Posterior surgical procedures are those procedures
|
|
|
- Robyn Jefferson
- 5 years ago
- Views:
Transcription
1 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including cervical spondylosis. However, complaints including pain and spasm is common in the postoperative period related to the widespread subperiostal dissection on the paraspinal muscles in the open posterior cervical interventions (18-60%). 3,5 In addition, in case there is any preoperative lordosis loss for posterior interventions or for multiple decompressions, the risk of development of deformity in the sagittal plane will be high. Posterior stabilization techniques will eliminate this risk; however, this will increase the operation time and blood loss. Furthermore, there is the potential risk of adjacent segment degeneration development. With these reasons, laminoforaminatomy, which is among the minimal invasive spinal surgery techniques gradually developing within the recent years, is used as a minimal invasive technique. This technique is gradually gaining importance with reasons including the minimal injury caused on the normal anatomical structures during the procedure, reducing of postoperative pain and hospital stay period, and most importantly, the minimal damage on the normal structures of the anatomical support structures minimizing the structural changes including kyphosis, etc. that can develop in time. 8,9 Advantages of Posterior Laminoforaminotomy Laminoforaminatomy allows the direct exposure of the nerve root and also allows better opening of the nerve root. At the same time, the nerve root can be decompressed easily without any need for fusion. Posterior Laminoforaminotomy Laminoforaminatomy does not impair the integrity of the intervertebral disc. There is no risk of complications including graft dislocation or pseudoarthrosis with this technique. Furthermore, patients will not need to wear collars for long periods of time in the preoperative period, and use of a soft cervical collar only for convenience for 1 to 2 weeks will suffice. The risk of tracheal or esophageal injuries that can be seen with anterior surgical techniques and the cerebrovascular complications that can develop in relation with carotid compression do not exist. Furthermore, since this is a minimal invasive intervention, the damages on the posterior muscular structures will be at a minimal level, and this will increase the comfort of the patient in the postoperative period. 4,7 Selection of Patients In line with all the decisions for any surgical intervention technique, evaluating the patient in detail is very important when making the decision also for this procedure. A good physical and neurological examination is important in the first place. Patients with mono-lateral radicular symptoms are suitable candidates for laminoforaminatomy in general. For example, patients with repeating symptoms with Spurling maneuver are ideal candidates for laminoforaminatomy, because the nerve root is compressed between the uncinate process and the facet joint in these patients, and removing the dorsal portion of the neural foramen will provide good surgical result. A good radiological examination following the clinical examination is indispensible for the decisionmaking process for the surgery. Posterior laminofotaminotomy is the proper choice if mono-lateral soft 47
2 48 disc or small lateral osteophytes are present radiologically to support the clinical picture. However, if the principal complaint of the patient is axial neck pain and foraminal narrowing and spinal chord compression are present together, such patients are not suitable for laminoforaminatomy. Moreover, if the hypermobility consistent with instability is present in the dynamic x-rays, posterior laminoforaminatomy will be contra-indicated in this patient group. Therefore, dynamic and static x-rays together with magnetic resonance (MR) images must be taken as a minimum before making the decision for the surgical intervention method, and in cases where MR does not suffice the computerized tomography (CT) images must be taken. In conclusion, the clinically suitable and unsuitable cases for posterior laminoforaminotomy can be listed as follows: Suitable patient group: Clinical picture of mono-lateral radiculopathy Posterolateral soft disc hernia appearance Lateral osteophyte appearance Unsuitable patient group: Axial pain getting ahead of the radiculopathy clinical picture Myelopathy findings Midline or hard disc herniation appearance Widespread osteophyte appearance OPLL Presence of instability Anatomy of Cervical Neural Foramina Being familiar with the 3-dimensional anatomy of the cervical neural