Lymphocytic colitis: clinical presentation and long term course
|
|
|
- Peter Simmons
- 5 years ago
- Views:
Transcription
1 Gut 1998;43: Gastroenterology, Department of Internal Medicine, University Hospital, Rämistrasse 100, CH-8091 Zürich, Switzerland B Mullhaupt U Güller M Fried G-I Practice, CH-5430 Wettingen, Switzerland R Güller Institute of Pathology, Kantonsspital Baden, CH-5400 Baden, Switzerland M Anabitarte Correspondence to: Dr B Müllhaupt. Accepted for publication 16 April 1998 Lymphocytic colitis: clinical presentation and long term course B Mullhaupt, U Güller, M Anabitarte, R Güller, M Fried Abstract Background Lymphocytic colitis is characterised by chronic watery diarrhoea with normal endoscopic or radiological findings and microscopic evidence of pronounced infiltration of the colonic mucosa with lymphocytes. Aim To investigate the long term clinical and histological evolution of the disease in a large group of patients with well characterised lymphocytic colitis. Methods Between 1986 and 1995 the histological diagnosis of lymphocytic colitis was obtained in 35 patients; 27 of these agreed to a follow up examination. All clinical, endoscopic, and histopathological records were reviewed at that time and the patients had a second endoscopic examination with follow up biopsies. Results The patients initially presented with the typical findings of lymphocytic colitis. After a mean (SD) follow up of 37.8 (27.5) months, diarrhoea subsided in 25 (93%) and histological normalisation was observed in 22 (82%) of the 27 patients. Progression from lymphocytic colitis to collagenous colitis was not observed. Conclusions Lymphocytic colitis is characterised by a benign course with resolution of diarrhoea and normalisation of histology in over 80% of patients within 38 months. Considering the benign course of the disease, the potential benefit of any drug treatment should be carefully weighed against its potential side evects. (Gut 1998;43: ) Keywords: lymphocytic colitis; colitis; diarrhoea The term microscopic colitis was first introduced by Read et al 1 in 1980 to describe a subset of patients with chronic watery diarrhoea of unknown origin, normal endoscopic or radiological findings, and microscopic evidence of an inflammatory infiltrate in the colonic mucosa. Biopsy samples typically show a dense lymphocytic infiltration of the surface epithelial layer. 2 Levison et al suggested replacing the ambiguous term microscopic colitis with lymphocytic colitis and regarding microscopic colitis as an umbrella term to cover all cases of colitis with abnormal histology but normal endoscopic or radiological appearance. 2 The clinical and histopathological features of lymphocytic colitis have been well described. 3 5 The long term course of the disease, however, is mostly known from case reports, and data from larger series describing the evolution of the disease are lacking. The aim of the present study was to characterise the clinical and histopathological long term course of the disease in a relatively large group of 27 patients with well documented lymphocytic colitis. Methods STUDY POPULATION Between 1986 and 1995 the histological diagnosis (index biopsy) of lymphocytic colitis was obtained in 35 outpatients. These patients were asked to participate in a follow up study evaluating the clinical and histological long term course of the disease. One patient was lost to follow up, four (11%) died from unrelated causes, and three (9%) refused to have a second endoscopic examination with biopsy. Therefore 27 (77%) patients could be fully evaluated in this investigation. CLINICAL DATA The clinical and endoscopic records were retrospectively reviewed at the follow up visit and all patients were asked to complete a questionnaire on (a) duration of diarrhoea, (b) stool frequency, (c) stool consistency, (d) other gastrointestinal symptoms including abdominal discomfort, urgency, incontinence, and weight loss, (e) concomitant diseases before and after index investigation, (f) drug history, (g) drugs used to treat lymphocytic colitis, and (h) treatment success. Each patient was asked to grade on a visual analogue scale from 0 to 10 howheorshewasavected by the symptoms of lymphocytic colitis (social impact score), 0 being not avected at all and 10 being severely avected. Diarrhoea was defined as three or more loose bowel movements per day. Stool consistency was classified as watery, viscous (like thick soup), soft (without form), or formed, as described by Read et al. 1 At the follow up visit, informed consent was obtained from each patient for a follow up flexible sigmoidoscopy with biopsy. INDEX COLONOSCOPY/FOLLOW UP SIGMOIDOSCOPY Patients were prepared for the initial colonoscopy with 3 litres of a polyethylene glycol solution taken orally. Biopsy specimens were taken from the terminal ileum and the ascending colon in all patients. The follow up biopsy samples were taken from the sigmoid colon in unprepared patients. HISTOPATHOLOGY The biopsy specimens were fixed in 4% phosphate buvered formaldehyde and embedded in parayn wax. To avoid changes in staining quality and section thickness, 5 mm
2 630 Mullhaupt, Güller, Anabitarte, et al Table 1 Characteristics of the 27 patients with lymphocytic colitis Mean (SD, range) age (years) (n=27) 60 (12, 28 74) Sex (F:M) 20:7 Mean (SD, range) stools/day (n=26) 4.9 (2.6) Mean (SD, range) duration of diarrhoea (months, n=26) 4.0 (3.4, 1 16) Stool consistency (n (%), n=26) Watery 6 (23) Viscous 9 (35) Soft 9 (35) Formed 2 (8) Figure 1 Histological findings at presentation (A) and follow up (B). Staining was with haematoxylin and eosin, original magnification was 250. (A) DiVusely increased surface intraepithelial lymphocytes and surface epithelial damage can be seen. In addition there is a chronic inflammatory infiltrate in the lamina propria and mild crypt distortion. (B) The intraepithelial lymphocytes as well as the inflammatory infiltrate in the lamina propria have disappeared and the surface epithelium is composed of tall columnar epithelial cells. sections from follow up and recut sections from index biopsy samples were stained with haematoxylin and eosin and Masson trichrome. The coded slides were evaluated by one of us (MA). The number of intraepithelial lymphocytes was obtained by counting the lymphocytes per 100 intercryptal epithelial cells. Three areas in each specimen were examined and the mean number of lymphocytes was expressed per 100 epithelial nuclei. The thickness of the subepithelial collagen band was measured with an optical micrometer (graded in 2.5 µm) using the Masson trichrome stain. A diagnosis of lymphocytic colitis was made if an increase in intraepithelial lymphocytes (normal 4.6 (1.5) intraepithelial lymphocytes per 100 intercryptal epithelial cells) was found without a thickened subepithelial collagen layer (<8 mm) and if only a slight disturbance of crypt architecture and discrete inflammatory infiltration of the lamina propria were seen. STATISTICAL ANALYSIS Descriptive statistics are reported as mean (SD) and including range or frequencies as appropriate. Comparisons were tested by paired or unpaired Student s t test. Correlations between diverent factors were analysed by linear regression analysis. Variables found to be significantly associated were then tested in a stepwise linear regression analysis. Statistical significance was assumed by a p value of less than 0.05 (two tailed analysis). Results CLINICAL, ENDOSCOPIC AND HISTOLOGICAL DATA AT INDEX VISIT Clinical data Table 1 shows the characteristics of the 27 patients who agreed to participate in the study. The mean (SD) age at diagnosis was 60 (12) years, range Twenty patients were women, corresponding to a 3:1 female preponderance. Colonoscopy was performed in 26 patients because of chronic watery diarrhoea of unknown cause and in one patient for unexplained chronic abdominal pain. In the latter patient, the colonoscopy disclosed a 3 mm polypoid lesion in the left colonic flexure. The 26 patients with diarrhoea reported 4.9 (2.6) bowel movements per day which lasted for a mean of 3.8 (3.4) months (range 1 16). At the time of endoscopy, four patients already noted normal bowel habits after a mean duration of diarrhoea of 4 (1.4) months. Stool consistency was watery in six patients (23%), viscous in nine (35%), soft in nine (35%), and formed in two (8%). Fifteen patients (54%) reported mild abdominal pain, 92% urgency of defecation, and 64% suvered some incontinence. Nine of the 27 patients lost a mean of 5.6 (3.4) kg within 2.6 (1.1) months. The social impact score of 5.5 (3.2) indicates that patients were considerably avected by the disease. Simple regression analysis showed a significant correlation between the social impact score and frequency of defecation, incontinence, and urgency (p<0.05). However, in a stepwise regression analysis only frequency of defecation and incontinence independently correlated with the social impact score. One patient was known to have coeliac disease. Five patients took non-steroidal antiinflammatory drugs (NSAIDs) on a regular basis, three of them low dose acetylsalicylic acid for cardiovascular reasons. One patient was receiving ranitidine. Endoscopic findings Total ileocolonoscopy was performed in all patients. None showed changes consistent with inflammatory bowel disease. In 17 patients diverticula were observed.
