Interstitial lung disease and anti-jo-1 antibodies: difference between acute and gradual onset
|
|
|
- Patience Banks
- 5 years ago
- Views:
Transcription
1 1 Service de Pneumologie et Réanimation Respiratoire, Hôpital Tenon, Paris, France; 2 Service de Pneumologie, Hôpital Avicenne, Bobigny, France; 3 Service de Pneumologie, Hôpital Bichat, Paris, France; 4 Service de Pneumologie, Hotel-Dieu, Paris, France; 5 Service de Pneumologie, Hôpital Européen G Pompidou, Paris, France; 6 Service de Pneumologie, Hôpital Béclère, Clamart, France; 7 Service de Pneumologie, Hôpital Foch, Suresnes, France; 8 Service de Pneumologie, Hôpital Calmette, Lille, France Correspondence to: Dr J Cadranel, Service de Pneumologie et Réanimation Respiratoire, Hôpital Tenon, 4 rue de la Chine, Paris Cedex 20, France; jacques. cadranel@tnn.aphp.fr Received 27 July 2006 Accepted 12 March 2007 Published Online First 8 June 2007 Interstitial lung disease and anti-jo-1 antibodies: difference between acute and gradual onset I Tillie-Leblond, 1,8 M Wislez, 1 D Valeyre, 2 B Crestani, 3 A Rabbat, 4 D Israel-Biet, 5 M Humbert, 6 L J Couderc, 7 B Wallaert, 8 J Cadranel 1 ABSTRACT Aim: A multicentre retrospective study was undertaken to examine patients with interstitial lung disease (ILD) with the initial clinical manifestation of an anti-synthetase syndrome (anti-jo-1 antibodies), and to analyse the characteristics and long-term outcome of these patients according to their clinical presentation (acute or gradual onset), treatment and adverse events related to treatment. Methods: 32 patients, 15 (47%) presenting with acute onset and associated respiratory insufficiency (group A) and 17 (53%) with gradual onset (group G) were examined. Myositis was diagnosed at admission in only 31% of cases and was observed during follow-up in 56% of cases, but the prevalence did not differ between the two groups. Results: Fever and radiological patterns including diffuse patchy ground-glass opacities, basal irregular lines and consolidation on high-resolution CT scan were more frequent in group A than in group G. More patients in group G had neutrophils in the bronchoalveolar lavage fluid and autoantibodies other than anti-jo-1 (rheumatoid factor, anti SSa/SSb) than in group A. The percentage of patients in whom the ILD improved at 3 months was significantly higher in group A than in group G (13/15 vs 9/17; p = 0.006). In contrast, after 12 months, most patients with ILD progression were in group A and were treated with corticosteroids alone. A combination of corticosteroids and an immunosuppressive drug was required in most cases (84%) at the end of the follow-up period. Severe adverse effects of treatment were observed and varicella zoster virus infection was frequent. Conclusions: Early testing for anti-synthetase antibodies, particularly anti-jo-1, and creatine kinase determination are useful procedures in patients presenting with ILD. Treatment with corticosteroids and immunosuppressive drugs is required in most patients. At the end of the study, around two-thirds of patients had stable ILD while the other third had disease progression with respiratory insufficiency. Interstitial lung disease (ILD) may be associated with systemic inflammatory disorders and autoantibody production. The development of ILD has been described in detail in patients with polymyositis and dermatomyositis, 1 10 and has been shown to increase morbidity and mortality in patients with myositis Anti-synthetase antibodies, including anti-jo-1 antibodies (antihistidyltrna synthase), are found in 20 30% of patients with myositis and are most frequent in those with polymyositis However, Schmidt et al, ina large series of patients, showed that the clinical picture of the anti-jo-1 antibody syndrome is Interstitial lung disease variable; indeed, most patients have features other than myositis at disease onset, including ILD. 20 Anti-Jo-1 antibodies have rarely been detected in patients with ILD as the sole manifestation of autoimmune disease. A study was undertaken to evaluate a large number of patients with anti-jo-1 antibodies who presented with ILD as the initial clinical manifestation, with or without extrarespiratory symptoms suggestive of connective tissue disease, and to describe the characteristics and long-term outcome of these patients according to their clinical presentation (acute or gradual onset), treatment and adverse events related to treatment. METHODS Study design and patient selection This multicentre study was conducted in 12 pulmonology departments of university hospitals from the Assistance Publique des Hôpitaux de Paris and Lille University Hospital. These teaching and tertiary care centres were contacted by and asked to identify patients with ILD and anti-jo-1 antibodies at initial evaluation from their registers. Only patients with clinical and radiological findings consistent with ILD, anti-jo-1 antibodies and a follow-up of at least 12 months before the study were included. Patients who had previously been diagnosed as having polymyositis, dermatomyositis or inclusion body myositis and who had been treated before lung involvement occurred, as well as those with dysphagia and/or a subsequent episode of aspiration pneumonia, were excluded from the study. However, patients with myositis (increase in creatine kinase (CK) and/or aldolase, myalgia) as well as arthalgia, Raynaud s phenomenon or skin manifestations before the respiratory symptoms occurred were not excluded from the study if these conditions were the initial manifestations of the anti-jo-1 syndrome. Data collection One physician (ITL) used a standard form to record the characteristics of patients from medical files and contacted the pneumology consultant. The data collected on the form included epidemiological characteristics, ILD characteristics, extrapulmonary manifestations on admission and outcome data evaluating the progression of ILD and extrarespiratory manifestations (at 3 months, 1 year and at the end of the follow-up period), survival and adverse events related to treatment. Thorax 2008;63: doi: /thx
2 Characteristics of ILD on admission Clinical symptoms assessed were cough, dyspnoea (NYHA) and haemoptysis. Crackles on auscultation were reported. Patients were assigned to two groups: acute (A) and gradual (G), based on an analysis of the histogram of distribution of the duration of onset (time in weeks between the first symptom and the diagnosis of anti-jo-1 syndrome) and the presence or absence of acute respiratory failure. Blood gas analysis in ambient air, carbon monoxide transfer factor (TLCO), total lung volume (TLV), slow vital capacity (SVC) and forced expiratory volume in 1 s (FEV 1 ) were reported. Particular attention was paid to high-resolution computed tomography (HRCT) scans of the lung which were reviewed and interpreted by two researchers (ITL and JC). The following characteristics were assessed and noted on a standard form: 25 irregular linear opacities (irregular thickening of interlobular septa), septal thickening (abnormal visualisation of interlobular septa), consolidation, ground-glass opacities, honeycombing, traction bronchiectasis and bronchiolectasis, pleural effusion and adenopathy. The predominance and location were described (eg, lower lobe predominance, peripheral predominance). Bronchoalveolar lavage (BAL) fluid was analysed and the results of cell component (differential counts) and microbacteriological analyses were recorded. Normal reference values 26 are:,15% lymphocytes,,5% neutrophils and,1% eosinophils. Transbronchial biopsy and surgical lung biopsy results analysed according to the classification of Katzenstein and Myers 25 were recorded. Characteristics of extrapulmonary manifestations on admission Weight loss, fever (.38uC), asthenia, cutaneous manifestations, arthralgia, arthritis, Raynaud s phenomenon, myalgia and muscle weakness were recorded. CK levels were recorded and values more than twice the upper limit of the normal range (2N) were considered abnormal. Electromyography (EMG) results were recorded. Myositis was defined as CK.2N and/or an EMG result consistent with the diagnosis of myositis and/or muscle weakness before corticosteroid treatment. 12 Outcome data for ILD and extrarespiratory symptoms The outcome data for ILD and extrarespiratory symptoms were evaluated at 3 months, 12 months and at the last date of follow-up. Treatment regimens (corticosteroids, immunosuppressive drugs) and changes in treatment during follow-up were recorded. The response to treatment of ILD was evaluated according to the ATS criteria. 