foramen is required to achieve the optimal surgical success. The lateral faces of the superior and inferior laminas from the posterior surround lateral part of the spinal channel. Ligamentum flavum is attached to two-thirds of the superior lamina at the ventral aspect of the lamina, while the same is attached only to the upper portion of the inferior lamina in the inferior aspect. In the lateral, ligamentum flavum end at 1-2mm medal of the neural foramen. The anterior border of the cervical neural foramen extends from rostral to the caudal following the posterolateral cortical side of the superior vertebral body, the intervertebral disc wrapped within the posterior longitudinal ligament, and a small portion of the posterolateral edge of the inferior vertebral body. In the posterior, neural foramen is limited from the rostral to the caudal with a portion of 1-2 mm of the superior facet, and the entire ventral face of the inferior facet follows this. Superior and inferior borders of the neural foramen consist of the pedicles of the superior and inferior vertebras, respectively. (Figures 1a and 1b) Figure 1: a and b: Relation with the facet joints of the cervical neural foramen and pedicles
3 Surgical Technique Position The best position for the patient is the one that will minimize blood loss and provide the best visual angle. Therefore prone or sitting positions can be used based on the experience and preference of the surgeon. Skull clamp with pins can be used for the sitting position, and crescent shaped halo or skull clamp again can be used for the prone position. Slight extension of the neck will provide comfort during the surgery, since it will cause opening of the distance between the facet joints. Fixing the position of the patient with the thought that position changes might be necessary during the surgery. Giving the reverse Trendelenburg position to the operation table in the last stage will be wise to direct the blood to the legs and abdomen. (Figure 2) Cervical Posterior Laminoforaminotomy lateral of the midline (ipsilateral) 2 cm in length will suffice for the single-space procedures. (Figure 3) If the intervention is made through a midline incision, the fascia is opened on the spinous process, and paravertebral muscles are dissected up to the lateral border of the lateral mass. For the interventions made from the lateral of the midline, the tubular dilatation systems of endoscopic systems are used to reach the lateral mass and lamina directly through the muscle fibers. The most important issue in this issue is to protect the capsule of the facet joint. 49 Figure 3: Midline skin incision about 2 cm long Figure 2: Surgical preparation; patient with the crescent shaped hood in prone position Skin Incision and Muscle Dissection It is important to determine the surgical area under the guidance of fluoroscopy. After placing a metal object (e.g. K-wire) at the lateral of the patient s neck, the projection of the fluoroscopy image of the wire on the skin will be marked, and will be determined as the midpoint of the skin incision for the single-space procedures. A skin incision at the midline or 1.5 cm Laminoforaminotomy After exposing the lamina and lateral masses, the microscope will be taken onto the field. The purpose is to expose the nerve root causing the clinical picture of radiculopathy. Using high-speed drill will facilitate the procedure in this stage. In the first place, the lower end of the lateral part of the lamina at the cephalic side of the space and the inferior articular process constituting the lateral mass will be resected with the help of the drill. In general, 1 to 2 mm resection of the inferior articular process will suffice. (Figure 4) Following the resection of the inferior articular process, the superior articular process constituting the lateral mass immediately beneath it will be exposed. The superior articular process will be resected till the pedicle making the lower border of the neural foramen is exposed. (Figure 5) In this stage, removal of the lateral part of the ligamentum flavum with the help of the Kerrison rongeur will ensure exposure of the nerve root. (Figure 6) Following the nerve root towards the lateral will contribute