3 Lymphocytic colitis 631 Table 2 Medical treatment regimens No of patients 5-Aminosalicyclic acid or sulfasalaopyrine 6 3 (50) Spasmolytics 13 7 (54) Loperamide 4 2 (50) Antibiotics 3 3 (100) Normalisation of stool frequency (n (%)) Histology All biopsy samples displayed the typical findings of lymphocytic colitis, with a notable increase in intraepithelial lymphocytes (34.7 (16.0)/100 intercryptal epithelial cells). 6 In addition, the samples showed a divuse inflammatory infiltration of the lamina propria and a flattening of the surface epithelium (fig 1A). No correlation was found between the number of intraepithelial lymphocytes and the number of bowel movements (data not shown). CLINICAL, ENDOSCOPIC, AND HISTOLOGICAL DATA AT FOLLOW UP Clinical data Patients were interviewed after a mean follow up of 37.8 (27.5) months (range 4 101). In 25 of the 27 patients (93%), stool frequency was normal. Two patients (7%) had persistent diarrhoea with 4.0 (1.4) bowel movements a day. Stool consistency was soft and viscous respectively. Information on treatment results was obtained in 22 patients; in two patients the data could not be evaluated, one had no diarrhoea, and two patients received no drug treatment. Six patients were treated with more than one medication. Normalisation of stool frequency was observed in three of six patients (50%) treated with 5-aminosalicylic acid or sulfasalazopyridine. Diarrhoea ceased in seven of 13 patients (54%), who received spasmolytics. Two of four patients (50%) treated with loperamide and all three patients receiving antibiotic treatment showed normalisation of bowel habits (table 2). Intraepithelial lymphocytes (%) Index biopsy Persisting diarrhoea (2/27) No diarrhoea (25/27) Follow up biopsy Figure 2 Persistence of diarrhoea plotted against percentage of intraepithelial lymphocytes. Results are expressed as mean (SEM). Histology In 22 patients (82%) the inflammatory infiltrate had completely disappeared (fig 1B) and in five patients the lymphocytic colitis persisted (19%). Progression from lymphocytic to collagenous colitis was not observed. Normalisation of bowel habits (25 out of 27) was associated with a statistically significant (p<0.001) decrease in intraepithelial lymphocytes (fig 2). Of these 25 patients, 22 had normal biopsy findings and three still had lymphocytic colitis despite normal bowel habits. However, none of the patients with persisting diarrhoea had a normal colonic biopsy result at follow up, and in all patients with normal colonic biopsy results diarrhoea had stopped (fig 2). Mean follow up time of patients with normal histology was 40 months as compared with 29 months in patients with persisting inflammatory change (p>0.05). Discussion Lymphocytic colitis is a recently described disease, which is characterised by chronic watery diarrhoea of unknown cause, essentially normal endoscopic and radiological findings, and pronounced lymphocytic infiltration of the colorectal mucosa. 1 6 The clinical and histological features of lymphocytic colitis have been well described, but the natural history has only been poorly characterised. In our long term study with a mean follow up of 38 months, we found that lymphocytic colitis is characterised by a benign course. Diarrhoea persisted in only two and the lymphocytic infiltrate in five patients. Normal histology at follow up was associated with normalisation of bowel habits in all patients, and unremitting diarrhoea was associated with persisting inflammatory changes of the colonic mucosa. Very divergent outcomes of lymphocytic colitis have been described, based mostly on case reports or studies with small patient numbers. At one end of the spectrum, lymphocytic colitis is described as a mild self limiting disease. 3 4 At the other end, one case has been reported with a fulminant course requiring colectomy. 7 At least as conflicting are the histological follow up data. Some authors report the disappearance of the inflammatory infiltrate with time. 8 Others describe persisting inflammation, in some cases with progression to collagenous colitis. 3 According to our data, lymphocytic colitis should be considered a benign disease with complete clinical and histological normalisation in over 80% of patients within three years. In our study, we did not observe any progression from lymphocytic colitis to collagenous colitis. It is still unclear whether lymphocytic and collagenous colitis should be considered as one disease, lymphocytic colitis representing the first phase of collagenous colitis, 9 10 or whether they are related but distinct entities. 11 The lack of progression from lymphocytic colitis to collagenous colitis observed in our study and the distinct immunological diverences between the two diseases 3 support the hypothesis that lymphocytic colitis and collagenous colitis are related but distinct diseases. Three patients in our series presented without diarrhoea at follow up but with persistent lymphocytic colitis, a course that has previously been described. 4 8 It is noteworthy that the mean follow up time of patients with
4 632 Mullhaupt, Güller, Anabitarte, et al normal histology was 40 months compared with 29 month in patients with persisting inflammatory changes. Even though this diverence did not reach statistical significance, probably because of the small sample size, one might argue that the longer the follow up, the higher the likelihood of histological normalisation. The persisting inflammatory infiltrate seen in patients with resolved diarrhoea may suggest that clinical normalisation precedes histological normalisation. The intraepithelial lymphocyte count significantly correlated with the presence or absence of diarrhoea, but not with its severity. A correlation between stool weight and lamina propria cellularity was previously observed in patients with collagenous and microscopic colitis. 12 Both studies therefore suggest that the inflammatory infiltrate, triggered by some unknown, probably luminal, factor is involved in the pathogenic process leading to chronic diarrhoea. It should be cautiously noted that biopsy specimens from index and follow up examinations in our patients were not taken from the same segment of the colon. The index investigation was always a complete ileocolonoscopy, and the follow up examination a flexible sigmoidoscopy only. Accordingly index biopsy specimens were usually obtained from the ascending colon, whereas all follow up samples were taken from the sigmoid colon. However, we do not believe that this explains the diverence in intraepithelial lymphocyte counts between index and follow up biopsy samples, as lymphocytic colitis usually avects the entire colon. Thus the intraepithelial lymphocyte count is quite similar between the various segments of the large bowel Therefore biopsy samples from the sigmoid colon may be considered to be representative of the entire colon. In a minority of patients, lymphocytic colitis can be present in the absence of diarrhoea. This has also been documented for collagenous colitis. 