Review Article Genetic Epidemiology, Hematological and Clinical Features of Hemoglobinopathies in Iran
|
|
|
- Cameron Mitchell
- 5 years ago
- Views:
Transcription
1 BioMed Research International Volume 2013, Article ID , 10 pages Review Article Genetic Epidemiology, Hematological and Clinical Features of Hemoglobinopathies in Iran Zohreh Rahimi 1,2 1 Medical Biology Research Center, Kermanshah University of Medical Sciences, Daneshgah Avenue, P.O. Box , Kermanshah, Iran 2 Department of Biochemistry, Medical School, Kermanshah University of Medical Sciences, Daneshgah Avenue, P.O. Box , Kermanshah, Iran Correspondence should be addressed to Zohreh Rahimi; rahimizus@yahoo.com Received 6 April 2013; Accepted 3 June 2013 Academic Editor: Bipin Savani Copyright 2013 Zohreh Rahimi. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. There is large variation in the molecular genetics and clinical features of hemoglobinopathies in Iran. Studying structural variants of hemoglobin demonstrated that the β-chain variants of hemoglobin S and D-Punjab are more prevalent in the Fars (southwestern Iran) and Kermanshah (western Iran) provinces, respectively. Also, α-chain variants of Hb Q-Iran and Hb Setif are prevalent in western Iran. The molecular basis and clinical severity of thalassemias are extremely heterogenous among Iranians due to the presence of multiethnic groups in the country.β-thalassemia is more prevalent in northern and southern Iran. Among 52 different β-thalassemia mutations that have been identified among Iranian populations, IVSII-1 G:A is the most frequent mutation in most parts of the country. The presence of IVS I-5 G:C mutation with high frequency in southeastern Iran might reflect gene flow from neighboring countries. A wide spectrum of α-thalassemia alleles has been detected among Iranians with α 3.7 kb as the most prevalent α-thalassemia mutation. The prevention program of thalassemia birth in Iran has reduced the birth rate of homozygous β-thalassemia since the implementation of the program in In this review genetic epidemiology, clinical and hematological aspects of hemoglobinopathies, and the prevention programs of β-thalassemia in Iran will be discussed. 1. Introduction Inherited disorders of hemoglobin, hemoglobinopathies, are the most common monogenic diseases. They are a group of autosomal recessive disorders that are classified to two main groups of thalassemia syndromes (α- and β-thalassemia) and structural variants of hemoglobins [1]. The presence of a structural variant along with reduced synthesis of hemoglobin is observed in Hb E [2]. The wide variation in the clinical manifestation of hemoglobin disorders could be attributed to the influence of various genetic modifiers and environmental factors. Heterogenous distribution ofthediseaseandthepresenceofhighvariationinthe phenotypic manifestation of a specific mutation are major problems with the development of programs for the control of the hemoglobinopathies [1]. High frequency of the hemoglobinopathies in some populations, especially in many tropical countries, reflects heterozygote advantage against severe malaria [1]. Also, consanguineous marriage plays an important role in high frequency of these disorders [3]. Iran a country with medium malaria endemicity and high rates of consanguineous marriage consisted of different ethnic groups with various prevalence and clinical feature of hemoglobinopathies. So, the knowledge of genetic epidemiology of hemoglobinopathies in the country will be of valuable help in the development of successful prevention programs and better diagnosis and management of hemoglobin disorders in Iran. 2. Malaria and Hemoglobinopathies Malaria disease is transmitted by anopheline mosquitoes. This disease is highly distributed in tropical and subtropical regions. Malaria hypothesis suggested by Haldane was based on the high carrier frequency of hemoglobinopathies in areas with malaria endemicity; a phenomenon protects carriers against malaria and might be due to the balanced
2 2 BioMed Research International polymorphism in human populations [4]. Epidemiologic, invitro,andinvivostudiessupportassociationbetween structural variants of Hb S, Hb C, and Hb E as well as αand β-thalassemia with areas of prevalence of Plasmodium falciparum [5]. The Hb S variant decreases the risk of infection by P. falciparum. The mechanism of red blood cells (RBC) resistance in sickle cell trait (AS) individuals could be due to the lack of parasite development and accelerating Hb S polymerization in low O 2 tension and higher rates of phagocytosis of parasiteinfected sickle erythrocyte by host immune cells [4, 5]. The Hb AS protects against all forms of malaria by elimination of parasites in 90% of Hb S cell populations. In Hb S carriers the selection occurs at the cost of the loss of homozygotes from sickle cell disease [4, 6]. The selective advantage of Hb C is greater in homozygous state (90%) than in Hb AC carriers (30%) [6]. The protection of β-thalassemia patients against malaria isduetodelayofswitchingfromfetaltoadulthemoglobin resulting in higher level of intracellular Hb F. The Hb F is more stable and stronger than Hb A and is partially resistant to digestion by proteolytic machine of parasite. So, Hb F containingredcellsareinadequatehostsforp. falciparum, and this hemoglobin protects the host from the lethality of malaria [5]. Also, the presence of higher levels of serum antibodies bound to β-thalassemic erythrocytes is the other mechanism provides the protection against malaria in these patients [4]. α-thalassemia is very prevalent in malaria endemic regions which protects against severe forms of P. falciparum infection. Theinfectederythrocytesofα-thalassemia patients have high levels of antibodies on their surface that promote antiparasite effects [4]. The protection of α + -thalassemia against malaria might be due to higher susceptibility of homozygotes to malaria in early life that immunize these individuals and make them resistance to malaria later [7]. The protectiveeffect of α-thalassemia is specific to severe malaria [6]. Iran as an eastern Mediterranean country with medium malaria endemicity [8] started the programof malaria eradication in Later in 1980 the program changed to malaria control program. Now this disease is mostly restricted to three southeastern provinces of Sistan-Baluchestan, Hormozgan,andKerman[9]. According to WHO malaria report Iran is classified in the preelimination stage of malaria [10]. Due to heterozygote advantage against P. falciparum malaria there is a high incidence of the β-thalassemia in Iran especially in northern and southern Iran as the ten provinces with high prevalence of β-thalassaemia are Gilan, Hormozgan, Khuzestan, Kohgiluyeh-Boyer-Ahmad, Fars, Bushehr, Sistan- Baluchestan, Kerman, and Isfahan in northern and southern Iran [11, 12]. The Sistan-Balouchestan province that is the most prevalent area for malaria comprises 42 60% of total malaria cases of Iran. Majority of infected cases (85%) with malaria were due to P. falciparum [13]. Isfahan province locatedincentraliranhasbeenclassifiedasthesixthmore prevalent province for malaria after Sistan-Balouchestan, Hormozgan, Kerman, Fars, and Tehran provinces [14]. The gene frequency of β-thalassaemia has been estimated to be with over 2.25 million carriers [15]. An overall rate of consanguineous marriage (majority first-cousin marriages)is38.6%(rangesfrom16to47%)iniran[15]. 3. Structural Variants 3.1. Hemoglobin S. The hemoglobin (Hb) S that results from glutamic acid valine amino acid substitution at position 6 of β-chain is the most clinically important structural variant of hemoglobin with highest frequency in Africa, Saudi Arabia, and India. Sickle cell disease (SCD) results from the homozygous state of the mutation, or a compound heterozygous state with one of structural variants of Hb D- Punjab, Hb O-Arab, Hb C, or β-thalassemia mutation in the other β-genes [16, 17]. First report of clinical and hematological features of sickle cell anemia in southern Iran demonstrated the high level of Hb F (18%) and mild clinical course of the disease in Iranian patients [18]. The prevalence of sickle cell trait and sickle cell anemia in southern Iran has been estimated to be around 1.43 and 0.1%, respectively [19]. In central Iran (southeast Isfahan) sickle cell trait was reported with a frequency of 8.33% [20]. In contrast, in western Iran the lowest frequency for this hemoglobin variant compared to structural variants of Hb D- Punjab,HbQ-Iran,andHbSetifwasreported[21] Hb D-Punjab. Hb D-Punjab (D-Los Angeles) is characterizedbysubstitutionofglutamineforglutamicacidat position of 121 of β-globin chain [22]. The presence of Hb D-Punjab in combination with an α-chain variant (Hb O- Indonesia) in an Iranian patient was reported 37 years ago by Rahbar et al. [23]. The case had no hemolytic disorders and clinical symptoms. Subsequent report indicated that in Kurdish population from western Iran Hb D-Punjab was the most prevalent structural β-globin variant [22]. Hb D-Punjab was detected as the second prevalent structuralvariantinsouthernprovinceofkhuzestan[24]. Mild clinical presentation of this variant in homozygous and combined heterozygous state with a β 0 -thalassemic mutation and also with concomitant presence of α-andβ 0 -thalassemia mutationshavebeenindicated[22]. Benign feature of Hb D- Punjab was confirmed by two separate reports of concomitant presence of this structural variant with β-thalassemia mutation of IVSII-1 G:A that produced a minor β-thalassemia picture [25, 26] Hb Q-Iran. Singlenucleotidemutationsinα1 or α2 genes produce abnormal α-chain hemoglobins. Hb Q disorders including Hb Q-Iran [α75 (EF4) Asp His],HbQ-Thailand [α74 (EF3) Asp His], and Hb Q-India [α64 (E13) Asp His] are important Hb variants. All of these hemoglobins are slow moving variants that migrate at the electrophoretic position of Hb S at alkaline ph [27, 28].IncarriersofHbQ- Iran this hemoglobin has a level of 17 19% and hematological indices are normal [29]. In recent studies from Kurdish population of western Iran this Hb variant was the second prevalent structural variant with a level of % and in carriers of this hemoglobin hematological indices were normal [21, 29].
