2 Key Measures for Prevention and Control of Ebola Virus Disease. 4 Key Measures for Prevention and Control of Ebola Virus Disease
|
|
|
- Derick Banks
- 5 years ago
- Views:
Transcription
1 Key Measures for Prevention and Control of Ebola Virus Disease Dr. Sergey Eremin Medical Officer World Health Organization Hosted by Dr. Benedetta Allegranzi September 16, 2014 INTRODUCTION TO EBOLA VIRUS DISEASE (EVD) 2 Ebola Virus Disease EVD spread through direct contact with body fluids (stool, vomit, blood, urine, saliva, semen, breast milk) of a sick person with EVD direct contact with the deceased person s body or discharge (funeral or burial preparation or ceremonies) plays a role in the transmission of Ebola by contact with surfaces or equipment contaminated by body fluids of an infected person R 0 for this outbreak ranges between 1.4 and 1.6 in Guinea, Sierra Leone and Liberia Similar to what was observed in previous outbreaks in DRC in 1995 and lower than the R in Uganda in 2000 It is lower than most of the cholera outbreaks seen in the west African region in the past decade (R 0 2.4) 3 Ebola Virus Disease Incubation 2-21 days In the current outbreak, in 90% of patients for whom information is available, <15 days Case fatality ratio 24-89% 54.9% for current outbreak Average time between symptom onset and death is 7 days approximately 50% of patients Average time form symptom onset to recovery is 15 days the other 50% of patients 4 Ebola Virus Disease Often sudden onset of fever, intense weakness, muscle pain, headache and sore throat Followed by vomiting, diarrhea, and in some cases, both internal and external bleeding The symptoms of EVD are not specific and are difficult to differentiate from other endemic or epidemic tropical diseases such as malaria, typhoid fever, leptospirosis etc Laboratory confirmation is key to monitor the diseases in the population and guide the triage of patient in health care facilities to prevent health-care associated infection in hospitalized patients Ebola Virus Disease Treatment is supportive but effective in reducing mortality Rehydration, intensive care Some potential specific treatment Monoclonal antibodies Very limited availability Limited information on safety & efficacy Other candidate drugs also in early stages of testing Vaccines in development In the environment the virus can be eliminated relatively easily with heat, alcohol-based products, and many commonly used disinfectants (e.g. sodium hypochlorite) 5 6 1
2 Key Measures for the Prevention and Control of Ebola Virus Key features of the outbreak in West Africa Localized outbreaks (hotspots or hubs of transmission) The initial epicenter is in the forest region along the border areas of Guinea, Liberia, and Sierra Leone It is amplified by intensive commercial and social activities. Other hotspots are in the densely populated urban areas with intense transmission in Monrovia (Liberia) and Freetown in Sierra Leone, and various rural areas in the affected countries. There is also limited transmission in Lagos and port Harcourt in Nigeria initiated through an imported case from Liberia as well as in Senegal (1 imported case from Guinea by land crossing) 7 Geographical distribution of new and total cases in Guinea, Liberia, and Sierra Leone Key interventions to stop EVD transmission 1. Early isolation of patients to prevent transmission at home and in the community In addition to isolation, Ebola treatment centres provide safe care and psychosocial support and contribute to surveillance through identification of contacts 2. Early detection of new Ebola cases through close monitoring of contacts and isolation of contacts when they show symptoms 3. Safe burials: to reduce transmission through contact with dead bodies, whether during preparation of the body for burial or during the funeral ceremony Laboratory diagnostic and social mobilization are critical to support the above mentioned interventions 8 Distribution of EVD cases by affected countries 4366 EVD cases and 2218 deaths in West Africa, as of September 7 9 EVD cases in HCW 10 WHO Interim IPC guidance for EVD Interim Infection Prevention and Control Guidance for Care of Patients with Suspected or Confirmed Filovirus Haemorrhagic Fever in Health-Care Settings, with Focus on Ebola August
3 Standard Precautions Infection prevention and control for GENERAL PATIENT CARE Routine precautions to be applied in ALL situations for ALL patients whether or not they appear infectious or symptomatic especially important for EVD because the initial manifestations are nonspecific Standard Precautions: key elements hand hygiene gloves gown BASED ON RISK ASSESSMENT BASED ON RISK ASSESSMENT facial protection BASED ON RISK ASSESSMENT (eyes, nose, mouth) respiratory hygiene and cough etiquette environmental cleaning and disinfection cleaning and disinfection of patient care equipment waste disposal injection safety and prevention of sharps injuries Samuel Aranda Standard Precautions Reduce the risk of transmission of microorganisms from both recognized and non-recognized sources of infection Apply to blood, all body fluids, secretions and excretions (except sweat) whether or not they contain visible blood; non-intact skin; and mucous membranes Main foundations Hand hygiene Use of PPE based on risk assessment Clean/safe environment Hand hygiene How to perform hand hygiene: Clean your hands by rubbing them with an alcohol based formulation, as the preferred mean for routine hygienic hand antisepsis if hands are not visibly soiled It is faster, more effective, and better tolerated by your hands than washing with soap and water. Wash your hands with soap and water when hands are visibly dirty or visibly soiled with blood or other body fluids or after using the toilet
4 Key Measures for the Prevention and Control of Ebola Virus How to handrub The 5 Moments apply to any setting where health care involving direct contact with patients takes place How to handwash Handwashing must last secs and should be performed by following all of the illustrated steps. 21 Handrubbing must be performed by following all of the illustrated steps. This takes only seconds! Use of PPE based on risk assessment 22 Patient placement Put suspected or confirmed cases in single isolation rooms with adjoining dedicated toilet or latrine showers sink equipped with running water, soap and single-use towels, alcohol-based hand rub dispensers stocks of personal protective equipment (PPE) stocks of medicines good ventilation screened windows, doors closed restricted access Infection prevention and control for DIRECT PATIENT CARE FOR SUSPECTED OR CONFIRMED PATIENTS WITH EVD
5 Patient placement Staff allocation if isolation rooms are unavailable, cohort these patients in specific confined areas Rigorously keep suspected and confirmed cases separate Ensure the items listed for isolation rooms are readily available Make sure that there is at least 1 meter (3 feet) distance between patient beds Ensure that clinical and non-clinical personnel are assigned exclusively to EVD patient care areas Ensure that members of staff do not move freely between the EVD isolation areas and other clinical areas during the outbreak Restrict all non-essential staff from EVD patient care areas Visitors Stopping visitors access to the patient is preferred If this is not possible, limit their number to include only those necessary for the patient s well-being and care, such as a child s parent Do not allow other visitors to enter the isolation rooms/ areas and ensure that any visitors wishing to observe the patient do so from an adequate distance (approximately 15 m or 50 feet) Before allowing visitors to EVD patients to enter the HCF, screen them for signs and symptoms of EVD Hand hygiene, PPE, and other precautions Ensure that all visitors use PPE and perform hand hygiene and are provided with related instructions prior to entry into the isolation room/area Ensure that all HCWs (including aides and cleaners) wear PPE according to the expected level of risk before entering the isolation rooms/areas and having contacts with the patients and/or the environment Personal clothing should not be worn for working in the patient areas. Scrub or medical suits should be worn Hand hygiene, PPE, and other precautions Carefully apply IPC precautions to avoid any possible unprotected direct contact with blood and body fluids when providing care to any patient with EVD, including suspected cases Perform hand hygiene: Before donning gloves and wearing PPE on entry to the isolation room/area Before any clean/aseptic procedures being performed on a patient After any exposure risk or actual exposure with the patient s blood and body fluids After touching (even potentially) contaminated surfaces/items/equipment in the patient s surroundings After removal of PPE, upon leaving the care area
