Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan
|
|
|
- Godwin Walker
- 5 years ago
- Views:
Transcription
1 University of Groningen Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document Version Publisher's PDF, also known as Version of record Publication date: 2006 Link to publication in University of Groningen/UMCG research database Citation for published version (APA): Schoen, P. J. (2006). Oral and maxillofacial rehabilitation of head and neck cancer patients Groningen: s.n. Copyright Other than for strictly personal use, it is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), unless the work is under an open content license (like Creative Commons). Take-down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. Downloaded from the University of Groningen/UMCG research database (Pure): For technical reasons the number of authors shown on this cover page is limited to 10 maximum. Download date:
2 The Use of Implant-Retained Mandibular Prostheses in the Oral Rehabilitation of Head and Neck Cancer Patients Chapter 2 A Review and Rationale for Treatment Planning Pieter J Schoen Harry Reintsema Gerry M Raghoebar Arjan Vissink Jan LN Roodenburg This chapter is an edited version of the manuscript: Schoen PJ, Reintsema H, Raghoebar GM, Vissink A, Roodenburg JLN (2004). The Use of Implant Retained Mandibular Prostheses in the Oral Rehabilitation of Head and Neck Cancer Patients. A Review and Rationale for Treatment Planning. Oral Oncology 40:
3 16
4 Introduction Surgical treatment of malignancies involving the oral cavity often results in an altered anatomical situation, which may severely hamper oral functioning. Surgical treatment is often combined with radiotherapy, which further worsens oral functioning. Amongst others salivary secretion is reduced, and speech, chewing (mastication), swallowing and aesthetics are in general impaired (Zlotolow et al. 1992; Mounsey & Boyd 1994; Hayter & Cawood 1996; Kwakman et al. 1997a; Roumanas et al. 1997; Reintsema et al. 1998; Visch et al. 2002; Vissink et al. 2003a; Vissink et al. 2003b). Due to the changed intra-oral conditions the possibilities to obtain proper stability and retention of a mandibular prosthesis are seriously at risk (Buchbinder et al. 1989; Hayter & Cawood 1996; Marker et al. 1997; Misiek & Chang 1998; Reintsema et al. 1998). For example, particularly after radiotherapy, the load-bearing capacity of both the native and reconstructed tissues is compromised (Buchbinder et al. 1989; Judy et al. 1991; Weischer et al. 1996; Visch et al. 2002). Until recently neither reconstructive surgery nor conventional prosthodontic techniques were capable to address these problems successfully (Sclaroff et al. 1994; Watzinger et al. 1996). A proper choice of reconstruction techniques in combination with implant supported or retained prosthodontics probably can attribute to better functional results in the oral rehabilitation of these patients (Buchbinder et al. 1989; Zlotolow et al. 1992; Franzen et al. 1995; Reychler et al. 1996; Schmelzeisen et al. 1996; McGhee et al. 1997; Roumanas et al. 1997; Wei et al. 1997; Gürlek et al. 1998; Misiek & Chang 1998; Urken et al. 1998; Granstrom et al. 1999; Weischer & Mohr 2001; Schultes et al. 2002). As a first effect, implants are used with increasing frequency for prosthetic support in patients who are treated for malignancies in the lower region of the oral cavity (Judy et al. 1991; Razavi et al. 1995; Marker et al. 1997; McGhee et al. 1997; Reintsema et al. 1998; Weischer & Mohr 2001). This includes reconstruction of the mandible and insertion of implants in patients who have been treated with radiotherapy, in spite of the well-documented adverse biologic changes that occur when soft and osseous tissues have been exposed to ionising radiation (Jacobsson et al. 1985; Taylor & Worthington 1993; Keller et al. 1997a; McGhee et al. 1997; Wang et al. 1998; Visch et al. 2002; Vissink et al. 2003a; Vissink et al. 2003b). Irradiated sites are thought to be at significant risk for tissue necrosis and loss of implants, if subjected to implant surgery (Granstrom et al. 1992a). Thus, the appropriateness of using implants in irradiated patients has been seriously questioned (Granstrom et al. 1999). Because of the radiation hazards mentioned, it might be reasonable to place implants prior to postoperative radiotherapy, preferably simultaneously with ablative surgery (Sclaroff et al. 1994; Razavi et al. 1995; Kwakman et al. 1997a; Marx & Morales 1998). 2 17
5 In this paper the literature regarding the treatment outcome of the use of implants for oral rehabilitation in edentulous patients within the scope of the oncological treatment in the lower region of the oral cavity is reviewed and a rationale for treatment planning is given. Methods The human studies published in international English language peer reviewed literature regarding the treatment outcome of the use of implants for oral rehabilitation in edentulous patients after ablative tumour surgery in the lower region of the oral cavity are reviewed. The search terms included head and neck neoplasm s, dental implants, radiotherapy, hyperbaric oxygen therapy (HBO) and edentulous mandible. Publications presented in abstract form were ignored and case reports were excluded. Due to differences in experimental set-up and (or) methodological shortcomings, it was not possible to execute a meta-analysis including a sufficient number of studies. In many studies a rather low number of patients is described. Placement of implants during ablative tumour surgery Pre ablative treatment planning Prosthodontic rehabilitation of an edentulous oncology patient should not be limited to the post-treatment stage, but has to be considered already in the planning of the cancer treatment. It should be an integral part of the treatment plan of a particular patient and drawn up in full co-operation with the other members of the head and neck oncology team (Judy et al. 1991; Sclaroff et al. 1994; Razavi et al. 1995; Chan et al. 1997; Reintsema et al. 1998). The oral status has to be recorded including the patient s history of functioning with his prostheses. Prostheses have to be checked for fit, stability, retention and occlusion. Special attention and experience of the prosthodontist is needed to estimate the possible effects of the chosen surgical and (or) radiotherapeutic treatment on posttreatment oral functioning. Especially the effects on the neutral zone (the dynamic space between the lips, the cheeks and the tongue that is available for a prosthesis) and the possible deviation of the mandible after surgery have to be taken into account (Razavi et al. 1995; Reintsema et al. 1998). The head and neck oncology team decides on the appropriate oncological treatment. This treatment is based on the characteristics of the tumour (clinical classification, pathology and imaging), the estimated size of the defect after ablative sur- 18
