Significance and pitfalls of percutaneous endoscopic lumbar discectomy for large central lumbar disc herniation
|
|
|
- Kerry Fields
- 5 years ago
- Views:
Transcription
1 Original Study Significance and pitfalls of percutaneous endoscopic lumbar discectomy for large central lumbar disc herniation Mikihito Kondo 1,2, Yasushi Oshima 1,2,3, Hirokazu Inoue 1,2,4, Yuichi Takano 1,2, Hirohiko Inanami 1,2, Hisashi Koga 1,2 1 Department of Orthopaedics, Iwai Orthopaedic Medical Hospital, Tokyo, Japan; 2 Department of Orthopaedic Surgery, Inanami Spine and Joint Hospital, Tokyo, Japan; 3 Department of Orthopaedic Surgery, The University of Tokyo, Tokyo, Japan; 4 Department of Orthopaedic Surgery, Jichi Medical University, Tochigi, Japan Contributions: (I) Conception and design: H Koga; (II) Administrative support: H Inanami; (III) Provision of study materials or patients: All authors; (IV) Collection and assembly of data: H Koga; (V) Data analysis and interpretation: H Koga; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Hisashi Koga, MD, PhD. Department of Orthopaedics, Iwai Orthopaedic Medical Hospital, Minamikoiwa Edogawa-ku, Tokyo , Japan. hkoga0808@gmail.com. Background: Percutaneous endoscopic lumbar discectomy (PELD) is a relatively less invasive treatment for lumbar disc herniation (LDH). The present study focused on the transforaminal approach (TFA) and investigated the significance of PELD via this approach for large central LDH. Methods: LDH that did not show cerebrospinal fluid (CSF) on axial T2-weighted magnetic resonance images was defined as large central LDH. PELD via the TFA was performed in 11 patients with large central LDH. Pre- and post-operative statuses were evaluated using the modified Japanese Orthopedic Association (mjoa) and Numerical Rating Scale (NRS) scores. Results: The patients mean age was 44.1 years; there was single-level involvement, mostly at L4/5 (seven cases). The mean recovery rate of the mjoa score was 48.7%, and mean pre- and post-operative NRS scores were 7.1 and 1.5, respectively. The mean operative time was 38.1 min. Although there were no major complications, the dura was accidentally punctured at the initial operative step for discography in one case. LDH recurred in one case at 5 months after the operation, and the patient was treated by PELD via the TFA on the contralateral side. Conclusions: The TFA for PELD is a safe, minimally invasive, effective treatment for large central LDH. However, the operator should pay attention to malpositioning of the flat and laterally expanded dural sac. Keywords: Percutaneous endoscopic lumbar discectomy (PELD); large central lumbar disc herniation (LDH); transforaminal approach (TFA); complication; minimally invasive Submitted Sep 27, Accepted for publication Dec 06, doi: /jss View this article at: Introduction Percutaneous endoscopic lumbar discectomy (PELD) is one of the most sophisticated operative procedures for the treatment of lumbar disc herniation (LDH) (1-3). The operative outcomes have already been extensively reported, and the results are comparable with those of conventional operative procedures such as open discectomy (4-9). However, PELD has an anatomical limitation for endoscope insertion. Three different operative approaches that complementing each other are available for PELD interlaminar, transforaminal, and posterolateral of which the transforaminal approach (TFA) is the most popular. Large central LDH is a challenge for spinal surgeons. The extent of laminectomy is larger with the conventional posterior approach than that for lateral LDH, and traction
2 80 Kondo et al. Significance of PELD for large LDH Figure 1 MRI findings of patients with accidental dural puncture during the initial operative step for discography. Pre-operative and post-operative sagittal and axial T2-weighted magnetic resonance images. MRI, magnetic resonance imaging. same vertebral level. For all patients, PELD via the TFA was conducted at only one vertebral level by a single surgeon (H Koga). Neurological examination, pre-operative computed tomography (CT), and magnetic resonance imaging (MRI) were used to identify the location and size of the LDH. Large central LDH was defined as herniation that did not show CSF on axial T2-weighted MRIs (Figure 1). Patients were followed up for an average of 8.7 months (range, 5 15 months) postoperatively. Pre- and postoperative neurological statuses were evaluated using the modified Japanese Orthopedic Association (mjoa) score. The recovery rate was determined as follows: recovery rate = post-operative mjoa pre-operative mjoa/23 (full score) pre-operative mjoa score 100. Corresponding leg pain was also evaluated using the Numerical Rating Scale (NRS) score. Statistical analysis was performed using the Student t-test. P values less than 0.05 were considered statistically significant. of the dural sac tends to be greater with this approach as well. Several surgeons have proposed solutions to these problems (10-14), one of which is use of the trans-dural approach. However, this approach has a potential risk of post-operative cerebrospinal fluid (CSF) leakage (11,12). Further, the bilateral approach has also been proposed as a solution (10,14), but both these procedures are highly invasive and the operative time is consequently prolonged. From our previous experience with TFA, we concluded that large central LDH is a good indication for PELD via the TFA. Here, we summarize this experience and confirm our conclusions. We also identified the pitfalls of PELD via the TFA in this retrospective analysis. In this article, we present the operative outcomes of PELD via the TFA for large central LDH and provide useful information for prevention of complications. Methods Between July 2016 and April 2017, 11 consecutive patients with large central LDH underwent PELD via the TFA conducted using a 7-mm diameter spinal full-endoscopic system (Richard Wolf GmbH, Knittlingen, Germany). All patients had radiculopathy resistant to medical treatment, epidural steroid injection, and/or nerve block. To clarify the surgical benefits of PELD via the TFA, we excluded patients who had previously undergone discectomy at the Surgical technique Patients were carefully log-rolled into the prone position. To enlarge the vertebral foramen, a pillow was placed between the operating table and anterior iliac crest. The surgery was performed with the patient under general anesthesia and simultaneous motor evoked potential (MEP) monitoring to avoid intraoperative discomfort and postoperative piriformis syndrome (15). During the operation, a fluoroscope was placed across the center of the operating table to ensure appropriate positioning. An 8-mm skin and fascia incision was made 7 10 cm lateral from the midline at the target disc level under fluoroscopic guidance, after which an 18-gauge spinal needle was inserted into the disc. Discography was performed with indigo carmine and a contrast medium in order to stain the herniated disc material. Following insertion of an obturator, a 45 angled-working sheath of diameter 7 mm was inserted. Then, an endoscope (diameter of working channel: 4.1 mm) was inserted and the annulus fibrosus, lateral part of the yellow ligament, and superior articular process (SAP) were confirmed (Figure 2). Generally, the herniated nucleus is located in the back of the annulus bulge; therefore, the approach side of the annulus was incised and the sequestered nucleus was explored using several types of forceps and dissectors (Figure 2). After complete removal, the compressed ventral surface of the dural sac or the large space between the posterior longitudinal ligament (PLL)