6 Hand hygiene Hand hygiene should be performed within the isolation rooms/areas every time it is needed according to the above indications during care to a patient, along with change of gloves When caring for patients in the same room, it is essential to organize the complete care to each patient before moving to the next and to perform hand hygiene between touching the patients Neglecting to perform hand hygiene after removing PPE will reduce or negate any benefits of the protective equipment. To perform hand hygiene Use an alcohol-based hand rub or soap and running water applying the correct technique recommended by WHO Always perform hand hygiene with soap and running water when hands are visibly soiled Alcohol-based hand rubs should be made available at every point of care (at the entrance and within the isolation rooms/ areas) and are the standard of care Alcohol-based hand rubs can be produced locally at the HCF level by following WHO recommendations and instructions Personal protective equipment PPE Correctly sized gloves (non-sterile examination gloves) when entering the patient care area Consider changing gloves if heavily soiled with blood or any body fluids while providing care to the same patient perform careful hand hygiene immediately after removal Always change gloves and perform hand hygiene immediately after removal, when moving from one patient to another while caring for patients in the same room. Consider double gloving when the quality of gloves appears to be poor (e.g., if holes and tears form rapidly during use) PPE A disposable, impermeable gown to cover clothing and exposed skin PPE when handling a case of EVD A medical mask and eye protection (eye visor, goggles or face shield) to prevent splashes to the nose, mouth and eyes Closed, puncture and fluid resistant shoes (e.g. rubber boots) to avoid contamination with blood or other body fluids or accidents with misplaced, contaminated sharp objects. If boots are not available, overshoes should be used but these must be removed while still wearing gloves and with caution to avoid hand contamination
7 Key Measures for the Prevention and Control of Ebola Virus PPE when handling a case of EVD Both dressing and undressing should be supervised by a trained member of the team. These instructions should be displayed on the wall in the dressing and undressing room: Different standards 40 min vs hours Human interaction and facial expressions Concerns about neck area exposure Resource implications Other HC settings When using PPE Taking off PPE Remove the most contaminated PPE items first. Avoid touching or adjusting PPE Remove gloves if they become torn or damaged Hand hygiene must be performed immediately after glove removal Perform hand hygiene whenever ungloved hands touch contaminated PPE items Change gloves between patients Perform hand hygiene before donning new gloves Avoid touching your eyes, mouth, or face with gloved or ungloved hands Be careful to avoid any contact between the soiled items (e.g. gloves, gowns) and any area of the face (i.e. eyes, nose or mouth) or non-intact skin Discard disposable items in a waste container 39 Protection depends on: 40 Aerosol-generating procedures adequate and regular supplies Avoid aerosol-generating procedures if possible adequate staff training Wear a respirator (FFP2 or EN certified equivalent or US NIOSH-certified N95) if any procedures that stimulate coughing or promote the generation of aerosols is planned to be performed proper hand hygiene appropriate human behavior e.g., aerosolized or nebulized medication administration, diagnostic sputum induction, bronchoscopy, airway suctioning, endotracheal intubation, positive pressure ventilation via face mask close supervision and support
8 Reusable equipment Carefully clean and decontaminate reusable equipment Rigorously use dedicated equipment (e.g. stethoscopes) for each patient If this is not possible, decontaminate the items between each patient contact For instance, if the stethoscope has to be used on different patients, it is essential that the full stethoscope (i.e. staff hand contact as well as patient contact surfaces) be thoroughly cleaned first with water and soap using appropriate PPE to remove organic matter and then wiped with alcohol. All waste generated during the decontamination process should be treated as infectious waste Equipment in isolation areas Items and equipment should not be moved between isolation rooms/areas and other areas of the HCF, unless they are appropriately discarded and disposed. For instance, the patient charts and records should be kept outside the isolation rooms/areas to avoid their contamination Use of injection equipment Each patient should have exclusively dedicated injection and parenteral medication equipment which should be disposed of at the point of care. Syringes, needles or similar equipment should never be reused. INJECTION SAFETY AND MANAGEMENT OF SHARPS Limit the use of needles and other sharp objects as much as possible. Limit the use of phlebotomy and laboratory testing to the minimum necessary for essential diagnostic evaluation and patient care If the use of sharp objects cannot be avoided: ENVIRONMENTAL CLEANING & MANAGEMENT OF LINEN
9 PPE to use when cleaning Wear heavy duty/rubber gloves, impermeable gown and closed shoes (e.g. boots) when cleaning the environment and handling infectious waste. Add facial protection (mask and goggle or face shield) and overshoes if boots are unavailable when undertaking cleaning activities with increased risk of splashes or in which contact with blood and body fluids is anticipated e.g., cleaning surfaces heavily soiled with vomit or blood or cleaning areas closer than 1 meter (3 feet) from a patient with symptoms like diarrhoea, bleeding or vomiting, etc.) Cleaning process Environmental surfaces or objects contaminated with blood, other body fluids, secretions or excretions should be cleaned and disinfected as soon as possible using standard hospital detergents/disinfectants (e.g. 0.5% chlorine solution) Application of disinfectants should be preceded by cleaning to prevent inactivation of disinfectants by organic matter Cleaning should always be carried out from clean areas to dirty areas, in order to avoid contaminant transfer cleaning process If locally prepared, prepare cleaning and disinfectant solutions every day Change cleaning solutions and refresh equipment frequently while being used during the day, as they will get contaminated quickly Follow your hospital protocols if available cleaning process Clean floors and horizontal work surfaces at least once a day with clean water and detergent. Cleaning with a moistened cloth helps to avoid contaminating the air and other surfaces with airborne particles. Allow surfaces to dry naturally before using them again. Dry sweeping with a broom should never be done. Rags holding dust should not be shaken out and surfaces should not be cleaned with dry rags cleaning process Management of linen Do not spray (i.e. fog) occupied or unoccupied clinical areas with disinfectant This is a potentially dangerous practice that has no proven disease control benefit Linen that has been used on patients can be heavily contaminated with body fluids (e.g. blood, vomit) and splashes may result during handling When handling soiled linen from patients, use gloves, impermeable gown, closed shoes (e.g., boots) and facial protection (mask and goggle or face shield)
