient s HGB remained within her baseline range of 8-9 g/dl with no recurrence of laboratory evidence of hyperhemolysis. Steroids and erythropoietin were slowly weaned. The patient had received pneumococcal and meningococcal vaccinations as part of routine SCD standard-of-care and continued on a prophylactic antibiotic regimen during her treatment. Currently, there is no consensus in the management of DHTR with ongoing hyperhemolysis in patients with SCD, when routine treatment measures are inadequate. This case highlights the potential contribution of ACP activation in DHTR hyperhemolysis. While new allo- and (cold) autoantibodies were identified during the second DHTR episode, no new allo- or autoantibodies were detected during the third episode. Hyperhemolysis, organ dysfunction, and activation of ACP was present during the 3 rd DHTR episode. The hemolysis associated with VOC, ACS or DHTR, results in elevated plasma heme, potentially saturating scavenging and detoxifying mechanisms of hemopexin and heme-oxygenase-1, respectively. 6,7 Elevations in free heme would then be predicted to lead to additional endothelial damage, vaso-occlusion and activation of the alternative complement pathway, while inhibiting the classical d
7 pathway A case of antibody-negative DHTR in which eculizumab was used to dampen the complement activation was recently reported. 12 This and other reports have suggested the involvement of complement pathway in SCD and DHTR ; the present case is novel in that we employed sensitive markers to assess and confirm the activation of the ACP cascade during recurrent episodes of DHTR and at steady-state (Supplemental Figure. 1). While these markers of the ACP do not necessarily shed light on the mechanism of ACP activation during DHTR, markedly elevated C5a, C5b-9 and most importantly Bb levels returned to normal levels as the patient recovered; plasma Bb levels provide a quantitative value of ACP activation. Plasma C3a levels were over 2.5 times above baseline but not over the normal range. Persistently elevated levels of CH50 even at day 127 could suggest continued low level baseline complement activation possibly due to ongoing chronic hemolysis. While the implementation of additional immunosuppressive therapies could have impacted this patient s outcome, the rapid response to eculizumab suggests that the reversal of hyperhemolysis may be due to the ability of eculizumab to block the downstream consequences of ACP. These laboratory and clinical findings strongly suggest that in this case, ACP was likely involved in DHTR with hyperhemolysis, and that ACP activation resolved after administration of eculizumab. However, as these are certainly correlative findings, definitely future studies are needed. As not all cases of DHTR may be accompanied by ACP activation or may benefit from eculizumab, analysis of ACP during DHTR episodes, especially when it is associated with hyperhemolysis and/or organ injury, may prove useful when assessing the potential benefit of eculizumab intervention. While additional studies are needed, including clinical assays that possess the ability to more e
8 completely assess complement function, early and appropriate administration of targeted therapy such as eculizumab may hold promise in the mitigation of potentially fatal complications in some patients. Future studies are needed to explore the mechanisms and potential role of prophylactic complement inhibition in patients with recurrent antibody-positive and antibody-negative DHTRs and those with minimal availability of antigen-compatible blood products. Acknowledgements The authors would like to thank the hematology and transfusion medicine teams at Children s Healthcare of Atlanta for their constructive review of the manuscript. No funding was used to conduct this study. Authorship Contributions S.C. collected and analyzed the data and wrote the manuscript. C.M.B., C.L.D., and M.O.Q. collected and analyzed the data and reviewed the manuscript. C.H.J., R.M.F., and S.R.S. analyzed the data and provided critical revisions to the manuscript. Disclosure of Conflicts of Interest There are no conflicts of interest to report References 1. Nickel RS, Horan JT, Fasano RM, et al. Immunophenotypic parameters and RBC alloimmunization in children with sickle cell disease on chronic transfusion. Am J Hematol. 2015;90(12): Vidler JB, Gardner K, Amenyah K, Mijovic A, Thein SL. Delayed haemolytic e
9 transfusion reaction in adults with sickle cell disease: a 5-year experience. Br J Haematol. 2015;169(5): Narbey D, Habibi A, Chadebech P, et al. Incidence and predictive score for delayed hemolytic transfusion reaction in adult patients with sickle cell disease. Am J Hematol. 2017;92(12): Habibi A, Mekontso Dessap A, Guillaud C, et al. Delayed hemolytic transfusion reaction in adult sickle-cell disease: presentations, outcomes, and treatments of 99 referral center episodes. Am J Hematol. 2016;91(10): Pirenne F, Bartolucci P, Habibi A. Management of delayed hemolytic transfusion reaction in sickle cell disease: Prevention, diagnosis, treatment. Transfus Clin Biol. 2017;24(3): Ghosh S, Tan F, Yu T, et al. Global Gene Expression Profiling of Endothelium Exposed to Heme Reveals an Organ-Specific Induction of Cytoprotective Enzymes in Sickle Cell Disease. Voolstra C, editor. PLoS One. 2011;6(3):e Adisa OA, Hu Y, Ghosh S, Aryee D, Osunkwo I, Ofori-Acquah SF. Association between plasma free haem and incidence of vaso-occlusive episodes and acute chest syndrome in children with sickle cell disease. Br J Haematol. 2013;162(5): Roumenina LT, Radanova M, Atanasov BP, et al. Heme Interacts with C1q and Inhibits the Classical Complement Pathway. J Biol Chem. 2011;286(18): Frimat M, Tabarin F, Dimitrov JD, et al. Complement activation by heme as a secondary hit for atypical hemolytic uremic syndrome. Blood. 2013;122(2): Ghosh S, Adisa OA, Chappa P, et al. Extracellular hemin crisis triggers acute chest syndrome in sickle mice. J Clin Invest. 2013;123(11): Belcher JD, Chen C, Nguyen J, et al. Heme triggers TLR4 signaling leading to endothelial cell activation and vaso-occlusion in murine sickle cell disease. Blood. 2014;123(3): Dumas G, Habibi A, Onimus T, et al. Eculizumab salvage therapy for delayed hemolysis transfusion reaction in sickle cell disease patients. Blood. 2016;127(8): Gupta S, Fenves A, Nance ST, Sykes DB, Dzik WS. Hyperhemolysis syndrome in a patient without a hemoglobinopathy, unresponsive to treatment with eculizumab. Transfusion. 2014;55(3): Boonyasampant M, Weitz IC, Kay B, Boonchalermvichian C, Liebman HA, e
