SUB-GROUPING PATIENTS WITH NON-SPECIFIC LOW BACK PAIN BASED ON CLUSTER ANALYSIS OF DISCRIMINATORY CLINICAL ITEMS
|
|
|
- Esther Gordon
- 5 years ago
- Views:
Transcription
1 J Rehabil Med 2013; 45: ORIGINAL REPORT SUB-GROUPING PATIENTS WITH NON-SPECIFIC LOW BACK PAIN BASED ON CLUSTER ANALYSIS OF DISCRIMINATORY CLINICAL ITEMS Evdokia Billis, PhD 1,2, Christopher J. McCarthy, PhD 3, Chris Roberts, PhD 2, John Gliatis, MD 4, Maria Papandreou, PhD 5, George Gioftsos, PhD 6 and Jacqueline A. Oldham, PhD 2 From the 1 Department of Physiotherapy, Technological Educational Institute (TEI) of Patras, Greece, 2 University of Manchester, Manchester, 3 Imperial College Healthcare NHS Trust, London, UK, 4 Orthopaedic Department, University Hospital of Patras, 5 Department of Physiotherapy, Technological Educational Institute (TEI) of Athens and 6 Department of Physiotherapy, Technological Educational Institute (TEI) of Lamia, Greece Objective: To identify potential subgroups amongst patients with non-specific low back pain based on a consensus list of potentially discriminatory examination items. Design: Exploratory study. Participants: A convenience sample of 106 patients with nonspecific low back pain (43 males, 63 females, mean age 36 years, standard deviation 15.9 years) and 7 physiotherapists. Methods: Based on 3 focus groups and a two-round Delphi involving 23 health professionals and a random stratified sample of 150 physiotherapists, respectively, a comprehensive examination list comprising the most discriminatory items was compiled. Following reliability analysis, the most reliable clinical items were assessed with a sample of patients with non-specific low back pain. K-means cluster analysis was conducted for 2-, 3- and 4-cluster options to explore for meaningful homogenous subgroups. Results: The most clinically meaningful cluster was a twosubgroup option, comprising a small group (n = 24) with more severe clinical presentation (i.e. more widespread pain, functional and sleeping problems, other symptoms, increased investigations undertaken, more severe clinical signs, etc.) and a larger less dysfunctional group (n = 80). Conclusion: A number of potentially discriminatory clinical items were identified by health professionals and sub-classified, based on a sample of patients with non-specific low back pain, into two subgroups. However, further work is needed to validate this classification process. Key words: non-specific low back pain; classification; subgrouping; Greece; cluster analysis. J Rehabil Med 2013; 45: Guarantor s address: Evdokia Billis, Lecturer in Physiotherapy, Department of Physiotherapy, Branch Department of Aigion, Technological Educational Institute (TEI) of Patras, Psaron 6, Aigion, GR-25100, Greece. ebillis@teipat.gr Submitted May 11, 2011; accepted September 17, 2012 INTRODUCTION The classification of patients with non-specific low back pain (NSLBP) into subgroups has a number of advantages. First, this approach is thought to be superior in guiding treatment compared with other approaches (1 4). Secondly, classifying patients based on their signs and symptoms has demonstrated diagnostic success in studies investigating specific low back pain (LBP) (5) and is a feasible, practical, cost-effective and clinically applicable process. Finally, clinical reasoning is facilitated by the utilization of diagnostic/prognostic classification systems, especially in cases where a specific cause of disease is indefinable (e.g. in NSLBP) (6). However, a primary shortcoming of classification systems is their subjective nature. Most classification systems have been developed using a judgmental rather than a statistical approach (basing their development on small samples and relying on clinicians personal experience and expertise); therefore this is likely to bias the process, and reduce the generalizability of the results (7, 8). Furthermore, little work has been undertaken to address issues of reliability and to ensure agreement on the selection of discriminatory criteria for the classifying criteria. As such, many classification systems lack validity and reliability, and do not lead to confidence in the derived subgroup profiling. Thus, although there is emerging evidence that classification systems are the best method for diagnosing and/or guiding treatment for NSLBP, basic steps towards their development require further elaboration. In view of the high incidence of LBP in the general population and the lack of an established NSLBP taxonomy adopted by clinicians, it would seem appropriate to implement basic steps in subgroup development by trying to reach consensus on reliable clinical items that are believed to be discriminatory for identifying different NSLBP subsets. Consensus amongst experienced clinicians has important benefits. First, if a high level of consensus is reached, it is more likely that these agreed items will be useful and worth further consideration and study. It is also possible that these items will suggest a degree of discriminative validity in identifying LBP subsets. Secondly, the outcomes may facilitate cross-cultural comparisons, since cultural trends in the diagnosis of LBP are suggested across different settings (7, 9). Thus, the aims of this study, which forms the second part of a two-part series of studies, were to explore consensus on potentially discriminatory clinical items in a NSLBP assessment list, and to identify whether homogenous sub-groups are 2013 The Authors. doi: / Journal Compilation 2013 Foundation of Rehabilitation Information. ISSN
2 178 E. Billis et al. being developed. The initial study (10) reported the inter-tester reliability of this discriminatory list, enabling the identification of reliable items, which then formed the examination procedure for investigating sub-group developments. METHODS Sample A convenience sample of Greek patients with NSLBP was invited to participate in the study. Patients were diagnosed and referred for physiotherapy by specialist doctors (mostly orthopaedic specialists) working predominantly within the private sector. The evaluations took place in 3 different testing sites (physiotherapy clinics) within Greece (Athens, Patras and Lamia) and volunteers were recruited consecutively as they visited each clinic over a 10-month period. Patients were excluded if: (i) their native language was not Greek, (ii) their LBP was due to specific spinal pathology, (iii) they had undergone lumbar surgery, (iv) they were pregnant, or (v) they had severe neurological problems (that influenced their cognitive or motor performance). A total of 106 patients with LBP consented to participate. In addition, 7 physiotherapists (5 men, 2 women), clinically experienced in treating LBP, agreed to perform the assessments (2 based in Athens, 2 in Patras and 3 in Lamia). Ethical approval was obtained from the ethics committees of the Technological Educational Institute (TEI) of Lamia, Greece and the University of Manchester, UK. Testing procedure The first study accompanying this publication (10) reports the intertester reliability of a suggested discriminatory list, derived from the consensus of a large number of health professionals (11, 12). This reliability study enabled the identification of items that presented with a kappa value of 0.41 or more, corresponding to moderate and substantial/excellent agreement (13). These items were included in a final examination list. Items with kappa value of less than 0.41 were excluded from the examination, as they were considered to be of low reliability. In addition, items with almost perfect percentage agreement (for which kappas could not be computed) were not included; the reason for their exclusion was the non-existence of positive findings on these items, which indicated that they would not have any discriminative ability (14), and were thus discarded from the examination. Based on these criteria, the final examination list comprised 82 items (51 oral questions and 31 clinical tests). Thus, each physiotherapist (PT) conducted a full clinical examination (Appendix I), addressing the items that were deemed reliable, as reported in the accompanying study (10). In the first section of the examination, which involved history-taking, the PT read each question from the examination booklet and recorded the answers. The second section involved a detailed physical examination. All PTs were familiarized with each testing procedure, following a training session directed by the principal investigator. Training was accompanied by a booklet summarizing the key examination points. Each PT assessed 15 patients, except for one PT who assessed 16. In addition, self-administered outcome measures for pain, disability and psychosocial status, which had undergone a cross-cultural validated adaptation procedure into the Greek language, and were highly recommended for use in LBP studies (15, 16) were also administered to the sample. For each patient the whole evaluation procedure lasted approximately 40 min (15 min for the questionnaires and 25 min for the examination). Data analysis To investigate whether there were distinct clinical subgroups within the sample, a cluster analysis approach was utilized. Cluster analysis is an exploratory procedure that aims to classify data into subgroups (17). In this study, a K-means non-hierarchical cluster analysis approach was utilized; this method is considered appropriate for producing exactly K different cluster solutions of maximum possible distinction. However, as this procedure cannot indicate how many clusters exist in the given data, in order to obtain an indication of the possible clustered options, hierarchical clustered modelling (14) was applied initially, and the dendrogram (formed by the hierarchical clustering) suggested further investigation of 2 6 cluster solutions. In addition, from the cluster analysis of 4 memberships, two of the groups contained two patients each, whose characteristics did not appear to be clinically different from the other two subgroup options. Thus, as this 4 membership option was not able to provide clinically meaningful results, a decision was made to stop the statistical cluster analysis at the 4 membership option. Thus, a K-means cluster analysis was carried out from 2- up to 4-group membership. K-means clustering generates an analysis of variance (ANOVA) table, whereby the mean on each item (for each cluster option) was explored to assess how distinct the within-cluster Table I. Characteristics of patients with non-specific low back pain (n = 106) Characteristics % (n) Outcome measures Mean (SD) Male 40.6 (43) VAS Present pain intensity 3.31 (2.63) Married/living with partner 47.2 (50) VAS Average pain intensity 4.11 (2.33) Urban place of stay 73.6 (78) VAS Pain at best 1.25 (1.44) Work VAS Pain at worst 7.52 (2.05) Public sector 26.4 (28) Private sector 30.1 (32) RMDQ 6.48 (5.17) Sedentary (e.g. secretary) 25.5 (27) Active/manual occupation 25.4 (27) ODI (15.28) Housewife/pensioner/student 49 (52) Health professionals seen FABQ Work (11.29) Specialist (orthopaedic, neurosurgeon etc.) 39.4 (42) FABQ Physical Activity (6.11) Physiotherapist 50.1 (54) Bed rest, days HAD Anxiety subscale 7.92 (4.35) (6) HAD Depression subscale 4.37 (3.11) (8) > (20) PCS Rumination 7.86 (4.67) Sick leave 3.8 (4) PCS Magnification 4.01 (3.03) Claiming compensation 0 (0) PCS Helplessness 7.48 (5.62) SD: standard deviation; VAS: visual analogue scale (0 10), RMDQ: Roland-Morris Disability Questionnaire (0 24), ODI: Oswestry Disability Index (0 100), FABQ: Fear-Avoidance Beliefs Questionnaire (FABQ Work: 0 42, FABQ Physical Activity: 0 24), HAD: Hospital Anxiety and Depression Scale (HAD subscales: 0 21), PCS: Pain Catastrophizing Scale (PCS Rumination: 0 16; PCS Magnification: 0 12; PCS Helplessness: 0 24).
