Newcastle Mitochondrial Disease Guidelines
|
|
|
- Chastity Skinner
- 5 years ago
- Views:
Transcription
1 Newcastle Mitochondrial Disease Guidelines Gastrointestinal Involvement in Adult Mitochondrial Disease: Screening and Initial Management November 2014 Updated December
2 Contents Introduction... 3 Patient-centred Care... 4 Key Priorities for Implementation Gastrointestinal Screening in Patients with Mitochondrial Disease Constipation Diarrhoea Upper GI dysmotility Weight loss/difficulty gaining weight Gastrointestinal Investigations in Symptomatic Patients Exclude other/contributing causes Directed Investigations Specialist Investigations Gastrointestinal Management in Patients with Mitochondrial Disease Prevention Treatment of upper GI symptoms Treatment of lower GI symptoms... Error! Bookmark not defined. 3.4 Specific Scenarios Notes on the scope of this guidance Audience Guideline Limitations Implementation Research recommendations Updating the guidelines Appendix A Appendix B: Treatment of Constipation Appendix C: The Guideline Development Group References
3 Introduction Mitochondrial disease is now recognized as the commonest form of inherited neuromuscular disease. 1 Multisystem disease is a hallmark of these disorders yet gastrointestinal involvement is often overlooked. Diseases defined by a gastrointestinal phenotype (eg. mitochondrial neurogastrointestinal encephalomyopathy (MNGIE) 2 ) are extremely rare, but gastrointestinal involvement is a frequent feature of more common forms of mitochondrial disease such as that due to the m.3243a>g mutation, where constipation, chronic intestinal pseudo-obstruction (CIPO) and significant dilatation of small and large bowel often complicate the clinical course. 3 The severity of symptoms may go unrecognised in these patients until they present in crisis. CIPO is now increasingly recognized in several mitochondrial disorders and successful management can prove difficult. 4-9 Gross faecal loading, CIPO, or commonly both may contribute to anorexia, nausea and vomiting, making administration of aperients and other drugs difficult, as well as hampering adequate fluid and calorific intake in a metabolically vulnerable group. Achieving bowel clearance and regularity of defaecation can be slow and is often associated with significant morbidity and sometimes mortality. In less severely affected patients, symptoms may be non-specific such as anorexia, nausea, abdominal pain and constipation. 10 It is common for these symptoms to have been labelled as irritable bowel syndrome prior to presentation. Patients who harbour a mutation in the MTTL-1 gene (m.3243a>g) are more commonly affected by gastrointestinal dysmotility compared to most other genotypes. Importantly, gastrointestinal involvement in mitochondrial disease is treatable, yet no current guidelines exist. Treatment is more likely to be effective if initiated early and for this reason it is important to screen all patients with mitochondrial disease at the point of diagnosis. 3
4 Patient-centred Care This guideline offers expert consensus advice on the care of patients with mitochondrial disease. The care of these patients and their treatment should take into account patients needs and preferences. People with mitochondrial disease should have the opportunity to make informed decisions about their care and treatment, in partnership with their healthcare professionals. If patients do not have the capacity to make decisions, healthcare professionals should follow the Department of Health guidelines Reference guide to consent for examination or treatment (2001), available from Healthcare professionals should also follow the code of practice accompanying the Mental Capacity Act (a summary of this code is available from Good communication between healthcare professionals and patients is essential. It should be supported by the best available information tailored to the patients needs. Treatment and care, and the information patients are given about it, should be culturally appropriate. It should also be accessible to people with additional needs such as physical, sensory or learning disabilities, and to people who do not speak or read English. If the patient agrees, families and carers should have the opportunity to be involved in decisions about treatment and care. Families and carers should also be given the information and support they need. 4
5 Key Priorities for Implementation In view of the diverse phenotypes of mitochondrial disease, we recommend that all patients diagnosed with mitochondrial disease should have a gastrointestinal assessment at baseline. This should include a clinical assessment (history and examination) utilizing the Bristol Stool Scale (BSS) where possible. Further investigation and follow-up should be based on the initial evaluation and reports of significant gastro-intestinal dysmotility will usually require a more comprehensive assessment including specialist advice, education and derivation of an individualized treatment plan. This document is intended for guidance only, and should not replace patientspecific management plans influenced by other factors such as patient preference. 5
6 1. Gastrointestinal Screening in Patients with Mitochondrial Disease Initial assessment should be made through directed history taking at the time of diagnosis and at regular intervals (eg. annual review and opportunities arising from unrelated GP visits), or if clinical status changes with development of symptoms suggestive of gastro-intestinal involvement. Upper and lower GI involvement usually coexist and both need to be considered. The assessment should include the following: 1.1 Constipation: review of daily bowel function aiming for normal stool consistency at least once every day. The Bristol stool scale (BSS) 11 should be used for assessment where possible. Patients with mitochondrial disease often fail to report constipation despite fulfilling diagnostic criteria - some patients not passing stools for more than five days. Common symptoms of early satiety, abdominal discomfort, bloating, and poor appetite are frequently experienced. Often these symptoms can lead to hospital admission and occasionally result in unnecessary surgical procedures, particularly where the association with mitochondrial disease is not appreciated. Overflow faecal incontinence due to constipation is also a common feature, which is often mistaken for diarrhoea (see below). 1.2 Diarrhoea: true diarrhoea is rarely due to mitochondrial disease and other causes should be excluded. Small volume loose stool can be due to overflow faecal incontinence as a result of constipation and rectal loading. This is best confirmed with a plain abdominal x-ray. Other treatable causes should be excluded and if diarrhoea is persistent small bowel bacterial overgrowth should be considered and discussed with a specialist mitochondrial unit or gastroenterology specialist. 6
7 1.3 Upper GI dysmotility: symptoms of early satiety, poor appetite, gastric reflux, upper abdominal discomfort and bloating may all be pointers toward upper GI dysmotility. Unless self-limiting, referral to a gastroenterologist is advised. Scintography and/or radio-opaque marker studies may be employed to help confirm a diagnosis of gastroparesis or slow transit constipation. 1.4 Weight loss/difficulty gaining weight: anorexia, early satiety and either weight loss or clear difficulty in gaining or regaining weight is very common in mitochondrial disorders. Weight loss and/or change in bowel habits usually needs reasonable exclusion of other causes. Dietetic assessment is important and patients should be screened for undernutrition using MUST (adults) and STAMP (children) nutritional screening tools. Early liaison with a dietician is recommended for nutritional management plans and prevention of further under-nutrition. 2. Gastrointestinal Investigations in Symptomatic Patients 2.1 Exclude other/contributing causes Routine bloods: FBC, U&Es, Ca2+, Glucose, HbA1c, TFT. Consider coeliac screen Drugs: numerous medications are associated with gastrointestinal side effects (eg. opiate analgesics). Risk/benefit ratios and available alternatives need to be considered Diet: High fibre diets can worsen constipation in many patients with mitochondrial disease particularly those with more severe symptoms. It may, in part, be due to weakened peristalsis. Dietetic assessment is helpful in identifying contributing dietary factors. 7