3 BioMed Research International Hb Setif. Hb Setif [α94 (G1) Asp Tyr] is an α-chain Hb variant with electrophoretic mobility similar to Hb S atalkalineph.hbsetifismuchlesssolublethanhba and induces pseudosickling of the red cells in vitro. This hemoglobin presents in a low percent (12 17%). Hb Setif has been found in Algeria, Iran, Lebanon, Saudi Arabia, Turkey, Italy, Malta, and Cyprus. This α-chain variant was found to be third prevalent structural variant among Kurdish population fromwesterniranwithalevelof %andnormal hematological indices in carriers of the hemoglobin [29] Epistatic Modifiers and Structural Variants Hb S. The β S mutation has been found to be in linkage disequilibrium with five distinct typical (common) β-globin gene cluster haplotypes. Four of these haplotypes are known as African haplotypes (Bantu, Benin, Senegal, and Cameroon), the fifth is the Arab-Indian haplotype, which was originally described in the eastern oases of Saudi Arabia and among the tribal Adivasi population of India [30]. In Iran genetic studies and determination of haplotype background of β S gene, for the first time, were conducted in central Iran which indicated that the β S gene was in linkage disequilibrium with the Arab-Indian haplotype in this area [20].Subsequently,insouthwesternIrantheassociationof β S gene with Arab-Indian haplotype was reported [31]. Mild clinical presentation of sickle cell anemia in southwestern Iran has been demonstrated with high level of Hb F and the elevation ratio of G γ : A γ chains in sickle cell anemia patients that was attributed to the presence of Xmn I polymorphic site associated with Arab-Indian haplotype [31, 32]. More analysis of β S gene from different provinces of southwestern Iran demonstrated that the most prevalent haplotype in variousethnicgroups(farsandarabs)wasthearab-indian haplotype [30]. However, around 33% of β S genes were correlated with African haplotype. These findings provided an evidence of multicentric origin of β S gene in southwestern Iran.Theprevalenceof α 3.7 kb mutation among SCD patients from southwestern Iran was around 37%. The beneficial effect of the presence of α + -thalassemia in SCD patients of southwesterniranwasappearedinlowerlevelsofmch and MCV [32]. In western Iran the β S gene was in linkage equilibrium with Benin haplotype [21] Hb D-Punjab. Molecular genetic studies indicated an association between β D -PunjabgenewithhaplotypeIand its unicentric origin in western Iran [22]. However, in two southern provinces of Fars and Hormozgan four haplotype backgrounds for β D -Punjab gene with the most prevalent haplotypei(67.5%)havebeenobserved[33] Hb Q-Iran. Higher expression of Hb Q-Iran with lower levels of MCV in carriers of this hemoglobin was observed with concomitant presence of this variant with α 3.7 kb mutation [21]. It has been suggested that Hb Q-Iran is a benign structural variant of Hb, which in combination with a β 0 - thalassemia mutation and in the presence of α + -thalassemia, produces only a minor β-thalassemia picture with moderate anemia and elevation of Hb F [34]. 4. Thalassemia Thalassaemias are characterized by decrease or absence production of α-or β-globin chains, which result in two main types of α- or β-thalassemia [35]. More than 200 different types of deletional and nondeletional mutations in α- or βglobin genes have been detected with diverse clinical manifestations, ranging from asymptomatic to profound fatal anemias in utero [36] β-thalassemia. β-thalassemia has a high prevalence (around 10%) in north, close to the Caspian sea and South of Iran close to the Persian Gulf. The prevalence of βthalassemia alleles in most parts of the country has been estimated to be 4 8% [37, 38]. Overall, there are 20,000 homozygote and 3,750,000 carriers of β-thalassaemia in Iran [39]. Finding 52 different mutations among Iranians and the presence of different mutations in 21% of consanguineous couples suggest the heterogeneous picture of β-thalassaemia mutations among Iranian populations [15]. So, many studies in various parts of Iran have been performed to establish the spectrum of β-thalassemia mutations to help the prenatal diagnosis Southern Iran. In reports from three ethnic groups of Southern provinces of Fars, Hormozgan, and Khuzestan different spectrum and prevalence of β-thalassemia mutations were obtained [24, 37, 40 42].IntheFarsprovince(withethnic background of Fars) IVS II-1 G:A and IVS I-6 T:C were the most prevalent β-thalassemic mutations with the frequencies of 31 and 15%, respectively, among 10 different mutations that were found in 26 studied chromosomes that suggested a genetic admixture and migrations for the presence of high number of β-thalassemic mutations in this area [40]. Second and third reports from this area confirmed the presence of IVS II-1 G:A as the most prevalent β-thalassemic mutation thatwasassociatedwithxmnipolymorphicsite[37, 41]. However, in other southern province of Hormozgan (with various ethnic groups of Fars, Arab, and Balouch) neighboring the Fars province the IVS I-5 G:C with a frequency of 69% was the most prevalent mutation followed by the IVS II-1 G:A (9.6%). In contrast with other provinces of Iran no IVS I-110 G:A or IVS I-1 G:A mutations were found in this area. Also, the severe phenotype of patients homozygous for the IVS II-745 C:G mutation was linked in cis to the 5 UTR +20 C:T transition [42]. In more recent study from Hormozgan province among 224 β-thalassaemia carriers mostly with Fars origin (98%), the IVS I-5 G:C mutation with a frequency of 71% was the most prevalent mutation followed by IVS II-1 G:A (12%) [12].Inthisprovinceduetomalariaselectionand high rates of consanguineous marriages hemoglobinopathies are common [12]. In another southern province of Khuzestan with Arab ethnic background three most common mutations including CD 36/37-T, IVS-II-1 G:A, and IVS-I-110 G:A at a frequency of 20.5, 20.0, and 14.2%, respectively, were detected
4 4 BioMed Research International [24]. The picture of β-thalassaemia mutations in this province is heterogenic with detecting 42 different types of mutations [24] Northern Iran. In three northern provinces of Mazandaran, Gilan, and Golestan, IVS-II-1 G : A with a frequency of 50% was the highest prevalent mutation followed by CD 30 G:C (7.7%). The CD 8 AA, CD 22/23/24 AAGTTGG, and IVS-I-5 G:C were the other common mutations in the area [43]. Similarly, in other studies from these northern provinces the IVS-II-1 G:A was the most prevalent mutation (56.1%) and the CD 30 G:C (8.1%) was the second prevalent mutation. However, CD 8/9 +G (6.1%), CD 22/23/24 AAGTTGG (3%), IVS-I-110 G:A (2.5%), IVS-I-5 G:C (2.3%), and IVS-II-745 C:G (2.3%) were the other common mutations [44]. High prevalence of IVS-II-1 G:A in northern Iran compared to other parts of Iran might be attributed to high rates of consanguineous marriages in this area [44]. In subsequent study from Mazandaran the frequency of IVS-II- 1 G:A mutation as the most prevalent mutation was 61% [45], and the CD 30 G:C with a frequency of 7.5% was the second prevalent mutation. Also, in provinces of East Azerbaijan and Ardabil, northwestern, the most frequent mutations in order of frequencies were IVS-II-1 G:A (21%), IVS-I-110 G:A (18%), CD 8/9 +G (14.5%), CD 8 AA (8%), and IVS-I-1 G:A (7.5%) [46]. In northeastern province of Khorasan in a small subset of chromosomes the CD 8/9 +G was the most frequent mutation (62.5%), and each of the three mutations of IVS-II-1 G:A, 36/37 T,andCD39C:Thadafrequencyof12.5%[43] Western Iran. The spectrum of β-thalassemia mutations in western Iran provinces of Kermanshah (mostly Kurds), Kurdistan (with Kurdish ethnic background), Lorestan (mostly Lors), Ilam (mostly Kurds), and Hamadan (mostly Fars) were identified [43, 47 49]. In the Kermanshah province twenty different mutations were identified that among them around 81% were of β 0 type mutation. Four most common mutations in this part of Iran were IVSII-1 G:A (32.97%), CD8/9 +G (13.51%), IVSI-110 (G:A) (8.38%), and CD 36/37 T(7.84%)[47]. Test of heterogeneity between different Iranian populations indicated that Kermanshah population is significantly different from the population of southern Iran (P < 0.004), degree of freedom (df =7), but considering the most frequent mutations, the spectrum of βthalassemia mutations in Kermanshah is similar to people from Lorestan, Ardabil, East Azerbaijan, Gilan, Mazandaran, Golestan, Tehran, and Isfahan [47]. The spectrum and frequency of β-thalassemia mutations in Kurdistan province have been found to be similar to the Kermanshah province. In the Kurdistan province IVS-II-1 G:A was the most frequent, comprising 35% of all mutations. Other common mutations were CD 8/9 +G (15.7%), IVS-I-1 G:A (8%), CD 5 CT (6.7%), CD 8 AA (6.7%), and IVS- I-110 G:A (6%) [48]. In the Lorestan province CD 36/37 T mutation, with a frequency of 33.8%, was the most common mutation. This mutation has been detected among Kurdish Jews [43]. The other most frequent mutations were IVS-II-1 G:A, IVS-I-110 G:A, and CD 8/9 +G with the frequencies of 27.7, 11.5, and 10.8%, respectively [49]. In two other western provinces of Hamadan and Ilam IVSII-1 G:A (29.4%) was the most prevalent mutation, and IVSI-110 G:A and CD 8 AA were the second and third prevalent mutations with frequencies of 19.6 and 11.7% [43] Central Iran. In a study from central provinces of Tehran, Isfahan, Yazd, Markazi, and Semnan the three most common mutations were IVS-II-1 G:A (28%), CD 8/9 +G (11.7%), and IVS-I-5 G:C (9.3%) [43]. In a subsequent report from the Isfahan province the presence of IVS-II-1 G:A (20.5%) as the most prevalent mutation was confirmed. However,thesecondprevalentmutationwasIVS-I-5G:C (11%) [50] Southeastern Iran. The high frequency of β-thalassemia alleles in the Sistan-Balouchestan province could be attributed to the selection pressure by malaria and high rates of consanguineous marriage among Balouch population. Around 90% of homozygous β-thalassemia patients of the province have ethnic background of Balouch [51]. In this province among Balouch population only IVS I- 5 G : C with an unusual frequency of 87.2% along with CD 8/9 +G with a frequency of 4% constituted about 91% of β-thalassemia mutations. The IVS I-5 G:C has been found as the most prevalent mutation among Sindh and Balouchestan provinces of Pakistan bordering Sistan-Balouchestan province of Iran [51]. Also, in southeastern province of Kerman IVS I-5 G:C was detected to be the high prevalent βthalassemic mutation (66.2%) followed in order of frequency by IVS II-1 G:A (6%) and CD 8/9 +G (4.9%) [52]. The spectrum of β-thalassemia mutations in various parts of Iran indicating the IVSII-1 G:A as the prevalent mutation in most part of Iran with the highest frequency in northern Iran and decreased its frequency toward southern Iran where IVS I-5 G:C is the highest prevalent mutation. The high frequency of Mediterranean mutation IVSII-1 G:A in Iran might be due to an independent origin of this mutation or genetic admixture. The Balouchestan province of Pakistan is known for the highest frequency of IVSI-5 G:C. The presence of this mutation as the most prevalent mutation in Southeastern Iranian province of Sistan-Balouchestan might be due to genetic admixture with the population of neighbor country of Pakistan. The same reason could explain the similar frequency of IVS I-5 G:C (69%) between southern Iranian province of Hormozgan and the southern neighbor of United Arab Emirates (66%) [43] Epistatic Modifiers and β-thalassemia. Genetic variants that results in differences in disease phenotype are known as modifier genes [53]. These modifiers include the presence of α-thalassemia (with reducing the globin chain imbalance) and/or the presence of genetic determinants (with increasing the production of Hb F) in adult life [53]. High frequency of α-thalassemia is observed in many populations with high prevalence of β-thalassemia [54]. The presence of αthalassemia in homozygous or compound heterozygous state of β-thalassemia ameliorates the clinical presentation of
