Laparoscopic Uterine Conservation in Uterovaginal Prolapse
|
|
|
- Dortha Douglas
- 5 years ago
- Views:
Transcription
1 SMGr up Laparoscopic Uterine Conservation in Uterovaginal Prolapse Hasan Cilgin Medicine Faculty of Kafkas University, Kars, Turkey *Corresponding author: Hasan Cilgin, Medicine Faculty of Kafkas University, Kars, Turkey, Tel: ; Published Date: November 03, 2017 ABSTRACT Objective: To evaluate outcomes and patient satisfaction in cases of uterine prolapse treated with laparoscopic hysteropexy while preserving the uterus in premenopausal cases. Materials and Methods: This is a retrospective cohort study that included all patients operated for prolapse by laparoscopic repair method while preserving the uterus between January 2011 and April Data included: patients pre-and post-operative symptoms, POP-Q and operative complications, post-operative pregnancy rate. Patients operated for prolapse were called by phone between April and July 2017 and control examinations were performed. The face-to-face survey method was used to assess the patient s satisfaction. Success was defined as prolapse below than stage 2, healing in preoperative symptoms and sexual relationship, postoperative pregnancy rate. Results: Fifty-two patients with pelvic organ prolapse stage 2-3 were included. Mean followup was 30 months. Success rate of the laparoscopic procedure aimed to repair uterine prolapse was 88,4% (46/52), with mean point C at -6 (range (-1) - (-9)). As a major intra operative complication a bowel injury as a major intra operative complication was occurred. The faceto-face questionnaire was conducted post-operatively 28 months on average. Conditions with 1
2 negative effects on quality of life, such as urinary, bowel and sexual functions, physical discomfort, psychological problems and embarrassment were evaluated. Ninety four percent of women were satisfied with the decision to preserve their uterus. Eighteen patients (34,6%) received prior consultation elsewhere for hysterectomy due to their prolapse, and decided to have the operation at our center in order to preserve the uterus. Conclusions: Uterine preservation applies from whichever way found to be a safe and effective treatment, even in cases with advanced uterine prolapse particularly desiring pregnancy. Most patients prefer to keep their uterus. Uterus preservation options should be discussed with every premenopausal and sexually active patient before surgery for pelvic organ prolapse. Keywords: Hysteropexy; Laparoscopy; Pelvic organ prolapsed; Uterine conservation; Uterovaginal prolapsed INTRODUCTION Pelvic organ prolapse (POP) is a definition of anatomical change. Some such changes may well be considered within the range of normality for certain women. A diagnosis of POP ideally demands clear clinical evidence, starting with a woman having symptoms related to the downward displacement of a pelvic organ [1]. POP has significant negative impact on the quality of life, including physical discomfort, sexual and psychological problems and embarrassment. The estimated prevalence of any degree of genital prolapse in women between 20 and 59 years is about 30% [2]. The lifetime risk of undergoing surgery for pelvic organ prolapse is estimated to be about 11% and around 30% will undergo repeat surgery for a recurrence of the prolapse [3]. The goals of surgery for POP include restoration of normal anatomy, to maintain or restore urinary, bowel and sexual functions and to improve quality of life. The traditional treatment for uterine prolapse has been the vaginal hysterectomy, even in the absence of uterine disease. Hysterectomy alone does not address the deficiencies in pelvic support and does not correct the underlying pathophysiology, hence the higher incidence of recurrence and vault prolapse [4,5]. Hysterectomy also leads to unnecessary removal of a healthy organ with associated increased morbidity, blood loss and operating time [6,7]. Uterine conservation is important for women who wish to preserve fertility and is seemingly associated with improvements in sexuality, confidence and self-esteem of women [8]. Women may also request preservation of the uterus due to personal beliefs or to retain a sense of identity [9], hence recently there has been much interest in preserving the uterus during prolapse surgery [10] and an increasing number of women are requesting uterine conservation [11]. Compared with hysterectomy and prolapse repair, hysteropexy is associated with a shorter operative time, less blood loss, and a faster return to work. Other advantages include maintenance of fertility, natural timing of menopause, and patient preference. Disadvantages include the lack of long-term prolapse repair outcomes and the need to continue surveillance for gynecological cancers [12]. Vaginal, abdominal, laparoscopic, 2