3 Journal of Spine Surgery, Vol 4, No 1 March and dural sac became visible (Figure 2). Finally, the annular tear and evacuated cavities were electrocoagulated using a bipolar radio-frequency electrode system (Elliquence, Baldwin, NY, USA), followed by careful endoscopic examination for epidural bleeding and hemostasis. After decompression, the working sheath was carefully removed, and the skin was closed with a single suture. Results cranial Figure 2 Intraoperative photographs. After reaching the vertebral foramen, we first confirmed the annulus fibrosus ( ), posterior longitudinal ligament (PLL) (arrow heads), and superior articular process (SAP) ( ). After puncturing the surface of the annulus fibrosus, we removed the sequestrated nucleus underneath the PLL by using several types of forceps. Subsequently, the PLL gradually shifted to the ventral side, and large spaces were finally visible on both the dorsal and ventral sides of the PLL. caudal Eleven patients were registered for this study; foraminoplasty was additionally conducted in two cases an initial case and one in which foraminal stenosis co-occurred with the LDH although it was not actually necessary for the initial case from the operative finding. Although we assumed that foraminoplasty might help to remove large LDH for the initial case, it was not indicated. Subsequently, we have not generally performed foraminoplasty for the treatment of large LDH. The mean patient age was 44.1 years (range, years), and the male/female ratio was 7/4. The most affected vertebral level was L4/5 (seven cases), followed by L3/4 (four cases). Especially for large LDH, definitive determination of the right or left location is relatively difficult from radiological scans. Therefore, we determined the side on which to conduct PELD via the TFA from the level corresponding to the most severe radiculopathy (Table 1). In one case (No. 7), in which the patient experienced severe bilateral pain and muscle weakness, we performed PELD on the left side, since the axial MRI clearly showed left-sided distribution. The mean operative time was 38.1 min (range, min), and the mean volume of the nucleus pulposus removed was 2.1 g (range, g); the mean blood loss was negligible in all patients (Table 1). The mean post-operative hospital stay was 3.5 days (range, 2 13 days); it was particularly long in case No. 7 because of the severe bilateral muscle weakness (Table 1). The mjoa score improved significantly from 8.3±3.58 to 16.8±2.85, and the recovery rate of this score was 48.7%±29.0%. The NRS scores also improved significantly from 7.1±1.68 to 1.5±1.49 (Table 2). Because of the severe pain and muscle weakness caused by large central LDH, patients experience gait disturbance (16). In the current case series, we also observed muscle weakness and/or gait disturbance in nine cases. Except one patient (No. 7), all the rest were discharged without any walking assistance. Even in case No. 7, the patient showed improved muscle weakness and could visit our out-patient clinic by walking without assistance after 1 month. During the follow-up period (range, 5 15 months; average, 8.7 months), LDH recurred in only one case, that of the oldest patient (case No. 5; 72-year-old patient) who also had spinal canal stenosis (SCS). This patient underwent a second PELD from the contralateral side 5 months after the first operation. We observed no major complications in this case series, although in one case (case No. 10) (Figure 1), the dura was accidentally punctured during the initial operative step for discography. The operation, however, was unremarkable. The post-operative course was normal, and the patient was discharged from hospital 3 days after the operation. As we perceived the malpositioning of the needle puncture at the initial stage of the operation, we changed the trajectory of the needle toward the caudal side and confirmed that it touched the lateral surface of SAP, after which it was adequately introduced into the vertebral disc (Figure 3). We did not observe dorsal displacement of the dural sac even during the operation (Figure 2). Therefore, we speculated that we had punctured the laterally expanded dural sac underneath the lateral part of the yellow ligament.
4 82 Kondo et al. Significance of PELD for large LDH Table 1 Summary of the detailed features of the 11 cases of large central LDH Case No. Sex Age (years) Chief complaint Gait disturbance Muscle weakness Disc level Spinal canal stenosis Approach side Skin incision** (cm) Foraminoplasty Operative time (min) Removed volume (g) Hospital stay (days) 1 M 22 Left leg pain (+) ( ) L3/4 ( ) L 7 (+) F 31 Right leg pain (+) EHL 4/5 L4/5 ( ) R 7 ( ) F 36 Left leg pain ( ) EHL 4/5 L4/5 ( ) L 7.5 ( ) M 32 Right leg pain ( ) EHL 4/5 L4/5 ( ) R 9 ( ) M 72 Bilateral leg pain ( ) ( ) L3/4 (+) R 7.5 ( ) F 29 Right leg numbness ( ) EHL 1/5 L4/5 ( ) R 9 ( ) M 66 Bilateral leg pain (+) TA 1/3 L3/4 ( ) L 8 ( ) F 67 Right leg pain (+) ( ) L4/5 (+) R 8 (+) M 47 Right leg pain ( ) Gastro 2/2 L4/5 ( ) R 9 ( ) M 42 Left leg pain (+) ( ) L3/4 ( ) L 8 ( ) M 41 Left leg pain ( ) ( ) L4/5 ( ) L 10 ( ) **, the distance from the midline to the skin incision; +, presence;, absence. EHL, extensor hallucis longus; TA, tibialis anterior; Gastro, gastrocnemius; LDH, lumbar disc herniation; M, male; F, female; L, left; R, right. Table 2 Surgical outcome of 11 cases Evaluation methods Average SD P value Follow-up period (months) mjoa score Pre-operative (months) Post-operative (months) <0.01 Recovery rate (%) NRS score (months) Pre-operative Post-operative <0.01 Recovery rate = post-operative mjoa pre-operative mjoa/23 (full score) pre-operative mjoa score 100. SD, standard deviation; mjoa, modified Japanese Orthopedic Association; NRS, Numerical Rating Scale.
