Cell Disease. Dr SM Donohue. Consultant Haematologist. Clinical Haematology
|
|
|
- Reginald Lucas
- 5 years ago
- Views:
Transcription
1 Full Title of Guideline: Guideline for Management of Acute Sickle Cell Disease. Author (include and role): Dr Consultant Haematologist Division & Speciality: Clinical Haematology Version: 2 Ratified by: Clinical Haematology Governance Scope (Target audience, For all staff working with acute problems state if Trust wide): related directly to sickle cell patients Review date (when this October 2020 version goes out of date): Explicit definition of patient group to which it applies All adult patients with acute problems directly related to sickle cell disease. (e.g. inclusion and exclusion criteria, diagnosis): Changes from previous N/A version (not applicable if this is a new guideline, enter below if extensive): Summary of evidence base this guideline has been created from: Based on Standards of care for adults with Sickle Cell Disease in preparation. This guideline has been registered with the trust. However, clinical guidelines are guidelines only. The interpretation and application of clinical guidelines will remain the responsibility of the individual clinician. If in doubt contact a senior colleague or expert. Caution is advised when using guidelines after the review date or outside of the Trust.
2 Table of Contents 1 Background Common presentations Arrangements for admission at NUH (adults) Assessment and initial management of patient with sickle cell disease Pain Areas of concern Pain management after first 90 minutes Alternative analgesics to consider Investigations Alteration of dose of analgesia Oxygen Thromboprophylaxis Antibiotics Transfusions Exchange Transfusion Other acute presentation Acute chest syndrome Clinical features Diagnosis Differential diagnosis Management Abdominal pain Differential diagnosis Clinical findings Investigations Management Priapism Management Osteomyelitis Acute stroke Acute anaemia Acute sequestration Haematuria Page 2 of 29 Lead Author: Submission Date: October 2017 Review Date: October 2020
3 11.9 Acute visual loss Patients reporting acute visual loss should be advised to attend the emergency ophthalmology clinic at QMC (close to A+E and with extended evening opening hours and at weekend) References Appendix 1 UHL Management of Painful Sickle Cell Crisis flow chart 18 Appendix 2 Acute Painful sickle cell crisis medical management in first 60minutes Appendix 3 Acute Painful Sickle Cell Crisis nursing management in first 60 minutes Appendix 4 Example of sickle cell disease admission document Appendix 5 Sickle Cell Crisis Pathway Appendix 6 Quick Reference Guide Lead Author: Submission Date: October 2017 Review Date: October 2020 Page 3 of 29
4 Guideline for Adults with Sickle Cell Disease: acute presentation 1 Background Sickle cell disease affects up to 15,000 people in the UK. Many of these patients will present acutely to a variety of hospitals in the country and may not be known already to staff at the hospital. Sickle cell disease (either HbSS or compound heterozygote states Hb SC, HbS/B-thalassaemia or other compound states) commonly gives rise to acute painful crises. The pain may occur in any part of the body but is commonly in the limbs. Pain in chest or abdomen should prompt consideration of alternative causes of pain in those sites (e.g. MI, acute appendicitis) but sickle cell pain is still the most likely cause. Sickle pain is very severe usually requiring opiate analgesia, may have a pain score of up to 10/10 and it is usually clear to the patient that this is their usual sickle pain (i.e. patients with sickle cell disease are the experts in their painful crises). The pathogenesis of sickle cell pain is thought to be due to deoxygenated sickle Hb forming large polymers which cause red cells to become deformed and irreversibly sickled leading to small vessel obstruction. Triggering factors are cold, dehydration and infection but often no specific trigger is found. 2 Common presentations severe pain pyrexia, tachycardia, tachypnoea, hypotension Increased pallor, breathlessness, exhaustion chest pain, consolidation on CXR, SaO 2 < 94% on air abdominal pain or distension, diarrhoea, vomiting severe thoracic/back pain headache, drowsiness, CVA,TIA or any abnormal CNS signs 3 Arrangements for admission at NUH (adults) Patients are advised to contact the Haematology acute mobile holder ( ) at City hospital when possible. The patient will be told where they can be seen (haematology wards or Speciality Receiving Unit (SRU)) or in Haematology day case. Page 4 of 29 Lead Author: Submission Date: October 2017 Review Date: October 2020
5 If seen on SRU and requiring admission for longer than 18 hours patients will normally have to be moved to another ward: Haematology wards, Burns ward or another available bed. Patients admitted via ambulance will generally be brought to City hospital but some patients (not known to service, self-presentation or with other issues which may be more appropriately managed in QMC) may be seen in A+E at QMC. If the patient is thought to have a sickle cell crisis they will be transferred to City hospital by ambulance after appropriate analgesia. In all cases the Haematology SpR must be informed (however an uncomplicated admission in the middle of the night could be discussed first thing the next morning) 4 Assessment and initial management of patient with sickle cell disease The general guide for these patients is to speedily assess them if they are known to the service (have ID cards from NHR, or have previous annual review or admission document in the document section of NotIS OR electronic patient record) then assess pain and observations speedily. 4.1 Pain If the pain is usual sickle cell pain and is severe (often patients will have tried their usual oral analgesia before), observations are stable and there are no unusual features analgesia should be given as before: check previous drug charts or dose as follows: Morphine 0.1 mg/kg IV repeated every 20 minutes until pain controlled. Analgesia must be administered within 30 minutes of admission (NICE CG143) If this IV dose is administered by a doctor, suggest diluting 10mg in 10ml saline (1mg/ml) giving 5mg and then titrating to effect over the next 5-10 minutes. Patients with no opioid tolerance may need up to 20mg. Patients with tolerance may need a higher starting dose and a higher total dose. Laxatives, antiemetics and thromboprophylaxis (unless contraindication) should be prescribed. Note baseline monitoring and do bloods (FBC, retics, U+Es, LFTs, CRP, LDH, Clotting, Group and save, Blood cultures if fever or suspicion of infection initially. Full admission clerking should be completed within 2 hours of admission) Page 5 of 29 Lead Author: Submission Date: October 2017 Review Date: October 2020
6 THEN: inform Haematology SpR, ask nursing staff to monitor every 30mins (BP, pulse, pain, temp, O 2 sats, respiratory rate, sedation) until pain controlled and then 2 hourly and put on fluid balance chart. Patient will usually require IV fluids, oxygen, thromboprophylaxis, analgesia regime, laxative and perhaps antiemetic and antipruritic. 4.2 Areas of concern Fever, neurological symptoms, priapism, swollen limbs, complaint of chest or abdominal pain, possibility of pregnancy Please see simplified SRU flow chart (appendix 2 & 3) for simplified guidance for first 60 minutes of admission, Leicester flow chart (appendix 1) for further guidance and appendix 4 for an example of admission document which it is hoped to provide for each sickle cell patient (they may carry a copy and a copy should be available on NotIS/electronic patient record) Entonox may be available in SRU. Those transferring from paediatric care may be treated with oral morphine and intranasal diamorphine is becoming available on paediatric areas and this may be available on the adult side. Those transferring from paediatric clinic and previously receiving oral analgesia should be continued on this Involvement of the Acute Pain Team if ongoing concern about pain relief is recommended Lead Author: Submission Date: October 2017 Review Date: October 2020 Page 6 of 29
7 4.3 Pain management after first 90 minutes Time from 1 st assessment 0-90mins Reason Action Comments Immediate control acute pain Morphine 0.1 mg/kg IV repeated every 20 minutes until pain controlled Can give SC >90mins >90mins Continued intermittent analgesia-administered by staff using an appropriate pain chart and checking every 30 minutes till pain controlled and at least every 4 hours thereafter PCA (patient controlled analgesia) If this IV dose is administered by a doctor, suggest diluting 10mg in 10ml saline (1mg/ml) giving 5mg and then titrating to effect over the next 5-10 minutes. Patients with no opioid tolerance may need up to 20mg. Patients with tolerance may need a higher starting dose and a higher total dose. THEN continued analgesia administered by staff or PCA. Morphine 0.1 mg/kg IV or SC every 2-4 hours. Extra doses if pain persistent (50% of given dose) after 1 hour. OR Morphine 1 mg/ml solution administered IV (PCAs at City currently fixed at 1mg/ml concentration) Background: 2-3 mg/hour (i.e. 2 to 3ml/hr) PCA bolus dose: 1-3mg/bolus Page 7 of 29
