Biology of soft tissue wound healing and regeneration consensus report of Group 1 of the 10th European Workshop on Periodontology
|
|
|
- Iris Morris
- 5 years ago
- Views:
Transcription
1 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich Year: 2014 Biology of soft tissue wound healing and regeneration consensus report of Group 1 of the 10th European Workshop on Periodontology Hämmerle, Christoph H F; Giannobile, William V Abstract: BACKGROUND: The scope of this consensus was to review the biological processes of soft tissue wound healing in the oral cavity and to histologically evaluate soft tissue healing in clinical and pre-clinical models. AIMS: To review the current knowledge regarding the biological processes of soft tissue wound healing at teeth, implants and on the edentulous ridge. Furthermore, to review soft tissue wound healing at these sites, when using barrier membranes, growth and differentiation factors and soft tissue substitutes. COLLECTION OF DATA: Searches of the literature with respect to recessions at teeth and soft tissue deficiencies at implants, augmentation of the area of keratinized tissue and soft tissue volume were conducted. The available evidence was collected, categorized and summarized. FUNDAMENTAL PRINCIPLES OF ORAL SOFT TISSUE WOUND HEALING: Oral mucosal and skin wound healing follow a similar pattern of the four phases of haemostasis, inflammation, proliferation and maturation/matrix remodelling. The soft connective tissue determines the characteristics of the overlaying oral epithelium. Within 7-14 days, epithelial healing of surgical wounds at teeth is completed. Soft tissue healing following surgery at implants requires 6-8 weeks for maturation. The resulting tissue resembles scar tissue. Well-designed pre-clinical studies providing histological data have been reported describing soft tissue wound healing, when using barrier membranes, growth and differentiation factors and soft tissue substitutes. Few controlled clinical studies with low numbers of patients are available for some of the treatments reviewed at teeth. Whereas, histological new attachment has been demonstrated in pre-clinical studies resulting from some of the treatments reviewed, human histological data commonly report a lack of new attachment but rather long junctional epithelial attachment and connective tissue adhesion. Regarding soft tissue healing at implants human data are very scarce. CONCLUSIONS: Oral soft tissue healing at teeth, implants and the edentulous ridge follows the same phases as skin wound healing. Histological studies in humans have not reported new attachment formation at teeth for the indications studied. Human histological data of soft tissue wound healing at implants are limited. CLINICAL RECOMMENDATIONS: The use of barriers membranes, growth and differentiation factors and soft tissue substitutes for the treatment of localized gingival/mucosal recessions, insufficient amount of keratinized tissue and insufficient soft tissue volume is at a developing stage. DOI: /jcpe Posted at the Zurich Open Repository and Archive, University of Zurich ZORA URL: Accepted Version Originally published at: Hämmerle, Christoph H F; Giannobile, William V (2014). Biology of soft tissue wound healing and regeneration consensus report of Group 1 of the 10th European Workshop on Periodontology. Journal
2 of Clinical Periodontology, 41(S15):S1-S5. DOI: /jcpe
3 10 th EWP, La Granja, Segovia, Spain Consensus Report for Working Group 1 Christoph H.F. Hämmerle 1 & William V. Giannobile 2 1 University of Zürich, Switzerland 2 University of Michigan, USA On Behalf of Working Group 1 Ingemar Abrahamsson (S) Javier Nuñez (E) Juan Blanco (E) Joerg Meyle (D) Dieter Bosshardt (CH) Frank Schwarz (D) Christer Dahlin (S) Anton Sculean (CH) Nikos Donos (UK) Andreas Stavropoulos (S) Jan Eirik Ellingsen (N) Hendrik Terheyden (D) Stefan Fickl (D) Fabio Vignoletti (E) 1
4 Reinhard Gruber (CH) Franz Weber (D) Christoph Goerlach (CH) Abstract: Background: The scope of this consensus was to review the biological processes of soft tissue wound healing in the oral cavity and to histologically evaluate soft tissue healing in clinical and preclinical models. Aims: To review the current knowledge regarding the biological processes of soft tissue wound healing at teeth, implants and on the edentulous ridge. Furthermore, to review soft tissue wound healing at these sites, when using barrier membranes, growth and differentiation factors and soft tissue substitutes. Collection of data: Searches of the literature with respect to recessions at teeth and soft tissue deficiencies at implants, augmentation of the area of keratinized tissue and soft tissue volume were conducted. The available evidence was collected, categorized and summarized. Fundamental principles of oral soft tissue wound healing: Oral mucosal and skin wound healing follow a similar pattern of the four phases of hemostasis, inflammation, proliferation, and maturation/matrix remodeling. The soft connective tissue determines the characteristics of the overlaying oral epithelium. Within 7-14 days, epithelial healing of surgical wounds at teeth is completed. Soft tissue 2