8 2.2 Directed Investigations Abdominal examination (including rectal examination): this is important to exclude masses, organomegaly, painless urinary retention (accompanying bowel involvement in some patients affected by m.3243a>g mutation), and to assess the degree and location of faecal loading Abdominal X-ray (AXR): this is helpful as a baseline investigation for future comparison in all cases presenting with gastrointestinal symptoms. Even in mild cases the AXR provides useful information and a baseline for future comparison. In some patients both small and large bowel can be chronically dilated and recognition of this can sometimes prevent unnecessary surgical intervention. Advanced abdominal imaging such as contrast CT abdomen and pelvis, or barium studies may need to be considered Bladder assessment: painless urinary retention can occur particularly in m.3243a>g patients with advanced multi-system disease. Clinical examination should detect this but ultrasound may be required. In some cases there may be associated hydroureter/hydronephrosis Specialist Opinion: except in mild and well-controlled cases we recommend discussion with a mitochondrial specialist and consideration of referral to a gastroenterologist. It is important that recognition of gastrointestinal dysmotility as part of the mitochondrial disorder spectrum is highlighted as otherwise unnecessary investigations may occur. 8
9 2.3 Specialist Investigations: Gastric emptying studies should be reserved for those patients in whom vomiting is prominent. Investigation of GI transit time may be employed to help confirm a diagnosis of slow transit constipation. Detailed discussion regarding the range of investigations available to the gastroenterologist is beyond the scope of this guideline but liaison with a specialist mitochondrial centre is advised. 3. Gastrointestinal Management in Patients with Mitochondrial Disease 3.1 Prevention Maintaining a regular bowel habit is much easier to achieve than treating established constipation. Early advice and recommendations are encouraged even in asymptomatic individuals Nutrition: Advice on healthy and well balanced diets is advocated for asymptomatic patients or those with only minor symptoms (Further details on healthy eating are available at British Dietitian Association s webpage, Those with constipation will require additional nutritional advice and may benefit from a low fibre diet, when constipation is refractory to other conventional measures such as increased fluid intake and macrogol or other osmotic laxatives. Referral to a gastroenterology dietitian is recommended for advice on preparation of a balanced, low fibre diet (avoiding seeds, pips, skins and stalks) containing adequate calorific/nutritional content and meal planning to optimize calorific intake to combat fatigue associated with mitochondrial dysfunction Fluid intake: good hydration is advised taking into account the needs regarding any other comorbidities (eg. cardiac or renal disease). Strict attention should be paid to fluid balance during inpatient hospital stays. Patients are often of low body mass (with lower intravascular volumes) 9
10 and may have existing cardiomyopathy or renal dysfunction. It is therefore important to be wary of fluid overload and cumulative volume of feeds, IV fluids, and IV medications (eg. anti-epileptic drugs) should be closely monitored Avoid fasting where possible: If nausea, anorexia, or encephalopathy prevent adequate enteral hydration then IV fluids (usually 5% dextrose) should be commenced. Nasogastric (NG) or nasojejunal (NJ) tube feeding should be considered for sedated/encephalopathic patients whose oral calorific intake is inadequate (for those without a preexisting PEG or other form of percutaneous feeding tube in situ). Low residue feeds are required. Regular low volume continuous administration is recommended as large boluses are often poorly tolerated due to gastric dysmotility and may result in vomiting of feeds. It is important to recognise gastroparesis however (see management below). Vomiting following feeds should be a red flag symptom and lead to the patient being placed nil by mouth (NBM). Sedated patients are at greater risk of aspiration and airway protection should be assessed Immobility: this can contribute to constipation so regular physical activity is recommended. Specific advice can be provided for those in whom disability limits their activities or in whom severe fatigue requires measures for energy conservation. Even in those with severe disability, regular changes in posture/positioning (eg. sitting out rather than remaining supine) is beneficial. This should be addressed during hospital admissions and intercurrent illness. 3.2 Treatment of upper GI dysmotility 10
11 3.2.1 Acute presentations (e.g. mimicking mechanical obstruction) This can occur in isolation or more frequently during inter-current Illness or following surgical procedures. These events are seen most commonly in patients carrying the m.3243a>g mutation and often accompany stroke-like episodes or hospitalisation for other reasons. Prompt recognition of clinical symptoms and radiological findings is crucial so that drainage of the stomach and small bowel content can be achieved with the insertion of wide-bore nasogastric (NG) tube ( Drip and suck ). Prominence of vomiting, particularly projectile vomiting or vomiting of bilious or faecal matter in the setting of a distended abdomen following oral intake should alert the clinician to this as a possible serious acute complication of CIPO. This can be particularly dangerous in patients unable to adequately protect their own airway such as those with encephalopathy, seizures, or bulbar dysfunction. Administration of gastrograffin is sometimes useful for both diagnostic and therapeutic purposes (excluding mechanical intestinal obstruction but also treating the pseudo-obstruction). Patients should be kept nil by mouth and enteral feeding is contra-indicated until the pseudoobstruction has resolved. IV fluids (with avoidance of Ringers lactate solution) should be commenced to provide adequate fluid intake. Total parenteral nutrition (TPN) should be considered early if prolonged fasting is likely. Concomitant faecal impaction should be treated as outlined in the section below (see section 3.3.3) Chronic upper GI dysmotility: effective treatment of upper GI symptoms is difficult so it is important to treat existing lower GI issues (eg. constipation) prior to considering the use of prokinetic agents such as erythroymycin. Metoclopramide and domperidone are no longer 11
12 advised as per MHRA guidelines (due to risks of extrapyramidal and cardiac side-effects respectively). In patients with refractory and intrusive symptoms, referral to a gastro-enterologist is recommended for further advice on pharmacological management or consideration of other treatment modalities (eg. jejunostomy). In patients with severe GI dysmotility symptoms and in whom percutaneous gastrostomy or jejunostomy insertion is considered, nasojejunostomy (NJ) feeding should be trialled for 6 weeks to identify the best artificial feeding modality to help alleviate symptoms and maximise nutritional absorption. For patients who already have a gastrostomy in situ, and have ongoing upper GI dysmotility symptoms that are unresponsive to prokinetic agents and modulation of their nutritional feeding regime, conversion to a jejunostomy tube is recommended as jejunal feeds in this instance are likely better tolerated and better absorbed. Alternative diagnosis such as peptic ulcer should be considered and investigated accordingly Small bowel bacterial overgrowth: If diarrhoea remains protracted after exclusion of overflow diarrhoea and treatment of faecal impaction, the possibility of small bowel bacterial overgrowth should be considered. Discussion with a gastroenterology specialist is advised as further tests (such as lactulose breath test and glucose breath test) 12 and eradication therapies (antibiotics eg rifaximin, metronidazole, ciprofloxacin, amoxicillin-clavulinate) 12,13 may be warranted. Note, prokinetic agents may have a role in the treatment of small bowel overgrowth. 3.3 Management of Lower GI dysmotility 12