10 Shulman IA. Life-threatening delayed hyperhemolytic transfusion reaction in a patient with sickle cell disease: effective treatment with eculizumab followed by rituximab. Transfusion. 2015;55(10): Chonat S, Chandrakasan S, Kalinyak KA, Ingala D, Gruppo R, Kalfa TA. Atypical haemolytic uraemic syndrome in a patient with sickle cell disease, successfully treated with eculizumab. Br J Haematol. 2016;175(4): Stowell SR, Winkler AM, Maier CL, et al. Initiation and Regulation of Complement during Hemolytic Transfusion Reactions. Clin Dev Immunol. 2012;2012: e
11 Table 1. Evaluation of complement pathway during DHTR episodes C3a ( ng/ml) C5a ( ng/ml) Bb ( mcg/ml)* SC5b-9 ( 244 ng/ml) CH50 ( units) C3 ( mg/dl) C4 ( mg/dl) DHTR #2 (Day 6) DHTR #3 (Day 13) Pre 1 st dose DHTR #3 (Day 38) Pre 2 nd dose * ND ND 135 ND ND ND 21.4 ND ND (Day 127) Clinic visit C3a - complement component fragment 3a, C5a - complement component fragment 5a, Bb complement component fragment Bb, sc5b-9 - soluble membrane attack complex, CH50 - screening test for total complement activity, C3 - complement component 3, C4 - complement component 4. ND- not done. All testing was obtained in a CLIA certified hospital-based clinical laboratory. All normal values are in parenthesis under each value except for day 13 *( mcg/ml) due to variability seen with different ELISA kits. DHTR#2 signifies the second DHTR episode at 13.5 years of age with complement evaluation on day 6 of presentation. The complement testing under DHTR#3 reflects the ACP pathway testing on the days just prior to administration of eculizumab on days 14 and 39. Testing at Day 127 reflects baseline complement levels during a routine sickle cell clinic appointment when the patient was well. Fragment Bb is a serine protease that in combination with hydrolyzed complement factor 3 (C3H 2 O) generates the formation of C3bBb (C3 convertase), which amplifies the cleavage of C3 to produce C3a and C3b which results in local inflammation and RBC opsonization respectively. 16 Anaphylatoxins, C3a and C5a are involved in local inflammation and tissue damage. Terminal complex, C5b-9 contributes to intravascular hemolysis. dd
12 Figure Legend Figure 1. A graphic representation of three DHTR episodes. A) DHTR episode #1. The patient received transfusion (T) on day -9 and presented with DHTR on day 1. B) DHTR episode #2. Hemolysis and absolute reticulocytopenia occurred nine days after transfusion (T). C) DHTR episode #3. Grey colored bars depict the time points when various treatments were administered. (D) DHTR episode #3 showing the doubling of creatinine to 1.0 mg/dl from baseline. Methylprednisolone at a dose of 50mg once daily was given initially on days 11 through day 18. Prednisolone weaning regimen was then started at 2 mg/kg/day on day 18 and completed on day 60. Erythropoietin was administered at the same dose of 300 IU/kg three times a week on days 11 through 14, and then given daily until day 18. Immunohematology work-up during three DHTR episodes: DHTR #1- DAT negative, anti-s (new) and anti-di a (new) detected. DHTR #2- DAT negative, anti-sd a (new) detected, and cold agglutinin detected in serum. Historical anti-s and anti-di a not seen. DHTR #3- DAT negative, anti-sda reconfirmed. Historical anti-s, anti-di a, and cold agglutinin not seen. Patient s current RBC antigen restrictions include: ABO/Rh compatible, CEK-, Fya-, Jkb- S-, Dia-, sickle-negative, crossmatch compatible units. HGB Hemoglobin, ARC Absolute Reticulocyte Count, LDH Lactate Dehydrogenase, IVIg Intravenous Immunoglobulin. dd
13
14 Supplemental Figure Legend Supplemental Figure 1. Overview of the Complement Pathways. The complement cascade is initiated by one or more of the three pathways; classical, mannose binding lectin (MBL) and the alternative pathway. All three pathways converge to form a C3 convertase that cleaves C3 in a continuous fashion to form C3b and C3a, creating an amplification loop. C3b associates with the C3 convertase to form a C5 convertase which in turn cleaves C5 to form C5a and C5b. Formation of C5b begins the initiation of the membrane attack complex (MAC- C5b-9) with the addition of C6 through C9. C5b-9 is involved in cell lysis while C3a and C5a are potent anaphylatoxins. The complement cascade is highly regulated through a variety of additional inhibitory factors that are not depicted in this figure. 1
Rationale for RBC Transfusion in SCD
 Rationale for RBC Transfusion in SCD Dilution of HgbS-containing RBCs via the addition of HgbA-containing cells from the blood of normal donors Suppression of erythropoietin release caused by the rise
Rationale for RBC Transfusion in SCD Dilution of HgbS-containing RBCs via the addition of HgbA-containing cells from the blood of normal donors Suppression of erythropoietin release caused by the rise
Title: Post-transfusion hyperhemolysis syndrome following gastrointestinal bleeding secondary to prehepatic portal hypertension
 Title: Post-transfusion hyperhemolysis syndrome following gastrointestinal bleeding secondary to prehepatic portal hypertension Authors: María de los Ángeles Mejías Manzano, Álvaro Giráldez Gallego, Yolanda
Title: Post-transfusion hyperhemolysis syndrome following gastrointestinal bleeding secondary to prehepatic portal hypertension Authors: María de los Ángeles Mejías Manzano, Álvaro Giráldez Gallego, Yolanda
ASH Draft Recommendations for SCD Related Transfusion Support
 ASH Draft Recommendations for SCD Related Transfusion Support INTRODUCTION American Society of Hematology (ASH) guidelines are based on a systematic review of available evidence. Through a structured process,
ASH Draft Recommendations for SCD Related Transfusion Support INTRODUCTION American Society of Hematology (ASH) guidelines are based on a systematic review of available evidence. Through a structured process,
Paroxysmal Nocturnal Hemoglobinuria
 Paroxysmal Nocturnal Hemoglobinuria Barry Skikne MD, FACP, FCP(SA) Professor of Hematology Division of Hematologic Malignancies and Cellular Therapeutics Cardinal Clinical Manifestations PNH Clonal disease
Paroxysmal Nocturnal Hemoglobinuria Barry Skikne MD, FACP, FCP(SA) Professor of Hematology Division of Hematologic Malignancies and Cellular Therapeutics Cardinal Clinical Manifestations PNH Clonal disease