4 50 to the sufficient bone decompression. Disc herniation is often seen in the caudal of the nerve root. Although rare, it must be kept in mind that it can also be at the cephalic side, like in the lumbar disc herniation. When the nerve root is gently retracted to the cephalic side, the extruded disc hernia will be seen right below the nerve root, or the disc hernia will be seen under the posterior longitudinal ligament. The most important issue into be remembered at this state is that the nerve root must never be retracted to the caudal. Retracting the nerve root to the caudal can damage the nerve root or the spinal chord. In case working on the nerve root from the cephalic side will be needed because the disc herniation is located on the cephalic side, the best thing to do is to remove more bone instead of retracting the nerve root to enlarge the working area so that no nerve retraction will be needed. Bleeding originating from the venous plexus is a condition commonly seen in this procedure after opening the foramen. Bleeding can be controlled with bipolar coagulation or with the help of small surgical pads. Use of materials like pads or cotton so as to compress the nerve root must be avoided. If the disc hernia is extruded, the small disc will be removed with the help of a rongeur. Against the possibility of presence of more small fragments, proximal and distal and caudal and cephalic faces of the nerve root will the screened using a like a nerve hook. After removing the free disc fragments, procedure can be terminated at this stage if it is thought that sufficient decompression has been ensured. If the posterior longitudinal ligament is intact, the posterior longitudinal ligament will be opened with the help of a blade after retracting the nerve root gently to the cephalic side. Disc material will be removed until it is seen that the nerve root is decompressed sufficiently. At this stage, care must be given to whether or not there are any free disc fragments left. Following sufficient hemostasis, layers will be closed like in any normal posterior cervical opening. Figure 4: Resection border until the surface of the superior articular process of the inferior articular process Figure 5: Removal of the inferior articular process up to the upper edge of the pedicle (P)
5 Figure 6: Laminoforaminotomy margins after the bone resection. (P: pedicle) Complications Cervical Posterior Laminoforaminotomy If dura tear had occurred, it is very important to repair the dura very well in order to prevent complications including CSF fistulas and related meningitis in the postoperative period. Use of tissue adhesives or barriers is recommended to prevent the CSF fistula to assist if needed. The suspicion that instability can occur in case the facet joint is removed partially. The instability risk will be less if 50% of the facet joint is preserved. In addition, preserving the facet capsule is important that is outside the working area to the extent possible. Another important complication is spinal chord or nerve root injury. Cephalic retraction of the nerve root must be avoided to reduce the risk of this complication. In addition, it is important to make the bone thinner with the help of high-speed drill when performing the bone decompression and to remove the bone using a very thin Kerrison rongeur. It has been reported that radicular complaints can increase temporarily in about 10% of the patients after laminoforaminatomy procedure, and temporary paresthesia can be seen. This is attributed to the possibility that dorsal sensorial and ventral motor roots within one dura fold or can be present in separate dura folds. 1,2,6 51 Laminoforaminatomy has some certain complications as well as the potential complications of any surgical procedures including bleeding or infection. Such complications include the following: Dura injury and related cerebrospinal fluid (CSF) fistulas Meningitis Air embolism (particularly in patients operated in sitting position) Pneumocephalus Instability Injury of the nerve root or dura Taking certain measures or taking care about some issues can reduce the occurrence of the complications. Preferring the prone position instead of sitting position will reduce the air embolism risk. The reverse Trendelenburg position will reduce the bleeding risk. Conclusion Anterior surgical procedures are effective methods currently being carried out by many surgeons. However, it must be kept in mind that posterior laminoforaminotomy can also be an effective method with much greater safety in patients with radiculopathy related to soft disc with lateral localization as the principal complaint. Dorsal cervical laminoforaminatomy technique is a procedure that preserves motion in patients without instability, which does not involve risks seen in anterior surgical procedures related to the grafts and implants, and again with smaller costs as compared to the anterior procedures. Therefore, posterior cervical laminoforaminotomy technique is the method that must always be remembered for the carefully selected patient group with cervical radiculopathy.