27 Improvement, stability or failure to respond was documented based on symptoms, HRCT scan and lung function test. All adverse effects related to treatment were recorded. Deaths were also recorded and classified according to whether they were attributable to the disease, treatment or neither. Statistical analysis All results were expressed as median (range). Comparisons were made by the non-parametric Mann-Whitney test and the Fisher exact test. RESULTS Characteristics of the population at initial evaluation (n = 32) All participating hospitals responded, but 5 of the 13 centres did not have any eligible cases. A total of 49 cases of ILD with anti- Jo-1 antibodies were reported between 1 January 1994 and 31 May 2004, of which 17 were excluded (10 because myositis was diagnosed and treated before ILD, 2 due to recurrent aspiration pneumonia and 5 because of inadequate follow-up). Thirty-two patients were therefore evaluated by indirect immunofluorescence on Hep2 cells (cytoplasmic fluorescence), extractable nuclear antigen detection by immunodiffusion (SSa, SSb, Scl70, RNP, Jo-1) and specific ELISA for anti-jo1 antibodies. These patients were assigned to two groups: (1) group A which comprised 15 patients with acute onset of ILD (median duration between first symptom and diagnosis 5 weeks (range 0 8)) and acute respiratory failure needing oxygen therapy; and (2) group G which comprised 17 patients with a gradual onset of ILD (median duration between first symptom and diagnosis 26 weeks (range10 124)). Analysis of respiratory and extrarespiratory manifestations according to initial presentation Significant differences in general characteristics, respiratory manifestations and extrarespiratory findings between the two groups are shown in tables 1 and 2. One of the patients in group G had a history of Grave s disease and another had a history of sarcoidosis (negative for anti-jo-1 antibody at that time); one patient in group A was in remission from breast cancer; and three patients (one in group A and two in group G) were being treated with systemic corticosteroids and hydroxychloroquine or methotrexate for seropositive rheumatoid arthritis (negative for anti-jo-1 antibody before the occurrence of ILD). There was no difference between the two groups in age at diagnosis or occupational exposure. We observed a high number of patients who had been exposed to cleaning products. Fever at admission and severe dyspnoea were more frequent in group A than in group G (table 2). In contrast, the proportion of cutaneous symptoms, arthralgia, myalgia and increased CK levels seemed to be similar in the two groups. EMG was performed in 28 patients with no differences in results between the two groups (table 2). Autoantibodies other than anti-jo-1 antibodies were detected in nine patients in group G but in only one in group A (p = 0.007). All were negative for anti-scl70 antibodies. Isolated rheumatoid factor was detected in three patients (one in group A and two in group G); isolated anti-ro/ssa and La/SSb antibodies were detected in four patients in group G; and a combination of rheumatoid factor, anti-ro/ssa and anti-la/ssb antibodies was detected in three patients in group G. Functional parameters Table 3 compares pulmonary function data in groups A and G. Three patients did not undergo functional testing on admission owing to the severity of ILD. In group A, median values of TLC, SVC, TLCO (expressed as percentages of normal predicted values) as well as arterial oxygen tension (PaO 2 ) measured at rest in room air and expressed in mm Hg were significantly lower than in group G. No patient had an obstructive pattern and FEV 1 did not differ between the two groups. HRCT scan results All patients underwent an HRCT scan. Table 4 shows the data obtained in the two groups. The predominantly inferior location was significantly more frequent in patients in group G, while consolidations were more frequent in group A. A combination of three patterns was observed in 80% of patients in group A: diffuse patchy ground-glass attenuation, basal predominance of irregular linear opacities and basal consolidations 54 Thorax 2008;63: doi: /thx
3 Table 1 Characteristics of the population on admission (n = 32) in groups A and G Parameters Group A (n = 15) Group G (n = 17) p Value Age at diagnosis (years)* 60 (40 72) 52 (32 73) NS Sex (M/F) 5/10 6/11 NS Occupational exposure 7 5 NS Cleaning products 4 4 Aluminum 1 Pesticides 1 Asbestos 1 Products used in dental 1 protheses Smokers 6 4 NS Group A, acute onset of interstitial lung disease; group G, gradual onset of interstitial lung disease. *Results are expressed as median (range). Comparisons were made using the Fisher exact test. (figs 1 and 2). Honeycombing and traction bronchiectasis or bronchiolectasis were infrequent in both groups. BAL and histological data BAL results (expressed as total cells and percentages of lymphocytes, neutrophils, eosinophils and macrophages) were available for 25 of the 32 patients and are summarised in fig 3. The median number of total cells and the percentage of macrophages, lymphocytes, neutrophils and eosinophils did not differ between groups A and G. However, the proportion of patients with.5% of neutrophils in BAL fluid was higher in group G (13/2) than in group A (3/8) (p = 0.004). The CD4:CD8 ratio of BAL lymphocytes was,1 in all 12 cases (5 in group A and 7 in group G) evaluated for BAL T lymphocyte CD4 and CD8 phenotyping. Histological data were obtained for 11 of the 32 patients (surgical lung biopsies (SB) in 6 cases and transbronchial biopsies (TBB) in 5 cases). Non-specific interstitial pneumonitis (NSIP) was diagnosed in 2 patients (2 SB; 1 in group A and 1 in group G) and suspected in 3 (3 TBB; 1 in group A and 2 in group G), cryptogenic organising pneumonitis (COP) was diagnosed in 2 patients (2 TBB; 2 in group A), usual interstitial pneumonitis (UIP) in 2 patients (2 SB; 2 in group G) and diffuse alveolar damage (DAD) associated with fibrosis and COP in 2 patients (2 SB; 2 in group A). Statistical analysis was not performed. We observed that DAD and COP were diagnosed only in group A. Evaluation during the first year in groups A and G At 3 months, two patients (6%) with in group A died on days 10 and 22 (the first was treated with corticosteroids only and the second with corticosteroids and cyclophosphamide; table 5). Both patients died from respiratory failure associated with DAD and, in one case, COP with fibrosis (necropsy). The percentage of patients showing improvement in ILD at 3 months was significantly higher in group A than in group G (13/15 vs 9/17; p = 0.004). In contrast, after 12 months (table 5), most patients in whom ILD continued to progress were in group A and were treated with corticosteroids alone. In group G, 88% of patients had stable ILD and most were on treatment with corticosteroids and immunosuppressive drugs (n = 10). Evaluation at the end of the follow-up period None of the 32 patients were lost to follow-up. The median duration of follow-up was 62 months (range ) for the overall population, 41 months (range ) in group A and Table 2 Comparison of symptoms, creatine kinase levels and results of electromyography at initial presentation in groups A and G Parameter Group A (n = 15) Asthenia Weight loss 7 4 Fever (.38.5uC) 10 4 Arthralgia 9 14 Arthritis 2 3 Clubbing 0 1 Isolated dyspnoea 8 10 Dyspnoea and dry cough 7 7 Crackles Raynaud s phenomenon 4 4 Sicca syndrome 1 2 Gottron s papules 2 1 Heliotrope rash 2 3 Mechanics hand 3 6 Dyspnoea NYHA III/IV 15 7 Myalgia 5 6 Creatine kinase Electromyography* 6 4 Autoantibodies{ 1 9 Group G (n = 17) Group A, acute onset of interstitial lung disease; group G, gradual onset of interstitial lung disease. *Electromyography showing myopathic pattern (perfomed in 28/32 patients. {Rheumatoid factor, Ro/SSa and La/SSb. 62 months (range ) in group G. Twenty-five patients (82%) were still alive and six (18%) had died. Two patients died from respiratory failure with acute interstitial pneumonitis in the first month of follow-up (group A) and one died from severe sepsis attributable to immunosuppressive drugs (group G). Three patients died from neoplasia: one from brain metastasis related to primary lung adenocarcinoma (group A), one from ovarian cancer (group G) and one from non-hodgkin lymphoma (group G). Among the 25 patients alive at the end of follow-up, 21 (84%) received immunosuppressants (cyclophosphamide in 8 patients, methotrexate in 4 and azathioprine in 9). ILD had remained stable in 17 of these 25 patients (based on dyspnoea, pulmonary function tests, TLCO, blood gas analysis and HRCT scan); 4 of these patients received corticosteroids alone, 12 were treated with corticosteroids and immunosuppressive drugs and one received immunosuppressive drugs alone. Eight patients displayed ILD progression with worsening of (or development of) honeycombing and traction bronchiectasis/bronchiolectasis on Table 3 Results of pulmonary function tests and arterial blood gas Parameter Group A Group G p Value TLC (%), n = (28 82) 69 (49 90) SVC (%), n = (25 88) 73 (43 86) 0.02 FEV 1 (%), n = (31 91) 67.5 (48 95) NS TLCO (%), n = (20 50) 46 (35 89) PaO 2 (mm Hg), 53 (42 68) 71 (61 89), n=32 Oxygen therapy on admission 15/15 2/ Results are expressed as median (range). The results for TLC, SVC, FEV 1 and TLCO were expressed as a percentage of the normal predicted value. Comparisons were evaluated by the Mann-Whitney test. Group A, acute onset of interstitial lung disease; group G, gradual onset of interstitial lung disease; TLC, total lung capacity; SVC, slow vital capacity; FEV 1, forced expiratory volume in 1 s; TLCO, carbon monoxide transfer factor; PaO 2, arterial oxygen tension. Thorax 2008;63: doi: /thx
