INFECTION CONTROL GUIDELINES _FOR MANAGEMENT OF SUSPECTED OR CONFIRMED EBOLA VIRUS DISEASE (EVD) 8 August 2014
|
|
|
- Sherman Copeland
- 5 years ago
- Views:
Transcription
1 INFECTION CONTROL GUIDELINES _FOR MANAGEMENT OF SUSPECTED OR CONFIRMED EBOLA VIRUS DISEASE (EVD) 8 August 2014
2 I T ABLE OF CONTENTS NO. TITLE PAGE I Introduction. 3 II Background. 3 III Case definition. 4 IV Laboratory Diagnosis 4 V Patient Placement. S VI Personal Protective Equipment (PPF). 5 I VII Patient Care Equipment. 6 Vin Patient Care Consid~rations. 6 IX Aerosol Generating Procedures (AGPs). 6 - X Environmental 1 nfection Control. 7 Xl SaCe Injection practices. 7 XII Duration of Infection Control Precautions. 7 XIII Monitoring and Management of Potentially Exposed 8 Healthcare Workers (HCWs). XIV Monitoring and Management ofpotentially Exposed Non- 8 HeaHhcare Workers (HeWs). XV Monitoring, Management, and Training of Visitors. 9 XVI Management or the deceased. 9 XVII References. 10 2
3 I. Introduction The Ministry of Health of Saudi Arabia has developed the following guidelines to meet the urgent need for up-to-date information and evidence-based recommendations for the safe care of patients with suspected or confinned Ebola virus disease (EVD) in healthcare facilities. The main bulk of the guidelines has been adapted from guidelines produced by the Centers for Disease Control and Prevention (CDC)[1-3] and the World Health Organization (WHO)[4]. Early recognition of EVD is critical for prompt implementation of infection control measures to prevent transmission ofthis contagious and deadly infection. II. Back round \4 Ebola virus disease (EVD), fonnerly known as Ebola haemorrhagic fever, is a severe, often fatal illness in humans that first appeared in 1976 in 2 simultaneous outbreaks, in Nzara, Sudan, and in Yambuku, Democratic Republic of Congo. The latter was in a village situated near the Ebola River, from which the disease takes its name. 4. The current EVD outbreak began in Guinea in December This outbreak now involves transmission in Guinea, Liberia, Sierra Leone, and lately Nigeria. As of 6 August 2014, the cumulative number of cases attributed to EVD in the four countries stands at 1779, including 961 deaths. The distribution and classification of the cases are as follows: Guinea, 495 cases (355 confirmed, 140 suspected), including 367 deaths; Liberia, 554 cases (148 confinned, and 406 suspected), including 294 deaths; Sierra Leone, 717 cases (631 confirmed, and 86 suspected), including 298 deaths; and Nigeria, 13 cases (0 confinned, and 13 suspected), including 2 deaths. This is currently the largest EVD outbreak ever recorded... EVD outbreaks have a case fatality rate of up to 900/0... EVD outbreaks occur primarily in remote villages in Central and West Africa, near tropical rainforests. ~ The virus is transmitted to people from wild animals and spreads in the human population through human-to-human transmission.,~ Fruit bats of the Pteropodidae family are considered to be the natural host of the Ebola virus.... Ebola is introduced into the human population tlu-ough close contact with the blood, secretions, organs or other bodily fluids of infected animals. In Africa, infection has been documented through the handling of infected chimpanzees, gorillas, fruit bats, monkeys, forest antelope and porcupines found ill or dead or in the rainforest. ~ Ebola then spreads in the community through human-to-human transmission, with infection resulting from direct contact (through broken skin or mucous membranes) with the blood, secretions, organs or other bodily fluids of infected people, and indirect contact with environments contaminated with such fluids. Burial ceremonies in which mourners have direct contact with the body of the deceased person can also playa role in the transmission of Ebola... Men who have recovered from the disease can still transmit the virus through their semen for up to 7 weeks after recovery from illness.... Severely ill patients require intensive supportive care. 3
4 .. No licensed specific treatment or vaccine is availabte for use in people or animals [II. Case Definition for Ebola Virus Disease (EVD) Suspected Case Illness in a person who has both consistent symptoms and risk factors as follows: Clinical criteria, which includes fever of greater than 38.6 o C, and additional symptoms such as severe headache, muscle pain, vomiting, diarrhea, abdomina] pain, or unexplained hemorrhage (gingival, nasal, cutaneous [petechiae, bruises, ecchymosis], gastrointestinal, rectal (gross or occult blood], urinary [gross or microscopic hematuria], vaginal, or puncture sites bleeding); AND Epidemiologic risk factors \vithin the past 3 weeks before the onset of symptoms, such as contact with blood or other body fluids of a patient known to have or suspected to have EVD; residence in-or travel to-an area where EVD transmission is active; or direct handling of dead or alive fruit bats, monkeys, chimpanzees, gorillas, forest antelope and porcupines from disease-endemic areas. Malaria diagnostics should also be a part of initial testing because it is a common cause of febrile illness in persons with a travel history to the affected countries. Confirmed Case A suspected case with laboratory-confirmed diagnostic evidence of Ebola virus infection. nosis. Laboratory tests to confirm EBV should only be performed in MOH-accredited laboratories and verified with a WHO-accredited reference laboratory. Extreme caution should be exercised in collecting, transporting, and shipping samples from EVD patients. To confirm EVD, blood samples from the patient should be collected in 2 types of tubes a) EDTA (CBC) blood tubes for the PCR test and viral isolation from plasma; and b) Plain tube (red-top) for antibody and antigen detection tests and viral isolation from serum. At least 2 EDT A and 2 plain tubes should be collected to be able to confirm the diagnosis in two independent laboratories. Please refer to the MOR Guidelines for Specimen Collection, Transport, Testing, and Submission for Patients with Suspected Infection with Ebala Virus Disease for details. 4
5 Laboratory tests used in diagnosis include: Within a few days after symptoms begin Antigen-capture enzyme-linked immunosorbent assay (ELISA) testing IgM ELISA Polymerase chain reaction (per) Virus isolation Later in disease course or after recovery Retrospectively in deceased patients IgM and IgG antibodies Immunohistochemistry testing per Virus isolation v. Patient Placement Isolation Units should be identified as EVD isolation units. These units should be able to function as a self-contained closed unit with no movement of patients in or out. Place the patient in a single room (containing a private bathroom) with the door closed Isolation units should maintain a log of all persons entering the patient's room Keep all routine supplies for patient care outside of the isolation room. Utilize isolation carts for extra supplies. Keep containers with decontamination solutions in the anteroom. Restrict entry to only those considered essential. Do not move patients in the isolation room/unit in or out unless absolutely necessary. Do not interchange staff in this area with other areas in the hospital. All persons entering the patient room should wear at least: o Gloves o Gown (fluid resistant or impenneable) o Eye protection (goggles or face shietd) o Face mask o Additional PPE might be required in certain situations (e.g., copious amounts of blood, other body fluids, vomit, or feces present in the environment), including but not limited to: Full body (overall) water-proof suit that covers the whole body from head to ankles. Double gloving Disposable shoe covers 5