10 management of linen Place soiled linen in clearly-labelled, leak-proof bags or buckets at the site of use Container surfaces should be disinfected before removal from the isolation room/area If there is any solid excrement such as faeces or vomit, scrape off carefully using a flat firm object and flush it down the toilet or in the sluice before linen is placed in its container If the linen is transported out of the patient room/area, it should be put in a separate container it should never be carried against the body Linen should be transported directly to the laundry area and laundered promptly with water and detergent management of linen For low-temperature laundering, wash linen with detergent and water, rinse and then soak in 0.05% chlorine for 30 minutes. Linen should then be dried according to routine standards and procedures. Washing contaminated linen by hand should be discouraged If washing machines are not available or power is not ensured, take the soiled linen out of the container and empty it into a large drum container of hot water and soap. Soak the linen in this drum and make sure it is totally covered with water Use a stick to stir; then throw out the water and refill the drum with clean water and add bleach and allow to soak for minutes. Remove the linen and then rinse in clean water. Remove excess water and spread out to dry. Avoid as much splashing as possible. If safe cleaning and disinfection of heavily soiled linen is not possible or reliable, burn the linen to avoid any unnecessary risks to individuals handling these items PPE for waste management WASTE MANAGEMENT Wear heavy duty/rubber gloves, impermeable gown, closed shoes (e.g. boots) and facial protection (mask and goggle or face shield), when handling infectious waste (e.g. solid waste or any secretion or excretion with visible blood even if it originated from a normally sterile body cavity) Goggles provide greater protection than visors from splashes that may come from below when pouring liquid waste from a bucket Avoid splashing when disposing of liquid infectious waste Waste collection Waste should be segregated at point of generation to enable appropriate and safe handling. Collect all solid, non-sharp, infectious waste using leakproof waste bags and covered bins. Bins should never be carried against the body (e.g. on the shoulder) Waste disposal Waste should be placed in a designated pit of appropriate depth (e.g. 2 m or about 7 feet) and filled to a depth of m (or about 3 5 feet). After each waste load, the waste should be covered with a layer of soil cm deep An incinerator may be used for short periods during an outbreak to destroy solid waste It is essential to ensure that total incineration has taken place Caution is required when handling flammable material and when wearing gloves due to the risk of burn injuries if gloves are ignited
11 waste disposal Waste should be placed in a designated pit of appropriate depth (e.g. 2 m or about 7 feet) and filled to a depth of m (or about 3 5 feet). After each waste load, the waste should be covered with a layer of soil cm deep An incinerator may be used for short periods during an outbreak to destroy solid waste It is essential to ensure that total incineration has taken place Caution is required when handling flammable material and when wearing gloves due to the risk of burn injuries if gloves are ignited waste disposal Placenta and anatomical samples should be buried in a separate pit The area designated for the final treatment and disposal of waste should have controlled access to prevent entry by animals, untrained personnel or children Waste such as faeces, urine and vomit, and liquid waste from washing, can be disposed of in the sanitary sewer or pit latrine. No further treatment is necessary Post-mortem examinations The coordinator and/or the IPC staff should be consulted for any decision making on post-mortem examinations. POST-MORTEM EXAMINATIONS Post-mortem examination of HF patient remains should be limited to essential evaluations only and should be performed by trained personnel post-mortem examinations Personnel examining remains should wear eye protection, mask, double gloves, disposable impermeable gowns, and closed shoes or boots. In addition, personnel performing autopsies of known or suspected HF patients should wear a particulate respirator (e.g., FFP2, or EN certified equivalent, or US NIOSH-certified N95) or a PAPR. When removing PPE, avoid any contact between soiled gloves or equipment and the face (i.e. eyes, nose or mouth) Hand hygiene should be performed immediately following the removal of PPE MANAGING EXPOSURE TO THE VIRUS
12 Key Measures for the Prevention and Control of Ebola Virus Percutaneous or muco-cutaneous exposure: what to do? Persons including HCWs with percutaneous or muco-cutaneous exposure to blood, body fluids, secretions, or excretions from a patient with suspected or confirmed HF should: immediately and safely stop any current tasks, leave the patient care area, safely remove PPE exposure during PPE removal can be just as dangerous immediately after leaving the patient care area, wash the affected skin surfaces or the percutaneous injury site with soap and water accordingly, irrigate mucous membranes (e.g. conjunctiva) with copious amounts of water or an eyewash solution, and not with chlorine solutions or other disinfectants 67 IPC training and reinforcement after training Importance of standard precautions in all outpatient and inpatient care Many HCW infections from failure to apply standard precautions, rather than PPE in treatment centre PPE - putting on and taking off is a skill not just knowledge that can be conveyed by demonstration needs practice needs ongoing supervision by dedicated supervisor Importance of safe work set-up and consistent practices 69 Managing exposure Immediately report the incident to the local coordinator This is a time-sensitive task and should be performed as soon as the HCW leaves the patient care unit Exposed persons should be medically evaluated including for other potential exposures (e.g., HIV, HCV) and receive follow-up care, including fever monitoring, twice daily for 21 days after the incident Immediate consultation with an expert in infectious diseases is recommended for any exposed person who develops fever within 21 days of exposure HCWs suspected of being infected should be cared for/isolated, and the IPC precautions must be applied until a negative diagnosis is confirmed Contact tracing and follow-up of family, friends, co-workers and other patients, who may have been exposed to Ebola virus through close contact with the infected HCW is essential 68 WHO Teleclass Schedule!"#$"%&'()'!""#$%&#"'%"(')*+,-*-".%&#"' /.0%.-1)2'%++0#%23-/'.#'0-(42-' 2% ,%.-('6%2.-0%-*)%7'83-' 0-/4,./'#9'%':40#+-%"'*4,&2-".0-' /.4(;'<=>?@!A!8B''!"#$%&'()"$*+,--.$/0+(1)"'&,2$$ *4,&0-/)/.%".'6%2.-0)%''!"#$/()34&,$5&"6&"(4.$/0+(1)"'&,2$$ *"&'2' >"8?#$!+2+)"$>+@)(.$/0+(1)"'&,2$$ 34/54674%'8' G-C'H@?'1,#6%,'2%*+%)1"'.#'-,)*)"%.-' 4"/%9-'.3-0%+-4&2')"I-2&#"/''!"#$A),)2)@&$='')-"&,1+.$/0+(1)"'&,2$$ 9+5:74%';' =46,)2'0-+#0&"1'%"('()/2,#/40-'#9'@J!' 0%.-/7'=#/)&$-')*+%2.'#0'2#"94/)#"K''!"#$B&"C&,,)$BDEFD;+,$G$B"#$784,$ E8H)2,+;.$</=$./%01')' L,#6%,'%++,)2%&#"'#9'6-3%$)#40'23%"1-' "-C'EFE'14)(-,)"-/'%"('*#0-' *#(-,/'%"(')"9-2&#"'2#".0#,'/.0%.-1)-/'' 70!"#$789)34$/8'8:;+,.$</=$$!"#$B+D4&)'$A8"-.$B&'(&$$!"#$%&'()'!*+*,+#&&'-./,#0)$' Patron Sponsors!!!"/%0$1",$2. 71!!!"!#$"%&'()*+,(-&. 12
Provider Health & Safety Alert Ebola Virus Disease September 30, 2014
 Provider Health & Safety Alert Ebola Virus Disease September 30, 2014 With the announcement of the first confirmed case of Ebola Virus Disease (EVD) in Dallas Texas, there could be interactions with individuals
Provider Health & Safety Alert Ebola Virus Disease September 30, 2014 With the announcement of the first confirmed case of Ebola Virus Disease (EVD) in Dallas Texas, there could be interactions with individuals
Personal Protective Equipment, Hand Hygiene and Surface Cleaning in the context of Ebola
 Personal Protective Equipment, Hand Hygiene and Surface Cleaning in the context of Ebola This publication and the information it contains is intended for distribution to, or use by, people in the following
Personal Protective Equipment, Hand Hygiene and Surface Cleaning in the context of Ebola This publication and the information it contains is intended for distribution to, or use by, people in the following
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING
 Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
 Health & Safety Manual Health Promotion & Wellness ROUTINE PRACTICES PROCEDURES INTRODUCTION The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
Health & Safety Manual Health Promotion & Wellness ROUTINE PRACTICES PROCEDURES INTRODUCTION The term Routine Practices is used to describe practices that were previously known as Universal Precautions.