4 Figure 1 High-resolution CT scan of the lung showing patchy groundglass pattern in the upper lobes. the HRCT scan and the need for long-term oxygen therapy; all eight were treated with a combination of corticosteroids and immunosuppressant drugs. Data comparing pulmonary function tests in patients with stable ILD and those with progressive ILD are shown in fig 4. The characteristics on admission were compared between the 8 patients with ILD progression and the 17 with stable disease. The proportion of patients with gradual onset of presentation (2/8 vs 6/17), honeycombing on HRCT scan (4/8 and 5/17) and an increase in neutrophils in BAL fluid (1/5 vs 6/12) did not differ between those who progressed and those with stable disease. Furthermore, the proportion of patients with progressive ILD with myositis at presentation (3/8 vs 9/17) or during follow-up (5/8 and 13/17) was as frequent as that of patients with stable ILD. Finally, the initial treatment of patients with progressive ILD was corticosteroids in six patients and corticosteroids combined with immunosuppressants in two. At the end of the follow-up period myositis was diagnosed in 18 patients (56%) (8 in group A and 10 in group G). It was associated with muscle weakness in 3 patients. In one case, nuclear magnetic resonance data linked myositis to corticosteroid treatment (group G). We failed to identify a relationship between the initial level of CK, the evolution of myositis and the outcome of ILD. Adverse events associated with treatment Seventeen patients (54%) experienced severe adverse effects linked to treatment (corticosteroids and/or immunosuppressants). Severe documented infections were reported in 11 cases and caused the death of one patient. Eight of the 11 severe infections concerned herpes zoster virus. No case of pneumocystosis was identified, although only five patients were given prophylactic sulphamethoxazole-trimethoprim treatment. Other adverse effects included organ failure, requiring hospitalisation in nine cases. There was no difference in adverse effects between groups A and G. DISCUSSION This study describes 32 patients who presented with initial ILD and anti-jo-1 antibodies but who were not diagnosed as polymyositis or dermatomyositis at initial evaluation. This population of patients, who were referred to tertiary care centres for respiratory symptoms and who were treated for ILD according to international recommendations, was reasonably homogeneous, making it possible to evaluate the course of ILD and, in particular, the response to treatment under standard conditions. However, the study does have some limitations. Figure 2 High-resolution CT scan of the lung showing basal irregular lines and basal consolidations. Patients whose ILD developed before the possibility of detecting anti-jo-1 antibodies, or patients with anti-jo-1 antibodies and myositis treated before developing ILD, were not included in the study. However, patients with extrarespiratory symptoms such as myositis, arthralgia, Raynaud s phenomenon or skin lesions were not excluded from the study. In the anti-synthetase syndrome, respiratory involvement is associated with fever (87% cases), myositis (77 90%), arthritis (50 94%) and Raynaud s phenomenon (62 93%). Although ILD is a recognised manifestation of the antisynthetase syndrome, identified in 75 89% of cases in the principal studies, it remains poorly defined. Jo-1 antibodies directed against histidyl-trna synthetase account for about 80% of all cases of anti-synthetase syndrome 12 and are not tissue- or disease-specific However, there is a strong link between anti-jo-1 antibodies and ILD: 75% of patients with ILD and polymyositis/dermatomyositis in the study by Schnabel et al had anti-jo-1 antibodies. 7 ILD may be associated with anti-jo-1 antibodies as the sole clinical manifestation. Recent case reports have described ILD in patients with anti-jo-1 antibodies without myositis Santy et al 24 reported NSIP in lung biopsies with CD8+ lymphocytic alveolar inflammation and anti-jo-1 antibodies without myositis in 3 patients and Friedman et al 22 identified 10 patients with anti-synthetase antibodies (anti-pl-12, Jo-1 and OJ) with ILD and no myositis. These two studies highlight the possible association of anti-synthetase antibodies with ILD, independently or as the sole manifestation of the anti-synthetase syndrome. The absence of myositis in these cases, and in 63% and 44% of patients at initial presentation and during follow-up in our study, requires further elucidation. In cases of isolated ILD associated with anti-synthetase antibodies, we cannot exclude the possibility of subclinical muscle involvement, as previously described In some cases, myositis may have been prevented or controlled well enough by drugs to escape detection. In the absence of clinically or electromyographically apparent myositis, no muscle biopsy was performed. It was also difficult to identify myositis during the follow-up period when corticosteroid treatment may also have induced myopathy. The study by Schmidt et al 20 also confirms the diversity of the clinical manifestations associated with anti-jo-1 antibodies. In 18 patients the clinical presentation was arthritis in 15 cases, myositis in 14 and ILD in 14. Only 4 patients had myositis at disease onset. One bias may result from the fact that patients with arthralgia and ILD were more likely to have prompted 56 Thorax 2008;63: doi: /thx
5 Table 4 Comparison of high-resolution CT scan features on admission in groups A (n = 15) and G (n = 17) Characteristics serological evaluation, including anti-jo-1 antibodies, than patients presenting with isolated respiratory manifestations. Nevertheless, in the centres involved in the study, screening of patients for systemic disorders in cases of ILD was systematic at initial presentation. Indeed, it was noted that, upon admission, at least 9 patients (28%) had ILD without an increase in CK, myositis, arthralgia or cutaneous disorders. Within the population studied, 32% were smokers, a proportion similar to the 30% observed in the French general population. 34 Occupational exposure was identified in 39% of our patients and 26% of our population were employed in the cleaning industry. We cannot exclude the possibility that cleaning ladies exposed to abrasive agents may have developed pulmonary inflammation, as demonstrated in animal models Exposure to toxic substances such as polymerising epoxy resin in Japan 21 or silica 36 has been shown to be associated with dermatomyositis and muscle weakness. Further studies are required to evaluate the impact of inhaled irritants, particularly in cleaning products, in order to identify a possible causal link between this occupation and ILD. Our population also presented other connective tissue diseases and cancers. Overlap syndromes have been described in myositis. We identified patients with rheumatoid arthritis and Sjögren syndrome. None of our patients had Group A (n = 15) Group G (n = 17) p Value Location Predominantly subpleural NS Predominantly inferior Patterns evaluated by HRCT scan Ground-glass attenuation NS Basal consolidation Septal thickening 6 6 NS Irregular lines NS Traction bronchiectasis/ 2 5 NS bronchiolectasis Honeycombing 2 7 NS Others Pleural effusion 2 1 NS Adenopathy 2 1 NS HRCT scan associated Diffuse patchy ground glass opacities Basal irregular lines Basal consolidations Group A, acute onset of interstitial lung disease; group G, gradual onset of interstitial lung disease. Comparisons were made using the Fisher exact test. Figure 3 Percentage of lymphocytes, neutrophils and eosinophils in bronchoalveolar lavage (BAL) fluid in 25/32 patients at presentation. Group A, acute onset of interstitial lung disease; group G, gradual onset of interstitial lung disease. systemic sclerosis. Sjögren syndrome is commonly associated with anti-jo-1 antibodies, and anti-ssa antibodies are also associated with anti-jo-1 without sicca syndrome. In our study, autoantibodies were more likely to be associated with the gradual onset of ILD. Cancer was identified during the followup period in three cases (lung, ovaries and non-hodgkin lymphoma). Cancer is more frequent in cases of dermatomyositis than in the general population, and is slightly more frequent in cases of polymyositis, but no epidemiological association has been demonstrated between the anti-synthetase syndrome and cancer. One particular feature of ILD associated with anti-jo-1 antibodies was the high frequency of acute onset with fever and respiratory insufficiency reported in 47% of our patients on admission. Acute interstitial pneumonitis is a rare presentation of ILD, reported in dermatomyositis Clawsson et al reported acute interstitial pneumonitis in three cases at initial presentation and during the course of anti-synthetase syndrome. 