5 Journal of Spine Surgery, Vol 4, No 1 March Figure 3 Pre-operative CT finings of patients with accidental dural puncture during the initial operative step for discography. Sagittal, axial, and three-dimensionally reconstructed CT images. The red lines indicate the scanning positions; the blue arrow indicates the first needle trajectory for accidental dural puncture; the yellow arrow indicates the corrected needle trajectory for appropriate PELD via the TFA; the sign indicates the SAP of the contralateral side. Note that cranial needle puncture is easier to reach the medial site of the annulus fibrosus. CT, computed tomography; PELD, percutaneous endoscopic lumbar discectomy; TFA, transforaminal approach; SAP, superior articular process. Discussion Large central LDH at low vertebral levels is the most common cause for cauda equina syndrome (CES), which is characterized by severe lower back pain, sciatica (often bilateral), saddle and/or genital sensory disturbance, bladder, bowel dysfunction, and sexual dysfunction (16). Surgical treatment delayed beyond 48 h leads to persistent bladder, bowel, and sexual dysfunction (17). Fortunately, we did not experience CES in the present series, although case No. 7 was essentially identical to CES. The patient s bilateral paresis persisted but was completely eliminated after 1 month. In cases of large central LDH, although the timing of the operation is vital, the operative procedure is also important in order to ensure a good prognosis. Previously used posterior approaches require several types of laminectomy and partial facetectomy for removal of large central LDH (18). Such procedures cause post-operative instability, and fusion operation may occasionally be required. Although some surgeons advocate the trans-dural approach, this approach has the potential disadvantage of post-operative CSF leakage (11,12). Further, these procedures are not only highly invasive but also requiring the prolonged operative time. The significance of PELD for large central LDH remains controversial. Choi et al. analyzed their experience of 10,228 cases and reported that the frequency of incomplete removal of LDH was high in the case of central LDH (19). On the other hand, Lee et al. reported good operative outcomes for six consecutive patients who presented with back and leg pain and/or weakness due to large central LDH and were treated using percutaneous endoscopic herniotomy via a unilateral intra-annular subligamentous approach (20). Li et al. also reported good operative outcomes in 16 consecutive patients with CES who underwent PELD (18). In the present article, we summarized 11 cases of large central LDH treated by PELD via the TFA. The operative outcomes were not inferior compared to previous outcomes of surgery for LDH (21-23). The surgeon can directly confirm the protruded annulus fibrosus under endoscopic visualization and can confirm the presence of an extruded nucleus under the annulus fibrosus by touching and on the basis of fluoroscopic imaging (Figure 2). Although special training under a skilled supervisor is required for surgeons to perform this surgery, PELD via the TFA is a promising surgical procedure for large central LDH. We have to carefully consider the operative indication for large central LDH combined with SCS. In general, SCS occurs in elderly patients and is frequently co-occurs with foraminal stenosis and a decrease in vertebral height, which results in a narrow working space at the vertebral foramen and prevents endoscopic manipulation. Case No. 5 was one
6 84 Kondo et al. Significance of PELD for large LDH such case; the removal was insufficient and the symptoms recurred early after the operation. For this patient, we should have beforehand performed sufficient foraminoplasty using a high-speed drill, or we should have combined the wide extent of laminectomy. Recently, several authors have emphasized the significance of foraminoplasty (24,25). Even during the operation, if considered necessary, foraminoplasty should definitely be performed to enlarge the working space. The advantage of the TFA is that it ensures safety in Kambin s triangle (26). This triangle is not completely safe in the case of large central LDH, because the dural sac becomes flat and laterally expanded because of the extreme compression caused by the LDH. If the needle is introduced more cranially, the trajectory of the needle puncture draws along with the lateral aspect of the inferior articular process (IAP). Thus, the dural sac may get punctured. We also encountered one such case (case No. 10). Further, since the lateral aspect of the SAP is not hypertrophic and smoothly transfers to the lateral aspect of the IAP, the trajectory of the needle puncture can easily be drawn more medially even along the lateral aspect of the SAP. To avoid injuries to the dura or the underlying cauda equina, the walking technique is very important, in which the operator confirms the anatomical structures (lateral surfaces of the IAP and SAP, the caudal pedicle, and annulus fibrosus) in a stepwise manner using the tip of the needle (1). Since the initial operative step of the needle puncture involves blind manipulation, fluoroscopic imagining in both lateral and anteroposterior views can help confirm the needle s position. Especially for higher vertebral levels, it must be kept in mind that the lateral aspect of the IAP draws nearer to the dural sac. PELD is a recently developed surgical technique that has the advantages of requiring a small incision size (8 mm), rapid recovery, short hospital stay, limited blood loss, less destruction of the surrounding tissues, and less post-operative pain. Nevertheless, some PELD-specific problems do exist. Especially for large central LDH, the co-occurrence of SCS or foraminal stenosis is one of the reasons for incomplete removal. The possibility of inappropriate puncture of the dural sac in the initial stage of PELD is another pitfall of this procedure. After overcoming these problems, PELD should be the first line of treatment for large central LDH. Conclusions The preliminary results obtained during our short followup period show that PELD via the TFA is feasible for the treatment of large central LDH. However, the operator should pay attention to malpositioning of the flat and laterally expanded dural sac in order to avoid dural and cauda equina injuries. Acknowledgements We would like to thank all the operating room staff for their technical assistance, and the medical records clerks who helped collect patient data. We would also like to thank all radiological department staff for recording CT and MRI data. This work was partly supported by a grant from the Iwai Medical Foundation. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. Ethical Statement: This study was approved by ethics committee of the Iwai Medical Foundation, and informed consent was obtained from the patients for publication of this study and any accompanying images. References 1. Sairyo K, Egawa H, Matsuura T, et al. State of the art: Transforaminal approach for percutaneous endoscopic lumbar discectomy under local anesthesia. J Med Invest 2014;61: Choi G, Lee SH, Deshpande K, et al. Working channel endoscope in lumbar spine surgery. J Neurosurg Sci 2014;58: Yeung AT. The Evolution and Advancement of Endoscopic Foraminal Surgery: One Surgeon s Experience Incorporating Adjunctive Techologies. SAS J 2007;1: Ahn SS, Kim SH, Kim DW, et al. Comparison of Outcomes of Percutaneous Endoscopic Lumbar Discectomy and Open Lumbar Microdiscectomy for Young Adults: A Retrospective Matched Cohort Study. World Neurosurg 2016;86: Chen HC, Lee CH, Wei L, et al. Comparison of percutaneous endoscopic lumbar discectomy and open lumbar surgery for adjacent segment degeneration and recurrent disc herniation. Neurol Res Int 2015;2015: Choi KC, Park CK. Percutaneous Endoscopic Lumbar