3 and robotic methods are defined in uterine preserving surgery but there is not yet a consensus on which of them should be chosen. In choosing the proper technique, the patient s general status, accompanying disease, correct indication, and the surgeon s experience are all important. The most studied approaches to hysteropexy are the vaginal sacrospinous ligament hysteropexy and the abdominal sacrohysteropexy, which have similar objective and subjective prolapse outcomes compared with hysterectomy and apical suspension. The advantages of the laparoscopic approach include reduced blood loss, decreased postoperative pain, lower rate of wound complications, decreased hospital stay and fewer adhesion formation, which is particularly beneficial to women wishing to preserve fertility [13,14]. Ureteric injury is also minimal compared to the vaginal approach, due to direct visualization of the ureters [15]. The laparoscopic approach also minimizes the possibility of contamination, if mesh is used and also induces less postoperative vaginal fibrosis [16]. Disadvantages of laparoscopic surgery include a steep learning curve and longer operating times. Pregnancy and delivery have been documented after vaginal and abdominal hysteropexy approaches, although very little is known about outcomes following parturition. It is unknown whether simultaneous hysterectomy during prolapse surgery is indispensable for effective treatment of this condition so we aimed to explore anatomic and functional outcomes in women undergoing hysteropexy by laparoscopic method and observe complication, recurrence and reoperation rates in these patients. MATERIAL AND METHODS In this study, 52 patients who underwent laparoscopic uterine preservation surgery for pelvic organ prolapse were evaluated between January 2011 and April Before operation, Papanicolaou smear were obtained from all women and women with a normal uterus as documented by a pelvic examination and routine endometrial sampling can undergo conservation of the uterus as part of the prolapse repair, assuming the risks and benefits of hysteropexy. Cervical elongation and stage 4 prolapsus according to POPQ were not included in the study. Before studying, hormone assays were performed to demonstrate that the patients were in the premenopausal period. Hysteropexy have been carefully reviewed by the physician and patient and the patient gives informed consent. The objective cure rates indicate anatomic outcomes after surgery and were measured by the improvement in the POP-Q (Point C) measurements. All laparoscopic procedures were performed through three trochars and homeostasis achieved with bipolar coagulation. After entering the wrist; the peritoneum was opened over the sacral promontory and right pelvic sidewall between the ureter and rectum toward the pouch of Douglas. Each broad ligament at the level of the cervico-uterine junction was also opened through the vascular area and the bladder dissected distally. Then, the uterus was suspended from the sacral promontory using a bifurcated polypropylene type-1 monofilament macro porous nonabsorbable mesh (Ethicon, USA), which, prior to sacral fixation, was wrapped around the cervix, via the broad ligament windows created. The two arms of the mesh were transfixed anterior 3
4 to the cervix with three non-absorbable polyester 2-0 sutures (Ethibond Excel TM; Ethicon). The anterior peritoneum in the cervico-ischemic region was dissected and 5 mm of Mersilene tape (Ethicon, USA) was tightly fastened to the front of the myometrium in the cervicismic area without uterine vessels dissipating laterally. All patients received information on the study and the computerized treatment of their data, their written informed consent was obtained. The study was approved by the hospital s Research and Ethics Committee ( /49, 01/03/2017). The data were analyzed for those who had completed at least eighteen months follow-up and patient satisfaction was measured by the Patient Global Impression of Improvement (PGI-I). The calculation of aggregated results is based on objective outcome measures. STATISTICAL ANALYSIS The process