13 3.3.1 Mild Constipation: For general short-term use stimulant laxatives such as docusate sodium or bisacodyl are a rational choice if the stool is hard. Early review of efficacy is important to avoid development of chronic issues. Some evidence suggests that docusate on its own may not be effective Moderate Constipation: bulk forming laxatives (eg fybogel) are generally unsuitable for patients with mitochondrial disease (See Appendix B). Therefore treatment should be: First line treatment: macrogols - eg Movicol 1-3 sachets daily in divided doses usually for up to 2 weeks. A maintenance dose of 1-2 sachets daily may be given Second line treatment: Bisacodyl or glycerol suppositories should be administered when the rectum is empty, but the colon is still loaded. They may still have a stimulant effect. Oral bisacodyl and combination therapy can also be considered Other drugs used in constipation: If gastrointestinal symptoms persist despite treatment with 2 laxatives for a period of 6 months then referral should be made to a gastroenterologist for consideration of treatment with prucalopride (2mg once daily) or Lubiprostone (start at 24 microgram once daily with food - and titrate up to 24 microgram twice daily if necessary) as per NICE guidance. EMA have recently approved the use of prucalopride in men; UK license imminent Trans-anal Irrigation: referral to a gastroenterology team experienced in the use of colonic irrigation should be considered both in the acute and chronic situations. In either scenario the 13
14 relative risks and benefits need to be carefully considered. Colonic irrigation as a maintenance therapy may prevent hospital admission if available through local community nursing teams, but needs to be considered on a case by case basis Surgical Intervention: this should be considered as a last resort and only after discussion with a mitochondrial specialist. In rare circumstances it is necessary to consider surgical evacuation and/or formation of a functioning ileostomy/colostomy. In those scenarios we recommend reference to published guidelines for Anaesthesia and Peri-Operative Care in Adult Mitochondrial Disease. Clinically relevant tissue samples (eg bowel wall) may be available at operation but mitochondrial studies will be hampered or impossible if samples are not collected fresh (not fixed) and frozen appropriately. Certainly examples exist where such interventions have improved quality of life where other treatment options had failed Other therapies: Abdominal massage as an adjunctive therapy may be useful in certain clinical scenarios Faecal loading/impaction: Use of phosphate enemas should be the first line management in cases of impaction to ensure rectal clearance followed by use of macrogols - eg Movicol 8 sachets daily dissolved in 1 litre of water and drunk within 6 hours, usually for a maximum of 3 days. Reduce to maintenance dose once desired effect realised. Phosphate enema is not suitable for regular use without the supervision of a gastroenterologist. 14
15 3.4 Subacute large bowel pseudo-obstruction The immediate treatment for subacute large bowel pseudo-obstruction is similar to that of subacute small bowel obstruction mimicking mechanical obstruction (please see section 3.2.1) and faecal impaction (see section ). In addition, for refractory cases of large bowel pseudo-obstruction, we would advise early liaison with a gastroenterologist/colorectal surgeon with experience in the management of pseudo-obstruction and a mitochondrial disease specialist. Surgical intervention is rarely necessary and should be considered a last resort after discussion with mitochondrial experts. Although the patient may have a markedly distended abdomen and dilated bowel loops on AXR, the clinical picture is not that of the acute abdomen. Additional treatments to consider include: Placement of a flatus tube: this may be of benefit when colonic dilatation extends to the rectum Endoscopic colonic decompression: this may be considered for refractory cases in the hands of an experienced gastroenterologist/colorectal surgeon. 3.5 Specific Scenarios Peri-Operative Care: Intestinal pseudo-obstruction may develop during illness and in the post-operative period and this commonly contributes to morbidity/mortality through anorexia, vomiting of oral or NGT/PEG delivered feeds, fluids, and medications, immobility and occasionally surgical intervention. Awareness and pre-operative assessment can minimise these risks (see published Anaesthetic and Per-Operative Care guidelines). It is vitally important to maintain hydration and calorific intake during these episodes Pregnancy: antenatal care should include advice regarding bowel care, with a focus on prevention where possible. Obstetricians should be 15
16 made aware of the diagnosis of mitochondrial disease at the booking appointment (see published Pregnancy in Mitochondrial Disease guidelines). Laxatives that are considered safe in pregnancy include docusate, lactulose, macrogols, senna and bisacodyl Aspiration pneumonia: treatment should be in accordance with the local hospital guidelines but there should be a low threshold for appropriate step-up in treatment (eg. antibiotics and/or transfer to a high dependency unit) to reflect the increased risks associated with the metabolic issues and multisystem disease. 16
17 4. Notes on the scope of this guidance The guideline was developed by experts in mitochondrial disease and gastrointestinal disease based at the Wellcome Trust Centre for Mitochondrial Research, Newcastle University, the Newcastle upon Tyne Hospitals NHS Foundation Trust and County Durham and Darlington NHS Foundation Trust. This group specified which aspects of the screening, diagnosis and management of gastrointestinal involvement in patients with mitochondrial disease was to be included and excluded. 4.1 Audience These guidelines are intended for use by the following people or organisations: all healthcare professionals commissioning organisations service providers 4.2 Guideline Limitations Limitations of these guidelines include: Lack of a firm evidence base for reference. Guidelines in mitochondrial disease are currently unable to adopt the evidencebased approach used by organisations such as NICE, and at present are predominantly based on consensus expert opinion. Further studies are needed (see research recommendations below). Specialist Mitochondrial Centres are located in Newcastle, London, and Oxford. The development of these centres represents an important advance in the care of patients with mitochondrial disease. 17
18 5. Implementation Integral to this guideline is publication of the benefits of access to a specialist clinic with experience in mitochondrial disease. Specialist mitochondrial clinics are provided by selected centres with the support of the NHS Highly Specialised Services. The accumulation of experience within these centres, and access to focussed multidisciplinary team input is designed to offer the best available care for patients with mitochondrial disease. Centres are currently located in Newcastle, London and Oxford. Patient education is an important aspect of the initial consultation, but also as a vital component of future care. We aim to provide an understanding of potential gastrointestinal involvement and the role of early recognition and good bowel care in preventing future complications and morbidity. Access to specialist clinics allows relevant genetic counselling and family tracing to facilitate the identification of those at risk of developing disease, or to formally diagnose those who may already be affected. Close liaison is required between the specialist centre itself and local services. We recommend local gastroenterology follow up where frequent or emergency central review is impractical. 18