6 Recommended PPE should be worn by Hews upon entry into patient rooms or care areas. ~pon exit fr.om the patient room or care area, PPE should be carefully removed and dtscarded Without contaminating one's eyes, mucous membranes, or clothing with potentially infectious materials. Hand hygiene should be perfonned immediately after removal of PPE. VII. Patient Care E ment Dedicated medical equipment (preferably disposable, when possible) should be used for the provision of patient care. All non-dedicated, non-disposable medical equipment used for patient care should be cleaned and disinfected according to manufacturer's instructions and hospital policies. VIII. Patient Care Considerations Limit the use of needles and other sharps as much as possible Phlebotomy, procedures, and laboratory testing should be limited to the minimum necessary for essential diagnostic evaluation and medical care All needles and sharps should be handled with extreme care and disposed in punctureproof, sealed containers IX. Aerosol Generatin Procedures AGPs) An aerosol-generating procedure (AGP) is defined as any medical procedure that can induce the production of aerosols of various sizes, including small «5 micron) particles. Aerosol-generating procedures that may be associated with an increased risk of infection transmission includes both elective procedures such as bronchoscopy, sputum induction, elective intubation and extubation, as well as emergency procedures such as cardiopulmonary resuscitation, initiation of Bile vel Positive Airway Pressure-BIPAP, emergency intubation, open suctioning of airways, manual ventilation via umbo bagging through a mask before intubation. Avoid AGPs for EVD patients. Additional precautions when performing aerosol-generating procedures: o Wear N95 masks -Every healthcare worker should wear a fit tested N95 mask (or an alternative respirator if fit testing failed e.g., powered air purifying respiratory or elastomeric respirator). Additionally, when putting on N95 mask, always check the seal. o Wear eye protection (i.e. goggles or a face shield that fully covers the front and sides ofthe face). o Wear a clean, non-sterile, long-sleeved water-proof gown and gloves (some ofthese procedures require sterile gloves). o Wear disposable shoe covers. 6
7 o Perform procedures in a negative pressure room. When a negative pressure room is not available, conduct the procedure in a private room. Room doors should be kept closed during the procedure except when entering or leaving the room, and entry and exit should be minimized during and shortly after the procedure. o Limit the number of persons present in the room to those essential for patient-care and support. o Perform hand hygiene before and after contact with the patient and his or her surroundings and after PPE removal. o Conduct environmental surface cleaning following procedures (see section below on environmental infection control). o If re-usable equipment or PPE (e.g. Powered air purifying respirator, elastomeric respirator, etc.) are used, they should be cleaned and disinfected according to manufacturer instructions and hospital policies. o Collection and handling of soiled re-usable respirators must be done by trained individuals using PPE as described above for routine patient care. x. Environmental Infection Control Diligent environmental cleaning and disinfection and safe handling of potentially contaminated materials is paramount, as blood, sweat, emesis, feces and other body secretions represent potentially infectious materials HeWs performing environmental cleaning and disinfection should wear recommended PPE (described above) and consider use of additional barriers (shoe and leg coverings, etc.) if needed. Face protection (face shield or facemask with goggles) should be worn when perfonning tasks such as liquid waste disposal that can generate splashes. Follow standard procedures, per hospital policy and manufacturers' instructions, for cleaning and/or disinfection of: o Environmental surfaces and equipment o Textiles and laundry o Food utensils and dishware ~I. Safe Il!iection Practices Facilities should follow safe injection practices as specified under Standard Precauti ons. Any injection equipment or parenteral medication container that enters the patient treatment area should be dedicated to that patient and disposed of at the point of use. XII. Duration of Infection Control Precautions Duration of precautions should be determined on a case-by-case basis. Factors that should be considered include, but are not limited to: presence of symptoms related to EVD, date symptoms resolved, other conditions that would require specific precautions (e.g., tuberculosis, Clostridium difficile) and available laboratory information 7
8 XIII. M,onitoring and Management of Potentially Exposed Healthcare Workers (HeWs Facilities should develop policies for monitoring and management of potentially exposed HCWs Perso~s with percut~eous or mucocutaneous exposures to blood, body fluids, secretions, or excretlons from a patient with suspected EVD should' o Stop working and im~edi~tely wash the affected skin surfaces with soa~ and water. Mucous mem?ranes (e.g., conjunctiva) should be irrigated with copious amounts ofwater or eyewash solution o Immediately contact occupational health/supervisor for assessment and access to postexposure.management services for al1 appropriate pathogens (e.g., Human ImmunodeficIency Virus, Hepatitis C, etc.) HCvy~ who. develop sudden onset of fever, intense weakness or muscle pains, vorni.hng, diarrhea, or any signs of hemorrhage after an unprotected expostrre (i,e. not weanng recommended PPE at the time ofpatient contact or through direct contact to blood or body fluids) to a patient with EVD should: o Not report to work or should immediately stop working o Notify their supervisor o Seek prompt medical evaluation and testing o Notify public health/infection control departments o Comply with work exclusion until they are deemed no longer infectious to others For asymptomatic HeWs who had an unprotected exposure (i.e. not wearing recommended PPE at the time of patient contact or through direct contact to blood or body fluids) to a patient with EVD: o Should receive medical evaluation and follow-up care including fever monitoring twice daily for 2l days after the last known exposure. o Hospitals should consider policies ensuring twice daily contact with exposed HeWs to discuss potential symptoms and document fever checks o May continue to work while receiving twice daily fever checks, based upon hospital policy and discussion with local, state, and federal public health authorities. o Asymptomatic HeWs are not allowed to travel by commercial conveyances (airplane, ship, and train), o Local travel for asymptomatic HCWs (e.g. taxi, bus) should be assessed in consultation with local public health authorities. XIV. Monitoring and Management of Potentially Exposed Non Healthcare Workers (NHCWs) in the Community The Department ofpublic Health in the Ministry of Health should identify and monitor all potentially exposed contacts who had close contact (within 1.5 meters) with a dead or alive patient after the onset of the patient's EVD illness. People who had close contact with the patient before the onset of his/her illness need not to be identified or monitored. Asymptomatic contacts should be contacted by the public health office at least once daily by phone for 21 days after the last contact to assess hislher health and this should be documented on daily basis in a logbook for each contact. The public health officer should inquire about any fever, intense weakness or muscle pains, vomiting, or 8