8 Dose duration:1 minute Every 30mins then every 1 hour for 6 hours and at least every 4 hours thereafter Monitor Lockout time:20-30 minutes Pain, sedation, vital signs, respiratory rate until pain controlled and stable then every 4 hours Reduced respiratory rate <10 per minute omit opioid analgesia (usually <8) Extra pain relief Prevent vomiting If severe respiratory depression <6 give 100 micrograms naloxone IV repeated every 2 min as necessary Give high flow oxygen by face mask 1) Paracetamol can be given IV in acute phase dose 1g over 15mins up to four times daily, maximum dose 4g 2) Ibuprofen, Diclofenac if no contraindication to NSAIDs 3) Local heat 4) TENS machine CONSIDER ALTERNATIVE DIAGNOSIS Prochlorperazine 5-10mg tds or cyclizine 50mg tds (avoid prolonged parenteral cyclizine use) Suggest use of paracetamol and NSAID unless contraindicated Optional Page 8 of 29
9 Ondansetron 4mg oral or s/c Laxative Lactulose 10ml bd, Senna 2-4 tablets bd, docusate Essential 100mg bd Antipruritic Hydroxyzine 25mg bd Optional Page 9 of 29
10 4.4 Alternative analgesics to consider Oxycodone, Ketamine, Methadone, fentanyl are alternatives but their use should always be discussed with a consultant and the Acute Pain team unless specifically indicated in that patient s documentation. 5 Investigations Patients presenting with sickle cell crisis require the following investigations: FBC and reticulocyte count U&E and LFT Blood cultures MSU Oxygen saturation (ABG if < 95% on air) Lp (if CNS symptoms, discuss with experienced haematologist first) Group and save Check %HbS if on transfusion regime or %HbF if on hydroxycarbamide The following may be required: CXR if chest signs/symptoms, (SO2 <95%, dyspnoea, cough, chest pain) XR is indicated if a patient develops localised bone pain and fever as osteomyelitis is a recognised and potentially serious complication of sickle cell disease CRP 6 Alteration of dose of analgesia Requirements for analgesia needs to be reconsidered on a daily basis at least when pain is well controlled aim to reduce dose by small amounts and switch to oral equivalents when patient is clearly improving (pain score / chart may be helpful) 7 Oxygen There is no good evidence for this being used routinely in all cases of painful crisis Page 10 of 29
11 Its use should be dictated by the clinical situation and oxygen saturations: If SaO 2 <95% on air, give O 2 by face mask Check arterial gases if SaO 2 on air is <95% Monitor SaO 2 while patient is on supplementary oxygen aiming to keep O 2 level > 98% If arterial po 2 (PaO 2 ) <10.7kPa use mask giving 35% inspired oxygen If arterial PaO 2 < 9.3kPa seek additional help generally by involving HDU outreach team 8 Thromboprophylaxis Sickle cell disorders are associated with an increased thrombotic potential All patients who are admitted with a severe sickling crisis who are immobile should be commenced on low molecular weight heparin prophylaxis Do not use TED stockings 9 Antibiotics If the patient is febrile or has a history suggestive of an infective cause of the sickle crisis they should be commenced on antibiotics Augmentin is the antibiotic of choice in most cases unless penicillin allergic Most patients are on oral penicillin maintenance which can be stopped and restarted when the course of Augmentin has been completed 10 Transfusions See Transfusion guideline for further guidance Patients with sickle cell disease often have a chronic anaemia of g/l which is normal for them Hb S has a lower oxygen affinity than Hb A so tissue oxygenation is better than expected It is useful to check the patient s steady state Hb level (eg from an OPD appointment) when reviewing their blood count The Hb may fall g/l during a sickle crisis but blood transfusion is NOT routinely indicated and in fact may exacerbate a crisis Page 11 of 29
12 Blood transfusions should only be used if there are symptoms of severe anaemia, or if the Hb has fallen >20g/l or is below 50 g/l. The transfusion should aim to return the Hb to the steady state level and the blood should be matched for Rhesus and Kell antigens, be sickle negative and as fresh as possible 10.1 Exchange Transfusion The aim of an exchange transfusion is to replace the sickle blood with Hb AA Exchange transfusion should be discussed with a Consultant The indications for urgent exchange transfusion are: o Sickle chest crisis o Cerebral sickling/acute ischaemic stroke o Multi-organ failure Red cell exchange is preferably done using the cell separator via the stem cell nurses who should be contacted on Ext or via the Haematology Day Case Unit Rarely emergency exchanges may have to be performed manually if necessary out of hours Routine elective exchange transfusion may be done for recurrent severe crises or pre-operatively Manual exchange transfusion may be necessary in an emergency (there will be a pack near specialist nurse desk on Fletcher ward) Blood should be Rhesus and Kell genotyped for the patient and Blood Bank should be contacted as soon as an exchange transfusion is planned Hb A and S levels should be sent to the haematology laboratory after exchange transfusion A Hb S level of <30% is the goal of this therapy 11 Other acute presentation 11.1 Acute chest syndrome This is a life threatening complication of sickle cell disease and can arise during a painful crisis or occur on admission Clinical features Some of the following may be present: chest pain (may be pleuritic) cough Page 12 of 29
13 shortness of breath hypoxia: oxygen sats <94% or more than 3% below baseline fever tachypnoea wheeze tachycardia fall in haemoglobin Chest signs (some or none may be present): crepitations bronchial breath sounds reduced air entry dullness to percussion rhonchi Diagnosis clinical suspicion CXR: new pulmonary infiltrate, sometimes normal arterial blood gasses FBC, U+Es, reticulocyte count, clotting screen, %Hb S (if recent transfusion), CRP, group and antibody screen Microbiology: blood and sputum culture, atypical serology, sputum viral DNA PCR culture, urine for legionella and pneumococcal antigens, nasopharyngeal aspirate if coryzal Differential diagnosis acute infection PE opiate toxicity fluid overload under-ventilation due to pain Management vigilance (4 hourly monitoring of pulse oximetry and respiratory rate increased to at least hourly if clinical suspicion of ACS) Early liaison with HDU / outreach team as transfer may be necessary involve Haematology SpR / Haematology Consultant Page 13 of 29
14 TRANSFUSION: simple top up especially if Hb decreased from baseline (post transfusion Hb <10); manual or automated exchange is preferable if deteriorating patient, widespread infiltrates, if top-up likely to result in increased viscosity (or limited response to top up), other problems (see transfusion guidelines) aim O2 saturation >96% chest physio check on appropriate broad spectrum antibiotics may need microbiology advice hydration essential but avoid fluid overload (use fluid chart) pain control must be continued with regular monitoring Nebulised bronchodilators may be helpful continue thromboprophylaxis, change dose if clinical suspicion of PE incentive spirometry may be helpful 11.2 Abdominal pain Differential diagnosis cholelithiasis pancreatitis referred pain from chest appendicitis acute splenic/hepatic sequestration Infection constipation ischaemia of bowel thrombosis e.g. renal vein vaso-occlusion Clinical findings tenderness lack of/heightened bowel sounds Investigations FBC, retics, U+Es, LFTs, coag, lipase, blood cultures, MSSU plain abdominal X-ray abdominal ultrasound / CT as guided by radiology Page 14 of 29
15 Management surgical opinion may prove useful but acute surgical intervention is rarely indicated discuss with senior haematologist maintain good hydration (generally IV fluids) close monitoring IV antibiotics if febrile (and with a view to covering likely GI pathogens) early recourse to ITU referral / outreach team 11.3 Priapism Two types: stuttering (recurrent episodes lasting <30 mins) or fulminant (>3 hours). Both are associated with pain and fulminant priapism is a medical emergency. Fulminant priapism may also occur in context of painful crisis in other body part. This is difficult to discuss with patients you may have to ask (or look in annual review records) Management hydration, analgesia, encourage micturition etilefrine 50mg may be given by mouth urgent urology (on call at CITY hospital) opinion should be sought if priapism persists after 3-4 hours then aspiration of corpora cavernosa (with or without irrigation) or intracavernous injection of dilute phenylephrine transfusion therapy is not thought useful in acute presentation 11.4 Osteomyelitis consider in any patient with hot painful limb as part of differential diagnosis of painful crisis x-ray not always helpful but should be done if osteomyelitis is considered include blood cultures for any febrile patient choice of broad spectrum antibiotics should include cover for likely pathogens (seek microbiology advice) 11.5 Acute stroke may be ischemic or haemorrhagic in adults diagnosis needs to be confirmed radiologically urgently Page 15 of 29