Transfusion Practices and Creation of a Registry for Patients with Sickle Cell Disease within the Atlanta Sickle Cell Consortium
 Transfusion Practices and Creation of a Registry for Patients with Sickle Cell Disease within the Atlanta Sickle Cell Consortium Annie Winkler MD Assistant Professor, Emory University Department of Pathology
Transfusion Practices and Creation of a Registry for Patients with Sickle Cell Disease within the Atlanta Sickle Cell Consortium Annie Winkler MD Assistant Professor, Emory University Department of Pathology
Delayed hemolytic transfusion reaction in the French hemovigilance system
 Delayed hemolytic transfusion reaction in the French hemovigilance system C. Rieux, G. Brittenham, D. Bachir, E. De Meyer, K. Boudjedir for the French hemovigilance network First Seminar on delayed hemolytic
Delayed hemolytic transfusion reaction in the French hemovigilance system C. Rieux, G. Brittenham, D. Bachir, E. De Meyer, K. Boudjedir for the French hemovigilance network First Seminar on delayed hemolytic
Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura
 Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura Kristen Knoph, PharmD, BCPS PGY2 Pharmacotherapy Resident Pharmacy Grand Rounds April 25, 2017 2016 MFMER slide-1 Objectives
Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura Kristen Knoph, PharmD, BCPS PGY2 Pharmacotherapy Resident Pharmacy Grand Rounds April 25, 2017 2016 MFMER slide-1 Objectives
Transfusions in Sickle Cell Disease: How, When and Why
 Transfusions in Sickle Cell Disease: How, When and Why James R. Eckman, MD Professor Emeritus of Hematology and Medical Oncology Emory University School of Medicine This work is supported by the Centers
Transfusions in Sickle Cell Disease: How, When and Why James R. Eckman, MD Professor Emeritus of Hematology and Medical Oncology Emory University School of Medicine This work is supported by the Centers
Brrrr, It s Cold In Here
 Brrrr, It s Cold In Here Kate Grogan, MD Transfusion Medicine Fellow Physician, BloodworksNW 4/24/15 Patient 20 year old female Viral illness Presents one week later with severe hemolysis Hgb 5.6 Increased
Brrrr, It s Cold In Here Kate Grogan, MD Transfusion Medicine Fellow Physician, BloodworksNW 4/24/15 Patient 20 year old female Viral illness Presents one week later with severe hemolysis Hgb 5.6 Increased
3/31/2014 PNH. Jack Goldberg MD FACP. Clinical Professor of Medicine University of Pennsylvania
 PNH Jack Goldberg MD FACP Clinical Professor of Medicine University of Pennsylvania 1 2 3 4 1 5 6 Historically Viewed as a Hemolytic Anemia Normal red blood cells are protected from complement attack by
PNH Jack Goldberg MD FACP Clinical Professor of Medicine University of Pennsylvania 1 2 3 4 1 5 6 Historically Viewed as a Hemolytic Anemia Normal red blood cells are protected from complement attack by
Soliris (eculizumab) DRUG.00050
 Market DC Soliris (eculizumab) DRUG.00050 Override(s) Prior Authorization Approval Duration 1 year Medications Soliris (eculizumab) APPROVAL CRITERIA Paroxysmal Nocturnal Hemoglobinuria I. Initiation of
Market DC Soliris (eculizumab) DRUG.00050 Override(s) Prior Authorization Approval Duration 1 year Medications Soliris (eculizumab) APPROVAL CRITERIA Paroxysmal Nocturnal Hemoglobinuria I. Initiation of
Hemolytic uremic syndrome: Investigations and management
 Hemolytic uremic syndrome: Investigations and management SAWAI Toshihiro M.D., Ph.D. Department of Pediatrics, Shiga University of Medical Science Otsu, JAPAN AGENDA TMA; Thrombotic micro angiopathy STEC-HUS;
Hemolytic uremic syndrome: Investigations and management SAWAI Toshihiro M.D., Ph.D. Department of Pediatrics, Shiga University of Medical Science Otsu, JAPAN AGENDA TMA; Thrombotic micro angiopathy STEC-HUS;
Understanding the Complement Cascade and Its Role in Cold Agglutinin Disease. 1 M-CAgD-US-3006 February 2018
 Understanding the Complement Cascade and Its Role in Cold Agglutinin Disease 1 February 2018 Instructions This information is provided as an educational resource for healthcare providers. It is not intended
Understanding the Complement Cascade and Its Role in Cold Agglutinin Disease 1 February 2018 Instructions This information is provided as an educational resource for healthcare providers. It is not intended
3/6/2017. Prevention of Complement Activation and Antibody Development: Results from the Duet Trial
 Prevention of Complement Activation and Antibody Development: Results from the Duet Trial Jignesh Patel MD PhD FACC FRCP Medical Director, Heart Transplant Cedars-Sinai Heart Institute Disclosures Name:
Prevention of Complement Activation and Antibody Development: Results from the Duet Trial Jignesh Patel MD PhD FACC FRCP Medical Director, Heart Transplant Cedars-Sinai Heart Institute Disclosures Name:
Introduction. A system of soluble enzymes and proteins. Complement components: C1 to C9, B, D and P
 Complement Introduction A system of soluble enzymes and proteins Complement components: C1 to C9, B, D and P When activated, each component is split into small and large (major) fragments a b *A horizontal
Complement Introduction A system of soluble enzymes and proteins Complement components: C1 to C9, B, D and P When activated, each component is split into small and large (major) fragments a b *A horizontal
Sickle cell disease and hyperhemolysis: epidemiology, riskfactorsand new therapeutic approaches in France
 Sickle cell disease and hyperhemolysis: epidemiology, riskfactorsand new therapeutic approaches in France WORLD APHERESIS ASSOCIATION AND FRENCH SOCIETY FOR HEMAPHERESIS April 27-29, 2016, PARIS-FRANCE
Sickle cell disease and hyperhemolysis: epidemiology, riskfactorsand new therapeutic approaches in France WORLD APHERESIS ASSOCIATION AND FRENCH SOCIETY FOR HEMAPHERESIS April 27-29, 2016, PARIS-FRANCE
SOLIRIS is a Complement Inhibitor Indicated for the Treatment of Patients With PNH to Reduce Hemolysis
 SOLIRIS (eculizumab) SOLIRIS is a Complement Inhibitor Indicated for the Treatment of Patients With PNH to Reduce Hemolysis SOLIRIS is the First and Only Approved Therapy for PNH SOLIRIS (eculizumab) [package
SOLIRIS (eculizumab) SOLIRIS is a Complement Inhibitor Indicated for the Treatment of Patients With PNH to Reduce Hemolysis SOLIRIS is the First and Only Approved Therapy for PNH SOLIRIS (eculizumab) [package