5 BioMed Research International 5 the disease due to the lower concentration of excess α-globin chains [55]. The IVS II-1 G:A among Kurdish population of Kermanshah province (western Iran) was strongly associated with haplotype III [56]. However, this mutation in southern Iran wasmostlyassociatedwithhaplotypei[57]. A frequency of 0.39 was obtained for the Xmn I polymorphic site in βthalassemia major patients of western Iran associated with elevation in G γ-chain level and G γ : A γ ratio and improved clinical features [58]. The increased numbers of γ-chains bind to excess α-globin chains produce Hb F and reduce globin chain imbalance [55].Further,the main molecular basis of the β-thalassemia intermedia phenotype in Iranian cases was determined to be the coinheritance of a positive Xmn I polymorphism with β-globin mutations resulted in increase Hb F production, coinheritance of α-globin defects, andmildpresentationofβ-globin mutations [59]. Also, HS- 111 and 3 HS1 in the promoter region of γ-globin gene in βthalassemia intermedia patients were associated with high level of Hb F [60] α-thalassemia. The α-thalassemias are classified into the α 0 -thalassemia with no synthesis of α-chains and α + - thalassemia with a reduction in synthesis of α-chains. The heterozygous and homozygous α 0 -thalassemia are designated as /αα and /, respectively.α + -Thalassemia in heterozygousandhomozygousstatesisrepresentedas α/αα and α/ α, respectively[61]. The severe α-thalassaemia mutations are restricted to Southeast Asia and some of the Mediterranean islands. The α + -thalassemia deletions are the most common forms of α-thalassemia with two major forms of α 3.7 kb and α 4.2 kb [1, 61]. Also, more than 70 nondeletional forms of α-thalassemia have been detected that might be coinherited with deletional mutations or other genetic modifiers results in diverse genotypic and/or phenotypic expressions [36]. Identification of molecular spectrum of α-thalassemia in southern Iran (Hormozgan province) revealed the two common alleles of α 3.7 kb (79.1%) and α 5nt( TGAGG) (4.3%) in this area [62]. Also, the presence of α 3.7 kb single gene deletion as the most frequently α-chain variant in southwestern provinces of Fars, Khuzestan, and Kohgiluyeh-Boyer-Ahmad was confirmed [63, 64]. In northern provinces of Mazandaran and Gilan 21 and 16 different α-globin alleles, respectively, were found that among them α 3.7 kb with frequencies of 44.9 and 42.5%, respectively, and α PolyA2(AATGAA) with frequencies of 18.2 and 12.4%, respectively, were the most prevalent mutations in this area. The frequency of α 5nt( TGAGG) was 6.5% in Mazandaran and7.1%ingilanprovinces[65, 66]. In Kerman province from southeastern Iran the spectrum of α-thalassemia mutations indicated α 3.7 kb as the most common mutation (83.8%) followed by α CD19( G) (5.7%) and α 5nt( TGAGG) (4.2%) [67]. In some cities of Kerman province such as Jiroft and Kahnooj with malaria endemicity the highest frequencies of α-thalassemia has been detected [67]. Overall, studying 8 different geographic areas of Iran indicated the presence of 16 different α-globin mutations that among them the α 3.7 kb mutation was found to be the most frequent α-thalassemia mutation, comprising 60.2% of αthalassemia alleles. The highest frequency of this mutation was observed in south (93%), and the lowest frequency of the mutation was detected in central (53.9%) Iran. Nine of these mutations including MED, α 4.2 kb, α PolyA2(AATGAA), α CS, α 5nt( TGAGG), α 20.5, α PolyA1(AATAAG), α CD19,andα CD59 reached to a polymorphic frequency (>1%) [68]. Hb H ( / α)isanunstablehbresultingfromdeletion of three α-globin genes and has a mild-to-moderate severe phenotype [69]. This Hb forms intracellular precipitates that results in early cell death. Hemolysis rather than ineffective erythropoiesis is the primary cause of anemia in Hb H disease. Many patients require intermittent transfusions. The clinical severity is strongly influenced by the type of mutation. Among Iranians the clinical diversity of Hb H disease (similar genotypes with different phenotypes) has been reported [70]. Deletions on chromosome 16 are responsible for 75% of Hb H mutations, and these deletions cause a milder form of the disorder. The remaining 25% of patients with Hb H disease have two deletions plus a point mutation or insertion in the α-globin gene. Nondeletional Hb H is often severe and likely requires transfusions. Hemoglobin Constant Spring (Hb CS) is the most common nondeletional α-thalassemia mutation associated with Hb H disease. The gene frequency of Hb CS reachesto8%insoutheastasia.thelaboratoryandclinical course of Hb H/CS disease are more severe than Hb H disease [71]. Studying molecular basis of Hb H disease in southwest Iran indicated the presence of six genotypes associated with Hb H disease in the area including α 3.7 kb / MED, α 3.7 kb /α T-Saudi α, α T-Saudi α/α T-Saudi α, α CS α/ MED, MED/α T-Turkish α,andtheatypicalformsofhbhdisease α 3.7 kb /α CS α. It has been suggested that the molecular background of Hb H disease in the southwest area of Iran is more similar to the Mediterranean type than to the Southeast Asian [72]. AstudyconductedonpatientswithHbHdiseaseto find the association between severity of phenotype according to Hb H genotype. This study revealed a subset of Hb H genotypes, including MED/α CS α, MED/α PolyA2(AATGAA) α, and α CS α/α CS α that was associated with a need for regular or irregular blood transfusions [73]. A map of Iran that depicts provinces with prevalence of hemoglobinopathies is presented in Figure 1. Also,the common types of hemoglobinopathies in different areas of Iran are demonstrated in Table Prevention Programs Due to large economic burden of treatment of β-thalassaemia patients for both affected individuals and national health budget a mandatory premarital screening program for βthalassaemia was established [15]. Preventingprogramsof βthalassaemia in Iran are more cost-effective than treatment of the disease [11]. In Iran, public education, screening, and prenatal diagnosis remarkably decreased the frequency of births of babies
6 6 BioMed Research International Table 1: Common types of hemoglobinopathies in various parts of Iran. Area α-chain variants β-chain variants α-thalassemia β-thalassemia Northern Iran Gilan α 3.7 kb (42.5%) IVS II-1 G : A (52.4%) Mazandaran α 3.7 kb (44.9%) IVS II-1 G : A (62.1%) Golestan IVS II-1 G : A (33.3%) Northwestern Iran East Azerbaijan and Ardabil IVSII-1G : A (21%) West Azerbaijan IVSII-1G : A (35%) Northeastern Iran Khorasan CD 8/9 +G (62.5%) Central Iran Isfahan Hb S IVS II-1 G : A (20.5 and 28%) Southwestern Iran Fars Hb S α 3.7 kb (71.7%) IVS II-1 G : A (24, 31 and 47.8%) Khuzestan Hb S Hb D-Punjab α 3.7 kb (62.6%) CD 36/37 T (20.5%) IVS II-1 G : A (20%) Western Iran Kermanshah Hb Q-Iran Hb D-Punjab IVS II-1 G : A (33%) Hb Setif Kurdistan IVS II-1 G : A (35%) Lorestan CD 36/37 T (33.8%) IVS II-1 G : A (27.7%) Southern Iran Hormozgan α 3.7 kb (79.1%) IVS I-5 G : C (69%) Southeastern Iran Sistan-Balouchestan IVS I-5 G : C (87.2%) Kerman α 3.7 kb (83.8%) IVS I-5 G : C (66.2%) Iranians (with different ethnicity) α 3.7 kb (60.2%) IVS II-1 G : A (34%) with severe forms of β-thalassaemia. Thalassemia carrier screening started from 1991 in Shiraz and then from 1995 in all provinces of Iran with the aims to reduce the burden of disorder by identifying those individuals at increased risk and to determine their reproductive risks and having an affected child. In 1997, the technical committee of prenatal diagnosis (PND) of β-thalassemia in the Ministry of Health and Medical Education was established to define the standard protocolsforpndthatresultedinareducedrateofβthalassemia incidence in the country [74]. At first the only method for prevention of β-thalassemia was premarital screening. In 2001, the laws of the country were modified to permit abortion of affected fetuses [15] then from 2002 theabortionbefore16-weekgestationalagewaspossible [39]. In southern and northern provinces of Iran where the prevalence of β-thalassemia is high the results of this program have been successful in decreasing the birth prevalence of β-thalassemia. However, the incidence of this condition has not been eliminated yet [39]. In this program, it is requiredthateverycoupletobetestedforβ-thalassemia by their red blood cell indices in order to receive a permit formarriageregistration.iftheresultsoftheprevioustest were conspicuous, the levels of hemoglobin A 2 and Hb electrophoresis were also determined. Couples who were both carriers received counseling. For those who ignored the recommendation and decided to marry, prenatal diagnosis and termination of pregnancy in case of an affected fetus have been offered [35, 74]. During this period the average of high risk couple initially deciding not to marry was 90% without detection of new cases of thalassemia [75]. Also, the trend for prenatal diagnosis among at-risk couples of Sistan- Balouchestan significantly increased from 2002 to 2010 [51]. Thalassemia screening program in Iran is a well-coordinated national approach in which screening is integrated with services for patients [76]. 6. Conclusion The molecular basis and clinical severity of α- and βthalassemia are extremely heterogenous among Iranians duetothepresenceofmultiethnicgroupsinthecountry. The presence of Mediterranean β-thalassemic mutation of
7 BioMed Research International 7 Ardabil East Azerbaijan Caspian Sea West Azerbaijan Kurdistan Hamadan Kermanshah Gilan Golestan Mazandaran Tehran Khorasan Lorestan Ilam Isfahan Khuzestan Kohgiluyeh- Boyer-Ahmad Fars Bushehr Persian Gulf Kerman Hormozgan Sistan-Baluchestan Oman Sea Figure 1: Map of Iran depicts provinces with prevalence of hemoglobinopathies. IVSII-1 G:A with highest frequency in most parts of the country might be attributed to the independent origin of this mutation or genetic admixture. However, the presence of IVS I-5 G:C mutation with high frequency in southeastern Iran might reflect gene flow from neighboring countries. A wide spectrum of α-thalassemia alleles has been detected among Iranians with α 3.7 kb as the most prevalent α-thalassemia mutation.therearefewavailablestudiesonthefrequency, genetic and clinical features of structural variants of Hb in Iran. All reports are from southwestern and western Iran indicated that the Hb S and Hb D-Punjab, respectively, have been studied in details as the most prevalent structural variants in these parts of the country. The prevention program of thalassemia birth in Iran by premarital screening, prenatal diagnosis, and termination of pregnancies has been a successful policy in reducing birth rate of homozygous βthalassemia and a large amount of medical expenses in Iran since the implementation of the program in However, it is still more work to achieve zero β-thalassemic birth. Genetic Terms Hb D-Punjab (D- Astructuralvariantofβ-globin chain Los Angeles): (CD 121 Glu Gln) Hb E: A structuralvariantofβ-globin chain (CD 26 Glu Lys) results in reduced synthesis of β-globin chain Hb Q-Iran: A structural variant of α-globin chain (α75 (EF4) Asp His) Hb Setif: A structuralvariantofα-globin chain (α94 (G1) Asp Tyr) Hb S: A structuralvariantofβ-globin chain (CD 6 Glu Val) Hb H: Deletion of three α-globin genes ( / α) α + -Thalassemia: Reduced synthesis of α-globin chains α 0 -Thalassemia: Complete absence of synthesis of α-globin chains β + -Thalassemia: Reduced synthesis of β-globin chains β 0 -Thalassemia: Complete absence of synthesis of β-globin chains. Conflict of Interests The author declares that there is no conflict of interests. References [1] D. J. Weatherall, Current trends in the diagnosis and management of haemoglobinopathies, Scandinavian Journal of Clinical and Laboratory Investigation,vol.67,no.1,pp.1 2,2007. [2] J. M. Old, Screening and genetic diagnosis of haemoglobinopathies, Scandinavian Journal of Clinical and Laboratory Investigation,vol.67,no.1,pp.71 86,2007. [3] D. J. Weatherall, The inherited diseases of hemoglobin are an emerging global health burden, Blood, vol. 115, no. 22, pp , [4] C. López,C.Saravia,A.Gomez,J.Hoebeke,andM.A.Patarroyo, Mechanisms of genetically-based resistance to malaria, Gene,vol.467,no.1-2,pp.1 12,2010. [5] H. L. Shear, L. Grinberg, J. Gilman et al., Transgenic mice expressing human fetal globin are protected from malaria by a novel mechanism, Blood, vol. 92, no. 7, pp , [6]T.N.Williams, Humanredbloodcellpolymorphismsand malaria, Current Opinion in Microbiology, vol. 9, no. 4, pp , 2006.