16 thrombolysis should be considered in sickle cell patients with acute cerebral thrombosis this should be discussed by the senior haematologist and the stroke physicians transfusion therapy should be given in order to reduce HbS to <30% but timing will require discussion those with subarachnoid haemorrhage may have multiple aneurysms 11.6 Acute anaemia presentation with pallor, extreme lethargy possible underlying pathologies: parvovirus infection, sequestration (see below), folate deficiency investigations: FBC and retics, parvovirus serology, urgent cross match (where possible genotyped and sickle negative) usual steady state Hb values may be helpful (from clinic visits) 11.7 Acute sequestration sudden enlargement of spleen (occasionally liver) in which blood is pooled in the organ leading to a severe reduction in circulating red cells and profound anaemia abdominal palpation will reveal an enlarged spleen urgent FBC and retics followed by urgent cross match (if possible genotyped and sickle negative red cells) as a top up transfusion 11.8 Haematuria Acute haematuria can be due to renal papillary necrosis and can be accompanied by ureteric colic (if obstructive) and can be associated with significant blood loss. The diagnosis may be confirmed on ultrasound but sometimes a CT scan is required. Treatment is supportive and occasionally urological support may be required for renal irrigation. Other causes of haematuria need to be borne in mind (e.g. renal cancers) Page 16 of 29
17 11.9 Acute visual loss Patients reporting acute visual loss should be advised to attend the emergency ophthalmology clinic at QMC (close to A+E and with extended evening opening hours and at weekend) 12 References 1. Rees et al (2003) Guidelines for the management of the acute painful crisis in sickle cell disease. British Journal of Haematology; 120: National Institute for Health and Care Excellence (2012) Sickle cell acute painful episode. CG143. London: National Institute for Health and Care Excellence. 3. Lottenberg R, Hassell KL. (2005) An evidence based approach to the treatment of adults with sickle cell disease. Hematology; Standards for the clinical care of Adults with sickle cell disease (2017) in preparation Page 17 of 29
18 Appendix 1 UHL Management of Painful Sickle Cell Crisis flow chart See following page Page 18 of 29
19 Developed by C. Chapman, Z. Suleman & M. Aheame Weight Kg Doctor to complete Is Pain adequately controlled after 20 mins? 3. Complete Initial Assessments 4. Assess Urine output and commence fluid balance 5. Take sample of urine +/- send for MC&S 6. Antibiotics to be given without delay in cases with acute sepsis (refer to UHL antimicrobial website) 7. Hydration please provide jug of water and encourage oral fluids to prevent further sickling. Inform doctor if patient unable to tolerate as patient will need IV fluids 8. Ensure patient is warm, provide extra blankets if necessary 9. Weigh the patient 10. Repeat the observations every 30 MINS until pain is resolved. Investigations Blood FBC, U&E, reticulocytes, LFT, CRP G&S +/- cultures Urine +/- MC&S Imaging CXR if dyspnoea, Sp02 <95%, fever, cough, chest pain Sickle Cell Disease: Painful crisis Patient Details Name: Guideline flowchart for Adults with Sickle Cell Disease: Acute Presentation DOB: To be followed when a patient with sickle cell disease presents Hosp No: to A&E unwell ED Nurse or Doctor to complete 1. Assessment of Pain & EWS score 2. Administer analgesia using WHO analgesic ladder and see box A Y Check Respiratory Rate every hour 1. Take history including Pain/infection/neurology/surgical history/vaccination/ precipitating event/recent transfusions 2. Examine inc CVS/RESP/Abdo/Neuro/ENT/Skin assess for signs of septic shock, pneumonia, CHF, acute chest syndrome / likely sources of infection 3. Investigations 4. VTE assessment +/- Dalteparin 5. Obtain IV access (avoid cannulating legs) Is the patient high risk? (see box C) N Any Red Flag Events? (see box D) N Assess Opiate Toxicity (see box B) Y Y A. Management of Pain Mild Pain: Paracetamol 0.5g -1g QDS +/- Codeine 1mg/kg +/- Ibuprofen 200mg TDS OR Diclofenac 50mg BD Moderate/Severe Pain: Add Morphine 100mcg/kg SC or IV repeat after 20 MINS if necessary. Then mcg/kg every 2-4 hours OR continuous infusion via PCA B. Are there signs of opiate toxicity? Likely if the following present Low Respiratory Rate : RR < 12 Hypoxia : Oxygen saturation SP02 <94% OR <9kPa PO2 Drowsiness Pin Point pupils If none of these present Safe to give another dose of morphine C. Is the patient high-risk? Previous ITU admission Previous blood / exchange transfusion? D. Red Flag Events Acute Chest Syndrome Aplastic Crisis (suspect if Hb < 2 units below baseline and reticulocytes are low/normal Stroke Priapism Acute Abdomen Splenic Sequestration Contact Haematology SpR via switchboard Contact Bed Bleep on 45XX if admission required Name of SpR:... Advice Given: Blood Transfusion Advised? Yes/No If Yes: Order Sickle negative blood Not for Blood transfusion unless discussed with Haematology SpR 6. Manage Pain according to Box A. 7. Patients unable to tolerate oral fluids need IV fluids (10-20mls/kg of 0.9% normal saline. Followed by maintenance fluids. Caution in patients with renal/cardiac problems. Close monitoring is advised. 8. Check blood results Page 19 of 29 N Is Pain adequately controlled? Y 9. Check if safe for discharge see box E N E. Safe for Discharge? Haematology Registrar Contacted? Yes/No Is Pain Controlled Yes/No Last morphine dose administered 4 hours ago Y/N EWS is 0 Yes/No If EWS > 0 have you discussed with Haem SpR Y/N If ALL answers are yes patient safe for discharge
20 Appendix 2 Acute Painful sickle cell crisis medical management in first 60minutes Triage as high priority Confirm diagnosis where possible (check photo- ID card if patient has one, check NotIS, notes) Initial Assessment: Site of pain Whether usual sickle pain and severity (use pain chart if possible) Ask about analgesics used, usual hospital analgesia and any allergies Check baseline monitoring (BP, Pulse, temp, O2 sats, respiratory rate) Give analgesia: usually opiates but if difficulty in establishing IV access subcutaneous or oral route might be preferred (buccal fentanyl could also be used) Must be given within 30 minutes of arrival. May need repeated if unsatisfactory relief When patient more comfortable check history further and examine (if either incomplete at this stage please complete within 2 hours of admission), note baseline monitoring and do bloods (FBC, retics, U+Es, LFTs, LDH, Clotting, Group and save, Blood cultures if fever or suspicion of infection) THEN: inform Haematology SpR, ask nursing staff to monitor every 30mins (BP, pulse, pain, temp, O2 sats, respiratory rate, sedation) till Page 20 of 29
21 pain controlled and then 2 hourly and put on fluid balance chart. Patient will usually require IV fluids, oxygen, thromboprophylaxis, analgesia regime, laxative and perhaps antiemetic and antipruritic Areas of concern: fever, neurological symptoms, priapism, swollen limbs, complaint of chest or abdominal pain, possibility of pregnancy 2017 Page 21 of 29
22 Appendix 3 Acute Painful Sickle Cell Crisis nursing management in first 60 minutes This is an acute medical emergency and such patients need attention and support as soon as they arrive in the department do baseline observations (BP, pulse, O2 sats, respiratory rate, pain score) doctor needs to be informed immediately of sickle cell patient with acute crisis in department reassure patient, ask site of pain and type (? like usual sickle pain) if there is opportunity prepare for IV access, fluid balance chart, pain chart (more copies available from resource file or sickle cell specialist nurse) needs to have observations checked as above and sedation level every 30 minutes until stable and pain free and then 2 hourly fluid balance must be checked and noted on chart Alert doctor to: chest and abdominal pain, priapism, high fever, neurological symptoms, swollen limbs or pregnancy Doreen Richards 2015 Page 22 of 29
23 Appendix 4 Example of sickle cell disease admission document See following page. Page 23 of 29
24 TO BE USED FOR NAMED PATIENT ONLY for PAINFUL SICKLE CRISIS Patient Name: #### ########## Hospital no: ####### NHS no: ### ### ##### Dob: 28/2/1984 Diagnosis: Hb SS Date of completion: 20/11/12 Date of review: 2014 Please see Sickle cell flow chart and guidance if unsure ask Haem SpR or contacts below Issue Usual analgesia for sickle crisis in Hospital* Other treatment Particular issues /complications Allergies Usual analgesia at home Other medication need for monitoring (Eg Hydroxycarbamide) Usual follow -up Management /comment Morphine 5-10 mg initially SC or IV, further 5mg every 20 minutes until pain controlled 5-10mg be repeated every 2 hours Fluids encourage at least oral intake of 1 litre every 8 hours otherwise IV may be required Enoxaparin if admitted (unless contraindication) Antiemetic Laxative Supplemental oxygen if sats <96% Pain Chart Previous weight loss please monitor Check! Tramadol None Please encourage op attendance * DO NOT GIVE OPIATES IF RESPIRATORY RATE <9, OXYGEN SATS <90% or drowsy seek medical advice first. Please let Haematology SpR know of admission. Further guidance may also be obtained from Dr Donohue (bleep 6822, sarah.donohue@nuh.nhs.uk) Doreen Richards (bleep7972, doreen.richards@nuh.nhs.uk) or sickle cell service ( ) Audit Time of arrival Time of first analgesia Pain score initially Pain score at 90- Page 24 of 29
25 TO BE USED FOR NAMED PATIENT ONLY for PAINFUL SICKLE CRISIS Patient Name: #### ########## Hospital no: ####### NHS no: ### ### ##### Dob: 28/2/1984 Diagnosis: Hb SS Date of completion: 20/11/12 Date of review: 2014 Please see Sickle cell flow chart and guidance if unsure ask Haem SpR or contacts below Monitoring as per guideline Other medication Other complications Bp, O2sats, p, temp, resp rate Laxative, LMWH etc 120min Any learning points? Oct 12 Page 25 of 29