19 6. Research recommendations 6.1 Natural history studies Comprehensive assessment of a large cohort of mitochondrial disease patients is required to document the effects of gastrointestinal dysmotility on morbidity and mortality within different genotypes/phenotypes. 6.2 Pharmacological agents and dietary supplements Further research involving randomised controlled trials of therapeutic agents efficacious for the treatment of gastrointestinal dysmotility in other disease states is needed to establish safety and efficacy data in mitochondrial cohorts. 7. Updating the guidelines The Newcastle Mitochondrial Guidelines are updated as needed so that recommendations take into account important new information. We check for new evidence every 2 years after publication, to decide whether all or part of the guideline should be updated. If important new evidence is published at other times, we may update the guidance prior to any scheduled changes. Last updated December
20 Appendix A Management of chronic upper and lower gastrointestinal symptoms in mitochondrial disease Clinical Assessment Upper GI symptoms Bloating and abdominal pain Gastric reflux Decreased appetite Early satiety and/or post-prandial nausea/vomiting Lower GI symptoms Bloating and abdominal pain Difficult/infrequent defaecation Abnormal Bristol Stool Chart Clinical evidence of faecal loading Consider Gastroparesis Review diet/medications Bloods & AXR Refer to gastroenterologist for consideration of scintography and/or radio-opaque examination Consider Constipation Review diet/medications Bloods & AXR Treatment options Implement low fibre diet Consider prokinetic agent (eg. erythromyci) Parenteral or Enteral feeding (preferably jejunostomy) may be considered if refractory symptoms/weight loss Treatment options Implement low fibre diet See Appendix B for treatment of: Mild constipation Moderate constipation Severe constipation/faecal impaction/ loading Treatment Failures Refer to Mitochondrial Centre Refer to gastroenterologist Consider colonic irrigation Consider other newer agents e.g. prucalopride, lubiprostone 20
21 Appendix B: Treatment of Constipation Mild Constipation Moderate Constipation Severe/Faecal Impaction 1 st Line Treatment Docusate sodium 100mg twice daily. This can be increased to 500mg daily on divided doses. 1 st Line Treatment Macrogols 1-3 sachets daily for 2 weeks and followed by 1-2 sachets daily as maintenance therapy. 1 st Line Treatment Phosphate enema 2 nd Line Treatment Bisacodyl or Glycerol suppositories 2 nd line Treatment Bisacodyl or Glycerol suppositories 2 nd Line Treatment Macrogol up to 8 sachets daily for 3 days Review daily NOTE: 1. Adopt low-fibre diet. Avoid bulk-forming laxatives e.g. Fybogel 2. All medications mentioned above should only be administered as prescribed. 21
22 Appendix C: The Guideline Development Group Sister Catherine Feeney Mitochondrial Disease Specialist Nurse Wellcome Trust Centre for Mitochondrial Research, Newcastle University Newcastle upon Tyne Hospitals NHS Foundation Trust Dr Andrew M Schaefer Consultant Neurologist Wellcome Trust Centre for Mitochondrial Research, Newcastle University Newcastle upon Tyne Hospitals NHS Foundation Trust Dr Gráinne S Gorman Honorary Consultant Neurologist Wellcome Trust Centre for Mitochondrial Research, Newcastle University Dr Yi Shiau Ng Clinical Research Associate Wellcome Trust Centre for Mitochondrial Research, Newcastle University Newcastle upon Tyne Hospitals NHS Foundation Trust Mrs Paula Hynd Lead Paediatric Dietitian Gastroenterology Great North Children s Hospital, Royal Victoria Infirmary Newcastle upon Tyne Hospitals NHS Foundation Trust Professor Yan Yiannakou Professor of Neuro-Gastroenterology University Hospital of North Durham County Durham and Darlington NHS Foundation Trust Dr Robert McFarland Clinical Senior Lecturer Wellcome Trust Centre for Mitochondrial Research, Newcastle University Newcastle upon Tyne Hospitals NHS Foundation Trust 22
23 Professor Douglass M Turnbull Professor of Neurology Wellcome Trust Centre for Mitochondrial Research, Newcastle University Newcastle upon Tyne Hospitals NHS Foundation Trust 23
24 References 1. Gorman GS, Schaefer AM, Ng Y, et al. Prevalence of nuclear and mitochondrial DNA mutations related to adult mitochondrial disease. Ann Neurol 2015; 77(5): Garone C, Tadesse S, Hirano M. Clinical and genetic spectrum of mitochondrial neurogastrointestinal encephalomyopathy. Brain 2011; 134(Pt 11): Sekino Y, Inamori M, Yamada E, et al. Characteristics of intestinal pseudo-obstruction in patients with mitochondrial diseases. World Journal of Gastroenterology 2012; 18(33): Amiot A, Tchikviladze M, Joly F, et al. Frequency of mitochondrial defects in patients with chronic intestinal pseudo-obstruction. Gastroenterology 2009; 137(1): Narbonne H, Paquis-Fluckinger V, Valero R, Heyries L, Pellissier JF, Vialettes B. Gastrointestinal tract symptoms in maternally inherited diabetes and deafness (MIDD). Diabetes & metabolism 2004; 30(1): Sekino Y, Inamori M, Yamada E, et al. Characteristics of intestinal pseudo-obstruction in patients with mitochondrial diseases. World journal of gastroenterology: WJG 2012; 18(33): Betts J, Barron MJ, Needham SJ, Schaefer AM, Taylor RW, Turnbull DM. Gastrointestinal tract involvement associated with the 3243A> G mitochondrial DNA mutation. Neurology 2008; 70(15): Giordano C, Powell H, Leopizzi M, et al. Fatal congenital myopathy and gastrointestinal pseudoobstruction due to POLG1 mutations. Neurology 2009; 72(12): Verny C, Amati-Bonneau P, Letournel F, et al. Mitochondrial DNA A3243G mutation involved in familial diabetes, chronic intestinal pseudo-obstruction and recurrent pancreatitis. Diabetes & metabolism 2008; 34(6): P. de Laat HEEZS, S. Knuijt, J.A.M. Smeitink, G.J.A. Wanten, M.C.H. Janssen. Dysphagia, malnutrition and gastrointestinal problems in patients with mitochondrial disease caused by the m3243a>g mutation. The Netherlands Journal of Medicine 2015; 73(1): Lewis SJ, Heaton KW. Stool form scale as a useful guide to intestinal transit time. Scandinavian journal of gastroenterology 1997; 32(9): Grace E, Shaw C, Whelan K, Andreyev HJN. Review article: small intestinal bacterial overgrowth prevalence, clinical features, current and developing diagnostic tests, and treatment. Alimentary pharmacology & therapeutics 2013; 38(7): Shah SC, Day LW, Somsouk M, Sewell JL. Meta-analysis: antibiotic therapy for small intestinal bacterial overgrowth. Alimentary pharmacology & therapeutics 2013; 38(8): Coggrave M, Norton C, Cody JD. Management of faecal incontinence and constipation in adults with central neurological diseases. The Cochrane database of systematic reviews 2014; 1: Cd (Last accessed 13th July 2015) 24
Gastrointestinal Involvement in Adult Mitochondrial Disease
 Newcastle Mitochondrial Disease Guidelines At a glance guidelines: Gastrointestinal Involvement in Adult Mitochondrial Disease For full guideline visit: http://www.newcastle-mitochondria.com/service/patient-care-guidelines/
Newcastle Mitochondrial Disease Guidelines At a glance guidelines: Gastrointestinal Involvement in Adult Mitochondrial Disease For full guideline visit: http://www.newcastle-mitochondria.com/service/patient-care-guidelines/
Clinical problems related to GI involvement in SSc
 Clinical problems related to GI involvement in SSc Incontinence Abdominal pain/distension Gastro-oesophageal Diarrhoea Weight loss/al Issues Constipation Management of incontinence Establish diagnosis
Clinical problems related to GI involvement in SSc Incontinence Abdominal pain/distension Gastro-oesophageal Diarrhoea Weight loss/al Issues Constipation Management of incontinence Establish diagnosis
Primary Care Constipation Guidelines. Version 1 November 2016
 Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
Newcastle Mitochondrial Disease Guidelines
 Newcastle Mitochondrial Disease Guidelines Respiratory Involvement in Adult Mitochondrial Disease: Screening and Initial Management First Published January 2011 Updated January 2013 1 Contents Introduction
Newcastle Mitochondrial Disease Guidelines Respiratory Involvement in Adult Mitochondrial Disease: Screening and Initial Management First Published January 2011 Updated January 2013 1 Contents Introduction
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