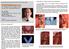
6 gery, the type of surgical reconstruction to be used to close the defect and to restore function, and the possible need for radiotherapy (Martin et al. 1994). Intra-oral defects caused by ablative surgery of malignancies in the lower region of the oral cavity mostly require a surgical reconstruction with soft tissue flaps without a need for bony reconstruction. Main problems of most soft tissue flaps are their bulky volume and absence of intrinsic mobility, which can severely restrict the neutral zone and thus complicate functioning of a mandibular prosthesis. In case of smaller tumours primary closure of the defect often can be achieved. Even this can result in a diminished mobility of the tongue, which may rise problems with e.g. speech (articulation) and swallowing, and again a restricted neutral zone due to loss of sulcular depth (Kwakman et al. 1997b). In case of loss of mandibular continuity, primary bony reconstruction of the defect is strongly preferred to restore function and to prevent soft tissue collapse (Urken et al. 1991a; Zlotolow et al. 1992; Navarro-Vila et al. 1996; Keller et al. 1997a; Urken et al. 1998). Unfortunately, this can not always be realised, mostly due to patient related factors like advanced vascular disease or poor general health. Therefore, before ablative surgery is performed, it has to be assessed whether implants might be of benefit for oral rehabilitation in the given situation. Considerations regarding placement of implants during ablative surgery Especially when it is likely that postoperative radiotherapy is indicated, some authors advice to insert implants immediately following the ablative procedure in the same session (Figs. 1,2) (Urken et al. 1989; Sclaroff et al. 1994; Kwakman et al. 1997a; Marx & Morales 1998; Mericske-Stern et al. 1999). The major advantages of implant placement during ablative surgery reported in literature include (Sclaroff et al. 1994; Wei et al. 1997; Urken et al. 1991a): Initial implant healing (osseointegration) takes place before irradiation; A Fig. 1. A 50-years old male patient with a T2N1 squamous cell carcinoma of the tongue. The patient underwent wide local excision of the tumour and a unilateral supra-omohyoid neck dissection. The surgical defect was reconstructed with a free radial forearm flap. Four implants were inserted simultaneously with the ablative procedure. Six weeks after ablative surgery, a fractionated radiotherapy scheme was started up to a cumulative dose of 64 Gy. 1A. Orthopantomogram 1.5 years after ablative surgery showing four implants and the suprastructure. 1B. Clinical view 1.5 years after ablative surgery showing the implants and suprastructure. Note the healthy aspect of the peri-implant tissues. B 2 19
7 A B The patient can benefit from the support of the implants in an earlier stage after treatment. Among others this support is important for the rehabilitation of speech and swallowing; The patient is saved from another surgical intervention; There is no need for adjunctive HBO therapy. C Fig. 2. A 54 years old female with a T4N0 squamous cell carcinoma of the mandibular gingiva. The patient was treated with wide local excision of the tumour, including a continuity resection of the mandible, and a unilateral modified radical neck dissection. The continuity of the mandible was restored with a free vascularized fibular transplant. Simultaneously four implants were inserted in the ventral part of the mandible. After six weeks the patient was subjected to a fractionated radiotherapy schedule up to a cumulative dose of 70 Gy. 2A. Orthopantomogram showing the situation before ablative surgery. The tumour did not invade the mandibular bone. 2B. Orthopantomogram 2 years after ablative surgery. The continuity of the mandible was restored with a fibular transplant. The four implants were inserted per ablationem. 2C. Clinical view showing the implants and suprastructure. Implant-surgery in a due to radiotherapy compromised area is avoided thus reducing the risk of late complications, such as development of osteoradionecrosis; A prerequisite of successful implant placement and prosthetic rehabilitation is proper handling of the soft tissues. Tension free closure of the surgical defect, either by primary closure or vascularised (free) flaps, has to be achieved to minimise the risk on development of dehiscence of bone near the implants (Haughey et al. 1994). A dehiscence may lead to improper implant healing and even to loss of the implants (Esser & Wagner 1997). Attention has also to be paid to mobility of the oral tissues to warrant proper functioning as impeded mobility of the oral tissues compromises the function of even the best prosthetic rehabilitation (Urken et al. 1991b). A major disadvantage of immediate implant insertion concerns the risk of improper implant positioning when ablative surgery will result in gross alterations in the anatomical situation and/or intermaxillary relationship, e.g. after mandibular continuity resections. Improperly positioned implants impair the prosthodontic treatment and can sometimes even not be used in the prosthodontic rehabilitation of a patient (Martin et al. 20
8 1994; Sclaroff et al. 1994; Schmelzeisen et al. 1996; Roumanas et al. 1997; Gürlek et al. 1998; Werkmeister et al. 1999). As a rule it is better to refrain from implantation during ablative surgery when proper positioning is doubted. Other disadvantages include the risk of interference with or delay of the oncological therapy, including radiation therapy, and the development of post-treatment complications caused by the implantation during ablative surgery (Sclaroff et al. 1994). These disadvantages are assessed to be of minor importance, especially when compared to the high risk on harmful tissue reactions to be encountered in case of implantation after radiotherapy (Granstrom et al. 1994). In addition, a twostage technique is advocated to minimise the risk on early post ablative complications as then the implants are covered by mucosa during radiation therapy (Granstrom et al. 1993b). Finally, by using multiple radiation fields backscatter doses can be minimised and are of minor concern (Mian et al. 1987; Wang et al. 1998). The last disadvantage of implantation during ablative surgery to be mentioned is the risk that inserted implants will not be used due to early tumour recurrence. This disadvantage is of minor importance because of the low morbidity of implant treatment in the lower jaw. Therefore, if