New phase 2 Clinical Trial Enrolling Now
 New phase 2 Clinical Trial Enrolling Now Warm Autoimmune Hemolytic Anemia (waiha) and Cold Agglutinin Disease (CAD) Designed for patients Age 18 or older With a primary diagnosis of waiha who had a recurrence,
New phase 2 Clinical Trial Enrolling Now Warm Autoimmune Hemolytic Anemia (waiha) and Cold Agglutinin Disease (CAD) Designed for patients Age 18 or older With a primary diagnosis of waiha who had a recurrence,
New phase 2 Clinical Trial Enrolling Now
 New phase 2 Clinical Trial Enrolling Now Warm Autoimmune Hemolytic Anemia (waiha) and Cold Agglutinin Disease (CAD) Designed for patients Age 18 or older With a primary diagnosis of waiha who had a recurrence,
New phase 2 Clinical Trial Enrolling Now Warm Autoimmune Hemolytic Anemia (waiha) and Cold Agglutinin Disease (CAD) Designed for patients Age 18 or older With a primary diagnosis of waiha who had a recurrence,
7/14/2014. SOLIRIS (eculizumab) SOLIRIS PNH Clinical Studies. SOLIRIS Blocks Terminal Complement. 86% Reduction in LDH: TRIUMPH and SHEPHERD
 Proximal Terminal Lactate Dehydrogenase (U/L) 7/1/1 SOLIRIS (eculizumab) Humanized First in Class Anti - C5 Antibody SOLIRIS (eculizumab) Human Framework Regions No mutations Germline SOLIRIS is a Complement
Proximal Terminal Lactate Dehydrogenase (U/L) 7/1/1 SOLIRIS (eculizumab) Humanized First in Class Anti - C5 Antibody SOLIRIS (eculizumab) Human Framework Regions No mutations Germline SOLIRIS is a Complement
PILOT STUDY OF ANTIGEN MATCHING FOR AUTOIMMUNE HEMOLYTIC ANEMIA
 PILOT STUDY OF ANTIGEN MATCHING FOR AUTOIMMUNE HEMOLYTIC ANEMIA Sharon Rice & Fred Plapp Saint Luke s Hospital Kansas City, MO CENTRALIZED TRANSFUSION SERVICE Antibody identification Antibody titer Antigen
PILOT STUDY OF ANTIGEN MATCHING FOR AUTOIMMUNE HEMOLYTIC ANEMIA Sharon Rice & Fred Plapp Saint Luke s Hospital Kansas City, MO CENTRALIZED TRANSFUSION SERVICE Antibody identification Antibody titer Antigen
Living with PNH 7/3/2013. Paroxysmal Nocturnal Hemoglobinuria (PNH): A Chronic, Systemic, and Life- Threatening Disease
 Living with PNH Laurence A. Boxer, MD University of Michigan Case Study 15 year old awakened in the morning with chest pain and a sore throat. She experienced chest pain all day accompanied with coughing
Living with PNH Laurence A. Boxer, MD University of Michigan Case Study 15 year old awakened in the morning with chest pain and a sore throat. She experienced chest pain all day accompanied with coughing
JPM Presentation January 9, 2018
 JPM Presentation January 9, 18 Forward looking statements Statements in this press release about future expectations, plans and prospects, as well as any other statements regarding matters that are not
JPM Presentation January 9, 18 Forward looking statements Statements in this press release about future expectations, plans and prospects, as well as any other statements regarding matters that are not
Delayed haemolytic transfusion reaction in adults with sickle cell disease: a 5-year experience
 research paper Delayed haemolytic transfusion reaction in adults with sickle cell disease: a 5-year experience Jennifer B. Vidler, 1,2 * Kate Gardner, 1,2 * Kenneth Amenyah, 2 Aleksandar Mijovic 2 and
research paper Delayed haemolytic transfusion reaction in adults with sickle cell disease: a 5-year experience Jennifer B. Vidler, 1,2 * Kate Gardner, 1,2 * Kenneth Amenyah, 2 Aleksandar Mijovic 2 and
Clinical decision making: Red blood cell alloantibodies
 Clinical decision making: Red blood cell alloantibodies Beth H. Shaz, MD Chief Medical Officer, VP New York Blood Center; Clinical Associate Professor Emory University School of Medicine 1 5 non-abo fatal
Clinical decision making: Red blood cell alloantibodies Beth H. Shaz, MD Chief Medical Officer, VP New York Blood Center; Clinical Associate Professor Emory University School of Medicine 1 5 non-abo fatal
DRUG NAME: Eculizumab Brand(s): Soliris DOSAGE FORM/ STRENGTH: 10 mg/ml (300 mg per vial)
 Preamble: A confirmed diagnosis of atypical hemolytic uremic syndrome (ahus) is required for eculizumab funding. The information below is to provide clinicians with context for how a diagnosis of ahus
Preamble: A confirmed diagnosis of atypical hemolytic uremic syndrome (ahus) is required for eculizumab funding. The information below is to provide clinicians with context for how a diagnosis of ahus
Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease
 Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease A Pocket Guide for the Clinician Susan E. Creary, MD, MSc 1 John J. Strouse, MD, PhD 2 1 The Ohio State University School of
Hydroxyurea and Transfusion Therapy for the Treatment of Sickle Cell Disease A Pocket Guide for the Clinician Susan E. Creary, MD, MSc 1 John J. Strouse, MD, PhD 2 1 The Ohio State University School of
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
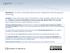 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
New Phase III Clinical Trial Enrolling Now
 New Phase III Clinical Trial Enrolling Now Paroxysmal Nocturnal Hemoglobinuria (PNH) Designed for Patients 1. At least 18 years of age 2. With a primary diagnosis of PNH confirmed by high-sensitivity flow
New Phase III Clinical Trial Enrolling Now Paroxysmal Nocturnal Hemoglobinuria (PNH) Designed for Patients 1. At least 18 years of age 2. With a primary diagnosis of PNH confirmed by high-sensitivity flow
Eculizumab chez les receveurs de greffe rénal à haut risque immunologique. Mark D. Stegall Mayo Clinic, Rochester, MN
 Eculizumab chez les receveurs de greffe rénal à haut risque immunologique Mark D. Stegall Mayo Clinic, Rochester, MN Disclosure. Dr Mark Stegall. Institution : Mayo Clinic, Rochester. Research contracts
Eculizumab chez les receveurs de greffe rénal à haut risque immunologique Mark D. Stegall Mayo Clinic, Rochester, MN Disclosure. Dr Mark Stegall. Institution : Mayo Clinic, Rochester. Research contracts
International PNH Interest Group Meeting Dec 8, 2017
 International PNH Interest Group Meeting Dec 8, 2017 APL-2 is a C3 inhibitor APL-2 Subcutaneous for PNH, AIHA & CDN Intravitreal for GA Peptides of the APL-2 family bind to a pocket of C3 and inhibit activation*
International PNH Interest Group Meeting Dec 8, 2017 APL-2 is a C3 inhibitor APL-2 Subcutaneous for PNH, AIHA & CDN Intravitreal for GA Peptides of the APL-2 family bind to a pocket of C3 and inhibit activation*