3 Sub-grouping NSLBP patients using cluster analysis 179 differences were in relation to the p-value and the magnitude of the F values. Thus, both F and p-values were used for descriptive purposes. Statistically significant p-values set at 95% level (p < 0.05) were also used to distinguish between items. Cross-tabulations on each item within each cluster solution were also utilized as a means to determine whether observed differences in magnitude across the clusters were clinically important in size; and from the resulting χ 2 values the strength of association of each variable assigned to each group was tested. Finally, the distribution of each item across the subgroups was used. All data were analysed in SPSS (version 15.0). RESULTS A total of 106 patients (43 males, 63 females) participated in the study, mean age 36 years (standard deviation (SD) 15.9 years, age range years). Fifty-eight patients (54.7%) had LBP for more than 12 weeks and, for most of them (87.7%), the pain was of a recurrent nature. The sample s profile and main examination findings are shown in Tables I and II, respectively. The examinations were conducted by 7 PTs with mean clinical experience with LBP of 11.8 years (range 7 19 years). K-means cluster analysis generated an ANOVA table, whereby each item s mean explored how distinct the clusters were. For each cluster option 104 patients were finally computed (2 were missed due to missing data). Two-cluster option The 2-subgroup option consisted of a small group of 24 patients with NSLBP and a larger group of 80 patients with NSLBP. A total of 29 items (21 from the patient s history and 8 from physical examination) yielded statistically significant values. The small group (Group 1) had greater severity in their presentation and outcome measures scores compared with Group 2. More than half of this subgroup s patients had pins and needles (58.3%), neck pain (75%), restricted lumbar movements ( %) and had their lumbar spines radiographed (83.3%), as opposed to less than half from the larger group ( %) with these Table II. Characteristics of the sample s symptoms and clinical presentation (n = 106) Clinical presentation characteristics % (n) Clinical examination findings % (n) Pain location Posture Mainly in the back 83.0 (88) Normal 29.2 (31) Mainly in the leg 10.4 (11) Lordotic 34.0 (36) L-sided back pain (body chart) 71.7 (76) Active movements (lumbar) R-sided back pain (body chart) 68.9 (73) Pain in flexion 33.0 (35) L buttock pain (body chart) 38.7 (41) Pain in extension 42.5 (45) R buttock pain (body chart) 34.9 (37) Pain in right-side flexion 17.9 (19) L foot (sole) pain (body chart) 7.5 (8) Centralization in flexion 38.7 (41) L foot pain (dorsum) (body chart) 2.8 (3) Combined movements Type of pain Restricted extension with R SF 38.7 (41) Dull 38.7 (41) Restricted extension with L SF 49.1 (52) Deep 69.8 (74) Pain in flexion with R SF 19.8 (21) Sharp 45.3 (48) Pain in extension with R SF 40.6 (43) Diffuse 34 (36) Pain in extension with L SF 47.2 (50) Pain and activity Restricted posterior pelvic tilt 37.7 (40) Mainly at rest 60.4 (64) Accessory (P A) movements Mainly in motion 55.7 (59) L1 pain reproduction 13.2 (14) Relieving positions Lying ) S1 pain reproduction 22.6 (24) Aggravating position Sitting 34.0 (36) Palpation (trigger points, etc.) Aggravating position Lying 15.1 (16) Upper lumbar area 22.6 (24) Chronicity of episode Sacroiliac area 24.5 (26) Chronic (over 12 weeks) 54.7 (58) Neurological examination Recurrent episode 87.7 (93) L2 dermatome abnormality 4.7 (5) LBP getting better 50.0 (53) L3 dermatome abnormality 4.7 (5) Diurnal pattern L4 dermatome abnormality 12.3 (13) Pain waking at night 18.9 (20) SLR Pain reproduction (positive test) 14.2 (15) Pain worse in the morning 42.5 (45) SLR Positive neurodynamic 18.9 (20) Other symptoms Therapists clinical impression Stiffness 44.3 (47) Closing pattern 45.3 (48) Pins and needles 32.1 (34) Impairment dysfunction 34.0 (36) Investigations Good prognosis for recovery 91.5 (97) Radiographs (X-ray) 52.8 (56) Biomedical domain of influence 91.5 (97) MRI 25.5 (27) Psychological/social domain of influence 6.5 (7) Medical history and other problems Neck ache 46.2 (49) Other musculoskeletal (deformity, leg length) 28.3 (30) Work and function Hobbies severely affected by LBP 40.6 (43) Daily activities severely affected by LBP 30.2 (32) Psychosocial exaggerated pain behaviour 39.6 (42) LBP: low back pain; L: left; R: right; SF: side flexion; MRI: magnetic resonance imaging; P-A: posteroanterior (glide); SLR: straight leg raise.
4 180 E. Billis et al. symptoms. In addition, the smaller group comprised more patients with deep pain, predominant leg pain, aggravation in lying and night pain. Two pain location items (left foot and anterior leg pain) were present in larger percentages (20.8% and 12.5%) in the small group compared with the larger one (3.7% and 0%), indicating greater peripheralization of symptoms. A larger proportion of the small group presented with stiffness (66.7%) and dragging feet (25%) and had undertaken MRI diagnostic tests (40%) compared with the larger group (36.2%, 2.5% and 18.7%, respectively). In addition, straight leg raise (SLR) presented with pain and positive responses in 33.3% and 37.5%, respectively, in the small group, compared with the large one (8.7% and 13.8%, respectively). Table III summarizes the ANOVA outputs, χ 2 scores and clinical item distributions for the two membership option (due to the large volume of data, 82 items being included, only statistically significant items are presented). Three-cluster option The 3-cluster option comprised a large group of patients (n = 73) and 2 smaller ones (n = 9 and n = 22 patients, respectively). Twenty-two history and 8 physical examination items achieved statistical significance. From the distribution of outcomes and clinical features, one of the groups (n = 22) appeared more severe compared with the other two groups in terms of referred and widespread (i.e. neck) pain, other symptoms, recurrent episodes, investigations and restricted movement. However, the other groups did not show any consistent differences (indicative of a particular pattern) in their characteristics. Table III. Cluster analysis output for 2 subgroups (presenting the items with p < 0.05) F-value χ 2 -test Group 1 (n = 24) Group 2 (n = 80) Clinical items, n (%) Left foot (sole) pain (body chart) (20.8) 3 (3.7) Left anterior leg pain (body chart) (12.5) 0 (0) Left foot pain in dorsum (body chart) (12.5) 0 (0) Deep pain (91.7) 50 (62.5) Mainly in back (pain) < (54.7) 74 (92.5) Mainly in leg (pain) < (33.3) 2 (2.5) Relieving position Lying (83.3) 44 (55) Aggravating position Lying (33.3) 7 (8.7) Pain getting worse (29.2) 9 (11.2) Diurnal Pain waking at night (40) 9 (11.2) Diurnal Pain preventing from sleeping < (37.5) 3 (3.7) Other symptoms Stiffness (66.7) 29 (36.2) Other symptoms Pins and needles (58.3) 19 (23.7) Other symptoms Dragging feet < (25) 2 (2.5) Investigations X-ray performed < (83.3) 34 (42.5) Investigations MRI performed (40) 15 (18.7) Investigations Other investigations performed < (37.5) 4 (5) Type of work Sedentary type (20.8) 43 (53.7) Type of work Involving carrying weights (25) 6 (7.5) Daily physical activities severely affected (58.3) 18 (22.5) Musculoskeletal problems Neck ache (75) 30 (37.5) Combined movements Restricted extension with R SF (66.7) 23 (28.7) Combined movements Restricted extension with L SF (62.5) 26 (32.5) Combined movements Painful flexion with R SF (66.7) 35 (43.7) Ba Posterior pelvic tilt-restricted (37.5) 12 (15) SLR Pain reproduction (33.3) 7 (8.7) SLR Positive neurodynamic test (37.5) 11 (13.8) P A glides Pain in L (25) 7 (8.7) Prognosis (83.3) 77 (96.2) Outcome measures, mean (SD) VAS Present pain intensity 4.86 (2.74) 2.96 (2.45) VAS Average pain intensity 6.83 (1.87) 3.55 (2.19) VAS Pain at best 2.46 (1.8) 1.08 (1.4) VAS Pain at worst 8.59 (1) 7.15 (2.25) Roland-Morris Disability Questionnaire (7.3) 5.98 (4.9) Oswestry Disability Index (ODI) (18.9) (14.13) FABQ Work (8.39) (12) FABQ Physical Activity (5.61) (6.06) HADS Anxiety 8.46 (4.84) 7.27 (4.03) HADS Depression 5.92 (3.63) 3.67 (2.62) PCS (total) (13.06) (10.76) MRI: magnetic resonance imaging; R: right; L: left; SF: side flexion; SLR: straight leg raise; P A: posteroanterior (glide); SD: standard deviation; VAS: visual analogue scale; FABQ: Fear-Avoidance Beliefs Questionnaire; HADS: Hospital Anxiety Depression Scale; PCS: Pain Catastrophizing Scale.