26 Appendix 5 Sickle Cell Crisis Pathway Sickle Cell Crisis - Acute Chest Syndrome : Management Pathway and Referral Pathway to the HDU and ITU Presentation with respiratory signs and symptoms (as below in the table) including hypoxia +/- new CXR infiltration Fever ++ Tachypnoea + Cough ++ Wheezing +/- Chest pain ++ Skeletal pain ++ Dyspnoea ++ Haemoptysis+ A high clinical suspicion is vital to early diagnosis Acute Chest Syndrome can be a severe life-threatening condition Stable patients can deteriorate rapidly to acute respiratory failure Think ahead of Exchange Transfusion and ITU input Investigations CXR, FBC, UEs, LFTs Blood group and screen (or crossmatch) Blood cultures Sputum cultures ABG Serology/urine for atypical respiratory organisms SpO2 95% (on air) on pulse oximetry or a fall in SpO2 of 3% or more from baseline steady state confirmed with ABG promptly Management Fluids, Pain relief, Oxygen, Antibiotics +/- bronchodilators Contact and inform on-call Consultant Haematologist for advice Above investigations may need to be repeated in the deteriorating patient Inform Blood Bank early on about possible blood transfusion requirement Exchange Transfusion need to be done on HDU/ITU and protocol is available from Haematologist Falling po2 Hb<70g/dl or po2(air) <9.0kPA Hb>70g/dl And/or Rapid deterioration plus indicators of severity po2(air) <8.0kPa pco2 >6.0kPa Top up transfusion ITU outreach team review Exchange transfusion ITU review Consideration of NIV/IV Page 26 of 29
27 Appendix 6 Quick Reference Guide EMSCT guidance on sickle cell disease acute management Good Practice Reference- to national /local guidelines Acute pain o Rapid assessment (basic NUH Guidance page 5 observations, check with patient) o Pain relief within 30 minutes - e.g. morphine 0.1mg/kg parenterally or patient has specific pain plan o Continued monitoring every 30 mins till pain relieved then 2 hourly o Then fuller assessment and investigations (FBC retics, u+es, LFTs, Gp and save, LDH, blood cultures if fever, haemoglobinopathy screen if indicated), CRP o ADD laxative, thromboprophylaxis, paracetamol, NSAID unless contraindicated o Iv fluids if insufficient oral intake o Supplemental oxygen if <SO2 <95% Fever o Blood cultures and MSSU, other cultures if symptoms Identify cause and treat within local guidance o Low threshold for antibiotics o Suspend penicillin V if on broad spectrum antibiotics Monitor CRP NUH Guidance page 6 Chest syndrome o Warning signs : chest pain, falling NUH Guidance page 12 oxygen saturation, SOB o Do CXR (look for widespread infiltrate but may be normal) o Check blood gasses o Consider HDU/ ITU transfer o Exchange transfusion Page 27 of 29
28 Priapism o If prolonged can be medical emergency (exercise, warm bath can help) o Analgesia o Early discussion with urology if >2hours, may need to aspirate o Alpha adrenergic blocker e.g. etilefrine may help o Transfusion therapy probably not helpful Neurological o Acute ischaemic or haemorrhagic stroke possible o Urgent imaging Acute sequestration Acute anaemia Page 28 of 29 o Thrombolysis indicated as for nonsickle patient o Urgent red cell exchange for ischaemic stroke? also for haemorrhagic o Sudden enlargement of spleen (occasionally liver) with blood pooling resulting in profound anaemia o Urgent blood transfusion required o Symptomatic anaemia (SOB, lethargy, pallor) with Haemoglobin usually falling by 25% of baseline or less 20g/l from steady state level o Top up transfusion may be necessary o Exclude other causes (e.g. parvovirus, bleeding, folate deficiency) Osteomyelitis o Consider in any febrile patient with swollen painful limb o Xray may not be helpful especially initially o Use broad spectrum antibiotics as per Trust guidance Haematuria o If painless may be papillary necrosis (pain only if accompanied by obstruction) o Monitor loss NUH Guidance page 15 NUH Guidance page 15 NUH Guidance page 16 NUH Guidance page 16 NUH Guidance page 15 NUH Guidance page 16
29 Visual loss o Us may be helpful, otherwise CT o If persistent, bladder irrigation may be helpful o NB other causes of haematuria o Any acute symptoms should be seen urgently - eye casualty at QMC NUH Guidance page 17 Page 29 of 29
Drug and Therapeutics committee, Clinical Haematology Directorate. Department of Haematology, Nottingham City Hospital
 Version: 5 Date: 03/08/2005 Date Ratified: 03/08/2005 Date Reviewed 3/08/2017 Date due for Review: August 2018 Approval: Author: Drug and Therapeutics committee, Clinical Haematology Directorate Dr Jennifer
Version: 5 Date: 03/08/2005 Date Ratified: 03/08/2005 Date Reviewed 3/08/2017 Date due for Review: August 2018 Approval: Author: Drug and Therapeutics committee, Clinical Haematology Directorate Dr Jennifer
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a)
 Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
ADULT (>16) ACUTE SICKLE PAIN GUIDELINE
 ADULT (>16) ACUTE SICKLE PAIN GUIDELINE ID 2013 065 Author s Name Dr Anna Wood Author s Job Title Consultant Haematologist Division Consultant Haematologist Department Haematology Version number 3 Ratifying
ADULT (>16) ACUTE SICKLE PAIN GUIDELINE ID 2013 065 Author s Name Dr Anna Wood Author s Job Title Consultant Haematologist Division Consultant Haematologist Department Haematology Version number 3 Ratifying
Aneurin Bevan University Health Board Sickle Cell Anaemia and Haemoglobinopathy Screening and Management in Pregnancy Guidelines
 Sickle Cell Anaemia and Haemoglobinopathy Screening and Management in Pregnancy Guidelines N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Sickle Cell Anaemia and Haemoglobinopathy Screening and Management in Pregnancy Guidelines N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Guidelines for Shared Care Centres and Community Staff
 Reference: CG1411 Written by: Dr Jenny Welch Peer reviewer Dr Jeanette Payne Approved: September 2015 Approved by D&TC: 10 th July 2015 Review Due: September 2018 Intended Audience This document contains
Reference: CG1411 Written by: Dr Jenny Welch Peer reviewer Dr Jeanette Payne Approved: September 2015 Approved by D&TC: 10 th July 2015 Review Due: September 2018 Intended Audience This document contains
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin
 Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin
 Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Version: 6 Date: 2 nd March 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Version: 6 Date: 2 nd March 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/
Title: Improving the patient experience for children with Sickle Cell Disease Author/Responsible Director: Carole Ribbins Director of Nursing
 Trust Board Paper S To: Trust Board From: Kate Wilkins Divisional Head of Nursing Hilliary Killer Children s CBU Nurse Lead and General Manager Liz James Matron, Children s CBU Date: 28 March 2013 All
Trust Board Paper S To: Trust Board From: Kate Wilkins Divisional Head of Nursing Hilliary Killer Children s CBU Nurse Lead and General Manager Liz James Matron, Children s CBU Date: 28 March 2013 All
Emergency Presentations of Sickle cell disease. Dr S Pancham Sickle Cell & Thalassaemia Centre City Hospital
 Emergency Presentations of Sickle cell disease Dr S Pancham Sickle Cell & Thalassaemia Centre City Hospital Aims Key features to elicit at presentation What complications to look for When to phone for
Emergency Presentations of Sickle cell disease Dr S Pancham Sickle Cell & Thalassaemia Centre City Hospital Aims Key features to elicit at presentation What complications to look for When to phone for
The Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 The Management of Acute Chest Syndrome in Children with Sickle Cell Disease Document Information Version: 4 Date: Dec 2013 Authors (incl. job title): Professor David Rees and Dr Sue Height, consultant
The Management of Acute Chest Syndrome in Children with Sickle Cell Disease Document Information Version: 4 Date: Dec 2013 Authors (incl. job title): Professor David Rees and Dr Sue Height, consultant
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
DOCUMENT CONTROL PAGE Title Title: UNDERGOING SPINAL DEFORMITY SURGERY Version: 2 Reference Number: Supersedes Supersedes: all other versions Description of Amendment(s): Revision of analgesia requirements
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm
 Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
PE Pathway. The charts are listed as follows:
 PE Pathway This document comprises 6 simple flow charts to assist clinicians in the investigation and treatment of suspected or confirmed Acute Pulmonary Emboli. The pathway has been put together using
PE Pathway This document comprises 6 simple flow charts to assist clinicians in the investigation and treatment of suspected or confirmed Acute Pulmonary Emboli. The pathway has been put together using
Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143
 Sickle cell disease: managing acute painful episodes in hospital Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Sickle cell disease: managing acute painful episodes in hospital Clinical guideline Published: 27 June 2012 nice.org.uk/guidance/cg143 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
A Care Pathway exists for the management of neutropenic fever. Copies of the care pathway document are available in EAU, A&E, Deanesly and CHU.