16 Only one of our patients did not present with diarrhoea. Slightly more than half of our patients presented with diarrhoea, urgency, and crampy abdominal pain, symptoms compatible with irritable bowel syndrome. It has already been pointed out that there is some clinical resemblance between irritable bowel syndrome and lymphocytic colitis. 3 Is lymphocytic colitis in these patients therefore an incidental finding only, unrelated to the clinical symptoms? There are several arguments against this assumption. Firstly, irritable bowel syndrome usually begins at a younger age than that of our study population; secondly, patients with irritable bowel syndrome usually complain of alternating constipation and diarrhoea; thirdly, they have a more insidious onset of the disease. Our patients with lymphocytic colitis had a sudden onset of diarrhoea, an observation also made in patients with collagenous colitis. 17 Importantly, the histological results of colonic biopsy specimens from patients with irritable bowel syndrome are always normal. The results of our study emphasise that, in patients with chronic watery diarrhoea and crampy abdominal pain, urgency, or incontinence, a colonoscopic investigation with biopsy is mandatory, before a diagnosis of irritable bowel syndrome can be entertained. The strongest argument, however, that lymphocytic colitis is not an incidental finding is provided by a recent study in which a marked reduction in colonic water absorption resulting from reduced active and passive sodium and chloride absorption was observed. 18 Furthermore chloride/bicarbonate exchange was also reduced. The inflammatory infiltrate of the colonic mucosa is therefore associated with a reduction in colonic fluid absorption, which probably contributes to the development of diarrhoea. Drugs such as ranitidine 19 and cyclo 3 fort, a phlebotonic drug commonly used in France, 20 have been implicated in the cause of lymphocytic colitis. In our study one patient was on ranitidine and none of our patients used cyclo 3 fort. It should be noted that five of our patients used NSAIDs. An association between NSAIDs and collagenous colitis has been reported, but a relation between NSAID intake and lymphocytic colitis has never been established. However, it cannot be ruled out that NSAIDs contribute to the development of lymphocytic colitis in these patients. Half of our patients responded favourably to treatment with 5-aminosalicylic acid or sulfosalazopyridine, spasmolytics, or loperamide. Even though no bacteriological investigations were performed and there is no clear evidence for an infectious aetiology of lymphocytic colitis, it is intriguing that all three patients treated with antibiotics showed prompt resolution of their symptoms. Similar results were reported in a recent publication, in which various antibiotics induced clinical remission in 63% of patients with collagenous colitis. 17 In another study, bacterial cytotoxins were found in the stool of a patient with collagenous colitis. 21 In addition, faecal diversion results in clinical and histological remission, with relapse on restoration of the faecal stream. 22 All these findings suggest that a luminal infectious agent may be involved in the pathogenesis of collagenous colitis and lymphocytic colitis. In summary, our study shows that lymphocytic colitis is characterised by a benign course, with normalisation of stool frequency and histology in over 80% of patients within 40 months. None of the patients with persisting diarrhoea had normal colonic biopsy results at follow up, and in all patients with normal colonic biopsy findings at follow up diarrhoea had stopped. Considering the benign course of the disease, we believe that the potential benefit of any long term drug treatment should be carefully weighed against its potential side evects. 1 Read NW, Kreis GJ, Read MG, et al. Chronic diarrhea of unknown origin. Gastroenterology 1980;78: Levison DA, Lazenby AJ, Yardley JH. Microscopic colitis cases revisited. Gastroenterology 1993;105: Giardiello FM, Lazenby AJ, Bayless TM, et al. Lymphocytic (microscopic) colitis: clinicopathologic study of 18 patients and comparison to collagenous colitis. Dig Dis Sci 1989;34:
5 Lymphocytic colitis Kingham JGC, Levison DA, Ball JA, et al. Microscopic colitis: a cause of chronic watery diarrhoea. BMJ 1982;285: Veress B, Löfberg R, Bergman L. Microscopic colitis syndrome. Gut 1995;36: Lazenby AJ, Yardley JH, Giardiello FM, et al. Lymphocytic ( microscopic ) colitis: a comparative histopathologic study with particular reference to collagenous colitis. Hum Pathol 1989;20: Bowling TE, Price AB, Al-Adnani M, et al. Interchange between collagenous and lymphocytic colitis in severe disease with autoimmune associations requiring colectomy: a case report. Gut 1996;38: Fasoli R, Jewell DP. Response to treatment of microscopic colitis. Ital J Gastroenterol 1994;26: Sylwestrowicz T, Kelly JK, Hwang WS, et al. Collagenous colitis and microscopic colitis: the watery diarrhea-colitis syndrome. Am J Gastroenterol 1989;84: Jessurun J, Yardley JH, Le EL, et al. Microscopic and collagenous colitis: diverent names for the same condition? Gastroenterology 1986;91: Yardley JH, Lazenby AJ, Giardiello FM, et al. Collagenous, microscopic, lymphocytic, and other gentle and more subtle forms of colitis. Hum Pathol 1990;21: Lee E, Schiller LR, Vendrell D, et al. Subepithelial collagen table thickness in colon specimens from patients with microscopic colitis and collagenous colitis. Gastroenterology 1992;103: Zeroogian JM, Chopra S. Collagenous colitis and lymphocytic colitis. Annu Rev Med 1994;45: El-Shabrawi M, Wilkinson ML, Portmann B, et al. Primary sclerosing cholangitis in childhood. Gastroenterology 1987; 92: Keller K, Koch HK. The use of PCNA expression and intraepithelial lymphocyte count in the diverential diagnosis of inflammatory bowel disease. Ital J Gastroenterol 1994; 26: Leigh C, Elahmady A, Mitros FA, et al. Collagenous colitis associated with chronic constipation. Am J Surg Pathol 1993;17: Bohr J, Tysk C, Eriksson S, et al. Collagenous colitis: a retrospective study of clinical presentation and treatment in 163 patients. Gut 1996;39: Bo-Linn GW, Vendrell DD, Lee E, et al. An evaluation of the significance of microscopic colitis in patients with chronic diarrhea. J Clin Invest 1985;75: Beaugerie L, Patey N, Brousse N. Ranitidine, diarrhoea, and lymphocytic colitis. Gut 1995;37: Beaugerie L, Luboinski J, Brousse N, et al. Drug induced lymphocytic colitis. Gut 1994;35: Andersen T, Andersen JR, Tvede M, et al. Collagenous colitis: are bacterial cytotoxins responsible? Am J Gastroenterol 1993;88: Järnerot G, Tysk C, Bohr J, et al. Collagenous colitis and fecal stream diversion. Gastroenterology 1995;109: Gut: first published as /gut on 1 November Downloaded from on 30 September 2018 by guest. Protected by copyright.