Newcastle Mitochondrial Disease Guidelines
 Newcastle Mitochondrial Disease Guidelines Epilepsy in Adult Mitochondrial Disease: Investigation and Management First published August 2010 Updated January 2013 1 Contents Introduction 3 Patient Centered
Newcastle Mitochondrial Disease Guidelines Epilepsy in Adult Mitochondrial Disease: Investigation and Management First published August 2010 Updated January 2013 1 Contents Introduction 3 Patient Centered
MOVICOL Junior Powder for Solution (macrogol 3350)
 MOVICOL Junior Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Product Description: Each sachet of MOVICOL Junior contains: Macrogol 3350 Sodium chloride Sodium bicarbonate Potassium chloride
MOVICOL Junior Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Product Description: Each sachet of MOVICOL Junior contains: Macrogol 3350 Sodium chloride Sodium bicarbonate Potassium chloride
MOVICOL HALF PI December MOVICOL-Half. Powder for Solution (macrogol 3350) Potassium 5.4 mmol/l. Bicarbonate 17 mmol/l
 MOVICOL -Half Powder for Solution (macrogol 3350) Product Name: Product Description: MOVICOL-Half Each sachet of MOVICOL-Half contains: Macrogol 3350 6.563 g Sodium chloride 175.4 mg Sodium bicarbonate
MOVICOL -Half Powder for Solution (macrogol 3350) Product Name: Product Description: MOVICOL-Half Each sachet of MOVICOL-Half contains: Macrogol 3350 6.563 g Sodium chloride 175.4 mg Sodium bicarbonate
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Nutrition support in adults: oral supplements, enteral and parenteral feeding.
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Lacrofarm Junior, powder for oral solution, sachet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet of contains the following active
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Lacrofarm Junior, powder for oral solution, sachet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet of contains the following active
EXENATIDE (BYETTA ) PROTOCOL, 5mcg and 10mcg SC injection pre-filled pens
 EXENATIDE (BYETTA ) PROTOCOL, 5mcg and 10mcg SC injection pre-filled pens This document should be read in conjunction with the current Summary of Product Characteristics http://www.medicines.org.uk 1.
EXENATIDE (BYETTA ) PROTOCOL, 5mcg and 10mcg SC injection pre-filled pens This document should be read in conjunction with the current Summary of Product Characteristics http://www.medicines.org.uk 1.
2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet of Macrovic Junior powder for oral solution contains the following active ingredients:
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Macrovic Junior powder for oral solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet of Macrovic Junior powder for oral solution
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Macrovic Junior powder for oral solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet of Macrovic Junior powder for oral solution
Guideline scope Diverticular disease: diagnosis and management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
MOVICOL Junior Chocolate Flavour Powder for Solution (macrogol 3350)
 MOVICOL Junior Chocolate Flavour Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Chocolate Flavour Product Description: Each sachet of MOVICOL Junior Chocolate contains: Macrogol 3350
MOVICOL Junior Chocolate Flavour Powder for Solution (macrogol 3350) Product Name: MOVICOL Junior Chocolate Flavour Product Description: Each sachet of MOVICOL Junior Chocolate contains: Macrogol 3350
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
MOVICOL Lemon-Lime Flavour Powder for Solution (macrogol 3350)
 MOVICOL Lemon-Lime Flavour Powder for Solution (macrogol 3350) Product Name: MOVICOL Lemon-Lime Flavour Product Description: Each sachet of MOVICOL Lemon-Lime contains: Macrogol 3350 Sodium chloride Sodium
MOVICOL Lemon-Lime Flavour Powder for Solution (macrogol 3350) Product Name: MOVICOL Lemon-Lime Flavour Product Description: Each sachet of MOVICOL Lemon-Lime contains: Macrogol 3350 Sodium chloride Sodium
A patient s guide to the. management of constipation following surgery
 A patient s guide to the management of constipation following surgery This leaflet has been designed to give you more information about using laxatives after your surgery. What is constipation? After your
A patient s guide to the management of constipation following surgery This leaflet has been designed to give you more information about using laxatives after your surgery. What is constipation? After your
Factsheet LINACLOTIDE (Constella ) Irritable Bowel Syndrome constipation predominant (IBS-C)
 North Central London Joint Formulary Committee Factsheet LINACLOTIDE (Constella ) Irritable Bowel Syndrome constipation predominant (IBS-C) Start date: September 2018 Review date: September 2021 Document
North Central London Joint Formulary Committee Factsheet LINACLOTIDE (Constella ) Irritable Bowel Syndrome constipation predominant (IBS-C) Start date: September 2018 Review date: September 2021 Document
Treat primary. symptoms. Offer general lifestyle advice. Manage IBS according to the dominant symptom. Follow up. Symptoms do not improve
 Treat primary symptoms Background information for clinicians Offer general lifestyle advice Background information for patients Manage IBS according to the dominant symptom Provenance Psychological symptoms
Treat primary symptoms Background information for clinicians Offer general lifestyle advice Background information for patients Manage IBS according to the dominant symptom Provenance Psychological symptoms
Nutritional Support in the Perioperative Period
 Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
EFFECTIVE SHARE CARE AGREEMENT. FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY
 Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
Irritable bowel syndrome in adults
 Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
CONTROLLED DOCUMENT. Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) Controlled Document Number: CG259
 Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Constipation an Old Friend. Presented by Dr. Keith Harris
 Constipation an Old Friend Presented by Dr. Keith Harris Irregularity and the Tricks of the Trade." CONSTIPATION What is constipation? INFREQUENT BOWEL MOVEMENTS DIFFICULTY DURING DEFECATION SENSATION
Constipation an Old Friend Presented by Dr. Keith Harris Irregularity and the Tricks of the Trade." CONSTIPATION What is constipation? INFREQUENT BOWEL MOVEMENTS DIFFICULTY DURING DEFECATION SENSATION
Nutritional assessment & support for the upper GI cancer patient
 Nutritional assessment & support for the upper GI cancer patient Catherine Fleuret Specialist Dietitian, The Royal Marsden Outline Nutritional status & implications The role of nutrition & the dietitian
Nutritional assessment & support for the upper GI cancer patient Catherine Fleuret Specialist Dietitian, The Royal Marsden Outline Nutritional status & implications The role of nutrition & the dietitian
Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT)
 Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT) Scope This protocol details pre, during and post BMT nutritional assessment and management for all forms of BMT undertaken by OxBMT,
Nutritional Protocol for Blood and Bone Marrow Transplantation (BMT) Scope This protocol details pre, during and post BMT nutritional assessment and management for all forms of BMT undertaken by OxBMT,
Understanding your take home medications from the surgical ward. Information for Patients
 Understanding your take home medications from the surgical ward Information for Patients i Information for Patients Please read this leaflet before taking the medications that have been prescribed for
Understanding your take home medications from the surgical ward Information for Patients i Information for Patients Please read this leaflet before taking the medications that have been prescribed for
MOVICOL Liquid Orange Flavour Concentrate for Oral Solution (macrogol 3350)
 MOVICOL Liquid Orange Flavour Concentrate for Oral Solution (macrogol 3350) NAME OF THE MEDICINE: MOVICOL Liquid Orange Flavour, Concentrate for Oral Solution. DESCRIPTION: A clear colourless solution.