 Subject: Neutropenic Fever Guideline for Junior Doctors Date of Implementation: January 2010 Date of Review: January 2012 Director Responsible for Implementation and Review: Policy location: Consultant
Subject: Neutropenic Fever Guideline for Junior Doctors Date of Implementation: January 2010 Date of Review: January 2012 Director Responsible for Implementation and Review: Policy location: Consultant
Haemophilia Suspected Bleed
 Haemophilia Suspected Bleed Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the management
Haemophilia Suspected Bleed Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the management
Blood Transfusions in Children with Haemoglobinopathies
 Blood Transfusions in Children with Haemoglobinopathies Version: 2 Date: 22 nd April 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/ committees involved in
Blood Transfusions in Children with Haemoglobinopathies Version: 2 Date: 22 nd April 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/ committees involved in
BJF Acute Pain Team Formulary Group
 Title Analgesia Guidelines for Acute Pain Management (Adults) in BGH Document Type Issue no Clinical guideline Clinical Governance Support Team Use Issue date April 2013 Review date April 2015 Distribution
Title Analgesia Guidelines for Acute Pain Management (Adults) in BGH Document Type Issue no Clinical guideline Clinical Governance Support Team Use Issue date April 2013 Review date April 2015 Distribution
PAEDIATRIC FEBRILE NEUTROPENIA CARE PATHWAY
 PAEDIATRIC FEBRILE NEUTROPENIA CARE PATHWAY Purpose: This document is intended as a guide to the investigation and management of children presenting in Salisbury District Hospital with suspected neutropenic
PAEDIATRIC FEBRILE NEUTROPENIA CARE PATHWAY Purpose: This document is intended as a guide to the investigation and management of children presenting in Salisbury District Hospital with suspected neutropenic
Protocol for the Management of Neutropenic Sepsis in Adult Patients P
 Protocol for the Management of Neutropenic Sepsis in Adult Patients P Version 2 Date April 2015 Review Date April 2016 Author Rachel Onions Change Approver Acute Oncology Team UHMBT. Version 2. CHANGE
Protocol for the Management of Neutropenic Sepsis in Adult Patients P Version 2 Date April 2015 Review Date April 2016 Author Rachel Onions Change Approver Acute Oncology Team UHMBT. Version 2. CHANGE
Managing Exacerbations of COPD (Version 3.0)
 Managing Exacerbations of COPD (Version 3.0) Guideline Readership This guideline is intended for use in patients with a confirmed diagnosis of a chronic obstructive pulmonary disease (COPD) exacerbation.
Managing Exacerbations of COPD (Version 3.0) Guideline Readership This guideline is intended for use in patients with a confirmed diagnosis of a chronic obstructive pulmonary disease (COPD) exacerbation.
Pulmonary Embolism Pathway
 Pulmonary Embolism Pathway Ambulatory Care Pathway Dr. A. Zafar, Dr. A. Rehman, Dr. T. Malik September, 2011. Patient Identification Label Pulmonary Embolism Pathway Clinical History Comments Hospital
Pulmonary Embolism Pathway Ambulatory Care Pathway Dr. A. Zafar, Dr. A. Rehman, Dr. T. Malik September, 2011. Patient Identification Label Pulmonary Embolism Pathway Clinical History Comments Hospital
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Sickle cell acute episode: management of an acute painful sickle cell episode in hospital 1.1 Short title Sickle cell acute
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Sickle cell acute episode: management of an acute painful sickle cell episode in hospital 1.1 Short title Sickle cell acute
Management of acute asthma in children in emergency department. Moderate asthma
 152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
Please inform the Diabetes Nurse Specialist that this patient has been admitted within 24hrs of admission.
 Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Sickle Cell Disease- Case studies
 Sickle Cell Disease- Case studies Subarna Chakravorty King s College Hospital 2017 Conditions requiring immediate admission Agonising pain (i.e. requiring opiate analgesia) Increased pallor, breathlessness,
Sickle Cell Disease- Case studies Subarna Chakravorty King s College Hospital 2017 Conditions requiring immediate admission Agonising pain (i.e. requiring opiate analgesia) Increased pallor, breathlessness,
Managing Emergencies
 Managing Emergencies Richard Ward, MSc, MRCP, FRCPath Director, Red Blood Cell Disorders Program, UHN Assistant Professor, Hematology, University of Toronto Chair, Canadian Hemoglobinopathy Association
Managing Emergencies Richard Ward, MSc, MRCP, FRCPath Director, Red Blood Cell Disorders Program, UHN Assistant Professor, Hematology, University of Toronto Chair, Canadian Hemoglobinopathy Association
Day care adenotonsillectomy in sleep apnoea
 Day care adenotonsillectomy in sleep apnoea Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Day care adenotonsillectomy in presence of sleep apnoea 1a 2a 2b Contact
Day care adenotonsillectomy in sleep apnoea Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Day care adenotonsillectomy in presence of sleep apnoea 1a 2a 2b Contact
Title Protocol for the Management of Asthma
 Document Control Title Protocol for the Management of Asthma Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and Resilience Department Version
Document Control Title Protocol for the Management of Asthma Author Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics and Resilience Department Version
CARE PATHWAY FOR CHILDREN AND YOUNG PERSONS WITH FEBRILE NEUTROPENIA, NEUTROPENIC SEPSIS OR SUSPECTED CENTRAL VENOUS LINE INFECTIONS
 CARE PATHWAY FOR CHILDREN AND YOUNG PERSONS WITH FEBRILE NEUTROPENIA, NEUTROPENIC SEPSIS OR SUSPECTED CENTRAL VENOUS LINE INFECTIONS This Care Pathway has been developed by a multidisciplinary team. It
CARE PATHWAY FOR CHILDREN AND YOUNG PERSONS WITH FEBRILE NEUTROPENIA, NEUTROPENIC SEPSIS OR SUSPECTED CENTRAL VENOUS LINE INFECTIONS This Care Pathway has been developed by a multidisciplinary team. It
Sickle cell disease. Fareed Omar 10 March 2018
 Sickle cell disease Fareed Omar 10 March 2018 Physiology Haemoglobin structure HbA2: 2α and 2δ chains (2-3%) HbF: 2α and 2γ chains (
Sickle cell disease Fareed Omar 10 March 2018 Physiology Haemoglobin structure HbA2: 2α and 2δ chains (2-3%) HbF: 2α and 2γ chains (
High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH
 High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH Contents: Page No. 1. Overview 2 2. Admission 3 3. Admission Checklist 5 4. Inpatient management during chemotherapy 6 5. Inpatient
High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH Contents: Page No. 1. Overview 2 2. Admission 3 3. Admission Checklist 5 4. Inpatient management during chemotherapy 6 5. Inpatient
Trust Guideline for the Management of Patient Controlled Analgesia (PCA) in Adults
 Patient Controlled Analgesia (PCA) in Adults A clinical guideline recommended for use For Use in: In all Clinical Areas By: Anaesthetists, Ward Nurses, Recovery Staff Acute Pain Service Staff For: Adult
Patient Controlled Analgesia (PCA) in Adults A clinical guideline recommended for use For Use in: In all Clinical Areas By: Anaesthetists, Ward Nurses, Recovery Staff Acute Pain Service Staff For: Adult
Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway
 Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway Dr Alex Williams, Oncology Specialty Doctor. Cheltenham General Hospital Oncology Centre
Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway Dr Alex Williams, Oncology Specialty Doctor. Cheltenham General Hospital Oncology Centre
Guideline for the Acute Management of Stroke in Paediatric Patients with Sickle Cell Disease
 Guideline for the Acute Management of Stroke in Paediatric Patients with Sickle Cell Disease Summary Outline of the presentation of stroke in paediatric patients with sickle cell disease, urgent investigations,
Guideline for the Acute Management of Stroke in Paediatric Patients with Sickle Cell Disease Summary Outline of the presentation of stroke in paediatric patients with sickle cell disease, urgent investigations,
Unwell returned traveller
 Unwell returned traveller Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date):
Unwell returned traveller Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date):
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM. Is This Strictly a Pain Episode? Decision 7: Referrals
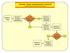 ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
STSTN Guidelines for the Diagnosis and Management of Acute Chest Syndrome in Adult Sickle Cell Disease Patients
 STSTN Guidelines for the Diagnosis and Management of Acute Chest Syndrome in Adult Sickle Cell Disease Patients Approved for publication January 2018 Review date January 2021 Lead editor Dr Rachel Kesse-Adu
STSTN Guidelines for the Diagnosis and Management of Acute Chest Syndrome in Adult Sickle Cell Disease Patients Approved for publication January 2018 Review date January 2021 Lead editor Dr Rachel Kesse-Adu
GUIDELINES ON THE MANAGEMENT OF PAIN DUE TO CANCER IN ADULTS
 GUIDELINES ON THE MANAGEMENT OF PAIN DUE TO CANCER IN ADULTS Bristol Palliative Care Collaborative Contact Numbers: Hospital Specialist Palliative Care Teams: North Bristol 0117 4146392 UH Bristol 0117
GUIDELINES ON THE MANAGEMENT OF PAIN DUE TO CANCER IN ADULTS Bristol Palliative Care Collaborative Contact Numbers: Hospital Specialist Palliative Care Teams: North Bristol 0117 4146392 UH Bristol 0117
Bleeding / Pain after Renal Biopsy Guideline
 Bleeding / Pain after Renal Biopsy Guideline This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances of the individual
Bleeding / Pain after Renal Biopsy Guideline This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances of the individual
Guidelines for the Immediate Management of Paediatric Patients with Sickle Cell Disease (SCD) and Acute Neurological Symptoms
 Guidelines for the Immediate Management of Paediatric Patients with Sickle Cell Disease (SCD) and Acute Neurological Symptoms Document Information Version: 2 Date: Sept 2014 Authors (incl. job title):
Guidelines for the Immediate Management of Paediatric Patients with Sickle Cell Disease (SCD) and Acute Neurological Symptoms Document Information Version: 2 Date: Sept 2014 Authors (incl. job title):
Children who are neutropenic and unwell, even if normothermic, should be assumed to have infection and be treated appropriately.
 PAEDIATRIC FEBRILE NEUTROPENIA CARE PATHWAY Purpose: This document is intended as a guide to the investigation and management of children presenting in Salisbury District Hospital with suspected neutropenic
PAEDIATRIC FEBRILE NEUTROPENIA CARE PATHWAY Purpose: This document is intended as a guide to the investigation and management of children presenting in Salisbury District Hospital with suspected neutropenic
FRACTURED NECK OF FEMUR CLINICAL PATHWAY
 FRACTURED NECK OF FEMUR CLINICAL PATHWAY Patient s... Hospital No. Date... Information Taken By. Designation History of Injury Date and of Event Clinical Assessment of Injury Affected Limb Right Left Reason:
FRACTURED NECK OF FEMUR CLINICAL PATHWAY Patient s... Hospital No. Date... Information Taken By. Designation History of Injury Date and of Event Clinical Assessment of Injury Affected Limb Right Left Reason:
Charlson Comorbidities (please TICK all that apply)
 Medical Clerking On Call Consultant: Date: Time: Grade: Specialty: Age: Presenting Complaint: CLINICIAN: GRADE: DATE/TIME: Past Medical History: Charlson Comorbidities (please TICK all that apply) Cancer
Medical Clerking On Call Consultant: Date: Time: Grade: Specialty: Age: Presenting Complaint: CLINICIAN: GRADE: DATE/TIME: Past Medical History: Charlson Comorbidities (please TICK all that apply) Cancer
PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain
 Index No: MMG43 PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain Version: 3.1 (Includes anti-emetics and naloxone) Date ratified: July 2013 Ratified by: (Name of Committee) Name
Index No: MMG43 PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain Version: 3.1 (Includes anti-emetics and naloxone) Date ratified: July 2013 Ratified by: (Name of Committee) Name
Analgesia for chest trauma - RVI
 Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Oxygen: Is there a problem? Tom Heaps Acute Physician
 Oxygen: Is there a problem? Tom Heaps Acute Physician Case 1 79-year-old female, diabetic, morbidly obese Admitted with LVF Overnight Reduced GCS?cause 15l NRB in situ ABG showed ph 6.9, pco 2 15.9kPa
Oxygen: Is there a problem? Tom Heaps Acute Physician Case 1 79-year-old female, diabetic, morbidly obese Admitted with LVF Overnight Reduced GCS?cause 15l NRB in situ ABG showed ph 6.9, pco 2 15.9kPa
MANAGEMENT OF DENGUE INFECTION IN ADULTS (Revised 2 nd Edition) QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 1 KEY MESSAGES Dengue is a dynamic disease and presented in three phases - febrile phase, critical phase and recovery phase. Clinical deterioration often occurs in the critical phase and is marked by plasma
1 KEY MESSAGES Dengue is a dynamic disease and presented in three phases - febrile phase, critical phase and recovery phase. Clinical deterioration often occurs in the critical phase and is marked by plasma
Transfusion-Related Acute Lung Injury (TRALI) and Strategies for Prevention. Khalid Abdulla Sharif, MD, MRCP (UK)*
 Bahrain Medical Bulletin, Vol. 29, No.4, December 2007 Transfusion-Related Acute Lung Injury (TRALI) and Strategies for Prevention Khalid Abdulla Sharif, MD, MRCP (UK)* Background: Transfusion-Related
Bahrain Medical Bulletin, Vol. 29, No.4, December 2007 Transfusion-Related Acute Lung Injury (TRALI) and Strategies for Prevention Khalid Abdulla Sharif, MD, MRCP (UK)* Background: Transfusion-Related
Title Protocol for the Management of Urinary Tract Infections for Adult Females and Children in MIUs and WICs
 Document Control Title Protocol for the Management of Urinary Tract Infections for Adult Females and Children in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate,
Document Control Title Protocol for the Management of Urinary Tract Infections for Adult Females and Children in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate,
Pathology Service User Guide Haematology
 Pathology Service User Guide Haematology St Richard s This section of the Pathology Service User Guide includes: Anticoagulant Therapy Information about the Anticoagulant Clinic Low Molecular Weight Heparin
Pathology Service User Guide Haematology St Richard s This section of the Pathology Service User Guide includes: Anticoagulant Therapy Information about the Anticoagulant Clinic Low Molecular Weight Heparin
Care in the Last Days of Life
 Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
BREAK 11:10-11:
 1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
StRs and CT doctors in haematology. September Folinic acid dose modified.