5 healing following surgery at implants requires 6-8 weeks for maturation. The resulting tissue resembles scar tissue. Well-designed pre-clinical studies providing histological data have been reported describing soft tissue wound healing, when using barrier membranes, growth and differentiation factors and soft tissue substitutes. Few controlled clinical studies with low numbers of patients are available for some of the treatments reviewed at teeth. Whereas, histological new attachment has been demonstrated in preclinical studies resulting from some of the treatments reviewed, human histological data commonly report a lack of new attachment but rather long junctional epithelial attachment and connective tissue adhesion. Regarding soft tissue healing at implants human data are very scarce. Conclusions: Oral soft tissue healing at teeth, implants and the edentulous ridge follows the same phases as skin wound healing. Histological studies in humans have not reported new attachment formation at teeth for the indications studied. Human histological data of soft tissue wound healing at implants is limited. Clinical Recommendations: The use of barriers membranes, growth and differentiation factors and soft tissue substitutes for the treatment of localized gingival/mucosal recessions, insufficient amount of keratinized tissue, and insufficient soft tissue volume is at a developing stage. Key words: periodontal/peri-implant wound healing, oral soft tissue, barrier membranes, growth and differentiation factors, scaffolds, soft tissue substitutes, pre-clinical studies, human histology 3
6 This consensus group evaluated in the first review the current evidence relating to the basic biological concepts of the oral wound healing response. As a part of the second review, a particular emphasis on early stage investigations of newly developed biological agents for periodontal soft tissue regeneration including barrier scaffolding matrices, biological agents (such as enamel matrix derivative, platelet-derived growth factor) and soft tissue substitutes was evaluated. The second review focused on preclinical and clinical studies with the requirement of histological biopsy material of the wound repair process. The scope of Workshop Group 1, focused on two key areas: 1) soft tissue wound healing around teeth and dental implants (Sculean et al., 2014); and 2) soft tissue wound healing at teeth, dental implants and the edentulous ridge with barrier membranes, growth and differentiation factors and soft tissue substitutes (Vignoletti et al., 2014). Soft tissue wound healing around teeth and dental implants (Sculean et al., 2014) The narrative review that was prepared by working group 1a focused on evaluating the wound healing concept in 3 key areas: Basic oral 4
7 biological principles, soft tissue healing around teeth, and soft tissue repair around dental implants. Summary of key points of the review: 1. Oral mucosal and skin wound healing follows a similar pattern of the four phases hemostasis, inflammation, proliferation and maturation/matrix remodeling. 2. Infection control is important for undisturbed oral wound healing and is a prerequisite for the transition of the inflammatory to the proliferative phase. 3. Granulation tissue derived from the periodontal ligament induces epithelial cells to form a keratinized masticatory gingiva. 4. The soft connective tissue determines the characteristics of the overlaying oral epithelium. 5. Epithelial healing around teeth following non-surgical and surgical periodontal therapy is completed after 7-14 days (Waerhaug, 1978, Novaes et al., 1969, Stahl et al., 1971). 6. Functional stability between the denuded root and soft tissue is achieved approximately 14 days after surgery (Hiatt et al., 1968). 7. The formation of the biologic width and maturation of the barrier function around transmucosal implants requires 6-8 weeks of healing (Berglundh et al., 2007, Tomasi et al., 2013, Schwarz et al., 2013). 8. The established peri-implant soft connective tissue resembles a scar tissue in composition, fiber orientation, and vasculature. 5
8 9. The peri-implant junctional epithelium may reach a greater final length under certain conditions such as implants placed into fresh extraction sockets versus conventional implant procedures in healed sites. Recommendations for Future Research Strategies for future research investigation to advance the field of oral wound healing around teeth and implants included the following target areas recommended by the expert review panel: -Need more information on the inductive influences of the connective tissue environment on tissue neogenesis. Study at the cellular and matrix levels could be important in determining environmental cues. Cell: cell interactions (e.g., epithelial-mesenchymal influences) may instruct cell fate and determination. Identification of the cytokine, chemokine and intercellular signaling networks that are involved in the wound healing process may better inform on regenerative and reparative approaches. The study of existing and newly discovered growth and differentiation factors may lead to new information on the repair and regeneration of oral tissues. Evidence gained from genetic models (i.e., transgenic and gene deletion) relevant to skin morphogenesis and regeneration may be instructive and translate to the oral wound healing situation. More study is warranted to examine the oral wound healing response in the 6