42 ILD presenting with acute respiratory distress and fever may be due to infection (particularly pneumocystis), hypersensitivity pneumonitis (environmental or iatrogenic), alveolar haemorrhage and, on rare occasions, idiopathic acute fibrosis (initially described by Hamman-Rich). In cases of anti-synthetase syndrome with acute ILD, treatment with a high dose of corticosteroids (and other immunosuppressive drugs) is necessary to prevent rapid death due to respiratory insufficiency We conclude that anti-jo-1 antibodies should be sought and CK determined in cases of ILD with an acute presentation. In 80% of patients with an acute presentation and in 35% of patients with gradual onset, the HRCT scan showed bilateral abnormalities with subpleural predominance, diffuse patchy ground-glass attenuation, basal consolidations and basal irregular linear opacities, possibly corresponding to NSIP in some patients In the study by Marguerie et al, 29 pulmonary fibrosis was identified in 15 of 19 patients with anti-jo-1 anibodies; 16 of the 19 patients had myositis. Fibrosis was the term used to describe ILD and HRCT scans were not available at that time. Recent studies have described the pathology of the lung in myositis ILD in polymyositis/dermatomyositis is identified principally as NSIP In the acute presentation, DAD, fibrosis and COP have also been reported UIP has only rarely been reported In our series, lung biopsies Thorax 2008;63: doi: /thx
6 Table 5 Evaluation of therapeutic response at 3 months and 1 year (n = 32) Time Group Improvement Stable Treatment failure/death 3 months Group A (n = 15) 13 (87%)* 0 0/2 (13%) (9 CS; 4 CS+IS) (1 CS; CS+IS) Group G (n = 17) 9 (53%) 7 (41%) 1 (6%)/0 (6 CS; 3 CS+IS) (5 CS; 2 CS+IS) (1 CS) 1 year Group A (n = 13) 0 8 (62%) 5 (38%) (4CS; 4CS+IS) (5 CS) Group G (n = 17) 0 15 (88%) 2 (12%) (5 CS; 10 CS+IS) (2 CS+IS) Group A, acute onset of interstitial lung disease; group G, gradual onset of interstitial lung disease; CS, corticosteroids; IS, immunosuppressive drugs. *Significantly different (p = 0.008) from group G at 3 months (Fisher exact test). in 5 of the 11 cases confirmed the frequency of NSIP. In the other cases, particularly those with an acute presentation, no lung biopsy was performed for ethical reasons. The poorer prognosis for patients with anti-synthetase syndrome compared with those with myositis without autoantibodies has been found to be related to ILD. In myositis, Arsura et al 11 found that 40 60% of patients with myositis and ILD died within 5 years. Data suggest that a combination of prednisolone and cyclophosphamide may improve the outcome in cryptogenic fibrosing alveolitis and lung fibrosis associated with connective tissue disease The first-line treatment for ILD with Jo-1 antibodies is corticosteroids. In some cases an initial pulse of intravenous cyclophosphamide or a combination of a corticosteroid with azathioprine 2 has been reported to induce remission. Santy et al showed that better responses were obtained if patients with Jo-1-positive ILD were treated with a combination of prednisone, azathioprine and cyclosporine Nawata et al, 54 Takizawa et al 44 and Schnabel et al 7 also suggested that ILD was frequently corticosteroid-resistant in patients with dermatomyositis/polymyositis. Schnabel et al 7 found that disease progression was associated with increased CK levels at initial evaluation, which contrasted with the findings of Nawata et al 54 who showed that patients with normal CK levels had a poorer prognosis. In our study we failed to identify a relationship between a poor outcome of ILD and the presence of myositis or an increase in CK levels. In the studies by Nawata et al and Schnabel et al, patients were diagnosed as dermatomyositis or polymyositis before ILD and they did not focus on anti-jo-1 antibodies Figure 4 Comparison of total lung capacity (TLC), slow vital capacity (SVC) and carbon monoxide transfer factor (TLCO) in patients with stable interstitial lung disease (ILD; n = 17) and those with ILD progression (n = 8) at initial evaluation (open columns) and at the end of the follow-up period (solid columns). Results are expressed as median percentage of normal predicted value. Schnabel et al differentiated two forms of ILD associated with polymyositis/dermatomyositis: one with a progressive and the other with a non-progressive course. 7 Based on an evaluation of 10 patients with progressive ILD, he concluded that disease activity should be evaluated based on the presence of groundglass opacities on the HRCT scan and neutrophils in the BAL fluid. In those patients, an intravenous pulse of cyclophosphamide in combination with prednisolone seemed be more effective than corticosteroid alone. 7 In our study, 87% of patients in group A and 53% of patients in group G showed improvements in ILD at 3 months. Most of the patients in the two groups were treated with corticosteroid alone. Some of the patients in group A suffered respiratory failure after 1 year; most of those patients had been treated with corticosteroid alone. Thus, ILD, particularly with an acute presentation, responds to corticosteroids but relapses are not completely prevented by corticosteroid alone. In group G, fewer relapses were observed during the first year but most of the patients had already been treated with a combination of corticosteroids and immunosuppressants. At the end of the follow-up period, ILD was stable in 68% of our patients, with no difference between the two groups. However, by that time, most patients had been treated with a combination of corticosteroids and immunosuppressants. The outcome was poor in about one-third of patients who suffered severe respiratory insufficiency. At the end of the study a few patients remained stable on corticosteroid alone. In conclusion, ILD may be associated with anti-jo-1 antibodies as the sole clinically apparent manifestation and is characterised by a high frequency of acute onset associated with respiratory insufficiency, fever and specific HRCT scan patterns. 58 Thorax 2008;63: doi: /thx
7 The immediate response to corticosteroid alone was good, but recurrences frequently occurred. At the end of the study about two-thirds of patients had stable ILD, while the other third displayed progression with respiratory insufficiency. A combination of corticosteroid and immunosuppressant drugs was required to control ILD in most cases. Severe adverse effects of treatment were observed and infection with varicella zoster virus was frequent. Early testing for anti-synthetase antibodies, particularly anti-jo-1, and CK determination are useful investigations in patients presenting with ILD, particularly when the latter is associated with acute onset, fever, basal consolidations, basal irregular lines and diffuse patchy ground-glass opacities on the HRCT scan; 47% of the patients included in this study presented with such a combination of signs. A prospective evaluation of patients with ILD is required to establish the true frequency of anti-jo-1 antibodies in idiopathic ILD. Competing interests: None. REFERENCES 1. Cottin V, Thivolet-Bejui F, Reynaud-Gaubert M, et al. Interstitial lung disease in amyopathic dermatomyositis, dermatomyositis and polymyositis. Eur Respir J 2003;22: Douglas WW, Tazelaar HD, Hartman TE, et al. Polymyositis-dermatomyositisassociated interstitial lung disease. Am J Respir Crit Care Med 2001;164: Fathi M, Dastmalchi M, Rasmussen E, et al. Interstitial lung disease, a common manifestation of newly diagnosed polymyositis and dermatomyositis. Ann Rheum Dis 2004;63: Grau JM, Miro O, Pedrol E, et al. Interstitial lung disease related to dermatomyositis. Comparative study with patients without lung involvement. J Rheumatol 1996;23: Kurasawa K, Nawata Y, Takabayashi K, et al. Activation of pulmonary T cells in corticosteroid-resistant and -sensitive interstitial pneumonitis in dermatomyositis/ polymyositis. Clin Exp Immunol 2002;129: Marie I, Hachulla E, Cherin P, et al. Interstitial lung disease in polymyositis and dermatomyositis. Arthritis Rheum 2002;47: Schnabel A, Reuter M, Biederer J, et al. Interstitial lung disease in polymyositis and dermatomyositis: clinical course and response to treatment. Semin Arthritis Rheum 2003;32: Schwartz MI. The lung in polymyositis. Clin Chest Med 1998;19: Schwartz MI, Matthay RA, Sahn SA, et