MOVICOL Liquid Orange Flavour Concentrate for Oral Solution (macrogol 3350) NAME OF THE MEDICINE: MOVICOL Liquid Orange Flavour, Concentrate for Oral Solution. DESCRIPTION: A clear colourless solution.
SUMMARY OF PRODUCT CHARACTERISTICS. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet contains the following active ingredients:
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Lacrofarm, powder for oral solution, sachet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet contains the following active ingredients:
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Lacrofarm, powder for oral solution, sachet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet contains the following active ingredients:
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Constipation An Overview. Definition Physiology of GI tract Etiology Assessment Treatment
 CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST
 COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST Paediatric Gastroenterology : Referral Base Common problems Feeding difficulties in infancy Recurrent
COMMON PROBLEMS IN PAEDIATRIC GASTROENTEROLOGY AKSHAY BATRA CONSULTANT PAEDIATRIC GASTROENTEROLOGIST Paediatric Gastroenterology : Referral Base Common problems Feeding difficulties in infancy Recurrent
PRODUCT INFORMATION RESONIUM A. Na m
 PRODUCT INFORMATION RESONIUM A NAME OF THE MEDICINE Non-proprietary Name Sodium polystyrene sulfonate Chemical Structure CH - 2 CH SO 3 Na + n CAS Number 28210-41-5 [9003-59-2] CH 2 CH SO - 3 m DESCRIPTION
PRODUCT INFORMATION RESONIUM A NAME OF THE MEDICINE Non-proprietary Name Sodium polystyrene sulfonate Chemical Structure CH - 2 CH SO 3 Na + n CAS Number 28210-41-5 [9003-59-2] CH 2 CH SO - 3 m DESCRIPTION
CONTINENCE MODULE 3 MIMIMUM STANDARDS FOR SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF CONSTIPATION AND FAECAL INCONTINENCE
 CONTINENCE MODULE 3 MIMIMUM STANDARDS FOR SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF CONSTIPATION AND FAECAL INCONTINENCE The minimum standards required to initiate specialised conservative treatment
CONTINENCE MODULE 3 MIMIMUM STANDARDS FOR SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF CONSTIPATION AND FAECAL INCONTINENCE The minimum standards required to initiate specialised conservative treatment
Suboptimal hydration harms patients.
 Suboptimal hydration harms patients. NHS Fife is committed to improving hydration management. To achieve this we need your help! In 2014 new fluid balance charts were implemented in the Victoria Hospital,
Suboptimal hydration harms patients. NHS Fife is committed to improving hydration management. To achieve this we need your help! In 2014 new fluid balance charts were implemented in the Victoria Hospital,
Percutaneous (Keyhole) Removal of Kidney Stone(s)
 Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact 4A, 4B or 4C ward
Who can I contact if I have a problem when I get home? If you experience any problems related to your surgery or admission once you have been discharged home. Please feel free to contact 4A, 4B or 4C ward
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Prescribing Guidance for the Treatment of Constipation in Children
 Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
Prescribing Guidance for the Treatment of Constipation in Children Effective Date: July 2007 Reviewed: September 2009 & December 2011 Review Date: December 2013 Gateshead Medicines Management Approved
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS OVERVIEW
 Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
SYMPTOM MANAGEMENT GUIDANCE FOR PATIENTS RECEIVING PALLIATIVE CARE AT ROYAL DERBY HOSPITAL
 SYMPTOM MANAGEMENT GUIDANCE FOR PATIENTS RECEIVING PALLIATIVE CARE AT ROYAL DERBY HOSPITAL If a patient is believed to be approaching the end of their life, medication should be prescribed in anticipation
SYMPTOM MANAGEMENT GUIDANCE FOR PATIENTS RECEIVING PALLIATIVE CARE AT ROYAL DERBY HOSPITAL If a patient is believed to be approaching the end of their life, medication should be prescribed in anticipation
Case Study. The 4-year journey of feeding intolerance of an enterally-fed child from 9 months of age. Synopsis. Introduction/Overview
 Case Study The 4-year journey of feeding intolerance of an enterally-fed child from 9 months of age Library image Emma Liesl Silbernagl, Clinical lead HEN Dietitian, Home Enteral Nutrition Team, Lewisham
Case Study The 4-year journey of feeding intolerance of an enterally-fed child from 9 months of age Library image Emma Liesl Silbernagl, Clinical lead HEN Dietitian, Home Enteral Nutrition Team, Lewisham
Malnutrition in Adults: Guidelines for Identification and Treatment
 Malnutrition in Adults: Guidelines for Identification and Treatment Signatures (e.g. chair of the ratifying committee and lay member) and date Signature...date Designation: Signature...date Designation
Malnutrition in Adults: Guidelines for Identification and Treatment Signatures (e.g. chair of the ratifying committee and lay member) and date Signature...date Designation: Signature...date Designation
STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA)
 STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA) DEFINITION OF ENTERAL FEEDING INTOLERANCE Gastrointestinal feeding intolerance are usually defined as: High gastric
STRATEGIES TO IMPROVE ENTERAL FEEDING TOLERANCE. IS IT WORTH IT? ENGELA FRANCIS RD(SA) DEFINITION OF ENTERAL FEEDING INTOLERANCE Gastrointestinal feeding intolerance are usually defined as: High gastric
Medicines and Technologies Programme Adoption Scoping Report MTG315 Peristeen
 Medicines and Technologies Programme Adoption Scoping Report MTG315 Peristeen SUMMARY for MTAC1 meeting Contributors questioned why NICE are writing guidance on this system alone when it is viewed and
Medicines and Technologies Programme Adoption Scoping Report MTG315 Peristeen SUMMARY for MTAC1 meeting Contributors questioned why NICE are writing guidance on this system alone when it is viewed and