8 8 BioMed Research International [7] D. Weatherall, J. Clegg, and D. Kwiatkowski, The role of genomics in studying genetic susceptibility to infectious disease, Genome Research,vol.7,no.10,pp ,1997. [8] A.Raeisi,F.Nikpoor,M.R.Kahkha,andL.Faraji, Thetrendof malaria in Islamic Republic Iran from 2002 to 2007, Hakim Research Journal,vol.12,pp.35 41,2009(Persian). [9] B. Farzinnia, A. Saghafipour, and M. R. Abai, Malaria situation and anopheline mosquitoes in Qom Province, Central Iran, Iranian Journal of Arthropod-Borne Diseases, vol.4,no.2,pp , [10] A. A. Hanafi-Bojd, H. Vatandoost, E. Philip et al., Malaria situation analysis and stratification in Bandar Abbas County, Southern Iran, , Iranian Journal of Arthropod-Borne Diseases,vol.4,no.1,pp.31 41,2010. [11] N. Ghotbi and T. Tsukatani, Evaluation of the national health policy of thalassaemia screening the Islamic Republic of Iran, Eastern Mediterranean Health Journal,vol.11,no.3,pp , [12] P. Nikuei, V. Hadavi, M. Rajaei, M. Saberi, F. Hajizade, and H. Najmabadi, Prenatal diagnosis for β-thalassemia major in the Iranian Province of Hormozgan, Hemoglobin,vol.32,no.6,pp , [13] A. Ebrahimzadeh, B. Fouladi, and A. Fazaeli, High rate of detection of mixed infections of Plasmodium vivax and Plasmodium falciparum in South-East of Iran, using nested PCR, Parasitology International,vol.56,no.1,pp.61 64,2007. [14] S. Soleimanifard, M. Akbari, M. Sabetghadam, and S. Saberi, Malaria situation in Isfahan in the last five years, Journal of Isfahan Medical School,vol.29,pp ,2011(Persian). [15] B. S. Strauss, Genetic counseling for thalassemia in the Islamic Republic of Iran, Perspectives in Biology and Medicine, vol.52, no. 3, pp , [16] D.J.Weatherall,J.B.Clegg,D.R.Higgs,andW.G.Wood, The hemoglobinopathies, in The Metabolic and Molecular Basis of Inherited Disease, C. R. Sriver, A. Beadet, W. S. Sly, and D. Valle, Eds.,vol.3,pp ,McGraw-Hill,NewYork,NY,USA, [17] Z. Rahimi and A. Parsian, Sickle cell disease and venous thromboembolism, Mediterranean Journal of Hematology and Infectious Diseases,vol.3,ArticleIDe ,2011. [18] M.Haghshenass,F.Ismail-Beigi,J.B.Clegg,andD.J.Weatherall, Mild sickle cell anaemia in Iran associated with high levels of fetal haemoglobin, Journal of Medical Genetics, vol. 14, no. 3, pp , [19] F. Habibzadeh, M. Yadollahie, M. Ayatollahie, and M. Haghshenass, The prevalence of sickle cell syndrome in South of Iran, Iranian Journal of Medical Sciences, vol. 24, pp , [20]S.Rahgozar,A.A.Poorfathollah,A.R.Moafi,andJ.M.Old, βsgene in Central Iran is in linkage disequilibrium with the Indian-Arab haplotype, The American Journal of Hematology, vol.65,no.3,pp ,2000. [21] Z. Rahimi, A. Muniz, and H. Mozafari, Abnormal hemoglobins among Kurdish population of Western Iran: Hematological and molecular features, Molecular Biology Reports, vol. 37, no. 1, pp , [22] Z. Rahimi, R. Akramipour, R. L. Nagel, A. S. Ahmadi, A. Merat, and F. Bahrehmand, The β-globin gene haplotypes associated with Hb D-Los Angeles [β121(gh4)glu Gln] in Western Iran, Hemoglobin, vol. 30, no. 1, pp , [23] S. Rahbar, G. Nowzari, and M. Poosti, A double heterozygous hemoglobin: hemoglobin O(Indonesia) and hemoglobin D(Punjab)inanindividual, The American Journal of Clinical Pathology, vol. 64, no. 3, pp , [24] H. Galehdari, B. Salehi, S. Azmoun, B. Keikhaei, K. M. Zandian, and M. Pedram, Comprehensive spectrum of the β-thalassemia mutations in Khuzestan, Southwest Iran, Hemoglobin, vol.34,no.5,pp ,2010. [25] Z. Rahimi, R. Akramipour, S. Korani, and R. L. Nagel, Hb D- punjab [β 121 (GH4) Glu Gln]/β0-thalassemia [IVSII.1(G A)] in two cases from an Iranian family: first report, The American Journal of Hematology, vol.81,no.4,pp , [26] M. T. Basmanj, M. Karimipoor, A. Amirian et al., Co-inheritance of hemoglobin D and β-thalassemia traits in three Iranian families: clinical relevance, Archives of Iranian Medicine, vol. 14, no. 1, pp , [27] P. A. Lorkin, D. Charlesworth, H. Lehmann, S. Rahbar, S. Tuchinda, and L. I. Eng, Two haemoglobins Q, α-74 (EF3) and α-75 (EF4) aspartic acid histidine, The British Journal of Haematology,vol.19,no.1,pp ,1970. [28] M. Aksoy, A. Gurgey, C. Altay et al., Some notes about Hb Q- India and Hb Q-Iran, Hemoglobin, vol. 10, no. 2, pp , [29] Z. Rahimi, M. Rezaei, R. L. Nagel, and A. Muniz, Molecular and hematologic analysis of hemoglobin Q-Iran and hemoglobin Setif in Iranian families, Archives of Iranian Medicine, vol. 11, no. 4, pp , [30] Z. Rahimi, A. Merat, N. Gerard, R. Krishnamoorthy, and R. L. Nagel, Implications of the genetic epidemiology of globin haplotypes linked to the sickle cell gene in Southern Iran, Human Biology,vol.78,no.6,pp ,2006. [31] Z. Rahimi, M. Karimi, M. Haghshenass, and A. Merat, βglobin gene cluster haplotypes in sickle cell patients from Southwest Iran, The American Journal of Hematology, vol. 74, no. 3, pp ,2003. [32] Z. Rahimi, A. Vaisi-Raygani, A. Merat, M. Haghshenass, and M. Rezaei, Level of hemoglobin F and G γ gene expression in sickle cell disease and their association with haplotype and XmnI polymorphic site in South of Iran, Iranian Journal of Medical Sciences,vol.32,no.4,pp ,2007. [33]M.Yavarian,M.Karimi,F.Paran,C.Neven,C.L.Harteveld, and P. C. Giordano, Multi centric origin of Hb D-Punjab [β121 (GH4)Glu Gln, GAA CAA], Hemoglobin, vol. 33, no. 6, pp , [34] Z. Rahimi, R. Akramipour, A. Vaisi-Raygani, R. L. Nagel, and A. Muniz, An Iranian child with HbQ-Iran [α75 (EF4) Asp His]/ α 3.7 kb /IVSII.1 G A: first report, Journal of Pediatric Hematology/Oncology,vol.29,no.9,pp ,2007. [35] N. E. Cousens, C. L. Gaff, S. A. Metcalfe, and M. B. Delatycki, Carrier screening forβ-thalassaemia: a review of international practice, European Journal of Human Genetics, vol. 18, no. 10, pp ,2010. [36] E. A. Rachmilewitz and P. J. Giardina, How I treat thalassemia, Blood, vol. 118, no. 13, pp , [37] Z. Rahimi, A. V. Raygani, A. Merat et al., Thalassemic mutationsinsoutherniran, Iranian Journal of Medical Sciences,vol. 31, no. 2, pp , [38] A. Valaei, F. Bayat, A. Kordafshari, S. Zeinali, and M. Karimipoor, A novel polymorphism causes a different restriction pattern by RsaI in the β-globin gene cluster: application in
9 BioMed Research International 9 prenatal diagnosis, Hemoglobin, vol.33,no.6,pp , [39] M. Karimi, N. Jamalian, H. Yarmohammadi, A. Askarnejad, A. Afrasiabi, and A. Hashemi, Premarital screening for βthalassaemia in Southern Iran: options for improving the programme, Journal of Medical Screening,vol.14,no.2,pp.62 66, [40] A.Merat,M.Haghshenas,Z.M.Pouretal., β-thalassemia in Southwestern Iran, Hemoglobin,vol.17,no.5,pp ,1993. [41] M. Karimi, H. Yarmohammadi, S. Farjadian et al., β-thalassemia intermedia from Southern Iran: IVS-II-1 (G A) is the prevalent thalassemia intermedia allele, Hemoglobin, vol.26, no. 2, pp , [42] M. Yavarian, C. L. Harteveld, D. Batelaan, L. F. Bernini, and P. C. Giordano, Molecular spectrum of β-thalassemia in the Iranian Province of Hormozgan, Hemoglobin,vol.25,no.1,pp.35 43, [43] H. Najmabadi, R. Karimi-Nejad, S. Sahebjam et al., The βthalassemia mutation spectrum in the iranian population, Hemoglobin, vol. 25, no. 3, pp , [44] P. Derakhshandeh-Peykar, H. Akhavan-Niaki, A. Tamaddoni et al., Distribution of β-thalassemia mutations in the Northern Provinces of Iran, Hemoglobin, vol. 31, no. 3, pp , [45] H. Akhavan-Niaki, P. Derakhshandeh-Peykar, A. Banihashemi et al., A comprehensive molecular characterization of β thalassemia in a highly heterogeneous population, Blood Cells, Molecules, and Diseases,vol.47,no.1,pp.29 32,2011. [46] M. A. H. Feizi, A. A. H. Feizi, N. Pouladi, M. Haghi, and P. Azarfam, Molecular spectrum of β-thalassemia mutations in Northwestern Iran, Hemoglobin, vol. 32, no. 3, pp , [47] Z. Rahimi, A. Muniz, and A. Parsian, Detection of responsible mutations for β thalassemia in the Kermanshah Province of Iran using PCR-based techniques, Molecular Biology Reports,vol.37, no. 1, pp , [48] M. Haghi, S. Khorshidi, M. A. H. Feizi, N. Pouladi, and A. A. H. Feizi, β-thalassemia mutations in the iranian kurdish population of kurdistan and west azerbaijan provinces, Hemoglobin, vol.33,no.2,pp ,2009. [49] A. A. Kiani, Y. Mortazavi, S. Zeinali, and Y. Shirkhani, The molecular analysis of β-thalassemia mutations in Lorestan Province, Iran, Hemoglobin, vol. 31, no. 3, pp , [50] R.Salehi,C.A.Fisher,P.A.Bignell,G.Eslami,andJ.M.Old, Identification of three novel mutations [-41 (A>C), codon 24 (G), and IVS-I-109 (-T)], in a study of β-thalassemia alleles in the Isfahan Region of Iran, Hemoglobin,vol.34,no.1,pp , [51] E. Miri-Moghaddam, A. Zadeh-Vakili, Z. Rouhani, M. Naderi, P. Eshghi, and A. K. Feizabad, Molecular basis and prenatal diagnosis of β-thalassemia among Balouch population in Iran, Prenatal Diagnosis, vol. 31, no. 8, pp , [52] N. Saleh-Gohari and M. R. Bazrafshani, Distribution of βglobin gene mutations in thalassemia minor population of kerman province, Iran, Iranian Journal of Public Health, vol. 39, no. 2, pp , [53] R. Galanello and R. Origa, β-thalassemia, Orphanet Journal of Rare Diseases, vol. 5, no. 1, article 11, [54] S. L. Thein, Genetic modifiers of β-thalassemia, Haematologica, vol. 90, no. 5, pp , [55] D. J. Weatherall, Single gene disorders or complex traits: lessons from the thalassaemias and other monogenic diseases, The British Medical Journal, vol. 321, no. 7269, pp , [56] Z. Rahimi, A. Muniz, R. Akramipour et al., Haplotype analysis of β thalassemia patients in Western Iran, Blood Cells, Molecules, and Diseases,vol.42,no.2,pp ,2009. [57] M. Yavarian, M. Karimi, E. Bakker, C. L. Harteveld, and P. C. Giordano, Response to hydroxyurea treatment in Iranian transfusion-dependent β-thalassemia patients, Haematologica, vol. 89, no. 10, pp , [58] H. Nemati, Z. Rahimi, and G. Bahrami, The Xmn1 polymorphic site 5 to the G γ geneanditscorrelationtothe G γ : A γ ratio, age at first blood transfusion and clinical features in β-thalassemia patients from Western Iran, Molecular Biology Reports,vol.37,no.1,pp ,2010. [59] M. T. Akbari, P. Izadi, M. Izadyar, K. Kyriacou, and M. Kleanthous, Molecular basis of thalassemia intermedia in Iran, Hemoglobin,vol.32,no.5,pp ,2008. [60] M. Hamid, F. Mahjoubi, M. T. Akbari, A. Arab, S. Zeinali, and M. Karimipoor, Molecular analysis ofγ-globin promoters, HS- 111 and 3 HS1, in β-thalassemia intermedia patients associated with high levels of Hb F, Hemoglobin, vol. 33, no. 6, pp , [61] D. R. Higgs and D. J. Weatherall, The α thalassaemias, Cellular and Molecular Life Sciences,vol.66,no.7,pp ,2009. [62]C.L.Harteveld,M.Yavarian,A.Zorai,E.D.Quakkelaar,P. van Delft, and P. C. Giordano, Molecular spectrum of αthalassemia in the Iranian population of hormozgan: three novel point mutation defects, The American Journal of Hematology,vol.74,no.2,pp ,2003. [63] K. Zandian, J. Nateghi, B. Keikhaie et al., α-thalassemia mutations in Khuzestan Province, Southwest Iran, Hemoglobin, vol.32,no.6,pp ,2008. [64] F. Hossein, R. Mohsen, M. Mohsen, and M. Taheri, α-thalassemia mutations in two provinces of Southern Iran: Fars & Kohkeloye and Bouyer Ahmad, Hemoglobin, vol. 36,no. 2, pp , [65] A. Tamaddoni, V. Hadavi, N. H. Nejad et al., α-thalassemia mutation analyses in mazandaran province, north iran, Hemoglobin,vol.33,no.2,pp ,2009. [66] V. Hadavi, M. Jafroodi, N. Hafezi-Nejad et al., α-thalassemia mutations in Gilan Province, North Iran, Hemoglobin, vol.33, no. 3-4, pp , [67] N. Saleh-Gohari and A. Khosravi-Mashizi, Spectrum of αglobin gene mutations in the Kerman province of Iran, Hemoglobin,vol.34,no.5,pp ,2010. [68] V.Hadavi,A.H.Taromchi,M.Malekpouretal., Elucidatingthe spectrum of α-thalassemia mutations in Iran, Haematologica, vol.92,no.7,pp ,2007. [69] S. T. Singer, Variable clinical phenotypes of α-thalassemia syndromes, TheScientificWorldJournal,vol.9,pp , [70] S. Zeinali, M. Fallah, and H. Bagherian, Heterogeneity of hemoglobin H disease in childhood, The New England Journal of Medicine, vol. 364, no. 21, pp , [71] A. R. Cohen, R. Galanello, D. J. Pennell, M. J. Cunningham, and E. Vichinsky, Thalassemia, Hematology/American Society of Hematology, Education Program, pp , [72]M.Yavarian,M.Karimi,A.Zorai,C.L.Harteveld,andP.C. Giordano, Molecular basis of Hb H disease in southwest Iran, Hemoglobin,vol.29,no.1,pp.43 50,2005. [73] S. Ebrahimkhani, A. Azarkeivan, N. Bayat et al., Genotypephenotype correlation in Iranian patients with Hb H disease, Hemoglobin,vol.35,no.1,pp.40 46,2011.
10 10 BioMed Research International [74] A. Samavat and B. Modell, Iranian national thalassaemia screening programme, The British Medical Journal, vol. 329, no. 7475, pp , [75]M.Ghanei,P.Adibi,M.Movahedietal., Pre-marriageprevention of thalassaemia: report of a 100,000 case experience in Isfahan, Public Health, vol. 111, no. 3, pp , [76] A. Christianson, A. Streetly, and A. Darr, Lessons from thalassaemia screening in Iran, The British Medical Journal,vol.329, no. 7475, pp , 2004.