Transfusion Reactions. Directed by M-azad March 2012
 Transfusion Reactions Directed by M-azad March 2012 Transfusion Reactions are Adverse reactions associated with the transfusion of blood and its components Transfusion reactions Non-threatening to fatal
Transfusion Reactions Directed by M-azad March 2012 Transfusion Reactions are Adverse reactions associated with the transfusion of blood and its components Transfusion reactions Non-threatening to fatal
Apellis Company Presentation October
 Apellis Company Presentation October 218 1 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding matters that
Apellis Company Presentation October 218 1 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding matters that
History. Chapter 13. Complement Components. Complement Pathways
 History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
M1 - Immunology, Winter 2008
 University of Michigan Deep Blue deepblue.lib.umich.edu 2008-09 M1 - Immunology, Winter 2008 Fantone, J.; Pietropaolo, M. T. Fantone, J., Pietropaolo, M. T. (2008, August 13). Immunology. Retrieved from
University of Michigan Deep Blue deepblue.lib.umich.edu 2008-09 M1 - Immunology, Winter 2008 Fantone, J.; Pietropaolo, M. T. Fantone, J., Pietropaolo, M. T. (2008, August 13). Immunology. Retrieved from
Jefferies Complement Therapeutics Summit April
 Jefferies Complement Therapeutics Summit April 218 1 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding
Jefferies Complement Therapeutics Summit April 218 1 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding
Safety and Efficacy of Eculizumab in Pediatric Patients With ahus, With or Without Baseline Dialysis
 SP281 Safety and Efficacy of Eculizumab in Pediatric Patients With ahus, With or Without Baseline Johan Vande Walle, 1 Larry A. Greenbaum, 2 Camille L. Bedrosian, 3 Masayo Ogawa, 3 John F. Kincaid, 3 Chantal
SP281 Safety and Efficacy of Eculizumab in Pediatric Patients With ahus, With or Without Baseline Johan Vande Walle, 1 Larry A. Greenbaum, 2 Camille L. Bedrosian, 3 Masayo Ogawa, 3 John F. Kincaid, 3 Chantal
ASFA 2015 Consensus Conference: RBC Exchange in Sickle Cell Disease
 ASFA 2015 Consensus Conference: RBC Exchange in Sickle Cell Disease Session 5B: SELECTION OF RED CELLS Araba Afenyi-Annan, MD, MPH Adjunct Assistant Professor Department of Pathology & Laboratory Medicine,
ASFA 2015 Consensus Conference: RBC Exchange in Sickle Cell Disease Session 5B: SELECTION OF RED CELLS Araba Afenyi-Annan, MD, MPH Adjunct Assistant Professor Department of Pathology & Laboratory Medicine,
Complement: History. Discovered in 1894 by Bordet. It represents lytic activity of fresh serum
 Complement: History Discovered in 1894 by Bordet It represents lytic activity of fresh serum Its lytic activity destroyed when heated at 56C for 30 min Complement functions Host benefit: opsonization to
Complement: History Discovered in 1894 by Bordet It represents lytic activity of fresh serum Its lytic activity destroyed when heated at 56C for 30 min Complement functions Host benefit: opsonization to
Remissions after long term use of romiplostim for immune thrombocytopenia
 Published Ahead of Print on September 1, 2016, as doi:10.3324/haematol.2016.151886. Copyright 2016 Ferrata Storti Foundation. Remissions after long term use of romiplostim for immune thrombocytopenia by
Published Ahead of Print on September 1, 2016, as doi:10.3324/haematol.2016.151886. Copyright 2016 Ferrata Storti Foundation. Remissions after long term use of romiplostim for immune thrombocytopenia by
Sickle Cell Disease. Edward Malters, MD
 Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
Apellis Company Presentation March 2019
 Apellis Company Presentation March 219 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding matters that
Apellis Company Presentation March 219 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding matters that
8/28/2018. Disclosures. Objectives. None. Automation to PreciseType and Everything in Between
 Automation to PreciseType and Everything in Between Jessie Singer MT(ASCP) Transfusion Medicine Children s Hospital Los Angeles None Disclosures Objectives Describe the application of molecular testing
Automation to PreciseType and Everything in Between Jessie Singer MT(ASCP) Transfusion Medicine Children s Hospital Los Angeles None Disclosures Objectives Describe the application of molecular testing
Automation to PreciseType and Everything in Between. Jessie Singer MT(ASCP) Transfusion Medicine Children s Hospital Los Angeles
 Automation to PreciseType and Everything in Between Jessie Singer MT(ASCP) Transfusion Medicine Children s Hospital Los Angeles None Disclosures Objectives Describe the application of molecular testing
Automation to PreciseType and Everything in Between Jessie Singer MT(ASCP) Transfusion Medicine Children s Hospital Los Angeles None Disclosures Objectives Describe the application of molecular testing
PNH PNH PNH 3/22/2016 PNH. Paroxysmal Nocturnal Hemoglobinuria (PNH): Current Thinking on the Disease PATHOGENESIS OF PNH
 3//1 PATHGENESIS F PIG-A gene Bone Marrow Failure Disease Scientific Symposium Rockville, March 17-1, 1 1 71 9 3 Paroxysmal Nocturnal Hemoglobinuria (): Current Thinking on the Disease 119 5 15 PRTEIN
3//1 PATHGENESIS F PIG-A gene Bone Marrow Failure Disease Scientific Symposium Rockville, March 17-1, 1 1 71 9 3 Paroxysmal Nocturnal Hemoglobinuria (): Current Thinking on the Disease 119 5 15 PRTEIN
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report
 Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
Paroxysmal Nocturnal Hemoglobinuria
 Paroxysmal Nocturnal Hemoglobinuria Current Thinking On the Disease Diagnosis and Treatment Ilene Ceil Weitz, MD Associate Clinical Professor of Medicine Jane Anne Nohl Division of Hematology Keck-USC
Paroxysmal Nocturnal Hemoglobinuria Current Thinking On the Disease Diagnosis and Treatment Ilene Ceil Weitz, MD Associate Clinical Professor of Medicine Jane Anne Nohl Division of Hematology Keck-USC
Apellis Company Presentation November
 Apellis Company Presentation November 2018 1 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding matters
Apellis Company Presentation November 2018 1 Forward looking statements Statements in this presentation about future expectations, plans and prospects, as well as any other statements regarding matters
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
When Selfies Go Bad!