there is a fair chance that these patients may benefit from an improved quality of life related to an implant supported prosthesis, it is recommended to also consider this procedure in advanced tumour cases that will be treated with curative intent. Number of implants and healing time According to the literature in patients with malignancies involving the lower region of the oral cavity a minimum of four implants is needed to achieve maximal implant support for the prosthesis and to relieve the vulnerable underlying soft-tissues, especially after radiotherapy (Weischer et al. 1996; Roumanas et al. 1997). Like in non-oncological cases, in non-irradiated head and neck cancer patients abutment connection can be performed after 3 months. If the patient has received irradiation in the implant region it is advised to wait 6 months after the implant placement before the abutment connection (Esser & Wagner 1997; Jisander et al. 1997; Larsen 1997). This way the implants are given some extra time for osseointegration and the early soft-tissue radiation effects will be resolved at the time of abutment connection (Hayter & Cawood 1996). It is questionable, however, whether the implants need this extra time since most of the osseointegration has taken place before the start of radiotherapy (Sclaroff et al. 1994; Marx & Morales 1998; Raghoebar et al. 2003b). The optimal head and neck oncology treatment related healing time of implants before loading is still in need of further research. By contrast, there is consensus that prosthodontic rehabilitation can start two weeks after abutment connection. 2 21
9 Placement of implants after ablative tumour surgery Post ablative treatment planning Edentulous patients who have completed their oncological treatment for oral cancer often experience great trouble with prosthodontic rehabilitation (Watzinger et al. 1996; Esser & Wagner 1997). Problems often encountered are an impaired function of the tongue, change in volume of the tongue, and lack of motor and sensory innervation (Urken et al. 1991b; Jacob et al. 1992; Zlotolow et al. 1992). The decreased mobility of the oral tissues may give rise to problems with food control and transportation during chewing and swallowing and cause decreased intelligibility of speech. These problems are worsened if the sensibility in the defect region is lost too (Schmelzeisen et al. 1996). An increase of the vertical dimension by introduction of a mandibular prosthesis even might lead to more severe complaints, because the tongue might have lost its ability to get in contact with the palate (Martin et al. 1994). This may impair speech and swallowing. Also control of the foodbolus by the tongue during chewing is restricted (Jacob et al. 1992; Zlotolow et al. 1992; Martin et al. 1994). Therefore some patients do not wear their mandibular prosthesis during eating as they experience eating without prosthesis less troublesome. It has been reported that these problems can be solved to some extent by lowering of the palatal contour of the maxillary prosthesis (Martin et al. 1994). To improve the mobility of the tongue a surgical release procedure (Steinhauser) can be considered (Kwakman et al. 1997b), but especially in the irradiated patient, the vascularity of flaps should not be jeopardised. Furthermore, due to reconstruction with bulky flaps as well as primary closure of defects the neutral zone can be severely compromised (Reintsema et al. 1998; Chandu et al. 2002). Many patients suffer from a reduced salivary secretion after irradiation, resulting in difficulties with amongst others chewing, swallowing and speech (Vissink et al. 2003a; Vissink et al. 2003b). The vulnerability of the atrophic oral mucosa, another effect of irradiation, is enhanced by the absence of the protective layer of saliva. Prosthetic loading of this atrophic mucosa is often not well tolerated, especially when the mandibular prosthesis is not stable (Hotz 1996; Wei et al. 1997; Marx & Morales 1998; Chiapasco 1999). Considerations regarding placement of implants after ablative surgery From the literature, it can be derived that implantretained mandibular overdentures can strongly reduce the problems with stability and retention of a denture and relief the underlying soft tissues, particularly if the occlusal load is beared by the implants (Roumanas et al. 1997; Weischer & Mohr 2001; Raghoebar et al. 2000). As in the non-oncological 22
10 patient, the bone in the interforaminal area of the mandible is available for implant insertion, as is the bone above the alveolar nerve in the posterior mandible when minimal resorption of the alveolar bone has occurred (Marker et al. 1997; Visch et al. 2002). If due to the ablative procedure (e.g. partial mandibulectomy) the alveolar bone has been denervated, the whole height of the remaining part of the mandible on the affected site can be used for implant placement (Keller et al. 1997a). Also, bone transplanted to restore mandibular continuity can be used for implant restoration (Fig. 3) (Urken et al. 1991b; Marx et al. 1996; Keller et al. 1997a; Marker et al. 1997). Patients who underwent a partial mandibulectomy without bony reconstruction might need a secondary reconstruction before implantation in the defect site can be considered to be a proper option (Keller et al. 1997a; Misiek & Chang 1998). In some cases, the soft tissues have been surgically reconstructed and continuity has been re-established with a reconstruction plate or a bone graft with an insufficient volume (e.g. costal grafts) for reliable implant placement. Another often encountered problem in these patients is the lack of soft tissues and scar formation in the area needed to cover a bone graft. This lack of soft tissues bears the increased risk of wound dehiscence following reconstruction and thus the increased risk on loss of grafted bone (Marx et al. 1996; Watzinger et al. 1996). In patients not treated with radiotherapy in the area A B C D Fig. 3. A 64 years old female with a T4N0 squamous cell carcinoma of the mandibular gingiva. The patient was treated with wide local excision of the tumour, including a continuity resection of the mandible, and bilateral supra-omohyoid neck dissection. The continuity of the mandible was restored with a free vascularized fibular transplant. Six weeks after the ablative procedure the patient received fractionated radiotherapy up to a cumulative dose of 60 Gy. After three years five implants were inserted in the neo-mandible (fibula). This procedure was performed using antibiotic prophylaxis, but without HBO. Shortly after abutment connection two implants were lost. 3A. Orthopantomogram before ablative surgery. Osteolysis of mandibular bone in the symphyseal region is clearly visible. 3B. Orthopantomogram three years after ablative surgery. The continuity of the mandible was restored with a fibular transplant. 3C. Orthopantomogram 1.5 years after insertion of the implants showing the three remaining implants and the suprastructure. 3D. Clinical view showing the implants and suprastructure. 2 23