9 face of the microbial challenge and local salivary molecules that may influence epigenetic changes of oral epithelia. -To identify host and immunological cellular and soluble factors that regulate the healing process during periodontal and peri-implant wound repair. Determine what genetic biologic phenotypes may regulate an exacerbated healing responses depending on immunologic profiles. It would also be valuable to study aging on oral soft tissue wound healing responses on cellular senescence and telomere length on stem cell progenitors contributing to the reparative process. -To investigate the mechanisms of connective tissue graft integration, revascularization and re-epithelialization as it relates to tissue remodeling (increases or decreases in tissue volume and quality) in different soft tissue biotype situations. -To identify the basic mechanisms and relevance of scar-like periimplant connective tissue and epithelial interface. To determine the mechanisms of connective tissue adhesion to the implant material surface. The field would be advanced to better understand the biological consequences of implant/abutment biomaterial surface characteristics on the influence of biologic width formation. The role of implant biomaterial surface characteristics on dental biofilm formation and proliferation should be considered. 7
10 Soft tissue wound healing at teeth, dental implants and the edentulous ridge when using barrier membranes, growth and differentiation factors and soft tissue substitutes (Vignoletti et al., 2014) The narrative review that was prepared by working group 1b focused on evaluating the histological results of the application of scaffolds, cells and biological on soft tissue wound healing at teeth, dental implants and the edentulous ridge. Data were collected from pre-clinical experiments and from patient treatments reporting histological outcomes. Clinical studies, regardless of the evidence level provided, not reporting histological outcomes are not included in this review. As a consequence a large body of data derived from well-designed clinical studies are not included in this review. The level of evidence available for this review was mostly limited to well-designed pre-clinical studies and to clinical case series or case reports. Few controlled clinical studies with low numbers of patients were available for some of the treatments reviewed. The studies available were mostly of short duration not exceeding 6 months. The studies available for evaluation were primarily associated with teeth. There was limited information available on soft tissue augmentation around implants. 8
11 Recessions at teeth and soft tissue deficiencies at dental implants Regarding recessions at teeth and soft tissue deficiencies at dental implants the following therapeutic approaches were evaluated: barrier membranes, growth and differentiation factors and soft tissue substitutes. Indications for the treatment of recessions at teeth and soft tissue deficiencies at dental implants include esthetic patient desires, root hypersensitivity and difficulty to perform plaque control. When evaluating the treatment approaches dealt with in this review, the coronally advanced flap (CAF) with and without a connective tissue graft (CTG) was used as a control. Available human histological data were often retrieved following treatment of hopeless teeth, very advanced or experimentally created defects. These extreme situations are far from the expected clinical use and, therefore, are suboptimal examples to assess the biological potential of these new technologies. Barrier membranes When barrier membranes were used at teeth in addition to CAF, increased amounts of new cementum, connective tissue attachment and reduced length of the junctional epithelium were observed. No significant differences were found related to these parameters between resorbable and non-resorbable membranes. The histological data revealed no adverse reactions resulting from the use of these materials. 9
12 The clinical differences between CAF with/without membranes were small in pre-clinical studies providing histology. Growth and differentiation factors The reason to introduce growth and differentiation factors is to induce new attachment formation in addition to the clinical coverage of the recession defect. Very little human histological data are available on the use of growth and differentiation factors. The factors reported in the review encompassed Enamel Matrix Derivative (EMD), Platelet Derived Growth Factor (PDGF) and Platelet Rich Plasma (PRP). The potential of EMD to promote new attachment has consistently been demonstrated in pre-clinical histological studies. Pre-clinical histological data is lacking comparing EMD to the standard of care. Histological data from humans, however, have failed to confirm new attachment formation. Favorable clinical data were reported in some of these human histological studies. In one histological study in humans PDGF (CAF+PDGF) exhibited new attachment formation in contrast to the control group (CAF+CTG). The clinical comparison in this study favored the controls regarding recession depth reduction and mean root coverage. In one pre-clinical histological study comparing CAF+CTG+PRP (test) versus the standard of care CAF+CTG, the test group showed more 10