 When Selfies Go Bad! Decoding Autoantibodies and Autoimmune Hemolytic Anemia D. Joe Chaffin, MD April 17, 2017 Outline Background Warm autoantibodies and WAIHA Cold autoantibodies and CAD Paroxysmal Cold
When Selfies Go Bad! Decoding Autoantibodies and Autoimmune Hemolytic Anemia D. Joe Chaffin, MD April 17, 2017 Outline Background Warm autoantibodies and WAIHA Cold autoantibodies and CAD Paroxysmal Cold
The use of the complement inhibitor eculizumab (Soliris R ) for treating Korean patients with paroxysmal nocturnal hemoglobinuria
 VOLUME 45 ㆍ NUMBER 4 ㆍ December 2010 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE The use of the complement inhibitor eculizumab (Soliris R ) for treating Korean patients with paroxysmal nocturnal
VOLUME 45 ㆍ NUMBER 4 ㆍ December 2010 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE The use of the complement inhibitor eculizumab (Soliris R ) for treating Korean patients with paroxysmal nocturnal
CD B T NK NKT!! 1
 CD B T NK NKT!! 1 2 !! 3 4 5 6 7 8 9 10 11 Biological effects of C5a 12 13 Opsonization and phagocytosis 14 15 http://www.med.sc.edu:85/book/wel come.htm 16 http://www.med.sc.edu:85/book/im munol-sta.htm
CD B T NK NKT!! 1 2 !! 3 4 5 6 7 8 9 10 11 Biological effects of C5a 12 13 Opsonization and phagocytosis 14 15 http://www.med.sc.edu:85/book/wel come.htm 16 http://www.med.sc.edu:85/book/im munol-sta.htm
A sickle in a pickle! by Julie Kirkegaard, MT(ASCP)SBB Community Blood Center, KC, MO and Elizabeth Jones, MT(ASCP)BB Saint Luke s Hospital, KC, MO
 A sickle in a pickle! by Julie Kirkegaard, MT(ASCP)SBB Community Blood Center, KC, MO and Elizabeth Jones, MT(ASCP)BB Saint Luke s Hospital, KC, MO A couple of definitions! Sickle Cell Disease- an autosomal
A sickle in a pickle! by Julie Kirkegaard, MT(ASCP)SBB Community Blood Center, KC, MO and Elizabeth Jones, MT(ASCP)BB Saint Luke s Hospital, KC, MO A couple of definitions! Sickle Cell Disease- an autosomal
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Case Report Title: Paroxysmal cold
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Case Report Title: Paroxysmal cold
Immunohematology (Introduction)
 Modified from Serotonin version Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood
Modified from Serotonin version Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood
History. Chapter 13. Complement Components. Complement Pathways
 History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
Webinar: Association of Hgb A Clearance & RBC Antibodies
 Webinar: Association of Hgb A Clearance & RBC Antibodies Second Webinar Session A second session of this webinar will be hosted Wednesday, July 12 2:00 PM EST (1800 GMT) Register at the link below: https://attendee.gotowebinar.com/rt/9012031991808089089
Webinar: Association of Hgb A Clearance & RBC Antibodies Second Webinar Session A second session of this webinar will be hosted Wednesday, July 12 2:00 PM EST (1800 GMT) Register at the link below: https://attendee.gotowebinar.com/rt/9012031991808089089
Anemia. A case-based approach. David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017
 Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Chapter 6: Blood Transfusion in the Management of Sickle Cell Disease
 Chapter 6: Blood Transfusion in the Management of Sickle Cell Disease Introduction Donor erythrocyte (red blood cell, RBC) transfusion was the first therapy used in SCD that targets the pathophysiology
Chapter 6: Blood Transfusion in the Management of Sickle Cell Disease Introduction Donor erythrocyte (red blood cell, RBC) transfusion was the first therapy used in SCD that targets the pathophysiology
Transforming Complement Therapeutics. October 2018
 Transforming Complement Therapeutics October 2018 Forward Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform Act of
Transforming Complement Therapeutics October 2018 Forward Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform Act of
Soliris. Soliris (eculizumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.85.11 Subject: Soliris Page: 1 of 5 Last Review Date: September 20, 2018 Soliris Description Soliris
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.85.11 Subject: Soliris Page: 1 of 5 Last Review Date: September 20, 2018 Soliris Description Soliris
Not So Benign Hematology Aplastic anemia, Paroxysmal Nocturnal Hemoglobinuria, atypical Hemolytic Uremic Syndrome, Thrombotic Thrombocytopenic Purpura
 Not So Benign Hematology Aplastic anemia, Paroxysmal Nocturnal Hemoglobinuria, atypical Hemolytic Uremic Syndrome, Thrombotic Thrombocytopenic Purpura Robert A. Brodsky, MD Johns Hopkins Family Professor
Not So Benign Hematology Aplastic anemia, Paroxysmal Nocturnal Hemoglobinuria, atypical Hemolytic Uremic Syndrome, Thrombotic Thrombocytopenic Purpura Robert A. Brodsky, MD Johns Hopkins Family Professor
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature
 Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
Soliris (eculizumab): Physician s guide to prescribing for patients with paroxysmal nocturnal haemoglobinuria (PNH)
 Soliris (eculizumab): Physician s guide to prescribing for patients with paroxysmal nocturnal haemoglobinuria (PNH) CONTENTS PAGE WHAT IS SOLIRIS? SOLIRIS INDICATIONS IMPORTANT SAFETY INFORMATION SOLIRIS
Soliris (eculizumab): Physician s guide to prescribing for patients with paroxysmal nocturnal haemoglobinuria (PNH) CONTENTS PAGE WHAT IS SOLIRIS? SOLIRIS INDICATIONS IMPORTANT SAFETY INFORMATION SOLIRIS
It s not just allo-antibodies that a red cell transfusion can stimulate
 It s not just allo-antibodies that a red cell transfusion can stimulate Associate Professor Ralph Green Laboratory Medicine RMIT University Melbourne, Australia Transfusion practice Minimise risk of transmitting
It s not just allo-antibodies that a red cell transfusion can stimulate Associate Professor Ralph Green Laboratory Medicine RMIT University Melbourne, Australia Transfusion practice Minimise risk of transmitting
Sickle Cell Disease Overview/Transfusion Support Wednesday, August 29, :00 p.m. 3:30 p.m. (ET) / 6:00p.m.-7:30 p.m. (GMT)
 Sickle Cell Disease Overview/Transfusion Support Wednesday, August 29, 2012 2:00 p.m. 3:30 p.m. (ET) / 6:00p.m.-7:30 p.m. (GMT) When this file is opened, Acrobat Reader will, by default, display the slides
Sickle Cell Disease Overview/Transfusion Support Wednesday, August 29, 2012 2:00 p.m. 3:30 p.m. (ET) / 6:00p.m.-7:30 p.m. (GMT) When this file is opened, Acrobat Reader will, by default, display the slides
Target cell lysis Opsonization Activation of the inflammatory response (e.g. degranulation, extravasation) Clearance of immune complexes
 Immunology Dr. John J. Haddad Chapter 13 Complement Major roles of complement (Figure 13-1): Target cell lysis Opsonization Activation of the inflammatory response (e.g. degranulation, extravasation) Clearance
Immunology Dr. John J. Haddad Chapter 13 Complement Major roles of complement (Figure 13-1): Target cell lysis Opsonization Activation of the inflammatory response (e.g. degranulation, extravasation) Clearance
Impact of ibrutinib dose intensity on patient outcomes in previously treated Waldenström macroglobulinemia
 Published Ahead of Print on May 17, 2018, as doi:10.3324/haematol.2018.191999. Copyright 2018 Ferrata Storti Foundation. Impact of ibrutinib dose intensity on patient outcomes in previously treated Waldenström
Published Ahead of Print on May 17, 2018, as doi:10.3324/haematol.2018.191999. Copyright 2018 Ferrata Storti Foundation. Impact of ibrutinib dose intensity on patient outcomes in previously treated Waldenström