11 to be reconstructed, free bone grafts, e.g. from the iliac crest, have been shown to be a good option. In irradiated patients, however, free grafts have to be avoided because of the risk of development of osteoradionecrosis (Barber et al. 1995; Marx et al. 1996). In these patients vascularised free flaps (fibula, scapula or ilium) or a Marx procedure (free bone graft in a crib with pre- and postoperative HBO) have to be considered (Urken et al. 1991b; Martin et al. 1992; Haughey et al. 1994; Moscoso et al. 1994; Barber et al. 1995; Marx et al. 1996; Navarro-Vila et al. 1996). The bulky volume of vascularised (free) flaps not uncommonly interferes with functioning of an (implantretained) overdenture. Therefore, there is often a need for correction of grafted tissues during implant insertion or abutment connection. After any form of re-establishment of continuity of the mandible, fabrication of a prosthetic set-up followed by a surgical template is recommended for planning of the proper location and angulation of the implants (Martin et al. 1994; Chan et al. 1997; Roumanas et al. 1997; Marx & Morales 1998). Improperly positioned or angulated implants impair the prosthodontic treatment and can sometimes even not be used in the prosthodontic rehabilitation of such a patient (Schmelzeisen et al. 1996; Roumanas et al. 1997). The presence of oral mucosa surrounding the implants is preferred to skin(grafts), because more problems of peri-implant skin tissue are encountered in comparison to mucosal tissue, both during healing and after abutment connec- tion (Taylor & Worthington 1993; Marx 1994; Chan et al. 1997; Kovacs 1998; Chiapasco 1999). Occasionally the free mucosa or skin present around the implants is replaced by palatal mucosal grafts (Martin et al. 1992; Beumer III et al. 1995; Ali et al. 1997; Chan et al. 1997; Wei et al. 1997). When two-stage implants are used a second operative procedure in irradiated tissue is necessary. The use of oral implants in irradiated tissue is not considered to be contra-indicated, although it has been reported that the risk on implant failure is increased with losses up to 35% (mean 13,6%, range 0-36%) (Albrektsson 1988; Buchbinder et al. 1989; Urken et al. 1991b; Granstrom et al. 1993a; Taylor & Worthington 1993; Ueda et al. 1993; Barber et al. 1995; Franzen et al. 1995; Eckert et al. 1996; Watzinger et al. 1996; Ali et al. 1997; Arcuri et al. 1997; Chan et al. 1997; Esser & Wagner 1997; Jisander et al. 1997; Keller et al. 1997a; Marker et al. 1997; McGhee et al. 1997; Andersson 1998; Brogniez et al. 1998; Marx & Morales 1998; Niimi et al. 1998; Betz et al. 1999; Mericske-Stern 1999; Weischer & Mohr 1999; Werkmeister et al. 1999; Goto et al. 2002; Schultes et al. 2002; Visch et al. 2002). In non-irradiated mandibles the implant survival rate is, in most studies, at least 90% (mean 96,1%, range 74,8-100%) (Batenburg et al. 1998a; Kovacs 2000). Handling of irradiated tissues General agreement exists about the obligatory use of a gentle surgical technique with minimal reflection of periosteum and the use of peri-operative 24
12 antibiotics to prevent wound healing disturbances (Granstrom et al. 1992a; Taylor & Worthington 1993; Larsen 1997). Additional measures to prevent implant loss or development of osteoradionecrosis, such as a pretreatment with HBO, have to be considered. HBO treatment claims to permanently improve the vascularisation of the bone and is assumed to have a positive effect on osseointegration of the implants (Granstrom 1992b; Granstrom et al. 1993a; Johnsson et al. 1999). Preferably one-stage implants are used, thus avoiding the need of a second surgical procedure (abutment connection) and a second period of HBO. The negative effects of radiation on osseointegration have been reported to depend on the location of implants, and the dose and fractionation of radiotherapy (Granstrom et al. 1992a; Jisander et al. 1997; Esposito et al. 1998). In general, doses over 40 to 50 Gy are thought to significantly impair the healing capacity of the bone with an inherent increase of the risk on complications when performing surgery (Aitasalo 1986; Beumer III 1995). Therefore, for implant placement after radiation therapy at intraoral sites being treated with total doses exceeding 50 Gy, the use of HBO for prevention of late complications has to be taken in consideration (Taylor & Worthington 1993; Beumer III 1995; Jisander et al. 1997; Chiapasco 1999). The real value and necessity of the HBO treatment in such cases still has to be proven in prospective clinical studies, however (Keller 1997b; Andersson et al. 1998; Coulthard et al. 2002). Timing of the implantation procedure with regard to the effects of irradiation on jawbone remains inconclusive. There are reports about an improvement in the bone healing capacity over a 12-months period following irradiation (Jacobsson et al. 1985), while others report a continuously progressive loss of capillaries in the mandible following irradiation (Marx & Johnson 1987). In agreement with the study of Marx is the study of Granström reporting the longer the period between irradiation and implantation the higher the risk on implant loss (Granstrom et al. 1994). Latter authors recommend implant insertion in a so called window between 1 to 6 months after radiation therapy (Marx & Johnson 1987; Granstrom et al. 1994). In this period the early radiation effects are resolved and long-term vascular changes associated with cancericidal radiation treatment may not have taken place. Also the bone is still relatively well vascularised. Number of implants and healing time In irradiated patients a minimum of four implants is recommended. These implants should be placed in optimally spaced locations for the best possible spread of occlusal loading (Martin et al. 1994; Weischer et al. 1996). When no radiotherapy is applied and lack of stabilisation of the mandibular prosthesis is the only problem encountered an implant-mucosal borne prosthesis, i.e. a mandibular overdenture supported by two implants, can be sufficient to restore function (Batenburg et al. 2 25