al. Interstitial lung disease in polymyositis and dermatomyositis: analysis of six cases and review of the literature. Medicine 1976;55: Tazelaar HD, Viggiano RW, Pickersgill J, et al. Interstitial lung disease in polymyositis and dermatomyositis. Am Rev Respir Dis 1990;141: Arsura EL, Greenberg AS. Adverse impact of interstitial pulmonary fibrosis on prognosis in polymyositis and dermatopolymyositis. Semin Arthritis Rheum 1988;18: Dalakas MC. Polymyositis and dermatomyositis. Lancet 2003;362: Marie I, Hachulla E, Hatron PY. Polymyositis and dermatomyositis: short term and longterm outcome, and predictive factors of prognosis. J Rheumatol 2001;28: Spath M, Schroder M, Schlotter-Weigel B, et al. The long-term outcome of anti-jo- 1-positive inflammatory myopathies. J Neurol 2004;251: Sultan SM, Ioannou Y, Moss K, et al. Outcome in patients with idiopathic inflammatory myositis: morbidity and mortality. Rheumatology 2002;41: Arnett FC, Hirsch TJ, Bias WB, et al. The Jo-1 antibody system in myositis: relationships to clinical features and HLA. J Rheumatol 1981;8: Bernstein RM, Morgan SH, Chapman J, et al. Anti-Jo-1 antibody: a marker for myositis with interstitial lung disease. BMJ (Clin Res Ed) 1984;289: Hochberg MC, Feldman D, Stevens MB, et al. Antibody to Jo-1 in polymyositis/ dermatomyositis: association with interstitial pulmonary disease. J Rheumatol 1984;11: Love LA, Leff R, Fraser DD, et al. A new approach to the classification of idiopathic inflammatory myopathy: myositis-specific autoantibodies define useful homogeneous patient groups. Medicine (Baltimore) 1991;70: Schmidt WA, Wetzel W, Friedlander R, et al. Clinical and serological aspects of patients with anti-jo-1 antibodies: an evolving spectrum of disease manifestations. Clin Rheumatol 2000;19: Yamakage A, Ishikawa H, Saito Y, et al. Occupational Scleroderma-like disorder occurring in men engaged in the polymerization of epoxy resins. Dermatologica 1980;161: Friedman AW, Targoff IN, Arnett FC. Interstitial lung disease with autoantibodies against aminoacyl-trna synthetases in the absence of clinically apparent myositis. Semin Arthritis Rheum 1996;26: Kinebuchi S, Mizuno K, Moriyama H, et al. Two cases of interstitial pneumonia with anti-jo-1 antibodies in the absence of myositis. Nihon Kokyuki Gakkai Zasshi 2003;41: Sauty A, Rochat T, Schoch OD, et al. Pulmonary fibrosis with predominant CD8 lymphocytic alveolitis and anti-jo-1 antibodies. Eur Respir J 1997;10: American Thoracic Society/European Respiratory Society. International Multidisciplinary Consensus Classification of the Idiopathic Interstitial Pneumonias. Am J Respir Crit Care Med 2002;165: BAL Cooperative Group Steering Committee. Am Rev Respir Dis 1990;141:S American Thoracic Society. Consensus. Idiopathic pulmonary fibrosis: diagnosis and treatment. International consensus statement. Am J Respir Crit Care Med 2000;161: Hengstman GJ, van Engelen BG, van Venrooij WJ. Myositis-specific autoantibodies: changing insights in pathophysiology and clinical associations. Curr Opin Rheumatol 2004;16: Marguerie C, Bunn CC, Beynon HLC, et al. Polymyositis, pulmonary fibrosis and autoantibodies to aninoacyl-trna synthase enzymes. Q J Med 1990;282: Kashiwabara K, Ota K. Rapidly progressive interstitial lung disease in a dermatomyositis patient with high levels of creatine phosphokinase, severe muscle symptoms and positive anti-jo-1 antibody. Intern Med 2002;41: Mathews MB, Bernstein RM. Myositis autoantibody inhibits histidyl-trna synthetase: a model for autoimmunity. Nature 1983;304: Nishikai M, Reichlin M. Heterogeneity of precipitating antibodies in polymyositis and dermatomyositis. Characterization of the Jo-1 antibody system. Arthritis Rheum 1980;23: Otero C, Illa I, Dalakas MC. Is there dermatomyositis without myositis? Neurology 1992;42: Le Faou AL, Scemama O. Epidemiology of tobacco smoking. Rev Mal Respir 2005;22:8S Hubbs A, Greskevitch M, Kuempel E, et al. Abrasive blasting agents: designing studies to evaluate relative risk. J Toxicol Environ Health A 2005;68: Love LA, Miller FW. Noninfectious environmental agents associated with myopathies. Curr Opin Rheum 1993;5: Serratrice J, Granel B, Pache X, et al. A case of polymyositis with anti-histidyl-t- RNA synthetase (Jo-1) antibody syndrome following extensive vinyl chloride exposure. Clin Rheumatol 2001;20: Brouwer R, Hengstman GJ, Vree Egberts W, et al. Autoantibody profiles in the sera of European patients with myositis. Ann Rheum Dis 2001;60: Troyanov Y, Targoff IN, Tremblay JL, et al. Novel classification of idiopathic inflammatory myopathies based on overlap syndrome features and autoantibodies: analysis of 100 French Canadian patients. Medicine (Baltimore) 2005;84: Hill CL, Zhang Y, Sigurgeirsson B. Frequency of specific cancer types in dermatomyositis or polymyositis: a population-based study. Lancet 2001;357: Ito M, Kaise S, Suzuki S, et al. Clinico-laboratory characteristics of patients with dermatomyositis accompanied by rapidly progressive interstitial lung disease. Clin Rheumatol 1999;18: Clawson K, OddisC. Adult respiratory distress syndrome in polymyositis patients with the anti Jo-1 antibody. Arthritis Rheum 1995;38: Temmesfeld-Wollbruck B, Morr H, Suttorp N, et al. Three cases of a fulminant course of idiopathic pulmonary fibrosis (Hamman-Rich syndrome). Pneumologie 1993;47: Takizawa H, Shiga J, Moroi Y, et al. Interstitial lung disease in dermatomyositis: clinicopathological study. J Rheumatol 1987;14: Akira M, Hara H, Sakatani M. Interstitial lung disease in association with polymyositis-dermatomyositis: long-term follow-up CT evaluation in seven patients. Radiology 1999;210: Veeraraghavan S, Latsi PI, Wells AU, et al. BAL findings in idiopathic nonspecific interstitial pneumonia and usual interstitial pneumonia. Eur Respir J 2003;22: Raghu G, Mageto YN, Lockhart D, et al. The accuracy of the clinical diagnosis of new-onset idiopathic pulmonary fibrosis and other interstitial lung disease: a prospective study. Chest 1999;116: Johnson MA, Kwan S, Snell NJ, et al. Randomised controlled trial comparing prednisolone alone with cyclophosphamide and low dose prednisolone in combination in cryptogenic fibrosing alveolitis. Thorax 1989;44: Tanaka F, Origuchi T, Migita K, et al. Successful combined therapy of cyclophosphamide and cyclosporine for acute exacerbated interstitial pneumonia associated with dermatomyositis. Intern Med 2000;39: Yoshida T, Koga H, Saitoh F, et al. Pulse intravenous cyclophosphamide treatment for steroid-resistant interstitial pneumonitis associated with polymyositis. Intern Med 1999;38: Dalakas MC. Therapeutic approach in patients with inflammatory myopathies. Semin Neurol 2003;23: Schnabel A, Reuter M, Gross WL. Intravenous pulse cyclophosphamide in the treatment of interstitial lung disease due to collagen vascular diseases. Arthritis Rheum 1998;41: Dawson JK, Abernethy VE, Lynch MP. Effective treatment of anti Jo-1 antibodypositive polymyositis with cyclosporin. Br J Rheumatol 1997;36: Nawata Y, Kurasawa K, Takabayashi K, et al. Corticosteroid resistant interstitial pneumonitis in dermatomyositis/polymyositis: prediction and treatment with cyclosporine. J Rheumatol 1999;26: Thorax 2008;63: doi: /thx
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
PL-7 and Anti-Jo-1 Antibodies. publication is available at link.sp
 NAOSITE: Nagasaki University's Ac Title Author(s) Comparison of Pulmonary Involvement PL-7 and Anti-Jo-1 Antibodies Tomonaga, Masaomi; Sakamoto, Noriho Tomoyuki; Harada, Tatsuhiko; Nakash Shintaro; Horai,
NAOSITE: Nagasaki University's Ac Title Author(s) Comparison of Pulmonary Involvement PL-7 and Anti-Jo-1 Antibodies Tomonaga, Masaomi; Sakamoto, Noriho Tomoyuki; Harada, Tatsuhiko; Nakash Shintaro; Horai,
Clinical Differences Between Interstitial Lung Disease Associated With Clinically Amyopathic Dermatomyositis and Classic Dermatomyositis
 CHEST Clinical Differences Between Interstitial Lung Disease Associated With Clinically Amyopathic Dermatomyositis and Classic Dermatomyositis Hiroshi Mukae, MD, PhD; Hiroshi Ishimoto, MD; Noriho Sakamoto,
CHEST Clinical Differences Between Interstitial Lung Disease Associated With Clinically Amyopathic Dermatomyositis and Classic Dermatomyositis Hiroshi Mukae, MD, PhD; Hiroshi Ishimoto, MD; Noriho Sakamoto,
Interstitial lung disease in patients with polymyositis, dermatomyositis and amyopathic dermatomyositis
 Rheumatology Advance Access published June 21, 2005 Rheumatology 2005; 1 of 5 doi:10.1093/rheumatology/keh723 Concise Report Interstitial lung disease in patients with polymyositis, dermatomyositis and
Rheumatology Advance Access published June 21, 2005 Rheumatology 2005; 1 of 5 doi:10.1093/rheumatology/keh723 Concise Report Interstitial lung disease in patients with polymyositis, dermatomyositis and
IPF: Epidemiologia e stato dell arte
 IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION!
 UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Interstitial lung diseases associated with amyopathic dermatomyositis
 Eur Respir J 2006; 28: 1005 1012 DOI: 10.1183/09031936.06.00038806 CopyrightßERS Journals Ltd 2006 Interstitial lung diseases associated with amyopathic dermatomyositis T. Suda*, T. Fujisawa*, N. Enomoto*,
Eur Respir J 2006; 28: 1005 1012 DOI: 10.1183/09031936.06.00038806 CopyrightßERS Journals Ltd 2006 Interstitial lung diseases associated with amyopathic dermatomyositis T. Suda*, T. Fujisawa*, N. Enomoto*,
Comparison of clinical course of polymyositis and dermatomyositis :a follow-up study in Tokushima University
 9 ORIGINAL Comparison of clinical course of polymyositis and dermatomyositis :a follow-up study in Tokushima University Hospital Kenji Tani, Reiko Tomioka,KeikoSato, Chiyuki Furukawa, Takeshi Nakajima,
9 ORIGINAL Comparison of clinical course of polymyositis and dermatomyositis :a follow-up study in Tokushima University Hospital Kenji Tani, Reiko Tomioka,KeikoSato, Chiyuki Furukawa, Takeshi Nakajima,
IPF - Inquadramento clinico
 IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation of an Antisynthetase Syndrome
 CASE REPORT http://dx.doi.org/10.4046/trd.2016.79.3.188 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:188-192 Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation
CASE REPORT http://dx.doi.org/10.4046/trd.2016.79.3.188 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:188-192 Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Usual interstitial pneumonia in rheumatoid arthritis-associated interstitial lung disease
 Eur Respir J 2010; 35: 1322 1328 DOI: 10.1183/09031936.00092309 CopyrightßERS 2010 Usual interstitial pneumonia in rheumatoid arthritis-associated interstitial lung disease E.J. Kim*, B.M. Elicker #, F.
Eur Respir J 2010; 35: 1322 1328 DOI: 10.1183/09031936.00092309 CopyrightßERS 2010 Usual interstitial pneumonia in rheumatoid arthritis-associated interstitial lung disease E.J. Kim*, B.M. Elicker #, F.
A case of a patient with IPF treated with nintedanib. Prof. Kreuter and Prof. Heussel
 A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
International consensus statement on idiopathic pulmonary fibrosis
 Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates
 Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia. Nitra and the Gangs.
 Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
Key words: CT scanners; interstitial lung diseases; polymyositis-dermatomyositis; x-ray
 Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Pulmonary fibrosis with predominant CD8 lymphocytic alveolitis and anti-jo-1 antibodies
 Eur Respir J 1997; 10: 2907 2912 DOI: 10.1183/09031936.97.10122907 Printed in UK all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903 1936 CASE STUDY Pulmonary fibrosis
Eur Respir J 1997; 10: 2907 2912 DOI: 10.1183/09031936.97.10122907 Printed in UK all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903 1936 CASE STUDY Pulmonary fibrosis
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
I n 2002 the American Thoracic Society (ATS) and
 1008 REVIEW SERIES Challenges in pulmonary fibrosis? 5: The NSIP/UIP debate Roland du Bois, Talmadge E King Jr... Among the idiopathic interstitial s, the two entities idiopathic pulmonary fibrosis (IPF)
1008 REVIEW SERIES Challenges in pulmonary fibrosis? 5: The NSIP/UIP debate Roland du Bois, Talmadge E King Jr... Among the idiopathic interstitial s, the two entities idiopathic pulmonary fibrosis (IPF)
Manish Powari Regional Training Day 10/12/2014
 Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Interstitial Lung Disease in Polymyositis and Dermatomyositis
 Arthritis & Rheumatism (Arthritis Care & Research) Vol. 47, No. 6, December 15, 2002, pp 614 622 DOI 10.1002/art.10794 2002, American College of Rheumatology ORIGINAL ARTICLE Interstitial Lung Disease
Arthritis & Rheumatism (Arthritis Care & Research) Vol. 47, No. 6, December 15, 2002, pp 614 622 DOI 10.1002/art.10794 2002, American College of Rheumatology ORIGINAL ARTICLE Interstitial Lung Disease
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines
 Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Diagnosing Idiopathic Pulmonary Fibrosis on Evidence-Based Guidelines Rebecca Keith, MD Assistant Professor, Division of Pulmonary and Critical Care Medicine National Jewish Health, Denver, CO Objectives
Non-neoplastic Lung Disease II
 Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
CASE REPORT. Introduction. Case Report
 doi: 10.2169/internalmedicine.9553-17 http://internmed.jp CASE REPORT Successful Treatment of Rapidly Progressive Unclassifiable Idiopathic Interstitial Pneumonia with Anti-melanoma Differentiation-associated
doi: 10.2169/internalmedicine.9553-17 http://internmed.jp CASE REPORT Successful Treatment of Rapidly Progressive Unclassifiable Idiopathic Interstitial Pneumonia with Anti-melanoma Differentiation-associated
Clinical Study A Clinical Analysis of Risk Factors for Interstitial Lung Disease in Patients with Idiopathic Inflammatory Myopathy
 Clinical and Developmental Immunology Volume 2013, Article ID 648570, 4 pages http://dx.doi.org/10.1155/2013/648570 Clinical Study A Clinical Analysis of Risk Factors for Interstitial Lung Disease in Patients
Clinical and Developmental Immunology Volume 2013, Article ID 648570, 4 pages http://dx.doi.org/10.1155/2013/648570 Clinical Study A Clinical Analysis of Risk Factors for Interstitial Lung Disease in Patients
Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment
 Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
P olymyositis (PM) and dermatomyositis (DM) are systemic
 297 EXTENDED REPORT Interstitial lung disease, a common manifestation of newly diagnosed polymyositis and dermatomyositis M Fathi, M Dastmalchi, E Rasmussen, I E Lundberg, G Tornling... See end of article
297 EXTENDED REPORT Interstitial lung disease, a common manifestation of newly diagnosed polymyositis and dermatomyositis M Fathi, M Dastmalchi, E Rasmussen, I E Lundberg, G Tornling... See end of article
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW
 SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome
 doi: 10.2169/internalmedicine.8955-17 http://internmed.jp CASE REPORT The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome Yoshimasa Hachisu 1, Yasuhiko Koga 1, Noriaki Sunaga 1,2, Chiharu
doi: 10.2169/internalmedicine.8955-17 http://internmed.jp CASE REPORT The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome Yoshimasa Hachisu 1, Yasuhiko Koga 1, Noriaki Sunaga 1,2, Chiharu
Test Name Results Units Bio. Ref. Interval
 LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
Clinical significance of serum surfactant protein D (SP-D) in patients with polymyositisudermatomyositis: correlation with interstitial lung disease
 Rheumatology 2002;41:1268 1272 Clinical significance of serum surfactant protein D (SP-D) in patients with polymyositisudermatomyositis: correlation with interstitial lung disease H. Ihn, Y. Asano, M.