9 Olarrnea, ana aavlse Inose wno nave any U1 lnc~e ~ylllvluul~ LU LiUIUC; IUUUC;UlalGlY LV a hospital for evaluation. Contacts should be advised to check and document their temperatures twice daily for 21 days and notify the public health office ifthey develop any fever (temperature more than 37.20C) or other illness within the follow up period. Asymptomatic contacts may continue their daily activities and go out of their home (e.g. to work, school, or shopping). If they develop any illness, they should promptly seek medical advice. Asymptomatic contacts are not allowed to travel by commercial conveyances (airplane, ship, and train). Local travel for asymptomatic individuals (e.g. taxi, bus) should be assessed in consultation with local public health authorities. Patients who have recovered from EVD should abstain from sexual activity for 2 months after recovery. Avoid entry of visitors into the patient's room. Exceptions may be considered on a case by case basis for those who are essential for the patient's wellbeing. Establish procedures for monitoring managing and training visitors. Visits should be scheduled and controlled to allow for: o Screening for EVD (e.g., fever and other symptoms) before entering or upon arrival to the hospital o Evaluating risk to the health of the visitor and ability to comply with precautions o Providing instruction, before entry into the patient care area on hand hygiene, limiting surfaces touched, and use ofppe according to the current facility policy while in the patient's room o Visitor movement within the facility should be restricted to the patient care area and an immediately adjacent waiting area. XVI. Management of the Deceased Body washing must be done in the hospital. No washing can be done outside ofthe hospital setting Hews dealing with the body should wear gloves, a gown, disposable shoe covers, and either a face shield that fully covers the front and sides of the face or goggles, and N95 mask. Put the body in double fluid-resistant body bag. After placing the body in the first bag, disinfect the outer surface of the bag using a hospital-approved disinfectant before placing the body in a second bag and then disinfect the outer surface of the second bag. AJl equipment, table and counter surfaces, stretchers, body boards and transport trolleys must be cleaned after every patient using hospital-approved disinfectants. 9
10 x VII. Keterences 1. Infection Prevention and Control Recommendations for Hospitalized Patients with Known or Suspected Ebola Hemorrhagic Fever in U.S. Hospitals. CDC 1 August Available at: ons.h tm l. 2. Safe Management ofpatients with Ebala Virus Disease (EVD) in U.S. Hospitals. CDC 6 August Available at: 3. Interim Guidance for Monitoring and Movement ofpersons with Ebola Virus Disease Exposure. CDC 8 August Available at: 4. Interim Infection Control Recommendations for Care of Patients with Suspected or Confirmed Filovirus (Ebola, Marburg) Hemorrhagic Fever. BDP/EPRJWHO, Geneva March Available at: recommendations filovirus.pdf?ua= I. 10
Media centre Ebola virus disease
 1 of 6 10/15/2014 10:59 AM Media centre Ebola virus disease Fact sheet N 103 Updated September 2014 Key facts Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, is a severe, often fatal
1 of 6 10/15/2014 10:59 AM Media centre Ebola virus disease Fact sheet N 103 Updated September 2014 Key facts Ebola virus disease (EVD), formerly known as Ebola haemorrhagic fever, is a severe, often fatal
Genus Ebolavirus is 1 of 3 members of the Filoviridae family (filovirus), along with genus Marburgvirus and genus Cuevavirus.
 EBOLA VIRUS Ebola virus disease (EVD) is a severe, often fatal illness, with a case fatality rate of up to 90%. It is one of the world s most virulent diseases.the infection is transmitted by direct contact
EBOLA VIRUS Ebola virus disease (EVD) is a severe, often fatal illness, with a case fatality rate of up to 90%. It is one of the world s most virulent diseases.the infection is transmitted by direct contact
Provider Health & Safety Alert Ebola Virus Disease September 30, 2014
 Provider Health & Safety Alert Ebola Virus Disease September 30, 2014 With the announcement of the first confirmed case of Ebola Virus Disease (EVD) in Dallas Texas, there could be interactions with individuals
Provider Health & Safety Alert Ebola Virus Disease September 30, 2014 With the announcement of the first confirmed case of Ebola Virus Disease (EVD) in Dallas Texas, there could be interactions with individuals
Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red
 Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red In this document: Summary Key Messages Ebola Cases and Deaths (West Africa) Ebola in U.S. Health Workers (in Liberia)
Key Points Ebola Virus Disease, West Africa Newly updated information is indicated in red In this document: Summary Key Messages Ebola Cases and Deaths (West Africa) Ebola in U.S. Health Workers (in Liberia)
EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers
 EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers VERSION 2 Interim Guidelines for Evaluation of US Patients Suspected of Having Ebola Virus Disease (EVD) This is a rapidly
EBOLA VIRUS Guidance for Michigan local health departments and healthcare providers VERSION 2 Interim Guidelines for Evaluation of US Patients Suspected of Having Ebola Virus Disease (EVD) This is a rapidly
Ebola Virus Disease (EVD) Essential information
 Ebola Virus Disease (EVD) Essential information Ebola Virus Disease (EVD) Origins The Ebola virus is named after the Ebola River in what was Zaire (now Democratic Republic of Congo) where the first outbreak
Ebola Virus Disease (EVD) Essential information Ebola Virus Disease (EVD) Origins The Ebola virus is named after the Ebola River in what was Zaire (now Democratic Republic of Congo) where the first outbreak
UTSW/BioTel EMS TRAINING BULLETIN October EMS TB Ebola Virus Disease (EVD)
 UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
UTSW/BioTel EMS TRAINING BULLETIN October 2014 EMS TB 14-006 Ebola Virus Disease (EVD) Purpose: 1. To inform & provide management recommendations to UTSW/BioTel EMS System EMS Providers about Ebola Virus
Ebola Virus Patient Advisory
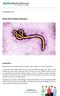 22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
22 September 2014 Ebola Virus Patient Advisory Introduction Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly
Questions and Answers on Ebola
 Updated: August 26, 2014 The 2014 Ebola outbreak is the largest Ebola outbreak in history and the first in West Africa. The current outbreak is affecting four countries in West Africa: Guinea, Liberia,
Updated: August 26, 2014 The 2014 Ebola outbreak is the largest Ebola outbreak in history and the first in West Africa. The current outbreak is affecting four countries in West Africa: Guinea, Liberia,