7 Journal of Spine Surgery, Vol 4, No 1 March Discectomy for L5-S1 Disc Herniation: Consideration of the Relation between the Iliac Crest and L5-S1 Disc. Pain Physician 2016;19:E Sinkemani A, Hong X, Gao ZX, et al. Outcomes of Microendoscopic Discectomy and Percutaneous Transforaminal Endoscopic Discectomy for the Treatment of Lumbar Disc Herniation: A Comparative Retrospective Study. Asian Spine J 2015;9: Gadjradj PS, van Tulder MW, Dirven CM, et al. Clinical outcomes after percutaneous transforaminal endoscopic discectomy for lumbar disc herniation: a prospective case series. Neurosurg Focus 2016;40:E3. 9. Sencer A, Yorukoglu AG, Akcakaya MO, et al. Fully endoscopic interlaminar and transforaminal lumbar discectomy: short-term clinical results of 163 surgically treated patients. World Neurosurg 2014;82: Bärlocher CB, Krauss JK, Seiler RW. Central lumbar disc herniation. Acta Neurochir (Wien) 2000;142: ; discussion Choi JW, Lee JK, Moon KS, et al. Transdural approach for calcified central disc herniations of the upper lumbar spine. J Neurosurg Spine 2007;7: Kim DS, Lee JK, Jang JW, et al. Clinical Features and Treatments of Upper Lumbar Disc Herniations. J Korean Neurosurg Soc 2010;48: Moon KH, Lee SH, Kong BJ, et al. An Oblique Paraspinal Approach for Intracanalicular Disc Herniations of the Upper Lumbar Spine: Technical Case Report. Operative Neurosurgery 2006;59:ONSE487-8; discussion ONSE Choi KC, Kim JS, Park CK. Percutaneous Endoscopic Lumbar Discectomy as an Alternative to Open Lumbar Microdiscectomy for Large Lumbar Disc Herniation. Pain Physician 2016;19:E Kim JE, Kim KH. Piriformis syndrome after percutaneous endoscopic lumbar discectomy via the posterolateral approach. Eur Spine J 2011;20: Gardner A, Gardner E, Morley T. Cauda equina syndrome: a review of the current clinical and medicolegal position. Eur Spine J 2011;20: Gleave JR, Macfarlane R. Cauda equina syndrome: what is the relationship between timing of surgery and outcome? Br J Neurosurg 2002;16: Li X, Dou Q, Hu S, et al. Treatment of cauda equina syndrome caused by lumbar disc herniation with percutaneous endoscopic lumbar discectomy. Acta Neurol Belg 2016;116: Choi KC, Lee JH, Kim JS, et al. Unsuccessful percutaneous endoscopic lumbar discectomy: a single-center experience of 10,228 cases. Neurosurgery 2015;76:372-80; discussion 380-1; quiz Lee SH, Choi KC, Baek OK, et al. Percutaneous Endoscopic Intra-annular Subligamentous Herniotomy for Large Central Disc Herniation. Spine (Phila Pa 1976) 2014;39:E Kang Q, Li X, Cheng Z, et al. Effects of release and decompression techniques on nerve roots through percutaneous transforaminal endoscopic discectomy on patients with central lumbar disc herniation. Exp Ther Med 2017;13: Phan K, Xu J, Schultz K, et al. Full-endoscopic versus micro-endoscopic and open discectomy: A systematic review and meta-analysis of outcomes and complications. Clin Neurol Neurosurg 2017;154: Ran J, Hu Y, Zheng Z, et al. Comparison of Discectomy versus Sequestrectomy in Lumbar Disc Herniation: A Meta-Analysis of Comparative Studies. PLoS One 2015;10:e Choi KC, Shim HK, Park CJ, et al. Usefulness of Percutaneous Endoscopic Lumbar Foraminoplasty for Lumbar Disc Herniation. World Neurosurg 2017;106: Li ZZ, Hou SX, Shang WL, et al. Modified Percutaneous Lumbar Foraminoplasty and Percutaneous Endoscopic Lumbar Discectomy: Instrument Design, Technique Notes, and 5 Years Follow-up. Pain Physician 2017;20:E Kambin P, Sampson S. Posterolateral percutaneous suction-excision of herniated lumbar intervertebral discs. Report of interim results. Clin Orthop Relat Res 1986;(207): Cite this article as: Kondo M, Oshima Y, Inoue H, Takano Y, Inanami H, Koga H. Significance and pitfalls of percutaneous endoscopic lumbar discectomy for large central lumbar disc herniation.. doi: / jss
Consideration of proper operative route for interlaminar approach for percutaneous endoscopic lumbar discectomy
 Original Study Consideration of proper operative route for interlaminar approach for percutaneous endoscopic lumbar discectomy Juichi Tonosu 1,2,3,4, Yasushi Oshima 1,2,3, Ryutaro Shiboi 1,2, Akihiko Hayashi
Original Study Consideration of proper operative route for interlaminar approach for percutaneous endoscopic lumbar discectomy Juichi Tonosu 1,2,3,4, Yasushi Oshima 1,2,3, Ryutaro Shiboi 1,2, Akihiko Hayashi
Percutaneous endoscopic lumbar discectomy via adjacent interlaminar space for highly down-migrated lumbar disc herniation: a technical report
 Case Report Percutaneous endoscopic lumbar discectomy via adjacent interlaminar space for highly down-migrated lumbar disc herniation: a technical report Yasushi Inomata 1,2, Yasushi Oshima 1,3,4, Hirokazu
Case Report Percutaneous endoscopic lumbar discectomy via adjacent interlaminar space for highly down-migrated lumbar disc herniation: a technical report Yasushi Inomata 1,2, Yasushi Oshima 1,3,4, Hirokazu
Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy
 Case Report Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy Ryutaro Shiboi 1,2, Yasushi Oshima 1,2,3, Takeshi Kaneko
Case Report Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy Ryutaro Shiboi 1,2, Yasushi Oshima 1,2,3, Takeshi Kaneko
A less invasive surgery using a full-endoscopic system for L5 nerve root compression caused by lumbar foraminal stenosis
 Original Study A less invasive surgery using a full-endoscopic system for L5 nerve root compression caused by lumbar foraminal stenosis Katsuhiko Ishibashi 1,2, Yasushi Oshima 1,2,3, Hirokazu Inoue 1,2,4,
Original Study A less invasive surgery using a full-endoscopic system for L5 nerve root compression caused by lumbar foraminal stenosis Katsuhiko Ishibashi 1,2, Yasushi Oshima 1,2,3, Hirokazu Inoue 1,2,4,
Minimal laminectomy using the interlaminar approach for percutaneous endoscopic lumbar discectomy
 Mini-invasive Surg 2017;1:56-62 DOI: 10.20517/2574-1225.2017.04 Topic: Percutaneous endoscopic system for spinal diseases Mini-invasive Surgery www.misjournal.net Open Access Minimal laminectomy using
Mini-invasive Surg 2017;1:56-62 DOI: 10.20517/2574-1225.2017.04 Topic: Percutaneous endoscopic system for spinal diseases Mini-invasive Surgery www.misjournal.net Open Access Minimal laminectomy using
Initial Clinical Outcomes of Percutaneous Full- Endoscopic Lumbar Discectomy Using an Interlaminar Approach at the L4-L5
 Pain Physician 2017; 20:E507-E512 ISSN 2150-1149 Retrospective Evaluation Initial Clinical Outcomes of Percutaneous Full- Endoscopic Lumbar Discectomy Using an Interlaminar Approach at the L4-L5 Jun-ichiro
Pain Physician 2017; 20:E507-E512 ISSN 2150-1149 Retrospective Evaluation Initial Clinical Outcomes of Percutaneous Full- Endoscopic Lumbar Discectomy Using an Interlaminar Approach at the L4-L5 Jun-ichiro
paracentral disc herniations, especially disc extrusions and disc sequestrations, remains challenging.