11 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Journal of Diabetes Research International Journal of Journal of Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Journal of Obesity Journal of Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Journal of Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
SHORT COMMUNICATION. of Medical Sciences, Isfahan, Iran 2 MRC Molecular Haematology Unit, Weatherall Institute of Molecular Medicine, John
 Hemoglobin, 34(1):115 120, (2010) Copyright Informa UK Ltd. ISSN: 0363-0269 print/1532-432x online DOI: 10.3109/03630260903554894 LHEM 0363-0269 1532-432X Hemoglobin, Vol. 34, No. 1, Dec 2009: pp. 0 0
Hemoglobin, 34(1):115 120, (2010) Copyright Informa UK Ltd. ISSN: 0363-0269 print/1532-432x online DOI: 10.3109/03630260903554894 LHEM 0363-0269 1532-432X Hemoglobin, Vol. 34, No. 1, Dec 2009: pp. 0 0
Review Article Iran J Ped Hematol Oncol. 2016, Vol6.No3, Spectrum of β-thalassemia Mutations in Iran, an Update
 Review Article Iran J Ped Hematol Oncol. 2016, Vol6.No3, 190-202 Spectrum of β-thalassemia Mutations in Iran, an Update Ali Bazi MSc 1, Ebrahim Miri-Moghaddam PhD 2,* 1 Faculty of Allied medical sciences,
Review Article Iran J Ped Hematol Oncol. 2016, Vol6.No3, 190-202 Spectrum of β-thalassemia Mutations in Iran, an Update Ali Bazi MSc 1, Ebrahim Miri-Moghaddam PhD 2,* 1 Faculty of Allied medical sciences,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/35456 holds various files of this Leiden University dissertation. Author: Hassan, Suha Mustafa Title: Toward prevention of Hemoglobinopathies in Oman Issue
Cover Page The handle http://hdl.handle.net/1887/35456 holds various files of this Leiden University dissertation. Author: Hassan, Suha Mustafa Title: Toward prevention of Hemoglobinopathies in Oman Issue
Research Article β-thalassemia Mutations among Transfusion-Dependent Thalassemia Major Patients in Northern Iraq
 SAGE-Hindawi Access to Research Molecular Biology International Volume 2010, Article ID 479282, 4 pages doi:10.4061/2010/479282 Research Article β-thalassemia Mutations among Transfusion-Dependent Thalassemia
SAGE-Hindawi Access to Research Molecular Biology International Volume 2010, Article ID 479282, 4 pages doi:10.4061/2010/479282 Research Article β-thalassemia Mutations among Transfusion-Dependent Thalassemia
Hematologic Features of Alpha Thalassemia Carriers
 IJMCM Summer 2012, Vol 1, No 3 Original Article Hematologic Features of Alpha Thalassemia Carriers Haleh Akhavan-Niaki 1,2, Reza Youssefi Kamangari 2, Ali Banihashemi 2, Vahid Kholghi Oskooei 1, Mandana
IJMCM Summer 2012, Vol 1, No 3 Original Article Hematologic Features of Alpha Thalassemia Carriers Haleh Akhavan-Niaki 1,2, Reza Youssefi Kamangari 2, Ali Banihashemi 2, Vahid Kholghi Oskooei 1, Mandana
Chronic disease program in Iran: Thalassemia control program
 Chronic disease program in Iran: Thalassemia control program Ghobad Moradi 1, Ebrahim Ghaderi 1 1 Assistant Proffesor, Department of Epidemiology and Biostatistics, Kurdistan Research Center for Social
Chronic disease program in Iran: Thalassemia control program Ghobad Moradi 1, Ebrahim Ghaderi 1 1 Assistant Proffesor, Department of Epidemiology and Biostatistics, Kurdistan Research Center for Social
IJHOSCR. A Large Cohort Study of Genotype and Phenotype Correlations of Beta- Thalassemia in Iranian Population. Original Article
 IJHOSCR International Journal of Hematology- Oncology and Stem Cell Research Original Article A Large Cohort Study of Genotype and Phenotype Correlations of Beta- Thalassemia in Iranian Population Fereshteh
IJHOSCR International Journal of Hematology- Oncology and Stem Cell Research Original Article A Large Cohort Study of Genotype and Phenotype Correlations of Beta- Thalassemia in Iranian Population Fereshteh
Level of Hemoglobin F and G g Gene Expression in Sickle Cell Disease and Their Association with Haplotype and XmnI Polymorphic Site in South of Iran
 IJMS Vol 32, No 4, December 2007 Original Article Level of Hemoglobin F and G g Gene Expression in Sickle Cell Disease and Their Association with Haplotype and XmnI Polymorphic Site in South of Iran Z.
IJMS Vol 32, No 4, December 2007 Original Article Level of Hemoglobin F and G g Gene Expression in Sickle Cell Disease and Their Association with Haplotype and XmnI Polymorphic Site in South of Iran Z.
b-globin Gene Cluster Haplotypes in Sickle Cell Patients From Southwest Iran
 American Journal of Hematology 74:156 160 (2003) b-globin Gene Cluster Haplotypes in Sickle Cell Patients From Southwest Iran Z. Rahimi, 1 M. Karimi, 2 M. Haghshenass, 2 and A. Merat 1 * 1 Department of
American Journal of Hematology 74:156 160 (2003) b-globin Gene Cluster Haplotypes in Sickle Cell Patients From Southwest Iran Z. Rahimi, 1 M. Karimi, 2 M. Haghshenass, 2 and A. Merat 1 * 1 Department of
The Spectrum of Mutations in 100 Thalassemic Carriers Referred to Ghaem Hospital of Mashhad
 Original Article The Spectrum of Mutations in 100 Thalassemic Carriers Referred to Ghaem Hospital of Mashhad Hamzehloei T PhD 1, Mohajer Tehran F PhD 1 Downloaded from ijpho.ssu.ac.ir at 15:54 IRDT on
Original Article The Spectrum of Mutations in 100 Thalassemic Carriers Referred to Ghaem Hospital of Mashhad Hamzehloei T PhD 1, Mohajer Tehran F PhD 1 Downloaded from ijpho.ssu.ac.ir at 15:54 IRDT on
The Beats of Natural Sciences Issue 3-4 (September-December) Vol. 3 (2016)
 Frequency of β (Beta Thalassaemia) Trait and Haemaglobin E (HbE) Trait: Case Study in a Thalassaemia Carrier Detection Camp in Gurudas College, West Bengal, India Mitu De Department of Botany, Gurudas
Frequency of β (Beta Thalassaemia) Trait and Haemaglobin E (HbE) Trait: Case Study in a Thalassaemia Carrier Detection Camp in Gurudas College, West Bengal, India Mitu De Department of Botany, Gurudas
Neonatal Screening for Genetic Blood Diseases. Shaikha Al-Arayyed, PhD* A Aziz Hamza, MD** Bema Sultan*** D. K. Shome, MRCPath**** J. P.
 Bahrain Medical Bulletin, Vol. 29, No. 3, September, 2007 Neonatal Screening for Genetic Blood Diseases Shaikha Al-Arayyed, PhD* A Aziz Hamza, MD** Bema Sultan*** D. K. Shome, MRCPath**** J. P. Bapat,PhD****
Bahrain Medical Bulletin, Vol. 29, No. 3, September, 2007 Neonatal Screening for Genetic Blood Diseases Shaikha Al-Arayyed, PhD* A Aziz Hamza, MD** Bema Sultan*** D. K. Shome, MRCPath**** J. P. Bapat,PhD****
Thalassemia in Iran in Last Twenty Years: the Carrier Rates and the Births Trend
 ORIGINAL ARTICLE IJBC 2013;6(1): 11-18 Thalassemia in Iran in Last Twenty Years: the Carrier Rates and the Births Trend Miri M 1, Tabrizi Namini M 1, Hadipour Dehshal M 1 *, Sadeghian Varnosfaderani F
ORIGINAL ARTICLE IJBC 2013;6(1): 11-18 Thalassemia in Iran in Last Twenty Years: the Carrier Rates and the Births Trend Miri M 1, Tabrizi Namini M 1, Hadipour Dehshal M 1 *, Sadeghian Varnosfaderani F
Dr. Ayman Mohsen Mashi, MBBS Consultant Hematology & Blood Transfusion Department Head, Laboratory & Blood Bank King Fahad Central Hospital, Gazan,
 Dr. Ayman Mohsen Mashi, MBBS Consultant Hematology & Blood Transfusion Department Head, Laboratory & Blood Bank King Fahad Central Hospital, Gazan, KSA amashi@moh.gov.sa 24/02/2018 β-thalassemia syndromes
Dr. Ayman Mohsen Mashi, MBBS Consultant Hematology & Blood Transfusion Department Head, Laboratory & Blood Bank King Fahad Central Hospital, Gazan, KSA amashi@moh.gov.sa 24/02/2018 β-thalassemia syndromes
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/346 holds various files of this Leiden University dissertation. Author: Hassan, Suha Mustafa Title: Toward prevention of Hemoglobinopathies in Oman Issue
Cover Page The handle http://hdl.handle.net/1887/346 holds various files of this Leiden University dissertation. Author: Hassan, Suha Mustafa Title: Toward prevention of Hemoglobinopathies in Oman Issue
Beta Thalassemia Frequency in Bahrain: A Ten Year Study. Shaikha Salim Al-Arrayed, MB,ChB, DHCG, PhD*
 Bahrain Medical Bulletin, Vol. 2, No. 2, June 200 Beta Thalassemia Frequency in Bahrain: A Ten Year Study Shaikha Salim Al-Arrayed, MB,ChB, DHCG, PhD* Background: Sickle-cell disease and Thalassanemia
Bahrain Medical Bulletin, Vol. 2, No. 2, June 200 Beta Thalassemia Frequency in Bahrain: A Ten Year Study Shaikha Salim Al-Arrayed, MB,ChB, DHCG, PhD* Background: Sickle-cell disease and Thalassanemia
The pros and cons of the fourth revision of thalassaemia screening programme in Iran
 Original Article The pros and cons of the fourth revision of thalassaemia screening programme in Iran J Med Screen 2017, Vol. 24(1) 1 5! The Author(s) 2016 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Original Article The pros and cons of the fourth revision of thalassaemia screening programme in Iran J Med Screen 2017, Vol. 24(1) 1 5! The Author(s) 2016 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Xmn1-158 γ G Variant in B-Thalassemia Intermediate Patients in South-East of Iran
 IJHOSCR Original Article Xmn1-158 γ G Variant in B-Thalassemia Intermediate Patients in South-East of Iran Ebrahim Miri-Moghaddam 1,2, Sara Bahrami 3, Majid Naderi 4, Ali Bazi 5, Morteza Karimipoor 6 1
IJHOSCR Original Article Xmn1-158 γ G Variant in B-Thalassemia Intermediate Patients in South-East of Iran Ebrahim Miri-Moghaddam 1,2, Sara Bahrami 3, Majid Naderi 4, Ali Bazi 5, Morteza Karimipoor 6 1
Genetic Modulation on the Phenotypic Diversity of Sickle Cell Disease
 Genetic Modulation on the Phenotypic Diversity of Sickle Cell Disease Malay B. Mukherjee Abstract Sickle cell hemoglobin is a β chain structural variant where valine is substituted for glutamic acid in
Genetic Modulation on the Phenotypic Diversity of Sickle Cell Disease Malay B. Mukherjee Abstract Sickle cell hemoglobin is a β chain structural variant where valine is substituted for glutamic acid in
Spectrum of -thalassemia mutations in Qazvin Province, Iran
 African Journal of Biotechnology Vol. x(xx), pp. xxx-xxx, xx xxxxx, 2011 Available online at http://www.academicjournals.org/ajb DOI:xxxxxxxx ISSN 1684 5315 2011 Academic Journals Full Length Research
African Journal of Biotechnology Vol. x(xx), pp. xxx-xxx, xx xxxxx, 2011 Available online at http://www.academicjournals.org/ajb DOI:xxxxxxxx ISSN 1684 5315 2011 Academic Journals Full Length Research
Genetic Modifiers of Sickle Cell Disease Severity. Kunle Adekile, MD, PhD Professor Department of Pediatrics Kuwait University
 Genetic Modifiers of Sickle Cell Disease Severity Kunle Adekile, MD, PhD Professor Department of Pediatrics Kuwait University Outline Hb Molecule and Genetic control of globin synthesis Pathophysiology
Genetic Modifiers of Sickle Cell Disease Severity Kunle Adekile, MD, PhD Professor Department of Pediatrics Kuwait University Outline Hb Molecule and Genetic control of globin synthesis Pathophysiology
Counselling and prenatal diagnosis. Antonis Kattamis, Greece
 Counselling and prenatal diagnosis Antonis Kattamis, Greece Epidemiology of Hemoglobinopathies 7% of world population carriers of hemoglobinopathies 500.000 newborns annually affected 300.000 : Thalassemias
Counselling and prenatal diagnosis Antonis Kattamis, Greece Epidemiology of Hemoglobinopathies 7% of world population carriers of hemoglobinopathies 500.000 newborns annually affected 300.000 : Thalassemias
MOLECULAR BASIS OF THALASSEMIA IN SLOVENIA
 MOLECULAR BASIS OF THALASSEMIA IN SLOVENIA Dijana Plaseska-Karanfilska, MD, PhD Research Centre for Genetic Engineering and Biotechnology Georgi D. Efremov, Macedonian Academy of Sciences and Arts, Skopje,
MOLECULAR BASIS OF THALASSEMIA IN SLOVENIA Dijana Plaseska-Karanfilska, MD, PhD Research Centre for Genetic Engineering and Biotechnology Georgi D. Efremov, Macedonian Academy of Sciences and Arts, Skopje,
Research Article Pattern of β-thalassemia and Other Haemoglobinopathies: A Cross-Sectional Study in Bangladesh
 International Scholarly Research Network ISRN Hematology Volume 2012, Article ID 659191, 6 pages doi:10.5402/2012/659191 Research Article Pattern of β-thalassemia and Other Haemoglobinopathies: A Cross-Sectional
International Scholarly Research Network ISRN Hematology Volume 2012, Article ID 659191, 6 pages doi:10.5402/2012/659191 Research Article Pattern of β-thalassemia and Other Haemoglobinopathies: A Cross-Sectional
The Spectrum of β -thalassemia Mutations in Isfahan Province of Iran
 Iranian J Publ Health, Vol. 37, No.2, 2008, Iranian pp.106-111 J Publ Health, Vol. 37, No.2, 2008, pp.106-111 Short Communication The Spectrum of β -thalassemia Mutations in Isfahan Province of Iran *P