12 June The average EVD case fatality rate has been around 50 per cent.
 12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
12 June 2015 Ebola virus was first identified in Sudan and Zaire in 1976. It belongs to the family of Filoviridae. It causes Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever. EVD is
Ebola Virus Diseases
 CDC/Dr F A Murphy Frequently Asked Questions on Ebola Virus Diseases Frequently asked questions on Ebola virus disease World Health Organization 2014 All rights reserved. Requests for publications, or
CDC/Dr F A Murphy Frequently Asked Questions on Ebola Virus Diseases Frequently asked questions on Ebola virus disease World Health Organization 2014 All rights reserved. Requests for publications, or
Ebola Virus Disease. Global Epidemiology and Surveillance in Hong Kong. as of 13 August 2014
 Ebola Virus Disease Global Epidemiology and Surveillance in Hong Kong as of 13 August 2014 Ebola Virus Disease (EVD) Ebola virus disease (EVD), (formerly known as Ebola haemorrhagic fever) is a severe,
Ebola Virus Disease Global Epidemiology and Surveillance in Hong Kong as of 13 August 2014 Ebola Virus Disease (EVD) Ebola virus disease (EVD), (formerly known as Ebola haemorrhagic fever) is a severe,
Ebola Virus Disease: Occupational Safety and Health
 Ebola Virus Disease: Occupational Safety and Health Joint WHO/ILO Briefing Note for Workers and Employers 25 August 2014 (update 5 September 2014) This briefing note is based on the existing WHO and ILO
Ebola Virus Disease: Occupational Safety and Health Joint WHO/ILO Briefing Note for Workers and Employers 25 August 2014 (update 5 September 2014) This briefing note is based on the existing WHO and ILO
saipem Ebola virus diseases EVD August 2014
 Ebola virus diseases EVD August 2014 Why Ebola generates such fear? Ebola is one of the world's most deadly diseases. It can kill up to 90% of people who developed Ebola virus disease. There is not treatment
Ebola virus diseases EVD August 2014 Why Ebola generates such fear? Ebola is one of the world's most deadly diseases. It can kill up to 90% of people who developed Ebola virus disease. There is not treatment
Summary of current outbreak in Guinea, Liberia and Sierra Leone
 ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
ALERT TO HEALTHCARE WORKERS: EBOLA VIRUS DISEASE OUTBREAK IN GUINEA, LIBERIA AND SIERRA LEONE, WEST AFRICA 04 April 2014 Summary of current outbreak in Guinea, Liberia and Sierra Leone In this update and
Confronting Ebola. Keeping NY patients and healthcare workers safe and healthy
 Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
Figure 1: Ebola Virus strengthens the framework for a scaled-up response.
 A n insight into ebola virus The outbreak of Ebola virus disease in West Africa continues to escalate, with 2615 cases and 1427 deaths reported from Guinea, Liberia, Nigeria, and Sierra Leone. Extensive
A n insight into ebola virus The outbreak of Ebola virus disease in West Africa continues to escalate, with 2615 cases and 1427 deaths reported from Guinea, Liberia, Nigeria, and Sierra Leone. Extensive
EBOLA FACTS. During this outbreak, most of the disease has spread through human-to-human transmission.
 EBOLA FACTS Ebola virus disease (formerly known as Ebola haemorrhagic fever) is a severe and often fatal illness, with a fatality rate of up to 90%. It is one of the world s most dreaded diseases. However,
EBOLA FACTS Ebola virus disease (formerly known as Ebola haemorrhagic fever) is a severe and often fatal illness, with a fatality rate of up to 90%. It is one of the world s most dreaded diseases. However,
Marburg virus disease
 Marburg virus disease Fact sheet available at http://www.who.int/mediacentre/factsheets/fs_marburg/en/ Updated 20 October 2017 Key facts Marburg virus disease (MVD), formerly known as Marburg haemorrhagic
Marburg virus disease Fact sheet available at http://www.who.int/mediacentre/factsheets/fs_marburg/en/ Updated 20 October 2017 Key facts Marburg virus disease (MVD), formerly known as Marburg haemorrhagic
CDC Health Advisory 04/29/2009
 H1N1 (Swine Flu) is a sub-type of Influenza A. Wexford Labs disinfectants are effective against Influenza A. Current CDC Recommendations for Environmental Control in the Healthcare Setting: CDC Health
H1N1 (Swine Flu) is a sub-type of Influenza A. Wexford Labs disinfectants are effective against Influenza A. Current CDC Recommendations for Environmental Control in the Healthcare Setting: CDC Health
Ebola. Wessex CPD Event 14/11/14. Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre Tel:
 Ebola Wessex CPD Event 14/11/14 Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre wessex@phe.gov.uk Tel: 0345 055 2022 Outline Background About the current outbreak Situation in the UK Clinical management
Ebola Wessex CPD Event 14/11/14 Dr Ishani Kar-Purkayastha, CCDC, Wessex PHE Centre wessex@phe.gov.uk Tel: 0345 055 2022 Outline Background About the current outbreak Situation in the UK Clinical management
Chapter 12. Preventing Infection. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Chapter 12 Preventing Infection Infection Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from
Chapter 11 PREVENTING INFECTION. Elsevier items and derived items 2010 by Mosby, Inc. an affiliate of Elsevier Inc. All rights reserved
 Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
Chapter 11 PREVENTING INFECTION Infection is a major safety and health hazard. The health team follows certain practices and procedures to protect patients, residents, visitors, and staff from infection.
Chapter 13. Preventing Infection. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
Chapter 13 Preventing Infection Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 13.1 Define the key terms and key abbreviations in this chapter. Identify what microbes need to live and grow.