13 new attachment formation than the control group. When comparing the two procedures, the residual recession was similar in this preclinical study. No human histological datum is available. Soft tissue substitutes The reason to introduce soft tissue substitutes is to avoid the harvesting procedure and the concomitant morbidity associated with autogenous soft tissue grafts, which presently are the standard of care. The following materials have been histologically evaluated: acellular dermal matrix graft (ADMG), collagen matrices (CM), human fibroblast-derived dermal substitute (HF-DDS), and human skin equivalents (bilayered cell therapy: BCT). In three pre-clinical studies ADMG or CM have shown histological results regarding the tissue-tooth interface similar to the standard of care CAF+CTG and CAF alone, respectively. Human histological data have mostly shown epithelial attachment and connective tissue adhesion with an absence of adverse reactions. Successful recession coverage was reported in some of these human histological studies. In one pre-clinical study with dental implants the histological results for CAF+CM revealed a tissue implant interfaces similar to CAF+CTG or CAF alone consisting of epithelial attachment and connective tissue adhesion. The amount of coverage of the soft tissue deficiencies was similar for the three procedures, however both 11
14 experimental groups improved tissue thickness when compared with CAF alone. No human histological datum is available. Presently, there are no histological data available for HF-DDS and BCT. Augmentation of keratinized tissue The standard of care for increasing the zone of keratinized tissue is the apically positioned flap (APF) with an autogenous graft with/without epithelium, i.e. FGG or CTG. Soft tissue substitutes The following materials have been histologically evaluated: acellular dermal matrix graft (ADMG), collagen matrices (CM), and human skin equivalents (bilayered cell therapy: BCT). Generally speaking, there is little histological data assessing these materials in this indication. The histological pre-clinical and clinical data available demonstrate these materials to be well integrated into the host connective tissues without adverse reactions. In one pre-clinical study similar histological appearance was described for the increased zone of keratinized tissue comparing APF+CM with APF in edentulous areas of the ridge. The clinical results of this histological study have shown similar and large amounts of gain of keratinized tissue. Another pre-clinical study compared APF+CM to APF for increasing the zone of keratinized tissue. A tissue-tooth interface was found 12
15 consisting of epithelial attachment and connective tissue adhesion similar in both groups. The gain in keratinized tissue was similar but small in both groups. In one human study comparing APF+CM from a different source and APF+FGG, a good integration and keratinization of the CM was found. The clinical results, however, reported smaller amounts of gain of keratinized tissue compared to the controls. ADMG was tested in a pre-clinical and two human studies for augmentation of keratinized tissue at teeth in combination with APF. Histology revealed good tissue integration and a small gain of keratinized tissue associated with the ADMG. In one clinical case aiming at increasing the zone of keratinized tissue at an implant site retrieval of a histological sample revealed inflammation and degeneration of the ADMG. BCT was tested in one human study together with an APF against APF+FGG. Histologically good integration and keratinization were found for both groups investigated. The FFG group revealed more gain of keratinized tissue. Augmentation of insufficient soft tissue volume The standard of care for increasing the volume of the soft tissue is the transplantation of an autogenous graft with/without epithelium, i.e. CTG or FGG. Soft tissue substitutes 13
16 A modified xenogenic collagen matrix (mcm) has been histologically evaluated for soft tissue augmentation and compared to the CTG in one pre-clinical study. The histological analysis demonstrated similar integration into the surrounding tissues. Concomitant clinical measurements of volume gain demonstrated results similar to the one obtained with the CTG. Implications for Future Research Since histological assessments may not be reliable to estimate the increase/ change in soft tissue thickness, these studies should consider different methodologies/ technologies (e.g. 3D digital imaging analysis). There is a need to properly define valid and reproducible preclinical models for the assessment of soft tissue regeneration procedures around teeth and implants. Future preclinical studies should be adequately powered and consider primary outcomes that are relevant for clinical situations (e.g., use of non-histologic surrogate measures that can be measured clinically). Success criteria associated with soft tissue augmentation around teeth and implants may differ and need to be defined separately. Future studies should elaborate on potential indications and the clinical relevance of new soft tissue augmentation procedures and long-term effects. 14