Iranian J Publ Health, Vol. 37, No.2, 2008, Iranian pp.106-111 J Publ Health, Vol. 37, No.2, 2008, pp.106-111 Short Communication The Spectrum of β -thalassemia Mutations in Isfahan Province of Iran *P
Thalassemias. Emanuela Veras, M.D. 01/08/2006
 Thalassemias Emanuela Veras, M.D. 01/08/2006 Structure and Function of normal Hemoglobin molecules: 2/3 1/3 β: increases from 6 th week of fetal life to 12 months of age At birth: HbF: 75-90% HbA: 10-25%
Thalassemias Emanuela Veras, M.D. 01/08/2006 Structure and Function of normal Hemoglobin molecules: 2/3 1/3 β: increases from 6 th week of fetal life to 12 months of age At birth: HbF: 75-90% HbA: 10-25%
Epidemiology, Care and Prevention of Hemoglobinopathies
 Epidemiology, Care and Prevention of Hemoglobinopathies Nasir Al-Allawi MBChB, PhD. Professor of Hematology College of Medicine University of Dohuk, IRAQ From Research to Practice Training Course in Sexual
Epidemiology, Care and Prevention of Hemoglobinopathies Nasir Al-Allawi MBChB, PhD. Professor of Hematology College of Medicine University of Dohuk, IRAQ From Research to Practice Training Course in Sexual
Prevalence of hemoglobin alpha-chain gene deletion in neonates in North of Iran
 European Review for Medical and Pharmacological Sciences Prevalence of hemoglobin alpha-chain gene deletion in neonates in North of Iran M.R. MAHDAVI, M. KOWSARIAN, H. KARAMI, A. MOHSENI, K. VAHIDSHAHI,
European Review for Medical and Pharmacological Sciences Prevalence of hemoglobin alpha-chain gene deletion in neonates in North of Iran M.R. MAHDAVI, M. KOWSARIAN, H. KARAMI, A. MOHSENI, K. VAHIDSHAHI,
Thalassemias:general aspects and molecular pathology
 Thalassemias:general aspects and molecular pathology Prof. Renzo Galanello Pediatric Clinic 2 University of Cagliari Ospedale Regionale Microcitemie-ASL8 HEMOGLOBINOPATHIES CLASSIFICATION Structurally
Thalassemias:general aspects and molecular pathology Prof. Renzo Galanello Pediatric Clinic 2 University of Cagliari Ospedale Regionale Microcitemie-ASL8 HEMOGLOBINOPATHIES CLASSIFICATION Structurally
Report of Beta Thalassemia in Newar Ethnicity
 Report of Beta Thalassemia in Newar Ethnicity Rajendra Dev Bhatt 1*, Surendra Koju 2, Prabodh Risal 1 Affiliations: 1 Department of Clinical Biochemistry, Dhulikhel Hospital, Kathmandu University Hospital
Report of Beta Thalassemia in Newar Ethnicity Rajendra Dev Bhatt 1*, Surendra Koju 2, Prabodh Risal 1 Affiliations: 1 Department of Clinical Biochemistry, Dhulikhel Hospital, Kathmandu University Hospital
Diagnostic difficulties in prevention and control program for thalassemia in Thailand: atypical thalassemia carriers
 Diagnostic difficulties in prevention and control program for thalassemia in Thailand: atypical thalassemia carriers Pranee Winichagoon Fucharoen Thalassemia Research Center Institute of Molecular Biosciences
Diagnostic difficulties in prevention and control program for thalassemia in Thailand: atypical thalassemia carriers Pranee Winichagoon Fucharoen Thalassemia Research Center Institute of Molecular Biosciences
JMSCR Vol 06 Issue 01 Page January 2018
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i1.102 HPLC based evaluation of Haemoglobinopathies
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i1.102 HPLC based evaluation of Haemoglobinopathies
Screening for haemoglobinopathies in pregnancy
 Policy Statement All Southern Health patients will receive clinical care that reflects best practice and is based on the best available evidence. Index of chapters within background 1. Prevalence of haemoglobinopathies
Policy Statement All Southern Health patients will receive clinical care that reflects best practice and is based on the best available evidence. Index of chapters within background 1. Prevalence of haemoglobinopathies
DONE BY : RaSHA RAKAN & Bushra Saleem
 DONE BY : RaSHA RAKAN & Bushra Saleem Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy
DONE BY : RaSHA RAKAN & Bushra Saleem Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy
4 Fahed Al Karmi Sufian Alhafez Dr nayef karadsheh
 4 Fahed Al Karmi Sufian Alhafez Dr nayef karadsheh Genetic variants of hemoglobin Hemoglobinopathies (abnormal variants of hemoglobin) are divided into: 1. Structural abnormalities: Any change in the genes
4 Fahed Al Karmi Sufian Alhafez Dr nayef karadsheh Genetic variants of hemoglobin Hemoglobinopathies (abnormal variants of hemoglobin) are divided into: 1. Structural abnormalities: Any change in the genes
High Hemoglobin F in a Saudi Child Presenting with Pancytopenia
 Case Report imedpub Journals http://www.imedpub.com Journal of Pediatric Care ISSN 2471-805X DOI: 10.21767/2471-805X.100002 High Hemoglobin F in a Saudi Child Presenting with Pancytopenia Abstract Saudi
Case Report imedpub Journals http://www.imedpub.com Journal of Pediatric Care ISSN 2471-805X DOI: 10.21767/2471-805X.100002 High Hemoglobin F in a Saudi Child Presenting with Pancytopenia Abstract Saudi
Quiz. What percentage of the world s population is a carrier of a hemoglobinopathy? Hemoglobinopathies in Pregnancy 1-2% 5-7% 8-12% 10-15%
 Hemoglobinopathies in Pregnancy Emily Parkhurst, MS, LCGC Kaiser West Los Angeles November 2017 Genetics Department Quiz What percentage of the world s population is a carrier of a hemoglobinopathy? 1-2%
Hemoglobinopathies in Pregnancy Emily Parkhurst, MS, LCGC Kaiser West Los Angeles November 2017 Genetics Department Quiz What percentage of the world s population is a carrier of a hemoglobinopathy? 1-2%
6.1 Extended family screening
 CHAPTER 6 CONCLUSION Cost benefit analysis of thalassemia screening programs have shown that the single years treatment for a β-thalassemia major patient was much higher than a total cost per case prevented.
CHAPTER 6 CONCLUSION Cost benefit analysis of thalassemia screening programs have shown that the single years treatment for a β-thalassemia major patient was much higher than a total cost per case prevented.
BRITISH BIOMEDICAL BULLETIN
 Journal Home Page www.bbbulletin.org BRITISH BIOMEDICAL BULLETIN Original A Long Term Screening of Iranian Populations with Thalassemia and Hemoglobinopathies Soudabeh Hosseini 1,2, Ebrahim Kalantar 3,2
Journal Home Page www.bbbulletin.org BRITISH BIOMEDICAL BULLETIN Original A Long Term Screening of Iranian Populations with Thalassemia and Hemoglobinopathies Soudabeh Hosseini 1,2, Ebrahim Kalantar 3,2
Cut off Determination of Discrimination Indices in Differential Diagnosis between Iron Deficiency Anemia and β- Thalassemia Minor
 IJHOSCR International Journal of Hematology- Oncology and Stem Cell Research Original Article Cut off Determination of Discrimination Indices in Differential Diagnosis between Iron Deficiency Anemia and
IJHOSCR International Journal of Hematology- Oncology and Stem Cell Research Original Article Cut off Determination of Discrimination Indices in Differential Diagnosis between Iron Deficiency Anemia and
Case Report Iron Depletion: An Ameliorating Factor for Sickle Cell Disease?
 International Scholarly Research Network ISRN Hematology Volume 2011, Article ID 473152, 4 pages doi:10.5402/2011/473152 Case Report Iron Depletion: An Ameliorating Factor for Sickle Cell Disease? P. C.
International Scholarly Research Network ISRN Hematology Volume 2011, Article ID 473152, 4 pages doi:10.5402/2011/473152 Case Report Iron Depletion: An Ameliorating Factor for Sickle Cell Disease? P. C.
Comprehensive Hemoglobin Analysis HBA1/2 (
 Comprehensive Hemoglobin Analysis HBA1/2 ( α-globin) and HBB (β-globin) mutation and deletion/duplication analysis and HBD (δ-globin) and HBG1/2 (γ-globin) mutation analysis Description: Hemoglobin (Hb)
Comprehensive Hemoglobin Analysis HBA1/2 ( α-globin) and HBB (β-globin) mutation and deletion/duplication analysis and HBD (δ-globin) and HBG1/2 (γ-globin) mutation analysis Description: Hemoglobin (Hb)
Prenatal diagnosis of different polymorphisms of β-globin gene in Ahvaz
 .Original rticle Prenatal diagnosis of different polymorphisms of β-globin gene in hvaz li Dehghanifard 1, Mohammad Shahjahani 2, Hamid Galehdari 3, Fakher Rahim 4, Fatemeh Hamid 5, Kaveh Jaseb 5, li min
.Original rticle Prenatal diagnosis of different polymorphisms of β-globin gene in hvaz li Dehghanifard 1, Mohammad Shahjahani 2, Hamid Galehdari 3, Fakher Rahim 4, Fatemeh Hamid 5, Kaveh Jaseb 5, li min
Proposed low-cost premarital screening program for prevention of sickle cell and thalassemia in Yemen Hafiz Al-Nood 1 Abdulrahman Al-Hadi 2
 RESEARCH PAPER Proposed low-cost premarital screening program for prevention of sickle cell and thalassemia in Yemen Hafiz Al-Nood 1 Abdulrahman Al-Hadi 2 ABSTRACT Address for Correspondence: Hafiz Al-Nood
RESEARCH PAPER Proposed low-cost premarital screening program for prevention of sickle cell and thalassemia in Yemen Hafiz Al-Nood 1 Abdulrahman Al-Hadi 2 ABSTRACT Address for Correspondence: Hafiz Al-Nood
Anemia s. Troy Lund MSMS PhD MD
 Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Hemoglobinopathies Diagnosis and management
 Hemoglobinopathies Diagnosis and management Morgan L. McLemore, M.D. Hematology/Leukemia Department of Hematology and Oncology Winship Cancer Institute at Emory University mlmclem@emory.edu Disclosures
Hemoglobinopathies Diagnosis and management Morgan L. McLemore, M.D. Hematology/Leukemia Department of Hematology and Oncology Winship Cancer Institute at Emory University mlmclem@emory.edu Disclosures
Research Article Clinical Features and Molecular Analysis of Hb H Disease in Taiwan
 BioMed Research International, Article ID 271070, 5 pages http://dx.doi.org/10.1155/2014/271070 Research Article Clinical Features and Molecular Analysis of Hb H Disease in Taiwan Yu-Hua Chao, 1,2,3 Kang-Hsi
BioMed Research International, Article ID 271070, 5 pages http://dx.doi.org/10.1155/2014/271070 Research Article Clinical Features and Molecular Analysis of Hb H Disease in Taiwan Yu-Hua Chao, 1,2,3 Kang-Hsi
Hemolytic anemias (2 of 2)
 Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Educational Items Section
 Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL AT INIST-CNRS Educational Items Section Hemoglobin genes; Sickle-cell anemia - Thalassemias Jean-Loup Huret, Xavier Troussard
Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL AT INIST-CNRS Educational Items Section Hemoglobin genes; Sickle-cell anemia - Thalassemias Jean-Loup Huret, Xavier Troussard
Original Paper. Inherited Haemoglobin Disorders Among Apparently Healthy Individuals- An Analysis of 105 Cases. Abstract
 Original Paper Inherited Haemoglobin Disorders Among Apparently Healthy Individuals- An Analysis of 105 Cases Salsabil MA 1, Islam M 2, Jahan D 3, Khan MA 4 Abstract Introduction: Inherited hemoglobin
Original Paper Inherited Haemoglobin Disorders Among Apparently Healthy Individuals- An Analysis of 105 Cases Salsabil MA 1, Islam M 2, Jahan D 3, Khan MA 4 Abstract Introduction: Inherited hemoglobin
Haemoglobin BY: MUHAMMAD RADWAN WISSAM MUHAMMAD
 Haemoglobin BY: MUHAMMAD RADWAN WISSAM MUHAMMAD Introduction is the iron-containing oxygen transport metalloprotein in the red blood cells Hemoglobin in the blood carries oxygen from the respiratory organs
Haemoglobin BY: MUHAMMAD RADWAN WISSAM MUHAMMAD Introduction is the iron-containing oxygen transport metalloprotein in the red blood cells Hemoglobin in the blood carries oxygen from the respiratory organs
The Prevalence of Mediterranean Mutation of Glucose-6-Phosphate Dehydrogenase (G6PD) in Zahedan
 Zahedan Journal of Research in Medical Sciences Journal homepage: www.zjrms.ir The Prevalence of Mediterranean Mutation of Glucose-6-Phosphate Dehydrogenase (G6PD) in Zahedan Alireza Nakhaee,* 1 Saeedeh
Zahedan Journal of Research in Medical Sciences Journal homepage: www.zjrms.ir The Prevalence of Mediterranean Mutation of Glucose-6-Phosphate Dehydrogenase (G6PD) in Zahedan Alireza Nakhaee,* 1 Saeedeh
Genetics of Thalassemia
 Genetics of Thalassemia Submitted by : Raya Samir Al- Hayaly Sura Zuhair Salih Saad Ghassan Al- Dulaimy Saad Farouq Kassir Sama Naal Salouha Zahraa Jasim Al- Aarajy Supervised by : Dr. Kawkab Adris Mahmod
Genetics of Thalassemia Submitted by : Raya Samir Al- Hayaly Sura Zuhair Salih Saad Ghassan Al- Dulaimy Saad Farouq Kassir Sama Naal Salouha Zahraa Jasim Al- Aarajy Supervised by : Dr. Kawkab Adris Mahmod
Prevalence of Thalassemia in Patients With Microcytosis Referred for Hemoglobinopathy Investigation in Ontario A Prospective Cohort Study
 Hematopathology / PREVALENCE OF THALASSEMIA IN ONTARIO Prevalence of Thalassemia in Patients With Microcytosis Referred for Hemoglobinopathy Investigation in Ontario A Prospective Cohort Study John D.