Paucicellular and Asymptomatic Lymphocytic Colitis Expanding the Clinicopathologic Spectrum of Lymphocytic Colitis
 Anatomic Pathology / PAUCICELLULAR AND ASYMPTOMATIC LYMPHOCYTIC COLITISA Paucicellular and Asymptomatic Lymphocytic Colitis Expanding the Clinicopathologic Spectrum of Lymphocytic Colitis Neal S. Goldstein,
Anatomic Pathology / PAUCICELLULAR AND ASYMPTOMATIC LYMPHOCYTIC COLITISA Paucicellular and Asymptomatic Lymphocytic Colitis Expanding the Clinicopathologic Spectrum of Lymphocytic Colitis Neal S. Goldstein,
C ollagenous colitis (CC) and lymphocytic colitis (LC)
 346 IFLAMMATORY BOWEL DISEASE Microscopic colitis: a common diarrhoeal disease. An epidemiological study in Örebro, Sweden, 1993 1998 M Olesen, S Eriksson, J Bohr, G Järnerot, C Tysk... See end of article
346 IFLAMMATORY BOWEL DISEASE Microscopic colitis: a common diarrhoeal disease. An epidemiological study in Örebro, Sweden, 1993 1998 M Olesen, S Eriksson, J Bohr, G Järnerot, C Tysk... See end of article
Lymphocytic colitis: a distinct clinical entity? A clinicopathological confrontation of lymphocytic and collagenous colitis
 Gut 1999;45:375 381 375 University Hospital Gasthuisberg, Leuven, Belgium F Baert G D Haens Pathology, University Hospital Gasthuisberg, Leuven, Belgium K Wouters K Geboes Catholic University of Louvain,
Gut 1999;45:375 381 375 University Hospital Gasthuisberg, Leuven, Belgium F Baert G D Haens Pathology, University Hospital Gasthuisberg, Leuven, Belgium K Wouters K Geboes Catholic University of Louvain,
Keep microscopic colitis in mind!
 Keep microscopic in mind! Information for gastroenterologists and pathologists D. Aust (Dresden), S. Miehlke (Hamburg) An initiative of the EUROPEAN MICROSCOPIC COLITIS GROUP Microscopic is a chronic inflammatory
Keep microscopic in mind! Information for gastroenterologists and pathologists D. Aust (Dresden), S. Miehlke (Hamburg) An initiative of the EUROPEAN MICROSCOPIC COLITIS GROUP Microscopic is a chronic inflammatory
Is microscopic colitis a missed diagnosis in diarrhea-predominant Irritable Bowel Syndrome?
 Received: 23.8.2007 Accepted: 15.6.2008 Is microscopic colitis a missed diagnosis in diarrhea-predominant Irritable Bowel Syndrome? Hamid Tavakkoli*, Farshad Sheikh Esmaeili**, Mohammad Hasan Emami***,
Received: 23.8.2007 Accepted: 15.6.2008 Is microscopic colitis a missed diagnosis in diarrhea-predominant Irritable Bowel Syndrome? Hamid Tavakkoli*, Farshad Sheikh Esmaeili**, Mohammad Hasan Emami***,
Clinical Characteristics of Microscopic Colitis in Korea: Prospective Multicenter Study by KASID
 Gut and Liver, Vol. 5, No. 2, June 2011, pp. 181-186 ORiginal Article Clinical Characteristics of Microscopic Colitis in Korea: Prospective Multicenter Study by KASID Young Sook Park*,, Dae Hyun Baek*,
Gut and Liver, Vol. 5, No. 2, June 2011, pp. 181-186 ORiginal Article Clinical Characteristics of Microscopic Colitis in Korea: Prospective Multicenter Study by KASID Young Sook Park*,, Dae Hyun Baek*,
Microscopic colitis: Is it a spectrum of inflammatory bowel disease?
 Online Submissions: http://www.wjgnet.com/esps/ wjg@wjgnet.com doi:10.3748/wjg.v19.i26.4252 World J Gastroenterol 2013 July 14; 19(26): 4252-4256 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2013 Baishideng.
Online Submissions: http://www.wjgnet.com/esps/ wjg@wjgnet.com doi:10.3748/wjg.v19.i26.4252 World J Gastroenterol 2013 July 14; 19(26): 4252-4256 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2013 Baishideng.