17 Patient-centered/ reported outcomes should be an integral part of the evaluation of new biotechnologies when compared with current standard procedures. Safety analyses and reporting should, in addition to local (e.g. clinical and histological) signs of potential immunologic responses, also consider assessment of antibody levels formed in response to xenogenic- or allogenic-derived biomaterials. Health economics should be considered in the assessment of interventions and the introduction of new technologies. Clinical Consequences The use of barriers membranes, growth and differentiation factors and soft tissue substitutes for the treatment of localized gingival/mucosal recessions, insufficient amount of keratinized tissue, and insufficient soft tissue volume is at a developing stage. The conduct of preclinical studies is advantageous in order to preselect potential candidate materials that can be safely used in early stage clinical trials. There continues to be a need for well designed, randomized, parallel-arm controlled clinical trials to further evaluate the efficacy of new technologies for the treatment of localized gingival/mucosal recessions, limited zones of keratinized tissue, and insufficient soft tissue volume. The potential influence of 15
18 relevant confounding clinical factors (e.g., flap design, suturing techniques) should also be carefully addressed. References: Berglundh, T., Abrahamsson, I., Welander, M., Lang, N. P. & Lindhe, J. (2007) Morphogenesis of the peri-implant mucosa: an experimental study in dogs. Clin Oral Implants Res 18, 1-8. doi: /j x. Hiatt, W. H., Stallard, R. E., Butler, E. D. & Badgett, B. (1968) Repair following mucoperiosteal flap surgery with full gingival retention. J Periodontol 39, doi: /jop Novaes, A. B., Kon, S., Ruben, M. P. & Goldman, H. M. (1969) Visualization of the microvascularization of the healing periodontal wound. 3. Gingivectomy. J Periodontol 40, doi: /jop Schwarz, F., Mihatovic, I., Becker, J., Bormann, K. H., Keeve, P. L. & Friedmann, A. (2013) Histological evaluation of different abutments in the posterior maxilla and mandible: an experimental study in humans. J Clin Periodontol 40, doi: /jcpe Sculean, A., Gruber, R. & Bosshardt, D. D. (2014) Soft tissue wound healing around teeth and dental implants. J Clin Periodontol 41. Stahl, S. S., Weiner, J. M., Benjamin, S. & Yamada, L. (1971) Soft tissue healing following curettage and root planing. J Periodontol 42, doi: /jop Tomasi, C., Tessarolo, F., Caola, I., Wennstrom, J., Nollo, G. & Berglundh, T. (2013) Morphogenesis of peri-implant mucosa revisited: an experimental study in humans. Clin Oral Implants Res. doi: /clr Vignoletti, F., Nunez, J. & Sanz, M. (2014) Soft tissue wound healing at teeth, dental implants and the edentulous ridge with scaffolds, cells and biologicals. J Clin Periodontol
19 Waerhaug, J. (1978) Healing of the dento-epithelial junction following subgingival plaque control. I. As observed in human biopsy material. J Periodontol 49, 1-8. doi: /jop
Biology of soft tissue wound healing and regeneration Consensus Report of Group 1 of the 10th European Workshop on Periodontology
 J Clin Periodontol 2014; 41 (Suppl. 15): S1 S5 doi: 10.1111/jcpe.12221 Biology of soft tissue wound healing and regeneration Consensus Report of Group 1 of the 10th European Workshop on Periodontology
J Clin Periodontol 2014; 41 (Suppl. 15): S1 S5 doi: 10.1111/jcpe.12221 Biology of soft tissue wound healing and regeneration Consensus Report of Group 1 of the 10th European Workshop on Periodontology
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Science Flash. Straumann Emdogain. Science Flash
 Science Flash Straumann Emdogain Science Flash TABLE OF CONTENTS -year success with Straumann Emdogain in intra-bony defects with enamel matrix proteins and guided tissue regeneration Comparison of recession
Science Flash Straumann Emdogain Science Flash TABLE OF CONTENTS -year success with Straumann Emdogain in intra-bony defects with enamel matrix proteins and guided tissue regeneration Comparison of recession
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
Over the years, mucogingival surgery
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
Morphology of periodontal defects, indications of periodontal surgery
 Morphology of periodontal defects, indications of periodontal surgery Dr. Ferenc Dőri PhD Semmelweis University Dept. of Periodontology Periodontium Gingiva + Cementum PDL (periodontal ligament) Alveolar