13 Fig a). After implant placement in irradiated sites in the mandible it generally is advised to wait 4-6 months before the abutment connection to allow the implants for some extra time for osseointegration (Taylor & Worthington 1993; Esser & Wagner 1997; Jisander et al. 1997; Larsen 1997; Marker et al. 1997; Marx & Morales 1998; Wagner et al. 1998). Pre-Surgical Evaluation (Expected) Prosthetic Problems Implant Surgery per Ablationem Radiotherapy No Radiotherapy 6 Months 3 Months Abutment Connection Abutment Connection Decision-making process for implant insertion in the mandible per ablationem. Proposed treatment regimen As described in the previous paragraphs, in edentulous patients the loss of hard and soft tissues after ablative surgery of tumours of the mandible, tongue or floor of the mouth might create severe problems in oral functioning. These problems often cannot be restored with conventional surgical or prosthodontic techniques. Radiation therapy worsens this situation and makes rehabilitation even more difficult. Implantology offers the opportunity to improve the oral rehabilitation of these patients by stabilisation of the prosthesis. An implant-supported prosthetic construction diminishes pain and may thus enhance the ability to regain essential functions such as speech, chewing and swallowing. Part of the compromised oral functioning is not prosthesis driven, however, but related to other effects of the cancer treatment including a lack of motor and sensory innervation of the oral tissues and hyposalivation. Therefore, a thorough consideration of the possible advantages and disadvantages is essential in the preoperative stage. For optimal treatment planning both maxillofacial prosthodontists and implant surgeons should be members of the multidisciplinary head and neck oncology team. Nowadays the application of implants is considered for all edentulous patients with a malignancy in the lower region of the oral cavity (Fig. 4). It is an integral part of the 26
14 care for the head and neck oncology patient. If post-operative radiation therapy might be part of the treatment plan, implants are inserted during ablative surgery if possible. Only if the oncological resection includes more than half of the symphyseal region no implants are inserted because of the grossly altered anatomical situation and intermaxillary relationship. This may lead to improper positioning and angulation of the implants in the reconstructed bone. In these cases, for the goal of secondary implant insertion and maximum chances for rehabilitation of function, the continuity of the mandible should be restored immediately, preferably with vascularised bone of sufficient quantity to insert implants in a later stage. In case of implant placement after fractionated radiotherapy with cumulative doses exceeding 40 to 50 Gy the application of HBO treatment before implant insertion must be considered for prevention of late complications, such as the development of osteoradionecrosis (Fig. 5). With regard to timing of the implant insertion after radiotherapy no evidence-based recommendations can be given due to lack of scientific evidence. Since most recurrences of oral malignancies manifest itself within one year after initial oncological treatment it may be prudent to wait at least one year with secondary implant placement. Evaluation if the Patient can benefit from Dental Implants Evaluation of Soft and Hard Tissues Implant Insertion with Antibiotic Prophylaxis either with or without HBO 6 Months Abutment Connection Correction and/or Reconstruction Soft/Hard Tissues 3-4 Months 2 Fig. 5. Decision-making process for insertion of implants in the mandible after radiotherapy. 27
15 Epilogue This review shows that there are still shortcomings in scientific evidence about the timing of implant insertion with regard to radiation therapy and about the indications and potential benefit of preventive HBO therapy. Future research should address these issues. There is a strong tendency towards implant insertion during ablative surgery in order to prevent surgery in irradiated tissue and to shorten the time for functional rehabilitation of the head and neck cancer patient. Implant placement during ablative surgery is doubted in case of loss of continuity of the mandible, even if the continuity of the mandible is restored with a bone transplant. As a rule it is better to refrain from implant placement during ablative surgery when proper positioning is doubted. One has to keep in mind that an implant-supported prosthesis is not a guarantee for uncompromised oral function post treatment, but it is considered a significant factor contributing to the well being of these patients. 28
16 29 2
17 30
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
Chapter 6. Pieter J Schoen Gerry M Raghoebar Jelte Bouma Harry Reintsema Arjan Vissink Wouter Sterk Jan LN Roodenburg
 Rehabilitation of Oral Function in Head and Neck Cancer Patients after Radiotherapy with Implant-Retained Dentures: Effects of Hyperbaric Oxygen Therapy Pieter J Schoen Gerry Raghoebar Jelte Bouma Harry
Rehabilitation of Oral Function in Head and Neck Cancer Patients after Radiotherapy with Implant-Retained Dentures: Effects of Hyperbaric Oxygen Therapy Pieter J Schoen Gerry Raghoebar Jelte Bouma Harry
P.J. Schoen *, H. Reintsema, G.M. Raghoebar, A. Vissink, J.L.N. Roodenburg. Review
 Oral Oncology (2004) 40 862 871 http://intl.elsevierhealth.com/journals/oron/ Review The use of implant retained mandibular prostheses in the oral rehabilitation of head and neck cancer patients. A review
Oral Oncology (2004) 40 862 871 http://intl.elsevierhealth.com/journals/oron/ Review The use of implant retained mandibular prostheses in the oral rehabilitation of head and neck cancer patients. A review
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness
 TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
Surgical treatment of malignancies involving the
 Oral Implants in Radiated Patients: A Systematic Review Giuseppe Colella, MD, DDS 1 /Rosangela Cannavale, DDS 2 /Monica Pentenero, DDS, MSc 3 / Sergio Gandolfo, MD, DDS 4 Purpose: Oral malignancy is often
Oral Implants in Radiated Patients: A Systematic Review Giuseppe Colella, MD, DDS 1 /Rosangela Cannavale, DDS 2 /Monica Pentenero, DDS, MSc 3 / Sergio Gandolfo, MD, DDS 4 Purpose: Oral malignancy is often
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
In Scandinavia, malignant tumors in the maxillofacial
 Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery
 Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery Pieter J Schoen Gerry M Raghoebar Robert P van Oort Harry Reintsema Bernard FAM van der Laan Fred R Burlage Jan LN Roodenburg
Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery Pieter J Schoen Gerry M Raghoebar Robert P van Oort Harry Reintsema Bernard FAM van der Laan Fred R Burlage Jan LN Roodenburg
Citation for published version (APA): Schortinghuis, J. (2004). Ultrasound stimulation of mandibular bone defect healing s.n.