11/1/2017. Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota. Cerilli & Greenson
 Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota Acute infectious (self-limited) colitis Focal active colitis Pseudomembranous colitis Ischemic colitis Collagenous
Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota Acute infectious (self-limited) colitis Focal active colitis Pseudomembranous colitis Ischemic colitis Collagenous
Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy
 IJMS Vol 33, No 2, June 2008 Original Article Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy H. Tabrizchie, M.J. Zahedie 1, M. Hayatbakhsh
IJMS Vol 33, No 2, June 2008 Original Article Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy H. Tabrizchie, M.J. Zahedie 1, M. Hayatbakhsh
Journal of Medical Case Reports 2010, 4:31
 Journal of Medical Case Reports This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Lymphocytic
Journal of Medical Case Reports This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Lymphocytic
Magnifying image-enhanced endoscopy for collagenous colitis
 Magnifying image-enhanced endoscopy for collagenous colitis Authors Masaaki Kobayashi 1, Takahiro Hoshi 1, Shin-ich Morita 1,TsutomuKanefuji 1, Takeshi Suda 1,GoHasegawa 2, Shuji Terai 3 Institutions 1
Magnifying image-enhanced endoscopy for collagenous colitis Authors Masaaki Kobayashi 1, Takahiro Hoshi 1, Shin-ich Morita 1,TsutomuKanefuji 1, Takeshi Suda 1,GoHasegawa 2, Shuji Terai 3 Institutions 1
Long-term follow-up of collagenous colitis after induction of clinical remission with budesonide
 Aliment Pharmacol Ther 2005; 22: 1115 1119. doi: 10.1111/j.1365-2036.2005.02688.x Long-term follow-up of collagenous colitis after induction of clinical remission with budesonide S. MIEHLKE*, A. MADISCH*,
Aliment Pharmacol Ther 2005; 22: 1115 1119. doi: 10.1111/j.1365-2036.2005.02688.x Long-term follow-up of collagenous colitis after induction of clinical remission with budesonide S. MIEHLKE*, A. MADISCH*,
What is your diagnosis? a. Lymphocytic colitis. b. Collagenous colitis. c. Common variable immunodeficiency (CVID) associated colitis
 Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Lymphocytic and Collagenous Colitis: Epidemiologic Differences and Similarities
 Dig Dis Sci (2013) 58:2970 2975 DOI 10.1007/s10620-013-2718-6 ORIGINAL ARTICLE Lymphocytic and Collagenous Colitis: Epidemiologic Differences and Similarities Amnon Sonnenberg Robert M. Genta Received:
Dig Dis Sci (2013) 58:2970 2975 DOI 10.1007/s10620-013-2718-6 ORIGINAL ARTICLE Lymphocytic and Collagenous Colitis: Epidemiologic Differences and Similarities Amnon Sonnenberg Robert M. Genta Received:
Case History B Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment
 Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
Collagenous colitis associated with small intestinal villous atrophy
 (Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
(Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
-2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine. -June 2008: Recurrence of rectal blood loss and urgency
 SD, male 40 yrs. old. (680718M467.) -2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine -June 2008: Recurrence of rectal blood loss and urgency Total colonoscopy: ulcerative rectitis,
SD, male 40 yrs. old. (680718M467.) -2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine -June 2008: Recurrence of rectal blood loss and urgency Total colonoscopy: ulcerative rectitis,
Collagenous gastritis and collagenous colitis: a report with sequential histological and ultrastructural findings
 Gut 1999;44:881 885 881 CASE REPORTS Wellcome Trust Research Laboratory, Christian Medical College and Hospital, Vellore 632004, India A B Pulimood B S Ramakrishna M M Mathan Correspondence to: Dr A B
Gut 1999;44:881 885 881 CASE REPORTS Wellcome Trust Research Laboratory, Christian Medical College and Hospital, Vellore 632004, India A B Pulimood B S Ramakrishna M M Mathan Correspondence to: Dr A B
Microscopic colitis syndrome
 880 Microscopic colitis syndrome Gut 1995; 36: 880-886 Department of Pathology B Veress Unit of Gastroenterology R Lofberg Karolinska Institute, Huddinge University Hospital, Huddinge, Sweden Department
880 Microscopic colitis syndrome Gut 1995; 36: 880-886 Department of Pathology B Veress Unit of Gastroenterology R Lofberg Karolinska Institute, Huddinge University Hospital, Huddinge, Sweden Department
Clinical Journal of Gastroenterology (2010) 3(1): Collagenous colitis appeared after 6-year administration of lansoprazole
 Clinical Journal of Gastroenterology (2010) 3(1):18-21. Collagenous colitis appeared after 6-year administration of lansoprazole Sawada, Koji ; Fujiya, Mikihiro ; Itabashi, Kentaro ; Suzuki, Yasuyuki ;
Clinical Journal of Gastroenterology (2010) 3(1):18-21. Collagenous colitis appeared after 6-year administration of lansoprazole Sawada, Koji ; Fujiya, Mikihiro ; Itabashi, Kentaro ; Suzuki, Yasuyuki ;
Role of bile acids and bile acid binding agents in patients with collagenous colitis
 170 Division of Gastroenterology, Department of Internal Medicine, Sahlgrenska University Hospital, S-413 45 Göteborg, Sweden K-A Ung R Gillberg A Kilander H Abrahamsson Correspondence to: Dr K-A Ung.
170 Division of Gastroenterology, Department of Internal Medicine, Sahlgrenska University Hospital, S-413 45 Göteborg, Sweden K-A Ung R Gillberg A Kilander H Abrahamsson Correspondence to: Dr K-A Ung.
Diagnostic difficulty arising from rectal recovery
 J Clin Pathol 1996;49:319-323 319 Cellular Pathology, Northwick Park and St Mark's NHS Trust, Harrow T S Levine A B Price Gastroenterology S Mitchell Histopathology, Heraklion University General Hospital,
J Clin Pathol 1996;49:319-323 319 Cellular Pathology, Northwick Park and St Mark's NHS Trust, Harrow T S Levine A B Price Gastroenterology S Mitchell Histopathology, Heraklion University General Hospital,
HDF Case Whipple s disease
 HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014
 INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014 Endoscopic biopsy samples of naïve colitides patients: Role of basal
INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014 Endoscopic biopsy samples of naïve colitides patients: Role of basal
The informed patient. Microscopic colitis. Collagenous and lymphocytic colitis. A. Tromm, Evangelisches Krankenhaus Hattingen (Germany)
 The informed patient Microscopic colitis Collagenous and lymphocytic colitis A. Tromm, Evangelisches Krankenhaus Hattingen (Germany) Publisher 2017 Falk Foundation e.v. All rights reserved. 4th revised
The informed patient Microscopic colitis Collagenous and lymphocytic colitis A. Tromm, Evangelisches Krankenhaus Hattingen (Germany) Publisher 2017 Falk Foundation e.v. All rights reserved. 4th revised