Morphology of periodontal defects, indications of periodontal surgery Dr. Ferenc Dőri PhD Semmelweis University Dept. of Periodontology Periodontium Gingiva + Cementum PDL (periodontal ligament) Alveolar
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
The treatment of destructive periodontal disease, due to specific periodontopathic
 1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
Soft-Tissue Success with the. Clinical Success. Proven Matrix. with the Proven. Geistlich Mucograft Geistlich Mucograft Seal
 Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Derma S O F T T I S S U E A U G M E N TAT I O N. Acellular dermal matrix
 Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
THE NATU R R E A G L E N P E R R O A M TI O O T N ER OF
 Hyaluronic Acid THE NATURAL PROMOTER OF 1 HYADENT BG & HYADENT HYALURONIC ACID-MODE OF ACTION ATTRACTS BLOOD THE NATURAL PROMOTER OF HYADENT BG, a highly concentrated and cross-linked hyaluronic acid gel,
Hyaluronic Acid THE NATURAL PROMOTER OF 1 HYADENT BG & HYADENT HYALURONIC ACID-MODE OF ACTION ATTRACTS BLOOD THE NATURAL PROMOTER OF HYADENT BG, a highly concentrated and cross-linked hyaluronic acid gel,
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
S John Wiley & Sons A/S. Published by John Wiley & Sons Ltd. Spain; 2 University of Milano, Milan, Italy
 J Clin Periodontol 2014; 41 (Suppl. 15): S92 S97 doi: 10.1111/jcpe.12215 Surgical techniques on periodontal plastic surgery and soft tissue regeneration: Consensus Report of Group 3 of the 10th European
J Clin Periodontol 2014; 41 (Suppl. 15): S92 S97 doi: 10.1111/jcpe.12215 Surgical techniques on periodontal plastic surgery and soft tissue regeneration: Consensus Report of Group 3 of the 10th European
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS
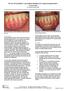 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Efficacy of soft tissue augmentation around dental implants and in partially edentulous areas: a systematic review
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Efficacy of soft tissue augmentation around dental implants and in partially
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Efficacy of soft tissue augmentation around dental implants and in partially
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alginate, tooth-shaped, for constructs, encapsulated pulp cells in, 589 590 Antibiotic paste, triple, change in root length and width
Index Note: Page numbers of article titles are in boldface type. A Alginate, tooth-shaped, for constructs, encapsulated pulp cells in, 589 590 Antibiotic paste, triple, change in root length and width
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
HDS PROCEDURE CODE GUIDELINES
 D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
D4000 - D4999 Local anesthesia is usually considered to be part of Periodontal procedures. General Guidelines 1. Periodontal services are only benefited when performed on natural teeth for treatment of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
TOOTH PRESERVATION _Zahnerhalt.indd UG :49:51 Uhr
 TOOTH PRESERVATION WHY REPAIR WHEN YOU CAN REGENERATE? Regeneration is the more natural and reliable way of restoring the positive properties of body-inherent processes. The aim of regeneration is to
TOOTH PRESERVATION WHY REPAIR WHEN YOU CAN REGENERATE? Regeneration is the more natural and reliable way of restoring the positive properties of body-inherent processes. The aim of regeneration is to
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
Tooth Retained Implant: No More an Oxymoron
 بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
More than regeneration.
 Straumann Product Emdogain Information More than regeneration. Patient comfort. Straumann Emdogain More than regeneration. Peace of mind. Tooth Preservation with Straumann Emdogain Periodontitis is associated
Straumann Product Emdogain Information More than regeneration. Patient comfort. Straumann Emdogain More than regeneration. Peace of mind. Tooth Preservation with Straumann Emdogain Periodontitis is associated
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Subject: Osseous Surgery Guideline #: Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017
 Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Clinical Guideline Subject: Osseous Surgery Guideline #: 04-205 Current Effective Date: 03/24/2017 Status: New Last Review Date: 07/10/2017 Description This document addresses the procedure of osseous
Immediate Implant Placement:
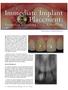 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Soft-Tissue Solutions from The Collagen Expert. Clinical Success with the Proven. Geistlich Mucograft Geistlich Mucograft Seal Geistlich Fibro-Gide
 Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Gingivectomy, excision gingival, each quadrant Gingivoplasty, each quadrant
 Dental in Nature Oral Surgery Effective CDT D3410 surgery - anterior D3421 surgery bicuspid (first root) D3425 surgery molar (first root) D3426 D3427 surgery (each additional root) Periradicular surgery
Dental in Nature Oral Surgery Effective CDT D3410 surgery - anterior D3421 surgery bicuspid (first root) D3425 surgery molar (first root) D3426 D3427 surgery (each additional root) Periradicular surgery