6 52 References 1. Ebraheim NA, Xu R, Bhatti RA, Yeasting RA. The projection of the cervical disc and uncinate process on the posterior aspect of the cervical spine. Surg Neurol 51: , Fager C. Introduction and historical perspective on posterior cervical spine surgery, in Dillon W, Fa S (eds): Posterior Cervical Spine Surgery. Philadelphia, Lippincott-Raven, 1998, Fessler RG, Khoo LT. Minimally invasive cervical microendoscopic foraminotomy: an initial clinical experience. Neurosurgery 51: S37-S45, Parker WD. Cervical laminoforaminotomy. J Neurosurg 96: , Ratliff JK, Cooper PR. Cervical laminoplasty: a critical review. J Neurosurg 98: , Raynor RB, Pugh J, Shapiro L. Cervical facetectomy and its effect on spine strength. J Neurosurg 63: , Russel SM, Benjamin V. Posterior surgical approach to the cervical neural foramen for intervertebral disc disease. Neurosurgery 54: , Santiago P, Fessler RG. Minimally invasive surgery for the management of cervical spondylosis. Neurosurgery 60: , Wang MY. Minimally invasive surgery in the cervical spine: recent advances. Curr Opin Orthop 18: , 2007
Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University, Wakayama, JAPAN
 SURGICAL TECHNIQUES/DECISION -MAKING IN CERVICAL SPINE SURGERY: Cervico-Thoracic Junction Pathology Radiculopathy Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University,
SURGICAL TECHNIQUES/DECISION -MAKING IN CERVICAL SPINE SURGERY: Cervico-Thoracic Junction Pathology Radiculopathy Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University,
Keyhole Approach for Posterior Cervical Discectomy: Experience on 84 Patients
 Original Article 7 Keyhole Approach for Posterior Cervical Discectomy: Experience on 84 Patients Author Y. Ş. Ça ǧ lar1, M. Bozkurt 1, G. Kahilogullari 1, H. Tu na 1, A. Bakir 2, F. To r u n 1, H. C. U
Original Article 7 Keyhole Approach for Posterior Cervical Discectomy: Experience on 84 Patients Author Y. Ş. Ça ǧ lar1, M. Bozkurt 1, G. Kahilogullari 1, H. Tu na 1, A. Bakir 2, F. To r u n 1, H. C. U
1. Introduction: 3. Surgical Procedures. 2. Indications. 3.a. Surgical Instruments. 3.b. Patient Positioning. 3.c. Surgical Technique
 1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
The rise of minimally invasive techniques
 O R I G I N A L A R T I C L E S Minimally Invasive Foraminotomy of the Cervical Spine: Improving Technique and Expanding Indications Laura A. Snyder, MD Justin C. Clark, MD Luis M. Tumialán, MD The minimally
O R I G I N A L A R T I C L E S Minimally Invasive Foraminotomy of the Cervical Spine: Improving Technique and Expanding Indications Laura A. Snyder, MD Justin C. Clark, MD Luis M. Tumialán, MD The minimally
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy
 Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
Image-Guided Minimally Invasive Decompression for Spinal (701126) (Formerly Image-Guided Minimally Invasive Lumbar Decompression for Spinal ) Medical Benefit Effective Date: 10/01/17 Next Review Date:
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Populations Interventions Comparators Outcomes Individuals: With lumbar spinal stenosis
 Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
Image-Guided Minimally Invasive Decompression for Spinal (701126) Medical Benefit Effective Date: 10/01/18 Next Review Date: 07/19 Preauthorization No Review Dates: 09/10, 07/11, 07/12, 07/13, 07/14, 07/15,
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Retro-odontoid pseudotumors are mass lesions formed
 SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
 The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
The spine is made of a column of bones. Each bone, or vertebra, is formed by a round block of bone, called a vertebral body. A bony ring attaches to the back of the vertebral body. When the vertebra bones
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
T.L.I.F. Surgical Technique. Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System.
 Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
SpineFAQs. Cervical Disc Replacement
 SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
VERTEBRIS cervical Full-endoscopic Spinal Instrumentation. Vertebris
 VERTEBRIS cervical Full-endoscopic Spinal Instrumentation Vertebris 2 VERTEBRIS cervical, full-endoscopic techniques Table of contents Vertebris VERTEBRIS cervical 4 Introduction 4 The full-endoscopic
VERTEBRIS cervical Full-endoscopic Spinal Instrumentation Vertebris 2 VERTEBRIS cervical, full-endoscopic techniques Table of contents Vertebris VERTEBRIS cervical 4 Introduction 4 The full-endoscopic
This procedure lacks scientific evidence of effectiveness, and is not covered.
 ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
ARBenefits Approval: 09-21-2011 Effective Date: 01-01-2012 Revision Date: Code(s): 0275T Medical Policy Title: Minimally Invasive, Image-Guided Lumbar Decompression for Spinal Stenosis Document: ARB0186
Bony framework of the vertebral column Structure of the vertebral column
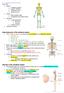 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW
 INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
Endoscopic transpedicular thoracic discectomy
 Neurosurg Focus 6 (5):Article 1, 1999 Endoscopic transpedicular thoracic discectomy Hae-Dong Jho, M.D., Ph.D. Department of Neurological Surgery, University of Pittsburgh School of Medicine, Pittsburgh,
Neurosurg Focus 6 (5):Article 1, 1999 Endoscopic transpedicular thoracic discectomy Hae-Dong Jho, M.D., Ph.D. Department of Neurological Surgery, University of Pittsburgh School of Medicine, Pittsburgh,
102 Posterior Cervical Arthrodesis
 102 Posterior Cervical Arthrodesis Gabriel Widi, Mohammed Faraz Khan, and Glen Manzano Indications Posterior and posterolateral access to the cervical spine: Laminectomy for decompression Intradural tumor
102 Posterior Cervical Arthrodesis Gabriel Widi, Mohammed Faraz Khan, and Glen Manzano Indications Posterior and posterolateral access to the cervical spine: Laminectomy for decompression Intradural tumor
The main causes of cervical radiculopathy include degeneration, disc herniation, and spinal instability.
 SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
SpineFAQs Cervical Radiculopathy Neck pain has many causes. Mechanical neck pain comes from injury or inflammation in the soft tissues of the neck. This is much different and less concerning than symptoms
Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar
 BIOMECHANICS OF SPINE Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar What is biomechanics? Biomechanics is the study of the consequences of application of external force on the spine Primary
BIOMECHANICS OF SPINE Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar What is biomechanics? Biomechanics is the study of the consequences of application of external force on the spine Primary
Cervical Spine Anatomy and Biomechanics. Typical Cervical Vertebra C3 6. Typical Cervical Vertebra Anterior 10/5/2017
 Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
ARCH Laminoplasty System
 Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Cervical Motion Preservation
 Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Surgical technique. SynCage-C short
 Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
Surgical technique SynCage-C short Table of contents Implants 2 Indications/contra-indications 3 Surgical technique 4 Image intensifier control Warning This description is not sufficient for immediate
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
NewBridge. Laminoplasty Fixation INTERNATIONAL EDITION
 NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Compression of the lumbar nerve roots and subsequent leg
 INVITED REVIEW ARTICLE Lumbar Decompression Using a Tubular Retractor System Sapan D. Gandhi, BS,* Christopher K. Kepler, MD, MBA,w and D. Greg Anderson, MDw Summary: Spinal stenosis and intervertebral
INVITED REVIEW ARTICLE Lumbar Decompression Using a Tubular Retractor System Sapan D. Gandhi, BS,* Christopher K. Kepler, MD, MBA,w and D. Greg Anderson, MDw Summary: Spinal stenosis and intervertebral
A Patient s Guide to Cervical Radiculopathy
 A Patient s Guide to Cervical Radiculopathy 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
A Patient s Guide to Cervical Radiculopathy 950 Breckinridge Lane Suite 220 Louisville, KY 40223 Phone: 502.708.2940 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION
 CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
T.L.I.F. Transforaminal Lumbar Interbody Fusion
 T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
Origin of lumbar spinal roots and their relationship to intervertebral discs
 Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
Cervical Microforaminotomy and Decompressive Laminectomy
 20 Cervical Microforaminotomy and Decompressive Laminectomy JARED D. AMENT, HEUM DAI KWON, and KEE D. KIM Overview Disorders of the cervical spine can cause radiculopathy, myelopathy, or both. Compression
20 Cervical Microforaminotomy and Decompressive Laminectomy JARED D. AMENT, HEUM DAI KWON, and KEE D. KIM Overview Disorders of the cervical spine can cause radiculopathy, myelopathy, or both. Compression
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Technique Guide. StenoFix. Interspinous distraction after surgical decompression.