5 Sub-grouping NSLBP patients using cluster analysis 181 Four-cluster option The 4-subgroup option entailed a large group (n = 79), a smaller one (n = 21) and two 2-patient groups. Eighteen out of 36 items achieved statistical significance; however, in view of the limited number of patients in the two subgroups, consistent distribution patterns or distinctive characteristics across groups were not obtained. DISCUSSION This study aimed to explore a list of reliable and potentially discriminatory items for NSLBP, on their ability to distinguish amongst different patient subsets. The sample utilized was predominantly recruited by medical referrals from the private sector, which is well developed in Greece (18), and consisted of a mix of patients with acute and chronic LBP, who were moderately disabled by LBP. The sample s profile had comparable features to that of some previous classification studies (19, 20), and a marginally less severe clinical profile compared with some others (21). Following cluster analysis within the 2-cluster option, the small group had a more severe clinical profile compared with the larger group. Based on the distribution of the clinical items on the 3- and 4-cluster options, it could be argued that they both included a small and a larger group that possessed similarities to the 2-subgroup option. However, in the 3-cluster option one of the smaller groups was not distinctively different to the other two, whereas for the 4-group option, two of the groups were extremely small and their distribution patterns did not subsequently indicate any clinically meaningful solutions. Thus, given the above information, the 2-subgroup option provided the most comprehensible and clinically meaningful presentation profiles (compared with the other 2-cluster options). Furthermore, despite outcome measures not being included in the cluster model, the scores for the small group on the outcomes of pain intensity, disability, anxiety, etc. were much higher, further verifying the presence of more severe cases in this group. Although direct comparisons between this study s two subgroups and previous classification reports are difficult to perform with accuracy due to methodological differences, some similarities are evident. Pain location, aggravating factors, 24-h pain patterns, pain response to movement, and symptom duration are criteria included in several European (19, 22, 23), Canadian (24), New Zealand (25) and US (26) studies. Similarly, a wide range of physical features have been utilized, most common of which are SLR (22 24, 27) and lumbar mobility pain provocation tests (28, 29). These similarities give weight to the inclusion of these factors in such classification approaches. From the studies limited to 2 3 subgroups, comparisons are still difficult due to variability in their designs and lack of reported detail on item distribution across the generated groups. Whilst Langworthy & Green (30) identified 3 criteria with similarity to this study (pain getting worse, night pain and exacerbation in lying), the subgroups distribution on these items was not detailed. Similarly, despite the interesting results in the study by Hill et al. (21) comparing 2 validated questionnaire instruments in their ability to identify subgroups requiring early intervention, limited information was given on their subgroups distribution characteristics. McCarthy et al. (19) were the only group that adopted a similar approach to this study and generated similar results. Their cluster analysis pointed towards two subgroups; a smaller more dysfunctional one (called the hypervigilant group), and a larger (less dysfunctional) one. Distribution of age, gender and outcome measures across their subgroups was comparable with this study. In addition, distribution on several clinical items (i.e. SLR test, upper lumbar palpation, pain provocation tests) pointed towards more positive (severe) responses for the hypervigilant group. The presence of a UK study (19) with similarities to this Greek one provides some confidence in our results, and their possible generalizability in wider population samples. Some issues were of clinical importance. First, a large set of signs, symptoms and clinical measures have been utilized. Secondly, most previous classification studies lack the standards required to be deemed methodologically rigorous (i.e. lack of statistically developing clusters, utilization of empirical methods, lack of item reliability, etc.). Thirdly, apart from utilizing a statistical procedure for generating subgroups, which is considered more sophisticated than utilizing other methods (i.e. observational or judgmental approaches) (8), the present study selected items suggested to be discriminatory by a consensus procedure involving a large and representative sample of health professionals dealing with NSLBP within Greece (11). In addition, only the most reliable of these selected items were utilized (10) in order to improve confidence and objectivity in outcomes. In addition, this study aimed to provide a meaningful, practical and useful taxonomy within the Greek healthcare setting. In view of existing cultural variations (7), it has not been assumed that classification systems developed in a given cultural setting can be adopted and utilized in the Greek setting. Therefore, this exploratory study tried to develop clinical subgroups based on practical, clinically applicable, reliable and generalizable classifying criteria. However, whether this approach is clinically useful as an assessment-based process for targeting treatment or as a prognostic guiding path is currently untested and needs to be further investigated. In terms of the methodology utilized, the K-means cluster approach was considered more appropriate than a hierarchical one because it is easy to use, reliable (no multiplicity effects, repeatable cluster generation, etc.), has the ability to produce distinct non-overlapping clusters (14, 17) and has been used in LBP exploratory studies (23, 30, 31). However, in view of its limitation in indicating a priori the exact number of existing clusters, a second clustering approach, the hierarchical method, a commonly used adjunct approach (17, 32), was utilized to verify the generated clusters and increase the validity of the findings (14). In addition, interpretation of the resulting partitions by descriptive means (as shown in Table III) was conducted, as recommended, for evaluating their clusters clinical utility (14). However, whilst cluster analysis has merit as a data-driven analysis procedure (as indicated above), it has pointed towards a relatively simple model of analysis,
6 182 E. Billis et al. which can provide only basic discrimination of data. Thus, given the complexity of the NSLBP problem, as well as the fact that there is currently no optimal classification scheme, it appears that further testing is required in order to ensure reproducibility and enhance credibility of the study s subgroups. Perhaps utilizing more complex analyses (such as neural networks or data-mining) or even combining approaches, to allow subgroups comparison and observation of similarities and differences between approaches would be desirable and beneficial. Interestingly, in Kent et al. s review (33) on the research methods utilized for sub-grouping LBP, they proposed a method framework comprising 6 stages, including hypothesis setting and testing studies, validation studies, as well as impact analyses studies. They highlighted the need for sub-grouping research to proceed through all phases of study, in order for the developed subgroups to gain credibility, generalizability and applicability within clinical practice. A limitation of the present study is that most discriminatory items utilized were biomedically based despite the profound role of psychosocial factors in NSLBP (34, 35). Psychosocial factors were excluded on the basis of their poor reliability. Nevertheless, certain social factors (work, hobbies, physical activities, etc.) and the psychosocial measures scores (Hospital Anxiety and Depression Scale, Fear-Avoidance Beliefs Questionnaire, Pain Catastrophizing Scale, presented in Table I) differed across the two groups, indicating greater psychosocial overlay for the small group compared with the large one. Interestingly, only 4 studies incorporated biopsychosocial elements in their classification (36 39); yet, they were utilized in a very different and, consequently, non-comparable way. Another limitation concerns the sample utilized, which was limited in terms of representing the more disabled patients; the presenting sample consisted of LBP patients with, in general, low levels of disability. This could have precluded the potential development of another subgroup with more dysfunctional features. However, this exploratory study constitutes only the first step towards developing a classification system within a particular cultural context. In conclusion, this cross-sectional exploratory study identified the existence of two distinct subgroups by utilizing a cluster analysis approach; a small group with more severe and widespread clinical signs and symptoms, and a large group with low severity, dysfunction and symptom presentation. This preliminary study forms the first step in developing a classification system within Greece based on discriminatory and reliable clinical criteria. However, despite its advantages, cluster analysis provides a simplistic method of subgroup research, and further work should thus explore each subgroup s clinical and diagnostic utility, in larger samples. ACKNOWLEDGEMENTS The authors would like to thank physiotherapists Ioannis Stathopoulos, Panagiotis Trigkas, Savvas Spanos, George Krekoukias and Nikolaos Strimpakos, as well as all the patients who participated in this study. This research was funded by the Manipulation Association of Chartered Physiotherapist s Elsevier Science and Doctoral Awards for Research in Manipulative Physiotherapy. REFERENCES 1. Fritz JM, Delitto A, Erhard RE. Comparison of classification-based physical therapy with therapy based on clinical practice guidelines for patients with acute low back pain: a randomized clinical trial. Spine 2003; 28: Brennan GP, Fritz JM, Hunter SJ, Thackeray A, Delitto A, Erhard RE. Identifying subgroups of patients with acute/subacute nonspecific low back pain: results of a randomized clinical trial. Spine 2006; 31: Childs JD, Fritz JM, Flynn TW, Irrgang JJ, Johnson KK, Majkowski GR, et al. A clinical prediction rule to identify patients with low back pain most likely to benefit from spinal manipulation: a validation study. Ann Intern Med 2004; 141: Kent P, Mjosund HL, Petersen DHD. Does targeting manual therapy and/or exercse improve patient outcomes in nonspecific low back pain? A systematic review. BMC Medicine 2010; 18: Vroomen PC, de Krom MC, Knottnerus JA. Diagnostic value of history and physical examination in patients suspected of sciatica due to disc herniation: a systematic review. J Neurol 1999; 246: Kent P, Keating JL. Classification in nonspecific low back pain: what methods do primary care clinicians currently use? Spine 2005; 30: Billis EV, McCarthy CJ, Oldham JA. Subclassification of low back pain: a cross-country comparison. Eur Spine J 2007; 16: Riddle DL. Classification and low back pain: a review of the literature and critical analysis of selected systems. Phys Ther 1998; 78: Aceves-Avila FJ, Ferrari R, Ramos-Remus C. New insights into culture driven disorders. Best Pract Res Clin Rheumatol 2004; 18: Billis E, McCarthy CJ, Gliatis J, Gittins M, Papandreou M, Oldham JA. Inter-tester reliability of discriminatory examination items for sub-classifying non-specific low back pain. J Rehabil Med 2012; 44: Billis E, McCarthy CJ, Gliatis J, Stathopoulos I, Papandreou M, Oldham JA. Which are the most important discriminatory items for subclassifying non-specific low back pain? A Delphi study among Greek health professionals. J Eval Clin Pract 2010; 16: Billis EV, McCarthy CJ, Stathopoulos I, Kapreli E, Pantzou P, Oldham JA. The clinical and cultural factors in classifying low back pain patients within Greece: a qualitative exploration of Greek health professionals. J Eval Clin Pract 2007; 13: Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics 1977; 33: Milligan GW, Cooper MC. Methodology review: clustering methods. Appl Psychol Meas 1987; 11: Pincus T, Santos R, Breen A, Burton AK, Underwood M. A review and proposal for a core set of factors for prospective cohorts in low back pain: a consensus statement. Arthritis Rheum 2008; 59: Bombardier C. Outcome assessments in the evaluation of treatment of spinal disorders: summary and general recommendations. Spine 2000; 25: Everitt BS, Landau S, Leese M. Cluster analysis. London: Arnold; Siskou O, Kaitelidou D, Papakonstantinou V, Liaropoulos L. Private health expenditure in the Greek health care system: where truth ends and the myth begins. Health Policy 2008; 88: McCarthy CJ, Roberts C, Gittins M, Oldham JA. A process of subgroup identification in non-specific low back pain using a standard clinical examination and cluster analysis. Physiother Res Int 2012; 2: George SZ, Delitto A. Clinical examination variables discriminate among treatment-based classification groups: a study of construct validity in patients with acute low back pain. Phys Ther 2005; 85: Hill JC, Dunn KM, Main CJ, Hay EM. Subgrouping low back pain:
7 Sub-grouping NSLBP patients using cluster analysis 183 a comparison of the STarT Back Tool with the Orebro Musculoskeletal Pain Screening Questionnaire. Eur J Pain 2010; 14: Coste J, Paolaggi JB, Spira A. Classification of nonspecific low back pain. II. Clinical diversity of organic forms. Spine 1992; 17: Coste J, Paolaggi JB, Spira A. Classification of nonspecific low back pain. I. Psychological involvement in low back pain. A clinical, descriptive approach. Spine 1992; 17: Spitzer W, LeBlanc F, Depuis M. Scientific approach to the assessment and management of activity related spinal disorders: report of the Quebec Task Force on Spinal Disorders. Spine 1987; 12: S16 S McKenzie R. The lumbar spine: mechanical diagnosis and therapy. Waikanae: Spinal Publications Ltd; Fritz JM, Cleland JA, Childs JD. Subgrouping patients with low back pain: evolution of a classification approach to physical therapy. J Orthop Sports Phys Ther 2007; 37: Bertilson BC, Bring J, Sjoblom A, Sundell K, Strender LE. Interexaminer reliability in the assessment of low back pain (LBP) using the Kirkaldy-Willis classification (KWC). Eur Spine J 2006; 15: McKenzie R. Subgroups in non specific spinal disorders. In: McKenzie R, editor. The lumbar spine: mechanical diagnosis and therapy. Waikanae: Spinal Publications Ltd; 1981, p Van Dillen LR, Sahrmann SA, Norton BJ, Caldwell CA, Mc- Donnell MK, Bloom NJ. Movement system impairment-based categories for low back pain: stage 1 validation. J Orthop Sports Phys Ther 2003; 33: Langworthy JM, Breen AC. Rationalizing back pain: the development of a classification system through cluster analysis. J Manipulative Physiol Ther 1997; 20: Bergstrom G, Bodin L, Jensen IB, Linton SJ, Nygren AL. Longterm, non-specific spinal pain: reliable and valid subgroups of patients. Behav Res Ther 2001; 39: Gironda RJ, Clark ME. Cluster analysis of the pain outcomes questionnaire. Pain Med 2008; 9: Kent P, Keating J, Leboeuf-Yde C. Research methods for subgrouping low back pain. BMC Med Res Methodol 2010; 10: Clays E, De BD, Leynen F, Kornitzer M, Kittel F, De BG. The impact of psychosocial factors on low back pain: longitudinal results from the Belstress study. Spine 2007; 32: Pincus T, Burton AK, Vogel S, Field AP. A systematic review of psychological factors as predictors of chronicity/disability in prospective cohorts of low back pain. Spine 2002; 27: E109 E Huyse FJ, Lyons JS, Stiefel FC, Slaets JP, de Jonge P, Fink P, et al. INTERMED : a method to assess health service needs. I. Development and reliability. Gen Hosp Psychiatry 1999; 21: Hill JC, Dunn KM, Lewis M, Mullis R, Main CJ, Foster NE, et al. A primary care back pain screening tool: identifying patient subgroups for initial treatment. Arthritis Rheum 2008; 59: O Sullivan P. Diagnosis and classification of chronic low back pain disorders: maladaptive movement and motor control impairments as underlying mechanism. Man Ther 2005; 10: Harper AC, Harper DA, Lambert LJ, Andrews HB, Lo SK, Ross FM, et al. Symptoms of impairment, disability and handicap in low back pain: a taxonomy. Pain 1992; 50:
8 184 E. Billis et al. Appendix I. Examination list Α. HISTORY 1. PRESENT SYMPTOMS BODY CHART. Please locate areas of pain, referred pain, etc. (A body chart diagram divided into 20 consecutively numbered body areas, for description of pain was provided) QUALITY OF PAIN. How would you describe your pain? Dull ache YES NO Intense pain YES NO Superficial YES NO Deep ache YES NO Sharp YES NO Diffuse YES NO Localized YES NO Mainly in the leg YES NO Mainly in the back YES NO PAIN BEHAVIOUR & POSTURES/ACTIVITIES When do you get your pain? At rest YES NO When moving/during movement YES NO Describe your most relieving position/activity Bending YES NO Sitting YES NO Standing YES NO Lying (describe position) YES NO Describe your most aggravating position/activity Bending YES NO Sitting YES NO Lying (describe position) YES NO Other: PAIN STATUS Is the pain getting better? YES NO Is the pain staying the same? YES NO Is the pain getting worse? YES NO 24-HOUR PAIN BEHAVIOUR. When do you mostly get your primary pain? Waking them at night YES NO Preventing them from getting back or getting to sleep YES NO Worse in the morning YES NO Worse in the evening YES NO CHARACTERISTICS OF OTHER SYMPTOMS Any symptoms other than pain? (Mark areas in body chart) Stiffness YES NO Pins and needles YES NO Dragging feet YES NO 2 HISTORY OF CONDITION/SYMPTOMS When did the symptoms start? months INVESTIGATIONS X-ray YES NO Blood tests YES NO MRI YES NO Other YES NO Is this the first pain episode? If YES go to section 3 YES NO PREVIOUS EPISODES Was previous episode(s) of the same type? YES NO 3 FUNCTION TYPE OF WORK. Describe the type of work Primarily sedentary YES NO Primarily repetitive movements YES NO Primarily carrying weights YES NO HOBBIES & DAILY ACTIVITIES Does the back problem severely affect the patient's hobbies? YES NO Describe how: Does the back problem severely affect the patient's level of daily physical activity? Describe how: YES NO 4 MEDICAL HISTORY
9 Sub-grouping NSLBP patients using cluster analysis 185 DRUG HISTORY Does any drug affect his back problem? YES NO Doses of NSAIDs If patient takes NSAIDs is the dose high? YES NO Dose: OTHER MUSCULOSKELETAL PROBLEMS Neck pain YES NO Leg length inequality YES NO PREVIOUS SURGERY YES NO Describe: GYNAECOLOGICAL HISTORY Does the patient have any menstrual or hormonal problems linked to the LBP? YES NO POST-NATAL BACKACHE Is the current linked with post-natal backache? YES NO 5 PSYCHOSOCIAL HISTORY Is the patient's behaviour affected by the following: Strongly Agree PAIN BEHAVIOUR OF THE PATIENT (i.e. fear of pain, expectation of pain to increase with activity/work, belief that pain is uncontrollable/harmful/hypervigilance, etc.) PSYCHOLOGICAL & EMOTIONAL STATUS Impact of patient's problem towards psychological status Does patient believe he has a pathological condition? Is patient clear of what things make him better/ worse? Neither agree Disagree Strongly agree nor disagree disagree Β. CLINICAL EXAMINATION Standing 6 OBSERVATION OF POSTURE. What posture best describes the patient? Normal YES NO Lordotic YES NO 7 ACTIVE MOVEMENTS LUMBAR RANGE HYPERMOBILE NORMAL RESTRICTED PAIN REPRODUCTION Flexion YES NO Extension YES NO Right-side flexion YES NO REPEATED MOVEMENTS Peripheralizing/ increasing symptoms No change Centralizing/reducing or alleviating symptoms Lumbar flexion COMBINED MOVEMENTS RESTRICTION PAIN REPRODUCTION Flexion with right-side flexion YES NO YES NO Extension with right-side flexion YES NO YES NO Extension with left-side flexion YES NO YES NO Based on the above movements the patient presents with Closing pattern YES NO Impairment dysfunction YES NO Supine 7 Active movements (continued) pelvic ROM Hypermobile Normal Restricted Reproducing pain Posterior pelvic tilt YES NO 8 NEUROLOGICAL EXAMINATION. Response of symptomatic side Symptomatic side: LEFT RIGHT SENSATION ABSENT REDUCED NORMAL HYPERSENSITIVE L2 L3 L4 NEURODYNAMIC TESTS VERY LIMITED LIMITED NORMAL Reproducing pain Positive response SLR YES NO YES NO Prone 9 PASSIVE JOINT ASSESSMENT & PALPATION ACCESSORY MOVEMENTS (P-A glides) Hypermobile Normal Restricted Increases symptoms / reproducing pain L1 YES NO S1 YES NO PALPATION (checking for tenderness, trigger points, etc.) Upper lumbar paraspinal areas YES NO Sacro-iliac area YES NO 10 CLINICAL REASONING Domain with strongest influence of patient's symptoms? Biomedical Psychological Social Prognosis? Good Poor P A: posteroanterior (glide); ROM: range of motion; LBP: low back pain; MRI: magnetic resonance imaging; NSAIDs: non-steroidal anti-inflammatory drugs.
Stynes, et al. (2016). Classification of patients with low back-related leg pain: a systematic review. BMC Musculoskeletal Disorders; 17:226
 The McKenzie Institute International 2016 Vol. 5, No. 2 LITERATURE REVIEWS Summary and Perspective of Recent Literature Paul Nelson, PT, Dip. MDT Stynes, et al. (2016). Classification of patients with
The McKenzie Institute International 2016 Vol. 5, No. 2 LITERATURE REVIEWS Summary and Perspective of Recent Literature Paul Nelson, PT, Dip. MDT Stynes, et al. (2016). Classification of patients with
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
DEVELOPMENT OF A CLINICAL EXAMINATION IN NON-SPECIFIC LOW BACK PAIN: A DELPHI TECHNIQUE
 J Rehabil Med 2006; 38: 263267 DEVELOPMENT OF A CLINICAL EXAMINATION IN NON-SPECIFIC LOW BACK PAIN: A DELPHI TECHNIQUE Christopher J. McCarthy, PhD 1, Alison Rushton, EdD 2, Vicky Billis, MSc 1, Frances
J Rehabil Med 2006; 38: 263267 DEVELOPMENT OF A CLINICAL EXAMINATION IN NON-SPECIFIC LOW BACK PAIN: A DELPHI TECHNIQUE Christopher J. McCarthy, PhD 1, Alison Rushton, EdD 2, Vicky Billis, MSc 1, Frances
A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT
 LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
COMPARISON BETWEEN THE EFFECTIVENESS OF MCKENZIE EXTENSION EXERCISES AND WILLIAM FLEXION EXERCISES FOR TREATMENT OF NON-SPECIFIC LOW BACK PAIN
 Original Article COMPARISON BETWEEN THE EFFECTIVENESS OF MCKENZIE EXTENSION EXERCISES AND WILLIAM FLEXION EXERCISES FOR TREATMENT OF NON-SPECIFIC LOW BACK PAIN Qurat-ul-Ain*, Iqra ishaq** *Physiotherapist
Original Article COMPARISON BETWEEN THE EFFECTIVENESS OF MCKENZIE EXTENSION EXERCISES AND WILLIAM FLEXION EXERCISES FOR TREATMENT OF NON-SPECIFIC LOW BACK PAIN Qurat-ul-Ain*, Iqra ishaq** *Physiotherapist
LUMBAR SPINE CASE 3. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1. L4-5, 5-S1 disc, facet (somatic)
 LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
Functional Tools Pain and Activity Questionnaire
 Job dissatisfaction (Bigos, Battie et al. 1991; Papageorgiou, Macfarlane et al. 1997; Thomas, Silman et al. 1999; Linton 2001), fear avoidance and pain catastrophizing (Ciccone and Just 2001; Fritz, George
Job dissatisfaction (Bigos, Battie et al. 1991; Papageorgiou, Macfarlane et al. 1997; Thomas, Silman et al. 1999; Linton 2001), fear avoidance and pain catastrophizing (Ciccone and Just 2001; Fritz, George
Supplementary Online Content
 Supplementary Online Content Fritz JM, Magel JS, McFadden M, et al. Early physical therapy vs usual care in patients with recent onset low back pain: a randomized clinical trial. JAMA. doi:10.1001/jama.2015.11648.