 University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Ultrasound stimulation of mandibular bone defect healing Schortinghuis, Jurjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
PROSTHETICREHABILITATION OFAHEMIMANDIBULECTOMY PATIENTWITHTWINOCCLUSION
 CASEREPORT PROSTHETICREHABILITATION OFAHEMIMANDIBULECTOMY PATIENTWITHTWINOCCLUSION Authors: Tejeswar Reddy B¹ Indira Padmaja B² Raja Reddy N³ 1 Post graduate, 2 Professor & HOD, 3 Reader, Address for correspondence:
CASEREPORT PROSTHETICREHABILITATION OFAHEMIMANDIBULECTOMY PATIENTWITHTWINOCCLUSION Authors: Tejeswar Reddy B¹ Indira Padmaja B² Raja Reddy N³ 1 Post graduate, 2 Professor & HOD, 3 Reader, Address for correspondence:
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
Maxillofacial prosthetics is a subspecialty of
 Invited Article Maxillofacial Prosthesis: A Review of Treatment Concepts for Better Prosthesis Prognosis Sanjay Prasad 1 ABSTRACT Maxillofacial prosthesis currently finds itself experiencing more change
Invited Article Maxillofacial Prosthesis: A Review of Treatment Concepts for Better Prosthesis Prognosis Sanjay Prasad 1 ABSTRACT Maxillofacial prosthesis currently finds itself experiencing more change
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report
 case report 10.5005/jp-journals-10031-1067 Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report 1 Ragini Sudhakar Sanaye, 2 Sabita M Ram, 3 Naisargi Shah, 4
case report 10.5005/jp-journals-10031-1067 Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report 1 Ragini Sudhakar Sanaye, 2 Sabita M Ram, 3 Naisargi Shah, 4
University of Groningen. Morbidity after neck dissection in head and neck cancer patients Wilgen, Cornelis Paul van
 University of Groningen Morbidity after neck dissection in head and neck cancer patients Wilgen, Cornelis Paul van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Morbidity after neck dissection in head and neck cancer patients Wilgen, Cornelis Paul van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
ISSN: Volume 4 Issue Faciomaxillary prosthesis in rehabilitation. After maxillectomy. A clinical study
 ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework
 Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
IMMEDIATE PARTIAL DENTURE PROSTHESIS - A CASE REPORT
 Case Report IMMEDIATE PARTIAL DENTURE PROSTHESIS - A CASE REPORT Abstract : 2 Vinaya Bhat & S. Sriram Balaji 2 Professor, P.G. Student, Department of Prosthodontics and Implantology, A.B. Shetty Memorial
Case Report IMMEDIATE PARTIAL DENTURE PROSTHESIS - A CASE REPORT Abstract : 2 Vinaya Bhat & S. Sriram Balaji 2 Professor, P.G. Student, Department of Prosthodontics and Implantology, A.B. Shetty Memorial
WILLIAM B. BOHANNAN DDS, MD PROFESSIONAL CORPORATION
 7.12.18 WILLIAM B. BOHANNAN DDS, MD RE: Samuel Bower Site #6 To whom it may concern: Mr. Bower and his parents wish to seek additionally opinions for site #6. They are trying to decide if further surgery
7.12.18 WILLIAM B. BOHANNAN DDS, MD RE: Samuel Bower Site #6 To whom it may concern: Mr. Bower and his parents wish to seek additionally opinions for site #6. They are trying to decide if further surgery
Cancer of the Oral Cavity
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Survey of Laryngeal Cancer at SBUH comparing 108 cases seen here from to the NCDB of 9,256 cases diagnosed nationwide in 2000
 Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY
 RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
RICHARD J. SORBERA, D.D.S. SHIBLY D. MALOUF, D.D.S., INC. DIPLOMATES AMERICAN BOARD OF ORAL AND MAXILLOFACIAL SURGERY INFORMATION AND CONSENT FOR IMPLANT SURGERY PURPOSE OF THIS FORM: State law requires
Locator retained mandibular complete prosthesis (isy Implant System)
 Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
Locator retained mandibular complete prosthesis (isy Implant System) Mucosa-supported complete prostheses with poor fit greatly reduce people's quality of life. This is why the importance of implant-supported
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Oral functional outcome after intraoral reconstruction with nasolabial flaps
 The British Association of Plastic Surgeons (2004) 57, 150 155 Oral functional outcome after intraoral reconstruction with nasolabial flaps E.I. Hofstra a, S.O.P. Hofer b, *, J.M. Nauta c, J.L.N. Roodenburg
The British Association of Plastic Surgeons (2004) 57, 150 155 Oral functional outcome after intraoral reconstruction with nasolabial flaps E.I. Hofstra a, S.O.P. Hofer b, *, J.M. Nauta c, J.L.N. Roodenburg
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Review article: Rehabilitation of glossectomy patient: Review
 Review article: Rehabilitation of glossectomy patient: Review Dr. Gunjan Gupta, Dr. Sunil Dhaded, Dr. Shalini B.N. A.M.E`S Dental College, Dept. of Prosthodontics, Raichur. India Corresponding author -
Review article: Rehabilitation of glossectomy patient: Review Dr. Gunjan Gupta, Dr. Sunil Dhaded, Dr. Shalini B.N. A.M.E`S Dental College, Dept. of Prosthodontics, Raichur. India Corresponding author -
Devoted to the Advancement of Implant Dentistry
 Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Contents Graduate Diploma of Dental Implantology
 Graduate Diploma of Dental Implantology Information Brochure Contents Graduate Diploma of Dental Implantology DOH 551 Introduction to Dental Implants and Basic Restorative Implantology Module 1 Fundamentals
Graduate Diploma of Dental Implantology Information Brochure Contents Graduate Diploma of Dental Implantology DOH 551 Introduction to Dental Implants and Basic Restorative Implantology Module 1 Fundamentals
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
ACRYLIC REMOVABLE PARTIAL DENTURE(RPD)
 ACRYLIC REMOVABLE PARTIAL DENTURE(RPD) is a dental prosthesis which artificially supplies teeth and associated structure in a partially edentulous arch, made from acrylic resin and can be inserted and
ACRYLIC REMOVABLE PARTIAL DENTURE(RPD) is a dental prosthesis which artificially supplies teeth and associated structure in a partially edentulous arch, made from acrylic resin and can be inserted and
Ninety percent of oral cancers are epidermoid
 Dental Prosthetic Reconstruction of Osseointegrated Implants Placed in Irradiated Bone Véronique Brogniez*/Patrice Lejuste**/Alain Pecheur***/Hervé Reychler**** Nineteen patients who were treated for oncologic
Dental Prosthetic Reconstruction of Osseointegrated Implants Placed in Irradiated Bone Véronique Brogniez*/Patrice Lejuste**/Alain Pecheur***/Hervé Reychler**** Nineteen patients who were treated for oncologic
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
World Journal of Pharmaceutical and Life Sciences WJPLS
 INTRODUCTION Awareness over the years in Dental Implants has increased. Research on newer materials and invention of newer techniques has certainly widened the scope of dental implants. However there are
INTRODUCTION Awareness over the years in Dental Implants has increased. Research on newer materials and invention of newer techniques has certainly widened the scope of dental implants. However there are
Pre prosthetic surgery
 Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
University of Groningen. Fracture of the distal radius Oskam, Jacob
 University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Fracture of the distal radius Oskam, Jacob IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
University of Groningen. Colorectal Anastomoses Bakker, Ilsalien
 University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
CLASSIFICATIONS. Established in 1994 as a subcommittee of the. Prosthodontic Care Committee
 CLASSIFICATIONS Established in 1994 as a subcommittee of the Prosthodontic Care Committee Committee Members Thomas J. McGarry, DDS, Chair Arthur Nimmo, DDS James F. Skiba, DDS Christopher R. Smith, DDS
CLASSIFICATIONS Established in 1994 as a subcommittee of the Prosthodontic Care Committee Committee Members Thomas J. McGarry, DDS, Chair Arthur Nimmo, DDS James F. Skiba, DDS Christopher R. Smith, DDS
Citation for published version (APA): Weert, E. V. (2007). Cancer rehabilitation: effects and mechanisms s.n.