 Orthopaedic Surgery SURGICAL TECHNOLOGY INTERNATIONAL XIX Transforaminal Endoscopic Lumbar Procedure for Disc Herniations: A "Between" Technique KAI-XUAN LIU, M.D, PH.D. ATLANTIC SPINAL CARE EDISON, NEW
Orthopaedic Surgery SURGICAL TECHNOLOGY INTERNATIONAL XIX Transforaminal Endoscopic Lumbar Procedure for Disc Herniations: A "Between" Technique KAI-XUAN LIU, M.D, PH.D. ATLANTIC SPINAL CARE EDISON, NEW
A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
 Pain Physician 2017; 20:E605-E609 ISSN 2150-1149 Case Report A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
Pain Physician 2017; 20:E605-E609 ISSN 2150-1149 Case Report A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
How I do it: percutaneous transforaminal endoscopic discectomy for lumbar disk herniation
 Acta Neurochirurgica (2018) 160:2473 2477 https://doi.org/10.1007/s00701-018-3723-5 HOW I DO IT - SPINE DEGENERATIVE How I do it: percutaneous transforaminal endoscopic discectomy for lumbar disk herniation
Acta Neurochirurgica (2018) 160:2473 2477 https://doi.org/10.1007/s00701-018-3723-5 HOW I DO IT - SPINE DEGENERATIVE How I do it: percutaneous transforaminal endoscopic discectomy for lumbar disk herniation
REFERENCE DOCTOR Percutaneous Endoscopic Discectomy Transforaminal / Interlaminar. Hyeun Sung Kim, MD, PhD,
 Percutaneous Endoscopic Discectomy Transforaminal / Interlaminar Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean
Percutaneous Endoscopic Discectomy Transforaminal / Interlaminar Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean
Foraminoplastic transfacet epidural endoscopic approach for removal of intraforaminal disc herniation at the L5-S1 level
 Case report Videosurgery Foraminoplastic transfacet epidural endoscopic approach for removal of intraforaminal disc herniation at the L5-S1 level Łukasz Kubaszewski 1, Jacek Kaczmarczyk 1, Andrzej Nowakowski
Case report Videosurgery Foraminoplastic transfacet epidural endoscopic approach for removal of intraforaminal disc herniation at the L5-S1 level Łukasz Kubaszewski 1, Jacek Kaczmarczyk 1, Andrzej Nowakowski
Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion
 Original Study Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion Tomohide Segawa 1, Hirohiko Inanami 1, Hisashi Koga 2 1 Department of Orthopaedic Surgery, Inanami Spine and
Original Study Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion Tomohide Segawa 1, Hirohiko Inanami 1, Hisashi Koga 2 1 Department of Orthopaedic Surgery, Inanami Spine and
JCSC INTRODUCTION. Rudolf Morgenstern, MD, PhD
 Diagnosis The lumbar lateral X-ray images in forward flexion and extension showed an anterior displacement of 10 mm in extension and of 6 mm in flexion measured with the methonline ML Comm JCSC DEGENERATIVE
Diagnosis The lumbar lateral X-ray images in forward flexion and extension showed an anterior displacement of 10 mm in extension and of 6 mm in flexion measured with the methonline ML Comm JCSC DEGENERATIVE
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Lumbar disc reherniation after transforaminal lumbar endoscopic discectomy
 Original Article Page 1 of 5 Lumbar disc reherniation after transforaminal lumbar endoscopic discectomy Thomas A. Kosztowski, David Choi, Jared Fridley, Michael Galgano, Ziya Gokaslan, Adetokunbo Oyelese,
Original Article Page 1 of 5 Lumbar disc reherniation after transforaminal lumbar endoscopic discectomy Thomas A. Kosztowski, David Choi, Jared Fridley, Michael Galgano, Ziya Gokaslan, Adetokunbo Oyelese,
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review
 Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
Back Pain Policies Summary
 Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Recurrent upper lumbar disc herniation treated via the transforaminal approach using microendoscopy-assisted lumbar discectomy: a case report
 Takagi et al. Journal of Medical Case Reports (2018) 12:110 https://doi.org/10.1186/s13256-018-1653-8 CSE REPORT Open ccess Recurrent upper lumbar disc herniation treated via the transforaminal approach
Takagi et al. Journal of Medical Case Reports (2018) 12:110 https://doi.org/10.1186/s13256-018-1653-8 CSE REPORT Open ccess Recurrent upper lumbar disc herniation treated via the transforaminal approach
Physician Reference Manual
 Nucleotome Physician Reference Manual Automated Percutaneous Lumbar Discectomy 900487-001-00, Page 1 Nucleotome Automated Percutaneous Lumbar Discectomy (APLD) Table of Contents Section 1 I. Description
Nucleotome Physician Reference Manual Automated Percutaneous Lumbar Discectomy 900487-001-00, Page 1 Nucleotome Automated Percutaneous Lumbar Discectomy (APLD) Table of Contents Section 1 I. Description
Hemorrhagic Facet Cyst in the Lumbar Spine Causing Contralateral Leg Symptoms: A Case Report
 Asian Spine Journal Vol. 5, No. 3, pp 196~200, 2011 http://dx.doi.org/10.4184/asj.2011.5.3.196 Hemorrhagic Facet Cyst in the Lumbar Spine Causing Contralateral Leg Symptoms: A Case Report Risa Utsunomiya,
Asian Spine Journal Vol. 5, No. 3, pp 196~200, 2011 http://dx.doi.org/10.4184/asj.2011.5.3.196 Hemorrhagic Facet Cyst in the Lumbar Spine Causing Contralateral Leg Symptoms: A Case Report Risa Utsunomiya,