 Technique Guide StenoFix. Interspinous distraction after surgical decompression. Table of Contents Introduction StenoFix 2 Indications and Contraindications 4 Surgical Technique Preoperative Planning
Technique Guide StenoFix. Interspinous distraction after surgical decompression. Table of Contents Introduction StenoFix 2 Indications and Contraindications 4 Surgical Technique Preoperative Planning
New York Science Journal 2017;10(8)
 Outcome of surgical intervention with different modalities in treatment of lumbar canal stenosis. Ahmed Mohamed Shaker Eidarous Elakhras 1, Ahmed M. El Sherif 2 and Mostafa Elsyed Mohamed 3 1 Neurosurgical
Outcome of surgical intervention with different modalities in treatment of lumbar canal stenosis. Ahmed Mohamed Shaker Eidarous Elakhras 1, Ahmed M. El Sherif 2 and Mostafa Elsyed Mohamed 3 1 Neurosurgical
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Disclosure. Thoracolumbar Tumors. Intraspinal Tumor Removal Options 6/4/2011. Minimally Invasive Approaches for Spinal Tumors
 Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
INTERVERTEBRAL FORAMEN STUDIES
 INTERVERTEBRAL FORAMEN STUDIES I. FORAMEN ENCROACHMENT ASSOCIATED WITH DISC HERNIATION* LEE A. HADLEY, M.D. t Syracuse, New York (Received for publication November ] 8, 1949) T HESE studies are the outgrowth
INTERVERTEBRAL FORAMEN STUDIES I. FORAMEN ENCROACHMENT ASSOCIATED WITH DISC HERNIATION* LEE A. HADLEY, M.D. t Syracuse, New York (Received for publication November ] 8, 1949) T HESE studies are the outgrowth
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
A Patient s Guide to Neck Pain. William T. Grant, MD
 A Patient s Guide to Neck Pain Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves in
A Patient s Guide to Neck Pain Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves in
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
Subaxial Cervical Spine Trauma. Introduction. Anatomic Considerations 7/23/2018
 Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
RETROLISTHESIS. Retrolisthesis. is found mainly in the cervical spine and lumbar region but can also be often seen in the thoracic spine
 RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
Aesculap Spine T-Space PEEK. Transforaminal Lumbar Interbody Fusion System
 Aesculap Spine T-Space PEEK Transforaminal Lumbar Interbody Fusion System Forword Growing socio-economic pressure in conjunction with the high incidence of spinal disorders and consequent conditions calls
Aesculap Spine T-Space PEEK Transforaminal Lumbar Interbody Fusion System Forword Growing socio-economic pressure in conjunction with the high incidence of spinal disorders and consequent conditions calls
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (8), Page
 The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (8), Page 7394-7399 Minimally Invasive Spinous Process Splitting Approach for Management of Lumbar Canal Stenosis Ali Mohammad AlGioushy,
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (8), Page 7394-7399 Minimally Invasive Spinous Process Splitting Approach for Management of Lumbar Canal Stenosis Ali Mohammad AlGioushy,
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Pathophysiology of lumbar disc degeneration: a review of the literature. Neurosurg Focus 13 (2): August, 2002
 Pathophysiology of lumbar disc degeneration: a review of the literature Neurosurg Focus 13 (2): August, 2002 MICHAEL D. MARTIN, M.D., CHRISTOPHER M. BOXELL, M.D., F.A.C.S., AND DAVID G. MALONE, M.D. FROM
Pathophysiology of lumbar disc degeneration: a review of the literature Neurosurg Focus 13 (2): August, 2002 MICHAEL D. MARTIN, M.D., CHRISTOPHER M. BOXELL, M.D., F.A.C.S., AND DAVID G. MALONE, M.D. FROM
A Patient s Guide to Cervical Radiculopathy
 A Patient s Guide to Cervical Radiculopathy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Cervical Radiculopathy 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
Alamo T Transforaminal Lumbar Interbody System Surgical Technique
 Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
SynCage-C short. Surgical Technique. This publication is not intended for distribution in the USA.
 SynCage-C short Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Implants 2 Indications/contra-indications
SynCage-C short Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Implants 2 Indications/contra-indications
The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra
 doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
Functional Anatomy and Exam of the Lumbar Spine. Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation
 Functional Anatomy and Exam of the Lumbar Spine Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation Disclosure Anatomical Review Quick Review of Bony and Ligamentous structures Discal anatomy
Functional Anatomy and Exam of the Lumbar Spine Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation Disclosure Anatomical Review Quick Review of Bony and Ligamentous structures Discal anatomy
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
mild Devices Kit - Instructions for Use
 INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Daniel J. Blizzard, MD, MS
 Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