 High dose Methotrexate and folinic acid rescue Full Title of Guideline: Author (include email and role): Division & Speciality: Clinical Guideline Review Date September 2018 GUIDELINE FOR THE USE OF HIGH
High dose Methotrexate and folinic acid rescue Full Title of Guideline: Author (include email and role): Division & Speciality: Clinical Guideline Review Date September 2018 GUIDELINE FOR THE USE OF HIGH
Blunt Chest Trauma (Rib Fracture) Management Guideline
 Blunt Chest Trauma (Rib Fracture) Management Guideline Midlands Critical Care, Trauma and Burns Networks Network: Midlands Trauma Networks Publication: Document purpose: Trauma Guidelines Document name:
Blunt Chest Trauma (Rib Fracture) Management Guideline Midlands Critical Care, Trauma and Burns Networks Network: Midlands Trauma Networks Publication: Document purpose: Trauma Guidelines Document name:
Treating acute painful sickle cell episodes in hospital
 Understanding NICE guidance Information for people who use NHS services Treating acute painful sickle cell episodes in hospital NICE clinical guidelines advise the NHS on caring for people with specific
Understanding NICE guidance Information for people who use NHS services Treating acute painful sickle cell episodes in hospital NICE clinical guidelines advise the NHS on caring for people with specific
Suspected Pulmonary embolus Ambulatory Pathway. Document Title. Date Issued/Approved: Date Valid From: 11/11/17. Date Valid To: 11/05/18
 POLICY UNDER REVIEW Please note that this policy is under review. It does, however, remain current Trust policy subject to any recent legislative changes, national policy instruction (NHS or Department
POLICY UNDER REVIEW Please note that this policy is under review. It does, however, remain current Trust policy subject to any recent legislative changes, national policy instruction (NHS or Department
The sickle cell outpatient service Information for adult patients with sickle cell disease
 The sickle cell outpatient service Information for adult patients with sickle cell disease This information sheet has been given to you to help answer some of the questions you may have about the outpatient
The sickle cell outpatient service Information for adult patients with sickle cell disease This information sheet has been given to you to help answer some of the questions you may have about the outpatient
Breathlessness in advanced disease. February 2017
 Breathlessness in advanced disease February 2017 Breathlessness Managing breathlessness in primary care Chronic breathlessness Acute exacerbation of breathlessness Breathlessness at end of life Breathlessness
Breathlessness in advanced disease February 2017 Breathlessness Managing breathlessness in primary care Chronic breathlessness Acute exacerbation of breathlessness Breathlessness at end of life Breathlessness
NEUTROPENIC SEPSIS IN ADULT PATIENTS. Consultant Clinical Oncologist CLINICAL GUIDELINE
 Lancashire Teaching Hospitals NHS Foundation Trust NEUTROPENIC SEPSIS IN ADULT PATIENTS KEY WORDS (To assist in searching for the Guideline on the Intranet suggested minimum 10 words ) REF NO: Neutropenic
Lancashire Teaching Hospitals NHS Foundation Trust NEUTROPENIC SEPSIS IN ADULT PATIENTS KEY WORDS (To assist in searching for the Guideline on the Intranet suggested minimum 10 words ) REF NO: Neutropenic
Dr Ben Edwards Consultant Anaesthetist Sheffield Teaching Hospitals
 Dr Ben Edwards Consultant Anaesthetist Sheffield Teaching Hospitals 70-75,000 #NOF per annum (costs 2 billion) 10% die within 1 month 33% die within 1 year Operative delays >48hs more than doubles risk
Dr Ben Edwards Consultant Anaesthetist Sheffield Teaching Hospitals 70-75,000 #NOF per annum (costs 2 billion) 10% die within 1 month 33% die within 1 year Operative delays >48hs more than doubles risk
TACO CASE STUDIES RTC JUNE Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner
 TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
GUIDELINES FOR MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION WITH ORAL ANTICOAGULANTS
 GUIDELINES FOR MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION WITH ORAL ANTICOAGULANTS This guideline covers the management of patients being treated with Vitamin K antagonists (VKA): Warfarin Acenocoumarol
GUIDELINES FOR MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION WITH ORAL ANTICOAGULANTS This guideline covers the management of patients being treated with Vitamin K antagonists (VKA): Warfarin Acenocoumarol
HYDROXYCARBAMIDE for Haematological conditions (Adults)
 Shared Care Guideline DRUG: Introduction: Contraindications & Warnings: HYDROXYCARBAMIDE for Haematological conditions (Adults) Indication: Hydroxycarbamide is an established treatment in haematological
Shared Care Guideline DRUG: Introduction: Contraindications & Warnings: HYDROXYCARBAMIDE for Haematological conditions (Adults) Indication: Hydroxycarbamide is an established treatment in haematological
Right Iliac Fossa Pain
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Right Iliac Fossa Pain Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Right Iliac Fossa Pain Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
FOLFIRINOX (Irinotecan, Oxaliplatin & infusional Fluorouracil) Cumbria, Northumberland, Tyne & Wear Area Team
 DRUG ADMINISTRATION SCHEDULE Day Drug Dose Route Diluent & Rate Glucose 5% 250ml Infusion Fast Running for Line Flush Day 1 Ondansetron 8mg IV bolus Via dextrose drip Dexamethasone 8mg IV bolus Via dextrose
DRUG ADMINISTRATION SCHEDULE Day Drug Dose Route Diluent & Rate Glucose 5% 250ml Infusion Fast Running for Line Flush Day 1 Ondansetron 8mg IV bolus Via dextrose drip Dexamethasone 8mg IV bolus Via dextrose
Glucocorticoid replacement, Steroids, Acute Illness Dr Rupa Ahluwalia, Consultant Physician (NNUH)
 For Use in: By: For: Division responsible for document: Key words: Name and job title of document author s: Name and job tile of document author s Line Manager: Supported by: Assessed and approved by the:
For Use in: By: For: Division responsible for document: Key words: Name and job title of document author s: Name and job tile of document author s Line Manager: Supported by: Assessed and approved by the:
Pain Management for Adult sickle cell disease patients: Information for patients, relatives and carers
 Pain Management for Adult sickle cell disease patients: Information for patients, relatives and carers Why you should read this leaflet This leaflet will give you the information necessary to manage your
Pain Management for Adult sickle cell disease patients: Information for patients, relatives and carers Why you should read this leaflet This leaflet will give you the information necessary to manage your
Rivaroxaban film coated tablets are available in 2 strengths for this indication: 15mg and 20mg.
 Primary Care Prescriber Information RIVAROXABAN (XARELTO ) Treatment of acute venous thromboembolism and prevention of recurrent venous thromboembolism INDICATION Rivaroxaban is a non-vitamin K antagonist
Primary Care Prescriber Information RIVAROXABAN (XARELTO ) Treatment of acute venous thromboembolism and prevention of recurrent venous thromboembolism INDICATION Rivaroxaban is a non-vitamin K antagonist
This guideline describes the care required for a patient receiving a red blood cell transfusion whilst undergoing extra corporeal therapies.
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guidelines for care of a patient receiving a red blood cell transfusion whilst undergoing extra corporeal therapies.
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guidelines for care of a patient receiving a red blood cell transfusion whilst undergoing extra corporeal therapies.
Post-Op Complications. Dr Georgina Elliot FY2 Doctor Barts Health NHS Trust
 Post-Op Complications Dr Georgina Elliot FY2 Doctor Barts Health NHS Trust What we will cover Overview of common post-op complications and when they occur 4 cases of common post-op complications How to
Post-Op Complications Dr Georgina Elliot FY2 Doctor Barts Health NHS Trust What we will cover Overview of common post-op complications and when they occur 4 cases of common post-op complications How to
Patient Profile. Patient s details Initials: IF Age: 40 Gender: Male. Weight: 139.7kg Height: 510 metres BMI: >47
 Patient Profile Patient background and medication list Reason for selecting profile Interesting depression case whereby there were several opportunities for intervention as a pharmacist to ensure drug-related
Patient Profile Patient background and medication list Reason for selecting profile Interesting depression case whereby there were several opportunities for intervention as a pharmacist to ensure drug-related
Palliative care for heart failure patients. Susan Addie
 Palliative care for heart failure patients Susan Addie Treatments The most common limiting and distressing complaint is of fatigue and breathlessness. Optimal treatment strategies relieve symptoms, improves
Palliative care for heart failure patients Susan Addie Treatments The most common limiting and distressing complaint is of fatigue and breathlessness. Optimal treatment strategies relieve symptoms, improves
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc)
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Guideline on the management of excessive coumarin anticoagulation in adults
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Guideline on the management of excessive coumarin anticoagulation in adults
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086)
 Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Dr Banu Kaya Consultant Haematologist Barts Health NHS Trust Royal London Hospital, London, UK SICKLE CELL AND THALASSAEMIA OVERVIEW
 Dr Banu Kaya Consultant Haematologist Barts Health NHS Trust Royal London Hospital, London, UK SICKLE CELL AND THALASSAEMIA OVERVIEW Objectives Gain awareness of haemoglobinopathy inheritance, pathophysiology
Dr Banu Kaya Consultant Haematologist Barts Health NHS Trust Royal London Hospital, London, UK SICKLE CELL AND THALASSAEMIA OVERVIEW Objectives Gain awareness of haemoglobinopathy inheritance, pathophysiology
CAUTION: You must refer to the intranet for the most recent version of this procedural document.