involved descriptive statistics and the descriptive data were presented as mean ± standard deviation, median and ratio. Non-parametric Mann-Whitney U test was used to compare the mean of the data among the groups. P <0.05 was considered significant. Statistical Package for Social Sciences (SPSS) for Windows 20 (SPSS for Windows, SPSS, Chicago) was used for statistical analysis. RESULTS During the study period of 6 years, there were a total of 94 pelvic organ prolapse in our university hospital and 52 cases eligible for study were diagnosed and treated by laparoscopic hysteropexy. Of the women included in the study, 11.5% were first gestations and 23.1% were second gestations. The proportion of women with 3 and over stories of pregnancy was 61.6%. When evaluated in terms of parity, 15.4% of women have delivered once, 3 and over the rate of women giving birth was 50%. 38.5% of the women who participated in the study had 1, 9.6% of them had a drop of 2 or more (Table1).The mean age and BMI of patients were 37±5 and 27.1±4.3 respectively. Table 1: Percent distribution of gravida, parity and abort us in laparoscopic hysteropexy. Gravida Number (n=52) (%) and over Parity and over Abort us and over Total
5 When evaluated the cases in terms of risk factors, 8 (15,4%) patients had chronic constipation, 14 (26,9%) patients had chronic obstructive pulmonary disease and 5 (9,6%) patients had genetic factors. 48,1% of women with a POP have no known risk factors. 37 of our patients were housewives and primary school graduates and 15 were university graduates. When patients were evaluated in terms of symptoms, uterine sagging 30 (57,7%), low back pain 14 (26,9%), unable to urinate 4 (7,7%), fullness in vagina 4 (7,7%) were the main symptoms mentioned. The mean duration of symptoms were 34±6 months and postoperative follow-up time of the cases were 41±23 months. 38 of the cases had laparoscopic sacrohystopexy alone and in 14 cases in addition to laparoscopic sacrohystopexy, laparoscopic abdominal Burch, transobturator tape and colporaphy anterior and posterior were performed in 6, 3, 3 and 2 of cases respectively. Table 2: Used surgical method, recurrence and pregnancy rate of the laparoscopic procedure. Surgical method Number (n=52) % Material Number (n=52) % Recurrence % Pregnancy number (n=43) % Laparoscopic sacrohysteropexy Tape Laparoscopic sacrohysteropexy+ addition surgery Mesh Nine patients had a pregnancy after operation in average of 24 month follow-up. Seven were in laparoscopic sacrohysteropexy and two were in laparoscopic sacrohysteropexy and addition surgery group. The average birth week was 35,4 ± 6. In 88,9% of cases, pregnancy reached 34 weeks and over. Intrauterine mort fetus was detected at 29th week in one of the cases, where mesh was used for hysteropexy. All patients who were pregnant after surgery, required delivery by scheduled caesarean section. The mesh around the cervix is comparable with abdominal cervical cerclage and cervical dilatation would be impossible in labor. Although potential difficulty with caesarean section due to mesh was a concern, a well formed lower segment had developed above the mesh. 5
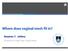
6 Figure 1: A pregnancy (14th week) after laparoscopic hysteropexy with mersilene tape. 9 patients (17,3% of women) who underwent a laparoscopic hysteropexy for a mean followup of 22 months postoperatively had uterine descensus of Pelvic Organ Prolapse Quantification System (POP-Q) stage II or greater. Four patients with recurrence of prolapse who have symptoms of prolapse needed further surgery to treat the recurrence (7,7% of women). Table 3: Postoperative complication and additional analgesic requirement. Complication Laparoscopic sacrohysteropexy (n=52) % Febrile morbidity(pneumonia) Urinary tract infection Analgesic requirement Laparoscopic sacrohysteropexy (n=52) Additional analgesic % Bowel injury Excessive blood loss Wound infection Urinary retention Major vessel injury Deep vein thrombosis Total dose of morphin Complications related to the laparoscopic sacrohysteropexy include major vessel injury (3,8%), deep vein thrombosis(1,7%), excessive blood loss (11,5%), rectal injury (1,7%), urinary tract infection (9,6%), and urinary retention (7,7%). Postoperative analgesia was required for 71% of cases. 6