Medical Treatment for Microscopic Colitis: A Community Hospital s Experience
 Original Article Gastroenterol Res. 2017;10(6):329-333 Medical Treatment for Microscopic Colitis: A Community Hospital s Experience Abdallah Haidar a, d, Savreet Kaur a, Nancy Jackson b, Jose Mari Parungao
Original Article Gastroenterol Res. 2017;10(6):329-333 Medical Treatment for Microscopic Colitis: A Community Hospital s Experience Abdallah Haidar a, d, Savreet Kaur a, Nancy Jackson b, Jose Mari Parungao
Aalborg Universitet. Budesonide treatment of collagenous colitis Bonderup, Ole Kristian. Publication date: 2008
 Aalborg Universitet Budesonide treatment of collagenous colitis Bonderup, Ole Kristian Publication date: 2008 Document Version Publisher's PDF, also known as Version of record Link to publication from
Aalborg Universitet Budesonide treatment of collagenous colitis Bonderup, Ole Kristian Publication date: 2008 Document Version Publisher's PDF, also known as Version of record Link to publication from
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Endoscopic mucosal biopsies are useful in distinguishing granulomatous colitis due to Crohn s disease from tuberculosis
 Gut 1999;45:537 541 537 Wellcome Research Unit, Department of Gastrointestinal Sciences, Christian Medical College and Hospital, Vellore 632 004, Tamilnadu, India A B Pulimood B S Ramakrishna G Kurian
Gut 1999;45:537 541 537 Wellcome Research Unit, Department of Gastrointestinal Sciences, Christian Medical College and Hospital, Vellore 632 004, Tamilnadu, India A B Pulimood B S Ramakrishna G Kurian
Chronic immune colitis in rabbits
 Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
Collagenous colitis presenting as spontaneous perforation in an 80 year old woman: Report of a Case
 Mitchell and Dugas BMC Gastroenterology (2016) 16:124 DOI 10.1186/s12876-016-0533-1 CASE REPORT Open Access Collagenous colitis presenting as spontaneous perforation in an 80 year old woman: Report of
Mitchell and Dugas BMC Gastroenterology (2016) 16:124 DOI 10.1186/s12876-016-0533-1 CASE REPORT Open Access Collagenous colitis presenting as spontaneous perforation in an 80 year old woman: Report of
Simple objective criteria for diagnosis of causes of
 5808 JClin Pathol 1997;50:580-585 Simple objective criteria for diagnosis of causes of acute diarrhoea on rectal biopsy Division of Pathology, Queen's Medical Centre, Nottingham, UK D Jenkins Department
5808 JClin Pathol 1997;50:580-585 Simple objective criteria for diagnosis of causes of acute diarrhoea on rectal biopsy Division of Pathology, Queen's Medical Centre, Nottingham, UK D Jenkins Department
Quantitative Assessment of the Subepithelial Collagen Band Does Not Increase the Accuracy of Diagnosis of Collagenous Colitis
 Anatomic Pathology / Collagen Thickness Quantitative Assessment of the Subepithelial Collagen Band Does Not Increase the Accuracy of Diagnosis of Collagenous Colitis Carlos A. Rubio, MD, PhD, 1 Abiel Orrego,
Anatomic Pathology / Collagen Thickness Quantitative Assessment of the Subepithelial Collagen Band Does Not Increase the Accuracy of Diagnosis of Collagenous Colitis Carlos A. Rubio, MD, PhD, 1 Abiel Orrego,
Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease
 Gut, 1979, 20, 141-148 Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease R. J. DICKINSON, H. M. GILMOUR, AND D. B. L. McCLELLAND' From the Department of Infectious
Gut, 1979, 20, 141-148 Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease R. J. DICKINSON, H. M. GILMOUR, AND D. B. L. McCLELLAND' From the Department of Infectious
What do we need for diagnosis of IBD
 What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
Patho Basic Chronic Inflammatory Bowel Diseases. Jürg Vosbeck Pathology
 Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Spontaneous Colonic Perforation in a Patient with Collagenous Colitis
 G & H C l i n i c a l C a s e S t u d i e s Spontaneous Colonic Perforation in a Patient with Collagenous Colitis Michael Bennett, MD 1 Hillary Tompkins, MD 1 Bridget Seymour, MD 2 Michael J. O Brien,
G & H C l i n i c a l C a s e S t u d i e s Spontaneous Colonic Perforation in a Patient with Collagenous Colitis Michael Bennett, MD 1 Hillary Tompkins, MD 1 Bridget Seymour, MD 2 Michael J. O Brien,
Inflammatory disorders of the intestines can be
 Seymour Katz, M.D., Series Editor Practical Approach to Microscopic Colitis and Inflammatory Bowel Disease by Noel R. Fajardo and Darrell S. Pardi INTRODUCTION Inflammatory disorders of the intestines
Seymour Katz, M.D., Series Editor Practical Approach to Microscopic Colitis and Inflammatory Bowel Disease by Noel R. Fajardo and Darrell S. Pardi INTRODUCTION Inflammatory disorders of the intestines
HDF Case CRYPTOSPORIDIOSE
 HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
... Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment.
 Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report
 Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
Pembrozulimab Induced Collagenous Colitis. Mokshya Sharma 1, MD, Santhosh Ambika 2, MD University of Nevada, Reno SOM
 Pembrozulimab Induced Collagenous Colitis Mokshya Sharma 1, MD, Santhosh Ambika 2, MD University of Nevada, Reno SOM Background Immune modulating therapy that targets PD1 pathway such as pembrozulimab
Pembrozulimab Induced Collagenous Colitis Mokshya Sharma 1, MD, Santhosh Ambika 2, MD University of Nevada, Reno SOM Background Immune modulating therapy that targets PD1 pathway such as pembrozulimab
MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS
 MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS Wai K. Leung Li Shu Fan Medical Foundation Professor in Gastroenterology Associate Dean (Human Capital), LKS Faculty of Medicine, University
MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS Wai K. Leung Li Shu Fan Medical Foundation Professor in Gastroenterology Associate Dean (Human Capital), LKS Faculty of Medicine, University
RATE OF MICROSCOPIC COLITIS AND CYTOKINE LEVELS IN PATIENTS WITH IRRITABLE BOWEL SYNDROME
 Acta Medica Mediterranea, 2015, 31: 103 RATE OF MICROSCOPIC COLITIS AND CYTOKINE LEVELS IN PATIENTS WITH IRRITABLE BOWEL SYNDROME FEYZULLAH UÇMAK¹, VEDAT GÖRAL 2, UĞUR FIRAT 3, NURIYE METE 4 ¹Department
Acta Medica Mediterranea, 2015, 31: 103 RATE OF MICROSCOPIC COLITIS AND CYTOKINE LEVELS IN PATIENTS WITH IRRITABLE BOWEL SYNDROME FEYZULLAH UÇMAK¹, VEDAT GÖRAL 2, UĞUR FIRAT 3, NURIYE METE 4 ¹Department
GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY
 Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Mucosal healing: does it really matter?
 Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Microscopic Colitis. Darrell S. Pardi, MD Inflammatory Bowel Disease Clinic Mayo Clinic
 Microscopic Colitis Darrell S. Pardi, MD Inflammatory Bowel Disease Clinic Mayo Clinic Research Disclosure Astra Zeneca, P&G, Salix* Consulting Salix* *This program is supported by Salix. Neither Mayo
Microscopic Colitis Darrell S. Pardi, MD Inflammatory Bowel Disease Clinic Mayo Clinic Research Disclosure Astra Zeneca, P&G, Salix* Consulting Salix* *This program is supported by Salix. Neither Mayo
Gastrooesophageal reflux disease. Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia
 Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
Case Report Collagenous Colitis Associated with Protein Losing Enteropathy in a Toddler
 Case Reports in Gastrointestinal Medicine, Article ID 209624, 4 pages http://dx.doi.org/10.1155/2014/209624 Case Report Collagenous Colitis Associated with Protein Losing Enteropathy in a Toddler Osama
Case Reports in Gastrointestinal Medicine, Article ID 209624, 4 pages http://dx.doi.org/10.1155/2014/209624 Case Report Collagenous Colitis Associated with Protein Losing Enteropathy in a Toddler Osama
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
ANATOMIC PATHOLOGY Original Article
 ANATOMIC PATHOLOGY Original Article Histology of the Mucosa in Sigmoid Colon Specimens With Diverticular Disease Observations for the Interpretation of Sigmoid Colonoscopic Biopsy Specimens NEAL S. GOLDSTEIN,
ANATOMIC PATHOLOGY Original Article Histology of the Mucosa in Sigmoid Colon Specimens With Diverticular Disease Observations for the Interpretation of Sigmoid Colonoscopic Biopsy Specimens NEAL S. GOLDSTEIN,
For the past 40 years, it has been standard practice to obtain
 ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
Microscopic colitis. A review
 bs_bs_banner Journal of Digestive Diseases 2013; 14; 277 281 doi: 10.1111/1751-2980.12046 Leading article Microscopic colitis. A review William R. BROWN* & Shalini TAYAL Departments of *Medicine & Pathology,
bs_bs_banner Journal of Digestive Diseases 2013; 14; 277 281 doi: 10.1111/1751-2980.12046 Leading article Microscopic colitis. A review William R. BROWN* & Shalini TAYAL Departments of *Medicine & Pathology,
Research Article Temporary Fecal Diversion in the Management of Colorectal and Perianal Crohn s Disease
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2015, Article ID 286315, 5 pages http://dx.doi.org/10.1155/2015/286315 Research Article Temporary Fecal Diversion in the Management
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2015, Article ID 286315, 5 pages http://dx.doi.org/10.1155/2015/286315 Research Article Temporary Fecal Diversion in the Management
Fujiya M, Saitoh Y, Watari J, Moriichi K, Kohgo Y.
 Digestive Endoscopy (2007) 19(s1):S145-S149. Auto-Fluorescence Imaging is useful to assess the activity of ulcerative colitis Fujiya M, Saitoh Y, Watari J, Moriichi K, Kohgo Y. Auto-Fluorescence Imaging
Digestive Endoscopy (2007) 19(s1):S145-S149. Auto-Fluorescence Imaging is useful to assess the activity of ulcerative colitis Fujiya M, Saitoh Y, Watari J, Moriichi K, Kohgo Y. Auto-Fluorescence Imaging
Clinico-pathological study of colonoscopic biopsies in patients with chronic diarrhea
 International Journal of Research in Medical Sciences Bhagyalakshmi A et al. Int J Res Med Sci. 2016 Jul;4(7):2738-2744 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20161942
International Journal of Research in Medical Sciences Bhagyalakshmi A et al. Int J Res Med Sci. 2016 Jul;4(7):2738-2744 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20161942
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Ulcerative Colitis. ulcerative colitis usually only affects the colon.
 Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis
 doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
Title: Fecal microbiota transplantation in recurrent Clostridium difficile infection in a patient with concomitant inflammatory bowel disease
 Title: Fecal microbiota transplantation in recurrent Clostridium difficile infection in a patient with concomitant inflammatory bowel disease Authors: Marta Gravito-Soares, Elisa Gravito-Soares, Francisco
Title: Fecal microbiota transplantation in recurrent Clostridium difficile infection in a patient with concomitant inflammatory bowel disease Authors: Marta Gravito-Soares, Elisa Gravito-Soares, Francisco
study was undertaken to assess the epidemiology, course and outcome of UC patients attending a hospital in Jordan.
 Ulcerative colitis (UC) is a relatively uncommon, chronic, recurrent inflammatory disease of the colon or rectal mucosa [1]. Often a lifelong illness, the condition can have a profound emotional and social
Ulcerative colitis (UC) is a relatively uncommon, chronic, recurrent inflammatory disease of the colon or rectal mucosa [1]. Often a lifelong illness, the condition can have a profound emotional and social
Cytokine Expression of Microscopic Colitis Including Interleukin-17
 Gut and Liver, Vol. 9, No. 3, May 2015, pp. 381-387 ORiginal Article Cytokine Expression of Microscopic Colitis Including Interleukin-17 Eunkyoung Park*, Young Sook Park*, Dae Rim Park*, Sung Ae Jung,
Gut and Liver, Vol. 9, No. 3, May 2015, pp. 381-387 ORiginal Article Cytokine Expression of Microscopic Colitis Including Interleukin-17 Eunkyoung Park*, Young Sook Park*, Dae Rim Park*, Sung Ae Jung,
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding
 Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Bowel cancer risk in the under 50s. Greg Rubin Professor of General Practice and Primary Care
 Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST QUESTIONS. Ver. #
 SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
Uncomplicated diverticular disease is not a common cause of colonic symptoms
 Alimentary Pharmacology and Therapeutics Uncomplicated diverticular disease is not a common cause of colonic symptoms J. Y. Kang*, B. Firwana*, A. E. Green*, H. Matthews*, A. Poullis*, A. Barnabas*, L.
Alimentary Pharmacology and Therapeutics Uncomplicated diverticular disease is not a common cause of colonic symptoms J. Y. Kang*, B. Firwana*, A. E. Green*, H. Matthews*, A. Poullis*, A. Barnabas*, L.
How to characterize dysplastic lesions in IBD?
 How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital
 IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
GUIDELINES FOR THE INITIAL BIOPSY DIAGNOSIS OF CHRONIC IDIOPATHIC INFLAMMATORY BOWEL DISEASE A STRUCTURED APPROACH TO COLORECTAL BIOPSY ASSESSMENT
 Guidelines for the Initial Biopsy Diagnosis of Chronic Idiopathic Inflammatory Bowel Disease 1 GUIDELINES FOR THE INITIAL BIOPSY DIAGNOSIS OF CHRONIC IDIOPATHIC INFLAMMATORY BOWEL DISEASE A STRUCTURED
Guidelines for the Initial Biopsy Diagnosis of Chronic Idiopathic Inflammatory Bowel Disease 1 GUIDELINES FOR THE INITIAL BIOPSY DIAGNOSIS OF CHRONIC IDIOPATHIC INFLAMMATORY BOWEL DISEASE A STRUCTURED
Level 2. Non Responsive Celiac Disease KEY POINTS:
 Level 2 Non Responsive Celiac Disease KEY POINTS: Celiac Disease (CD) is an autoimmune condition triggered by ingestion of gluten leading to intestinal damage and a variety of clinical manifestations.