Posterior decompression via total laminectomy and
 CASE REPORT J Neurosurg Spine 27:352 356, 2017 Anterior lumbar discectomy and fusion for acute cauda equina syndrome caused by recurrent disc prolapse: report of 3 cases Kimberly-Anne Tan, MBBS, 1,2 Mathew
CASE REPORT J Neurosurg Spine 27:352 356, 2017 Anterior lumbar discectomy and fusion for acute cauda equina syndrome caused by recurrent disc prolapse: report of 3 cases Kimberly-Anne Tan, MBBS, 1,2 Mathew
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Retro-odontoid pseudotumors are mass lesions formed
 SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Transforaminal Endoscopic Discectomy for Treatment of Central Disc Herniation: Surgical Techniques and Clinical Outcome
 Pain Physician 2018; 21:E113-E123 ISSN 2150-1149 Retrospective Review Transforaminal Endoscopic Discectomy for Treatment of Central Disc Herniation: Surgical Techniques and Clinical Outcome Yapeng Wang,
Pain Physician 2018; 21:E113-E123 ISSN 2150-1149 Retrospective Review Transforaminal Endoscopic Discectomy for Treatment of Central Disc Herniation: Surgical Techniques and Clinical Outcome Yapeng Wang,
MOHAMED LOTFY, M.D.*; SAMEH A. SAKR, M.D.* and ASHRAF E. ZAGHLOUL, M.D.**
 Med. J. Cairo Univ., Vol. 84, No. 1, December: 1463-1469, 216 www.medicaljournalofcairouniversity.net Extensive Laminectomy for Redo Lumbar Discectomy; Could it Be A Successful Alternative Option in Stable
Med. J. Cairo Univ., Vol. 84, No. 1, December: 1463-1469, 216 www.medicaljournalofcairouniversity.net Extensive Laminectomy for Redo Lumbar Discectomy; Could it Be A Successful Alternative Option in Stable
Index 377 Index A Alajouanine, T. H., 6 Ancient medicine, management of back and leg pain, 1 3 Anesthesia, microendoscopic discectomy, 364, 365 minima
 Index 377 Index A Alajouanine, T. H., 6 Ancient medicine, management of back and leg pain, 1 3 Anesthesia, microendoscopic discectomy, 364, 365 minimally invasive lumbar surgery, 75, 76 percutaneous transpedicular
Index 377 Index A Alajouanine, T. H., 6 Ancient medicine, management of back and leg pain, 1 3 Anesthesia, microendoscopic discectomy, 364, 365 minimally invasive lumbar surgery, 75, 76 percutaneous transpedicular
Case Report A Rare Case of Progressive Palsy of the Lower Leg Caused by a Huge Lumbar Posterior Endplate Lesion after Recurrent Disc Herniation
 Case Reports in Orthopedics Volume 2016, Article ID 5963924, 4 pages http://dx.doi.org/10.1155/2016/5963924 Case Report A Rare Case of Progressive Palsy of the Lower Leg Caused by a Huge Lumbar Posterior
Case Reports in Orthopedics Volume 2016, Article ID 5963924, 4 pages http://dx.doi.org/10.1155/2016/5963924 Case Report A Rare Case of Progressive Palsy of the Lower Leg Caused by a Huge Lumbar Posterior
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
Hongyu Song 1, Wenhao Hu 1, Zhongguo Liu 2, Yongyu Hao 1 and Xuesong Zhang 1*
 Song et al. Journal of Orthopaedic Surgery and Research (2017) 12:162 DOI 10.1186/s13018-017-0662-4 RESEARCH ARTICLE Percutaneous endoscopic interlaminar discectomy of L5 S1 disc herniation: a comparison
Song et al. Journal of Orthopaedic Surgery and Research (2017) 12:162 DOI 10.1186/s13018-017-0662-4 RESEARCH ARTICLE Percutaneous endoscopic interlaminar discectomy of L5 S1 disc herniation: a comparison
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Long-term Follow-up Results of Percutaneous Endoscopic Lumbar Discectomy. Sang Soo Eun, MD, Sang Ho Lee, MD, PhD, and Luigi Andrew Sabal, MD
 Pain Physician 2016; 19:E1161-E1166 ISSN 2150-1149 Retrospective Evaluation Long-term Follow-up Results of Percutaneous Endoscopic Lumbar Discectomy Sang Soo Eun, MD, Sang Ho Lee, MD, PhD, and Luigi Andrew
Pain Physician 2016; 19:E1161-E1166 ISSN 2150-1149 Retrospective Evaluation Long-term Follow-up Results of Percutaneous Endoscopic Lumbar Discectomy Sang Soo Eun, MD, Sang Ho Lee, MD, PhD, and Luigi Andrew
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
Case Report Transpedicular Endoscopic Surgery for Highly Downmigrated L5-S1 Disc Herniation
 Case Reports in Medicine Volume 2019, Article ID 5724342, 9 pages https://doi.org/10.1155/2019/5724342 Case Report Transpedicular Endoscopic Surgery for Highly Downmigrated L5-S1 Disc Herniation Guntram
Case Reports in Medicine Volume 2019, Article ID 5724342, 9 pages https://doi.org/10.1155/2019/5724342 Case Report Transpedicular Endoscopic Surgery for Highly Downmigrated L5-S1 Disc Herniation Guntram
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Nursing review section of Surgical Neurology International: Part 1 lumbar disc disease
 SNI: Neurosurgical Nursing OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article Nursing review
SNI: Neurosurgical Nursing OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article Nursing review
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients
 Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves
 2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves Joseph S. Cheng, M.D., M.S. Associate Professor of Neurological Surgery, Orthopedic Surgery, and Rehabilitation