Modes of Transmission of Influenza A H1N1v and Transmission Based Precautions (TBPs)
 Modes of Transmission of Influenza A H1N1v and Transmission Based Precautions (TBPs) 8 January 2010 Version: 2.0 The information contained within this document is for the use of clinical and public health
Modes of Transmission of Influenza A H1N1v and Transmission Based Precautions (TBPs) 8 January 2010 Version: 2.0 The information contained within this document is for the use of clinical and public health
CDC Ebola Response Team
 Ebola Preparations from the Healthcare Epidemiologists Perspective August 25th, 2014 CDC Ebola Response Team Barbara Knust, DVM, MPH Epidemiology Team Lead Tim Uyeki, MD Clinical Team Lead Nancy Cornish,
Ebola Preparations from the Healthcare Epidemiologists Perspective August 25th, 2014 CDC Ebola Response Team Barbara Knust, DVM, MPH Epidemiology Team Lead Tim Uyeki, MD Clinical Team Lead Nancy Cornish,
TRAVEL ADVISORY TO PREVENT THE IMPORTATION OF EBOLA INTO SOUTH AFRICA
 TRAVEL ADVISORY TO PREVENT THE IMPORTATION OF EBOLA INTO SOUTH AFRICA The purpose of this advisory is to notify travellers about the Ebola disease outbreak and inform them about preventative measures they
TRAVEL ADVISORY TO PREVENT THE IMPORTATION OF EBOLA INTO SOUTH AFRICA The purpose of this advisory is to notify travellers about the Ebola disease outbreak and inform them about preventative measures they
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING
 Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
Appendix C. RECOMMENDATIONS FOR INFECTION CONTROL IN THE HEALTHCARE SETTING Infection Control Principles for Preventing the Spread of Influenza The following infection control principles apply in any setting
CIRCULAR LETTER No
 CIRCULAR LETTER No 06-204 0.0.203 To: MASTER CREW MEMBERS 07 th August, 204 URGENT Due to the serious nature of the outbreak of the Ebola virus in West Africa, the following 5 safe precautions to be strictly
CIRCULAR LETTER No 06-204 0.0.203 To: MASTER CREW MEMBERS 07 th August, 204 URGENT Due to the serious nature of the outbreak of the Ebola virus in West Africa, the following 5 safe precautions to be strictly
Swine Flu. Background. Interim Recommendations. Infectious Period. Case Definitions for Infection with Swine-origin
 Page 1 of 5 Swine Flu Interim Guidance for Emergency Medical Services (EMS) Systems and 9-1-1 Public Safety Answering Points (PSAPs) for Management of Patients with Confirmed or Suspected Swine- Origin
Page 1 of 5 Swine Flu Interim Guidance for Emergency Medical Services (EMS) Systems and 9-1-1 Public Safety Answering Points (PSAPs) for Management of Patients with Confirmed or Suspected Swine- Origin
Information for Primary Care: Managing patients who require assessment for Ebola virus disease Updated 17 Oct 2014
 Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
Prevention and Control of Healthcare-Associated Norovirus
 Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
Purpose: Audience: Policy: To prevent healthcare-associated norovirus infections in patients, employees, contract workers, volunteers, visitors and students and to control and eradicate norovirus infections
EBOLA INFORMATION KIT 20 to 26 October 2014 MEMBERS NEWS HUNTING SERVICES FUND LEGISLATION CALENDAR GENERAL SHOP POPULAR ARTICLES
 HOME ABOUT PHASA MEMBERS NEWS HUNTING SERVICES FUND LEGISLATION CALENDAR GENERAL SHOP DOWNLOAD: PROFESSIONAL HUNTER STATUS SECTION 16A (click to download) DOWNLOADS NEWSLETTERS F.A.Q TWITTER FACEBOOK Home
HOME ABOUT PHASA MEMBERS NEWS HUNTING SERVICES FUND LEGISLATION CALENDAR GENERAL SHOP DOWNLOAD: PROFESSIONAL HUNTER STATUS SECTION 16A (click to download) DOWNLOADS NEWSLETTERS F.A.Q TWITTER FACEBOOK Home
Infection Prevention & Control
 Infection Prevention & Control are staffed at each Sentara Hospital to assist with any infection prevention & control issues or concerns: Sentara Albemarle Hospital 252-384-4141 Sentara Careplex Hospital
Infection Prevention & Control are staffed at each Sentara Hospital to assist with any infection prevention & control issues or concerns: Sentara Albemarle Hospital 252-384-4141 Sentara Careplex Hospital
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE
 PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
PANDEMIC INFLUENZA PHASE 6 INFECTION CONTROL RECOMMENDATIONS TEMPLATE (Updated September 7, 2006) Information and concept courtesy Of the San Francisco Public Health Department Table of Contents Pandemic
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
EDUCATIONAL COMMENTARY EMERGING INFECTIOUS DISEASES WITH GLOBAL IMPACT
 Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn CE Credits under Continuing Education on
Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn CE Credits under Continuing Education on
Infection Control Recommendations on Avian Influenza A (H7N9) ICB / CHP
 Infection Control Recommendations on Avian Influenza A (H7N9) ICB / CHP As of 23 rd April 2013 No. of Confirmed Case: 108 No. of death: 22 Report Area First Report Date No. of confirmed case No. of death
Infection Control Recommendations on Avian Influenza A (H7N9) ICB / CHP As of 23 rd April 2013 No. of Confirmed Case: 108 No. of death: 22 Report Area First Report Date No. of confirmed case No. of death
TRAVEL ADVISORY TO PREVENT THE IMPORTATION OF EBOLA INTO SOUTH AFRICA
 TRAVEL ADVISORY TO PREVENT THE IMPORTATION OF EBOLA INTO SOUTH AFRICA The purpose of this advisory is to notify travellers about the Ebola disease outbreak and inform them about preventative measures they
TRAVEL ADVISORY TO PREVENT THE IMPORTATION OF EBOLA INTO SOUTH AFRICA The purpose of this advisory is to notify travellers about the Ebola disease outbreak and inform them about preventative measures they
Infection Prevention and Control - General Orientation
 Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE
 LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE For Residents & Instructors ggbha.org Updated 6/18/2018 This learning module must be reviewed by residents
LEARNING MODULE: INFECTION CONTROL BLOODBORNE PATHOGENS ISOLATION PRECAUTIONS PHARMACEUTICAL WASTE For Residents & Instructors ggbha.org Updated 6/18/2018 This learning module must be reviewed by residents
Statements about Ebola: True or false? Part 1 Commented version for trainers only!
 Statements about Ebola: True or false? Part 1 Commented version for trainers only! The questions and answers are designed to revise key messages of the training. If necessary, you may adapt the questions
Statements about Ebola: True or false? Part 1 Commented version for trainers only! The questions and answers are designed to revise key messages of the training. If necessary, you may adapt the questions
What employees should know about UNIVERSAL PRECAUTIONS. They re work practices that help prevent contact with blood and certain other body fluids.