A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts
 J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Modified Pedicle Grafting: A Novel Noninvasive Technique for Soft Tissue Augmentation Around Maxillary Dental Implants
 Original Article Modified Pedicle Grafting: A Novel Noninvasive Technique for Soft Tissue Augmentation Around Maxillary Dental Implants Seyed Hossein Mohseni Salehi 1, Afshin Khorsand 2, Sahar Chokami
Original Article Modified Pedicle Grafting: A Novel Noninvasive Technique for Soft Tissue Augmentation Around Maxillary Dental Implants Seyed Hossein Mohseni Salehi 1, Afshin Khorsand 2, Sahar Chokami
Conventional immediate implant placement and immediate placement with socket-shield technique Which is better
 International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
International Journal of Clinical Medicine Research 2014; 1(5): 176-180 Published online December 30, 2014 (http://www.aascit.org/journal/ijcmr) ISSN: 2375-3838 Conventional immediate implant placement
Nicholas Caplanis DMD MS 6/13/2012
 Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Geistlich Fibro-Gide. The Alternative Soft-Tissue Graft
 Geistlich Fibro-Gide The Alternative Soft-Tissue Graft Geistlich Fibro-Gide shows comparable results to connective tissue grafts in terms of change in soft-tissue volume over time., This demonstrates that
Geistlich Fibro-Gide The Alternative Soft-Tissue Graft Geistlich Fibro-Gide shows comparable results to connective tissue grafts in terms of change in soft-tissue volume over time., This demonstrates that
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT
 TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
SPECIALIST CURRICULUM 2019/2020
 Dental Regeneration SPECIALIST CURRICULUM 2019/2020 by the University Medical Center Hamburg-Eppendorf (UKE) PROF. DR. DR. RALF SMEETS - Head of Division Regenerative Orofacial Medicine, University Medical
Dental Regeneration SPECIALIST CURRICULUM 2019/2020 by the University Medical Center Hamburg-Eppendorf (UKE) PROF. DR. DR. RALF SMEETS - Head of Division Regenerative Orofacial Medicine, University Medical
2017 WORLD WORKSHOP. Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March DOI: /jcpe.12957
 Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
International Journal of Implant Dentistry. Julia Hehn 1*, Thomas Schwenk 2, Markus Striegel 2 and Markus Schlee 3
 Hehn et al. International Journal of Implant Dentistry (2016) 2:13 DOI 10.1186/s40729-016-0044-4 International Journal of Implant Dentistry RESEARCH The effect of PRF (platelet-rich fibrin) inserted with
Hehn et al. International Journal of Implant Dentistry (2016) 2:13 DOI 10.1186/s40729-016-0044-4 International Journal of Implant Dentistry RESEARCH The effect of PRF (platelet-rich fibrin) inserted with
Management of miller class II gingival recession by laterally positioned pedicle flap revised technique
 Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY
 MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
ANATOMY OF THE PERIODONTIUM. Dr. Fatin Awartani
 ANATOMY OF THE PERIODONTIUM Part II Cementum and Alveolar bone Associate Professor Periodontal division King Saud university Cementum Calcified mesenchymal tissue that forms the outer covering of the anatomic
ANATOMY OF THE PERIODONTIUM Part II Cementum and Alveolar bone Associate Professor Periodontal division King Saud university Cementum Calcified mesenchymal tissue that forms the outer covering of the anatomic
Vertical and/or horizontal alveolar
 CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
CLINICAL. Free gingival grafts to manage recession when and how? Matthew B M Thomas CLINICAL
 CLINICAL CLINICAL Free gingival grafts to manage recession when and how? Matthew B M Thomas Gingival recession results from displacement of the gingival margin below the cemento-enamel junction leading
CLINICAL CLINICAL Free gingival grafts to manage recession when and how? Matthew B M Thomas Gingival recession results from displacement of the gingival margin below the cemento-enamel junction leading
SURGICAL TREATMENT OF GINGIVAL RECESSION WITH SOFT TISSUE GRAFT PROCEDURE
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2018243.2149 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Jul-Sep;24(3) Literature review
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2018243.2149 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Jul-Sep;24(3) Literature review
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
Regaining Your Gum Tissue. Soft-Tissue Regeneration With Geistlich Mucograft
 Regaining Your Gum Tissue Soft-Tissue Regeneration With Geistlich Mucograft Why is Healthy Gum Tissue So Important? Gum tissue can recede due to grinding of the teeth, thin insufficient gum tissue, as
Regaining Your Gum Tissue Soft-Tissue Regeneration With Geistlich Mucograft Why is Healthy Gum Tissue So Important? Gum tissue can recede due to grinding of the teeth, thin insufficient gum tissue, as
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in
 Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth. Jose A. Moreno Rodríguez and Raúl G.