Hematopathology / PREVALENCE OF THALASSEMIA IN ONTARIO Prevalence of Thalassemia in Patients With Microcytosis Referred for Hemoglobinopathy Investigation in Ontario A Prospective Cohort Study John D.
SICKLE CELL DISEASE. Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH. Assistant Professor FACULTY OF MEDICINE -JAZAN
 SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
Research Article Profiling β Thalassemia Mutations in Consanguinity and Nonconsanguinity for Prenatal Screening and Awareness Programme
 Advances in Hematology Volume 2015, Article ID 625721, 5 pages http://dx.doi.org/10.1155/2015/625721 Research Article Profiling β Thalassemia Mutations in Consanguinity and Nonconsanguinity for Prenatal
Advances in Hematology Volume 2015, Article ID 625721, 5 pages http://dx.doi.org/10.1155/2015/625721 Research Article Profiling β Thalassemia Mutations in Consanguinity and Nonconsanguinity for Prenatal
Evaluation of hemoglobinopathy screening results of a six year period in Turkey
 Evaluation of hemoglobinopathy screening results of a six year period in Turkey Seçil Gunher Arıca, Ebru Turhan, Cahit Özer, Vefik Arıca, Dilek Benk Şilfeler, Đbrahim Şilfeler, Ayşe Betül Altun Vol. 4
Evaluation of hemoglobinopathy screening results of a six year period in Turkey Seçil Gunher Arıca, Ebru Turhan, Cahit Özer, Vefik Arıca, Dilek Benk Şilfeler, Đbrahim Şilfeler, Ayşe Betül Altun Vol. 4
Premarital Screening of Beta Thalassemia Minor in north-east of Iran
 Original Article Premarital Screening of Beta Thalassemia Minor in north-east of Iran Hashemizadeh H MSc 1, Noori R MSc 2 1. Department of Nursing, Quchan Branch, Islamic Azad University, Quchan, Iran.
Original Article Premarital Screening of Beta Thalassemia Minor in north-east of Iran Hashemizadeh H MSc 1, Noori R MSc 2 1. Department of Nursing, Quchan Branch, Islamic Azad University, Quchan, Iran.
Corporate Medical Policy
 Corporate Medical Policy Genetic Testing for Alpha Thalassemia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_alpha_thalassemia 9/2013 7/2017 7/2018 7/2017 Description
Corporate Medical Policy Genetic Testing for Alpha Thalassemia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_alpha_thalassemia 9/2013 7/2017 7/2018 7/2017 Description
In adults, the predominant Hb (HbA) molecule has four chains: two α and two β chains. In thalassemias, the synthesis of either the α or the β chains
 Thalassaemias Thalassemia Thalassemia is an inherited autosomal recessive blood disease. Associated with absence or reduction in a or b globin chains. Reduced synthesis of one of the globin chains can
Thalassaemias Thalassemia Thalassemia is an inherited autosomal recessive blood disease. Associated with absence or reduction in a or b globin chains. Reduced synthesis of one of the globin chains can
Fourteen-Year Experience of Prenatal Diagnosis of Thalassemia in Iran
 Original Paper Community Genet 2006;9:93 97 DOI: 10.1159/000091486 Fourteen-Year Experience of Prenatal Diagnosis of Thalassemia in Iran a, b b a Hossein Najmabadi Alireza Ghamari Farhad Sahebjam a a a
Original Paper Community Genet 2006;9:93 97 DOI: 10.1159/000091486 Fourteen-Year Experience of Prenatal Diagnosis of Thalassemia in Iran a, b b a Hossein Najmabadi Alireza Ghamari Farhad Sahebjam a a a
The Challenging Diagnosis of Treacherous Hemoglobinopathies
 The Challenging Diagnosis of Treacherous Hemoglobinopathies David F. Keren, M.D. Professor of Pathology The University of Michigan dkeren@med.umich.edu Objectives Use Capillary Electrophoresis and HPLC
The Challenging Diagnosis of Treacherous Hemoglobinopathies David F. Keren, M.D. Professor of Pathology The University of Michigan dkeren@med.umich.edu Objectives Use Capillary Electrophoresis and HPLC
Thalassaemia and other haemoglobinopathies
 EXECUTIVE BOARD EB118/5 118th Session 11 May 2006 Provisional agenda item 5.2 Thalassaemia and other haemoglobinopathies Report by the Secretariat PREVALENCE OF HAEMOGLOBINOPATHIES 1. Haemoglobinopathies,
EXECUTIVE BOARD EB118/5 118th Session 11 May 2006 Provisional agenda item 5.2 Thalassaemia and other haemoglobinopathies Report by the Secretariat PREVALENCE OF HAEMOGLOBINOPATHIES 1. Haemoglobinopathies,
Evaluation of the Molecular basis of KLF1 Gene in Iranian Thalassemia individuals with borderline hemoglobin A2
 Advances in Bioresearch Adv. Biores., Vol 7 (5) September 2016: 11-15 2016 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
Advances in Bioresearch Adv. Biores., Vol 7 (5) September 2016: 11-15 2016 Society of Education, India Print ISSN 0976-4585; Online ISSN 2277-1573 Journal s URL:http://www.soeagra.com/abr.html CODEN: ABRDC3
HEMOLYTIC ANEMIA DUE TO ABNORMAL HEMOGLOBIN SYNTHESIS
 Hemolytic Anemia Due to Abnormal Hemoglobin Synthesis MODULE 19 HEMOLYTIC ANEMIA DUE TO ABNORMAL HEMOGLOBIN SYNTHESIS 19.1 INTRODUCTION There are two main mechanisms by which anaemia is produced (a) Thalassemia:
Hemolytic Anemia Due to Abnormal Hemoglobin Synthesis MODULE 19 HEMOLYTIC ANEMIA DUE TO ABNORMAL HEMOGLOBIN SYNTHESIS 19.1 INTRODUCTION There are two main mechanisms by which anaemia is produced (a) Thalassemia:
George R. Honig Junius G. Adams III. Human Hemoglobin. Genetics. Springer-Verlag Wien New York
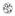 George R. Honig Junius G. Adams III Human Hemoglobin Genetics Springer-Verlag Wien New York George R. Honig, M.D., Ph.D. Professor and Head Department of Pediatrics, College of Medicine University of Illinois
George R. Honig Junius G. Adams III Human Hemoglobin Genetics Springer-Verlag Wien New York George R. Honig, M.D., Ph.D. Professor and Head Department of Pediatrics, College of Medicine University of Illinois
Journal of Medical Science & Technology
 Page82 Original Article Journal of Medical Science & Technology Open Access Screening for hemoglobinopathies among patients in a government hospital and health clinics in Perlis, Malaysia Chin Yuet Meng
Page82 Original Article Journal of Medical Science & Technology Open Access Screening for hemoglobinopathies among patients in a government hospital and health clinics in Perlis, Malaysia Chin Yuet Meng
The Distribution of Human Differences. If all this genetic variation is so recent and continuous, why do we think of it in categorical terms?
 Expansion Routes of Homo sapiens ~40-25,000 b.p. The Distribution of Human Differences ~120-100,000 b.p. ~50-40,000 b.p. ~20-15,000 b.p. - - - Coastal Route Circa 10-3,500 b.p. If all this genetic variation
Expansion Routes of Homo sapiens ~40-25,000 b.p. The Distribution of Human Differences ~120-100,000 b.p. ~50-40,000 b.p. ~20-15,000 b.p. - - - Coastal Route Circa 10-3,500 b.p. If all this genetic variation
Below are the sections of the DNA sequences of a normal hemoglobin gene and the mutated gene that causes sickle cell disease.
 Sickle Cell Analysis Directions: Read the information below to complete the two tables. A person with sickle-cell disease has the genotype: Hb s Hb s. People who have this condition have two abnormal genes,
Sickle Cell Analysis Directions: Read the information below to complete the two tables. A person with sickle-cell disease has the genotype: Hb s Hb s. People who have this condition have two abnormal genes,
db-thalassemia Patients With Homozygous Xmn-1 Polymorphism That Are Characterized By A Milder Phenotype
 ISPUB.COM The Internet Journal of Hematology Volume 7 Number 2 db-thalassemia Patients With Homozygous Xmn-1 Polymorphism That Are Characterized By A Milder S Ashraf Citation S Ashraf. db-thalassemia Patients
ISPUB.COM The Internet Journal of Hematology Volume 7 Number 2 db-thalassemia Patients With Homozygous Xmn-1 Polymorphism That Are Characterized By A Milder S Ashraf Citation S Ashraf. db-thalassemia Patients
An economic review of the national screening policy to prevent thalassemia major in Iran
 Discussion Paper No.562 An economic review of the national screening policy to prevent thalassemia major in Iran Ghotbi N., Tsukatani T. December 2002 Kyoto Institute of Economic Research Kyoto University
Discussion Paper No.562 An economic review of the national screening policy to prevent thalassemia major in Iran Ghotbi N., Tsukatani T. December 2002 Kyoto Institute of Economic Research Kyoto University
Molecular Basis of α-thalassemia in Iran
 REVIEW ARTICLE Iranian Biomedical Journal 22(1): 6-14 January 2018 Molecular Basis of α-thalassemia in Iran Atefeh Valaei 1, Morteza Karimipoor *1, Alireza Kordafshari 1 and Sirous Zeinali *1,2 1 Department
REVIEW ARTICLE Iranian Biomedical Journal 22(1): 6-14 January 2018 Molecular Basis of α-thalassemia in Iran Atefeh Valaei 1, Morteza Karimipoor *1, Alireza Kordafshari 1 and Sirous Zeinali *1,2 1 Department
Unraveling Hemoglobinopathies with Capillary Electrophoresis
 Session Number 2002 Unraveling Hemoglobinopathies with Capillary Electrophoresis David F. Keren, M.D. Professor of Pathology Division Director, Clinical Pathology The University of Michigan dkeren@med.umich.edu
Session Number 2002 Unraveling Hemoglobinopathies with Capillary Electrophoresis David F. Keren, M.D. Professor of Pathology Division Director, Clinical Pathology The University of Michigan dkeren@med.umich.edu
The Distribution of Human Differences. If all this genetic variation is so recent and continuous, why do we think of it in categorical terms?