2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves Joseph S. Cheng, M.D., M.S. Associate Professor of Neurological Surgery, Orthopedic Surgery, and Rehabilitation
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
Case Report Discoscopic Findings of High Signal Intensity Zones on Magnetic Resonance Imaging of Lumbar Intervertebral Discs
 Case Reports in Orthopedics, Article ID 245952, 5 pages http://dx.doi.org/10.1155/2014/245952 Case Report Discoscopic Findings of High Signal Intensity Zones on Magnetic Resonance Imaging of Lumbar Intervertebral
Case Reports in Orthopedics, Article ID 245952, 5 pages http://dx.doi.org/10.1155/2014/245952 Case Report Discoscopic Findings of High Signal Intensity Zones on Magnetic Resonance Imaging of Lumbar Intervertebral
Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous endoscopic laser lumbar discectomy Symptomatic lumbar disc prolapse
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous endoscopic laser lumbar discectomy Symptomatic lumbar disc prolapse
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
The Clinical Outcomes of Transforaminal Percutaneous Endoscopic Discectomy in Treating Lumbar Disc Herniation: A Review
 Open Journal of Orthopedics, 2018, 8, 57-66 http://www.scirp.org/journal/ojo ISSN Online: 2164-3016 ISSN Print: 2164-3008 The Clinical Outcomes of Transforaminal Percutaneous Endoscopic Discectomy in Treating
Open Journal of Orthopedics, 2018, 8, 57-66 http://www.scirp.org/journal/ojo ISSN Online: 2164-3016 ISSN Print: 2164-3008 The Clinical Outcomes of Transforaminal Percutaneous Endoscopic Discectomy in Treating
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
Surgical considerations in patients with lumbar spinal root anomalies
 Paraplegia 30 (1992) 370-375 1992 International Medical Society of Paraplegia Surgical considerations in patients with lumbar spinal root anomalies M N Pamir MD,! M MOzek MD,2 A F Ozer MD, G E Kele MD,
Paraplegia 30 (1992) 370-375 1992 International Medical Society of Paraplegia Surgical considerations in patients with lumbar spinal root anomalies M N Pamir MD,! M MOzek MD,2 A F Ozer MD, G E Kele MD,
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
1. Introduction: 3. Surgical Procedures. 2. Indications. 3.a. Surgical Instruments. 3.b. Patient Positioning. 3.c. Surgical Technique
 1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
NUCLEOPLASTY PERCUTANEOUS DISC DECOMPRESSION
 NUCLEOPLASTY PERCUTANEOUS DISC DECOMPRESSION ISSUE Blue Shield has received requests for coverage of nucleoplasty percutaneous disc decompression for herniated discs. The Medical Policy Committee on Quality
NUCLEOPLASTY PERCUTANEOUS DISC DECOMPRESSION ISSUE Blue Shield has received requests for coverage of nucleoplasty percutaneous disc decompression for herniated discs. The Medical Policy Committee on Quality
ASJ. Asian Spine Journal. Introduction
 Asian Spine Journal 190 Ko Ikuta Clinical et al. Study Asian Spine J 2013;7(3):190-195 http://dx.doi.org/10.4184/asj.2013.7.3.190 Asian Spine J 2013;7(3):190-195 Translaminar Microendoscopic Herniotomy
Asian Spine Journal 190 Ko Ikuta Clinical et al. Study Asian Spine J 2013;7(3):190-195 http://dx.doi.org/10.4184/asj.2013.7.3.190 Asian Spine J 2013;7(3):190-195 Translaminar Microendoscopic Herniotomy
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Endoscopic Spine Surgery: Distance Patients Will Travel for Minimally Invasive Spine Surgery
 Pain Physician 2017; 20:E145-E149 ISSN 2150-1149 Retrospective Review Endoscopic Spine Surgery: Distance Patients Will Travel for Minimally Invasive Spine Surgery Albert Edward Telfeian, MD, PhD, Menno
Pain Physician 2017; 20:E145-E149 ISSN 2150-1149 Retrospective Review Endoscopic Spine Surgery: Distance Patients Will Travel for Minimally Invasive Spine Surgery Albert Edward Telfeian, MD, PhD, Menno
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy
 Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
Axial Lumbosacral Interbody Fusion. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
This procedure lacks scientific evidence of effectiveness, and is not covered.
 ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
Percutaneous endoscopic discectomy: Gold standard technique for single level intervertebral disc prolapse
 2018; 4(3): 586-590 ISSN: 2395-1958 IJOS 2018; 4(3): 586-590 2018 IJOS www.orthopaper.com Received: 11-05-2018 Accepted: 12-06-2018 Dr. Hardik Sethi M.S. Ortho, Senior Resident Dept. Of Orthopaedics Govt.
2018; 4(3): 586-590 ISSN: 2395-1958 IJOS 2018; 4(3): 586-590 2018 IJOS www.orthopaper.com Received: 11-05-2018 Accepted: 12-06-2018 Dr. Hardik Sethi M.S. Ortho, Senior Resident Dept. Of Orthopaedics Govt.
Variations in arterial supply to the lower lumbar spine
 Eur Spine J (2016) 25:4181 4187 DOI 10.1007/s00586-016-4427-2 ORIGINAL ARTICLE Variations in arterial supply to the lower lumbar spine Fumitake Tezuka 1 Toshinori Sakai 1 Toshihiko Nishisho 1 Yoichiro
Eur Spine J (2016) 25:4181 4187 DOI 10.1007/s00586-016-4427-2 ORIGINAL ARTICLE Variations in arterial supply to the lower lumbar spine Fumitake Tezuka 1 Toshinori Sakai 1 Toshihiko Nishisho 1 Yoichiro
Some of the electrothermal intradiscal procedures are briefly described.