Ebola Virus Disease (EVD) Essential information
 Ebola Virus Disease (EVD) Essential information Ebola Virus Disease (EVD) Origins The Ebola virus is named after the Ebola River in what was Zaire (now Democratic Republic of Congo) where the first outbreak
Ebola Virus Disease (EVD) Essential information Ebola Virus Disease (EVD) Origins The Ebola virus is named after the Ebola River in what was Zaire (now Democratic Republic of Congo) where the first outbreak
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE
 PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
بسم اهلل الرحمن الرحيم
 بسم اهلل الرحمن الرحيم INFECTION CONTROL MEASURES AGAINST H1N1 VIRUS; PHASE II Microbiology Diagnostics and Infection Control UNIT () Mansoura University Hospitals Prof. Mohammad Abou el-ela Director of
بسم اهلل الرحمن الرحيم INFECTION CONTROL MEASURES AGAINST H1N1 VIRUS; PHASE II Microbiology Diagnostics and Infection Control UNIT () Mansoura University Hospitals Prof. Mohammad Abou el-ela Director of
Guideline Norovirus Outbreak
 POLICY: To control for the spread of the Norovirus infection & optimise the rehabilitation of those affected. www.hh.net.nz for Infection Control Policy [NZS: 4134: 2008] REFERENCE: A+ Guidelines for the
POLICY: To control for the spread of the Norovirus infection & optimise the rehabilitation of those affected. www.hh.net.nz for Infection Control Policy [NZS: 4134: 2008] REFERENCE: A+ Guidelines for the
Media centre Ebola virus disease
 1 of 6 10/15/2014 10:59 AM Media centre Ebola virus disease Fact sheet N 103 Updated September 2014 Key facts Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, is a severe, often fatal
1 of 6 10/15/2014 10:59 AM Media centre Ebola virus disease Fact sheet N 103 Updated September 2014 Key facts Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, is a severe, often fatal
EBOLA FACTS. During this outbreak, most of the disease has spread through human-to-human transmission.
 EBOLA FACTS Ebola virus disease (formerly known as Ebola haemorrhagic fever) is a severe and often fatal illness, with a fatality rate of up to 90%. It is one of the world s most dreaded diseases. However,
EBOLA FACTS Ebola virus disease (formerly known as Ebola haemorrhagic fever) is a severe and often fatal illness, with a fatality rate of up to 90%. It is one of the world s most dreaded diseases. However,
SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/ April Swine Flu-Information Sheet
 SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/09 Swine Flu-Information Sheet To date 2 cases of swine Influenza A (H1N1) have been confirmed in individuals in Scotland. Other
SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/09 Swine Flu-Information Sheet To date 2 cases of swine Influenza A (H1N1) have been confirmed in individuals in Scotland. Other
Ebola Virus Diseases
 CDC/Dr F A Murphy Frequently Asked Questions on Ebola Virus Diseases Frequently asked questions on Ebola virus disease World Health Organization 2014 All rights reserved. Requests for publications, or
CDC/Dr F A Murphy Frequently Asked Questions on Ebola Virus Diseases Frequently asked questions on Ebola virus disease World Health Organization 2014 All rights reserved. Requests for publications, or
What employees should know about UNIVERSAL PRECAUTIONS. They re work practices that help prevent contact with blood and certain other body fluids.