 What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
USE OF PERSONAL PROTECTION EQUIPMENT. Standard and Isolation precautions Ana M. Bonet 6/2017
 USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
USE OF PERSONAL PROTECTION EQUIPMENT Standard and Isolation precautions Ana M. Bonet 6/2017 Three principal elements required for an infection to occur: a source or reservoir, a susceptible host with a
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
The Ebola Virus. By Emilio Saavedra
 The Ebola Virus By Emilio Saavedra Etiological Agents: Ebolavirus is the etiologic agent. [1] There are four main families of viruses that are agents of Ebola (hemorrhagic fever). [1] These four families
The Ebola Virus By Emilio Saavedra Etiological Agents: Ebolavirus is the etiologic agent. [1] There are four main families of viruses that are agents of Ebola (hemorrhagic fever). [1] These four families
WHO SOUTHERN SUDAN HEALTH UPDATE May 2004
 WHO SOUTHERN SUDAN HEALTH UPDATE SPECIAL EDITION: EBOLA Ebola outbreak confirmed in Yambio, Western Equatoria World Health Organization leads international response team to contain the outbreak Photo by:
WHO SOUTHERN SUDAN HEALTH UPDATE SPECIAL EDITION: EBOLA Ebola outbreak confirmed in Yambio, Western Equatoria World Health Organization leads international response team to contain the outbreak Photo by:
EBOLA 101. Update for EMS System Stakeholders. Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Nor Cal EMS Version 10/25/2014
 EBOLA 101 Update for EMS System Stakeholders Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Nor Cal EMS Version 10/25/2014 Conference 1 Version #1 Date 10/25/14 Content good for current situation 10/25/14
EBOLA 101 Update for EMS System Stakeholders Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Nor Cal EMS Version 10/25/2014 Conference 1 Version #1 Date 10/25/14 Content good for current situation 10/25/14
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
بسم اهلل الرحمن الرحيم
 بسم اهلل الرحمن الرحيم INFECTION CONTROL MEASURES AGAINST H1N1 VIRUS; PHASE II Microbiology Diagnostics and Infection Control UNIT () Mansoura University Hospitals Prof. Mohammad Abou el-ela Director of
بسم اهلل الرحمن الرحيم INFECTION CONTROL MEASURES AGAINST H1N1 VIRUS; PHASE II Microbiology Diagnostics and Infection Control UNIT () Mansoura University Hospitals Prof. Mohammad Abou el-ela Director of
MARITIME AUTHORITY OF JAMAICA EBOLA VIRUS DISEASE TO: (I) (II) ALL MANAGERS AND OPERATORS OF JAMAICAN REGISTERED VESSELS (III)
 MARITIME AUTHORITY OF JAMAICA EBOLA VIRUS DISEASE Circular No. 14-10-10 p Revision 00 Page (s) 1of 3 TO: (I) ALL OWNERS, MASTERS OF JAMAICAN REGISTERED VESSELS (II) ALL MANAGERS AND OPERATORS OF JAMAICAN
MARITIME AUTHORITY OF JAMAICA EBOLA VIRUS DISEASE Circular No. 14-10-10 p Revision 00 Page (s) 1of 3 TO: (I) ALL OWNERS, MASTERS OF JAMAICAN REGISTERED VESSELS (II) ALL MANAGERS AND OPERATORS OF JAMAICAN
Making Sense Of The Ebola Virus
 Fodder for young minds Making Sense Of The Ebola Virus By Meera Dolasia on September 29, 2014 CCSS NAS-6 Grades: 5-8 Word Search Every few years, a new pandemic hits the globe and sends shivers down everyone's
Fodder for young minds Making Sense Of The Ebola Virus By Meera Dolasia on September 29, 2014 CCSS NAS-6 Grades: 5-8 Word Search Every few years, a new pandemic hits the globe and sends shivers down everyone's
This SOP applies to all staff employed by NHS Greater Glasgow & Clyde and locum staff on fixed term contracts and volunteer staff.
 Page 1 of 8 SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients clinical
Page 1 of 8 SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients clinical
2 Key Measures for Prevention and Control of Ebola Virus Disease. 4 Key Measures for Prevention and Control of Ebola Virus Disease
 Key Measures for Prevention and Control of Ebola Virus Disease Dr. Sergey Eremin Medical Officer World Health Organization Hosted by Dr. Benedetta Allegranzi September 16, 2014 INTRODUCTION TO EBOLA VIRUS
Key Measures for Prevention and Control of Ebola Virus Disease Dr. Sergey Eremin Medical Officer World Health Organization Hosted by Dr. Benedetta Allegranzi September 16, 2014 INTRODUCTION TO EBOLA VIRUS
EBOLA. Harford County Health Department October 22, 2014
 EBOLA Harford County Health Department October 22, 2014 Zaire ebolvirus The 2014 Ebola outbreak concerns the most deadly of the five Ebola viruses, Zaire ebolvirus, which has killed 79 percent of the people
EBOLA Harford County Health Department October 22, 2014 Zaire ebolvirus The 2014 Ebola outbreak concerns the most deadly of the five Ebola viruses, Zaire ebolvirus, which has killed 79 percent of the people
Infection Prevention and Control (IPC)
 Infection Prevention and Control (IPC) Standard Operating Procedure for CHICKENPOX (VARICELLA ZOSTER VIRUS) in a healthcare setting WARNING This document is uncontrolled when printed. Check local intranet
Infection Prevention and Control (IPC) Standard Operating Procedure for CHICKENPOX (VARICELLA ZOSTER VIRUS) in a healthcare setting WARNING This document is uncontrolled when printed. Check local intranet
Dr. Johnmark Opondo MB. ChB. (Nairobi UON), MPH ( Emory) Deputy Medical Health Officer Saskatoon Health Region
 Dr. Johnmark Opondo MB. ChB. (Nairobi UON), MPH ( Emory) Deputy Medical Health Officer Saskatoon Health Region OBJECTIVES 1. To understand the basic science behind EVD 2. To review the issues behind the
Dr. Johnmark Opondo MB. ChB. (Nairobi UON), MPH ( Emory) Deputy Medical Health Officer Saskatoon Health Region OBJECTIVES 1. To understand the basic science behind EVD 2. To review the issues behind the
SUBJECT: ISOLATION PRECAUTIONS REFERENCE #6003 PAGE: 1 DEPARTMENT: REHABILITATION SERVICES OF: 6 EFFECTIVE:
 PAGE: 1 STANDARD PRECAUTIONS: Precautions which are designed for care of all patients, regardless of diagnosis or presumed infection status to reduce the risk of transmission from both recognized and unrecognized
PAGE: 1 STANDARD PRECAUTIONS: Precautions which are designed for care of all patients, regardless of diagnosis or presumed infection status to reduce the risk of transmission from both recognized and unrecognized
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS
 INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
INFLUENZA A PREVENTION GUIDELINES FOR HEALTH CARE WORKERS What about Influenza A (H1N1)? Influenza A (H1N1) is a highly contagious acute respiratory disease caused by Type A influenza virus strain H1N1.