 Expansion Routes of Homo sapiens ~40-25,000 b.p. The Distribution of Human Differences ~120-100,000 b.p. ~50-40,000 b.p. ~20-15,000 b.p. - - - Coastal Route Circa 10-3,500 b.p. If all this genetic variation
Expansion Routes of Homo sapiens ~40-25,000 b.p. The Distribution of Human Differences ~120-100,000 b.p. ~50-40,000 b.p. ~20-15,000 b.p. - - - Coastal Route Circa 10-3,500 b.p. If all this genetic variation
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/188/35456 holds various files of this Leiden University dissertation. Author: Hassan, Suha Mustafa Title: Toward prevention of Hemoglobinopathies in Oman Issue
Cover Page The handle http://hdl.handle.net/188/35456 holds various files of this Leiden University dissertation. Author: Hassan, Suha Mustafa Title: Toward prevention of Hemoglobinopathies in Oman Issue
Line Probe Assay for Detection of Alpha Thalassemia: A Pilot Study
 Line Probe Assay for Detection of Alpha Thalassemia: A Pilot Study Menon PK *, Nimmakayalu M, Bylappa SK, Kumar M, Abdalhaleem HM Center for Advanced Biomedical Research and Innovation, Gulf Medical University,
Line Probe Assay for Detection of Alpha Thalassemia: A Pilot Study Menon PK *, Nimmakayalu M, Bylappa SK, Kumar M, Abdalhaleem HM Center for Advanced Biomedical Research and Innovation, Gulf Medical University,
Thalassemia is one of the most common genetic
 ORIGINAL ARTICLE Thalassemia in Iran Epidemiology, Prevention, and Management Hassan Abolghasemi, MD,*w Ali Amid, MD,* Sirous Zeinali, PhD,z Mohammad H. Radfar, MD,* Peyman Eshghi, MD,*y Mohammad S. Rahiminejad,
ORIGINAL ARTICLE Thalassemia in Iran Epidemiology, Prevention, and Management Hassan Abolghasemi, MD,*w Ali Amid, MD,* Sirous Zeinali, PhD,z Mohammad H. Radfar, MD,* Peyman Eshghi, MD,*y Mohammad S. Rahiminejad,
Gamma gene expression in haemoglobin disorders
 Gamma gene expression in haemoglobin disorders Innovative therapies for Red Cell and Iron related disorders EHA / ESH : April 16-18, Cascais, Portugal Swee Lay Thein King s College London School of Medicine
Gamma gene expression in haemoglobin disorders Innovative therapies for Red Cell and Iron related disorders EHA / ESH : April 16-18, Cascais, Portugal Swee Lay Thein King s College London School of Medicine
The diagnosis of Hemoglobinopathies
 1ST IFCC, EFLM, AFCB CONFERENCE "LABORATORY MEDICINE: MEETING THE NEEDS OF MEDITERRANEAN NATIONS" Rome, Italy 02/07/2018 The diagnosis of Hemoglobinopathies Dr Antonino Giambona Unit of Hematology of Rare
1ST IFCC, EFLM, AFCB CONFERENCE "LABORATORY MEDICINE: MEETING THE NEEDS OF MEDITERRANEAN NATIONS" Rome, Italy 02/07/2018 The diagnosis of Hemoglobinopathies Dr Antonino Giambona Unit of Hematology of Rare
Carrying Beta Thalassaemia A carrier can use this booklet to
 Carrying Beta Thalassaemia A carrier can use this booklet to help explain carrying beta to their partner, blood relatives and others. show to any health professional (doctor, nurse or midwife) they see
Carrying Beta Thalassaemia A carrier can use this booklet to help explain carrying beta to their partner, blood relatives and others. show to any health professional (doctor, nurse or midwife) they see
Human Genetic Diseases. AP Biology
 Human Genetic Diseases 1 2 2006-2007 3 4 5 6 Pedigree analysis Pedigree analysis reveals Mendelian patterns in human inheritance data mapped on a family tree = male = female = male w/ trait = female w/
Human Genetic Diseases 1 2 2006-2007 3 4 5 6 Pedigree analysis Pedigree analysis reveals Mendelian patterns in human inheritance data mapped on a family tree = male = female = male w/ trait = female w/
HAEMOGLOBINOPATHIES. Editing file. References: 436 girls & boys slides 435 teamwork slides. Color code: Important. Extra.
 HAEMOGLOBINOPATHIES Objectives: normal structure and function of haemoglobin. how the globin components of haemoglobin change during development, and postnatally. the mechanisms by which the thalassaemias
HAEMOGLOBINOPATHIES Objectives: normal structure and function of haemoglobin. how the globin components of haemoglobin change during development, and postnatally. the mechanisms by which the thalassaemias
THALASSEMIA AND COMPREHENSIVE CARE
 1 THALASSEMIA AND COMPREHENSIVE CARE Melanie Kirby MBBS, FRCP (C), Hospital for Sick Children, Toronto Associate Professor of Paediatrics, University of Toronto. Objectives 2 By the end of this presentation,
1 THALASSEMIA AND COMPREHENSIVE CARE Melanie Kirby MBBS, FRCP (C), Hospital for Sick Children, Toronto Associate Professor of Paediatrics, University of Toronto. Objectives 2 By the end of this presentation,
4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour
 4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour Anemia Decreased blood production Increased blood loss Hemolytic Hemorrhage Extravascular Intravascular Hemolytic (Further classification( Extrinsic Intrinsic
4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour Anemia Decreased blood production Increased blood loss Hemolytic Hemorrhage Extravascular Intravascular Hemolytic (Further classification( Extrinsic Intrinsic
The Making of the Fittest: Natural Selection in Humans
 INTRODUCTION MENDELIAN GENETICS, PROBABILITY, PEDIGREES, AND CHI-SQUARE STATISTICS Hemoglobin is a protein found in red blood cells (RBCs) that transports oxygen throughout the body. The hemoglobin protein
INTRODUCTION MENDELIAN GENETICS, PROBABILITY, PEDIGREES, AND CHI-SQUARE STATISTICS Hemoglobin is a protein found in red blood cells (RBCs) that transports oxygen throughout the body. The hemoglobin protein
Research Article Hb A1c Separation by High Performance Liquid Chromatography in Hemoglobinopathies
 Scientifica Volume 2016, Article ID 2698362, 4 pages http://dx.doi.org/10.1155/2016/2698362 Research Article Hb A1c Separation by High Performance Liquid Chromatography in Hemoglobinopathies Vani Chandrashekar
Scientifica Volume 2016, Article ID 2698362, 4 pages http://dx.doi.org/10.1155/2016/2698362 Research Article Hb A1c Separation by High Performance Liquid Chromatography in Hemoglobinopathies Vani Chandrashekar
Utility of hemoglobin electrophoresis to detect hemoglobinopathies in adults not presenting with hematological problems
 Original Research Article Utility of hemoglobin electrophoresis to detect hemoglobinopathies in adults not presenting with hematological problems G. J. Vani Padmaja 1*, S. S. S. Quadri 1, O. Shravan Kumar
Original Research Article Utility of hemoglobin electrophoresis to detect hemoglobinopathies in adults not presenting with hematological problems G. J. Vani Padmaja 1*, S. S. S. Quadri 1, O. Shravan Kumar
Thalassemia Maria Luz Uy del Rosario, M.D.
 Thalassemia Maria Luz Uy del Rosario, M.D. Philippine Society of Hematology and Blood Transfusion Philippine Society of Pediatric Oncology What is Thalassemia Hereditary Hemoglobin disorder Hemolytic anemia
Thalassemia Maria Luz Uy del Rosario, M.D. Philippine Society of Hematology and Blood Transfusion Philippine Society of Pediatric Oncology What is Thalassemia Hereditary Hemoglobin disorder Hemolytic anemia
Chem*3560 Lecture 4: Inherited modifications in hemoglobin
 Chem*3560 Lecture 4: Inherited modifications in hemoglobin Genetic modifications fall into two classes: Thalassemias, which are the result of failure to express globin genes. Thalassa is Greek for the
Chem*3560 Lecture 4: Inherited modifications in hemoglobin Genetic modifications fall into two classes: Thalassemias, which are the result of failure to express globin genes. Thalassa is Greek for the
Natural Selection In Humans (Sickle Cell Anemia)
 Natural Selection In Humans (Sickle Cell Anemia) Background Information Hemoglobin is a protein found in red blood cells Transports oxygen to body tissues Individuals homozygous for the sickle cell allele
Natural Selection In Humans (Sickle Cell Anemia) Background Information Hemoglobin is a protein found in red blood cells Transports oxygen to body tissues Individuals homozygous for the sickle cell allele
Genetic Testing for α-thalassemia
 Medical Policy Manual Genetic Testing, Policy No. 52 Genetic Testing for α-thalassemia Next Review: January 2019 Last Review: January 2018 Effective: February 1, 2018 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Genetic Testing, Policy No. 52 Genetic Testing for α-thalassemia Next Review: January 2019 Last Review: January 2018 Effective: February 1, 2018 IMPORTANT REMINDER Medical Policies
7.03 Lecture 26 11/14/01
 Now we are going to consider how allele frequencies change under the influence of mutation and. First, we will consider mutation. Mutation A µ a µ = q mut = Phenylketonuria (PKU) allele frequency q 0.1
Now we are going to consider how allele frequencies change under the influence of mutation and. First, we will consider mutation. Mutation A µ a µ = q mut = Phenylketonuria (PKU) allele frequency q 0.1
Genetic Diversity of 3-thalassemia Mutations in Pakistani Population
 Genetic Diversity of 3-thalassemia Mutations in Pakistani Population Bushra Khateeb,Tariq Moatter,Asim M. Shaghil,Sarwat Haroon,Ghulam N. Kakepoto ( Department of Pathology, The Aga Khan University Hospital,
Genetic Diversity of 3-thalassemia Mutations in Pakistani Population Bushra Khateeb,Tariq Moatter,Asim M. Shaghil,Sarwat Haroon,Ghulam N. Kakepoto ( Department of Pathology, The Aga Khan University Hospital,
Epidemiological Study among Thalassemia Intermedia Pediatric Patients
 Med. J. Cairo Univ., Vol. 78, No. 2, December 651-655, 2010 www.medicaljournalofcairouniversity.com Epidemiological Study among Thalassemia Intermedia Pediatric Patients NERMEEN KADDAH, M.D.; KHALED SALAMA,
Med. J. Cairo Univ., Vol. 78, No. 2, December 651-655, 2010 www.medicaljournalofcairouniversity.com Epidemiological Study among Thalassemia Intermedia Pediatric Patients NERMEEN KADDAH, M.D.; KHALED SALAMA,
We are IntechOpen, the first native scientific publisher of Open Access books. International authors and editors. Our authors are among the TOP 1%
 We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
We are IntechOpen, the first native scientific publisher of Open Access books 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our authors are among the 151 Countries
Research Article Prevalence of Deletional Alpha Thalassemia and Sickle Gene in a Tribal Dominated Malaria Endemic Area of Eastern India
 ISRN Hematology, Article ID 745245, 6 pages http://dx.doi.org/10.1155/2014/745245 Research Article Prevalence of Deletional Alpha Thalassemia and Sickle Gene in a Tribal Dominated Malaria Endemic Area
ISRN Hematology, Article ID 745245, 6 pages http://dx.doi.org/10.1155/2014/745245 Research Article Prevalence of Deletional Alpha Thalassemia and Sickle Gene in a Tribal Dominated Malaria Endemic Area
Haemoglobinopathy Case Studies. Dr Jill Finlayson Department of Haematology Pathwest Laboratory Medicine
 Haemoglobinopathy Case Studies Dr Jill Finlayson Department of Haematology Pathwest Laboratory Medicine Case 1 KB, 36y M Refugee Afghanistan Screening bloods Hb 101 g/l RCC 3.75 x10 12 /L MCV 90 fl MCH
Haemoglobinopathy Case Studies Dr Jill Finlayson Department of Haematology Pathwest Laboratory Medicine Case 1 KB, 36y M Refugee Afghanistan Screening bloods Hb 101 g/l RCC 3.75 x10 12 /L MCV 90 fl MCH
GENETIC FACTORS INFLUENCING HEMOGLOBIN
 Southeast Asian J Trop Med Public Health GENETIC FACTORS INFLUENCING HEMOGLOBIN F LEVEL IN β-thalassemia/hb E DISEASE Waraporn Ruangrai and Sumalee Jindadamrongwech Department of Pathology, Faculty of
Southeast Asian J Trop Med Public Health GENETIC FACTORS INFLUENCING HEMOGLOBIN F LEVEL IN β-thalassemia/hb E DISEASE Waraporn Ruangrai and Sumalee Jindadamrongwech Department of Pathology, Faculty of
Research Article Decreasing Prevalence of Transfusion Transmitted Infection in Indian Scenario
 e Scientific World Journal, Article ID 173939, 4 pages http://dx.doi.org/10.1155/2014/173939 Research Article Decreasing Prevalence of Transfusion Transmitted Infection in Indian Scenario Tulika Chandra,
e Scientific World Journal, Article ID 173939, 4 pages http://dx.doi.org/10.1155/2014/173939 Research Article Decreasing Prevalence of Transfusion Transmitted Infection in Indian Scenario Tulika Chandra,
Clinical Characteristics of Pediatric Thalassemia in Korea: A Single Institute Experience
 ORIGINAL ARTICLE Pediatrics http://dx.doi.org/10.3346/jkms.2013.28.11.1645 J Korean Med Sci 2013; 28: 1645-1649 Clinical Characteristics of Pediatric Thalassemia in Korea: A Single Institute Experience
ORIGINAL ARTICLE Pediatrics http://dx.doi.org/10.3346/jkms.2013.28.11.1645 J Korean Med Sci 2013; 28: 1645-1649 Clinical Characteristics of Pediatric Thalassemia in Korea: A Single Institute Experience