Supplementary Online Content Fritz JM, Magel JS, McFadden M, et al. Early physical therapy vs usual care in patients with recent onset low back pain: a randomized clinical trial. JAMA. doi:10.1001/jama.2015.11648.
Dethroning the Clinical Prediction Rule WPTA Fall Conference 2017
 Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
ORIGINAL CONTRIBUTION
 Interexaminer Reliability of Three Methods of Combining Test Results to Determine Side of Sacral Restriction, Sacral Base Position, and Innominate Bone Position Henry C. Tong, MD; Oscar G. Heyman, DO;
Interexaminer Reliability of Three Methods of Combining Test Results to Determine Side of Sacral Restriction, Sacral Base Position, and Innominate Bone Position Henry C. Tong, MD; Oscar G. Heyman, DO;
orthopaedic physical therapy world. Clinical prediction rules are decision-making tools that
 Introduction by the Series Editor I think it is safe to say that the advent of clinical prediction rules has caused quite a stir in the orthopaedic physical therapy world. Clinical prediction rules are
Introduction by the Series Editor I think it is safe to say that the advent of clinical prediction rules has caused quite a stir in the orthopaedic physical therapy world. Clinical prediction rules are
Session Objectives. Why We Need to Diagnose 4/2/18. Diagnosis: Defining the Patient Problem A prerequisite for treatment
 Diagnosis: Defining the Patient Problem A prerequisite for treatment Marcia Spoto PT, DC, OCS Nazareth College of Rochester Session Objectives 1. Appreciate the role of Physical Therapist (PT) diagnosis
Diagnosis: Defining the Patient Problem A prerequisite for treatment Marcia Spoto PT, DC, OCS Nazareth College of Rochester Session Objectives 1. Appreciate the role of Physical Therapist (PT) diagnosis
Improving Decision-Making in Low Back Pain: How to Target the Right Treatment at the Right Patient
 Evidence Based Examination Stats No not stats Patient Values & Expectations SNNOUT Sensitivity a highly 'SeNsitive' test, when Negative rules OUT disease (SN-N-OUT). Individual Clinical Expertise EBM Best
Evidence Based Examination Stats No not stats Patient Values & Expectations SNNOUT Sensitivity a highly 'SeNsitive' test, when Negative rules OUT disease (SN-N-OUT). Individual Clinical Expertise EBM Best
Physiotherapy Interventions for Low Back Pain - Subgrouping Patients with Improved Efficacy. Raymond Tsang. SPT, QMH FHKCOP 24 April 2010.
 Physiotherapy Interventions for Low Back Pain - Subgrouping Patients with Improved Efficacy Raymond Tsang SPT, QMH FHKCOP 24 April 2010 Background Low back pain (LBP) is a common condition encountered
Physiotherapy Interventions for Low Back Pain - Subgrouping Patients with Improved Efficacy Raymond Tsang SPT, QMH FHKCOP 24 April 2010 Background Low back pain (LBP) is a common condition encountered
Physical examination of the patient with back pain
 Physical examination of the patient with back pain Mitchell K Freedman DO Clinical Associate Professor at Sidney Kimmel Medical College of Thomas Jefferson University Hospital Goals of Lecture Discuss
Physical examination of the patient with back pain Mitchell K Freedman DO Clinical Associate Professor at Sidney Kimmel Medical College of Thomas Jefferson University Hospital Goals of Lecture Discuss
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Paul Allan Regional Clinical Lead - South. Lumbar Spine. Assessment & Differential Diagnosis
 Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
13/09/2012. Flexion. Extension
 The McKenzie Method in 2012 Mechanical Diagnosis & Therapy of the Spine & Extremities Outline Section 1 History and background Principles, evidence overview Section2 The natural history of musculoskeletal
The McKenzie Method in 2012 Mechanical Diagnosis & Therapy of the Spine & Extremities Outline Section 1 History and background Principles, evidence overview Section2 The natural history of musculoskeletal
Outcome of Spine Injections on the basis of MRI Findings. Personal use only. Tobias Dietrich Kantonsspital St.Gallen
 Outcome of Spine Injections on the basis of MRI Findings Tobias Dietrich Kantonsspital St.Gallen Evidence for Spinal Injections? Pe Skeletal Radiology 2010 rso na lu se moderate- to-strong evidence supporting
Outcome of Spine Injections on the basis of MRI Findings Tobias Dietrich Kantonsspital St.Gallen Evidence for Spinal Injections? Pe Skeletal Radiology 2010 rso na lu se moderate- to-strong evidence supporting
Summary and Perspective of Recent Literature Brian McClenahan, PT, Dip. MDT, FAAOMPT
 The McKenzie Institute International 2016 Vol. 5, No. 1 LITERATURE REVIEWS Summary and Perspective of Recent Literature Brian McClenahan, PT, Dip. MDT, FAAOMPT Apeldoorn, A et al. 2016. The influence of
The McKenzie Institute International 2016 Vol. 5, No. 1 LITERATURE REVIEWS Summary and Perspective of Recent Literature Brian McClenahan, PT, Dip. MDT, FAAOMPT Apeldoorn, A et al. 2016. The influence of
Does the Manual Therapy Technique Matter?
 Does the Manual Therapy Technique Matter? Joshua A. Cleland, DPT, OCS Assistant Professor, Physical Therapy Program, Franklin Pierce College, Concord, NH and Physical Therapist, Rehabilitation Services
Does the Manual Therapy Technique Matter? Joshua A. Cleland, DPT, OCS Assistant Professor, Physical Therapy Program, Franklin Pierce College, Concord, NH and Physical Therapist, Rehabilitation Services
Move Better, Feel Better: What Can Physical Therapy Do For You
 Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Perspective. Treatment-Based Classification System for Low Back Pain: Revision and Update
 Perspective Treatment-Based Classification System for Low Back Pain: Revision and Update Muhammad Alrwaily, Michael Timko, Michael Schneider, Joel Stevans, Christopher Bise, Karthik Hariharan, Anthony
Perspective Treatment-Based Classification System for Low Back Pain: Revision and Update Muhammad Alrwaily, Michael Timko, Michael Schneider, Joel Stevans, Christopher Bise, Karthik Hariharan, Anthony
Psychological predictors of recovery from low back pain: a prospective study
 George and Beneciuk BMC Musculoskeletal Disorders DOI 10.1186/s12891-015-0509-2 RESEARCH ARTICLE Open Access Psychological predictors of recovery from low back pain: a prospective study Steven Z George
George and Beneciuk BMC Musculoskeletal Disorders DOI 10.1186/s12891-015-0509-2 RESEARCH ARTICLE Open Access Psychological predictors of recovery from low back pain: a prospective study Steven Z George
By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT, DPT, LAT, CSCS
 The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
Randomised Controlled Trial for Low Back Pain
 INSPIRING THE WORLD TO MOVE WELL Randomised Controlled Trial for Low Back Pain A T 10 WEEKS, ViMove PATIENTS SHOWED SIGNIFICANT IMPROVEMENT IN ALL KEY MEASURES. IMPROVEMENTS WERE SUSTAINED OR IMPROVED
INSPIRING THE WORLD TO MOVE WELL Randomised Controlled Trial for Low Back Pain A T 10 WEEKS, ViMove PATIENTS SHOWED SIGNIFICANT IMPROVEMENT IN ALL KEY MEASURES. IMPROVEMENTS WERE SUSTAINED OR IMPROVED
Low back pain in a Nutshell Paul Manjaly. Paul Manjaly
 Low back pain in a Nutshell Paul Manjaly Paul Manjaly Pain: An unpleasant sensory and emotional experience which follows actual or potential tissue damage or is described in terms of such damage Unpleasant
Low back pain in a Nutshell Paul Manjaly Paul Manjaly Pain: An unpleasant sensory and emotional experience which follows actual or potential tissue damage or is described in terms of such damage Unpleasant
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Exercise for Rehabilitation and Treatment: Summary of Research
 Exercise for Rehabilitation and Treatment: Summary of Research Summarizing research findings to evaluate the effectiveness of exercise for rehabilitation and treatment of orthopedic conditions Summary
Exercise for Rehabilitation and Treatment: Summary of Research Summarizing research findings to evaluate the effectiveness of exercise for rehabilitation and treatment of orthopedic conditions Summary
Supplemental Video Available at
 The Use of a Lumbar Spine Manipulation Technique by Physical Therapists in Patients Who Satisfy a Clinical Prediction Rule: A Case Series Joshua A. Cleland, DPT, PhD, OCS 1 Julie M. Fritz, PT, PhD, ATC
The Use of a Lumbar Spine Manipulation Technique by Physical Therapists in Patients Who Satisfy a Clinical Prediction Rule: A Case Series Joshua A. Cleland, DPT, PhD, OCS 1 Julie M. Fritz, PT, PhD, ATC
Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme
 Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme Background Low back pain (LBP) is now recognised as the leading disabling condition in the world. LBP is a highly variable
Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme Background Low back pain (LBP) is now recognised as the leading disabling condition in the world. LBP is a highly variable
International Journal of Medical And Pharmaceutical Sciences
 www.iaard.net IAARD Journals eissn: 2456-0103 International Journal of Medical And Pharmaceutical Sciences IAARD- International Journal of Medical and Pharmaceutical Sciences, 2017, 3(1),9-13 Comparing
www.iaard.net IAARD Journals eissn: 2456-0103 International Journal of Medical And Pharmaceutical Sciences IAARD- International Journal of Medical and Pharmaceutical Sciences, 2017, 3(1),9-13 Comparing
Straight Leg Raising Test a snapshot summary of evidence (May 2013) Key messages
 Straight Leg Raising Test a snapshot summary of evidence (May 2013) Key messages The passive straight leg raising test (PSLR) is commonly used as an aid to the diagnosis of Lower Back Pain and is considered
Straight Leg Raising Test a snapshot summary of evidence (May 2013) Key messages The passive straight leg raising test (PSLR) is commonly used as an aid to the diagnosis of Lower Back Pain and is considered
Case Report. Classification, Intervention, and Outcomes for a Person With Lumbar Rotation With Flexion Syndrome. Key Words:
 Case Report Key Words: Classification, Intervention, and Outcomes for a Person With Lumbar Rotation With Flexion Syndrome Background and Purpose. The purpose of this case report is to describe the classification,