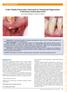 A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
Puneet Mehta et al. /JPR:BioMedRx: An International Journal 2013,1(7), Available online through
 Research Article ISSN: 988 Puneet Mehta et al. /JPR:BioMedRx: An International Journal,(7),777 Available online through http://jprsolutions.info The therapeutic and regenerative effects of Periosteum in
Research Article ISSN: 988 Puneet Mehta et al. /JPR:BioMedRx: An International Journal,(7),777 Available online through http://jprsolutions.info The therapeutic and regenerative effects of Periosteum in
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Scientific & Clinical Evidence Jason membrane
 Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
The International Journal of Periodontics & Restorative Dentistry
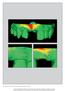 The International Journal of Periodontics & Restorative Dentistry 575 Novel Collagen Matrix to Increase Tissue Thickness Simultaneous with Guided Bone Regeneration and Implant Placement in Esthetic Implant
The International Journal of Periodontics & Restorative Dentistry 575 Novel Collagen Matrix to Increase Tissue Thickness Simultaneous with Guided Bone Regeneration and Implant Placement in Esthetic Implant
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Avita Rath, 1 Smrithi Varma, 2 and Renny Paul Case Presentation. 1. Background
 Case Reports in Dentistry Volume 2016, Article ID 9289634, 5 pages http://dx.doi.org/10.1155/2016/9289634 Case Report Two-Stage Mucogingival Surgery with Free Gingival Autograft and Biomend Membrane and
Case Reports in Dentistry Volume 2016, Article ID 9289634, 5 pages http://dx.doi.org/10.1155/2016/9289634 Case Report Two-Stage Mucogingival Surgery with Free Gingival Autograft and Biomend Membrane and
Over the years, mucogingival surgery
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Michael K. McGuire* and E. Todd Scheyer*
 Long-Term Results Comparing Xenogeneic Collagen Matrix and Autogenous Connective Tissue Grafts With Coronally Advanced Flaps for Treatment of Dehiscence-Type Recession Defects Michael K. McGuire* and E.
Long-Term Results Comparing Xenogeneic Collagen Matrix and Autogenous Connective Tissue Grafts With Coronally Advanced Flaps for Treatment of Dehiscence-Type Recession Defects Michael K. McGuire* and E.
Periosteal fenestration: A single stage surgical procedure for root coverage along with vestibular deepening
 2017; 3(2): 14-18 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2017; 3(2): 14-18 2017 IJADS www.oraljournal.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. Hoti Lal Gupta MDS, Professor and Head
2017; 3(2): 14-18 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2017; 3(2): 14-18 2017 IJADS www.oraljournal.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. Hoti Lal Gupta MDS, Professor and Head
TOPICS. T O P I C S Day 2. Introduction Surgical challenges to treat esthetic implant failures Treatment options & case reports Conclusions
 T O P I C S Day 2 Implant placement post extraction with simultaneous contour augmentation using GBR: When immediate, when early, when late? CAD-CAM technology and zirconia: new opportunities for esthetic
T O P I C S Day 2 Implant placement post extraction with simultaneous contour augmentation using GBR: When immediate, when early, when late? CAD-CAM technology and zirconia: new opportunities for esthetic
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Gum Graft? Patient Need a. Does My. 66 JANUARY 2017 // dentaltown.com. by Dr. Brian S. Gurinsky
 by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
Peri-implant Augmentation
 Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
CASE REPORT. George A. Mandelaris,* Mei Lu, and Alan L. Rosenfeld* x
 CASE REPORT The Use of a Xenogeneic Collagen Matrix as an Interpositional Soft-Tissue Graft to Enhance Peri-Implant Soft-Tissue Outcomes: A Clinical Case Report and Histological Analysis George A. Mandelaris,*
CASE REPORT The Use of a Xenogeneic Collagen Matrix as an Interpositional Soft-Tissue Graft to Enhance Peri-Implant Soft-Tissue Outcomes: A Clinical Case Report and Histological Analysis George A. Mandelaris,*
Pattern of bone resorption after extraction
 Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
ndisch Péter PERIODONTAL REGENERATION AND WOUND HEALING Windisch Pét 2017.
 PERIODONTAL REGENERATION AND WOUND HEALING 2017. ndir HEALTHY PERIODONTIUM DISEASED ndir Periodontitis Reparation Regeneration ndir W ind W ind isc i W nd isc h P i W nd isc h é in is h Pé d c P t e nd
PERIODONTAL REGENERATION AND WOUND HEALING 2017. ndir HEALTHY PERIODONTIUM DISEASED ndir Periodontitis Reparation Regeneration ndir W ind W ind isc i W nd isc h P i W nd isc h é in is h Pé d c P t e nd
3D-REGENERATIVE TISSUE GRAFT
 bone & tissue regeneration botiss biomaterials mucoderm 3D-REGENERATIVE TISSUE GRAFT Scientific basics and clinical cases native soft tissue stable three-dimensional 1 botiss regeneration system Straumann
bone & tissue regeneration botiss biomaterials mucoderm 3D-REGENERATIVE TISSUE GRAFT Scientific basics and clinical cases native soft tissue stable three-dimensional 1 botiss regeneration system Straumann