A BSL-1 lab houses activities that require only standard microbial practices. These include:
 BSL-1 A BSL-1 lab houses activities that require only standard microbial practices. These include: Work should be performed on an open lab bench or table Spills must be decontaminated immediately Infectious
BSL-1 A BSL-1 lab houses activities that require only standard microbial practices. These include: Work should be performed on an open lab bench or table Spills must be decontaminated immediately Infectious
ISOLATION METHODS Kaya Süer.MD
 ISOLATION METHODS Kaya Süer.MD NEU Medical Faculty Infectious Diseases and Clinical Microbiology ISOLATION Infected and colonized patients other patients, hospital visitors health personnel prevention
ISOLATION METHODS Kaya Süer.MD NEU Medical Faculty Infectious Diseases and Clinical Microbiology ISOLATION Infected and colonized patients other patients, hospital visitors health personnel prevention
U.S. CDC s Response to the Ebola Outbreak
 U.S. CDC s Response to the Ebola Outbreak CAPSCA Global Meeting Cairo, Egypt November 17-19, 2014 Susan Lippold, MD, MPH Ebola Response, Global Migration Task Force Division of Global Migration and Quarantine
U.S. CDC s Response to the Ebola Outbreak CAPSCA Global Meeting Cairo, Egypt November 17-19, 2014 Susan Lippold, MD, MPH Ebola Response, Global Migration Task Force Division of Global Migration and Quarantine
Product Considerations for Standard, Contact and Droplet Precautions
 Product Considerations for Standard, Contact and Droplet Precautions On July 30, 2014, the CDC released its Infection Prevention and Control Recommendations for Hospitalized Patients with Known or Suspected
Product Considerations for Standard, Contact and Droplet Precautions On July 30, 2014, the CDC released its Infection Prevention and Control Recommendations for Hospitalized Patients with Known or Suspected
Ebola Virus Transmission
 Ebola Virus Zoonotic virus bats the most likely reservoir, although species unknown Spillover event from infected wild animals (e.g., fruit bats, monkey, duiker) to humans, followed by human-human transmission
Ebola Virus Zoonotic virus bats the most likely reservoir, although species unknown Spillover event from infected wild animals (e.g., fruit bats, monkey, duiker) to humans, followed by human-human transmission
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
EBOLA VIRUS AWARENESS
 EBOLA VIRUS AWARENESS Yvonne S. Butler, MD Assistant Professor; Obstetrics and Gynecology Global Women s Health Program Liberia Chevron-Liberia / BIPAI Partnership Baylor College of Medicine Texas Children
EBOLA VIRUS AWARENESS Yvonne S. Butler, MD Assistant Professor; Obstetrics and Gynecology Global Women s Health Program Liberia Chevron-Liberia / BIPAI Partnership Baylor College of Medicine Texas Children
Respiratory Protection and Swine Influenza
 PAGE 1 TechUpdate Respiratory Protection and Swine Influenza Frequently asked Questions The U.S. Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) have recently issued
PAGE 1 TechUpdate Respiratory Protection and Swine Influenza Frequently asked Questions The U.S. Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO) have recently issued
Ebola Virus Disease: the Facts, Response & the Way Forward. Dr. Abraham Idokoko Ebola Emergency Operations Centre (EEOC), Lagos.
 Ebola Virus Disease: the Facts, Response & the Way Forward. Dr. Abraham Idokoko Ebola Emergency Operations Centre (EEOC), Lagos. 2 Yearly trend of Emergence of New Infectious Diseases Globally, an average
Ebola Virus Disease: the Facts, Response & the Way Forward. Dr. Abraham Idokoko Ebola Emergency Operations Centre (EEOC), Lagos. 2 Yearly trend of Emergence of New Infectious Diseases Globally, an average
FOR INFECTION TO OCCUR: Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV
 OCCUPATIONAL EXPOSURE TO BLOODBORNE PATHOGENS Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV FOR INFECTION TO OCCUR: A germ Bloodborne
OCCUPATIONAL EXPOSURE TO BLOODBORNE PATHOGENS Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV FOR INFECTION TO OCCUR: A germ Bloodborne
Diseases that are commonly transmitted by exposure to blood. Most common are: Hepatitis B and C HIV
 Diseases that are commonly transmitted by exposure to blood Most common are: Hepatitis B and C HIV applies to all persons who may reasonably anticipate contact with blood or other potentially infectious
Diseases that are commonly transmitted by exposure to blood Most common are: Hepatitis B and C HIV applies to all persons who may reasonably anticipate contact with blood or other potentially infectious
Cleaning for Infection
 Cleaning for Infection Nov. 7, 2014 Prevention Bill Balek, ISSA & Craig Carter, Lonza Inc. ISSA/INTERCLEAN 2014 Sponsored by Cleaning: Often Viewed as a Cost True Value of Cleaning Investment Asset Preservation
Cleaning for Infection Nov. 7, 2014 Prevention Bill Balek, ISSA & Craig Carter, Lonza Inc. ISSA/INTERCLEAN 2014 Sponsored by Cleaning: Often Viewed as a Cost True Value of Cleaning Investment Asset Preservation
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT
 AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
AMBULANCE DECONTAMINATION GUIDELINES SUSPECTED INFLUENZA PATIENT Reprinted with the Permission of John Hill, President Iowa EMS Association Following are general guidelines for cleaning or maintaining
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Personal Protective Equipment, Hand Hygiene and Surface Cleaning in the context of Ebola
 Personal Protective Equipment, Hand Hygiene and Surface Cleaning in the context of Ebola This publication and the information it contains is intended for distribution to, or use by, people in the following
Personal Protective Equipment, Hand Hygiene and Surface Cleaning in the context of Ebola This publication and the information it contains is intended for distribution to, or use by, people in the following
OBJECTIVES PEOPLE AS RESERVOIRS. Reservoir
 Module C EPIDEMIOLOGY AND RISK OF INFECTION IN OUTPATIENT SETTINGS Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine OBJECTIVES Discuss the infectious process Review
Module C EPIDEMIOLOGY AND RISK OF INFECTION IN OUTPATIENT SETTINGS Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine OBJECTIVES Discuss the infectious process Review
Case Scenario 2: Exit Screening at Airport
 EVD Event Management Workshops FACILITATOR GUIDE Case Scenario 2: Exit Screening at Airport Implementing exit screening at an airport of a country, with initial cases of Ebola Virus Disease transmission
EVD Event Management Workshops FACILITATOR GUIDE Case Scenario 2: Exit Screening at Airport Implementing exit screening at an airport of a country, with initial cases of Ebola Virus Disease transmission
Doc: 1.9. Course: Patient Safety Solutions. Topic: Infection prevention and control. Summary
 Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Infection Prevention To navigate, click the Page Up or Page Down keys on your keyboard
 Infection Prevention To navigate, click the Page Up or Page Down keys on your keyboard Welcome to Infection Prevention This course is intended to present a brief overview of various infection control topics.
Infection Prevention To navigate, click the Page Up or Page Down keys on your keyboard Welcome to Infection Prevention This course is intended to present a brief overview of various infection control topics.