7 DISCUSSION Pelvic organ prolapse (POP) is described as the protrusion of pelvic organs to the vegan and is an important health problem especially in patients of older age. Nowadays, most women with POPs prefer uterine protective surgery because of changes in lifestyle, beliefs, desire for pregnancy, and understanding of the role of uterus in sexual function. For this reason, the need for more minimally invasive surgery, reduced intra operative and postoperative risks, and newer surgical procedures involving a faster recovery period are increased in POP surgery. The aims of surgery for POP comprise restoration of normal anatomy, to sustain or restore urinary, bowel and sexual functions and to improve quality of life. Conservative treatment of uterovaginal prolapse (observation, pessary or pelvic floor physical therapy) in women with uterovaginal prolapse should be the first-line treatment for women planning an attempted pregnancy. However, hysteropexy can be considered in women who have severe prolapse or whose symptoms cannot be corrected by conservative treatment. In women with symptomatic uterine prolapse requiring surgery we obtained good anatomical cure rates of 82,7% with laparoscopic hysteropexy by mean follow-up of 30 months. Significant improvements in point C measurements on the POP-Q staging were achieved and this improvement was continued over the follow-up period. Quality of life questionnaire to evaluate the subjective improvement was used and significant subjective improvements in vaginal (prolapse) symptoms, sexual wellbeing and related quality of life were observed. The subjective success in our study was 96%, failure and reoperation rates were 17, 3%, 7,7% respectively. Our study had a long follow-up period but had no an independent assessor examining the patients postoperatively. Our major complications with laparoscopic hysteropexy included major vessel injury, rectal perforation, deep vein thrombosis and pneumonia. The overall risk of these major complications was around 13%. Postoperative pains were more common minor complications that needed analgesic requirement rates of 71%. Other minor complications reported with laparoscopic hysteropexy were urinary retention, urinary tract and port-site infections, and constipation. The overall risk of minor complications was around 25%. The overall risk of any complication (major or minor) was 38%. A study conducted by Gracia M et al. found that laparoscopic subtotal hysterectomy with sacral colpopexy had statistically significant superior anatomic cure rates compared to laparoscopic hysteropexy [17]. Another study comparing laparoscopic hysteropexy to laparovaginal hysterectomy with uterosacral colpopexy had a similar conclusion, but also found that reoperation rates were similar in the two groups [18]. However as the comparator surgeries used were different in three studies, these groups are not comparable, and further randomized trials may be needed to draw any conclusion about the efficacy of laparoscopic hysteropexy when compared to other surgeries for prolapse. 7
8 In the large cohort study by Rahmanou et al. [5], 91% of the women underwent at least one additional concomitant procedure that was performed once apical support was achieved with hysteropexy. Although 86% of them had posterior colpoperineorrhaphy, significant subjective improvements in vaginal (prolapse) symptoms, sexual wellbeing and related quality of life were observed. Compared to this study, our work is more realistic in respect of the circumstances mentioned above because in our study only 27% of the women underwent at least one additional concomitant procedure [19]. Since our case numbers are not sufficient to make a conclusion in cases of laparoscopic hysteropexy further research is needed in order to assess in isolation (excluding the cases with concomitant vaginal surgery) the effects of the hysteropexy on the quality of the sexual life. One of the most commonly used methods to protect the uterus in pelvic organ prolapse is sacrospinous hysteropexy, and a large study evaluating this procedure showed a 84% satisfaction rate [20]. Studies using POP-Q measurements have evaluated objective or anatomical success as improvement of apical measurement represented by C-point. The overall POP-Q stage, POP-Q stage 0 or stage 1 was considered anatomic success in all studies. İn majority of studies above 90% of anatomical or objective treatment rates were reported. Final healing rates indicate postoperative anatomical results and are measured by improvement in POP-Q (Point C) measurements. We investigated that similar subjective success rates could be