Chapter 5 Gastroenterology. Dose. Route. Units. Given. Dose. Route. Units. Given
 Chapter 5 Gastroenterology Georgia Woodfield TERLIPRESSIN CIPROFLOXACIN 2 initial dose 500 Every 4 hours until bleeding controlled can be reduced to 1 after initial dose if side effects develop or if patient
Chapter 5 Gastroenterology Georgia Woodfield TERLIPRESSIN CIPROFLOXACIN 2 initial dose 500 Every 4 hours until bleeding controlled can be reduced to 1 after initial dose if side effects develop or if patient
2 QUALITATIVE AND QUANTITATIVE COMPOSITION
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Compound Macrogol 13.72 g powder for oral solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet of Compound Macrogol 13.72 g
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Compound Macrogol 13.72 g powder for oral solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet of Compound Macrogol 13.72 g
PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS. A08/S/d Colorectal: Faecal Incontinence (Adult)
 A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
ROLE OF A DIETITIAN & KEEPING HYDRATED. Emily Capener Haematology Dietitian UHW
 ROLE OF A DIETITIAN & KEEPING HYDRATED Emily Capener Haematology Dietitian UHW We will cover: PART 1 What is a dietitian Where do dietitans work About an acute dietitians role - Screening - Food charts
ROLE OF A DIETITIAN & KEEPING HYDRATED Emily Capener Haematology Dietitian UHW We will cover: PART 1 What is a dietitian Where do dietitans work About an acute dietitians role - Screening - Food charts
GROUP PROTOCOL FOR THE MANAGEMENT OF CONSTIPATION IN PATIENTS IN CLOZAPINE CLINICS. Version 1 (reviewed unchanged January 2018)
 GROUP PROTOCOL FOR THE MANAGEMENT OF CONSTIPATION IN PATIENTS IN CLOZAPINE CLINICS Version 1 (reviewed unchanged January 2018) RATIFYING COMMITTEE Drugs and Therapeutics Group DATE ORIGINALLY 29 th October2014
GROUP PROTOCOL FOR THE MANAGEMENT OF CONSTIPATION IN PATIENTS IN CLOZAPINE CLINICS Version 1 (reviewed unchanged January 2018) RATIFYING COMMITTEE Drugs and Therapeutics Group DATE ORIGINALLY 29 th October2014
Management of GI Issues in Duchenne. Kent Williams, MD Assistant Professor Nationwide Children s Hospital Columbus Ohio
 Management of GI Issues in Duchenne Kent Williams, MD Assistant Professor Nationwide Children s Hospital Columbus Ohio Objectives Current GI recommendations What is known and not known Case Presentation:
Management of GI Issues in Duchenne Kent Williams, MD Assistant Professor Nationwide Children s Hospital Columbus Ohio Objectives Current GI recommendations What is known and not known Case Presentation:
Issues in Enteral Feeding: Aspiration
 Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
SUMMARY OF THE PRODUCT CHARACTERISTICS. The content of electrolyte ions per sachet when made up to 125 ml of solution.
 SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Molaxole powder for oral solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet contains following active substances Macrogol
SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Molaxole powder for oral solution 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each sachet contains following active substances Macrogol
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES
 OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
Bowel cancer risk in the under 50s. Greg Rubin Professor of General Practice and Primary Care
 Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE. Coeliac disease: recognition, assessment and management of coeliac disease
 Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Appendix B: NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Coeliac disease: recognition, assessment and management of coeliac disease 1.1 Short title Coeliac disease 2 The remit
Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW. Date: 17/10/2016
 EXPERT MEDICAL REPORT FOR THE COURT ON BREACH OF DUTY Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW Date: 17/10/2016 -------------------------------------------------------------------
EXPERT MEDICAL REPORT FOR THE COURT ON BREACH OF DUTY Prepared by: Dr Katherine Brown Fir Lea House Whitecross Newquay Cornwall TR8 4LW Date: 17/10/2016 -------------------------------------------------------------------
Home Total Parenteral Nutrition for Adults
 Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Understanding & Alleviating Constipation. Living (Well!) with Gastroparesis Program Warm-Up Class
 Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
London Strategic Clinical Networks. My AKI. Guidance for patients with, or recovering from, acute kidney injury
 London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
Technology appraisal guidance Published: 15 December 2010 nice.org.uk/guidance/ta211
 Prucalopride for the treatment of chronic constipation in women Technology appraisal guidance Published: 15 December 2010 nice.org.uk/guidance/ta211 NICE 2018. All rights reserved. Subject to Notice of
Prucalopride for the treatment of chronic constipation in women Technology appraisal guidance Published: 15 December 2010 nice.org.uk/guidance/ta211 NICE 2018. All rights reserved. Subject to Notice of
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
June By: Reza Gholami
 ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation
 Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation Version: 1.3 Issued: Review date: Author: Melanie Drewett The procedural aspects of this guideline can be
Wessex Care Pathway for Term Infants Referred with Bilious Vomiting for Exclusion of Malrotation Version: 1.3 Issued: Review date: Author: Melanie Drewett The procedural aspects of this guideline can be
Amy-Jo Hooley Specialist Clinical Pharmacist
 Gut Decontamination Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Safe Administration
Gut Decontamination Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Safe Administration
Buccal Midazolam For the treatment of prolonged epileptic seizures, clusters of epileptic seizures and status epilepticus.