Transforming Complement Therapeutics. June 2018
 Transforming Complement Therapeutics June 2018 Forward Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform Act of 1995,
Transforming Complement Therapeutics June 2018 Forward Looking Statements This presentation contains "forward-looking statements" within the meaning of the Private Securities Litigation Reform Act of 1995,
Topic (6): The Complement System
 Topic (6): The Complement System Introduction The complement system is a complex system of many different glycoproteins. It comprises several plasma proteins that sequentially activate each other by proteolytic
Topic (6): The Complement System Introduction The complement system is a complex system of many different glycoproteins. It comprises several plasma proteins that sequentially activate each other by proteolytic
Complement. History. Chapter 7. Complement Components. Complement Pathways. Pathways of complement activation
 History Chapter 7 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
History Chapter 7 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
Transfusion in Sickle Cell Disease What the guidelines [are likely to] say. Dr Bernard Davis Whittington Hospital, London
![Transfusion in Sickle Cell Disease What the guidelines [are likely to] say. Dr Bernard Davis Whittington Hospital, London Transfusion in Sickle Cell Disease What the guidelines [are likely to] say. Dr Bernard Davis Whittington Hospital, London](/thumbs/85/91702350.jpg) Transfusion in Sickle Cell Disease What the guidelines [are likely to] say Dr Bernard Davis Whittington Hospital, London Background to BCSH Guideline Rationale Current guidance in disparate publications
Transfusion in Sickle Cell Disease What the guidelines [are likely to] say Dr Bernard Davis Whittington Hospital, London Background to BCSH Guideline Rationale Current guidance in disparate publications
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13
 Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Antibody identification. Antibody specificity
 Red blood cell (RBC) transfusions are frequently used in sickle-cell anaemia (SCA) patients to treat and prevent the complications of their disease. Acute simple transfusions are usually used to treat
Red blood cell (RBC) transfusions are frequently used in sickle-cell anaemia (SCA) patients to treat and prevent the complications of their disease. Acute simple transfusions are usually used to treat
CURRENT COURSE OFFERINGS
 The American Red Cross offers regular educational opportunities as a convenient way for healthcare providers to receive relevant blood banking and transfusion medicine information. The bi-monthly sessions,
The American Red Cross offers regular educational opportunities as a convenient way for healthcare providers to receive relevant blood banking and transfusion medicine information. The bi-monthly sessions,
Lifetime risk and characterization of red blood cell alloimmunization in chronically transfused patients with sickle cell disease
 Woldie et al. 1 ORIGINAL ARTICL PR RVIWD OPN ACCSS Lifetime risk and characterization of red blood cell alloimmunization in chronically transfused patients with sickle cell disease Woldie I., Swerdlow
Woldie et al. 1 ORIGINAL ARTICL PR RVIWD OPN ACCSS Lifetime risk and characterization of red blood cell alloimmunization in chronically transfused patients with sickle cell disease Woldie I., Swerdlow
Siklos (hydroxyurea) NEW PRODUCT SLIDESHOW
 Siklos (hydroxyurea) NEW PRODUCT SLIDESHOW Introduction Brand name: Siklos Generic name: Hydroxyurea Pharmacological class: Antimetabolite Strength and Formulation: 100mg, 1000mg+; tabs; +triple-scored
Siklos (hydroxyurea) NEW PRODUCT SLIDESHOW Introduction Brand name: Siklos Generic name: Hydroxyurea Pharmacological class: Antimetabolite Strength and Formulation: 100mg, 1000mg+; tabs; +triple-scored
Antibody Information
 Antibody Information Rh Blood Group System Anti-D is an IgG antibody directed against the D antigen in the Rh blood group system. Anti-D is Newborn. Patients with Anti-D should receive D- blood (Rh negative).
Antibody Information Rh Blood Group System Anti-D is an IgG antibody directed against the D antigen in the Rh blood group system. Anti-D is Newborn. Patients with Anti-D should receive D- blood (Rh negative).
CASE STUDIES IN CLINICAL APPLICATIONS OF THERAPEUTIC PLASMA EXCHANGE
 CASE STUDIES IN CLINICAL APPLICATIONS OF THERAPEUTIC PLASMA EXCHANGE Eric Rosa, MLS (ASCP) CM Medical Laboratory Scientist Transfusion Service April 18, 2018 Objectives Explain the process of a therapeutic
CASE STUDIES IN CLINICAL APPLICATIONS OF THERAPEUTIC PLASMA EXCHANGE Eric Rosa, MLS (ASCP) CM Medical Laboratory Scientist Transfusion Service April 18, 2018 Objectives Explain the process of a therapeutic
Anemia s. Troy Lund MSMS PhD MD
 Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Suvasini Modi Complement System Activation of Membrane attacking complex (MAC) and its effect and regulation
 Figure- 1 https://en.wikipedia.org/wiki/complement_system Suvasini Modi Complement System Activation of Membrane attacking complex (MAC) and its effect and regulation Content Introduction Activation of
Figure- 1 https://en.wikipedia.org/wiki/complement_system Suvasini Modi Complement System Activation of Membrane attacking complex (MAC) and its effect and regulation Content Introduction Activation of
Case Study. Michael Losos, MD, 1 Diane Hamad, MLS(ASCP), 1 Sarita Joshi, MD, 2 Scott Scrape, MD, 1 Jian Chen, MD, PhD 1 * ABSTRACT
 Warm Autoimmune Hemolytic Anemia and Direct Antiglobulin Testing With a False- Negative Result in a 53-Year-Old Man: The DAT Will Set You Free Michael Losos, MD, 1 Diane Hamad, MLS(ASCP), 1 Sarita Joshi,
Warm Autoimmune Hemolytic Anemia and Direct Antiglobulin Testing With a False- Negative Result in a 53-Year-Old Man: The DAT Will Set You Free Michael Losos, MD, 1 Diane Hamad, MLS(ASCP), 1 Sarita Joshi,
INVESTIGATION OF ADVERSE TRANSFUSION REACTIONS TABLE OF RECOMMENDED TESTS. Type of Reaction Presentation Recommended Tests Follow-up Tests
 Minor Allergic (Urticarial) Urticaria, pruritis, flushing, rash If skin reaction only and mild hives/ rash
Minor Allergic (Urticarial) Urticaria, pruritis, flushing, rash If skin reaction only and mild hives/ rash
Pathophysiology 7/18/2012 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA
 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA OUTLINE OF DISCUSSION WHAT IS IT WHO GETS IT NATURAL HISTORY TYPES RISKS COURSE TREATMENTS SYMPTOMS PREGNANCY Pathophysiology Acquired hematopoietic stem cell disorder
PAROXYSMAL NOCTURNAL HEMOGLOBINURIA OUTLINE OF DISCUSSION WHAT IS IT WHO GETS IT NATURAL HISTORY TYPES RISKS COURSE TREATMENTS SYMPTOMS PREGNANCY Pathophysiology Acquired hematopoietic stem cell disorder
Approach to a patient with suspected blood transfusion reaction. Raju Vaddepally, MD
 Approach to a patient with suspected blood transfusion reaction Raju Vaddepally, MD Goals Detection of Acute Transfusion Reactions (ATR) Clinical and Laboratory Evaluation of ATR Management of individual
Approach to a patient with suspected blood transfusion reaction Raju Vaddepally, MD Goals Detection of Acute Transfusion Reactions (ATR) Clinical and Laboratory Evaluation of ATR Management of individual
NM-96: A Small Molecule For The! Treatment of Acute Sickle Crisis!! Life Science Summit 10/29/14! Steven Isaacman, Ph.D.!