achieved with laparoscopic sacroshysteropexy. Therefore, we suggested that this procedure was comparable to conventional uterine protective techniques and in present study because of the no need for lateralization of the uterine vessels with the laparoscopic hysteropexy technique applied during the procedure, there was no major bleeding due to trauma of these vessels. One advantage of the laparoscopic hysteropexy operation was that there was no risk of slipping due to tissue passage (through myometrium). Until now, there is no specific study on pregnancy after hysteropexy. However, multiple pregnancy cases and delivery have been reported in larger outcome trials. In a similar way, little is known about how pregnancy and birth affects hysteropexy. However; more cases with longer follow-up are required to consolidate the data for pregnancy and hysteropexy. Since all of our pregnant cases had passed 12 months longer than their birth were called to assess the effect of pregnancy on hysteropexy. According to the outcomes pregnancy has no harmful affect on apical support in women post-hysteropexy, quality of life and sexual function. The repair remained intact and there was no recurrence of the prolapse one year after delivery. Although the pregnancy outcomes were favorable and none had a recurrence of the prolapse after delivery, the numbers are too small to draw any meaningful conclusion. Further data is needed about pregnancies after laparoscopic hysteropexy. Although to date, there are not enough data to make a standard recommendation regarding the type of hysteropexy in women who desire future pregnancy, and there is not a recommended mode of delivery in our current study achieved pregnancy rate of was 20.9% (9/43) and all patients who were pregnant after surgery, required delivery by scheduled 8
9 caesarean section; so this study suggests that uncomplicated pregnancy to full term is possible following laparoscopic hysteropexy technique. Compared with the current literature, our recurrent rate was slightly higher. This is due to the fact that our mean follow-up period is longer than these studies and that in most cases we were applied mersilene tape as a laparoscopic hysteropexy technique. Our study is retrospective and does not have a separate control group. This is the limiting feature of our work. On the other hand, it is not ethically appropriate to plan a prospective randomized controlled trial in cases that are candidates for hysteropexy. Another handicap of our work was that women with stage IV uterovaginal prolapse or cervical elongation were excluded because the available studies note a very high rate of prolapse recurrence in these patients and other was not independent assessor examining the patients postoperatively. This suggests that more long term data is needed to draw definitive conclusions of the long term efficacy and durability of laparoscopic hysteropexy CONCLUSION Women who require surgery to correct uterovaginal prolapse and who are seeking protection of the uterus should be recommended for hysteropexy as one of the options and should be consulted about the relatively low evidence of these procedures. They should be informed that the procedure has a successful rate in terms of the rate of anatomical treatment and resolution of symptoms after surgery. Failure rates are usually low, but if the prolapse is repeated, reoperation may be necessary. In present study, laparoscopic hysteropexy was associated with more than 82,7% of good anatomic healing rates, so surgical correction of uterovaginal prolapse is a feasible alternative for women who need and want to protect their uterus due to various reasons. However uterinesparing procedures require further research but remain an acceptable option for most patients with uterovaginal prolapse after a balanced and unbiased discussion reviewing the advantages and disadvantages of this approach. We think that it is the most important point of careful selection of patients for laparoscopic uterine-sparing procedure in the light of our data. References 1. Haylen BT, Maher CF, Barber MD, Camargo S, Dandolu V, et al. An International Urogynecological Association (IUGA)/ International Continence Society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int Urogynecol J 2016; 27: Samuelsson EC, Victor FT, Tibblin G, Svärdsudd KF. Signs of genital prolapse in a Swedish population of women 20 to 59 years of age and possible related factors. Am J Obstet Gynecol. 1999; 180: Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol. 1997; 89: Marchionni M, Bracco GL, Checcucci V, Carabaneanu A, Coccia EM, et al. True incidence of vaginal vault prolapse. Thirteen years of experience. J Reprod Med. 1999; 44: Rahmanou P, White B, Price N, Jackson S. Laparoscopic hysteropexy: 1- to 4-year follow-up of women postoperatively. Int Urogynecol J. 2014; 25:
10 6. Fayyad AM, Siozos CS. Safety and one year outcomes following vaginally assisted laparoscopic uterine sacropexy (VALUES) for advanced uterine prolapse. Neurourol Urodyn. 2014; 33: Zucchi A, Lazzeri M, Porena M, Mearini L, Costantini E. Uterus preservation in pelvic organ prolapse surgery. Nat Rev Urol. 2010; 7: Neuman M, Lavy Y. Conservation of the prolapsed uterus is a valid option: medium term results of a prospective comparative study with the posterior intravaginal slingoplasty operation. Int Urogynecol J. Pelvic Floor Dysfunct. 2007; 18: Gutman R, Maher C. Uterine-preserving POP. Surgery. Int Urogynecol J. 2013; 24: Gracia M, Perello M, Bataller E, Espuña M, Parellada M, et al. Comparison between laparoscopic sacral hysteropexy and subtotal hysterectomy plus cervicopexy in pelvic organ prolapse: a pilot study. Neurourol Urodyn. 2015; 34: Korbly NB, Kassis NC, Good MM, Richardson ML, Book NM, et al. Patient preferences for uterine preservation and hysterectomy in women with pelvic organ prolapse. Am J Obstet Gynecol. 2013; 209: 471.e1-e Beri M, Ridgeway, MD. Does prolapse equal hysterectomy? The role of uterine conservation in women with uterovaginal prolapse. American Journal of Obstetrics & Gynecology Price N, Slack A, Jackson SR. Laparoscopic hysteropexy: the initial results of a uterine suspension procedure for uterovaginal prolapse. BJOG. 2010; 117: Freeman RM, Pantazis K, Thomson A, Frappell J, Bombieri L, et al. A randomized controlled trial of abdominal versus laparoscopic sacrocolpopexy for the treatment of post-hysterectomy vaginal vault prolapse: LAS study. Int Urogynecol J. 2013; 24: Cutner A, Kearney R, Vashisht A. Laparoscopic uterine sling suspension: a new technique of uterine suspension in women desiring surgical management of uterine prolapse with uterine conservation. BJOG. 2007; 114: Chen G, Ling B, Li J, Xu P, Hu W, et al. Laparoscopic extraperitoneal uterine suspension to anterior abdominal wall bilaterally using synthetic mesh to treat uterovaginal prolapse. J Minim Invasive Gynecol. 2010; 17: Gracia M, Perello M, Bataller E, Espuña M, Parellada M, et al. Comparison between laparoscopic sacral hysteropexy and subtotal hysterectomy plus cervicopexy in pelvic organ prolapse: A pilot study. Neurourol Urodyn. 2015; 34: Bedford ND, Seman EI, O Shea RT, Keirse MJ. Effect of uterine preservation on outcome of laparoscopic uterosacral suspension. J Minim Invasive Gynecol. 2013; 20: Rahmanou P, White B, Price N, Jackson S. Laparoscopic hysteropexy: 1- to 4-year follow-up of women postoperatively. Int Urogynecol J. 2014; 25: Dietz V, Huisman M, de Jong JM, Heintz PM, Vander vaart CH. Functional outcome after sacrospinous hysteropexy for uterine descensus. Int Urogynecol J Pelvic Floor Dysfunct. 2008; 19:
Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases.
 Research Article http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases. Hasan Çılgın*
Research Article http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases. Hasan Çılgın*
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
University College Hospital
 University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
An Unusual Case of Prolapse Uterus
 An Unusual Case of Prolapse Uterus Sarita Channawar*, Nagendra Sardesh Pande** Abstract A 12 year old girl, operated earlier for ectopia vesica, pubic diathesis and vaginal at - resia presented to us with
An Unusual Case of Prolapse Uterus Sarita Channawar*, Nagendra Sardesh Pande** Abstract A 12 year old girl, operated earlier for ectopia vesica, pubic diathesis and vaginal at - resia presented to us with
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation in Treatment of Vaginal Vault Prolapse
 ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
The UK National Prolapse Survey: 10 years on
 Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Infracoccygeal sacropexy using mesh for uterine prolapse repair
 Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO
 AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy
 Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Facing Gynecologic Surgery?
 Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of uterine suspension using mesh (including sacrohysteropexy) to repair uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of uterine suspension using mesh (including sacrohysteropexy) to repair uterine prolapse
Laparoscopic hysteropexy
 Page 1 of 10 Laparoscopic hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Page 1 of 10 Laparoscopic hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Laparoscopic Hysteropexy
 Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
American Journal of Obstetrics and Gynecology
 American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
Surgery for vaginal vault prolapse. Patient decision aid
 Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Motility Disorders. Pelvic Floor. Colorectal Center for Functional Bowel Disorders (N = 701) January 2010 November 2011
 Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Dear Mrs. Burch and editors of the BMJ,
 Dear Mrs. Burch and editors of the BMJ, We are pleased that our manuscript entitled: Sacrospinous hysteropexy versus vaginal hysterectomy with uterosacral ligament suspension in women with uterine prolapse
Dear Mrs. Burch and editors of the BMJ, We are pleased that our manuscript entitled: Sacrospinous hysteropexy versus vaginal hysterectomy with uterosacral ligament suspension in women with uterine prolapse
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 301.681.3400 OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is surgery to remove the uterus. It is a very common type of surgery for women in the United States. Removing your uterus means
301.681.3400 OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is surgery to remove the uterus. It is a very common type of surgery for women in the United States. Removing your uterus means
Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal Prolapse: A Series of 32 Cases
 ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Surgery for women with apical vaginal prolapse(review)
 Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Introduction to GYN Specialties
 Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Changing trends of surgical approaches for uterine prolapse: an 11-year population-based nationwide descriptive study
 Int Urogynecol J (2012) 23:865 872 DOI 10.1007/s00192-011-1647-1 ORIGINAL ARTICLE Changing trends of surgical approaches for uterine prolapse: an 11-year population-based nationwide descriptive study Ming-Ping
Int Urogynecol J (2012) 23:865 872 DOI 10.1007/s00192-011-1647-1 ORIGINAL ARTICLE Changing trends of surgical approaches for uterine prolapse: an 11-year population-based nationwide descriptive study Ming-Ping
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Total vs Subtotal Hysterectomy
 Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
12/1/13. What are Pelvic Floor Disorders? What is the Pelvic Floor? Facts. Prevalence of Urinary InconOnence. What s New in Pelvic Floor Disorders?
 What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
Two-thirds of the almost one-half million
 Minimally Invasive Surgery New data and the guidance of our professional societies are bringing us closer to clarity in understanding the superiority of minimally invasive techniques of hysterectomy Amy
Minimally Invasive Surgery New data and the guidance of our professional societies are bringing us closer to clarity in understanding the superiority of minimally invasive techniques of hysterectomy Amy
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Sacrospinous Fixation Operation
 Sacrospinous Fixation Operation Information for patients Gynaecology Department Phone no: 01625 661161 East Cheshire NHS Trust www.eastcheshire.nhs.uk @eastcheshirenhs Ref: 11485 Review: 10/2015 Revised
Sacrospinous Fixation Operation Information for patients Gynaecology Department Phone no: 01625 661161 East Cheshire NHS Trust www.eastcheshire.nhs.uk @eastcheshirenhs Ref: 11485 Review: 10/2015 Revised
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
Degree of uterine prola pse
 by R. MITRA,* M.S., D.G.O. J Before the middle of the nineteenth century very little attention was directed towards the advancement of knowledge about the anatomical supports of the genital organs or towards
by R. MITRA,* M.S., D.G.O. J Before the middle of the nineteenth century very little attention was directed towards the advancement of knowledge about the anatomical supports of the genital organs or towards
ORIGINAL ARTICLE. Alper Biler 1, I. Egemen Ertas 1, Gokhan Tosun 1, Ismet Hortu 2, Unal Turkay 3, Ozge E. Gultekin 4, Gulfem Igci 3 ABSTRACT
 ORIGINAL ARTICLE Vol. 44 (5): 996-1004, September - October, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0692 Perioperative complications and short-term outcomes of abdominal, laparoscopic, and laparoscopic
ORIGINAL ARTICLE Vol. 44 (5): 996-1004, September - October, 2018 doi: 10.1590/S1677-5538.IBJU.2017.0692 Perioperative complications and short-term outcomes of abdominal, laparoscopic, and laparoscopic
Tension-free Vaginal Tape for Urodynamic Stress Incontinence
 Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Long-term Results of Tension-free Vaginal Tape Insertion for Urodynamic Stress Incontinence in Chinese Women at Eight-year Follow-up: a Prospective Study YM CHAN MBBS, MRCOG, FHKAM (O&G), DCG, DCH, DFM,
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Vaginal Parity and Pelvic Organ Prolapse
 The Journal of Reproductive Medicine Vaginal Parity and Pelvic Organ Prolapse Lieschen H. Quiroz, M.D., Alvaro Muñoz, Ph.D., Stuart H. Shippey, M.D., Robert E. Gutman, M.D., and Victoria L. Handa, M.D.
The Journal of Reproductive Medicine Vaginal Parity and Pelvic Organ Prolapse Lieschen H. Quiroz, M.D., Alvaro Muñoz, Ph.D., Stuart H. Shippey, M.D., Robert E. Gutman, M.D., and Victoria L. Handa, M.D.