Rheumatology 2002;41:1268 1272 Clinical significance of serum surfactant protein D (SP-D) in patients with polymyositisudermatomyositis: correlation with interstitial lung disease H. Ihn, Y. Asano, M.
Evidence Review: Title. Month/ Year. Evidence Review:
 Evidence Review: Title Month/ Year Evidence Review: Rituximab for connective tissue disease associated interstitial lung disease October 2014 Standard Operating Procedure: NHS England Evidence Review:
Evidence Review: Title Month/ Year Evidence Review: Rituximab for connective tissue disease associated interstitial lung disease October 2014 Standard Operating Procedure: NHS England Evidence Review:
An earlier and more confident diagnosis of idiopathic pulmonary fibrosis
 Eur Respir Rev 2012; 21: 124, 141 146 DOI: 10.1183/09059180.00000812 CopyrightßERS 2012 REVIEW: IPF An earlier and more confident diagnosis of idiopathic pulmonary fibrosis Roland M. du Bois ABSTRACT:
Eur Respir Rev 2012; 21: 124, 141 146 DOI: 10.1183/09059180.00000812 CopyrightßERS 2012 REVIEW: IPF An earlier and more confident diagnosis of idiopathic pulmonary fibrosis Roland M. du Bois ABSTRACT:
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
Pathologic Assessment of Interstitial Lung Disease
 Pathologic Assessment of Interstitial Lung Disease Dry and itchy? It could be eczema or fungal infection. We don t need to worry, the drugs aren t that dangerous. Kirk D. Jones, MD UCSF Dept. of Pathology
Pathologic Assessment of Interstitial Lung Disease Dry and itchy? It could be eczema or fungal infection. We don t need to worry, the drugs aren t that dangerous. Kirk D. Jones, MD UCSF Dept. of Pathology
Epidemiology and classification of smoking related interstitial lung diseases
 Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
Disclosures. Clinical Approach: Evaluating CTD-ILD for the pulmonologist. ILD in CTD. connective tissue disease or collagen vascular disease
 Disclosures Clinical Approach: Evaluating CTD-ILD for the pulmonologist Industry relationships: Actelion, atyr Pharma, Boehringer-Ingelheim, Genentech- Roche, Gilead Aryeh Fischer, MD Associate Professor
Disclosures Clinical Approach: Evaluating CTD-ILD for the pulmonologist Industry relationships: Actelion, atyr Pharma, Boehringer-Ingelheim, Genentech- Roche, Gilead Aryeh Fischer, MD Associate Professor
Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia
 Respiratory Medicine (2005) 99, 234 240 Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia Jiro Fujita a,, Yuji Ohtsuki b, Takeo Yoshinouchi c, Ichiro Yamadori d, Shuji
Respiratory Medicine (2005) 99, 234 240 Idiopathic non-specific interstitial pneumonia: as an autoimmune interstitial pneumonia Jiro Fujita a,, Yuji Ohtsuki b, Takeo Yoshinouchi c, Ichiro Yamadori d, Shuji
Rapidly Progressive Pulmonary Fibrosis Following the Onset of Diffuse Alveolar Hemorrhage in Sjögren s Syndrome: An Autopsy Case Report
 CASE REPORT Rapidly Progressive Pulmonary Fibrosis Following the Onset of Diffuse Alveolar Hemorrhage in Sjögren s Syndrome: An Autopsy Case Report Yusuke Tomita 1,2, Shunsuke Mori 3, Nobuyuki Arima 4,
CASE REPORT Rapidly Progressive Pulmonary Fibrosis Following the Onset of Diffuse Alveolar Hemorrhage in Sjögren s Syndrome: An Autopsy Case Report Yusuke Tomita 1,2, Shunsuke Mori 3, Nobuyuki Arima 4,
Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases
 CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas
 Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas Rishi Raj MD Director, Interstitial Lung Diseases Program Clinical Professor of Pulmonary and Critical Care Medicine Stanford University
Hypersensitivity Pneumonitis Common Diagnostic and Treatment Dilemmas Rishi Raj MD Director, Interstitial Lung Diseases Program Clinical Professor of Pulmonary and Critical Care Medicine Stanford University
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS
 USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
In medicine, the term overlap is very common, to the extent that there is even a
 Case Report Payam Mehrian (MD) 1 Ali Cheraghvandi (MD) 2 Atousa Droudnia (PhD) 3 Firouzeh Talischi (MD) 4 Saeid Fallah Tafti (MD) *5 Shahram Kahkouee (MD) 6 Hamidreza Jamaati (MD) 7 1. Pediatric Respiratory
Case Report Payam Mehrian (MD) 1 Ali Cheraghvandi (MD) 2 Atousa Droudnia (PhD) 3 Firouzeh Talischi (MD) 4 Saeid Fallah Tafti (MD) *5 Shahram Kahkouee (MD) 6 Hamidreza Jamaati (MD) 7 1. Pediatric Respiratory
Disclosures. Fibrotic lung diseases: Basic Principles, Common Problems, and Reporting. Relevant financial relationships: None. Off-label usage: None
 Fibrotic lung diseases: Basic Principles, Common Problems, and Reporting Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona
Fibrotic lung diseases: Basic Principles, Common Problems, and Reporting Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona
Test Name Results Units Bio. Ref. Interval
 135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
Progress in Idiopathic Pulmonary Fibrosis
 Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis
 Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
Prognostic Significance of Histopathologic Subsets in Idiopathic Pulmonary Fibrosis JULIE A. BJORAKER, JAY H. RYU, MARK K. EDWIN, JEFFREY L. MYERS, HENRY D. TAZELAAR, DARRELL R. SCHROEDER, and KENNETH
Citation Clinical rheumatology (2011), 30(3)
 A case of antisynthetase syndrome i Titlepatient with anti-pl-12 antibody fo etanercept. Ishikawa, Yuki; Yukawa, Naoichiro; Author(s) Ohmura, Koichiro; Fujii, Takao; Usu Tsuneyo Citation Clinical rheumatology
A case of antisynthetase syndrome i Titlepatient with anti-pl-12 antibody fo etanercept. Ishikawa, Yuki; Yukawa, Naoichiro; Author(s) Ohmura, Koichiro; Fujii, Takao; Usu Tsuneyo Citation Clinical rheumatology
Clinical and Pathological Findings of Interstitial Lung Disease Patients with Anti-Aminoacyl-tRNA Synthetase Autoantibodies
 ORIGINAL ARTICLE Clinical and Pathological Findings of Interstitial Lung Disease Patients with Anti-Aminoacyl-tRNA Synthetase Autoantibodies Yoshimizu Koreeda 1, Ikkou Higashimoto 1, Masuki Yamamoto 1,
ORIGINAL ARTICLE Clinical and Pathological Findings of Interstitial Lung Disease Patients with Anti-Aminoacyl-tRNA Synthetase Autoantibodies Yoshimizu Koreeda 1, Ikkou Higashimoto 1, Masuki Yamamoto 1,
Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy
 Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy Jeff Swigris, DO, MS Director, ILD Program National Jewish Health Disclosures Speaker - Boehringer Ingelheim and Genentech Objectives Describe
Overview of Idiopathic Pulmonary Fibrosis: Diagnosis and Therapy Jeff Swigris, DO, MS Director, ILD Program National Jewish Health Disclosures Speaker - Boehringer Ingelheim and Genentech Objectives Describe
Annual Rheumatology & Therapeutics Review for Organizations & Societies
 Annual Rheumatology & Therapeutics Review for Organizations & Societies A Rheumatologist s Approach to Interstitial Lung Disease Outline ILD classification and patterns in CTD The clinical landscape and
Annual Rheumatology & Therapeutics Review for Organizations & Societies A Rheumatologist s Approach to Interstitial Lung Disease Outline ILD classification and patterns in CTD The clinical landscape and