 www.nanometicslab.com! NM-96: A Small Molecule For The! Treatment of Acute Sickle Crisis!! Life Science Summit 10/29/14! Steven Isaacman, Ph.D.!! Founder & CEO!! Nanometics LLC! About Nanometics! Founded
www.nanometicslab.com! NM-96: A Small Molecule For The! Treatment of Acute Sickle Crisis!! Life Science Summit 10/29/14! Steven Isaacman, Ph.D.!! Founder & CEO!! Nanometics LLC! About Nanometics! Founded
An Approach to the Patient Refractory to Platelets Transfusion. Harold Alvarez, MD
 Harold Alvarez, MD Objectives Explain the etiology of platelet refractoriness Discuss the different types of platelet refractoriness Describe how platelet refractoriness is diagnosed Discuss different
Harold Alvarez, MD Objectives Explain the etiology of platelet refractoriness Discuss the different types of platelet refractoriness Describe how platelet refractoriness is diagnosed Discuss different
Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition
 Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood lost by hemorrhage or to correct
Immunohematology (Introduction) References: -Blood Groups and Red Cell Antigens (Laura Dean) -Cellular and molecular immunology, 8 th edition Introduction to replace blood lost by hemorrhage or to correct
Soliris Medical Policy Prior Authorization Program Summary
 Soliris Medical Policy Prior Authorization Program Summary Precertification/Prior Authorization may be required under certain plans. Please verify each member s benefits. OBJECTIVE The intent of the Soliris
Soliris Medical Policy Prior Authorization Program Summary Precertification/Prior Authorization may be required under certain plans. Please verify each member s benefits. OBJECTIVE The intent of the Soliris
Transfusion Reactions
 Transfusion Reactions From A to T Provincial Blood Coordinating Program Daphne Osborne MN PANC (C) RN We want you to know Definition Appropriate actions Classification Complete case studies Transfusion
Transfusion Reactions From A to T Provincial Blood Coordinating Program Daphne Osborne MN PANC (C) RN We want you to know Definition Appropriate actions Classification Complete case studies Transfusion
AIHA The Laboratory Perspective on Testing. Tom Bullock Joint UK NEQAS (BTLP) & BBTS BBT SIG Annual Meeting 20 th November 2018
 AIHA The Laboratory Perspective on Testing Tom Bullock Joint UK NEQAS (BTLP) & BBTS BBT SIG Annual Meeting 20 th November 2018 Auto Immune Haemolytic Anaemia (AIHA) BSH guideline (Hill et al. 2017): AIHA
AIHA The Laboratory Perspective on Testing Tom Bullock Joint UK NEQAS (BTLP) & BBTS BBT SIG Annual Meeting 20 th November 2018 Auto Immune Haemolytic Anaemia (AIHA) BSH guideline (Hill et al. 2017): AIHA
Redbud, Morton Arboretum, Lisle / GR
 Redbud, Morton Arboretum, Lisle / GR 1 Polyagglutination in a Child with Pneumococcal Hemolytic Uremic Syndrome Glenn Ramsey, L. Maria Samuels Northwestern University Lurie Children s Hospital of Chicago
Redbud, Morton Arboretum, Lisle / GR 1 Polyagglutination in a Child with Pneumococcal Hemolytic Uremic Syndrome Glenn Ramsey, L. Maria Samuels Northwestern University Lurie Children s Hospital of Chicago
Boot Camp Transfusion Reactions
 Boot Camp Transfusion Reactions Dr. Kristine Roland Regional Medical Lead for Transfusion Medicine, VCH Objectives By the end of this session, you should be able to: Describe in common language the potential
Boot Camp Transfusion Reactions Dr. Kristine Roland Regional Medical Lead for Transfusion Medicine, VCH Objectives By the end of this session, you should be able to: Describe in common language the potential
What is meant by Thrombotic Microangiopathy (TMA)?
 What is meant by Thrombotic Microangiopathy (TMA)? Thrombotic Microangiopathy (TMA) is a group of disorders characterized by injured endothelial cells, microangiopathic hemolytic anemia (MAHA), with its
What is meant by Thrombotic Microangiopathy (TMA)? Thrombotic Microangiopathy (TMA) is a group of disorders characterized by injured endothelial cells, microangiopathic hemolytic anemia (MAHA), with its
Ibrutinib Withdrawal Symptoms in Patients with Waldenström Macroglobulinemia
 Published Ahead of Print on February 22, 2018, as doi:10.3324/haematol.2017.186908. Copyright 2018 Ferrata Storti Foundation. Ibrutinib Withdrawal Symptoms in Patients with Waldenström Macroglobulinemia
Published Ahead of Print on February 22, 2018, as doi:10.3324/haematol.2017.186908. Copyright 2018 Ferrata Storti Foundation. Ibrutinib Withdrawal Symptoms in Patients with Waldenström Macroglobulinemia
Transfusion Guidelines in AIHA; Indications, Compatibility Testing and Administration.
 Transfusion Guidelines in AIHA; Indications, Compatibility Testing and Administration. Lawrence D. Petz, M.D. Emeritus Professor University of California Los Angeles, California, U.S.A.; Medical Director
Transfusion Guidelines in AIHA; Indications, Compatibility Testing and Administration. Lawrence D. Petz, M.D. Emeritus Professor University of California Los Angeles, California, U.S.A.; Medical Director
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques
 Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques 5850/5980 University Avenue, PO Box 9700 Halifax, NS, B3K 6R8 1.902.470.7429
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques 5850/5980 University Avenue, PO Box 9700 Halifax, NS, B3K 6R8 1.902.470.7429