Case Report Key Words: Classification, Intervention, and Outcomes for a Person With Lumbar Rotation With Flexion Syndrome Background and Purpose. The purpose of this case report is to describe the classification,
Pain Care Doesn t Have to Be Torture
 Pain Care Doesn t Have to Be Torture How explaining pain to your patient can change the conversation and promote alliance and self-efficacy efficacy PRESENTED BY NORA STERN, PT, MSPT PROVIDENCE ST. JOSEPH
Pain Care Doesn t Have to Be Torture How explaining pain to your patient can change the conversation and promote alliance and self-efficacy efficacy PRESENTED BY NORA STERN, PT, MSPT PROVIDENCE ST. JOSEPH
Physical Therapists and Physicians
 Physical Therapists and Physicians Working Together for Optimal Patient Outcomes 2018 Spine Care and Physiatry Symposium Objectives 1. Understand key points from Providence system spine pathway work, particularly
Physical Therapists and Physicians Working Together for Optimal Patient Outcomes 2018 Spine Care and Physiatry Symposium Objectives 1. Understand key points from Providence system spine pathway work, particularly
LOTHIAN LUMBAR SPINE PATHWAYS
 LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Critical Appraisal of a Diagnostic Paper (Diagnosis of Lumbar Spinal Stenosis)
 Critical Appraisal of a Diagnostic Paper (Diagnosis of Lumbar Spinal Stenosis) Goal: To enhance skills in assessing an article related to diagnostic testing in terms of validity and applying results to
Critical Appraisal of a Diagnostic Paper (Diagnosis of Lumbar Spinal Stenosis) Goal: To enhance skills in assessing an article related to diagnostic testing in terms of validity and applying results to
Efficacy of segmental versus global core stabilization exercises for patients with chronic low back pain (LBP)
 Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2011 Efficacy of segmental versus global core stabilization exercises for patients with chronic low back pain
Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2011 Efficacy of segmental versus global core stabilization exercises for patients with chronic low back pain
Low back pain (FS-17)
 Low back pain (FS-17) Nadine Foster (United Kingdom) Jonathan Hill (United Kingdom) Peter O Sullivan (Australia) John Childs (United States of America) Mark Hancock (Australia) This material is provided
Low back pain (FS-17) Nadine Foster (United Kingdom) Jonathan Hill (United Kingdom) Peter O Sullivan (Australia) John Childs (United States of America) Mark Hancock (Australia) This material is provided
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
Managing back pain a new approach
 Managing back pain a new approach David Rogers Clinical Lead Functional Restoration Service Extended Scope Physiotherapist Royal Orthopaedic Hospital Setting the scene Back pain is one of the most common
Managing back pain a new approach David Rogers Clinical Lead Functional Restoration Service Extended Scope Physiotherapist Royal Orthopaedic Hospital Setting the scene Back pain is one of the most common
YOU ARE THE BEST OPTION FOR LOW BACK PAIN
 YOU ARE THE BEST OPTION FOR LOW BACK PAIN Amy Garrigues PT, DPT Orthopaedic Clinical Specialist Fellow, American Academy of Orthopaedic and Manual Physical Therapists LBP in past 3 months 25% 307% 220%
YOU ARE THE BEST OPTION FOR LOW BACK PAIN Amy Garrigues PT, DPT Orthopaedic Clinical Specialist Fellow, American Academy of Orthopaedic and Manual Physical Therapists LBP in past 3 months 25% 307% 220%
When Clinical Reasoning Overrules the Evidence
 When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
A Syndrome (Pattern) Approach to Low Back Pain. History
 A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
Understanding lower back pain
 NHS Buckinghamshire Musculoskeletal Integrated Care Service Understanding lower back pain Author; James Lee BSc, MSc, MSCP Illustrations: Sarah Geear BA Hons Spinal anatomy The spine is made up of 33 bony
NHS Buckinghamshire Musculoskeletal Integrated Care Service Understanding lower back pain Author; James Lee BSc, MSc, MSCP Illustrations: Sarah Geear BA Hons Spinal anatomy The spine is made up of 33 bony
MDT and the Relevant Lateral Component: Strategies for the Challenging Cervical Spine Patient
 MDT and the Relevant Lateral Component: Strategies for the Challenging Cervical Spine Patient Ron Schenk PT, PhD, OCS, FAAOMPT, Dip MDT Amy Fletcher PT, DPT, FAAOMPT, Dip MDT Brian McClenahan PT, MS, OCS,
MDT and the Relevant Lateral Component: Strategies for the Challenging Cervical Spine Patient Ron Schenk PT, PhD, OCS, FAAOMPT, Dip MDT Amy Fletcher PT, DPT, FAAOMPT, Dip MDT Brian McClenahan PT, MS, OCS,
1/22/2016 PATIENT SUBGROUPING. Patient Subgrouping. Psychologically Informed Physical Therapy Practice: Pragmatic Application for Low Back Pain
 Patient Subgrouping Jason Beneciuk, PT, PhD, MPH Research Assistant Professor University of Florida Brooks Rehabilitation PHHP Research Collaboration Psychologically Informed Physical Therapy Practice:
Patient Subgrouping Jason Beneciuk, PT, PhD, MPH Research Assistant Professor University of Florida Brooks Rehabilitation PHHP Research Collaboration Psychologically Informed Physical Therapy Practice:
The Relationship Between Clinical Activity And Function In Ankylosing Spondylitis Patients
 Bahrain Medical Bulletin, Vol.27, No. 3, September 2005 The Relationship Between Clinical Activity And Function In Ankylosing Spondylitis Patients Jane Kawar, MD* Hisham Al-Sayegh, MD* Objective: To assess
Bahrain Medical Bulletin, Vol.27, No. 3, September 2005 The Relationship Between Clinical Activity And Function In Ankylosing Spondylitis Patients Jane Kawar, MD* Hisham Al-Sayegh, MD* Objective: To assess
Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia
 Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain
 Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain Archives of Physical Medicine and Rehabilitation November 2005, Volume 86, Issue 11, pp 2075-2080
Conservative Correction of Leg-Length Discrepancies of 10 mm or Less for the Relief of Chronic Low Back Pain Archives of Physical Medicine and Rehabilitation November 2005, Volume 86, Issue 11, pp 2075-2080
Regional Review of Musculoskeletal System: Head, Neck, and Cervical Spine Presented by Michael L. Fink, PT, DSc, SCS, OCS Pre- Chapter Case Study
 Regional Review of Musculoskeletal System: Presented by Michael L. Fink, PT, DSc, SCS, OCS (20 minutes CEU Time) Subjective A 43-year-old male, reported a sudden onset of left-sided neck and upper extremity
Regional Review of Musculoskeletal System: Presented by Michael L. Fink, PT, DSc, SCS, OCS (20 minutes CEU Time) Subjective A 43-year-old male, reported a sudden onset of left-sided neck and upper extremity
BEHAVIORAL ASSESSMENT OF PAIN MEDICAL STABILITY QUICK SCREEN. Test Manual
 BEHAVIORAL ASSESSMENT OF PAIN MEDICAL STABILITY QUICK SCREEN Test Manual Michael J. Lewandowski, Ph.D. The Behavioral Assessment of Pain Medical Stability Quick Screen is intended for use by health care
BEHAVIORAL ASSESSMENT OF PAIN MEDICAL STABILITY QUICK SCREEN Test Manual Michael J. Lewandowski, Ph.D. The Behavioral Assessment of Pain Medical Stability Quick Screen is intended for use by health care
MOTOR VEHICLE ACCIDENT PAIN CHART
 MOTOR VEHICLE ACCIDENT PAIN CHART Name Today s Date (D/M/Y) Area of Concern What is the WORST pain you have ever experienced? (other than the pain you are experiencing NOW!) What was the date of this painful
MOTOR VEHICLE ACCIDENT PAIN CHART Name Today s Date (D/M/Y) Area of Concern What is the WORST pain you have ever experienced? (other than the pain you are experiencing NOW!) What was the date of this painful
Approaches to Low Back Pain
 Approaches to Low Back Pain NECOM/MaAOHN Annual Conference December 4, 2014 Moderator: John W. Burress, MD, MPH, FACOEM Panelists: Mark Crislip, MD Kathryn Mueller, MD, MPH, FACOEM Tony Tannoury, MD Donald
Approaches to Low Back Pain NECOM/MaAOHN Annual Conference December 4, 2014 Moderator: John W. Burress, MD, MPH, FACOEM Panelists: Mark Crislip, MD Kathryn Mueller, MD, MPH, FACOEM Tony Tannoury, MD Donald
The Effects of Mckenzie Exercsies for Patients with Low Back Pain, Our Experience
 The Effects of Mckenzie Exercsies for Patients with Low Back Pain, Our Experience Emela Muji} Skiki}, MD, MSc. Trebinjac Suad, MD, PhD. Visoka Zdravstvena {kola, Sarajevo Abstract Objective: To investigate
The Effects of Mckenzie Exercsies for Patients with Low Back Pain, Our Experience Emela Muji} Skiki}, MD, MSc. Trebinjac Suad, MD, PhD. Visoka Zdravstvena {kola, Sarajevo Abstract Objective: To investigate
CHIROPRACTIC -HOW IT AFFECTS YOU. Dr Milan Hari M- CHIRO. S.A GT Practitioner 07 June 2013
 CHIROPRACTIC -HOW IT AFFECTS YOU. Dr Milan Hari M- CHIRO. S.A GT Practitioner 07 June 2013 Chiropractic Chiropractic focuses on disorders of the musculoskeletal system and the nervous system, and the effects
CHIROPRACTIC -HOW IT AFFECTS YOU. Dr Milan Hari M- CHIRO. S.A GT Practitioner 07 June 2013 Chiropractic Chiropractic focuses on disorders of the musculoskeletal system and the nervous system, and the effects
Slump stretching in the management of non-radicular low back pain: A pilot clinical trial $
 ARTICLE IN PRESS Manual Therapy 11 (2006) 279 286 Original article Slump stretching in the management of non-radicular low back pain: A pilot clinical trial $ Joshua A. Cleland a,b,, John D. Childs c,
ARTICLE IN PRESS Manual Therapy 11 (2006) 279 286 Original article Slump stretching in the management of non-radicular low back pain: A pilot clinical trial $ Joshua A. Cleland a,b,, John D. Childs c,
Cox Technic Case Report #126 published at (sent December 2013 ) 1
 Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN
 EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN Dr.U.Ganapathy Sankar, Ph.D Dean I/C, SRM College of Occupational Therapy, SRMUniversity, Kattankulathur, KancheepuramDistrict, Tamil
EFFECIVENESS OF THE WILLIAMS EXCERCISE IN MECHANICAL LOW BACK PAIN Dr.U.Ganapathy Sankar, Ph.D Dean I/C, SRM College of Occupational Therapy, SRMUniversity, Kattankulathur, KancheepuramDistrict, Tamil