 University of Groningen Cancer rehabilitation Weert, Ellen van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Cancer rehabilitation Weert, Ellen van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
An Introduction to Dental Implants
 An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
Reconstruction with fibular osteocutaneous free flap in patients with mandibular osteoradionecrosis
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
EVERYONE I M P L A N T C O M P A N Y
 A SMILE FOR EVERYONE I M P L A N T C O M P A N Y WHAT IS AN IMPLANT? A dental implant is an effective alternative to the root of a tooth. It consists of a titanium screw only a few millimetres in size.
A SMILE FOR EVERYONE I M P L A N T C O M P A N Y WHAT IS AN IMPLANT? A dental implant is an effective alternative to the root of a tooth. It consists of a titanium screw only a few millimetres in size.
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.
 This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
ARTICLE IN PRESS. Available online at British Journal of Oral and Maxillofacial Surgery xxx (2011) xxx xxx
 Available online at www.sciencedirect.com British Journal of Oral and Maxillofacial Surgery xxx (2011) xxx xxx Computed tomography-guided implant surgery for dental rehabilitation in mandible reconstructed
Available online at www.sciencedirect.com British Journal of Oral and Maxillofacial Surgery xxx (2011) xxx xxx Computed tomography-guided implant surgery for dental rehabilitation in mandible reconstructed
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT
 Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT About Implants 01. What if a tooth is lost and the toothless area is left alone? 02. Do you want to restore the confidence in your appearance? 03.
Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT About Implants 01. What if a tooth is lost and the toothless area is left alone? 02. Do you want to restore the confidence in your appearance? 03.
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Prosthodontic Surgery Interactions in Head and Neck Cancer Patients Tailored for Surgeons
 LECTURE AND COURSE PROGRAM Prosthodontic Surgery Interactions in Head and Neck Cancer Patients Tailored for Surgeons Wednesday, September 5 th, 2018 Clinic for Maxillofacial Surgery, 8 Dr Subotica Street
LECTURE AND COURSE PROGRAM Prosthodontic Surgery Interactions in Head and Neck Cancer Patients Tailored for Surgeons Wednesday, September 5 th, 2018 Clinic for Maxillofacial Surgery, 8 Dr Subotica Street
Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases
 Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases Mehmet Kürkcü, DDS, MSc, PhD, a Mehmet Emre Benlidayı, DDS, b Cem Kurtoğlu, DDS, PhD, c and
Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases Mehmet Kürkcü, DDS, MSc, PhD, a Mehmet Emre Benlidayı, DDS, b Cem Kurtoğlu, DDS, PhD, c and
Survival of dental implants in patients with oral cancer treated by surgery and radiotherapy: a retrospective study
 Pompa et al. BMC Oral Health 2015, 15:5 RESEARCH ARTICLE Open Access Survival of dental implants in patients with oral cancer treated by surgery and radiotherapy: a retrospective study Giorgio Pompa, Matteo
Pompa et al. BMC Oral Health 2015, 15:5 RESEARCH ARTICLE Open Access Survival of dental implants in patients with oral cancer treated by surgery and radiotherapy: a retrospective study Giorgio Pompa, Matteo
Mandibular ridge changes after adaptation. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss
 (Journal of Dental Outlook, Vol.110, Vol.6:1021~1027, Japan 2007. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss Dr. Jiro Abe Abe Dental Clinic
(Journal of Dental Outlook, Vol.110, Vol.6:1021~1027, Japan 2007. An issue of shortened dental arch to be considered from changes of soft tissues after unattended tooth loss Dr. Jiro Abe Abe Dental Clinic
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Safety and esthetics with
 Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
Nagri D et al. Linear occlusion and Neutral Zone recording for severely resorbed ridges
 Doi:10.21276/ledent.2018.02.01.02 Case Report LINEAR OCCLUSION AND NEUTRAL ZONE RECORDING USING TISSUE CONDITIONER REPORT OF A SEVERELY RESORBED RIDGE Divya Nagri, 1Ashish Kakkar, 2Neeraj Mittal, 3Lovely
Doi:10.21276/ledent.2018.02.01.02 Case Report LINEAR OCCLUSION AND NEUTRAL ZONE RECORDING USING TISSUE CONDITIONER REPORT OF A SEVERELY RESORBED RIDGE Divya Nagri, 1Ashish Kakkar, 2Neeraj Mittal, 3Lovely
REMOVABLE PROSTHODONTICS
 REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
Laser Assembled and CAD/CAM Prosthetic Frameworks for the Debilitated Mandible. Robert Schneider, DDS, MS
 Laser Assembled and CAD/CAM Prosthetic Frameworks for the Debilitated Mandible Robert Schneider, DDS, MS University of Iowa Hospitals and Clinics Hospital Dentistry Institute Division of Maxillofacial
Laser Assembled and CAD/CAM Prosthetic Frameworks for the Debilitated Mandible Robert Schneider, DDS, MS University of Iowa Hospitals and Clinics Hospital Dentistry Institute Division of Maxillofacial
Viability of dental implants in head and neck irradiated patients: A systematic review
 CLINICAL REVIEW David W. Eisele, MD, Section Editor Viability of dental implants in head and neck irradiated patients: A systematic review Edson Virgılio Zen Filho, DDS, MSc, 1 Elen de Souza Tolentino,
CLINICAL REVIEW David W. Eisele, MD, Section Editor Viability of dental implants in head and neck irradiated patients: A systematic review Edson Virgılio Zen Filho, DDS, MSc, 1 Elen de Souza Tolentino,
DOCTORAL DISSERTATION. A Clinical and Radiolagical-Imaging Correlative Study in. the Evaluation of Dental-Implants-Based Prosthetic Restorations
 DOCTORAL DISSERTATION A Clinical and Radiolagical-Imaging Correlative Study in the Evaluation of Dental-Implants-Based Prosthetic Restorations Doctoral candidate Ioan Sebastian Cernuşcă-Miţariu CONTENTS