 What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
Ebola Virus Disease: Occupational Safety and Health
 Ebola Virus Disease: Occupational Safety and Health Joint WHO/ILO Briefing Note for Workers and Employers 25 August 2014 (update 5 September 2014) This briefing note is based on the existing WHO and ILO
Ebola Virus Disease: Occupational Safety and Health Joint WHO/ILO Briefing Note for Workers and Employers 25 August 2014 (update 5 September 2014) This briefing note is based on the existing WHO and ILO
Information for Primary Care: Managing patients who require assessment for Ebola virus disease Updated 17 Oct 2014
 Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
Infection Control Blood Borne Pathogens. Pines Behavioral Health
 Infection Control Blood Borne Pathogens Pines Behavioral Health Definition: Infection control is preventing the spread of germs that cause illness and infection. Infection control starts with understanding
Infection Control Blood Borne Pathogens Pines Behavioral Health Definition: Infection control is preventing the spread of germs that cause illness and infection. Infection control starts with understanding
Infection Prevention and Control Induction Program. GRICG May 2015
 Infection Prevention and Control Induction Program GRICG May 2015 What is an infection? An infection occurs when invading microorganisms cause ill health Viruses Bacteria Fungi Parasites Prions Pain, tenderness,
Infection Prevention and Control Induction Program GRICG May 2015 What is an infection? An infection occurs when invading microorganisms cause ill health Viruses Bacteria Fungi Parasites Prions Pain, tenderness,
USE OF PERSONAL PROTECTION EQUIPMENT. Standard and Isolation precautions Ana M. Bonet 6/2017
 USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Doc: 1.9. Course: Patient Safety Solutions. Topic: Infection prevention and control. Summary
 Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Modes of Transmission of Influenza A H1N1v and Transmission Based Precautions (TBPs)
 Modes of Transmission of Influenza A H1N1v and Transmission Based Precautions (TBPs) 8 January 2010 Version: 2.0 The information contained within this document is for the use of clinical and public health
Modes of Transmission of Influenza A H1N1v and Transmission Based Precautions (TBPs) 8 January 2010 Version: 2.0 The information contained within this document is for the use of clinical and public health
Guidelines for the Control of a Suspected or Confirmed Outbreak of Viral Gastroenteritis (Norovirus) in an Assisted Living Facility or Nursing Home
 Guidelines for the Control of a Suspected or Confirmed Outbreak of Viral Gastroenteritis (Norovirus) in an Assisted Living Facility or Nursing Home The following is a summary of guidelines developed to
Guidelines for the Control of a Suspected or Confirmed Outbreak of Viral Gastroenteritis (Norovirus) in an Assisted Living Facility or Nursing Home The following is a summary of guidelines developed to
Prevention and Control of Healthcare-Associated Norovirus
 Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
Chapter 12. Preventing Infection. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Infection Control. Chapter 11 Intro to HST
 Infection Control Chapter 11 Intro to HST All health care workers must understand basic infection control Key terms Pathogen: germ Microorganism: small, living organism that is not visible to the naked
Infection Control Chapter 11 Intro to HST All health care workers must understand basic infection control Key terms Pathogen: germ Microorganism: small, living organism that is not visible to the naked
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT
 AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red
 Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red In this document: Summary Key Messages Ebola Cases and Deaths (West Africa) Ebola in U.S. Health Workers (in Liberia)
Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red In this document: Summary Key Messages Ebola Cases and Deaths (West Africa) Ebola in U.S. Health Workers (in Liberia)
Chapter 11 PREVENTING INFECTION. Elsevier items and derived items 2010 by Mosby, Inc. an affiliate of Elsevier Inc. All rights reserved
 Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
8. Infection Prevention And Control
 PATIENT SAFETY 436 TEAM 8. Infection Prevention And Control Objectives: List The Modes Of Infection Transmission In Health-care Settings Explain Main Causes And Types Of Health Care-associated Infection
PATIENT SAFETY 436 TEAM 8. Infection Prevention And Control Objectives: List The Modes Of Infection Transmission In Health-care Settings Explain Main Causes And Types Of Health Care-associated Infection
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS
 INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
Chapter 13. Preventing Infection. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
CDC Health Advisory 04/29/2009
 H1N1 (Swine Flu) is a sub-type of Influenza A. Wexford Labs disinfectants are effective against Influenza A. Current CDC Recommendations for Environmental Control in the Healthcare Setting: CDC Health
H1N1 (Swine Flu) is a sub-type of Influenza A. Wexford Labs disinfectants are effective against Influenza A. Current CDC Recommendations for Environmental Control in the Healthcare Setting: CDC Health
Infection Control Update
 Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
Infectious Disease Control Oi Orientation. Providence Health & Services
 Infectious Disease Control Oi Orientation ti Providence Health & Services Infection Control Who is at risk of infection & why? Exposures and Outcomes What tools do we use to reduce risk? Surveillance Analysis
Infectious Disease Control Oi Orientation ti Providence Health & Services Infection Control Who is at risk of infection & why? Exposures and Outcomes What tools do we use to reduce risk? Surveillance Analysis
EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers
 EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers VERSION 2 Interim Guidelines for Evaluation of US Patients Suspected of Having Ebola Virus Disease (EVD) This is a rapidly
EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers VERSION 2 Interim Guidelines for Evaluation of US Patients Suspected of Having Ebola Virus Disease (EVD) This is a rapidly
Infection Control Precautions during the Clinical Management of Injecting Drug Users with Possible, Probable or Confirmed Anthrax
 Infection Control Precautions during the Clinical Management of Injecting Drug Users with Possible, Probable or Confirmed Anthrax (Adapted from guidance developed by Health Protection Scotland and HPA
Infection Control Precautions during the Clinical Management of Injecting Drug Users with Possible, Probable or Confirmed Anthrax (Adapted from guidance developed by Health Protection Scotland and HPA
Guideline for Infection Prevention at Medical Facilities
 Guideline for Infection Prevention at Medical Facilities March 26, 2007 Pandemic Influenza Experts Advisory Committee 129 130 Pandemic Influenza Preparedness Guidelines (From Phase 4 Onwards) Guidelines
Guideline for Infection Prevention at Medical Facilities March 26, 2007 Pandemic Influenza Experts Advisory Committee 129 130 Pandemic Influenza Preparedness Guidelines (From Phase 4 Onwards) Guidelines
June 4, Page 1 of 5 POLICY STATEMENT
 POLICY STATEMENT This policy has been written to inform all staff, clients, relatives and other visitors to the homes of service users about the risks associated with MRSA, AIDS and HIV hazards in the
POLICY STATEMENT This policy has been written to inform all staff, clients, relatives and other visitors to the homes of service users about the risks associated with MRSA, AIDS and HIV hazards in the
SARS Infection Control in Healthcare Settings
 SARS Infection Control in Healthcare Settings William A. Rutala, Ph.D., M.P.H. University of North Carolina (UNC) Hospitals and UNC School of Medicine Infection Control Considerations Hospitals must protect
SARS Infection Control in Healthcare Settings William A. Rutala, Ph.D., M.P.H. University of North Carolina (UNC) Hospitals and UNC School of Medicine Infection Control Considerations Hospitals must protect
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
"BLOODBORNE PATHOGENS IN COMMERCIAL AND LIGHT INDUSTRIAL FACILITIES"
 MAJOR PROGRAM POINTS "BLOODBORNE PATHOGENS IN COMMERCIAL AND LIGHT INDUSTRIAL FACILITIES" Training for THE OSHA BLOODBORNE PATHOGENS STANDARD Quality Safety and Health Products, for Today... and Tomorrow
MAJOR PROGRAM POINTS "BLOODBORNE PATHOGENS IN COMMERCIAL AND LIGHT INDUSTRIAL FACILITIES" Training for THE OSHA BLOODBORNE PATHOGENS STANDARD Quality Safety and Health Products, for Today... and Tomorrow