 Medical Coverage Policy Minimally Invasive Intradiscal and Annular Procedures for Back Pain EFFECTIVE DATE: 10 01 2004 POLICY LAST UPDATED: 07 18 2017 OVERVIEW This policy addresses a variety of minimally
Medical Coverage Policy Minimally Invasive Intradiscal and Annular Procedures for Back Pain EFFECTIVE DATE: 10 01 2004 POLICY LAST UPDATED: 07 18 2017 OVERVIEW This policy addresses a variety of minimally
Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report
 Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Risk factors for failure of single-level percutaneous endoscopic lumbar discectomy
 spine clinical article J Neurosurg Spine 23:320 325, 2015 Risk factors for failure of single-level percutaneous endoscopic lumbar discectomy *Hongwei Wang, MD, PhD, 1 Yue Zhou, MD, PhD, 2 Changqing Li,
spine clinical article J Neurosurg Spine 23:320 325, 2015 Risk factors for failure of single-level percutaneous endoscopic lumbar discectomy *Hongwei Wang, MD, PhD, 1 Yue Zhou, MD, PhD, 2 Changqing Li,
Huan-Chieh Chen, 1 Chih-Hsun Lee, 1 Li Wei, 1 Tai-Ngar Lui, 1 and Tien-Jen Lin 1,2. 1. Introduction
 Neurology Research International Volume 2015, Article ID 791943, 5 pages http://dx.doi.org/10.1155/2015/791943 Clinical Study Comparison of Percutaneous Endoscopic Lumbar Discectomy and Open Lumbar Surgery
Neurology Research International Volume 2015, Article ID 791943, 5 pages http://dx.doi.org/10.1155/2015/791943 Clinical Study Comparison of Percutaneous Endoscopic Lumbar Discectomy and Open Lumbar Surgery
Thoracic disc herniation: Postero-lateral approach
 Thoracic disc herniation: Postero-lateral approach Antonino Raco MD Professor and Chairman of Neurosurgery Department of Neurosciences, Mental Health and Sense Organs (NESMOS), Sapienza Università di Roma
Thoracic disc herniation: Postero-lateral approach Antonino Raco MD Professor and Chairman of Neurosurgery Department of Neurosciences, Mental Health and Sense Organs (NESMOS), Sapienza Università di Roma
With an annual incidence of 5 cases per focus Neurosurg Focus 40 (2):E3, 2016
 neurosurgical focus Neurosurg Focus 40 (2):E3, 2016 Clinical outcomes after percutaneous transforaminal endoscopic discectomy for lumbar disc herniation: a prospective case series Pravesh S. Gadjradj,
neurosurgical focus Neurosurg Focus 40 (2):E3, 2016 Clinical outcomes after percutaneous transforaminal endoscopic discectomy for lumbar disc herniation: a prospective case series Pravesh S. Gadjradj,
Clinical and Radiological Findings of Nerve Root Herniation after Discectomy of Lumbar Disc Herniation
 www.jkns.or.kr J Korean Neurosurg Soc 52 : 62-66, 2012 http://dx.doi.org/10.3340/jkns.2012.52.1.62 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2012 The Korean Neurosurgical Society Case Report
www.jkns.or.kr J Korean Neurosurg Soc 52 : 62-66, 2012 http://dx.doi.org/10.3340/jkns.2012.52.1.62 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2012 The Korean Neurosurgical Society Case Report
Retrospective Study. Pain Physician 2018; 21:E401-E408 ISSN
 Pain Physician 2018; 21:E401-E408 ISSN 2150-1149 Retrospective Study Percutaneous Endoscopic Lumbar Discectomy for All Types of Lumbar Disc Herniations (LDH) Including Severely Difficult and Extremely
Pain Physician 2018; 21:E401-E408 ISSN 2150-1149 Retrospective Study Percutaneous Endoscopic Lumbar Discectomy for All Types of Lumbar Disc Herniations (LDH) Including Severely Difficult and Extremely
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Revisional Percutaneous Full Endoscopic Disc Surgery for Recurrent Herniation of Previous Open Lumbar Discectomy
 Asian Spine Journal Vol. 5, No. 1, pp 1~9, 2011 doi:10.4184/asj.2011.5.1.1 Revisional Percutaneous Full Endoscopic Disc Surgery for Recurrent Herniation of Previous Open Lumbar Discectomy Kyung Hyun Shin
Asian Spine Journal Vol. 5, No. 1, pp 1~9, 2011 doi:10.4184/asj.2011.5.1.1 Revisional Percutaneous Full Endoscopic Disc Surgery for Recurrent Herniation of Previous Open Lumbar Discectomy Kyung Hyun Shin
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment
 Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Current Spine Procedures
 SPINE BOOT CAMP: WHAT YOU DON T KNOW MAY COST YOU! David Abraham, M.D. The Reading Neck and Spine Center Reading, PA Current Spine Procedures Epidural/Transforaminal Injections Lumbar Procedures Laminectomy
SPINE BOOT CAMP: WHAT YOU DON T KNOW MAY COST YOU! David Abraham, M.D. The Reading Neck and Spine Center Reading, PA Current Spine Procedures Epidural/Transforaminal Injections Lumbar Procedures Laminectomy
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Automated Percutaneous and Endoscopic Discectomy. Original Policy Date
 MP 7.01.13 Automated Percutaneous and Endoscopic Discectomy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.13 Automated Percutaneous and Endoscopic Discectomy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Corporate Medical Policy
 Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
Corporate Medical Policy Axial Lumbosacral Interbody Fusion File Name: Origination: Last CAP Review: Next CAP Review: Last Review: axial_lumbosacral_interbody_fusion 6/2009 10/2017 10/2018 10/2017 Description
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Unique Complications of Percutaneous Endoscopic Lumbar Discectomy and Percutaneous Endoscopic Interlaminar Discectomy
 Pain Physician 2018; 21:E105-E112 ISSN 2150-1149 Retrospective Review Unique Complications of Percutaneous Endoscopic Lumbar Discectomy and Percutaneous Endoscopic Interlaminar Discectomy Chuanli Zhou,
Pain Physician 2018; 21:E105-E112 ISSN 2150-1149 Retrospective Review Unique Complications of Percutaneous Endoscopic Lumbar Discectomy and Percutaneous Endoscopic Interlaminar Discectomy Chuanli Zhou,
REFERENCE DOCTOR Thoracolumbar Trauma MIS Options. Hyeun Sung Kim, MD, PhD,
 Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Lumbar disc prolapse. Done by : Areej Al-Hadidi
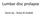 Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Orthopedic Coding Changes for 2012
 Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