The Use of a Modified Treatment Based Classification System to Treat an Adolescent with Imaging Evidence of a Herniated Disc
 The Use of a Modified Treatment Based Classification System to Treat an Adolescent with Imaging Evidence of a Herniated Disc Jennifer Balla, SPT, 1 Steven Z. George, PT, PhD 2 ABSTRACT Background and Purpose:
The Use of a Modified Treatment Based Classification System to Treat an Adolescent with Imaging Evidence of a Herniated Disc Jennifer Balla, SPT, 1 Steven Z. George, PT, PhD 2 ABSTRACT Background and Purpose:
Int J Physiother. Vol 1(5), , December (2014) ISSN:
 Int J Physiother. Vol (5), 79-85, December (04) ISSN: 348-8336 ABSTRACT L. V. S. Pravallika C. Shanthi 3 K. Madhavi Background: Chronic nonspecific low back pain (CNSLBP) i.e., low back pain of at least
Int J Physiother. Vol (5), 79-85, December (04) ISSN: 348-8336 ABSTRACT L. V. S. Pravallika C. Shanthi 3 K. Madhavi Background: Chronic nonspecific low back pain (CNSLBP) i.e., low back pain of at least
Reliability and validity of the International Spinal Cord Injury Basic Pain Data Set items as self-report measures
 (2010) 48, 230 238 & 2010 International Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc ORIGINAL ARTICLE Reliability and validity of the International Injury Basic Pain Data Set items
(2010) 48, 230 238 & 2010 International Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc ORIGINAL ARTICLE Reliability and validity of the International Injury Basic Pain Data Set items
Key words: Neural Stretch,Pelvic Traction,VAS (Visual Analogue Scale),ODI (Oswestry Disability Index), LBP (Low Back Pain).
 Original study Short-term effect of lower limb neural stretch versus pelvic traction along with spinal extension exercises on pain and disability in patients with lower back pain with radiculopathy: A
Original study Short-term effect of lower limb neural stretch versus pelvic traction along with spinal extension exercises on pain and disability in patients with lower back pain with radiculopathy: A
EFFECT OF COMBINING SLUMP STRETCHING WITH CONVENTIONAL PHYSIOTHERAPY IN THE TREATMENT OF SUBACUTE NON- RADICULAR LOW BACK PAIN
 TJPRC: International Journal of Physiotherapy & Occupational Therapy (TJPRC: IJPOT) ISSN(P): Applied; ISSN(E): 2455-1996 Vol. 2, Issue 2, Dec 2016, 9-16 TJPRC Pvt. Ltd. EFFECT OF COMBINING SLUMP STRETCHING
TJPRC: International Journal of Physiotherapy & Occupational Therapy (TJPRC: IJPOT) ISSN(P): Applied; ISSN(E): 2455-1996 Vol. 2, Issue 2, Dec 2016, 9-16 TJPRC Pvt. Ltd. EFFECT OF COMBINING SLUMP STRETCHING
Research Report. Preliminary Evaluation of a Modified STarT Back Screening Tool Across Different Musculoskeletal. pain conditions.
 Research Report Preliminary Evaluation of a Modified STarT Back Screening Tool Across Different Musculoskeletal Pain Conditions Katie A. Butera, Trevor A. Lentz, Jason M. Beneciuk, Steven Z. George Background.
Research Report Preliminary Evaluation of a Modified STarT Back Screening Tool Across Different Musculoskeletal Pain Conditions Katie A. Butera, Trevor A. Lentz, Jason M. Beneciuk, Steven Z. George Background.
CLINICAL NOTES. Aust. J. Physiother. 26:5, October,
 CLINICAL NOTES COMBINED MOVEMENTS IN THE CERVICAL SPINE (C2-7) THEIR VALUE IN EXAMINATION AND TECHNIQUE CHOICE Brian C. Edwards Private Practitioner Lecturer in Manipulative Therapy, Western Australian
CLINICAL NOTES COMBINED MOVEMENTS IN THE CERVICAL SPINE (C2-7) THEIR VALUE IN EXAMINATION AND TECHNIQUE CHOICE Brian C. Edwards Private Practitioner Lecturer in Manipulative Therapy, Western Australian
Physiatrist Approaches to Pain Management: Functional Outcomes
 Ameet Nagpal, MD Dr. Nagpal is a board certified PM&R and Pain Medicine physician who is a Clinical Assistant Professor in the Department of Anesthesiology at the University of Texas Health Science Center
Ameet Nagpal, MD Dr. Nagpal is a board certified PM&R and Pain Medicine physician who is a Clinical Assistant Professor in the Department of Anesthesiology at the University of Texas Health Science Center
Clinical diagnosis of hip dysfunction
 Clinical diagnosis of hip dysfunction Trish Wisbey-Roth Specialist Sport Physiotherapist (FACP), Olympic Physio, Masters of Sport Physiotherapy ( AIS/UC) Active Rehabilitation Consultant. Case Study: Jane,
Clinical diagnosis of hip dysfunction Trish Wisbey-Roth Specialist Sport Physiotherapist (FACP), Olympic Physio, Masters of Sport Physiotherapy ( AIS/UC) Active Rehabilitation Consultant. Case Study: Jane,
CAN WE PREDICT SURGERY FOR SCIATICA?
 7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
Rebecca Courtney, PT, DPT. Supervisor, Ochsner HealthyBack
 Rebecca Courtney, PT, DPT Supervisor, Ochsner HealthyBack What is the Healthy Back Program? A comprehensive treatment approach for patients with sub-acute chronic neck and back pain Includes MD assessment,
Rebecca Courtney, PT, DPT Supervisor, Ochsner HealthyBack What is the Healthy Back Program? A comprehensive treatment approach for patients with sub-acute chronic neck and back pain Includes MD assessment,
Chiropractic Health Plan - Diagnosis of Low Back Pain
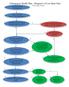 Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Innovative Spine Care Technology
 Extentrac Elite Innovative Spine Care Technology US FDA 510(k) K031996, K980021 China FDA Kazakhstan FDA #C3 2009/05629 United States Patents 6,905,508 6,923,825 7,309,347 Additional United States and
Extentrac Elite Innovative Spine Care Technology US FDA 510(k) K031996, K980021 China FDA Kazakhstan FDA #C3 2009/05629 United States Patents 6,905,508 6,923,825 7,309,347 Additional United States and
CERVICAL SPINE TIPS A
 CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
10/16/2017 ATHLETIC LOW BACK PAIN: RISK FACTORS AND PRINCIPLES FOR EFFECTIVE RETURN TO SPORT. How Do Patients Present? The Journey to Return to Sport
 ATHLETIC LOW BACK PAIN: RISK FACTORS AND PRINCIPLES FOR EFFECTIVE RETURN TO SPORT Phil Glasgow PhD, MCSP How Do Patients Present? Technique Sport Specific Mobility Effective Force Generation Strength Subqualities
ATHLETIC LOW BACK PAIN: RISK FACTORS AND PRINCIPLES FOR EFFECTIVE RETURN TO SPORT Phil Glasgow PhD, MCSP How Do Patients Present? Technique Sport Specific Mobility Effective Force Generation Strength Subqualities
Sciatica. 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) Website: philip-bayliss.com
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Sciatica Nagging, burning pain radiating down the back of the leg, or dull throbbing pain in the buttocks
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Sciatica Nagging, burning pain radiating down the back of the leg, or dull throbbing pain in the buttocks
Low back pain (LBP) is the reason for seeking care in nearly 50% of
 [ clinical commentary ] Julie M. Fritz, PT, PhD, ATC 1 Joshua A. Cleland, PT, PhD, OCS, FAAOMPT 2 John D. Childs, PT, PhD, MBA, OCS, FAAOMPT 3 Subgrouping Patients With Low Back Pain: Evolution of a Classification
[ clinical commentary ] Julie M. Fritz, PT, PhD, ATC 1 Joshua A. Cleland, PT, PhD, OCS, FAAOMPT 2 John D. Childs, PT, PhD, MBA, OCS, FAAOMPT 3 Subgrouping Patients With Low Back Pain: Evolution of a Classification
A World of Hurt: A Guide to Classifying Pain Overview Course November 11-12, 2017
 A World of Hurt: A Guide to Classifying Pain Course January 14-15, 2018 COURSE DESCRIPTION A World of Hurt: A Guide to Classifying Pain Overview Course November 11-12, 2017 This two-day course introduces
A World of Hurt: A Guide to Classifying Pain Course January 14-15, 2018 COURSE DESCRIPTION A World of Hurt: A Guide to Classifying Pain Overview Course November 11-12, 2017 This two-day course introduces
Improving Thoracic Mobility
 Improving Thoracic Mobility By William J. Hanney DPT, PhD, ATC, CSCS Course Description A lack of thoracic mobility can have broad clinical implications and evidence suggests addressing mobility in this
Improving Thoracic Mobility By William J. Hanney DPT, PhD, ATC, CSCS Course Description A lack of thoracic mobility can have broad clinical implications and evidence suggests addressing mobility in this
Low Back Pain in Computer Professionals A Comparison Between Yogasanas And Mckenzie Treatment Approaches
 Index Copernicus Value- 56.65 Volume 5 Issue 06 June-2017 Pages-6507-6512 ISSN(e):2321-7545 Website: http://ijsae.in DOI: http://dx.doi.org/10.18535/ijsre/v5i06.02 Low Back Pain in Computer Professionals
Index Copernicus Value- 56.65 Volume 5 Issue 06 June-2017 Pages-6507-6512 ISSN(e):2321-7545 Website: http://ijsae.in DOI: http://dx.doi.org/10.18535/ijsre/v5i06.02 Low Back Pain in Computer Professionals
Reliability of Measuring Trunk Motions in Centimeters
 Reliability of Measuring Trunk Motions in Centimeters MARGARET ROST, SANDRA STUCKEY, LEE ANNE SMALLEY, and GLENDA DORMAN A method of measuring trunk motion and two related motions using a tape measure
Reliability of Measuring Trunk Motions in Centimeters MARGARET ROST, SANDRA STUCKEY, LEE ANNE SMALLEY, and GLENDA DORMAN A method of measuring trunk motion and two related motions using a tape measure
Eighty percent of patients with chronic back pain (CBP)
 SPINE Volume 37, Number 8, pp 711 715 2012, Lippincott Williams & Wilkins HEALTH SERVICES RESEARCH Responsiveness and Minimal Clinically Important Change of the Pain Disability Index in Patients With Chronic
SPINE Volume 37, Number 8, pp 711 715 2012, Lippincott Williams & Wilkins HEALTH SERVICES RESEARCH Responsiveness and Minimal Clinically Important Change of the Pain Disability Index in Patients With Chronic
Medical Report. Prepared for the court by Dr Sample Expert. Date: 04/03/2016. Section A - Claimant s Details. Mr Harry Test Potter 07/07/1970
 Medical Report Prepared for the court by Dr Sample Expert Date: 04/03/2016 Section A - Claimant s Details Claimant s full name Date of birth Mr Harry Test Potter 07/07/1970 Address Hogwarts Castle Hogwarts
Medical Report Prepared for the court by Dr Sample Expert Date: 04/03/2016 Section A - Claimant s Details Claimant s full name Date of birth Mr Harry Test Potter 07/07/1970 Address Hogwarts Castle Hogwarts
Presuming all the above symptoms are not present, pain is more likely to be mechanical and caused by a sprain, strain or poor posture.