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION
 TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
12 June The average EVD case fatality rate has been around 50 per cent.
 12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
Diseases that are commonly transmitted by exposure to blood. Most common are: Hepatitis B and C HIV
 Diseases that are commonly transmitted by exposure to blood Most common are: Hepatitis B and C HIV applies to all persons who may reasonably anticipate contact with blood or other potentially infectious
Diseases that are commonly transmitted by exposure to blood Most common are: Hepatitis B and C HIV applies to all persons who may reasonably anticipate contact with blood or other potentially infectious
Clinical Aspects Fever (94%), cough (92%), sore throat (66%) 25% diarrhea and 25% vomiting Around 9% requiring i hospitalization ti Age groups: only 5
 Novel H1N1 Influenza June 19, 2009 CHICA Manitoba Evelyn Lo H1N1-the story In April of 2009, CDC was alerted to 2 children in California with a novel strain of H1N1 influenza At about the same time, Mexico
Novel H1N1 Influenza June 19, 2009 CHICA Manitoba Evelyn Lo H1N1-the story In April of 2009, CDC was alerted to 2 children in California with a novel strain of H1N1 influenza At about the same time, Mexico
APPLIED EDUCATIONAL SYSTEMS. Infection Control. Health Science and Technology Education. Table of Contents
 Infection Control and Technology Education Microorganisms Microorganisms are small living bodies that are not visible to the naked eye. Nonpathogens - maintain body processes Pathogens cause infection
Infection Control and Technology Education Microorganisms Microorganisms are small living bodies that are not visible to the naked eye. Nonpathogens - maintain body processes Pathogens cause infection
Bloodborne Pathogens Training. July 26, 2012
 Bloodborne Pathogens Training July 26, 2012 Introduction As sure as the sun comes up every day, children end up with scraped knees, cuts, and bruises. Students of all ages hurt themselves on the playground,
Bloodborne Pathogens Training July 26, 2012 Introduction As sure as the sun comes up every day, children end up with scraped knees, cuts, and bruises. Students of all ages hurt themselves on the playground,
Universal Precautions
 Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM
 Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Infection Prevention and Control - General Orientation
 Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Viral or Suspected Viral Gastroenteritis Outbreaks
 Viral or Suspected Viral Gastroenteritis Outbreaks Information for Directors and Staff of Early Childhood Education and Care Services Introduction Gastroenteritis outbreaks in early childhood education
Viral or Suspected Viral Gastroenteritis Outbreaks Information for Directors and Staff of Early Childhood Education and Care Services Introduction Gastroenteritis outbreaks in early childhood education
At the end of this session, the participants will be able to:
 At the end of this session, the participants will be able to: Verbalize definitions related to infection control List modes of transmission of infections and portals of entry of bacteria Explain universal
At the end of this session, the participants will be able to: Verbalize definitions related to infection control List modes of transmission of infections and portals of entry of bacteria Explain universal
Pandemic Influenza Infection Control Measures
 NHS Greater Glasgow & Clyde Partnerships Pandemic Influenza Infection Control Measures Guidance for Community Staff April 2009 Introduction This presentation aims to provide you with the key information
NHS Greater Glasgow & Clyde Partnerships Pandemic Influenza Infection Control Measures Guidance for Community Staff April 2009 Introduction This presentation aims to provide you with the key information
INFECTION CONTROL ADVICE:
 INFECTION CONTROL ADVICE: Severe Respiratory Illness from novel or emerging pathogens e.g Middle East Respiratory Syndrome Coronavirus (MERS-CoV) and Avian influenza (e.g. A/H7N9, A/H5N1) June 2015 Version:
INFECTION CONTROL ADVICE: Severe Respiratory Illness from novel or emerging pathogens e.g Middle East Respiratory Syndrome Coronavirus (MERS-CoV) and Avian influenza (e.g. A/H7N9, A/H5N1) June 2015 Version:
Ebola Virus Patient Advisory
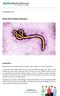 22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
Health care workers (HCWs) caring for suspected (clinically diagnosed) or confirmed cases of. Influenza A(H1N1)v FREQUENTLY ASKED QUESTIONS
 Health care workers (HCWs) caring for suspected (clinically diagnosed) or confirmed cases of Questions found here: FREQUENTLY ASKED QUESTIONS What is pandemic flu? What is the difference between seasonal
Health care workers (HCWs) caring for suspected (clinically diagnosed) or confirmed cases of Questions found here: FREQUENTLY ASKED QUESTIONS What is pandemic flu? What is the difference between seasonal
UTSW/BioTel EMS TRAINING BULLETIN October EMS TB Ebola Virus Disease (EVD)
 UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
Summary of current outbreak in Guinea, Liberia and Sierra Leone
 ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
Infection Prevention Special Needs Shelters. Jacqueline Whitaker RN MS LHRM CPHQ CIC FAPIC
 Infection Prevention Special Needs Shelters Jacqueline Whitaker RN MS LHRM CPHQ CIC FAPIC Infection Prevention: Objectives and Your Role Know the client population and its impact on the special needs shelter
Infection Prevention Special Needs Shelters Jacqueline Whitaker RN MS LHRM CPHQ CIC FAPIC Infection Prevention: Objectives and Your Role Know the client population and its impact on the special needs shelter
Bloodborne Pathogen Refresher Training
 Bloodborne Pathogen Refresher Training This program will review your occupational risks and the steps that you and the County must take to reduce your risks of exposure. Employees must report any occupational
Bloodborne Pathogen Refresher Training This program will review your occupational risks and the steps that you and the County must take to reduce your risks of exposure. Employees must report any occupational
Standard Precautions & Mercury Spill Management. Dr. Richa Mishra, Assistant Professor Dept, of Microbiology SGPGIMS, Lucknow
 Standard Precautions & Mercury Spill Management Dr. Richa Mishra, Assistant Professor Dept, of SGPGIMS, Lucknow OVERVIEW Briefly 3 Components, Hand hygiene Needle stick injury Personal protective equipment
Standard Precautions & Mercury Spill Management Dr. Richa Mishra, Assistant Professor Dept, of SGPGIMS, Lucknow OVERVIEW Briefly 3 Components, Hand hygiene Needle stick injury Personal protective equipment
MARITIME AUTHORITY OF JAMAICA EBOLA VIRUS DISEASE TO: (I) (II) ALL MANAGERS AND OPERATORS OF JAMAICAN REGISTERED VESSELS (III)
 MARITIME AUTHORITY OF JAMAICA EBOLA VIRUS DISEASE Circular No. 14-10-10 p Revision 00 Page (s) 1of 3 TO: (I) ALL OWNERS, MASTERS OF JAMAICAN REGISTERED VESSELS (II) ALL MANAGERS AND OPERATORS OF JAMAICAN
MARITIME AUTHORITY OF JAMAICA EBOLA VIRUS DISEASE Circular No. 14-10-10 p Revision 00 Page (s) 1of 3 TO: (I) ALL OWNERS, MASTERS OF JAMAICAN REGISTERED VESSELS (II) ALL MANAGERS AND OPERATORS OF JAMAICAN
CHAPTER 7 Medical/Surgical Asepsis and Infection Control
 CHAPTER 7 Medical/Surgical Asepsis and Infection Control 1 Slide 1 Microorganisms Microscopic. Naturally present on and in the human body and environment. Some microorganisms (pathogens) cause specific
CHAPTER 7 Medical/Surgical Asepsis and Infection Control 1 Slide 1 Microorganisms Microscopic. Naturally present on and in the human body and environment. Some microorganisms (pathogens) cause specific
Figure 1: Ebola Virus strengthens the framework for a scaled-up response.