Level 2 Non Responsive Celiac Disease KEY POINTS: Celiac Disease (CD) is an autoimmune condition triggered by ingestion of gluten leading to intestinal damage and a variety of clinical manifestations.
Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R.
 UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R.
 UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
embedded tissue-sections has the advantage of permanence of the sections and is more suitable for
 Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Journal of. The Yield of Mapping Biopsy from Apparent Endoscopically Normal Colon and Correlation with Symptoms
 Journal of Gastroenterology and Hepatology Research Online Submissions: http://www.ghrnet.org/index./joghr/ doi:.65/j.issn.2224-2.24..46 Journal of GHR 24 July 2 (7): 68-72 ISSN 2224-2 (print) ISSN 2224-65
Journal of Gastroenterology and Hepatology Research Online Submissions: http://www.ghrnet.org/index./joghr/ doi:.65/j.issn.2224-2.24..46 Journal of GHR 24 July 2 (7): 68-72 ISSN 2224-2 (print) ISSN 2224-65
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Colon Investigation. Flexible Sigmoidoscopy
 Colon Investigation Flexible Sigmoidoscopy What is a flexible sigmoidoscopy? Flexible sigmoidoscopy is a frequently performed test to investigate the lower part of the bowel. This is an endoscopic test
Colon Investigation Flexible Sigmoidoscopy What is a flexible sigmoidoscopy? Flexible sigmoidoscopy is a frequently performed test to investigate the lower part of the bowel. This is an endoscopic test
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON
 TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
fever a persistent unexplained change in bowel habit in somebody over 50 years of age a family history of bowel or ovarian cancer.
 If you have had these symptoms for some time, if they come and go but never completely go away, then go and see your doctor. In practice, IBS is a diagnosis of exclusion. There is no test or marker that
If you have had these symptoms for some time, if they come and go but never completely go away, then go and see your doctor. In practice, IBS is a diagnosis of exclusion. There is no test or marker that
Polyps Adenomas Lipomas
 30 Chapter 2 CT Colonography Chapter 2 Polyps Adenomas Lipomas Case 8 Case 9 Case 10 Case 11 Case 12 Case 13 Case 14 Case 15 Case 16 Case 17 Case 18 Pseudopolyp Polyp after intravenous administration of
30 Chapter 2 CT Colonography Chapter 2 Polyps Adenomas Lipomas Case 8 Case 9 Case 10 Case 11 Case 12 Case 13 Case 14 Case 15 Case 16 Case 17 Case 18 Pseudopolyp Polyp after intravenous administration of
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
How to differentiate Segmental Colitis Associated with Diverticulosis and Inflammatory Bowel Diseases?
 How to differentiate Segmental Colitis Associated with Diverticulosis and Inflammatory Bowel Diseases? Alessandro Armuzzi Lead IBD Unit Complesso Integrato Columbus Fondazione Policlinico Gemelli Università
How to differentiate Segmental Colitis Associated with Diverticulosis and Inflammatory Bowel Diseases? Alessandro Armuzzi Lead IBD Unit Complesso Integrato Columbus Fondazione Policlinico Gemelli Università
Pouchitis and Cuffitis A bloody mess. Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board
 Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
Standard of care Inflammatory Bowel Disease (IBD)
 Standard of care Inflammatory Bowel Disease (IBD) Inflammatory bowel disease (IBD) Tens of thousands of Australians live with the debilitating symptoms of Crohn s disease or ulcerative colitis the two
Standard of care Inflammatory Bowel Disease (IBD) Inflammatory bowel disease (IBD) Tens of thousands of Australians live with the debilitating symptoms of Crohn s disease or ulcerative colitis the two
Three-dimensional structure of the human small intestinal mucosa in health and disease
 Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
Authors and Disclosures
 Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
Role of Carbon Dioxide-Releasing Suppositories in the Treatment of Chronic Functional Constipation A Double-Blind, Randomised, Placebo-Controlled Trial M. Lazzaroni; V. Casini; G. Bianchi Porro Authors
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS
 SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
This is a repository copy of Development and Validation of a Scoring System to Identify Patients With Microscopic Colitis.
 This is a repository copy of Development and Validation of a Scoring System to Identify Patients With Microscopic Colitis. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/97306/
This is a repository copy of Development and Validation of a Scoring System to Identify Patients With Microscopic Colitis. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/97306/
Inflammatory Bowel Disease Ischemic bowel disease
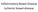 Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
Protein-losing Enteropathy Associated with Collagenous Colitis Cured by Withdrawal of a Proton Pump Inhibitor
 SE REPORT Protein-losing Enteropathy ssociated with ollagenous olitis ured by Withdrawal of a Proton Pump Inhibitor Tomonori Ozeki, Naotaka Ogasawara, Shinya Izawa, Mari Mizuno, Kenichiro Yanamoto, Hisatsugu
SE REPORT Protein-losing Enteropathy ssociated with ollagenous olitis ured by Withdrawal of a Proton Pump Inhibitor Tomonori Ozeki, Naotaka Ogasawara, Shinya Izawa, Mari Mizuno, Kenichiro Yanamoto, Hisatsugu
Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate.
 NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND. Fabrizio Parente
 NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
Kids Like to Break the Rules: Gastrointestinal Pathology in Children
 Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Patterns of Colonic Involvement at Initial Presentation in Ulcerative Colitis A Retrospective Study of 46 Newly Diagnosed Cases
 Anatomic Pathology / PATTERNS OF INVOLVEMENT IN ULCERATIVE COLITIS Patterns of Colonic Involvement at Initial Presentation in Ulcerative Colitis A Retrospective Study of 46 Newly Diagnosed Cases Marie
Anatomic Pathology / PATTERNS OF INVOLVEMENT IN ULCERATIVE COLITIS Patterns of Colonic Involvement at Initial Presentation in Ulcerative Colitis A Retrospective Study of 46 Newly Diagnosed Cases Marie
Spectrum of Diverticular Disease. Outline
 Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
Spectrum of Disease ACG Postgraduate Course January 24, 2015 Lisa Strate, MD, MPH Associate Professor of Medicine University of Washington, Seattle, WA Outline Traditional theories and updated perspectives
Bloating, Flatulence, and
 A 45-Year-Old Man With Recurrent Abdominal Pain, Bloating, Flatulence, and Intermittent Loose Stools Anthony J. Lembo, MD Associate Professor of Medicine Harvard Medical School Director, GI Motility Laboratory
A 45-Year-Old Man With Recurrent Abdominal Pain, Bloating, Flatulence, and Intermittent Loose Stools Anthony J. Lembo, MD Associate Professor of Medicine Harvard Medical School Director, GI Motility Laboratory