UIP Possibile e Probabile
 UIP Possibile e Probabile Sergio Harari U.O. di Pneumologia e UTIR Servizio di Emodinamica e Fisiopatologia Respiratoria Ospedale San Giuseppe - Milano Current definition of IPF IPF is a distinct type
UIP Possibile e Probabile Sergio Harari U.O. di Pneumologia e UTIR Servizio di Emodinamica e Fisiopatologia Respiratoria Ospedale San Giuseppe - Milano Current definition of IPF IPF is a distinct type
Challenges in the Diagnosis of Interstitial Lung Disease
 Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after smoking cessation
 Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
T he diagnostic evaluation of a patient with
 546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
Limitations of Corticosteroids and Cytotoxic Agents in Treating Idiopathic Pulmonary Fibrosis
 Idiopathic Pulmonary Fibrosis Limitations of Corticosteroids and Cytotoxic Agents in Treating Idiopathic Pulmonary Fibrosis JMAJ 46(11): 475 482, 2003 Kingo CHIDA Associate Professor, Second Division,
Idiopathic Pulmonary Fibrosis Limitations of Corticosteroids and Cytotoxic Agents in Treating Idiopathic Pulmonary Fibrosis JMAJ 46(11): 475 482, 2003 Kingo CHIDA Associate Professor, Second Division,
Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
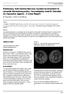 ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
Patient with FVC>90% predicted. Demosthenes Bouros, Vasilios Tzilas University of Athens
 Patient with FVC>90% predicted Demosthenes Bouros, Vasilios Tzilas University of Athens CASE OVERVIEW A 63-year-old, male patient with progressive exertional dyspnoea lasting for 2 years and dry cough
Patient with FVC>90% predicted Demosthenes Bouros, Vasilios Tzilas University of Athens CASE OVERVIEW A 63-year-old, male patient with progressive exertional dyspnoea lasting for 2 years and dry cough
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
Common things are common, but not always the answer
 Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Idiopathic inflammatory myopathies and the lung
 EUROPEAN RESPIRATORY UPDATE IDIOPATHIC INFLAMMATORY MYOPATHIES Idiopathic inflammatory myopathies and the lung Jean-Christophe Lega 1,2, Quitterie Reynaud 1, Alexandre Belot 3, Nicole Fabien 4, Isabelle
EUROPEAN RESPIRATORY UPDATE IDIOPATHIC INFLAMMATORY MYOPATHIES Idiopathic inflammatory myopathies and the lung Jean-Christophe Lega 1,2, Quitterie Reynaud 1, Alexandre Belot 3, Nicole Fabien 4, Isabelle
9/15/11. Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September Scleroderma. Hard skin
 Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September 2011 Scleroderma Hard skin 1 No diagnostic test for scleroderma Pathogenesis is unknown prominent features of disease reflect
Dr. Vivien Hsu Director, UMDNJ Scleroderma Program New Brunswick, NJ September 2011 Scleroderma Hard skin 1 No diagnostic test for scleroderma Pathogenesis is unknown prominent features of disease reflect
Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan
 CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
Chest imaging II. Interstitial lung diseases
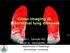 Chest imaging II. Interstitial lung diseases Dávid L. Tárnoki MD, PhD Ádám D. TárnokiMD, PhD Department of Radiology Semmelweis University Topics 1. Interstitial lung diseases 2. Occupational lung diseases
Chest imaging II. Interstitial lung diseases Dávid L. Tárnoki MD, PhD Ádám D. TárnokiMD, PhD Department of Radiology Semmelweis University Topics 1. Interstitial lung diseases 2. Occupational lung diseases
Case 1 : Question. 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random
 Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
Tools to Aid in the Accurate Diagnosis of. Connective Tissue Disease
 Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
Anti-synthetase syndrome
 Anti-synthetase syndrome Floranne C. Ernste, M.D. The Myositis Association Annual Conference Louisville, KY September 7, 2018 2017 MFMER slide-1 Disclosures Octapharma: clinical trial support Genentech:
Anti-synthetase syndrome Floranne C. Ernste, M.D. The Myositis Association Annual Conference Louisville, KY September 7, 2018 2017 MFMER slide-1 Disclosures Octapharma: clinical trial support Genentech:
Challenges in the Diagnosis of Interstitial Lung Disease
 Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
Challenges in the Diagnosis of Interstitial Lung Disease Kirk D. Jones, MD UCSF Dept. of Pathology kirk.jones@ucsf.edu Overview New Classification of IIP Prior classification Modifications for new classification
The connective tissue disorders (CTDs), also. Pivotal clinical dilemmas in collagen vascular diseases associated with interstitial lung involvement
 Eur Respir J 2009; 33: 882 896 DOI: 10.1183/09031936.00152607 CopyrightßERS Journals Ltd 2009 REVIEW Pivotal clinical dilemmas in collagen vascular diseases associated with interstitial lung involvement
Eur Respir J 2009; 33: 882 896 DOI: 10.1183/09031936.00152607 CopyrightßERS Journals Ltd 2009 REVIEW Pivotal clinical dilemmas in collagen vascular diseases associated with interstitial lung involvement
Rapidly Progressive Interstitial Lung Disease in a
 CASE REPORT Rapidly Progressive Interstitial Lung Disease in a Dermatomyositis Patient with High Levels of Creatine Phosphokinase, Severe Muscle Symptomsand Positive Anti-Jo-1 Antibody Kosuke Kashiwabara
CASE REPORT Rapidly Progressive Interstitial Lung Disease in a Dermatomyositis Patient with High Levels of Creatine Phosphokinase, Severe Muscle Symptomsand Positive Anti-Jo-1 Antibody Kosuke Kashiwabara
CLEARING THE AIR ON DIFFUSE PARENCHYMAL (INTERSTITIAL) LUNG DISEASE (ILD)
 CLEARING THE AIR ON DIFFUSE PARENCHYMAL (INTERSTITIAL) LUNG DISEASE (ILD) David Northrop MBA, RRT Assistant Director of Respiratory Therapy Services The University of Kansas Health System Clinical Assistant
CLEARING THE AIR ON DIFFUSE PARENCHYMAL (INTERSTITIAL) LUNG DISEASE (ILD) David Northrop MBA, RRT Assistant Director of Respiratory Therapy Services The University of Kansas Health System Clinical Assistant
Imaging: how to recognise idiopathic pulmonary fibrosis
 REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
HRCT in Diffuse Interstitial Lung Disease Steps in High Resolution CT Diagnosis. Where are the lymphatics? Anatomic distribution
 Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy
 Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
Overview of Diagnostic Autoantibodies in Inflammatory Myopathy Minoru Satoh, M.D., Ph.D. Research Associate Professor of Medicine Division of Rheumatology and Clinical Immunology University of Florida
Radiological Imaging of Drug-Induced Pulmonary Lesions
 Review Article imedpub Journals www.imedpub.com Journal of Clinical Radiology and Case Reports Radiological Imaging of Drug-Induced Pulmonary Lesions D souza M *, Rajiah P, Khan A and Irion K Department
Review Article imedpub Journals www.imedpub.com Journal of Clinical Radiology and Case Reports Radiological Imaging of Drug-Induced Pulmonary Lesions D souza M *, Rajiah P, Khan A and Irion K Department