 A n insight into ebola virus The outbreak of Ebola virus disease in West Africa continues to escalate, with 2615 cases and 1427 deaths reported from Guinea, Liberia, Nigeria, and Sierra Leone. Extensive
A n insight into ebola virus The outbreak of Ebola virus disease in West Africa continues to escalate, with 2615 cases and 1427 deaths reported from Guinea, Liberia, Nigeria, and Sierra Leone. Extensive
CHEROKEE COUNTY SCHOOL DISTRICT
 For Protection against Infectious Diseases Universal Precautions refers to a set of basic procedures designed to protect against infectious diseases that are transferred by blood and body fluids. Using
For Protection against Infectious Diseases Universal Precautions refers to a set of basic procedures designed to protect against infectious diseases that are transferred by blood and body fluids. Using
Infection Control Sec. 1, Unit 5 Part 1
 Infection Control Sec. 1, Unit 5 Part 1 Introduction Infections are a significant cause of illness, disease and death for residents that reside in certain living situations including nursing facilities.
Infection Control Sec. 1, Unit 5 Part 1 Introduction Infections are a significant cause of illness, disease and death for residents that reside in certain living situations including nursing facilities.
LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE
 LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE For Residents & Instructors ggbha.org Updated 6/18/2018 This learning module must be reviewed by residents
LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE For Residents & Instructors ggbha.org Updated 6/18/2018 This learning module must be reviewed by residents
Marburg virus disease
 Marburg virus disease Fact sheet available at http://www.who.int/mediacentre/factsheets/fs_marburg/en/ Updated 20 October 2017 Key facts Marburg virus disease (MVD), formerly known as Marburg haemorrhagic
Marburg virus disease Fact sheet available at http://www.who.int/mediacentre/factsheets/fs_marburg/en/ Updated 20 October 2017 Key facts Marburg virus disease (MVD), formerly known as Marburg haemorrhagic
Bloodborne Pathogens Training For School Personnel
 Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
OBJECTIVES PEOPLE AS RESERVOIRS. Reservoir
 Module C EPIDEMIOLOGY AND RISK OF INFECTION IN OUTPATIENT SETTINGS Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine OBJECTIVES Discuss the infectious process Review
Module C EPIDEMIOLOGY AND RISK OF INFECTION IN OUTPATIENT SETTINGS Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine OBJECTIVES Discuss the infectious process Review
Under Secretary of Ministry of Health. Authorized by: State of Kuwait Ministry of Health Infection Control Directorate
 State of Kuwait Ministry of Health Infection Control Directorate Title: Infection Control Guidelines within Healthcare Settings When Caring for Confirmed Cases, Probable Cases, and Cases Under Investigations
State of Kuwait Ministry of Health Infection Control Directorate Title: Infection Control Guidelines within Healthcare Settings When Caring for Confirmed Cases, Probable Cases, and Cases Under Investigations
EBOLA PREVENTION **For Extensive Procedures, Refer to Avmor's Ebola Pandemic Presentation
 EBOLA PREVENTION **For Extensive Procedures, Refer to Avmor's Ebola Pandemic Presentation PROTECTIVE GEAR 1 Be sure environmental services staff wear recommended personal protective equipment including,
EBOLA PREVENTION **For Extensive Procedures, Refer to Avmor's Ebola Pandemic Presentation PROTECTIVE GEAR 1 Be sure environmental services staff wear recommended personal protective equipment including,
MODULE B. Objectives. Infection Prevention. Infection Prevention. N.C. Nurse Aide I Curriculum
 DHSR/HCPR/CARE NAT I Curriculum - July 2013 1 N.C. Nurse Aide I Curriculum MODULE B Infection Prevention Objectives Relate the chain of infection to the work of a nurse aide in long-term care facilities.
DHSR/HCPR/CARE NAT I Curriculum - July 2013 1 N.C. Nurse Aide I Curriculum MODULE B Infection Prevention Objectives Relate the chain of infection to the work of a nurse aide in long-term care facilities.
ANNEX I: INFECTION CONTROL GUIDELINES FOR PANDEMIC INFLUENZA MANAGEMENT
 ANNEX I: INFECTION CONTROL GUIDELINES FOR PANDEMIC INFLUENZA MANAGEMENT During an influenza pandemic, adherence to infection control practices is extremely important to prevent transmission of influenza.
ANNEX I: INFECTION CONTROL GUIDELINES FOR PANDEMIC INFLUENZA MANAGEMENT During an influenza pandemic, adherence to infection control practices is extremely important to prevent transmission of influenza.
Infection Prevention and Control (IPC)
 Infection Prevention and Control (IPC) Standard Operating Procedure for CHICKENPOX (VARICELLA ZOSTER VIRUS) in a healthcare setting WARNING This document is uncontrolled when printed. Check local intranet
Infection Prevention and Control (IPC) Standard Operating Procedure for CHICKENPOX (VARICELLA ZOSTER VIRUS) in a healthcare setting WARNING This document is uncontrolled when printed. Check local intranet
Bloodborne Pathogens For School Employees
 Bloodborne Pathogens For School Employees Waynesboro Public Schools Bloodborne Pathogens Training and Annual Review Created on May 5, 2010 Reviewed/Revised April 6, 2017 Introduction In an educational
Bloodborne Pathogens For School Employees Waynesboro Public Schools Bloodborne Pathogens Training and Annual Review Created on May 5, 2010 Reviewed/Revised April 6, 2017 Introduction In an educational
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Hepatitis B is a virus that attacks the liver. It is highly infectious. Hepatitis B is transmitted primarily
 BLOOD BORNE PATHOGENS TRAINING FOR SCHOOL STAFF Blood Borne Pathogen (BBP): A blood borne pathogen is defined as an organism found in human blood or other infected body fluids that may cause disease in
BLOOD BORNE PATHOGENS TRAINING FOR SCHOOL STAFF Blood Borne Pathogen (BBP): A blood borne pathogen is defined as an organism found in human blood or other infected body fluids that may cause disease in
SUBJECT: Management of Human Body Fluids/Waste (Bloodborne Pathogens)
 Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
Bloodborne Pathogens in the Workplace
 Bloodborne Pathogens in the Workplace 1 What Are Bloodborne Pathogens? They are viruses, bacteria, and other microorganisms that: Are carried in a person s bloodstream Cause disease If a person comes in
Bloodborne Pathogens in the Workplace 1 What Are Bloodborne Pathogens? They are viruses, bacteria, and other microorganisms that: Are carried in a person s bloodstream Cause disease If a person comes in
Infection Prevention and Control Annual Education Authored by: Infection Prevention and Control Department
 Infection Prevention and Control Annual Education 2017 Authored by: Infection Prevention and Control Department Objectives After you complete this Computer-Based Learning (CBL) module, you should be able