IH0300: Droplet Precautions. Infection Prevention and Control Section 04H IH0300 (Droplet Precautions) Page 1. EFFECTIVE DATE: September 2006
 Page 1 IH0300: Droplet Precautions EFFECTIVE DATE: September 2006 REVISED DATE: April 2011, September 2014 February 2015, November 2016 REVIEWED DATE: 1.0 PURPOSE Droplet Precautions refer to infection
Page 1 IH0300: Droplet Precautions EFFECTIVE DATE: September 2006 REVISED DATE: April 2011, September 2014 February 2015, November 2016 REVIEWED DATE: 1.0 PURPOSE Droplet Precautions refer to infection
MODULE B. Objectives. Infection Prevention. Infection Prevention. N.C. Nurse Aide I Curriculum
 DHSR/HCPR/CARE NAT I Curriculum - July 2013 1 N.C. Nurse Aide I Curriculum MODULE B Infection Prevention Objectives Relate the chain of infection to the work of a nurse aide in long-term care facilities.
DHSR/HCPR/CARE NAT I Curriculum - July 2013 1 N.C. Nurse Aide I Curriculum MODULE B Infection Prevention Objectives Relate the chain of infection to the work of a nurse aide in long-term care facilities.
Safety Committee Prototypical Safety Program Manual
 1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
Infection Prevention and Control Annual Education Authored by: Infection Prevention and Control Department
 Infection Prevention and Control Annual Education 2017 Authored by: Infection Prevention and Control Department Objectives After you complete this Computer-Based Learning (CBL) module, you should be able
Infection Prevention and Control Annual Education 2017 Authored by: Infection Prevention and Control Department Objectives After you complete this Computer-Based Learning (CBL) module, you should be able
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
Bloodborne Pathogens. Kathleen Stefek, RN, MSN
 Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION
 TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
TOPIC 4 HANDLING HEALTH PROTECTION & SAFETY PRACTICES FOR MEDICAL STAFF & WASTE HANDLERS TRAINING & PUBLIC EDUCATION Who Is AT RISK? Basic Questions Key Points General Principles Waste Handling Minimum
Infection Control Update
 Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
Infection Control Update This presentation provides essential information that regulatory agencies e.g., JC, NJDOH, CMS expect you to know about Infection Control. MBA/January 2016 Infection Control Elements
Worker Protection and Infection Control for Pandemic Flu
 Factsheet #2 What Workers Need to Know About Pandemic Flu Worker Protection and Infection Control for Pandemic Flu An influenza pandemic will have a huge impact on workplaces throughout the United States.
Factsheet #2 What Workers Need to Know About Pandemic Flu Worker Protection and Infection Control for Pandemic Flu An influenza pandemic will have a huge impact on workplaces throughout the United States.
Title: Supplementary guidelines on handling of
 Revised 1 st July 2006 Page 1 of 7 Supplementary Guideline on Handling of Clinical Specimens in the Laboratory (Revised July 2006) The following guidelines are supplementary to existing standard laboratory
Revised 1 st July 2006 Page 1 of 7 Supplementary Guideline on Handling of Clinical Specimens in the Laboratory (Revised July 2006) The following guidelines are supplementary to existing standard laboratory
BLOODBORNE PATHOGENS. 30 Minutes
 BLOODBORNE PATHOGENS 30 Minutes AGENDA Define bloodborne pathogens Recognize OSHA standards related to bloodborne pathogens Identify employer responsibilities related to compliance with OSHA standards
BLOODBORNE PATHOGENS 30 Minutes AGENDA Define bloodborne pathogens Recognize OSHA standards related to bloodborne pathogens Identify employer responsibilities related to compliance with OSHA standards
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Epidemiology and Risk of Infection in outpatient Settings
 Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Epidemiology and Risk of Infection in outpatient Settings
 Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Module C Epidemiology and Risk of Infection in outpatient Settings Statewide Program for Infection Control and Epidemiology (SPICE) UNC School of Medicine Objectives Discuss the infectious process through
Information for Health Care Workers
 Information for Health Care Workers This Bulletin highlights precautions to be taken by health care workers who may be exposed to blood and body fluids. In general, workers should minimize direct contact
Information for Health Care Workers This Bulletin highlights precautions to be taken by health care workers who may be exposed to blood and body fluids. In general, workers should minimize direct contact
Infection Control Program (ICP) ICP Components 1. Exposure Determination 2. Control Methods A. Universal Precautions
 Compliance Assistance Guideline for the February 27, 1990, OSHA Instruction CPL 2 2.44B Enforcement Procedures for Occupational Exposure to Hepatitis B Virus and Human Immunodeficiency Virus from the U.S.
Compliance Assistance Guideline for the February 27, 1990, OSHA Instruction CPL 2 2.44B Enforcement Procedures for Occupational Exposure to Hepatitis B Virus and Human Immunodeficiency Virus from the U.S.
Chapter 7 8/23/2016. Asepsis and Infection Control. Asepsis. Asepsis (Cont.) Microorganisms. Infection control and prevention
 Chapter 7 Asepsis and Infection Control All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Asepsis Microorganisms Tiny microscopic entities capable
Chapter 7 Asepsis and Infection Control All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Asepsis Microorganisms Tiny microscopic entities capable
SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/ April Swine Flu-Information Sheet
 SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/09 Swine Flu-Information Sheet To date 2 cases of swine Influenza A (H1N1) have been confirmed in individuals in Scotland. Other
SCOTTISH AMBULANCE SERVICE Strategic Co-ordination Centre (SCC) Bulletin 01/09 Swine Flu-Information Sheet To date 2 cases of swine Influenza A (H1N1) have been confirmed in individuals in Scotland. Other
SARS Infection Control in Healthcare Settings
 SARS Infection Control in Healthcare Settings William A. Rutala, Ph.D., M.P.H. University of North Carolina (UNC) Hospitals and UNC School of Medicine Infection Control Considerations Hospitals must protect
SARS Infection Control in Healthcare Settings William A. Rutala, Ph.D., M.P.H. University of North Carolina (UNC) Hospitals and UNC School of Medicine Infection Control Considerations Hospitals must protect
Guideline for Infection Prevention at Medical Facilities
 Guideline for Infection Prevention at Medical Facilities March 26, 2007 Pandemic Influenza Experts Advisory Committee 129 130 Pandemic Influenza Preparedness Guidelines (From Phase 4 Onwards) Guidelines
Guideline for Infection Prevention at Medical Facilities March 26, 2007 Pandemic Influenza Experts Advisory Committee 129 130 Pandemic Influenza Preparedness Guidelines (From Phase 4 Onwards) Guidelines
School District of Indian River County
 School District of Indian River County Bloodborne Pathogens Exposure Control Program In Schools Program Objectives To eliminate or minimize all exposures to bloodborne pathogens (HIV, HBV). To identify
School District of Indian River County Bloodborne Pathogens Exposure Control Program In Schools Program Objectives To eliminate or minimize all exposures to bloodborne pathogens (HIV, HBV). To identify