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
30/06/2014. Gynaecological Surgery. Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London WHAT IS LAPAROSCOPIC SURGERY?
 Gynaecological Surgery Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London Laparoscopic surgery techniques Common complications of laparoscopic surgery Intra-operative injuries:
Gynaecological Surgery Mr Alfred Cutner, Consultant Gynaecologist, University College Hospital, London Laparoscopic surgery techniques Common complications of laparoscopic surgery Intra-operative injuries:
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse
 SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
van IJsselmuiden et al. BMC Women's Health 2014, 14:112
 van IJsselmuiden et al. BMC Women's Health 2014, 14:112 STUDY PROTOCOL Open Access Hysteropexy in the treatment of uterine prolapse stage 2 or higher: a multicenter randomized controlled non-inferiority
van IJsselmuiden et al. BMC Women's Health 2014, 14:112 STUDY PROTOCOL Open Access Hysteropexy in the treatment of uterine prolapse stage 2 or higher: a multicenter randomized controlled non-inferiority
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Laparoscopic Sacrohysteropexy
 Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
Professor Christian Phillips BSc Hons BM DM FRCOG Consultant Gynaecologist and Urogynaecologist Laparoscopic Sacrohysteropexy What is a prolapse? Uterine prolapse is a bulge or lump in the vagina caused
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Hysterectomy Fact versus fiction. Richard Dover Specialist Gynaecologist
 Hysterectomy Fact versus fiction Richard Dover Specialist Gynaecologist Disclaimer Disclaimer Hysterectomy An update? Myths busted? HYSTERECTOMY Retro-chic! HMB Important cause of morbidity Affects
Hysterectomy Fact versus fiction Richard Dover Specialist Gynaecologist Disclaimer Disclaimer Hysterectomy An update? Myths busted? HYSTERECTOMY Retro-chic! HMB Important cause of morbidity Affects
A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy
 Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
FRANZCOG Training Program Logbook Procedure List and Classification
 FRANZCOG Training Program Logbook Procedure List and Classification This logbook procedure list provides sites and trainees with the major/minor classification of procedures in the online logbook. As detailed
FRANZCOG Training Program Logbook Procedure List and Classification This logbook procedure list provides sites and trainees with the major/minor classification of procedures in the online logbook. As detailed
Aetiology 1998 Bump & Norton Theoretical model
 Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications
 Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Women s Health. Product innovation. Commitment. We are committed to you... and advancing the quality of your patient care.
 II Commitment We are committed to you... and advancing the quality of your patient care. Boston Scientific is always there for you, your physicians and your patients. We are anchored in our guiding principle
II Commitment We are committed to you... and advancing the quality of your patient care. Boston Scientific is always there for you, your physicians and your patients. We are anchored in our guiding principle
Las Vegas Urogynecology
 Las Vegas Urogynecology 7500 Smoke Ranch Road - #200 Las Vegas, NV 89128 Telephone: (702) 233-0727 Fax: (702) 233-4799 Physician's Surgical Procedure Disclosure and Patient s Consent TO THE PATIENT: You
Las Vegas Urogynecology 7500 Smoke Ranch Road - #200 Las Vegas, NV 89128 Telephone: (702) 233-0727 Fax: (702) 233-4799 Physician's Surgical Procedure Disclosure and Patient s Consent TO THE PATIENT: You
COMPARATION AMONG THE MAIN HYSTERECTOMY ROUTES
 COMPARATION AMONG THE MAIN HYSTERECTOMY ROUTES Olsen, PR (Medical Student, UFRGS, Porto Alegre, Brazil); Souza, CAB (PhD HCPA, Porto Alegre, Brazil); Chapon, R (Post Graduate Student, UFRGS, Porto Alegre,
COMPARATION AMONG THE MAIN HYSTERECTOMY ROUTES Olsen, PR (Medical Student, UFRGS, Porto Alegre, Brazil); Souza, CAB (PhD HCPA, Porto Alegre, Brazil); Chapon, R (Post Graduate Student, UFRGS, Porto Alegre,