Infection Prevention and Control Annual Education 2017 Authored by: Infection Prevention and Control Department Objectives After you complete this Computer-Based Learning (CBL) module, you should be able
Infection Control Recommendations on Avian Influenza A (H7N9) ICB / CHP
 Infection Control Recommendations on Avian Influenza A (H7N9) ICB / CHP As of 23 rd April 2013 No. of Confirmed Case: 108 No. of death: 22 Report Area First Report Date No. of confirmed case No. of death
Infection Control Recommendations on Avian Influenza A (H7N9) ICB / CHP As of 23 rd April 2013 No. of Confirmed Case: 108 No. of death: 22 Report Area First Report Date No. of confirmed case No. of death
2017 Infection Prevention and Control/Flu/TB/Basics Test Answer Key
 Name: School: Instructor: Date: 2017 Infection Prevention and Control/Flu/TB/Basics Test Answer Key For questions about this test, contact Infection Prevention and Control at 678-312-3308. 1. When do you
Name: School: Instructor: Date: 2017 Infection Prevention and Control/Flu/TB/Basics Test Answer Key For questions about this test, contact Infection Prevention and Control at 678-312-3308. 1. When do you
Avian Influenza (H5N1)
 State of Kuwait Ministry of Health Infection Control Directorate Avian Influenza (H5N1) Infection Control Emergency Plan & Guidelines For health care facilities 2005 Influenza A (H5N1) Infection Control
State of Kuwait Ministry of Health Infection Control Directorate Avian Influenza (H5N1) Infection Control Emergency Plan & Guidelines For health care facilities 2005 Influenza A (H5N1) Infection Control
PHYSICIAN PRACTICE ENHANCEMENT PROGRAM Assessment Standards. Infection Prevention and Control: Infection Prevention and Control Fundamentals
 PHYSICIAN PRACTICE ENHANCEMENT PROGRAM Assessment Standards : Fundamentals PHYSICIAN PRACTICE ENHANCEMENT PROGRAM Assessment Standards 2016 INFECTION PREVENTION AND CONTROL FUNDAMENTALS Infection prevention
PHYSICIAN PRACTICE ENHANCEMENT PROGRAM Assessment Standards : Fundamentals PHYSICIAN PRACTICE ENHANCEMENT PROGRAM Assessment Standards 2016 INFECTION PREVENTION AND CONTROL FUNDAMENTALS Infection prevention
This SOP applies to all staff employed by NHS Greater Glasgow & Clyde and locum staff on fixed term contracts and volunteer staff.
 Page 1 of 8 SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients clinical
Page 1 of 8 SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients clinical
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens. At School
 Bloodborne Pathogens At School Introduction What are bloodborne pathogens? What diseases do they cause? How do you protect yourself from being exposed? With a little knowledge, you can guard your health
Bloodborne Pathogens At School Introduction What are bloodborne pathogens? What diseases do they cause? How do you protect yourself from being exposed? With a little knowledge, you can guard your health
Blood Borne Pathogen Training For Employees of Shawnee Schools Prepared by Elaine Troyer, RN
 Blood Borne Pathogen Training For Employees of Shawnee Schools Prepared by Elaine Troyer, RN As an employee of a school, it s probably not one of the challenges that you signed on for, but unfortunately
Blood Borne Pathogen Training For Employees of Shawnee Schools Prepared by Elaine Troyer, RN As an employee of a school, it s probably not one of the challenges that you signed on for, but unfortunately
Bloodborne Pathogens
 Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Ebola. Wessex CPD Event 14/11/14. Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre Tel:
 Ebola Wessex CPD Event 14/11/14 Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre wessex@phe.gov.uk Tel: 0345 055 2022 Outline Background About the current outbreak Situation in the UK Clinical management
Ebola Wessex CPD Event 14/11/14 Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre wessex@phe.gov.uk Tel: 0345 055 2022 Outline Background About the current outbreak Situation in the UK Clinical management
CDC Ebola Response Team
 Ebola Preparations from the Healthcare Epidemiologists Perspective August 25th, 2014 CDC Ebola Response Team Barbara Knust, DVM, MPH Epidemiology Team Lead Tim Uyeki, MD Clinical Team Lead Nancy Cornish,
Ebola Preparations from the Healthcare Epidemiologists Perspective August 25th, 2014 CDC Ebola Response Team Barbara Knust, DVM, MPH Epidemiology Team Lead Tim Uyeki, MD Clinical Team Lead Nancy Cornish,
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Confronting Ebola. Keeping NY patients and healthcare workers safe and healthy
 Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
IN THE KNOW. As scientists learn. Additional. This inservice will. In 1996, the CDC took. In the 1830's, parents.
 A Little History of Infection Control In the 1830's, parents protected their children from infections by having them wear a piece of leather across their chests. It was also believed that sunlight and
A Little History of Infection Control In the 1830's, parents protected their children from infections by having them wear a piece of leather across their chests. It was also believed that sunlight and
Bloodborne Pathogens 29 CFR
 Bloodborne Pathogens 29 CFR 1910.1030 Revised OSHA Bloodborne Pathogens Compliance Directive (CPL2-2.44D) Could You Contract a Disease at Work? Administering first aid? Cleaning the restrooms? Using a
Bloodborne Pathogens 29 CFR 1910.1030 Revised OSHA Bloodborne Pathogens Compliance Directive (CPL2-2.44D) Could You Contract a Disease at Work? Administering first aid? Cleaning the restrooms? Using a
Infection Control 2.5 Contact Hours Presented by: CEU Professor
 Infection Control 2.5 Contact Hours Presented by: CEU Professor www.ceuprofessoronline.com Copyright 2009 The Magellan Group, LLC. All Rights Reserved. Reproduction and distribution of these materials
Infection Control 2.5 Contact Hours Presented by: CEU Professor www.ceuprofessoronline.com Copyright 2009 The Magellan Group, LLC. All Rights Reserved. Reproduction and distribution of these materials
Folks: The attached information is just in from DOH. The highlights:
 Folks: The attached information is just in from DOH. The highlights: ALL ILI (influenza-like illness) should be considered to be flu. It doesn't matter if it's H1N1, or some other strain. It all spreads
Folks: The attached information is just in from DOH. The highlights: ALL ILI (influenza-like illness) should be considered to be flu. It doesn't matter if it's H1N1, or some other strain. It all spreads
STANDARD OPERATING PROCEDURE #714 USE OF MPTP IN NHPS
 STANDARD OPERATING PROCEDURE #714 USE OF MPTP IN NHPS 1. PURPOSE This Standard Operating Procedure (SOP) describes the guidelines for the use of 1-methyl-4-phenyl-1,2,3,6- tetrahydropyridine (MPTP) in
STANDARD OPERATING PROCEDURE #714 USE OF MPTP IN NHPS 1. PURPOSE This Standard Operating Procedure (SOP) describes the guidelines for the use of 1-methyl-4-phenyl-1,2,3,6- tetrahydropyridine (MPTP) in