 Procedure for the use of Intravenous Iron Dextran (CosmoFer ) Sharepoint Location Sharepoint Index Directory Clinical Policies and Guidelines General Policies and Guidelines/ Haematology And blood transfusion
Procedure for the use of Intravenous Iron Dextran (CosmoFer ) Sharepoint Location Sharepoint Index Directory Clinical Policies and Guidelines General Policies and Guidelines/ Haematology And blood transfusion
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
CLINICAL GUIDELINE FOR MANAGEMENT OF NEUTROPENIC SEPSIS IN ADULT CANCER PATIENTS (this guideline excludes haematology patients)
 CLINICAL GUIDELINE FOR MANAGEMENT OF NEUTROPENIC SEPSIS IN ADULT CANCER PATIENTS (this guideline excludes haematology patients) 1. Aim/Purpose of this Guideline 1.1. Systemic cancer treatments and immunological
CLINICAL GUIDELINE FOR MANAGEMENT OF NEUTROPENIC SEPSIS IN ADULT CANCER PATIENTS (this guideline excludes haematology patients) 1. Aim/Purpose of this Guideline 1.1. Systemic cancer treatments and immunological
ABDOMINAL PAIN (SEE ALSO ABDOMINAL AORTIC ANEURYSM)
 ABDOMINAL PAIN (SEE ALSO ABDOMINAL AORTIC ANEURYSM) Evaluating abdominal pain is difficult misdiagnosis of this symptom generates more formal complaints than any other clinical mistake made in our department.
ABDOMINAL PAIN (SEE ALSO ABDOMINAL AORTIC ANEURYSM) Evaluating abdominal pain is difficult misdiagnosis of this symptom generates more formal complaints than any other clinical mistake made in our department.
Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant
 Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant All medical RCC transfusions (but only 1 in 3 haematology or oncology cases) in 3 x one week periods Medical specialties include:
Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant All medical RCC transfusions (but only 1 in 3 haematology or oncology cases) in 3 x one week periods Medical specialties include:
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance)
 North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
Trust Guideline for the Management of: Condition or Procedure in Adults and / or Children
 Trust Guideline for the Management of: Condition or Procedure in Adults and / or Children A clinical guideline recommended For use in: By: For: Division responsible for document: Key words: Name of document
Trust Guideline for the Management of: Condition or Procedure in Adults and / or Children A clinical guideline recommended For use in: By: For: Division responsible for document: Key words: Name of document
A Clinical Guideline for the use of Intravenous Aminophylline in Acute Severe Asthma in Children
 For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
Title Protocol for the Management of Asthma in the Minor Injuries Units
 Document Control Title Protocol for the Management of Asthma in the Minor Injuries Units Author Karen Watts Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics
Document Control Title Protocol for the Management of Asthma in the Minor Injuries Units Author Karen Watts Author s job title Professional Lead, Minor Injuries Unit Directorate Emergency Services, Logistics
Clinical guideline for acute wheeze & asthma in children 5 years and over Hospital care
 Clinical guideline for acute wheeze & asthma in children years and over Hospital care Airedale NHS Trust Bradford Teaching Hospitals NHS Foundation Trust NHS Bradford and Airedale DOB: A&E/Hospital : Weight:
Clinical guideline for acute wheeze & asthma in children years and over Hospital care Airedale NHS Trust Bradford Teaching Hospitals NHS Foundation Trust NHS Bradford and Airedale DOB: A&E/Hospital : Weight:
Moving from child to adult sickle cell disease services
 What will happen when I move from child to adult? When you move over from child to adult sickle cell services you will be under the care of the Sickle Cell and Thalassaemia (SCaT) team at City Hospital.
What will happen when I move from child to adult? When you move over from child to adult sickle cell services you will be under the care of the Sickle Cell and Thalassaemia (SCaT) team at City Hospital.
Hydroxyurea (Hydroxycarbamide) - Guidelines for treating children with Sickle Cell Disease
 Hydroxyurea (Hydroxycarbamide) - Guidelines for treating children with Sickle Cell Disease Document Information Version: 2 Date: July 2014 Authors (incl. job title): Dr Moira Dick Consultant Paediatrician
Hydroxyurea (Hydroxycarbamide) - Guidelines for treating children with Sickle Cell Disease Document Information Version: 2 Date: July 2014 Authors (incl. job title): Dr Moira Dick Consultant Paediatrician
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
CLINICAL POLICY FOR THE USE OF INTRANASAL DIAMORPHINE FOR ANALGESIA IN CHILDREN ATTENDING THE PAEDIATRIC EMERGENCY DEPARTMENT, SASH
 CLINICAL POLICY FOR THE USE OF INTRANASAL DIAMORPHINE FOR ANALGESIA IN CHILDREN ATTENDING THE PAEDIATRIC EMERGENCY DEPARTMENT, SASH Background Adequate analgesia is a vital aspect of early management of
CLINICAL POLICY FOR THE USE OF INTRANASAL DIAMORPHINE FOR ANALGESIA IN CHILDREN ATTENDING THE PAEDIATRIC EMERGENCY DEPARTMENT, SASH Background Adequate analgesia is a vital aspect of early management of
Clinical guideline: manual red cell exchange in patients with sickle cell disease
 Clinical guideline: manual red cell exchange in patients with sickle cell disease HN-504b Introduction Most patients with sickle cell anaemia are relatively asymptomatic despite baseline Hb concentrations
Clinical guideline: manual red cell exchange in patients with sickle cell disease HN-504b Introduction Most patients with sickle cell anaemia are relatively asymptomatic despite baseline Hb concentrations
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques
 Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques 5850/5980 University Avenue, PO Box 9700 Halifax, NS, B3K 6R8 1.902.470.7429
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d Oncologie et Hématologie Pédiatrique des Provinces Atlantiques 5850/5980 University Avenue, PO Box 9700 Halifax, NS, B3K 6R8 1.902.470.7429
Fever in children aged less than 5 years
 Fever in children aged less than 5 years A fever is defined as a temperature greater than 38 degrees celsius Height and duration of fever do not identify serious illness. However fever in children younger
Fever in children aged less than 5 years A fever is defined as a temperature greater than 38 degrees celsius Height and duration of fever do not identify serious illness. However fever in children younger
Sickle Cell Disease. Edward Malters, MD
 Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
Sickle Cell Disease Edward Malters, MD Introduction Vaso-occlusive phenomena and hemolysis are the clinical hallmarks of Sickle Cell Disease (SCD) Inherited disorder due to homozygosity for the abnormal
Transfusion in Sickle Cell Disease What the guidelines [are likely to] say. Dr Bernard Davis Whittington Hospital, London
![Transfusion in Sickle Cell Disease What the guidelines [are likely to] say. Dr Bernard Davis Whittington Hospital, London Transfusion in Sickle Cell Disease What the guidelines [are likely to] say. Dr Bernard Davis Whittington Hospital, London](/thumbs/85/91702350.jpg) Transfusion in Sickle Cell Disease What the guidelines [are likely to] say Dr Bernard Davis Whittington Hospital, London Background to BCSH Guideline Rationale Current guidance in disparate publications
Transfusion in Sickle Cell Disease What the guidelines [are likely to] say Dr Bernard Davis Whittington Hospital, London Background to BCSH Guideline Rationale Current guidance in disparate publications
Paediatric Wheeze and pneumonia. RCH Asthma RCH bronchiolitis RCH pneumonia Dr S Rajapaksa
 Paediatric Wheeze and pneumonia RCH Asthma RCH bronchiolitis RCH pneumonia Dr S Rajapaksa Case Charlotte is a 2 ½ year old who presents to ED with shortness of breath and wheeze. She had been picked up
Paediatric Wheeze and pneumonia RCH Asthma RCH bronchiolitis RCH pneumonia Dr S Rajapaksa Case Charlotte is a 2 ½ year old who presents to ED with shortness of breath and wheeze. She had been picked up
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway
 Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
1.1.2 CPAP therapy is used for patients who are suffering from an acute type 1 respiratory failure (Pa02 <8kPa with a normal or low Pac02).
 Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