 Oxfordshire Clinical Commissioning Group, Oxford University Hospitals NHS Trust and Oxfordshire Health NHS Foundation Trust Shared Care Protocol and Information for GPs Buccal Midazolam For the treatment
Oxfordshire Clinical Commissioning Group, Oxford University Hospitals NHS Trust and Oxfordshire Health NHS Foundation Trust Shared Care Protocol and Information for GPs Buccal Midazolam For the treatment
Authors and Disclosures
 Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
Subtotal and Total Gastrectomy
 DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
UK Inflammatory Bowel Disease Audit. A summary report on the quality of healthcare provided to people with inflammatory bowel disease
 UK Inflammatory Bowel Disease Audit A summary report on the quality of healthcare provided to people with inflammatory bowel disease Section heading UK IBD Audit summary report 2014 This summary report
UK Inflammatory Bowel Disease Audit A summary report on the quality of healthcare provided to people with inflammatory bowel disease Section heading UK IBD Audit summary report 2014 This summary report
Gastrointestinal obstruction Dr Iain Lawrie
 Gastrointestinal obstruction Dr Iain Lawrie Consultant and Honorary Clinical Senior Lecturer in Palliative Medicine The Pennine Acute Hospitals NHS Trust / The University of Manchester iain.lawrie@pat.nhs.uk
Gastrointestinal obstruction Dr Iain Lawrie Consultant and Honorary Clinical Senior Lecturer in Palliative Medicine The Pennine Acute Hospitals NHS Trust / The University of Manchester iain.lawrie@pat.nhs.uk
Tertiary, regional and local pelvic floor service providers: the future. model? Andrew Williams
 Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
Factsheet. Buccolam (midazolam) 10mg in 2mL oromucosal solution. Management of seizures in adult patients
 North Central London Joint Formulary Committee Factsheet Buccolam (midazolam) 10 mg in 2 ml oromucosal solution Management of seizures in adult patients Start date: May 2017 Review date: May 2020 Document
North Central London Joint Formulary Committee Factsheet Buccolam (midazolam) 10 mg in 2 ml oromucosal solution Management of seizures in adult patients Start date: May 2017 Review date: May 2020 Document
Managing constipation in residential care
 Managing constipation in residential care Amanda Lee Lecturer, Hull University ; PhD Candidate, Gastroesophageal cancers Key Points Constipation is a major problem in residential care Early detection and
Managing constipation in residential care Amanda Lee Lecturer, Hull University ; PhD Candidate, Gastroesophageal cancers Key Points Constipation is a major problem in residential care Early detection and
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
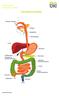 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
Late effects of treatment for colorectal cancer. Claire Taylor Macmillan Nurse Consultant St Mark s Hospital
 Late effects of treatment for colorectal cancer Claire Taylor Macmillan Nurse Consultant St Mark s Hospital The number of people living with cancer is set to double from 2m to 4m by 2030 Source: Maddams
Late effects of treatment for colorectal cancer Claire Taylor Macmillan Nurse Consultant St Mark s Hospital The number of people living with cancer is set to double from 2m to 4m by 2030 Source: Maddams
Intra-gastric balloon procedure. Information for patients Sheffield Centre for Weight Loss Surgery
 Intra-gastric balloon procedure Information for patients Sheffield Centre for Weight Loss Surgery Introduction The intra-gastric balloon is designed to provide short term weight loss therapy. It is a temporary
Intra-gastric balloon procedure Information for patients Sheffield Centre for Weight Loss Surgery Introduction The intra-gastric balloon is designed to provide short term weight loss therapy. It is a temporary
TREATMENTS FOR TYPE 2 DIABETES. Susan Henry Diabetes Specialist Nurse
 TREATMENTS FOR TYPE 2 DIABETES Susan Henry Diabetes Specialist Nurse How can we improve outcomes in Type 2 diabetes? Earlier diagnosis Better patient education Stress central role of lifestyle management
TREATMENTS FOR TYPE 2 DIABETES Susan Henry Diabetes Specialist Nurse How can we improve outcomes in Type 2 diabetes? Earlier diagnosis Better patient education Stress central role of lifestyle management
Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate.
 NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
Muscular Dystrophy UK s Adult North Star Network. Care recommendations for adults with Duchenne a consultation
 Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
Haemorrhoidectomy. Colorectal Surgery. Patient Information
 Haemorrhoidectomy Colorectal Surgery Patient Information What are haemorrhoids? Haemorrhoids, also know as piles, are soft fleshy lumps just inside the back passage (anus). They have a rich blood supply
Haemorrhoidectomy Colorectal Surgery Patient Information What are haemorrhoids? Haemorrhoids, also know as piles, are soft fleshy lumps just inside the back passage (anus). They have a rich blood supply
Community and Mental Health Services. Palliative Care. Criteria and
 Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Right Iliac Fossa Pain
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Right Iliac Fossa Pain Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Right Iliac Fossa Pain Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Amyloidosis & the GI Tract
 Amyloidosis & the GI Tract John O. Clarke, M.D. Director, Esophageal Program Clinical Associate Professor of Medicine Stanford University john.clarke@stanford.edu 2017 Topics to cover 1) Patterns of GI
Amyloidosis & the GI Tract John O. Clarke, M.D. Director, Esophageal Program Clinical Associate Professor of Medicine Stanford University john.clarke@stanford.edu 2017 Topics to cover 1) Patterns of GI
Percutaneous removal of kidney stone(s): procedurespecific information
 PATIENT INFORMATION Percutaneous removal of kidney stone(s): procedurespecific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British
PATIENT INFORMATION Percutaneous removal of kidney stone(s): procedurespecific information What is the evidence base for this information? This leaflet includes advice from consensus panels, the British
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Small bowel enema. Radiology Department
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Small bowel enema Radiology Department The leaflet tells you about having a small bowel enema enteroclysis. It explains what
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Small bowel enema Radiology Department The leaflet tells you about having a small bowel enema enteroclysis. It explains what
Specialist Palliative Care Service Referral Criteria and Guidance
 Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
ADULT (>16) ACUTE SICKLE PAIN GUIDELINE
 ADULT (>16) ACUTE SICKLE PAIN GUIDELINE ID 2013 065 Author s Name Dr Anna Wood Author s Job Title Consultant Haematologist Division Consultant Haematologist Department Haematology Version number 3 Ratifying
ADULT (>16) ACUTE SICKLE PAIN GUIDELINE ID 2013 065 Author s Name Dr Anna Wood Author s Job Title Consultant Haematologist Division Consultant Haematologist Department Haematology Version number 3 Ratifying
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA
 GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
Having MR Small Bowel (MR Enterography)
 Having MR Small Bowel (MR Enterography) Information for Patients In this leaflet: Introduction 2 What is an MR Small Bowel?..2 What do I need to do to before my scan?....2 Where do I go when I arrive at
Having MR Small Bowel (MR Enterography) Information for Patients In this leaflet: Introduction 2 What is an MR Small Bowel?..2 What do I need to do to before my scan?....2 Where do I go when I arrive at
University College Hospital. Subtotal and Total Gastrectomy. Gastrointestinal Services Division
 University College Hospital Subtotal and Total Gastrectomy Gastrointestinal Services Division If you need a large print, audio or translated copy of the document, please contact us on 020 3447 9202. We
University College Hospital Subtotal and Total Gastrectomy Gastrointestinal Services Division If you need a large print, audio or translated copy of the document, please contact us on 020 3447 9202. We
Engagement Report for Clinical Commissioning Policies
 Engagement Report for Clinical Commissioning Policies Unique Reference Number Policy Title Lead Commissioner Clinical Reference Group 1670 Total pancreatectomy with islet auto transplant for chronic pancreatitis
Engagement Report for Clinical Commissioning Policies Unique Reference Number Policy Title Lead Commissioner Clinical Reference Group 1670 Total pancreatectomy with islet auto transplant for chronic pancreatitis