DOCTORAL DISSERTATION A Clinical and Radiolagical-Imaging Correlative Study in the Evaluation of Dental-Implants-Based Prosthetic Restorations Doctoral candidate Ioan Sebastian Cernuşcă-Miţariu CONTENTS
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
University of Groningen. Immediate dental implant placement in the aesthetic zone Slagter, Kirsten
 University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Immediate dental implant placement in the aesthetic zone Slagter, Kirsten IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Lia Kosmidou, DDS, MS*/Joseph A. Toljanic, DDS**/ William J. Moran, DMD, MD, FACS***/William R. Panje, MD, FACS****
 The Use of Percutaneous Implants for the Prosthetic Rehabilitation of Orbital Defects in Irradiated Cancer Patients: A Report of Clinical Outcomes and Complications Lia Kosmidou, DDS, MS*/Joseph A. Toljanic,
The Use of Percutaneous Implants for the Prosthetic Rehabilitation of Orbital Defects in Irradiated Cancer Patients: A Report of Clinical Outcomes and Complications Lia Kosmidou, DDS, MS*/Joseph A. Toljanic,
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Component parts of Chrome Cobalt Removable Partial Denture
 Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW
 MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
A Study of Classification Systems for Maxillectomy Defects
 A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery
 ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y
 A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
Management of malignant tumors
 CASE REPORT Rehabilitation of a Patient With Mandibular Resection Using Osteointegrated Implants: A Case Report Sema Murat, DDS, PhD* Ayhan Gurbuz, DDS, PhD Kivanc Kamburoglu, DDS, MSc, PhD This case report
CASE REPORT Rehabilitation of a Patient With Mandibular Resection Using Osteointegrated Implants: A Case Report Sema Murat, DDS, PhD* Ayhan Gurbuz, DDS, PhD Kivanc Kamburoglu, DDS, MSc, PhD This case report
ISPUB.COM. Habitual Centric: A Case Report. Manisha, N Kathuria, A Gupta, N Gupta INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
ISPUB.COM The Internet Journal of Geriatrics and Gerontology Volume 6 Number 2 Habitual Centric: A Case Report Manisha, N Kathuria, A Gupta, N Gupta Citation Manisha, N Kathuria, A Gupta, N Gupta. Habitual
Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete Denture and Mandibular Teeth supported Overdenture
 Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Prosthetic Rehabilitation of Maxillectomy Defects- Clinical Outcomes
 Prosthetic Rehabilitation of Maxillectomy Defects- Clinical Outcomes Eleni D. Roumanas DDS Division of Advanced Prosthodontics and Weintraub Center for Reconstructive Biotechnology UCLA School of Dentistry
Prosthetic Rehabilitation of Maxillectomy Defects- Clinical Outcomes Eleni D. Roumanas DDS Division of Advanced Prosthodontics and Weintraub Center for Reconstructive Biotechnology UCLA School of Dentistry
Prosthetic RehabilitationofaPatientwithAlzheimersDiseaseusingaCombinedBallBarandClipRetainedImplantSupportedOverdentureA Case Report
 Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Global Journal of Medical Research: J Dentistry & Otolaryngology Volume 17 Issue 2 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online
Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report
 Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
The removable implant supported prosthesis for the upper jaw
 Implant placement in the atrophied maxilla The removable implant supported Drs. Alan Rosenfeld and George Mandelaris Diplomates, American Board of Periodontology Initial Exam: Patient with ill fitting,
Implant placement in the atrophied maxilla The removable implant supported Drs. Alan Rosenfeld and George Mandelaris Diplomates, American Board of Periodontology Initial Exam: Patient with ill fitting,
Maryland AGD AE and Socket Grafting. Advanced Implant Mentoring Rob D Orazio, DDS. Day 1 Morning 1
 Page1 Page2 advancedimplantmentoring.com Page3 7:30am 8:00am Continental Breakfast & Registration 8:00am 9:30am Lecture- Effects of Tooth Loss on Bone -Site Preservation and Augmentation 9:30am 9:45am
Page1 Page2 advancedimplantmentoring.com Page3 7:30am 8:00am Continental Breakfast & Registration 8:00am 9:30am Lecture- Effects of Tooth Loss on Bone -Site Preservation and Augmentation 9:30am 9:45am
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT
 ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
University of Groningen. Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella
 University of Groningen Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Implant treatment for patients with severe hypodontia Filius, Marieke Adriana Pieternella IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Implant survival in patients with oral cancer: A 5-year follow-up
 Journal section: Oral Surgery Publication Types: Research doi:0.47/jced.5497 http://dx.doi.org/0.47/jced.5497 Implant survival in patients with oral cancer: A 5-year follow-up Rafael Flores-Ruiz, Lizett
Journal section: Oral Surgery Publication Types: Research doi:0.47/jced.5497 http://dx.doi.org/0.47/jced.5497 Implant survival in patients with oral cancer: A 5-year follow-up Rafael Flores-Ruiz, Lizett
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Prosthodontic Rehabilitation with Overdenture Using Modified Impression Technique: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
"Artless solution to resolve the problem of retention in resorbed alveolar ridge cases"
 Article ID: ISSN 2046-1690 "Artless solution to resolve the problem of retention in resorbed alveolar ridge cases" Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor,
Article ID: ISSN 2046-1690 "Artless solution to resolve the problem of retention in resorbed alveolar ridge cases" Peer review status: No Corresponding Author: Dr. Khurshid Mattoo, Assistant Professor,
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