 Page 1 of 8 View this article online at: patient.info/health/back-pain-exercises Back Pain Exercises Back pain is very common but in most cases is not caused by a serious problem. Most cases of back pain
Page 1 of 8 View this article online at: patient.info/health/back-pain-exercises Back Pain Exercises Back pain is very common but in most cases is not caused by a serious problem. Most cases of back pain
Premier Orthopedic Spine Center
 Premier Orthopedic Spine Center Atrium Medical Center Professional Buliding 200 Medical Center Dr., Ste. 375 Middletown, Ohio 45005 Neck Questionnaire Patient Date Family Physician The onset of my neck
Premier Orthopedic Spine Center Atrium Medical Center Professional Buliding 200 Medical Center Dr., Ste. 375 Middletown, Ohio 45005 Neck Questionnaire Patient Date Family Physician The onset of my neck
Psychosocial and psychological
 STEVEN Z. GEORGE, PT, PhD 1 JULIE M. FRITZ, PT, PhD, ATC 2 JOHN D. CHILDS, PT, PhD 3 Investigation of Elevated Fear-Avoidance Beliefs for Patients With Low Back Pain: A Secondary Analysis Involving Patients
STEVEN Z. GEORGE, PT, PhD 1 JULIE M. FRITZ, PT, PhD, ATC 2 JOHN D. CHILDS, PT, PhD 3 Investigation of Elevated Fear-Avoidance Beliefs for Patients With Low Back Pain: A Secondary Analysis Involving Patients
Is it useful for chronic pain patients? Therapeutic Patient Education (TPE) Psycho-education Cognitive Behavioral Therapy (CBT) Françoise LAROCHE, MD
 Is it useful for chronic pain patients? Therapeutic Patient Education (TPE) Psycho-education Cognitive Behavioral Therapy (CBT) Françoise LAROCHE, MD Pain and Rheumatologic Department Saint-Antoine Hospital
Is it useful for chronic pain patients? Therapeutic Patient Education (TPE) Psycho-education Cognitive Behavioral Therapy (CBT) Françoise LAROCHE, MD Pain and Rheumatologic Department Saint-Antoine Hospital
Evaluating Sagittal Spinal Posture During Functional Tasks:
 Evaluating Sagittal Spinal Posture During Functional Tasks: Can Kinematics Differentiate Between Non-specific Chronic Low Back Pain Subgroups And Healthy Controls? Rebecca Hemming*, Liba Sheeran, Robert
Evaluating Sagittal Spinal Posture During Functional Tasks: Can Kinematics Differentiate Between Non-specific Chronic Low Back Pain Subgroups And Healthy Controls? Rebecca Hemming*, Liba Sheeran, Robert
Exercise for Neck Pain
 Exercise for Neck Pain Deborah Falla @Deb_Falla Centre of Precision Rehabilitation for Spinal Pain School of Sport, Exercise and Rehabilitation Sciences College of Life and Environmental Sciences University
Exercise for Neck Pain Deborah Falla @Deb_Falla Centre of Precision Rehabilitation for Spinal Pain School of Sport, Exercise and Rehabilitation Sciences College of Life and Environmental Sciences University
TREATMENT OF CHRONIC MECHANICAL NECK PAIN IN AN OUTPATIENT ORTHOPEDIC SETTING
 TREATMENT OF CHRONIC MECHANICAL NECK PAIN IN AN OUTPATIENT ORTHOPEDIC SETTING Clinical Problem Solving II Allison Walsh PATIENT OVERVIEW Age: 22 years Gender: Female Chief Complaint: Cervical pain, cervicogenic
TREATMENT OF CHRONIC MECHANICAL NECK PAIN IN AN OUTPATIENT ORTHOPEDIC SETTING Clinical Problem Solving II Allison Walsh PATIENT OVERVIEW Age: 22 years Gender: Female Chief Complaint: Cervical pain, cervicogenic
Classification, treatment and outcomes of a patient with lumbar extension syndrome
 Physiotherapy Theory and Practice, 21(3):181 196, 2005 Copyright # Taylor & Francis Inc. ISSN: 0959-3985 print/1521-0510 online DOI: 10.1080/09593980500212987 Classification, treatment and outcomes of
Physiotherapy Theory and Practice, 21(3):181 196, 2005 Copyright # Taylor & Francis Inc. ISSN: 0959-3985 print/1521-0510 online DOI: 10.1080/09593980500212987 Classification, treatment and outcomes of
During the initial visit, Centralization was observed in 52.9% and partial Centralization in 21.9%.
 The McKenzie Institute International 2017 Vol. 6, No. 1 LITERATURE REVIEWS Summary and Perspective of Recent Literature Jacky Otéro, PT, Cert. MDT and Richard Rosedale, PT, Dip. MDT Otéro J, Bonnet F.
The McKenzie Institute International 2017 Vol. 6, No. 1 LITERATURE REVIEWS Summary and Perspective of Recent Literature Jacky Otéro, PT, Cert. MDT and Richard Rosedale, PT, Dip. MDT Otéro J, Bonnet F.
Dynamic Spinal Visualization and Vertebral Motion Analysis
 Dynamic Spinal Visualization and Vertebral Motion Analysis Policy Number: 6.01.46 Last Review: 2/2019 Origination: 2/2006 Next Review: 2/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Dynamic Spinal Visualization and Vertebral Motion Analysis Policy Number: 6.01.46 Last Review: 2/2019 Origination: 2/2006 Next Review: 2/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society
 Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Michele Thompson, P.T. Regional Therapy Director Dr. Joy Hamilton Regional Medical Director
 Michele Thompson, P.T. Regional Therapy Director Dr. Joy Hamilton Regional Medical Director Work Related Work Injuries Related Injuries Workshop Effective Management of Work- Related Musculoskeletal Disorders
Michele Thompson, P.T. Regional Therapy Director Dr. Joy Hamilton Regional Medical Director Work Related Work Injuries Related Injuries Workshop Effective Management of Work- Related Musculoskeletal Disorders
Natural Evolution of Lumbar Spinal Stenosis
 Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Institute of Holistic Healthcare. Certificate in Orthopaedic Manipulative Therapy PROSPECTUS
 Institute of Holistic Healthcare Certificate in Orthopaedic Manipulative Therapy PROSPECTUS 2019 Contents Contents... 1 Aims:... 2 Objectives:... 2 Format of the Program:... 3 Program... 3 Continuing Professional
Institute of Holistic Healthcare Certificate in Orthopaedic Manipulative Therapy PROSPECTUS 2019 Contents Contents... 1 Aims:... 2 Objectives:... 2 Format of the Program:... 3 Program... 3 Continuing Professional
Use of Therapeutic Neuroscience Education to address Psychosocial Factors Associated with Acute Low Back Pain: A Case Report
 Use of Therapeutic Neuroscience Education to address Psychosocial Factors Associated with Acute Low Back Pain: A Case Report Physiotherapy Theory and Practice (in press) Kory Zimney, PT, DPT, CSMT YOUR
Use of Therapeutic Neuroscience Education to address Psychosocial Factors Associated with Acute Low Back Pain: A Case Report Physiotherapy Theory and Practice (in press) Kory Zimney, PT, DPT, CSMT YOUR
PREVALENCE OF RISK FACTORS ASSOCIATED WITH NON-SPECIFIC BACK PAIN AMONG FEMALE PATIENTS IN AFIRM
 Original Research Article PREVALENCE OF RISK FACTORS ASSOCIATED WITH NON-SPECIFIC BACK PAIN AMONG FEMALE PATIENTS IN AFIRM Samina Ghulam *, Amjad Sharif, Quratulain Saeed. Physiotherapy Department, Armed
Original Research Article PREVALENCE OF RISK FACTORS ASSOCIATED WITH NON-SPECIFIC BACK PAIN AMONG FEMALE PATIENTS IN AFIRM Samina Ghulam *, Amjad Sharif, Quratulain Saeed. Physiotherapy Department, Armed
